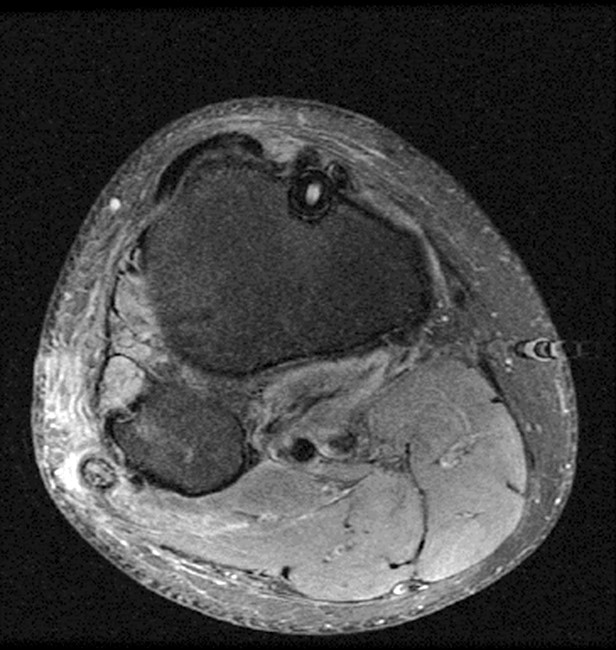
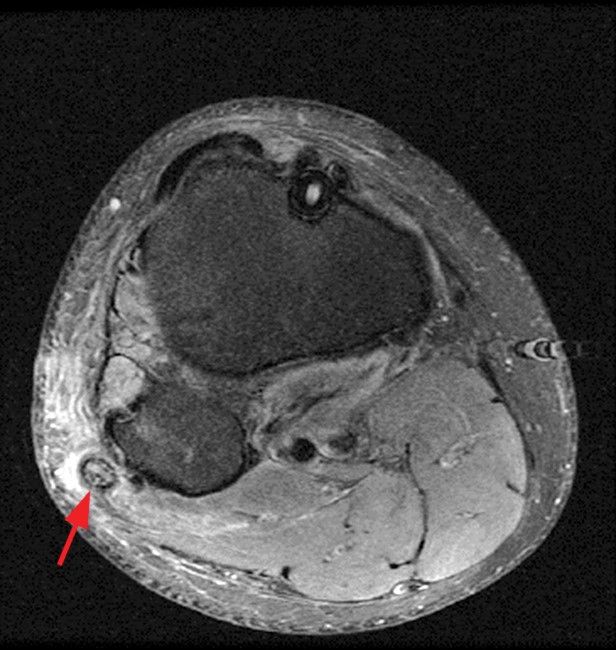
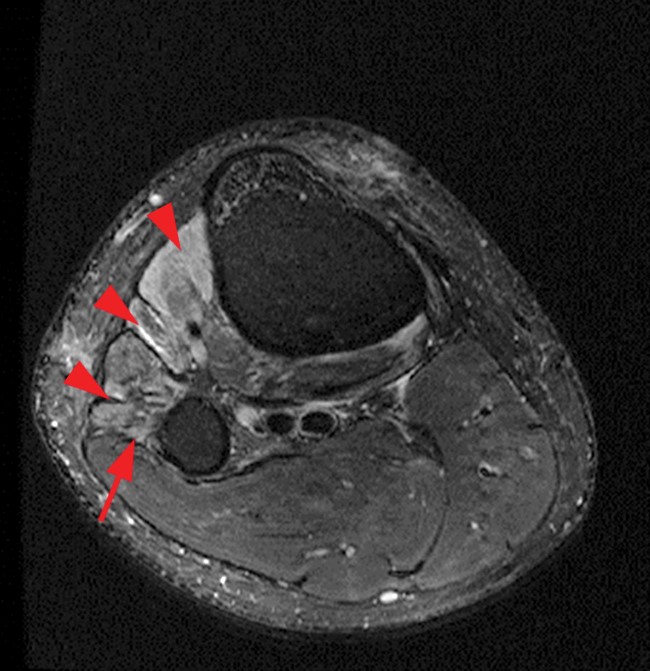
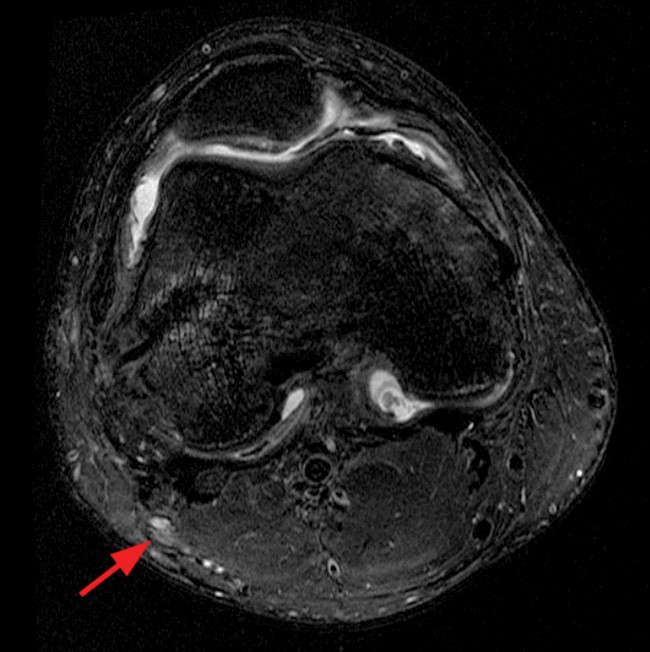
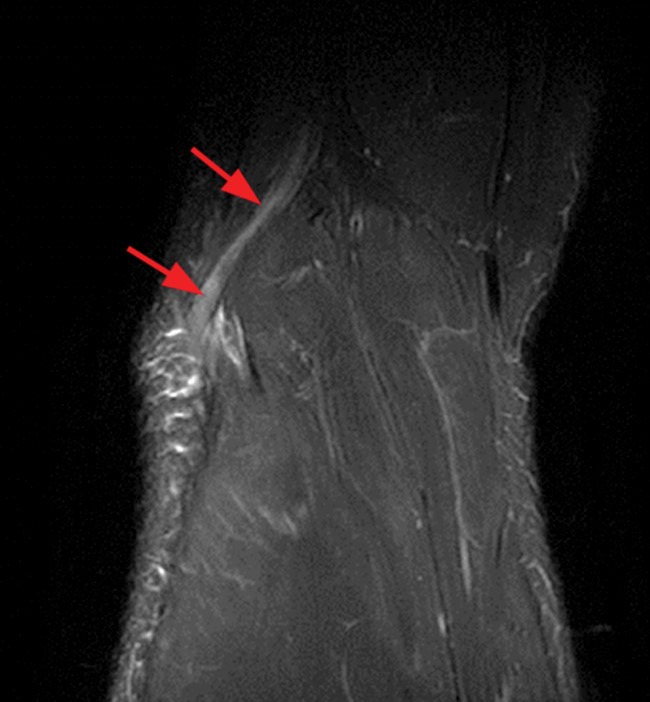
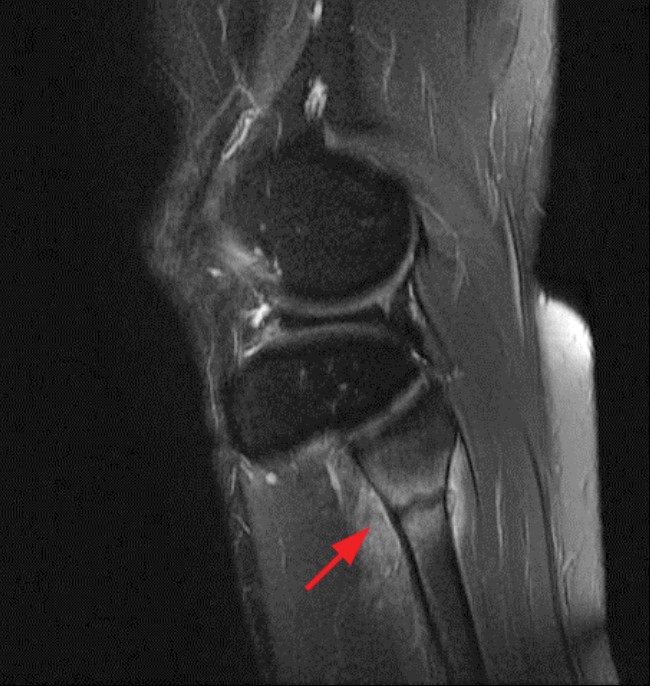
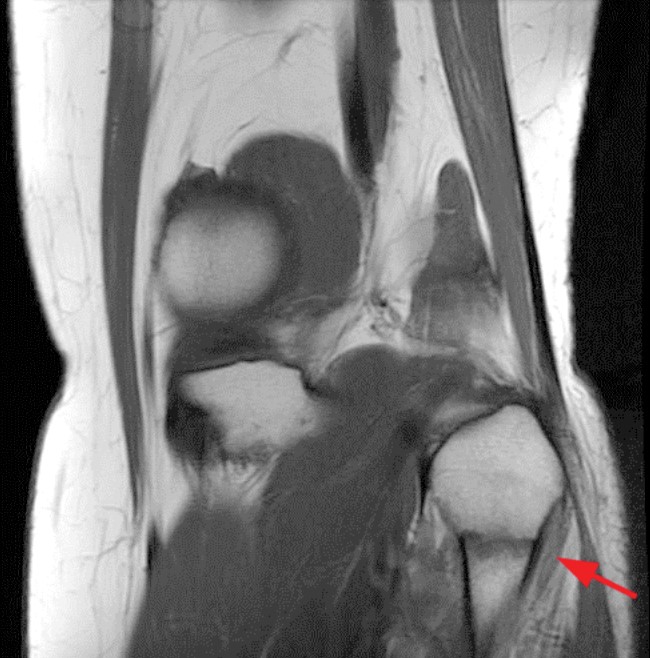
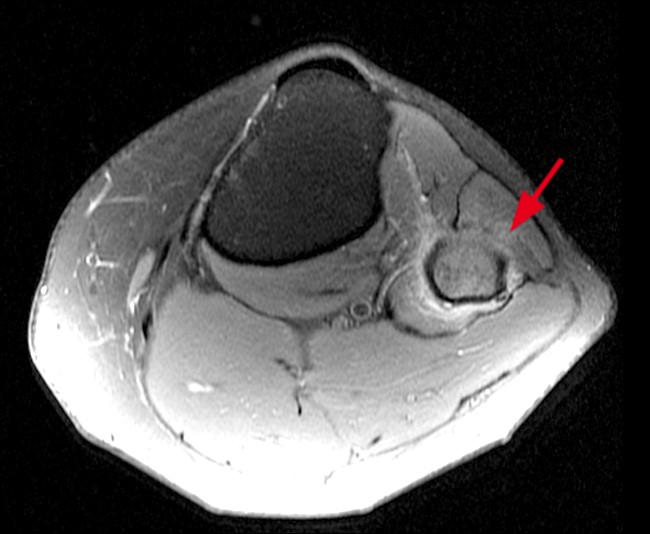
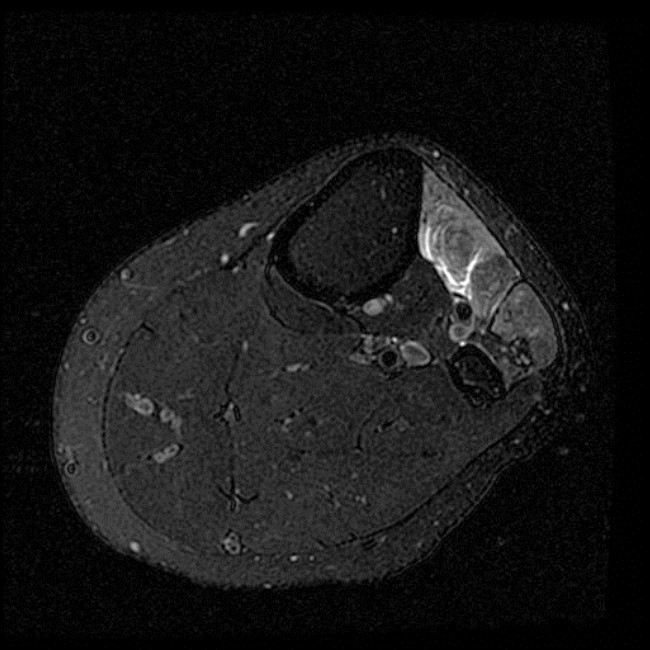
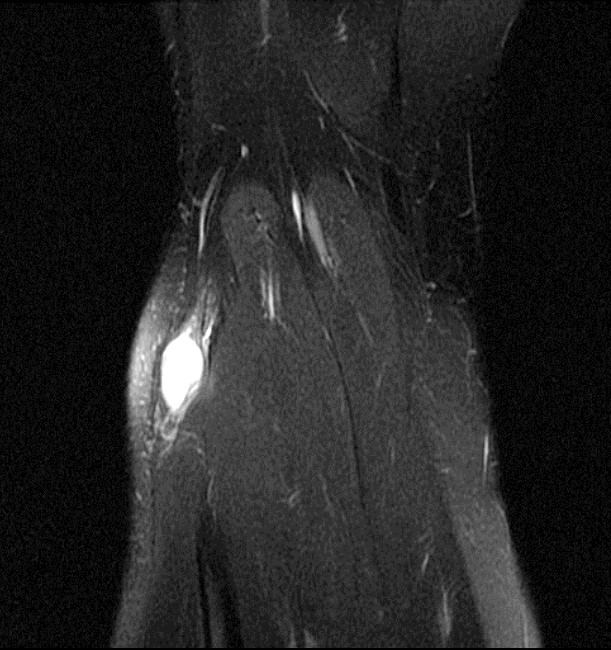
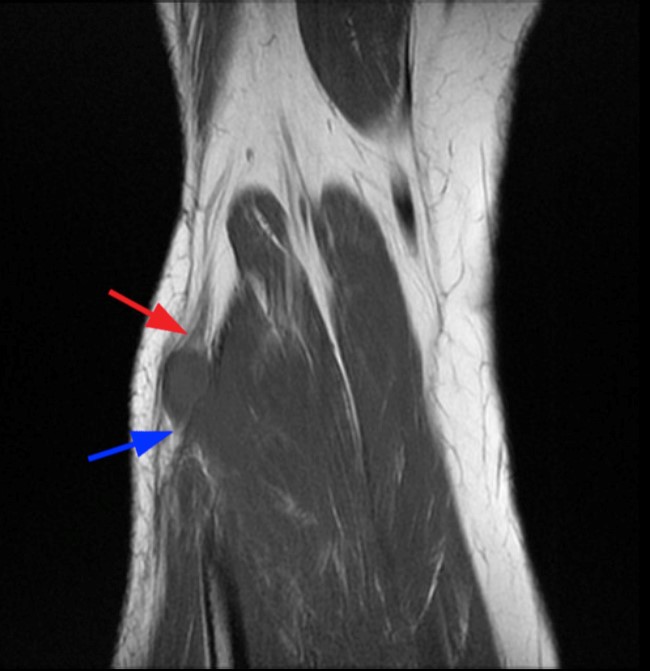
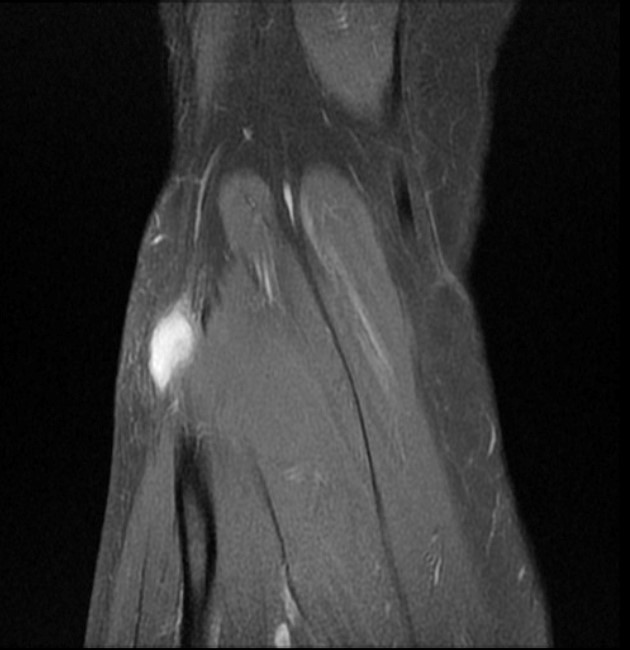
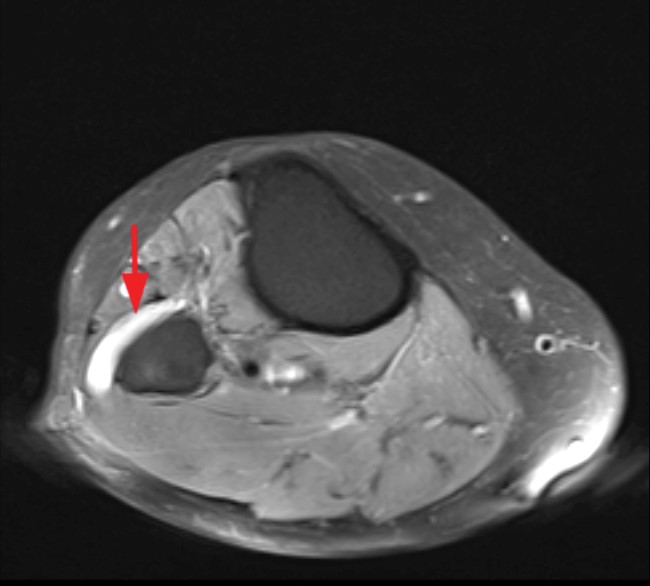
Clinical History and Unknown Case: A 17-year-old male presents with foot drop 4 months following surgery for an ACL tear and a posterolateral corner injury. Axial fat-suppressed proton density-weighted (1a), axial fat-suppressed T2-weighted (1b,c) and coronal fat-suppressed T2-weighted (1d) images are provided.
What are the findings? What is your diagnosis?
Findings:
Figure 2:
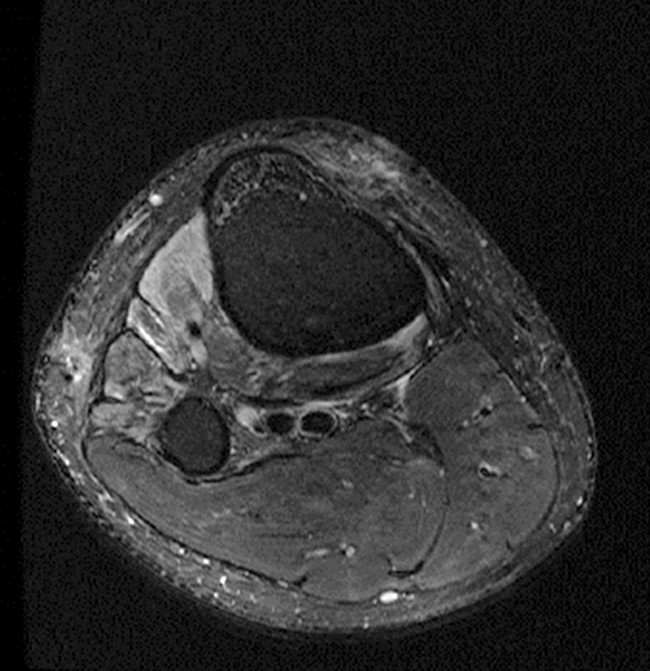
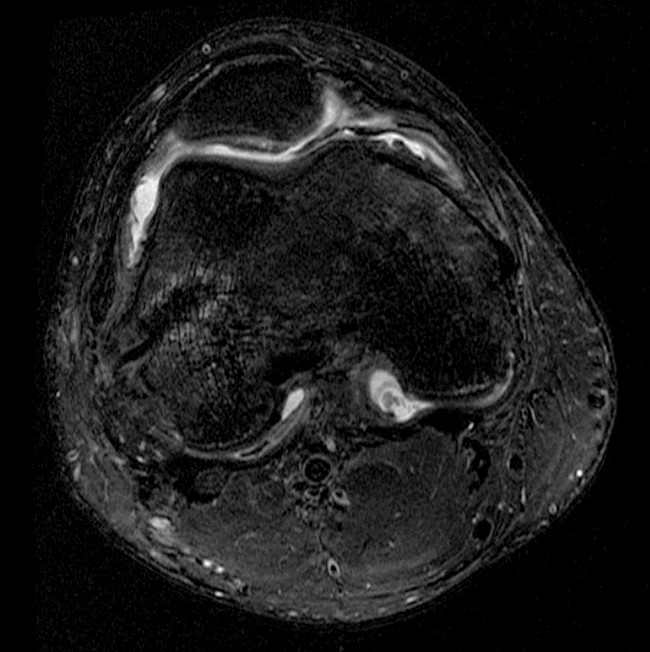
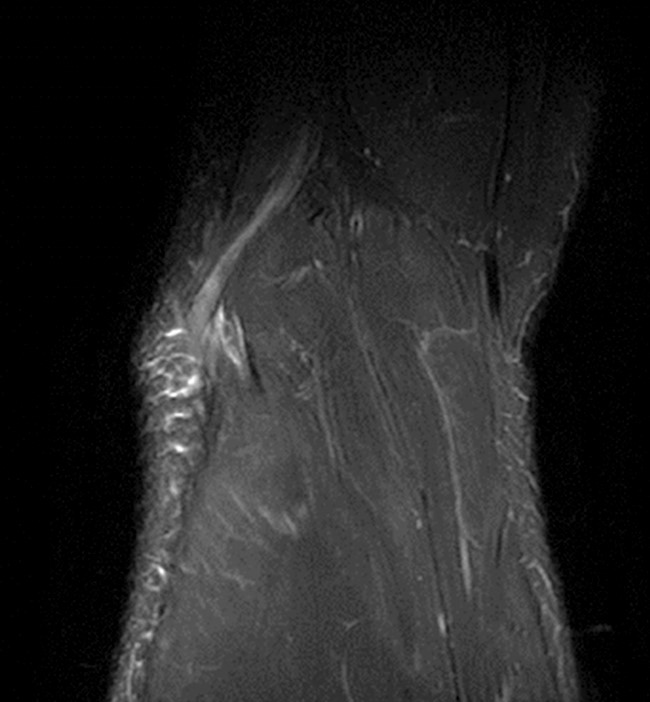
(2a) The axial fat suppressed proton density-weighted image demonstrates thickening and irregularity of the common peroneal nerve (arrow) at the level of the fibular neck. (2b) The axial fat suppressed T2-weighted image demonstrates denervation edema in the anterior compartment muscles (arrowheads). The common peroneal nerve is located immediately lateral to the fibular neck (arrow) within the peroneal tunnel. (2c) The axial fat suppressed T2-weighted image of the common peroneal nerve at the level of the femoral condyles reveals focal fascicular enlargement and increased signal intensity of the nerve (arrow). (2d) The coronal fat suppressed T2-weighted image demonstrates increased signal in the common peroneal nerve (arrows) below the bifurcation of the sciatic nerve.
Diagnosis:
Common peroneal nerve injury following anterior cruciate ligament tear and posterolateral corner injury.
Introduction:
Common peroneal nerve (CPN) injuries can occur in isolation from blunt or penetrating injury to the nerve or as a component of trauma to the knee with associated osseous, meniscal, and/or ligamentous injuries. CPN injury has been observed in up to 44% of cases of multiligamentous knee injuries involving the posterolateral corner with disruption of the biceps femoris tendon or an avulsion fracture of the fibular head. 1 The CPN is prone to injury due in part to at least 6 anatomical factors. The symptoms of a CPN injury include foot drop and loss of sensation over the anterolateral aspect of the leg. Standard MRI sequences of the knee with adequate coverage and the addition of axial T1-weighted spin echo images can be very useful in determining the location, extent, and associated factors involved with a CPN injury. Furthermore, dedicated neurography protocols can be employed to better evaluate the CPN owing to an increased sensitivity to the detection of signal changes in the nerve.2, 3 The chosen field of view should include the entire course of the CPN from the level of the sciatic bifurcation to that of the deep and superficial divisions of the CPN to ensure proximal lesions are not missed.
Pertinent Anatomy of the Common Peroneal Nerve:
The course and appearance of the tibial nerve and CPN distal to the bifurcation of the sciatic nerve have received a great deal of attention, but these nerves can be visualized more proximally as well. Due to an abundance of epineural fat in the sciatic nerve, the separate tibial and peroneal fascicular bundles can usually be distinguished from one another from the level of the sciatic plexus to the sciatic nerve bifurcation with the peroneal division being the more lateral of the two. 4 In approximately 7% of normal persons, these fascicular bundles can be seen to separate in the pelvis when coursing adjacent to the piriformis muscle, with the CPN fascicles coursing through the muscle and rejoining the tibial nerve fascicles at the inferior aspect of the piriformis muscle. 5 In most persons, however, the tibial nerve and CPN fascicles remain separately organized within a common sciatic nerve sheath from the pelvis superiorly to the sciatic nerve bifurcation inferiorly without intermingling of fascicles.2,4 The tibial nerve and CPN components of the sciatic nerve physically split at or above the popliteal fossa in the distal third of the thigh to form the CPN and tibial nerve proper. Both nerves give off branches just after their division, including the communicating peroneal nerve and lateral sural cutaneous nerve from the CPN and the medial sural cutaneous nerve from the tibial nerve. 6 The medial and lateral sural cutaneous nerves typically combine to form the sural nerve.2 Together, these proximal branches provide sensation to the lateral aspect of the leg.6 The tibial nerve descends along the back of the leg close to the popliteal artery and vein at the level of the knee and distally to the plantar aspect of the heel and foot. The CPN descends obliquely from a midline to lateral position in the fat overlying the biceps femoris muscle and the lateral head of the gastrocnemius muscle, wrapping around the proximal aspect of the fibular neck before it courses medially to pierce the anterior fascia between the heads of the peroneus longus muscle (peroneal tunnel) and enter the anterior compartment of the leg.2,6 Just prior to entering the peroneal tunnel, the nerve is superficial to the fibular head-neck junction in the subcutaneous fat along the lateral aspect of the knee, a site vulnerable to injury related to direct compression.
Figure 3:
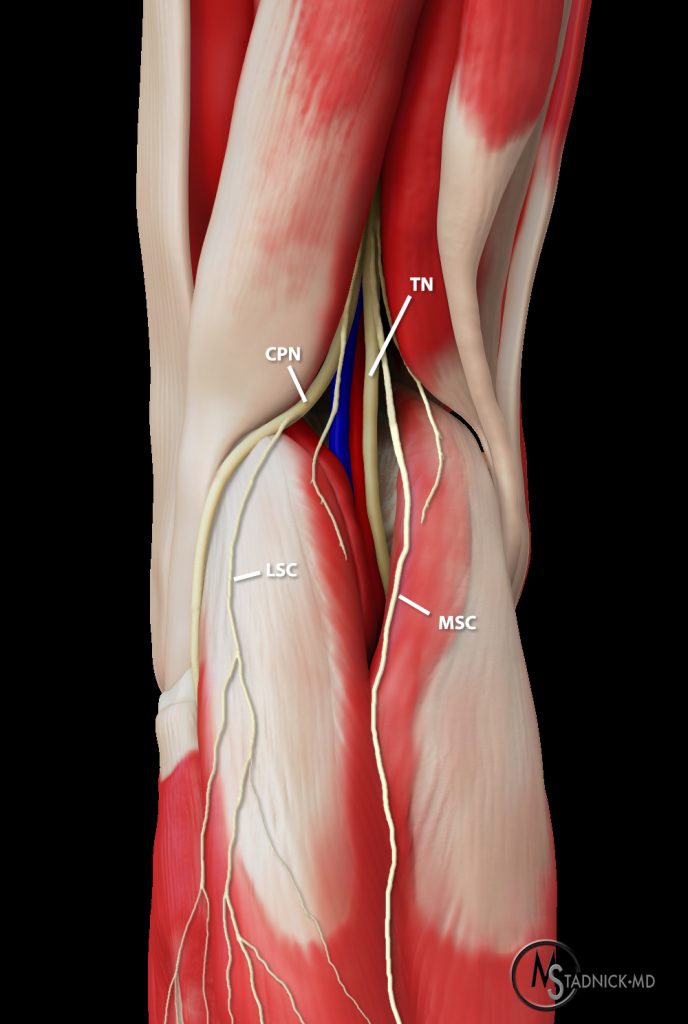
(3a) 3D rendering of the posterolateral aspect of the knee demonstrating the branching of the sciatic nerve into the common peroneal (CPN) and tibial nerves (TN), as well as the lateral sural cutaneous (LSC) and medial sural cutaneous (MSC) nerve contributions.
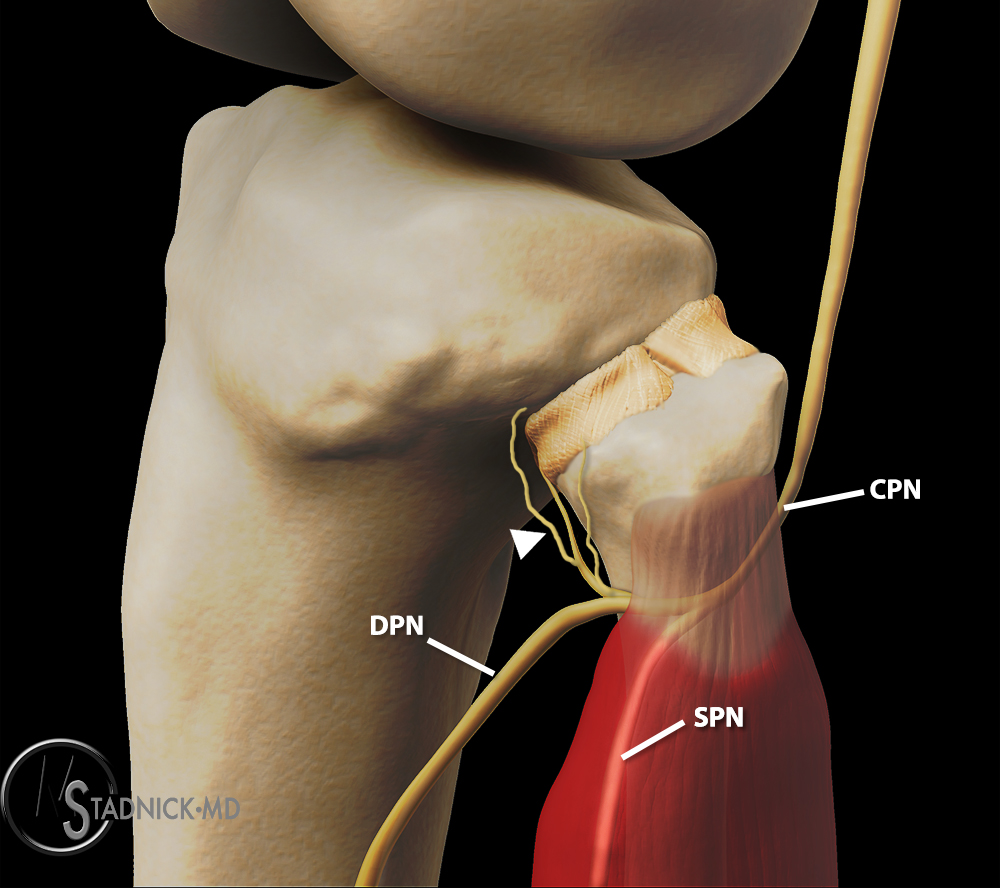
(3b) 3D rendering of the lateral aspect of the knee demonstrating the course of the common peroneal nerve (CPN) below the proximal head of the peroneus longus muscle within the fibular tunnel. The common peroneal nerve branches into the superficial peroneal nerve (SPN) and deep peroneal nerve (DPN) and also provides branches to the proximal tibiofibular joint (arrowhead).
The CPN divides into a superficial peroneal nerve (SPN) and a deep peroneal nerve (DPN) supplying muscles in the lateral and anterior compartments of the leg, respectively.6 Additionally, a recurrent articular branch angles superiorly toward the anterior aspect of the proximal tibiofibular articulation.7 The exact level of SPN and DPN branching is variable, occurring at or below the level of the fibular neck (80% of knees), above the peroneal tunnel between the fibular neck and the knee joint (10% of knees), or above the knee joint line (9% of knees).3 The SPN and DPN course inferiorly in the anterior aspect of the leg to the foot where further branching occurs. The DPN and SPN branches can usually be distinguished from each other with the branches of the DPN situated anterior to the branches of the SPN.6
Understanding the muscle and sensory distribution of the CPN can be helpful in identifying the location of injury to the nerve. Denervation changes in the muscles controlled by the CPN can be a useful sign indicating the specific nerve that is involved and the degree of injury that has been sustained (axonotmesis or neurotmesis, discussed later). Above the bifurcation of the CPN and tibial nerve in the lower thigh, the CPN division of the sciatic nerve supplies the short head of the biceps femoris muscle, but the long head of the biceps femoris muscle is supplied by the tibial division of the sciatic nerve.6 Below the bifurcation of the sciatic nerve, the CPN proper supplies the muscles in the anterior and lateral compartments of the leg via the DPN and SPN. The DPN is predominantly a motor nerve and supplies the muscles of the anterior compartment of the leg: tibialis anterior, extensor digitorum longus, extensor hallucis longus, and peroneus tertius muscles. The DPN also has a unique sensory distribution, supplying sensation to the first web-space between the first and second toes. The SPN provides motor function to the muscles of the lateral compartment of the leg: peroneus brevis and peroneus longus muscles. The SPN supplies sensory innervation to the anterolateral aspect of the distal two-thirds of the leg as well as the dorsum of the foot. The tibial nerve is responsible for the motor function of the muscles of the posterior leg and calf: gastrocnemius, soleus, tibialis posterior, flexor hallucis longus, and flexor digitorum longus muscles.6 The communicating peroneal nerve, lateral sural cutaneous nerve, medial sural cutaneous nerve, and sural nerve together provide sensation to the lateral aspect of the leg, ankle, and foot.6
Pathology of the Common Peroneal Nerve:
There are several anatomic features of the peroneal nerve and its surroundings that make the nerve more susceptible to injury.3,6
- Due to the superficial location and relative paucity of fat surrounding the CPN as it courses over the lateral aspect of the fibular head, the nerve is prone to injury from external laceration or blunt trauma.
- The nerve is predisposed to stretch-type injuries due to its fixed position both proximally in the pelvis and at the level of the fibular head.6
- The course of the CPN through the fibular tunnel formed between the tendons of peroneus longus and soleus muscles and the bony floor of the proximal fibula predisposes to nerve compression.
- Variant anatomical position of the short head or, less commonly, long head of the biceps femoris muscle can lead to narrowing of the muscular tunnel between the biceps femoris muscle and lateral head of the gastrocnemius muscle through which the nerve must pass, resulting in less adipose cushioning of the CPN and a greater risk of compression.
- Variation in the location of the CPN bifurcation, with the division into the SPN and DPN occurring more proximally, can predispose to injury during certain arthroscopic procedures (Figure 4).
- Additional branches of the CPN including the articular branch, lateral sural cutaneous nerve, and peroneal communicating branch may also sustain injuries.
Figure 4:
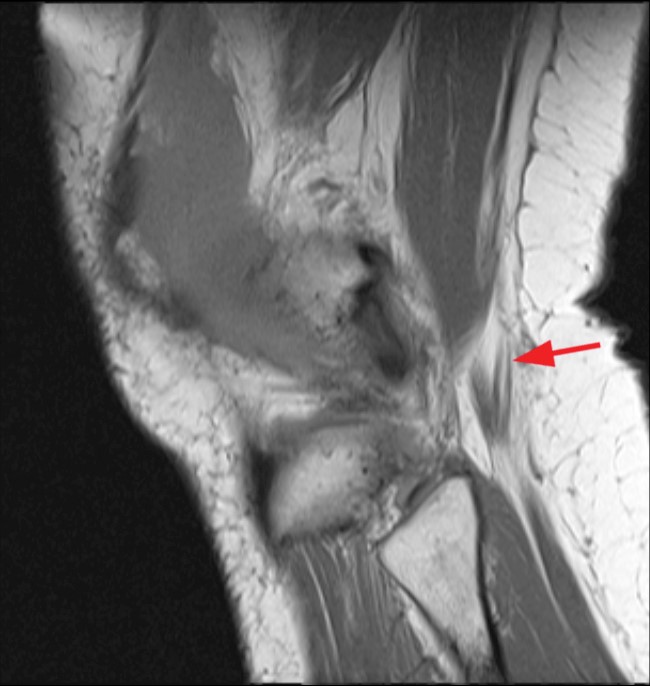
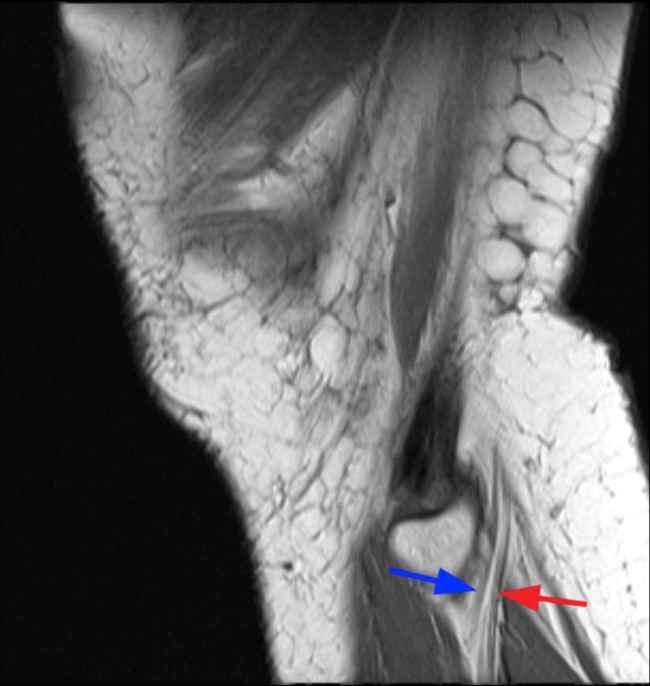
(4a) Sagittal T1-weighted image showing bifurcation of the CPN above the knee joint line (arrow). (4b) Sagittal T1-weighted image slightly more lateral to figure 4a showing bifurcation of the CPN above the joint line. The SPN (red arrow) and DPN (blue arrow) are seen at the level of the fibular neck.
Identifying an Injured Nerve
Findings indicative of nerve injury can be divided into direct and indirect features. Direct features include an increased size of the nerve, increased size and signal of the individual fascicles, increased signal intensity of the nerve, and deviation from the normal anatomical course of the nerve. Indirect features include loss of the normal perineural fat planes related to fibrosis or mass lesions and changes of denervation to the muscles supplied by the nerve. 8 Correlation with clinical findings and electromyography can be useful when isolating the nerve injuries.
Grading Nerve Injury
There are three grades of nerve injury that can further be divided into 5 categories. According to the Seddon classification, these three grades are neurapraxia, axonotmesis, and neurotmesis.8,9,10,11 Neurapraxia represents the least amount of damage to the nerve with dysfunction but no interruption of axons, indicating injury only to the myelin sheath. This is typically seen as signal hyperintensity of the nerve on T2-weighed images and enlargement of the nerve without associated denervation changes of the muscle. This may resolve within weeks to a few months if there is no Wallerian degeneration and the axon remains intact (Figure 5).
Figure 5:
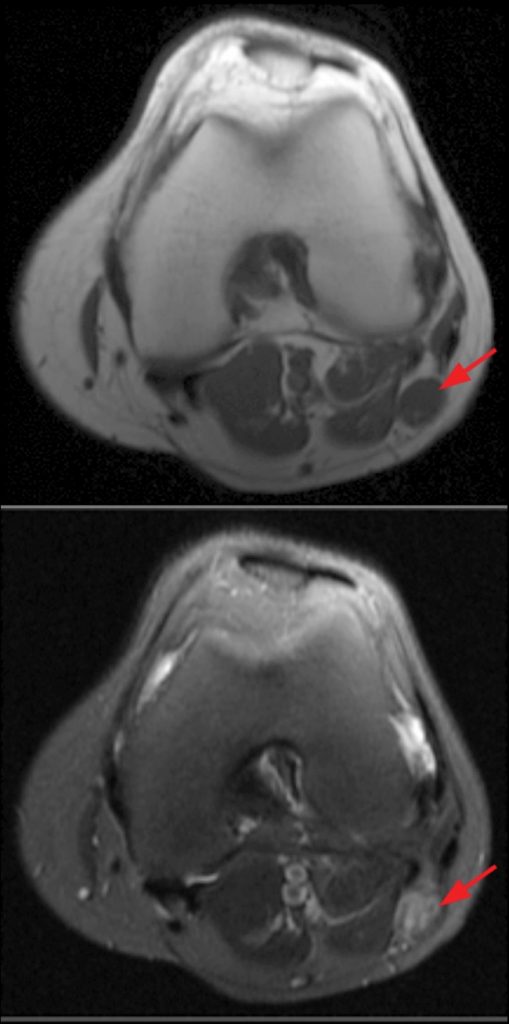
35 year-old woman with leg pain that developed while running on a treadmill.(5a) Sagittal fat-suppressed T2-weighted image demonstrates periosseus edema surrounding the common peroneal nerve (arrow) at the level of a nondisplaced stress fracture of the fibular neck. (5b) Coronal T1-weighted image demonstrates the nondisplaced stress fracture of the fibular neck at the same level that the common peroneal nerve courses through the peroneal tunnel (arrow). (5c) Axial fat-suppressed proton density-weighted image demonstrates periosseus edema at the level of the stress fracture that surrounds the CPN as it courses around the lateral aspect of the fibular neck (arrow). Note that there are no denervation changes in the muscles of the anterior compartment of the lower leg. In spite of this, the patient presented with clinical and EMG findings of CPN irritation.
Axonotmesis is the next higher degree of severity, reflecting discontinuity of the axons with Wallerian degeneration but variable preservation of the surrounding connective tissue (i.e. perineurium, endoneurium, and epineurium). This manifests as signal hyperintensity of the nerve on T2-weighed images with associated denervation changes in the muscles. The highest grade injury, termed neurotmesis, occurs when there is complete disruption of the axons and surrounding connective tissue elements (i.e. perineurium, endoneurium, and epineurium). Sunderland further divides these three grades of injury into five categories, with I representing neurapraxia, II-IV representing increasing severity of axonotmesis, and V representing neurotmesis.11,12
Traumatic Neuromas
In higher grade injuries, regenerating nerves are not able to re-establish an organized fascicular course and instead develop into a tumor-like tangle of neuronal elements and fibrous tissue.3,10 Grade IV injuries often result in a neuroma in continuity formation (Figure 6) while grade V injuries result in a neuroma in a completely severed nerve (i.e. terminal/end bulb neuroma and stump neuroma) (Figure 7).
Figure 6:
(6a) Axial fat-suppressed T2-weighted image demonstrating denervation edema in the muscles of the anterior compartment. (6b) Axial fat-suppressed T2-weighted image demonstrating neuroma in continuity (arrow) in the proximal CPN just below the bifurcation of the sciatic nerve. (6c) Curved planar fat-suppressed T2-weighted image demonstrating sequential focal enlargement of the CPN (arrows) consistent with neuroma in continuity.
Figure 7:
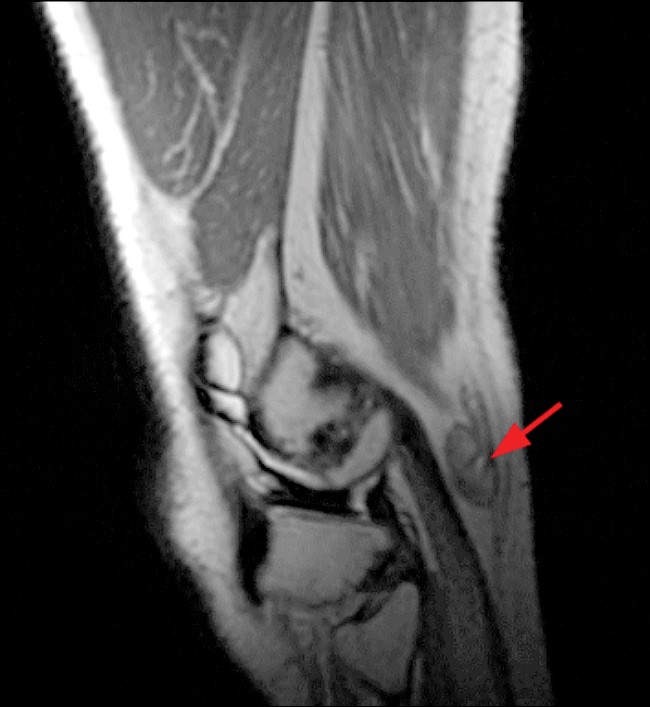
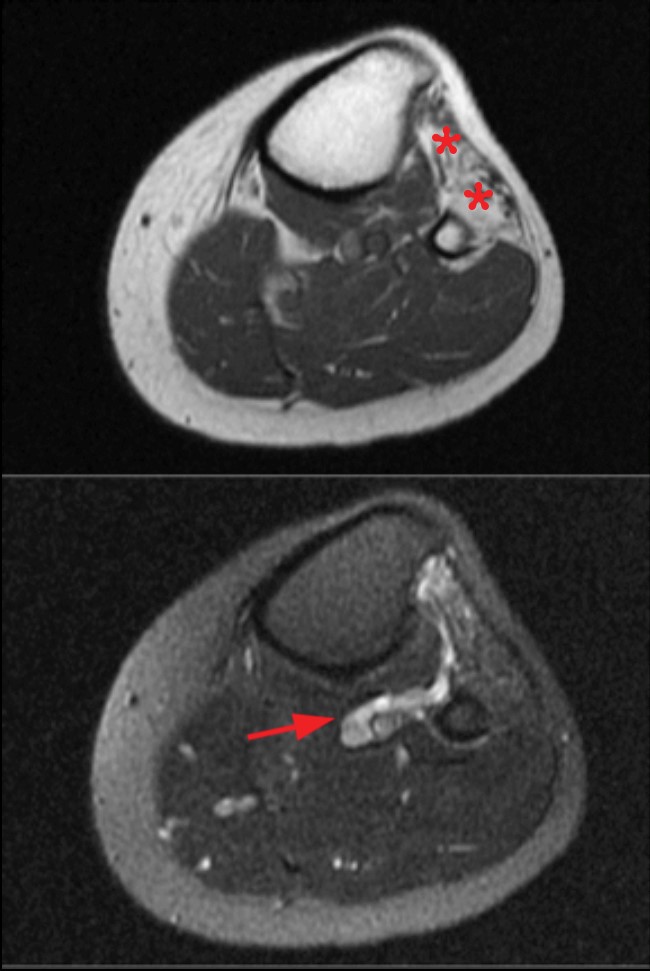
(7a) Sagittal T2-weighted image demonstrating terminal, or end-bulb, neuroma (arrow) years after a penetrating injury to this region. (7b) Axial T1-weighted (above) and fat-suppressed T2-weighted (below) images demonstrating fatty atrophy (asterisks) of the muscles of the anterior compartment after CPN transection referenced in figure 7a. There is also extraneural ganglion extension adjacent to the neurovascular bundle (arrow). 7c Axial T1-weighted (above) and fat-suppressed T2-weighted (below) images of the CPN terminal neuroma in figure 7a, which demonstrates T1 isointensity to muscle and T2 mild hyperintensity (arrows). Terminal neuromas do not typically enhance.
Although stump neuromas and end bulb neuromas both represent a similar process of disorganized axonal mass-like growth, stump neuromas are necessarily associated with amputation of the limb.
A neuroma in continuity may have variable appearances including spindle-shaped, lateral (eccentric), bulbous, and dumbbell-shaped related to the differing degree of disruption of the axons and connective tissue within the nerve bundle. Lateral and spindle-shaped neuromas are more likely to have axons remaining in continuity while bulbous and dumbbell-shaped neuromas are more likely to reflect neurotmesis.3,13
Peripheral Nerve Sheath Tumors
Peripheral nerve sheath tumors (PNST) can involve any segment of the CPN. Such tumors have characteristic MR imaging features, including the split fat sign and target sign, that generally allow differentiation from traumatic lesions of the nerve 3 (Figure 8).
Figure 8:
51 year old woman with a posterolateral soft tissue mass about the knee.
(8a) Coronal fat-suppressed T2-weighted image reveals marked T2 hyperintensity of the mass. (8b) Coronal T1-weighted image showing the nerve entering (red arrow) and exiting (blue arrow) the mass. (8c) Coronal post contrast fat-suppressed T1-weighted image with avid enhancement of the mass.
The split fat sign refers to a thin rim of fat surrounding the mass on T1-weighted images, which may taper at the proximal and distal aspects of the tumor. The target sign is characterized by an area of signal hypointensity on T2-weighted images in the center of the mass. The presence of surrounding scarring, lack of a split fat or target sign, and absence of abnormal enhancement further help to distinguish neuroma in continuity from neurogenic tumors.14
Peroneal Nerve Ganglion Cysts
Extraneural ganglion cysts of the CPN are much more common compared to the frequency of intraneural ganglia, with approximately 350 reported cases as of 2008.15 The CPN is, however, by far the most common location for intraneural ganglion cysts. Clinical and electromyographic findings are more pronounced with intraneural ganglia as the perineurium restricts expansion of these ganglia and thus increases the intraneural pressure.16 Intraneural ganglia are virtually always symptomatic with pain or neuropathy, or both, which preferentially affects the DPN and the muscles in the anterior compartment of the lower leg.15 The treatment of intraneural and extraneural ganglion cysts is not the same, such that differentiation between the two is important. Furthermore, in some cases, both intraneural and extraneural ganglia may coexist.
MR imaging and operative dissection have consistently documented a connection between the articular branch of the CPN and the proximal tibiofibular joint with the latter being the site of origin of intraneural ganglion cysts (Figure 9a).
Figure 9:
74 year old woman with sensation of a mass lateral to the fibula for a month.
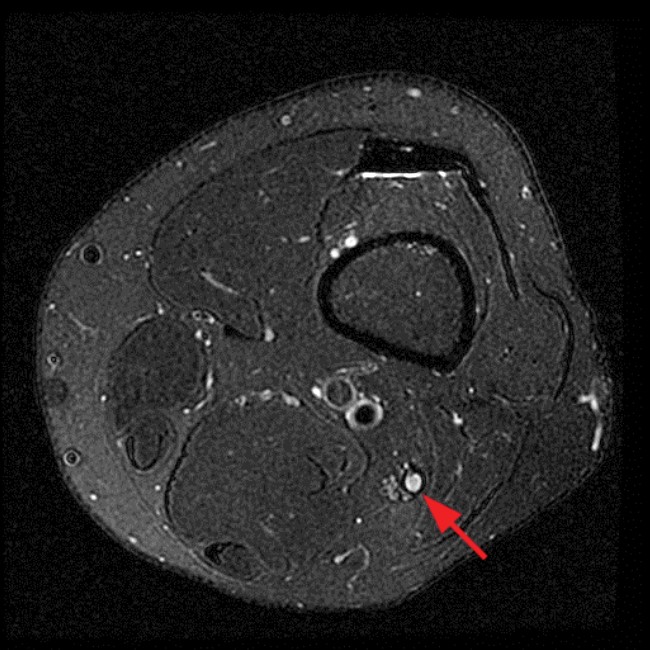
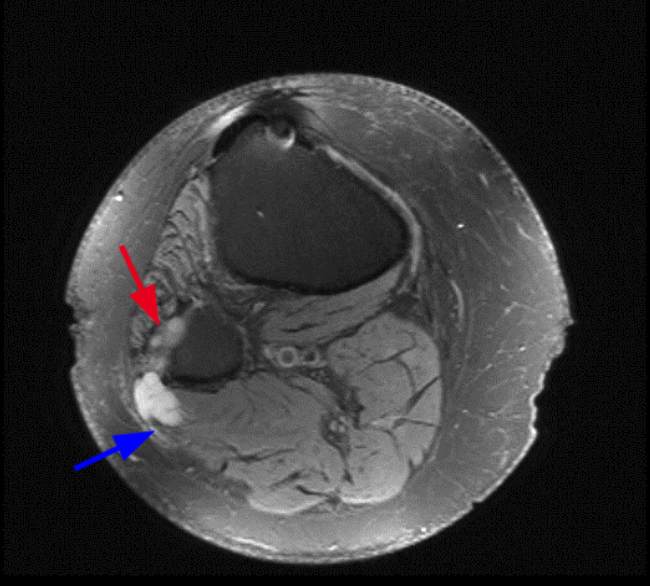
(9a) Axial fat suppressed proton density-weighted image showing a ganglion (arrow) coursing around the fibular neck, directed retrograde along the course of the CPN. The source of the cyst was the anterior aspect of the proximal tibiofibular joint.
61 year old man with right knee pain.
(9b) Axial fat suppressed proton density-weighted image showing cystic changes in the CPN relating to an intraneural ganglion cyst. Note the signet ring sign (blue arrow) and transverse limb sign (red arrow) (9c) Coronal fat suppressed T2-weighted image showing cystic changes in the CPN relating to an intraneural ganglion cyst (asterisk). Note the enlargement of the nerve and extension of fluid between the fascicles proximally (arrows).
Reports, most notably by Spinner and collaborators15, have detailed MR imaging signs that allow accurate diagnosis of intraneural ganglia of the CPN. These signs are based on a 12-hour clock face that is superimposed at various levels of the fibular head and neck. At the level of the mid-portion of the fibular head, the signet ring sign (cyst within the CPN) and tail sign (connection of the cyst to the proximal tibiofibular joint) can been seen at the 4 to 5 o’clock and 11 to 12 o’clock positions, respectively (Figure 10).
Figure 10:
(10a) A 3D rendering demonstrates an intraneural ganglion cyst of the common peroneal nerve with the locations of the tail sign (red) and signet sign (blue) at the mid-fibular head level, and the transverse limb sign (green) at the fibular neck.
A clock face superimposed on these regions with 12 o’clock anterior, 3 o’clock lateral, 6 o’clock posterior, and 9 o’clock medial. At the mid-fibular head level, the signet ring sign is between the 4 and 5o’clock positions (Figure 10 (b) blue circle) and the tail sign at the 11 o’clock and 12 o’clock positions (Figure 10 (b) red circle). At the mid-fibular neck, the transverse limb sign is between 12 and 2 o’clock positions (Figure 10 (c) red area).
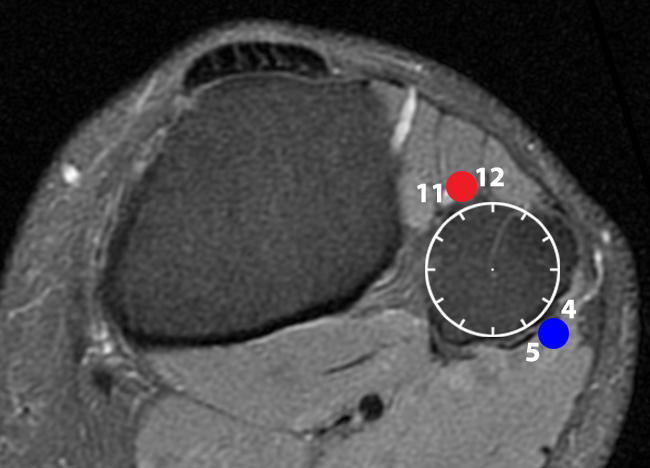
(10b) On this axial proton density-weighted fat-suppressed image at the level of the mid-fibular head, the blue circle represents the location of the “signet ring” sign at the 4 to 5 o’clock position and the red circle represents the location of the “tail” sign at the 11 to 12 o’clock position.
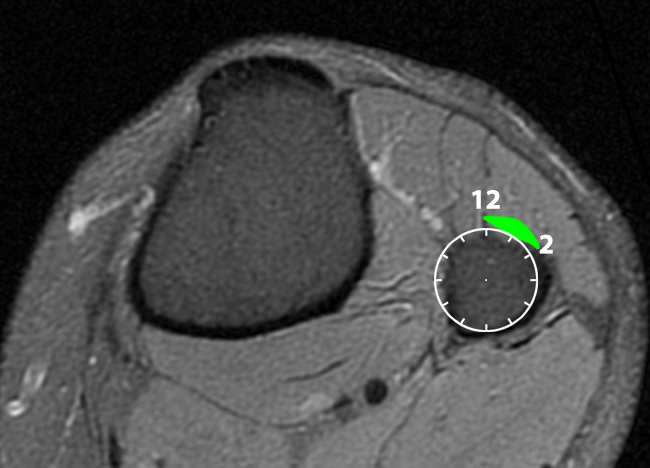
(10c) On this axial proton density-weighted fat-suppressed image at the level of the fibular neck, the green area represents the location of the “transverse limb” sign between the 12 and 2 o’clock positions.
The transverse limb sign (cyst within the articular branch of the CPN) is best seen at the fibular neck level, between the 12 to 2 o’clock positions.15 (Figure 9b and c).
Determining whether a ganglion cyst at the anterior aspect of the proximal tibiofibular joint is intraneural or extraneural requires an understanding of the differences in appearance between these two types of ganglion cysts. The site from which extraneural ganglion cysts arise is more variable than the site of origin of intraneural ganglion cysts, with extraneural ganglion cysts often more superiorly located along the proximal tibiofibular joint as compared with intraneural ganglia. Additionally, the shape and direction of cyst extension are more variable in cases of extraneural ganglion cysts compared with intraneural ganglia, with the intraneural ganglia following a more predictable concave upward arc. Extraneural ganglion cysts may develop in close proximity to the CPN, abutting the nerve in such a way that their relationship results in a pseudo-signet ring sign; however, close inspection will demonstrate a fat plane between the cyst and nerve and no cyst within the articular branch of the nerve.15 A true signet ring sign will exhibit no fat plane between the ganglion and the nerve and the location is classically at the 4 to 5 o’clock position.
Treatment of Injuries of the Common Peroneal Nerve:
The treatment of CPN injury is dependent on the severity of the injury and whether the nerve remains in continuity. Neurapraxia may recover within a few weeks to a few months from the time of injury with only conservative treatment.14 Fully separated nerves (neurotmesis) require urgent surgical repair for any hope of recovery.2 If the outer epineurium of the nerve sheath is intact, there is potential for the nerve to regenerate spontaneously; however, the higher the grade of injury, the less likely this will occur spontaneously. Surgical exploration and neurolysis of adhesions are often sufficient to improve function in an injured nerve. In some cases, however, resection of the nerve or neuroma and nerve reconstruction are required. Terminal neuromas in noncritical sensory nerves can be treated by resecting the neuroma and inserting the terminal nerve into a muscle to prevent neuroma formation.14 Lateral neuromas can occur after surgical repair 14(i.e. neuroma after nerve repair) and should not be confused with a tumor or failure of the repair.
The optimal treatment for ganglia of the CPN is unknown.15 Treatment of intraneural ganglia can consist of cyst decompression, articular branch ligation, and resection arthroplasty of the proximal tibiofibular joint. Prognostic factors related to motor recovery include: duration of symptoms, extent of compression, size and length of the cyst, and neural anatomy of the tibialis anterior muscle. Recurrence rates have been reported to be as low as 10%, but this likely is an underestimation.16 Ultrasound-guided cyst aspiration has been reported as a treatment option for intraneural ganglia 17,18, showing promising results in anecdotal case reports.
Conclusion
The CPN is the most commonly injured nerve in the lower extremities 6. A reasonable degree of suspicion for such injury is warranted when evaluating a patient with injuries to multiple ligaments or a knee dislocation. Even in the absence of such severe injury, the CPN may be compromised. Therefore, when assessing MR examinations of the knee, the CPN and its major branches should be identified and assessed. Knowledge of regional anatomy is fundamental to the accurate identification of abnormalities of the CPN and its branches.
References
- Oshima T, Nakase J, Numata H, Takata Y, Tsuchiya H. Common Peroneal Nerve Palsy with Multiple-Ligament Knee Injury and Distal Avulsion of the Biceps Femoris Tendon. Case Rep Orthop. 2015;2015:306260. doi:10.1155/2015/306260. ↩
- Chhabra A, Faridian-Aragh N, Chalian M, et al. High-resolution 3-T MR neurography of peroneal neuropathy. Skeletal Radiol. 2012;41(3):257-271. doi:10.1007/s00256-011-1146-y. ↩
- Van den Bergh FRA, Vanhoenacker FM, De Smet E, Huysse W, Verstraete KL. Peroneal nerve: Normal anatomy and pathologic findings on routine MRI of the knee. Insights Imaging. 2013;4(3):287-299. doi:10.1007/s13244-013-0255-7. ↩
- Petchprapa CN, Rosenberg ZS, Sconfienza LM, Cavalcanti CFA, La Rocca Vieira R, Zember JS. MR Imaging of Entrapment Neuropathies of the Lower Extremity Part 1. The Pelvis and Hip. RadioGraphics. 2010;30(4):983-1000. doi:10.1148/rg.304095135. ↩
- Beaton L, Anson B. The sciatic nerve and the piriformis muscle: their interrelation a possible cause of coccygodynia. J Bone Jt Surg Am. 1938;20:686-688. http://jbjs.org/article.aspx?articleID=9139 ↩
- Donovan A, Rosenberg ZS, Cavalcanti CF. MR Imaging of Entrapment Neuropathies of the Lower Extremity Part 2. The Knee, Leg, Ankle, and Foot. RadioGraphics. 2010;30(4):1001-1019. doi:10.1148/rg.304095188. ↩
- Spinner RJ, Desy NM, Amrami KK. Cystic transverse limb of the articular branch: a pathognomonic sign for peroneal intraneural Ganglia at the superior tibiofibular joint. Neurosurgery. 2006;59(1):157-66-66. doi:10.1227/01.NEU.0000219820.31012.22. ↩
- Soldatos T, Andreisek G, Thawait GK, et al. High-Resolution 3-T MR Neurography of the Lumbosacral Plexus. RadioGraphics. 2013;33(4):967-987. doi:10.1148/rg.334115761. ↩
- SEDDON HJ. THREE TYPES OF NERVE INJURY. Brain. 1943;66(4):237-288. doi:10.1093/brain/66.4.237. ↩
- Chhabra A, Andreisek G, Soldatos T, et al. MR Neurography: Past, Present, and Future. Am J Roentgenol. 2011;197(3):583-591. doi:10.2214/AJR.10.6012. ↩
- Grinsell D, Keating CP. Peripheral Nerve Reconstruction after Injury: A Review of Clinical and Experimental Therapies. Biomed Res Int. 2014;2014:698256. doi:10.1155/2014/698256. ↩
- SUNDERLAND S. A classification of peripheral nerve injuries producing loss of function. Brain. 1951;74(4):491-516. http://www.ncbi.nlm.nih.gov/pubmed/14895767. ↩
- Joel A. DeLisa, Bruce M. Gans NEW. Physical Medicine and Rehabilitation : Principles and Practice. ↩
- Chhabra A, Williams EH, Wang KC, Dellon AL, Carrino JA. MR neurography of neuromas related to nerve injury and entrapment with surgical correlation. AJNR Am J Neuroradiol. 2010;31(8):1363-1368. doi:10.3174/ajnr.A2002. ↩
- Spinner RJ, Luthra G, Desy NM, Anderson ML, Amrami KK. The clock face guide to peroneal intraneural ganglia: critical “times” and sites for accurate diagnosis. Skeletal Radiol. 2008;37(12):1091-1099. doi:10.1007/s00256-008-0545-1. ↩
- Spinner RJ, Atkinson JLD, Scheithauer BW, et al. Peroneal intraneural ganglia: the importance of the articular branch. Clinical series. J Neurosurg. 2003;99(2):319-329. doi:10.3171/jns.2003.99.2.0319. ↩
- Jose J, Fourzali R, Lesniak B, Kaplan L. Ultrasound-guided aspiration of symptomatic intraneural ganglion cyst within the tibial nerve. Skeletal Radiol. 2011;40(11):1473-1478. doi:10.1007/s00256-011-1209-0. ↩
- Liang T, Panu A, Crowther S, Low G, Lambert R. Ultrasound-Guided Aspiration and Injection of an Intraneural Ganglion Cyst of the Common Peroneal Nerve. HSS J. 2013;9(3):270-274. doi:10.1007/s11420-013-9345-9. ↩