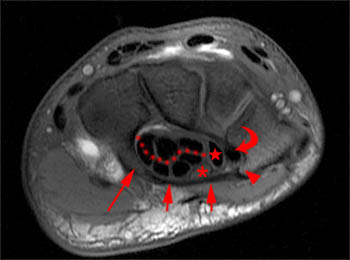
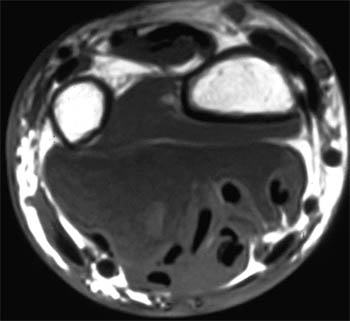
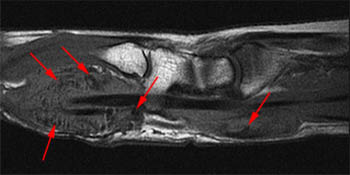
Clinical History: A 55-year-old man developed slowly progressive swelling of the right hand and wrist over the previous several months. Fat-suppressed T2-weighted axial image just proximal to the wrist (1a) and fat-suppressed T1-weighted post-contrast axial images at the levels of the metacarpal shafts (1b) and metacarpal heads (1c) are provided. What are the findings? What is the differential diagnosis?
Findings
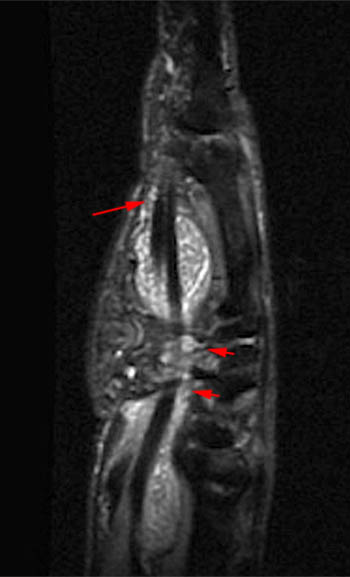
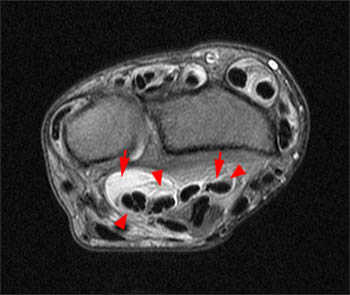
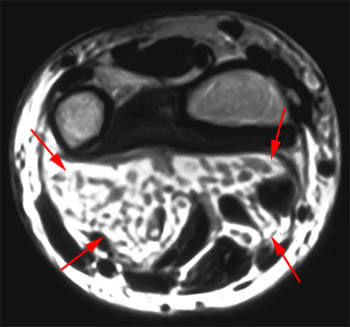
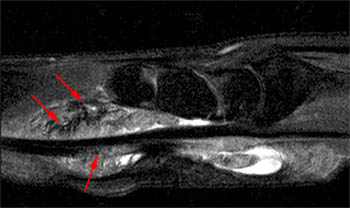
Figure 2:
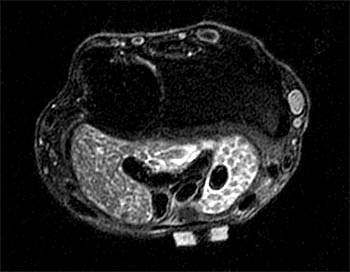
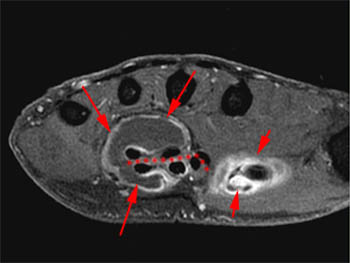
A fat-suppressed T2-weighted axial image at the level of the distal forearm reveals distension of the palmar bursae by complex material consisting of numerous low signal foci against a background of fluid signal intensity. The smaller radial bursa (short arrows) surrounds the flexor pollicis longus tendon (star). The larger ulnar bursa (long arrows) envelops the flexor digitorum superficialis and profundus tendons (dotted line). The flexor carpi radialis (asterisk) and flexor carpi ulnaris (arrowhead) tendons are extra-bursal in location.
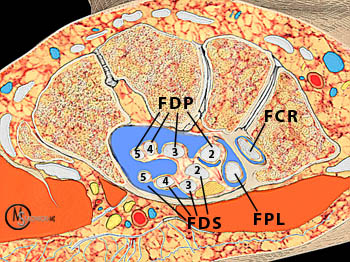
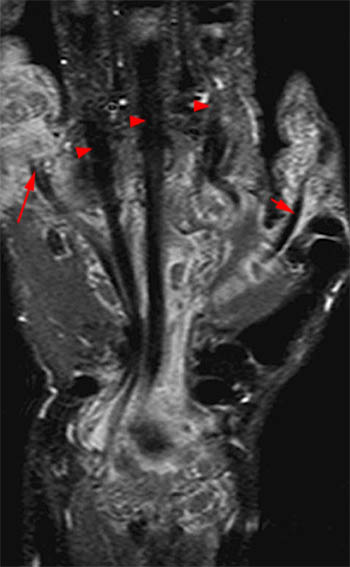
Figure 3:
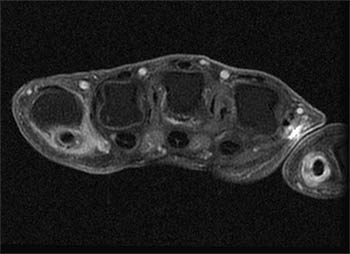
A fat-suppressed T1-weighted post-contrast axial image at the level of the metacarpal shafts reveals avid synovial enhancement of the ulnar (long arrows) and radial (short arrows) bursae. Note that the low signal foci seen in (A) do not enhance. Observe the two-tiered arrangement of the flexor digitorum profundus tendons (above dotted line) and flexor digitorum superficialis tendons (below dotted line).
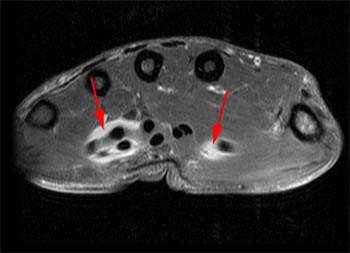
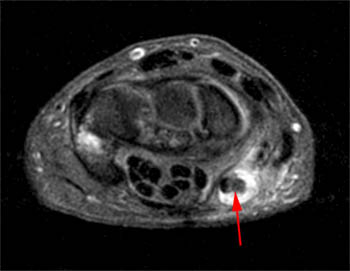
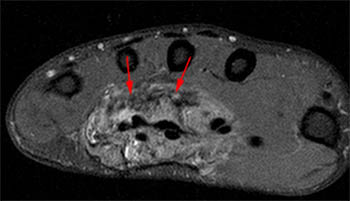
Figure 4:
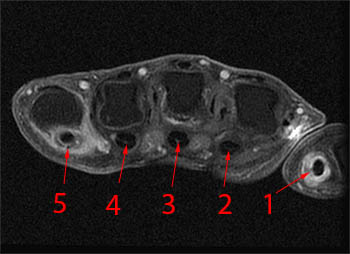
A fat-suppressed T1-weighted post-contrast axial image at the level of the metacarpal heads showing extension of synovitis into the digital flexor tendon sheaths of the thumb (1) and little finger (5). There is no involvement of the flexor tendon sheaths of the index, long, and ring fingers (2, 3, 4).
Diagnosis
Classic ‘horseshoe abscess’ (in this case, related to atypical mycobacteria) that has spread through communicating synovial pathways, which include the ulnar and radial bursae proximally and the flexor tendon sheaths of the thumb and little finger distally. The differential diagnosis will be discussed in subsequent sections.
A variety of infectious and noninfectious diseases involve the synovial sheaths of the hand and wrist. On the flexor side, these synovial sheaths consist of the two palmar bursae-the ulnar bursa and the radial bursa-and the digital flexor tendon sheaths. To properly characterize such diseases, the radiologist should be familiar with the relevant anatomy and its implications on patterns of disease progression.
Anatomy
Flexor Tendons of the Wrist
In contrast to the extensor tendons of the wrist, which are segregated into six extensor compartments, the flexor tendons observe a simpler organizational scheme. Of the 12 flexor tendons normally found at the level of the wrist, only three do not traverse the carpal tunnel: (1) the palmaris longus tendon, superficial to the tunnel; (2) the flexor carpi radialis tendon, radial to the tunnel; and (3) the flexor carpi ulnaris tendon, on the ulnar side of the tunnel. The other nine flexor tendons pass through the carpal tunnel, a fibro-osseous tunnel defined by the carpal bones dorsally and the flexor retinaculum volarly. In the axial plane, the carpus forms an arch that is concave on the palmar side.
Figure 5:
A fat-suppressed T1-weighted axial image from an MR arthrogram of the wrist in a healthy 24-year-old man. The transverse carpal ligament (short arrows) extends from the hook of the hamate (long arrow) to the tubercle of the trapezium (arrowhead), forming the floor of the carpal tunnel. At the radial aspect of the carpal tunnel, the flexor digitorum tendons are arranged in two rows (separated by dotted line), the profundus tendons deep to the superficialis tendons. The flexor pollicis longus tendon (star) is positioned at the radial aspect of the tunnel, separated from the flexor carpi radialis tendon (curved arrow) by a ligamentous reflection of the transverse carpal ligament. The median nerve is indicated (asterisk).
This arch forms the dorsal margin of the carpal tunnel demarcated by four bony prominences: the pisiform and scaphoid tubercle proximally and the hook of the hamate and tubercle of the trapezium distally1. Tendons passing through the carpal tunnel are secured in place by the flexor retinaculum, which forms the volar margin of the carpal tunnel. The flexor retinaculum, which is generally considered synonymous with the transverse carpal ligament, extends in a proximal to distal direction from the distal radius to the base of the third metacarpal and attaches to the four bony prominences mentioned above. The flexor retinaculum thickens at the level of its attachments to the hamate and trapezium, which is also where the carpal tunnel is narrowest. The transverse diameter of the carpal tunnel averages 2 cm at this level, expanding to 2.5 cm at both its proximal and distal margins1. On MRI, this ‘hourglass’ configuration is depicted on coronal images through the carpal tunnel, becoming more conspicuous in the presence of bursitis (6a).
The nine flexor tendons traversing the carpal tunnel consist of the flexor pollicis longus (FPL) tendon to the thumb along with four pairs of flexor digitorum tendons serving the index (FD2), long (FD3), ring (FD4), and little fingers (FD5), each pair consisting of a superficialis tendon and a profundus tendon. (Although the superficialis and profundus tendons originate from separate superficialis and profundus muscles in the forearm, the abbreviation ‘FD’ will be used for brevity to refer to both tendons as a pair, unless otherwise specified). The flexor digitorum superficialis and profundus tendons-inserting respectively on the middle and distal phalanges-are located at the ulnar aspect of the canal and arranged in two rows, the profundus tendons dorsal to the superficialis tendons. On axial images through the carpal tunnel, the four superficialis tendons often show a U-shaped configuration with the superficialis tendons of FD3 and FD4 volar to the superficialis tendons of FD2 and FD5 (5a). The median nerve occupies a superficial position within the carpal tunnel, located just deep to the flexor retinaculum.
Palmar Bursae and Tendon Sheaths
The term ‘tendon sheath’ is broadly used to describe histologically distinct tissues. The classic two-layered tendon sheath is only found in certain tendons in locations of mechanical stress. The two layers consist of an outer fibrous sheath and an inner synovial sheath. The synovial sheath is composed of two sheets of synovial cells-a visceral sheet applied to the surface of the tendon and a parietal sheet applied to the inner aspect of the surrounding fibrous sheath-separated by a capillary layer of synovial fluid2,3.
Synovial tendon sheaths and bursae are fluid-filled sacs lined by a synovial membrane, acting to decrease friction between adjacent structures, allowing smooth, gliding movement. They are located throughout the body in locations where tendons are closely apposed to bones and rigid fibrous structures. The flexor tendons of the carpal tunnel are enveloped in two palmar bursae: the ulnar bursa and the radial bursa. The ulnar and radial bursae begin proximal to the carpal tunnel, usually near the distal margin of the pronator quadratus muscle, and they extend distally to the level of the mid-palm, allowing for longitudinal excursion of the tendons during normal wrist movement3. These bursae extend over a longer distance than the extensor tendon sheaths, a difference likely related to the greater range of wrist motion that takes place in flexion compared with extension4.
The smaller radial bursa surrounds the flexor pollicis longus tendon. The larger ulnar bursa surrounds the eight flexor digitorum tendons, doing so by means of three invaginations: a deep invagination between the carpal bones and the profundus tendons, a middle invagination between the profundus and superficialis tendons, and a superficial invagination between the superficialis tendons and the flexor retinaculum5. These invaginations arise from a common space at the ulnar side of the tendons adjacent to the FD5 tendon (7a). Although there are several anatomic variations in the communication patterns between the ulnar bursa, the radial bursa, and the digital flexor tendon sheaths6, a typical anatomic arrangement found in the majority of persons has been established through anatomic dissection as well as tenography in cadavers5,6,7,8.
Typical Patterns of Communication
Communication between the radial bursa and the FPL tendon sheath is the rule, reported in 100% of cases in both anatomic and imaging studies5,6. Communication between the ulnar bursa and the FD5 tendon sheath is slightly less common, occurring in approximately 80% of persons. Communication between the ulnar and radial bursae at the level of the carpal tunnel is common, occurring in 50%-100% of persons5,8. An ‘intermediate bursa’ consisting of accessory synovial sacs along the FD2 tendon has been identified as a site of communication between the radial and ulnar bursae5 (8a).
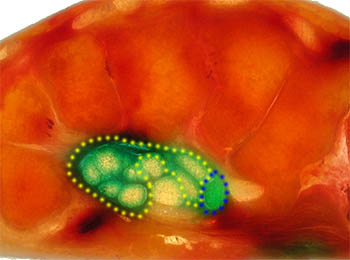
Figure 8:
Cadaveric section through the carpal tunnel depicting communication of the radial bura (blue dotted lines) and the ulnar bursa (yellow dotted lines). Green gelatin, previously injected into the FPL tendon sheath at the level of the proximal phalanx, is seen within both the radial and ulnar bursae.
The ulnar bursa typically does not communicate with the digital flexor tendon sheaths of the index, long, and ring fingers, but rather it terminates via short digital projections at the level of the metacarpal bones, the precise level varying within and between persons (9a, 10a).
Figure 9:
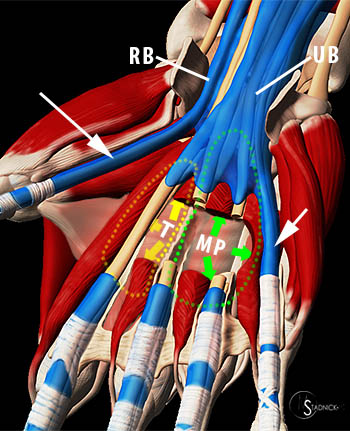
The typical anatomic relationship of the palmar bursae to the digital flexor tendon sheaths showing continuity of the radial bursa (RB) with the FPL tendon sheath (long arrow) and the ulnar bursa (UB) with the FD5 tendon sheath (short arrow). The tendon sheaths of FD2, FD3, and FD4 do not typically communicate with the ulnar bursa. The thenar and midpalmar concept of deep palmar spaces is also depicted with the thenar (T) and midpalmar (MP) spaces divided by a midpalmar septum and found deep to the flexor tendons and lumbrical muscles which have been partially resected. Some anatomic investigations do not support the existence of a midpalmar septum and instead combine the thenar and midpalmar spaces into a single 'central palmar space' (see text).
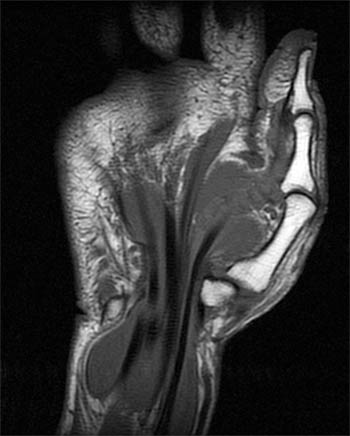
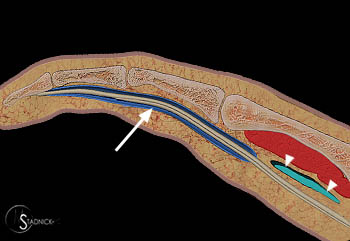
Figure 10:
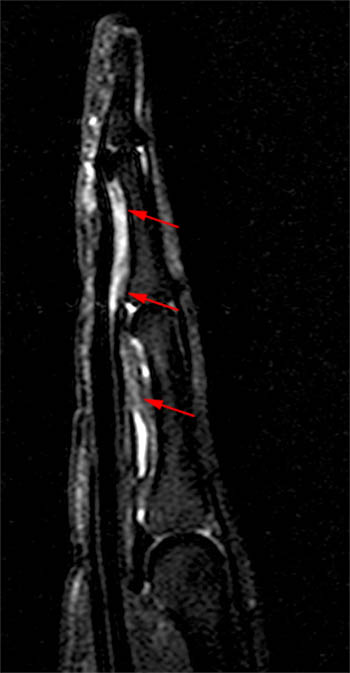
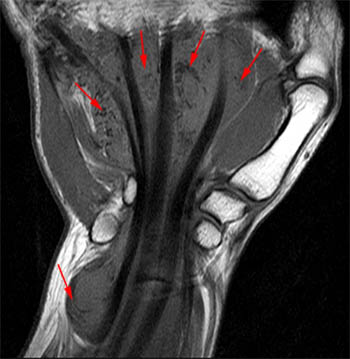
A fat-suppressed sagittal T2-weighted image from the same patient in the opening case demonstrates distension of the ulnar bursa with rice body formation secondary to atypical mycobacteria. Note the terminal digital projections of the ulnar bursa at the level of the metacarpal shaft (long arrow). The level of the carpal tunnel is denoted (short arrows).
Once they exit the digital projections, the flexor tendons continue distally without a synovial sheath for a short distance (1 to 3 cm) until they become enveloped by their respective tendon sheaths beginning at the level of the metacarpal heads and extending to the distal phalanges.
Synovial sheaths provide tendons with greater freedom of movement. The thumb and little finger are distinguished by greater range of motion than the other fingers, which may explain why the FPL and FD5 tendons are typically invested in a continuous synovial sheath. Similarly, observing that the range of flexion at the fingers exceeds the range of extension, it is not surprising that synovial tendon sheaths are present only on the flexor side3.
Anatomic Variations
Several variant patterns of communication have been described in the literature. In a series of 367 cases, there was continuity of the ulnar bursa with the tendons sheaths of the index finger in 5.1%, long finger in 4.0%, and ring finger in 3.5%8. Other variations include FD2 and FD3 tendon sheaths arising from the radial bursa6 and a single FD2 tendon sheath extending from the carpal tunnel to the distal phalanx without evidence of bursal communication8.
Digital Flexor Tendon Sheaths & Deep Palmar Spaces
In the fingers, normal flexion is facilitated by close apposition of the flexor tendons and the phalanges via the thickenings in the outer fibrous sheath known as the pulley system (see MRI Web Clinic December 2005). This proximity also facilitates the direct extension of infection between the tendon sheath and the apposing bones and joints and explains the frequent association of infectious tenosynovitis with adjacent osteomyelitis and septic arthritis. Infection may also spread by migrating within the confines of the tendon sheath, which is often readily apparent on MRI.
Any tenosynovial process-infectious, inflammatory, neoplastic-of the FPL or FD5 tendon sheaths, given typical anatomy, will have the potential to spread from one tendon sheath into the other tendon sheath via the palmar bursae. In cases of infection, this results in the classic horseshoe abscess, which, with MRI, can be demonstrated in its entirety in the coronal plane (11a) or inferred from sequential axial images (as in the opening case). Proximal extension into the forearm via the carpal tunnel may also occur.
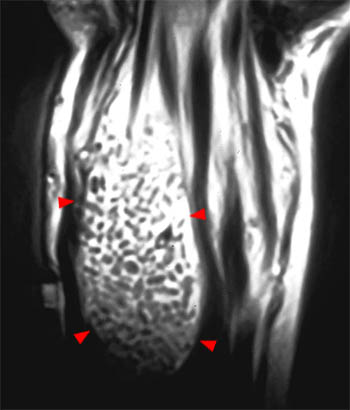
Figure 11:
A fat-suppressed T1-weighted post-contrast coronal image of the hand at the level of the carpal tunnel in a 58-year-old woman with horseshoe abscess due to tuberculosis. Note involvement of the the FPL (short arrow) and FD5 (long arrow) tendon sheaths. The digital flexor sheaths of FD2, FD3, and FD4 are spared (arrowheads).
Tenosynovitis of the FD2, FD3, and FD4 tendon sheaths is less likely to reach the level of the wrist given the typically discontinuous relationship of these tendon sheaths with the ulnar bursa. Instead, inflammatory processes can spill from the open proximal ends of these tendon sheaths into the deep palmar spaces. Suppurative infections reaching the deep palmar spaces threaten the intrinsic muscles of the hand; without expedient surgical drainage, compartment syndrome and tissue necrosis may result.
Of the deep spaces of the hand, the central palmar space is of particular interest with respect to the digital flexor tendon sheaths. This is a potential space deep to the flexor tendons and lumbrical muscles and superficial to the interossei muscles, bound radially by the thenar eminence and on the ulnar side by the hypothenar eminence. Based largely on the work of Kanavel9, this space has traditionally been divided into two separate spaces by a ‘midpalmar septum’, conceptualized as an effective barrier against the spread of infection from one space to the other. Thenar space designates the region radial to the midcarpal septum and contiguous with the FD2 tendon sheath, which is separate from the midpalmar space on the ulnar side of the septum, contiguous with the FD3 and FD4 tendon sheaths (10a). Although this model still predominates in the literature, it has been rejected by some subsequent investigations10 in favor of a single central palmar space with 7 intermediate septa, which partially divide the distal portion of the central palmar space into canals for the flexor tendons, lumbrical muscles, and neurovascular bundles.
While these models predict different patterns of spread of infection within the central palmar space, they define the same pathway for such spread from the flexor tendon sheaths into this potential deep space of the hand.
Flexor Tendons Outside The Carpal Tunnel
The palmaris longus tendon and the flexor carpi ulnaris tendon are not typically surrounded by synovial sheaths. The flexor carpi radialis (FCR) tendon, however, is invested in a synovial sheath as it travels adjacent to the carpal tunnel at its radial aspect, sequestered within its own fibro-osseous tunnel by a reflection of the flexor retinaculum. It then passes along the volar aspect of the scaphoid and trapezium, intimate with the overlying capsule of the triscaphe (scapho-trapezio-trapezoid) joint11, en route to its insertion on the base of the second metacarpal. An understanding of this anatomic relationship is important when evaluating the FCR tendon on MRI.
Pathology
The synovial sheaths of the wrist and hand may be involved by infectious and non-infectious inflammatory disease and, less commonly, infiltrative tumor and tumor-like conditions.
General Discussion and MRI Findings
Tenosynovitis refers to inflammation of a synovial tendon sheath and may be focal or diffuse. MRI findings of tenosynovitis include increased fluid signal within the tendon sheath, tendon sheath distension, and synovial proliferation. If an intravenous contrast agent is administered, there is typically synovial enhancement, especially in cases of infectious tenosynovitis12. Synovial thickening may be a prominent feature, especially in chronic or indolent processes.
The etiology of tenosynovitis is often difficult to distinguish based solely on the MRI appearance and generally requires clinical correlation. If tenosynovitis is seen bilaterally, an inflammatory non-infectious origin should be favored13.
Stenosing tenosynovitis-distinct from typical tenosynovitis-is characterized by adhesion of a tendon to a tendon sheath with associated increased tenosynovial fluid. On MRI, these adhesions typically demonstrate a hypointense, irregular appearance13.
Bursitis represents inflammation of a bursa and has imaging features similar to tenosynovitis. When inflammatory synovial tissue is present within the radial or ulnar bursa of the carpal tunnel, the process should be termed bursitis, rather than tenosynovitis5. The term tenosynovitis should be applied only to an inflammatory process within a tendon sheath (e.g., flexor tendon sheaths). The radial bursa and ulnar bursa are not typically visible on MRI unless they are abnormally distended by fluid or synovial proliferation.
Rice bodies are small fibrinous bodies that develop in the setting of chronic synovial inflammation and which are often visible on MRI. Classic teaching commonly associates rice bodies with Mycobacterium tuberculosis and rheumatoid arthritis. However, numerous chronic inflammatory conditions have been associated with rice body formation. Sarcoidosis can produce a similar appearance14.
Infectious Etiologies
Infectious flexor tenosynovitis and septic palmar bursitis are usually caused by direct implantation from puncture15 or bite wounds (13a, 14a). Less commonly, the cause is hematogenous spread-characteristic of Neisseria gonorrhea-or contiguous spread from an adjacent source of infection, including entities specific to the hand, such as a felon or paronychia16.
Infectious flexor tenosynovitis and septic palmar bursitis are most commonly caused by bacterial infections, with the most frequent microorganisms including Staphylococcus aureus, Streptococcus pyogenes, and gram-negative rods18,19,20. Bacterial infections become symptomatic within hours to days from the time of insult. The four classic clinical signs of Infectious tenosynovitis described by Kanavel are: (1) tenderness to palpation, (2) fusiform swelling of the digit, (3) flexed resting position of the involved finger, and (4) severe pain with passive extension17. A detailed clinical history and diagnostic fluid sampling are key components in guiding treatment. Empiric antibiotic therapy is initiated quickly to prevent the complications of Infectious tenosynovitis, such as adhesion formation, tendon or tendon sheath necrosis, and debilitating alterations in tendon function. Early surgical intervention is often advocated20, with techniques ranging from open drainage to closed-catheter irrigation. Additional bacterial, mycobacterial, fungal, and parasitic agents have been implicated. Patient characteristics and exposure history may provide clues to a specific microorganism.
Figure 13:
A short tau inversion recovery (STIR) sagittal image in a 19-year-old man who suffered a bite wound during an altercation demonstrates periarticular soft tissue edema at the extensor aspect of the 3rd MCP joint (arrow), with associated septic arthritis (arrowhead) and FD3 tenosynovitis(short arrows). Note the 3rd MCP joint held in flexion, one of Kanavel's classic signs of infectious tenosynovitis.
Mycobacterial Infections
Mycobacterium tuberculosis and a variety of atypical mycobacteria have been implicated in infectious flexor tenosynovitis and septic palmar bursitis.
Although uncommon, cases of tuberculous tenosynovitis and bursitis are increasing in frequency, a phenomenon attributed to growing elderly and immunocompromised populations and rising drug resistance,18,21.
Atypical mycobacterial infections involving the musculoskeletal system are most frequently present within the wrist and hand20. This association may be related to the increased risk for infectious inoculation via penetrating injuries and the abundance of synovium in the hand14. Mycobacterium marinum is a common causative species, and was first isolated in 1926 from dead saltwater fish at the Philadelphia Aquarium19. The clinical history of exposure to contaminated water is critical to the accurate diagnosis of M. marinum infection.
Unlike pyogenic infections, mycobacterial infections have a more indolent course, typically presenting over weeks to months and often with less severe symptoms. Due to the indolent course, diagnosis is often delayed; therefore, imaging can play an important role in raising the possibility of mycobacterial infection21,22,23.
Reported data have suggested that increased synovial thickening and rice body formation are findings on MRI that suggest mycobacterial infection over other causative agents21,22,23. Proper clinical management requires a high index of suspicion as cultures are frequently negative. Empiric pharmacotherapy, often in conjunction with tenosynovectomy, is the accepted treatment20.
Inflammatory, Non-infectious Etiologies
Rheumatoid Arthritis
Manifestations of rheumatoid arthritis include tenosynovitis and palmar bursitis. The MRI findings of rheumatoid arthritis are nonspecific and include synovial proliferation, thickened enhancing synovium, and increased tenosynovial fluid volumes24 (15a,16a).
Figure 15:
A fat-suppressed proton density axial image just proximal to the carpal tunnel demonstrates increased tenosynovial fluid (short arrows) and synovial proliferation (arrowheads) in the radial and ulnar bursae as well as multiple extensor tendon sheaths in this 45-year-old female with rheumatoid arthritis.
Seronegative Arthropathies
The most commonly encountered disease processes in this group are ankylosing spondylitis, psoriatic arthritis, reactive arthritis, and enteropathic arthritis. On MRI, nonspecific findings of tenosynovitis and bursitis generally do not allow differentiation of these entities based solely on imaging characteristics27.
Gout
Gout is caused by elevated serum urate levels, which leads to deposition of monosodium urate crystals (tophi) in and around joints. The MRI findings include a nonspecific tenosynovitis, with the most specific imaging features being an enhancing tophus adjacent to an osseous erosion, resulting in an overhanging edge of native eroded bone27,29.
Calcium Pyrophosphate Dihydrate Crystal Deposition Disease
Calcium pyrophosphate dihydrate crystal deposition (CPPD) can occur in the flexor tendon sheaths. The resulting inflammatory process can present clinically as carpal tunnel syndrome30,31. CPPD crystal deposition disease typically demonstrates nonspecific tenosynovitis and variable enhancement following intravenous contrast administration. With MRI, detection of chrondrocalcinosis in the hand can be difficult; therefore, correlation with radiography can play an important role in accurate diagnosis.
Hydroxyapatite Deposition Disease
Calcium hydroxyapatite crystal deposition disease (HADD) is most commonly seen about the shoulder, but it can be present in or around any joint of the body. The flexor carpi ulnaris tendon is the most common site of involvement in the hand31,32. The typical MRI findings are calcific deposits regional to the flexor tendons that demonstrate decreased signal intensity on all imaging sequences. Tenosynovitis, bone marrow edema, and osseous erosions may be present.
Sarcoidosis
Sarcoidosis is characterized by noncaseating granulomata. The musculoskeletal system is involved in approximately 1-13% of patients with this disease. MRI findings in sarcoidosis include tenosynovitis, tendinosis, bursitis, and rice bodies (17a,18a,19a). Often, a synovial or soft tissue biopsy is necessary to confirm the diagnosis33.
Flexor Carpi Radialis (FCR) Tenosynovitis
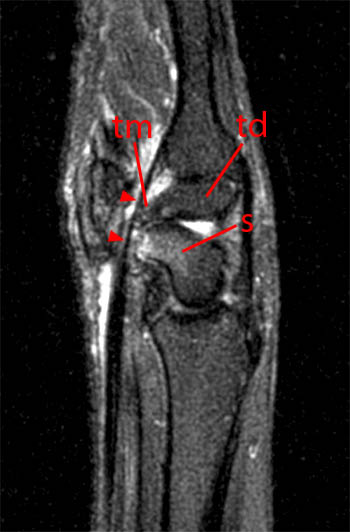
The FCR tendon is invested with its own synovial sheath and generally remains isolated from disease of the palmar bursae. Rather, FCR tendinopathy is frequently associated with articular disease of the triscaphe joint, a consequence of their intimate anatomic relationship. Physical proximity makes the FCR tendon vulnerable to mechanical compression arising from triscaphe joint osteoarthritis; chronic attritional changes from encroaching osteophytes may manifest as tendinosis, tenosynovitis, or tearing of the FCR tendon (S,T). Furthermore, developmental or acquired communications between the triscaphe joint capsule and the FCR tendon sheath allow effusion, inflammation, or infection to extend from the joint into the tendon sheath11.
Tumors and Tumor-like Conditions of the Synovial Sheaths
Pigmented Villonodular Synovitis (PVNS) and Giant Cell Tumor of the Tendon Sheath (GCT)
PVNS and GCT are histologically identical benign synovial proliferative diseases. They can be categorized into four clinicopathologic subtypes based on morphology (focal or diffuse) and location (intra-articular or extra-articular)35. The familiar giant cell tumor of the tendon sheath is the focal, extra-articular form of the disease, most often presenting as a nodular mass along the volar aspects of the fingers. Simple excision is usually curative. The diffuse, extra-articular form of the disease is less common and much more aggressive, widely infiltrating soft tissues and frequently recurring following excision. On MRI, diffuse-type GCT (also termed extra-articular PVNS) appears similar to conventional (intra-articular) PVNS (22a-22d) with lobulated margins, hemosiderin deposition, and contrast enhancement.
Figure 22:
38-year-old woman with diffuse-type GCT (PVNS). T1-weighted sagittal (22a), fat-suppressed T1-weighted post-contrast sagittal (22a), T1-weighted coronal (22c), and fat-suppressed T1-weighted post-contrast axial (22d) images demonstrate the hourglass configuration of infiltrative, enhancing soft tissue within the palmar bursae. Scattered foci of low signal intensity are compatible with hemosiderin (arrows).
Tenosynovial and Bursal Chondromatosis
Tenosynovial and bursal chondromatosis is an uncommon benign neoplastic process that frequently affects the flexor tendon sheaths and palmar bursae and is histologically similar to intra-articular synovial chondromatosis. The typical MRI appearance consists of T1 intermediate and T2 hyperintense foci, which demonstrate mild enhancement with a peripheral and septal pattern after administration of intravenous contrast. Additional suggestive MRI features include a fusiform shape and location within a tendon sheath or bursa36.
Management
The management of flexor tenosynovitis and palmar bursitis depends on the specific disease process. In cases of infection, fluid sampling is typically necessary to confirm the diagnosis and isolate a particular organism15. Prompt initiation of appropriate antimicrobial therapy is an important component of treatment, as failure to treat infectious tenosynovitis and septic bursitis in a rapid manner may result in tendon or tendon sheath necrosis, osteomyelitis, or septic arthritis, among other potential complications20,34.
The inflammatory arthropathies are treated with pharmacologic regimens tailored to the specific disease process (e.g., disease-modifying anti-rheumatic drugs for rheumatoid arthritis in its earliest stages in an attempt to reduce morbidity)27. Tumors are typically treated with surgical resection, and tumor-like synovial processes are commonly treated with synovectomy.
Conclusion
Central to the imaging evaluation of the digital flexor sheaths and palmar bursae is an understanding of typical pathways of synovial communication and their implications on patterns of disease spread. A familiarity with the range of infectious, inflammatory, and neoplastic conditions that affect these structures, coupled with an understanding of the underlying anatomy, will benefit the radiologist in his or her practice.
References
1 Yugueros P, Berger RA. Carpal Tunnel Syndrome (2007): 10-12; Jan 2007.
2 Khan KM, Cook JL, Bonar F, Harcourt P, Astrom M. Histopathology of common tendinopathies. Update and implications for clinical management. Sports Med. 1999 Jun;27(6):393-408.
3 Benjamin M, Kaiser E, Milz S. Structure-function relationships in tendons: a review. J Anat. 2008 Mar;212(3):211-28.
4 Wood Jones F (1944a) The Principles of Anatomy as Seen in the Hand. London: Balli?re, Tindall and Cox.
5 Aguiar RO, Gasparetto EL, Escuissato DL, Marchiori E, Trudell DJ, Haghighi P, Resnick D. Radial and ulnar bursae of the wrist: cadaveric investigation of regional anatomy with ultrasonographic-guided tenography and MR imaging. Skeletal Radiol. 2006 Nov;35(11):828-32.
6 Fussey JM, Chin KF, Gogi N, Gella S, Deshmukh SC. An anatomic study of flexor tendon sheaths: a cadaveric study. J Hand Surg Eur Vol. 2009 Dec;34(6):762-5.
7 Resnick D. Roentgenographic anatomy of the tendon sheaths of the hand and wrist: tenography. Am J Roentgenol Radium Ther Nucl Med. 1975 May;124(1):44-51.
8 Scheldrup, EW. Tendon sheath patterns in the hand; an anatomical study based on 367 hand dissections. Surg Gynecol Obstet. 1951 Jul;93(1):16-22.
9 Kanavel, AB. Infections of the Hand, 6th Edition. 1934: 23-91. London: Bailliere, Tindall & Cox.
10 Bojsen-Moller F, Schmidt L. The palmar aponeurosis and the central spaces of the hand. J Anat. 1974 Feb;117(Pt 1):55-68.
11 Parellada AJ, Morrison WB, Reiter SB, Carrino JA, Kloss LA, Glickman PL, McLean M, Culp RW. Flexor carpi radialis tendinopathy: spectrum of imaging findings and association with triscaphe arthritis. Skeletal Radiol. 2006 Aug;35(8):572-8.
12 Ragheb D, Stanley A, Gentili A, et. al. MR imaging of the Finger Tendons: Normal Anatomy and Commonly Encountered Pathology. European Journal of Radiology. 2005;56:296-306.
13 Chhabra, A. et al. Current Perspectives on 3T MR imaging of the wrist. Radiographics. 2012; 32:879-896.
14 Chau CLF, Griffith JF, Chan PT, et al. Rice-Body Formation in Atypical Mycobacterial Tenosynovitis and Bursitis: Findings on Sonography and MR Imaging. AJR Am J Roengeol. 2003;180:1455-1459.
15 Berquist TH. MRI of the Musculoskeletal System, 6th ed. Philadelphia: Lippincott Williams & Wilkins, 2012.
16 Resnick D. Diagnosis of Bone and Joint Disorders, 4th ed. Philadelphia: W.B. Saunders Company, 2002.
17 Kanavel A. Infections of the Hand: A Guide to the Surgical Treatment of Acute and Chronic Suppurative Processes in the Fingers, Hand and Forearm, 7th ed. Lea & Febiger, Philadelphia, 1939.
18 Tehranzadeh J, Ter-Oganesyan RR, and Steinbach LS. Musculoskeletal disorders associated with HIV infection and AIDS. Part I: Infectious musculoskeletal conditions. Skeletal Radiol. 2004;33: 249-259.
19 Small LN, Ross JJ. Suppurative Tenosynovitis and Septic Bursitis. Infect Dis Clin N Am. 2005;19:991-1005.
20 Abrams RA and Botte MJ. Hand Infections: Treatment Recommendations for Specific Types. J Am Acad Orthop Surg. 1996;4:219-230.
21 Hsu C, Lu H and Shih T. Tuberculosis Infection of the Wrist: MRI Features. AJR Am J Roentgenol. 2004;183:623-628.
22 Yao DC, Sartoris, DJ. Musculoskeletal Tuberculosis. Radiology Clinics of North America, 1995;33:679-689.
23 Hoffman KL, Berman, Ag, Hoffman DK, et al. Tuberculosis tenosynovitis of the flexor tendons of the wrist: MR imaging with pathologic correlation. Skeletal Radiol. 1996; 24:180-188.
24 McQueen FM, Stewart N, Crabbe J, et al. Magnetic resonance imaging of the wrist in early rheumatoid arthritis reveals a high prevalence of erosions at four months after symptom onset. Ann Rheum Dis. 1998;57:350-356.
25 Tehranzadeh J, Asikyan O, Anavium A, et al. Enhanced MR imaging of tenosynovitis of hand and wrist in inflammatory arthritis. Skeletal Radiol. 2006;25:814-822.
26 McGonagle D, Conaghan PG, O’Connor P, et al. The relationship between synovitis and bone changes in early untreated rheumatoid arthritis: a controlled magnetic resonance imaging study. Arthritis Rheum. 1999;42:1706-1711.
27 Jbara M, Patana M, Kazmi F, and Beltran J. MR Imaging: Arthropathies and Infectious Conditions of the Elbow, Wrist, and Hand. Radiol Clin N Am. 2006; 44:625-642.
28 McGonagle D, Gibbon W, Emery P. Classification of inflammatory arthritis by enthesitis. Lancet. 1998;352:1137-1140.
29 Chung CB and Steinbach LS. MRI of the Upper Extremity: Shoulder, Elbow, Wrist and Hand. Philadelphia; Lippincott, Williams and Wilkins, 2009.
30 Rate AJ, Parkinson RW, Meadows TH, Freemont AJ. Acute carpal tunnel due to pseudogout. J Hand Surg Br. 1992;17(2):217-8.
31 Steinbach, LS. Calcium Pyrophosphate dihydrate and calcium hydroxyapatite crystal deposition diseases: imaging perspectives. Radiol Clin N Am. 2004;42:185-205.
32 Garcia GM, McCord GC, Kumar R. Hydroxyapatite crystal deposition disease. Semin Musculoskelet Radiol. 2003;7:187-193.
33 Lee EY, Rubin DA, and Brown DM. Recurrent Mycobacterium marinum tenosynovitis of the wrist mimicking extraarticular synovial chondromatosis on MR images. Skeletal Radiol. 2004;33(7):405-408.
34 Schnall SB, Vu-Rose T, Holton PD, et al. Tissue Pressure in Pyogenic Flexor Tenosynovitis of the Finger. J Bone Joint Surg. 1996;78-B:793-795.
35 Lucas DR. Tenosynovial giant cell tumor: case report and review. Arch Pathol Lab Med. 2012 Aug;136(8):901-6.
36 Walker EA, Murphey MD, and Fetsch JF. Imaging characteristics of tenosynovial and bursal chondromatosis. Skeletal Radiol. 2011;40:317-325.