Clinical history:
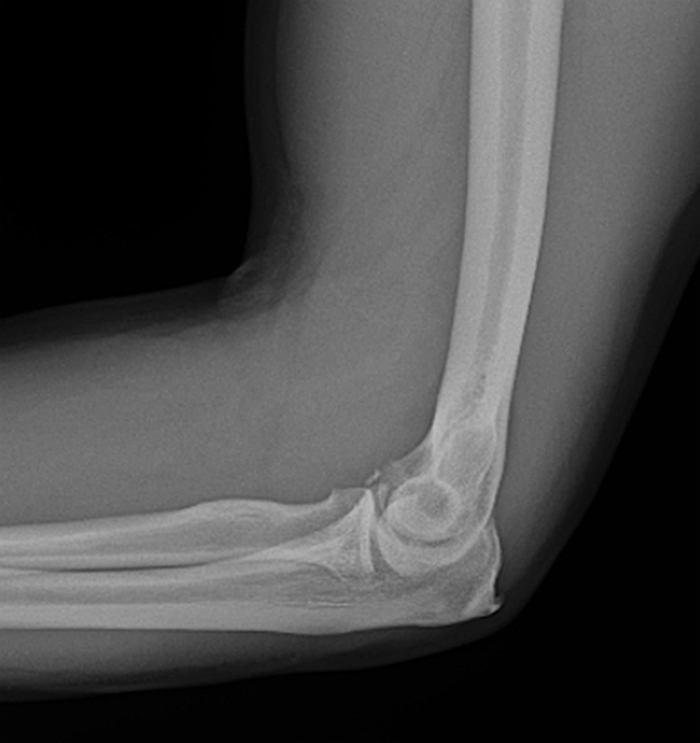
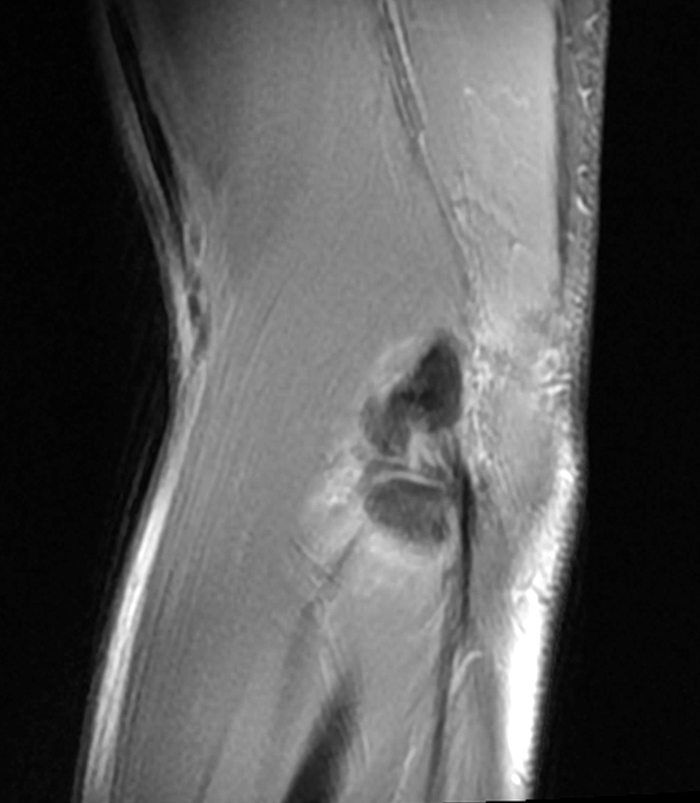
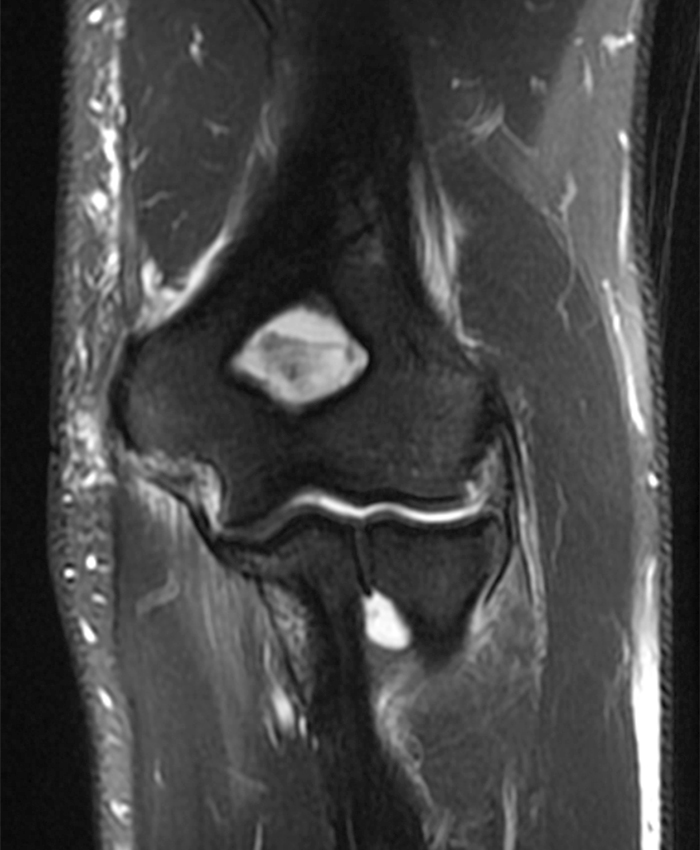
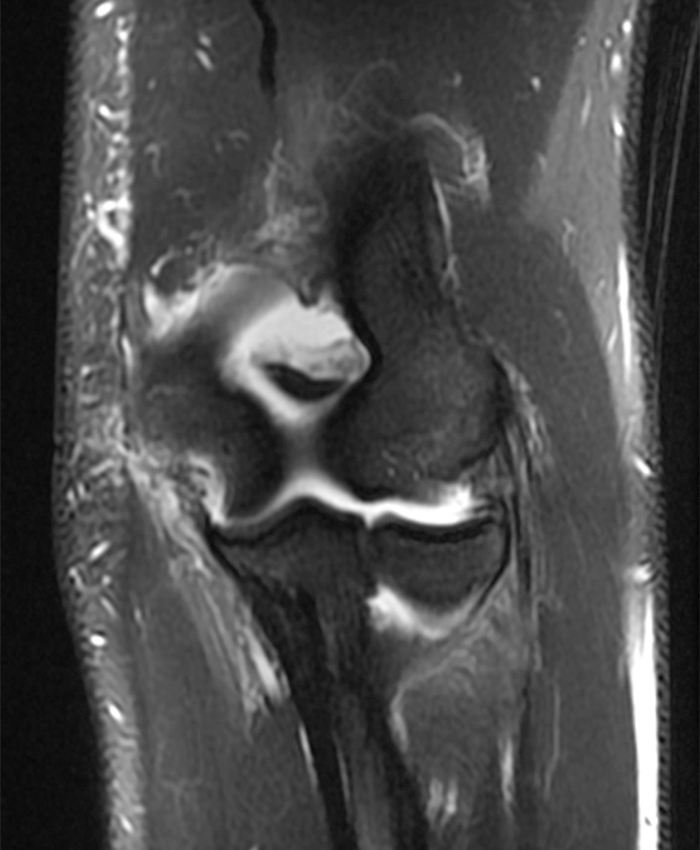
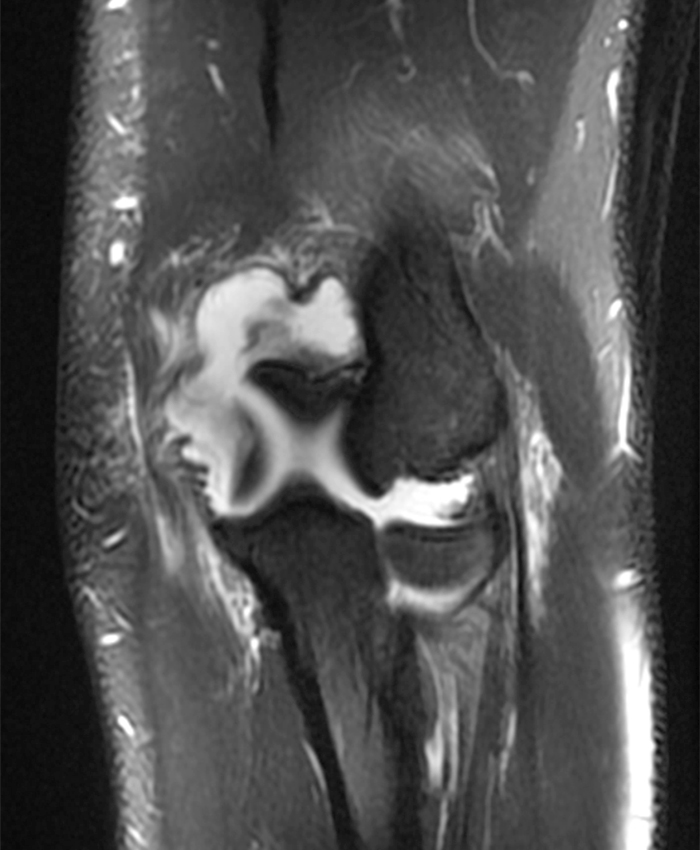
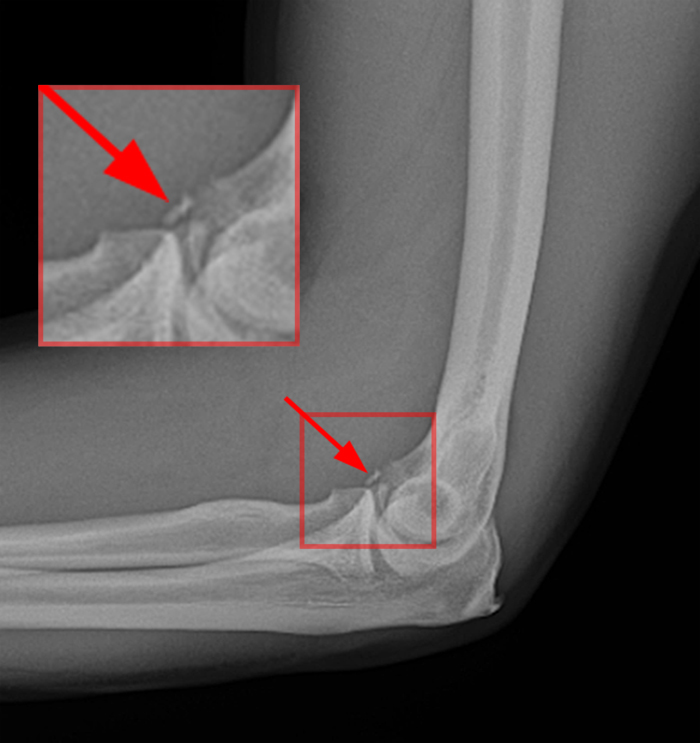
A 41-year-old man presented with left elbow pain after slipping on a wet floor and falling onto the left arm 1 week prior. Pain involved both the anterior and posterior aspects of the elbow, influenced by how the arm was moved from one position to another. An initial lateral radiograph (1a) and fat-suppressed proton density-weighted sagittal (2a-d) and T2-weighted coronal MRI (3a-c) images are made available for review. What are the findings? What is your diagnosis?
Findings:
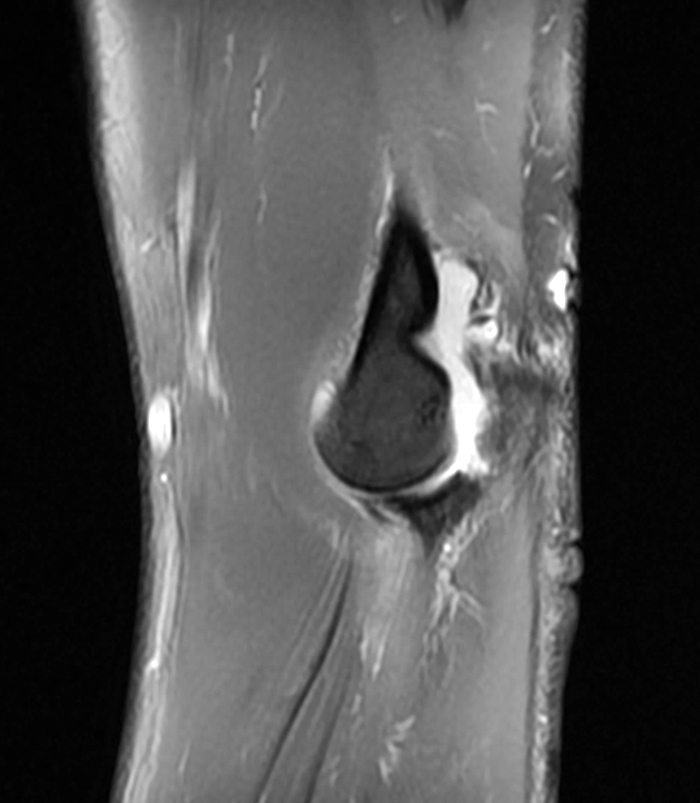
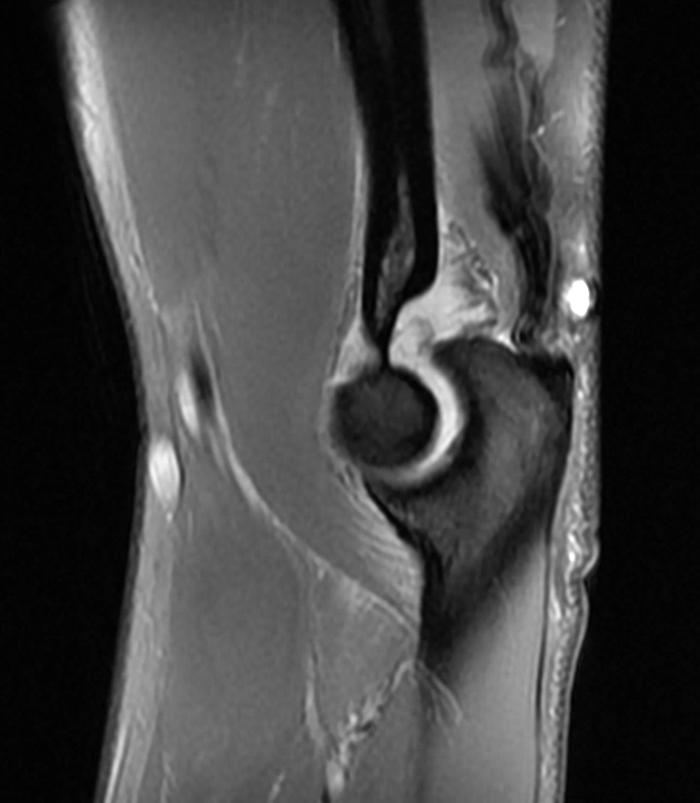
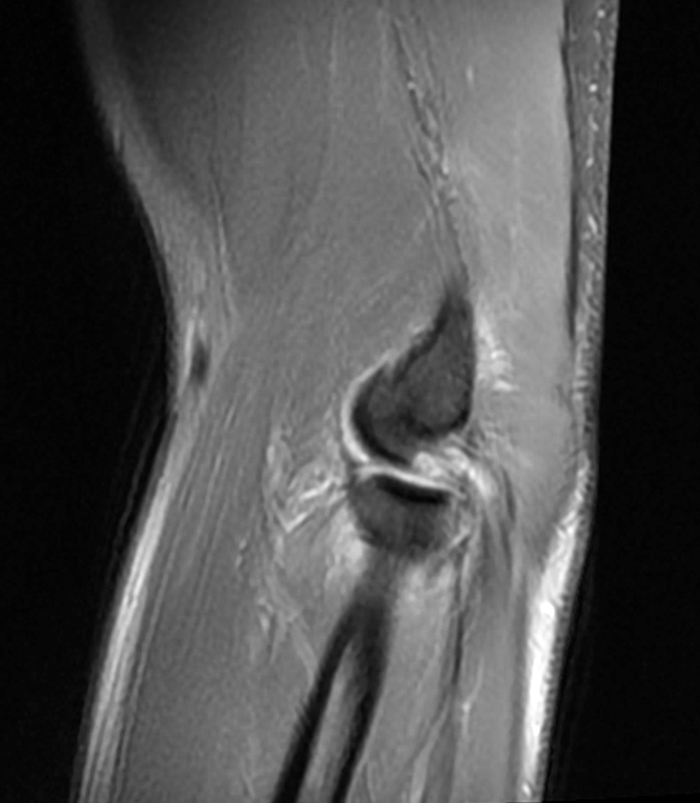
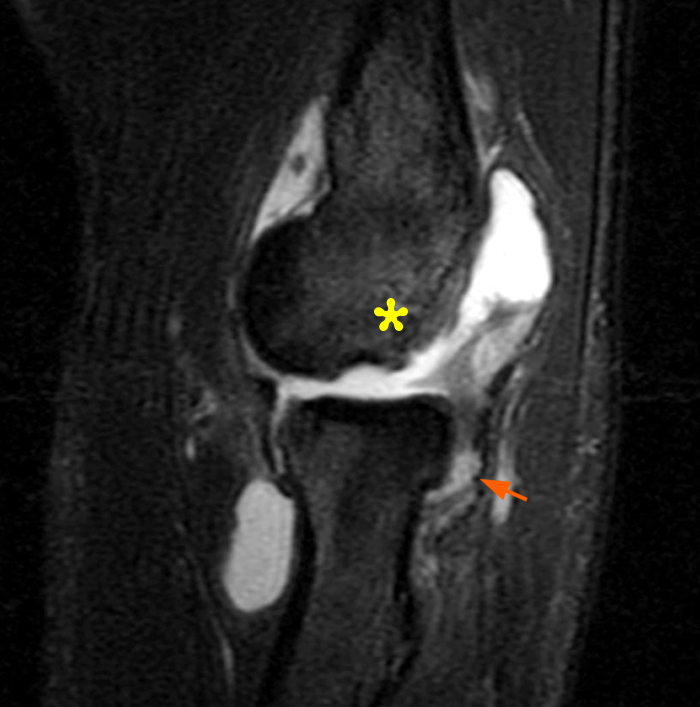
Figure 5:
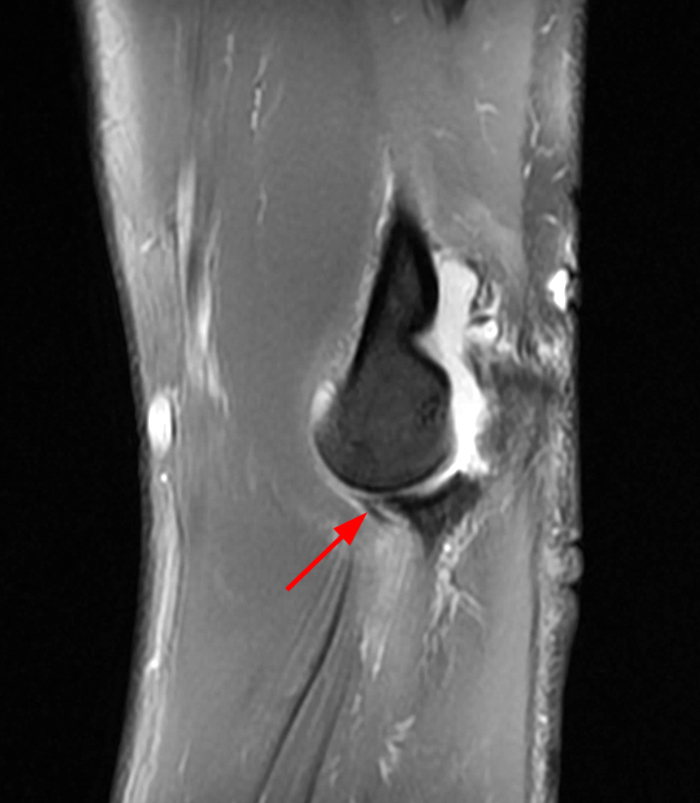
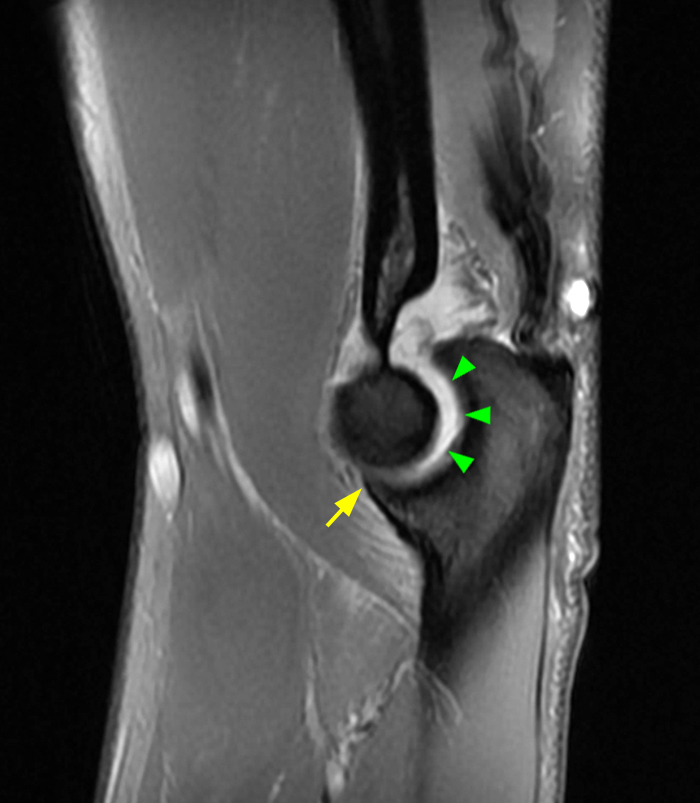
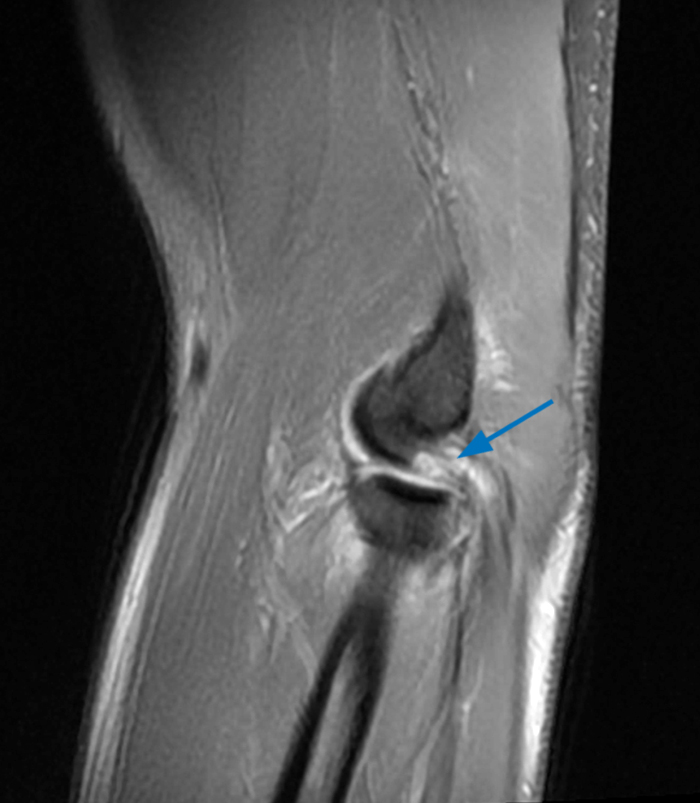
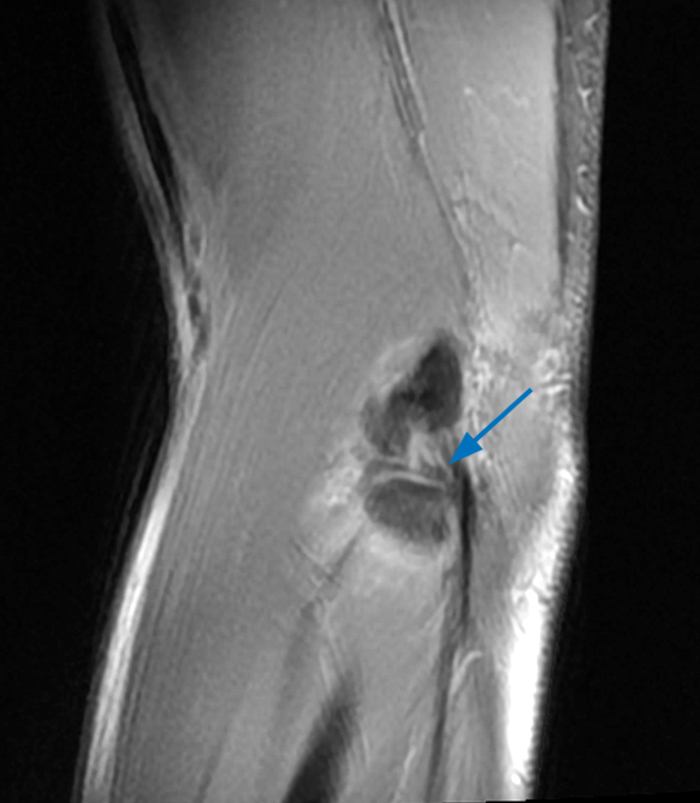
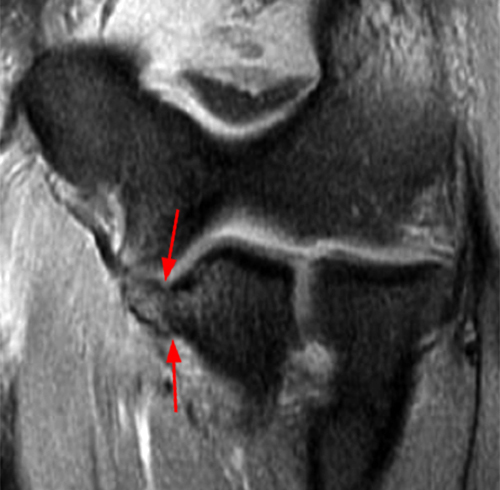
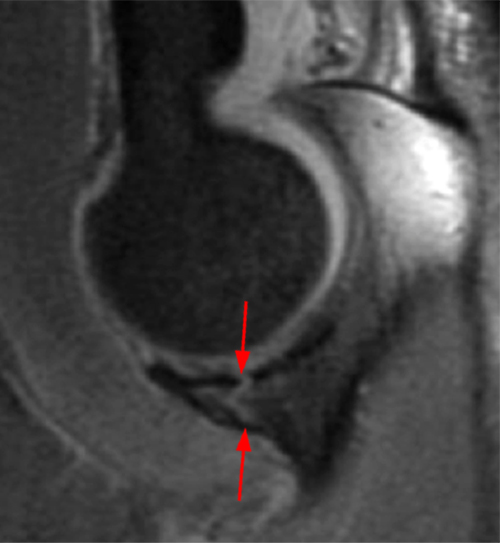
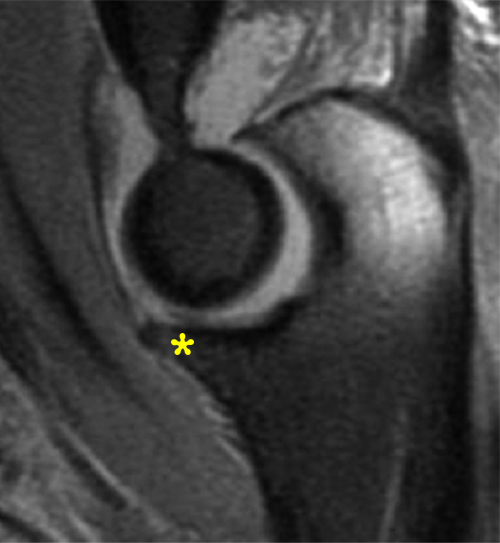
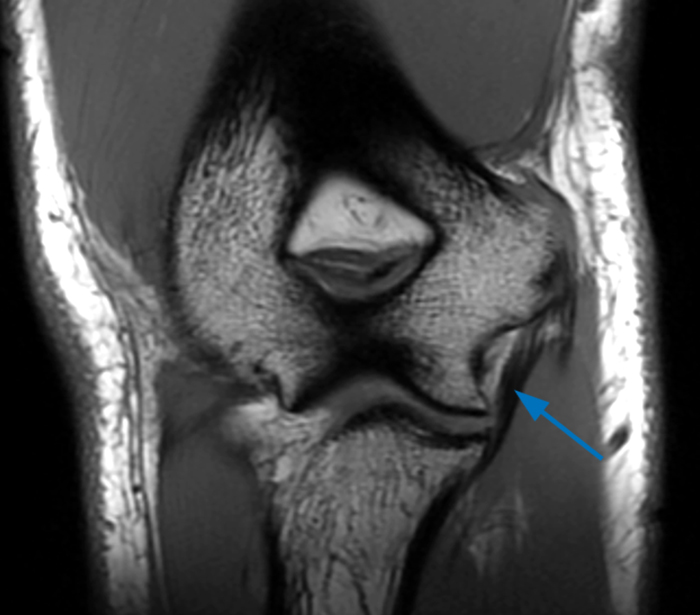
a-c: The sagittal proton density-weighted fat-suppressed images (from medial to lateral) confirm the small fracture of the anteromedial facet of the coronoid process (a; long red arrow), an intact tip of the coronoid process (b; short yellow arrow), and widening of the ulnotrochlear aspect of the joint with anterior subluxation of the trochlea relative to the trochlear notch of the ulna (b; arrowheads). There is also a moderate grade partial tear of the proximal aspect of the lateral ulnar collateral ligament (c,d; long blue arrows) and adjacent soft tissue edema.
Figure 6:
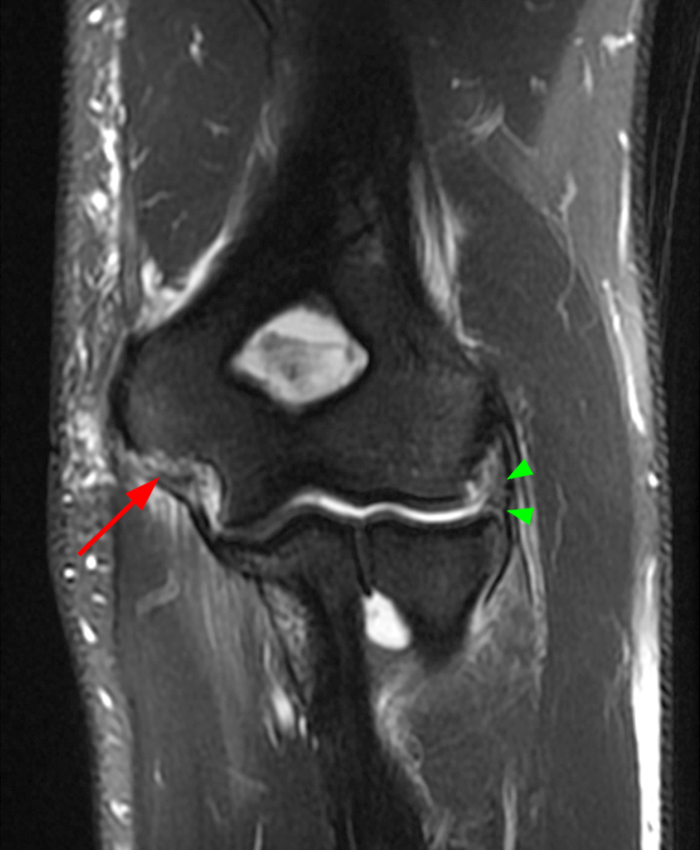
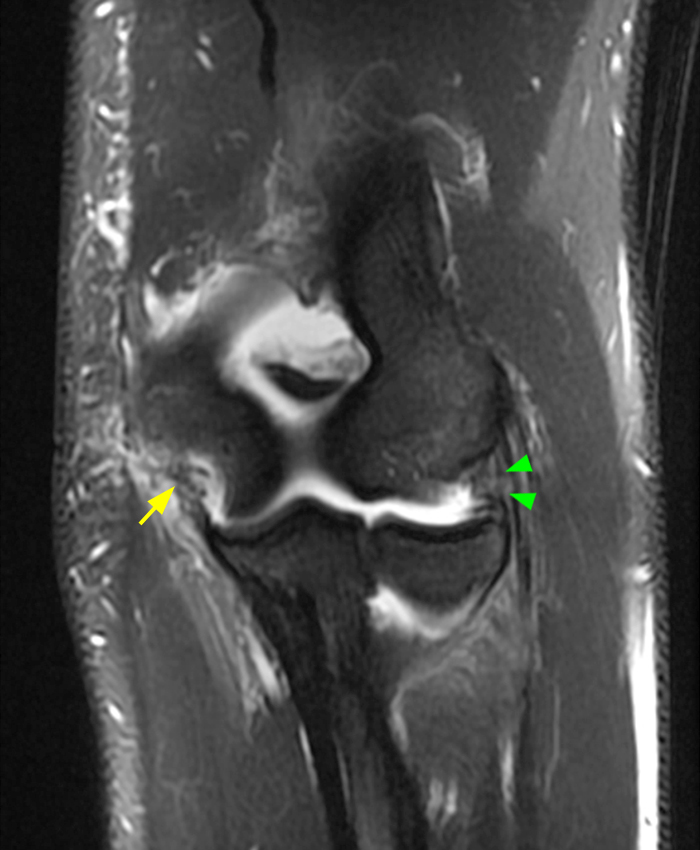
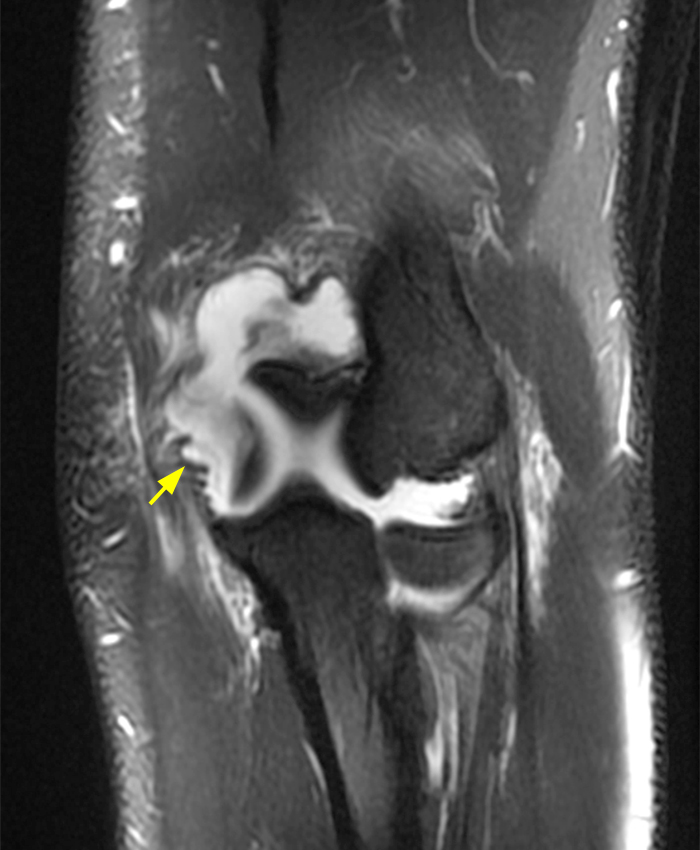
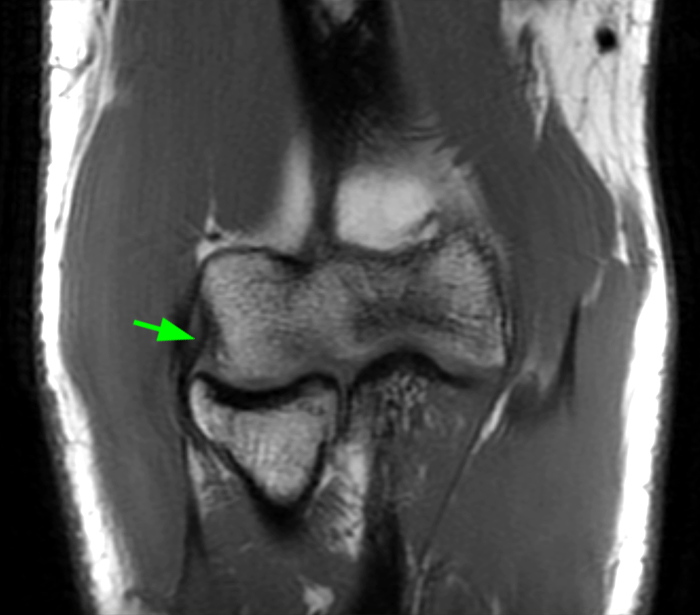
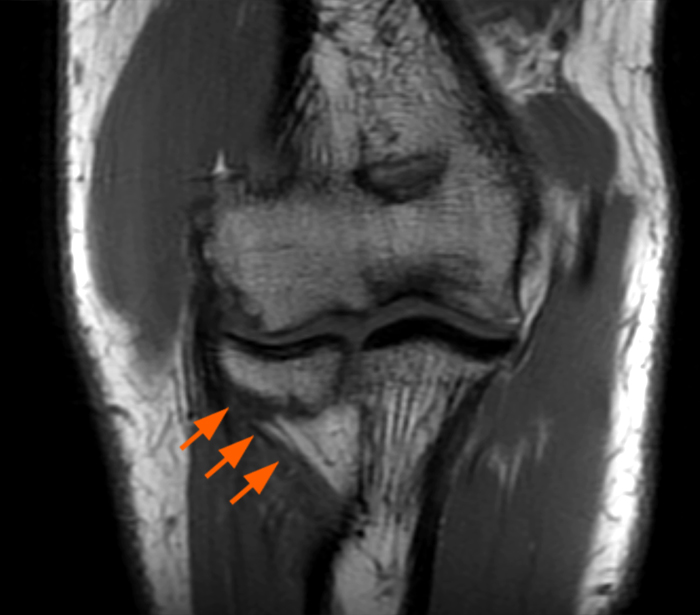
a-c: The T2-weighted fat-suppressed coronal images (from anterior to posterior) show moderate grade partial tearing of the proximal aspect of the anterior bundle (a; long red arrow) and high grade partial tearing of the proximal aspect of the posterior bundle (b,c; short yellow arrows) of the ulnar collateral ligament at the medial epicondyle of the humerus, and partial tearing of the proximal aspect of the radial collateral ligament (a-b; arrowheads). The proximal aspect of the lateral ulnar collateral ligament is not well assessed in these three images. There is edema within the supinator and flexor muscles without associated tearing of the common extensor or flexor tendons.
Diagnosis
Fracture of the anteromedial facet of the coronoid process with injuries to the anterior and posterior bundles of the ulnar collateral ligament and to the lateral ligaments, consistent with varus posteromedial rotatory instability of the elbow (PMRI).
Introduction
Varus posteromedial rotatory instability (PMRI) is one of two major types of traumatic rotatory elbow instability, the other being (valgus) posterolateral rotatory instability (PLRI). PMRI is a relatively new entity, having been described only since 2003 (originally by O’Driscoll and colleagues) and mainly in the orthopaedic literature.1 In fact, to date, PMRI has been largely neglected in the imaging literature. Both PMRI and PLRI imply forceful trauma to the elbow joint although their mechanisms of injury are not the same. With either type of injury, conventional radiographic findings may be subtle or entirely absent. When combined with clinical data, MRI generally allows a specific diagnosis of PMRI and PLRI based on characteristic ligamentous and sometimes osseous abnormalities. Thus, radiologists play an important role in correct diagnosis by detailing the site and degree of injury so that these patients may be treated promptly and appropriately.
Overview of Rotational Injuries of the Elbow
Normal elbow stability relies on a number of osseous and ligamentous structures. Fundamental to this stability is an elbow “lock” related to the apposing curved bone surfaces of the trochlea of the humerus and the trochlear notch of the ulna, which itself is composed of the coronoid process anteriorly and the olecranon posteriorly. Because of this lock, many injury vectors applied to the elbow produce one or more initial fractures followed by fracture displacement, the so-called fracture-dislocations of the elbow. There are two rotational mechanisms of injury, however, that may “unlock” the elbow leading to either joint subluxation or joint dislocation without requiring a major fracture or even any fracture about the elbow. PLRI is one of these, representing a specific instability, or injury mechanism during which there is external rotatory subluxation of the ulnotrochlear portion of the joint and posterolateral dislocation of the radial head relative to the capitellum, while a congruent proximal radioulnar joint is maintained. PLRI involves axial loading, often generated by a fall on an outstretched hand, with additional valgus and external rotation and supination forces, culminating in its final stage as an elbow dislocation (See Videos). Although not uniformly present, a distinctive fracture that is seen in some persons with PLRI is designated the Osborne-Cotterill lesion (Figure 7), representing an osteochondral fracture of the posterolateral surface of the capitellum, sometimes accompanied by a corresponding fracture in the anterior aspect of the radial head related to abnormal contact of these two bone surfaces.2
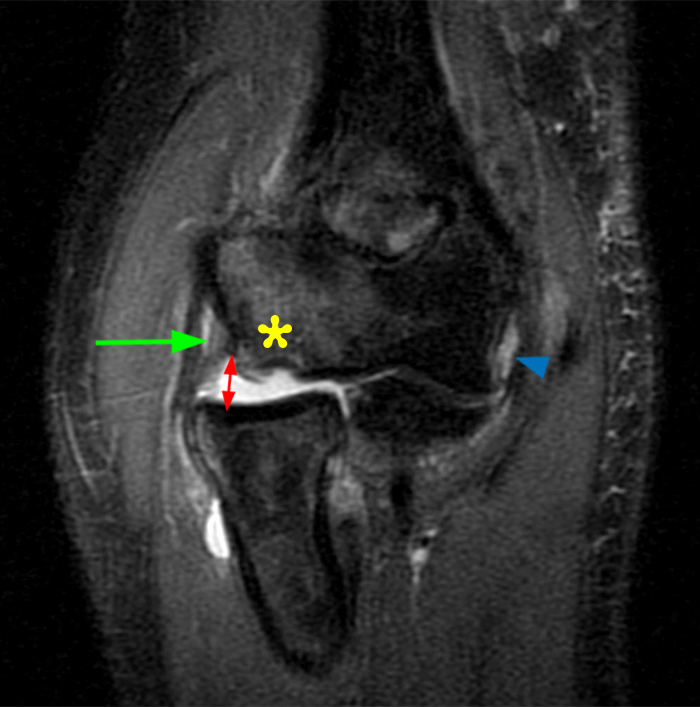
Figure 7:
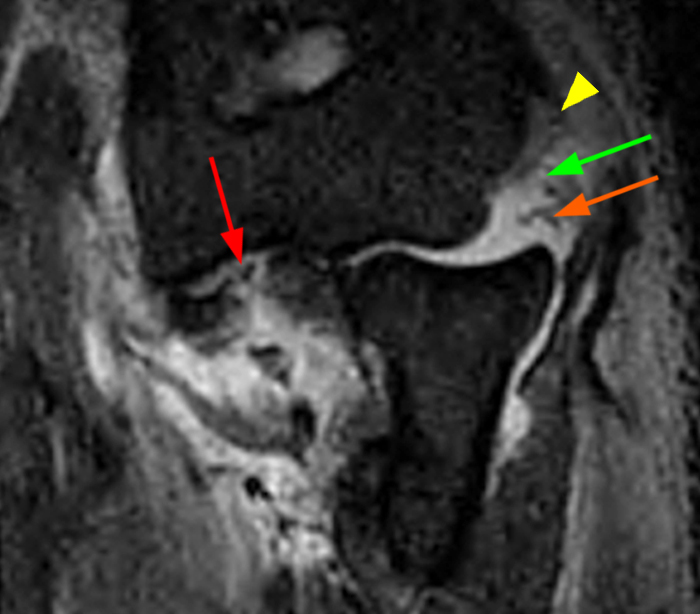
a-b: PLRI. The T2-weighted fat-suppressed sagittal image (a) shows posterior subluxation of the radial head relative to the capitellum and a small impaction fracture of the posterior aspect of the capitellum with surrounding bone marrow edema (asterisk) in this patient with a recent elbow dislocation from a bicycling injury. This fracture, which is seen in some cases of PLRI, is known as an Osborne-Cotterill lesion. The lateral ulnar collateral ligament is also torn (short orange arrow). The coronal T2-weighted fat-suppressed image (b) shows widening of the radiocapitellar joint (red double-sided arrow), the capitellar fracture and bone marrow edema (asterisk), injury to the anterior bundle of the ulnar collateral ligament (arrowhead), and an edematous radial collateral ligament (green long arrow), which was also torn in this case.
The second rotational mechanism is PMRI, a specific pattern of instability, or injury, that also occurs with axial loading, again generally related to a fall on an outstretched hand. In PMRI, however, the fall is often with the shoulder in a flexed and abducted position and the elbow in varus alignment, which causes the trochlea to shift anteriorly, contacting the anteromedial aspect of the coronoid process without posterior displacement of the radial head.1 The resulting motion – pronation and internal rotation – combined with the varus force is usually accompanied by a characteristic fracture of the coronoid process (See Videos), a region that has been designated (although incorrectly) as the anteromedial “facet”. The term anteromedial “facet” will be retained for this clinic in order to promote consistency with the orthopaedic literature. PMRI is also characterized by injuries to the lateral ligamentous complex and the posterior bundle of the ulnar collateral ligament.
Anatomy and Function
The elbow joint is classified as both a hinge and a pivot joint and, as such, has a greater degree of inherent stability when compared to other joints such as the hip and glenohumeral joint. In fact, isolated dislocations of the elbow joint without an accompanying fracture are rare.
The elbow contains three functional regions, or “articulations” – the ulnohumeral articulation, the radiocapitellar articulation, and the proximal radioulnar articulation. The elbow joint is stabilized by both static and dynamic elements, consisting of osseous structures, ligaments, muscles, and tendons that can be classified into primary stabilizers and secondary stabilizers (Figure 8). These stabilizers are organized like the walls that defend a fortress. The outer wall is composed of the three primary stabilizers, all static in nature – the ulnohumeral articulation, the anterior bundle of the ulnar collateral ligament, and the lateral ulnar collateral ligament. The inner wall, which becomes more important when the outer wall is violated, is composed of three secondary stabilizers, two dynamic and one static in nature – the radiocapitellar articulation, the flexor/pronator muscles and tendons, and the extensor muscles and tendons. In addition, a number of dynamic constraints provide further elbow stabilization, consisting of the anconeus, triceps, and brachialis muscles.
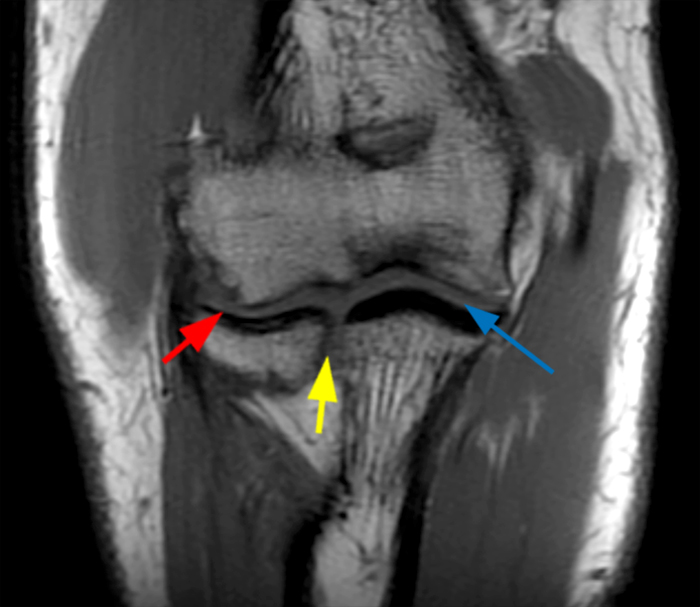
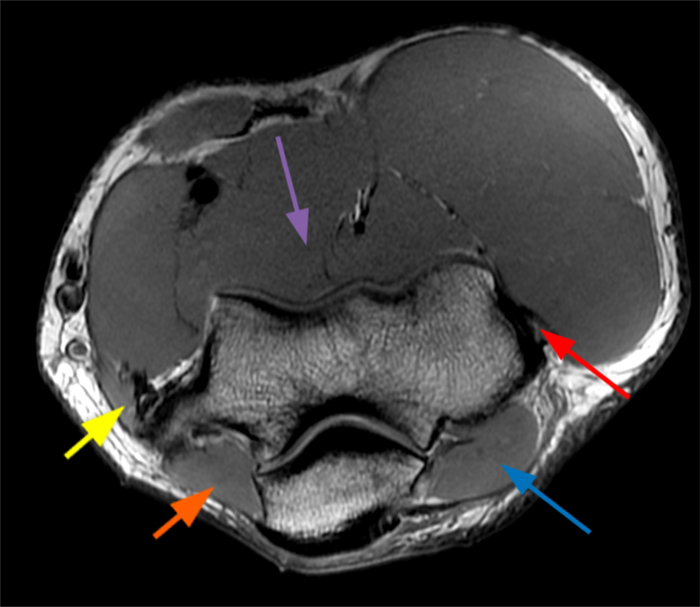
Figure 8:
a-b: Stabilizers of the elbow joint. The coronal T1-weighted image (a) shows a normal, congruent elbow joint with three functional regions: the radiocapitellar compartment (red short arrow), the proximal radioulnar compartment (yellow short arrow), and the ulnohumeral compartment (blue long arrow), without any joint incongruity. The axial T1-weighted image (b) shows the relationship of the flexor muscles and tendon medially (yellow short arrow) with an additional accessory anconeus epitrochlearis muscle in this case (orange short arrow), the common extensor tendon laterally (red arrow), the anconeus muscle laterally (blue arrow), and the brachialis muscle anteriorly (purple arrow), structures that serve as important secondary stabilizers of the elbow.
Two specific structures bear special importance to PMRI, particularly in relation to the injury mechanism: the coronoid process of the ulna and the ulnar collateral ligament. The coronoid process of the ulna is important to the stability of the ulnohumeral articulation as it deepens the trochlear notch of the ulna and anchors the humeral trochlea in place, preventing its anterior translation. Even small fractures of the coronoid process may have devastating long-term effects with regard to elbow stability and function if they are not recognized and treated promptly and, as such, these fractures are often surgically repaired. The coronoid process also serves as the insertion site for both the anterior bundle of the ulnar collateral ligament (via the sublime tubercle and sublime ridge) and the tendon of the brachialis muscle.3 The sublime tubercle protrudes medially and is continuous with the anteromedial aspect of the coronoid process which, as noted previously, is sometimes referred to as the anteromedial facet despite lacking a true flat surface. It is also referred to as the anteromedial rim of the coronoid process. The anteromedial facet is then continuous centrally with the tip of the coronoid process, which is the most anterior aspect of the entire coronoid process. The anteromedial facet is more susceptible to fracture as only 40% of it is supported by the ulnar metaphysis.4 Despite its relative lack of structural support, the anteromedial facet plays an important role in resisting posterior subluxation of the ulna and both posteromedial and posterolateral rotatory forces.
Classification of Fractures of the Coronoid Process
The classification system of fractures of the coronoid process introduced by O’Driscoll and colleagues in 2003 recognizes the importance of the anteromedial facet of the coronoid process (Figure 9). Although other investigators in describing fractures of the coronoid process have emphasized additional classification schemes, the O’Driscoll classification is emphasized here as it is most applicable to the topic of PMRI. Therefore, in the text that follows, any references to types or subtypes of fractures of the coronoid process will refer to the O’Driscoll classification system only.
Figure 9:
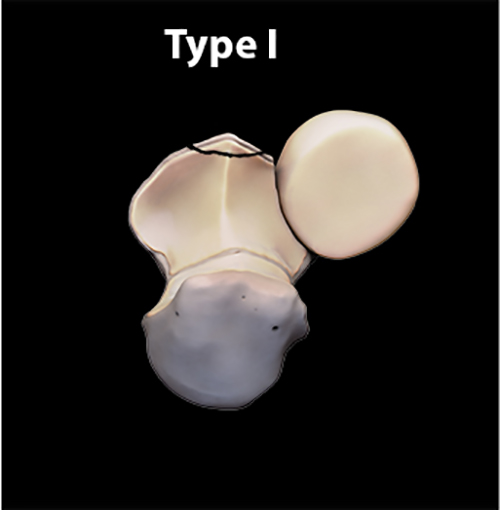
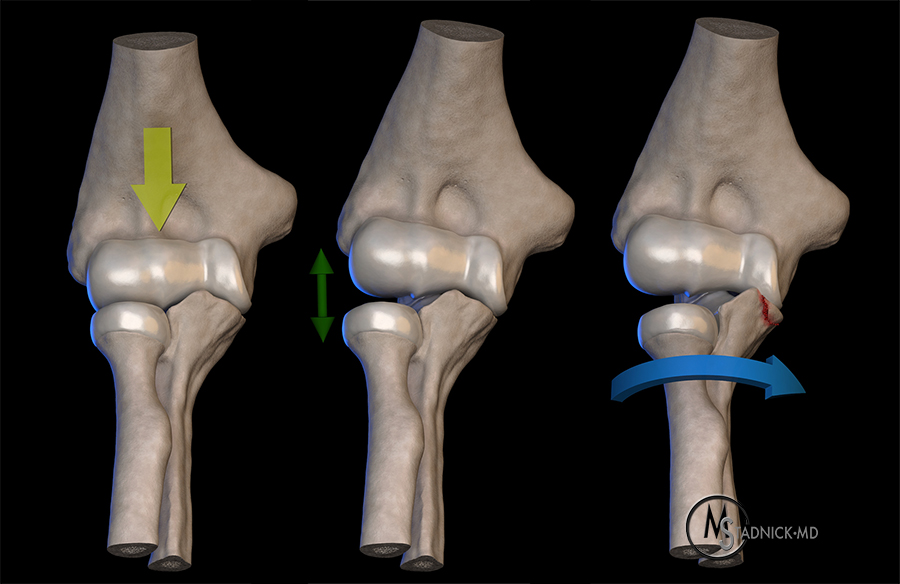
3D renderings demonstrate the O’Driscoll coronoid process fracture classification.
(A) Type I fracture involves the tip of the coronoid process and consists of two subtypes (not shown).
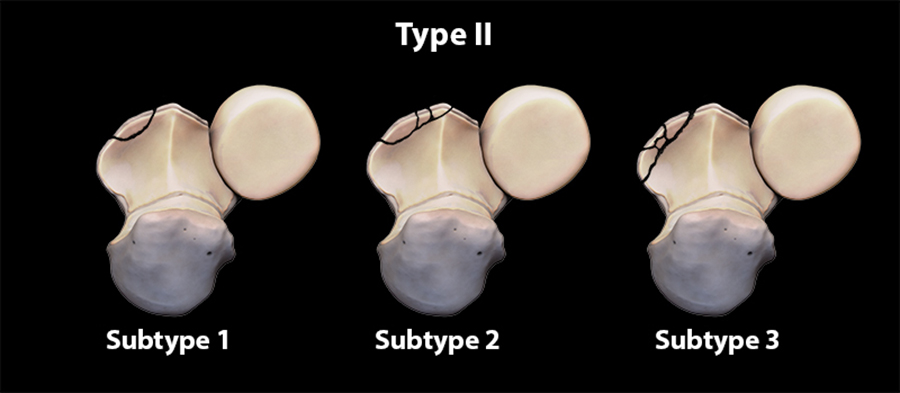
(B) Type II fracture involves the anteromedial facet of the coronoid process. Subtype 1 of this fracture involves only the anteromedial facet; subtype 2 involves the anteromedial facet and coronoid process tip; subtype 3 involves the anteromedial facet and sublime tubercle.
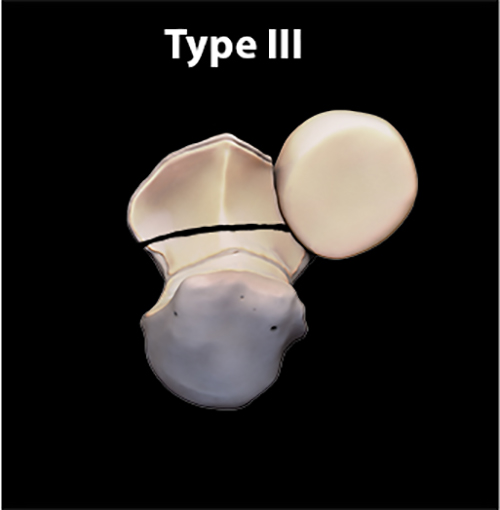
(C) Type III fracture involves the base of the coronoid process and has two subtypes (not shown).
The three main categories of coronoid fractures, which we will describe using Roman numerals, are the tip of the coronoid process (type I, with two subtypes), the anteromedial facet of the coronoid process (type II, with three subtypes), and the basal aspect of the coronoid process (type III, with two subtypes). Coronoid tip (type I) fractures are usually seen in either the so-called “terrible triad” injury (elbow dislocation with radial head and coronoid fractures) or the PLRI injury and occur along the coronal plane of the coronoid process itself. To be classified as a type I injury, the fracture must be confined to the tip of the coronoid process and must not extend as far medial as the sublime tubercle. The two subtypes of the type I fracture of the tip of the coronoid process are based on the size of the resulting bone fragment; subtype 1 indicates a fracture fragment, that in the anteroposterior plane, is less than 2mm from the edge of the tip; and subtype 2 indicates a fracture fragment greater than 2mm in the anteroposterior plane, but a fragment involving less than one third of the coronoid body and not involving the sublime tubercle medially.1
Fractures of the anteromedial portion of the coronoid process (type II) are further classified into 3 subtypes (Figures 10,11). Subtype 1 fractures are in an oblique plane (i.e., with orientation between true sagittal and coronal planes) and involve only the anteromedial facet whereas subtype 2 fractures are comminuted and extend slightly more laterally, involving the anteromedial facet and the tip of the coronoid process. Subtype 3 fractures are also comminuted but extend slightly more medially, involving the anteromedial facet and extending through the attachment of the anterior bundle of the ulnar collateral ligament at the sublime tubercle.1 Subtype 3 fractures can also occasionally involve the tip of the coronoid process. While these last fractures may appear small, they can lead to both elbow instability and incongruity of the apposing surfaces of the trochlea and the trochlear notch. Indeed, in some cases, the trochlea may appear to articulate only with the fracture and not with the remainder of the trochlear notch.1 The resulting joint widening, or “gapping,” places abnormally high loads at the fracture site in the ulnohumeral joint, which may predispose to early and significant post-traumatic osteoarthrosis.1
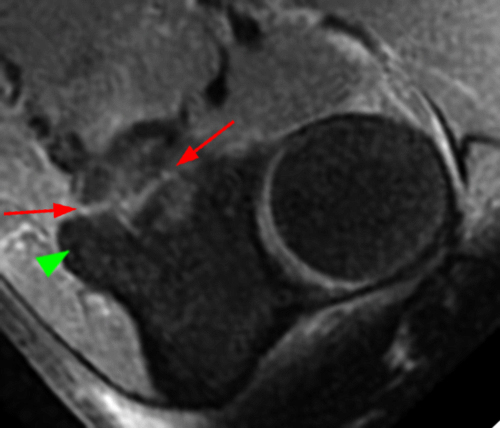
Figure 10:
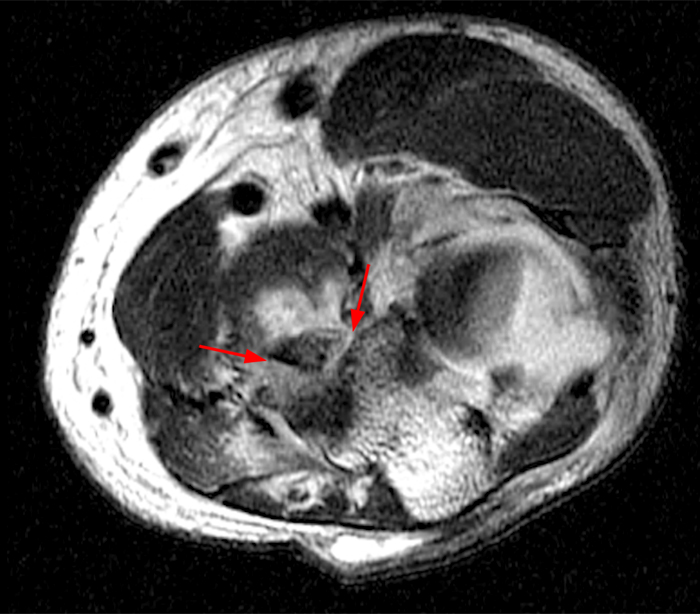
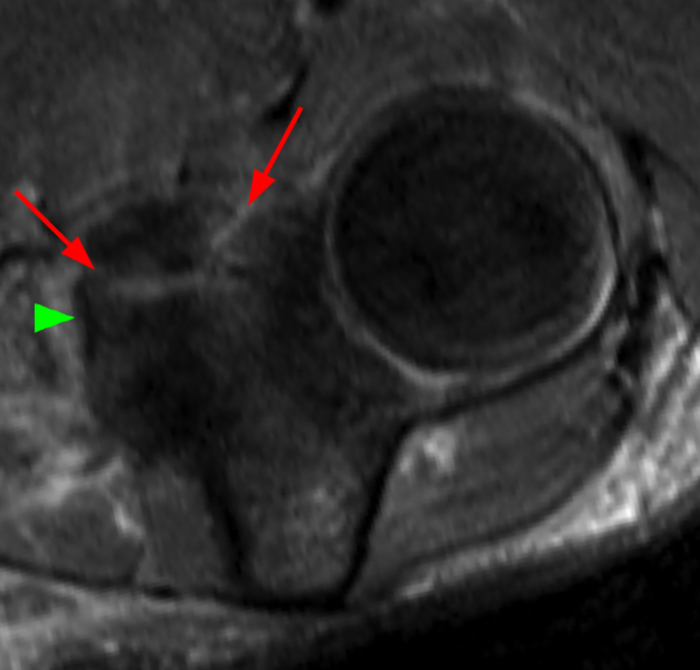
a-d: PMRI. T2-weighted fat-suppressed images show an O’Driscoll type II, subtype 1 fracture of the coronoid process involving only the anteromedial facet (red arrows) and sparing the sublime tubercle (green arrowhead), as shown on transverse (a), coronal (b), and two sagittal images (c,d), with image c medial to image d. Note that the tip of the coronoid process is intact although linear artifact makes it difficult to fully appreciate on this single image (yellow asterisk). The coronoid tip is not included in image a.
Figure 11:
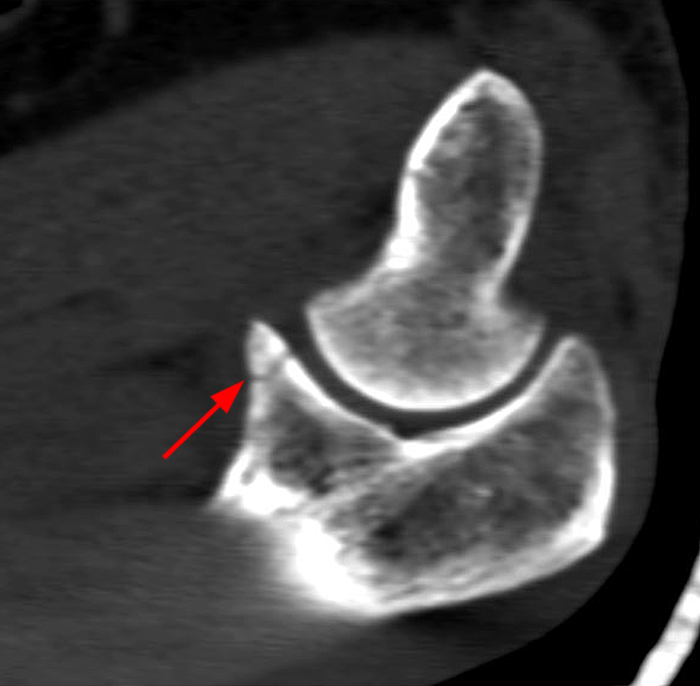
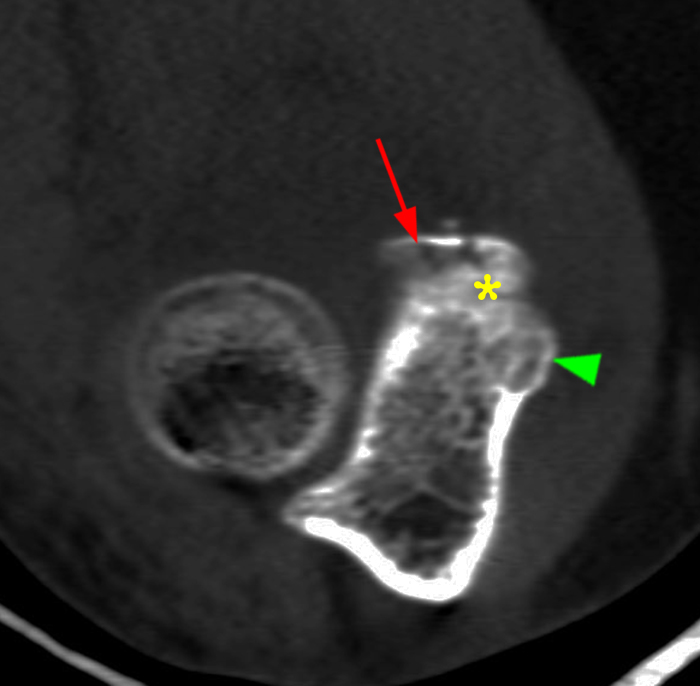
a-b: PMRI. The sagittal and axial CT images demonstrate an O’Driscoll type II, subtype 2 fracture of the coronoid process with involvement of both the tip (red arrows) and the anteromedial facet (yellow asterisk) of the coronoid process, but sparing the sublime tubercle (green arrowhead).
Basal coronoid fractures (type III) extend deeper into the trochlear notch, requiring involvement of at least half of the total anteroposterior dimension of the coronoid process.1 The type III fractures are often a component of an olecranon fracture-dislocation and may consist of multiple comminuted bone fragments or a single larger bone fragment. Interestingly, these fractures tend to have less severe concomitant soft tissue injuries when compared to those accompanying the more subtle fractures of the tip or anteromedial facet. With regard to the further classification of the type III basal coronoid fracture, a subtype 1 injury does not involve the olecranon, whereas a subtype 2 injury has an associated olecranon fracture.1
Injuries of the Medial and Lateral Ligamentous Complexes
Figure 12:
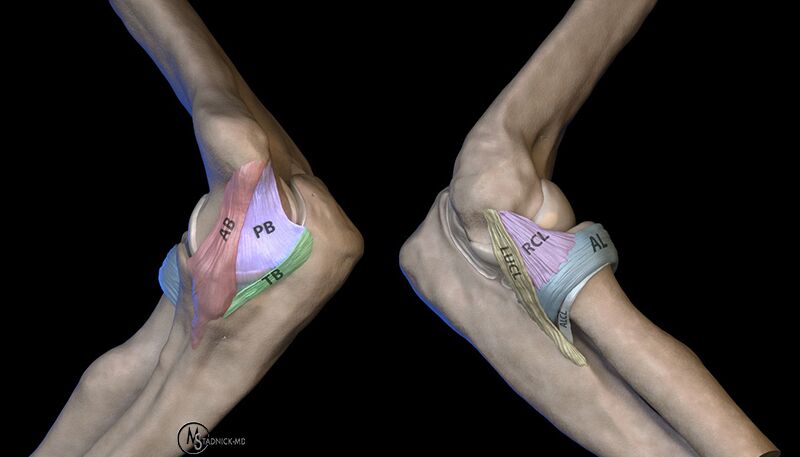
3D renderings depict the anatomy of the medial ligamentous complex (left) and lateral ligamentous complex (right). (Click on the link below to activate the interactive animation, then hold-left click and drag to the right – Caution Large File) Click Here to Activate 3D Animation
Figure 13:
a-d: Normal ligaments of the elbow. The coronal T1-weighted images (a-c) demonstrate normal ligamentous anatomy including the radial collateral ligament (a; green short arrow), lateral ulnar collateral ligament posterior to the radial head (b; orange short arrows), and the anterior bundle of the ulnar collateral ligament (c; blue long arrow). The axial T1-weighted image (d) shows a normal posterior bundle of the ulnar collateral ligament (red long arrow) serving as the floor of the cubital tunnel, with an accessory anconeus epitrochlearis muscle (blue asterisk) in this case coursing superficial to the ulnar nerve (yellow short arrow).
Injuries of the medial and lateral ligamentous complexes are also a key component in most persons with PMRI. The anterior bundle of the ulnar collateral ligament is composed of two bands (anterior and posterior bands) and is attached proximally to the inferior aspect of the medial epicondyle of the humerus and distally to the sublime tubercle and sublime ridge of the coronoid process. The anterior and posterior bands are reciprocal in function with inherent differences in laxity that vary with the degree of flexion at the elbow. Both bands may be injured simultaneously or successively during an injury to the joint, or one band may be injured in the absence of an injury to the other band. The anterior bundle as a whole is a primary restraint to valgus stress, except in maximal elbow extension, a position in which the posterior bundle of the ulnar collateral ligament becomes the primary stabilizer. The posterior bundle attaches proximally to the posterior aspect of the medial epicondyle, and this bundle attaches distally to the medial aspect of the olecranon, thus forming the floor of the cubital tunnel. The transverse bundle of the ulnar collateral ligament, which connects the distal attachments of the anterior and posterior bundles, is variably present in humans, does not have a proven contribution to elbow stability, and will not be emphasized in this discussion.
While the anterior bundle of the ulnar collateral ligament complex, not surprisingly, is often disrupted in fractures of the anteromedial facet of the coronoid process (particularly subtype 3 injuries), the status of the posterior bundle in PMRI is becoming increasingly clear. If an injured posterior bundle of the ulnar collateral ligament complex is not repaired in conjunction with injuries of the anterior bundle of the ulnar collateral ligament in the setting of PMRI, persistent joint incongruity and instability may result.5 Additionally, isolated posterior bundle injuries have been shown to lead to clinical findings of PMRI without coexisting injuries of the lateral ligamentous complex, with or without fractures of the anteromedial facet of the coronoid process.6 In fact, injury of the posterior bundle of the medial ligamentous complex may account for those cases of isolated elbow subluxations without a fracture.6,7 An injury of the posterior bundle of the ulnar collateral ligament, however, is not required for clinical instability or subtle joint incongruence in the setting of both a fracture of the anteromedial facet of the coronoid process and a radial collateral ligament injury.8
The radial collateral ligament, the lateral ulnar collateral ligament, or both ligaments are usually injured in the setting of PMRI, but such injury is not required. Both lateral ligaments have a common proximal attachment at the lateral epicondyle. Distally, the radial collateral ligament attaches to both the annular ligament and the supinator muscle, whereas the lateral ulnar collateral ligament passes posterior to the radial head, attaching to the supinator crest of the ulna and serving as a posterior stabilizer of the radial head.
Clinical History, Presentation, and Physical Examination
PLRI. This animation demonstrates the typical mechanism of a fall on an outstretched hand with valgus force and external rotation/supination at the forearm, resulting in posterolateral rotatory instability and dislocation and the common accompanying bony injuries. (Anterior view of the elbow top left and lateral view of the elbow bottom left)
PMRI. This animation depicts the posteromedial rotatory instability mechanism resulting from a fall on an outstretched hand with the shoulder flexed and abducted resulting in axial loading and varus force at the elbow with pronation of the forearm. This results in a characteristic coronoid process fracture involving the anteromedial aspect. (Anterior view of the elbow top left and posterior view of the elbow top right)
A person with PMRI typically presents with a history of a fall, usually on an outstretched hand. The exact details of the fall (e.g., varus or valgus stress, internal or external rotation) may not be recalled. Careful questioning may indicate that the elbow felt like it “was out of place” or there was a sensation of clicking, popping, or slipping. Subsequently, the injured person may note a feeling of instability when an axial load is placed on the elbow. On physical examination, crepitus in or about the elbow may be evident during joint motion related to incongruence of the ulnohumeral articulation.9
If the injured person is not assessed immediately but rather seeks attention weeks after the initial injury, the patient may present with local pain about and contracture of the elbow. There may also be clinical evidence of ulnar neuropathy, especially if the posterior bundle of the ulnar collateral ligament is injured.
Figure 14:
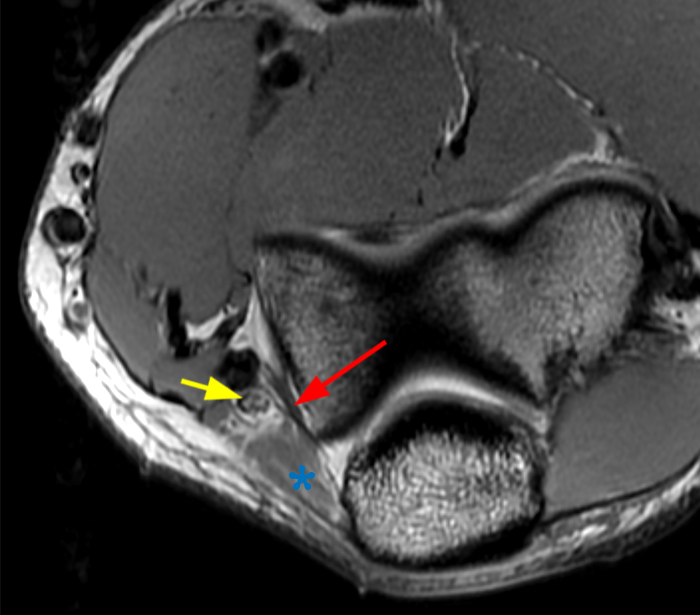
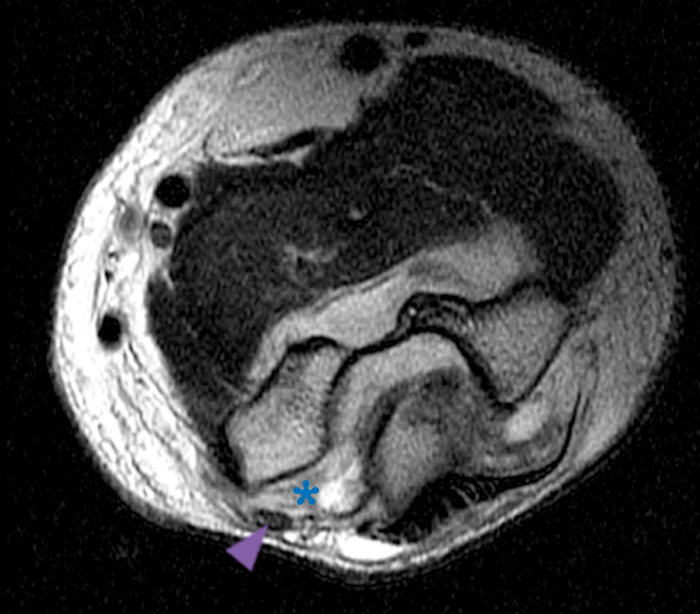
a-c: PMRI. The coronal T2-weighted fat-suppressed image (a) shows a complete tear of the common extensor tendon (yellow arrowhead), radial collateral ligament (green arrow), and lateral ulnar collateral ligament (orange arrow) at their humeral attachments in addition to a fracture of the anteromedial facet of the coronoid process (red arrow). The axial T1-weighted images (b,c) show disruption of the cubital tunnel retinaculum (blue asterisk), medial subluxation of the ulnar nerve (purple arrowhead) at the medial epicondyle (b), and a fracture of the anteromedial facet (c) (red arrows).
Clinical signs of PMRI are often nonspecific. Although provocative maneuvers can be performed to assess for joint instability, pain may limit the utility of these maneuvers in the acute setting, and full analysis may require physical examination under anesthesia at the time of surgery.10 Unlike PLRI in which stress testing – such as the pivot shift test, chair sign, and pushup sign – has been proven to be reliable for accurate diagnosis, stress testing used to confirm varus instability in PMRI is not as well validated.10 The hyperpronation test (i.e., passive hyperpronation at 90 degrees of elbow flexion while palpating for ulnohumeral subluxation) and the gravity-assisted varus stress test (i.e., elbow moved from extension to flexion with the shoulder abducted and the forearm in neutral position to elicit instability/pain/crepitus as a positive result) are two of the more popular bedside tests for the diagnosis of PMRI, although other tests exist.10
Additionally, the medial and lateral joint lines should be palpated to assess for tenderness of the underlying medial and lateral ligamentous complexes that may indicate injuries to these structures. Evaluation for ulnar neuropathy is also warranted.
Key Imaging Findings
Figure 15:
Interactive animation demonstrates the mechanism of action for PMRI. The injury occurs with axial loading, varus force, and pronation and internal rotation at the elbow, which causes an anterior shift of the trochlea and results in a fracture of the anteromedial aspect of the coronoid process. Injury to the lateral ligamentous complex and posterior bundle of the medial collateral ligament may also occur. (Click on the link below to activate the interactive animation, then hold-left click and drag to the right – Caution Large File) Click Here to Activate 3D Animation
The accurate diagnosis of PMRI generally requires correlation of clinical and imaging data, as many of the imaging features of this condition, whether they are provided by conventional radiography, CT scanning, or MRI, or combinations of these, lack specificity. As an example of this, injuries to one or more of the lateral supporting structures of the elbow, often seen in cases of PMRI, accompany other mechanisms of injury including PLRI. Likewise, injuries involving the anterior or posterior bundle or both bundles of the medial ligamentous complex of the elbow are evident in valgus injuries, PLRI, PMRI, and other mechanisms. Rather, it is the fracture pattern of the coronoid process of the ulna that may provide the most important (albeit not diagnostic) clue to accurate diagnosis of PMRI, although this fracture is not present in all cases.
The type I fractures involving the tip of the coronoid process are usually seen in either PLRI or the terrible triad injury. When this type of fracture is present, imaging may also reveal concomitant radial head fractures or an Osborne-Cotterill lesion, as well as malalignment at both the ulnotrochlear and the radiocapitellar compartments of the elbow joint. When imaging reveals evidence of a type II fracture, with involvement of the anteromedial facet of the coronoid process, PMRI should be strongly considered. Type III fractures, which involve the base of the coronoid process, occur with olecranon fracture-dislocations.
Although there are several general reviews of the subject of patterns of fracture of the coronoid process, there is only one study evaluating data related to the frequencies of the various subtypes of the type II coronoid fracture in patients with PMRI, and this study involves only a small group of patients. In this latter study of 27 PMRI patients with type II fractures only, subtype 1 fractures were not present, subtype 2 fractures were the most common, occurring in 60% of the patients, and subtype 3 fractures were evident in 40% of the patients.11 Despite the lack of subtype 1 fractures in the aforementioned study, the small sample size in this study limits the power of these observations. Indeed, we have seen the subtype 1 fracture in our practice in persons with clinical evidence of PMRI, as shown in Figures 10, 14, and 16. Additionally, owing to the inherent subjectivity in the delineation of the boundaries of the anteromedial facet, there is variability in the methods and imaging techniques used to study fractures of the coronoid process.
Figure 16:
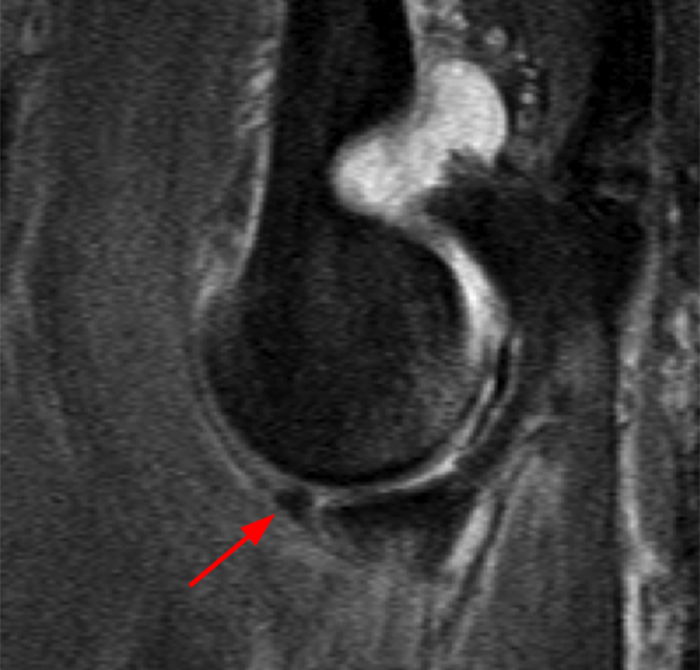
a-b: PMRI. The type II, subtype 1 fracture of the coronoid process in this patient involves only the anteromedial facet of the coronoid process (red arrows), sparing the sublime tubercle (green arrowhead) of the coronoid process as clearly shown in the axial (a) and sagittal (b) T2-weighted fat-suppressed MR images. Note that both the sagittal and axial images are at the level of the anteromedial facet and not the tip of the coronoid process.
Based on our own experience with cases of PMRI, the identification of a subtype 1 fracture of the anteromedial facet of the coronoid process and the absence of a radial head fracture (which, if present, would suggest either a terrible triad or PLRI injury), are important clues to the possible presence of PMRI, and this diagnosis should be considered when the clinical findings are being assessed. Further, fractures of the anteromedial facet that also involve the sublime tubercle or tip of the coronoid process, or both, are also compatible with the diagnosis of PMRI but they clearly are not diagnostic of this condition. Additional conventional radiographic findings that can be present (although not uniformly) in PMRI include an avulsion fracture of the lateral epicondyle, subtle ulnohumeral joint incongruity, and a widened radiocapitellar interosseous distance (generally indicating complete disruption of the lateral collateral ligament complex). Additionally, a “double crescent sign” on radiographs is considered pathognomonic for these fractures of the anteromedial facet and consists of a double subchondral curvilinear radiodensity related to a displaced bone fragment paralleling the remaining contour of the coronoid process. This results in a loss of alignment between the medial aspect of the coronoid process and apposing articular surface of the distal humerus.12
When the fracture is not evident in conventional radiographs, CT scanning or MRI will generally indicate an injury to the anteromedial facet, appearing as a distinct fracture line with either imaging method or, with MRI, a bone contusion. One of the pitfalls in diagnosis is to mistake the location of this fracture as the tip of the coronoid process, but careful analysis of all of the imaging planes will eliminate this mistake. The transverse images will reveal that the fracture is located below the joint line at the level of the radial head and 1-2 images inferior to the level of the coronoid tip. Typically, in this plane, the fracture has a coronal or coronal-oblique orientation. In the coronal images, this fracture is clearly seen to be medial to the tip of the coronoid process. The appearance of the fracture line in the sagittal images may appear confusing until it is realized that the specific image showing the fracture is also medial to the tip of the coronoid process. As mentioned previously, in some cases of PMRI, the fracture of the coronoid process of the ulna is not isolated to the anteromedial facet alone but, rather, extends to the sublime tubercle (subtype 2) or to the tip of the coronoid process (subtype 3), or even in both directions (also subtype 3).1
The degree of ligamentous involvement is optimally assessed on MRI. Accurate localization of the injury to one or both bundles of the ulnar collateral ligament or to one or more of the ligaments of the lateral ligamentous complex, or to both the medial and lateral ligaments, requires knowledge of the full course of these ligaments. MRI can also demonstrate the degree of ulnohumeral incongruence and surrounding soft tissue injuries. MRI or CT scanning can be useful in the search for coexisting intraarticular bodies that may limit complete reduction of a subluxed or dislocated joint.
Management
While the fractures of the anteromedial facet of the coronoid process in PMRI are frequently small, surgical fixation is often recommended. If left untreated, persistent instability related to incongruence of the ulnohumeral aspect of the joint, particularly when the elbow is subjected to varus stress, will lead to rapid post-traumatic osteoarthrosis owing to the intense forces that are directly placed on the trochlea at its contact point with the fractured coronoid process.13 The exact surgical technique used for fixation of the fracture of the coronoid process depends on the fracture subtype. A fracture of the anteromedial facet alone (subtype 1) is initially reduced and then fixed with any buttressing that is deemed necessary owing to the lack of bone support from the ulnar metaphysis. Fractures gauged as subtype 2 or 3, or both (i.e., involving the tip or sublime tubercle of the coronoid process, or both of these) require additional hardware fixation at sites of fracture comminution to fully support either the ulnohumeral aspect of the joint (subtype 2) or the sublime tubercle and ulnar collateral ligament (subtype 3).1 In addition to fracture fixation, coexisting lateral ligamentous injuries and injuries to either the anterior bundle or the posterior bundle of the ulnar collateral ligament, or to both bundles, can be repaired at the same time as fracture fixation to restore full joint stability.6 Finally, if the fracture fragment is small and there is no evidence of varus instability with provocative maneuvers, conservative management may be adequate, requiring close follow-up surveillance for the subsequent development of osteoarthrosis.
Conclusion
PMRI is a distinct rotational elbow injury that has been described only recently in the orthopaedic literature. Owing to the risk of accelerated osteoarthrosis and persistent varus instability of the elbow with axial loading when the diagnosis and treatment of PMRI are delayed, radiologists need to become aware of its major imaging findings. In addition to injuries of the lateral and medial ligamentous complexes of the elbow, which may lack specificity, a characteristic but not diagnostic fracture of the anteromedial facet of the coronoid process is seen in some (but not all) cases of PMRI. Such a fracture should stimulate a search for clinical findings of PMRI in order to ensure that correct diagnosis of this condition is not delayed.
References
- O’Driscoll SW, Jupiter JB, Cohen MS, Ring D, McKee MD. Difficult elbow fractures: pearls and pitfalls. Instr Course Lect of the American Academy of Orthopaedic Surgeons. 2003;52:113-34. ↩
- Jeon IH, Min WK, Micic ID, Cho HS, Kim PT. Surgical treatment and clinical implication for posterolateral rotatory instability of the elbow: Osborne-Cotterill lesion of the elbow. J Trauma. 2011 Sep;71(3):E45-9. ↩
- Malagelada F, Dalmau-Pastor M, Jordi V, Golano P. Elbow Anatomy. In: Sports Injuries. Berlin, Heidelberg: Springer; 2014. 10.1007/978-3-642-36801-1_38-1. ↩
- Park SM, Lee JS, Jung JY, Kim JY, Song KS. How should anteromedial coronoid facet fracture be managed? A surgical strategy based on O’Driscoll classification and ligament injury. J Shoulder Elbow Surg. 2015 Jan;24(1):74-82. ↩
- Morrey BF. Reconstruction of the posterior bundle of the medial collateral ligament: a solution for posteromedial olecranon deficiency—a case report. J Shoulder Elbow Surg 2012;21:e16-9. ↩
- Gluck MJ, Beck CM, Golan EJ, Nasser P, Shukla DR, Hausman MR. Varus posteromedial rotatory instability: a biomechanical analysis of posterior bundle of the medial ulnar collateral ligament reconstruction. J Shoulder Elbow Surg. 2018 Jul;27(7):1317-1325. ↩
- Golan EJ, Shukla DR, Nasser P, Hausman M. Isolated ligamentous injury can cause posteromedial elbow instability: a cadaveric study. J Shoulder Elbow Surg. 2016 Dec;25(12):2019-2024. ↩
- Hwang JT, Shields MN, Berglund LJ, Hooke AW, Fitzsimmons JS, O’Driscoll SW. The role of the posterior bundle of the medial collateral ligament in posteromedial rotatory instability of the elbow. Bone Joint J. 2018 Aug;100-B(8):1060-1065. ↩
- Lenich A, Siebenlist S, Imhoff AB. Traumatic Rotatory Instability of Elbow: Posterolateral Rotatory Instability (PLRI) and Posteromedial Rotatory Instability (PMRI). Acute Elbow Trauma. Strategies in Fracture Treatments. Springer; 2019, Chapter 2. ↩
- Chan K, Athwal GS. Varus Posteromedial Rotatory Instability. In: Tashjian RZ (ed), The Unstable Elbow. Switzerland: Springer; 2017. ↩
- McLean JM, Kempston MP, Pike JM, Goetz TJ, Daneshvar P. Varus posteromedial rotatory instability of the elbow: injury pattern and surgical experience of 27 acute consecutive surgical patients. J Orthop Trauma. 2018 Dec;e469-e474. ↩
- Sanchez-Sotelo J, O’Driscoll SW, Morrey BF. Medial oblique compression fracture of the coronoid process of the ulna. J Shoulder Elbow Surg. 2005;14(1):60-4. ↩
- Pollock JW, Brownhill J, Ferreira L, McDonald CP, Johnson J, King G. The effect of anteromedial facet fractures of the coronoid and lateral collateral ligament injury on elbow stability and kinematics. J Bone Joint Surg Am. 2009 Jun;91(6):1448-58. ↩