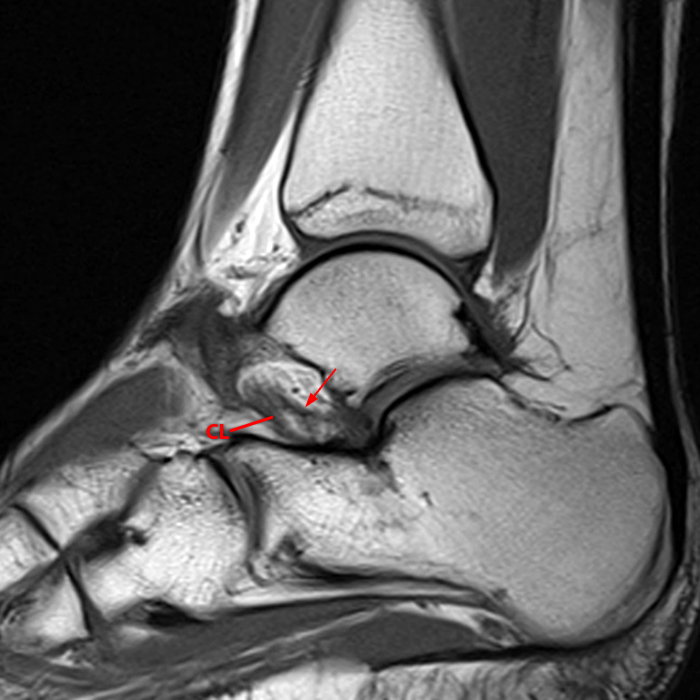
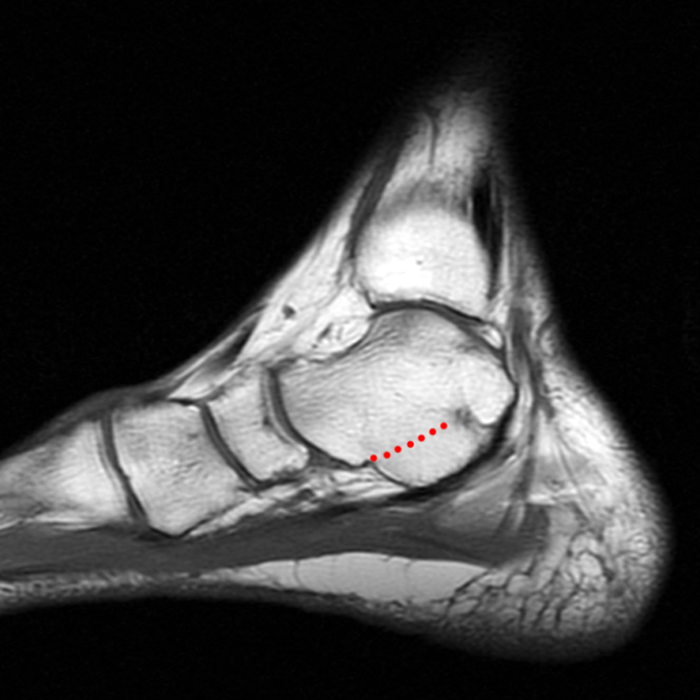
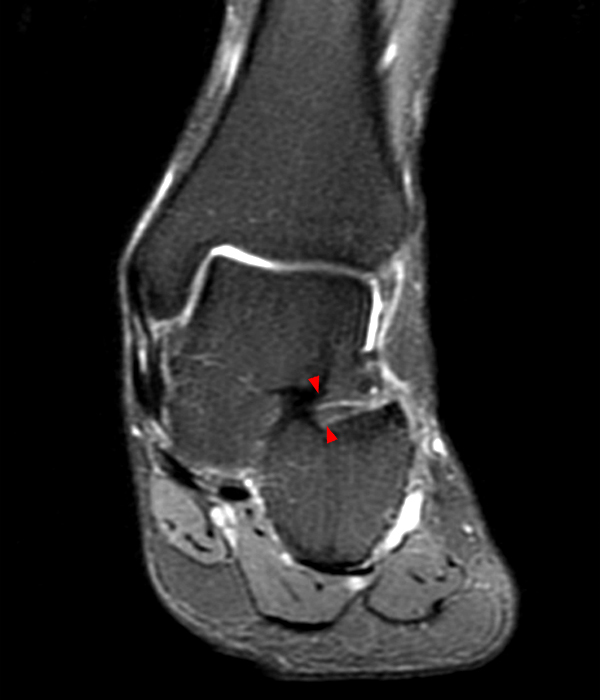
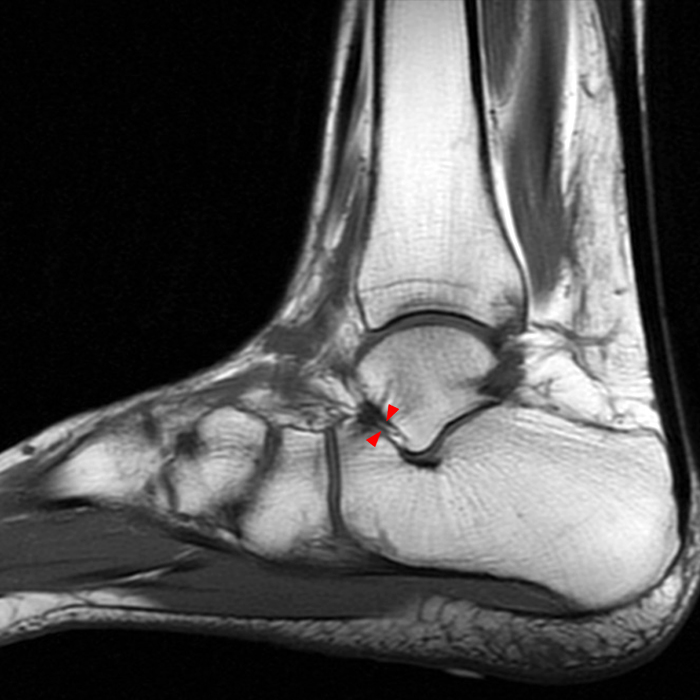
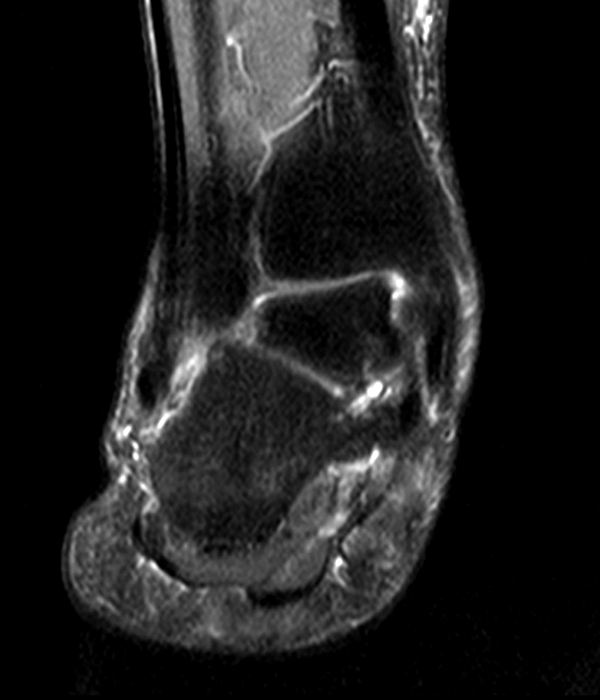
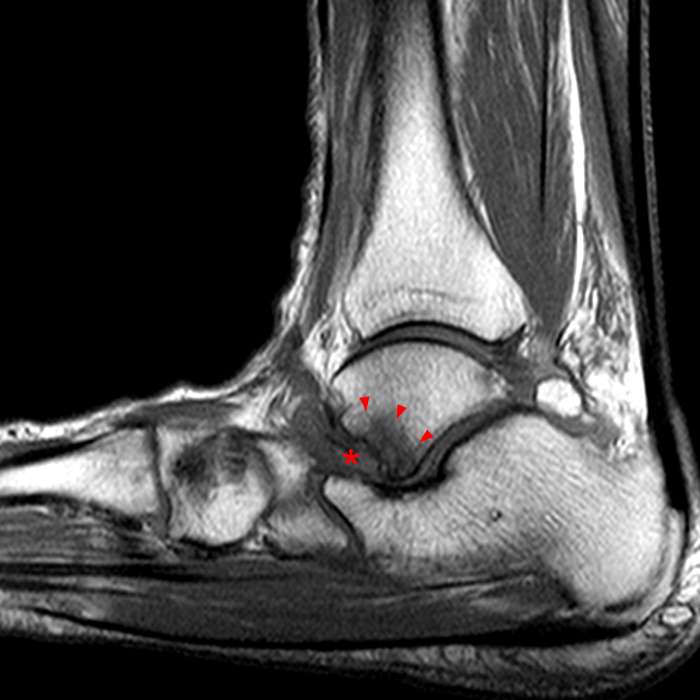
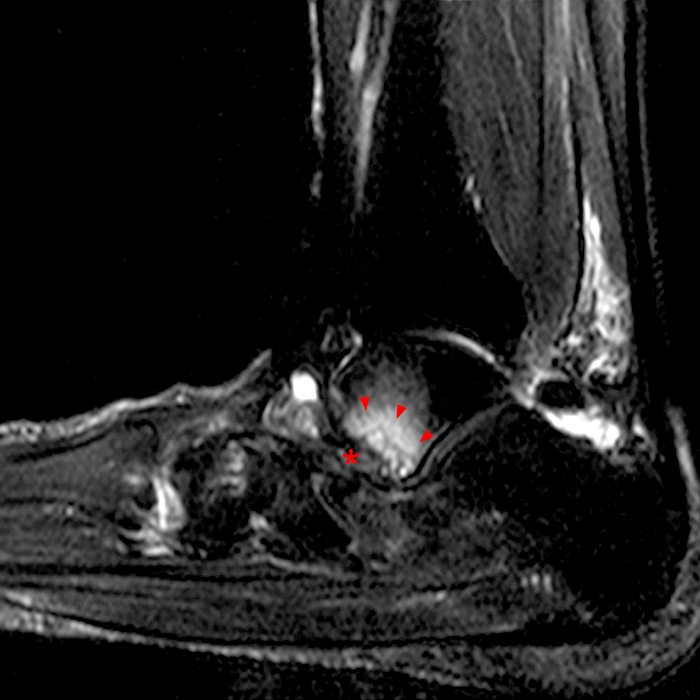
Case 1: A 28 year old female presents to an orthopaedic surgeon with lateral left ankle pain, tenderness to palpation, and a sensation of instability. She reports left ankle injury 3 weeks ago.
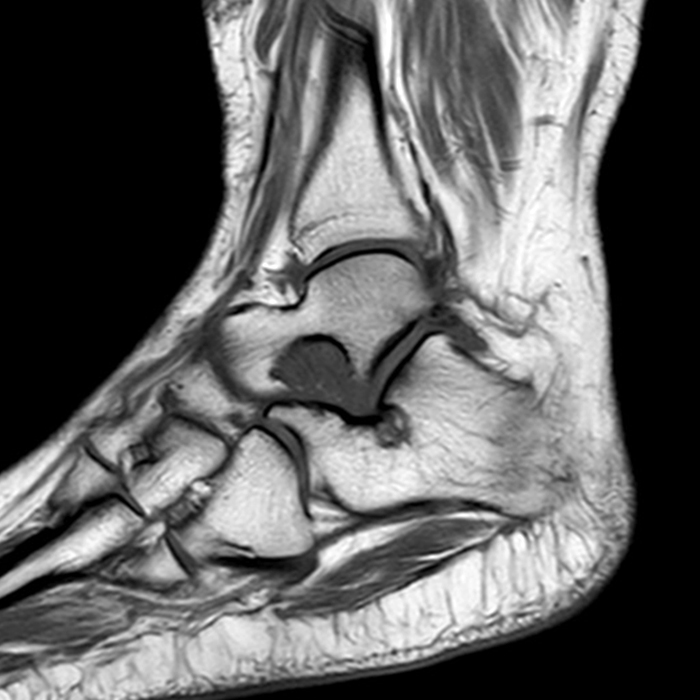
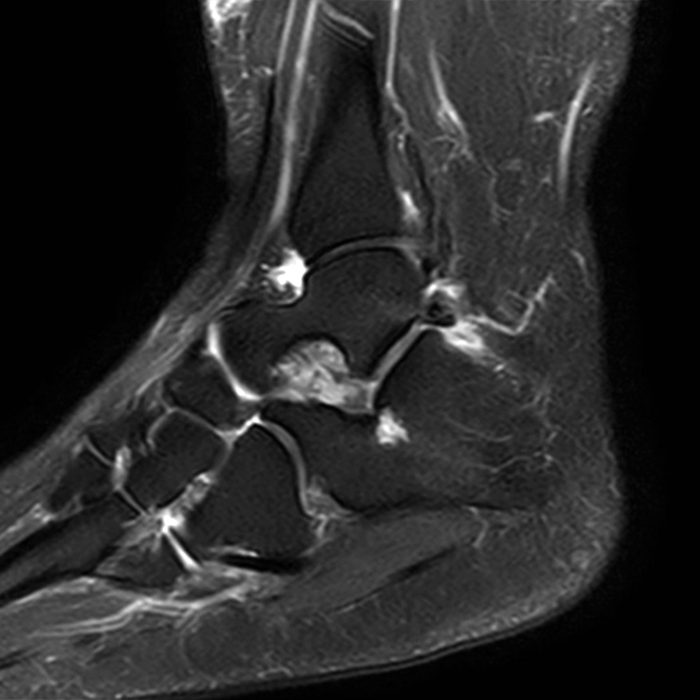
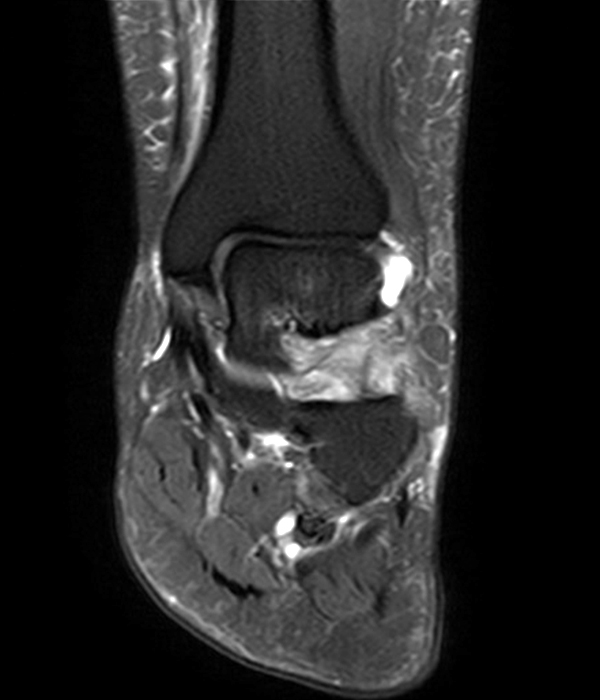
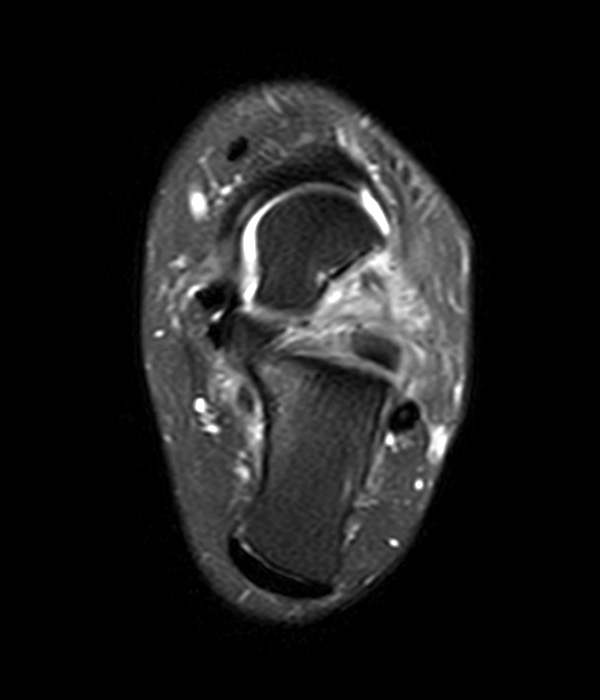
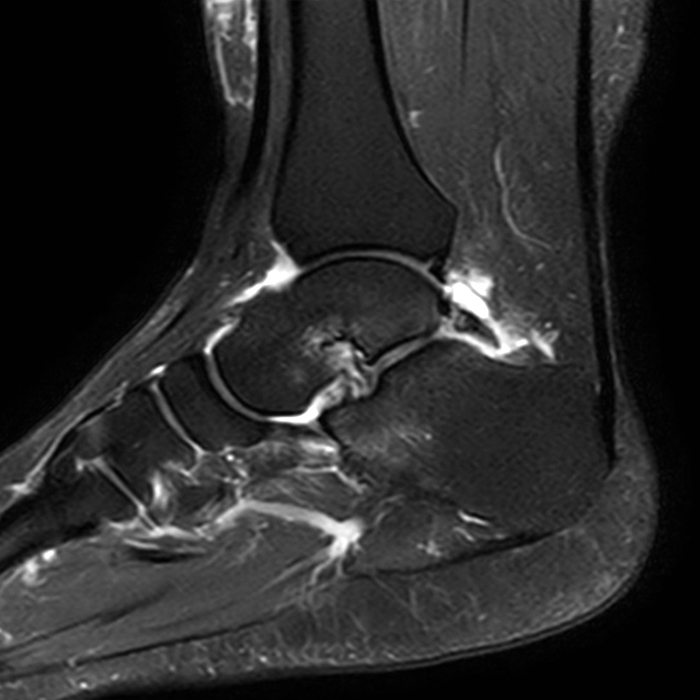
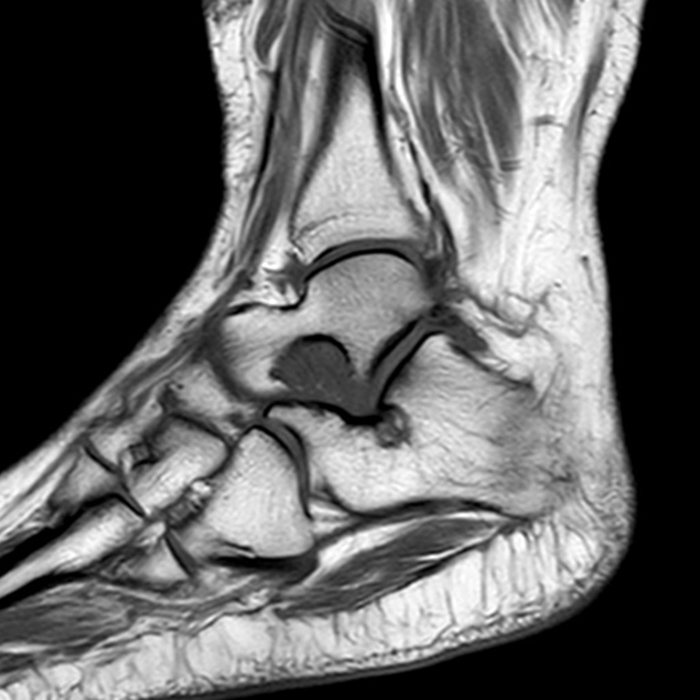
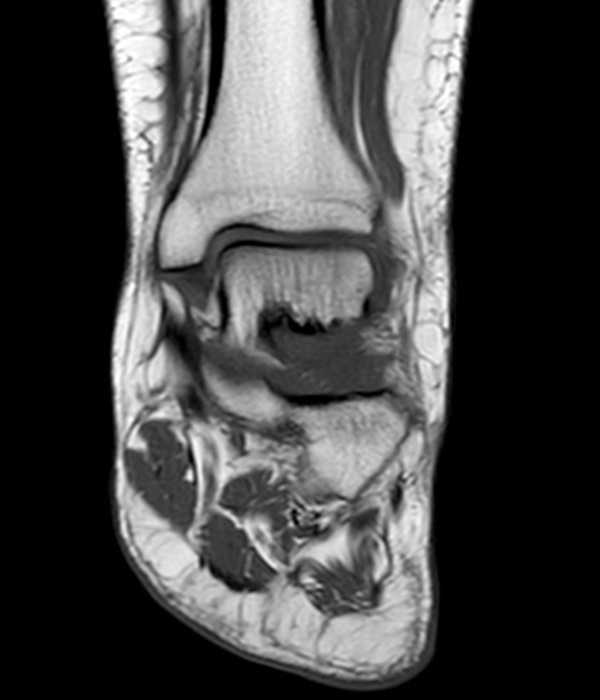
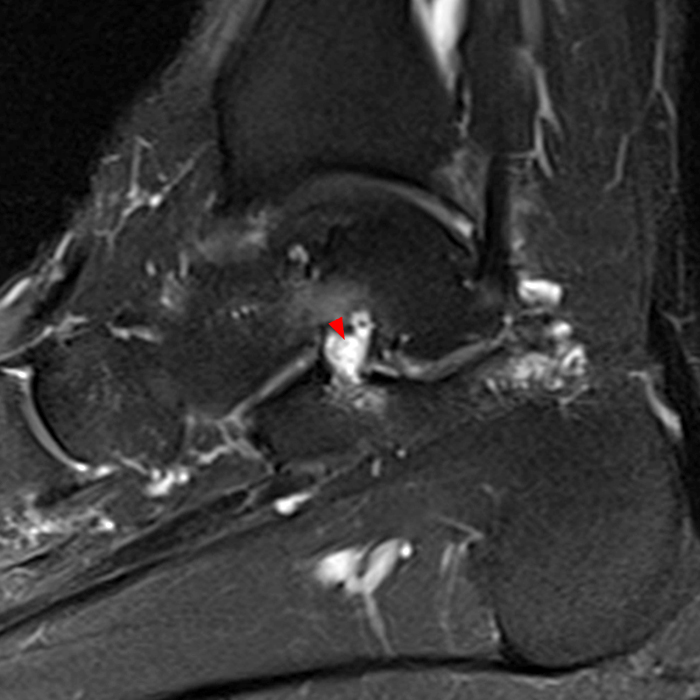
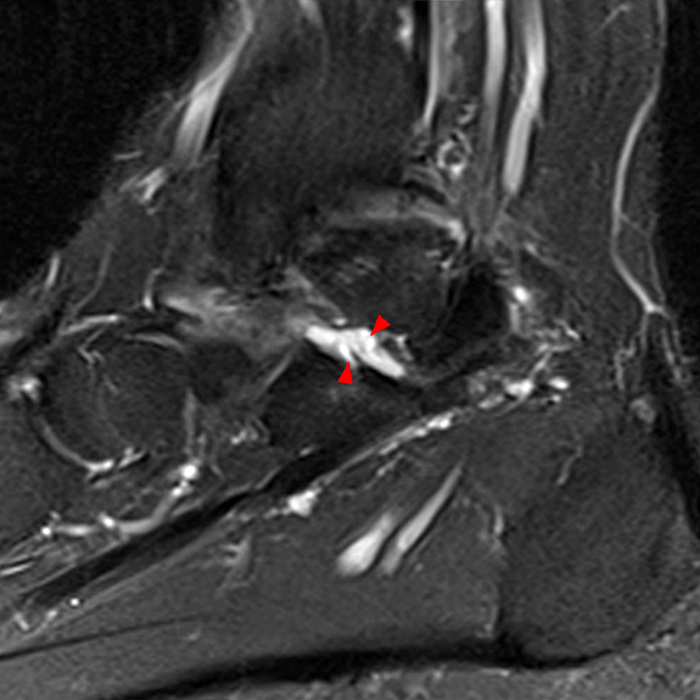
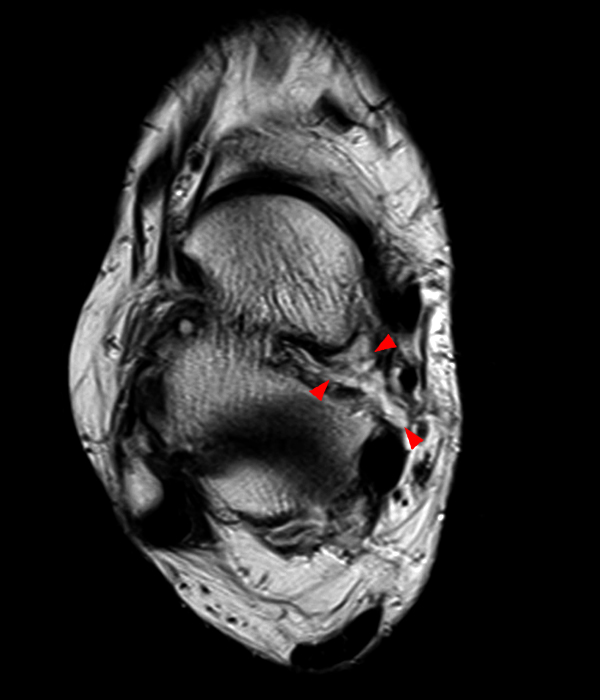
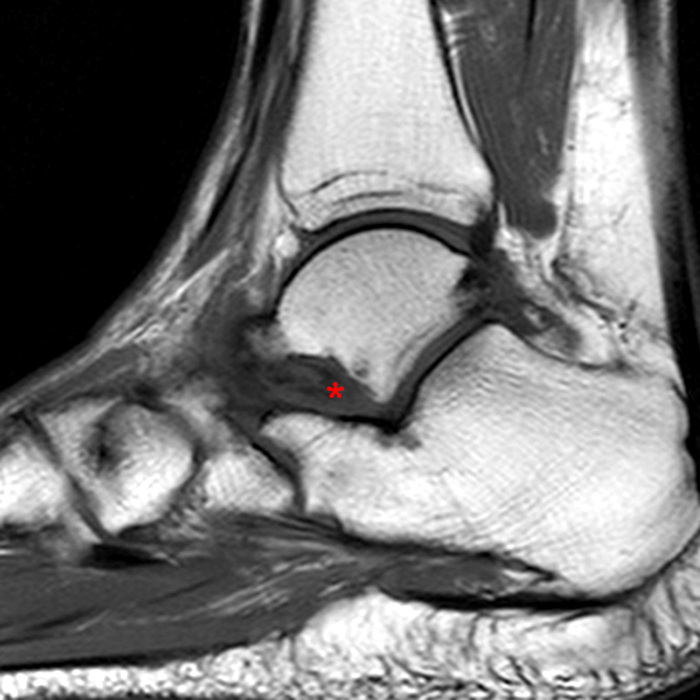
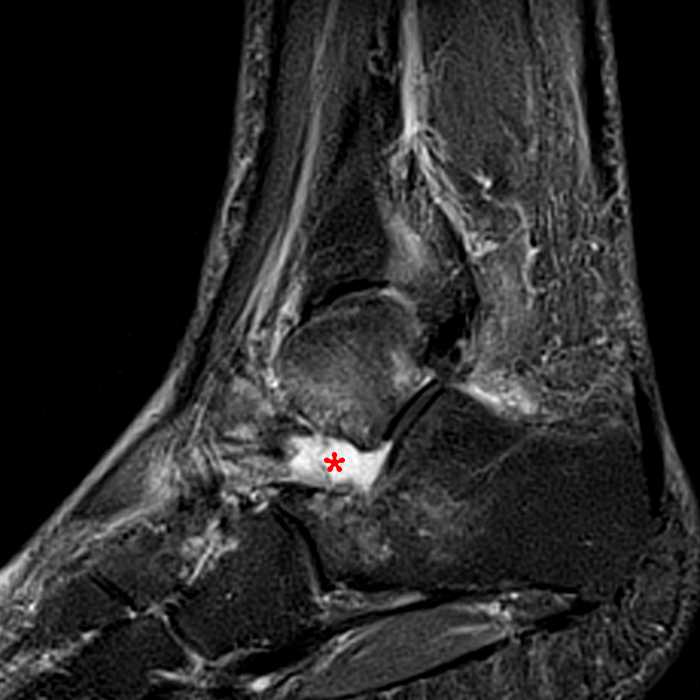
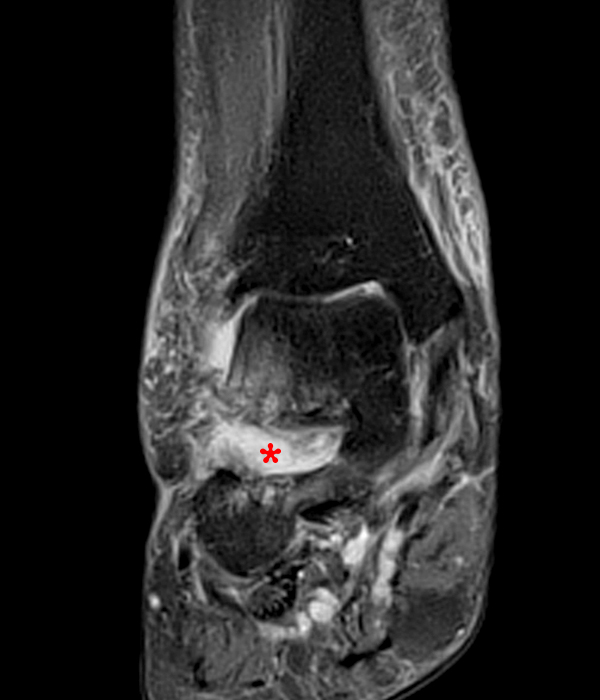
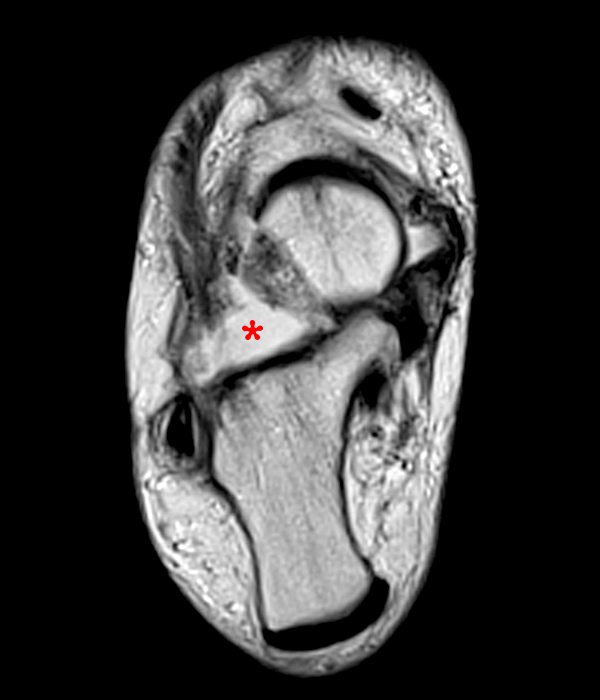
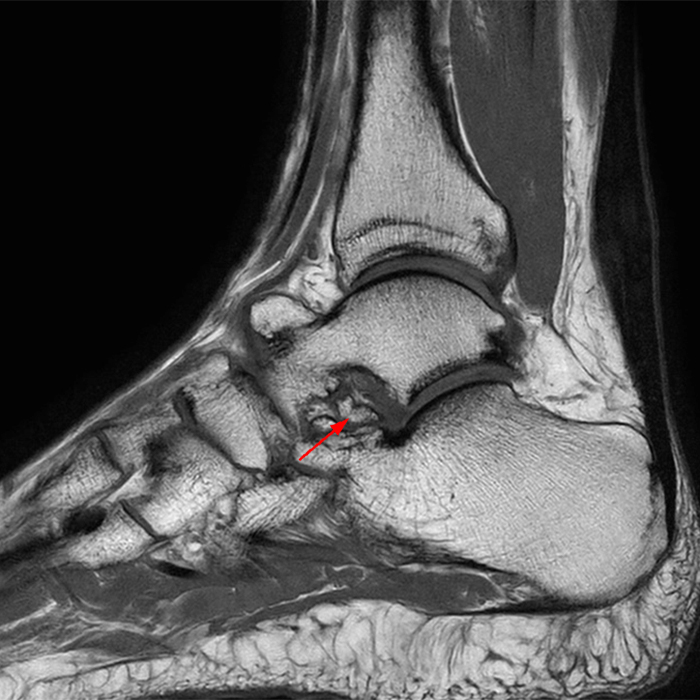
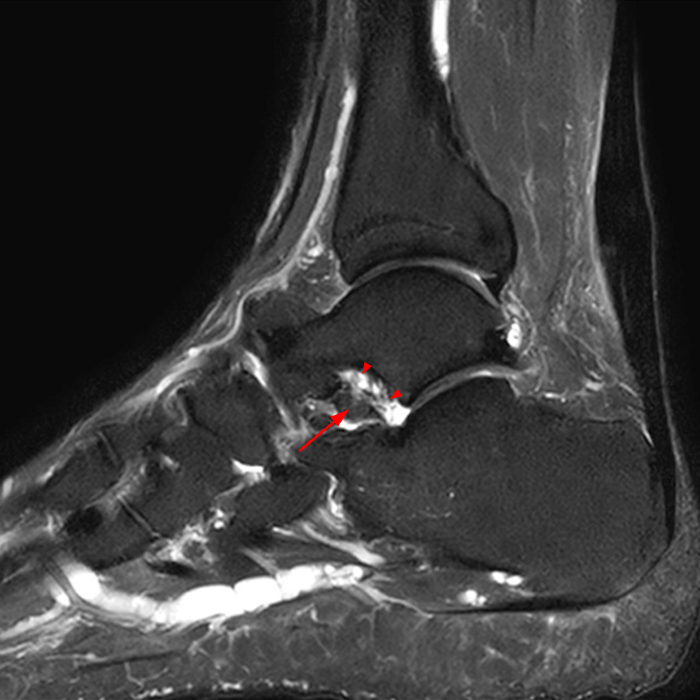
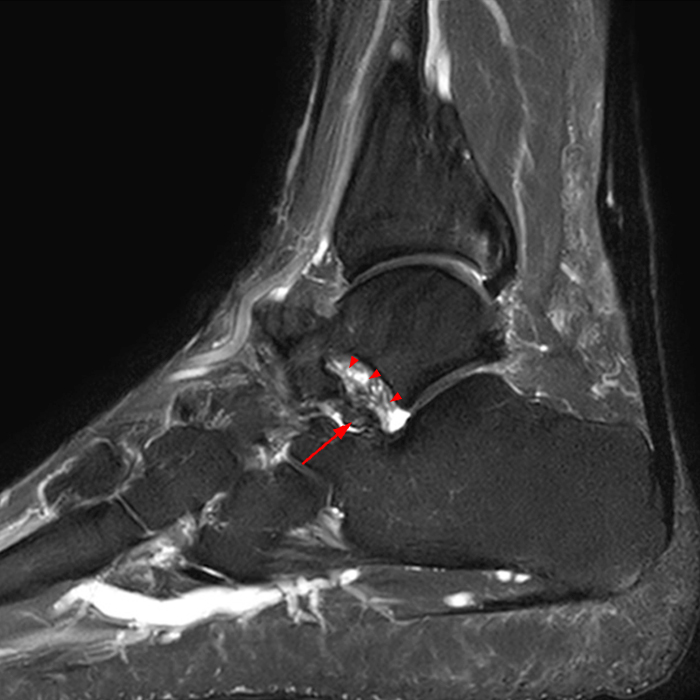
MRI of the ankle was performed. Sagittal T1-weighted and fat suppressed proton density-weighted images (Images 1A and 1B), coronal T1-weighted and fat suppressed T2-weighted images (Images 1C and 1D), axial fat suppressed T2-weighted (Image 1E), and a more medial sagittal fat suppressed T2-weighted image (Image 1F) are provided. What are the findings, and what is the diagnosis?
Findings
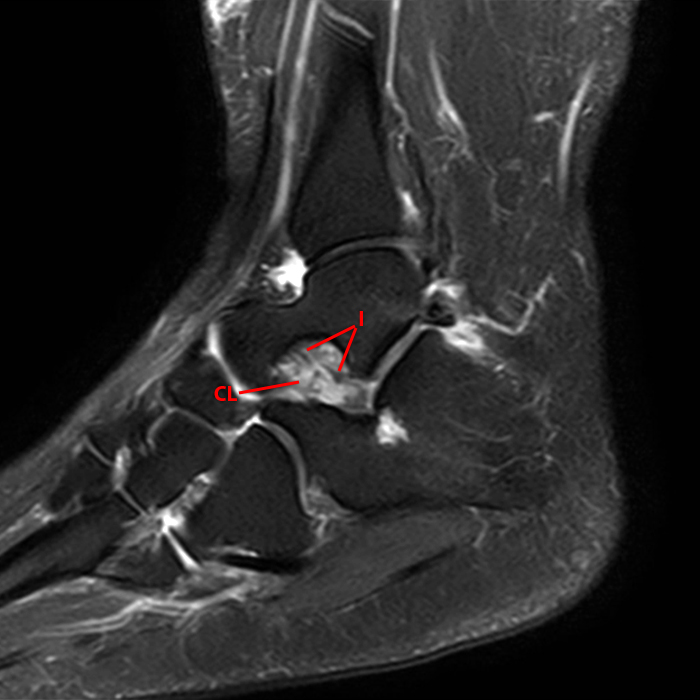
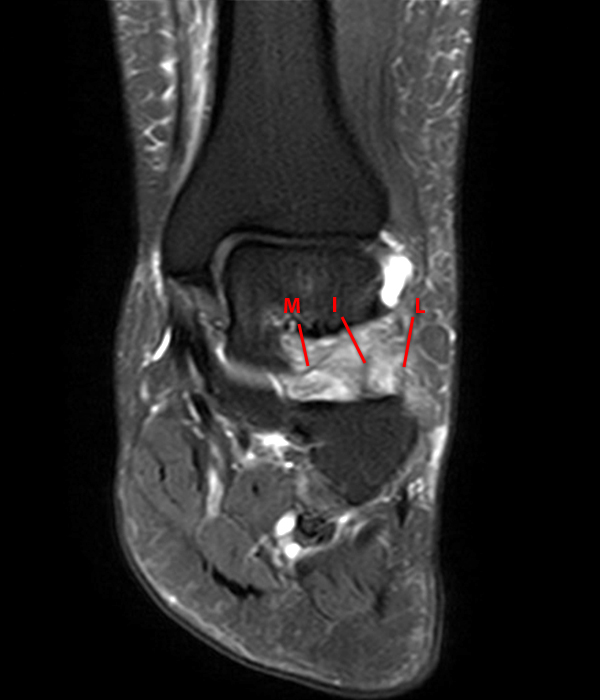
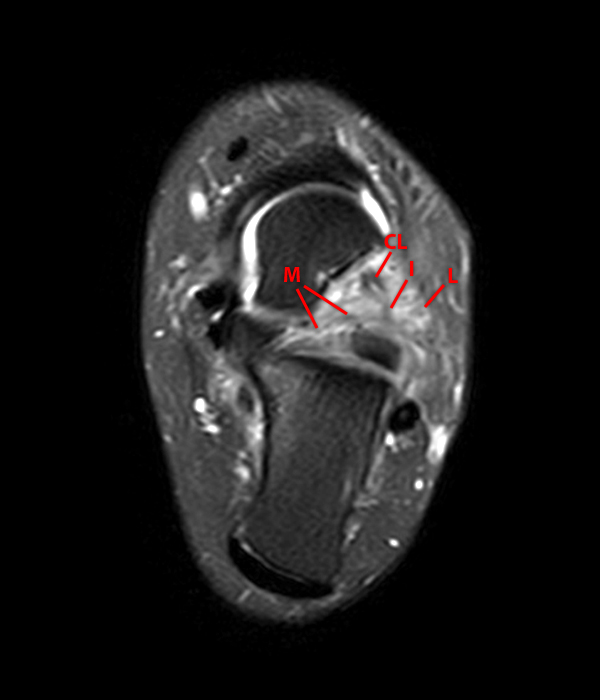
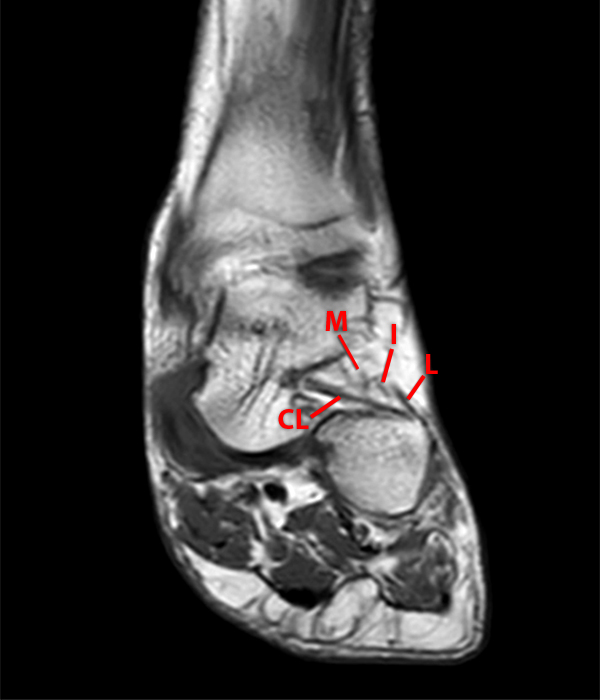
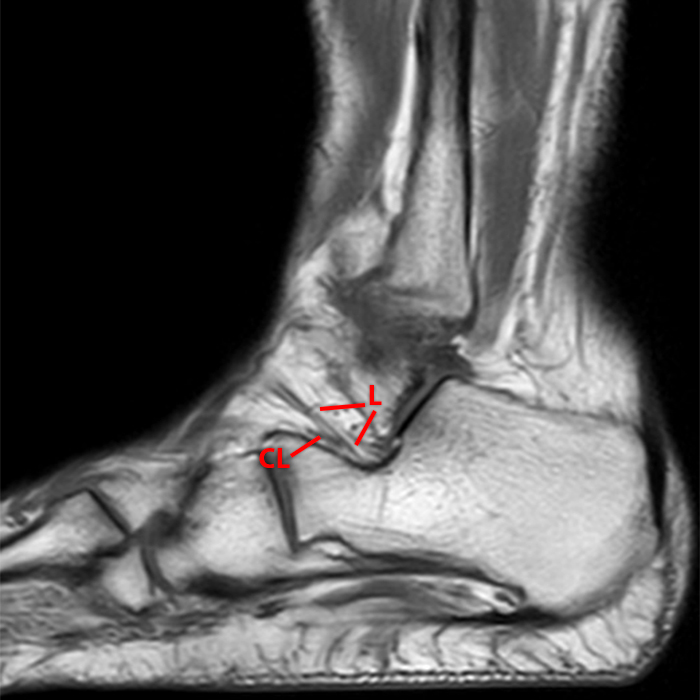
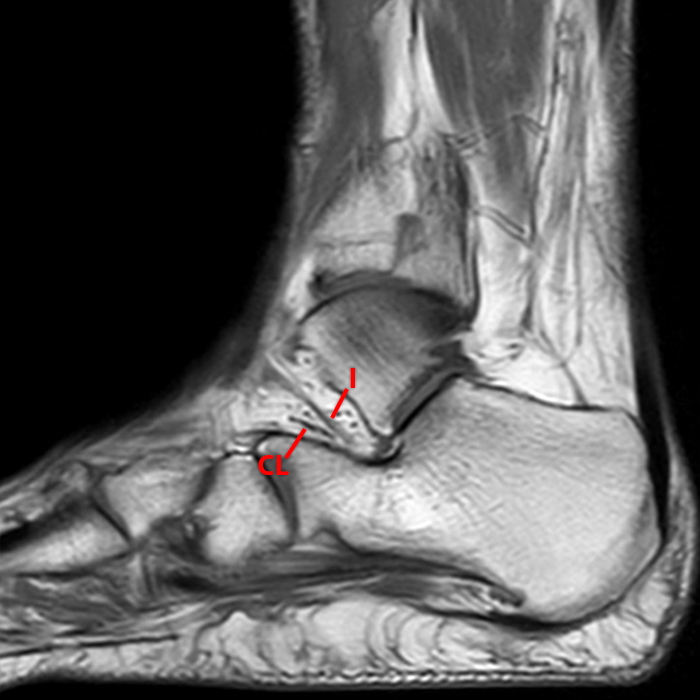
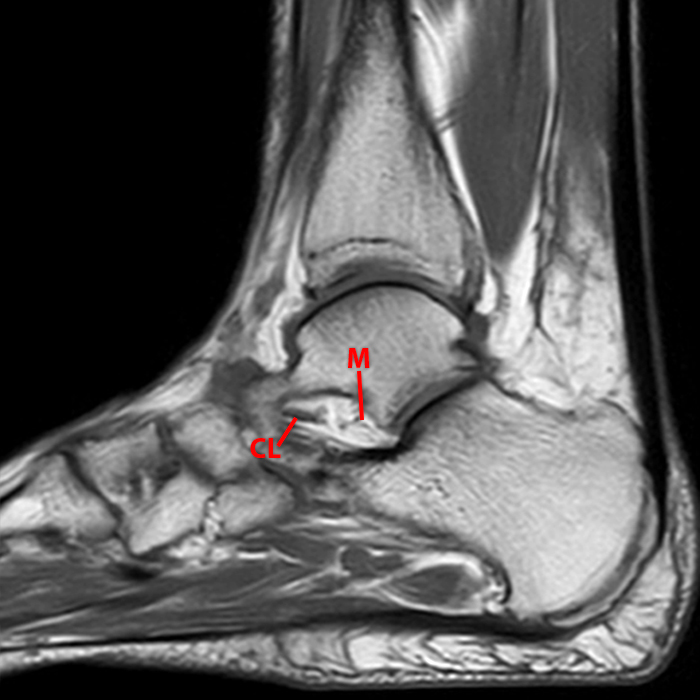
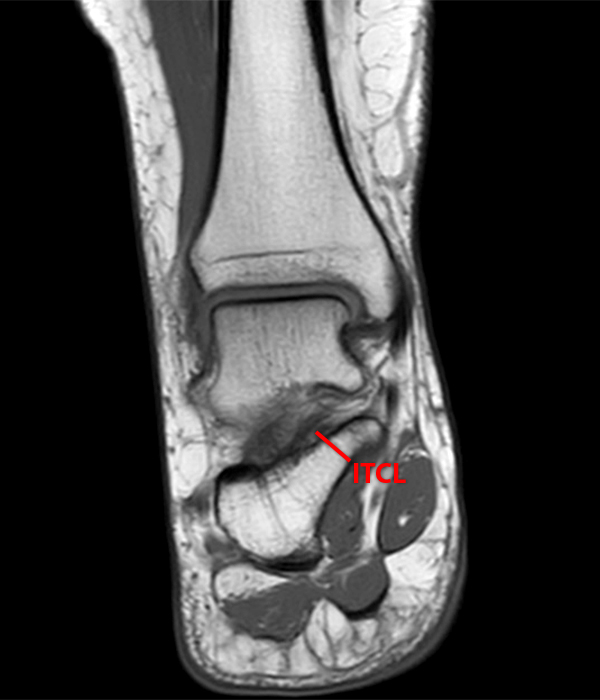
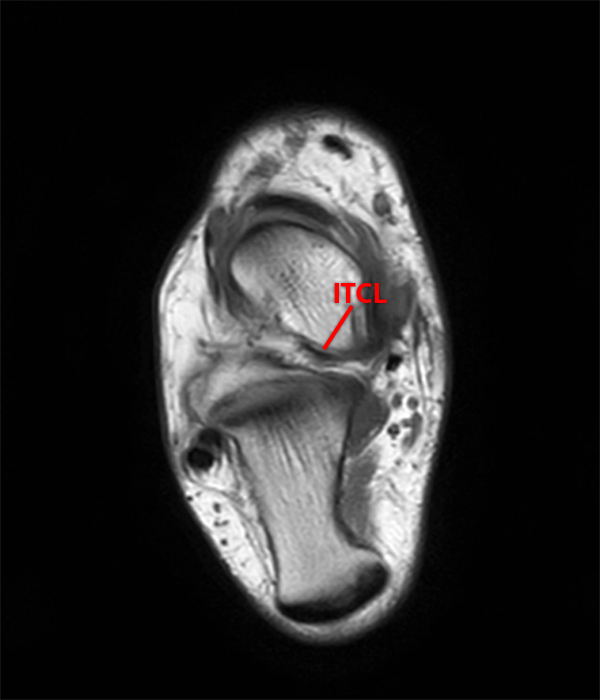
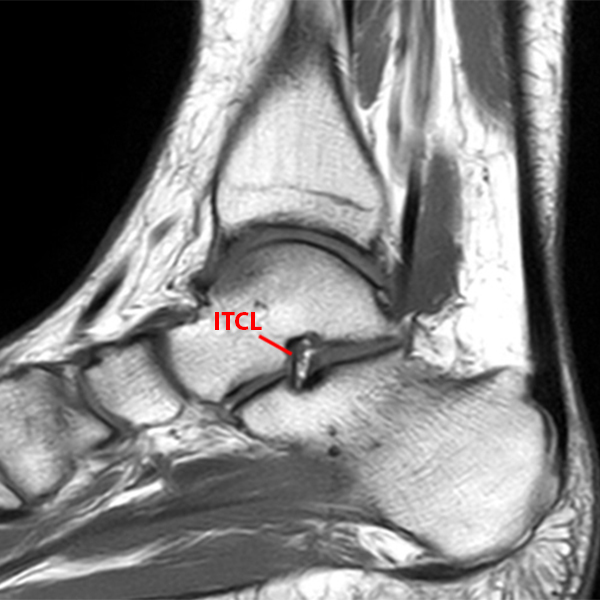
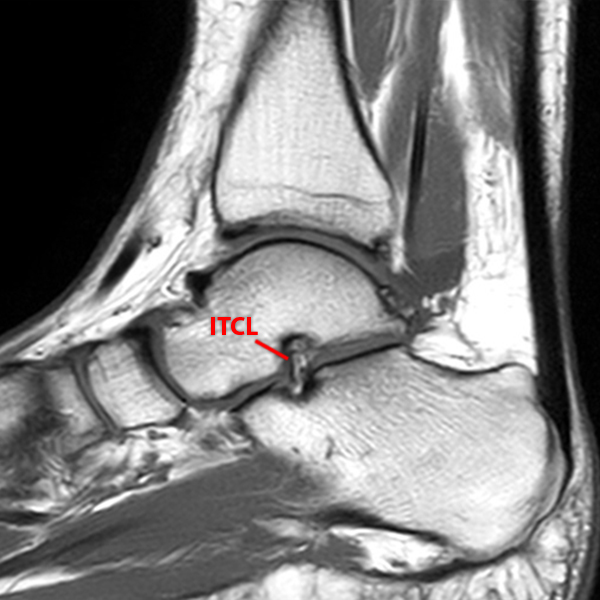
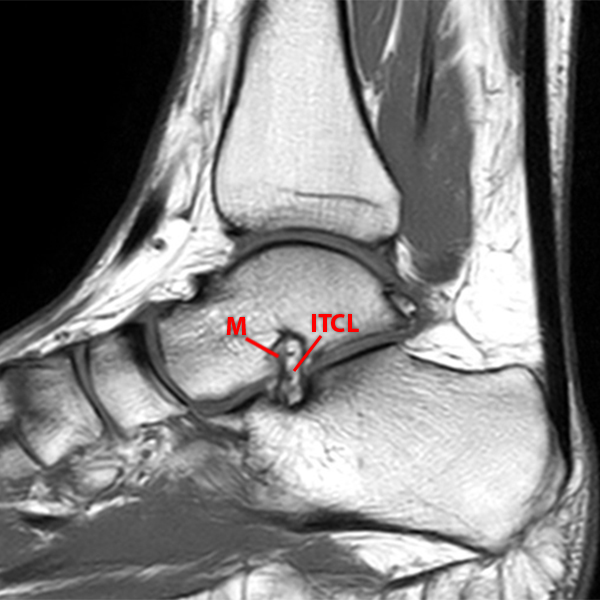
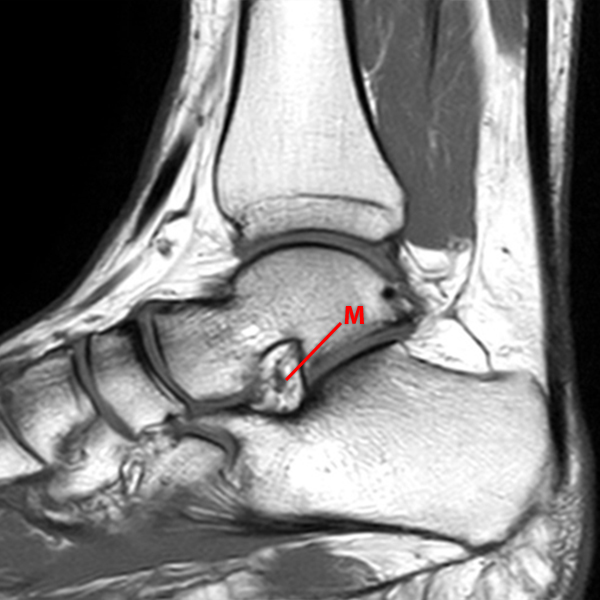
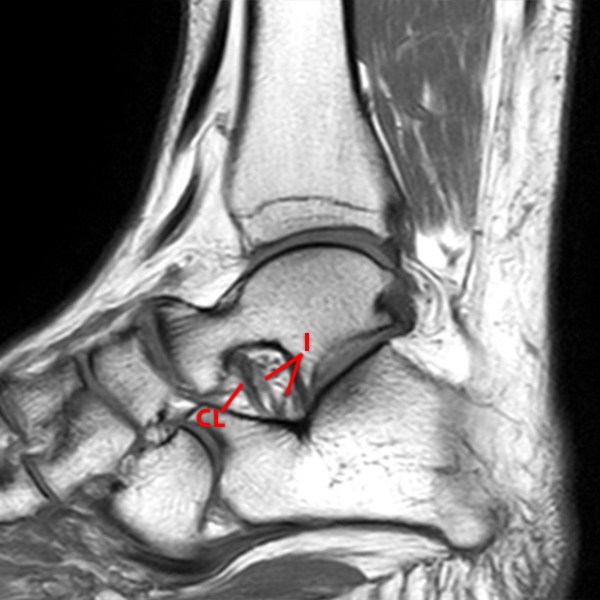
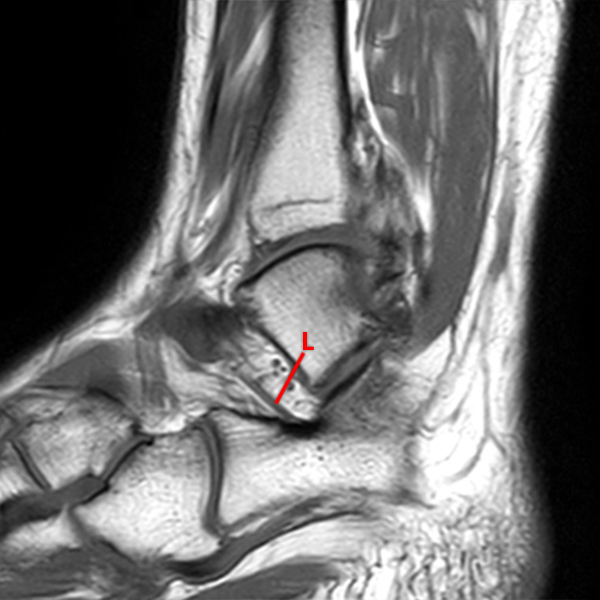
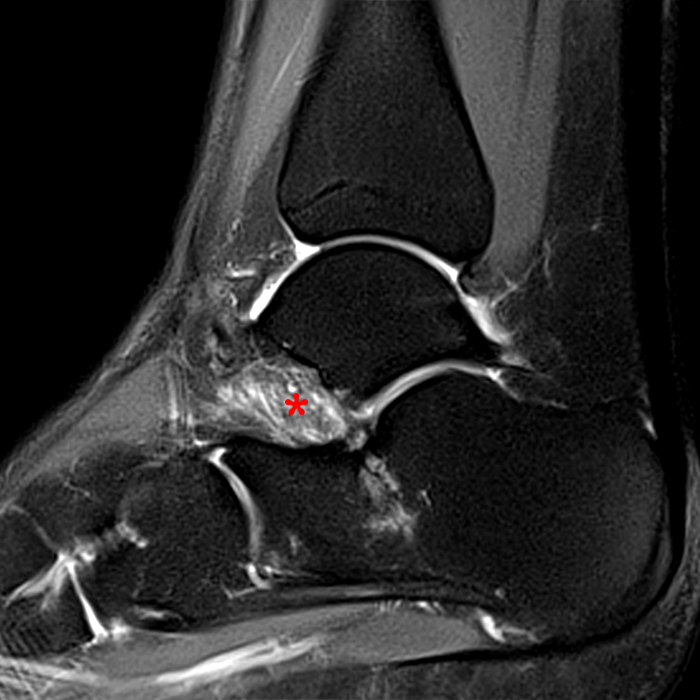
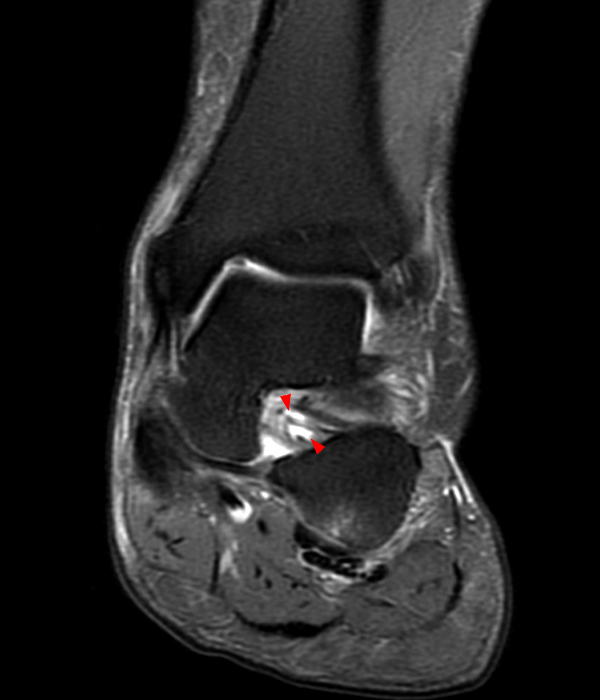
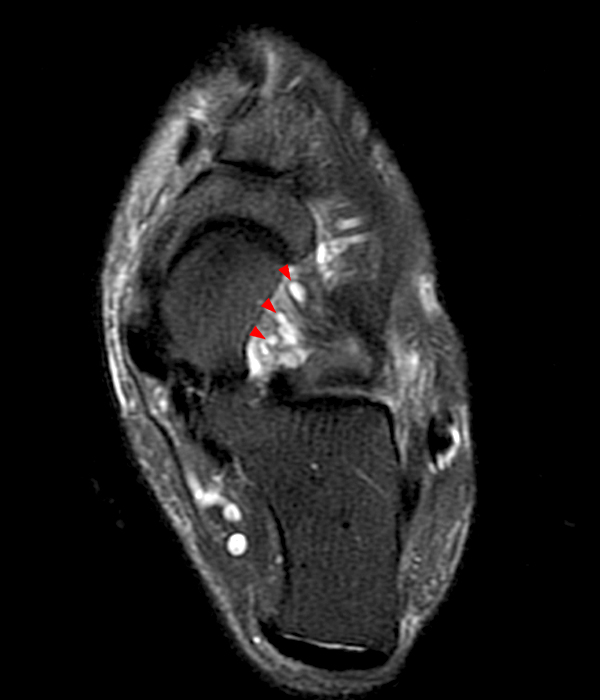
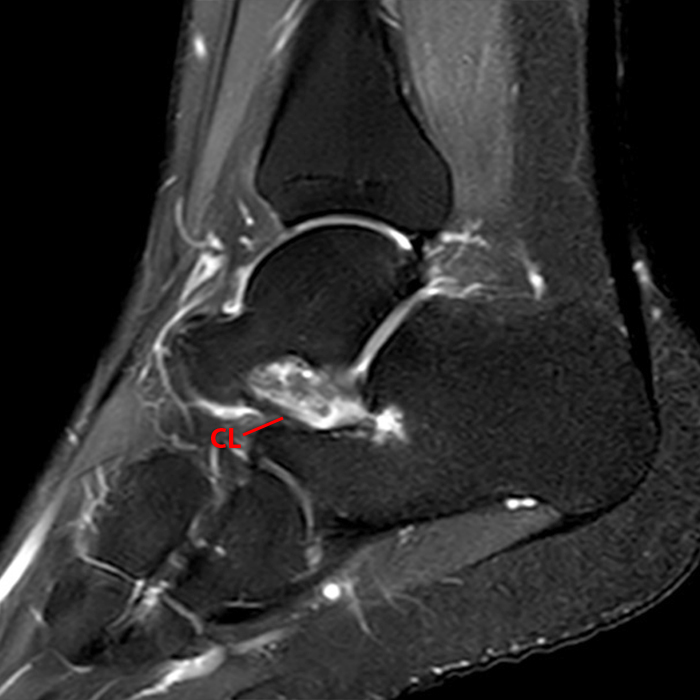
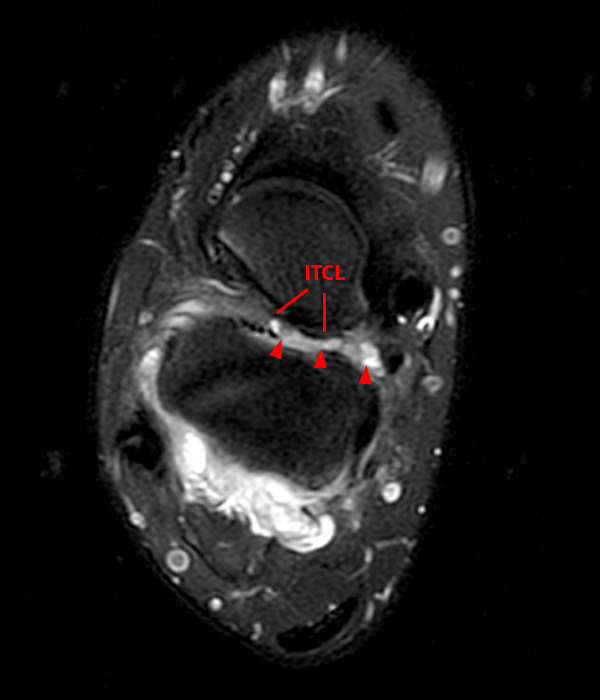
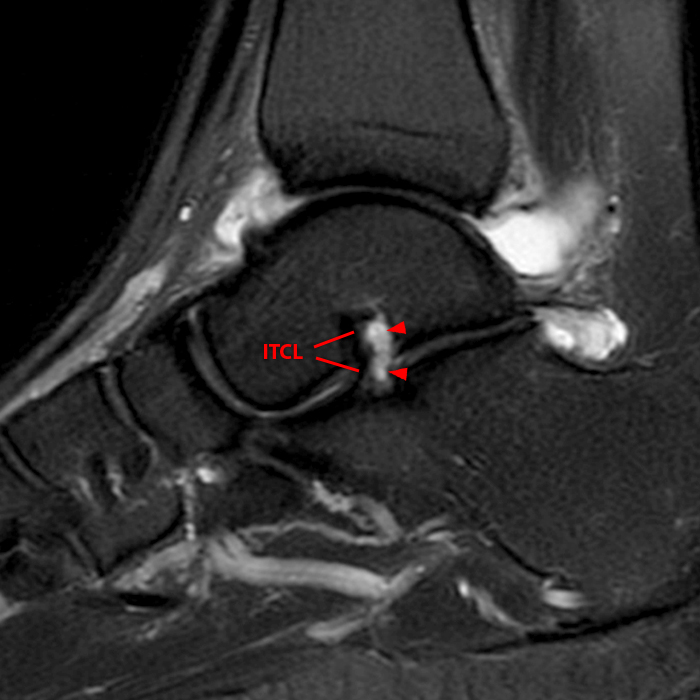
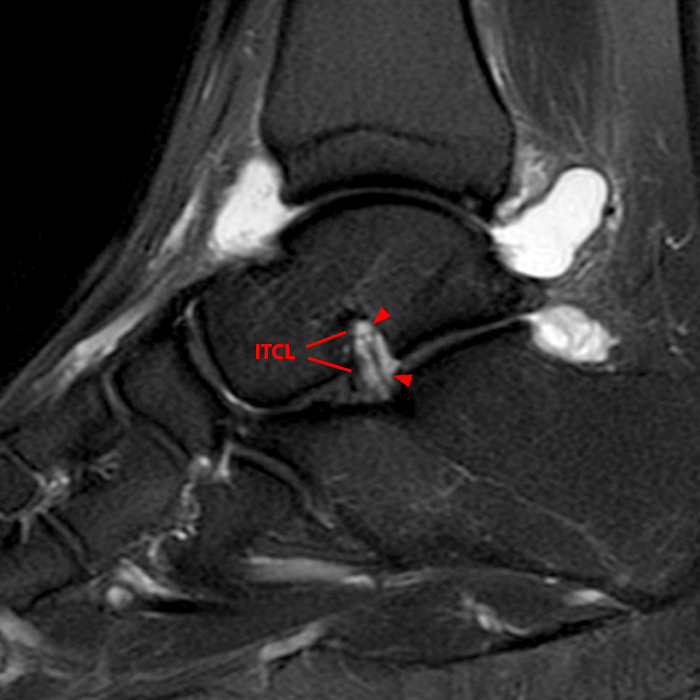
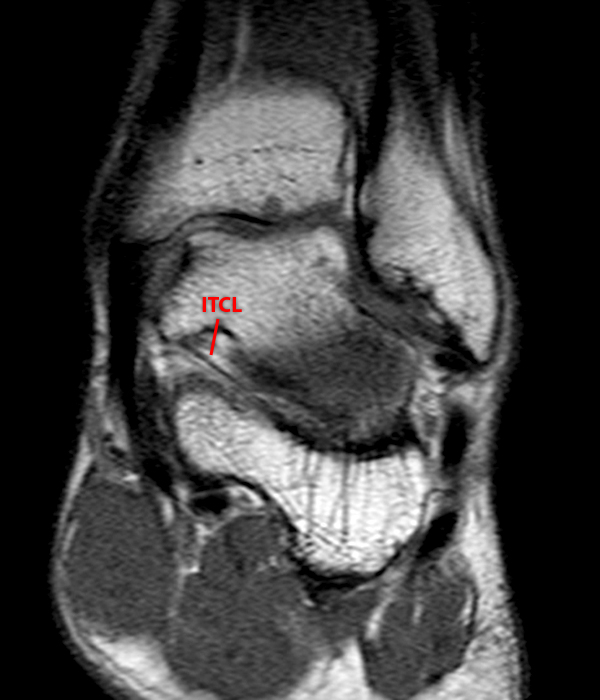
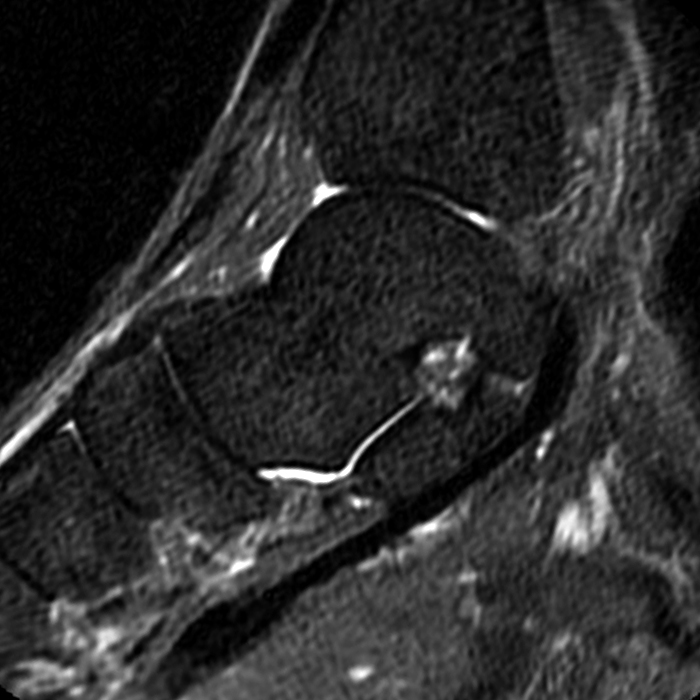
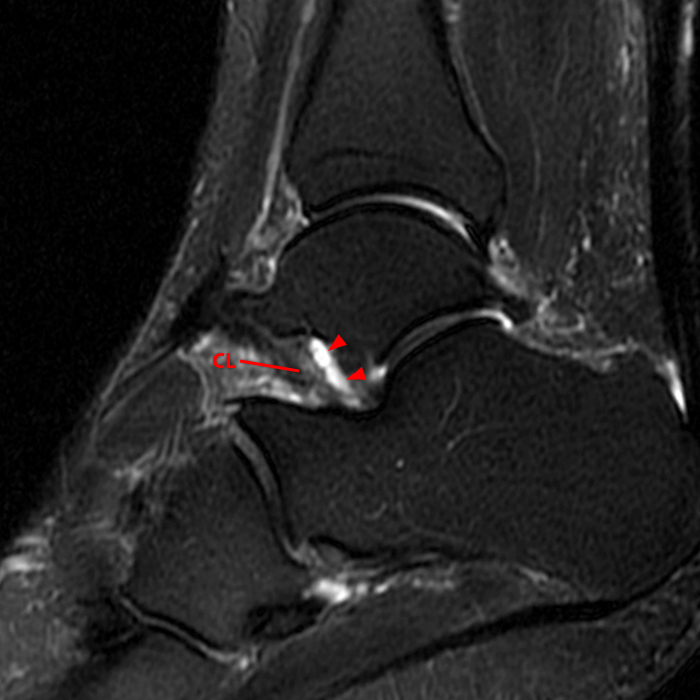
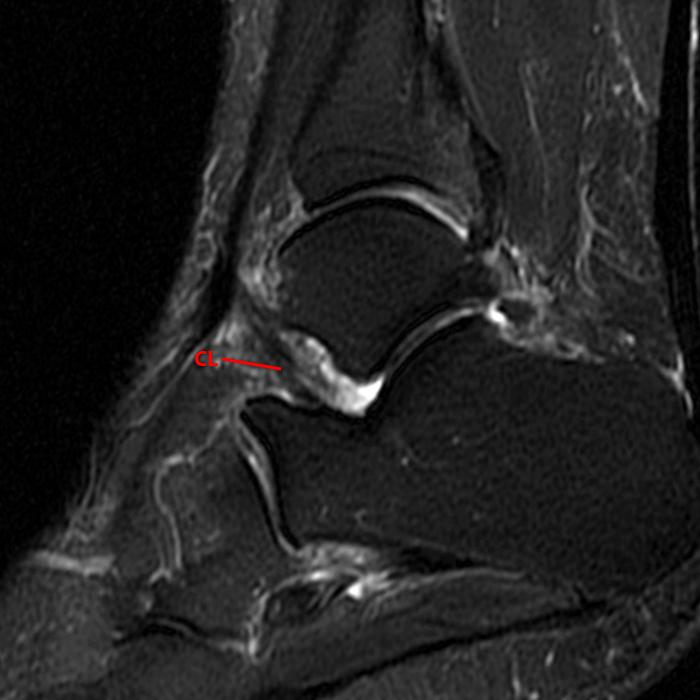
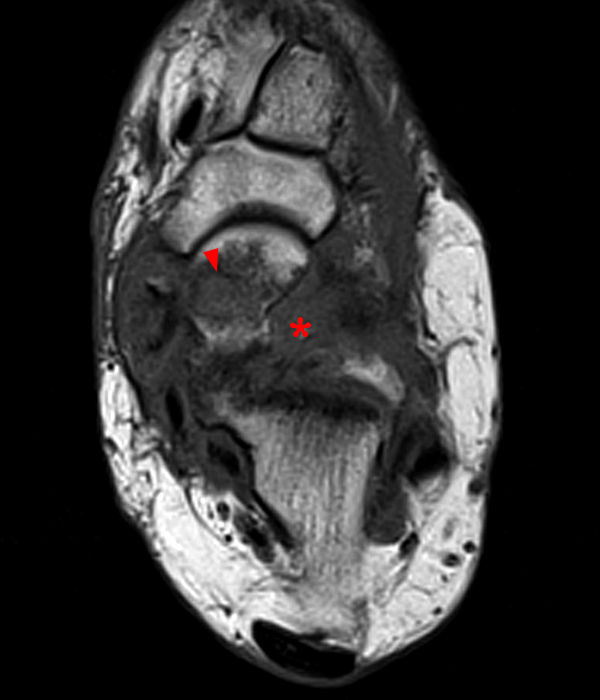
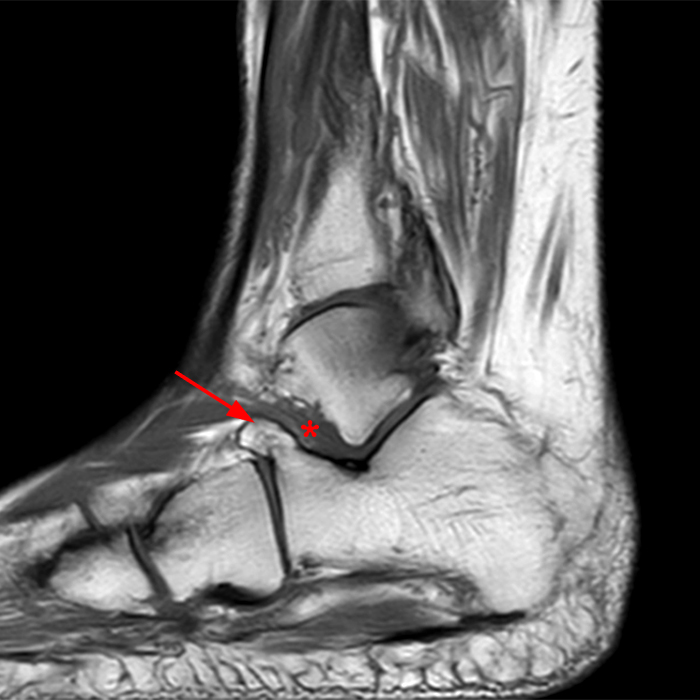
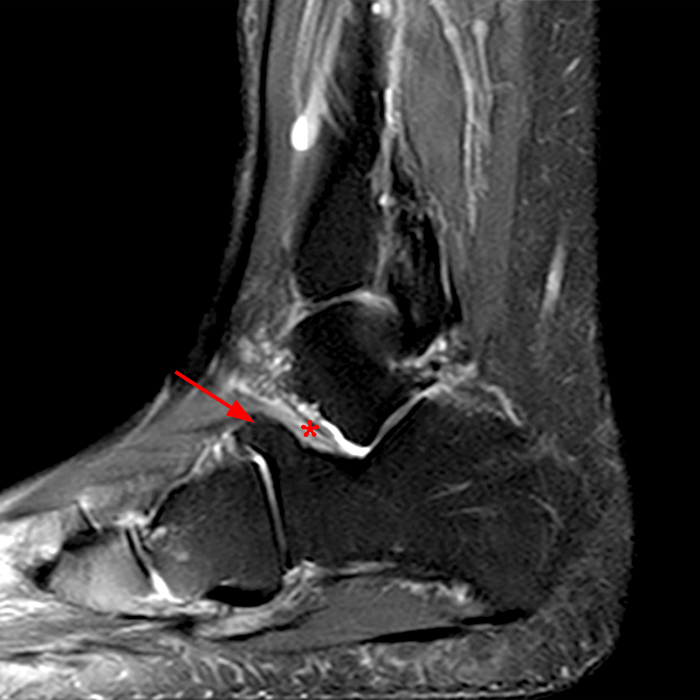
Sagittal (Images 2A and 2B), coronal (Images 2C and 2D), and axial (Image 2E) images through the sinus tarsi demonstrate diffuse soft tissue edema in the sinus. The cervical ligament (CL), intermediate (I) and lateral (L) roots of the inferior extensor retinaculum are increased in signal and not well defined, consistent with sprains.
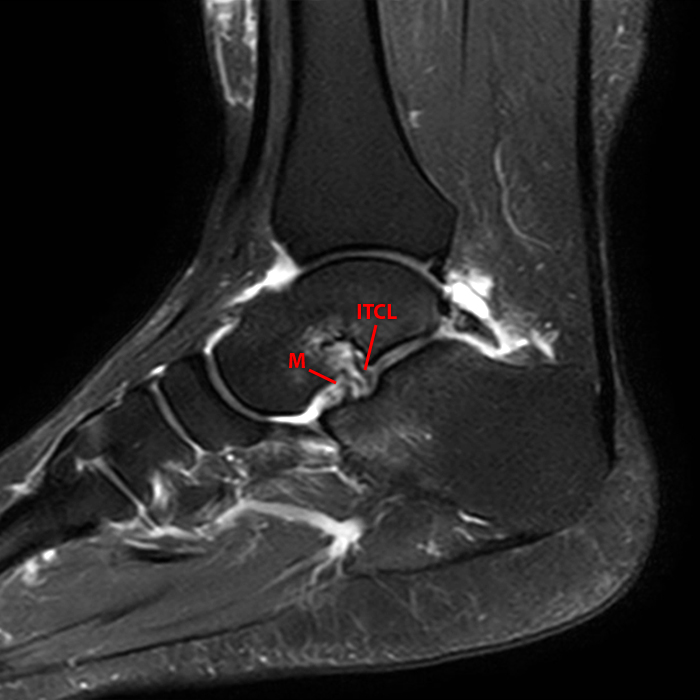
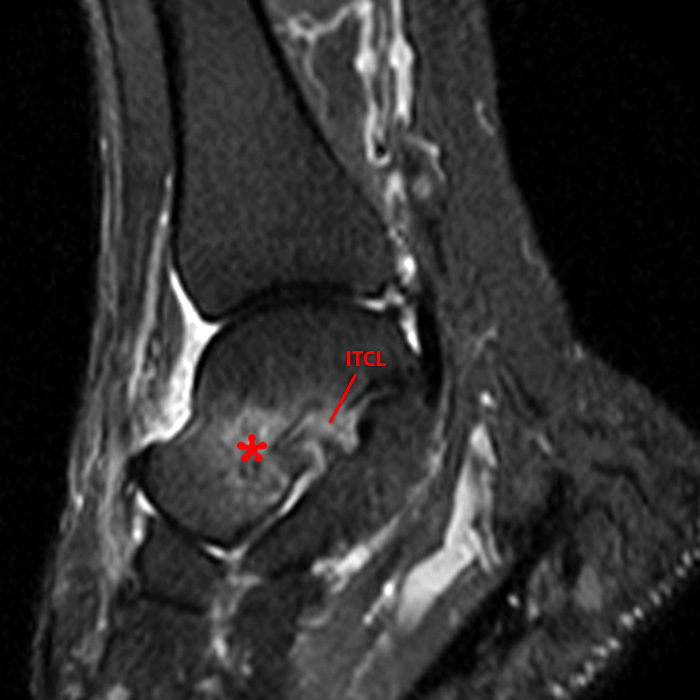
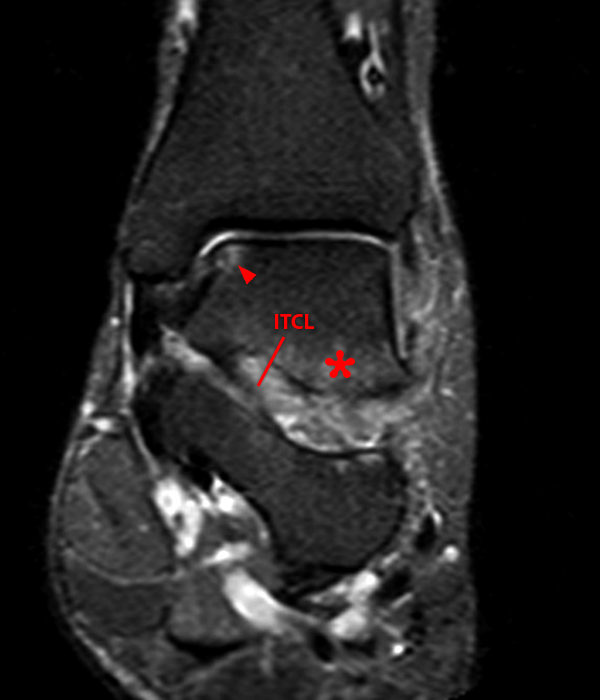
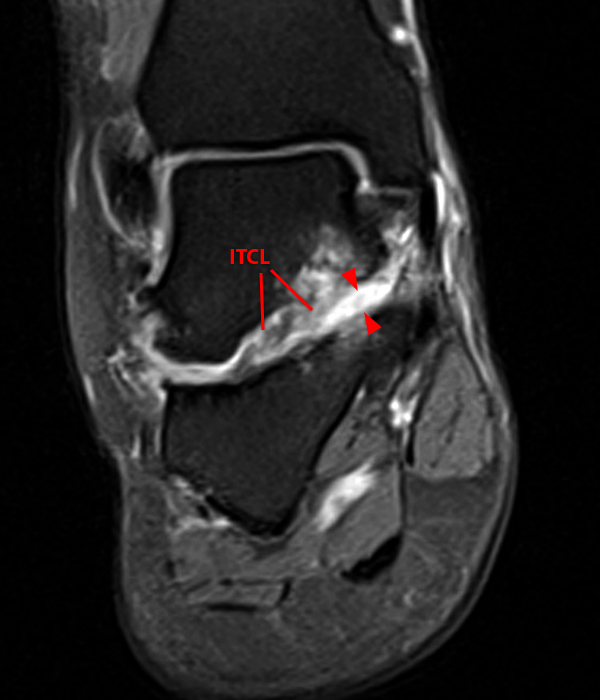
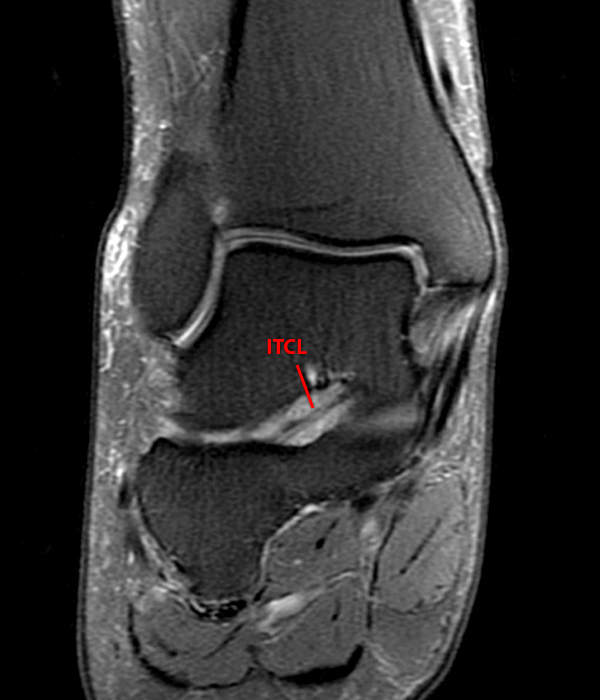
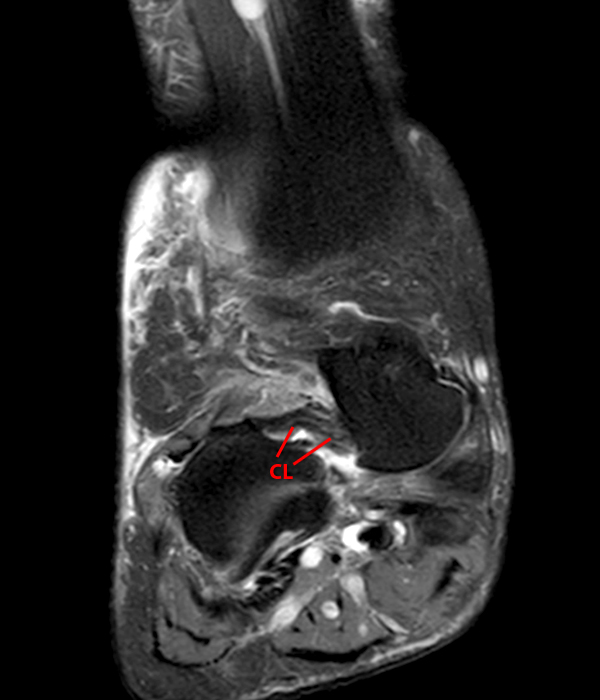
A more medially located sagittal image (Image 2F) visualizes part of the tarsal canal. Edema extends into the tarsal canal, with irregularity of the interosseous talocalcaneal ligament (ITCL) and medial (M) root of the inferior extensor retinaculum indicating sprain of both ligaments.
Diagnosis
These MRI findings are consistent with posttraumatic sinus tarsi syndrome.
Introduction
The sinus tarsi syndrome was first described in the medical literature in 1958.1 Overall incidence is unknown, but it is generally considered uncommon and without consistent gender predilection.2,3
Components of the sinus tarsi syndrome include lateral hindfoot pain, tenderness to palpation over the sinus tarsi, a sensation of instability in the hindfoot, and relief by injection of local anesthetic into the sinus.2,3,4,5 Patients typically present in the third to fourth decade of life with a history of ankle sprain. Zwipp et al. described a more severe variant called the canalis tarsi syndrome, which includes medial hindfoot pain in addition to the typical lateral symptoms.5
Taillard et al. reported approximately 70% of the patients in their literature review were posttraumatic; the remainder were due to inflammatory or crystal deposition arthritis, foot deformity, or chronic hindfoot instability.4 On a retrospective series of sinus tarsi abnormalities detected on MRI, 79% of patients had concomitant lateral ankle ligament abnormalities; there was also an association with posterior tibial tendon tears.6
Anatomy
The sinus tarsi, also known as the tarsal sinus, is defined as the anatomical space between the neck of the talus and anterosuperior calcaneus. It is roughly cone-shaped, with the wider portion directed anteriorly and laterally. The medial portion of the sinus narrows to a transverse cylindrical space called the tarsal canal (or canali tarsi), which terminates posterior to the sustentaculum tali of the calcaneus. The sinus tarsi and canali tarsi divide the subtalar (talocalcaneal) joint into the anterior and posterior compartments.7,8,9,10
Contents of the sinus tarsi include ligaments, adipose connective tissue, branches of the peroneal and posterior tibial arteries which anastomose in the sinus, the cutaneous dorsolateral nerve (a branch of the superficial peroneal nerve), and proprioceptive nerve endings.11
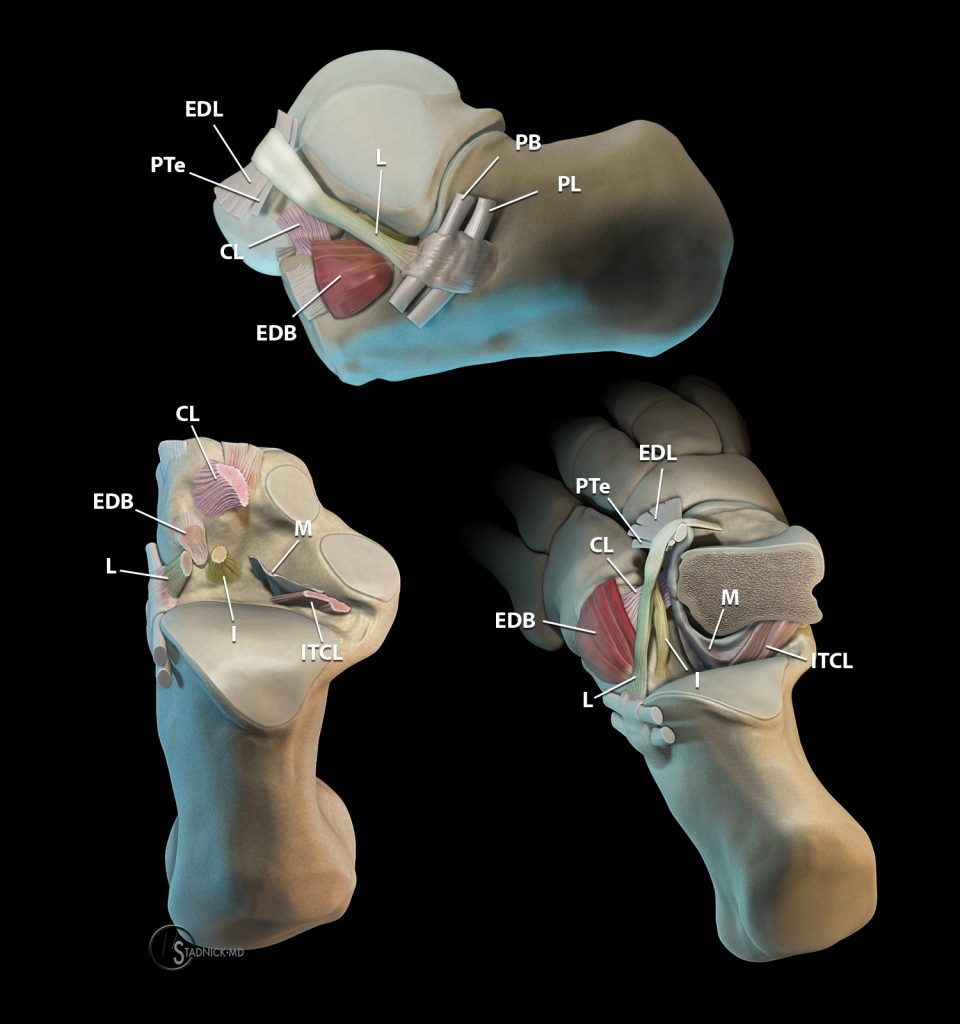
Most authors describe five ligaments in the sinus tarsi (Image 3): The interosseous ligament, the cervical ligament, and the medial, intermediate, and lateral roots of the inferior extensor retinaculum.
- The most medial ligament is the interosseous talocalcaneal ligament (abbreviated as ITCL or interosseous ligament); other names for this ligament in the literature include the talocalcaneal ligament or ligament of the tarsal canal. The interosseous ligament extends between the talus and calcaneus in the tarsal canal, and functions to stabilize the subtalar joint.11,12,13
- The cervical ligament (also called the Fick ligament, oblique talocalcaneal ligament, or lateral talocalcaneal ligament) is located anterior and lateral to the interosseous ligament. It attaches to inferolateral talar neck and dorsal neck of the calcaneus. The cervical ligament limits inversion, and also stabilizes the subtalar joint.11,12,13
- The roots of the inferior extensor retinaculum anchor the lateral stem of the retinaculum to the calcaneus, restricting excursion of the extensor tendons and limiting ankle inversion. The medial root of the inferior extensor retinaculum is located posterior and medial to the cervical ligament, attaching to the calcaneus at the floor of the medial sinus, often merging with the calcaneal attachment of the interosseous ligament.11,12,13
- The intermediate root of the inferior extensor retinaculum. Also called the intermediary root, this structure attaches to the calcaneus just posterior to the cervical ligament, coursing anteriorly and superiorly over the medial margin of the extensor digitorum longus tendon.11,12,13
- The lateral root of the inferior extensor retinaculum. This structure loops around the lateral margin of the extensor digitorum longus tendon, merging with the intermediate root to form a sling-like structure over the tendon. The lateral fibers course posteriorly and laterally, attaching to the lateral cortex of the calcaneus or blending with the deep fascia.11,12,13
Figure 3:
3D renders illustrate the major ligamentous structures within the sinus tarsi region including the interosseous talocalcaneal ligament (ITCL), the lateral (L), intermediate (I), and medial (M) roots of the inferior extensor retinaculum, and the cervical ligament (CL). The extensor digitorum brevis (EDB) and extensor digitorum longus (EDL) muscles, and the peroneus tertius (PTe), peroneus brevis (PT), and peroneus longus (PL) tendons are also labeled.
Kjaersgaard et al. reported that experimental cutting of the interosseous and cervical ligaments in cadaver specimens resulted in mild subtalar instability, with increased range of motion less than 2.6 degrees in any plane.14 Disruption of the interosseous ligament resulted in the largest degree of abnormal motion in their series. This correlates with a high incidence of interosseous ligament tears at surgery for sinus tarsi syndrome; 10 out of 14 patients (71%) reported by Frey et al.15 and 29 of 33 patients (88%) reported by Lee et al.16 were found to have complete or partial tears of the interosseous ligament. The interosseous ligament therefore appears to be the most functionally important of the sinus tarsi ligaments, experimentally and clinically.
On MR imaging of the normal sinus tarsi, the ligaments are usually best seen on T1-weighted or non-fat suppressed proton density-weighted images, appearing as dark linear structures outlined by hyperintense fat signal. If there is significant edema in the sinus, the ligaments may be better visualized on fat suppressed intermediate or T2-weighted images, being outlined by T2-hyperintense edema.10,17
Case 2 – Normal MRI anatomy of the cervical ligament and roots of the inferior extensor retinaculum in a 60 year old female. A coronal T1-weighted image (Image 4A) includes most of the cervical ligament coursing from superomedial to inferolateral, surrounded by fat signal. Superior to the cervical ligament, 3 hypointense foci correspond to the medial, intermediate, and lateral roots of the inferior extensor retinaculum. Contiguous sagittal T1-weighted images in the same patient from lateral to medial (Images 4B through 4E) show the cervical ligament (CL) anteriorly in the sinus, with the lateral root (L) on image 4B, intermediate root (I) on 4C, and portions of the medial root (M) on images 4D and 4E.
The sinus tarsi ligaments are often oblique to the imaging planes obtained on MR imaging, and therefore will be visualized in cross section on contiguous slices. Occasionally the coronal images will visualize most of the cervical or interosseous ligaments on a single slice. Similarly, sagittal images may include most of the intermediate or lateral roots of the inferior extensor retinaculum on a single image. (Cases 2 and 3)
Case 3- Normal anatomy of the sinus tarsi ligaments in a 39 year-old female. Coronal (Image 5A) and axial (Image 5B) T1-weighted images through the tarsal canal and sinus tarsi visualize most of the interosseous talocalcaneal ligament (ITCL) on single slices. Contiguous sagittal T1-weighted images from medial to lateral (Images 5C through 5J) include the interosseous talocalcaneal ligament (Images 5C-5E), medial root (M) of the inferior extensor retinaculum (Image 5F-5G), intermediate root (I) of the inferior extensor retinaculum (Images 5H and 5I), and lateral root (L) of the inferior extensor retinaculum (Image 5J). The cervical ligament (CL) is visible anterior to the roots of the inferior extensor retinaculum on Images 5G through 5I.
Pathology
While the clinical features of sinus tarsi syndrome are well-defined, the underlying cause of symptoms appears to be heterogeneous and multifactorial. Because most cases are posttraumatic, many authors have theorized that sprains of the interosseous and/or cervical ligaments leads to subtalar joint instability and excessive force transmitted into the sinus tarsi. This causes inflammation, synovitis, hemosiderin deposition, and fibrosis in the sinus, resulting in pain and tenderness.3,4,5,6,15,18
However, up to 30% of patients with sinus tarsi syndrome do not report significant injury. Numerous alternative etiologies have been proposed in the literature, including irritation or damage to the proprioceptive and nociceptive nerve endings in the sinus, hypertrophy of adipose tissue in the sinus, synovial herniation or protrusion into the sinus from the adjacent subtalar joints, impeded venous outflow from the sinus, or compression of the sinus due to alteration of hindfoot alignment. Space occupying lesions in the sinus such as ganglion cyst or tumor; and inflammatory processes such as crystal deposition arthropathy, inflammatory arthritis, or PVNS have been reported to cause sinus tarsi syndrome.6,18
Because of the heterogeneity of reported causes, some authors have even questioned the use of the term “sinus tarsi syndrome” and advocated its replacement by more specific diagnoses such as interosseous ligament tear, arthrofibrosis, or subtalar arthritis.15 Currently, however, the terminology is still considered useful, since most patients will respond to conservative therapy and identifying a specific underlying etiology is not required for effective treatment of these patients.19
Imaging Findings
MRI is considered the best imaging modality for evaluation of the sinus tarsi and surrounding structures. Radiographs are usually normal, though subtalar arthrosis may be radiographically visible in some patients. Arthrography is invasive and relatively insensitive compared to MRI.6,11,20,21,22
Ultrasound evaluation of the sinus is feasible, although published reports are limited. Hypoechoic regions in the sinus on ultrasound have been reported to correlate with edema-like signal on MRI in a patient with clinical sinus tarsi syndrome.23,24
Nuclear medicine bone scan can demonstrate increased activity in the midfoot on perfusion and blood pool imaging, with localization to the subtalar region on SPECT.25,26 CT can provide excellent osseous evaluation, but is not as sensitive as MRI for soft tissue lesions.
Soft tissue edema in the sinus due to contusion or inflammation is commonly seen after trauma, resulting in diffusely increased signal throughout the sinus on fat suppressed fluid sensitive MR images. Diffuse edema may coalesce into small cysts in the sinus. (Cases 4 and 5)
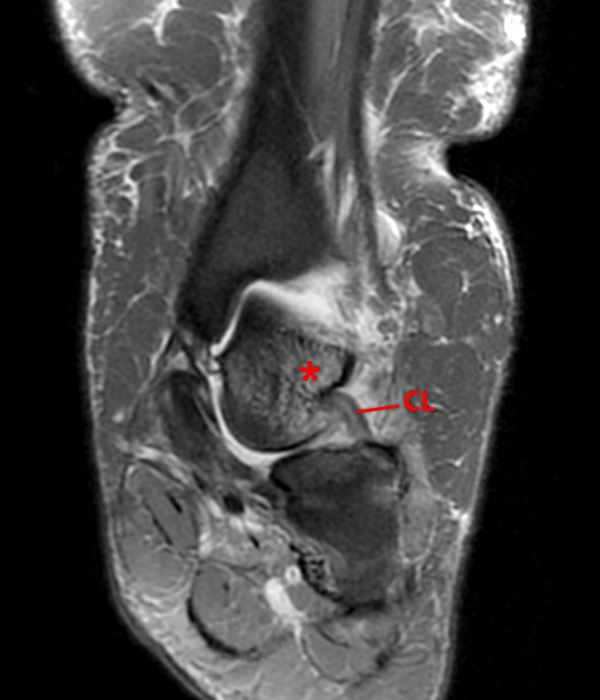
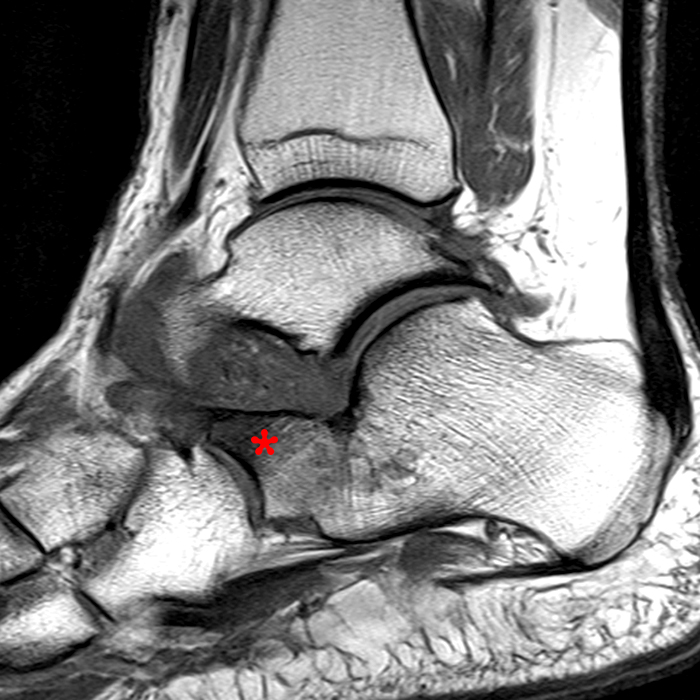
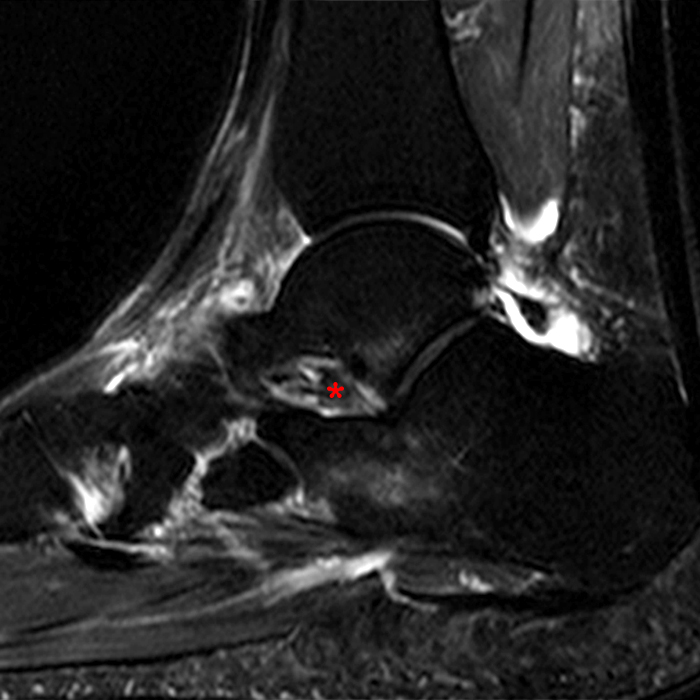
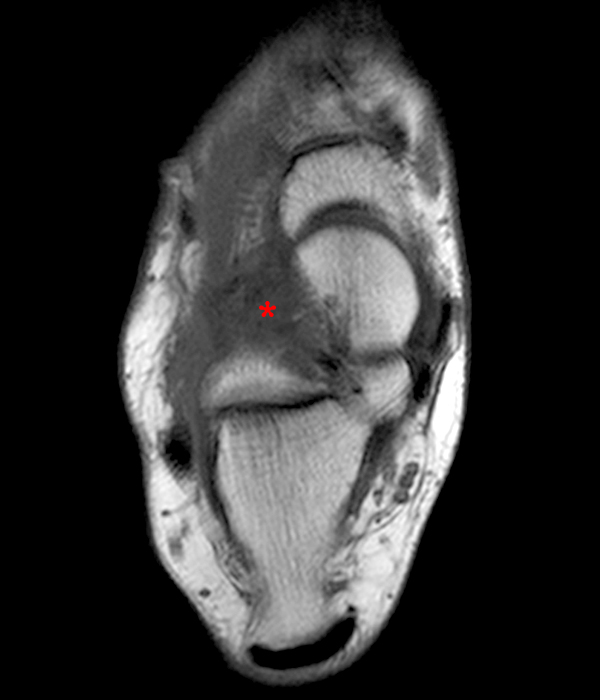
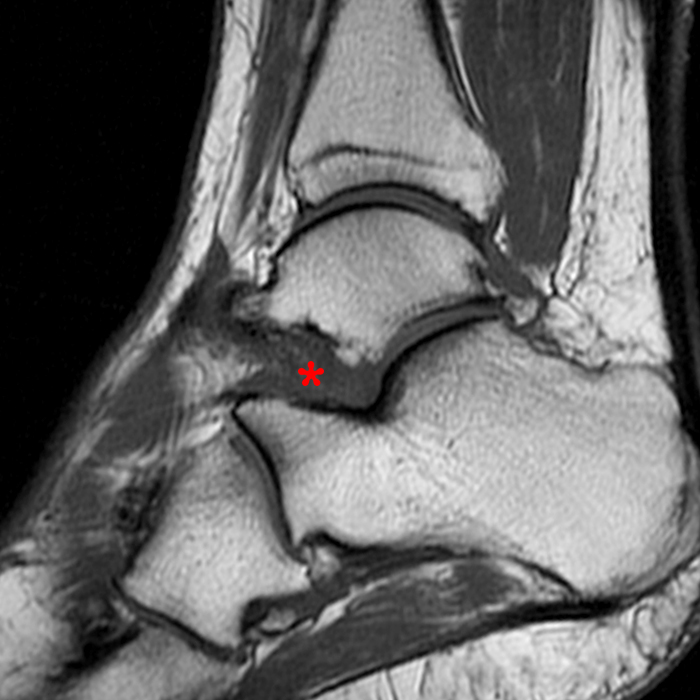
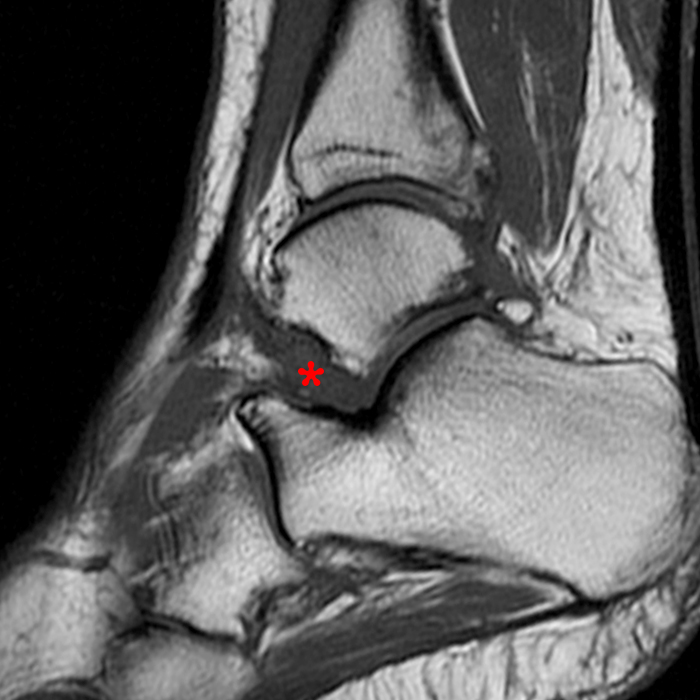
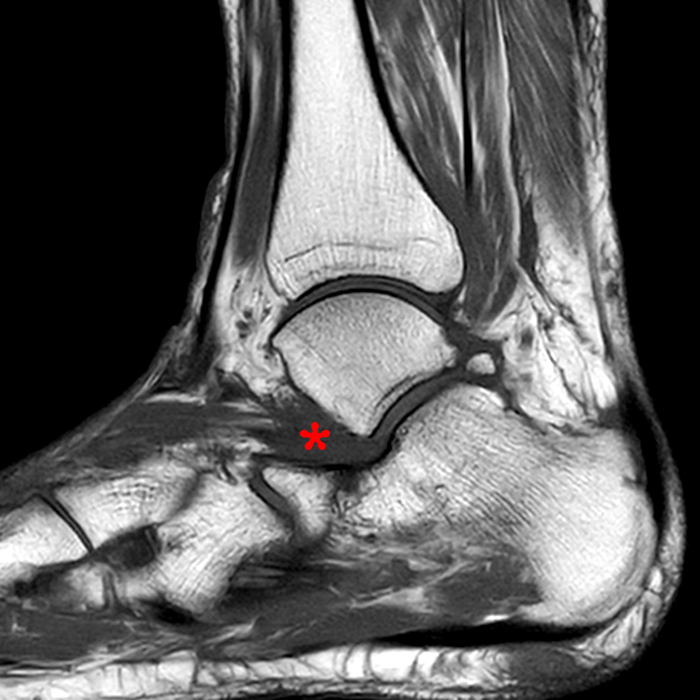
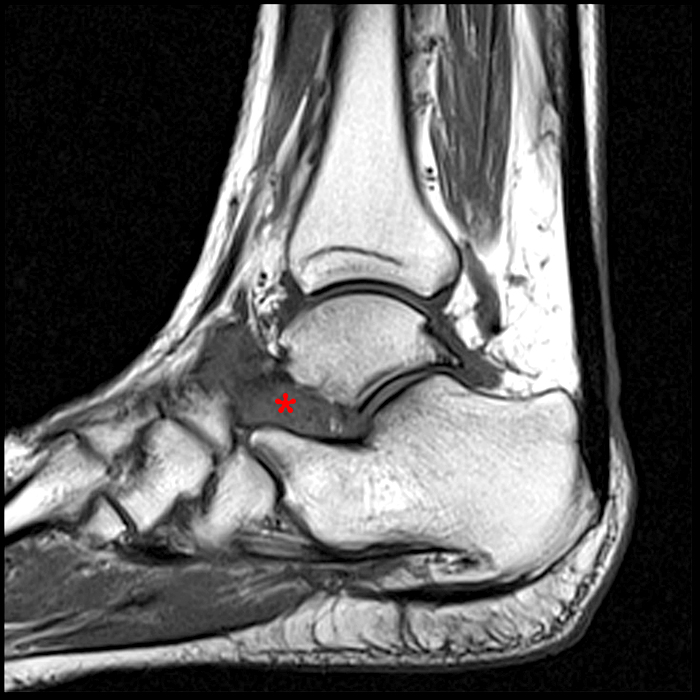
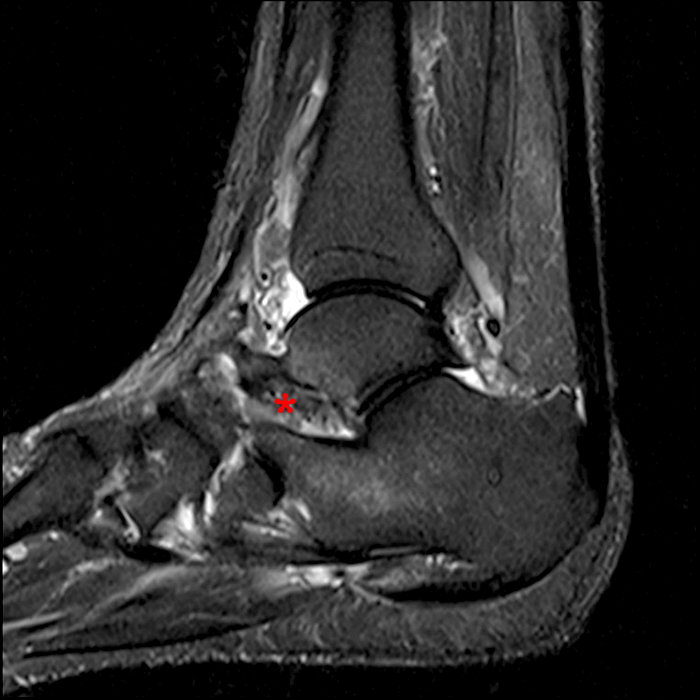
Case 4 – Acute injury in a 19 year old female, right ankle trauma 3 days ago. Sagittal T1-weighted (Image 6A) and fat suppressed fast spin-echo T2-weighted (Image 6B) images demonstrate mild edema (asterisk) in the sinus tarsi adjacent to the cervical ligament (CL) and roots of the inferior extensor retinaculum (arrow), without evidence for ligament disruption.
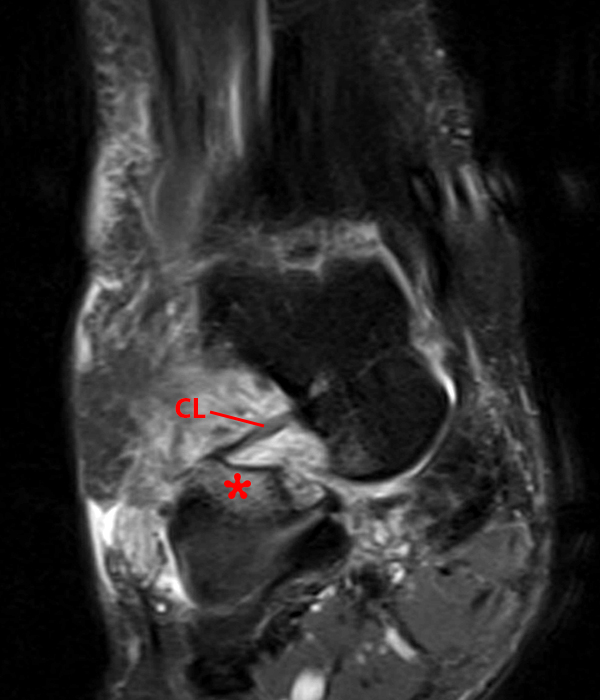
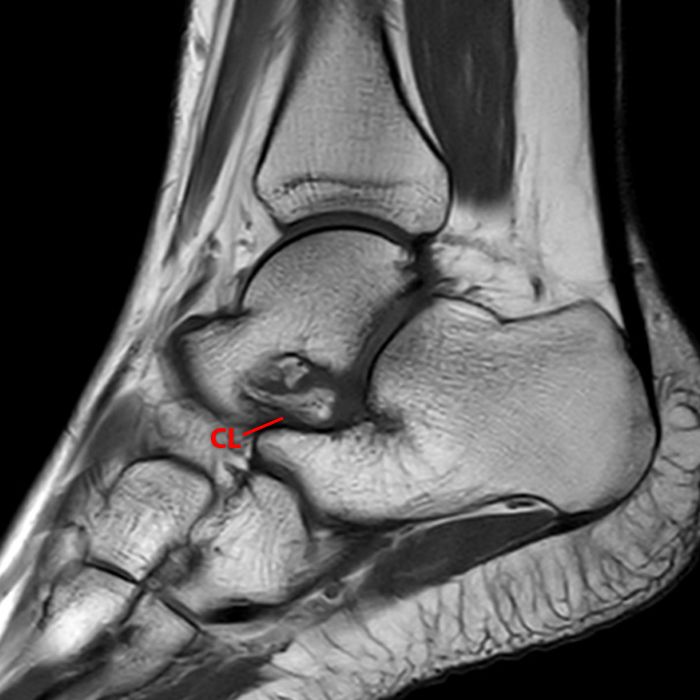
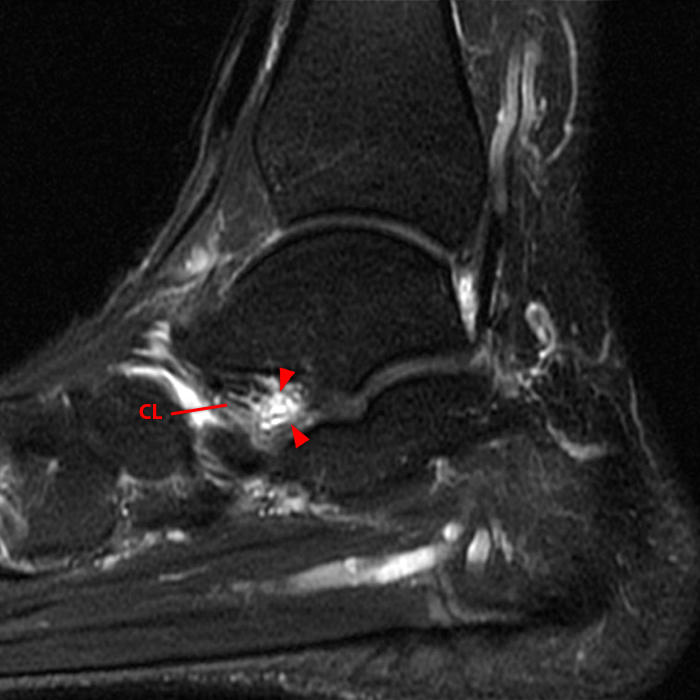
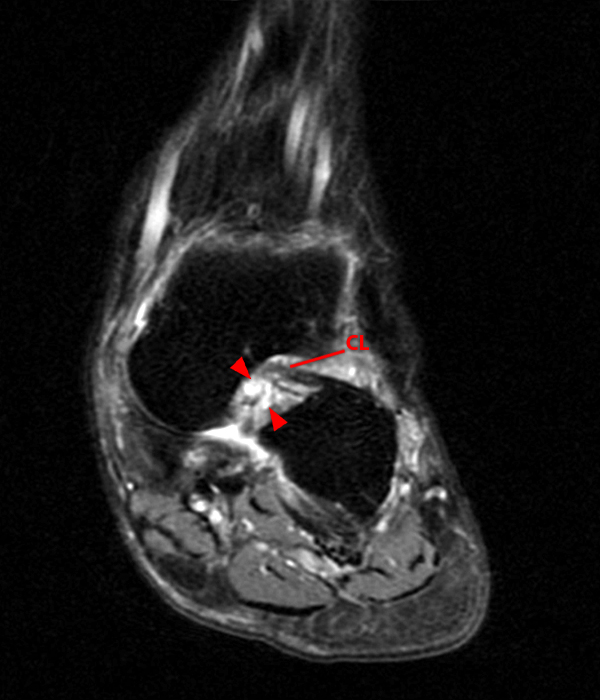
Case 5 – Acute injury in a 52 year-old female, s/p fall 1 week ago with lateral hindfoot pain. Sagittal (Image 7A), coronal (Image 7B), and axial (Image 7C) fat-suppressed fast spin-echo T2-weighted images reveal small cysts (arrowheads) and edema adjacent to the cervical ligament and roots of the inferior extensor retinaculum, without disruption of the ligaments.
Sinus tarsi ligament injury can be visualized on MRI as thickening and increased intrasubstance signal, attenuation, or discontinuity. (Cases 6 through 10) Fibrosis with amorphous T1- and T2-hypointense material occupying part or all of the sinus is frequently seen in chronic sinus tarsi syndrome, but is relatively nonspecific.6,11,20,21,22 (Cases 11 and 12)
Case 6 – Acute injury with cervical ligament sprain. 52 year-old female with direct trauma to the left foot 2 days ago. The cervical ligament (CL) is thickened and increased in signal with surrounding soft tissue edema on sagittal T1-weighted (Image 8A), sagittal fast spin-echo T2-weighted (Image 8B), and coronal fat suppressed fast spin-echo T2-weighted (Image 8C) images. A bone contusion is also visible in the lateral talus (asterisks).
Case 7 – Acute injury with sprain of the cervical ligament and roots of the inferior extensor retinaculum. 35 year-old male with fall 3 days ago. Sagittal T1-weighted (Image 9A), fat suppressed fast spin-echo T2-weighted (Image 9B), and coronal fat suppressed fast spin-echo T2-weighted (Image 9C) images reveal edema and fluid signal in the sinus tarsi. The cervical ligament (CL) and intermediate (I) root of the inferior extensor retinaculum are increased in signal, consistent with sprain. A bone contusion is present in the anterior calcaneus (asterisks).
Case 8 – Subacute injury with tear of the roots of the inferior extensor retinaculum in a 17 year-old male. Previous trauma 6 weeks ago. Sagittal T1-weighted (Image 10A), fat suppressed fast spin-echo T2-weighted (Image 10B), and coronal fat suppressed fast spin-echo T2-weighted (Image 10C) images show mild increased signal in the cervical ligament (CL), consistent with sprain. Edema and fluid intensity signal are present in the sinus tarsi posterior to the cervical ligament. The roots of the inferior extensor retinaculum are not identifiable, consistent with tear.
Case 9 – Acute sprain of the interosseous ligament in a 65 year-old female, injury 1 week prior to MRI. Sagittal (Image 11A) and coronal (Image 11B) fat suppressed fast spin-echo T2-weighted images demonstrate increased signal in the interosseous ligament (ITCL) with surrounding soft tissue edema in the sinus tarsi and tarsal canal. A bone contusion in the neck of the talus (asterisks)and osteochondral injury at the medial talar dome (arrowhead) are also visible.
Case 10 – Acute injury with sinus tarsi and tarsal canal syndrome. 48 year-old male with trauma 3 weeks ago, medial and lateral hindfoot pain. A coronal fat suppressed fast spin-echo T2-weighted image (Image 12A) reveals irregularity and intrasubstance increased signal in the interosseous ligament (ITCL), consistent with severe sprain. Adjacent fluid extends medially into a cyst occupying the tarsal canal (arrowheads) on sagittal fat suppressed fast spin-echo T2-weighted images (Images 12B and 12C) and an axial fast spin-echo T2-weighted image (Image 12D).
Case 11 – Chronic sinus tarsi syndrome in a 59 year-old female. Sagittal T1-weighted (Image 13A) and fat suppressed fast spin-echo T2 (Image 13B), along with axial T1-weighted (Image 13C) images demonstrate hypointense soft tissue material occupying the sinus tarsi (asterisks) on all imaging sequences, consistent with fibrosis. No visible disruption of the ligaments.
Case 12 – Chronic injury with sinus tarsi syndrome. 69 year-old male with trauma several years ago, lateral hindfoot pain. Sagittal (Image 14A) and coronal (Image 14B) fat-suppressed fast spin-echo T2-weighted images show thickening and mild increased signal in the interosseous talocalcaneal ligament (ITCL), consistent with chronic sprain. A sagittal T1-weighted image (Image 14C) demonstrates hypointense fibrosis and edema occupying much of the sinus tarsi. Sagittal (Image 14D) and coronal (Image 14E) fat-suppressed fast spin-echo T2-weighted images show thickening and mild increased signal in the cervical ligament (CL), consistent with chronic sprain, with cystic change (arrowheads) posterior to the ligament.
Space occupying lesions in the sinus usually consist of ganglion cysts. (Case 18) Gout or other deposition diseases can cause synovitis and crystal deposition in the sinus. (Case 20) PVNS, rheumatoid arthritis, psoriatic, and other inflammatory arthritides can involve the subtalar joints and sinus, causing sinus tarsi syndrome.6,11,20,21 There is one reported case of neoplasm (metastatic endometrial adenocarcinoma) involving the sinus tarsi.27 Osteoid osteomas in the talus or calcaneus adjacent to the sinus have been reported as a cause of sinus tarsi syndrome.28
Case 13 – Chronic sinus tarsi and tarsal canal syndrome. 21 year-old male with previous ankle injury 6 months ago. Axial (Image 15A) and sagittal (Images 15B and 15C) fat suppressed fast spin-echo T2-weighted images reveal chronic sprain of the interosseous talocalcaneal ligament (ITCL) with irregular morphology. A septated cyst posterior to the interosseous ligament protrudes (arrowheads) medially into the tarsal canal. Incidentally noted are prominent tibiotalar and subtalar joint effusions with synovial hypertrophy, suggesting synovitis.
Case 14 – Chronic injury with attenuation of the interosseous talocalcaneal ligament. 36 year- old male with history of ankle sprain several years ago, subtalar instability and sinus tarsi syndrome. Coronal T1-weighted (Image 16A), sagittal T1-weighted (Image 16B) and fat suppressed fast spin-echo T2-weighted (Image 16C) images through the tarsal canal show a thin interosseous talocalcaneal ligament (ITCL) without significant soft tissue edema, consistent with chronic partial tear of the ligament.
Case 15 – Chronic sprain of the interosseous talocalcaneal ligament. 40 year-old male with previous injury 8 months ago. Coronal fat suppressed fast spin-echo proton density-weighted (Image 17A) and sagittal fat suppressed fast spin-echo T2-weighted (Image 17B) images reveal intrasubstance increased signal in the interosseous ligament (ITCL) with adjacent edema.
Case 16 – Chronic sprain of the cervical ligament with sinus tarsi syndrome. 63 year-old female with injury 1 year ago and persistent pain. Sagittal T1-weighted (Images 18A and 18B) and fat suppressed fast spin-echo T2-weighted images (Images 18C and 18D) demonstrate thickening, irregularity and mild increased signal in the cervical ligament (CL), consistent with chronic sprain. Adjacent fibrosis (asterisks) and small cysts (arrowheads) in the posterior sinus.
Case 17 – Chronic sprain of cervical ligament, sinus tarsi fibrosis. 61 year-old female with lateral ankle pain. Axial (Image 19A) and sagittal (Image 19B) T1-weighted images demonstrate hypointense fibrosis (asterisks) in the sinus tarsi. Sagittal (Image 19C) and coronal (Image 19D) fat suppressed fast spin-echo T2-weighted images through the cervical ligament reveal thickening and increased signal in the ligament (CL), consistent with chronic sprain.
Case 18 – Chronic sinus tarsi syndrome with ganglion cyst occupying the sinus. 64 year-old female with persistent lateral pain for 2 years. Sagittal (Image 20A) and coronal (Image 20B) fat suppressed fast spin-echo T2-weighted images, along with an axial fast spin-echo T2-weighted image (Image 20C) show a large ganglion cyst (asterisks) occupying most of the sinus tarsi. The sinus tarsi ligaments are not visible, consistent with chronic ligament tears.
Case 19 – Chronic injury with heterotopic ossification in the sinus tarsi and sinus tarsi syndrome. 45 year-old male with history of inversion injury 4 years ago. Sagittal T1-weighted (Images 21A and 21B) and fat suppressed fast spin-echo T2-weighted (Images 21C and 21D) images reveal a corticated ossicle (arrow) with internal fatty marrow in the usual location of the cervical ligament. Small cysts (arrowheads) are present in the posterior sinus tarsi.
Case 20 – Gout involving the subtalar joint and sinus tarsi. 76 year-old female with a history of gout presents with sinus tarsi syndrome. Sagittal T1-weighted (Image 22A) and fat suppressed fast spin-echo T2-weighted (Image 22B) images demonstrate erosions (arrowheads) involving the middle subtalar joint. Sagittal T1-weighted (Image 22C) and fat-suppressed fast spin-echo T2-weighted (Image 22D) images, along with an axial T1-weighted image (Image 22E) reveal intermediate to hypointense soft tissue material (asterisks) occupying the sinus tarsi, likely representing fibrosis and crystal deposition with tophus formation.
Hindfoot valgus, tarsal coalition, or fracture can result in anatomic narrowing of the sinus tarsi or tarsal canal; this may predispose to inflammation, edema, synovitis and fibrosis in the sinus.15,29,30
(Cases 21 through 23)
Case 21 – Chronic healed fracture with osteophyte narrowing the sinus tarsi. 77 year-old male with sinus tarsi syndrome and history of previous calcaneal fracture. Sagittal T1-weighted (Image 23A) and fat suppressed fast spin-echo T2-weighted (Image 23B) images demonstrate a healed fracture with hypertrophy of the anterior process of the calcaneus (arrow), causing narrowing of the sinus tarsi with mild edema and fibrosis (asterisks) in the sinus.
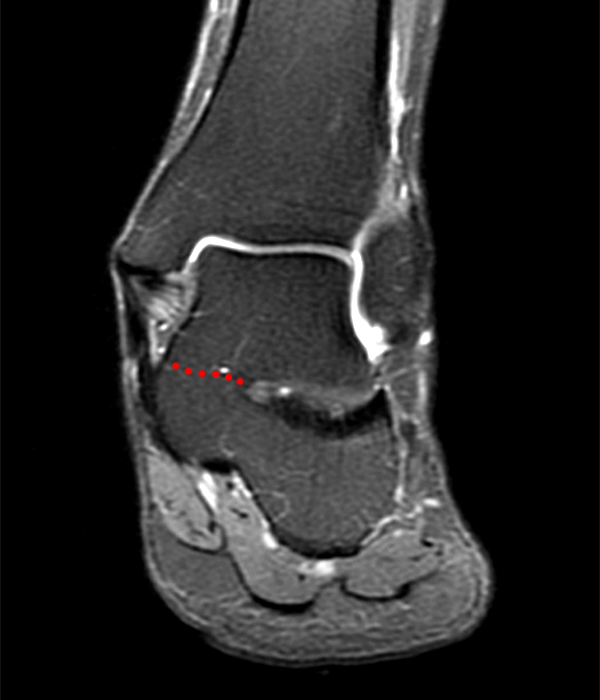
Case 22 – Middle subtalar coalition causing sinus tarsi narrowing. 49 year-old male with chronic lateral ankle pain. Coronal fat suppressed fast spin-echo proton density-weighted (Image 24A) and sagittal T1-weighted (Image 24B) images show complete bony fusion of the middle subtalar joint (dotted lines). Coronal fat suppressed fast spin-echo proton density-weighted (Image 24C) and sagittal T1-weighted (Image 24D) images through the sinus tarsi reveal severe narrowing of the sinus (arrowheads).
Case 23 – Hindfoot valgus with lateral hindfoot impingement and sinus tarsi syndrome. 67 year- old female with chronic hindfoot pain. A coronal fat suppressed fast spin-echo proton density-weighted image (Image 25A) reveals prominent valgus angulation of the calcaneus. Sagittal T1-weighted (Image 25B) and fat suppressed fast spin-echo T2-weighted (Image 25C) images through the sinus tarsi show subcortical cysts and marrow edema (arrowheads) in the inferior lateral process of the talus, consistent with lateral hindfoot impingement. The sinus tarsi is narrowed (asterisks) due to the alteration of talocalcaneal alignment, with fibrosis occupying the sinus.
Lee et al. reported MRI sensitivities of 71% or higher for cervical ligament tears, synovial thickening, and sinus tarsi fat alterations. However, sensitivity for interosseous ligament tears was only 44% in their series of 30 cases.31
Treatment
Initial treatment usually consists of activity restriction, orthotics, physical therapy, and functional rehabilitation.3,32 If the patient experiences relief by injection of anesthetic into the sinus, repeated injection of steroid and local anesthetic into the sinus can be performed once per week for up to 6 weeks.4,5 Oral analgesics may be given along with injections. Conservative treatment has been reported to result in cure or significant improvement of symptoms in 57 to 83% of patients.4,5,33
If a patient does not improve after conservative treatment, open or arthroscopic exploration of the sinus allows debridement of synovitis and fibrosis, and surgical reconstruction of the ligaments as needed. Surgical intervention is reported to achieve satisfactory results in most patients. In refractory cases, subtalar arthrodesis may be indicated.4,5,16,18,34,35
Conclusion
The sinus tarsi syndrome is a well-defined, uncommon clinical entity with various etiologies. MRI provides excellent definition of sinus tarsi anatomy and good detection of findings associated with the clinical syndrome, including abnormalities in the tarsal canal. Early detection of sinus tarsi lesions by imaging facilitates appropriate patient management.
References
- O’Connor, D.: Sinus tarsi syndrome. A clinical entity. J. Bone Joint Surg. (Am.) 1958; 40, 720. ↩
- Kjaersgaard-Andersen P, Andersen K, Søballe K, Pilgaard S. Sinus tarsi syndrome: presentation of seven cases and review of the literature. J Foot Surg. 1989;28(1):3-6. ↩
- Helgeson K. Examination and intervention for sinus tarsi syndrome. N Am J Sports Phys Ther. 2009;4(1):29-37. ↩
- Taillard, W., Meyer, J., Garcia, J. et al. The sinus tarsi syndrome. International Orthopaedics 1981; 5, 117–130. ↩
- Zwipp H, Bemmerl JG, Holch M, Thermann H, Maschek HJ, Sinus tarsi and canalis tarsi syndromes. A post-traumatic entity, Foot and Ankle Surgery, 1996; Volume 2, Issue 3, 181-188. ↩
- Lektrakul N, Chung CB, Lai YM, et al. Tarsal sinus: arthrographic, MR imaging, MR arthrographic, and pathologic findings in cadavers and retrospective study data in patients with sinus tarsi syndrome. Radiology. 2001;219(3):802-810. ↩
- Cahill DR. The anatomy and function of the contents of the human tarsal sinus and canal. Anat. Rec., 1965; 153: 1-17. ↩
- Jotoku T, Kinoshita M, Okuda R, Abe M. Anatomy of ligamentous structures in the tarsal sinus and canal. Foot Ankle Int. 2006;27(7):533-538. ↩
- Yamaguchi R, Nimura A, Amaha K, et al. Anatomy of the Tarsal Canal and Sinus in Relation to the Subtalar Joint Capsule. Foot Ankle Int. 2018;39(11):1360-1369. ↩
- Beltran J, Munchow AM, Khabiri H, Magee DG, McGhee RB, Grossman SB. Ligaments of the lateral aspect of the ankle and sinus tarsi: an MR imaging study. Radiology. 1990;177(2):455-458. ↩
- Klein MA, Spreitzer AM. MR imaging of the tarsal sinus and canal: normal anatomy, pathologic findings, and features of the sinus tarsi syndrome. Radiology. 1993;186(1):233-240. ↩
- Li SY, Hou ZD, Zhang P, Li HL, Ding ZH, Liu YJ. Ligament structures in the tarsal sinus and canal. Foot Ankle Int. 2013;34(12):1729-1736. ↩
- Mittlmeier T, Rammelt S. Update on Subtalar Joint Instability. Foot Ankle Clin. 2018;23(3):397-413. ↩
- Kjaersgaard-Andersen P, Wethelund JO, Helmig P, Søballe K. The stabilizing effect of the ligamentous structures in the sinus and canalis tarsi on movements in the hindfoot. An experimental study. Am J Sports Med. 1988 Sep-Oct;16(5):512-6. ↩
- Frey C, Feder KS, DiGiovanni C. Arthroscopic evaluation of the subtalar joint: does sinus tarsi syndrome exist? Foot Ankle Int. 1999;20(3):185-191. ↩
- Lee KB, Bai LB, Song EK, Jung ST, Kong IK. Subtalar arthroscopy for sinus Tarsi syndrome: arthroscopic findings and clinical outcomes of 33 consecutive cases. Arthroscopy. 2008 Oct;24(10):1130-4. ↩
- Thacker P, Mardis N. Ligaments of the tarsal sinus: improved detection, characterisation and significance in the paediatric ankle with 3-D proton density MR imaging. Pediatr Radiol. 2013;43(2):196-201. ↩
- Pisani G, Pisani PC, Parino E. Sinus tarsi syndrome and subtalar joint instability. Clin Podiatr Med Surg. 2005;22(1):63-vii. ↩
- Arshad Z, Bhatia M. Current concepts in sinus tarsi syndrome: A scoping review. Foot Ankle Surg. 2020 Sep 16:S1268-7731(20)30183-1. ↩
- Dozier TJ, Figueroa RT, Kalmar J. Sinus tarsi syndrome. J La State Med Soc. 2001;153(9):458-461. ↩
- Beltran J. Sinus tarsi syndrome. Magn Reson Imaging Clin N Am. 1994;2(1):59-65. ↩
- Breitenseher MJ, Haller J, Kukla C, et al. MRI of the sinus tarsi in acute ankle sprain injuries. J Comput Assist Tomogr. 1997;21(2):274-279. ↩
- Stella SM, Ciampi B, Orsitto E, Melchiorre D, Lippolis PV. Sonographic visibility of the sinus tarsi with a 12 MHz transducer. J Ultrasound. 2014 Dec 13;19(2):107-13. ↩
- Stella SM, Ciampi B, Orsitto E, Melchiorre D, Lippolis PV. Sonographic visibility of the sinus tarsi with a 12 MHz transducer. J Ultrasound. 2014 Dec 13;19(2):107-13. ↩
- Usmani S, Abu Al Huda F, Al Kandari F. Three-Phase 99mTc MDP Bone Scintigraphy and SPECT-CT in Sinus Tarsi Syndrome. Clin Nucl Med. 2016 Apr;41(4):e208-10. ↩
- Mahato A, Mukherjee PB, Jha DK, Pandit AG, M V. Sinus Tarsi Syndrome: Diagnosed on 99mTc-MDP bone SPECT/CT. Asia Ocean J Nucl Med Biol. 2020 Spring;8(2):153-156. ↩
- Pieters RS, Galvin J. The rare presentation of sinus tarsi syndrome secondary to metastasis in a patient with endometrial carcinoma. Radiol Case Reports 2011;6:414. ↩
- Scarfi G, Veneziani C, D’Orazio P. Sinus tarsi syndrome caused by osteoid osteoma: a report of two cases. Foot Ankle Surg 2006;12:157–60. ↩
- Lawrence DA, Rolen MF, Haims AH, Zayour Z, Moukaddam HA. Tarsal Coalitions: Radiographic, CT, and MR Imaging Findings. HSS J. 2014 Jul;10(2):153-66. ↩
- Bali K, Prabhakar S, Gahlot N, Dhillon MS. Neglected lateral process of talus fracture presenting as a loose body in tarsal canal. Chin J Traumatol. 2011;14(6):379-82 ↩
- Lee KB, Bai LB, Park JG, Song EK, Lee JJ. Efficacy of MRI versus arthroscopy for evaluation of sinus tarsi syndrome. Foot Ankle Int. 2008;29(11):1111-1116. ↩
- Shear MS, Baitch SP, Shear DB. Sinus tarsi syndrome: The importance of biomechanically-based evaluation and treatment, Archives of Physical Medicine and Rehabilitation, Volume 74, Issue 7, 1993, Pages 777-781. ↩
- Akiyama K, Takakura Y, Tomita Y, Sugimoto K, Tanaka Y, Tamai S. Neurohistology of the sinus tarsi and sinus tarsi syndrome. J Orthop Sci. 1999;4(4):299-303. ↩
- Lowy A, Schilero J, Kanat IO. Sinus tarsi syndrome: a postoperative analysis. J Foot Surg. 1985 Mar-Apr;24(2):108-12. ↩
- Oloff LM, Schulhofer SD, Bocko AP. Subtalar joint arthroscopy for sinus tarsi syndrome: a review of 29 cases. J Foot Ankle Surg. 2001;40(3):152-157. ↩