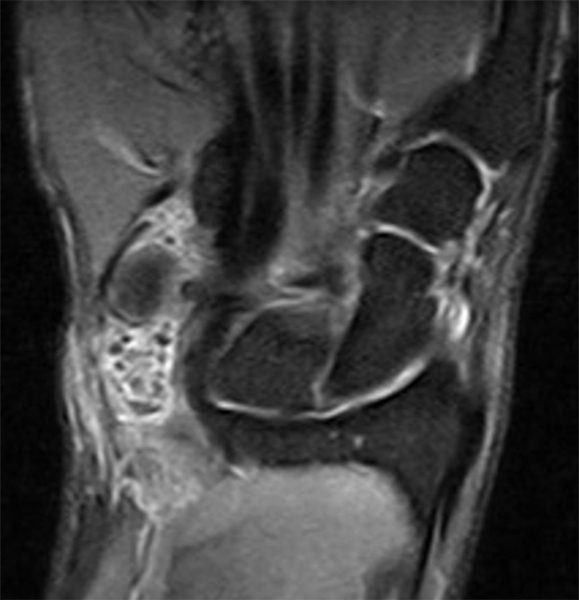
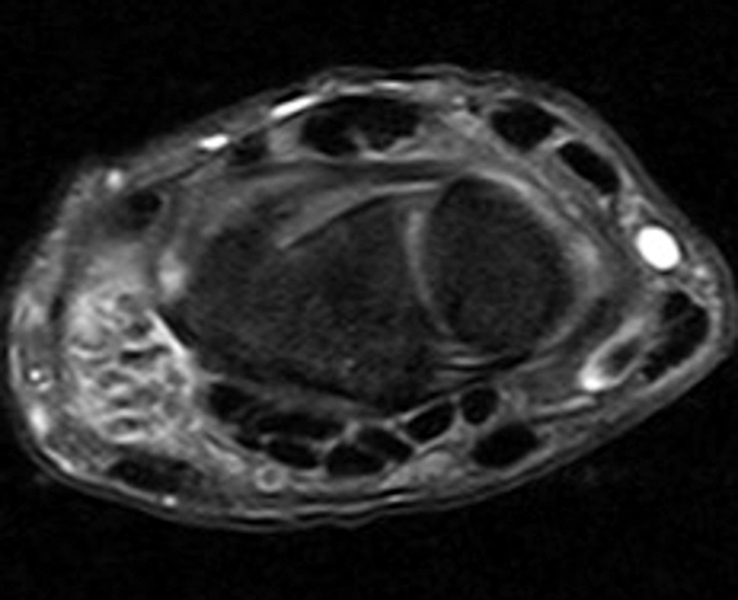
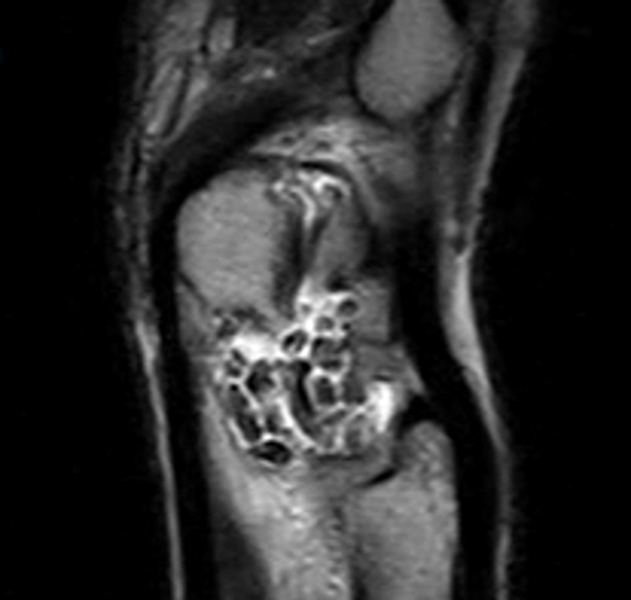
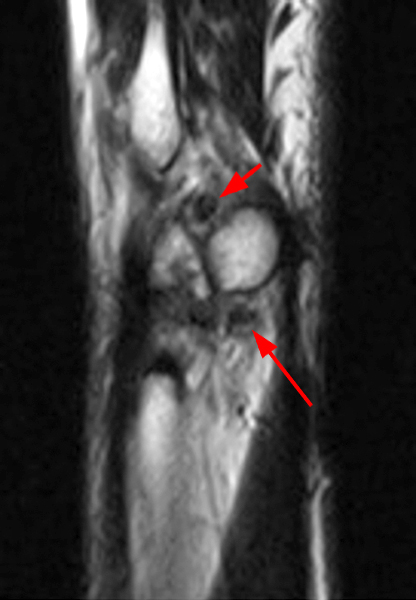
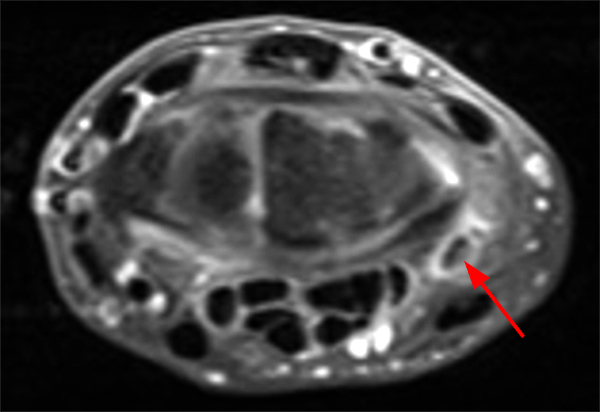
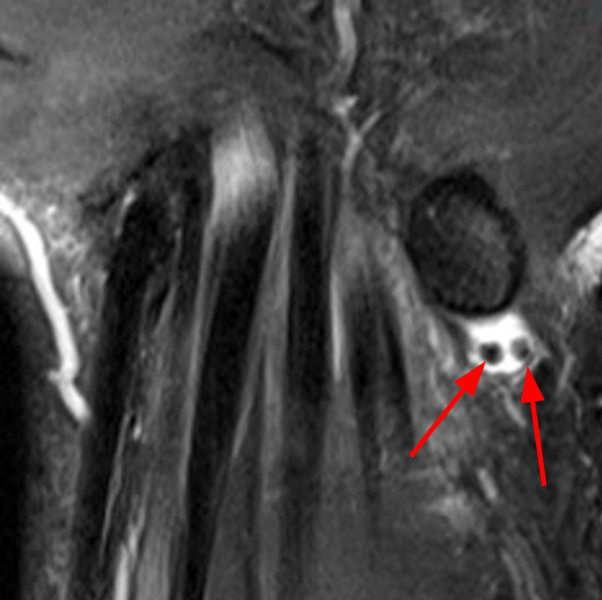
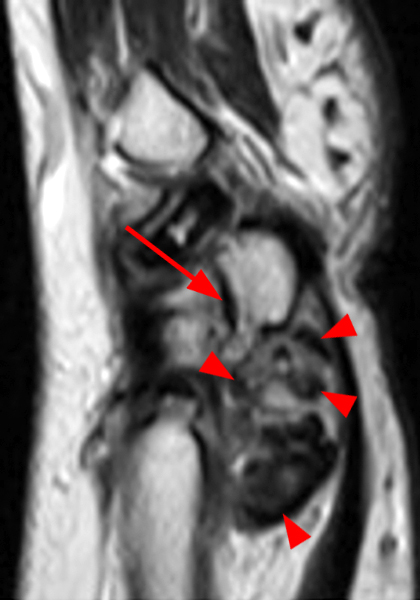
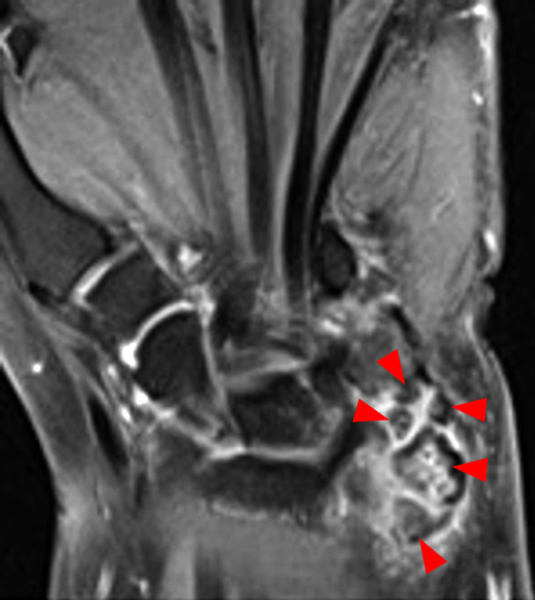
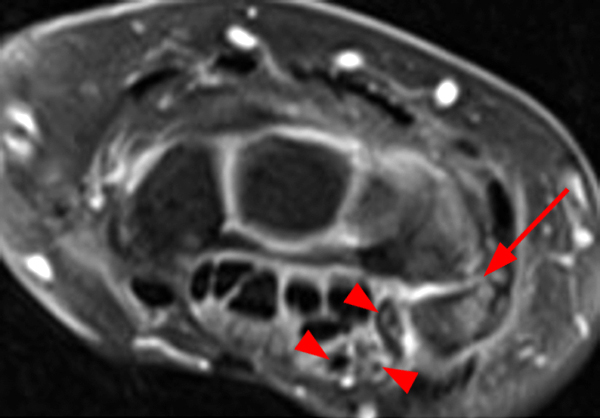
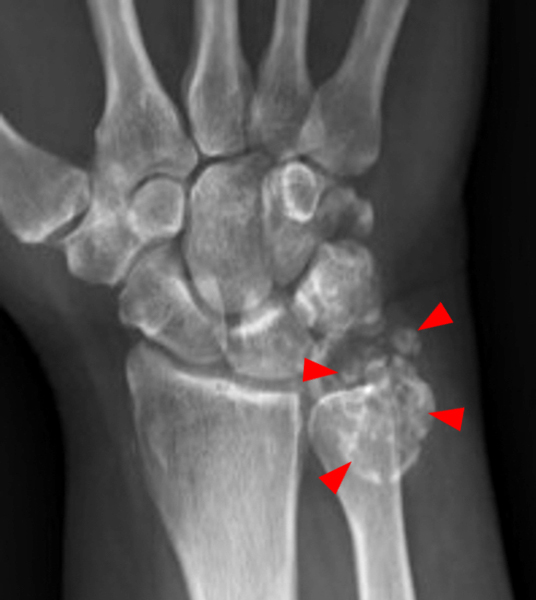
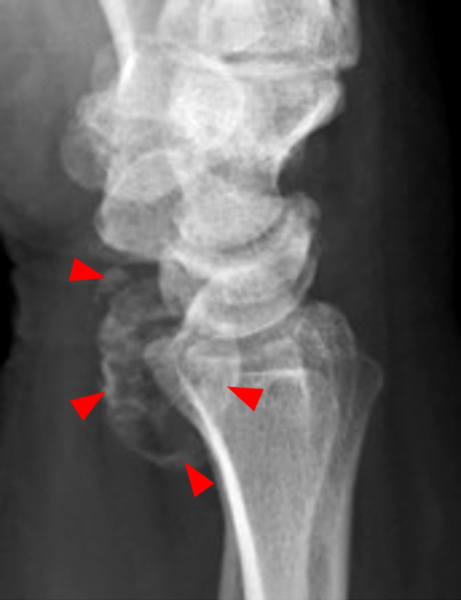
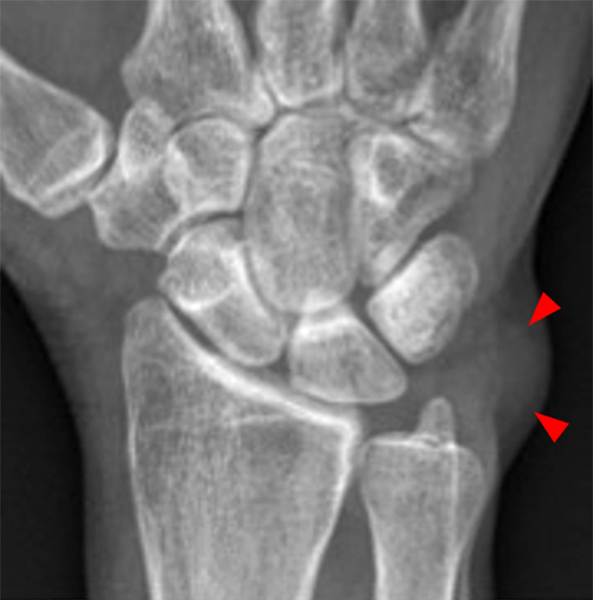
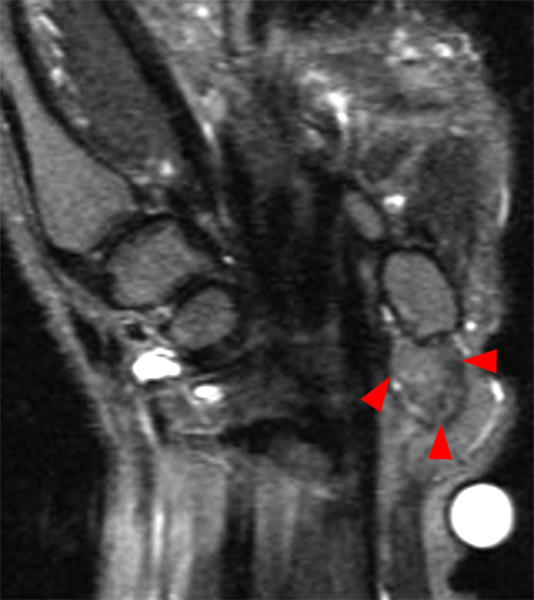
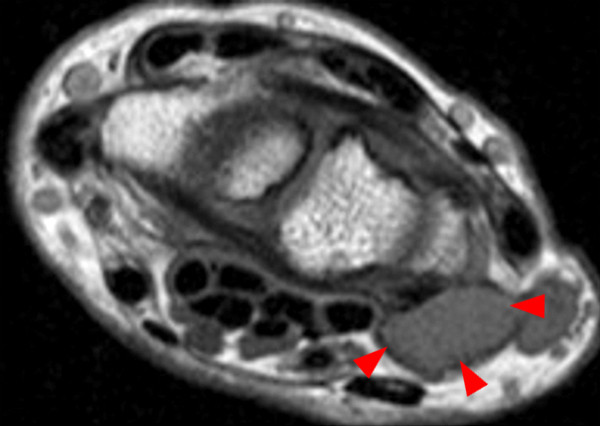
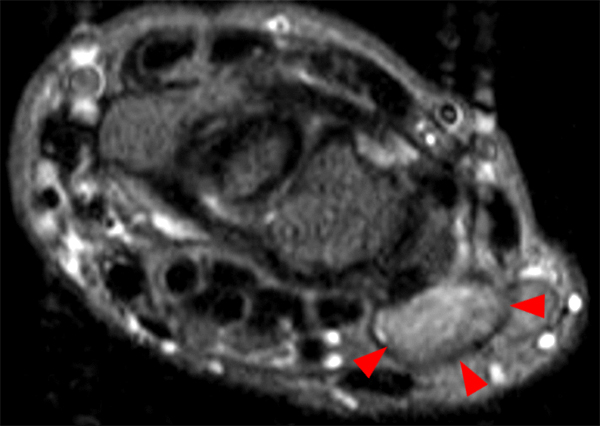
Clinical History: A 49-year-old male presents with left wrist pain for over 1 year. Coronal (1A and 1B) and axial (1C) fat-suppressed proton-density-weighted images and a sagittal T2-weighted image (1D) of the wrist are provided. What are the findings? What is your diagnosis?
Findings
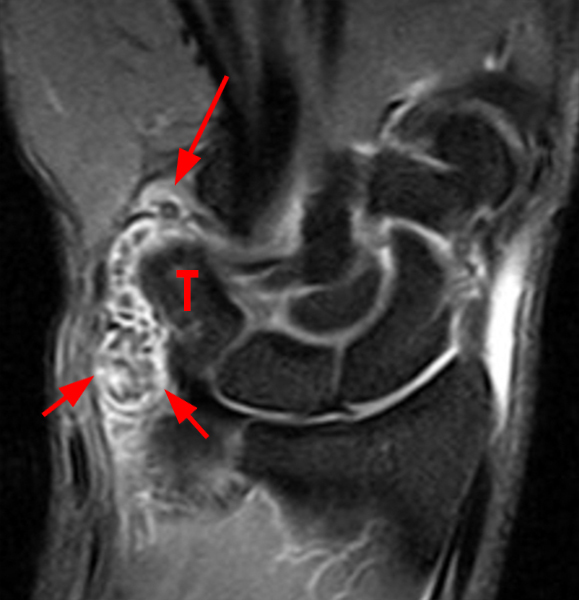
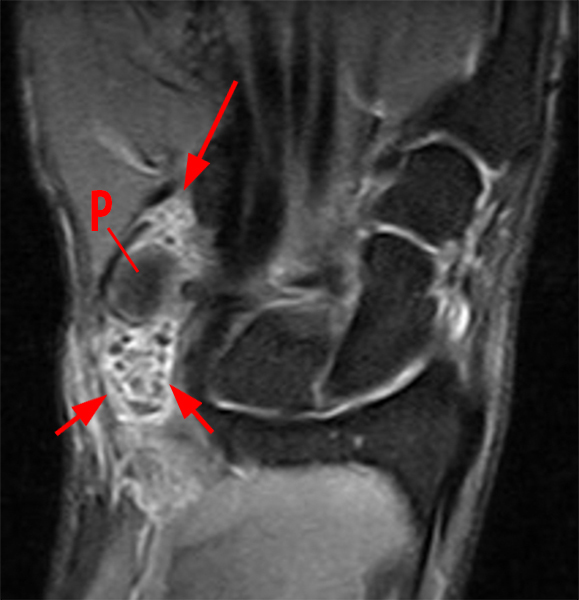
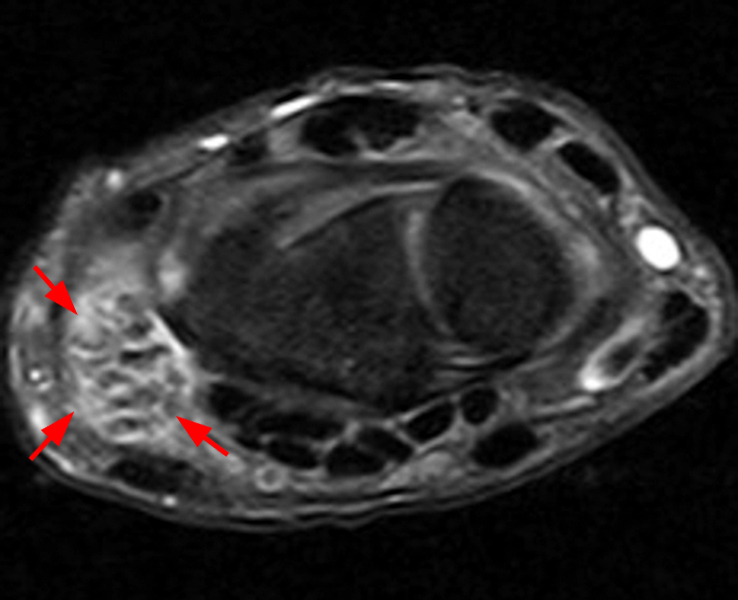
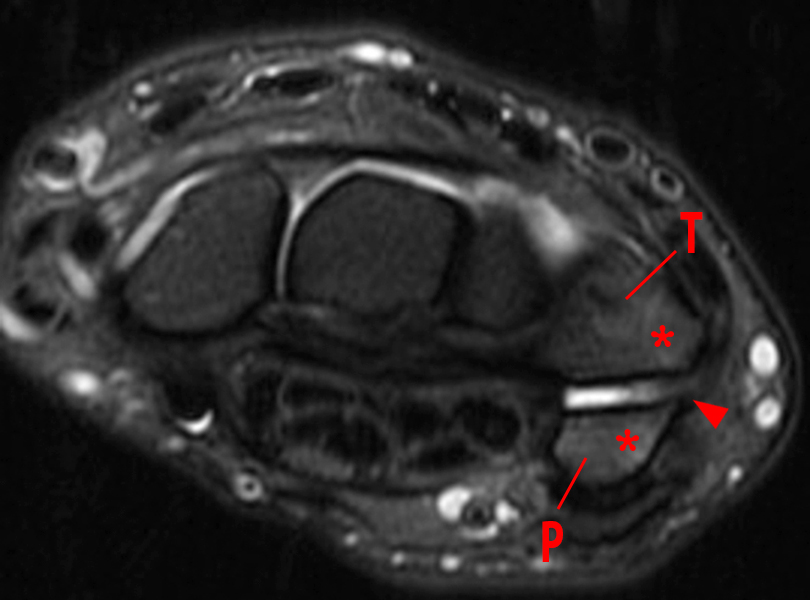
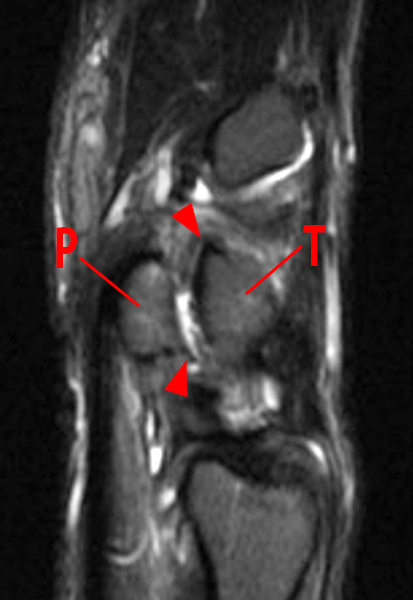
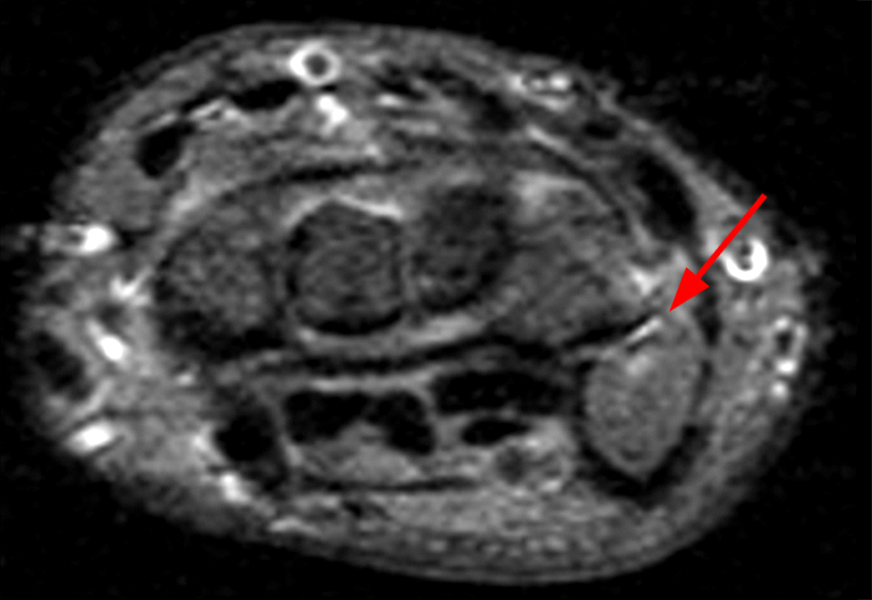
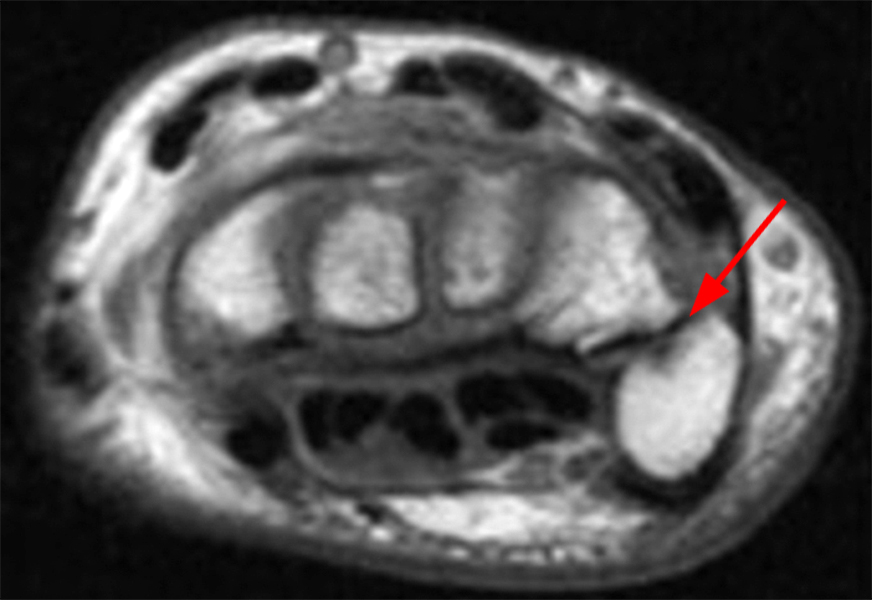
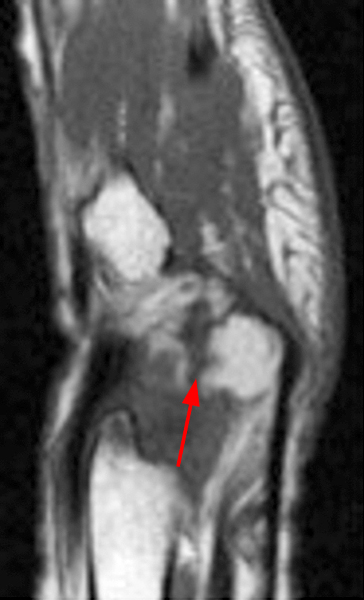
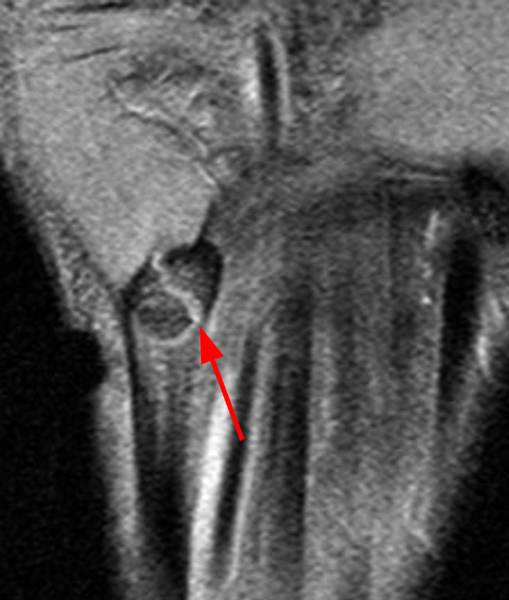
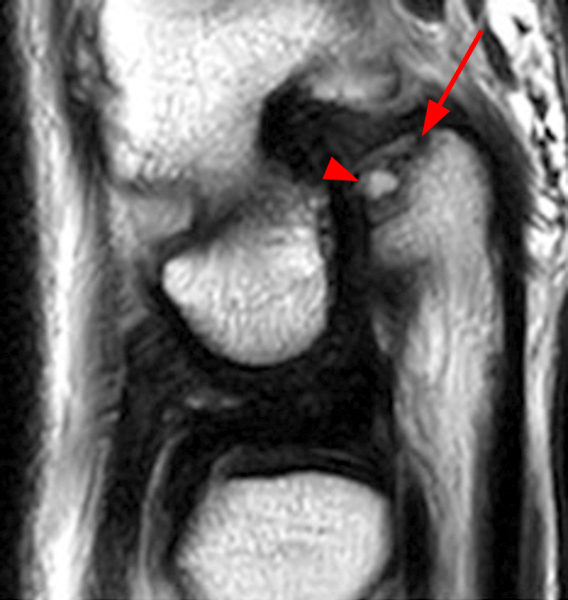
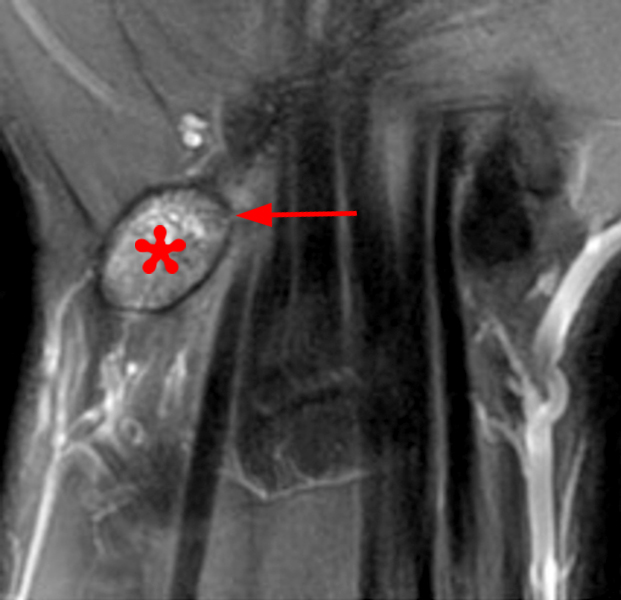
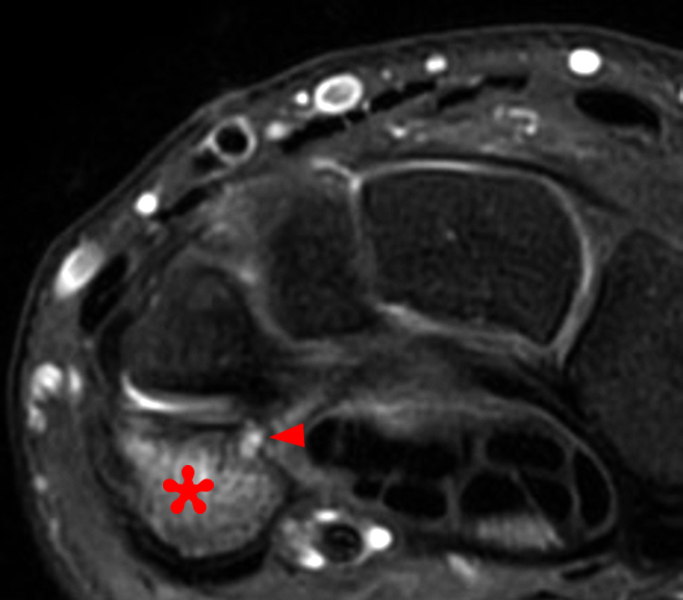
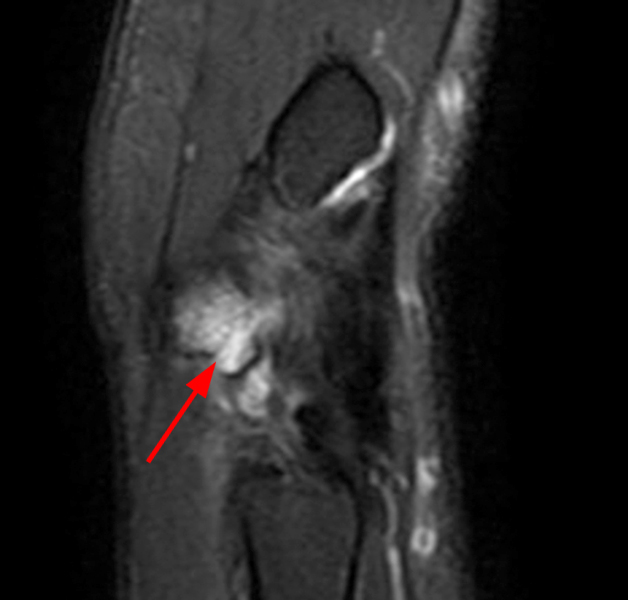
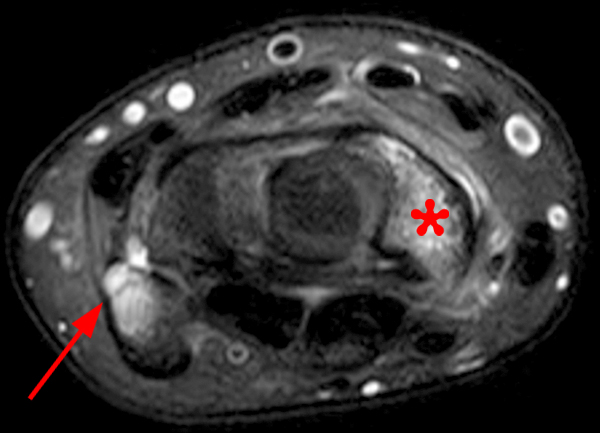
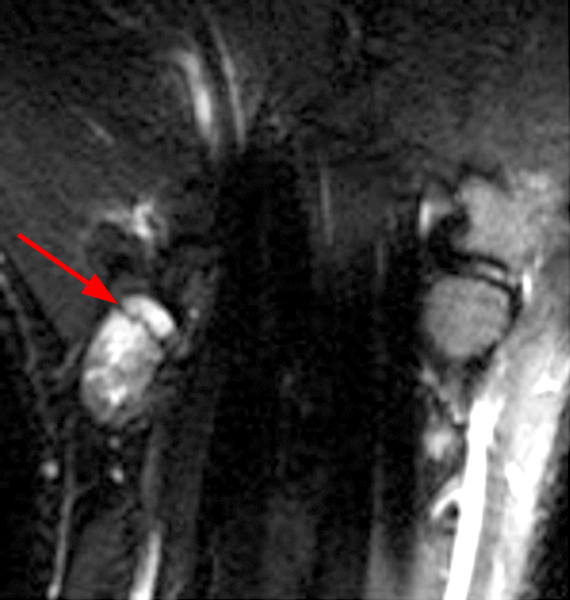
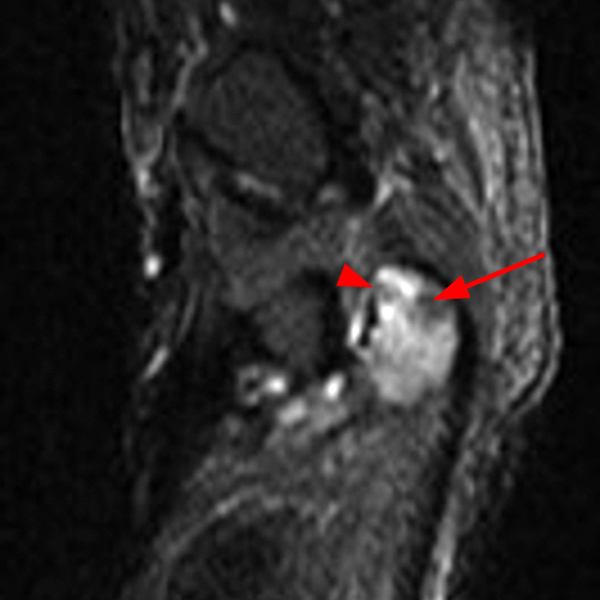
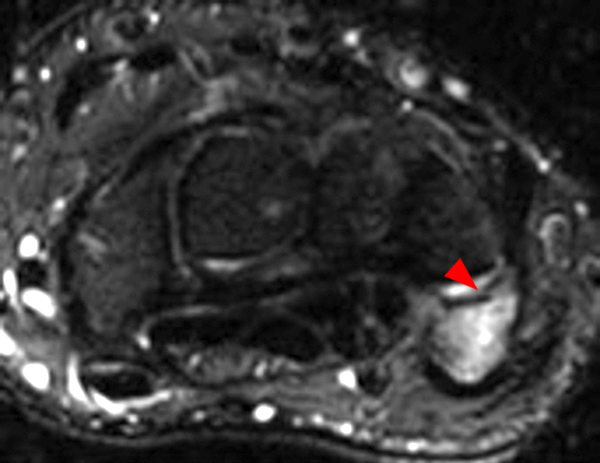
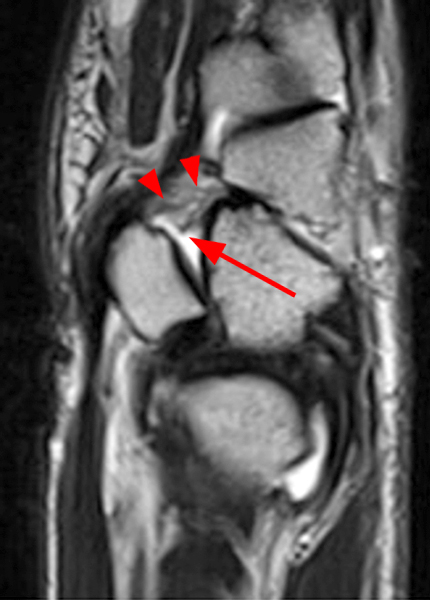
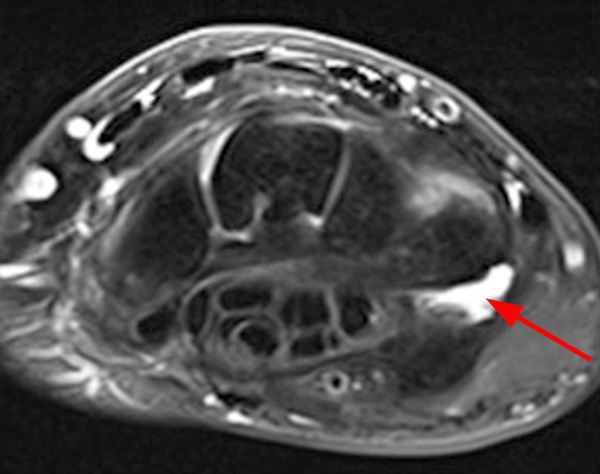
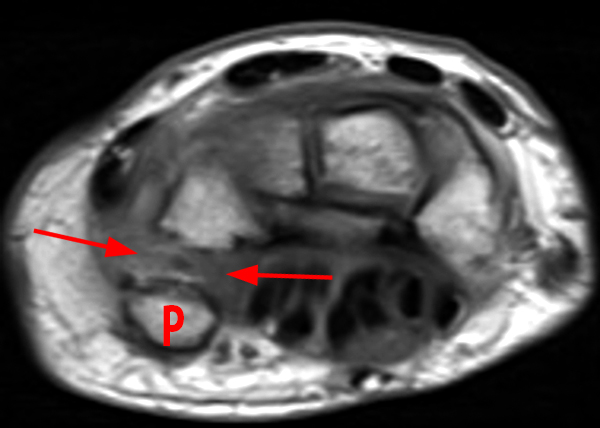
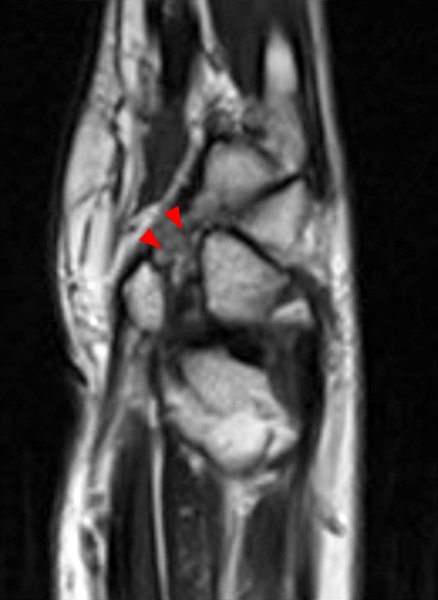
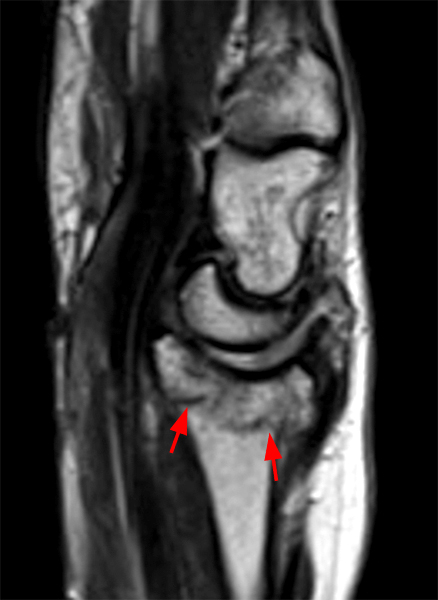
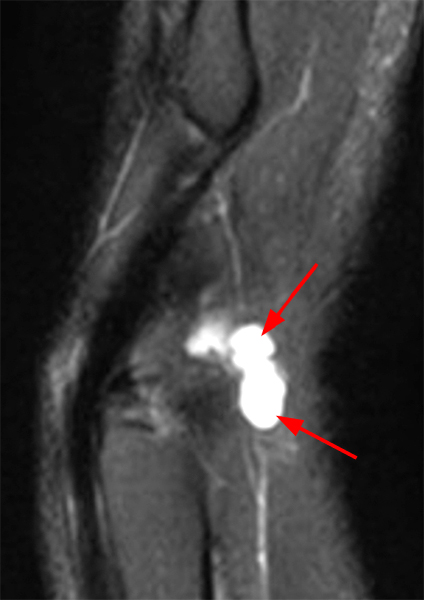
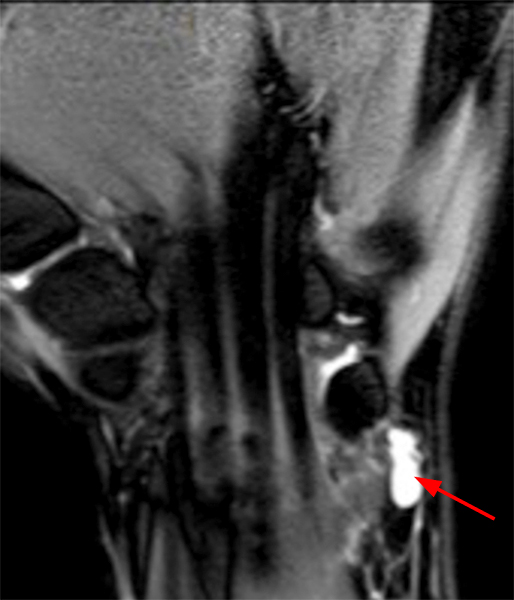
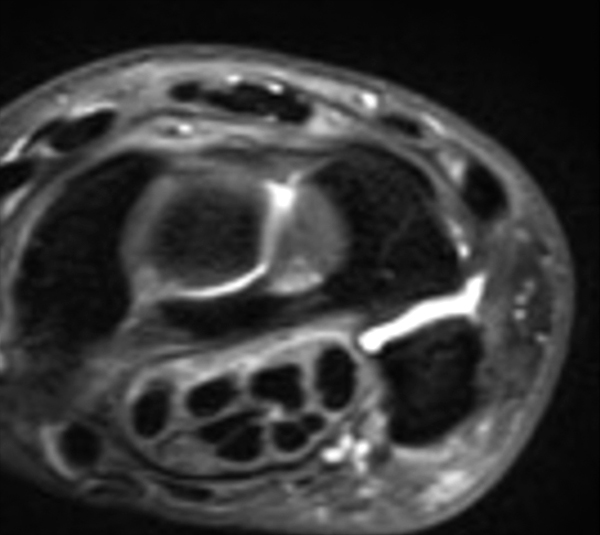
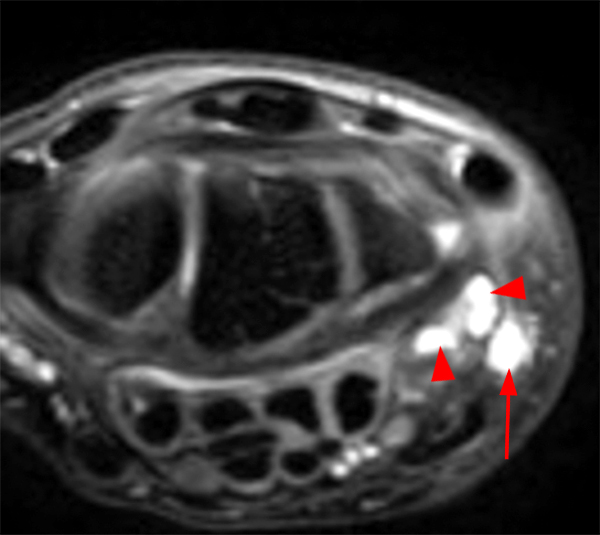
Figure 2:
Coronal (2A and 2B) and axial (2C) fat-suppressed proton-density-weighted images and the sagittal T2-weighted image (2D) of the wrist demonstrate severe distention of the proximal (short arrows) and distal (long arrows) recesses of the pisotriquetral joint with innumerable small calcified and cartilaginous loose bodies. Mild degenerative arthritis of the pisotriquetral joint (arrowheads) is noted. The pisiform (P) and triquetrum (T) are indicated.
Diagnosis
Primary synovial osteochondromatosis of the pisotriquetral joint.
Introduction
Lesions within or adjacent to the pisotriquetral (PT) joint are a significant but under-appreciated cause of wrist pain. This pain may be caused by acute trauma or may be chronic in nature due to osteoarthritis or other pathology within or adjacent to the PT joint. PT joint disorders should be considered in the setting of pain and tenderness at the palmar and ulnar aspects of the wrist, particularly if the pain is increased by flexion and/or ulnar deviation of the wrist.
Anatomy
The pisiform is the smallest of the carpal bones and contributes indirectly to wrist and hand function through its multiple soft tissue attachments and its articulation with the triquetrum. Damage to the surrounding structures can lead to instability and dysfunction of the PT joint.
There are four primary stabilizers of the pisiform (Figure 3), which include the flexor carpi ulnaris (FCU) tendon, the pisohamate ligament (PHL), the pisometacarpal ligament (PML), and the pisotriquetral ulnar ligament (PTUL).1,2 The bulk of the FCU inserts on the palmar aspect of the proximal pisiform, with additional strands extending to join fibers of the PHL and PML. In flexion, the FCU pulls the pisiform proximally and palmarly, widening the joint space. In extension, the pisiform displaces distally with narrowing of the joint space. The pisiform increases wrist flexion forces by enhancing the force of the FCU. The PHL extends from the palmar distal aspect of the pisiform bone to the hook of the hamate bone. The PML extends from the palmar distal aspect of the pisiform bone to the bases of the fourth and fifth metacarpals, coursing through the concavity along the ulnar aspect of the hook of the hamate. The PML is thinner and longer than the PHL. The PTUL is a thickening of the capsule on the ulnar aspect of the joint, lying below the extensor retinaculum, and not well distinguished from the extensor retinaculum on MR due to the thin nature of these structures.
Secondary stabilizers of the pisiform include the flexor retinaculum and extensor retinaculum. The muscular insertion of the abductor digiti minimi covers the majority of the distal and medial pole of the pisiform and the PML. (Figure 3).
The pisiform forms the ulnar border of the proximal end of Guyon’s canal (Figure 4), in close relation with the ulnar neurovascular bundle which lies on the lateral aspect of the pisiform. Ulnar neuropathy may be caused by PT joint instability, as increased motion of the pisiform may cause nerve irritation or compression by distorting the anatomy of Guyon’s canal. The PT joint forms the ulnar border of the carpal tunnel and is closely related to the flexor tendons of the small finger.
The PT joint has a loose capsule which provides little or no stability. The proximal recess of the PT joint is smooth and round, and communicates with the radiocarpal joint in 82%.3 The distal recess of the PT joint is smaller than the proximal recess.
While radiographs may demonstrate fractures, dislocation or osteoarthritis near the pisiform and PT joint, CT and MR are useful for occult fractures or avulsions. MR imaging provides superior visualization of the anatomic structures surrounding the PT joint. MR arthrography is uncommonly performed, though has been shown to enhance the visualization of structures around the PT joint and improve assessment of the chondral surfaces of the pisiform and triquetrum (Figure 3).3
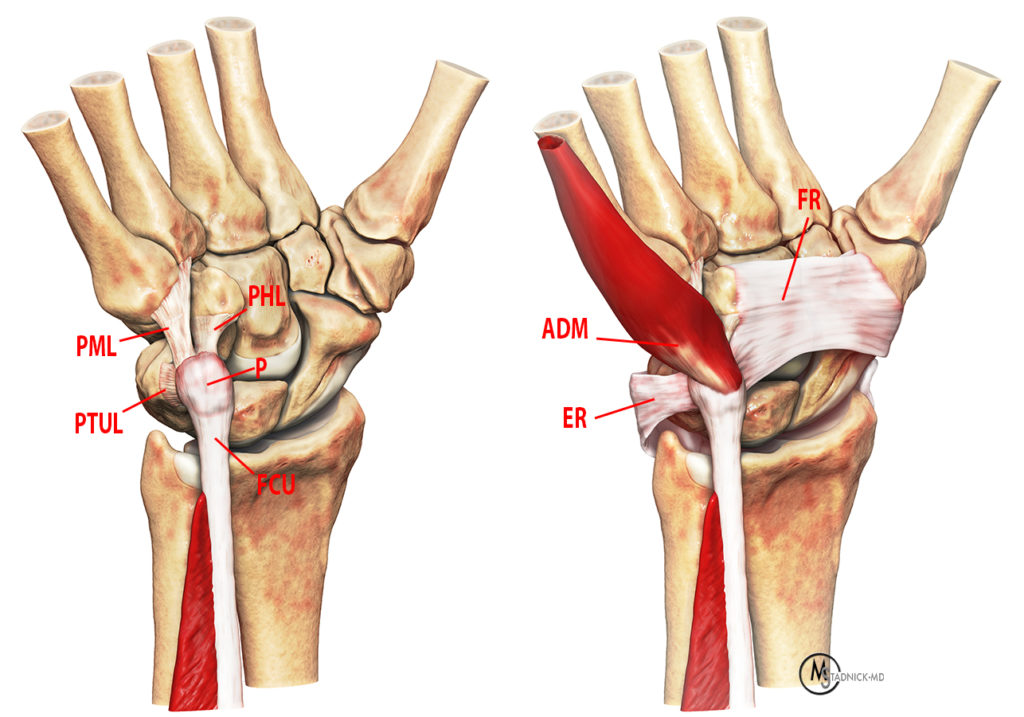
Figure 3:
The primary stabilizers of the pisiform (P) are the flexor carpi ulnaris (FCU) tendon, pishohamate ligament (PHL), pisometacarpal ligament (PML), and the pisotriquetral ulnar ligament (PTUL). The secondary stabilizers of the pisiform are the flexor retinaculum (FR) and the extensor retinaculum (ER). The abductor digiti minimi (ADM) arises primarily from the pisiform.
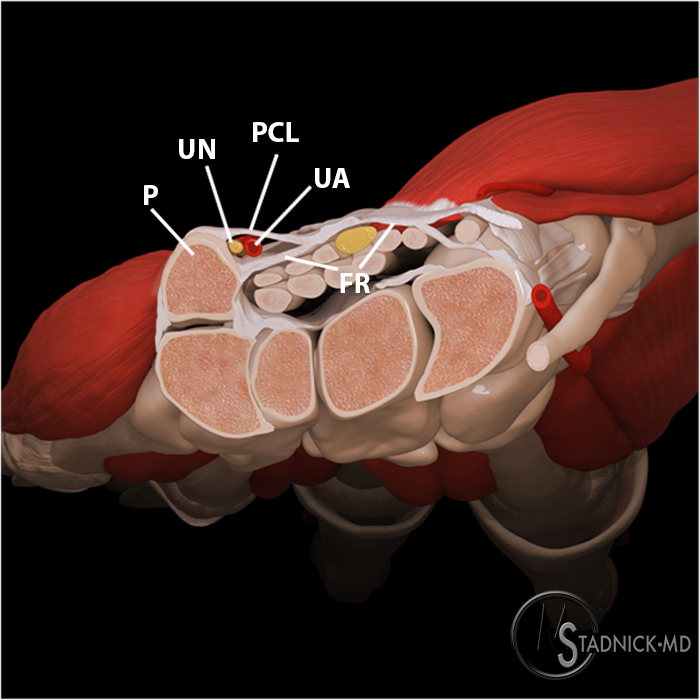
Figure 4:
Axial view at the level of the proximal to mid pisiform demonstrates Guyon's canal and the carpal tunnel. The ulnar artery (UA) and ulnar nerve (UN) lie close to the pisiform (P) within Guyon’s canal. The pisiform (P) forms the ulnar boundary, the palmar carpal ligament (PCL) forms the roof, and the flexor retinaculum (FR) forms the floor and radial boundary of Guyon’s canal at this level. The flexor retinaculum separates Guyon’s canal from the carpal tunnel.
Pathology
Osteoarthritis
Degenerative changes of the PT joint are common, although often remain undiagnosed at clinical and radiographic evaluation.4 Osteoarthritis (OA) is more easily diagnosed on CT or MRI, although X-rays may demonstrate joint space narrowing, subchondral sclerosis, osteophytes and/or loose bodies. MR allows for evaluation of the articular surfaces and for detection of subchondral edema.5,6 Cartilaginous lesions at the PT joint are mainly peripheral in location, less frequently global, and rarely involve the central portion of the joint. Most of the osteophytes are proximal or distal rather than medial or lateral, as osteoarthritis arises from movements of the joint that are more accentuated in the proximal-distal direction.3
Pisotriquetral OA may be classified as primary, secondary, or post-surgical.1 Primary OA typically affects women over 50 years of age with no history of past trauma, is usually bilateral, and demonstrates a progressive onset of pain.
Secondary OA may be post-traumatic or related to overuse (microtrauma). Untreated articular fracture of the pisiform or triquetrum may lead to development of pain months after a fall on an extended wrist. Alternatively, soft tissue injuries may lead to instability of the PT joint, which can lead to secondary osteoarthritis and/or ulnar nerve irritation in Guyon’s canal. Indirect microtrauma at the PT joint may be related to repetitive and powerful contractions of the FCU in activities such as racket sports, which leads to compression and torsion stresses on the joint, or may be due to direct repetitive microtrauma in the case of hand workers or volleyball players.
Post-surgical osteoarthritis has been reported after carpal tunnel surgery, although this is rare.5 The flexor retinaculum is a secondary stabilizer of the pisotriquetral joint, and its release in carpal tunnel decompression surgery may contribute to pisotriquetral dysfunction with pain, likely secondary to the medial translation of the pisiform.1
Osteoarthritis of the PT joint may be treated conservatively with NSAIDs and physical therapy, and with local injection of steroids. Excision of the pisiform bone (pisiformectomy) may help with restoring function and alleviating symptoms when conservative treatment is not sufficient (Figure 7). Pisiformectomy results have been shown to be good with patients rarely experiencing long-term disability. A study by Lam et al. showed minimal functional disability during normal daily life, and the majority of patients were able to return to their previous level of activity following pisiformectomy.6
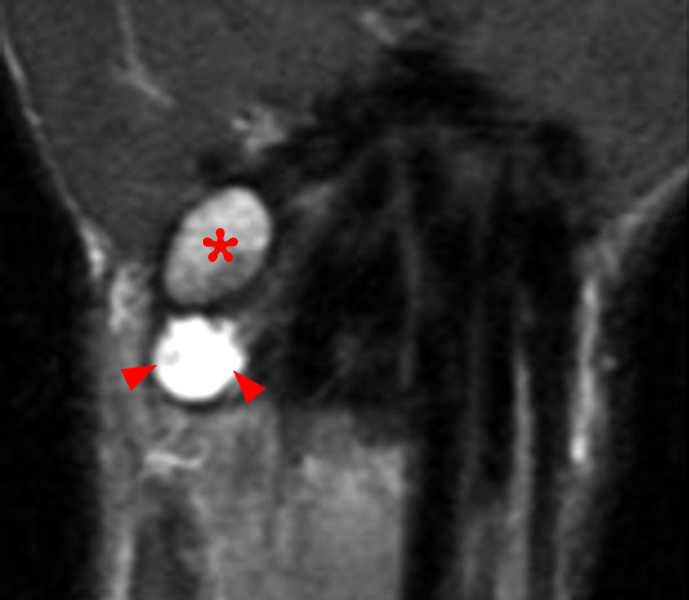
Figure 5:
Axial (5A) and sagittal (5B) T2 fat-suppressed T2-weighted images demonstrate joint space narrowing, mild subchondral edema (asterisks), and small osteophytes (arrowheads) at the pisotriquetral joint in a patient with ulnar sided wrist pain, compatible with osteoarthritic changes. The pisiform (P) and triquetrum (T) are indicated.
Figure 6:
55-year-old patient with increasing pain, with no history of trauma. Coronal (6A) and axial (6B) STIR images, and a sagittal proton-density weighted image (6C) demonstrate joint space narrowing at the PT joint with prominent subchondral marrow edema within the pisiform (asterisk), and a joint effusion in the proximal recess (arrowheads).
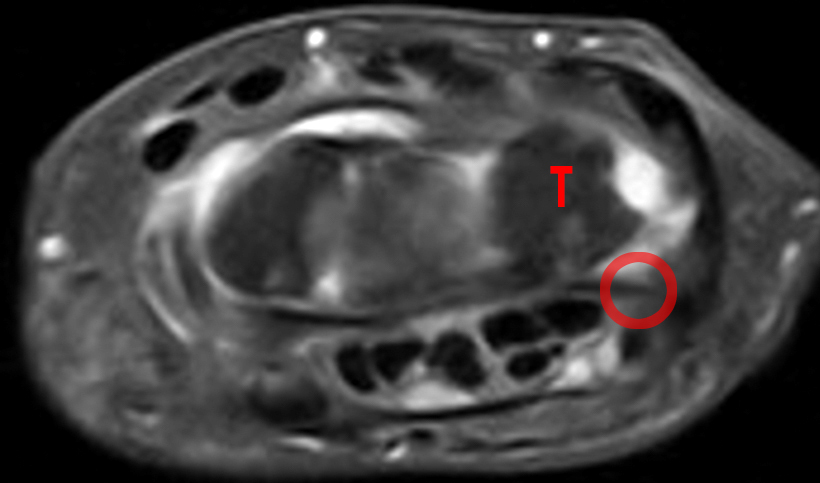
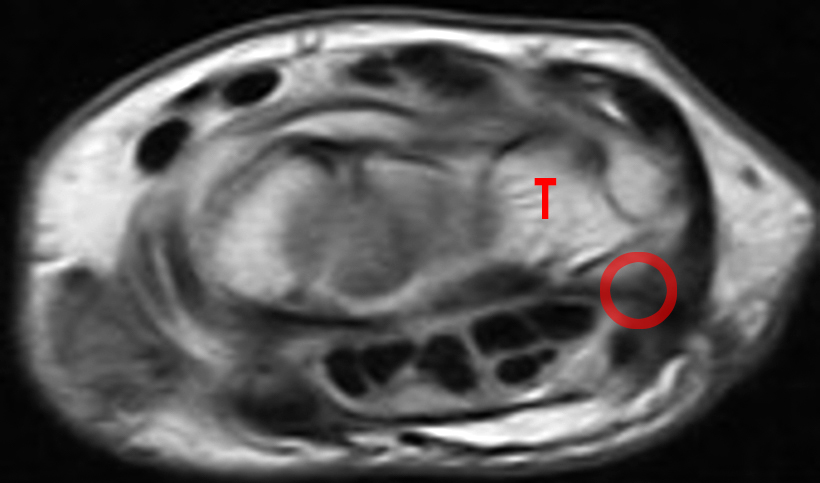
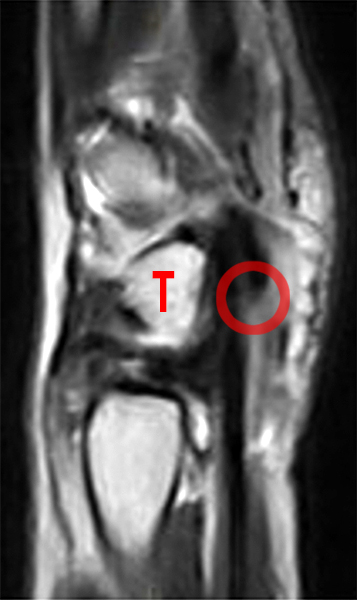
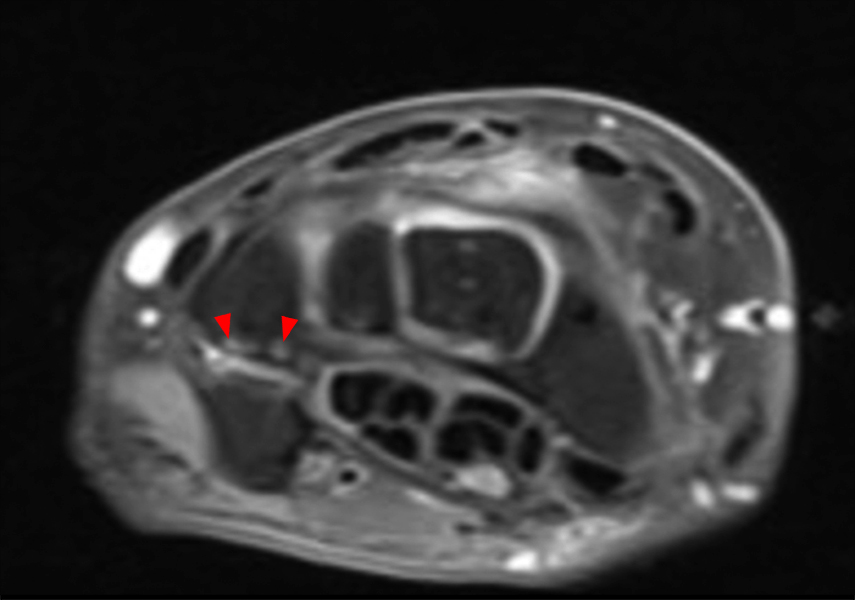
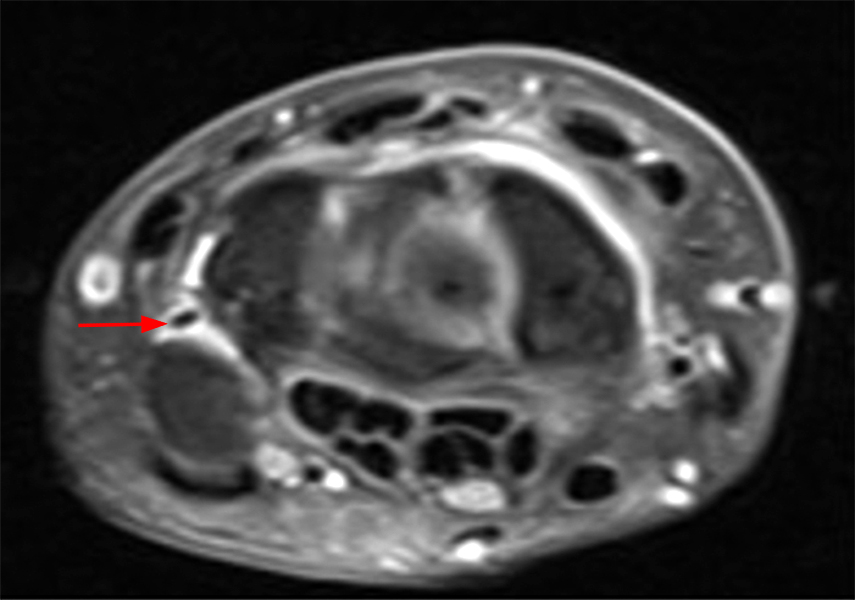
Figure 7:
Osteoarthritic changes at the PT joint, with subsequent pisiformectomy for treatment. Axial STIR (7A) and T1 (7B), and sagittal T1-weighted (7C) images demonstrate OA at the PT joint (arrows).
Axial fat-suppressed proton density-weighted (7D), axial proton density-weighted (7E), and sagittal T2-weighted (7F) images obtained one year later show interval resection of the pisiform for treatment of the pain related to the PT joint. The triquetrum is indicated (T), and the pisiform is absent (red circle).
Loose Bodies
Loose bodies may accumulate in the proximal or distal recesses of the PT joint and contribute to ulnar-sided wrist pain, impingement, and/or intermittent locking (Figures 8-10). Loose bodies may be the result of a specific traumatic event, or may be related to chronic repetitive trauma. The exact origin of the loose body is speculative, though may be presumed to be from the triquetrum or pisiform if arthritic changes are present at the PT joint.7 Since the PT joint has been shown to communicate with the radiocarpal joint3, presumably loose bodies could migrate and become trapped in the PT joint. Primary (Figure 2) or secondary (Figure 11) osteochondromatosis can rarely occur at the PT joint.
Excision of PT loose bodies may provide satisfactory relief of symptoms in patients without significant underlying joint degeneration.7 In patients with associated chondromalacia or osteoarthritis of the PT joint, pisiformectomy may provide symptomatic relief of ulnar-sided wrist pain as previously discussed.
Figure 8:
Osteoarthritic changes at the PT joint with loose bodies. Coronal (8A) and axial (B-D) fat-suppressed proton density-weighted images demonstrate OA at the PT joint with mild subchondral degenerative changes (arrowheads). Several loose bodies are present in the proximal recess (arrows).
Figure 11:
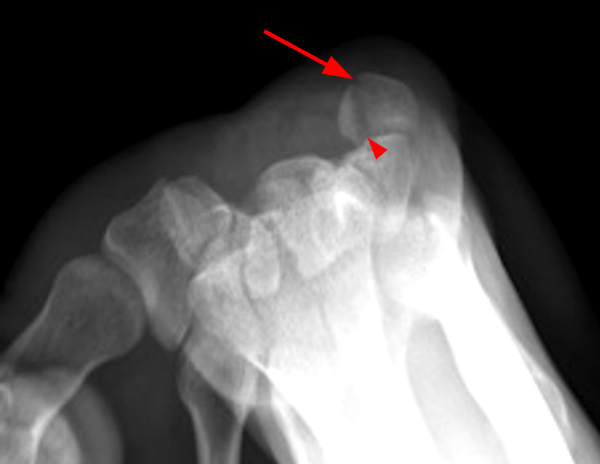
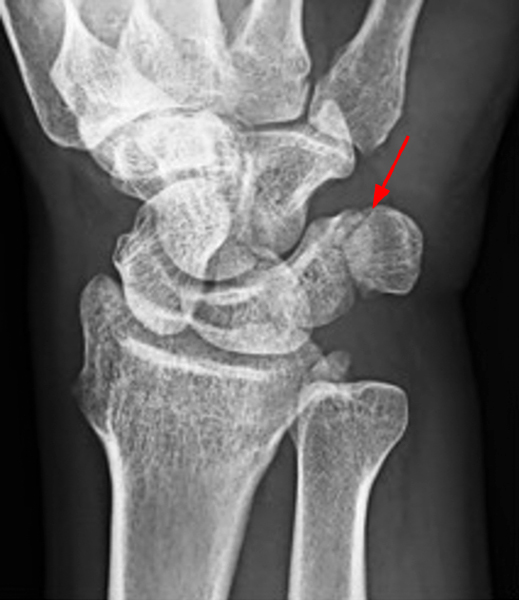
Secondary osteochondromatosis. Sagittal T2-weighted (11A), coronal (11B) and axial (11C) fat-suppressed proton density-weighted images show multiple loose bodies (arrowheads) of variable size, which were visible on x-rays (11D,E). Osteoarthritic changes are seen at the PT joint (arrow).
Trauma
Fractures of the pisiform are rare, accounting for 1-2% of all carpal fractures.8 These fractures are best seen on CT or MR, though may occasionally be visualized on special radiographic views such as the carpal tunnel view (Figure 12A). Pisiform fractures may be isolated (Figures 12, 13) or associated with other wrist fractures or bone bruises (Figure 14). Fractures or the pisiform may result from a direct impaction injury related to a fall, a stress injury from repetitive microtrauma, or an avulsion injury related to major contraction of the FCU. Intraarticular fractures may predispose to secondary osteoarthritic changes at the PT joint (Figure 15). The ulnar nerve should be carefully evaluated in the setting of trauma at the pisiform or PT joint given its proximity to the pisiform.
Nearly all pisiform fractures can be treated with immobilization in a cast or splint for 4–6 weeks. Transverse fractures are at higher risk of non-union due to contraction forces of the FCU. Pisiformectomy is an option for widely displaced comminuted fractures or for athletes who wish to return quickly to sport.8
Ligamentous injury at the PT joint may be suspected (Figures 16, 17) if the joint space is wider than 4 mm, the loss of parallelism of the joint surface exceeds 20°, or if the proximal or distal displacement of the pisiform in relation to the triquetrum amounts to more than 15 % of the joint surface.1 Very rarely the pisiform may be dislocated without fracture and displaced radially.
Figure 13:
Intra-articular pisiform fracture in a 28-year-old with ulnar sided pain after sliding into a base 4 weeks ago. Ballcatcher radiograph (13A), sagittal T2-weighted (13B), and coronal (13C) and axial (13D) fat-suppressed proton density-weighted images demonstrate a small intra-articular fracture involving the dorsal distal radial pisiform (arrows). Marrow edema (asterisk) and a small subchondral cyst (arrowhead) are noted at the pisiform. These fractures can predispose to OA at the PT joint.
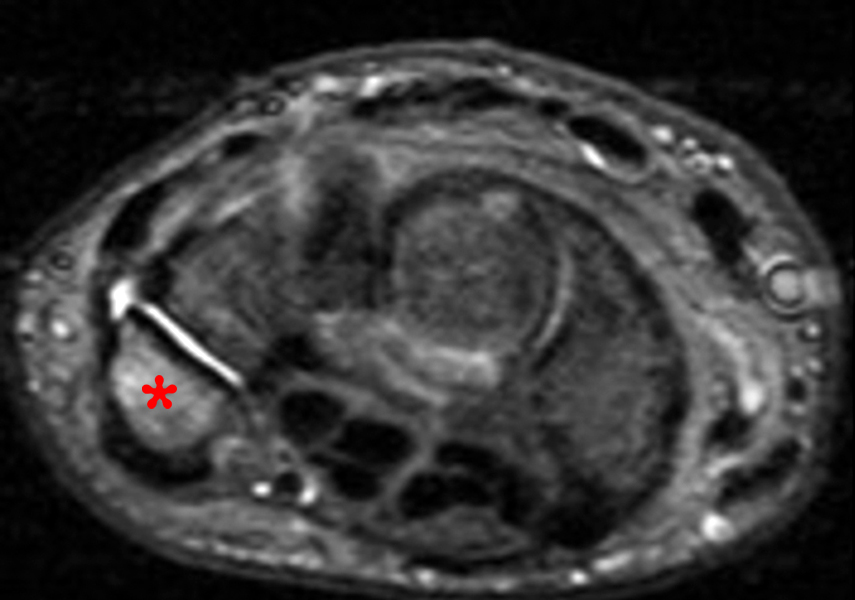
Figure 14:
23-year-old male patient status post fall with ulnar sided wrist pain. Sagittal (14A) and axial (14B) fat-suppressed T2-weighted images demonstrate a mildly displaced fracture (arrows) at the proximal medial edge of the pisiform. This patient also had a nondisplaced fracture of the scaphoid (asterisk).
Figure 15:
Intra-articular fracture in a 19-year-old male after a fall. Coronal fat-suppressed T2 -weighted (15A) and sagittal (15B) and axial (15C) STIR images demonstrate a fracture (arrows) of the distal pisiform, with intraarticular extension seen on the sagittal and axial images (arrowheads).
Figure 16:
Asymmetric widening of the PT joint in a 67-year-old patient with ulnar sided wrist pain and history of distal radius fracture. Sagittal T2-weighted (16A) and axial (16B) fat-suppressed T2-weighted images show widening of the distal portion of the PT joint (arrows), which may suggest capsular and/or ligamentous injury. Indistinctness of the distal capsular structures is noted (arrowheads).
Figure 17:
Post-traumatic widening of the PT joint in a 77-year-old patient with acute left wrist pain and concern for a mass at the volar wrist. Axial proton density-weighted image (17A) and sagittal T2-weighted images (17B,C) demonstrate widening of the pisotriquetral joint (arrows) compatible with capsular and ligamentous tearing, and relative volar displacement of the pisiform (P) which likely accounted for the palpable abnormality. The distal capsular structures are noted to be thickened and irregular (arrowheads). A fracture of the distal radius is noted. This patient also had numbness in the middle and ring fingers, and close evaluation of the ulnar nerve is always warranted in the setting of pisiform and/or PT joint injuries.
Ganglion Cysts
Ganglion cysts can arise from the PT joint (Figure 18), causing ulnar-sided pain, swelling, or ulnar neuropathy. The cyst may extend into Guyon’s canal and compress or directly infiltrate the ulnar nerve.9 MRI allows for detection of the cyst and can demonstrate the origin of the cyst for purposes of operative planning.
Figure 18:
31-year-old patient with ulnar sided wrist pain for 3 weeks, with suspected ganglion cyst. Sagittal fat-suppressed T2-weighted (18A,B), and coronal (18C,D) and axial (18E-G) fat-suppressed proton density-weighted images demonstrate a 12 x 9 x 7 mm lobulated ganglion cyst (arrows) at the volar aspect of the proximal pisotriquetral recess (arrowheads).
Other
Rheumatologic disorders
The pisotriquetral joint is a synovial joint and thus may be affected by rheumatologic disorders, such as rheumatoid arthritis, psoriatic arthritis, juvenile idiopathic arthritis, or crystal deposition disease.1
Tenosynovial giant cell tumors (TGCT, formerly PVNS and GCTTS)
Reported cases of TGCT located in the hand and wrist are scarce, though can occur (Figure 19). Tenosynovial giant cell tumors (TGCT) are a group of rare, benign tumors that involve the synovium, bursae and tendon sheath. The World Health Organization (WHO) classified these tumors in 2013, defining two distinct types of tenosynovial giant cell tumor: 1) Localized TGCT, previously known as giant cell tumor of the tendon sheath (GCTTS), and 2) Diffuse TGCT, formerly known nodular tenosynovitis and pigmented villonodular synovitis (PVNS). TGCTs are benign, though can grow and cause damage to the surrounding tissues. Symptoms can include pain, swelling and limitation of movement of the joint. Surgery is the main treatment option.
Figure 19:
Ulnar sided wrist mass in a patient with pain and swelling for 3-4 months. Soft tissue swelling was noted on radiographs (arrowheads) (19A). Coronal STIR (19B), sagittal T1-weighted (19C), axial T1-weighted (19D) and STIR (19E) MR images demonstrate a 2.2 x 1.4 x 1.0 cm soft tissue mass (arrowheads) deep to the skin marker, which extends from the proximal aspect of the pisotriquetral recess to the subcutaneous tissues, appearing hypointense on the STIR sequences and isointense to muscle on the T1 images. No significant surrounding edema or cystic components are seen. This was favored to represent tenosynovial giant cell tumor (TGCT) and excision was recommended.
Conclusion
Ulnar-sided wrist pain is a common complaint, and pisotriquetral lesions are a significant but under-recognized cause of these pains. MR imaging allows for visualization of the anatomic structures in and around the PT joint, which should be closely evaluated in the setting of ulnar sided wrist pain.
References
- Moraux A, et al. Pisotriquetral joint disorders: an under-recognized cause of ulnar side wrist pain. Skeletal radiology. 2014 Jun;43(6):761-73. ↩
- Pevny T, et al. Ligamentous and tendinous support of the pisiform, anatomic and biomechanical study. J Hand Surg (Am). 1995;20(2):299–304. ↩
- Theumann NH, et al. Pisotriquetral joint. Assessment with MR imaging and MR arthrography. Radiology. 2002;222(3):763–70. ↩
- Belliappa PP, et al. Excision of the pisiform in piso-triquetral osteoarthritis. J Hand Surg Br. 1992;17(2):133–6. ↩
- Seradge H, et al. Piso-triquetral pain syndrome after carpal tunnel release. J Hand Surg Am. 1989;14(5):858–62. ↩
- Lam KS, et al. Wrist function after excision of the pisiform. The Journal of Hand Surgery: British & European Volume. 2003 Feb 1;28(1):69-72. ↩
- Steinmann SP, et al. Pisotriquetral loose bodies. The Journal of hand surgery. 1997 Sep 1;22(5):918-21. ↩
- Pan T, et al. Uncommon carpal fractures. European Journal of Trauma and Emergency Surgery. 2016 Feb;42(1):15-27. ↩
- Chen WA, et al. An ulnar intraneural ganglion arising from the pisotriquetral joint: case report. J Hand Surg Am. 2011;36(1):65–7. ↩