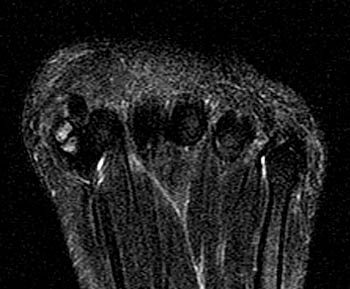
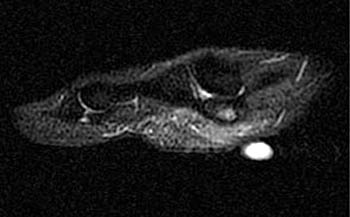
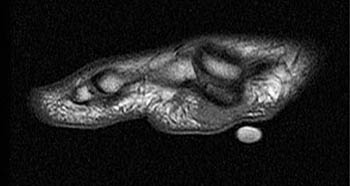
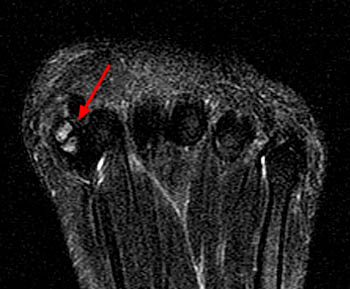
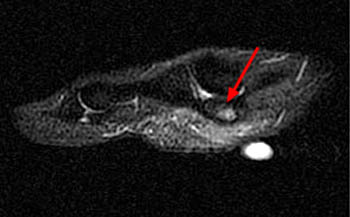
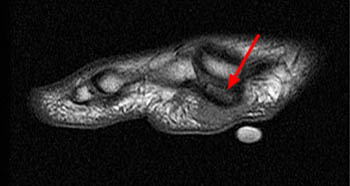
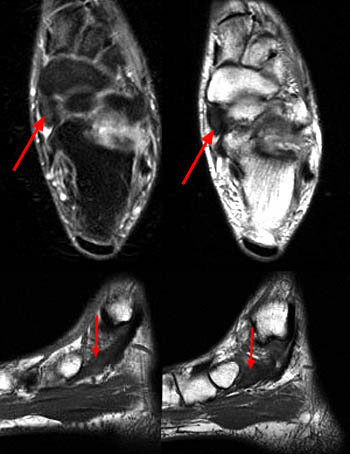
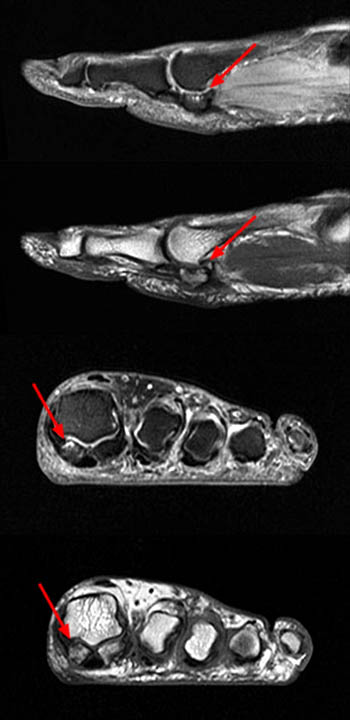
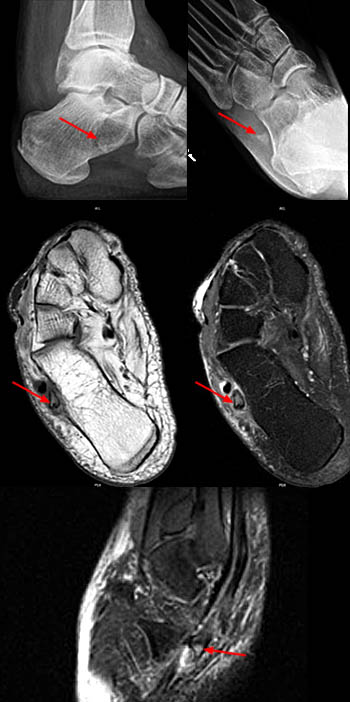
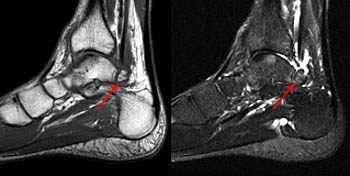
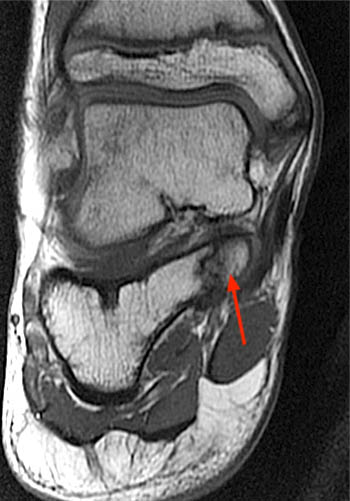
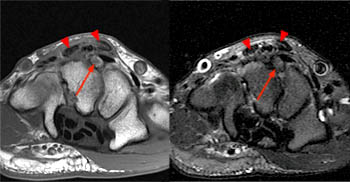
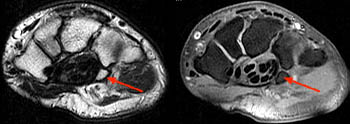
Clinical History: A 20-year-old female college tennis player presents with a long-standing history of intermittent, fluctuating pain at the plantar aspect of the first metatarsophalangeal joint, increasing over the past 3-4 months. A marker was placed over the region of pain. Axial T2-weighted fat-suppressed (1a), sagittal STIR (1b), and sagittal T1-weighted (1c) MR images are provided. What are the findings? What is your diagnosis?
Findings
Diagnosis: Sesamoiditis of the medial sesamoid of the first metatarsophalangeal joint.
Introduction
The term sesamoid is used for certain small nodular foci composed of bone, cartilage, or both that are shaped like a sesame seed1. Sesamoid bones are common in humans, and vary in number. As many as 42 sesamoid bones can be found within a single person2. The most common sesamoid bones are those of the foot, including the hallucal sesamoids, lesser metatarsal sesamoids, interphalangeal joint sesamoid of the great toe, os peroneum, sesamoid within the anterior tibial tendon, and sesamoid within the posterior tibial tendon; those of the hand, including the pollicis sesamoids, second and fifth metacarpal sesamoids, interphalangeal joint sesamoid of the thumb, and pisiform; as well as the patella and fabella. This web clinic will review sesamoid bones as well as accessory ossicles, with an emphasis on the MR imaging findings.
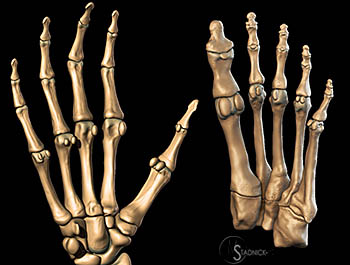
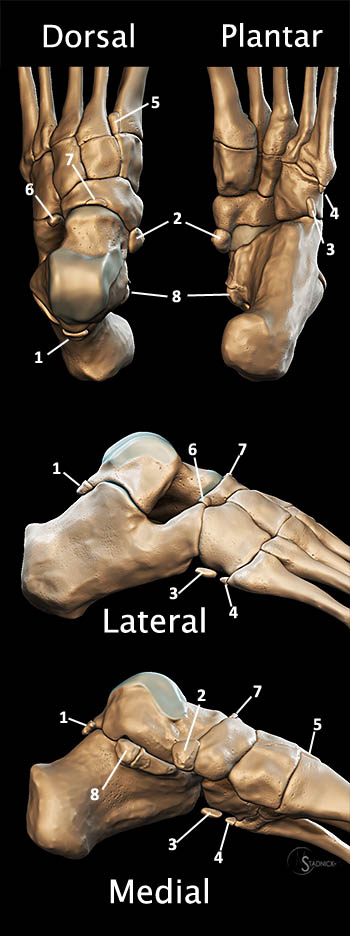
Figure 5:
3D graphics of the sesamoid distribution in the hand and foot. Sesamoids are most constantly present about the metacarpophalangeal joint and interphalangeal joint of the thumb, and the metatarsophalangeal joint and interphalangeal joint of the great toe. Inconstant sesamoids may be located about any metacarpophalangeal, metatarsophalangeal, or interphalangeal joint.
Anatomy and Function
Sesamoid bones are small round or ovoid bones embedded in certain tendons, usually related to joint surfaces3. Sesamoid bones not only protect tendons from damage, but also can increase the efficiency or mechanical advantage of their associated muscle. They accomplish this as part of a gliding mechanism by modifying pressure, decreasing friction, and altering muscle pull.
The sesamoid osseous surfaces are covered by cartilage and are intimate with a synovial-lined cavity4. There are two types of sesamoid bones, designated Type A and Type B5. In Type A, the sesamoid bone is located adjacent to an articulation, with its tendon incorporated into the joint capsule (i.e., patella and the hallucis and pollicis sesamoids). In Type B, the sesamoid is located at sites where tendons are angled about bony surfaces and separated from the underlying bone by a bursa (i.e., sesamoid of the peroneus longus tendon). Both types of sesamoid bones are closely associated with a synovial lining and articular cartilage, the key components of a synovial joint4.
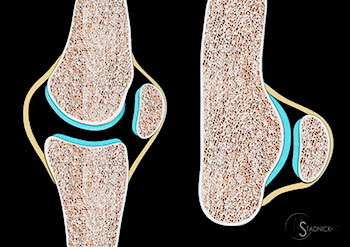
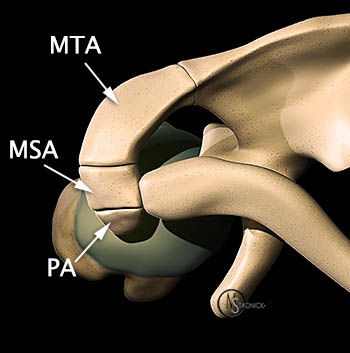
Figure 6:
Sesamoid anatomy4: Two types of sesamoid(s): Type A (left) in which the sesamoid is found adjacent to an articulation; Type B (right) in which a bursa separates the sesamoid from the adjacent bone. Both sesamoid types are closely associated with a synovial lining and articular cartilage (blue).
Fibrocartilaginous sesamoids also exist, specifically in tendons that wrap around bony or fibrous pulleys, such as within the peroneus longus tendon as it bends around the cuboid or within the posterior tibial tendon near the medial malleolus. The formation of fibrocartilage is an adaptation to help maintain tendon structure by resisting compression or shear6. The fibrous tissue provides flexibility and toughness, and the cartilaginous tissue provides elasticity7. Other adaptations to protect the tendon include formation of a sesamoid bone (i.e., os peroneum) or thickening and flattening of the tendon8. Tendons containing fibrocartilaginous regions include those that most commonly contain sesamoid bones (peroneus longus and posterior tibial), suggesting that the fibrocartilaginous modification may predispose to endochondral ossification9. Fibrocartilaginous nodules can alter the tendon appearance; therefore, recognizing their existence is important so as to not mistake the appearance for tendon pathology, such as tendinosis, partial tears, or complete tears.
The peroneus longus muscle originates from the lateral condyle of the tibia, proximal aspect of the fibula, and intermuscular septa and adjacent fascia and inserts at the plantar aspect of the medial cuneiform, proximal aspect of the first metatarsal, and occasionally at the base of the second metatarsal. The peroneus longus tendon courses around the lateral malleolus and along the lateral aspect of the calcaneus before changing direction, as it courses beneath the cuboid prior to its distal insertions. An os peroneum is present in about 20% of the population. When present, it is usually located at the calcaneocuboid joint, in the region of wrap-around just before the cuboid tunnel8. In the absence of an os peroneum, a fibrocartilaginous nodule can be found in the same region. This fibrocartilaginous nodule can increase the fat-saturated T2-weighted MRI signal of the peroneus longus tendon, simulating the appearance of a tendon tear8.
The posterior tibial muscle originates from the posterior aspect of the tibia, medial aspect of the fibula, interosseous membrane, and intermuscular septa and deep fascia. The posterior tibial tendon courses posterior to the medial malleolus with the major tendon inserting on the tuberosity of the navicular and plantar aspect of the medial cuneiform. The sesamoid in the posterior tibial tendon is a normal and frequent finding responsible for a focal, isolated, off-center focus of increased intratendinous signal (7) and/or a bulbous appearance of the posterior tibial tendon, which occurs prior to the tendon division at the level of the spring ligament (plantar calcaneonavicular ligament)7.
Vogel et al. found that the composition of the distal posterior tibial tendon, as it passes inferior to the medial malleolus, is different when compared to the more proximal region of this tendon, containing cells having a round rather than elongated shape, with a higher glycosaminoglycan-hyaluronic acid content, and a significant amount of large as well as small proteoglycans. These alterations in composition do not consistently differ with advancing age after puberty, leading the authors to conclude that the development of fibrocartilaginous morphology and proteoglycan composition is a normal adaptive response of tissue at this location10. According to Delfaut et al., the MR signal intensity of fibrocartilage depends on its collagen fiber organization. Well-organized collagen fibers and few chondrocytes and lacunae exhibit low signal intensity, indistinguishable from tendon fibers. Thus, in the presence of these well-organized collagen fibers, the bulbous aspect of the posterior tibial tendon is the only feature of a fibrocartilaginous nodule. In contrast, less well organized fibrocartilage displays increased MR signal intensity, which is located laterally off-center7.
Differentiating posterior tibial tendinosis from a fibrocartilaginous nodule can be challenging. On MR imaging, tendinosis is characterized by tendon thickening and increased intra-tendinous signal. A posterior tibial fibrocartilaginous nodule can be distinguished from tendinosis by its location opposite to the spring ligament, focal nature, and laterally off-center increased intratendinous signal intensity or low signal intensity bulbous aspect. In addition, normal fibrocartilage is not associated with paratendonitis, which often accompanies tendon pathology7. Furthermore, on contrast enhanced images, normal fibrocartilage does not have hypervascularization and should not enhance versus the neovascularization as seen in tendon degeneration7.
Figure 7:
Fibrocartilaginous nodule of the distal posterior tibial tendon in a 61-year-old man. Axial proton density-weighted fat-suppressed (top left), axial proton density-weighted (top right), and sagittal T1-weighted (bottom left and bottom right) MR images demonstrate laterally off center intratendinous increased signal intensity (arrow) within the distal posterior tibial tendon, compatible with a fibrocartilaginous nodule.
In contrast to the sesamoid of the posterior tibial tendon, which is completely or partially embedded in the tendon before its division into smaller tendon slips, separated from the tuberosity by up to 6 mm, and located opposite the region of the spring ligament and talar head, the os tibiale externum (accessory navicular bone) is partially embedded in the main tendinous portion distal to the division of the posterior tibial tendon, and located closer to the tuberosity of the navicular11.
Development
Sesamoid bones are generally thought to form from a combination of biological and mechanical factors, including skeletal geometry, posture, and muscular activity2. Most sesamoids begin as cartilaginous nodules that then undergo endochondral ossification during early to late childhood, between the ages of 3 and 12 years2. For example, at the first metatarsophalangeal joint, islands of undifferentiated connective tissue are recognized as precartilaginous by the tenth week of fetal life. The next steps in sesamoid maturation at the first metatarsophalangeal joint include chondrofication and integration into the joint capsule (12 weeks) and ossification (eighth year)4. Sesamoids as cartilaginous nodules in the fetus are more numerous than in the adult3, suggesting that physical activity probably plays a role in selecting and regulating the degree of development.
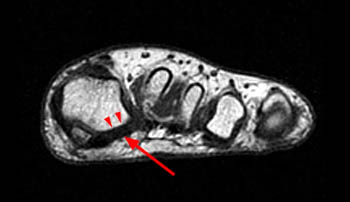
According to Le Minor, congenital absence of the constant hallucial sesamoids is rare, with absence of the medial sesamoid being more common, and must be differentiated from total resorption of the sesamoid due to infection or surgical excision. With congenital absence of the lateral hallux metatarsophalangeal sesamoid, there is additional absence of the normal intersesamoidean crest and of both sesamoidean grooves of the metatarsal head (8). In contrast, with resorption or surgical excision, the normal morphology of the metatarsal head should be maintained. In one report, no functional disturbances resulted from the absence of the lateral hallux metatarsophalangeal sesamoid12; however, metatarsophalangeal pain has been reported in the setting of absence of the medial sesamoid bone13. Congenital absence of the medial sesamoid has also been associated with hallux abducto valgus deformity14.
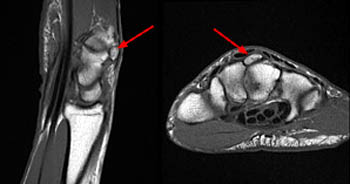
Figure 8:
Congenital absence of the lateral hallux metatarsophalangeal sesamoid in a 20-year-old man. Coronal T1-weighted MR image demonstrates absence of the lateral hallux metatarsophalangeal sesamoid (arrow) accompanied by slight convexity of the sesamoidean groove of the metatarsal head (arrowheads).
Pathophysiology
In the setting of trauma, sesamoid bone abnormalities consist of acute fracture, stress fracture, and dislocation. It is often difficult to differentiate a fractured hallucal sesamoid from a bipartite hallucal sesamoid (9). Imaging clues to differentiate a fractured single medial sesamoid from a bipartite medial hallucal sesamoid include: the fractured sesamoid is usually slightly larger than the lateral sesamoid while the bipartite sesamoid has a much larger medial sesamoid than lateral sesamoid; the fractured sesamoid shows a sharp, radiolucent, uncorticated line between the two fragments while the bipartite sesamoid has two corticated components; the fractured sesamoid fragments often fit together like pieces of a puzzle while the bipartite sesamoid has two components that do not fit together snugly; the fractured sesamoid will show increased uptake on a 99mTc-MDP bone scan while the bipartite sesamoid may not; and the recently fractured sesamoid may demonstrate bone marrow edema while the bipartite sesamoid may not15. Additional signs of a fractured sesamoid include bone displacement or soft tissue swelling.
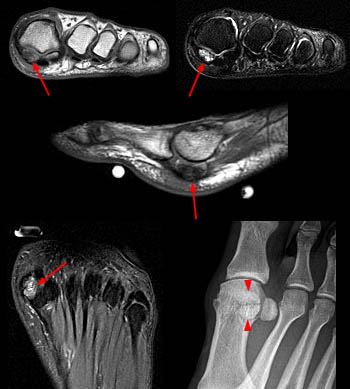
Figure 9:
Fracture of the medial sesamoid of the first metatarsophalangeal joint in a 49-year-old woman. Radiograph (top left) shows a fractured medial sesamoid (arrow) of the first metatarsophalangeal joint. Corresponding axial T1-weighted MR image (top right) demonstrates the fracture (arrow). Coronal T1-weighted (bottom left) and T2-weighted fat-suppressed (bottom right) MR images demonstrate marrow edema within the osseous fragments (arrowheads).
Dislocations of the great toe sesamoid bones are the result of plantar capsule ruptures secondary to propulsive injuries16. Radiographically, dislocations are diagnosed by displacement. The 99mTc-MDP bone scan is usually negative, unless there is an accompanying fracture. “Turf toe” is a severe hyperextension injury of the metatarsophalangeal joint characterized by disruption of the plantar capsule, injury of the flexor hallucis brevis tendon and, in some cases, a transverse fracture with separation of one or both sesamoid bones (10)16.
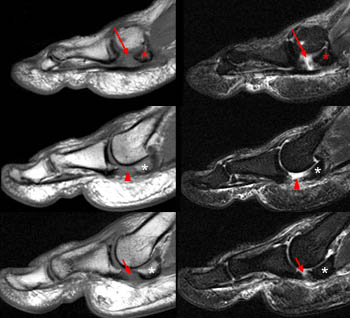
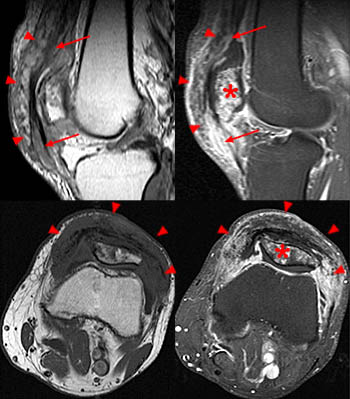
Figure 10:
Turf toe injury in a 28-year-old man. Sagittal T1-weighted (left) and sagittal STIR (right) MR images of the first metatarsophangeal joint through the medial (top images) and lateral (middle and lower images) sesamoids show capsuloligamentous injury, characterized by complete tearing of the medial sesamoid phalangeal ligament (red arrows) with slight proximal migration of the medial sesamoid bone (red asterisks); high-grade, near complete tearing of the lateral sesamoid phalangeal ligament (short arrows) with slight proximal migration of the lateral sesamoid bone (white asterisks); and tearing of the plantar plate (arrowheads) of the metatarsophalangeal joint.
Chronic stress can lead to painful conditions in the hallux sesamoids, clinically described as sesamoiditis. Causes of the pain include stress fractures, stress reaction, osteoarthritis, and osteonecrosis. On 99mTc-MDP bone scans, focally increased activity can be seen in the setting of sesamoiditis. With MRI, bone marrow edema is present in most cases of sesamoiditis (11). With CT scanning, subtly increased sclerosis would favor a diagnosis of osteonecrosis. The pathogenesis of osteonecrosis of the hallux sesamoid bones is the interruption of bone blood supply secondary to fracture, dislocation, infection, or repetitive injury leading to ischemic necrosis of bone16.
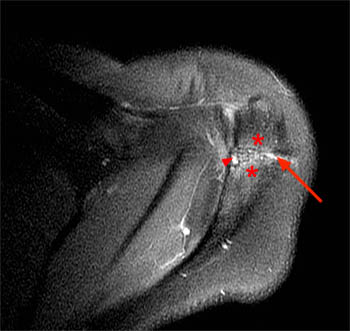
Figure 11:
Sesamoiditis in a 34-year-old man who injured his medial sesamoid two years prior to imaging while playing squash. Coronal T1-weighted (top left), coronal T2-weighted fat-suppressed (top right), sagittal T1-weighted (middle), and axial proton density-weighted fat-suppressed (bottom left) MR images show intense edema within a bipartite medal sesamoid of the first metatarsophalangeal joint (arrows), compatible with sesamoiditis. Radiograph (bottom right) confirms the bipartite medial sesamoid (arrowheads).
Both osteomyelitis and septic arthritis can involve the sesamoid bones. Whether the sesamoid bone is primarily involved or, more frequently, is secondarily involved following infection of the adjacent joint, radiographic findings are bone fragmentation, resorption, and/or subluxation4. With MRI, the marrow will reveal low signal intensity with T1-weighted imaging, high signal intensity with T2-weighted imaging, and enhancement following intravenous contrast administration (12, 13).
Figure 12:
Osteomyelitis of the tibial sesamoid of the first metatarsophalangeal joint in a 58-year-old diabetic man. Axial T2-weighted fat-suppressed (top left), axial T1-weighted (top right), coronal T2-weighted fat-suppressed (middle left), and coronal T1-weighted (middle right) MR images demonstrate soft tissue ulceration (arrowheads) at the medial aspect of the first metatarsophalangeal joint with underlying osseous erosion of the medial aspect of the tibial hallux metatarsophalangeal sesamoid (arrows) and with associated marrow edema. The corresponding radiograph (bottom) confirms osseous erosion of the medial aspect of the tibial sesamoid (short arrow).
Figure 13:
Chronic granulomatous (mycobacterium gordonae) infection in a 59-year-old man. Sagittal T1-weighted (top left), sagittal T1-weighted fat-suppressed post-contrast (top right), axial T1-weighted (bottom left), and axial T1-weighted fat-suppressed post-contrast (bottom right) MR images show a markedly enhancing, infiltrative process involving the region of the prepatellar bursa (arrowheads) and within the subcutaneous tissues, extending into the patellar (arrows) and quadriceps (arrows) tendons and into the substance of the majority of the bony patella (asterisks).
Osteoarthritis commonly affects the sesamoid bones, especially the sesamoids of the first metatarsophalangeal (K) and first metacarpophalangeal joints. Radiographic findings include non-uniform joint space loss, osteophyte formation, bony eburnation, and flattening of a portion of the sesamoid4,16. CT scanning is useful to detect bone sclerosis and fragmentation, and MRI allows evaluation of associated marrow and soft tissue changes15. Diffuse idiopathic skeletal hyperostosis (DISH) can mimic osteoarthritis of the sesamoids but is characterized by bony proliferation and spiculation4.
Figure 14:
Mild osteoarthritis of the articulation between the first metatarsal head and medial sesamoid in a 62-year-old woman. Sagittal proton density-weighted (top), sagittal T1-weighted (second from top), axial proton density-weighted fat-suppressed (second from bottom), and axial T2-weighted (bottom) MR images of the first metatarsophalangeal joint demonstrate cystic changes and osteophyte formation about the articulation between the first metatarsal head and medial sesamoid (arrows).
In rheumatoid arthritis, synovial inflammation leads to pannus which then destroys cartilage and subchondral bone4. Furthermore, adjacent tenosynovitis can lead to surface resorption and destruction of the sesamoid4. Radiographically, rheumatoid arthritis is manifested by bone resorption and erosions, uniform joint space loss, and soft tissue swelling16. At the great toe, progressive hallux valgus deformity is associated with dislocation of the sesamoids as a result of joint destruction4. In the seronegative spondyloarthropathies (psoriasis, reactive arthritis, ankylosing spondylitis), sesamoid “periostitis” can be seen, which is similar to the bony proliferation or “whiskering” that can be found about all involved articulations in these disorders4, likely representing enthesitis16.
Crystal deposition diseases, such as gout and calcium pyrophosphate dihydrate (CPPD) crystal deposition disease, are characterized by crystal deposition within the cartilage and bone of the sesamoids resulting in erosions in gout (15), and cystic changes and sclerosis of bone and chondrocalcinosis in CPPD crystal deposition disease4. Both of these disorders can involve simultaneously the great toe metatarsophalangeal and metatarsal-sesamoid joints4. As these two disorders can occur separately or together, joint aspiration and crystal evaluation are often required to confirm the diagnosis16.
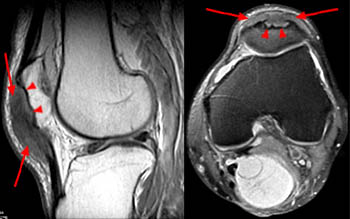
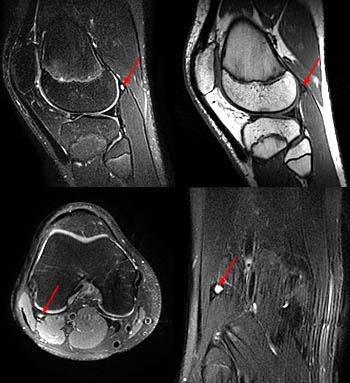
Figure 15:
Gout involving the patella of a 71-year-old man. Sagittal T1-weighted (left) and axial proton density-weighted fat-suppressed (right) MR images demonstrate a low signal intensity prepatellar mass (arrows) with erosion (arrowheads) of the anterior aspect of the patellar cortex, compatible with a synovial inflammatory mass.
Tumors, both benign and malignant, can occasionally involve the sesamoid bones. In particular, although infrequently, tumors can affect the patella (16). Primary intraosseous tumors of the patella account for approximately 0.12% of all primary bone tumors17. The majority of primary bone tumors are benign, with the most common being giant cell tumor and chondroblastoma18. The most common malignant tumors include metastases, osteosarcoma, and hemangioendothelioma17. Myeloma involving the patella is rare19. When a focal intra-osseous mass is identified within the patella, other conditions that can mimic tumors should be considered, such as a brown tumor in hyperparathyroidism, osteomyelitis, intraosseous gout, and intraosseous ganglion17.
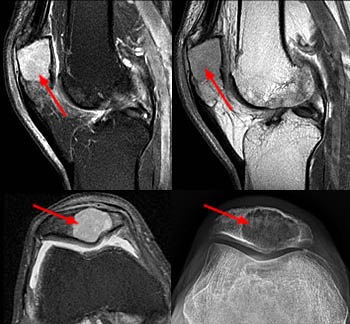
Figure 16:
68-year-old man with plasmacytoma of the patella. Sagittal proton density-weighted fat-suppressed (top left), sagittal proton density-weighted (top right), and axial proton density-weighted fat-suppressed (middle) MR images demonstrate a T2 hyperintense, T1 slightly hyperintense to muscle lesion within the patella (arrows). Corresponding radiograph (bottom) shows a lytic lesion within the patella (arrow).
Painful os peroneum syndrome (POPS) is a cause of lateral plantar foot pain and results from a spectrum of conditions that can present in either the acute or chronic setting. The acute presentation results from sudden trauma, frequently a supination and/or inversion injury of the ankle; the chronic presentation results from repetitive injuries of the foot. The POPS spectrum includes: an acute os peroneum fracture or diastasis of a multipartite os peroneum, which may result in discontinuity of the peroneus longus tendon; chronic os peroneum fracture or diastasis of a multipartite os peroneum with callus formation, which may result in stenosing peroneus longus tenosynovitis; attrition or partial rupture of the peroneus longus tendon; frank rupture of the peroneus longus tendon with discontinuity proximal or distal to the os peroneum (17); and the presence of an extremely large peroneal tubercle that entraps the peroneus longus tendon and/or the os peroneum during tendon excursion20.
Figure 17:
Painful os peroneum syndrome in a 56-year-old man. Lateral and oblique radiographs (top left and right respectively) of the foot show proximal retraction of an os peroneum (arrows). Axial T1-weighted (middle left), axial proton density-weighted (middle right), and sagittal T2-weighted fat-suppressed (bottom) MR images confirm complete tearing of the peroneus longus tendon at the level of the os peroneum (arrows).
The fabella syndrome is a cause of posterolateral knee pain in patients who have a fabella, a sesamoid bone located within the lateral head of the gastrocnemius muscle, posterior to the lateral femoral condyle (18). The symptoms of the fabella syndrome are intermittent posterolateral knee pain, which is worsened by knee extension and typically reproducible by direct pressure over the fabella21. Zipple et al. described possible sources of posterolateral knee pain in the fabella syndrome, including either compressive or tensile forces on the fabellofibular ligament, compressive irritation of the gastrocnemius tendon, compression of the fabella against the femoral condyle leading to periosteal inflammation, compression of the posterior capsule by the fabella, or compression of neural tissue of the common peroneal nerve between the fabella and fibular head22.
Figure 18:
Fabella syndrome in a 15-year-old teenager. Sagittal T2-weighted fat-suppressed (top left), sagittal T1-weighted (top right), axial proton density-weighted fat-suppressed (bottom left), and coronal T2-weighted fat-suppressed (bottom right) MR images demonstrate bone marrow edema involving the fabella (arrows), reflecting stress changes, without fracture.
Accessory Ossicles
Accessory bones, or ossicles, are normal anatomic variants derived from unfused primary or secondary ossification centers. Both sesamoids and accessory ossicles are small, well-corticated, and round or ovoid in shape, may be bipartite or multipartite, are found close to a bone or joint, may be unilateral or bilateral, and are subject to significant morphological variations15. In contrast to sesamoid bones, which function to protect and sometimes increase efficacy of a tendon, accessory ossicles have no known function15. Both sesamoid bones and accessory ossicles can undergo pathologic changes and become symptomatic. Similar to sesamoid bones, accessory ossicles are subject to traumatic, infectious, and arthritic conditions as previously described. Accessory ossicles can also undergo specific ossicle-related painful syndromes, comparable to the os peroneum syndrome and the fabella syndrome.
The os trigonum is located posterior to the talus (20). An ossification center forms between the ages of 8 and 13 years and usually fuses with the talus within 1 year19. In approximately 7% of the population, however, this ossification center fails to fuse and is referred to as the os trigonum19. The os trigonum is corticated and articulates with the lateral tubercle of the posterior process of the talus through a fibrocartilaginous synchondrosis.
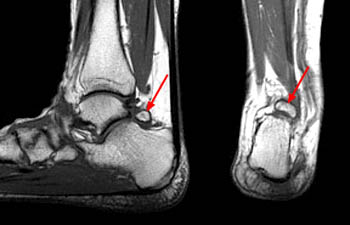
The os trigonum syndrome, a cause of posterior ankle impingement, refers to symptoms secondary to pathology of the lateral tubercle of the posterior talar process. This syndrome can result from multiple causes, including disruption of the cartilaginous synchondrosis between the os trigonum and the lateral talar tubercle as a result of repetitive microtrauma and chronic inflammation23. MR imaging findings consist of marrow edema within the talus and/or os trigonum, fluid in the synchondrosis, fluid surrounding the os trigonum, and soft tissue changes (21). MR can also show associated findings, such as flexor hallucis longus stenosing tenosynovitis and degenerative changes about the synchondrosis or between the os trigonum and adjacent calcaneus.
Figure 21:
Os trigonum syndrome in a 46-year-old man. Sagittal T1-weighted (left) and T2-weighted fat-suppressed (right) MR images demonstrate a large and irregular os trigonum with cystic changes and marrow edema in both the os and the parent bone (arrows) suggesting abnormal motion of the ossicle.
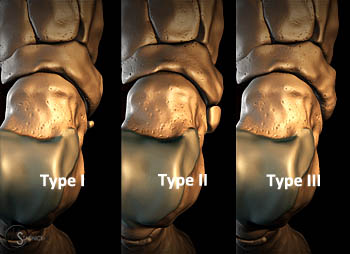
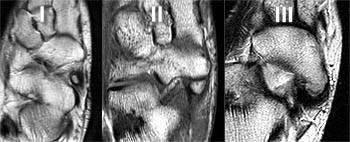
The accessory navicular bone is located adjacent to the posteromedial tuberosity of the navicular bone in 4-21% of the population24. There are three types of accessory navicular bones based on morphology (22). The type I, or os tibiale externum, is a sesamoid bone within the posterior tibial tendon near the navicular insertion. This ossicle may be separated up to 5 mm from the navicular tuberosity. The type II accessory navicular bone, or os naviculare, is the most common variant. It is separated from the navicular bone by 1 to 2 mm and connected to the navicular bone by a cartilaginous synchondrosis. Most or the entire posterior tibial tendon inserts on the type II navicular bone19. The type III accessory navicular bone, or cornuate navicular bone, is a prominent navicular tuberosity, which is essentially a fused type II accessory navicular bone.
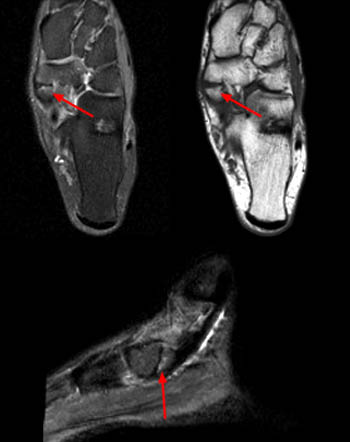
Of the three types of accessory navicular bones, the type II is most commonly symptomatic, causing medial foot pain. MR imaging findings of painful accessory navicular bones are marrow edema in the accessory navicular bone and within the synchondrosis, signifying osteonecrosis, inflammation, and destruction of the cartilage cap, findings compatible with chronic stress-related injury (24)25. MR can also lead to identification of associated posterior tibial tendon pathology.
The os intermetatarseum is located between the medial cuneiform and the base of the first and second metatarsals (25). This os is rarely a source of pathology, but it is often confused with a fracture. Infrequently, the os intermetatarseum may cause dorsal midfoot pain secondary to compression of the medial branch of the deep peroneal nerve19.
Figure 25:
Os intermetatarseum in a 58-year-old woman. Axial proton density-weighted (top left), sagittal T1-weighted (top right), and coronal T1-weighted (bottom) MR images demonstrate an os intermetatarseum (arrows) extending from the medial cuneiform anteriorly (dorsal to the first and second proximal intermetatarsal region). This osseous excrescence could irritate the terminal branches of the deep peroneal nerve, causing dorsal foot pain.
The os vesalianum is located proximal to the base of the fifth metatarsal. This os is rarely a source of pathology; however, painful syndromes of the forefoot have been associated with it. This ossicle should be differentiated from the normal ossification center of the tuberosity of the fifth metatarsal (that is parallel to the metatarsal shaft), avulsion fractures of the fifth metatarsal apophysis (that usually lie in a transverse plane), and avulsion fractures of the base of the fifth metatarsal bone (that involve the insertion site of the peroneus brevis tendon or lateral cord of the plantar aponeurosis)24.
The os supranaviculare is located at the dorsal aspect of the talonavicular joint. This ossicle is rarely symptomatic. The os supranaviculare should be differentiated from cortical avulsion fractures of the dorsal aspect of the navicular bone, which are typically thin slivers of bone. The lack of soft tissue swelling, the lack of a donor site, and the lack of focal tenderness also support a diagnosis of os supranaviculare.
The os sustentaculi is located at the posterior aspect of the sustentaculum tali, to which it is connected by a fibrocartilaginous synchondrosis (26). This ossicle may become painful secondary to chronic shearing forces with resultant early degenerative changes24. MR imaging will demonstrate marrow edema adjacent to the synchondrosis. The os sustentaculi should be differentiated from the rare isolated fracture of the sustentaculum tali, which has irregular margins and an incomplete cortical surface.
The os acromiale results from failure of fusion of one of the three acromial ossification centers. The anterior ossification center is termed the preacromion, the middle ossification center is designated the mesoacromion (27), and the posterior ossification center is termed the metaacromion. These ossification centers usually fuse between the ages of 22 and 25 years. The persistent os acromiale can theoretically lead to shoulder impingement syndromes as a result of the downward pull of the deltoid muscle, depressing the os19.
The os styloideum, or carpal boss, is located at the dorsal aspect of the base of the second and third metacarpals (29). The term carpal boss refers to an unmovable bony protuberance in this region, encompassing both the os styloideum and degenerative osteophytes. Potential symptoms of a carpal boss include pain and a limited range of motion, which may relate to an overlying ganglion or bursitis, an anterior tendon slipping over this bony prominence, or osteoarthritis at this site (30)26.
The os hamulus is an unfused hook of the hamate. This ossicle can be difficult to differentiate from a fracture of the hook of hamate (31).
Of interest, it has been proposed that some ossicles may actually be post-traumatic derivatives of avulsion fractures rather than accessory centers of ossification. For example, the os calcaneus secondarius may result from an avulsion fracture of the anterosuperior calcaneal process at the bifurcate ligament attachment site, the os subtibiale may result from an avulsion fracture of the medial malleolus, and the os subfibulare may be the result of a lateral malleolar avulsion fracture. As a general rule, an ovoid, small, and well-corticated appearance favors the diagnosis of accessory ossicle24, but the distinction between an accessory ossicle and avulsion fracture can often be difficult.
Conclusion
Sesamoid bones and accessory ossicles vary in prevalence and appearance. They are usually incidental findings on imaging studies, and it is important not to mistake them for pathology, such as fractures. These bones can become symptomatic due to a variety of traumatic, infectious, arthritic, and neoplastic conditions. Additionally, accessory ossicles, as well as certain sesamoid bones, can undergo specific ossicle-related painful syndromes. MRI is very useful in evaluating pathology of the sesamoid bones and accessory ossicles. Furthermore, MRI enables adjacent soft tissue evaluation. Knowledge of the location, imaging characteristics, and associated clinical entities is important for proper image interpretation of alterations affecting sesamoid bones and accessory ossicles.
References
1 “sesamoid.” Dictionary.com Unabridged. Random House, Inc. 06 Mar. 2014. Dictionary.com
2 Sarin VK, Erickson GM, Giori NJ, Giori NJ, Bergman AG, Carter DR. Coincident development of sesamoid bones and clues to their evolution. Anat Rec (New Anat). 1999; 257:174-180.
3 Gray H. Anatomy of the Human Body. Philadelphia: Lea & Febiger, 1918; Bartleby.com, 2000. www.bartleby.com/107/.
4 Resnick D, Niwayama G, Feingold ML. The sesamoid bones of the hands and feet: participators in arthritis. Radiology. 1977; 123:57-62.
5 Warwick R, Williams PL. Gray’s Anatomy. Philadelphia: W.B. Saunders Co., 35th British edition. 1973; 384-385.
6 Benjamin M, Ralphs JR. Fibrocartilage in tendons and ligaments – an adaptation to compressive load. J Anat. 1998; 193:481-494.
7 Delfaut EM, Demondion X, Bieganski A, Cotten H, Mestdagh H, Cotten A. The fibrocartilaginous sesamoid: a cause of size and signal variation in the normal distal posterior tibial tendon. Eur Radiol. 2003; 13:2642-2649.
8 Didolkar MM, Malone AL, Nunley JA, Dodd LG, Helms CA. Pseudotear of the peroneus longus tendon on MRI, secondary to a fibrocartilaginous node. Skeletal Radiol. 2012; 41:1419-1425.
9 Benjamin M, Qin S, Ralphs JR. Fibrocartilage associated with human tendons and their pulleys. J Anat. 1995; 187:625-633.
10 Vogel KG, Ordog A, Pogany G, Olah J. Proteoglycans in the compressed region of human tibialis posterior tendon and in ligaments. Journal of Orthopaedic Research. 1993; 11:68-77.
11 Bareither DJ, Muehleman CM, Feldman NJ. Os tibiale externum or sesamoid in the tendon of tibialis posterior. J Foot Ankle Surg. 1995; 34(5):429-434.
12 Le Minor JM. Congenital absence of the lateral metatarso-phalangeal sesamoid bone of the human hallux: a case report. Surgical and Radiologic Anatomy. 1999; 21(3): 225-227.
13 Kanatli U, Ozturk AM, Ercan NG, Ozalay M, Daglar B, Yetkin H. Absence of the medial sesamoid bone associated with metatarsophalangeal pain. Clin Anat. 2006; 19(7):634-639.
14 Zinsmeister BJ, Edelman R. Congenital absence of the tibial sesamoid: a report of two cases. J Foot Surg. 1985; 24(4):266-268.
15 Nwawka OK, Hayashi D, Diaz LE, Goud AR, Arndt III WF, Roemer FW, Malguria N, Guermazi A. Sesamoids and accessory ossicles of the foot: anatomical variability and related pathology. Insights Imaging. 2013; 4:581-593.
16 Taylor JA, Sartoris DJ, Huang G, Resnick DL. Painful conditions affecting the first metatarsal sesamoid bones. Radiographics. 1993; 13:817-830.
17 Singh J, James SL, Kroon HM, Woertler K, Anderson SE, Davies AM. Tumour and tumour-like lesions of the patella – a multicentre experience. Eur Radiol. 2009; 19:701-712.
18 Mercuri M, Casadei R. Patellar tumors. Clin Orthop Relat Res. 2001; 389:35-46.
19 Kalantari BN, Seeger LL, Motamedi K, Chow K. Accessory ossicles and sesamoid bones: spectrum of pathology and imaging evaluation. Applied Radiology. 2007; 28-37.
20 Sobel M, Pavlov H, Geppert MJ, Thompson FM, DiCarlo EF, Davis WH. Painful os peroneum syndrome: a spectrum of conditions responsible for plantar lateral foot pain. Foot Ankle Int. 1994; 15:112-124.
21 Weiner DS, Macnab I. The “fabella syndrome”: an update. J Pediatric orthopaedics. 1982; 2:405-408.
22 Zipple JT, Hammer RL, Loubert PV. Treatment of fabella syndrome with manual therapy: a case report. J Ortho Sports Phys Ther. 2003; 33:33-39.
23 Karasick D, Schweitzer ME. The os trigonum syndrome: imaging features. AJR. 1996; 166:125-129.
24 Mellado JM, Ramos A, Salvado E, Camins A, Danus M, Sauri A. Accessory ossicles and sesamoid bones of the ankle and foot: imaging findings, clinical significance and differential diagnosis. Eur Radiology. 2003; 13:L164-177.
25 Choi YS, Lee KT, Kang HS, Kim EK. MR imaging findings of painful type II accessory navicular bone: correlation with surgical and pathologic studies. Korean J Radiol. 2004; 5:274-279.
26 Conway WF, Destouet JM, Gilula LA, Bellinghausen HW, Weeks PM. The carpal boss: an overview of radiographic evaluation. Radiology. 1985; 156:29-31.