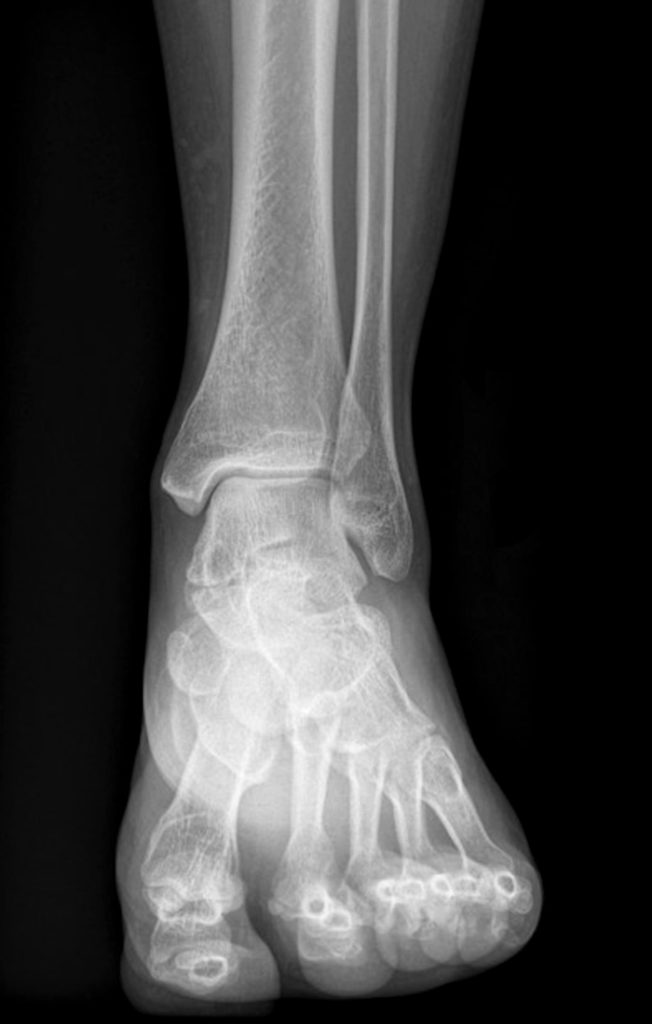
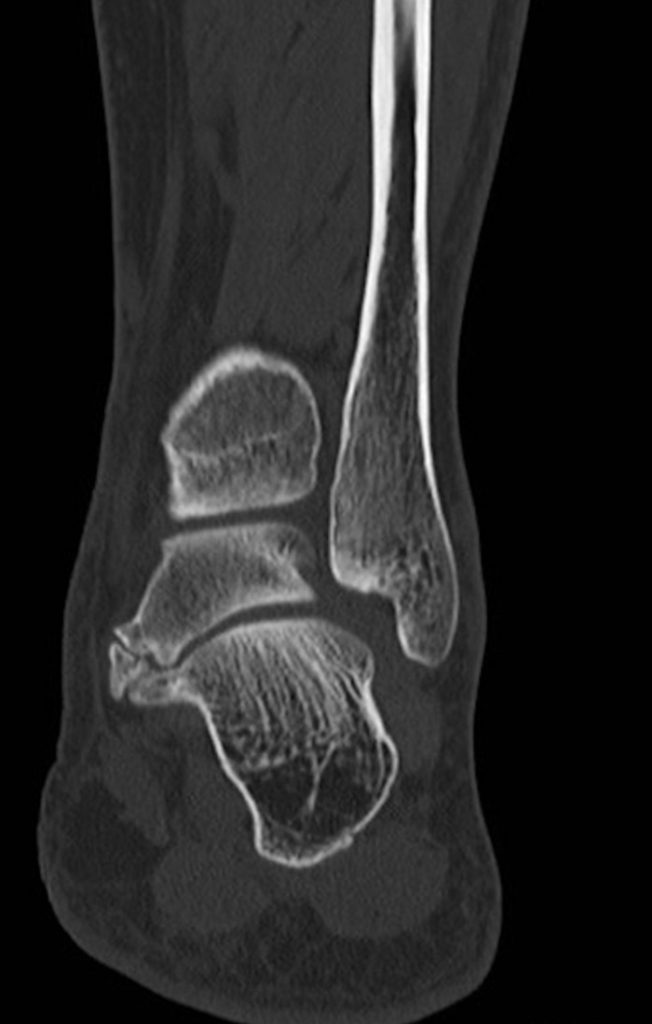
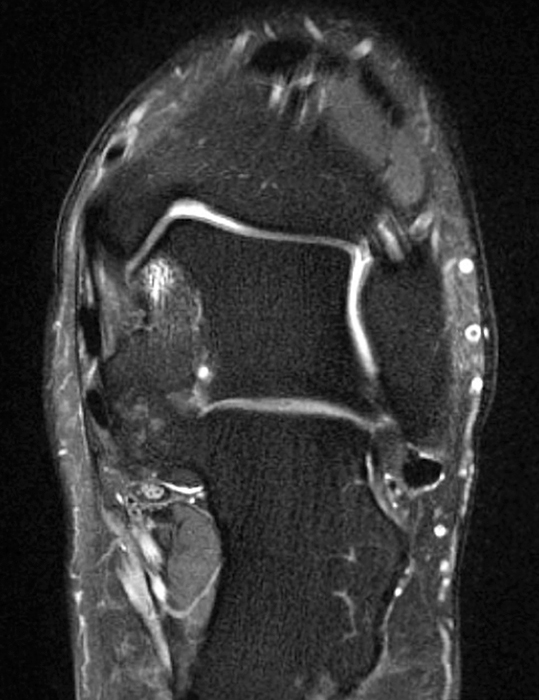
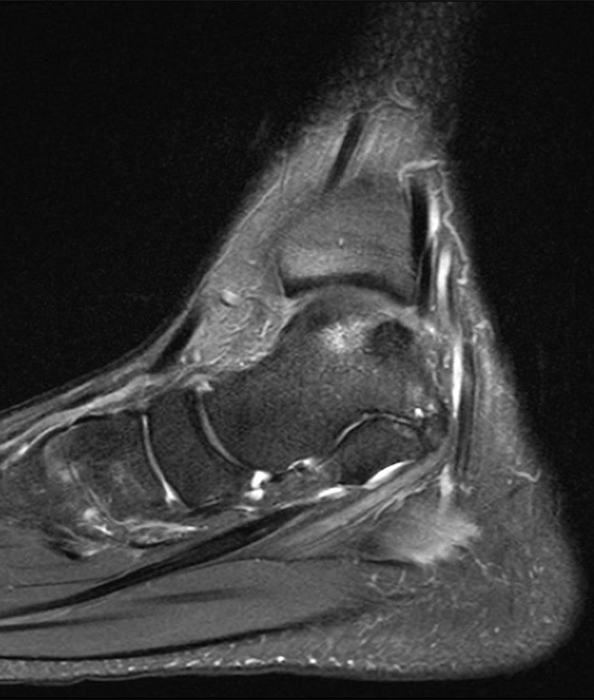
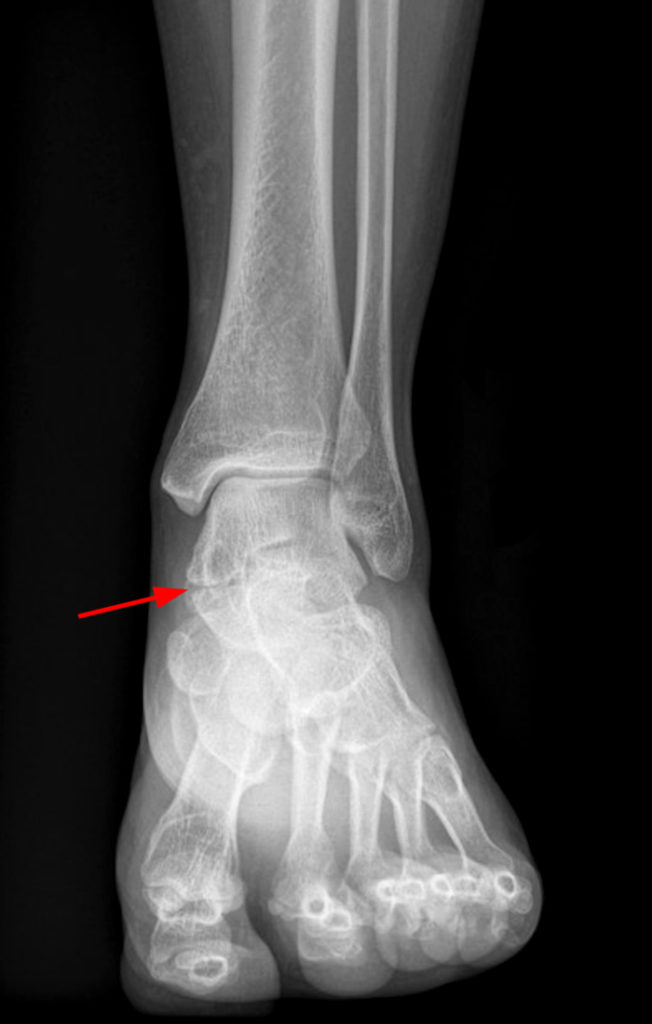
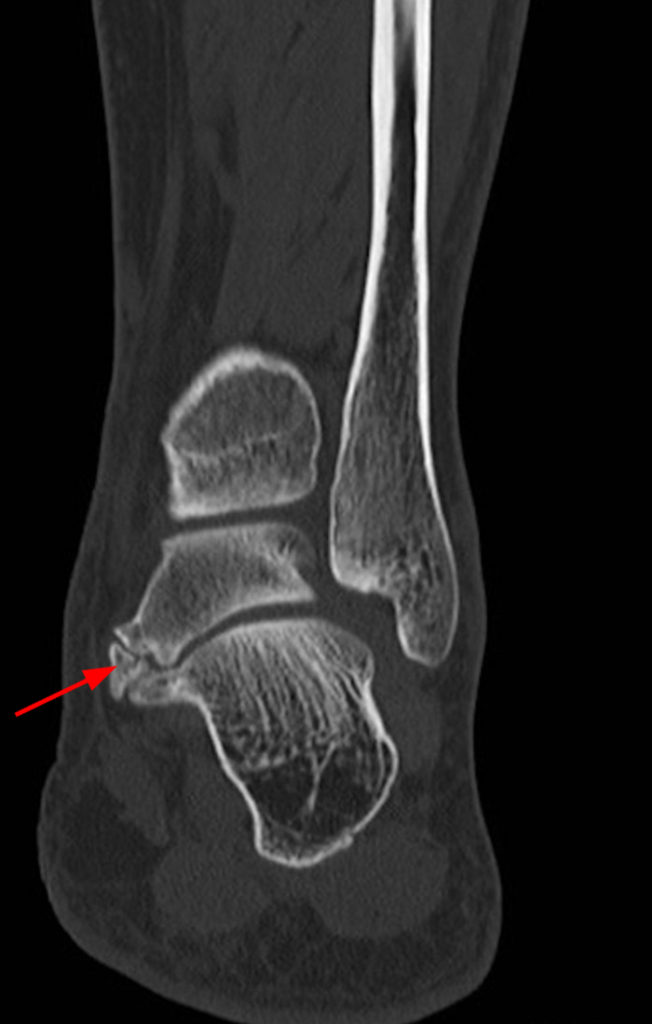
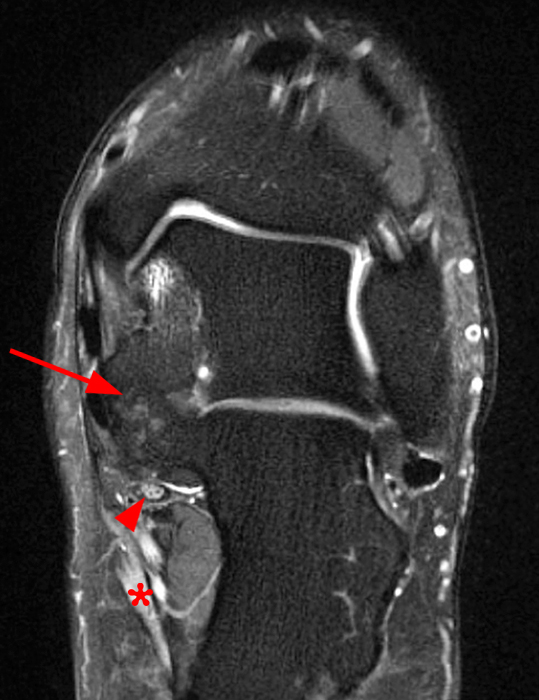
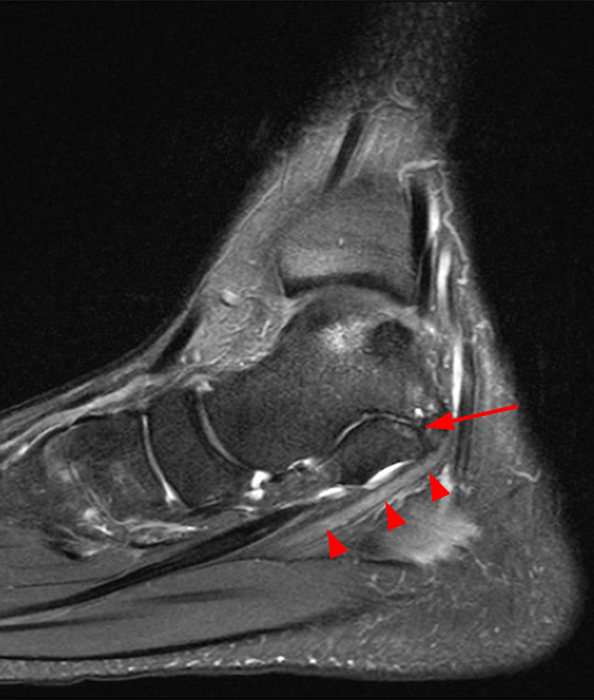
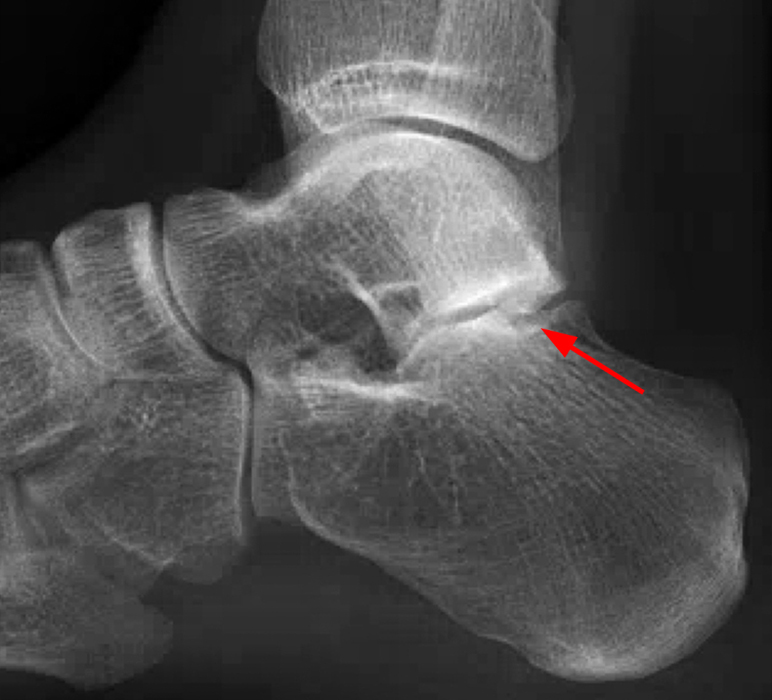
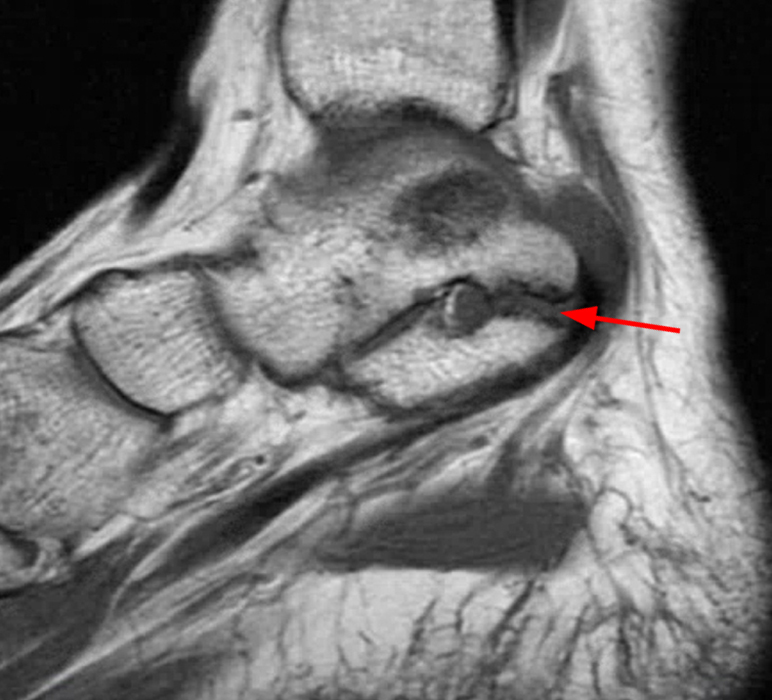
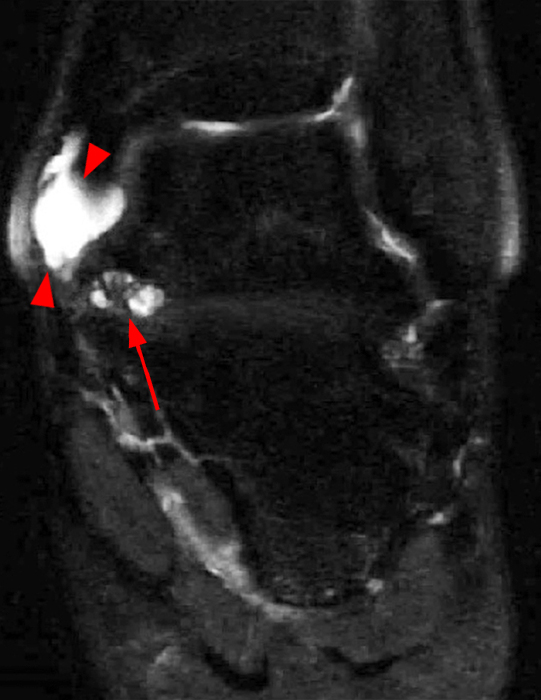
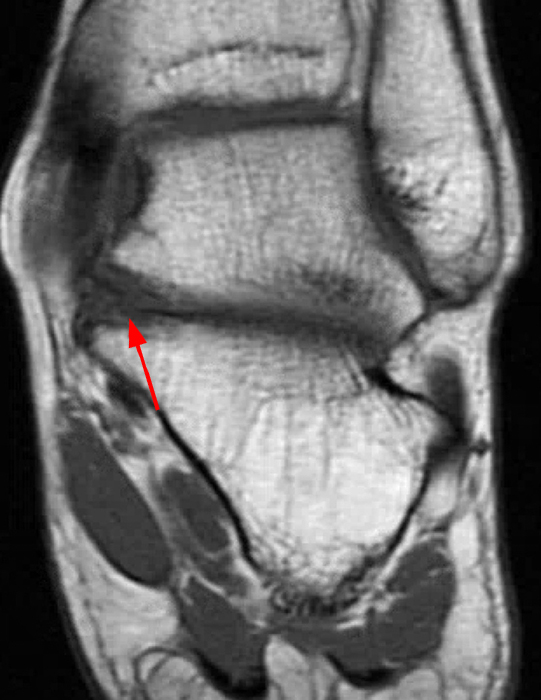
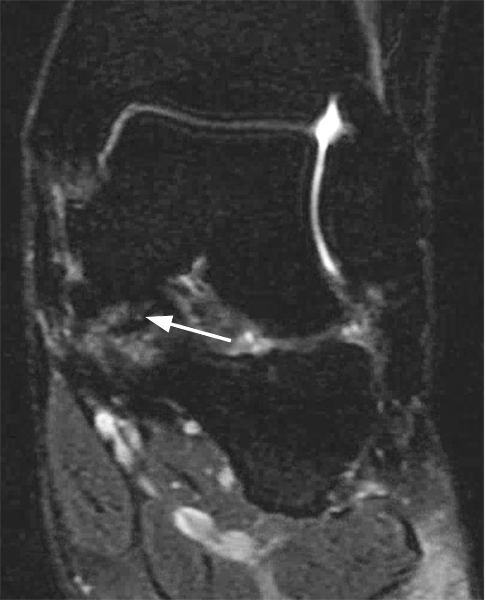
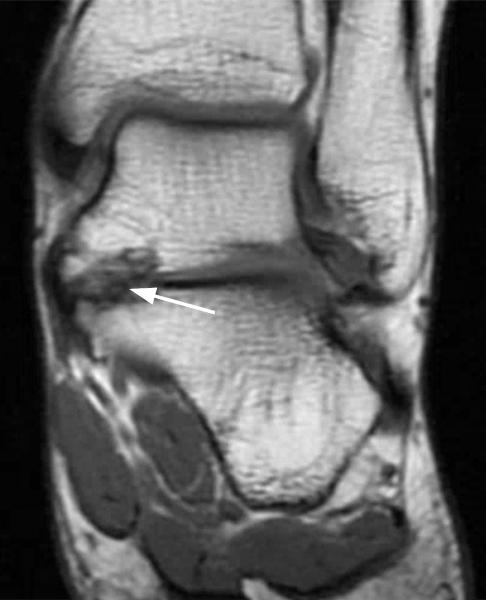
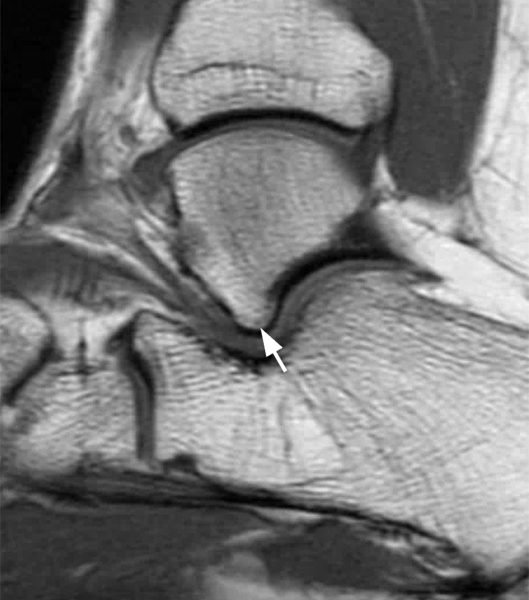
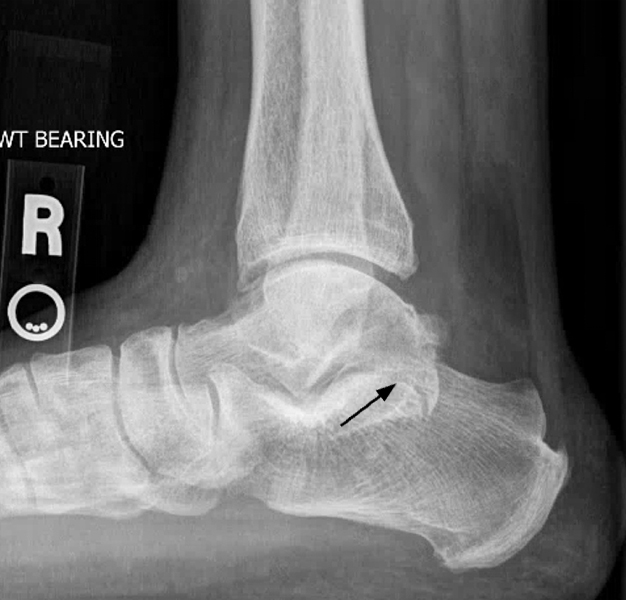
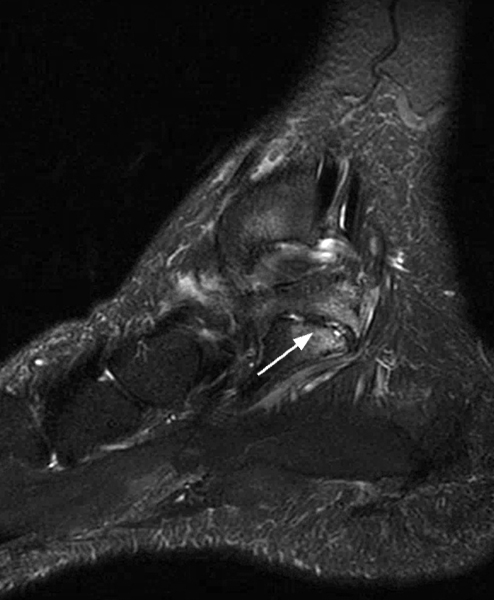
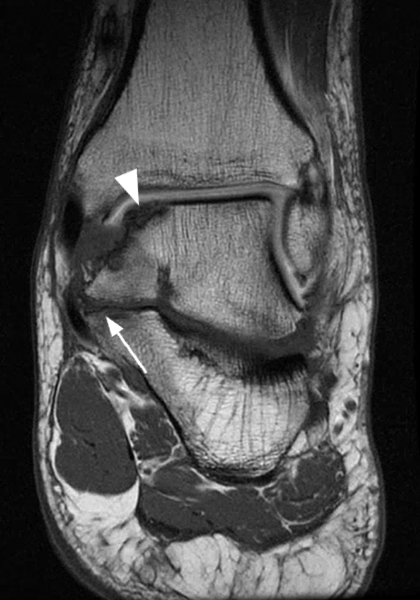
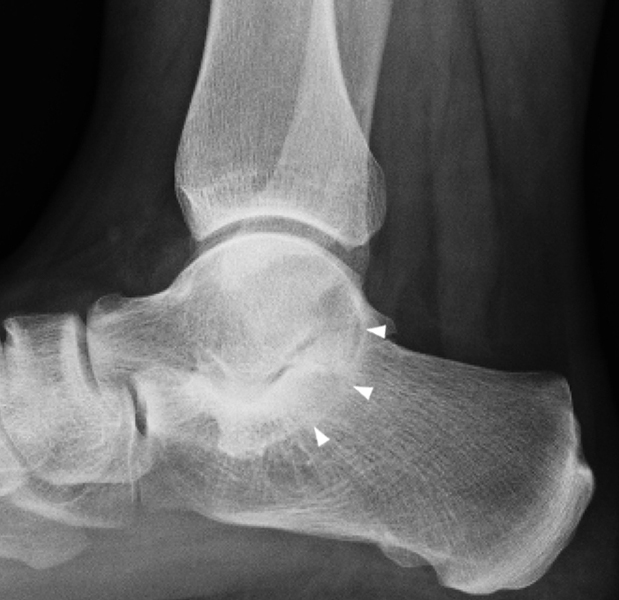
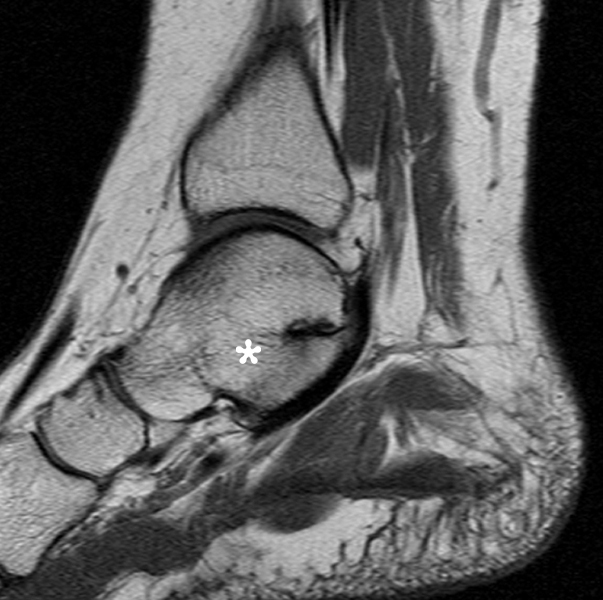
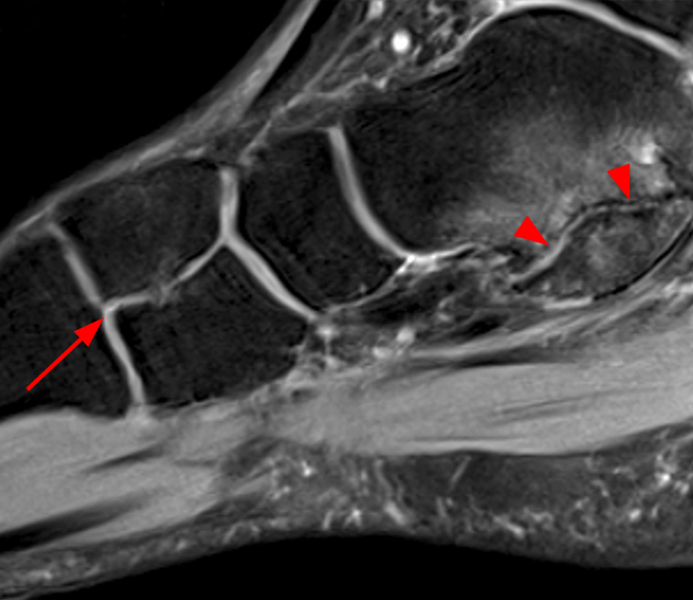
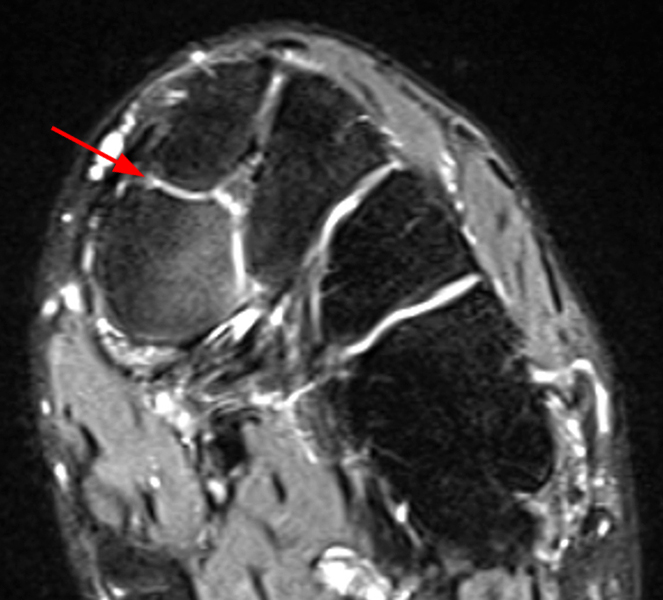
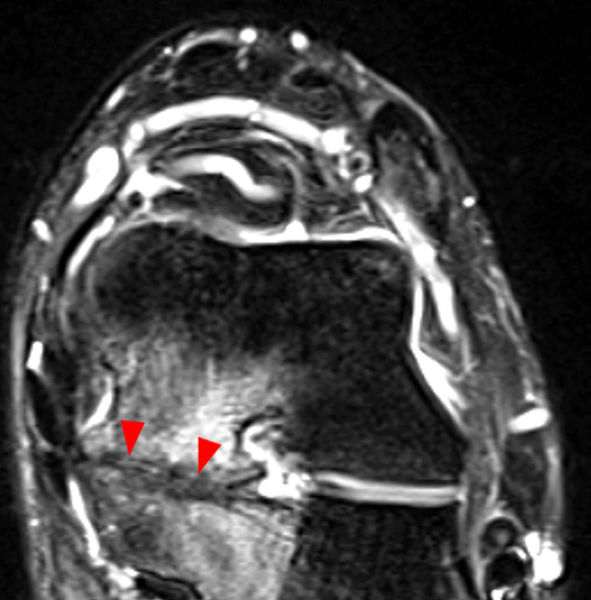
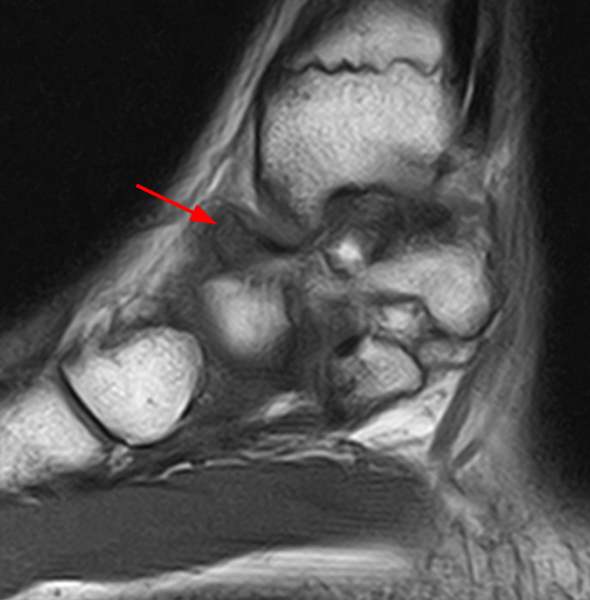
Clinical History: A 37-year-old man presented with left ankle pain that began while serving in the military. The pain is aggravated by prolonged standing and walking, and it prevents him from running. An anteroposterior (AP) radiograph (1A), coronal CT image (1B), and coronal oblique (1C), and sagittal (1D) T2-weighted fat-suppressed (T2 FS) magnetic resonance (MR) images are provided. What are the findings? What is your diagnosis?
Findings
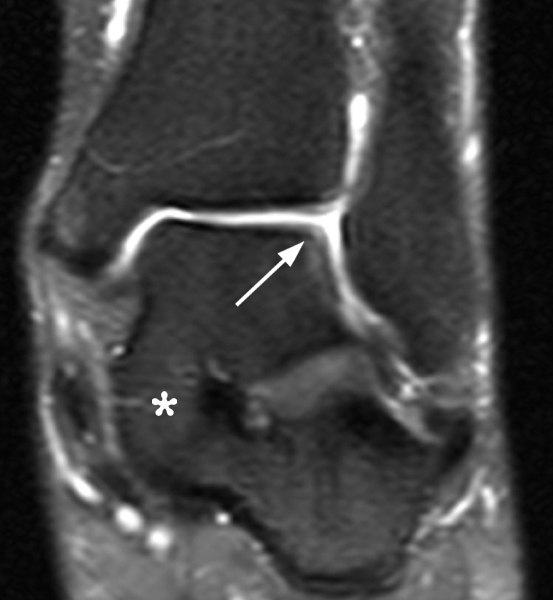
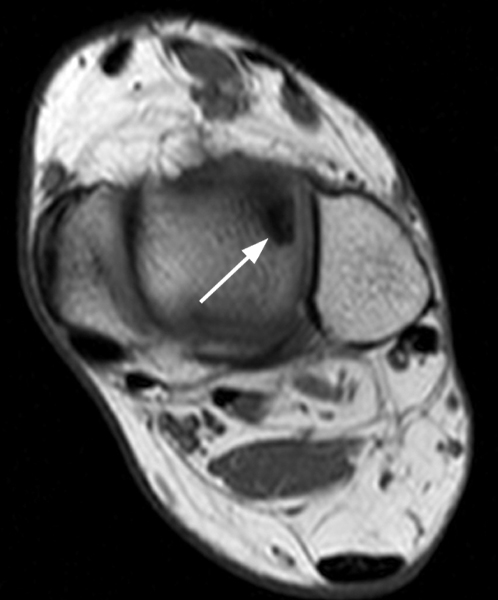
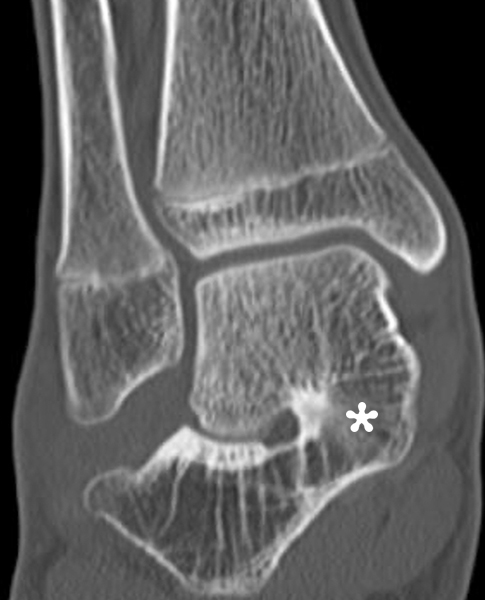
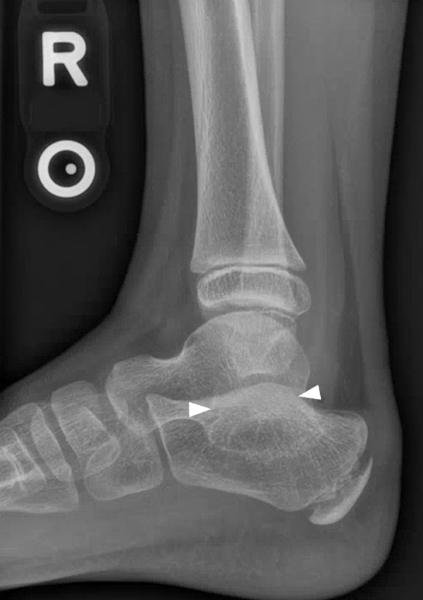
Figure 2:
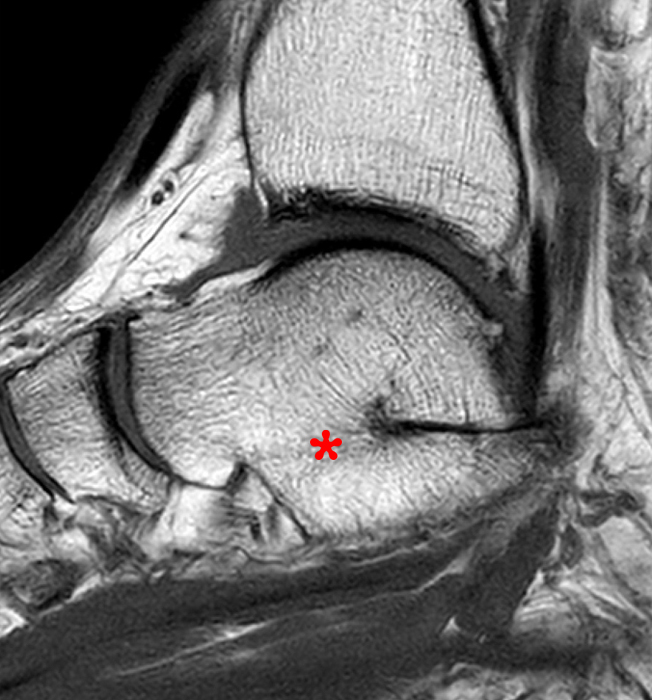
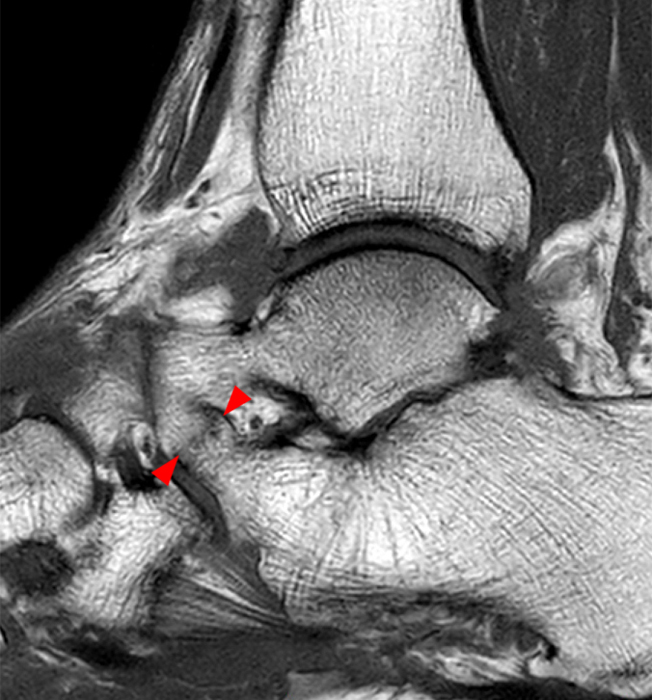
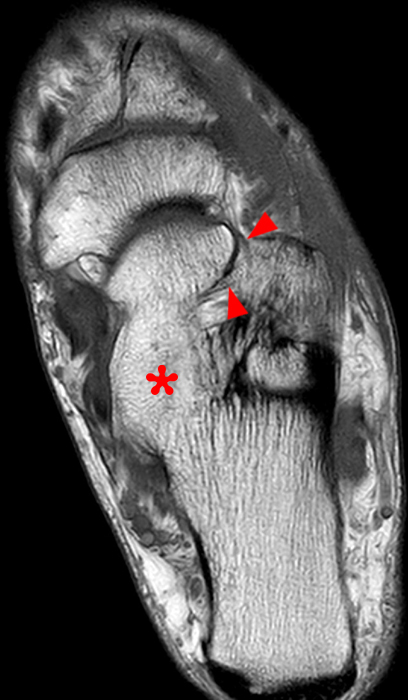
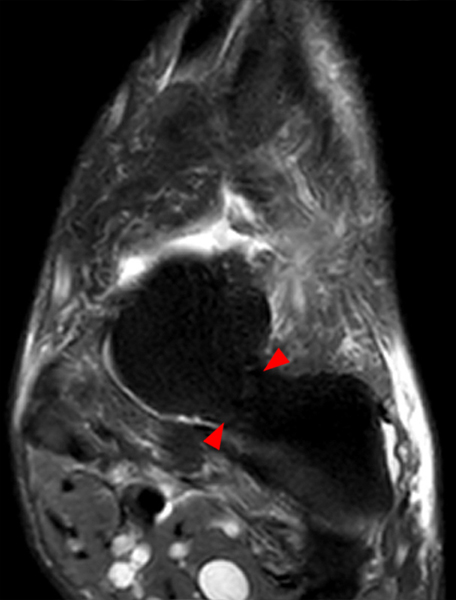
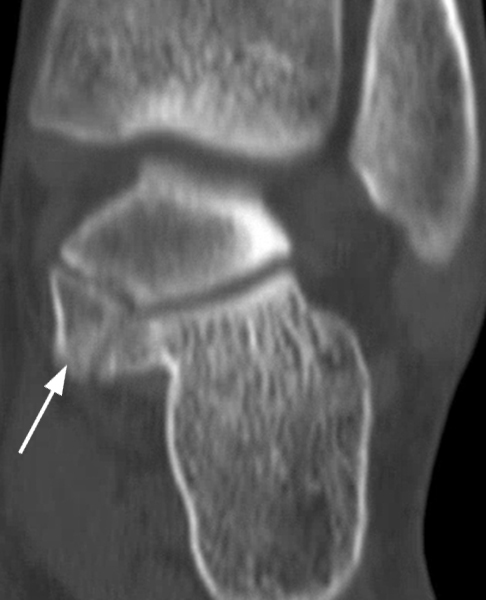
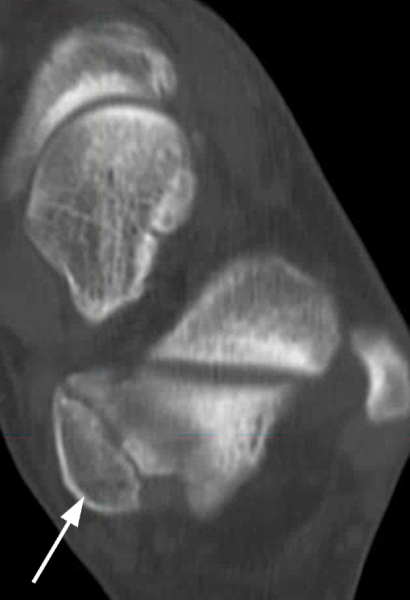
The AP radiograph (2A) demonstrates a talocalcaneal coalition (arrow). This is confirmed on the coronal CT image (2B), which demonstrates an extra-articular, non-osseous coalition located just posterior to the middle facets of the talus and calcaneus with an os sustentaculum (arrow). The coronal oblique (2C) and sagittal (2D) T2-weighted fat-suppressed MR images demonstrate increased signal and size of the medial plantar nerve (arrowheads) as it passes adjacent to the site of coalition (arrow), with accompanying edema of the abductor hallucis muscle compatible with denervation (asterisk). Images courtesy of Karen C. Chen, M.D.
Diagnosis
Extra-articular talocalcaneal coalition causing medial plantar neuropathy
Talocalcaneal Articulations
Understanding the complex anatomy of the talocalcaneal articulations is critical to the identification of abnormal union between these two tarsal bones. There are two separate articulations between the talus and calcaneus: the subtalar joint and the talocalcaneonavicular joint. The subtalar joint, sometimes designated the posterior subtalar joint, is comprised of two facets: the convex posterior facet of the calcaneus and the apposing concave posterior facet of the talus (Figures 3 and 4). The talocalcaneonavicular joint, sometimes designated the anterior subtalar joint, is comprised of the concave talar facet on the posterior surface of the navicular bone and four talocalcaneal facets: the concave middle and anterior facets of the calcaneus and the apposing middle and anterior facets of the talus. The middle facet of the calcaneus is designated the sustentaculum tali.
Figure 3:
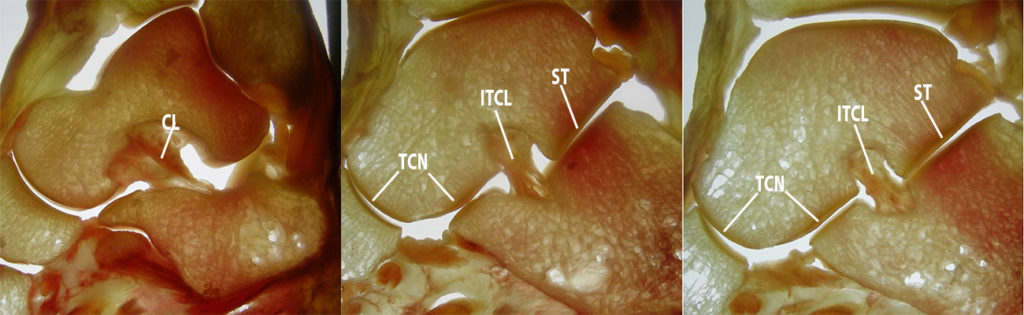
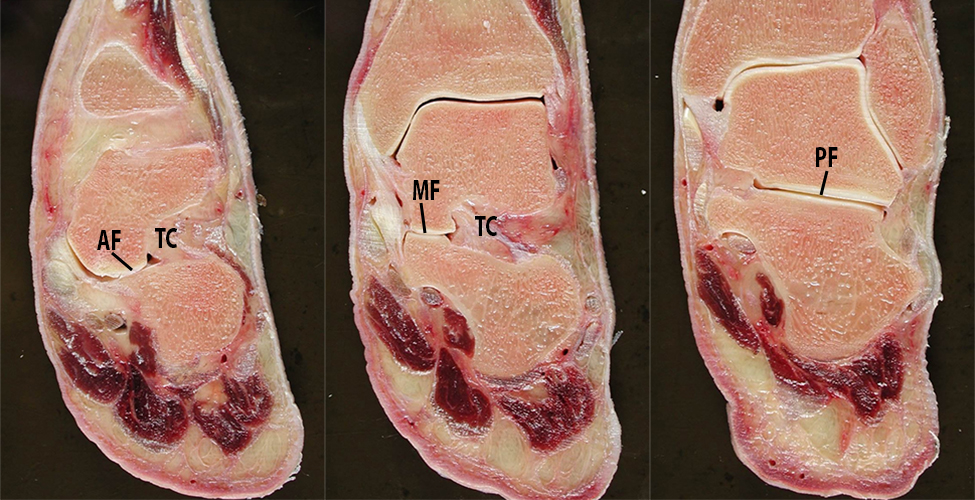
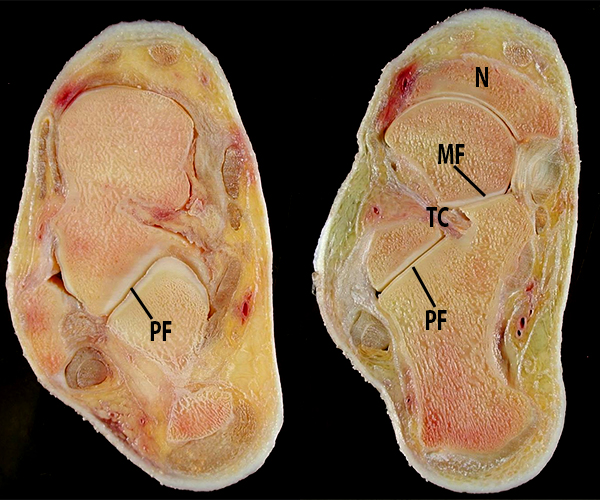
Anatomy of the normal talocalcaneal articulations. Serial sagittal sections (3A) from lateral to medial. Laterally, the cervical ligament (CL) is seen within the tarsal sinus between the inferolateral aspect of the talar neck and the dorsal neck of the calcaneus. More medially, the interosseous talocalcaneal ligament (ITCL) extends between the talus and calcaneus in the tarsal canal, which separates the subtalar joint (ST) from the talocalcaneonavicular joint (TCN). The latter joint has both: 1) a vertical component between the convex articular surface of the talar head and the concave articular surface of the navicular bone; and 2) a horizontal component between the plantar surface of the talus and the dorsal surface of the calcaneus. Serial coronal sections (3B) from anterior to posterior demonstrate the anterior (AF) and middle facets (MF) of the talocalcaneonavicular articulation, which are separated from the posterior facets (PF) of the subtalar articulation by the tarsal canal (TC). Axial sections (3C) demonstrate the posterior facets of the talus and calcaneus at the subtalar joint (left) (PF), and a more plantar axial section (right) demonstrates the middle facets of the talus and calcaneus (MF) of the talocalcaneonavicular joint separated from the posterior subtalar joint by the tarsal canal (TC). The navicular bone (N) is also visualized.
Figure 4:
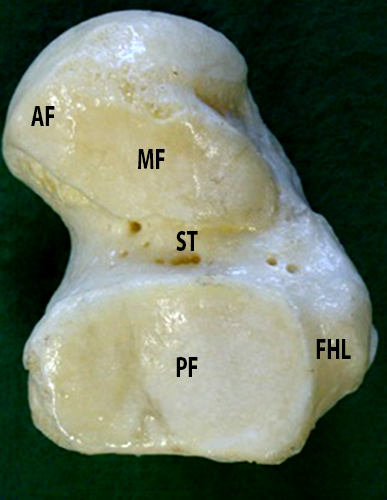
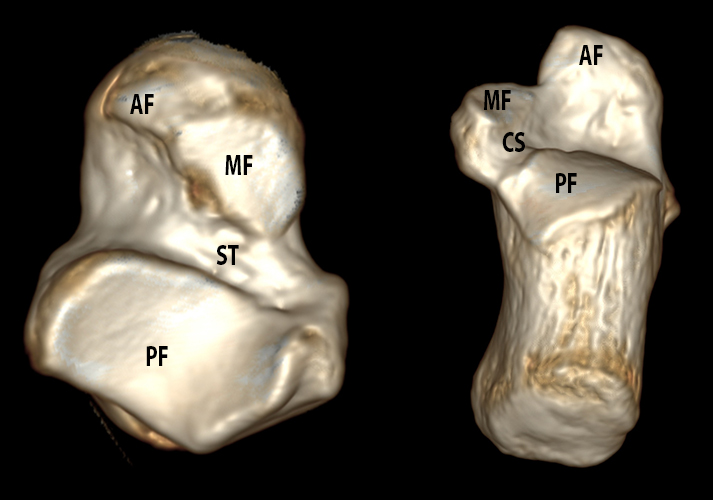
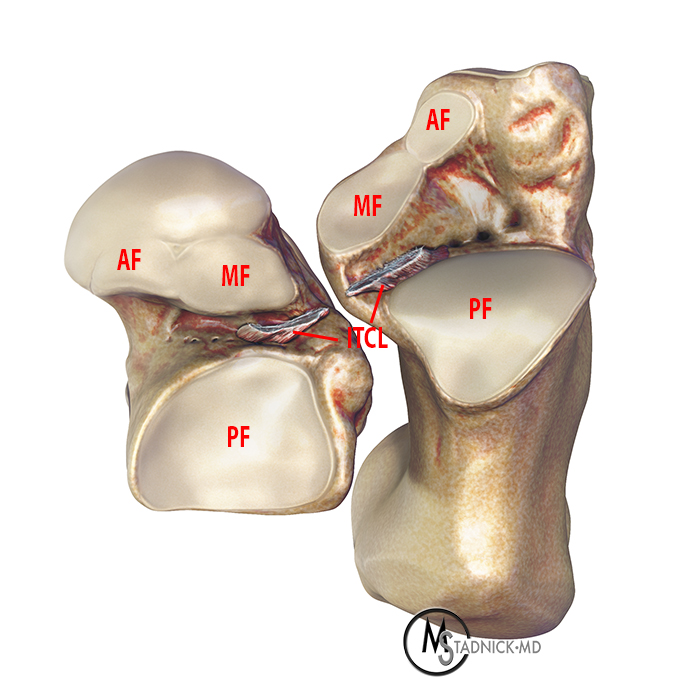
Anatomy of the normal talocalcaneal facets. Photograph of the plantar surface of a talar specimen (4A), volume-rendered CT images (4B) of the plantar surface of the talus (left) and the dorsal aspect of the calcaneus (right), and illustrations of the plantar surface of the talus and dorsal surface of the calcaneus (4C) demonstrate the normal relationships of the anterior (AF), middle (MF), and posterior facets (PF) of the talus and calcaneus. Note the convex posterior facet of the calcaneus and concave posterior facet of the talus. Similarly, the concave anterior and middle facets of the calcaneus are paired with the convex anterior and middle facets of the talus. Between the middle and posterior facets of the talus is the sulcus tali (ST). Between the middle and posterior facets of the calcaneus is the calcaneal sulcus (CS). The sulcus tali and calcaneal sulcus form the tarsal canal, where the ITCL (cut) normally extends from the talus to the calcaneus. The groove for the flexor hallucis longus tendon (FHL) lies just medial to the posterior talar facet.
Although, as above, three pairs of talocalcaneal facets are commonly described, cadaveric studies have shown several normal variants in the articulating facets of both the talus and calcaneus. A variation in a calcaneal facet is generally matched by the same variation in the adjacent talar facet and vice versa. The normal variants that have been described include absent anterior talocalcaneal facets, conjoined (also referred to as common, combined, continuous, or fused) anterior and middle facets, and continuous anterior, middle, and posterior facets.1,2,3,4,5,6,7 The missing anterior facets and conjoined anterior and middle facets have also been reported on MR imaging.8 Interestingly, the classically described configuration of three pairs of facets is not the most common anatomic variant. Cadaveric studies have shown that the most common variant is the conjoined anterior and middle facets, which has been reported to occur in 53-62% of studied populations.2,4,5 The number of facets may have implications for subtalar joint mechanics, with studies demonstrating both greater joint mobility1 and a higher prevalence of subtalar arthritis when the anterior and middle facets are conjoined as compared to three separate pairs of talocalcaneal facets.4
Whether the anterior and middle facets are conjoined or independent, the subtalar and talocalcaneonavicular joints are separated by the tarsal canal, which widens anterolaterally as the tarsal sinus. In approximately 20% of persons, the subtalar joint communicates with the tibiotalar joint.9
This short review of the anatomy of the plantar surface of the talus and the dorsal surface of the calcaneus not only explains the complexity of the talocalcaneal articulations but also underscores the inconsistent references to these joints that can be found in the literature. In summary, there are only two “subtalar” joints (i.e., anterior talocalcaneonavicular joint and posterior subtalar joint), six facets on the surfaces of the calcaneus and talus, and three sets of apposing facets on these surfaces (i.e., anterior, middle, and posterior facets), with common anatomic variations in the number of these facets. Further, normally, there is no communication between these two subtalar joints but, as noted above, there may be communication between the posterior subtalar joint and ankle.
Epidemiology and Etiology
Tarsal coalitions are abnormal unions occurring between or among adjacent tarsal bones. The type of tissue at the site of union may be bone (synostosis), cartilage (synchondrosis), or fibrous tissue (syndesmosis). In one early publication, the incidence of tarsal coalition was reported to be less than 1%10, although it is believed that this number likely is an underestimation of the true prevalence as many people with tarsal coalitions are asymptomatic and may never seek medical attention or undergo imaging. Indeed, more recent studies have shown higher frequencies of tarsal coalition, with one investigation of 667 consecutive ankle MR imaging studies demonstrating an incidence of 11.5%.11 Historically, it has been reported that the most common types of osseous coalitions were calcaneonavicular coalitions (53%), followed in frequency by talocalcaneal coalitions (37%), without specification of which talocalcaneal facets were affected.12 The reported frequencies of tarsal coalitions may be most inaccurate for those coalitions that affect the talocalcaneal articulations, as these two joints, as well as their multiple facets, are more difficult to define on conventional radiographs when compared to the space between the calcaneus and navicular bone that is the site of fusion in cases of calcaneonavicular coalition. The application of CT scanning to the assessment of patients with suspected tarsal coalition has allowed for more accurate detection of talocalcaneal coalitions, including those that are occult on radiographic examination. Further, CT scanning (as well as MR imaging), when compared to conventional radiography, has provided a far more vivid display of the facets that comprise the talocalcaneal articulations and has allowed differentiation of the most common location of talocalcaneal coalition, the middle talocalcaneal facets (Figure 5), from less frequent sites of talocalcaneal coalition that include the posterior facets, anterior facets (Figure 6), and even extra-articular sites (Figure 7).13,14
Figure 5:
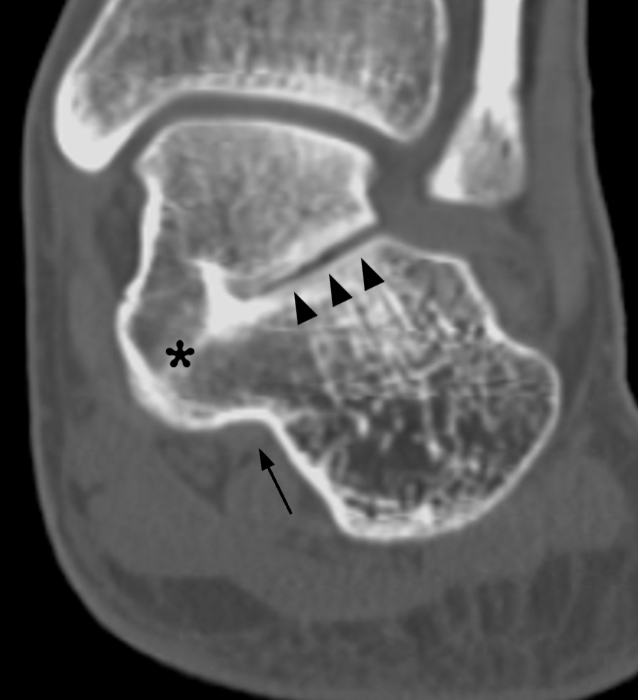
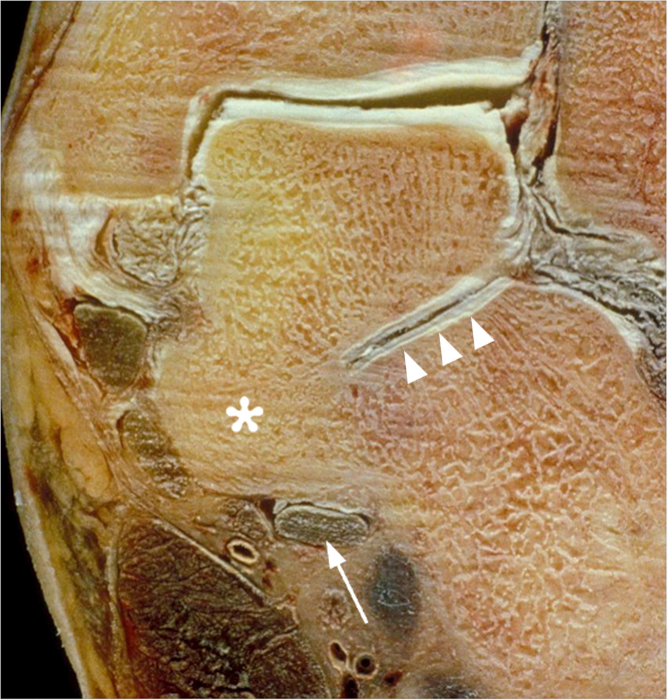
Radiologic-pathologic correlation using a CT image in a patient with an osseous talocalcaneal coalition of the middle facets (5A) and in a coronal section of a cadaveric specimen with an almost identical coalition (5B). The coronal CT image demonstrates an osseous coalition at the level of the middle talocalcaneal facets (5A, asterisk), which is also noted in a photograph of a coronal section of the cadaveric specimen (5B, asterisk). Note the medial downward angulation of the posterior subtalar joint (arrowheads), which typically has a more horizontal or slight medial upward orientation, as well as the proximity of the flexor hallucis longus tendon (arrows) to the coalition. Also note the ball-and-socket appearance of the ankle joint in the CT image in the patient.
Figure 6:
Coalition involving the anterior and middle talocalcaneal facets in a 60-year-old man with ankle pain. Sagittal T1-weighted image shows a middle facet talocalcaneal coalition medially (6A, asterisk) and an anterior facet talocalcaneal coalition slightly more laterally (6B, arrowheads). The coalitions are again seen on the axial T1-weighted image (6C). Coronal oblique proton density fat-suppressed images again show the anterior facet talocalcaneal coalition (6D) (arrowheads) and the middle facet talocalcaneal coalition (6E) (asterisk). Subchondral marrow edema corresponding to sites of osteochondral injury involve both the tibial plafond and the lateral talar dome (6E) (short arrows).
Figure 7:
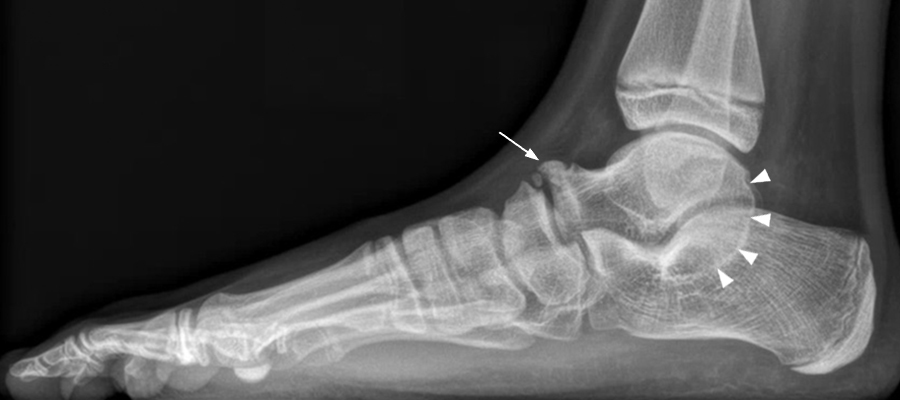
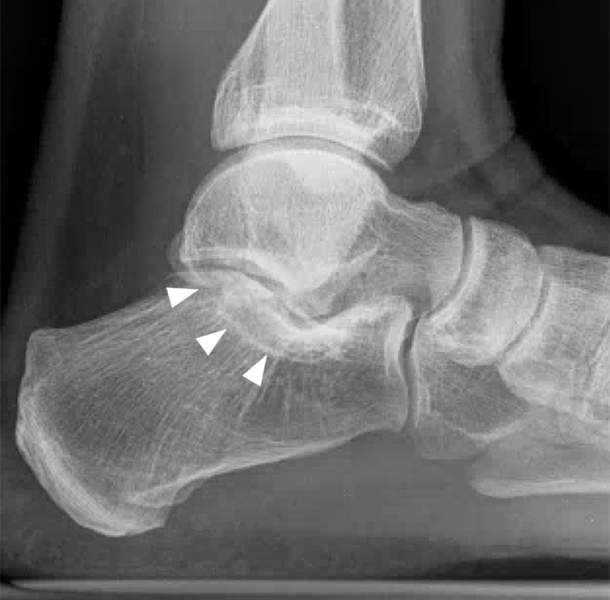
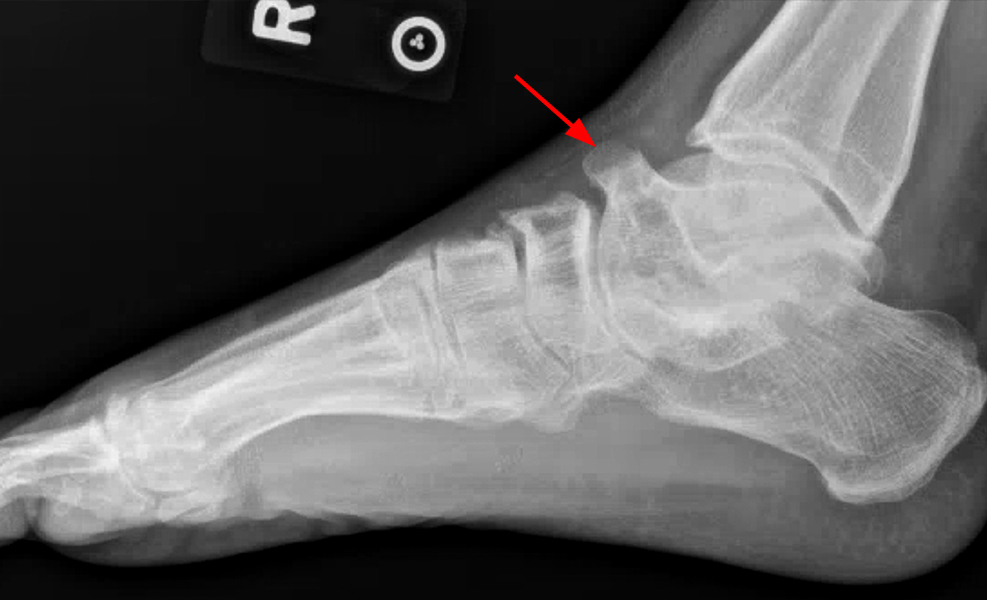
Extra-articular talocalcaneal coalition in a 27-year-old woman with a palpable right medial ankle mass after an injury to the ankle 1 year prior to presentation. Lateral radiograph (7A) suggests an extra-articular talocalcaneal coalition (arrow), which is subsequently confirmed on sagittal T1-weighted (T1) (7B), coronal T2 FS (7C), and coronal T1-weighted (7D) MR images (arrows). The coronal fat-suppressed T2-weighted MR image also demonstrates a ganglion cyst apparently arising from the fibrocartilaginous synchondrosis (arrowheads).
A male predominance has been reported for tarsal coalitions.13 There is no association between tarsal coalition and any particular racial background.15 Some anthropologic studies, however, have shown that the frequency of specific sites of coalition may differ among various populations. For example, calcaneonavicular coalitions are more common among populations of European ancestry, whereas naviculo-medial cuneiform coalitions are more common in people of South African descent.16 As many as 56% of persons with talocalcaneal coalitions have bilateral involvement.13,16,17,18
Autosomal dominant inheritance of tarsal coalitions was suggested by Wray and Herndon based on the finding that three successive generations in the same family all demonstrated calcaneonavicular coalitions19, and subsequently by Leonard, who found a high frequency of tarsal coalition (31%) of first-degree relatives of persons with tarsal coalition.11 In more recent literature, a mutation in the gene encoding fibroblast growth receptor 3 has been associated with tarsal coalitions.20
One proposed etiology for tarsal coalitions has been the incorporation of accessory ossicles of the foot; however, this mechanism fails to explain why coalitions have been found in developing fetuses. An alternative and widely accepted explanation is that tarsal coalitions result from the failure of mesenchymal tissue to undergo differentiation and segmentation during development.11
Clinical Findings/Presentation
Tarsal coalitions may present as vague generalized foot pain or, more focally, as pain in the region of the tarsal sinus. Pain may be aggravated with activity, particularly with attempted inversion. The onset of symptoms has classically been described to occur around the age of 12 – 16 years in cases of talocalcaneal coalition, later than in cases of calcaneonavicular coalitions, although as many as 26% of persons with tarsal coalition may remain asymptomatic.21 Persons of greater body weight also tend to present with clinical findings of talocalcaneal coalition at an earlier age, findings that include limited subtalar motion and pes planus.
As a result of the restriction of subtalar motion and rigid flat foot that accompany tarsal coalition, the peroneal muscles adapt to the long-term deformity by shortening, producing a condition that has been called “peroneal spastic flatfoot,”22 When a patient with a coalition attempts to invert the foot, the shortened peroneal muscles contract to protect the subtalar joint, resulting in the clinical finding of peroneal spasm.23 Although tarsal coalition may result in peroneal spastic flatfoot, not all cases of peroneal spastic flatfoot are associated with tarsal coalition. Specifically, peroneal muscle contraction has been described to also occur with other causes of subtalar irritation including inflammatory arthritis, osteomyelitis, accessory anterolateral talar facets, talar osteochondral injuries, trauma, and tumor.24 Interestingly, some of these conditions, including accessory anterolateral talar facet and talar osteochondral abnormalities, are themselves associated with tarsal coalition, as will be discussed in this article.
Imaging Findings
In the following section, information dealing only with talocalcaneal coalitions is emphasized, with limited attention to other sites of tarsal coalition.
Conventional Radiography
Conventional AP, lateral, and oblique radiographs are frequently interpreted as negative in the setting of a talocalcaneal coalition. It has been suggested that the axial (Harris) view may display the most common site of talocalcaneal coalition, the middle facets of the talus and calcaneus, revealing narrowing and irregularity of the interosseous space between these two facets or loss of the normal parallel position of the middle facets with respect to the posterior facets.22
In addition to direct visualization of the site of bone union, there are several secondary radiographic signs that suggest the presence of a talocalcaneal coalition, including: talar beaking, broadening of the lateral process of the talus, narrowing of the space between the posterior talocalcaneal facets, absence of the middle talocalcaneal facets, dysmorphic appearance of the sustentaculum tali, and the radiographic “C-sign” (Figure 8).25,26,27 Lateur et al. described the radiographic “C-sign” as a line formed by the medial outline of the talar dome and inferior outline of the sustentaculum tali, which these investigators found was present in 18 cases of coalitions involving either the middle or posterior talocalcaneal facets discovered on CT or MR imaging.27 In one study of 55 feet with talocalcaneal coalitions, 36 of which were histologically confirmed, the sensitivity and specificity of the “C-sign” were 49% and 91%, respectively.28 Subgroup analysis demonstrated that the “C-sign” was less sensitive when the coalition was small or the patient was skeletally immature. The combination of other radiographic signs may be more sensitive and specific. Retrospective review of radiographs of 37 feet, including 15 with talocalcaneal coalitions, demonstrated a sensitivity of 100% and specificity of 88% for the diagnosis of the coalition utilizing the combination of three radiographic signs: dysmorphic sustentaculum tali, non-visualization of the middle talocalcaneal facets, and shortening of the talar neck.29
Figure 8:
Secondary radiographic findings of talocalcaneal coalition. Weight-bearing lateral radiograph from a 13-year-old boy with ankle pain demonstrates pes planus with a “continuous C-sign” formed by the medial outline of the talar dome and the inferior outline of the sustentaculum tali (arrowheads) and a talar beak (arrow).
Abnormal union of the talus and calcaneus may also occur at a site that does not involve any of the talocalcaneal facets. These coalitions are termed extra-articular talocalcaneal coalitions. Extra-articular talocalcaneal coalitions may occur anterolaterally or posteromedially, and the latter may or may not be associated with an os sustentaculum. The anterolateral extra-articular talocalcaneal coalition occurs anterior to the posterior talocalcaneal articulation and lateral to the anterior talocalcaneonavicular joint at the lateral margin of the tarsal sinus.30 The posteromedial extra-articular talocalcaneal coalition occurs between the posterior talocalcaneal facets and the middle talocalcaneal facets, typically involving the posterior margin of the sustentaculum tali and the medial tubercle of the posterior process of the talus.31,32 Coalitions at this location may occur either without or with an os sustentaculum, a small accessory bone between the sustentaculum tali and the medial talar process (Figure 9).33,34
Figure 9:
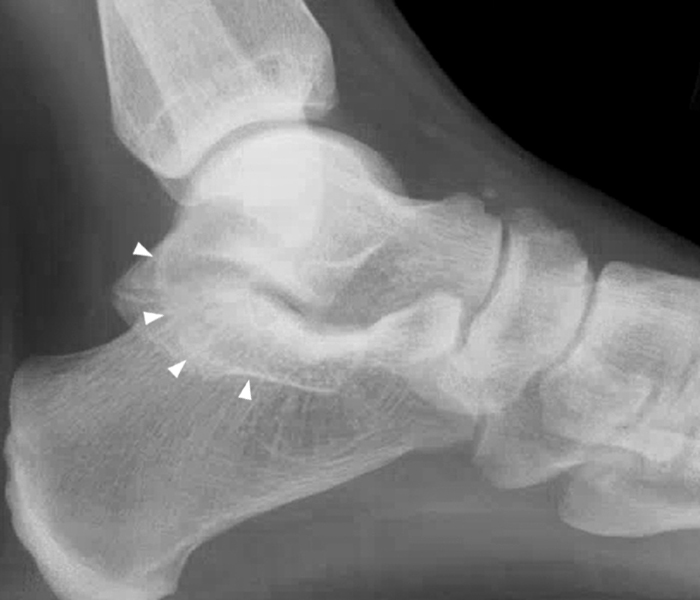
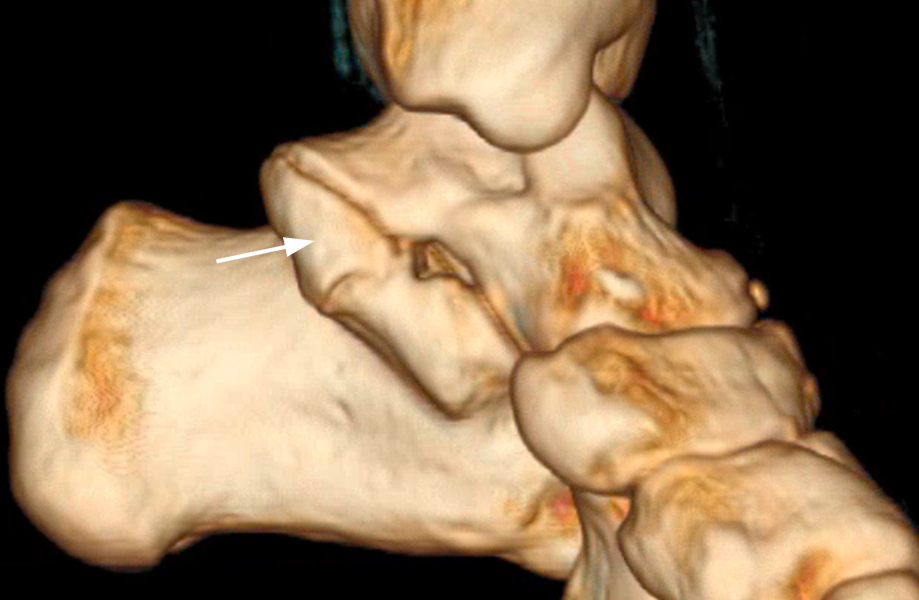
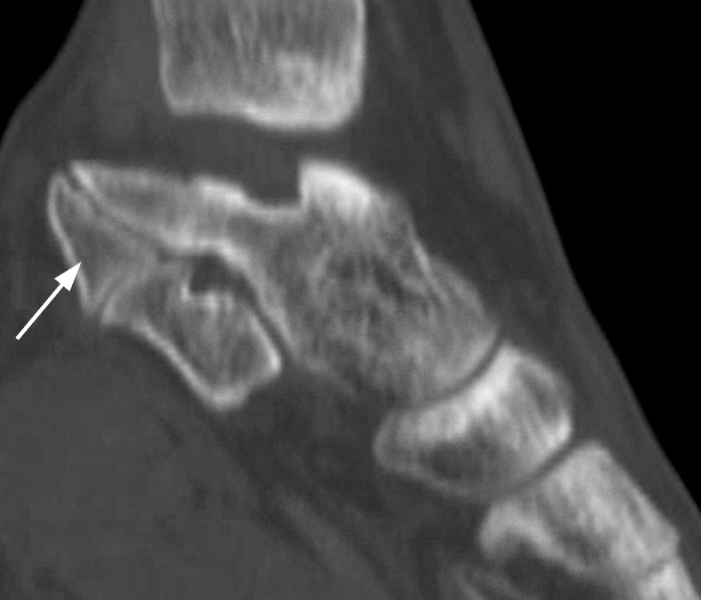
Posteromedial extra-articular talocalcaneal coalition with an os sustentaculum. This 29-year-old woman had left ankle pain after a twisting injury. Lateral radiograph (9A) shows a continuous C-sign (arrowheads) suspicious for a talocalcaneal coalition. On the subsequently obtained CT, a 3D reconstruction image (9B), and sagittal (9C), coronal (9D), and axial (9E) images demonstrate the posteromedial extra-articular talocalcaneal coalition with an os sustentaculum (arrows).
As noted in the discussion of the clinical presentation of talocalcaneal coalition, normal subtalar motion is restricted in the presence of a talocalcaneal coalition, and the normal forward gliding motion of the calcaneus under the talus becomes a hinge-like motion with the navicular dorsiflexing on the talus. This results in chronic repetitive periosteal stripping at the dorsal aspect of the talus at the talonavicular joint, which produces the talar beak.18
CT and MR Imaging
CT may allow for the detection of coalitions that are not evident on radiographs, as reported in one study in which CT demonstrated talocalcaneal coalitions in 5 persons, 4 of whom had radiographs that were interpreted as being normal.35 For talocalcaneal coalitions involving the middle facets, CT images in the coronal plane demonstrate bridging across the middle facets.36 When the coalition is osseous, the CT images show a bony bar bridging the facets. When the coalition is non-osseous, the interosseous space between the middle facets of the talus and calcaneus may be narrowed with accompanying bone irregularity, proliferation, and cystic changes in one or both middle facets. Additionally, the sustentaculum tali may have a different configuration, sloping medially and downward instead of upward.37
MR imaging, when compared to CT, has been shown to be equally sensitive for the detection of tarsal coalition.37 As with CT, talocalcaneal coalitions are frequently better seen in the MR images in the coronal plane. With bony coalitions, the MR images demonstrate marrow continuity at the location of the coalition. When the coalition is cartilaginous, the MR images demonstrate signal intensity similar to that of fluid or cartilage in the region of the abnormality. Fibrous coalitions are seen as bridging tissue of low signal intensity on all sequences. MR imaging also demonstrates associated periarticular bone changes, including the presence and extent of marrow edema. The periarticular marrow edema may be an important feature that allows for the identification of subtle unsuspected coalitions.37
Comparison of MR imaging and CT in patients with talocalcaneal coalition has demonstrated the superiority of MR imaging in the detection of incomplete osseous coalitions and non-osseous coalitions.38,39 MR imaging may also better depict additional conditions that are associated or coexist with talocalcaneal coalitions.
Disease Associations
Medial plantar neuropathy and tendon entrapment
Tendons or nerves that pass near the site of a talocalcaneal coalition may be entrapped or irritated by it. In one study of 67 ankle MR imaging studies with talocalcaneal coalitions, there was associated attenuation of or tenosynovitis about the flexor hallucis longus tendon in 39%, of the flexor digitorum longus tendon in 39%, and of the posterior tibialis tendon in 13%. In 6 ankles (9%), there were increased caliber and signal of the medial plantar nerve, as in our case, indicative of neuritis due to chronic friction applied to the nerve.
Accessory anterolateral talar facet (AALTF)
Tarsal coalitions have also been associated with another type of variant anatomy that can be accompanied by foot pain, the AALTF. In a retrospective review of 187 patients with either an AALTF, any tarsal coalition, or sinus tarsi syndrome, or any combination of these findings, with an AALTF defined as a facet with a length greater than 3 mm in the sagittal plane, Alqahtani et al. reported a frequency of an AALTF of 31.55% and a frequency of any tarsal coalition of 37.43%.40 Additionally, in this review, among patients with a tarsal coalition, the most common type of coalition was a calcaneonavicular coalition, followed by an extra-articular talocalcaneal coalition. The authors found a significant association between an AALTF and the presence of either an extra-articular talocalcaneal coalition or a talocalcaneal coalition involving the middle facets (Figure 10). Additionally, the length of the AALTF was greater in patients with an extra-articular talocalcaneal coalition compared to those without an extra-articular talocalcaneal coalition. Similarly, patients with a middle facet talocalcaneal coalition had a greater AALTF length compared to those without a middle facet talocalcaneal coalition.
Figure 10:
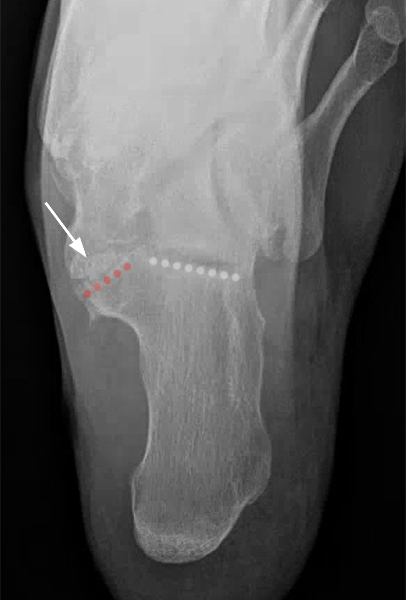
Middle facet talocalcaneal coalition and AALTF. 50-year-old woman with a history of numerous ankle sprains who now has persistent lateral ankle pain and instability. Lateral radiograph (10A) shows a “continuous C-sign” (arrowheads). The axial view (10B) demonstrates a non-osseous middle-facet talocalcaneal coalition (arrow) with loss of the normal parallelism between the middle facet (red dotted line) and the posterior facet (white dotted line) of the calcaneus. The coalition is confirmed on the coronal T2-weighted fat-suppressed (10C) and T1-weighted (10D) MR images, which also demonstrate associated reactive marrow and cystic changes, best visualized on the coronal T2-weighted fat-suppressed image (10C). An accessory anterolateral talar facet (AALTF) is seen on the sagittal T1 MR image (10E) (short arrow). Images courtesy of Brady K. Huang, M.D.
Osteochondral Injury
Patients with tarsal coalitions may also have an increased frequency of osteochondral injury of the talar dome. In a retrospective case series of 57 ankles in 57 patients with tarsal coalition, 50.9% of the patients had a concomitant osteochondral injury of the talar dome, much higher than the prevalence of talar osteochondral injury reported in the literature (Figures 11 and 12).41 The occurrence of an osteochondral injury of the talar dome in cases of coalition is thought to be the result of altered biomechanics at the level of the ankle involving the talar articular surface that are related to limited subtalar motion caused by the talocalcaneal fusion.
Figure 11:
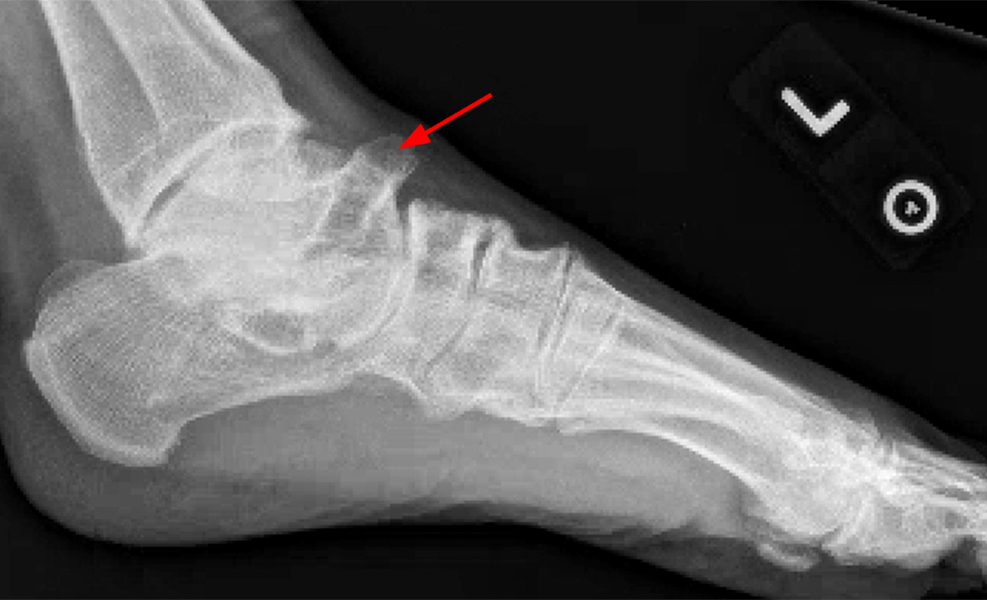
Talocalcaneal coalition and osteochondral injury. 47-year-old man with atraumatic right ankle pain and swelling for 5 years. Lateral radiograph shows an extra-articular talocalcaneal coalition (11A, arrow), which is confirmed on the sagittal fat-suppressed T2-weighted MR image (11B, arrow). The coronal T1-weighted MR image (11C) also demonstrates the non-osseous coalition (arrow), as well as osteochondral injury of the medial talar dome (arrowhead).
Figure 12:
Talocalcaneal coalition and osteochondral injury. 20-year-old woman with right ankle pain. Lateral radiograph (12A) demonstrates continuous C-sign (arrowheads), with a bony coalition involving the middle talocalcaneal facets on the sagittal T1 MR image (12B, asterisk). The coronal PD FS (12C) and axial T1 MR images (12D) also demonstrate the coalition (asterisk) with subchondral edema and irregularity of the subchondral bone plate at the lateral talar dome compatible with osteochondral injury (arrows).
Multiple coalitions and ball and socket ankle joint
Multiple tarsal coalitions may occur in the same foot, both in persons with a variety of congenital syndromes, as well as in persons without such syndromes (Figure 13). One retrospective study reported that in persons with tarsal coalition, as many as 20% had more than one site of abnormal tarsal union.42 In the setting of restricted subtalar motion due to either one or multiple tarsal coalitions, the development of a ball-and-socket tibiotalar joint, which allows inversion/eversion motion at the level of the ankle that normally occurs at the level of the subtalar joints, would appear to be an adaptive developmental change (Figure 14).43,44,45
Figure 13:
Talocalcaneal and calcaneonavicular coalitions occurring in the same foot. 17-year-old man with decreased range of motion in the right ankle. Sagittal (13A), axial (13B) and coronal (13C) CT images demonstrate the presence of both a non-osseous calcaneonavicular coalition (arrowheads) and an osseous talocalcaneal coalition involving the middle facets (asterisks).
Figure 14:
Ball-and-socket tibiotalar joint. Radiographs from an 8-year-old girl with ankle pain. The mortise view (14A) demonstrates a ball-and-socket configuration of the tibiotalar joint (asterisk) and a talocalcaneal coalition involving the middle facets (arrow). On the lateral view (14B), the middle facet and posterior subtalar joint are not well seen (arrowheads), related to the presence of a talocalcaneal coalition.
Bipartite medial cuneiform
Similar to the theorized pathogenesis of tarsal coalition, the cause of a bipartite medial cuneiform appears to be an abnormality of mesenchymal differentiation. In the case of bipartite medial cuneiform, a malsegmentation defect results in two ossification centers which form separate dorsal and plantar segments, the latter of which is usually larger.46 It is a rare variant, with reported frequencies ranging from 0.1 to 2.4%.47 At least one case of both a tarsal coalition and a bipartite medial cuneiform has been reported in the literature, and we have encountered two cases of talocalcaneal coalition with an associated bipartite medial cuneiform, one of which is included here (Figure 15).48
Figure 15:
Talocalcaneal coalition and bipartite medial cuneiform. 27-year-old man with left ankle pain. Sagittal proton density fat-suppressed (15A) and sagittal T1-weighted (15B) MR images demonstrate a bipartite medial cuneiform (arrow) and a coalition of the middle talocalcaneal facets (arrowheads). Coronal fat-suppressed T2-weighted image also shows the bipartite medial cuneiform (15C, arrow). Coronal fat-suppressed T2-weighted image more proximally (15D) shows the talocalcaneal coalition (arrowheads) with accompanying reactive marrow edema. Images courtesy of Emily Lee, M.D.
Other associations
Tarsal coalitions have also classically been described in association with other conditions and syndromes, including multiple synostoses, hereditary symphalangism, fibular hemimelia, phocomelia, Apert syndrome, and Nievergelt-Pearlman syndrome.43,49,50
Differential Diagnosis
Talar beak
The talar beak, as previously discussed, has been described as a secondary radiographic finding in cases of tarsal coalition. Of note, however, there are several bony prominences that may occur along the dorsal surface of the talar head and neck that may easily be misinterpreted as a talar beak, leading to a misdiagnosis of a talocalcaneal coalition.51 The talar ridge is a normal bony prominence at the site of attachment of the talonavicular ligament and tibiotalar joint capsule. The normal talar ridge may hypertrophy because of abnormal traction or generalized enthesopathy (Figure 16). More proximally, at the margin of the trochlear surface, talar osteophytes may develop as a response to osteoarthrosis of the tibiotalar joint. The true talar beak arises from the dorsal surface of the talus, in the region of the talar ridge, as a large and triangular bony excrescence that slopes distally and ends near the articular margin of the talonavicular space.
Figure 16:
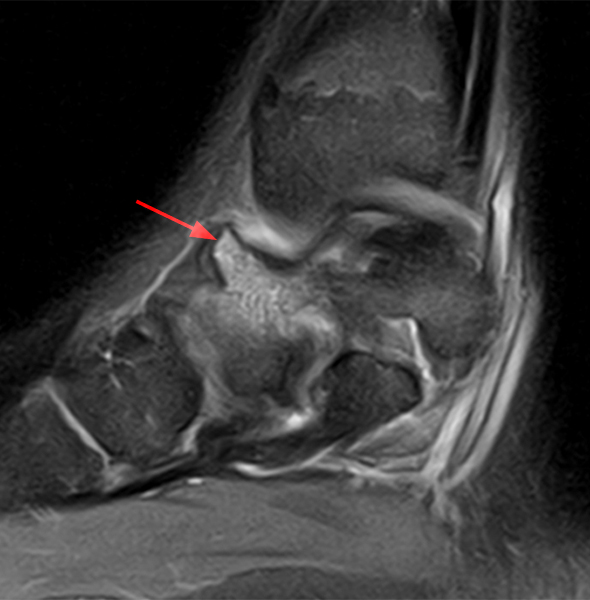
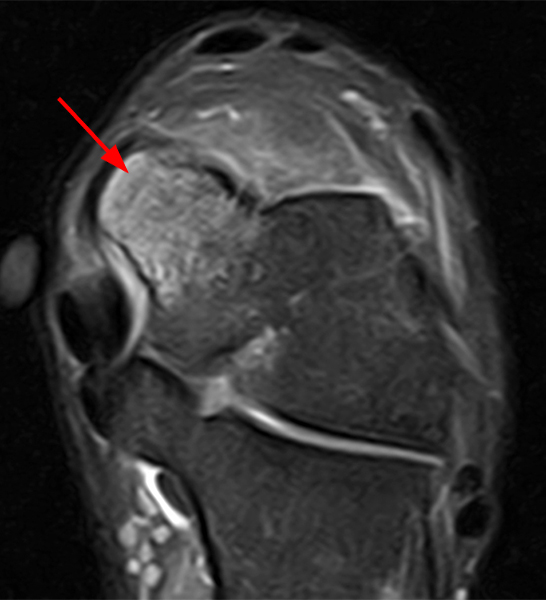
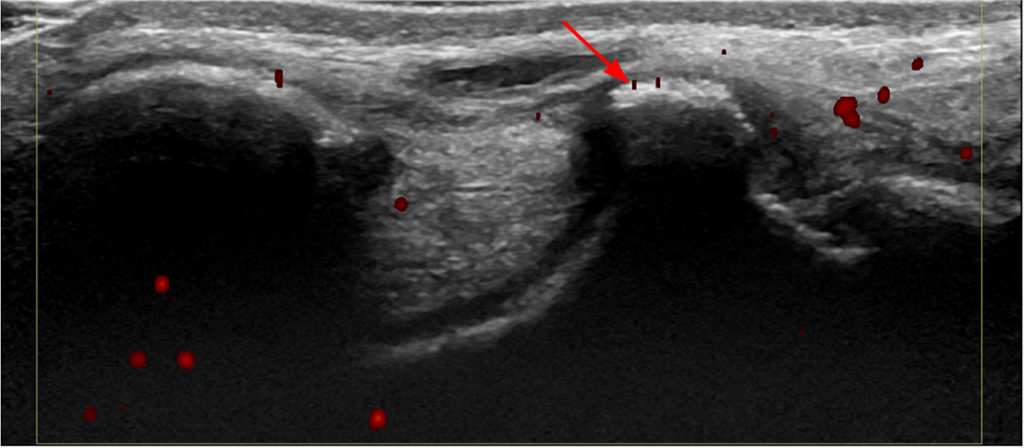
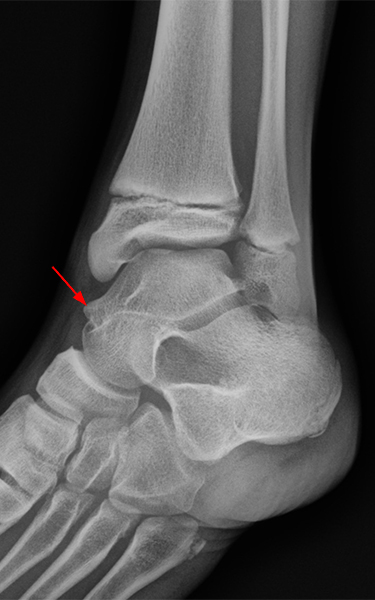
Hypertrophied talar ridge causing anteromedial ankle impingement. A 16-year-old boy presented with medial ankle pain. Sagittal T1-weighted (16A) and fat-suppressed T2-weighted (16B) images, as well as a coronal fat-suppressed T2-weighted (16C) image, demonstrate an edematous hypertrophied talar ridge (arrow) which mimics a talar beak. The same talar bone outgrowth was also seen on ultrasonography (16D, arrow). Review of the patient’s radiographs obtained four years previously showed a less conspicuous talar ridge (arrow) on the mortise view (16E). Images courtesy of Cláudia Borges Fontan Câmara, M.D.
Acquired Coalition
In addition to congenital coalition, abnormal ankylosis between or among tarsal bones may occur in cases of infection or inflammation, leading to obliteration of the normal joint space. Septic arthritis, juvenile idiopathic arthritis, adult-onset rheumatoid arthritis, and spondyloarthropathies are among the conditions that can lead to bone ankyloses in one or more of the intertarsal joints (Figure 17). In such cases, it may be difficult to distinguish an acquired coalition from a congenital coalition. One diagnostic clue, however, is the presence of a developmental ball and socket ankle joint, which generally indicates that whatever the process that led to talocalcaneal coalition, it occurred at a very young age.
Figure 17:
Prominent talar beaks related to rigid motion in a 35-year-old man with rheumatoid arthritis. Lateral views of the right (17A) and left (17B) foot demonstrate prominent bilateral talar beaks (arrows) due to severe joint space loss in the posterior subtalar joint related to rheumatoid arthritis with resultant acquired talocalcaneal coalition and loss of subtalar motion. Images courtesy of Tudor H. Hughes, M.B.B.S, M.D., F.R.C.R.
Treatment and Prognosis
Treatment of talocalcaneal coalitions typically begins with conservative measures, including the application of hard-soled shoes, foot or ankle-stabilizing orthoses, arch inserts, and short leg walking casts, as well as the use of non-steroidal anti-inflammatory medications or corticosteroid injection for pain relief. Non-operative treatment has been reported to improve symptoms in 22-46% of patients.52 When the patient does not respond to conservative management, which is more common with talocalcaneal coalitions than with calcaneonavicular and talonavicular coalitions, resection of the coalition with fat graft interposition may be performed. When degenerative changes are already present, arthrodesis is typically performed. One study of 14 feet in 12 patients who underwent resection of a talocalcaneal coalition and placement of a bioresorbable implant showed excellent or good results in 78.5% of patients, with 92.8% of patients showing an improvement in subtalar range of motion.53 More recently, of 93 patients with talocalcaneal coalitions treated with excision and fat graft interposition, 84% showed excellent or good outcomes.54 Better outcomes following resection are reported when the initial coalition involved less than or equal to 50% of the area of the posterior talocalcaneal facets.55
Conclusion/Summary
Talocalcaneal coalitions are common causes of rigid flatfoot and foot pain. The most frequent site of involvement is the middle facets of the talocalcaneonavicular articulation. Diagnosis based on conventional radiography alone may be difficult, demonstrating only secondary findings but failing to display the coalition itself. CT and MR imaging can better demonstrate the location and extent of abnormal union, with the latter method providing additional information, including the presence of marrow edema which may be a clue to the diagnosis of a coalition. Additionally, CT and MR imaging also allow for more rapid detection of associated abnormalities, including medial plantar neuropathy or tendon entrapment, an AALTF, and osteochondral injury. Treatment of tarsal coalition typically begins with conservative measures, with surgical resection or arthrodesis reserved for those patients who fail to exhibit improvement with conservative management.
References
- Anjaneyulu, K., Philips, C., Tamang, B.K., and Kumar, A. (2014). Patterns of talar articulating facets in adult human calcanei from North-East India and their clinical correlation. Asian Journal of Medical Sciences 5, 89–93. https://doi.org/10.3126/ajms.v5i4.9486. ↩
- Ayoob, A., Maeseneer, M.D., Shahabpour, M., Roy, P.V., Barbaix, E., and QIng, S. (2010). The talocalcaneal unit: pictorial review of anatomy and pathologic conditions on multi detector ct. Journal of the Belgian Society of Radiology 93, 20–27. https://doi.org/10.5334/jbr-btr.34. ↩
- Drayer-Verhagen, F. (1993). Arthritis of the subtalar joint associated with sustentaculum tali facet configuration. J Anat 183, 631–634. ↩
- Hyer, C.F., Lee, T., Block, A.J., and VanCourt, R. (2002). Evaluation of the anterior and middle talocalcaneal articular facets and the evans osteotomy. The Journal of Foot and Ankle Surgery 41, 389–393. https://doi.org/10.1016/S1067-2516(02)80085-0. ↩
- Jung, M.-H., Choi, B.Y., Lee, J.Y., Han, C.S., Lee, J.S., Yang, Y.C., and Cho, B.P. (2015). Types of subtalar joint facets. Surg Radiol Anat 37, 629–638. https://doi.org/10.1007/s00276-015-1472-1. ↩
- Rühli, F. j., Solomon, L. b., and Henneberg, M. (2003). High prevalence of tarsal coalitions and tarsal joint variants in a recent cadaver sample and its possible significance. Clinical Anatomy 16, 411–415. https://doi.org/10.1002/ca.10146. ↩
- Scranton, P.E., and McDermott, J.E. (1997). Pathologic Anatomic Variations in Subtalar Anatomy. Foot Ankle Int. 18, 471–476. https://doi.org/10.1177/107110079701800803. ↩
- Shahabpour, M., Devillé, A., Van Roy, P., Vaes, P., De Mey, J., and De Maeseneer, M. (2011). Magnetic Resonance Imaging of anatomical variants of the subtalar joint. Surg Radiol Anat 33, 623–630. https://doi.org/10.1007/s00276-011-0788-8. ↩
- Resnick, D. (1974). Radiology of the Talocalcaneal Articulations. Radiology 111, 581–586. https://doi.org/10.1148/111.3.581. ↩
- Leonard, M.A. (1974). The inheritance of tarsal coalition and its relationship to spastic flat foot. The Journal of Bone and Joint Surgery. British Volume 56-B, 520–526. https://doi.org/10.1302/0301-620X.56B3.520. ↩
- Nalaboff, K.M., and Schweitzer, M.E. (2008). MRI of tarsal coalition: frequency, distribution, and innovative signs. Bull NYU Hosp Jt Dis 66, 14–21. ↩
- Stormont, D.M., and Peterson, H.A. (1983). The Relative Incidence of Tarsal Coalition. Clinical Orthopaedics and Related Research (1976-2007) 181, 28. ↩
- Herzenberg, J.E., Goldner, J.L., Martinez, S., and Silverman, P.M. (1986). Computerized Tomography of Talocalcaneal Tarsal Coalition: A Clinical and Anatomic Study. Foot & Ankle 6, 273–288. https://doi.org/10.1177/107110078600600601. ↩
- Pineda, C., Resnick, D., and Greenway, G. (1986). Diagnosis of Tarsal Coalition with Computed Tomography. Clinical Orthopaedics and Related Research (1976-2007) 208, 282. ↩
- Rankin, E.A., and Baker, G.I. (1974). Rigid Flatfoot in the Young Adult. Clinical Orthopaedics and Related Research® 104, 244–248. ↩
- Case, D.T., and Burnett, S.E. (2012). Identification of tarsal coalition and frequency estimates from skeletal samples. International Journal of Osteoarchaeology 22, 667–684. https://doi.org/10.1002/oa.1228. ↩
- Conway, J.J., and Cowell, H.R. (1969). Tarsal Coalition: Clinical Significance and Roentgenographic Demonstration. Radiology 92, 799–811. https://doi.org/10.1148/92.4.799. ↩
- Jack, E.A. (1954). Bone anomalies of the tarsus in relation to “peroneal spastic flat foot.” The Journal of Bone and Joint Surgery. British Volume 36-B, 530–542. https://doi.org/10.1302/0301-620X.36B4.530. ↩
- Wray, J.B., and Herndon, C.N. (1963). Hereditary Transmission of Congenital Coalition of the Calcaneus to the Navicular. JBJS 45, 365–372. ↩
- Graham Jr., J.M., Braddock, S.R., Mortier, G.R., Lachman, R., Van Dop, C., and Jabs, E.W. (1998). Syndrome of coronal craniosynostosis with brachydactyly and carpal/tarsal coalition due to Pro250Arg mutation in FGFR3 gene. American Journal of Medical Genetics 77, 322–329. https://doi.org/10.1002/(SICI)1096-8628(19980526)77:4<322::AID-AJMG14>3.0.CO;2-K. ↩
- Cowell, H.R. (1972). Talocalcaneal Coalition and New Causes of Peroneal Spastic Flatfoot. Clinical Orthopaedics and Related Research® 85, 16. ↩
- Harris, R., and Beath, T. (1948). Etiology of peroneal spastic flat foo. JBJS 30. ↩
- Cowell, H.R., and Elener, V. (1983). Rigid Painful Flatfoot Secondary to Tarsal Coalition. Clinical Orthopaedics and Related Research® 177, 54. ↩
- Berkeley, R., Tennant, S., and Saifuddin, A. (2021). Multimodality imaging of the paediatric flatfoot. Skeletal Radiol 50, 2133–2149. https://doi.org/10.1007/s00256-021-03806-8. ↩
- Crim, J. (2008). Imaging of Tarsal Coalition. Radiologic Clinics of North America 46, 1017–1026. https://doi.org/10.1016/j.rcl.2008.09.005. ↩
- Lateur, L.M., Van Hoe, L.R., Van Ghillewe, K.V., Gryspeerdt, S.S., Baert, A.L., and Dereymaeker, G.E. (1994). Subtalar coalition: diagnosis with the C sign on lateral radiographs of the ankle. Radiology 193, 847–851. https://doi.org/10.1148/radiology.193.3.7972836. ↩
- Rozansky, A., Varley, E., Moor, M., Wenger, D.R., and Mubarak, S.J. (2010). A radiologic classification of talocalcaneal coalitions based on 3D reconstruction. J Child Orthop 4, 129–135. https://doi.org/10.1007/s11832-009-0224-3. ↩
- Taniguchi, A., Tanaka, Y., Kadono, K., Takakura, Y., and Kurumatani, N. (2003). C Sign for Diagnosis of Talocalcaneal Coalition. Radiology 228, 501–505. https://doi.org/10.1148/radiol.2282020445. ↩
- Crim, J.R., and Kjeldsberg, K.M. (2004). Radiographic Diagnosis of Tarsal Coalition. American Journal of Roentgenology 182, 323–328. https://doi.org/10.2214/ajr.182.2.1820323. ↩
- Solomon, L., Ruhli, F., Ferris, L., Taylor, J., and Henneberg, M. (2007). Non-Osseous Extra-Articular Anterolateral Talocalcaneal Coalition: A Case Report. J Orthop Surg (Hong Kong) 15, 91–93. https://doi.org/10.1177/230949900701500121. ↩
- McNally, E.G. (1999). Posteromedial subtalar coalition: imaging appearances in three cases. Skeletal Radiol 28, 691–695. https://doi.org/10.1007/s002560050575. ↩
- Phyo, N., Pressney, I., Khoo, M., Welck, M., and Saifuddin, A. (2020). The radiological diagnosis of extra-articular posteromedial talocalcaneal coalition. Skeletal Radiol 49, 1413–1422. https://doi.org/10.1007/s00256-020-03440-w. ↩
- Bloom, R.A., Libson, E., Lax, E., and Pogrund, H. (1986). The assimilated os sustentaculi. Skeletal Radiol 15, 455–457. https://doi.org/10.1007/BF00355105. ↩
- Yun, S.J., Jin, W., Kim, G.Y., Lee, J.H., Ryu, K.N., Park, J.S., and Park, S.Y. (2015). A Different Type of Talocalcaneal Coalition With Os Sustentaculum: The Continued Necessity of Revision of Classification. American Journal of Roentgenology 205, W612–W618. https://doi.org/10.2214/AJR.14.14082. ↩
- Stoskopf, C.A., Hernandez, R.J., Kelikian, A., Tachdjian, M.O., and Dias, L.S. (1984). Evaluation of Tarsal Coalition by Computed Tomography. Journal of Pediatric Orthopaedics 4, 365–369. ↩
- Newman, J.S., and Newberg, A.H. (2000). Congenital Tarsal Coalition: Multimodality Evaluation with Emphasis on CT and MR Imaging. RadioGraphics 20, 321–332. https://doi.org/10.1148/radiographics.20.2.g00mc03321. ↩
- Emery, K.H., Bisset III., G.S., Johnson, N.D., and Nunan, P.J. (1998). Tarsal coalition: a blinded comparison of MRI and CT. Pediatric Radiology 28, 612–616. https://doi.org/10.1007/s002470050430. ↩
- Masciocchi, C., D’Archivio, C., Barile, A., Fascetti, E., Zobel, B.B., Gallucci, M., and Passariello, R. (1992). Talocalcaneal coalition: computed tomography and magnetic resonance imaging diagnosis. European Journal of Radiology 15, 22–25. https://doi.org/10.1016/0720-048X(92)90197-H. ↩
- Wechsler, R.J., Schweitzer, M.E., Deely, D.M., Horn, B.D., and Pizzutillo, P.D. (1994). Tarsal coalition: depiction and characterization with CT and MR imaging. Radiology 193, 447–452. https://doi.org/10.1148/radiology.193.2.7972761. ↩
- Alqahtani, E., Fliszar, E., Resnick, D.L., and Huang, B.K. (2020). Accessory anterolateral talar facet associated with tarsal coalition: prevalence and cross-sectional characterization. Skeletal Radiol 49, 417–424. https://doi.org/10.1007/s00256-019-03293-y. ↩
- Cheng, K.Y., Fuangfa, P., Shirazian, H., Resnick, D., and Smitaman, E. (2022). Osteochondritis dissecans of the talar dome in patients with tarsal coalition. Skeletal Radiol 51, 191–200. https://doi.org/10.1007/s00256-021-03800-0. ↩
- Clarke, D.M. (1997). Multiple Tarsal Coalitions in the Same Foot. Journal of Pediatric Orthopaedics 17, 777–780. ↩
- Bohne, W.H.O. (2001). Tarsal coalition. Current Opinion in Pediatrics 13, 29–35. ↩
- Brahme, F. (1961). Upper Talar Enarthrosis. Acta Radiologica os-55, 221–224. https://doi.org/10.1177/028418516105500307. ↩
- Channon, G., and Brotherton, B. (1979). The ball and socket ankle joint. The Journal of Bone and Joint Surgery. British Volume 61-B, 85–89. https://doi.org/10.1302/0301-620X.61B1.422641. ↩
- Chang, G.H., Chang, E.Y., Chung, C.B., and Resnick, D.L. (2014). Bipartite Medial Cuneiform: Case Report and Retrospective Review of 1000 Magnetic Resonance (MR) Imaging Studies. Case Reports in Medicine 2014, e130979. https://doi.org/10.1155/2014/130979. ↩
- Elias, I., Dheer, S., Zoga, A.C., Raikin, S.M., and Morrison, W.B. (2008). Magnetic resonance imaging findings in bipartite medial cuneiform – a potential pitfall in diagnosis of midfoot injuries: a case series. J Med Case Reports 2, 272. https://doi.org/10.1186/1752-1947-2-272. ↩
- Watts, A., Duncan, N., and Davies, M. (2017). Bipartite Medial Cuneiform and Calcaneonavicular Coalition in a Single Individual. International Journal of Anatomy and Research 5, 3634–3637. ↩
- Sartoris, D.J., and Resnick, D.L. (1985). Tarsal Coalition. Arthritis & Rheumatism 28, 331–338. https://doi.org/10.1002/art.1780280314. ↩
- Vincent, K.A. (1998). Tarsal Coalition and Painful Flatfoot. JAAOS – Journal of the American Academy of Orthopaedic Surgeons 6, 274–281. ↩
- Resnick, D. (1984). Talar ridges, osteophytes, and beaks: a radiologic commentary. Radiology 151, 329–332. https://doi.org/10.1148/radiology.151.2.6709899. ↩
- Kulik, S.A., and Clanton, T.O. (1996). Tarsal Coalition. Foot Ankle Int. 17, 286–296. https://doi.org/10.1177/107110079601700509. ↩
- Giannini S, Ceccarelli F, Vannini F, Baldi E. Operative Treatment of Flatfoot With Talocalcaneal Coalition. Clin Orthop Relat Res. 2003;411:178–87. ↩
- Gantsoudes, G.D., Roocroft, J.H., and Mubarak, S.J. (2012). Treatment of Talocalcaneal Coalitions. Journal of Pediatric Orthopaedics 32, 301–307. https://doi.org/10.1097/BPO.0b013e318247c76e. ↩
- Wilde, P., Torode, I., Dickens, D., and Cole, W. (1994). Resection for symptomatic talocalcaneal coalition. The Journal of Bone and Joint Surgery. British Volume 76-B, 797–801. https://doi.org/10.1302/0301-620X.76B5.8083272. ↩