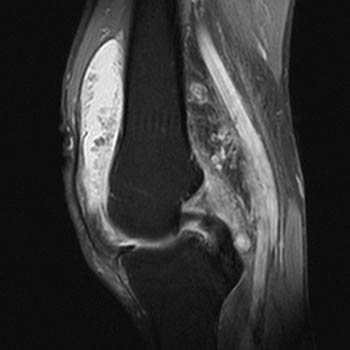
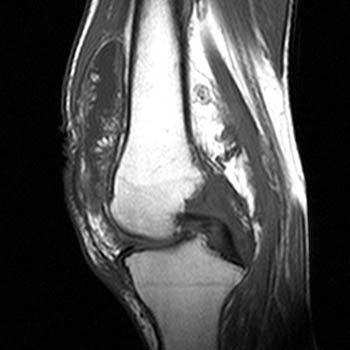
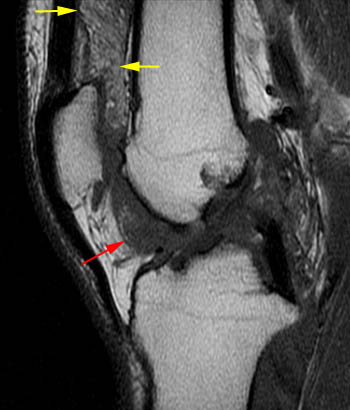
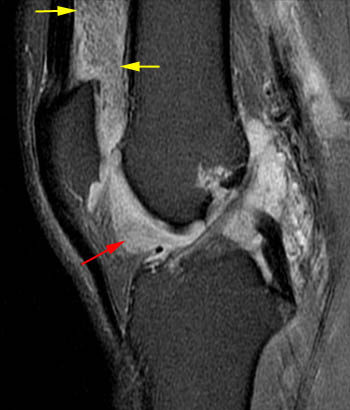
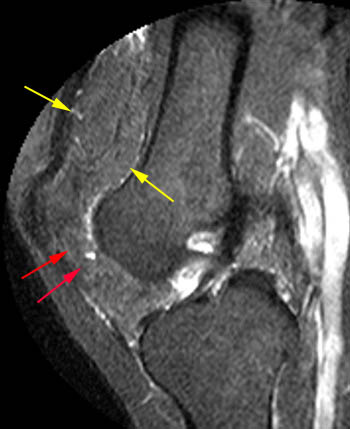
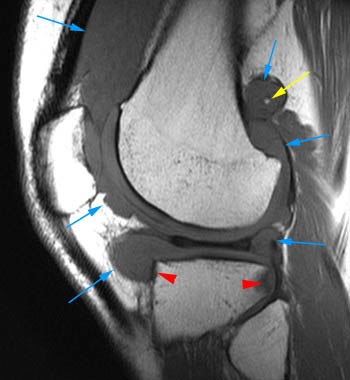
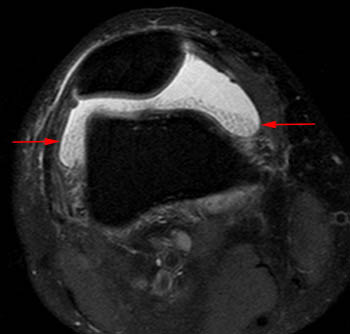
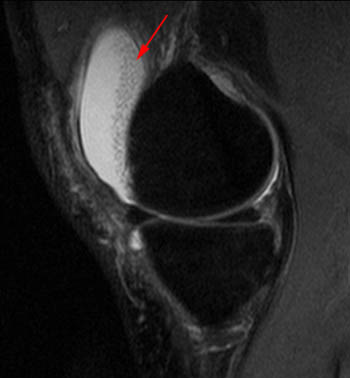
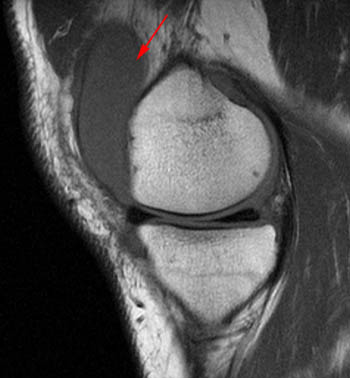
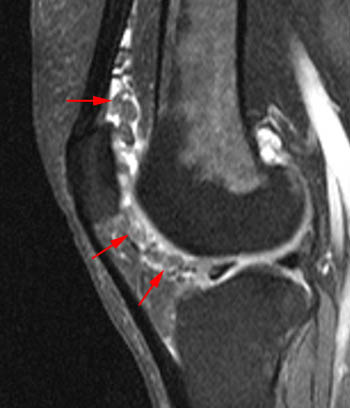
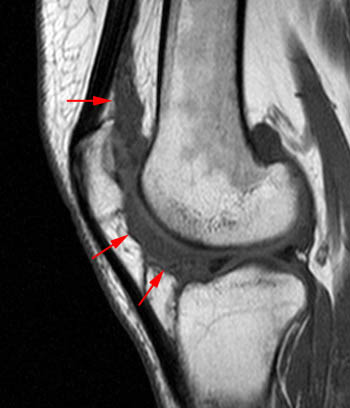
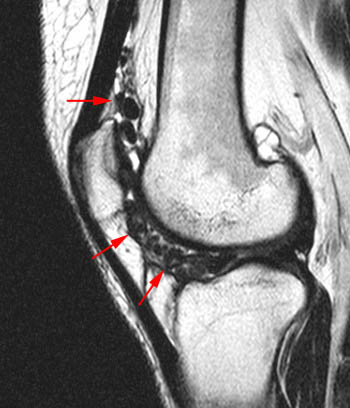
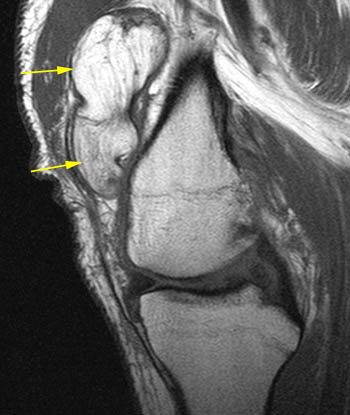
Clinical History: A 78 year-old male complains of a distal thigh mass for six months. MRI of the distal thigh was performed. Corresponding (1a) sagittal fat-suppressed proton density (PD FS) and (1b) T1-weighted images are presented. What are the findings? What is your diagnosis?
Findings
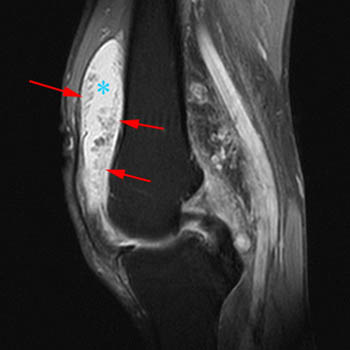
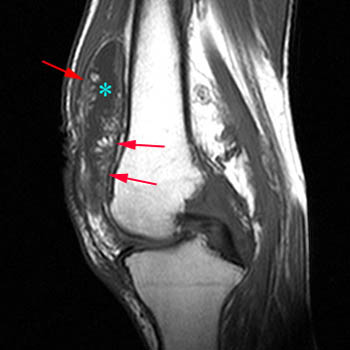
Figure 2:
(2a) The fat-suppressed proton density-weighted sagittal image demonstrates an large effusion (blue asterisk) distending the suprapatellar recess and outlining prominent frond-like tissue (red arrows) which projects inward. (2b) The frond-like tissue projecting into the joint has bright signal intensity on the T1-weighted sagittal image, compatible with fat.
Diagnosis
Villous lipomatous proliferation of the synovial membrane (lipoma arborescens).
Introduction
Lipoma arborescens is a “lipoma-like” benign villous proliferation of synovium with replacement of the subsynovial connective tissue by mature fat cells. It is not a neoplasm, but rather thought to be a nonspecific reactive response to chronic synovial irritation, whether from mechanical or inflammatory insults. Other terms that have been used in the literature include diffuse lipoma of the joint, diffuse synovial lipoma, diffuse articular lipomatosis, fatty infiltration of the synovial membrane, or villous lipomatous proliferation of the synovial membrane. The latter two emphasize the non-neoplastic nature of this lesion.
The condition is frequently described as rare, but imaging diagnosis was very difficult prior to the advent of MRI2. It turns out that mild subsynovial fatty infiltration is not uncommon, although more extensive lesions which acquire the term lipoma arborescens are less common. Patients are typically in the 5th – 7th decades, but lipoma arborescens also occurs in young patients with chronic arthritis. One report described men affected more often than women7, but a more extensive series showed no significant gender predilection11.
Associations
Lipoma arborescens is nearly always associated with underlying degenerative joint disease, chronic rheumatoid arthritis2,10, or prior trauma. An effusion is typically present, and can be produced by the lesion or from the underlying arthritis2. Rare cases of a primary lesion without an underlying chronic articular process have been reported. Some authors have proposed two separate categories of lipoma arborescens, an idiopathic “primary” type occurring in younger patients, and a much more common “secondary” type most often seen in elderly patients11. Lipoma arborescens is unilateral in most cases11 but bilateral lesions may be found in patients with underlying bilateral chronic arthropathy.
Pathology
The name lipoma arborescens reflects its gross appearance, that of a fatty mass with a branching villous growth pattern. Microscopically, there is synovial hyperplasia with scattered chronic inflammatory cells and abundant deposition of mature adipocytes in the subsynovial tissue5. The adipocytes are accompanied by nutrient blood vessels and are covered by several layers of synovial cells. Synovium responds to irritation by increased capillary blood flow, influx of inflammatory cells, and synovial proliferation. As this becomes chronic, fat cells may also infiltrate the subsynovial tissue.
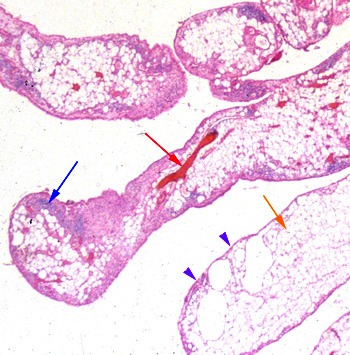
Figure 4:
Lipoma arborescens, pathology slide. Synovial villi enlarged by abundant mature adipocytes (orange arrow). Note the variable degrees of fatty infiltration of the subsynovial tissues. The synovial layer is only a few cells thick (purple arrowheads). Capillaries (red arrow) and small amounts of chronic inflammatory cells (blue arrow) are present. [Image courtesy of John F Carroll, MD]
MRI diagnosis
MRI demonstrates frond-like areas projecting inward from the synovium with signal equal to fat on all imaging sequences. If intravenous Gadolinium contrast is administered, enhancement can be seen of the chronically inflamed overlying synovium, but no enhancement is seen in the underlying fat. The fatty proliferation may be of such degree that it forms a mass, but mild cases with a pattern of diffuse villous proliferation are much more common. Villi may be small and feathery in appearance or they may be more bulky fatty lobules. Osseous erosions have been reported secondary to lipoma arborescens8, although when present they are more often due to underlying arthritis.
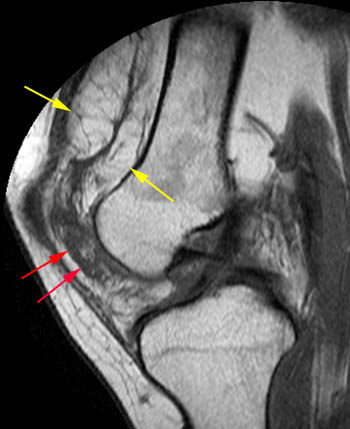
Figure 5:
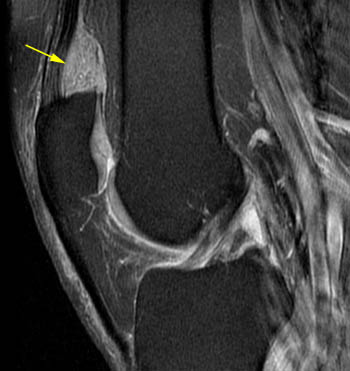
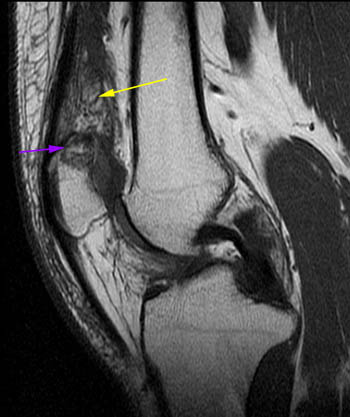
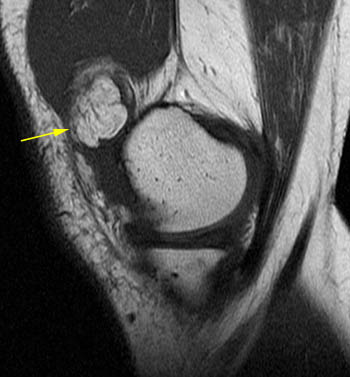
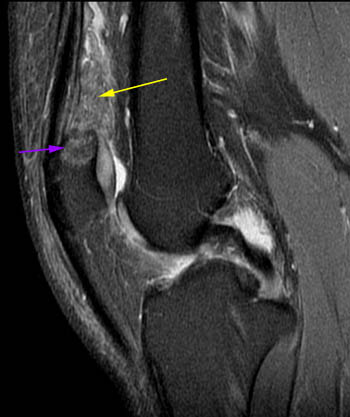
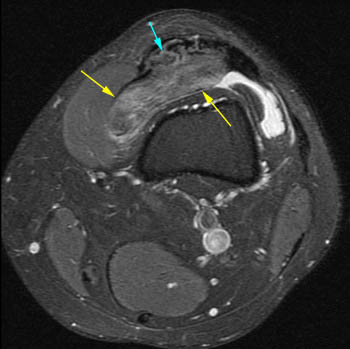
Lipoma arborescens. 42 year old with posterior left knee pain. (5a) A sagittal T1-weighted image demonstrates a large primarily fat-signal mass-like area (yellow arrows) filling much of the suprapatellar bursa. The innumerable individual villi are small in this case, with small quantities of interposed fluid, creating a feathery appearance. (5b) An area posterior to the infrapatellar fat pad which resembles fluid on the T1-weighted sequence has intermediate signal on the sagittal PD FS sequence, compatible with an area of hypertrophic synovium little or no fat deposition (red arrows). When lipoma arborescens develops in patients with chronic synovitis, patients also often have such areas of synovial thickening without fat deposition. (5c) Axial PD FS MR image showing the large feathery-appearing lipoma arborescens filling the suprapatellar recess.
Figure 6:
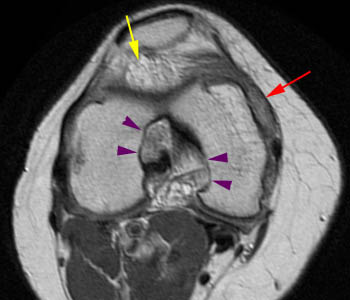
Lipoma arborescens. 35 year-old female with a history of rheumatoid arthritis. (6a) The T1-weighted sagittal image demonstrates severe mass-like hypertrophy of subsynovial fat (yellow arrows), primarily in the suprapatellar recess. In this patient, the villi are primarily larger and more rounded, forming lobules. (6b) The low to intermediate signal intensity between the areas of high signal fat on the T1 weighted images (red arrows) is low in signal on the corresponding STIR sagittal image, indicating that this is not fluid. This is chronic "burned out" synovitis or fibrous pannus which remains in the suprapatellar recess, adjacent to the infrapatellar fat pad, and medial to the medial femoral condyle. (6c) The axial PD FSE image shows intercondylar notch widened by chronic erosions (purple arrowheads), compatible with juvenile chronic arthritis (JCA) during childhood. Each of these findings was also present in the opposite knee (not shown).
Figure 7:
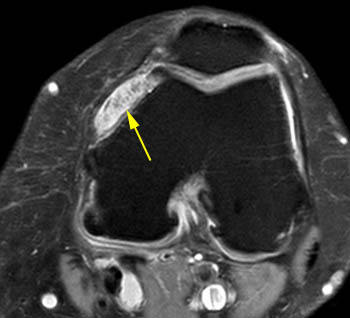
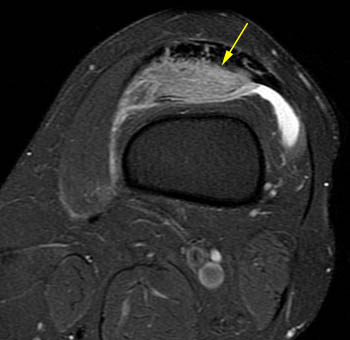
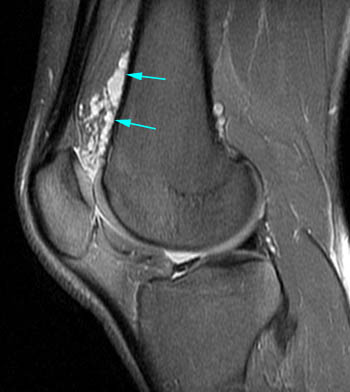
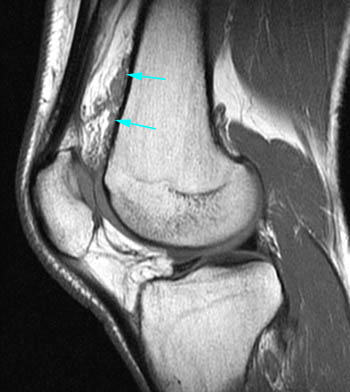
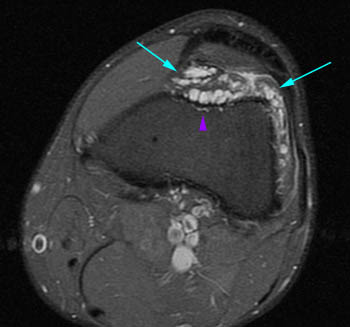
Lipoma arborescens. 61 year-old male with worsening chronic diffuse knee pain. (7a) A sagittal T1-weighted image demonstrates severe medial compartment osteoarthritis with marginal osteophytes, subchondral changes, and an extensive complex tear of the medial meniscus (red arrows). Mild villous frond-like fatty subsynovial hyperplasia (yellow arrow) is present in the suprapatellar bursa. (7b) The axial fat-suppressed proton density-weighted image confirms the villous tissue outlined by joint fluid. Cases like this are much more frequent than those manifesting as large fatty masses.
Differential diagnosis on MRI
Lipoma arborescens has characteristic features that usually make it a straightforward MRI diagnosis. However, other entities occurring as filling defects in the suprapatellar recess may cause confusion.
Small filling defects outlined by effusion in the suprapatellar bursa are most obvious on sequences where fluid is bright (such as T2-weighted or fat-suppressed proton-density imaging sequences). Correlation with T1-weighted images allows us to better assess the nature of this tissue. Findings which remain isointense to fat on all imaging sequences are reliably confirmed as fat. If in addition a sclerotic peripheral rim is present, the appearance is typical for osseous loose bodies.
Figure 8:
Osseous loose bodies / secondary osteochondromatosis from underlying severe osteoarthritis. An osseous loose body (red arrow) is located anteriorly, projecting into the posterior margin of the infrapatellar fat pad. This exhibits high T1 signal intensity from fatty marrow content. It has a thin surrounding cortex. A smaller loose body with less fat content is located posteriorly and one with very little fatty marrow is located superiorly (purple arrows). Large osteophytes project from the patella and femur. Severe chondral loss and associated subchondral degenerative changes (blue arrowheads) are evident at the patellofemoral joint.
If signal is intermediate on T1-weighted images, the tissue may be hyaline cartilage, such as from synovial chondromatosis. In this condition, multiple nodules of hyaline cartilage form in subsynovial connective tissue. The small lobules of hyaline cartilage may calcify centrally, forming areas with numerous punctate foci of very low signal. The cartilage is distributed throughout the joint, within the suprapatellar recess as well as low anterior and posterior locations, including within Baker’s cysts. Osseous erosions are often present.
Figure 9:
Primary synovial chondromatosis. 36 year-old male with chronic knee pain and locking. (9a) Innumerable small chondral bodies (blue arrows) throughout the joint are outlined by fluid on the fat-suppressed proton density images. (9b) The T1-weighted sagittal image shows no fat content except for a single tiny focus (yellow arrow) located in a posterior chondral body, from developing ossification. Small erosions (red arrowheads) are forming at the posterior and anterior margins of the lateral tibial plateau. (9c) A popliteal cyst is also markedly distended by chondral bodies, several of which demonstrate central calcification (purple arrows).
Intermediate signal intensity can also be seen with fibrinous tissue, such as “rice bodies” which may accompany rheumatoid arthritis. These are typically very small in size and numerous. Dependent positioning reflects that they are free in the joint rather than fixed to the synovium.
Figure 10:
41 year-old male with medial knee pain. (10a and 10b) Fat-suppressed proton density axial and sagittal images demonstrate numerous tiny intermediate signal nodules (red arrows), layering dependently, outlined by joint fluid. (10c) The T1-weighted image demonstrates no fat signal in the tiny bodies, which are made up of fibrinous tissue and cannot be distinguished from fluid on this sequence (red arrow shows corresponding location). The dependent layering indicates that these are mobile particles rather than affixed to the synovium.
Very low signal on all imaging sequences may indicate the presence of calcium. Numerous small foci of calcification are often seen in synovial chondromatosis.
Low to intermediate signal intensity on T1-weighted images and low signal intensity on T2-weighted or gradient echo sequences is more often seen with hemosiderin deposition. Variable quantities of hemosiderin are deposited heterogeneously in larger areas in pigmented villonodular synovitis (PVNS) or hemosiderotic synovitis (such as from trauma or hemophilia). Hemosiderin deposition can also often be found in rheumatoid arthritis.
Figure 11:
Pigmented villonodular synovitis. (11a) Extensive villonodular synovial proliferation (red arrows) throughout the knee, outlined by joint fluid, with low signal intensity from hemosiderin. Involvement of the suprapatellar recess, the infrapatellar fat pad, and posteriorly. Note that on the fat-suppressed proton density-weighted image, the signal intensity is moderately low in the lesion. Since it is isointense to fat, this can be misleading. (11b) Correlation with the T1-weighted sequence shows that this is clearly not fat. (11c) The T2-weighted image demonstrates very low signal intensity, compatible with hemosiderin. Knee MRI studies performed without a T2 weighted sequence may be misleading in this assessment, since the signal is not very low on the proton density images. Correlation with scout gradient echo images is sometimes helpful in confirming low signal.
It may be difficult to determine if an edematous fatty mass located anteriorly is projecting into the suprapatellar recess or if it is the quadriceps fat pad itself. An edematous fat pad may develop from quadriceps fat pad impingement (see prior MRI Web Clinic of September 2008). With chronic mechanical impingement and inflammation, the fat pad may hypertrophy, causing an appearance compatible with lipoma arborescens.
Figure 12:
Quadriceps fat pad impingement. 52 year-old male with knee pain and swelling. (12a, 12b, 12c) T1-weighted sagittal and fat-suppressed proton density sagittal and axial images demonstrate an edematous quadriceps fat pad (yellow arrow), most likely from fat pad impingement. It is difficult to distinguish whether the edematous fatty tissue is only in the fat pad, or if there may be fatty synovial hyperplasia projecting into the joint.
Figure 13:
Quadriceps fat pad impingement and lipoma arborescens. 44 year-old male with medial knee pain. (13a) A fatty mass compatible with lipoma arborescens (yellow arrows) projects into the suprapatellar bursa and is contiguous with the quadriceps fat pad. This has a feathery appearance on the T1-weighted images near midline. (13b) A more medially positioned T1-weighted image shows a more mass-like appearance. (13c and 13d) Fat-suppressed sagittal and axial proton density images show both areas to be edematous from impingement. Secondary changes in the upper margin of the patella (purple arrow). (13d) Edema is also found in the adjacent portion of the quadriceps tendon (blue arrow). Chicken or egg? Chronic impingement causes fatty hypertrophy. Fatty hypertrophy causes mechanical impingement.
Synovial hemangioma (venous malformation) is an uncommon lesion which may be intraarticular or extraarticular. It has a characteristic appearance that may at first glance be confused with lipoma arborescens. However, the signal intensities are reversed – the lobulated lesions are bright on fat-suppressed images, but lower in signal on T1-weighted images. Venous malformations are comprised of low-flow serpiginous vessels with signal intensity typical of fluid. These are separated by small amounts of fat. Calcified phleboliths may be also present.
Figure 14:
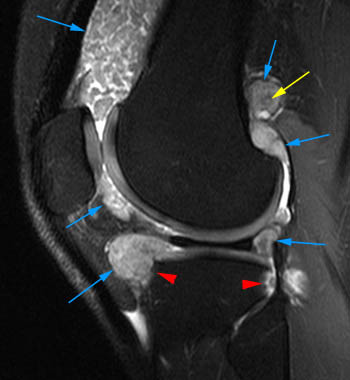
Synovial hemangioma (venous malformation).(14a) Sagittal fat-suppressed proton density-weighted image demonstrates an appearance typical of a venous malformation, with serpiginous vessels of fluid signal intensity (blue arrowheads). Signal voids that are seen with high-flow vessels are not present. (14b) The lesion is surrounded by prominent prefemoral fat, resembling lipoma arborescens on this T1-weighted image. However, rather than anteriorly positioned fat projecting into a joint and being outlined by fluid, the similar appearance is produced by the converse, a posteriorly positioned serpiginous fluid-filled mass projecting anteriorly, outlined by prefemoral fat. (14c) The hemangioma has slight intra-osseous involvement beneath the anterior femoral cortex (purple arrowhead) as seen on this axial fat-suppressed proton density-weighted image.
A true intraarticular lipoma is a rare lesion characterized by a localized rounded mass of adipose tissue rather than multiple villi. There is no associated synovial proliferation, but rather a thin fibrous capsule. Intraarticular lipomas can be sessile or pedunculated.
Figure 15:
Intraarticular lipoma. A large rounded fatty mass (yellow arrows) is found in the medial portion of the suprapatellar recess on this T1-weighted image. Unlike lipoma arborescens, it is not comprised of small lobules or villi. A lipoma had been resected from this site many years earlier and this lesion was recurrent. Mild fibrosis at the upper margin is from prior surgery.
Intraarticular liposarcoma is a rare lesion which we have not encountered in our practice. Liposarcomas occur in two main forms, most commonly low grade myxoid liposarcoma, found in young adults, and less commonly high grade pleomorphic liposarcoma, found in older patients. Liposarcomas are typically found proximal to the knee or elbow, with high grade lesions most often found in the buttocks, abdomen, or groin. Low grade lesions are well-differentiated and have high fat content. One case report3 described a mass in the knee which resembled a lipoma on MRI and at arthroscopy. Histologically they found a low grade myxoid liposarcoma. They concluded that all lipomas at unusual sites, such as the knee, should be investigated for possible malignancy. Another case report9 described a high-grade pleomorphic intra-articular liposarcoma of the knee. The MRI showed a lesion more closely resembling PVNS, with multifocal nodules anteriorly and posteriorly. These had intermediate signal, not matching fat, and thus should not be mistakenly diagnosed as lipoma arborescens.
Other Locations
Although lipoma arborescens is most often found at the suprapatellar recess of the knee, it can occur wherever there is synovium. It occurs in other joints and bursae (hip, shoulder, wrist, elbow), and more rarely in the tendon sheaths (a few reports in tendon sheaths at the ankle and one at the wrist – usually with accompanying involvement of the adjacent joint)4. We have encountered several in the shoulder, both in the joint and in the subacromial-subdeltoid bursa. As with previously reported cases in the shoulder6, nearly all of our patients had chronic rotator cuff tears.
Figure 16:
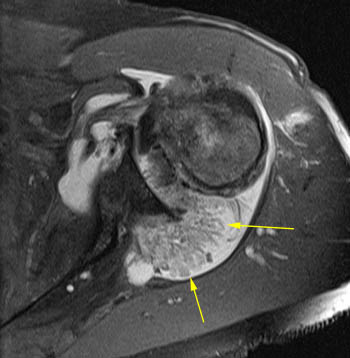
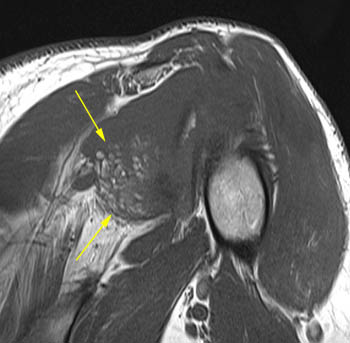
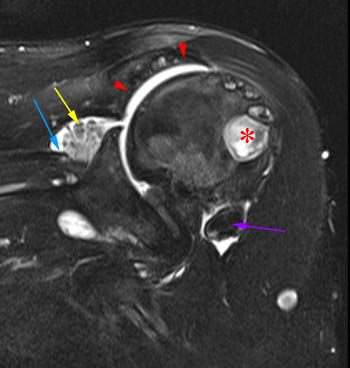
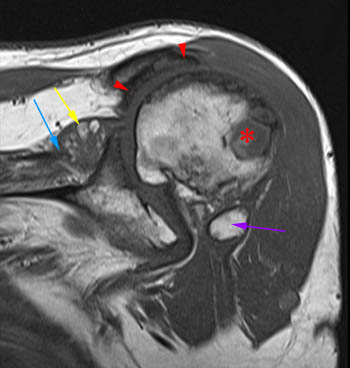
Lipoma arborescens of the shoulder. 56 year-old male with chronic bilateral shoulder pain. (16a) Axial gradient echo sequence shows abundant feathery tissue projecting into the joint. (16b) A posteriorly positioned coronal T1-weighted image shows the tissue to be fatty in nature. Coronal fat-suppressed T2-weighted (14c) and T1-weighted (16d) images.A chronic massive full thickness tear (blue arrow), with severe glenohumeral hyaline cartilage loss and remodeling of the undersurface of the acromion (red arrowheads) from chronic superior humeral subluxation (cuff arthropathy). A large effusion, fatty villous synovial hyperplasia (yellow arrows), and at least one large osseous loose body (purple arrow) are present. A large fibro-osseous cyst is also noted in the greater tuberosity (*).
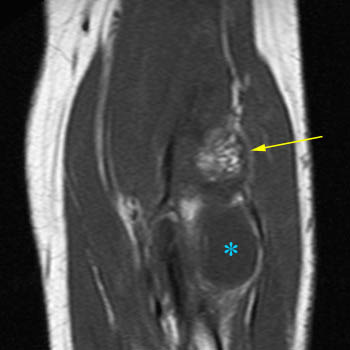
Figure 17:
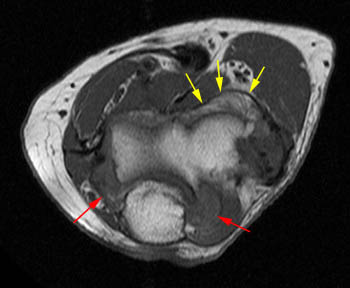
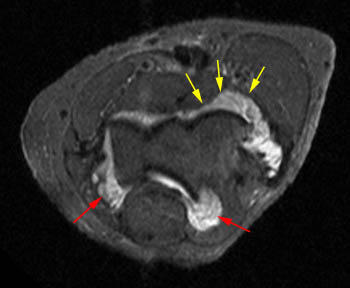
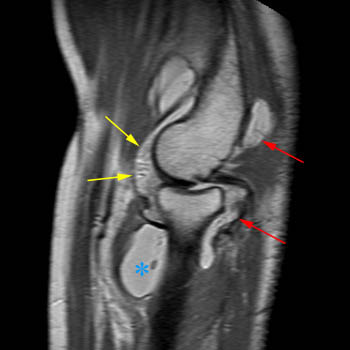
Lipoma arborescens of the elbow. 66 year-old female with chronic elbow pain. A fatty feathery-appearing mass is seen anterior to the capittelum on T1-weighted (17a) and fat-suppressed proton density-weighted (17b) axial images. (17b) Synovitis without fat deposition (red arrows) is seen posteriorly. (17c) A large effusion (blue asterisk) is present, helping to outline lipoma arborescens (yellow arrows) anterior to the capitellum. The water-weighted sequences nicely outline the areas of synovial hypertrophy, but the T1-weighted images reveal the different tissue content of the areas. (17d) Coronal T1-weighted image.
Significance
Lipoma arborescens most often develops in the setting of chronic underlying arthritis. The underlying arthritis is the primary problem requiring treatment and the subsynovial fatty proliferation is a usually a secondary feature. In patients without underlying arthritis, this may rarely be a primary process and the cause of recurring effusions, or a marker of underlying chronic synovitis. If large or mass-like, lipoma arborescens can cause pain or limit range of motion. When found on MRI exams, this benign process should not be mistaken for liposarcoma.
Treatment
When indicated, synovectomy can be curative1. However, if underlying chronic arthritis remains, recurrence is possible.
Conclusion
Villous subsynovial lipomatous proliferation is an uncommon response to chronic synovial irritation, whether mechanical or inflammatory in nature. It is typically found in chronically arthritic joints, most often in the suprapatellar recess of the knee, but also in other joints, bursae, and even tendon sheaths. Occasionally this process becomes mass-like and more deserving of the term lipoma arborescens. Features on MRI are distinctive. Many radiologists, rheumatologists, and orthopaedic surgeons will encounter this in their practice and should not mistake it for neoplasm or other pathology.
References
1 Blais RE, LaPrade RF, Chaljub G, Adesokan A. The arthroscopic appearance of lipoma arborescens of the knee. Arthroscopy 1995;11(5):623-627.
2 Coll JP, Ragsdale BD, Chow B, Daughters TC. Best Cases from the AFIP: Lipoma Arborescens of the Knees in a Patient with Rheumatoid Arthritis. Radiographics 2011 Mar-Apr;31(2):333-7.
3 Khan AM, Cannon S, Levack B. Primary Intra-Articular Liposarcoma of the Knee. Case Report. J Knee Surg 2003 Apr;16(2):107-9.
4 Moukaddam H, Smitaman E, Haims AH. Lipoma arborescens of the peroneal tendon sheath. J Magn Reson Imaging 2011 Jan;33(1):221-4.
5 Murphey MD, Carroll JF, Flemming DJ, Pope TL, Gannon FH, Kransdorf MJ. From the archives of the AFIP: benign musculoskeletal lipomatous lesions. Radiographics 2004 Sep-Oct;24(5):1433-66.
6 Nisolle J, Blouard E, Bardrez V, Boutsen Y, De Cloedt P, Esselinckx W. Subacromial-subdeltoid lipoma arborescens associated with a rotator cuff tear. Skeletal Radiol 1999;28(5):283-285.
7 O’Connell JX. Pathology of the Synovium. Am J Clin Pathol 2000;114:773-784.
8 Ryu KN, Jaovisidha S, Schweitzer M, Motta AO, Resnick D. MR imaging of lipoma arborescens of the knee joint. AJR Am J Roentgenol 1996 Nov;167(5):1229-32.
9 Shaerf DA, Mann B, Alorjani M, Aston W, Saifuddin A. High-grade intra-articular liposarcoma of the knee. Skeletal Radiol 2011 Mar; 40(3):363-5.
10 Weston WJ. The intra-synovial fatty masses in chronic rheumatoid arthritis. Br J Radiol 1973;46:213-216.
11 Vilanova JC, Barceló J, Villalón M, Aldomà J, Delgado E, Zapater I. MR imaging of lipoma arborescens and the associated lesions. Skeletal Radiol 2003 Sep;32(9):504-9. Epub 2003 Jun 17.