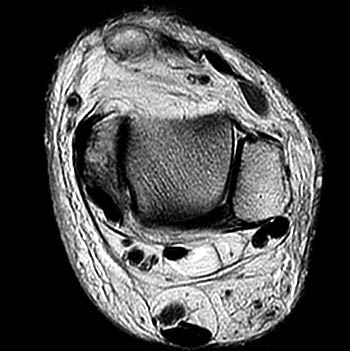
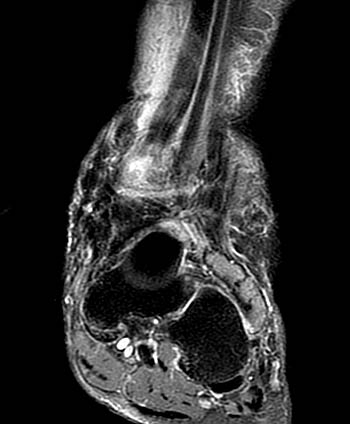
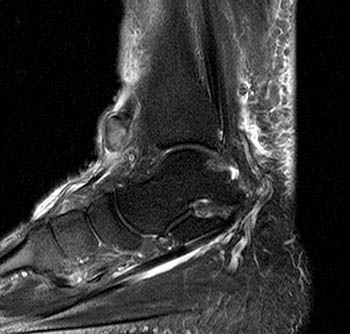
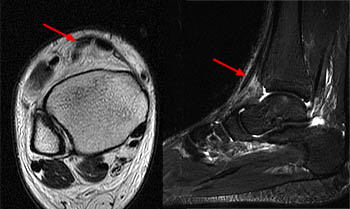
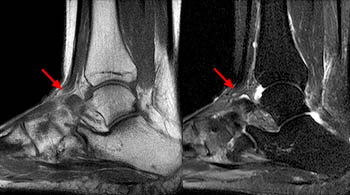
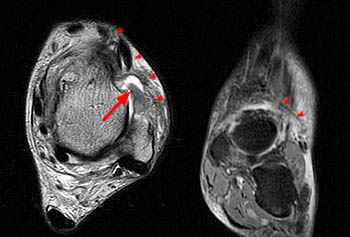
Clinical History: A 62 year-old woman fell while descending the steps from her front porch. She presents to the orthopaedist 3 weeks later, reporting weakness of the left foot and a palpable mass over the anterior left ankle. MRI of the ankle was obtained with axial fast spin-echo T2-weighted (1a), coronal fat suppressed proton density-weighted (1b), and sagittal fat suppressed fast spin-echo T2-weighted images (1c). What are the findings? What is your diagnosis?
Findings
Figure 2:
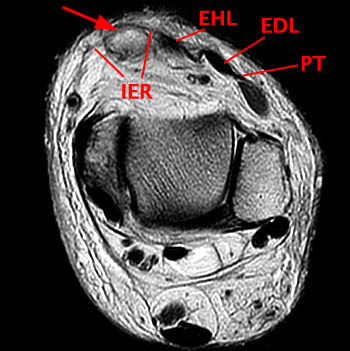
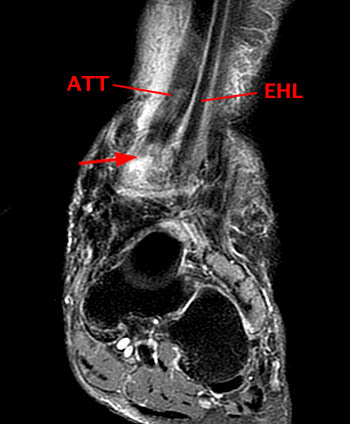
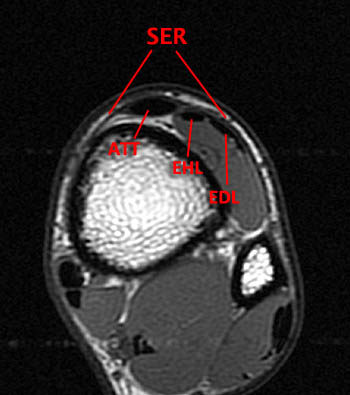
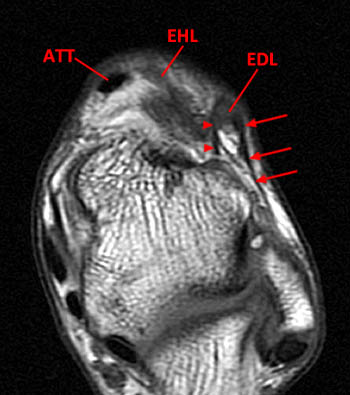
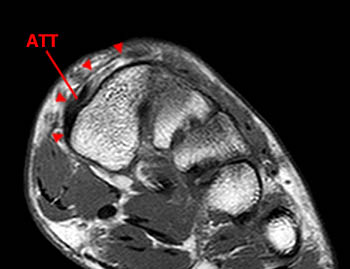
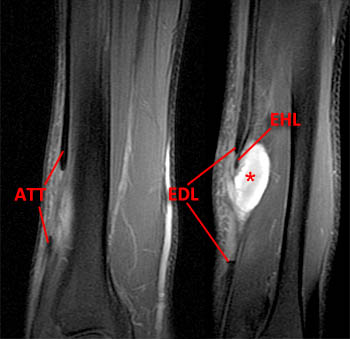
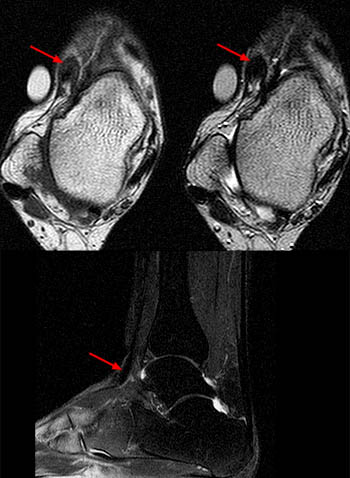
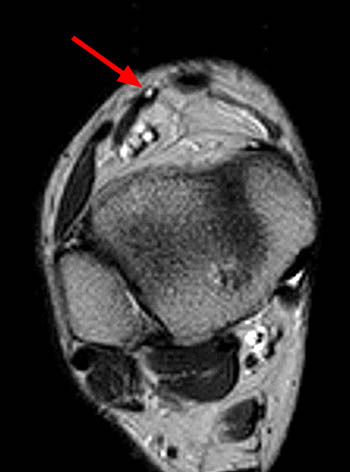
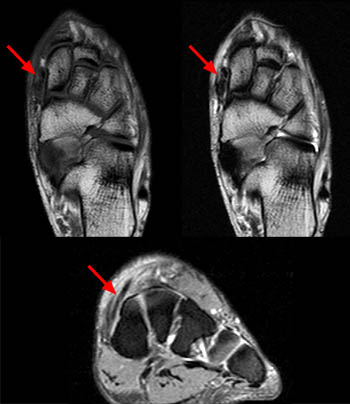
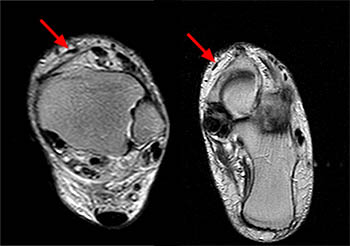
(2a)The axial fast spin-echo T2-weighted image was obtained just below the tibial plafond. At this level, the anterior tibial tendon (ATT) is normally seen in cross section as a black oval structure anterior to the joint. On this image, the tendon sheath of the ATT is distended with T2-hyperintense material (arrow), but the tendon is not visible. The extensor hallucis longus (EHL), extensor digitorum longus (EDL), and peroneus tertius tendons (PT) are visible anteriorly. A portion of the oblique superomedial limb of the inferior extensor retinaculum (IER) is visible on either side of the empty ATT sheath.
Figure 4:
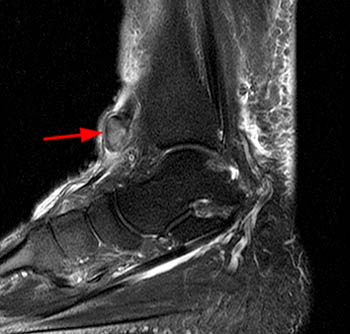
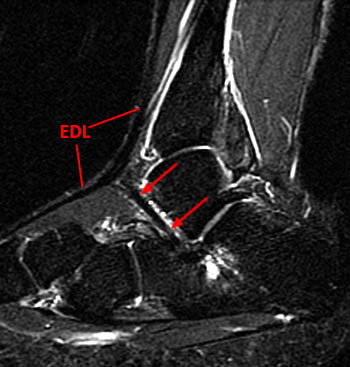
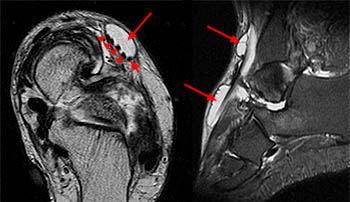
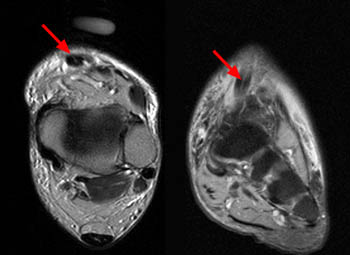
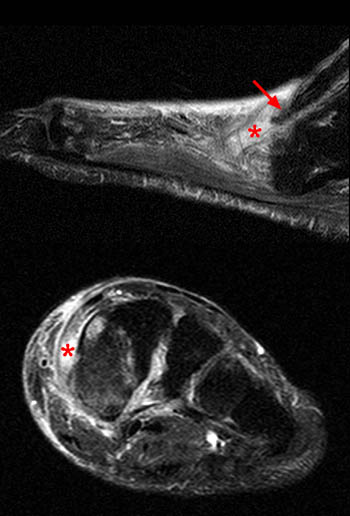
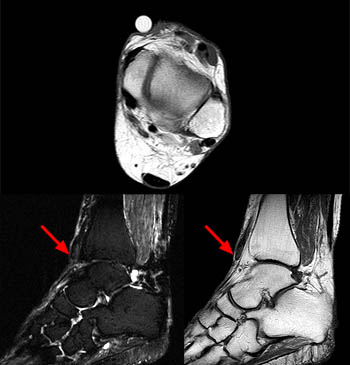
(4a) The sagittal fat suppressed fast spin-echo T2-weighted image visualizes the retracted torn ATT just anterior to the medial distal tibia (arrow), corresponding to the palpable mass on physical examination. The torn end of the tendon displays a thickened bulbous morphology, with increased intrasubstance signal.
Diagnosis: Complete rupture of the anterior tibial tendon.
Introduction
Most ruptures of the anterior tibial tendon occur in patients over the age of 50, with a male preponderance. Patients often present with gait abnormality and foot drop. On physical examination, a palpable mass may be present over the anterior ankle corresponding to the retracted tendon, with no palpable tendon distal to the mass. Initial symptoms are often mild, which can result in delayed presentation and missed diagnoses.1,2,3
Ankle extensor tendon disorders are less commonly reported in the medical literature than other ankle tendon pathology. The incidence of extensor tendon abnormalities is uncertain. Complete rupture of the anterior tibial tendon is described as “rare” by some authors1,4, but also has been reported as the third most common tendon rupture in the lower extremity, behind Achilles and patellar tendon tears.5
Review of Radsource cases over the past 10 years utilizing keyword database search found 31 cases of complete anterior tibial tendon rupture, and a total of 447 cases of ankle extensor tendinopathy (342 involving the anterior tibial tendon, 67 involving the extensor hallucis longus, and 38 involving the extensor digitorum longus or peroneus tertius). Most of these patients had additional coexisting ankle or hindfoot pathology.
Anatomy
Dorsiflexion of the foot is normally produced by three muscles and tendons which cross the tibiotalar joint anteriorly; from medial to lateral, these are the tibialis anterior, or anterior tibial tendon (ATT); extensor hallucis longus (EHL); and extensor digitorum longus (EDL). Most humans also possess a fourth small muscle lateral to these, the peroneus tertius (PT). (The mnemonic “Tom Hates Dick Passionately” may be useful to remember the usual tendon order at the level of the tibiotalar joint.) All four of these muscles are innervated by the deep peroneal nerve, and all four tendons normally possess synovial tendon sheaths. The muscles and tendons pass under the superior extensor retinaculum above the tibiotalar joint, and the inferior extensor retinaculum at and below the tibiotalar joint6,7 (see Figure 5a).
Figure 5:
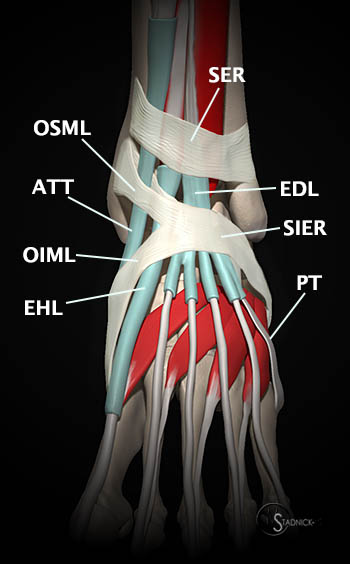
(5a) This 3D representation of the extensor retinacular anatomy demonstrates the superior extensor retinaculum (SER) and the inferior extensor retinaculum including the stem of the inferior extensor retinaculum (SIER), the oblique superomedial limb (OSML), and the oblique inferomedial limb (OIML). The extensor retinaculum acts as a pulley, stabilizing the anterior tibial (ATT), extensor hallucis longus (EHL), extensor digitorum longus (EDL), and the peroneus tertius (PT) tendons.
The tibialis anterior is the major extensor of the ankle, estimated to provide 80% of dorsiflexion strength. The muscle originates from the lateral tibia and interosseous membrane, inserting on the base of the first metatarsal and medial first cuneiform. Occasionally, the distal tendon may insert only on the cuneiform.1
The extensor hallucis longus originates from the mid fibula and interosseous membrane, inserting at the base of the distal phalanx of the great toe.
The extensor digitorum longus originates from the anterior fibula and interosseous membrane. The common tendon divides (usually under the extensor retinacula) into four separate tendons, inserting on the phalanges of the second through fifth toes.
The peroneus tertius is present in 83% to 95% of the population.8,9 It originates from the distal fibula and interosseous membrane, inserting distally on the base of the fifth metatarsal. The peroneus tertius shares a common tendon sheath with the extensor digitorum longus.
The extensor retinacula act as pulleys for the extensor tendons and restrain their motion over the anterior aspect of the ankle and foot. The superior extensor retinaculum is a fibrous band of tissue extending transversely above the tibiotalar joint, attaching to the lateral malleolus and lateral crest of the distal fibula laterally, and to the medial malleolus and anterior tibia medially. It is continuous with the flexor retinaculum medially and superior peroneal retinaculum laterally.6
The inferior extensor retinaculum has a more complex morphology, resembling a sideways letter “Y” over the anterior tibotalar joint and dorsal midfoot. The “stem” portion is lateral, with 3 roots (medial, intermediary, and lateral) originating from the calcaneus and sinus tarsi, coursing over the EDL and peroneus tertius tendons. Medially, the stem bifurcates into the oblique superomedial limb and oblique inferomedial limb. The oblique superomedial limb attaches to the anterior aspect of the medial malleolus. The oblique inferomedial limb courses inferiorly to the medial foot at the cuneonavicular joint. In 25% of the population, a third oblique superolateral limb is also present, extending superiorly from the stem.6
Figure 6:
(6a) Superior extensor retinaculum. An axial T1-weighted image acquired approximately 2.5 cm above the talar dome shows the superior extensor retinaculum (SER) as a thin low signal band just anterior to the extensor tendons and muscles.
(6b) Oblique superomedial limb of inferior extensor retinaculum. Axial T1-weighted image obtained through the tibial plafond, just above the tibiotalar joint shows a thin dark linear structure extending transversely just anterior to the EHL and EDL, consistent with the oblique superomedial limb of the inferior extensor retinaculum (arrows). In the region of the ATT, the retinaculum splits into superficial and deep layers (arrowheads), encasing the ATT and its tendon sheath in a fibrous tunnel. The deep layer is usually relatively thick compared to the superficial layer, as in this example.
(6c) Roots of the inferior extensor retinaculum. Axial T1-weighted image acquired 1.8 cm inferior to the talar dome shows two of the three roots of the inferior extensor retinaculum just medial (arrowheads) and lateral (arrows) to the EDL, forming a sling-like structure which restrains motion of the EDL. The medial band-like structure is the intermediary root. The lateral structure is the lateral root.
Figure 7:
(7a) Intermediary root of the inferior extensor retinaculum. Sagittal STIR image of the ankle visualizes the EDL curving over the anterior ankle. The dark band of tissue extending superiorly and anteriorly toward the tendon from the sinus tarsi is the intermediary root of the inferior extensor retinaculum.
Figure 8:
(8a) Oblique inferomedial limb of the inferior extensor retinaculum. Coronal T1-weighted image of the midfoot through the distal medial cuneiform shows the distal ATT near its insertion. The thin dark band of tissue extending transversely superficial to the tendon is the oblique inferomedial limb of the inferior extensor retinaculum. The ATT insertion is usually located several centimeters anterior to the ankle and may be difficult to visualize on a standard ankle MRI protocol; additional images of the midfoot may be useful if insertional ATT disease is suspected.
Technical Considerations in Ankle MR Imaging
Obtaining high quality MR imaging of the ankle presents a number of specific challenges. A limited field of view (usually 16 cm or less) is needed to achieve diagnostic spatial resolution. Neutral angulation of the foot is best accommodated by a dedicated coil, such as an extremity coil with a “chimney” to maximize patient comfort and minimize motion artifact. Uniform fat suppression is highly desirable, and also best achieved with a dedicated extremity coil designed for ankle imaging. Placing the entire foot in a quadrature head coil can be used to obtain relatively uniform fat suppression, but may result in a lower signal-to-noise ratio.10,11
Multiplanar imaging in the sagittal, axial and coronal planes should be routinely obtained. The tendons change directions as they cross the ankle, and need to be examined in all 3 planes.11 Tendon curvature can result in artifactual signal within ankle tendons due to “magic angle effect”; this phenomenon occurs when collagen fibers are oriented at 54.74 degrees relative to the main magnetic field of the MRI scanner. Collagenous structures such as tendons and ligaments are normally hypointense on MR imaging due to internuclear dipole interactions, which result in lower signal from protons bound to collagen. When the collagen fibers are oriented at 54.74 degrees relative to the main magnetic field of the MR scanner, these dipole interactions are reduced, resulting in relative increased signal on short TE sequences.12 This can mimic tendinosis on T1- and proton density-weighted images.11,12
Longer TE images demonstrate less magic angle effect. Reduction of magic angle artifact can also be accomplished by positioning the foot in plantar flexion (thereby reducing curvature of the tendons), or using STIR sequences. The anterior tibial tendon is the least affected of all ankle tendons by the magic angle effect, probably due to its relatively straight course.11,13,14
Tendon Pathology and MR Imaging
A number of systemic diseases are associated with tendon disease. Ochronosis, Ehlers-Danlos syndrome, and Marfan syndrome are hereditary disorders which can manifest tendon abnormalities. Amyloidosis, gout, hydroxyapatite deposition or hyperlipidemia can result in deposition disease within or adjacent to tendons. Inflammatory diseases such as lupus, rheumatoid arthritis, seronegative spondyloarthropathies and sarcoidosis can cause tendon and tenosynovial inflammation, frequently multifocal and bilateral.15,16 (Case 9a)
Systemic corticosteroids and corticosteroids injected into tendon sheaths are associated with tendon ruptures.1,2 Quinolone antibiotics such as ciprofloxacin are associated with tendon disorders at a rate of 15 to 20 per 100,000 patients treated, most often involving the Achilles tendon.17 Direct trauma, foreign bodies, fractures or penetrating injuries can cause tendon tears.15,18 (Case 10a)
All of the above etiologies together account for less than 10% of tendon ruptures.15 Laceration and violent force can cause acute tendon tear in a normal tendon, but this is rather uncommon. The vast majority of tendon ruptures occur spontaneously or after modest trauma in chronically degenerated tendons; this has been called “acute-on-chronic” tendon rupture in the literature.1,2,3,5,15
Figure 9:
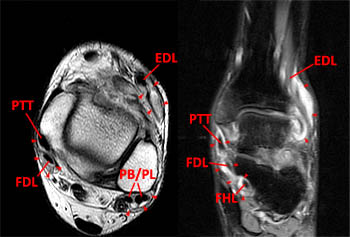
(9a) Rheumatoid arthritis in a 33 year-old male with chronic ankle pain. The axial fast spin-echo T2-weighted image (left) and coronal fat saturated proton density-weighted image (right) show T2-hyperintense signal and intermediate signal debris (arrowheads) in the tendon sheaths of the EDL and peroneus tertius, posterior tibial tendon (PTT), flexor digitorum longus (FDL), flexor hallucis longus (FHL), and peroneal tendons (PB/PL).
Figure 10:
(10a) Complete transection of ankle extensor tendons due to anterior leg laceration in a 17 year-old male. Sagittal fat saturated proton density-weighted images demonstrate complete discontinuity of the tibialis anterior (left), extensor hallucis longus and extensor digitorum longus (right). A well-defined gap separates the proximal and distal tendon fragments. A hematoma (asterisk) is located deep to the EHL and EDL tendons.
Degenerative tendinopathy can be broadly divided into four categories: tenosynovitis (or peritendinitis), tendinosis, partial tear, and complete tear (rupture). Each of these has characteristic MR imaging findings, and may coexist in the same tendon.11,19
Tenosynovitis (Cases 11a-13a) refers to inflammation of the synovial tendon sheath. This is most frequently visualized on MRI as T2-hyperintense signal close to fluid intensity surrounding the tendon, distending the tendon sheath. The tendon sheath may contain heterogeneous mixed signal material due to thickened synovium and debris; this finding should raise concern for infection or systemic inflammatory arthropathy. In chronic cases, the T2-hyperintense component may be diminished with residual intermediate to low signal fibrosis in the tendon sheath.7,11
Figure 11:
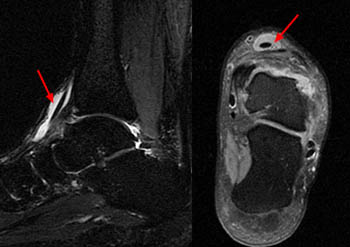
(11a) Tenosynovitis of the anterior tibial tendon in a 44 year-old male. The patient presented with a palpable mass and mild tenderness over the anterior ankle. Sagittal fat saturated T2-weighted (left) and axial fat saturated proton density-weighted (right) images demonstrate fluid-intensity signal surrounding the ATT, distending the tendon sheath.
Figure 12:
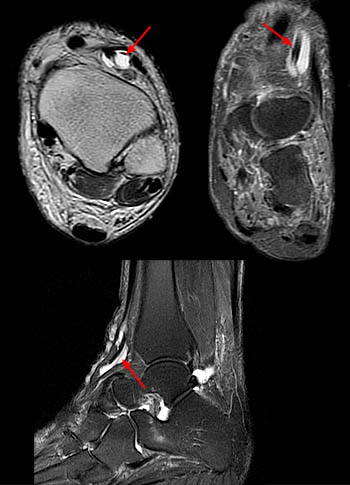
(12a) Tenosynovitis of the extensor hallucis longus. A 77 year-old female patient reported difficulty walking and anterior ankle pain. Axial fast spin echo T2-weighted (left), coronal fat saturated proton density-weighted (right) and sagittal fat saturated proton density-weighted (bottom) images show fluid signal and a mesotendon in the extensor hallucis longus tendon sheath.
Figure 13:
(13a) Tenosynovitis of the extensor digitorum longus and peroneus tertius in a 73 year-old male with anterior ankle pain. Axial fast spin echo T2-weighted (left) and sagittal fat saturated proton density-weighted (right) images show prominent distention of the shared tendon sheath of the EDL and PT (arrows). Fluid in the tendon sheath delineates the five separate tendons of the EDL and PT on the axial image; the most lateral tendon is the PT (short arrow), and the four medial tendons of the EDL (arrowheads) insert on the second through fifth toes.
Tendinosis (Cases 14a-16a) indicates deposition of fibrous tissue and degeneration within the tendon substance, thought to be due to chronic microtrauma which exceeds the reparative ability of the tendon. Predisposing factors include age, decreased vascularity, overuse, and a sudden increase in activity levels.15 On MR imaging, tendinosis can manifest as tendon thickening without abnormal signal, or increased intrasubstance signal on short TE (T1-weighted or proton density-weighted) sequences with little or no abnormality on T2-weighted imaging. In the anterior tibial tendon, a short axis diameter greater than 5 mm within 3 cm of the distal insertion has been reported to have a sensitivity of 94% and specificity of 98% for tendinosis.11,20,21
Figure 14:
(14a) Tendinosis of the anterior tibial tendon. A 74 year-old male reported left ankle pain and swelling. Axial T1-weighted (left) and fast spin echo T2-weighted (right) images through the navicular and distal anterior tibial tendon demonstrate thickening of the tendon (arrows), measuring 8 mm in short axis. A coronal fat saturated fast spin echo proton density-weighted image (bottom) shows the diffuse thickening extending to the distal insertion on the medial first cuneiform. The tendon remains normal in signal on all imaging sequences.
Figure 15:
(15a) Tendinosis of the extensor hallucis longus. A 17 year-old male basketball player reports anterior right ankle pain. Axial fast spin echo T2-weighted (left) and sagittal fat saturated fast spin echo T2-weighted (right) images show focal thickening of the extensor hallucis longus over the anterior tibiotalar joint (arrows), with mild surrounding peritendinous edema.
Figure 16:
(16a) Tendinosis of the extensor digitorum longus. A 40 year-old female presented with a palpable anterior ankle mass. Axial T1-weighted (left) and fast spin echo T2-weighted (right) images through a skin marker placed on the palpable abnormality reveal focal thickening of the extensor digitorum longus tendon (arrows), with mild increased signal in the tendon on the T1-weighted image. A sagittal fat saturated T2-weighted image (bottom) also shows the area of focal thickening, without increased intrasubstance signal.
Partial tendon tears (Cases 17a-20a) may be visualized on MRI as intrasubstance signal abnormality on T2-weighted images, abnormal tendon diameter, or both. Acute partial tears can be associated with edema and increased tendon diameter. Partial tears can extend longitudinally along the long axis of the tendon, sometimes splitting the tendon into separate fiber bundles. Partial tears can also result in decreased diameter of the remaining tendon as the torn fibers become retracted and scarred. As edema and fluid in the partial tear decreases over time, tendon signal can normalize; these tears may only be identifiable by decreased tendon diameter.20,21,22
Figure 17:
(17a) Partial longitudinal tear of the anterior tibial tendon in a 74 year-old female with anterior left ankle pain. Axial fast spin echo T2-weighted (left) and coronal fat saturated fast spin echo proton density-weighted (right) images show an abnormal T2-hyperintense cleft extending longitudinally in the tendon.
Figure 19:
(19a) Partial tear of the distal anterior tibial tendon in a 39 year-old male with anterior ankle and medial foot pain. Axial T1-weighted (left) and fast spin echo T2-weighted (right) images through the medial cuneiform reveal thinning of the tendon, increased intrasubstance signal on the T2-weighted image, and splitting of the tendon (arrows). A coronal fat saturated fast spin echo proton density-weighted image (bottom) also demonstrates thinning, increased intrasubstance signal and adjacent peritendinous edema (arrow).
Figure 20:
(20a) Chronic partial tear of the anterior tibial tendon in an 80 year-old female. Axial fast spin echo T2-weighted images acquired just above the tibiotalar joint (left) and at the talonavicular joint (right) demonstrate that the ATT is severely decreased in cross sectional diameter, appearing smaller than the EHL throughout the ankle. No internal signal abnormality, adjacent edema or fluid in the tendon sheath.
Complete tear or rupture of a tendon (Cases 21a-23a) results in a visible defect between the proximal and distal fragments of the tendon. The gap is often occupied by fluid or hemorrhage in acute cases. In chronic tears, fluid and edema around the tendon defect decreases and the tear may become less conspicuous. A detailed description of the rupture location, size of the defect, and quality of the remaining tendon tissue in the MRI report is useful for treatment planning. Most anterior tibial tendon ruptures occur within 3 cm of the distal insertion, possibly due to relatively decreased vascularity in this region.1,3,6,21
Figure 21:
(21a) Acute rupture of the distal anterior tibial tendon at the insertion on the medial cuneiform and base of first metatarsal. A 58 year-old female suffered foot and ankle injury in a motor vehicle accident four days prior to MRI. Sagittal (top) and coronal (bottom) fat saturated fast spin echo proton density-weighted images reveal discontinuity and retraction of the anterior tibial tendon (arrow) from its distal insertion. Fluid is present in the empty distal tendon sheath (asterisks), with adjacent soft tissue edema.
Figure 22:
(22a) Chronic anterior tibial tendon rupture in an 87 year-old female with a previous history of anterior tibial tendinosis. Axial T1-weighted (top) image at the top of the talar dome demonstrates absence of the ATT deep to the skin marker. Sagittal STIR (left) and T1-weighted (right) images reveal complete discontinuity and retraction of the anterior tibial tendon (arrows), but no significant fluid in the tendon defect or tendon sheath.
Figure 23:
(23a) Chronic rupture of the extensor hallucis longus in a 43 year-old female with anterior pain and inability to extend the great toe. Sagittal T1-weighted (left) and fat saturated fast spin echo proton density-weighted images (right) show abrupt termination of the EHL over the anterior talus (arrows), without associated edema or fluid.
Extensor retinaculum injury is uncommon, and can be traumatic or postsurgical. Disruption of the retinaculum can result in bowstringing or dislocation of the extensor tendons. Sprain of the retinaculum can result in pain and fibrosis around the retinaculum.6,23,24,25
Figure 24:
(24a) Acute sprain of the inferior extensor retinaculum. A 50 year old female sprained her left ankle, tearing the anterior talofibular ligament (ATFL). Axial fast spin echo T2-weighted (left) and coronal fat saturated fast spin echo proton density-weighted images (right) obtained one week after the injury reveals thickening and increased signal in the stem and lateral root of the inferior extensor retinaculum (arrowheads), with adjacent edema. The ATFL tear is visible posterior to the extensor retinaculum on the axial image (arrow).
Treatment
Conservative treatment is indicated for less severe cases of extensor tendinopathy, and may include rest, bracing or immobilizing the ankle, modification of footwear, and physical therapy. Systemic nonsteroidal anti-inflammatory medication may be useful if an inflammatory component is suspected. Local injection of steroids in the tendon sheath can reduce symptoms, but may predispose the patient to tendon rupture and should be utilized with caution. Arthroscopic debridement can be performed in refractory cases of tenosynovitis which are unresponsive to noninvasive therapy.1,2,24,26
Complete rupture of the anterior tibial tendon can result in a substantial functional deficit, since this tendon provides 80% of dorsiflexion strength. Surgical repair of ruptured tendons can be performed with direct primary repair if the tendon fragments can be approximated, or with interpositional graft or tendon transfer if necessary. Early diagnosis facilitates primary surgical repair and results in a lower postoperative complication rate. Some dorsiflexion deficit remains in most patients after anterior tibial tendon repair. Younger patients and those with active lifestyles benefit to a greater extent from early repair, but surgery has been shown to significantly improve function in patients with both acute and chronic ATT ruptures.1,2,27,28,29
Conclusion
Extensor tendon pathology at the ankle joint is less frequently reported in the medical literature than diseases of other ankle tendons, but is not uncommon in clinical practice. Review of the Radsource experience revealed 447 cases over the past 10 years, including 31 cases of complete rupture of the anterior tibial tendon. MRI is a sensitive and accurate imaging modality for evaluation of the ankle tendons, and can be particularly useful when multiple disease entities coexist or physical examination is equivocal.
References
1 Anagnostakos K, Bachelier F, Fürst OA, Kelm J. Rupture of the anterior tibial tendon: three clinical cases, anatomical study, and literature review. Foot Ankle Int 2006;27(5):330-339.
2 Gwynne-Jones D, Garneti N, Wyatt M. Closed tibialis anterior tendon rupture: a case series. Foot Ankle Int 2009;30(8):758-762.
3 Gallo RA, Kolman BH, Daffner RH, Sciulli RL, Roberts CC, DeMeo PJ. MRI of tibialis anterior tendon rupture. Skeletal Radiol. 2004 Feb;33(2):102-6.
4 Dunfee WR, Dalinka MK, Kneeland JB. Imaging of athletic injuries to the ankle and foot. Radiol Clin North Am. 2002 Mar;40(2):289-312, vii.
5 Jozsa L, Kannus P. Spontaneous rupture of tendons. In: Human tendons: anatomy, physiology and pathology. Champaign, Ill: Human Kinetics Publishers, 1997; 254-325.
6 Lee MH, Chung CB, Cho JH, et al. Tibialis anterior tendon and extensor retinaculum: imaging in cadavers and patients with tendon tear. AJR Am J Roentgenol 2006;187(2):W161-W168.
7 Ng JM, Rosenberg ZS, Bencardino JT, Restrepo-Velez Z, Ciavarra GA, Adler RS. US and MR imaging of the extensor compartment of the ankle. Radiographics. 2013 Nov-Dec;33(7):2047-64.
8 Cheung YY, Rosenberg ZS. MR imaging of accessory muscles around the ankle. MRI Clinics of North America 2001; 9(3):465-473.
9 Sookur PA, Naraghi AM, Bleakney RR, Jalan R, Chan O, White LM. Accessory muscles: anatomy, symptoms, and radiologic evaluation. Radiographics 2008; 28:481-499.
10 Moshirfar A, Campbell JT, Khanna AJ, Byank RP, Bluemke DA, Wenz JF Sr. Magnetic resonance imaging of the ankle: techniques and spectrum of disease. J Bone Joint Surg Am. 2003;85-A Suppl 4:7-19.
11 Sadro C, Dalinka M. Magnetic Resonance Imaging of the Tendons of the Ankle and Foot. University of Pennsylvania Orthopaedic Journal 2000;13:1-9.
12 Erickson SJ, Cox IH, Hyde JS, Carrera GF, Strandt JA, Estkowski LD. Effect of tendon orientation on MR imaging signal intensity: a manifestation of the “magic angle” phenomenon. Radiology 1991;181(2):389-392.
13 Mengiardi B, Pfirrmann CW, Schöttle PB, Bode B, Hodler J, Vienne P, Zanetti M. Magic angle effect in MR imaging of ankle tendons: influence of foot positioning on prevalence and site in asymptomatic subjects and cadaveric tendons. Eur Radiol. 2006 Oct;16(10):2197-206.
14 Srikhum W, Nardo L, Karampinos DC, Melkus G, Poulos T, Steinbach LS, Link TM. Magnetic resonance imaging of ankle tendon pathology: benefits of additional axial short-tau inversion recovery imaging to reduce magic angle effects. Skeletal Radiol. 2013 Apr;42(4):499-510.
15 Järvinen M, Józsa L, Kannus P, Järvinen TL, Kvist M, Leadbetter W. Histopathological findings in chronic tendon disorders. Scand J Med Sci Sports. 1997 Apr;7(2):86-95.
16 Aydingöz U, Aydingöz O. Spontaneous rupture of the tibialis anterior tendon in a patient with psoriasis. Clin Imaging. 2002 May-Jun;26(3):209-11.
17 Lewis T, Cook J. Fluoroquinolones and Tendinopathy: A Guide for Athletes and Sports Clinicians and a Systematic Review of the Literature. J Athl Train. 2014 Apr 24.
18 Ebrahimi FV, Tofighi M, Khatibi H. Closed tibial fracture associated with laceration of tibialis anterior tendon. J Foot Ankle Surg 2010;49(1):e19-e22.
19 Hodgson RJ, O’Connor PJ, Grainger AJ. Tendon and ligament imaging. Br J Radiol. 2012 Aug;85(1016):1157-72.
20 Beischer AD, Beamond BM, Jowett AJ, O’Sullivan R. Distal tendinosis of the tibialis anterior tendon. Foot Ankle Int 2009;30(11):1053-1059.
21 Mengiardi B, Pfirrmann CW, Vienne P, et al. Anterior tibial tendon abnormalities: MR imaging findings. Radiology 2005;235(3):977-984.
22 Saadeh K, Susan Ackerman S. Partial Tear of the Anterior Tibialis Tendon. Appl Radiol. 2007;36(3):38-41.
23 Demondion X, Canella C, Moraux A, Cohen M, Bry R, Cotten A. Retinacular disorders of the ankle and foot. Semin Musculoskelet Radiol. 2010 Sep;14(3):281-91.
24 Maquirriain J, Sammartino M, Ghisi JP, Mazzuco J. Tibialis anterior tenosynovitis: Avoiding extensor retinaculum damage during endoscopic debridement. Arthroscopy. 2003 Feb;19(2):E9.
25 Akhtar M, Levine J. Dislocation of extensor digitorum longus tendons after spontaneous rupture of the inferior retinaculum of the ankle. Case report. J Bone Joint Surg Am. 1980 Oct;62(7):1210-1.
26 Markarian GG, Kelikian AS, Brage M, Trainor T, Dias L. Anterior tibialis tendon ruptures: an outcome analysis of operative versus nonoperative treatment. Foot Ankle Int 1998;19(12):792-802.
27 Kopp FJ, Backus S, Deland JT, O’Malley MJ. Anterior tibial tendon rupture: results of operative treatment. Foot Ankle Int. 2007 Oct;28(10):1045-7.
28 Sammarco VJ, Sammarco GJ, Henning C, Chaim S. Surgical repair of acute and chronic tibialis anterior tendon ruptures. J Bone Joint Surg Am. 2009 Feb;91(2):325-32.
29 Mann’s Surgery of the Foot and Ankle by Michael J. Coughlin, Charles L. Saltzman, and Robert B. Anderson, 9th edition published by Elsevier, chapter 24.