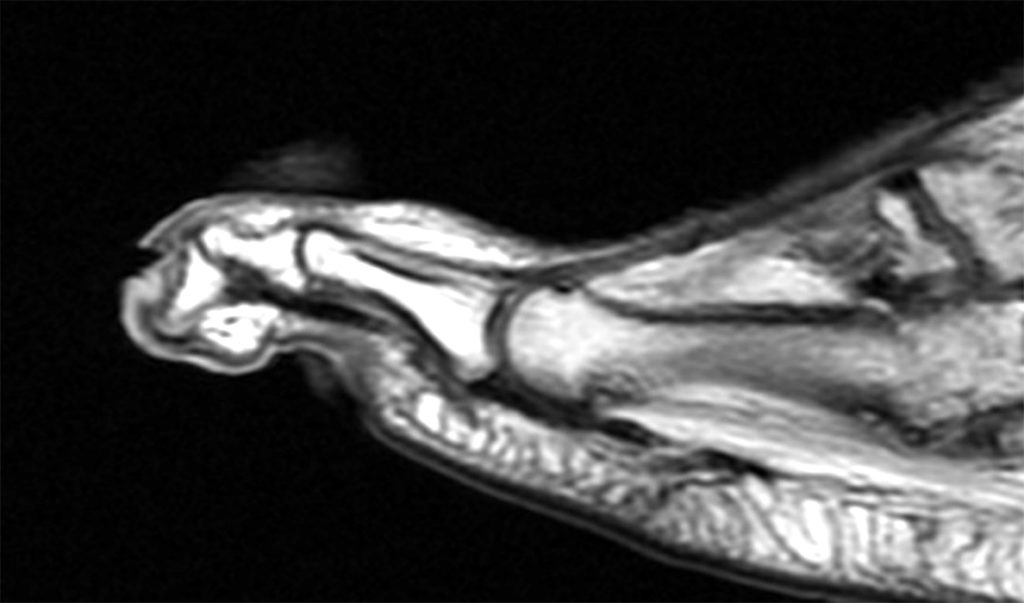
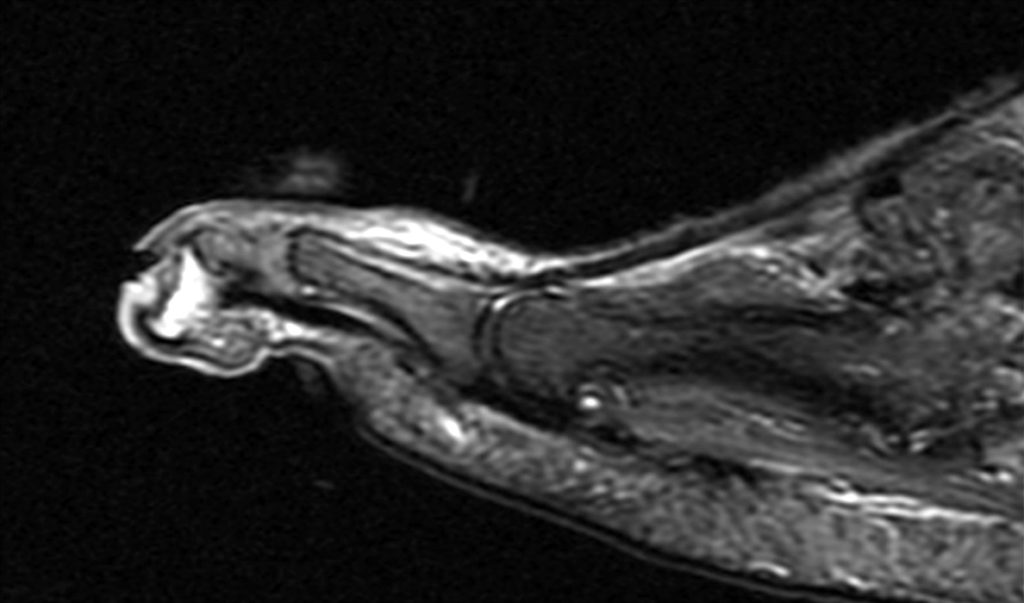
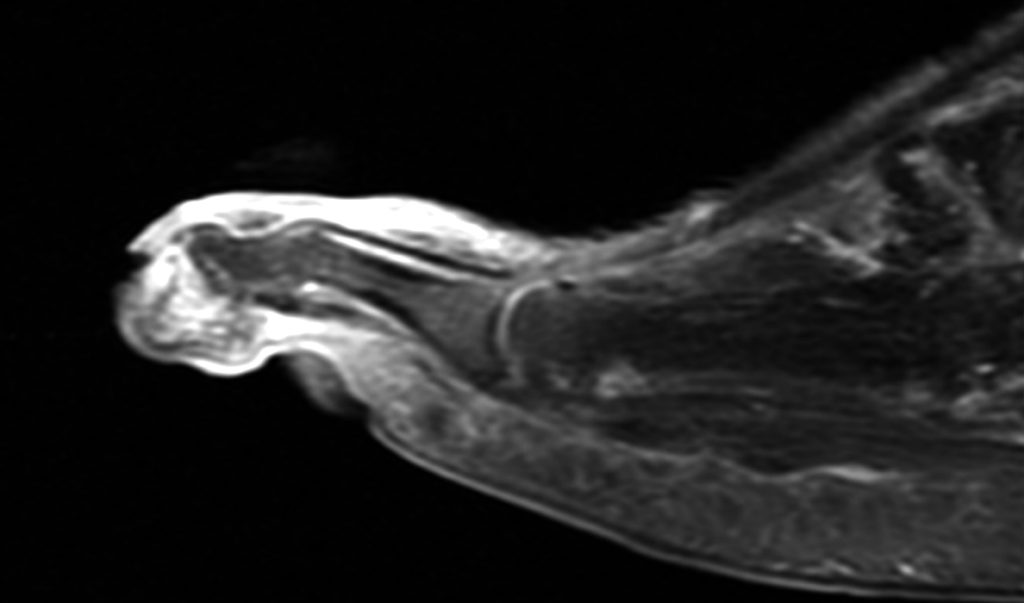
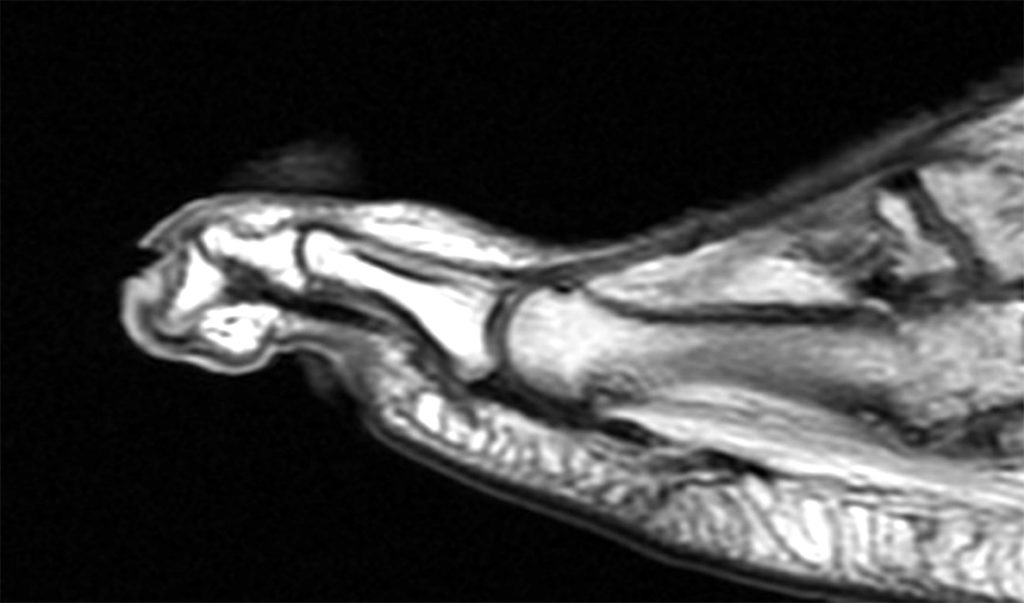
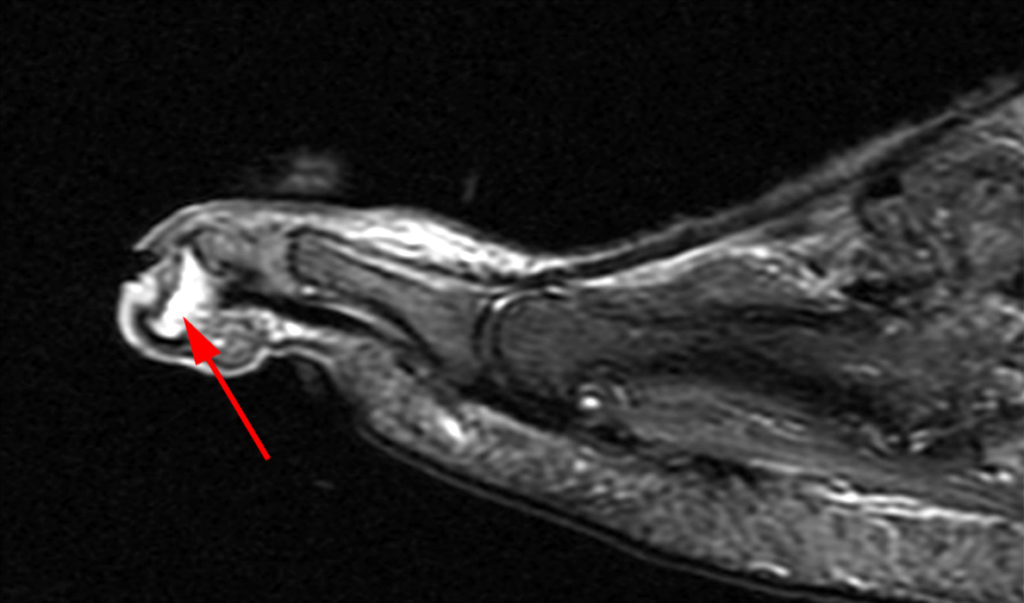
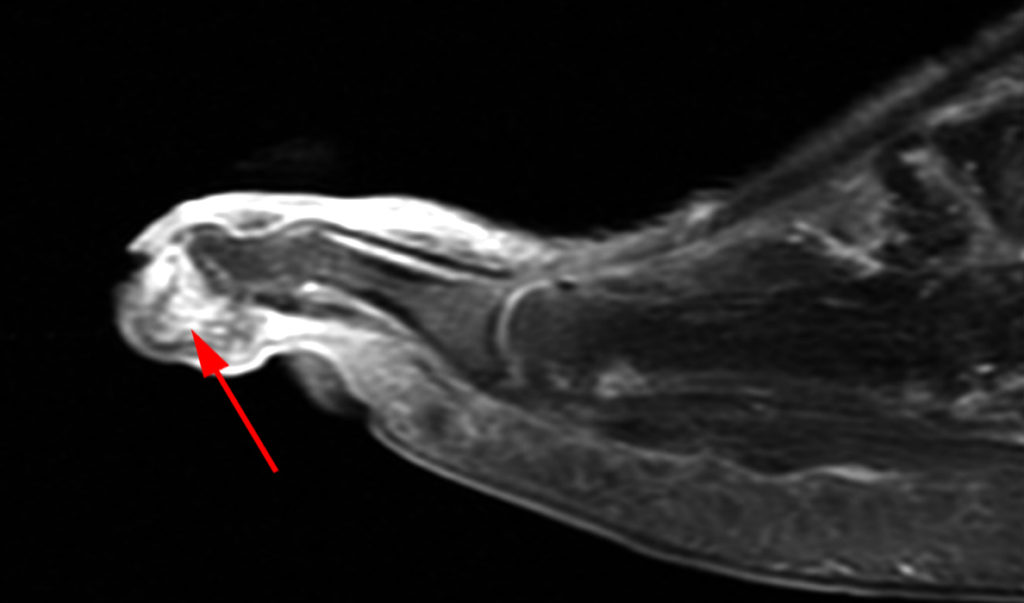
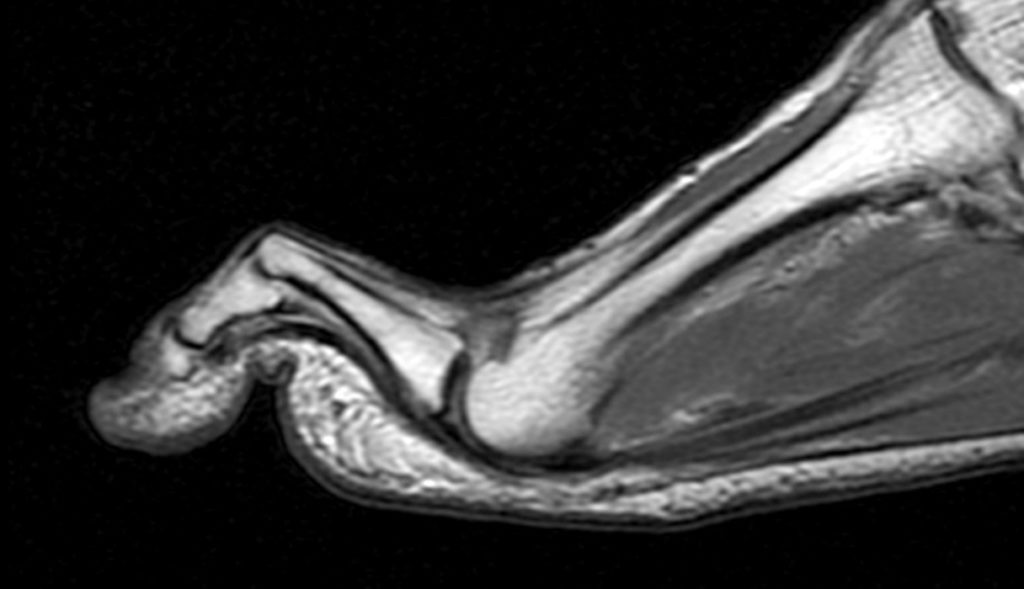
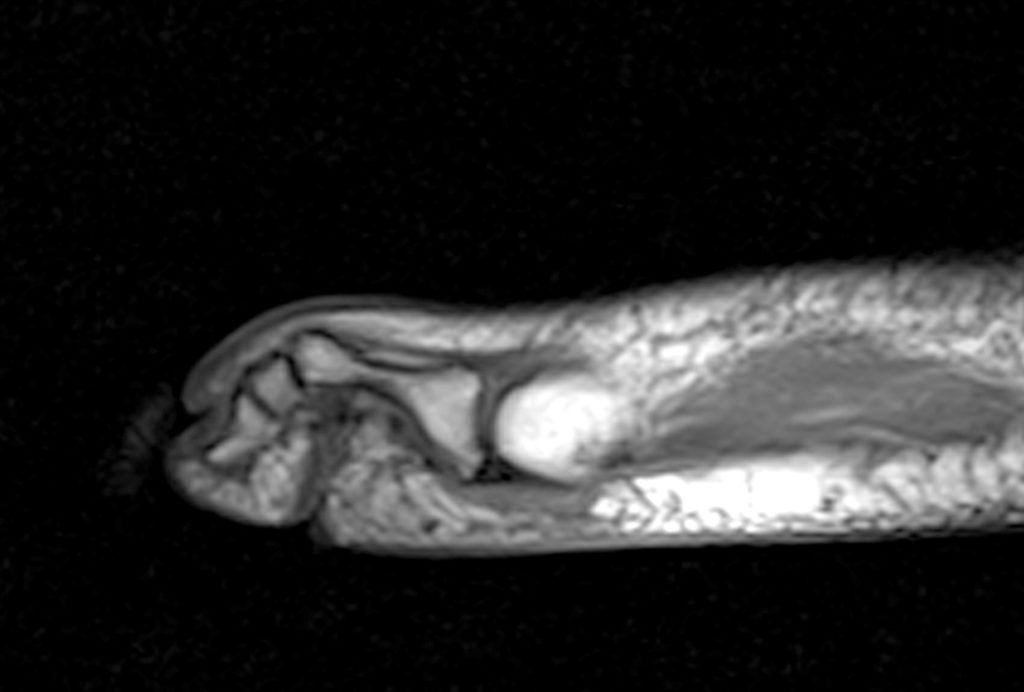
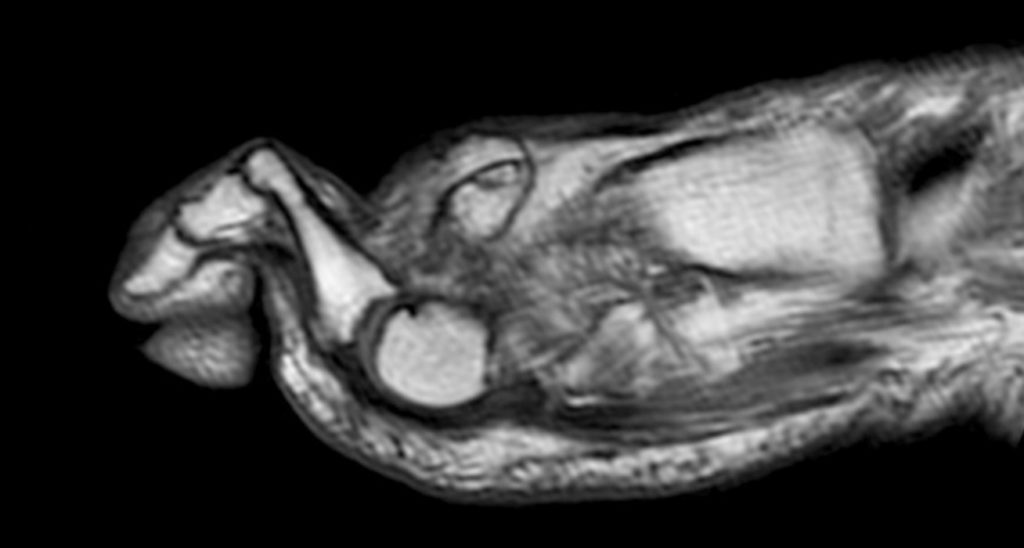
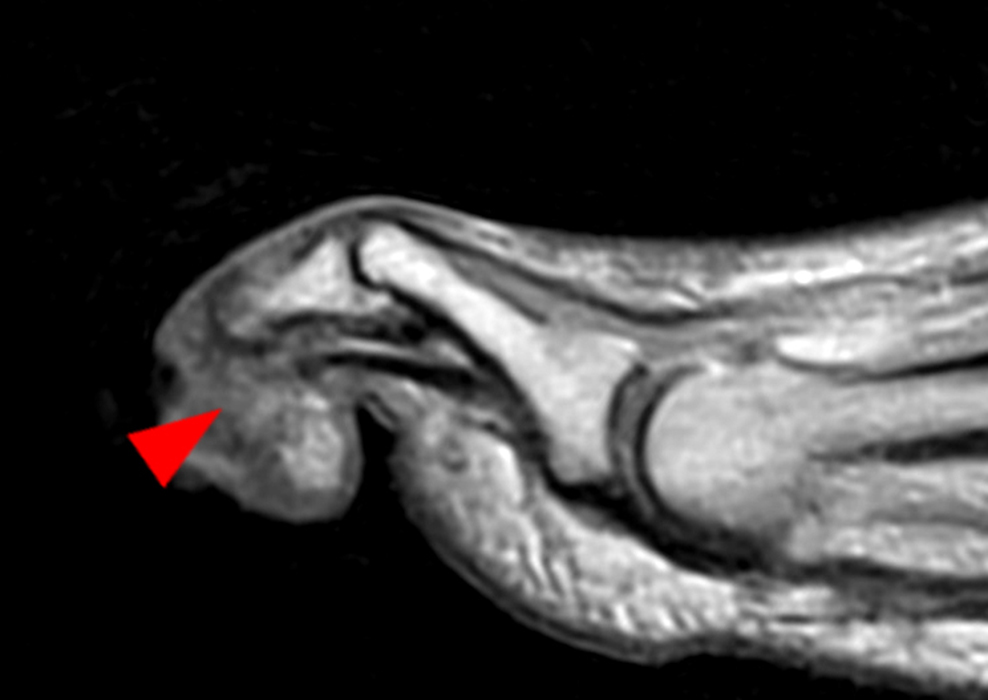
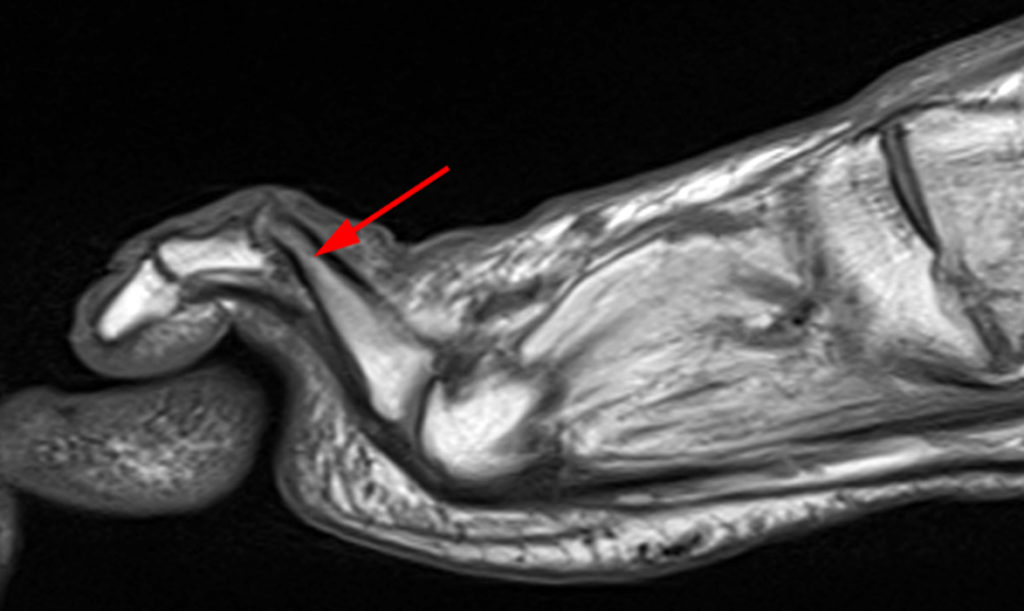
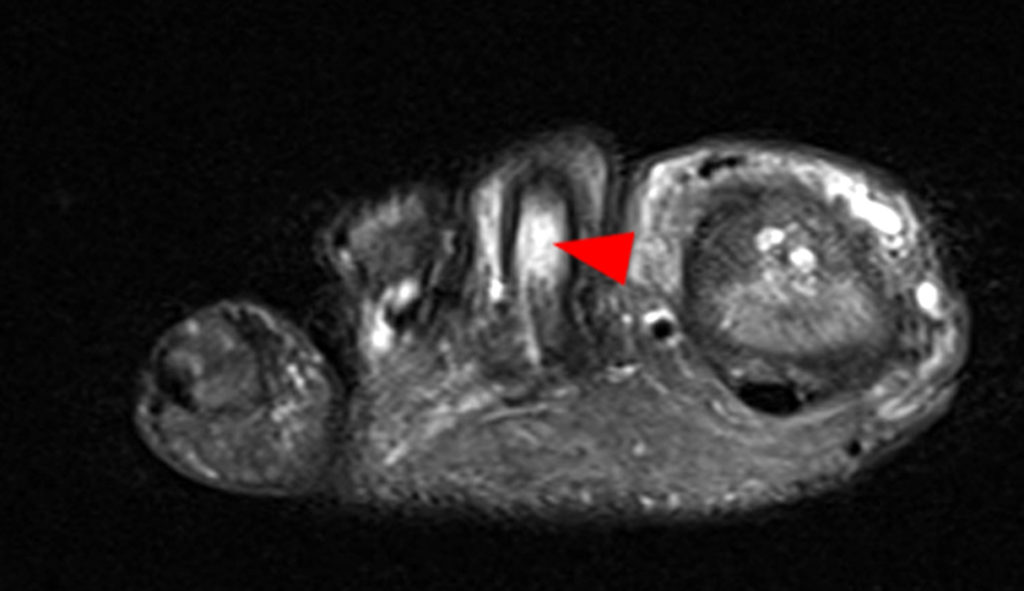
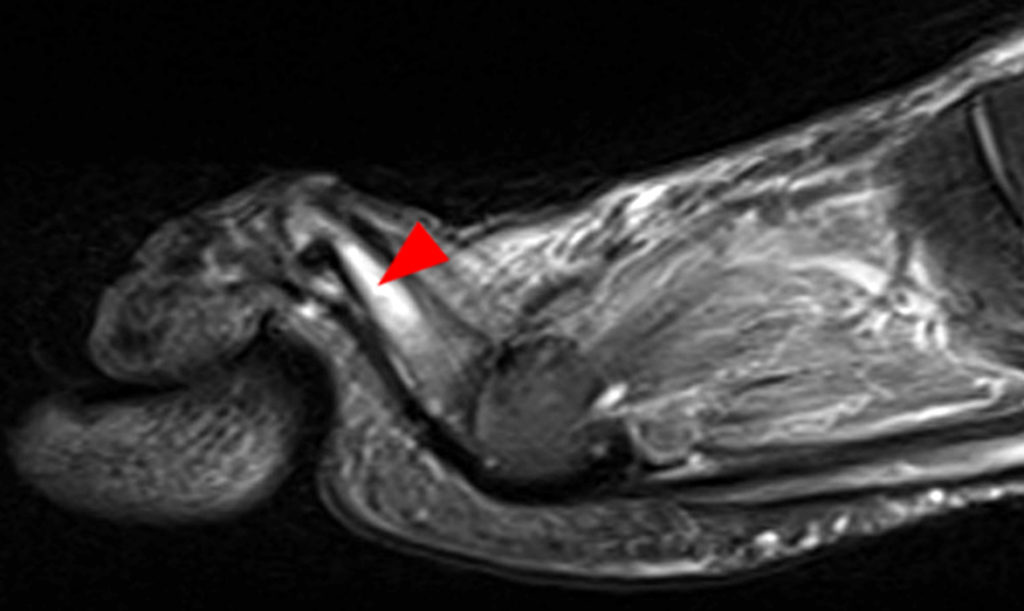
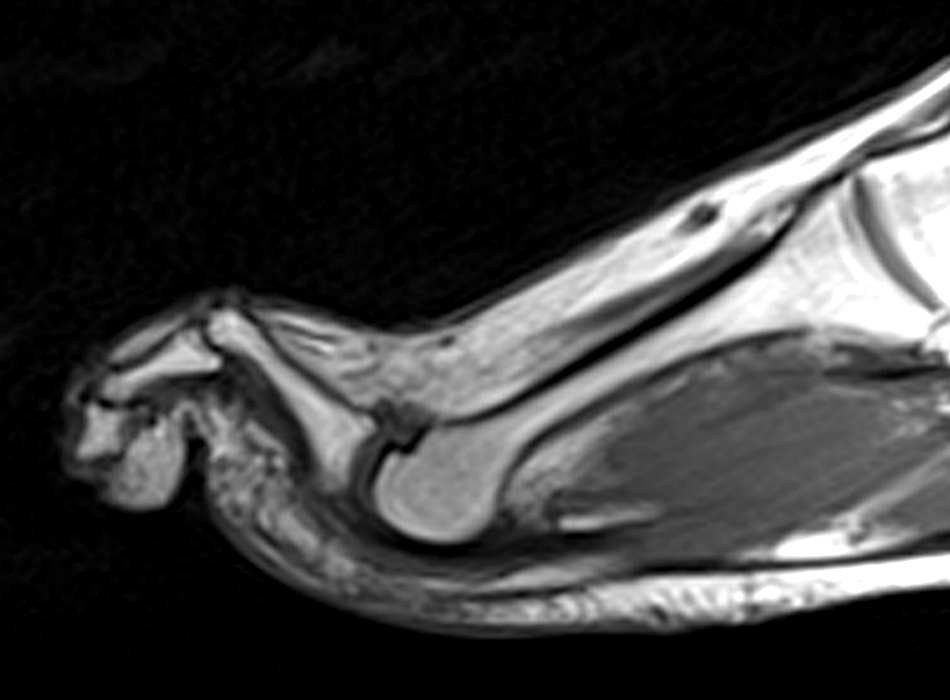
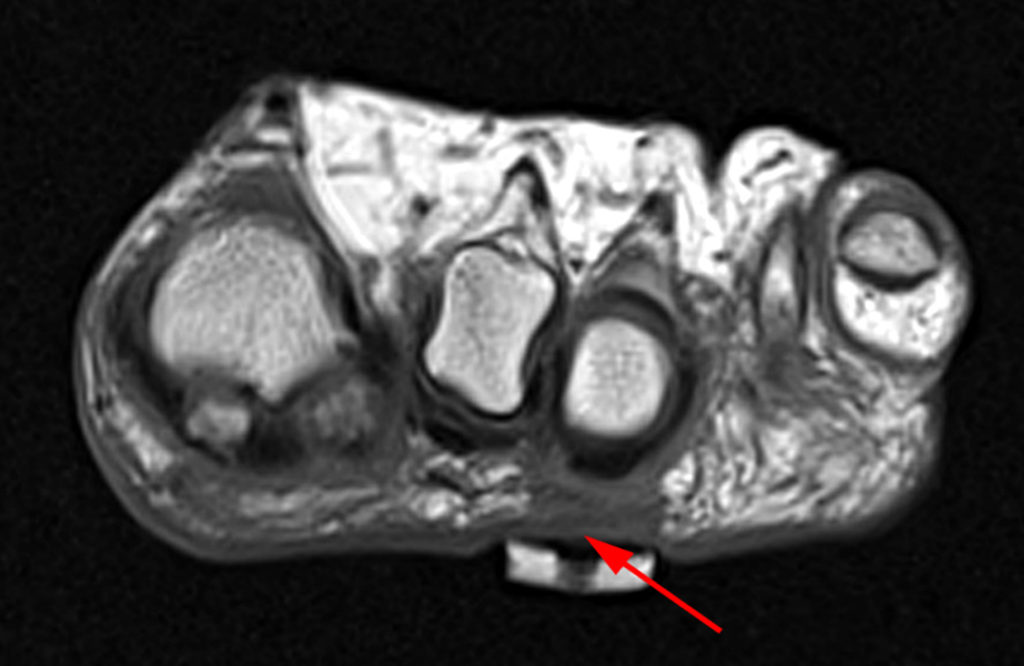
Clinical History: A 50-year-old female presents with pain and swelling for 3 weeks. MRI was performed because of clinical suspicion for osteomyelitis. Sagittal proton density-weighted, sagittal STIR, and post-gadolinium sagittal T1-weighted with fat suppression images through the 4th toe are provided (Figure 1). What are the findings? What is your diagnosis?
Findings
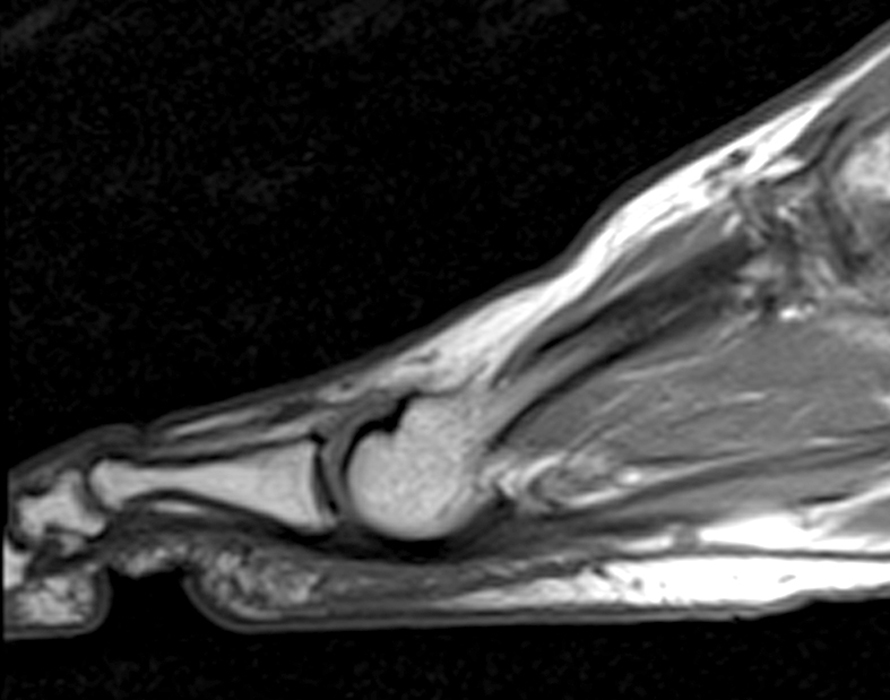
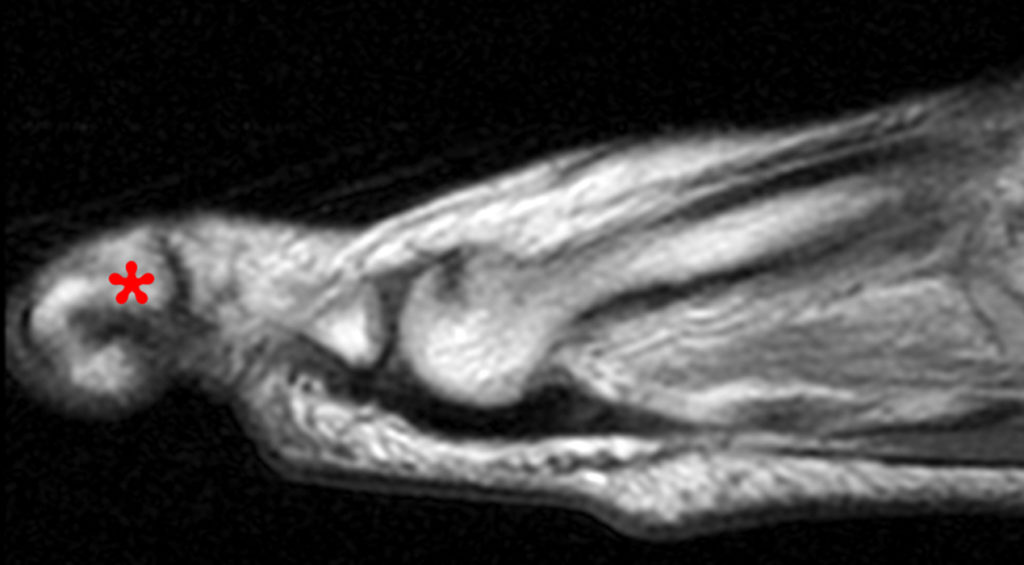
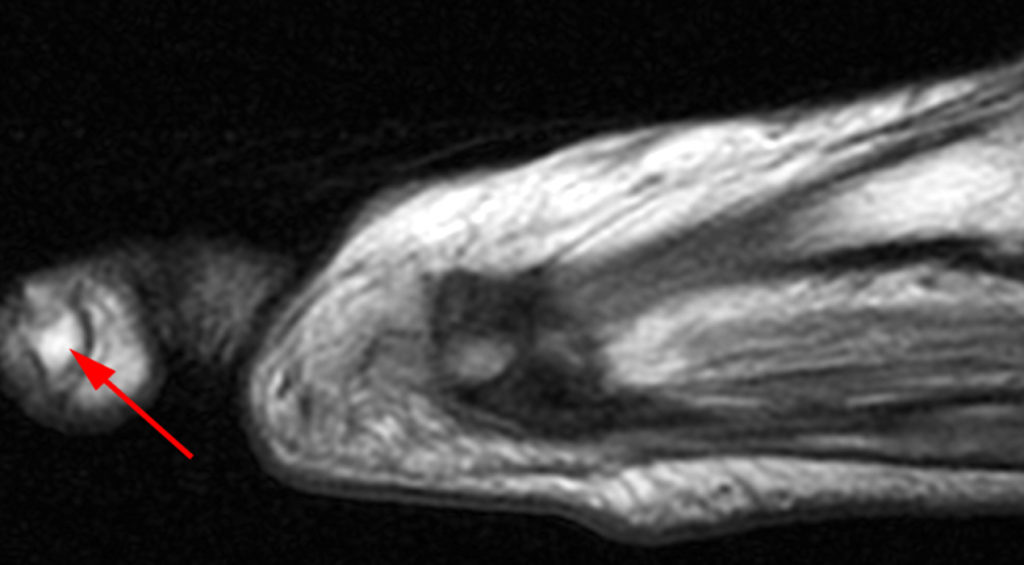
Figure 2:
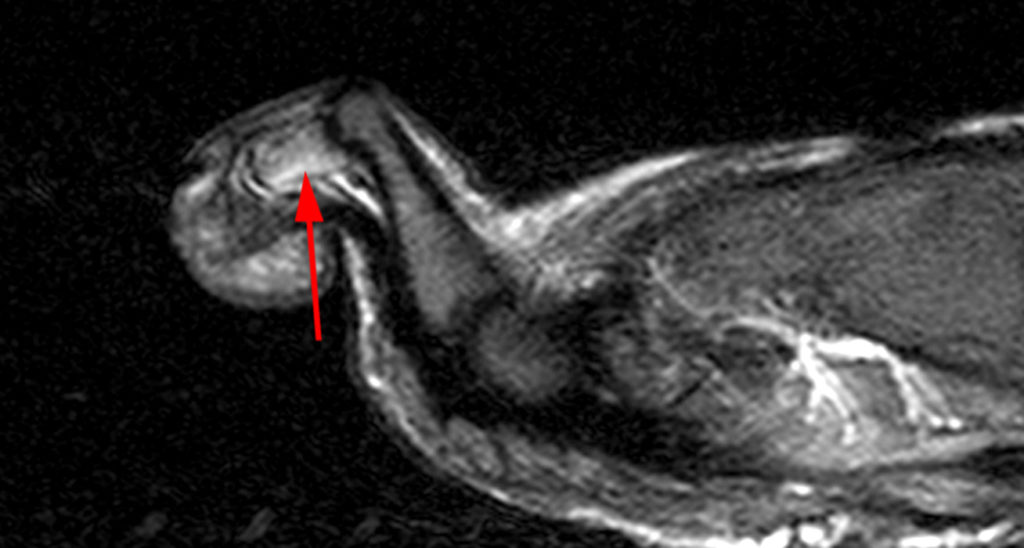
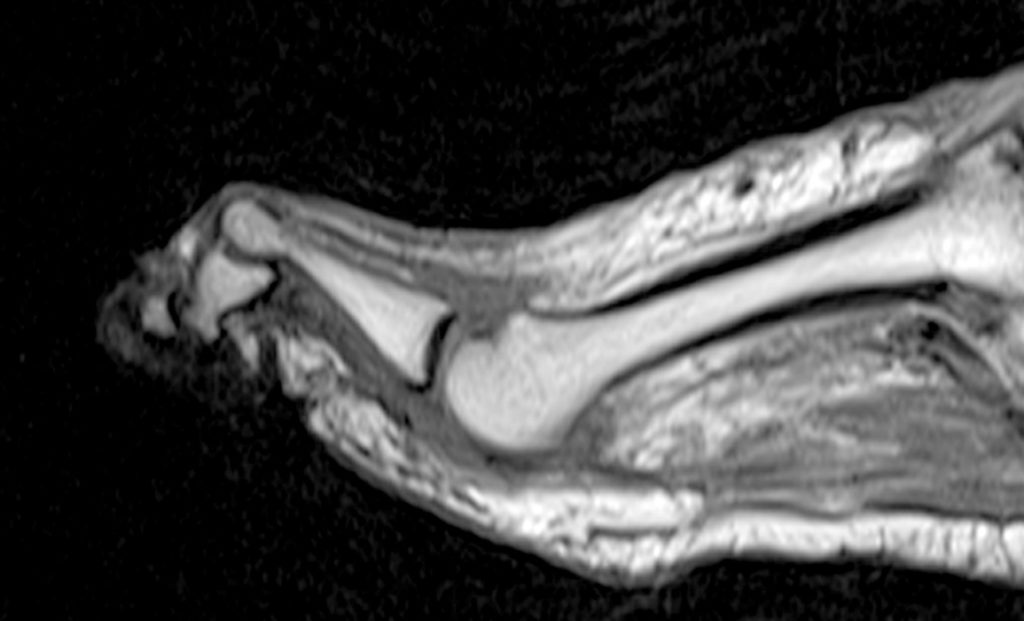
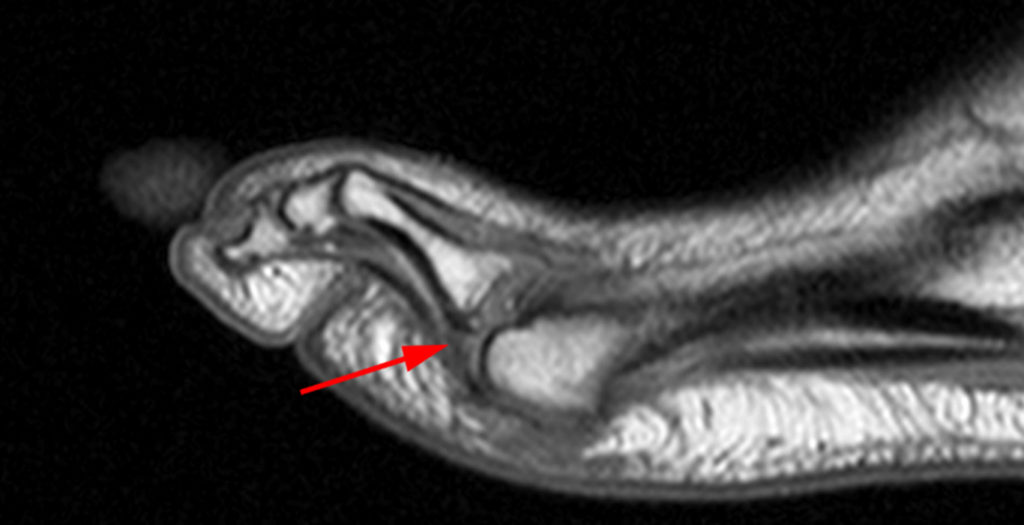
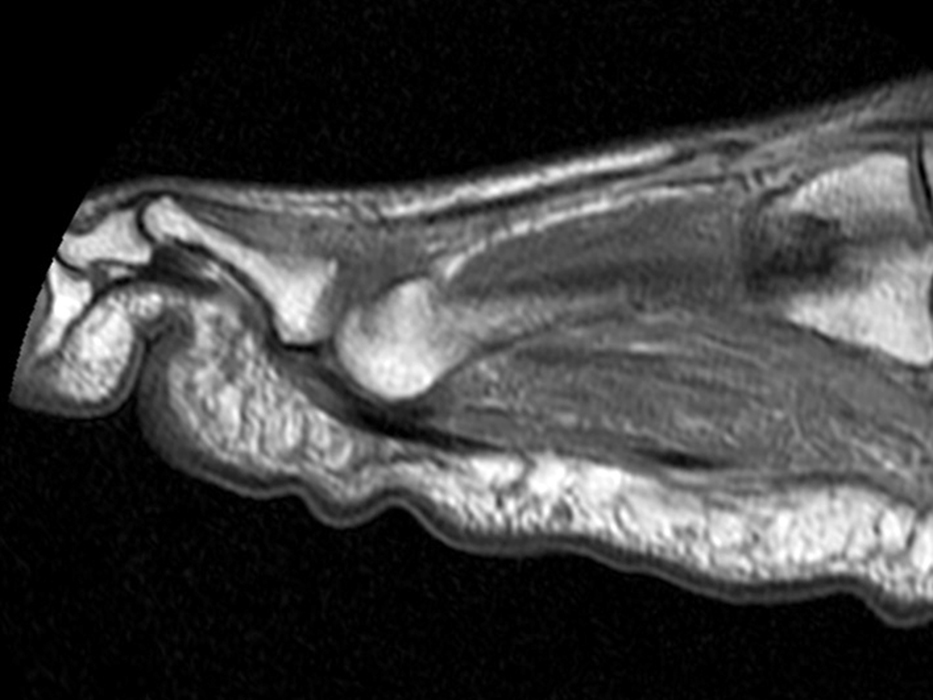
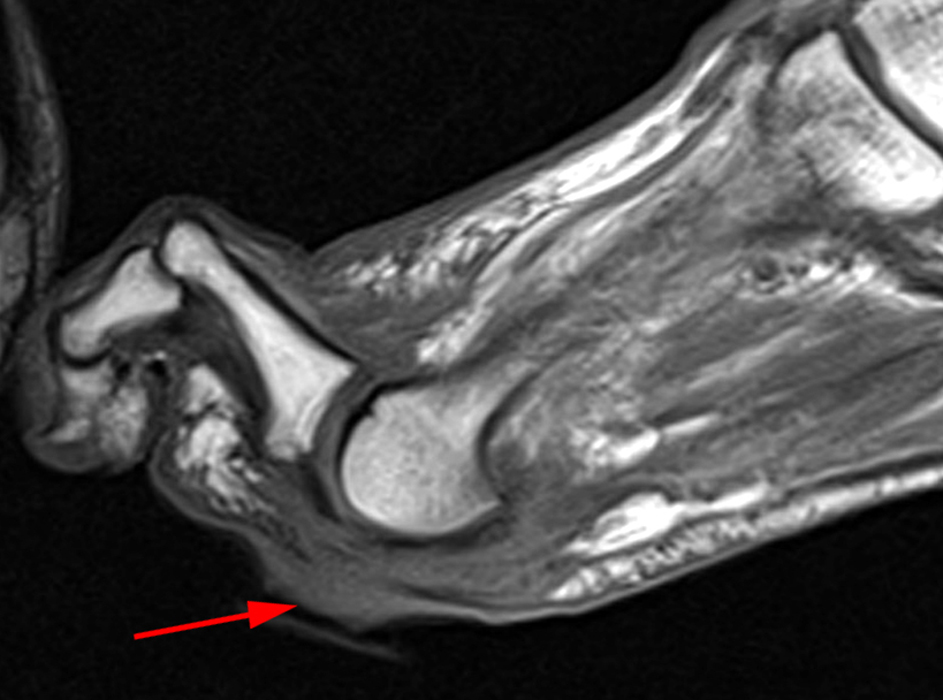
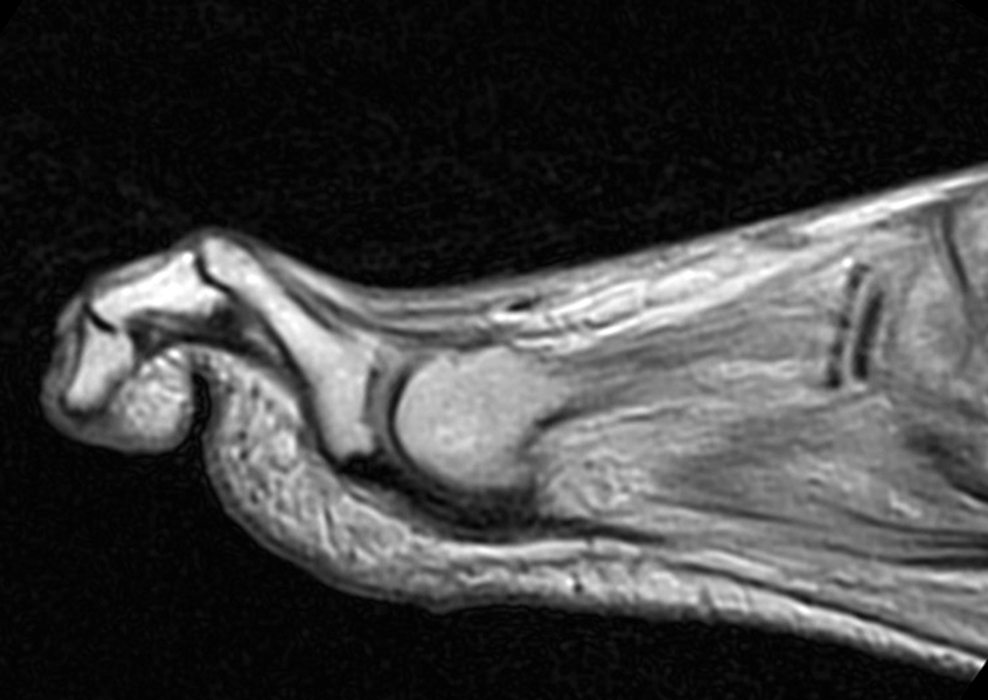
Figure 2: Sagittal proton-density weighted (2a), sagittal STIR (2b), and post gadolinium sagittal T1-weighted fat suppressed (2c) images through the 4th toe demonstrate a mallet toe deformity with the anatomy best appreciated on the proton-density weighted image (2a) showing hyperflexion of the DIP joint with normal alignment at the PIP and MTP joints. The STIR image (2b) demonstrates severe increased signal of the distal phalanx consistent with marrow edema (arrow). The T1 post gadolinium series (2c) demonstrates prominent enhancement of the distal phalanx (arrow).
Diagnosis
4th mallet toe deformity, complicated by osteomyelitis of the distal phalanx.
Introduction
Toe deformities are common, especially in the elderly, and are usually diagnosed clinically. With radiographic imaging alone, it is often difficult to properly characterize these deformities due to overlapping of the digits on lateral radiographs. The potential complications associated with the deformities can be well characterized with MR imaging.
Characterization of Lesser Toe Deformities
Hammer Toe
Figure 3:
In hammertoe deformity, flexion at the PIP joint results in increased pressure often accompanied by callus formation (red arrow). The extensor tendons are most tightly attached to the extensor sling and plantar aspect of the proximal phalanx resulting in extension at the MTP joint with less extension force distally at the middle and distal phalangeal insertions. The resulting hammertoe deformity is characterized by hyperflexion at the PIP joint with hyperextension of the MTP joint, and in late stage, hyperextension of the DIP joint.
In a hammer toe, the primary deformity is hyperflexion at the proximal interphalangeal (PIP) joint (Figure 5). There can also be hyperextension at the metatarsophalangeal (MTP) (Figure 4) and/or the distal interphalangeal (DIP) joints (Figure 7). A major cause of hammer toe deformities is improper footwear, usually presenting in the fifth and sixth decades of life, but hammer toes can also be associated with hallux valgus, inflammatory arthritis, and trauma, the latter due to an acute rupture of the central slip of the extensor tendon which may cause the deformity.1,2 The pull of the extensor tendons is mainly transmitted to the MTP joint via the extensor sling. The extensors are therefore unable to correct the PIP joint deformity, but hyperextension may occur at the MTP joint instead (Figure 6). This may progress to MTP joint instability as the plantar plate becomes attenuated (Figure 8).3,4 The DIP joint remains largely unaffected or may become hyperextended (Figure 7) by the pull of the extensors via the lateral slips. At first, a hammer toe may maintain flexibility. However, eventually the tendon can contract and tighten, causing a permanent, fixed deformity. Shoes can rub against the raised portion of the toe or toes, causing painful corns or calluses and even ulcerations leading to osteomyelitis (Figure 6). Common associated findings with a hammer toe are a long second toe, tight toe box (footwear), diabetes, inflammatory arthritis (with synovitis weakening the plantar plate), and hallux valgus deformity. Surgical management is indicated for progressive deformity, fixed contractures, dorsal toe ulcerations, and osteomyelitis.
Figure 5:
44-year-old female presents with clinical complaint of plantar fasciitis with both MR ankle and foot imaging performed. Sagittal T1-weighted image through the 5th toe demonstrates hyperflexion at the PIP joint and mild hyperextension at the MTP joint, findings of early mallet toe deformity. The patient also had an early mallet toe deformity of the 2nd toe. (Figure 10).
Figure 6:
75 y/o male presented in April 2015 following trauma to the great toe and subsequent soft tissue infection. The sagittal T1 series (6a) demonstrates marked hyperflexion of the PIP joint, severe hyperextension of the MTP joint, and preservation of normal alignment of the DIP joint of the 2nd toe representing a hammer toe deformity. The patient returned in July 2016 following amputation of the great toe and with cellulitis of the 2nd toe. Sagittal STIR series at that time (6b) demonstrates increased signal within the middle phalanx (arrow) consistent with edema and suggestive of osteomyelitis. Again demonstrated is hyperflexion of the PIP joint and hyperextension of the MTP joint and new mild hyperflexion of the DIP joint, progressing to early claw toe deformity.
Figure 7:
68-year-old female status post 2nd toe debridement with cellulitis. The sagittal proton density-weighted image demonstrates advanced hammer toe deformity with hyperflexion of the PIP joint and hyperextension of the MTP and DIP joints. The patient also had a hammer toe deformity of the 3rd digit and claw toe deformities of the 4th and 5th digits (Figure 13).
Figure 8:
45-year-old male presented with dislocation of the 4th and 5th toes and pain. The sagittal T1-weighted image through the 5th digit demonstrates a hammer toe deformity with hyperflexion of the PIP joint as well as hyperextension and dorsal subluxation of the MTP joint and tear of the plantar plate (arrow).
Mallet Toe
Figure 9:
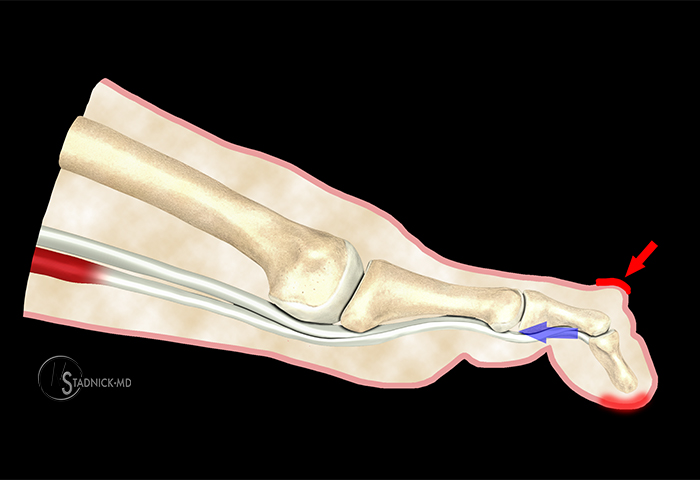
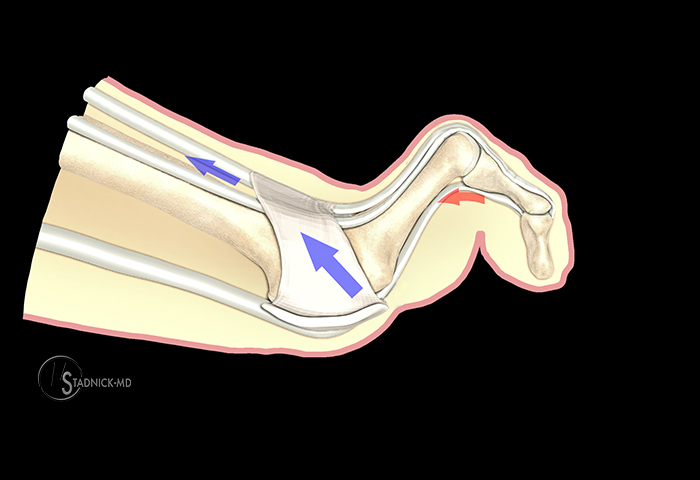
Mallet toe deformity occurs with excessive or unopposed flexor digitorum longus tendon force at the DIP joint (blue arrow). The classic mallet toe deformity is an isolated hyperflexion of the PIP joint. Callus formation dorsal to the DIP joint (red arrow) and tenderness or callus at the tip of the toe may occur from excessive pressure.
Mallet toe is a rare, isolated flexion deformity of the DIP joint of the foot (Figure 10). Thus, good case examples were difficult to find for presentation. The DIP joint deformity in mallet toes is often attributed to overly tight footwear (tight toe box). Initially the distal interphalangeal joint flexes due to direct pressure from the shoe (Figure 11). Eventually the flexor digitorum longus tendon (FDL) tightens, causing a persistent deformity. The mallet deformity is flexible in the early stages, but as the collateral ligaments and capsule tighten, the deformity becomes fixed. This may be associated with callous formation at the tip of the toe and pressure on and subsequent deformity of the nail.5 The cause of a mallet toe is often rupture of the distal aspect of the extensor tendon with an unopposed flexor tendon. It may also be related to contracture of the FDL tendon, trauma, and a long digit.
Figure 10:
44-year-old female presents with clinical complaint of plantar fasciitis with both MR ankle and foot imaging performed. Sagittal T1-weighted image through the 2nd toe incompletely demonstrates mild plantar flexion of the DIP joint with preservation of normal alignment of the MTP and PIP joints consistent with early mallet toe deformity. The patient also had a hammer toe deformity of the 5th digit. (Figure 5).
Claw Toe
Figure 12:
Claw toe deformity can become fixed with chronic hyperextension at the MTP joint from the action of the extensor tendons at the MTP joint (blue arrows) and chronic shortening of the flexor tendons (red arrow). The typical claw toe deformity demonstrates hyperextension of the MTP joint and hyperflexion at the PIP and DIP joints.
The claw toe deformity is defined as hyperextension of the MTP joint of the foot with hyperflexion of the PIP and DIP joints (Figure 13). It is considered more severe but less common than a hammer toe deformity. A claw toe is commonly seen in neuromuscular disorders and thus usually involves all of the lesser toes.6 Initially this clawing may be flexible and only noticeable on walking. When the MTP joint becomes chronically hyperextended, the intrinsic muscles shorten and can therefore no longer produce flexion at the MTP joint and the extensor tendons are unopposed.7 The flexors are pulled taut and flex the PIP and DIP joints. Over time the plantar plate tears, subluxation occurs at the MTP joint, and the deformity becomes permanent.3 In both claw and hammer toes, eventually the toes cannot be brought into contact with the ground during walking. More force is then taken over the metatarsal heads which can result in metatarsalgia and soft tissue changes (Figures 14 and 17) as well as increased susceptibility to osteomyelitis (Figures 15 and 16).3 Common pathologies associated with a claw toe are diabetes, trauma (injury to the undersurface of foot leads to progressive contracture of the FDP), synovitis/inflammatory arthritis, Charcot-Marie-Tooth disease, and other neuromuscular disorders.
Figure 13:
68-year-old female status post 2nd toe debridement for cellulitis. Sagittal T1-weighted image of the 4th toe demonstrates hyperflexion of the PIP and DIP joints and mild hyperextension of the MTP joint consistent with claw toe deformity. The patient also had a hammer toe deformity of the 3rd digit (Figure 7) and claw toe deformity of the 5th digit.
Figure 14:
78-year-old male presents with a plantar ulceration. Sagittal T1-weighted image demonstrates hyperextension of the MTP joint and hyperflexion at the PIP and DIP joints consistent with a claw toe deformity. Abnormal pressure on the plantar forefoot likely contributed to the ulceration (arrow).
Figure 15:
60-year-old male presented with 3rd toe ulceration and swelling. Sagittal proton density-weighted imaging of the 2nd toe (15a) demonstrates hyperflexion at the PIP and DIP joints and mild hyperextension of the MTP joint consistent with claw toe deformity. Similar findings of the 4th toe were also present. Axial proton density-weighted image (15b) shows increased signal of the distal phalanx of the 3rd toe consistent with edema (arrow). Sagittal proton density-weighted image of the 3rd toe (15c) demonstrates erosive changes of the distal phalanx (arrowhead) consistent with osteomyelitis.
Figure 16:
58-year-old diabetic male imaged to evaluate a chronic non-healing ulcer of the great toe. Sagittal T1-weighted image (16a) demonstrates hyperextension of the MTP joint, moderate hyperflexion of the PIP joint, and mild hyperflexion of the PIP joint of the 2nd toe, consistent with claw toe. Decreased T1 signal is present within the distal end of the proximal phalanx suggesting edema (arrow). Coronal (16b) and sagittal (16c) fat-suppressed T2-weighted images demonstrate increased signal (arrowheads) confirming edema. The findings are compatible with osteomyelitis.
Figure 17:
71-year-old male with history of “hammer toe” deformity and pain. The sagittal T1-weighted image (17a) demonstrates hyperextension of the MTP joint along with hyperflexion of the PIP and DIP joints consistent with claw toe deformity. A similar deformity of the 3rd toe was demonstrated on sagittal views. Coronal T1-weighted image (17b) demonstrates decreased signal within the subcutaneous space fat plantar to the 3rd MTP joint (arrow) consistent with chronic pressure related changes, likely due to the altered mechanics.
Discussion
Lesser toe deformities are common and are associated with significant morbidity including pain, callus formation, and ulcerations/infection. In the elderly, they can even lead to gait instability and subsequent falls. The metatarsal (MT) heads take a considerable proportion of the body weight during walking, particularly the first, second, and third toes. The lesser toes increase the surface area for weight-bearing and share the load with the MT heads. This can only occur if the toes remain extended and in contact with the ground during walking.8
The lesser toes usually have a distal, middle, and proximal phalanx. Supporting structures of the joints are medial and lateral collateral ligaments and the joint capsules. Each of the lesser toes has two flexor tendons, the flexor digitorum longus (FDL) and the flexor digitorum brevis (FDB). The attachments in the toes are similar to the flexor digitorum superficialis and flexor digitorum profundus attachments in the fingers. The FDL travels deep to the FDB and attaches to the plantar aspect of the base of the distal phalanx. The FDB travels plantar (superficial) to the FDL dividing into two slips just proximal to the PIP joint and then attaches to the plantar base of the middle phalanx. The FDL is responsible for flexing the DIP joint and the FDB for flexing the PIP joint.
The extensor mechanism of the lesser toes is more complex. The extensor digitorum longus (EDL) tendon passes dorsal and central to the MTP joint and is joined at this level by the extensor digitorum brevis (EBD) tendon from the lateral side (except for the fifth toe where the EDB is absent). The tendons then trifurcate into a central slip, which attaches to the middle phalanx, and medial and lateral slips which attach onto the base of the distal phalanx.3 The proximal phalanx does not receive a direct extensor tendon attachment, rather the extensor tendons form a sling-like aponeurotic structure which encircles the MTP joint. This apparatus merges with the plantar plate before inserting on the plantar base of the proximal phalanx. It is termed the extensor sling and extends the MTP joint.3
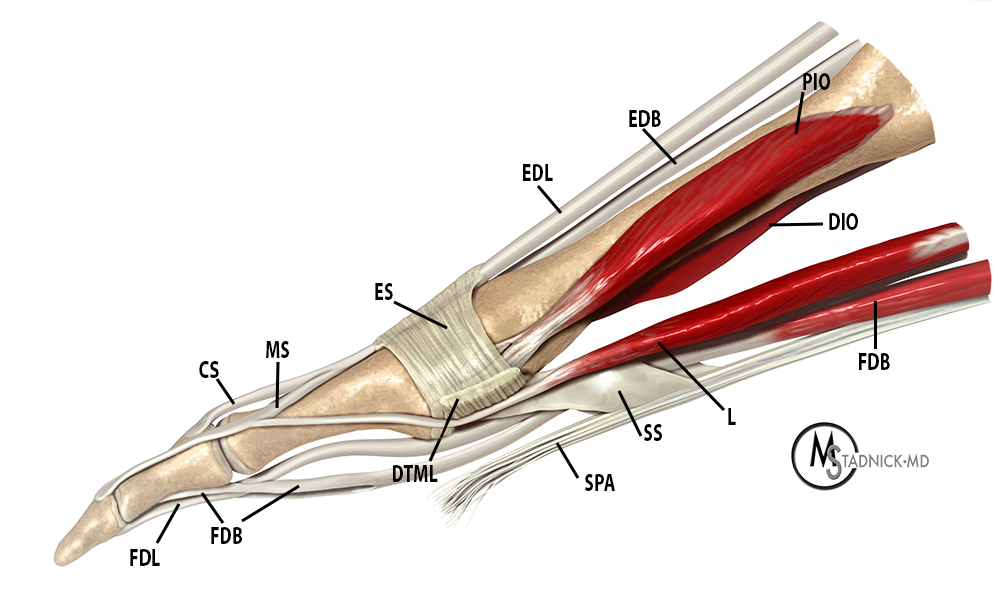
Figure 18:
A medial view of the 3rd digit demonstrates relevant musculotendinous, ligamentous, and aponeurotic anatomy. Abbreviations: extensor digitorum longus (EDL), extensor digitorum brevis (EDB), extensor sling (ES), central slip of the extensor apparatus (CS), medial slip of the extensor apparatus (MS), flexor digitorum longus (FDL), flexor digitorum brevis (FDB), 2nd lumbrical muscle (L), plantar interosseous muscle (PIO), dorsal interosseous muscle (DIO), deep transverse metatarsal ligament (DTML), superficial plantar aponeurosis (SPA), and sagittal septum plantar aponeurosis (SS).
The plantar fascia is an important anatomic structure relative to deformities of the lesser toes. It is an aponeurotic structure arising from the calcaneus and inserting on the proximal phalanx of each toe. In conjunction with the osseous arch of the foot the plantar fascia forms a “truss.” Hyperextension of the MTP joint tightens the plantar fascia, pulling the calcaneus and MT heads towards each other, and thus increases the height of the longitudinal arch, referred to as the “windlass” mechanism. In contrast, during weight-bearing, the downward force exerted on the talus flattens out the longitudinal arch. The plantar fascia stretches, as the MT heads and calcaneus move apart, which in turn exerts a strong plantar flexion force at the MTP joint. This is termed the “reverse windlass: mechanism and is essential for maintaining toe contact with the ground during walking.3,9
Although lesser toe deformities can be brought on acutely due to trauma, most have a chronic, gradual onset. Etiologies of the deformities are ill-fitting or high-heeled footwear, inflammatory arthritis, synovitis, diabetes mellitus, and neuromuscular disorders.
The etiology of both hammer toe and mallet toe deformities can be narrow, ill-fitting footwear. The toes are forced to conform to a small toe box, buckle, and become deformed, initially flexible then subsequently fixed.6 Other than ill-fitting shoes, the specific cause of a mallet toe is often unknown. Although most cases are idiopathic, the deformity can also develop after a hammer toe repair, possibly due to scarring and contracture of the flexor tendon.6
A hammer toe or claw toe deformity may also be caused by a muscle imbalance in association with neuromuscular diseases, such as Charcot-Marie-Tooth disease, Friedreich ataxia, cerebral palsy, myelodysplasia, multiple sclerosis, and degenerative disk disease. A hammer toe or claw toe deformity also may be seen in patients with an insensate foot associated with diabetes.6 Occasionally, after fractures of the tibia or other trauma, a progressive hammer toe deformity is observed and is likely the result of nerve or muscle injury from elevated compartment pressures in the involved leg or foot.6 Plantar plate injuries can be a primary cause of toe deformity or a result of chronic long-term hyperextension of the MTP joints.10,11,12,13
There are both conservative and operative treatment options, aimed at restoring alignment, reducing discomfort, and attempting to eliminate potential complications.
Conclusion
Although evaluation of and characterization of lesser toe deformities is not in itself typically a common indication for MR imaging, the modality is an excellent means for evaluation of important complications related to these deformities. MR imaging will often assist in surgical planning as well as determining the cause of deformities. The three major types of lesser toe deformities described in this Web Clinic can be easily and properly characterized once the types are understood.
References
- Coughlin MJ. Lesser toe deformities. In: Coughlin MJSC, Anderson RB, eds. Mann’s surgery of the foot and ankle. Ninth ed Elsevier; 2014:322-424. ↩
- Coughlin MJ, Dorris J, Polk E. Operative repair of the fixed hammertoe deformity. Foot Ankle Int. 2000 Feb; 21(2):94-104. ↩
- Malhotra K, Davda K, Singh D. The pathology and management of lesser toe deformities. EFORT Open Rev.2016; 1:409-419. ↩
- Veljkovic A, Lansang E, Lau J. Forefoot tendon transfers. Foot Ankle Clin. 2014 Mar; 19(1):123-37. ↩
- Shirzad K, Kiesau CD, DeOrio JK, Parekh SG. Lesser toe deformities. J Am Acad Orthop Surg. 2011; 1:9505-9514. ↩
- Coughlin MJ. Lesser Toe Deformities. https://musculoskeletalkey.com/lesser-toe-deformities-2/. ↩
- Myerson MS, Shereff MJ. The pathological anatomy of claw and hammer toes. J Bone Joint Surg Am. 1989 Jan; 71(1):45-9. ↩
- Hughes J, Clark P, Klenerman L. The importance of the toes in walking. J Bone Joint Surg Br. 1990 Mar; 72(2):245-51. ↩
- HICKS JH. The mechanics of the foot. II. The plantar aponeurosis and the arch. J Anat. 1954 Jan; 88(1):25-30. ↩
- Deland JT, Lee KT, Sobel M, DiCarlo EF. Anatomy of the plantar plate and its attachments in the lesser metatarsal phalangeal joint. Foot Ankle Int. 1995; 16(8):480–486. ↩
- Coughlin, MJ. Subluxation and dislocation of the second metatarsophalangeal joint. Orthop Clinics of North Am. 1989; 20(4):539–551. ↩
- Nery C, Coughlin MJ, Baumfeld D, Mann TS. Lesser metatarsophalangeal joint instability: prospective evaluation and repair of plantar plate and capsular insufficiency. Foot Ankle Int. 2012; 33(4):301–311. ↩
- Stainsby GD. Pathological anatomy and dynamic effect of the displaced plantar plate and the importance of the integrity of the plantar plate-deep transverse metatarsal ligament tie-bar. Ann R Coll Surg Engl.1997; 79(1):58–68. ↩