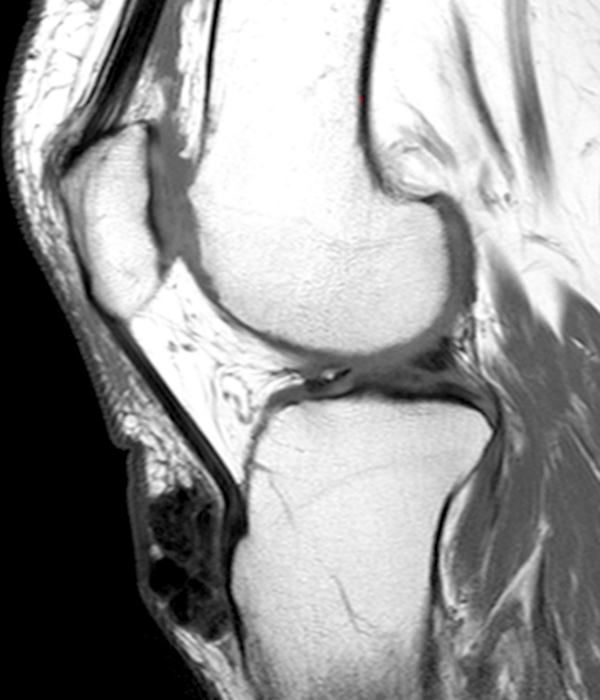
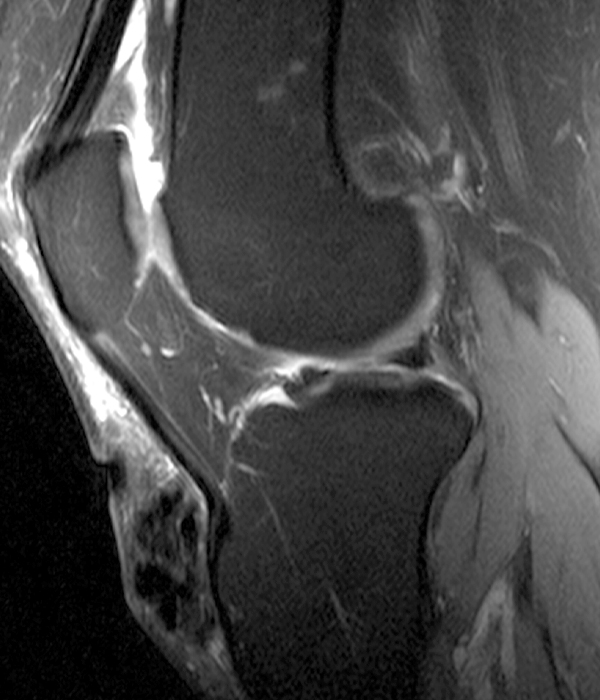
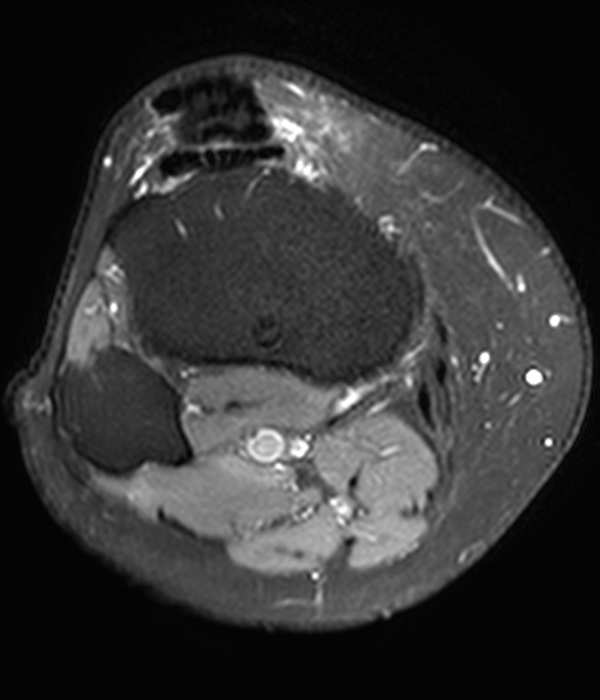
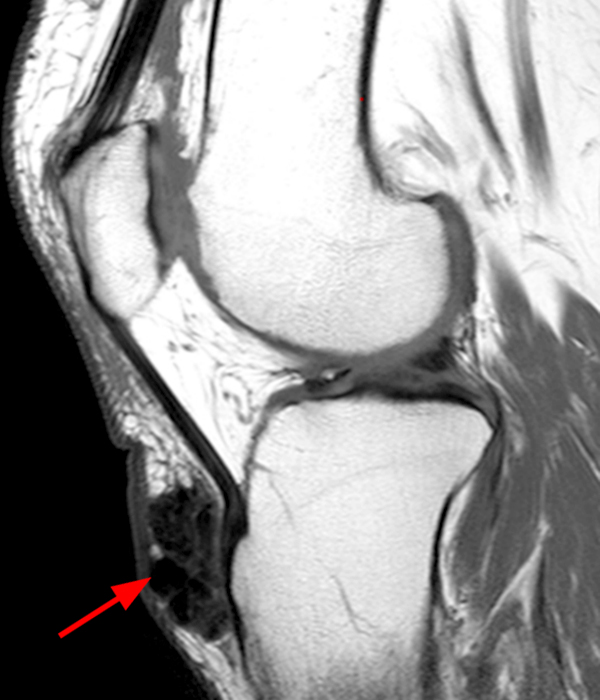
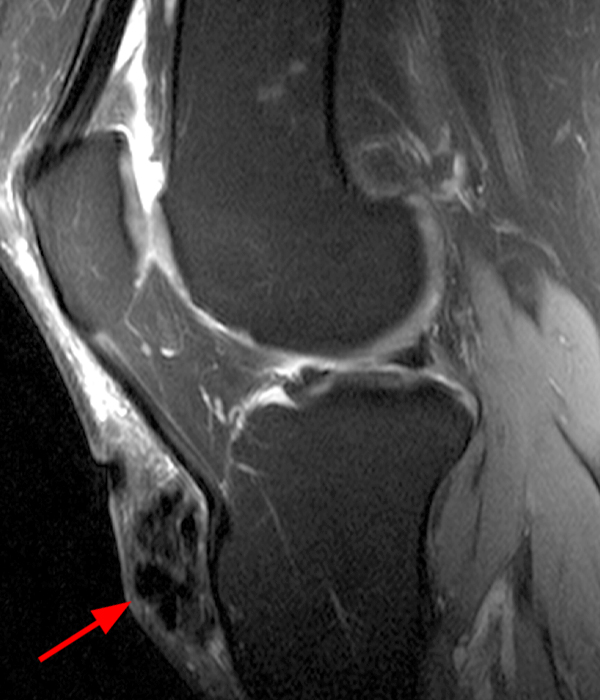
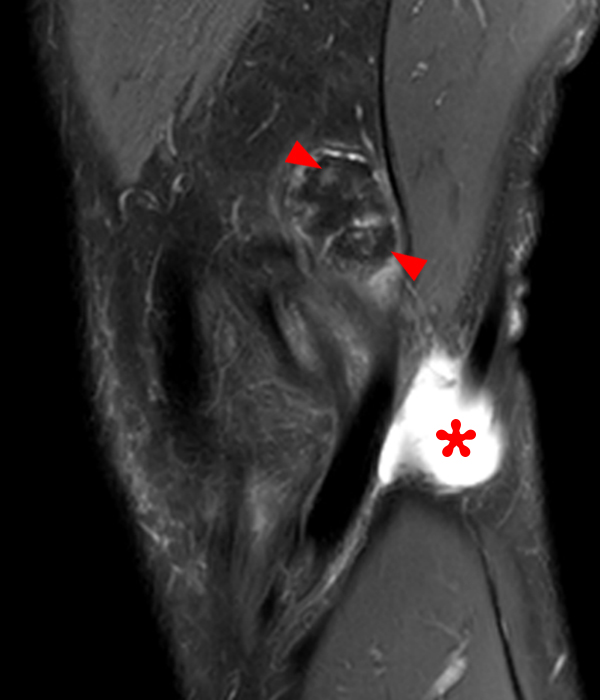
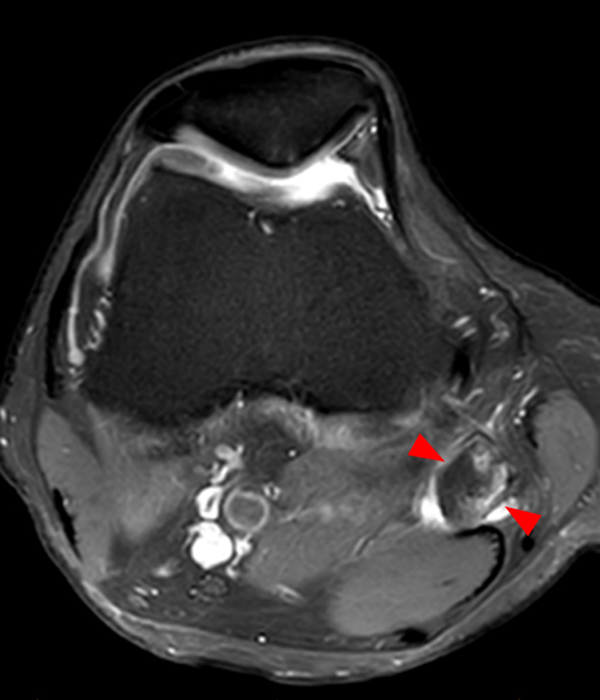
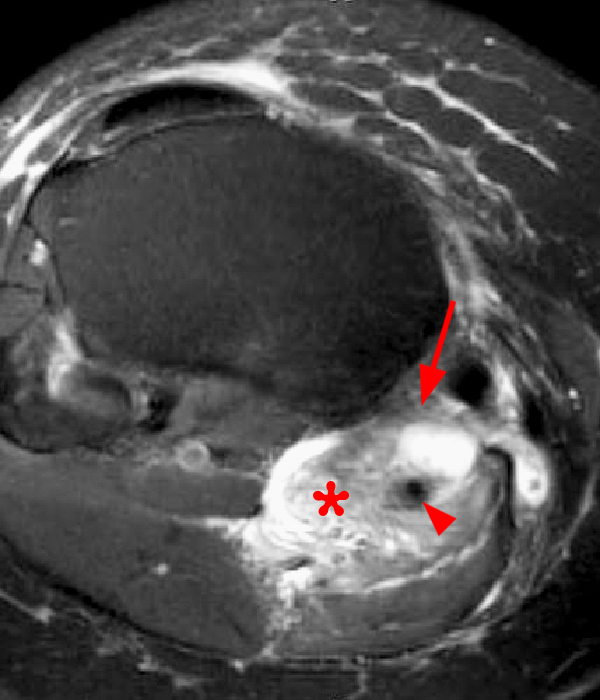
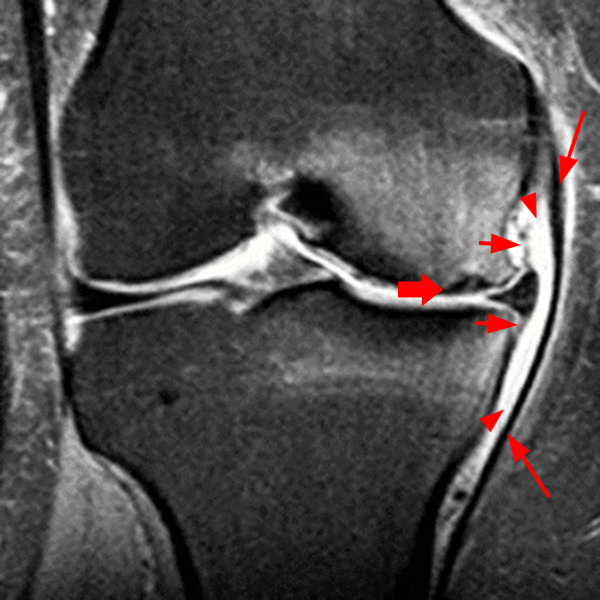
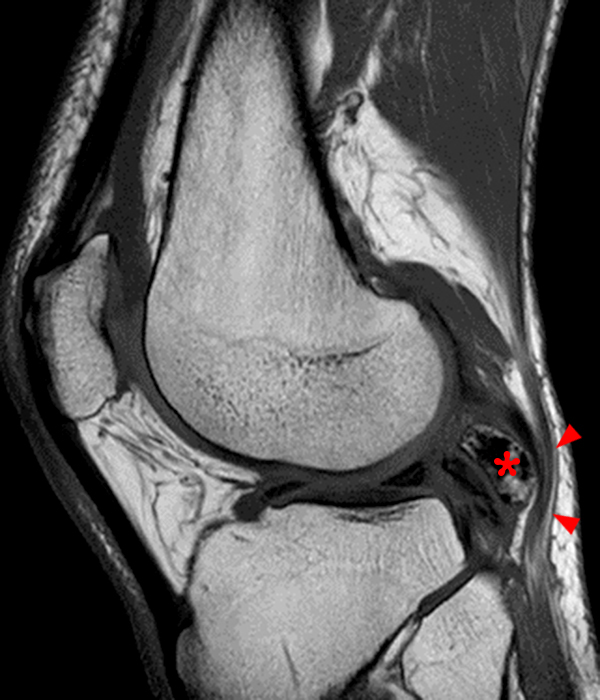
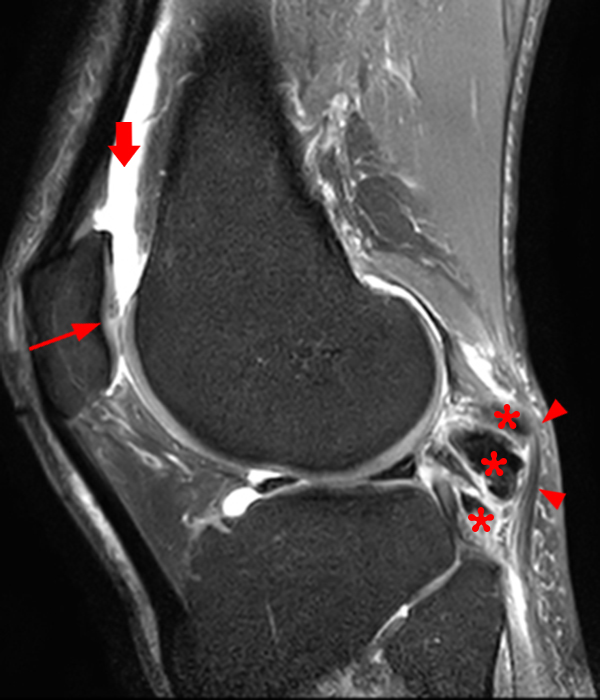
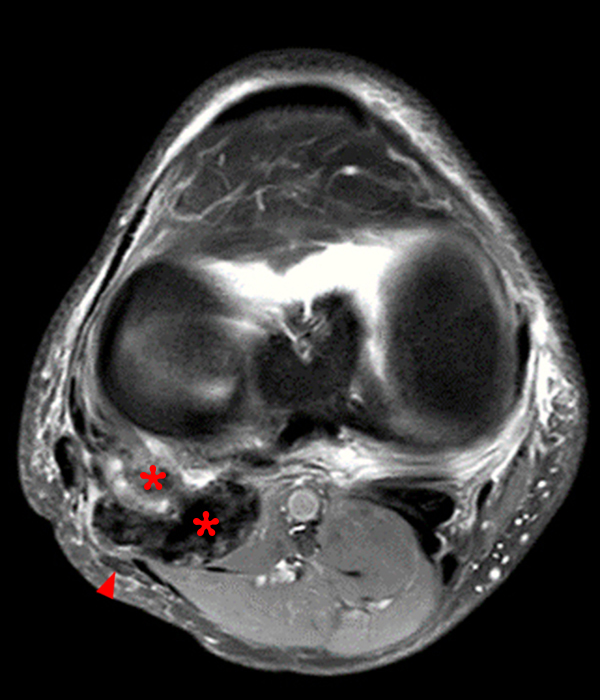
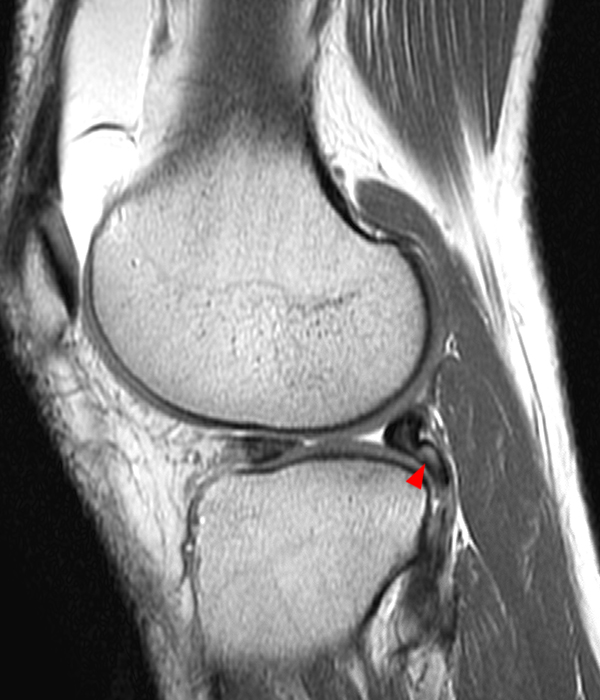
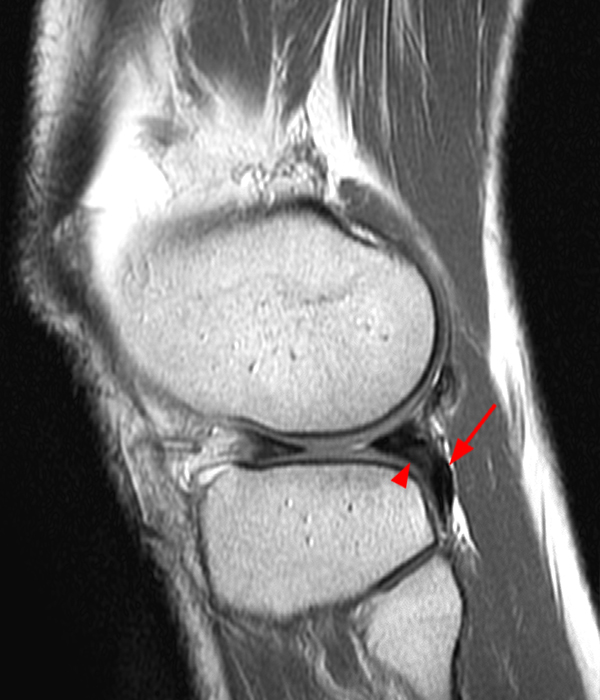
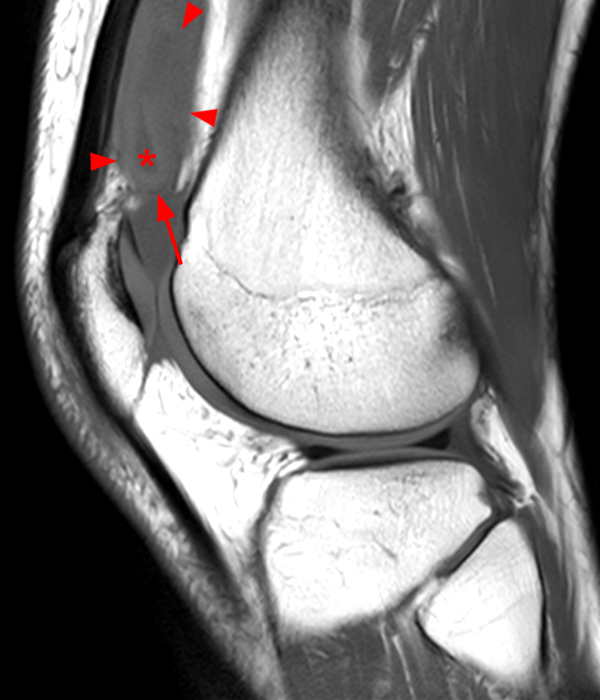
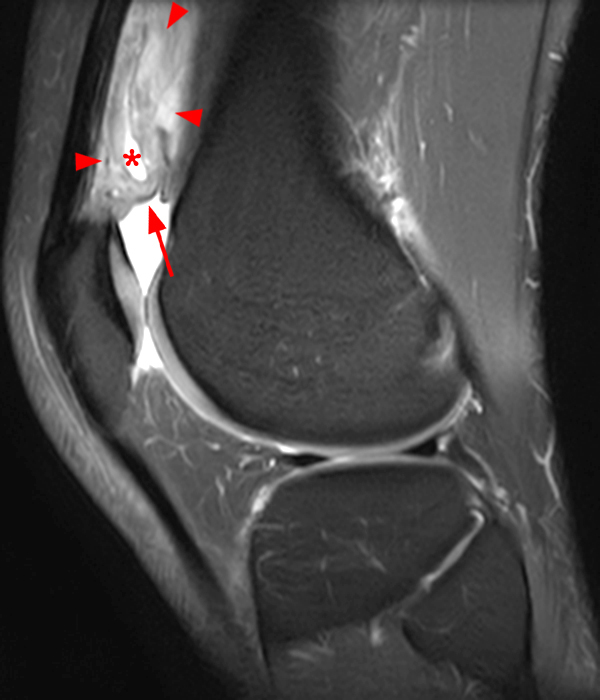
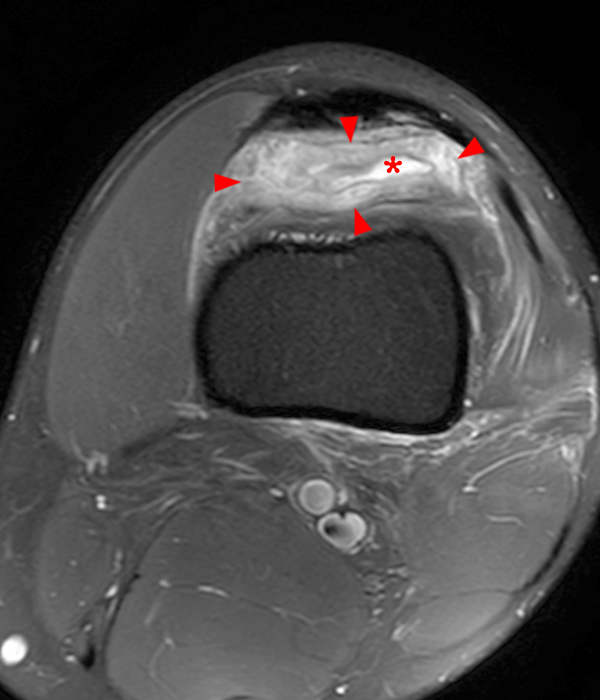
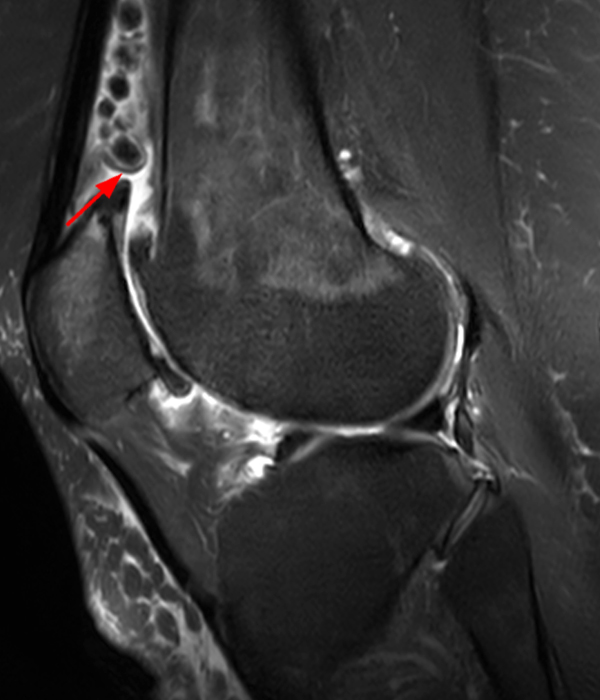
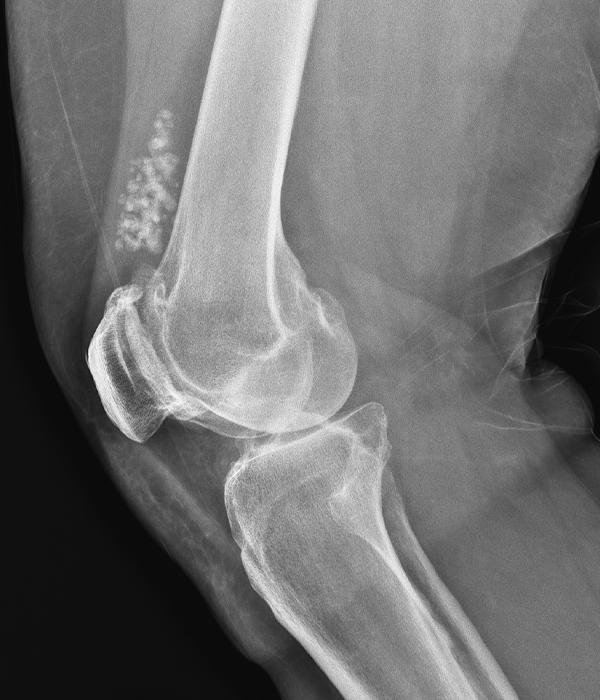
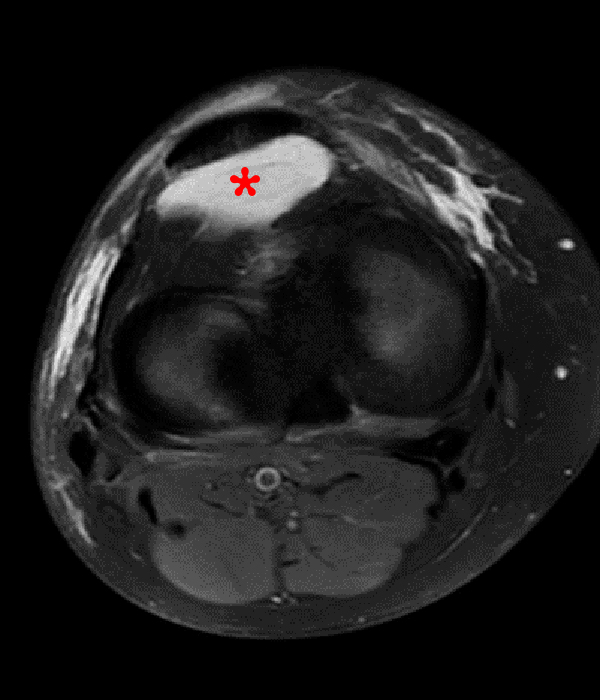
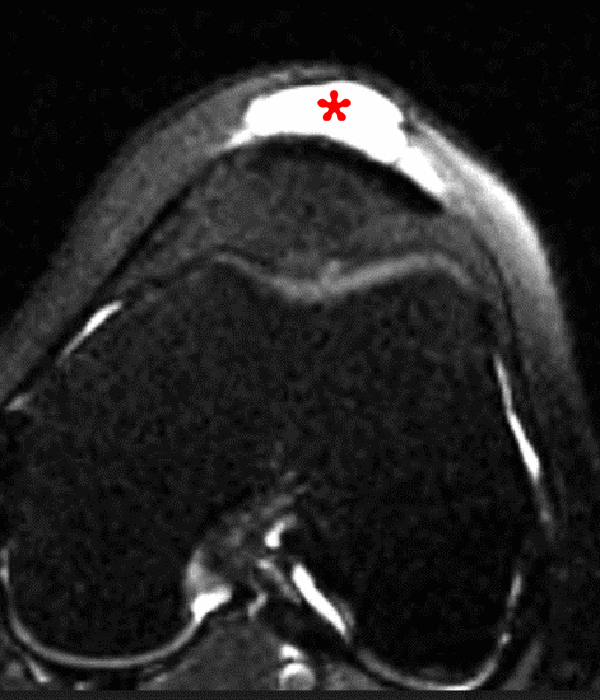
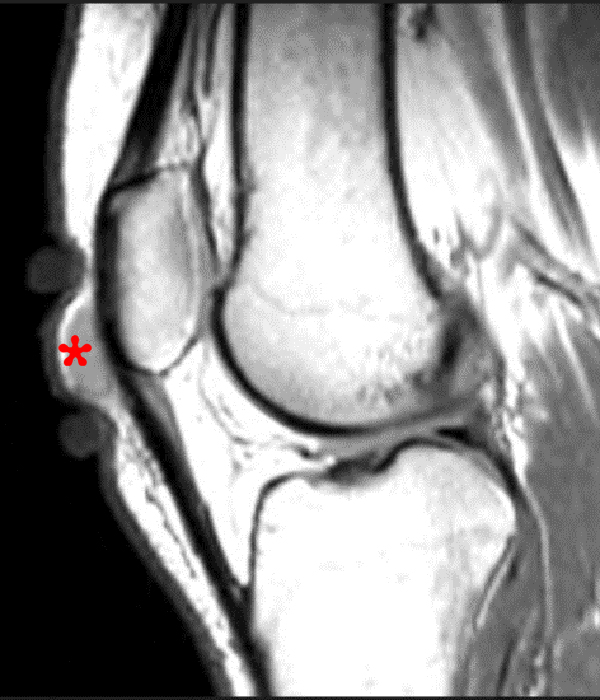
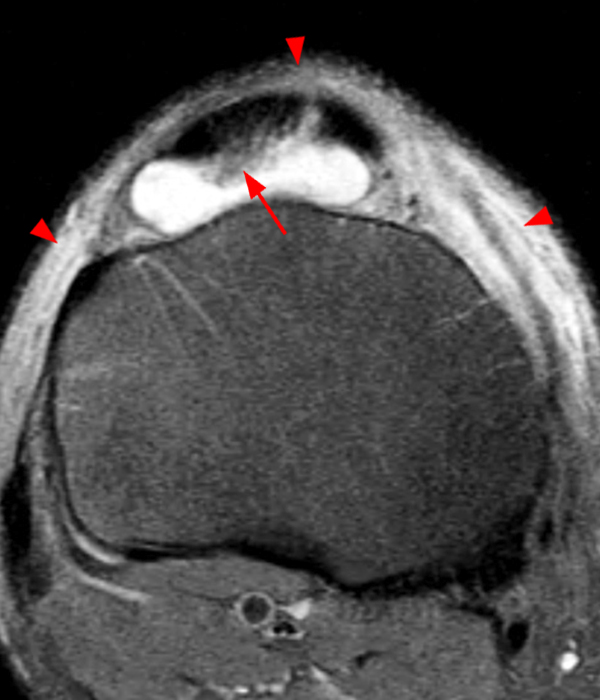
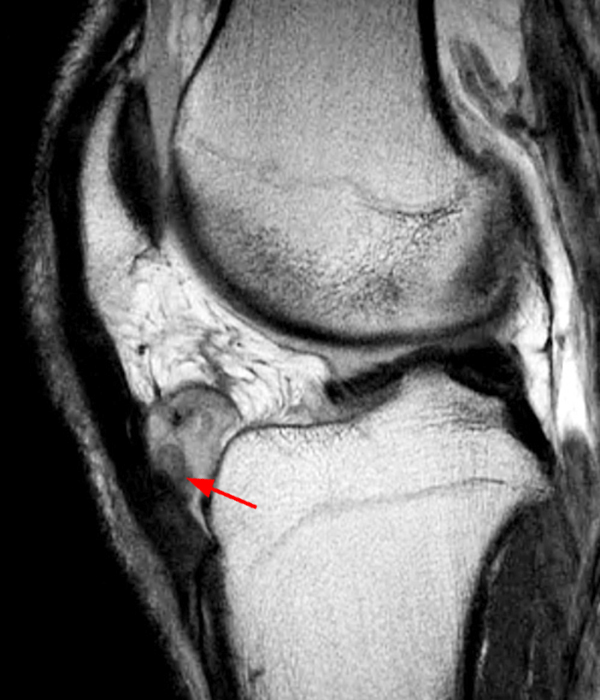
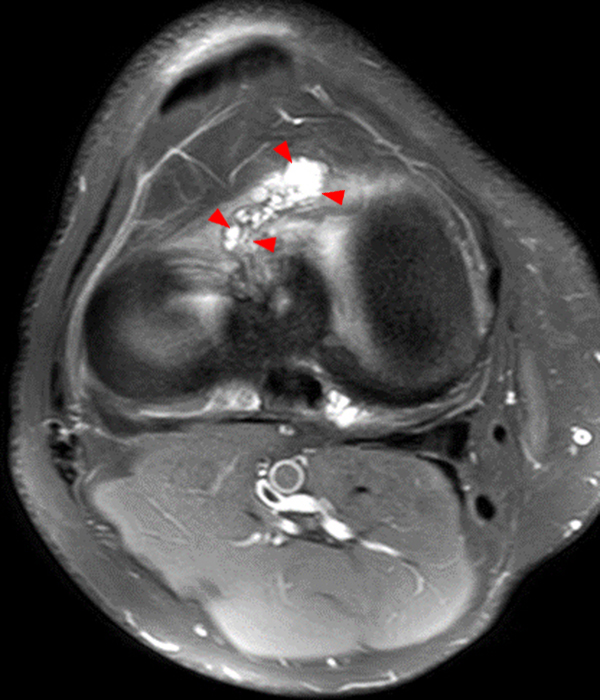
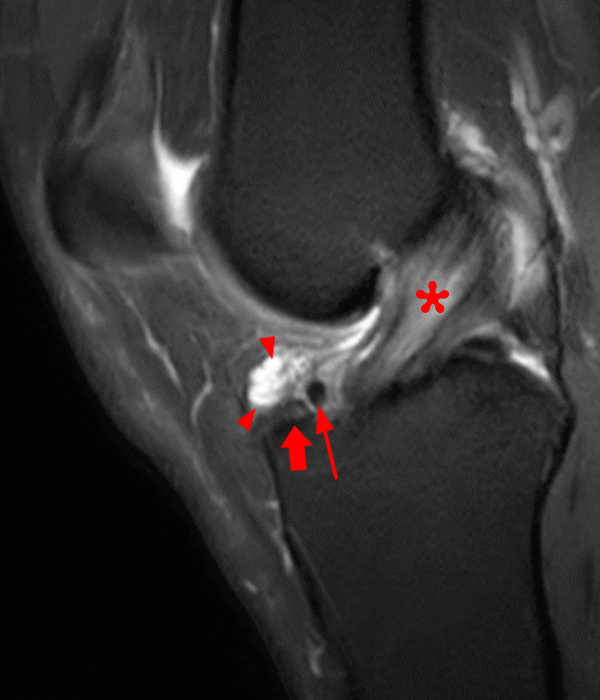
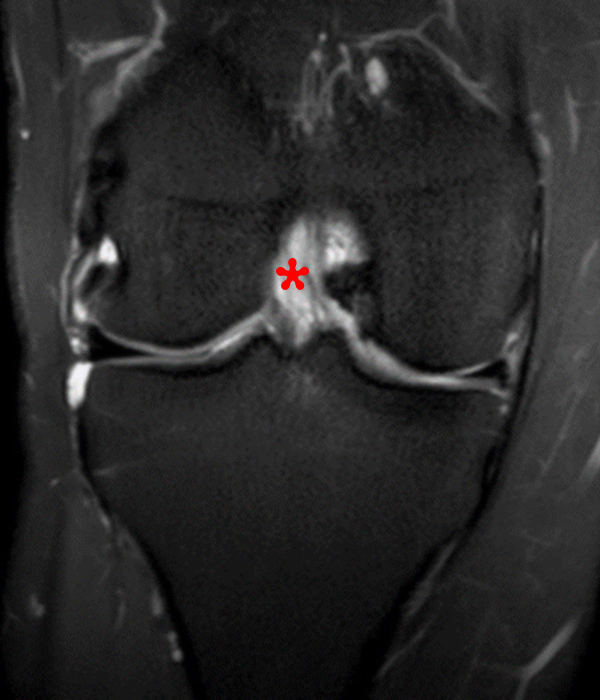
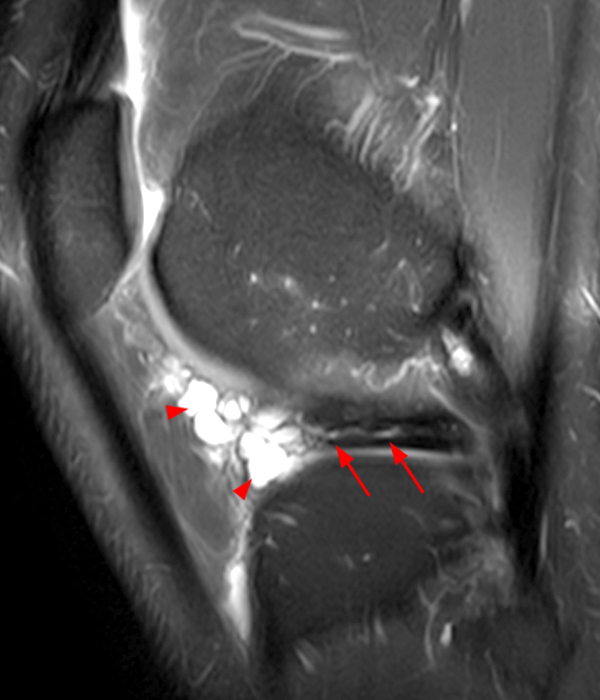
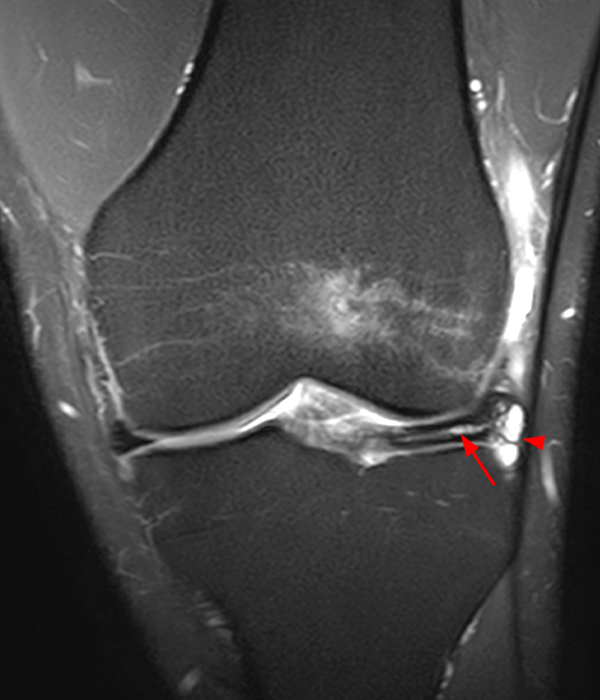
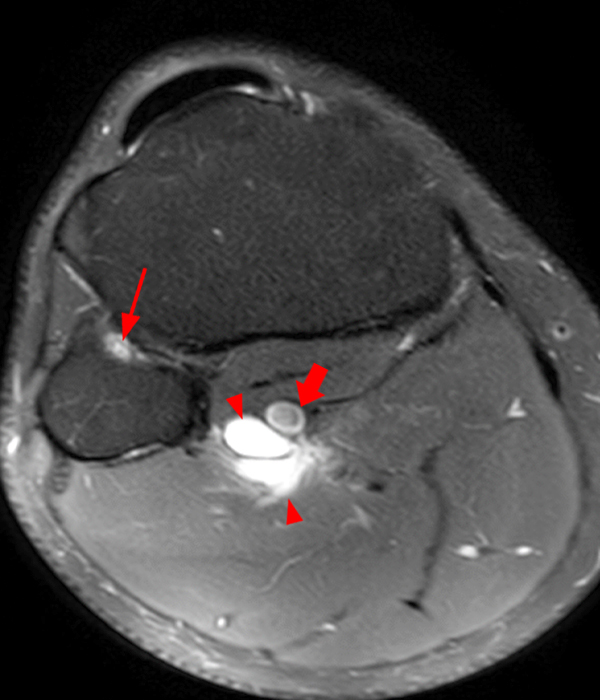
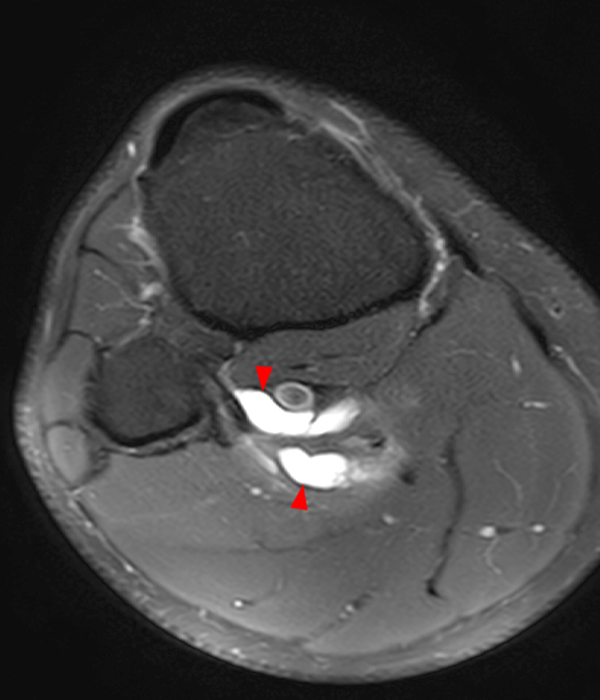
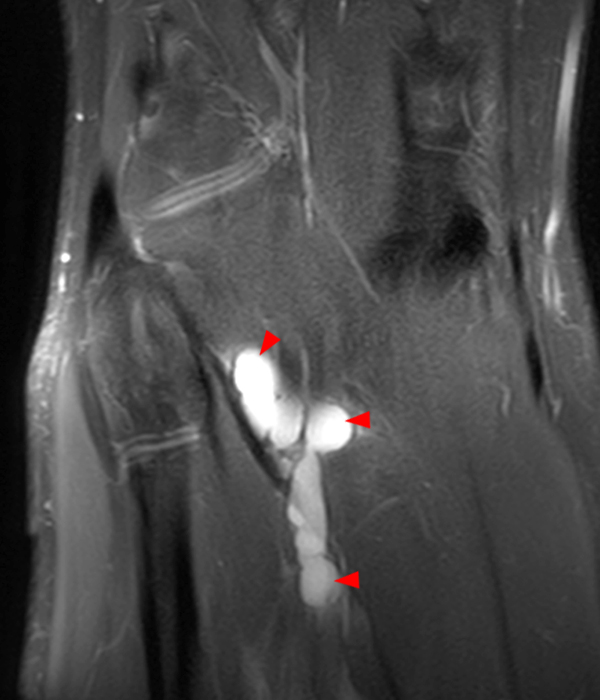
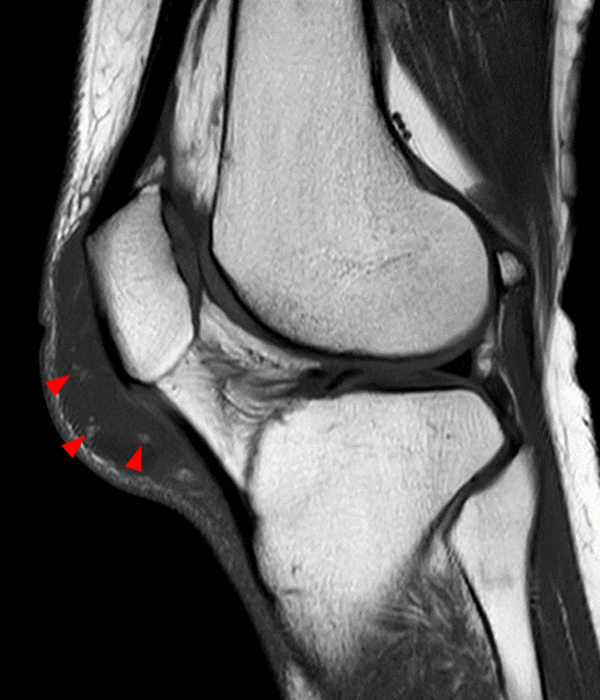
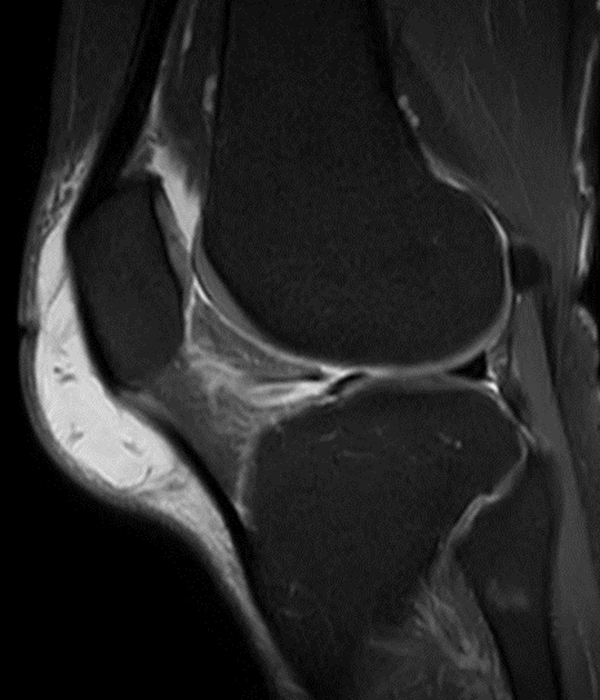
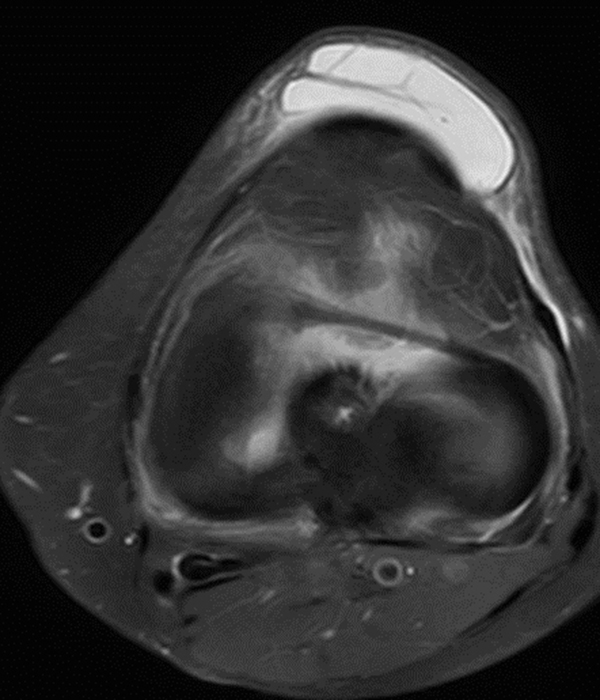
Clinical History: A 73 year-old male complains of a gradually enlarging “knot” on the anterior knee for 8 years. He previously worked laying tile. Sagittal T1-weighted (1A), sagittal fat-suppressed proton density-weighted (1B), and axial fat-suppressed proton density-weighted (1C) images are shown. What are the pertinent imaging findings and diagnosis?
Findings
Figure 2:
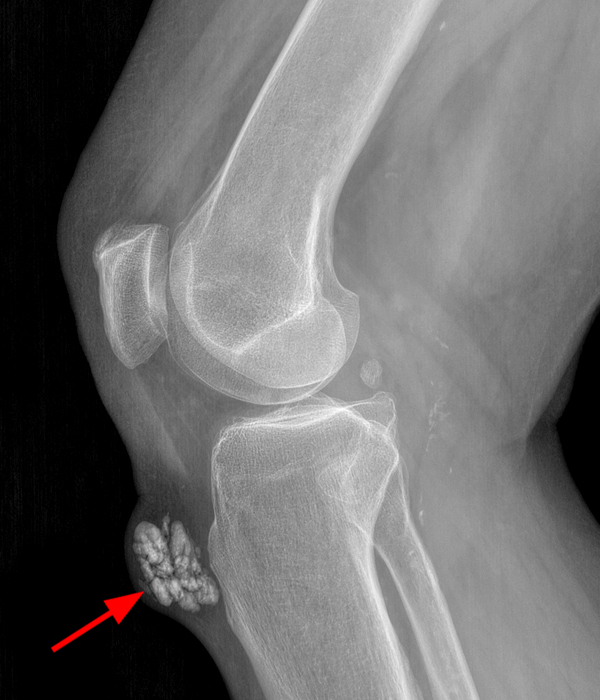
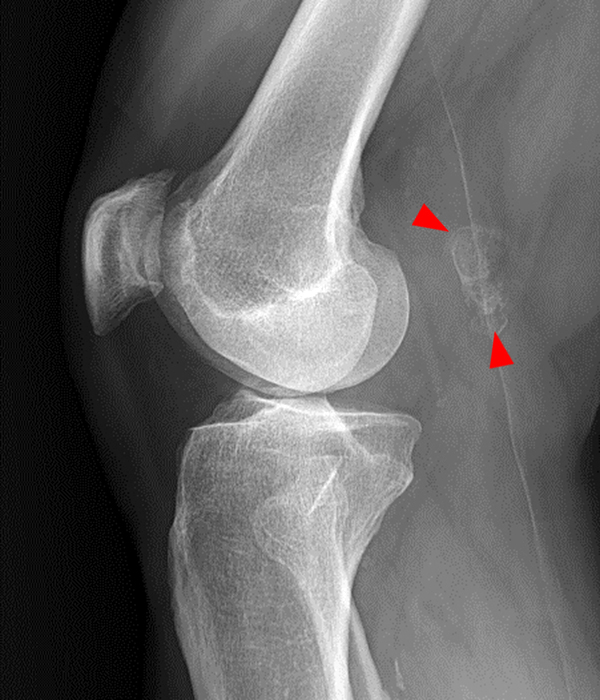
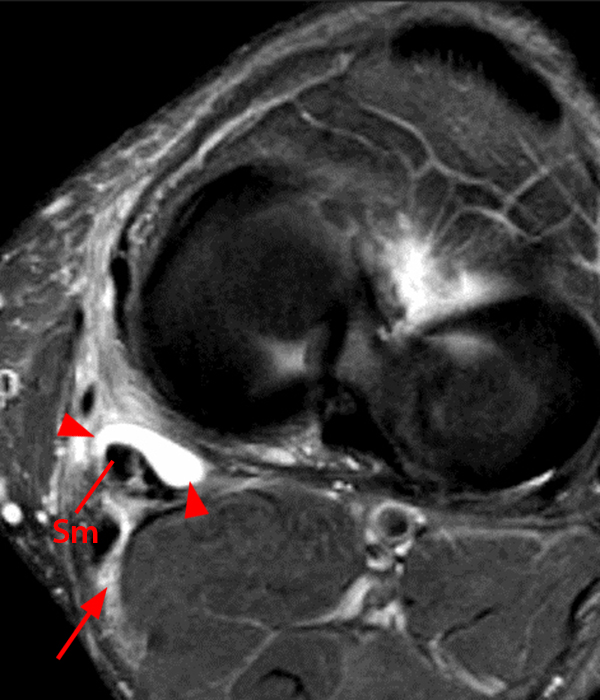
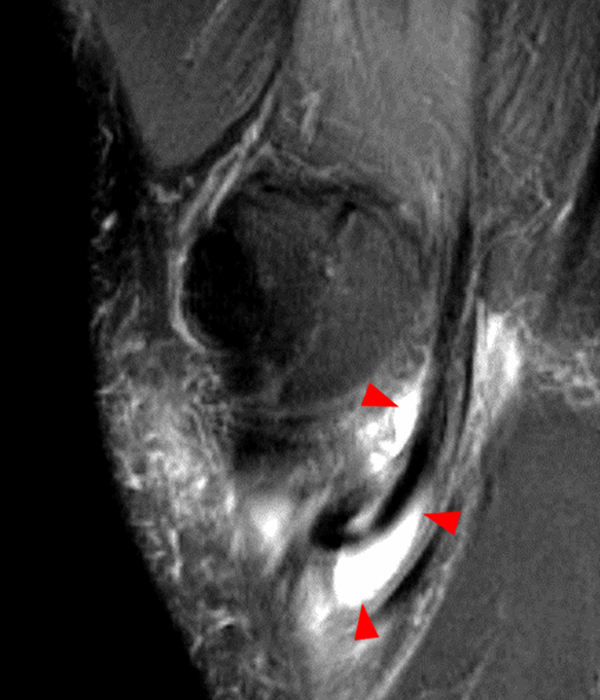
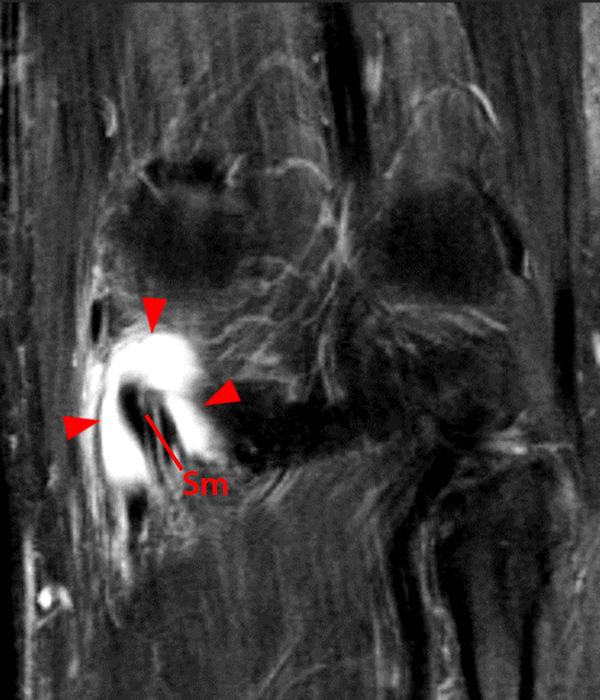
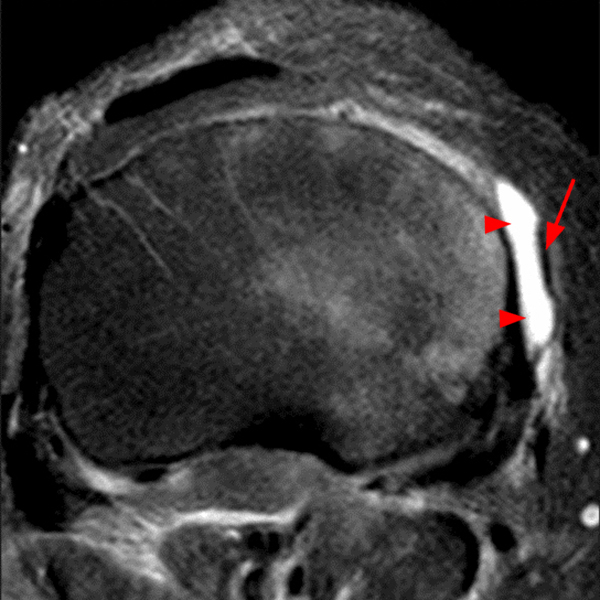
An elliptical region of marked signal hypointensity on T1 and fat-suppressed proton density-weighted images is seen in the midline subcutaneous tissues superficial to the anterior tibial tuberosity and patellar tendon (arrows), with mild prepatellar and infrapatellar subcutaneous edema. The underlying tendon and osseous structures are normal. Figure 2D is the corresponding lateral knee radiograph showing clustered calcific deposits (arrow) in the region of the pretibial abnormality.
Diagnosis
Chronic calcific superficial infrapatellar bursitis (“housemaid’s knee” or “clergyman’s knee”). This was treated successfully with resection.
Introduction
Bursal distension and other cystic lesions about the knee are frequently encountered findings on MR imaging of the knee. It is important for those interpreting MRI of the knee to be familiar with the normally occurring anatomic bursa of the knee, potential clinical presentations, usual and variable imaging appearances, and differential diagnostic considerations. The aim of this web clinic is to review the anatomy of bursa of the knee and to discuss commonly occurring soft tissue cystic lesions around the knee.
Bursae of the Knee: Function and Anatomy
Definition and Function
Anatomic or primary bursae are synovial lined periarticular structures, which occur normally developmentally, contain variable amounts of fluid, and serve to reduce motion or pressure induced friction between adjacent anatomic periarticular structures, often between bone and the overlying soft tissues. An adventitial bursa describes an acquired fluid filled soft tissue abnormality that develops at a pathologic or iatrogenic site of increased friction between two structures, often between bone or hardware and the overlying soft tissues. The latter may not be synovial lined.
Anatomy
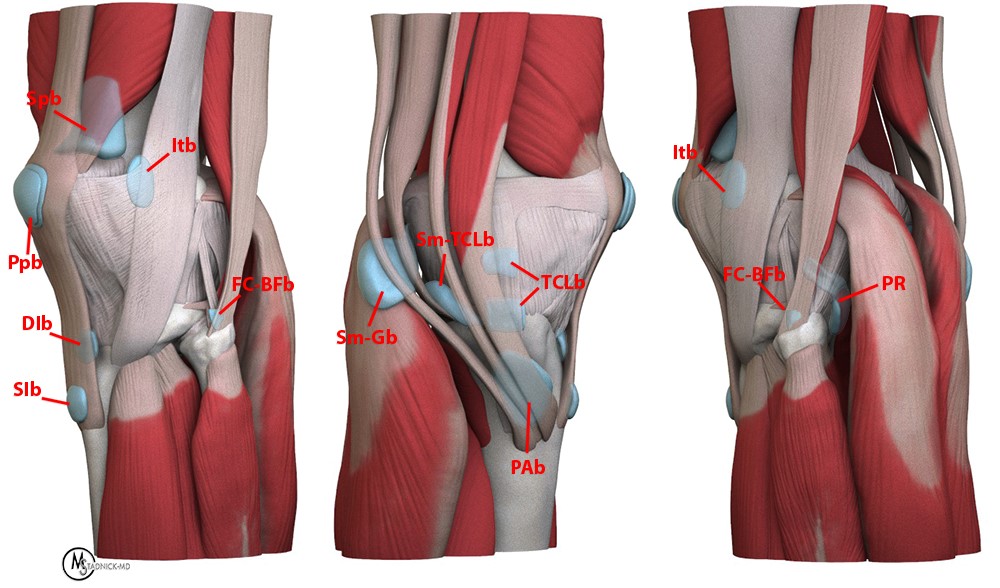
Figure 3:
Multiple views of a 3D render demonstrate the locations of the bursa at the knee. Anterior bursa: suprapatellar (Spb), prepatellar (Ppb), superficial infrapatellar (SIb), deep infrapatellar (DIb); Medial and Posteromedial: pes anserine (PAb), tibial collateral (TCL-b), semimembranosus-tibial collateral (Sm-TCLb), and semimembranosus-gastrocnemius (Sm-Gb); Lateral and Posterolateral: iliotibial (Itb), popliteal recess (PR), fibular collateral-biceps femoris (FC-BFb). (Click on image below for 3D interactive view. Click-drag to rotate, scroll to zoom.)
Anterior Bursae
The Suprapatellar bursa or recess is an anterior midline structure located deep to the distal quadriceps and superficial to the pre-femoral fat pad and distal femur. This communicates widely with the knee joint in most adults functioning as a recess due to the involution of an embryonic septum that exists between the bursa and the remaining joint, which occurs at about the third fetal month.1,2 A suprapatellar plica is often seen, representing a shelf-like membranous remnant of part of that septum. In approximately 16% of adults, an isolated suprapatellar bursa may be present due to failure of the embryonic septum to involute leaving a complete septum. Distension of this bursa may mimic a mass in the pre-femoral region.3 A persistent partial septum or suprapatellar plica may trap chondral or osteochondral bodies in the suprapatellar recess.4 See Figure 15.
Prepatellar, Superficial and Deep Infrapatellar bursae: The prepatellar bursa lies superficial to the quadriceps continuation and is centered in the midline though it may extend slightly medially or laterally relative to the patella. Surgical and cadaveric studies have shown the prepatellar bursa to be trilaminar or bilaminar in nature,5 though on routine clinical MRI, that compartmentalization is often not apparent. The superficial infrapatellar bursa resides superficial to the anterior tibial tuberosity and patellar tendon insertion, and the deep infrapatellar bursa lies just deep to the distal patellar tendon. The latter frequently contains a small amount of fluid in asymptomatic knees.6 Normally none of these bursae communicate with the knee joint.1
Medial and Posteromedial Bursa
The pes anserine bursa is located anteromedially, about 3-4 cm caudal to the joint line and does not typically communicate with the joint. It is interposed between the distal tibial collateral ligament insertion and the distal sartorius, gracilis and semitendinosus tendons. The combined insertions of these tendons have a webbed configuration, which has been likened to that of a goose’s foot, from which is derived their Latin name, pes anserinus tendons.7 The Tibial collateral or MCL bursa has been found to be present in 90% of adults and in cadaveric specimens, separate femoral and tibial portions of the bursa were frequently seen.8 Distension of the MCL bursa typically appears as a vertically oriented well defined fluid collection extending along the medial aspect of the femoral and tibial cortices, being centered deep to the superficial MCL (tibial collateral ligament) between it and the deep MCL (the meniscofemoral and meniscotibial ligaments), typically occurring in association with medial compartment and or medial capsuloligamentous pathology.8,9 Distinction between fluid in the MCL bursa and a medial parameniscal cyst may be difficult, though usually medial parameniscal cysts are centered more posteriorly, and usually communication of a parameniscal cyst with a meniscal tear or focus of intra-meniscal degeneration is present.8 Additionally, parameniscal cysts are often more loculated and sometimes contain more inspissated contents.
The Semimembranosus-tibial collateral bursa is located along the posteromedial joint line, cranial to the pes anserine bursa, and was found to be consistently present in a cadaveric analysis of 50 knees.10,11 It has an inverted U or J configuration with a superficial distal arm and a deep proximal arm that drapes around the distal semimembranosus tendon.
The Semimembranosus-gastrocnemius bursa or recess (Sm-Gb) arises between the semimembranosus tendon and the medial head of the gastrocnemius, within the posteromedial popliteal fossa, cranial to the joint line at the level of the upper medial femoral condyle. They most often extend caudally, though they may extend in any direction.12 The bursa communicates with the knee joint in most adults and thus is sometimes referred to by many as a recess, being comprised of a distal gastrocnemius bursa and a proximal semimembranosus bursa, which sometimes are partially separated by a septum.13 The reported prevalence of this communication has varied dependent upon the population being studied, and the mode of investigation. It has been reported as occurring in 30-50% of cadaveric dissections, 50% in arthrograms of normal knees, 55% in open surgical excision, and 37% in diagnostic arthroscopies.14,15,16,17 Lindgren et al. studied 80 cadaver knee joints and concluded that communication of the Sm-Gb with the knee joint is acquired, due to degeneration of the capsule, occurring with greater frequency in older individuals, in more than 50% of those over the age of 50 years and in no patient under 10 years of age. The communication occurs via a slit-like defect in the posteromedial capsule most often measuring 15-20 mm, where the medial gastrocnemius tendon exits the joint.17,18 Various studies have shown unidirectional flow of fluid from the knee joint into the Sm-Gb, though the precise nature of that valvular mechanism is controversial with some proposing a Bunsen or ball valve mechanism and others theorizing that the dynamic actions of the semimembranosus, semitendinosus and gastrocnemius myotendinous units in flexion and extension contribute to a functional unidirectional communication.17,19,20
Lateral and Posterolateral Bursa
The Iliotibial Bursa is believed to be an adventitial bursa that may develop between the iliotibial tract and the lateral femoral condyle, possibly with extension further distally in the compartment like space between the iliotibial tract, and the lateral meniscocapsular ligaments in the setting of chronic inflammation and iliotibial band syndrome.21,22,23
The Popliteus Recess or Popliteus Hiatus occurs at the posterolateral corner of the knee, posterior to the posterior horn lateral meniscus around the popliteus tendon. It routinely communicates with the knee, may extend caudally deep to the popliteus myotendinous junction, and may communicate with the proximal tibiofibular joint in 10% of adults.24,25
The Fibular collateral- biceps femoris bursa has an inverted J shape in the axial plane with a curved short arm extending around the anteromedial portion of the distal fibular collateral ligament near the insertion, and a longer lateral limb lying along the superficial lateral aspect of the fibular collateral ligament. Terry et al. found this to be consistently present in cadaveric dissection of 30 knees, though other investigators discussing the anatomy of the posterolateral knee did not note the bursa to be uniformly present.26
Bursae of the Knee: Clinical Presentations and MRI Appearance
Bursae about the knee may or may not communicate with the joint, and with a few exceptions normally contain minimal or no fluid, such that they may not be detectable on MRI. Small amounts of fluid may be seen within some bursae and recesses in the absence of symptoms, particularly the semimembranosus gastrocnemius bursa, the deep infrapatellar bursa, the suprapatellar recess, the popliteal recess (hiatus) and occasionally the pes bursa. Though the significance of the finding of fluid within bursae of the knee on MRI is primarily determined by clinical factors, the MRI observation of prominent bursal distension, mild circumferential bursal wall thickening, adjacent soft tissue edema and/or reactive marrow edema, neurovascular impingement and indicators of bursal rupture (further discussed below) are imaging features that suggest symptomatic bursitis. Bursae that contain fluid may appear simple, demonstrating homogeneous fluid equivalent signal on T1 and T2-weighted images, or they may be complex and multiloculated with thin internal septations. Following administration of intravenous gadolinium, thin peripheral and/or septal enhancement is typical of bursae. Because synovial fluid may be absorbed by the synovial cell bursal lining, but fibrin and other debris typically is not, cyst contents may become inspissated or mineralized. Bursae containing proteinaceous or hemorrhagic material may demonstrate hyperintensity on T1-weighted images, while those containing calcification or hemosiderin will exhibit intrinsic low signal on T1 and T2-weighted images (see test case figure 1). Bursa may contain chondroid or osteochondral bodies, which may represent extruded joint bodies, or these may develop de novo due to chondro-metaplasia.27 Chondral or osteochondral bodies within bursa can enlarge over time as they may be nourished by synovium.
A distended semimembranosus-gastrocnemius bursa is the most commonly encountered fluid collection about the knee1,28 The term “Baker’s cyst” is now often used to describe distension of this anatomic bursa, after clinical observations in 8 patients with popliteal fossa swelling were described by William M. Baker in 1877.29 In adults these bursae frequently communicate with the knee joint and are most likely to occur in knees with an effusion due to traumatic or degenerative internal derangement, osteoarthritis, inflammatory or crystal deposition related arthropathy or other diseases of the synovium including PVNS and primary synovial osteochondromatosis.26 The reported prevalence of distension of this bursa varies, dependent upon the age and nature of the study population, defining criteria and imaging modality utilized, ranging from 5-32% of adults being evaluated for suspected internal derangement by MRI and arthrography, respectively. Higher detection rate using arthrography has been postulated to be due to iatrogenic distension of previously collapsed bursae.30 In an MRI evaluation of 102 asymptomatic knees, Tschirch et al. found prevalence of Sm-Gb of 19%, with the majority having a maximal size of 30 mm or less. In contradistinction, the majority of cases of semimembranosus-gastrocnemius bursal distension in pediatric patients, excluding those with juvenile rheumatoid arthritis (JRA), are not associated with effusion and intra-articular pathology and are thought to occur spontaneously due to local trauma or irritation involving the bursa.31,32 Pediatric patients with JRA and an effusion commonly develop semimembranosus- gastrocnemius bursal cysts.33
Baker’s cysts most commonly present in adults as a painless posteromedial swelling, but if large they may lead to limited range of motion. They may be associated with knee pain, though the pain is often due to the intraarticular pathology, rather than the cyst itself. Large cysts may lead to claudication due to mass effect upon the popliteal artery. Sudden onset of pain and swelling may occur mimicking thrombophlebitis, most often after cyst rupture due to overdistension and or trauma. Uncommonly, cyst rupture may be associated with compartment syndrome or with concomitant thrombophlebitis.34,35,36 Though bursal rupture is most often seen in the setting of a large Baker’s cyst, fluid may also extravasate from a distended posterolateral popliteus recess (hiatus) in which case the clinical presentation may mimic a lateral gastrocnemius muscle strain. In the setting of bursal rupture, MRI will show edema tracking in the fascial planes along the caudal, cranial medial or lateral aspects of the cyst, possibly with loss of smooth peripheral contour in the region of rupture and overlying subcutaneous edema. Though Sm-Gb cysts most often extend inferiorly and medially, they may extend along the fascial planes in any direction from the bursal origin, and may also dissect into adjacent musculature of the distal thigh and proximal calf.37 Particularly when large or complex the imaging appearance of a large semimembranosus gastrocnemius bursal may be confusing, but identification of a neck between the semimembranosus and gastrocnemius tendons confirms the diagnosis.
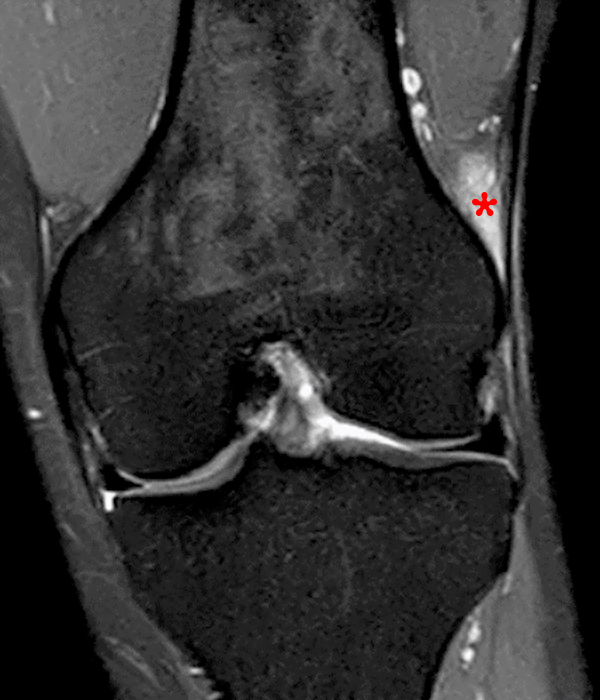
Figure 4:
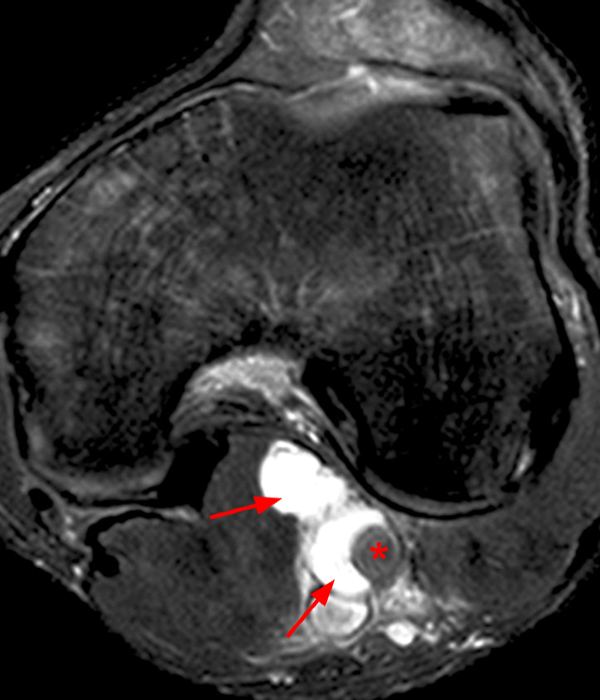
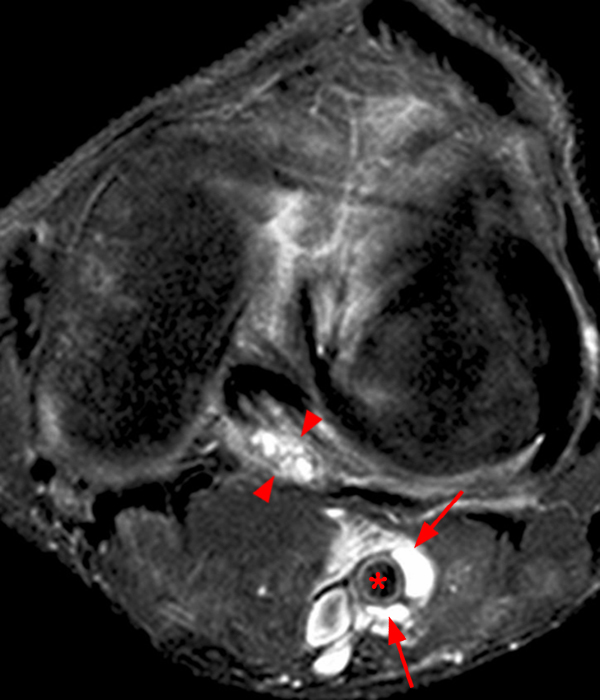
Sagittal T1-weighted (4A), sagittal fat suppressed proton density-weighted (4B), axial fat suppressed proton density- weighted images just above the joint line (4C) and at the distal femoral metaphysis (4D) with a corresponding lateral radiograph (4E) show the typical location and fluid equivalent signal within a Sm-Gb cyst at the level of the joint (asterisk). Several large ossicles (arrowheads) are noted with the superior aspect of the Sm-Gb, positioned proximal to the medial head gastrocnemius and deep to the distal semimembranosus. Ossicles within bursa may enlarge as they are nourished by the synovium.
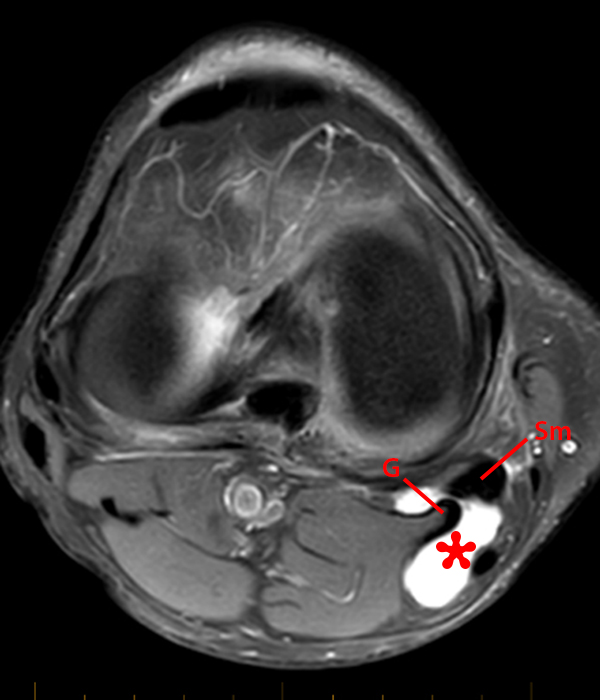
Figure 5:
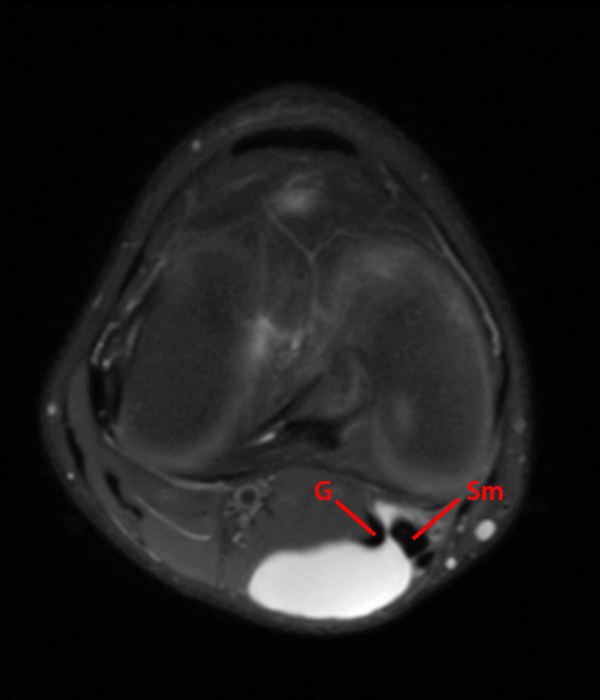
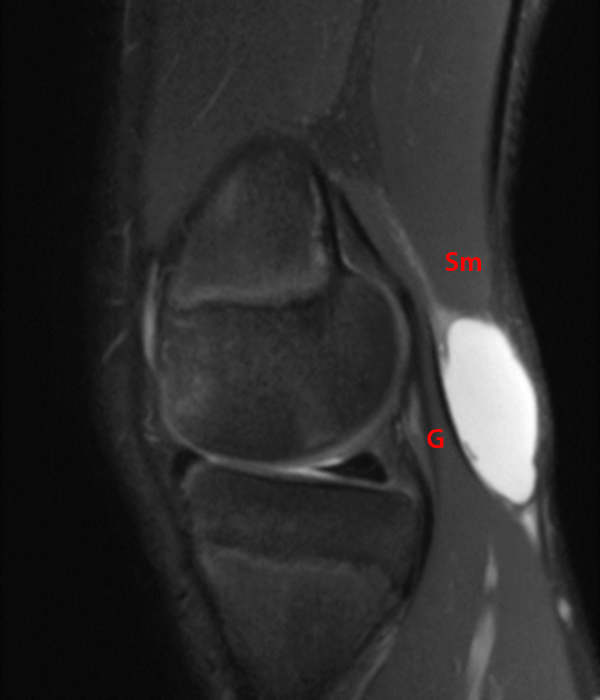
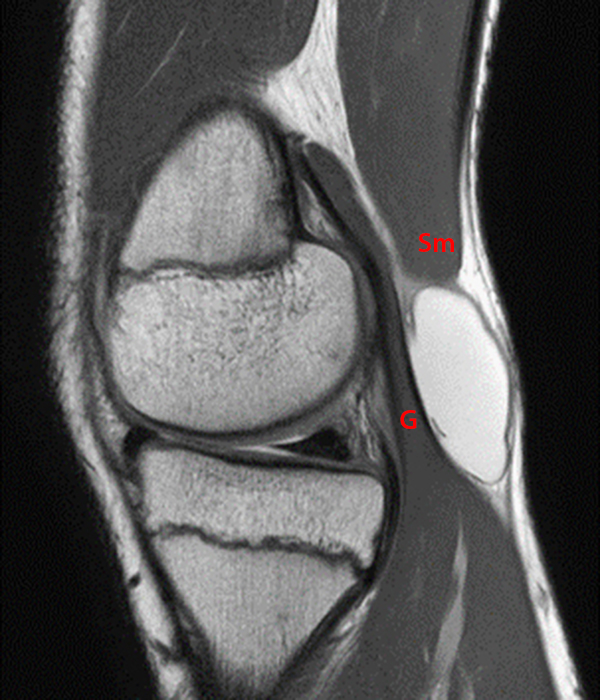
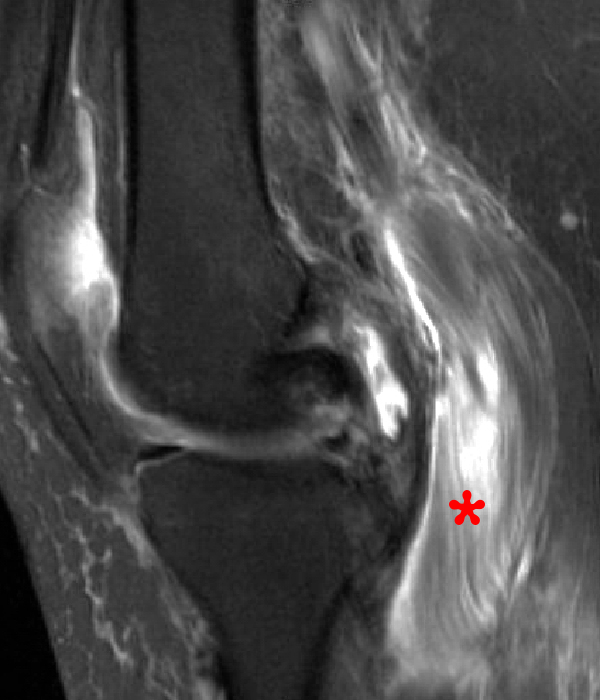
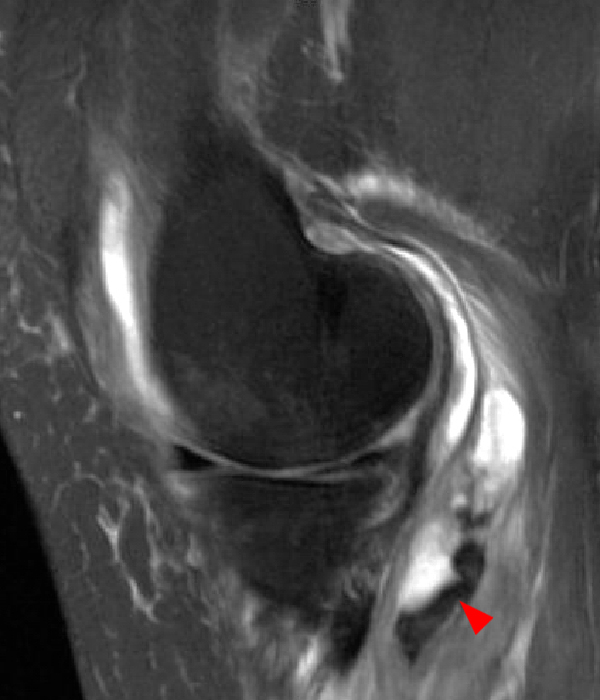
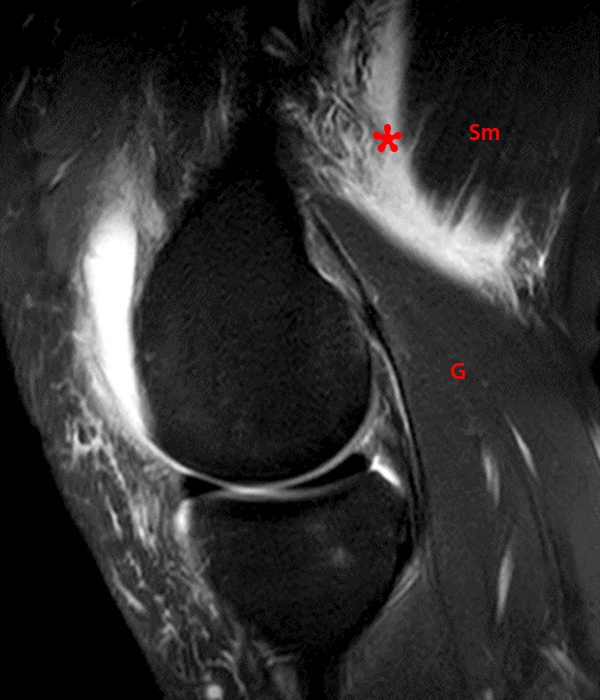
14-year-old male with no known injury or past medical history, complains of 2.5 weeks posteromedial swelling. Axial (5A) and sagittal (5B) fat-suppressed proton-density weighted images and sagittal (5C) proton density-weighted images show a circumscribed fluid collection in the distribution of the Sm-Gb, extending between semimembranosus (Sm) and medial gastrocnemius (G) tendons. Notably, there is no associated effusion and no meniscal, chondral, or ligamentous abnormality. In the pediatric population, excluding those with JRA and effusion and contrasting with findings in most adults, semimembranosus gastrocnemius bursal distension most often is not associated with effusion or intra- articular pathology, and is thought to occur due to local trauma or irritation to the bursa.
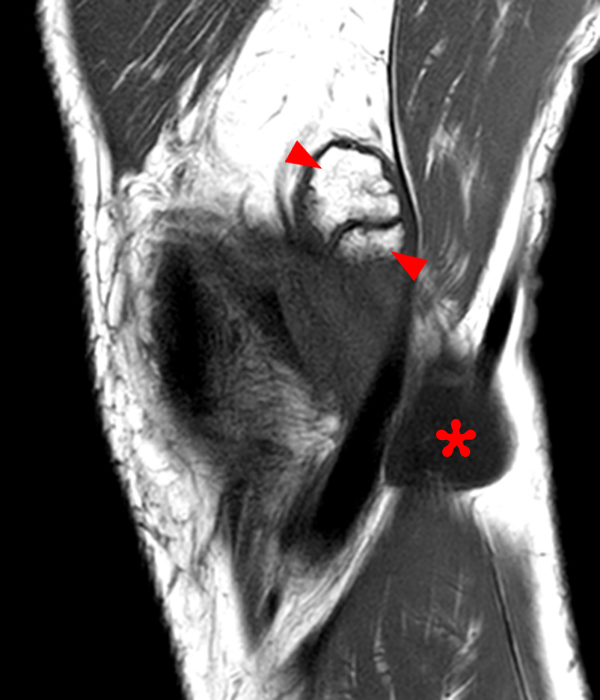
Figure 6:
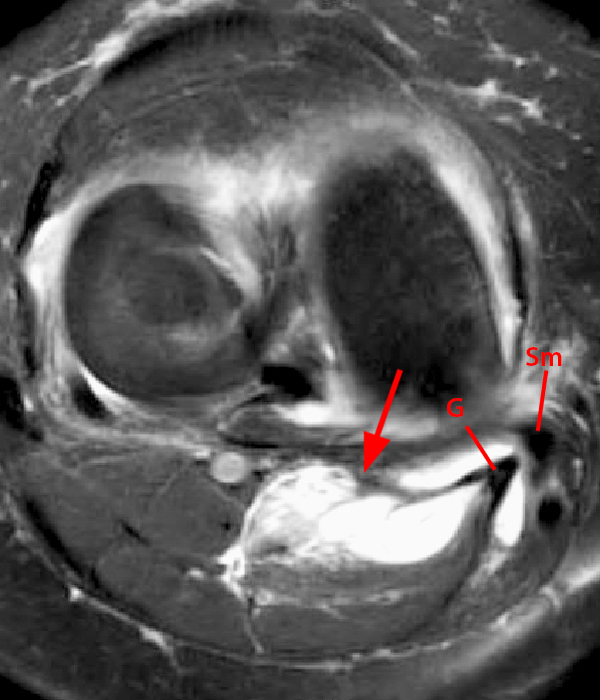
65 year-old female who presented to the emergency room with sudden onset severe calf pain and swelling also referred to as “Pseudo-thrombophlebitis Syndrome.” Venous doppler exam was negative for DVT. Axial fat suppressed proton density-weighted images just above (6A) and caudal (6B) to the joint line, show fluid within the Sm-Gb with expected extension between the proximal medial gastrocnemius (G) and distal (Sm) semimembranosus tendons. There are findings of bursal rupture with poorly defined lateral margins of the bursa (arrow on 6A and 6B). The above axial and additional sagittal fat suppressed proton density-weighted images (6C and 6D) show ill-defined edema tracking caudally intramuscularly within the deep medial gastrocnemius (asterisk) and within the adjacent fat planes. Globular signal hypointensity (arrowheads) within the posteroinferior aspect of the bursa represents hemorrhagic debris.
Figure 7:
Fat suppressed proton density-weighted axial images at the distal femoral metaphysis just superior to the femoral condyles (7A) and further superiorly (7B) and a sagittal fat suppressed proton density weight image (7C) through the medial aspect of the knee show fluid in the Sm-Gb with findings of recent rupture at the superior margin of the bursa, with fluid extending superiorly between the semimembranosus (Sm) and gastrocnemius (G) muscles, indistinct bursal margins and fluid extending along the fascial planes along the superior aspect of the bursa (asterisks).
Semimembranosus-tibial collateral bursitis usually presents with nonspecific posteromedial pain, aggravated with activity. MR images show distension of the inverted U or J-shaped bursa partially draped over the semimembranosus, at the posteromedial joint line and abutting the posterior horn medial meniscus. Distension of this bursa may coexist with semimembranosus, pes anserine and or semimembranosus gastrocnemius bursal distension, though they do not typically communicate.8,11,38,39
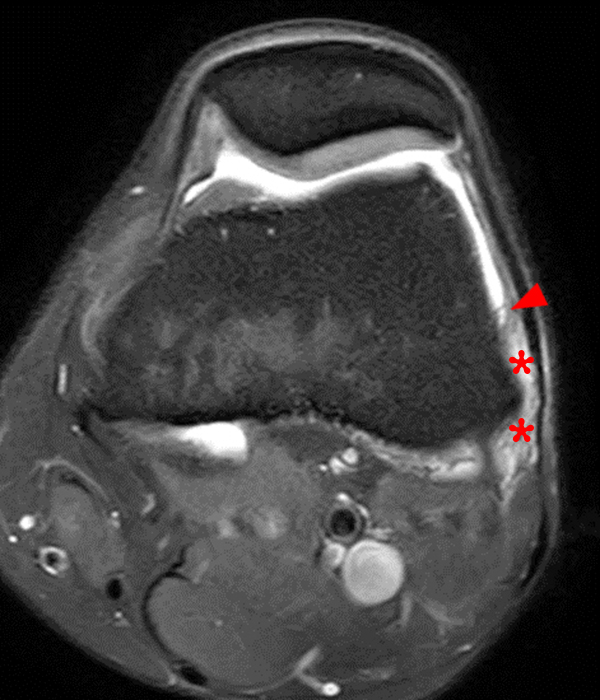
Figure 8:
Axial (8A), sagittal (8B), and coronal (8C) fat-suppressed proton density-weighted images show a distended semimembranosus-tibial collateral bursal fluid collection (arrowheads) draping over the direct insertion of the semimembranosus tendon (Sm). The characteristic inverted U shape of the distended semimembranosus-TCL bursa is best seen on the coronal (8C) image, and an inverted partial U or J shape around the semimembranosus tendon is seen on sagittal image (8B). Mild soft tissue edema is seen adjacent to the distended bursa, a finding which may be associated with a symptomatic bursitis. Trace fluid is seen within the Sm-Gb (arrow) on axial image (8A).
Tibial collateral bursitis may present with pain along the medial joint line mimicking a medial meniscal tear or chondral abnormality. The bursa is visible only if distended with fluid, which is usually indicative of pathology. Tibial collateral bursitis does not often occur in isolation and may be associated with traumatic, degenerative, or inflammatory medial compartment pathology, severe genu valgus, and flat foot deformity. It has also been described in professional motorcycling and equestrian athletes.8 MRI will show a circumscribed fluid collection centered deep to the tibial collateral ligament interposed between it the meniscofemoral and meniscotibial ligaments, often with a bilobular appearance on axial images.1 At times only the tibial or femoral component of the bursa will be distended with fluid.
Figure 9:
Axial (9A) and coronal (9B) fat-suppressed proton density-weighted images demonstrate tibial collateral bursitis with an elongated fluid collection (arrowheads) interposed between the superficial tibial collateral ligament (arrows) and the meniscofemoral and meniscotibial portions of the deep MCL (short arrows). On axial images the distended bursa has a characteristic bi-lobulated appearance as it bulges slightly superficially around the anterior and posterior margins of the tibial collateral ligament (arrowheads). This characteristic location and configuration and homogeneous intrinsic fluid equivalent signal may help to differentiate fluid in the tibial collateral bursa from medial parameniscal cysts or other juxta-articular ganglia, which often have intrinsic septations and sometimes intrinsic signal characteristics consistent with more inspissated contents. Coronal image 9B also shows a small subchondral stress fracture (block arrow) of the medial femoral condyle with associated marrow edema and medial compartment chondral loss. A tear of the posterior root medial meniscus was also present (not shown).
Pes anserine bursitis classically causes pain and or swelling medial and caudal to the joint line, which is often aggravated with crossing one leg over another, rising from a seated position or climbing stairs. It may be associated with vague medial pain mimicking medial meniscal tear(7). It often occurs in runners, basketball and racquetball players due to repetitive overuse, though it may also be seen in the setting of direct trauma, increased valgus or rotatory stresses upon the knee 40. There is also an increased incidence in middle age obese women, those with diabetes, osteoarthritis, medial meniscal or chondral pathology. Small amounts of fluid within the bursa may be asymptomatic. More prominent fluid collections, with or without a thickened synovial lining, and semi-solid appearance with complex contents have been described in symptomatic and chronic pes bursitis.38,40,41
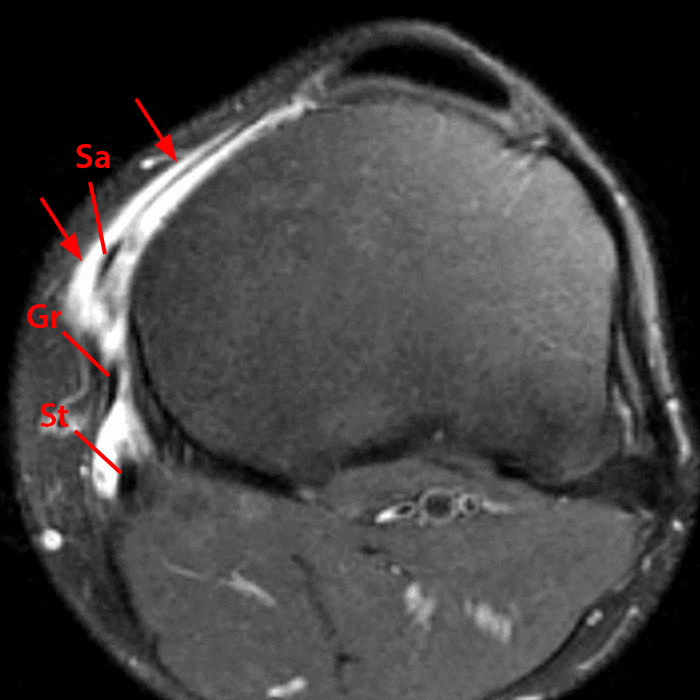
Figure 10:
Sagittal (10A) and axial (10B) fat suppressed proton density-weighted images of a 30 year-old long distance runner with a several week history of worsening anteromedial knee pain, show marked pes anserine bursitis. Note fluid and synovitis centered along the deep aspect of the insertional sartorius (Sa), gracilis (Gr) and semitendinosus (St) tendons. The conjoined insertions of these tendons have a webbed configuration which has been likened to that of a goose’s foot, from which their Latin name pes (foot) anserinus (goose) is derived. Mild soft tissue edema is seen along the anterior and superficial aspect of the pes tendons (arrows), suggestive of a symptomatic bursal collection.
Similarly, iliotibial band syndrome often occurs due to sport related overuse in cyclists and runners, particularly those training on sloped surfaces, with the more inferiorly positioned lower extremity being affected. It has also recognized in football, soccer, basketball players, and skiers. Other factors associated with greater incidence of IT band syndrome include genu varus, overpronation of the foot, hip adductor weakness, and a prominent lateral epicondyle.21–23,42 Though historically this syndrome was attributed to friction related to the movement of the ITB anterior and posterior to the lateral femoral condyle, some investigators have challenged this theory, suggesting that a compression or impingement like syndrome affecting the vascularized fatty tissue deep to the iliotibial tract may better reflect the etiology21,22,43 Despite some debate regarding the pathogenesis, the syndrome relatively consistently presents with lateral or anterolateral pain that may sometimes mimic lateral compartment pathology. MRI most often shows ill-defined edema within a compartment like space bounded laterally by the iliotibial tract laterally, and medially by the lateral femoral condyle, the periphery of the lateral meniscus and meniscocapsular ligaments. Thickening of the iliotibial band may or may not be seen. A minority of patients with iliotibial band syndrome develop a discrete fluid collection within the same space deep to the distal iliotibial band, thought to represent adventitial bursal development.
Figure 11:
28 year-old cyclist complaining of several month history of worsening lateral knee pain, aggravated by activity. Coronal (11A) and axial (11B) fat-suppressed proton density-weighted images show development of an iliotibial bursa (asterisks) deep to the iliotibial band near the level of the lateral epicondyle. On axial images it is important to note that this fluid deep to the iliotibial band does not simply represent an effusion, as it is posterior to and separate from the posterolateral synovial reflection (arrowhead).
Pain and or swelling posterior and laterally, caudal to the joint line may be seen due to distension of the popliteus bursa, or due to a synovial cyst or ganglion arising from the proximal tibiofibular joint. The latter may be associated with clinical and or imaging findings of compression neuropathy due to direct mass effect upon or epineural extension involving branches of the peroneal or tibial nerves.1,44,45,46
Figure 12:
63 year-old female presenting with gradually worsening chronic posterolateral knee pain. She complains of intermittent tingling in the lower leg and has recently noticed a “knot” along the posterolateral knee. The patient was referred to an orthopaedist with concern for mass. Sagittal T1-weighted (12A) and fat-suppressed proton density-weighted sagittal (12B) and axial (12C) images show several large ossicles (asterisks) and a small amount of fluid within the distended popliteus recess (hiatus), corresponding with findings on a lateral radiograph (12D), and with the palpable mass. These ossicles likely represent extruded chondral or osteochondral bodies which may have gradually enlarged over time, as they are nourished by synovium. Sagittal and axial images show associated mass effect upon the common peroneal nerve (arrowheads). Note also patellar chondral fissuring (arrow) and small effusion (block arrow).
Figure 13:
Contiguous sagittal proton density-weighted images through the lateral femorotibial compartment (13A and 13B). In addition to extruded ossicles, the popliteus recess or hiatus may contain extruded meniscal flaps from the posterior horn and or body of the lateral meniscus. The above images show abnormal morphology of the posterior horn lateral meniscus, with a moderate flap (arrowheads) which had arisen from posterior horn and posterior body (the latter not shown) which has extruded anterior to the popliteus tendon (arrow) in the popliteus recess. Extruded flaps in this location are important to point out on preoperative MRI, as they are difficult to appreciate arthroscopically if unsuspected.
Fluid normally occurs in the suprapatellar recess, though a symptomatic suprapatellar bursitis may occur usually in the setting of a complete suprapatellar plica. Patients commonly present with suprapatellar pain and swelling, often with concern for a mass involving the distal thigh.
Figure 14:
Sagittal T1-weighted (14A), sagittal (14B) and axial (14C) fat-suppressed proton density-weighted images show suprapatellar bursitis with a complete suprapatellar plica (arrows), synovial edema and thickening (arrowheads), and a small amount of fluid (asterisks) in the developmentally isolated suprapatellar fossa. This 32 year-old male presented with insidious onset of suprapatellar pain and swelling after questionable minor trauma, with clinical concern for mass within the anterior distal thigh. Symptoms resolved with rest and suprapatellar steroid injection.
Figure 15:
54 year-old-female complains of anterior knee pain and swelling for years. Sagittal T1-weighted (15A), sagittal fat-suppressed proton density-weighted (15B), axial fat-suppressed proton density-weighted (15C), and lateral radiographic (15D) images show multiple small osteochondral bodies in the suprapatellar bursa with a small effusion and severe patellofemoral osteoarthritis. The curvilinear intermediate to low signal structure (arrow 15B) represents a partial suprapatellar plica.
A small amount of fluid may be seen in the infrapatellar bursa as a normal finding. Symptomatic deep infrapatellar bursitis most often shows more extensive fluid in the bursa with or without inflammation in the adjacent soft tissues, usually seen in jumper’s and runners, sometimes in association with patellar tendinosis or Osgood- Schlatter’s disease.42,47 Prepatellar and superficial infrapatellar bursitis may be seen in the setting of acute direct trauma and are also commonly associated with chronic repetitive microtrauma, most often due to occupational kneeling as has been called clergyman’s knee, housemaid’s knee, or carpet layer’s knee. In these cases, bursal imaging may show features of intrinsic hemorrhage or mineralization. Mineralization may also occur in the setting of tophaceous gout (see figure-18) which in the knee, has a predilection for the extensor tendons, anterior bursa and fat pad, as well as the intercondylar notch and popliteus tendon insertion.48,49 Infectious prepatellar or infrapatellar bursitis, most often due to staphylococcus aureus, may complicate chronic occupational related bursitis or penetrating anterior trauma. In addition to an increased prevalence of prepatellar and superficial bursitis, an increased incidence of multiloculated cysts of the popliteus recess or bursa has been reported in occupational kneelers.50
Figure 16:
30 year-old male with anterior knee pain after a fall. Sagittal (16A) and axial (16B) fat- suppressed proton density-weighted images show marked distension of the deep infrapatellar bursa with small amount of synovitis (asterisks), a small effusion (arrow), and moderate infrapatellar subcutaneous edema (arrowheads). The findings represented a post-traumatic deep infrapatellar bursitis and resolved with conservative measures.
Figure 17:
Axial fat suppressed t2 weighted image (17A) and sagittal proton density-weighted image (17B) in a 45 year-old carpet layer complaining of several month history of anterior pain and palpable mass, show prepatellar bursitis (asterisks) corresponding to the mass, which was marked with vitamin E capsules.
Figure 18:
64 year-old male with one-week history of worsening anterior knee pain and swelling. Axial fat-suppressed proton density-weighted (18A) and sagittal proton density-weighted (18B) images of the knee show marked fluid and focal synovitis within the deep infrapatellar bursa. An ill-defined nodular soft tissue abnormality (tophus) demonstrating intermediate signal intensity on both images is seen, within the anterior aspect of the bursa (arrows) partially invading deep fibers of the distal patellar tendon. Note marked inflammatory edema within the adjacent soft tissues (arrowheads). The findings represented (clinically proven) tophaceous gout.
Differential Considerations
Synovial cyst refers to any synovial lined periarticular or peritendinous fluid collection. The term has been used in the literature synonymously with bursa, though most use it to describe synovial lined fluid collections that are acquired rather than being uniformly present developmentally.
Ganglia describes benign periarticular, intra-articular, subchondral or periosteal cystic structures which contain viscous fluid rich in hyaluronic acids and other mucopolysaccharides.51 They may arise from the joint capsule, ligaments, bursae, subchondral or subperiosteal bone adjacent to many joints, and have variable communication with the joint.1 Their precise etiology remains unclear with theorized origins including mesenchymal cell metaplasia and proliferation, versus mucoid connective tissue degeneration related to repetitive microtrauma, versus synovial herniation through a capsular defect. Although histologically they may often be differentiated from synovial cysts because they are lined by a dense fibroconnective tissue capsule with flat spindle cells rather than synovial cells, this distinction is less than perfect as ganglia may become synovialized1,52 Synovial cysts and ganglia are often not distinguishable on MRI, though this distinction is likely primarily of academic interest, as it usually does not directly alter management. More importantly, MRI does allow delineation of many other features of periarticular cysts that will often directly impact treatment, such as lesion size, location, effect upon adjacent structures, findings of rupture, as well as the nature and extent of associated intraarticular pathology.
Intraarticular ganglia have been reported with a prevalence of up to 1% of knee MR imaging53,54 and may be seen within or adjacent to the cruciate ligaments, most commonly occurring near the tibial insertion of the ACL and the adjacent anterior root lateral meniscus. Cruciate ligament ganglia may be associated with mucoid degeneration of the cruciate ligaments, likely representing different manifestations of the same pathogenesis. These ganglia may be asymptomatic, or dependent upon their size and location may be associated with pain mimicking a meniscal tear, clicking, or limited range of motion. Instability is not usually an associated finding.1,51,53,55
They may dissect into Hoffa’s fat pad and may occur posterior to the PCL, where they should be differentiated from posteromedial parameniscal cysts.1,9,56
Figure 19:
45-year-old male complains of knee clicking, pain and decreased range of motion. Axial (19A), sagittal (19B), and coronal (19C) fat- suppressed proton density-weighted images show mucoid degeneration of the ACL (asterisks) with a prominent multiloculated peri-cruciate ligament ganglion (arrowheads) associated with the distal fibers of the ACL, extending anterior to insertional fibers along the posterior central portion of Hoffa’s fat pad, partially overlying the cephalad aspect of the anterior root lateral meniscus (block arrow) and the transverse meniscal ligament (arrow).
Juxta-articular ganglia (or synovial cysts) may be observed posterior to the distal femoral metaphysis, adjacent to the capsule, near the medial or lateral head gastrocnemius origins, and are often multiloculated. Unlike in cases of semimembranosus-gastrocnemius bursal distension, no extension between the semimembranosus gastrocnemius tendons is seen in medial lesions. In a small series of 10 cases only one patient presented with suspected popliteal fossa mass, none showed obvious MRI communication with the joint and none required surgical excision.57
Parameniscal and intrameniscal cysts have been theorized to develop when synovial fluid is pushed through a meniscal tear accumulating within or at the periphery of a torn or degenerated meniscus, or due to a myxoid degenerative process involving the meniscus. They have been found to have a prevalence of about 4% of knee MRI’s in 2 studies, one in symptomatic and another in asymptomatic knees.1,6,58 Parameniscal cysts typically appear as circumscribed T2 hyperintense structures with an epicenter at the joint line near the peripheral meniscal margin. Several studies have shown direct communication of parameniscal cysts with a meniscal tear in up to 98%, though the frequency of that association depends upon the definition used for meniscal tear. In cases in which communication with an articular surface tear is not identified, one may see communication with intra-meniscal degeneration which does not meet strict criteria for tear.51,58,59 They occur both medially and laterally, and most often are associated with tears having a horizontal component,9,58 commonly presenting with joint line pain with or without swelling. When large they may migrate away from the meniscal margin, in a distribution dependent upon the regional capsuloligamentous planes of the knee. Differentiation of these cysts from other periarticular ganglia is important as recurrence is common if only parameniscal cyst aspiration or excision is performed. Best treatment outcomes for symptomatic parameniscal cysts have been shown to include cyst decompression as well as the appropriate arthroscopic treatment of associated meniscal pathology.58,60,61 Medial parameniscal cysts should be differentiated from fluid within the MCL bursa, semimembranosus-TCL, and pes anserinus bursa. Communication with a meniscal tear (or horizontal intrasubstance degeneration) and location different from characteristic confines of the anatomic bursae, will allow differentiation. Edema around the MCL may occur in the setting of recent trauma and has also been described in the absence of recent trauma, having significant association with medial and lateral meniscal tears and chondromalacia.62 Such peri-ligamentous and meniscocapsular edema is ill defined, and readily distinguished from parameniscal cyst or medial bursal distension.
Figure 20:
Axial (20A), sagittal (20B), and coronal (20C) fat-suppressed proton density weighted images demonstrate a large multiloculated lateral parameniscal cyst (arrowheads) communicating with a horizontal tear (arrows) involving the body through anterior horn lateral meniscus, extending into the anterior lateral gutter and into lateral aspect of Hoffa’s fat pad.
Synovial cysts or ganglia associated with the proximal tibiofibular joint appear as fusiform or multiloculated cystic collections along the distal aspect of the fibular head, with a pedicle of communication with the tibiofibular joint. The knee joint communicates with the proximal tibiofibular joint in 10% of individuals, and cysts of the proximal tibiofibular joint have a greater incidence in those with chronic knee effusions.9,42 Cysts may cause direct compression of the common peroneal nerve near the fibular head or may dissect along the epineurium of the common peroneal nerve and its branches or the articular branch of the tibial nerve with associated findings of denervation edema at MRI, and clinical findings of neuropathy.1,9,42 Ganglia of the proximal tibiofibular joint may occasionally cause pressure erosion of the adjacent bone,9 which can raise concern regarding an osseous lesion, though the sclerotic margination and adjacent ganglion communicating with the joint space allow diagnosis.
Figure 21:
37 year-old male with recurrent lateral calf pain and swelling, following several prior cyst aspirations. Axial fat suppressed proton density weighted images at the level of the proximal tibiofibular joint and more caudally (21A-C), sagittal (21D) and coronal (21E) fat suppressed proton density-weighted images are shown. These reveal a small effusion of the proximal tibiofibular joint (arrows) and an elongated multiloculated synovial cyst or ganglion (arrowheads) likely arising from the posterior inferior aspect of the proximal tibiofibular joint extending caudally within the lateral soleus abutting the neurovascular structures (block arrow points to the popliteal artery. The posterior tibial nerve lies just posterior to it. Review of serial images showed the popliteal vein to be locally effaced). If possible, it is important to identify and report the neck of communication of any symptomatic ganglion with a nearby joint, as it usually needs to be resected or ligated to prevent recurrence.
Morel-Lavallee lesions (also called Morel-Lavallee effusions) are a consideration in the differential diagnosis of anterior bursal collections. Though classically occurring lateral to the greater trochanter, these may involve the extensor aspect of the knee in contact athletes particularly wrestlers and football players, who have suffered a traumatic injury with shear forces tangential to the fascial planes. This results in a closed degloving injury which separates the subcutaneous fat from the underlying fascia and causes injury to small perforating capillaries and lymphatics. History and physical exam may sufficiently diagnosis the condition, but when utilized MRI will usually show a large lenticular fluid collection centered in the perifascial space deep to the subcutaneous fat with variable intrinsic signal characteristics consistent with contained fluid, hemorrhagic material and often globules of fat or lymphatic material.63,64,65 The peripheral margins of the collections may demonstrate acute margins related to the delamination of the subcutaneous fat from underlying fascia, and signal hypo-intensity on all sequences due to fibrous or hemosiderin laden pseudo-capsule. Eccentric medial, lateral and or proximal extension into the mid-thigh, beyond the normal confines of the prepatellar bursa is often seen. Due to their large size and extent, propensity to re-accumulate and lack of synovial lining, management of these collections differs from that of anterior bursa, often involving aspiration and compression banding, sometimes with sclerodesis or open evacuation of refractory lesions.
Figure 22:
24 year-old football player with slowly worsening and recurrent anterior swelling following an injury when tackled 8 months prior. No recent trauma. Limited flexion due to swelling. Sagittal T1-weighted (22A), sagittal (22B) and axial (22C) fat-suppressed proton density weighted images show a large fluid collection in the prepatellar region, with multiple small foci of fat interspersed throughout the fluid, (arrowheads), a clue combined with history that the lesion represents a Morel-Lavallee lesion.
Post-traumatic or coagulopathy related hematomas may occur about the knee with the clinical history and MRI signal characteristics of hemorrhage usually leading to proper diagnosis.
Cystic adventitial disease of the popliteal artery is a very rare condition in which ganglia develop within the popliteal artery adventitia compromising blood flow, and potentially leading to claudication.45,66,67 The etiology is uncertain though synovial origin is favored with synovial fluid theorized to dissect through a capsular rent and along an articular vascular branch. MRI is a component of preoperative workup of patients with cystic adventitial disease, to identify any joint connections which should be ligated operatively.45
Figure 23:
50 year-old male with vague knee pain and claudication. Axial fat-suppressed proton density- weighted images just cranial to (23A) and at the joint line (23B) and a sagittal midline fat-suppressed proton density-weighted image (23C) show findings of cystic adventitial disease of the popliteal artery with confluent multiloculated ganglia (arrows) circumferentially involving the adventitia of the popliteal artery (asterisks). Axial and sagittal images show the deep aspect of the ganglia extend toward the posterior central capsule, with small multiloculated component positioned posterior to the PCL, just deep to the posterior central capsule at the joint line (arrowheads). This likely site of articular communication is important to point out on preoperative MRI to guide operative ligation, and prevention of recurrence.
Certain solid tumors, especially myxomatous lesions, nerve sheath tumors, necrotic sarcomas, and vascular lesions may mimic cystic structures. These should be considered when any solid component other than a thin peripheral wall or septa is present, when the location is not in keeping with a recognized bursa or common ganglion location, when invasion of surrounding structures is present, or when contents are heterogeneous and differ from fluid or complex fluid. In uncertain cases, injection of intravenous contrast agent may be useful to distinguish cystic from solid or vascular lesions.
Treatment
Many periarticular and intraarticular fluid collections, particularly those that are small, are asymptomatic requiring no treatment. Symptomatic bursae occurring in the setting of athletic overuse may be treated with rest, non-steroidal medication, corrective training measures, shoe wear or orthotics. Identification and treatment of treatable associated intraarticular pathology is important in the management of symptomatic semimembranosus gastrocnemius bursal cysts, and other synovial cysts that communicate with the knee joint. This may be supplemented with aspiration, often with steroid injection. Surgical resection is often reserved for recalcitrant symptomatic bursae, synovial cysts, and ganglia or those impinging upon neurovascular structures. The identification of pedicles of cyst extension and joint communication on preoperative MRI is important in preoperative planning to guide the ligation of any joint communication and complete cyst resection, such that the risk of cyst recurrence is diminished.
Conclusion
Cystic lesions and bursal distension about the knee joint are commonly occurring findings. While some lesions are asymptomatic, others may be associated with swelling, limited range of motion, pain due to impingement upon adjacent structures, or symptoms related to associated intraarticular pathology. MRI aids in characterization and treatment of symptomatic periarticular cystic or bursal collections by localizing them, delineating their relationship to adjacent structures, defining associated intra-articular pathology, and differentiating them from solid lesions or alternate causes of periarticular swelling.
A special thanks to Mike Stadnick, MD for illustrations in Figure 3, to David Rubin, MD for providing multiple cases used in this web clinic and to Liz Carpenter, MD for providing the case used in Figure 14.
References
- Steinbach LS, Stevens KJ. Imaging of Cysts and Bursae About the Knee. Radiologic Clinics of North America. 2013;51:433–54. ↩
- Andrew L Deutsch, MD., Donald Resnick, M.D., Murray K. Dalinka, M.D., Louis Gilula, M.D., Larry Danzig, M.D., Jose Guerra, Jr. M.D. and Fred H. Dunn MD. Synovial plicae of the knee. Diagnostic Radiol. 1981;141:627–34. ↩
- Ehlinger M, Moser T, Adam P, Simon P, Bonnomet F. Complete suprapatellar plica presenting like a tumor. Orthop Traumatol Surg Res. 2009;95(6):447–50. ↩
- Tsao MD L. Synovial Plicae of the Knee. MRI Web Clinic November 2018. ↩
- Aguiar RO, Viegas FC, Fernandez RY, Trudell D, Haghighi P, Resnick D. The prepatellar bursa: cadaveric investigation of regional anatomy with MRI after sonographically guided bursography. AJR Am J Roentgenol. 2007;188(4):355–8. ↩
- Tschirch FTC, Schmid MR, Pfirrmann CWA, Romero J, Hodler J, Zanetti M. Prevalence and size of meniscal cysts, ganglionic cysts, synovial cysts of the popliteal space, fluid-filled bursae, and other fluid collections in asymptomatic knees on MR imaging. Am J Roentgenol. 2003; ↩
- Burdett MD P. Pes Anserinus Bursitis. Radsource MRI Web Clinic September 2007. ↩
- De Maeseneer M, Shahabpour M, Van Roy F, Goossens A, De Ridder F, Clarijs J, et al. MR imaging of the medial collateral ligament bursa: Findings in patients and anatomic data derived from cadavers. Am J Roentgenol. 2001;177(4):911–7. ↩
- Howell MD G. Infrapatellar Ganglion Cyst. Radsource MRI Web Clinic March 2012. ↩
- Rothstein CP, Laorr A, Helms CA, Tirman PFJ. Semimembranosus-tibial collateral ligament bursitis: MR imaging findings. Am J Roentgenol. 1996; ↩
- Hennigan ASP, Universit MD, Clancy SC. The Semimembranosus-Tibial Collateral Ligament Bursa. Anatomical Study and Magnetic Resonance Imaging. J Bone Jt Surg. 1994;76-A(9):1322–7. ↩
- Stein D, Cantlon M, Mackay B, Hoelscher C. Cysts about the knee: Evaluation and Management. J Am Acad Orthop Surg. 2013;21(8):469–79. ↩
- Lee KR, Neff R, Arnett R. Cystic Masses of the Knee: Arthrographic and CT Evaluation. Knee, The. 1987;(February):329–34. ↩
- Calvisi V, Zoccali C. Arthroscopic patterns of the poster-medial aspect of the knee joint: Classification of the gastrocnemius-semimembranosus gateway and its relationship with Baker’s cyst. Muscles Ligaments Tendons J. 2016;6(4):492–8. ↩
- Handy JR. Popliteal Cysts in adults: A review. Semin Arthritis Rheum. 2001;31(2):108–18. ↩
- Frush TJ, Noyes FR. Baker’s Cyst: Diagnostic and Surgical Considerations. Sports Health. 2015;7(4):359–65. ↩
- Rauschning W. Anatomy and function of the communication between knee joint and popliteal bursae. Ann Rheum Dis. 1980;39(4):354–8. ↩
- Lindgren PG, Willen R. Gastrocnemio-semimembranosus bursas and its relation to the knee joint. Acta radiol. 1977;18(5):497–511. ↩
- Jayson MI, Dixon AS. Valvular mechanisms in juxta-articular cysts. Ann Rheum Dis. 1970;29(4):415–20. ↩
- Herman AM, Marzo JM. Popliteal cysts: A current review. Vol. 37, orthopaedics. 2014. p. 678–84. ↩
- Flato R, Passanante GJ, Skalski MR, Patel DB, White EA, Matcuk GR. The iliotibial tract: imaging, anatomy, injuries, and other pathology. Skeletal Radiol. 2017;46(5):605–22. ↩
- Muhle C, Ahn JM, Yeh LR, Bergman GA, Boutin RD, Schweitzer M, et al. Iliotibial band friction syndrome: MR imaging findings in 16 patients and MR arthrographic study of six cadaveric knees. Radiology. 1999;212(1):103–10. ↩
- Stadnick MD M. Iliotibial Band Friction Syndrome. Radsource MRI Web Clinic April 2005. ↩
- Wigley RD. Popliteal cysts: Variations on a theme of Baker. Semin Arthritis Rheum. 1982;12(1):1–10. ↩
- Janzen L, Peterfy G, Genant K. Pictorial Essay Cystic Lesions Findings Around the Knee Join : MR Imaging. Am J Roentgenol. 1994;163:155–61. ↩
- LaPrade MD R, Hamilton MD C. The Fibular Collateral Femoris Bursa Ligament-Biceps Study *. Am J Sports Med. 1997;25(4):439–43. ↩
- Torreggiani WC, Al-Ismail K, Munk PL, Roche C, Keogh C, Nicolaou S, et al. The imaging spectrum of Baker’s (Popliteal) cysts. Clin Radiol. 2002;57(8):681–91. ↩
- Petscavage-Thomas JM, Walker EA, Logie CI, Clarke LE, Duryea DM, Murphey MD. Soft-tissue myxomatous lesions: Review of salient imaging features with pathologic comparison. Radiographics. 2014;34(4):964–80. ↩
- Baker WM. On the Formation of Synovial Cysts in the Leg in.1 (6).pdf. Clin Orthop Relat Res. 1994;299:2–10. ↩
- Fielding JR, Franklin PD, Kustan J. Popliteal cysts: a reassessment using magnetic resonance imaging. Skeletal Radiol. 1991;20(6):433–5. ↩
- Harcke HT, Niedzielski A, Thacker MM. Popliteal cysts in children: Another look. J Pediatr Orthop Part B. 2016;25(6):539–42. ↩
- De Maeseneer M, Debaere C, Desprechins B, Osteaux M. Popliteal cysts in children: Prevalence, appearance and associated findings at MR imaging. Pediatr Radiol. 1999;29(8):605–9. ↩
- Szer IS, Klein-Gitelman M, DeNardo BA, McCauley RG. Ultrasonography in the study of prevalence and clinical evolution of popliteal cysts in children with knee effusions. J Rheumatol. 1992 Mar;19(3):458–62. ↩
- Schimizzi AL, Jamali AA, Herbst KD, Pedowitz RA. Acute compartment syndrome due to ruptured baker cyst after nonsurgical management of an anterior cruciate ligament tear: A case report. Am J Sports Med. 2006;34(4):657–60. ↩
- Hamlet M, Galanopoulos I, Mahale A, Ashwood N. Ruptured Baker’s cyst with compartment syndrome: An extremely unusual complication. BMJ Case Rep. 2012;(December):1–3. ↩
- Gordon G V., Edell S, Brogadir SP, Schumacher HR, Schimmer BM, Dalinka M. Baker’s Cysts and True Thrombophlebitis: Report of Two Cases and Review of the Literature. Arch Intern Med. 1979;139(1):40–2. ↩
- Fang CSJ, McCarthy CL, McNally EG. Intramuscular dissection of Baker’s cysts: Report on three cases. Skeletal Radiol. 2004;33(367–371). ↩
- Forbes JR, Helms CA, Janzen DL. Acute pes anserine bursitis: MR imaging. Radiology. 1995;194(2):525–7. ↩
- Rothstein CP, Laorr A, Helms CA, Tirman PFJ. Semimembranosus-tibial collateral ligament bursitis: MR imaging findings. Am J Roentgenol. 1996;166(4):875–7. ↩
- Rennie WJ, Saifuddin A. Pes anserine bursitis: Incidence in symptomatic knees and clinical presentation. Skeletal Radiology. 2005;34:395–8. ↩
- Zeiss J, Coombs RJ, Booth Jr RL, Saddemi S. Chronic Bursitis Presenting as a Mass in the Pes Anserine Bursa: MR Diagnosis. J Comput Assist Tomogr. 1993;17(1):137–40. ↩
- Janzen DL, Peterfy CG, Forbes JR, Tirman PFJ, Genant HK. Cystic lesions around the knee joint: MR imaging findings. Am J Roentgenol. 1994;163:155–61. ↩
- Fairclough J, Hayashi K, Toumi H, Lyons K, Bydder G, Phillips N, et al. The functional anatomy of the iliotibial band during flexion and extension of the knee: Implications for understanding iliotibial band syndrome. J Anat. 2006;208(3):309–16. ↩
- Millard MD W, Bruno MD C, Huang MD B, Resnick MD D. Common Peroneal Nerve Abnormalities. Radsource MRI Web Clinic June 2017. ↩
- Desy NM, Spinner RJ. The etiology and management of cystic adventitial disease. J Vasc Surg (Internet). 2014;60(1):235-245.e11. Available from: http://dx.doi.org/10.1016/j.jvs.2014.04.014 ↩
- Spinner RJ, Mokhtarzadeh A, Schiefer TK, Krishnan KG, Kliot M, Amrami KK. The clinico-anatomic explanation for tibial intraneural ganglion cysts arising from the superior tibiofibular joint. Skeletal Radiol. 2007;36(4):281–92. ↩
- Kjellin MD I. Subacute and Chronic Avulsion Injuries of the Extensor Mechanism of the Knee. Radsource MRI Web Clinic March 2014. ↩
- Vu S. MR Imaging of Tophaceous Gout. Am Roentgen Ray Soc. 1997;168(February):523–7. ↩
- Ko KH, Hsu YC, Lee HS, Lee CH, Huang GS. Tophaceous gout of the knee: Revisiting MRI patterns in 30 patients. J Clin Rheumatol. 2010;16(5):209–14. ↩
- Rytter S, Jensen LK, Bonde JP, Egund N. MR imaging of intra- and periarticular cyst-like lesions of the knee joint in workers with occupational kneeling. Int J Rheumatol. 2012;1–10. ↩
- Beaman FD, Peterson JJ. MR Imaging of Cysts, Ganglia, and Bursae About the Knee. Magn Reson Imaging Clin N Am. 2007;15(1):39–52. ↩
- Wu JS, Hochman MG. Soft-tissue tumors and tumorlike lesions: A systematic imaging approach. Vol. 253, Radiology. 2009. p. 297–316. ↩
- Bergin D, Morrison WB, Carrino JA, Nallamshetty SN, Bartolozzi AR. Anterior Cruciate Ligament Ganglia and Mucoid Degeneration: Coexistence and Clinical Correlation. Am J Roentgenol. 2004;182(5):1283–7. ↩
- Bui-Mansfield L, Youngberg RA. Intraarticular Ganglia of the Knee: Prevalence, Presentation, Etilogy, and Management. Am J Roentgenol. 1997;168:123–7. ↩
- Stadnick MD M. ACL Ganglion Cysts. Radsource MRI Web Clinic April 2004. ↩
- Lektrakul N, Skaf A, Yeh LR, Roger B, Schweitzer M, Blasbalg R, et al. Pericruciate Meniscal Cysts Arising from Tears of the Posterior Horn of the Medial Meniscus: MR Imaging Features that Simulate Posterior Cruciate Ganglion Cysts. Am J Roentgenol. 1999;(June):1575–9. ↩
- James SLJ, Connell DA, Bell J, Saifuddin A. Ganglion cysts at the gastrocnemius origin: A series of ten cases. Skeletal Radiol. 2007;36(2):139–43. ↩
- Campbell SE, Sanders TG, Morrison WB. MR imaging of meniscal cysts: Incidence, location, and clinical significance. Am J Roentgenol. 2001;177(2):409–13. ↩
- Anderson JJ, Connor GF, Helms CA. New observations on meniscal cysts. Skeletal Radiol. 2010;39(12):1187–91. ↩
- Reagan WD, McConkey JP, Loomer RL, Davidson RG. Cysts of the lateral meniscus: Arthroscopy versus arthroscopy plus open cystectomy. Arthrosc J Arthrosc Relat Surg. 1989;5(4):274–81. ↩
- Cowden CH, Barber FA. Meniscal cysts: treatment options and algorithm. J Knee Surg. 2014;27(2):105–11. ↩
- Blankenbaker DG, De Smet AA, Fine JP. Is intra-articular pathology associated with MCL edema on MR imaging of the non-traumatic knee? Skeletal Radiol. 2005;34(8):462–7. ↩
- Borrero CG, Maxwell N, Kavanagh E. MRI findings of prepatellar Morel-Lavallée effusions. Skeletal Radiol. 2008;37(5):451–5. ↩
- De Coninck T, Vanhoenacker F, Verstraete K. Imaging features of Morel-Lavallée lesions. J Belgian Soc Radiol. 2017;101:1–8. ↩
- Carroll MD J. Morel-Lavallee Lesions. Radsource MRI Web Clinic June 2010. ↩
- Wilbur MD A, Woelfel MD G, Flanigan MD DP, Spigos MD D. Adventitial cystic disease of the popliteal artery. Radiology. 1985;155:63–4. ↩
- Peruyera PDC, Velasco MB, Cervin J. Cystic adventitial disease of the popliteal artery : Two case reports and a review of the literature. Vascular. 2015;23(2):204–10. ↩