Clinical History: A 25-year-old female presents with acute knee pain and instability following a skiing injury. The injury involved pivoting on a planted leg, a subsequent pop sensation and a fall. What are your findings? What is your diagnosis?
Findings
Figure 2:
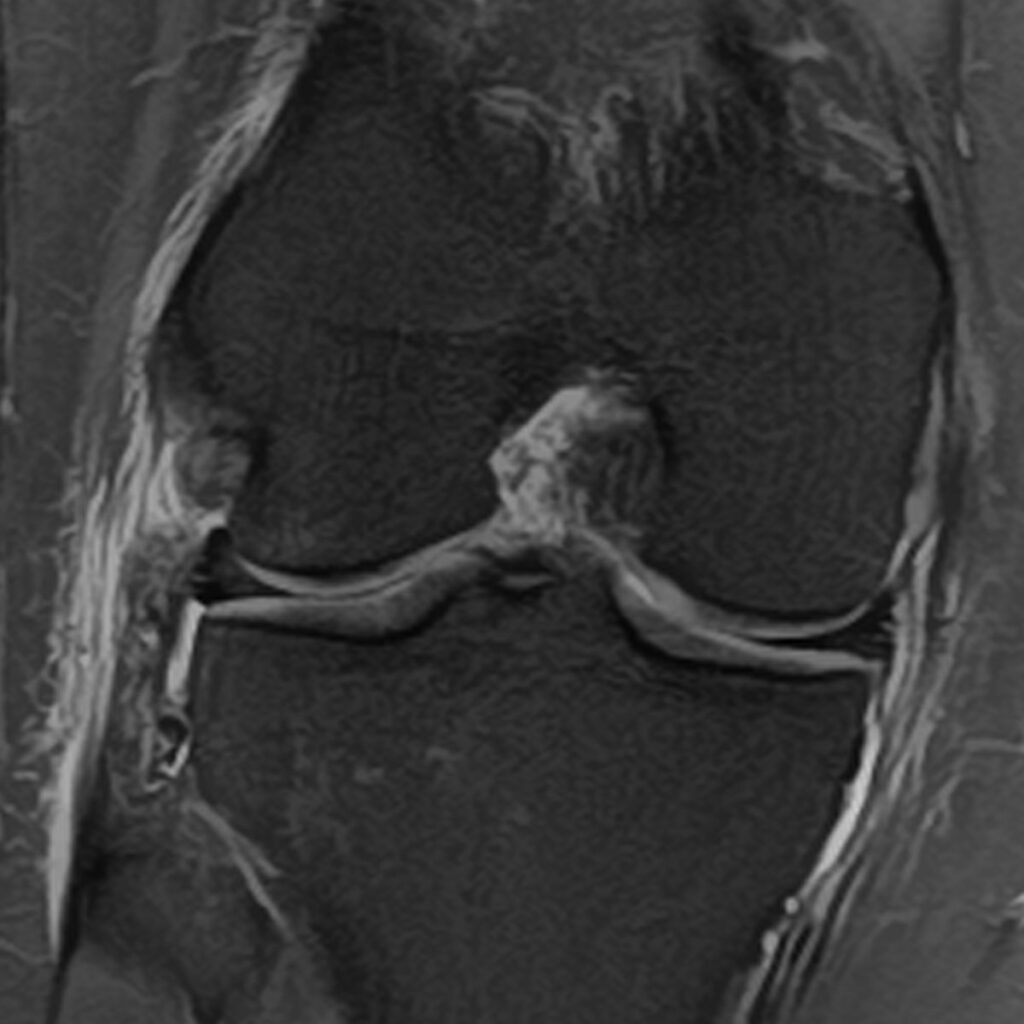
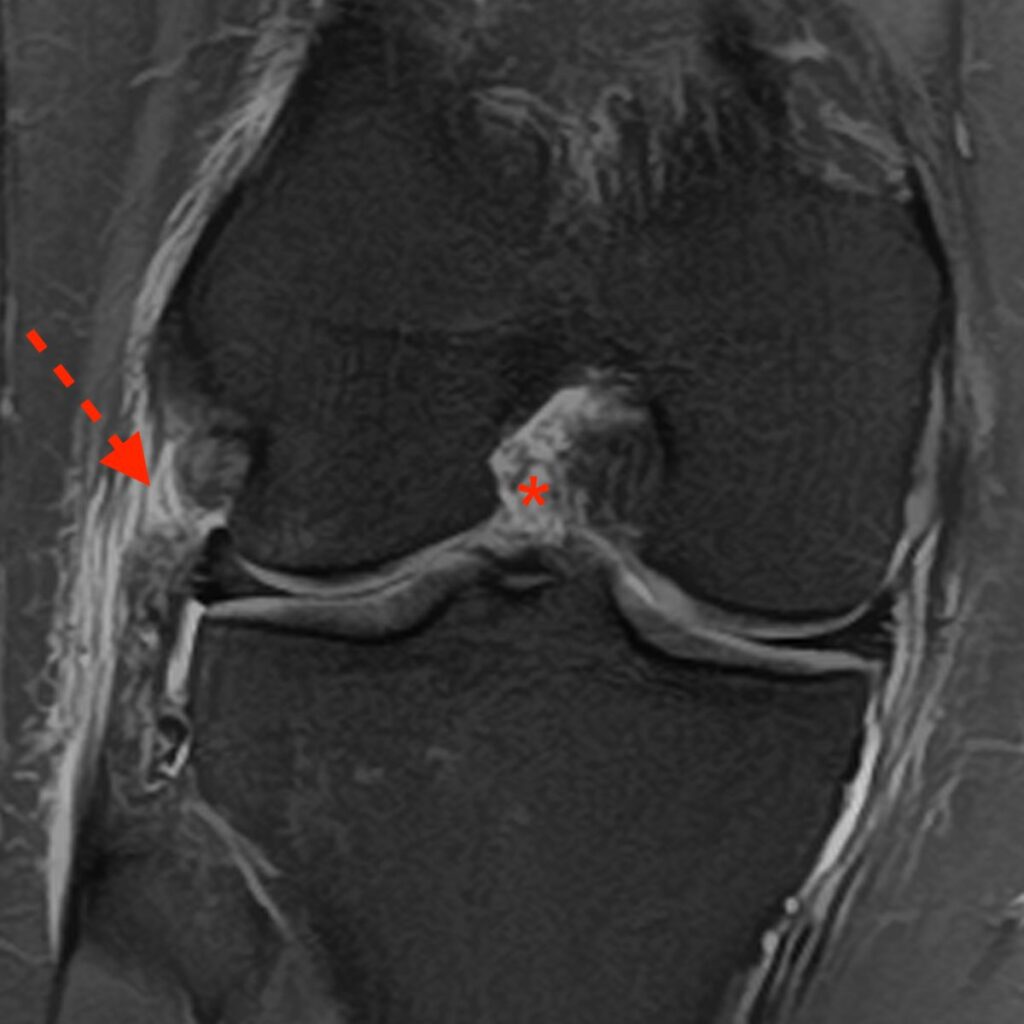
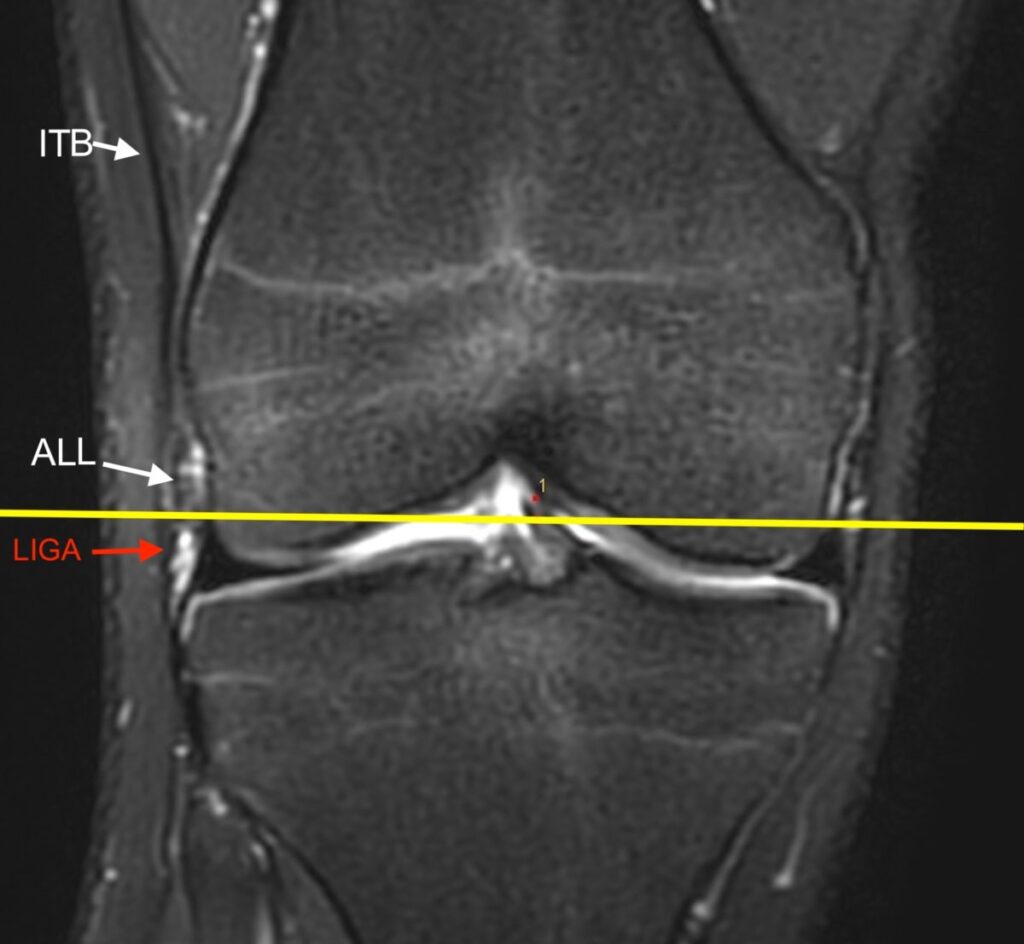
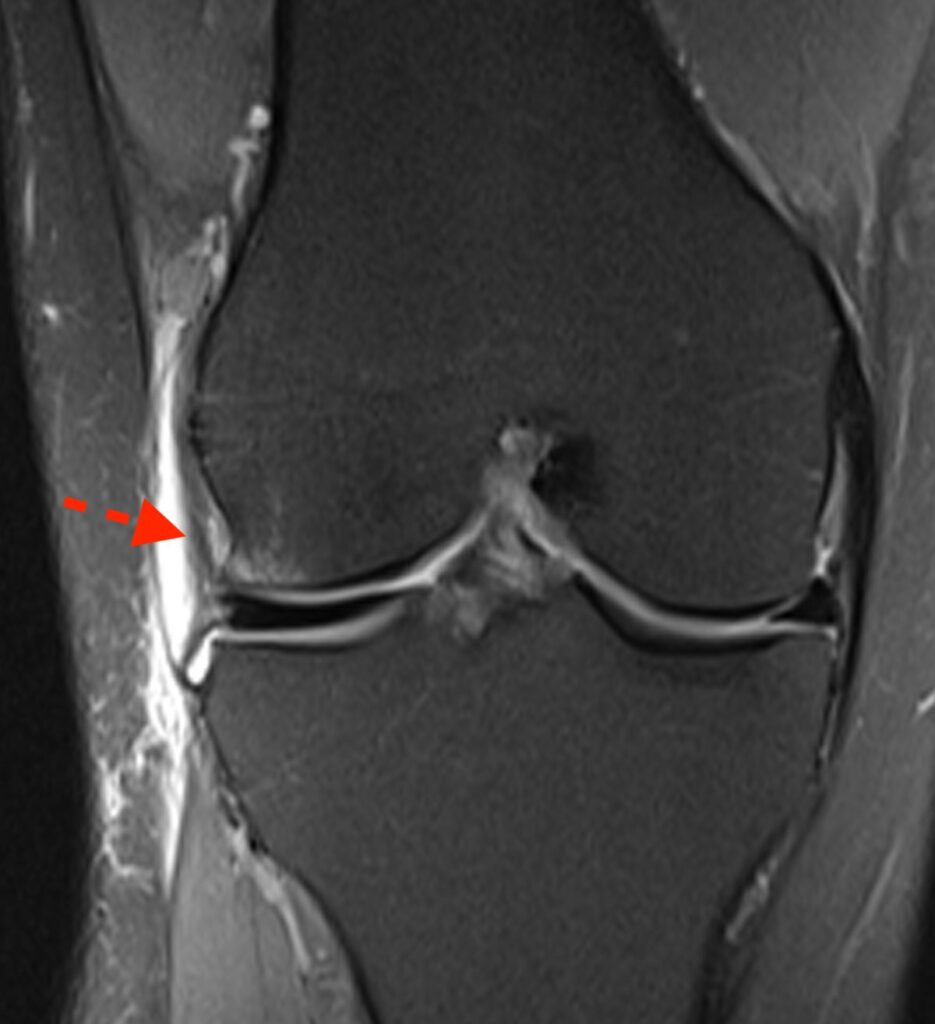
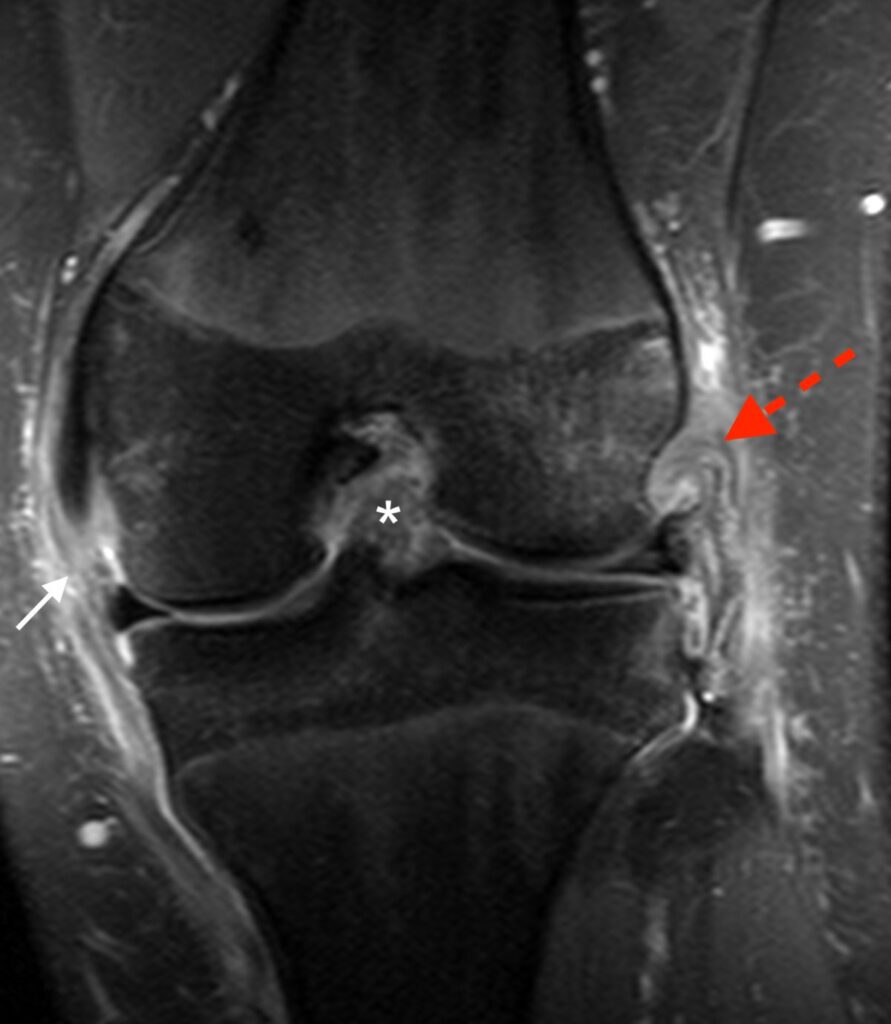
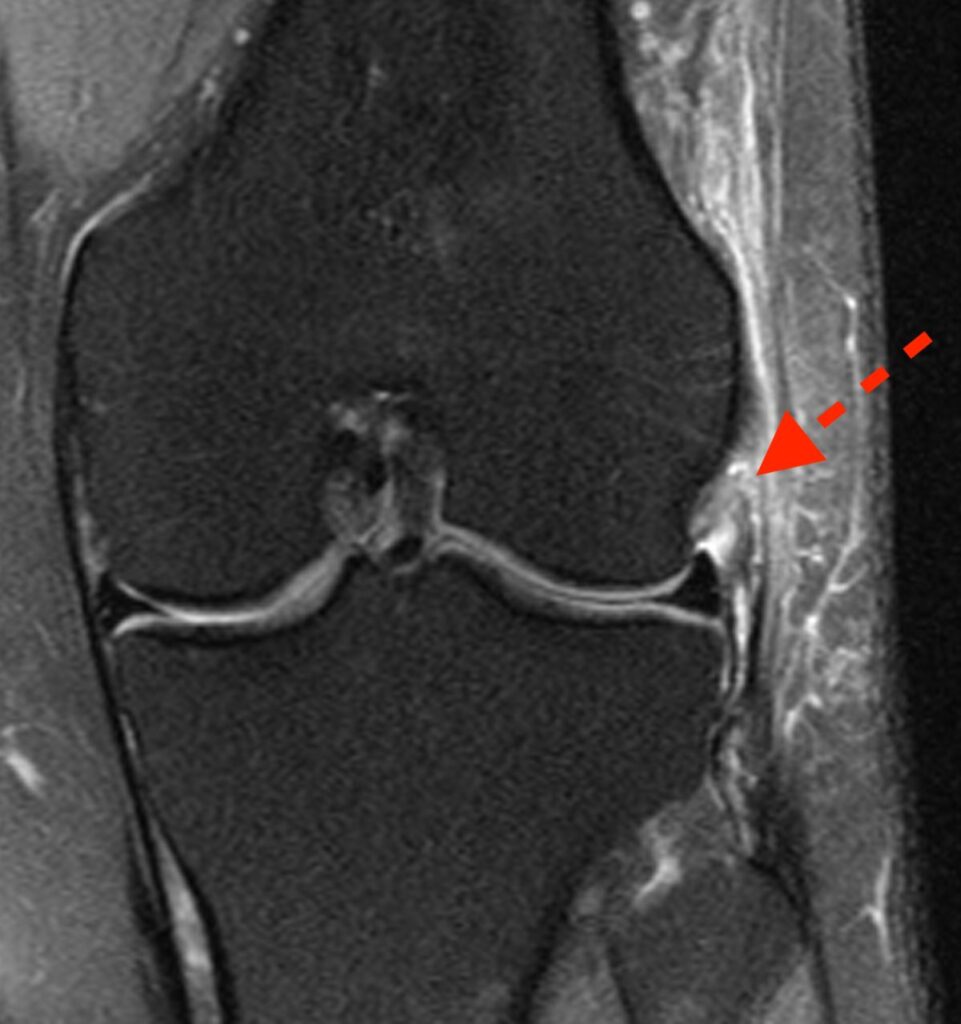
2a: Coronal fat-suppressed proton density-weighted image demonstrates a disrupted anterolateral ligament (dashed arrow) and a disrupted anterior cruciate ligament (*).
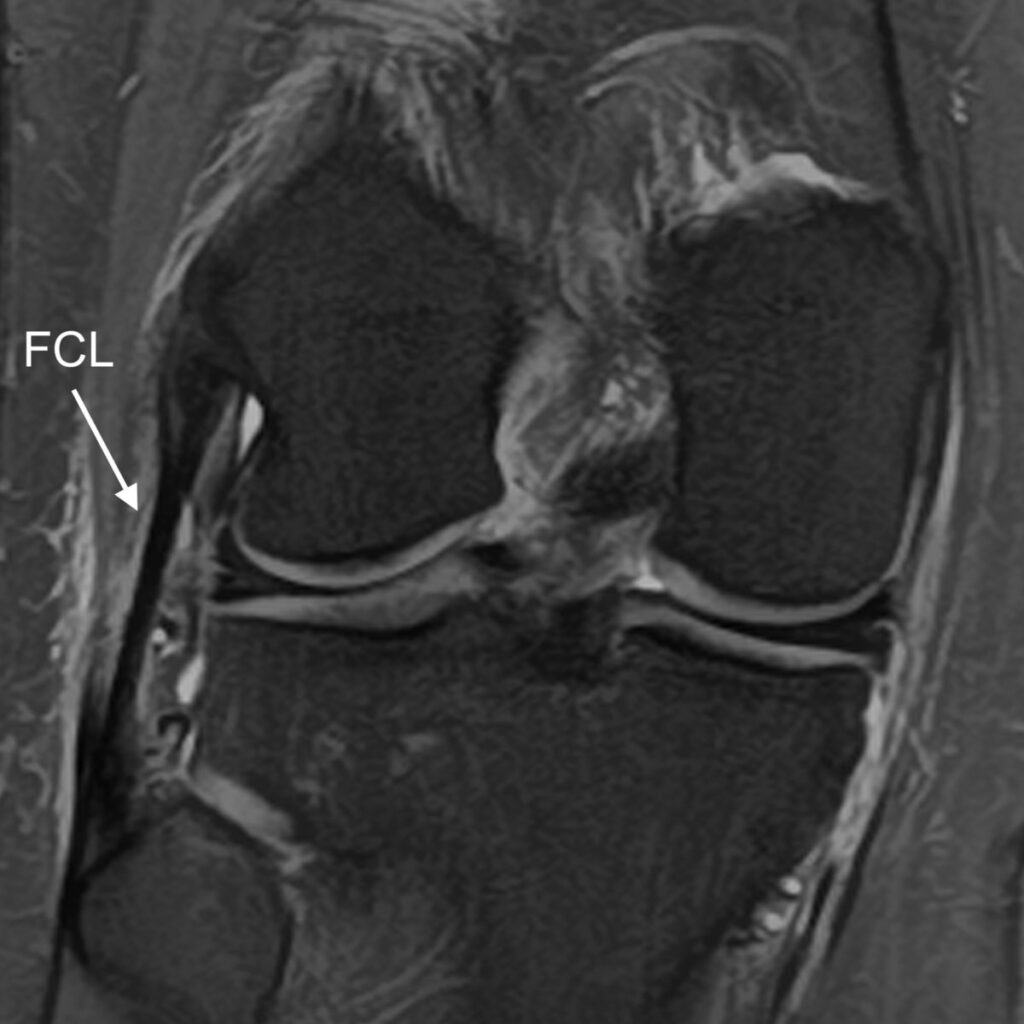
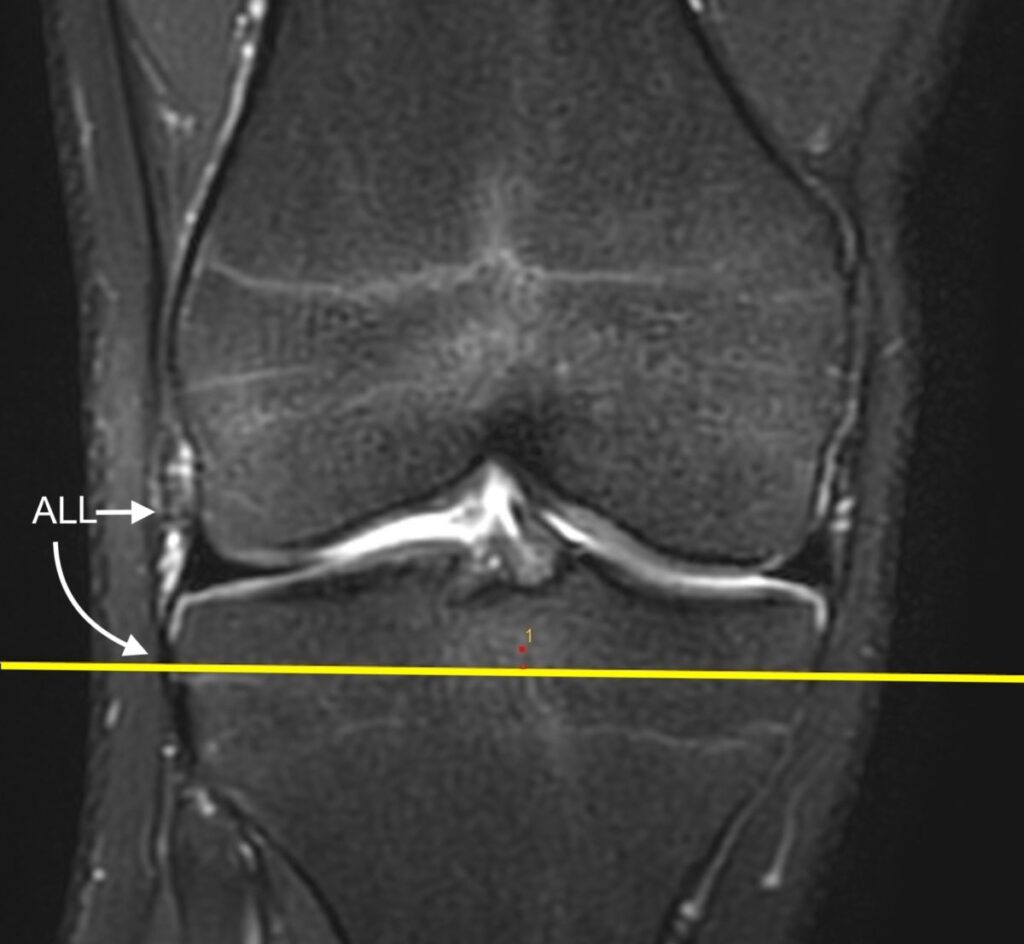
2b: Coronal image located slightly more posteriorly demonstrates an intact fibular collateral ligament (FCL).
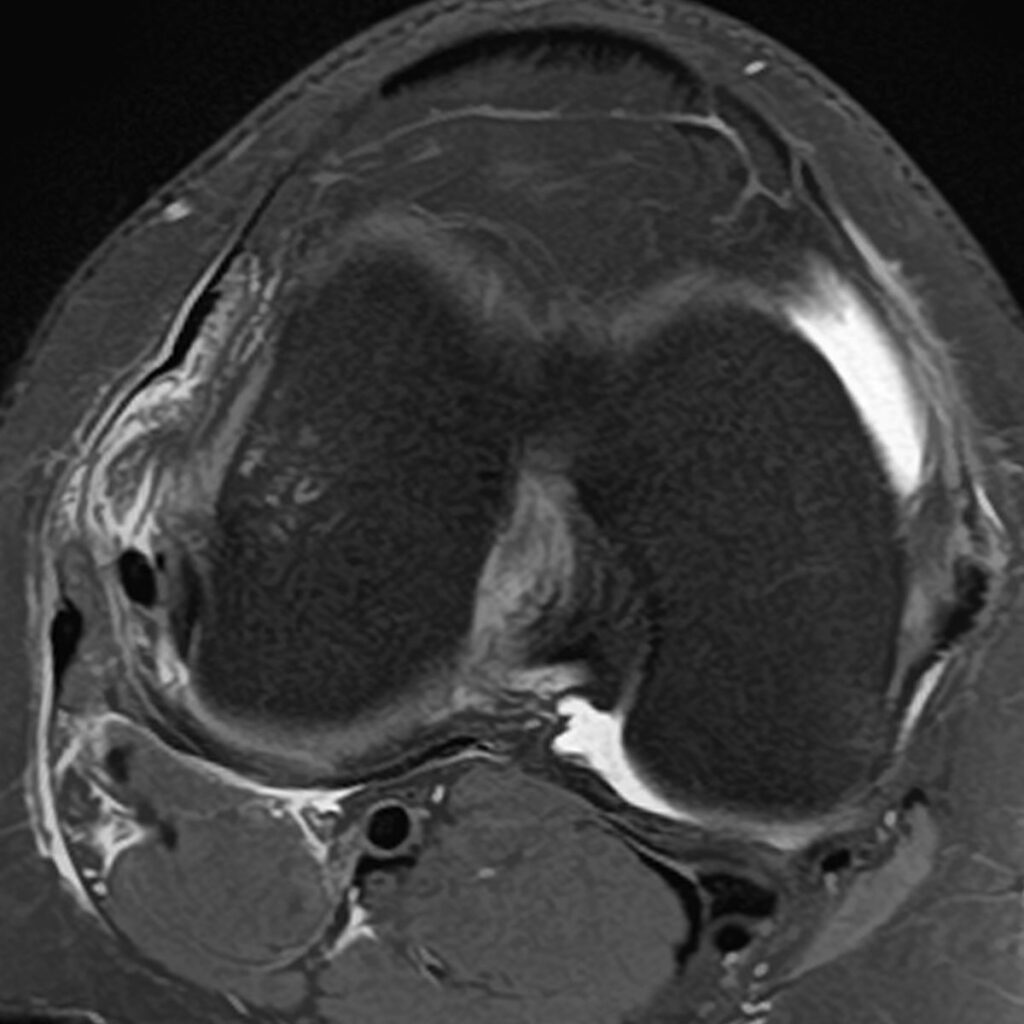
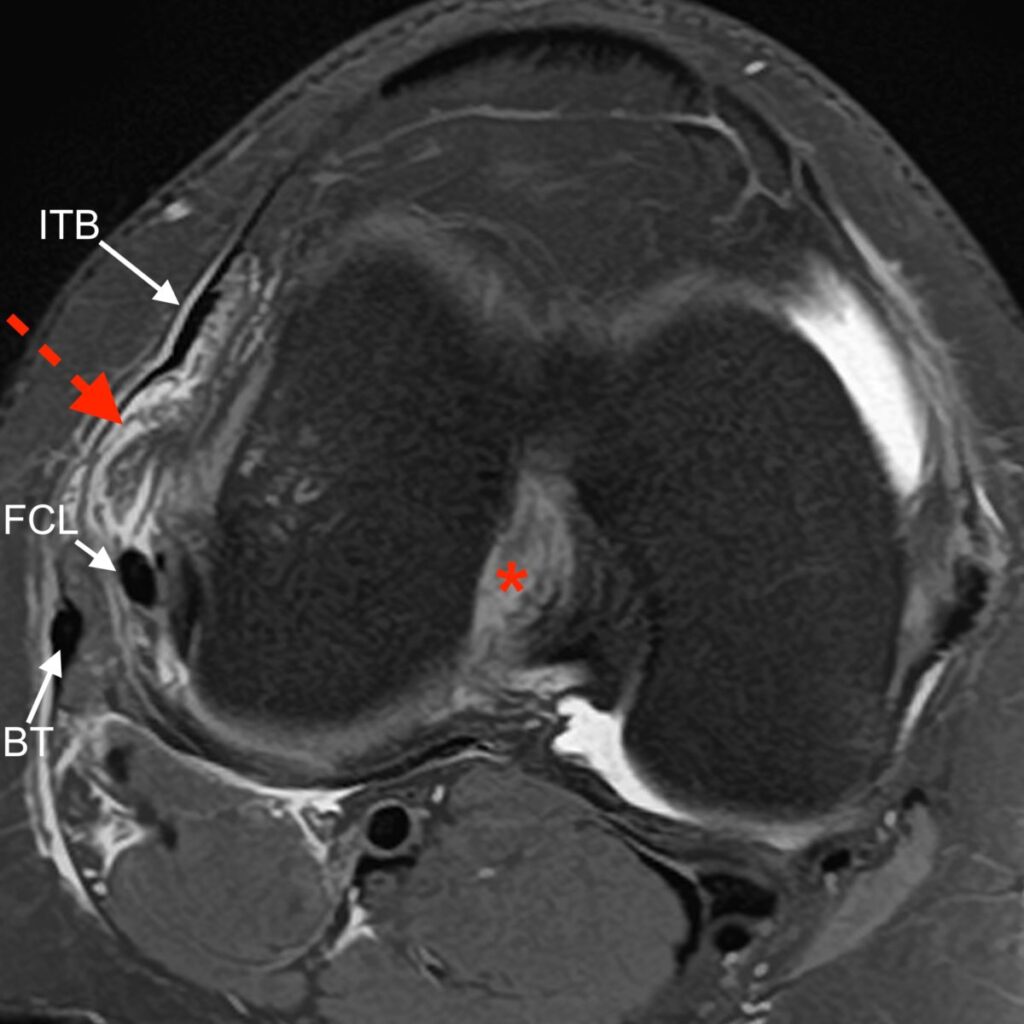
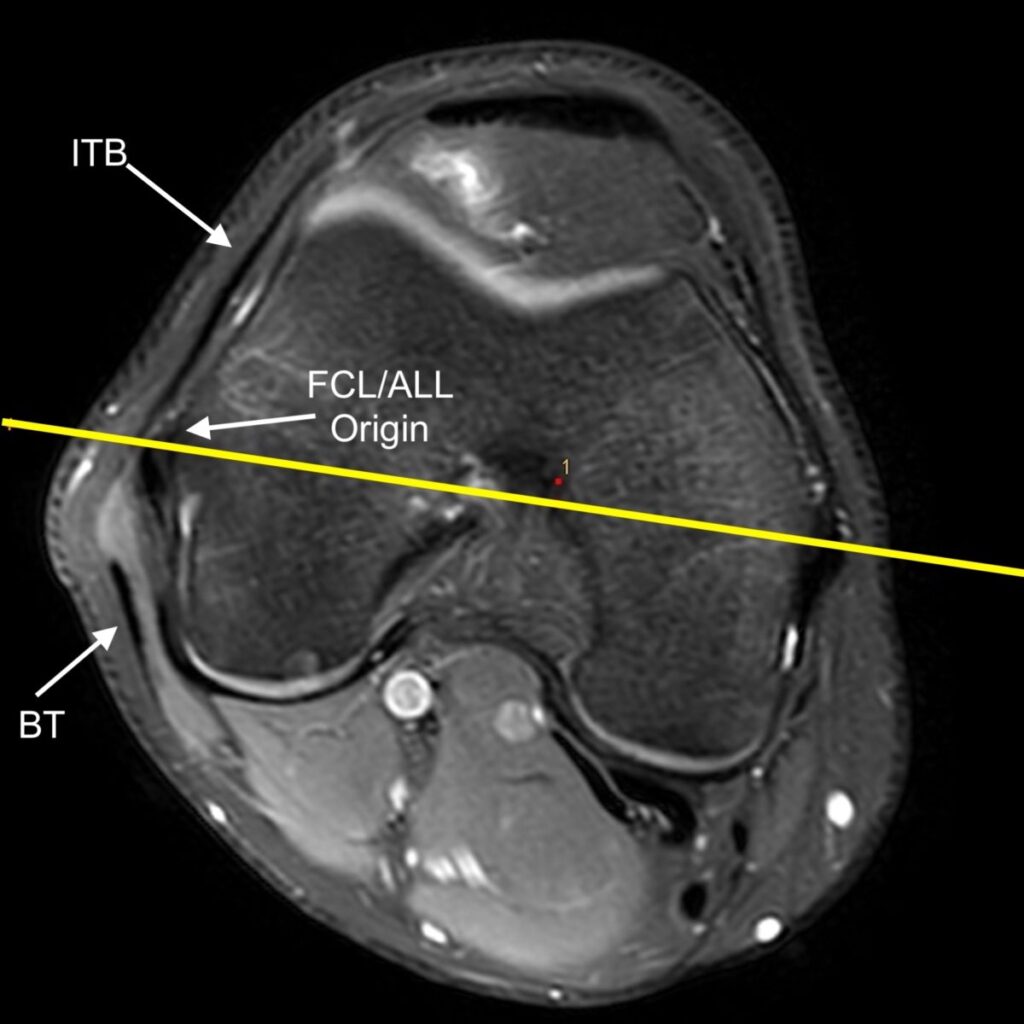
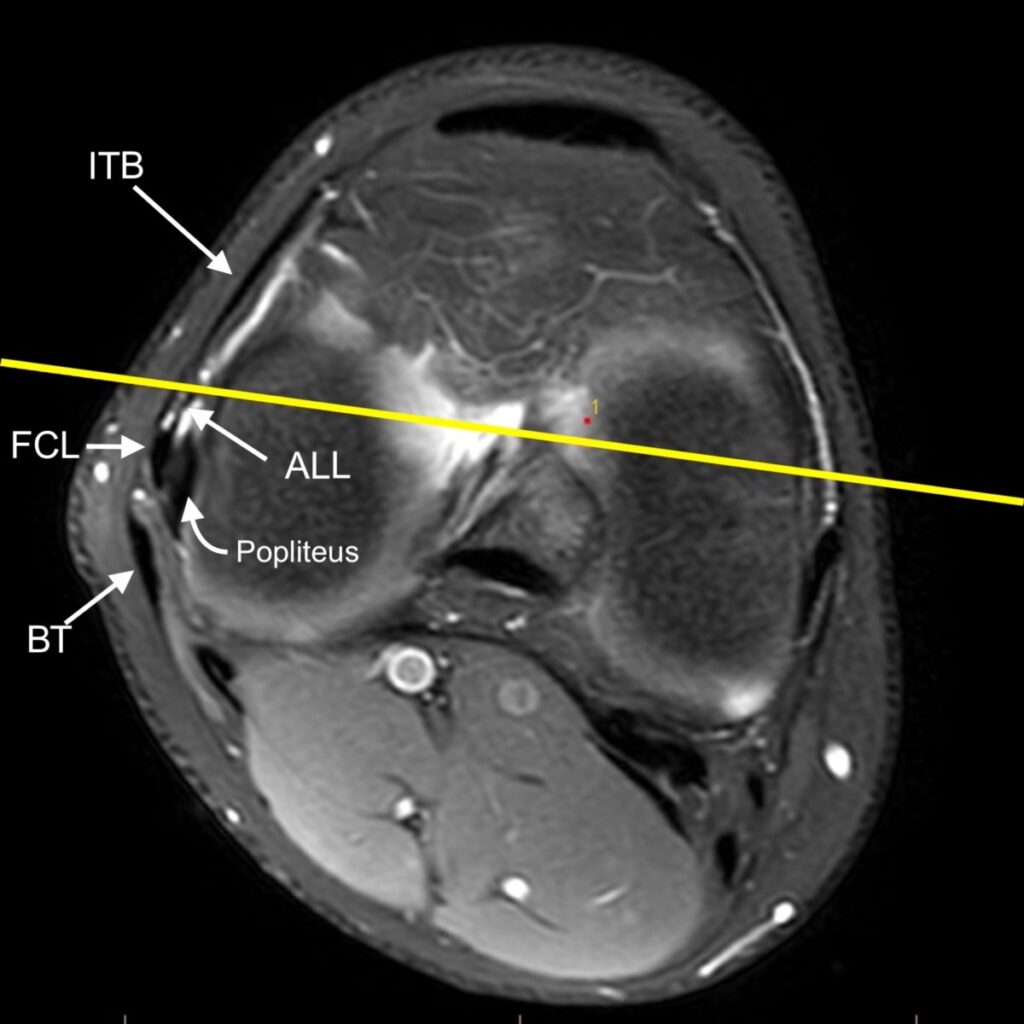
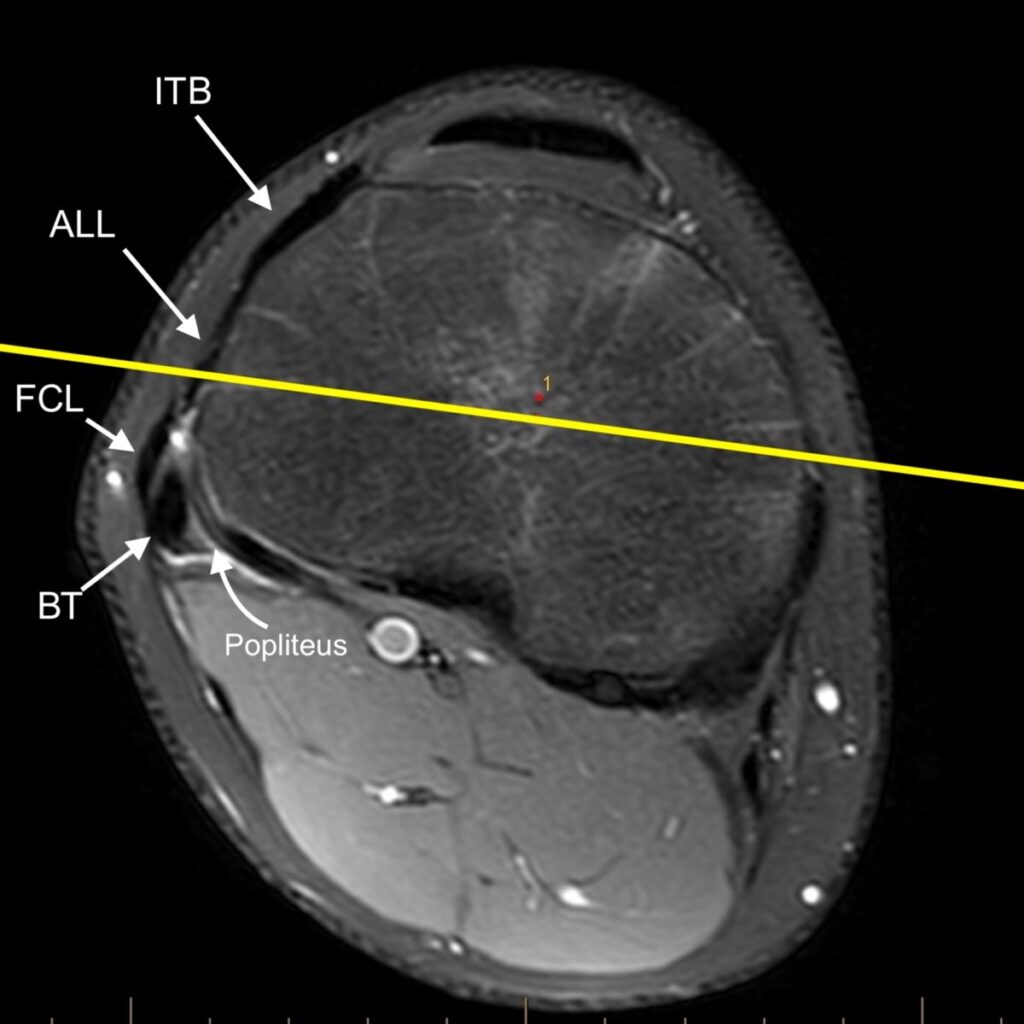
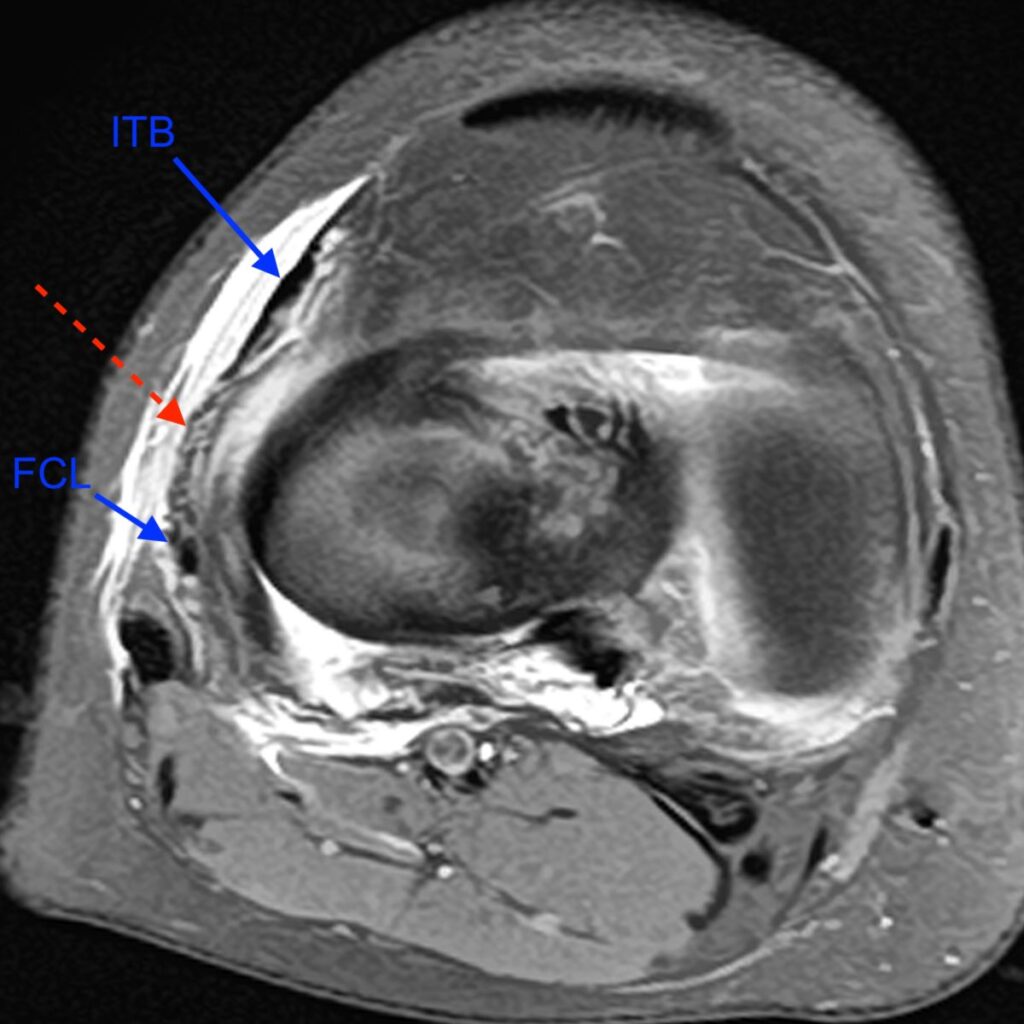
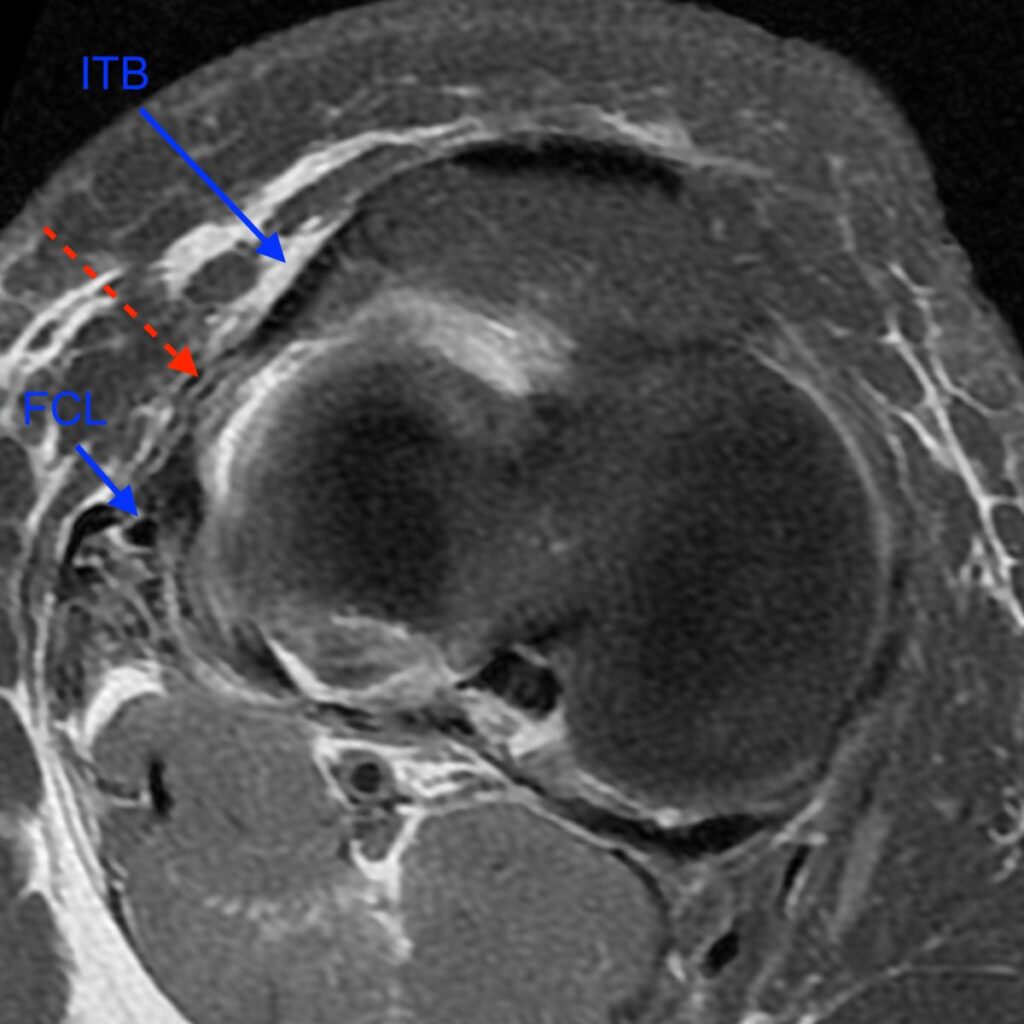
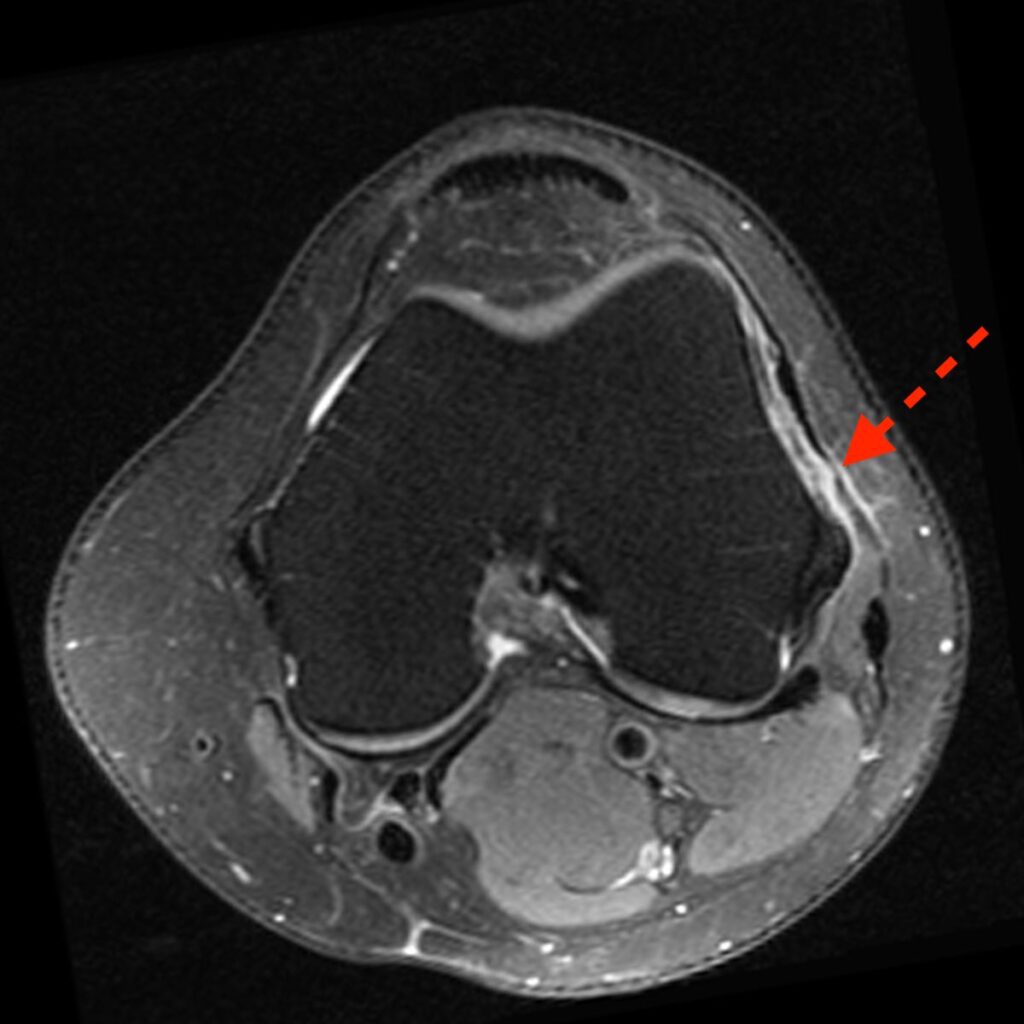
3c: Axial fat-suppressed proton density-weighted image demonstrates a disrupted anterolateral ligament (dashed arrow) and disrupted anterior cruciate ligament (*). The distal iliotibial band (ITB), fibular collateral ligament (FCL), and distal biceps femoris tendon (BT) are also labeled.
Diagnosis
Tear of the anterolateral ligament.
Introduction
In 1879, Segond1 first described the anterolateral ligament (ALL) of the knee as a “pearly, resistant, fibrous band which invariably showed extreme amounts of tension during forced internal rotation” at the location of the eponymous Segond fracture. Since Segond’s initial ‘pearly band’ description, multiple anatomic labels for the structure were subsequently described including ‘mid-third lateral capsular ligament’, capsule-osseous layer of the iliotibial band’, and ‘anterolateral ligament’ 2,3,4 In 2013, an anatomic article by Claes et al. generated renewed interest and clarification of the structure, finding a distinct well-defined ALL in 97% of their gross anatomic dissections.2 Claes also hypothesized that the ALL controls internal tibial rotation and therefore affects the pivot-shift mechanism. This web clinic reviews the gross and MRI anatomy of the ALL, imaging of ALL tears, and treatment options.
Gross Anatomy
According to Claes’ findings2,5, the ALL is a distinct ligamentous structure along the knee, connecting the femur with the tibia. The ALL is easily distinguishable from the thinner joint capsule, located more anteriorly. In addition to the femoral and tibial attachments, the ALL also has meniscal attachment. Each of these three attachments can be considered when analyzing the anatomy of an ALL. The proximal attachment of the ALL is located at the lateral femoral condyle, slightly anterior and distal to the fibular collateral ligament (FCL). The posterior fibers of the ALL blend with the proximal portion of the FCL in the majority of cases. The middle portion of the ALL runs obliquely towards the anterolateral proximal tibia, with a strong connection to the periphery of the lateral meniscus mid body. The meniscal attachments can be divided into meniscofemoral and meniscotibial attachments. The lateral inferior geniculate artery and vein are located between the lateral meniscus periphery and the ALL at the level of the joint line. The distal attachment of the ALL is located along the anterolateral tibia, forming a thick capsular insertional fold, approximately 5.4 mm distal to the tibial plateau, midway between the lateral border of Gerdy’s tubercle and the anterior margin of the fibular head.2,3
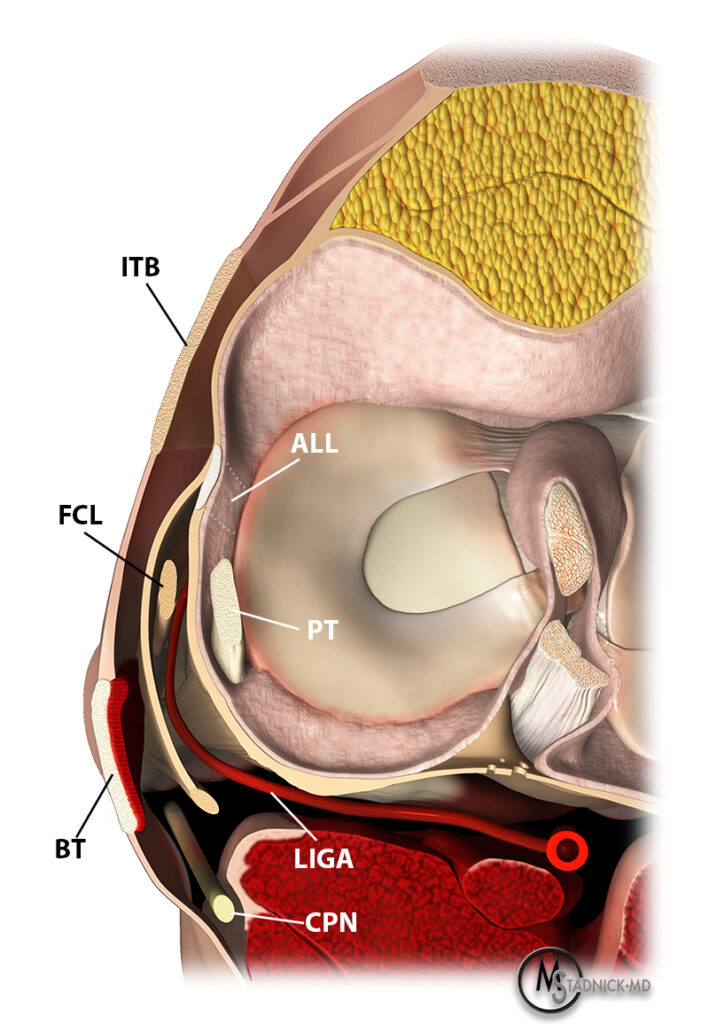
Figure 4:
Axial knee rendering demonstrates the normal intra-capsular course of anterolateral ligament (ALL) with the surrounding layered anatomy. The distal iliotibial band (ITB), fibular collateral ligament (FCL), biceps tendon (BT), popliteus tendon (PT), lateral inferior geniculate artery (LIGA), and common peroneal nerve (CPN) are also labeled.
MRI Anatomy
The ALL can be visualized with MRI3,6 and is best seen on high resolution fat-suppressed proton density coronal and axial images. Using PACS software cross-referencing tools is also helpful to triangulate the anatomy. On coronal imaging, the proximal ALL is difficult to differentiate from the proximal FCL, which lies in close proximity. As previously mentioned, the ALL typically arises slightly anterodistal to the FCL. As the ALL continues distally, it passes superficial to the popliteus tendon, subsequently bifurcating into meniscal and tibial attachments. This bifurcation occurs just proximal to the level of the lateral inferior genicular artery, which is a reproducible landmark on coronal imaging. The meniscal attachment occurs just proximal to the artery, while the tibial attachment occurs about 5 mm distal to the lateral tibial plateau3,5 (figure 5e). On axial imaging, it is helpful to first identify the biceps femoris tendon (BF), FCL, and iliotibial band (ITB), arranged from posterior to anterior (figures 5b, d, f). Next, identify the FCL at the level of the lateral femoral condyle attachment. While the ALL arises slightly anterodistal to the FCL, it is easiest to group two structures into the same location on axial imaging (figure 5b). On more distal axial imaging, the ALL continues its anteroinferior course. Just proximal to the lateral inferior geniculate artery, the ALL bifurcates into its meniscal attachment (difficult to resolve on axial imaging) and ultimately to its distal tibial attachment. The tibial branch attachment of the ALL is located 5 mm distal to the lateral tibial articular surface, halfway between the FCL and ITB (figure 5f).
Figure 5:
5a, b: Normal MR ALL Anatomy - Proximal
Cross-referenced coronal (figure 5a) and axial (figure 5b) fat-suppressed proton density-weighted images at the level of the proximal ALL demonstrate the FCL and ALL origins at the lateral femoral condyle, which lie in close proximity. The fibular collateral ligament (FCL), popliteus tendon, lateral inferior geniculate artery (LIGA), biceps tendon (BT), and iliotibial band (ITB) are also labeled for orientation.
5c, d: Normal MR ALL Anatomy - Mid
Cross-referenced coronal (figure 5c) and axial (figure 5d) fat-suppressed proton density-weighted images at the level of the mid ALL. The ALL passes superficial to the popliteus tendon, subsequently bifurcating into meniscal and tibial attachments. This bifurcation occurs just proximal to the level of the lateral inferior genicular artery (LIGA), best seen on coronal imaging. The fibular collateral ligament (FCL), popliteus tendon, biceps tendon (BT), and iliotibial band (ITB) are again labeled for orientation.
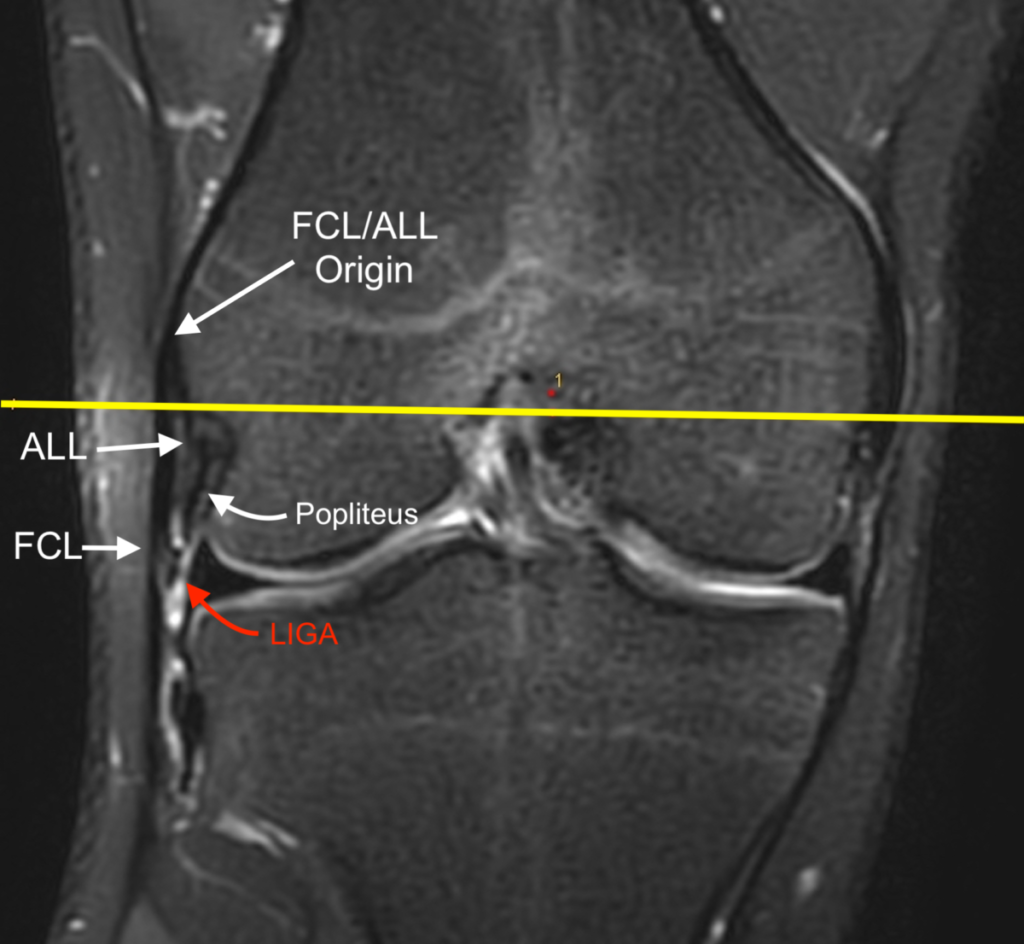
5e, f: Normal MR ALL Anatomy - Distal
Cross-referenced coronal (figure 5e) and axial (figure 5f) fat-suppressed proton density-weighted images at the level of the distal ALL. The meniscal and tibial attachments of the ALL can be seen on the coronal image (figure 5e). The tibial branch attachment of the ALL is located 5 mm distal to the lateral tibial articular surface, halfway between the FCL and ITB.
MRI Appearance of ALL Tears
ALL tears are most commonly seen in conjunction with tears of the anterior cruciate ligament (ACL). While identifying the ALL can be challenging due to its small size, oblique orientation, and proximity to other structures, it is helpful to maintain a high index of suspicion for ALL injury when an ACL tear is present. In a study by Feretti et al7, ALL abnormalities were seen in 88.2% of acutely ACL-injured knees imaged at 1.5 tesla MRI. An abnormal ALL is characterized by caliber changes, signal alterations, wavy, discontinuous, or irregular fibers. Tearing of the adjacent lateral capsule is also a common association, reported to coexist in 88% of cases. Lateral bone bruises are often present, and the adjacent genicular vessels may also show displacement or irregularity.
Figure 6:
ALL tear – Example 2
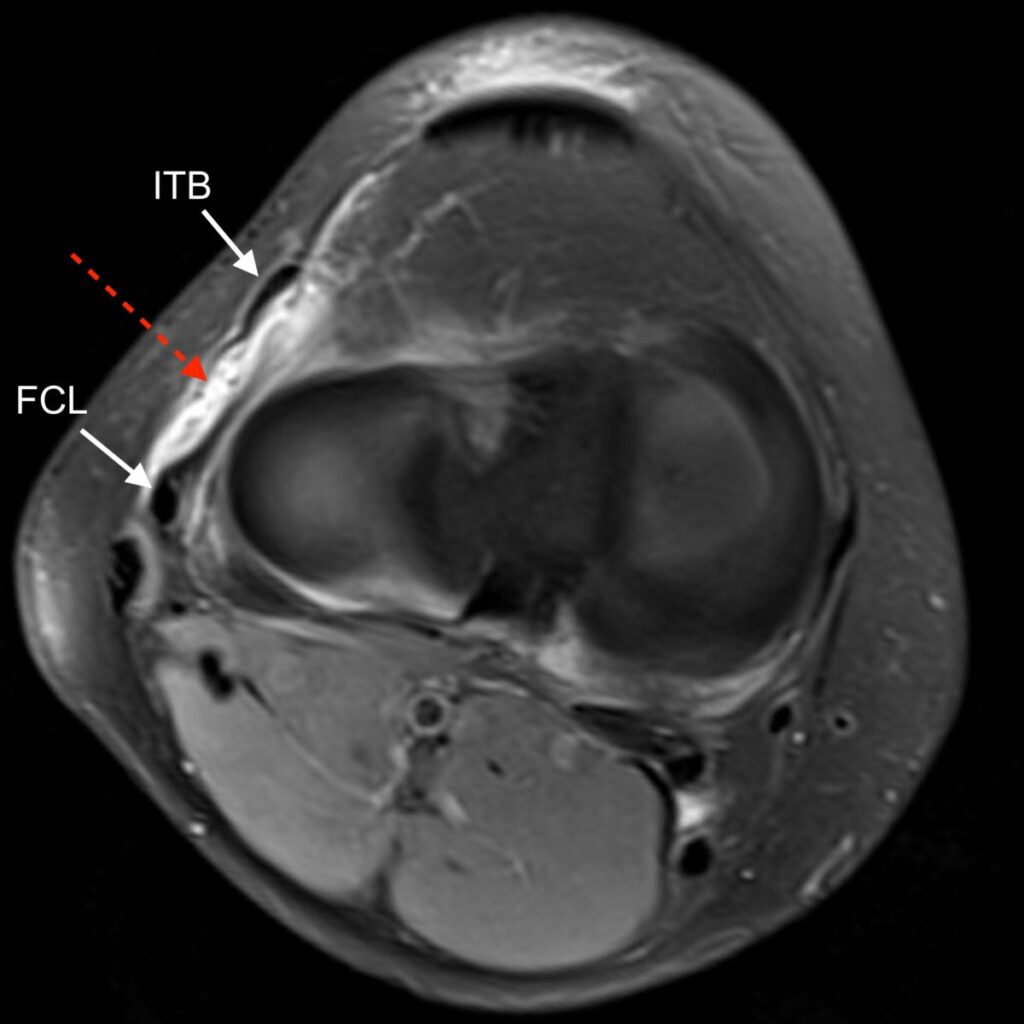
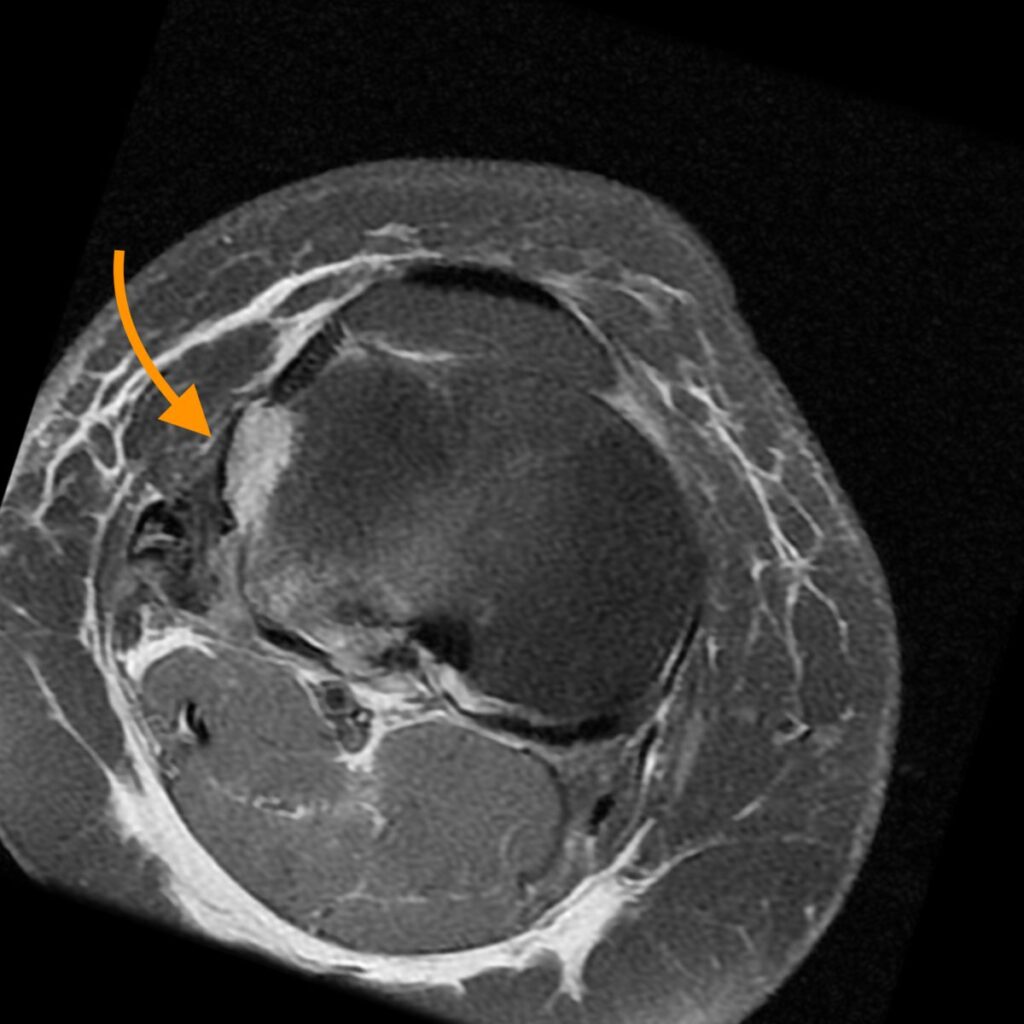
6a: Axial fat-suppressed proton density-weighted image demonstrating a disrupted anterolateral ligament (dashed arrow). The iliotibial band (ITB) fibular collateral ligament (FCL) are also labeled.
6b: Coronal image located slightly more anteriorly demonstrating a disrupted anterolateral ligament (dashed arrow).
Figure 7:
ALL tear – Example 3
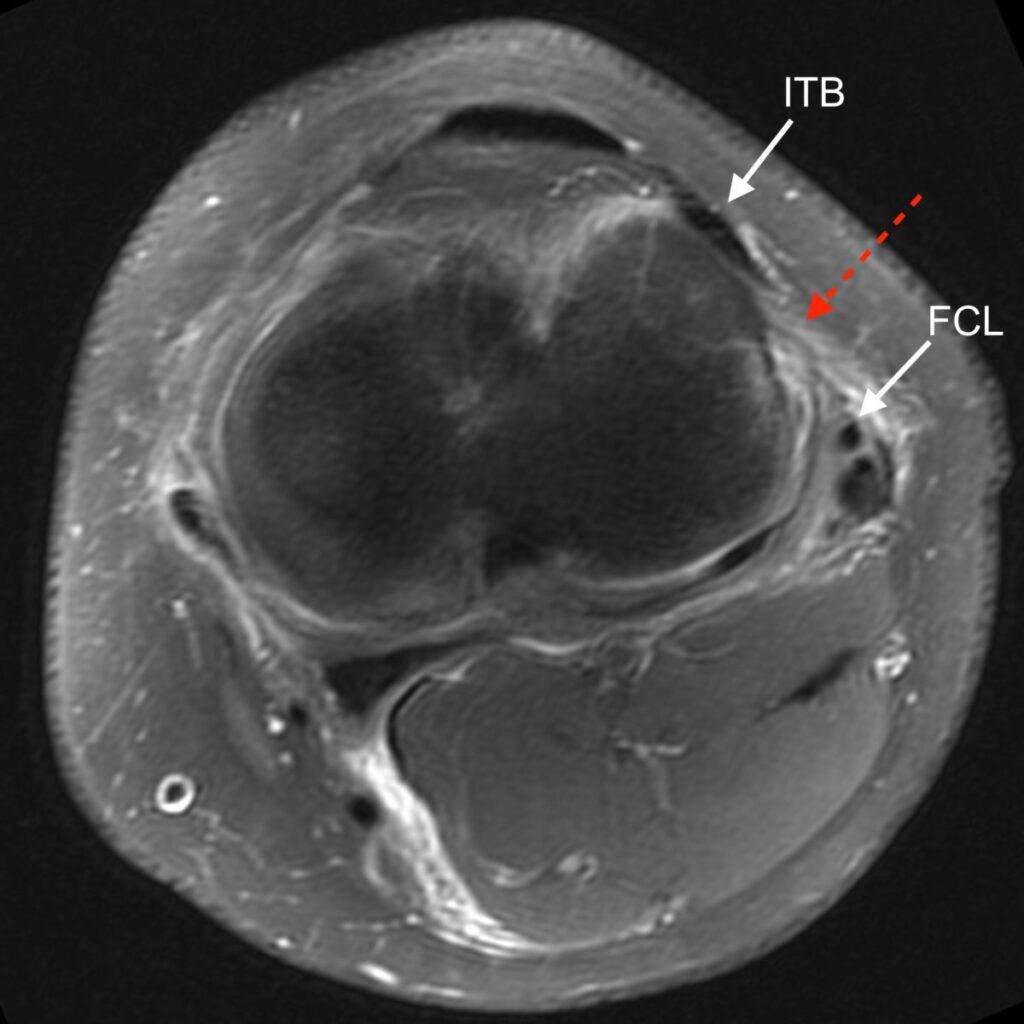
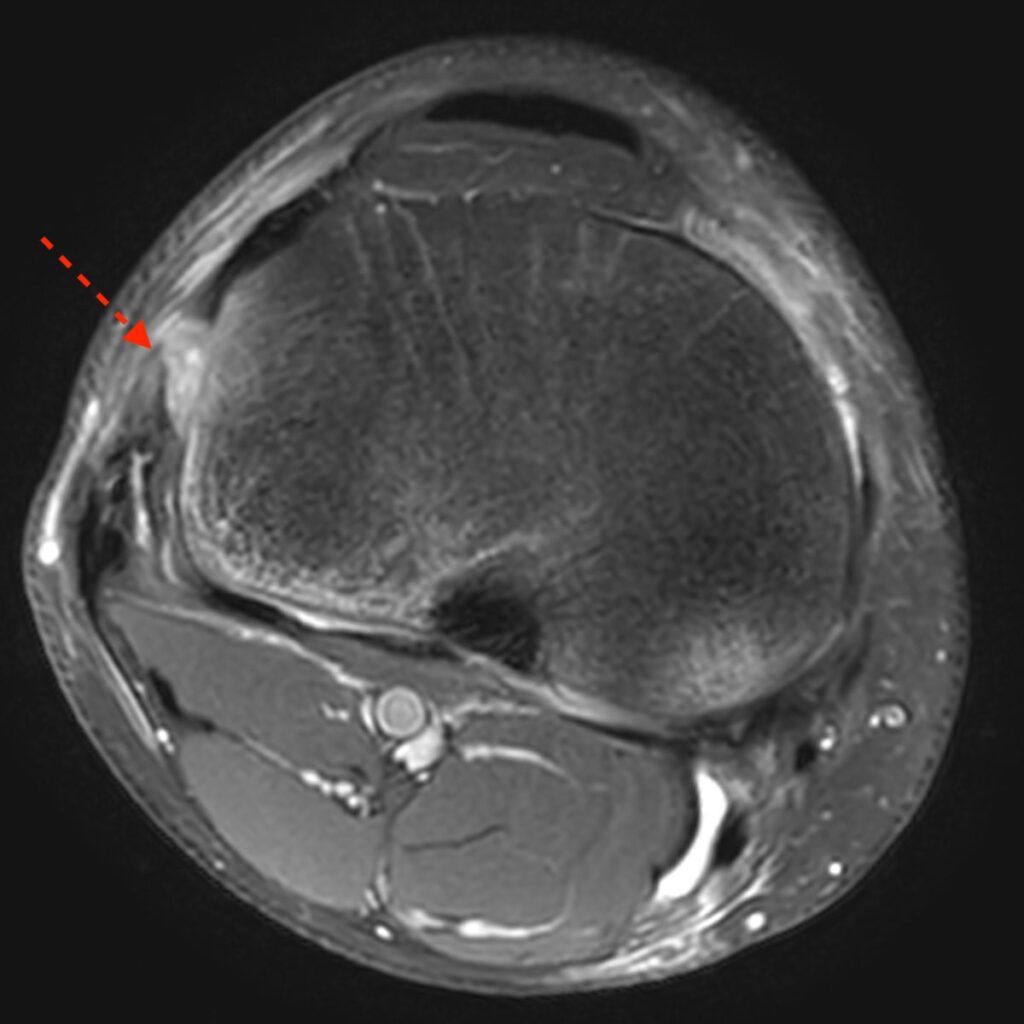
7a: Axial fat-suppressed proton density-weighted image demonstrating a disrupted anterolateral ligament (dashed arrow). The iliotibial band (ITB) and fibular collateral ligament (FCL) are again labeled.
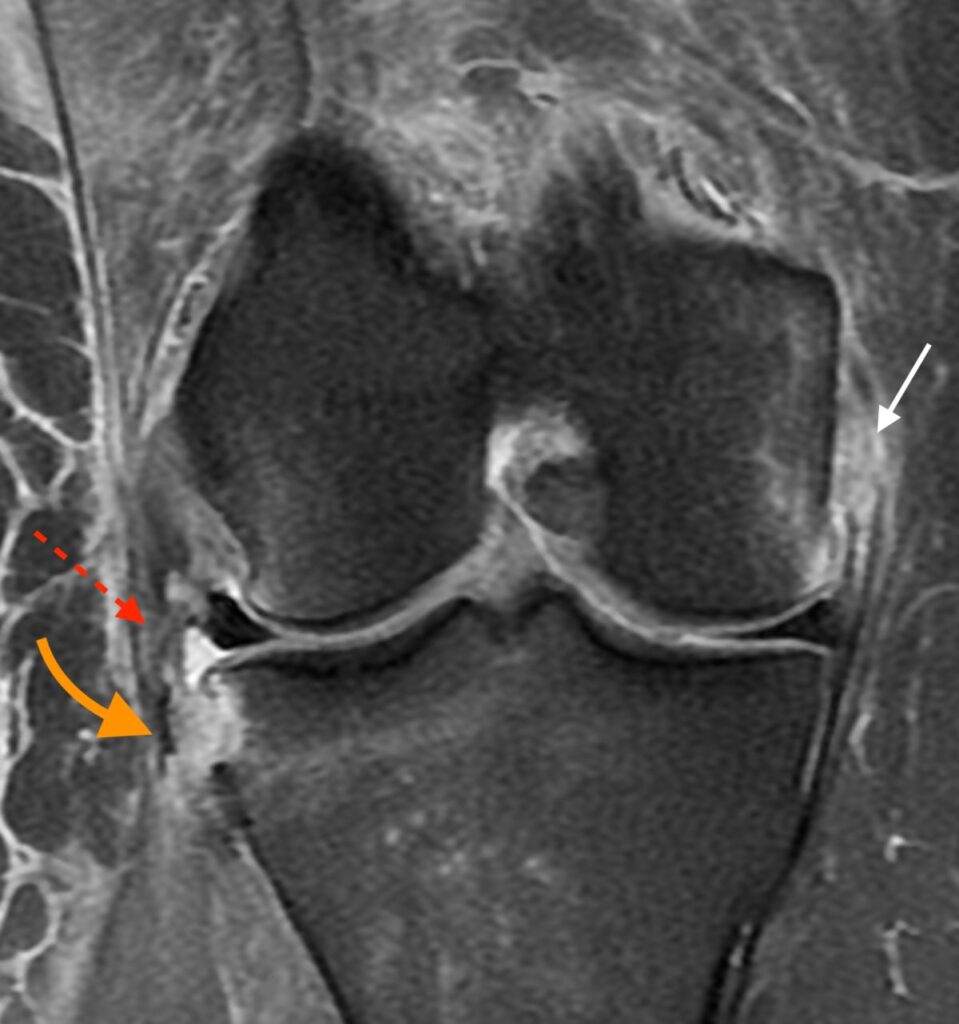
7b: Coronal image located slightly more anteriorly demonstrating a disrupted anterolateral ligament (dashed arrow). I high grade MCL sprain (white arrow) is also present.
Figure 8:
Segond fracture with ALL tear
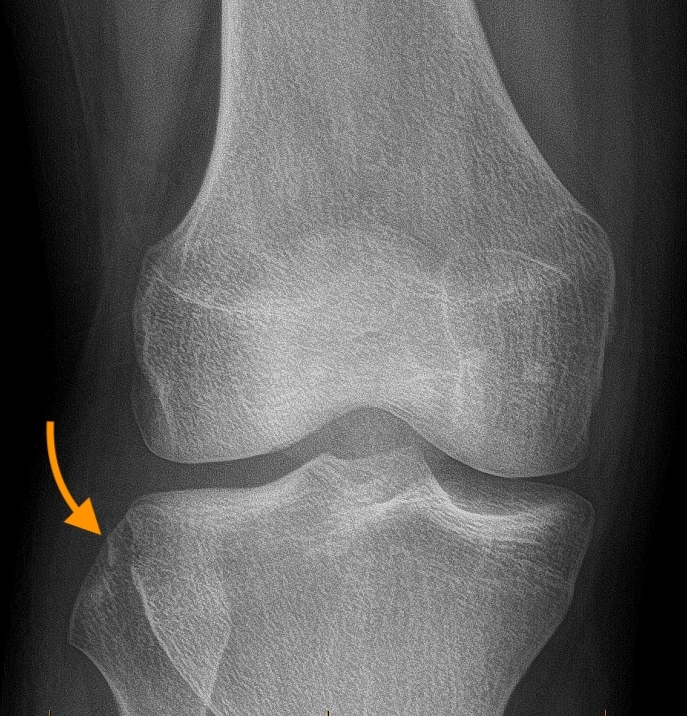
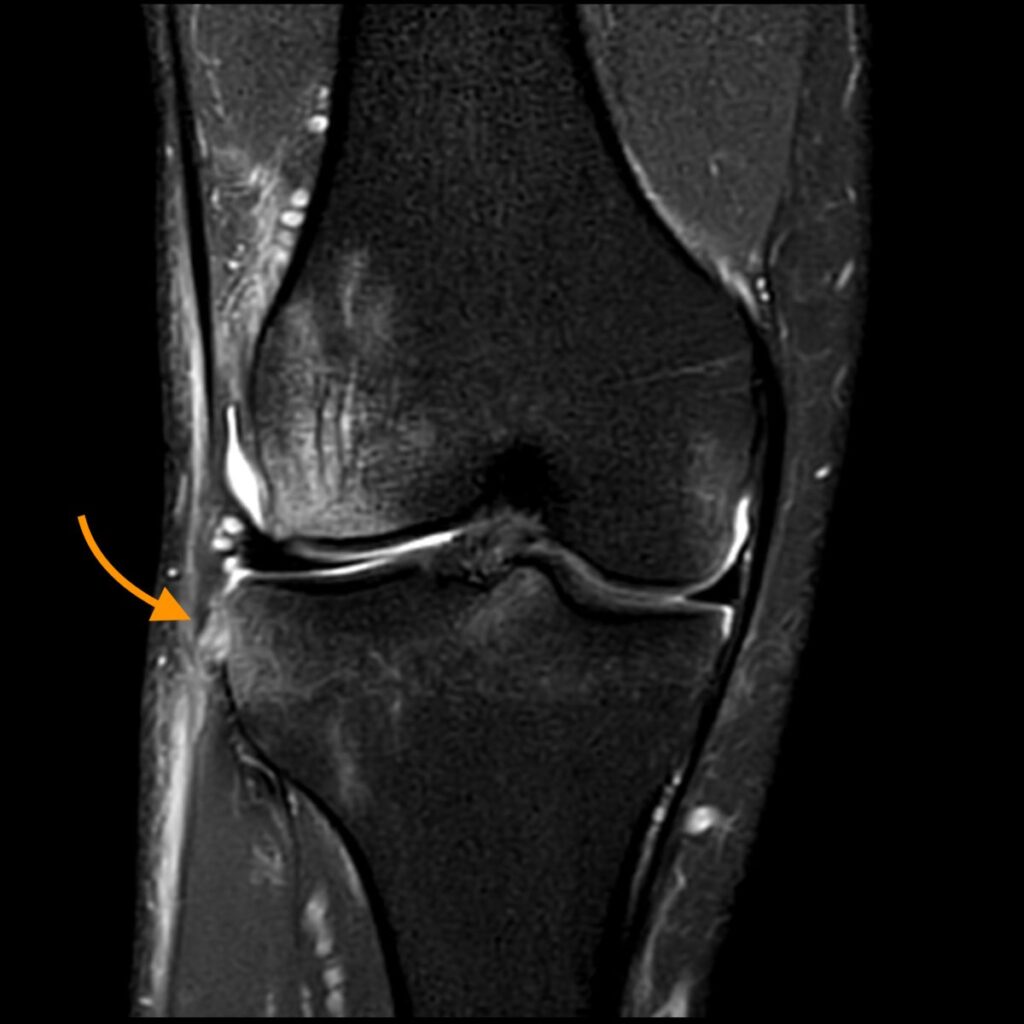
8a: Frontal x-ray image demonstrates a slightly displaced cortical avulsion fracture of the anterolateral tibia (Segond fracture).
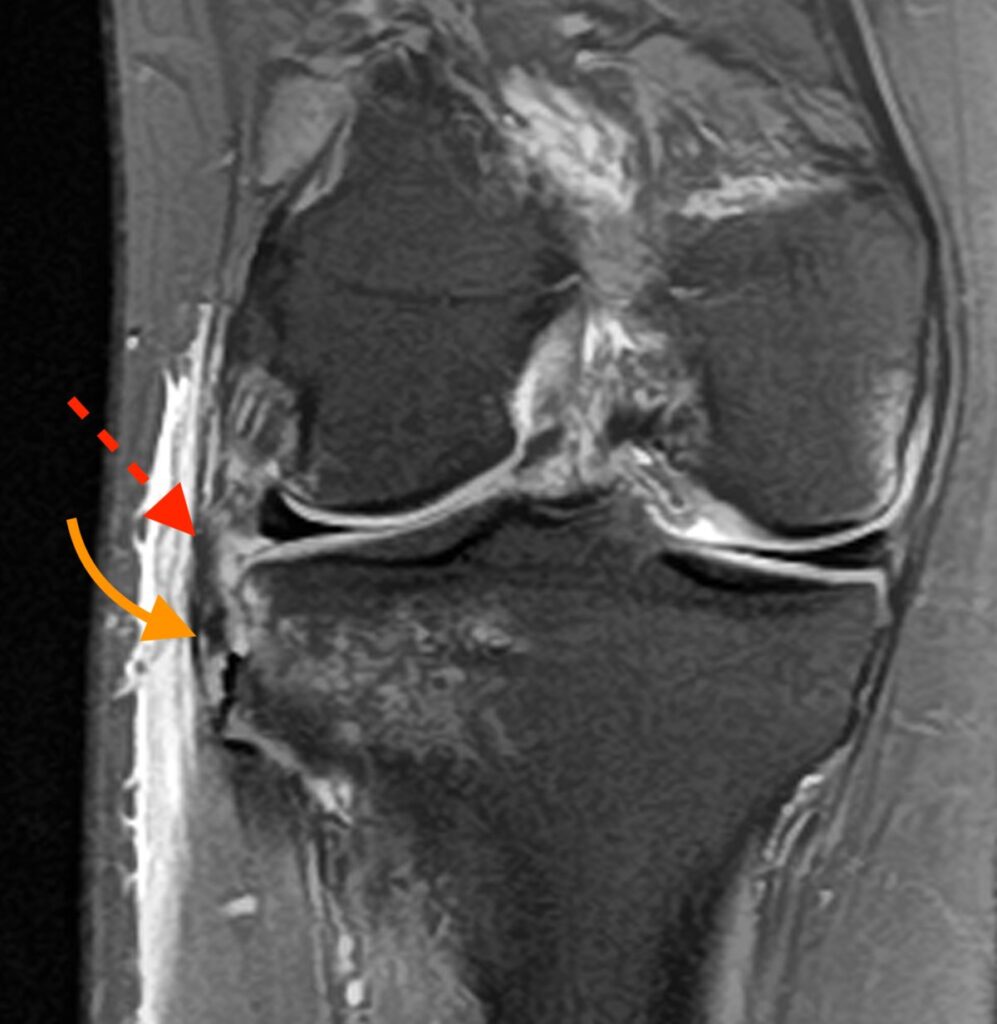
8b: Coronal fat-suppressed proton density-weighted image shows the low signal Segond fracture (curved arrow) and adjacent disrupted ALL (dashed arrow).
8c: Axial fat-suppressed proton density-weighted image confirms the disrupted anterolateral ligament (dashed arrow), with surrounding edema.
Figure 9:
Segond fracture with ALL tear - Example 2
9a: Axial fat-suppressed proton density-weighted image demonstrates a disrupted ALL (dashed arrow).
9b: Axial image slightly more inferior demonstrates a mildly displaced Segond fracture fragment (curved arrow).
9c: Coronal fat-suppressed proton density-weighted image confirms the Segond fracture (curved arrow) and disrupted ALL (dashed arrow). A proximal medial collateral ligament tear is also present (straight arrow).
Treatment
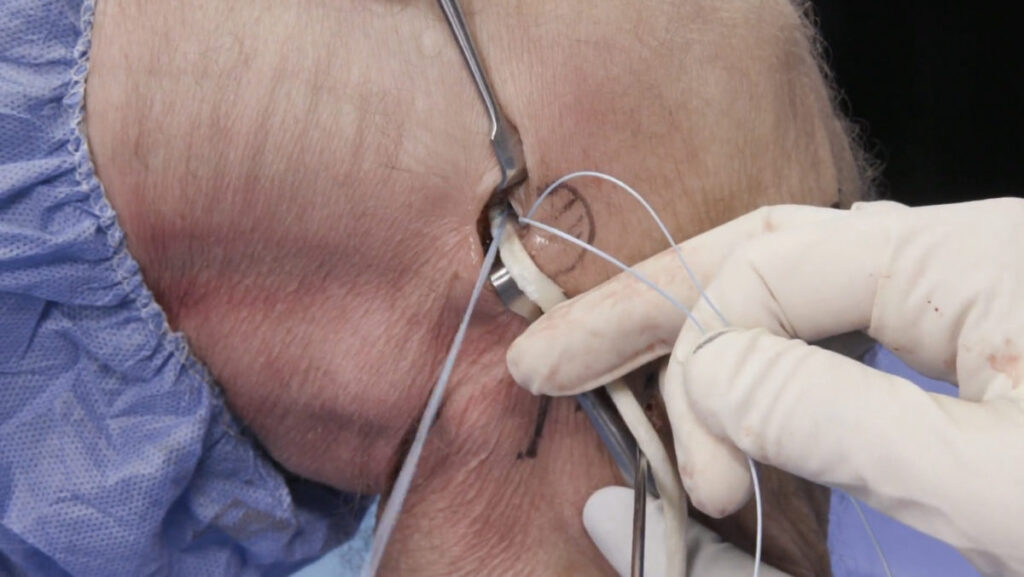
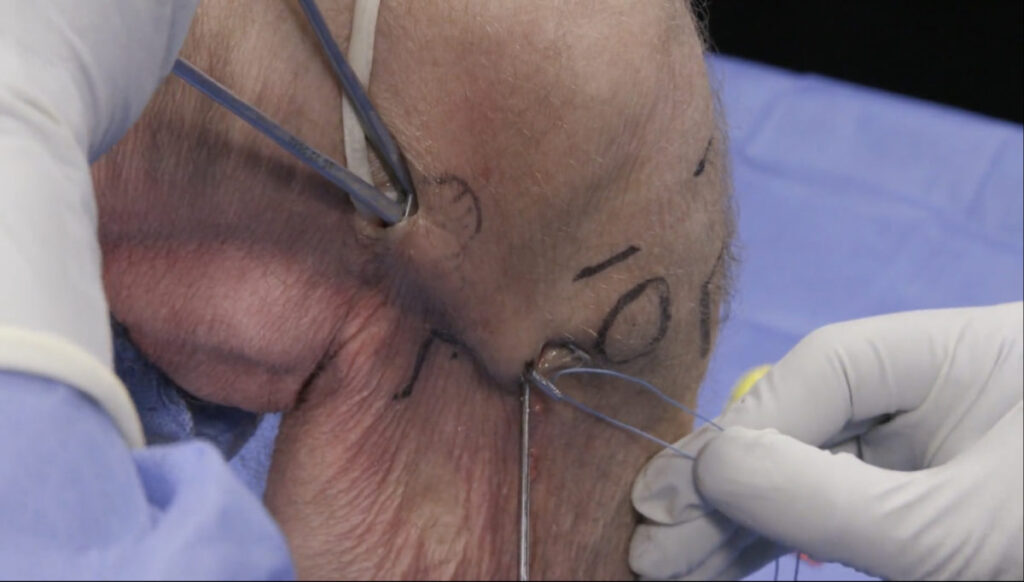
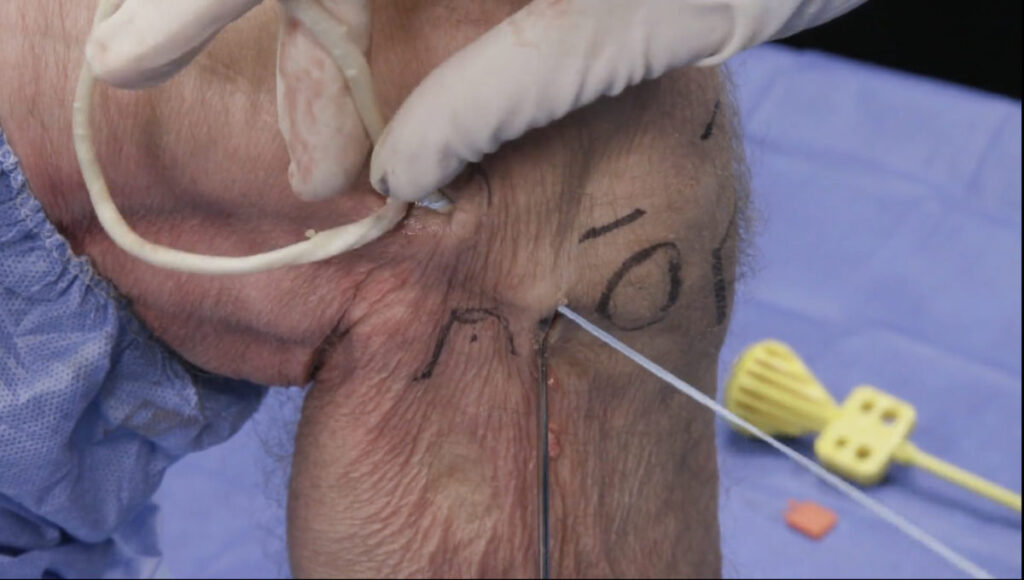
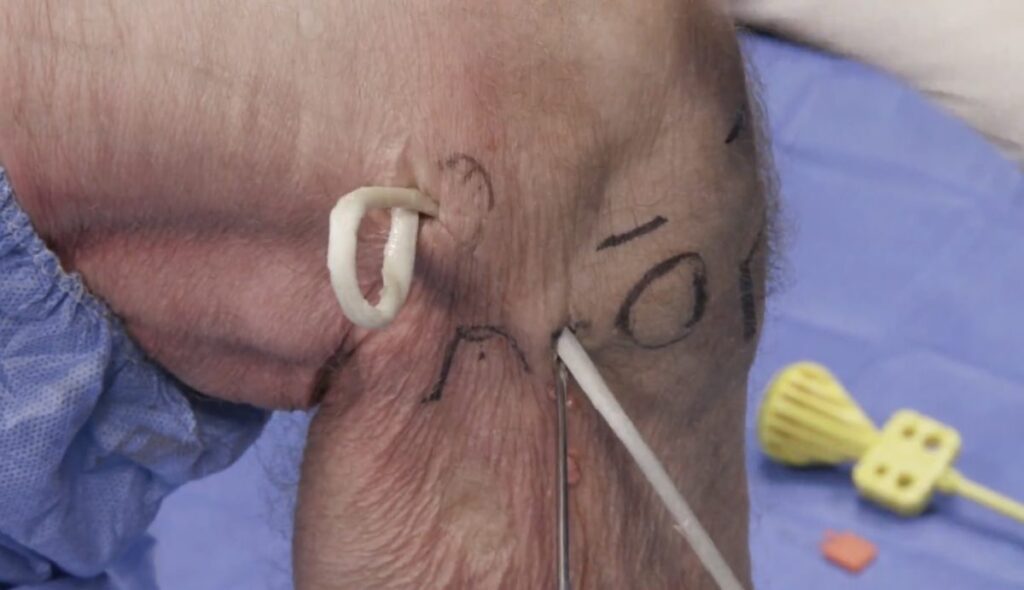
Some surgeons may opt to perform a reconstruction of the ALL in conjunction with an ACL repair. The indications for ALL reconstruction are not clearly defined in the literature and are often based on the surgeon’s experience. Some of the reported guidelines for considering an ALL reconstruction include: revision ACL reconstruction, grade III pivot-shift injury (clearly positive in neutral rotation and particularly conspicuous in external rotation), participation in contact/pivoting/cutting sports, competitive athletes, and age ≤ 25 years.8,9,10 ALL reconstruction is typically performed extra-articularly, using a gracilis tendon autograft. After the surface anatomy is identified and marked, femoral and tibial stab incisions are made. A femoral incision is made slightly proximal and posterior to the lateral epicondyle; a tibial incision is made halfway between the fibular head and Gerdy’s tubercle. The gracilis tendon graft is then anchored to the lateral femoral condyle. A hemostat is used to dissect from the femoral incision to the tibial incision, deep to the iliotibial band and superficial to the fibular collateral ligament. The graft is then pulled through the tunnel to the tibial incision, using a passing suture. The graft is anchored to the tibia, tension is adjusted, and the unused portion of the graft is then cut.11
Figure 12:
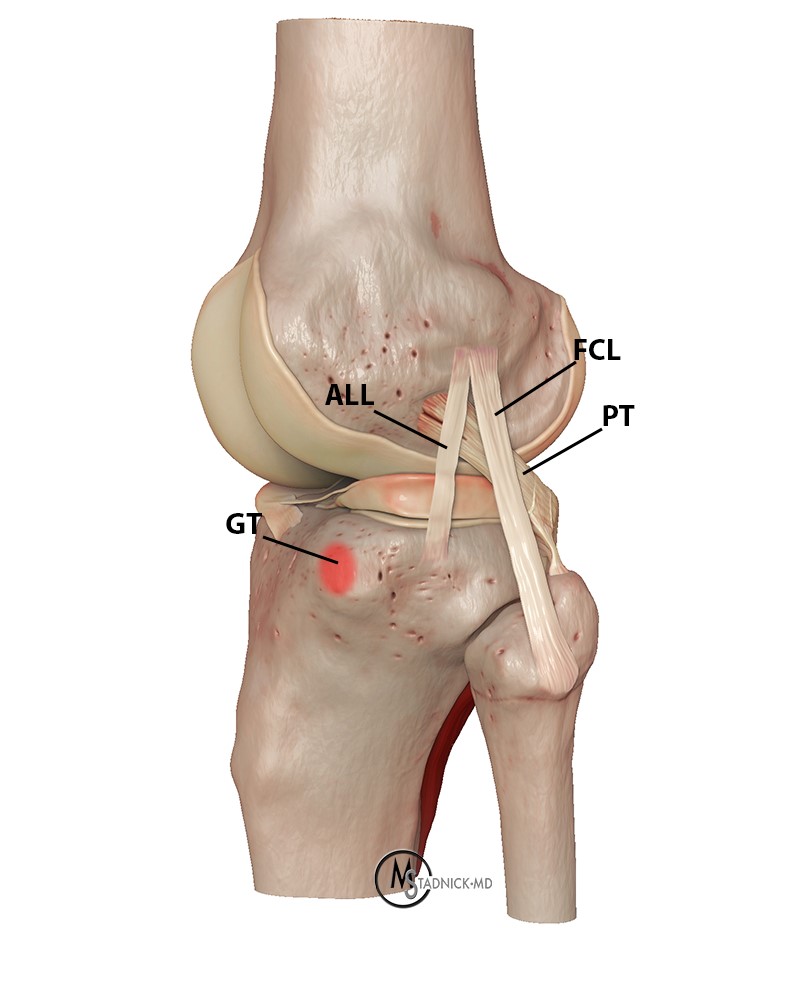
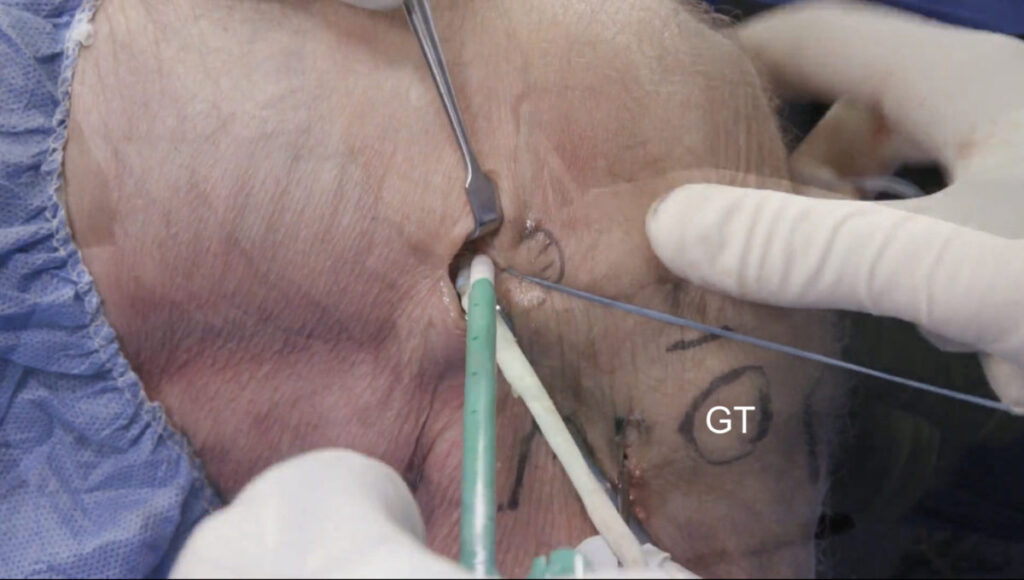
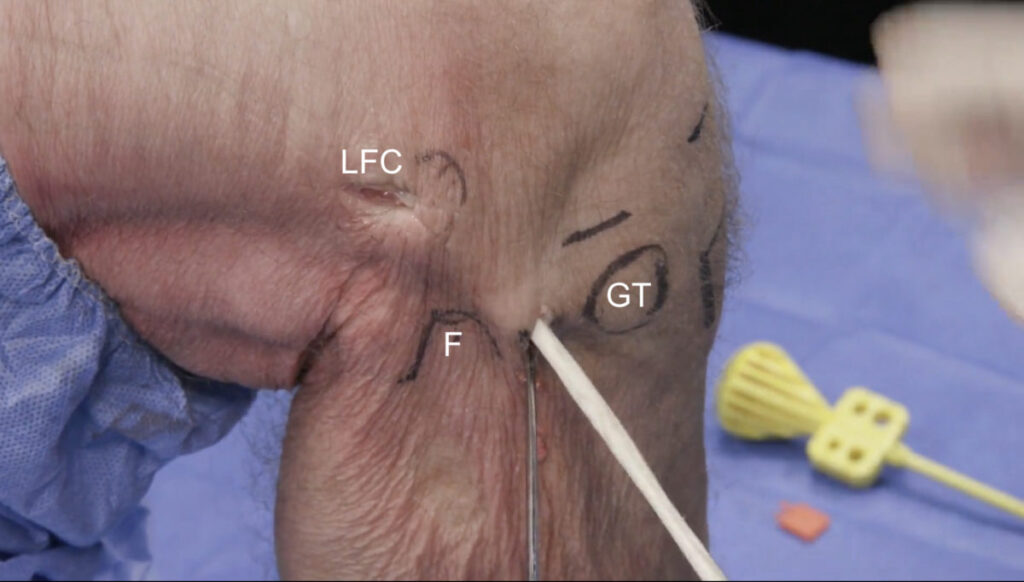
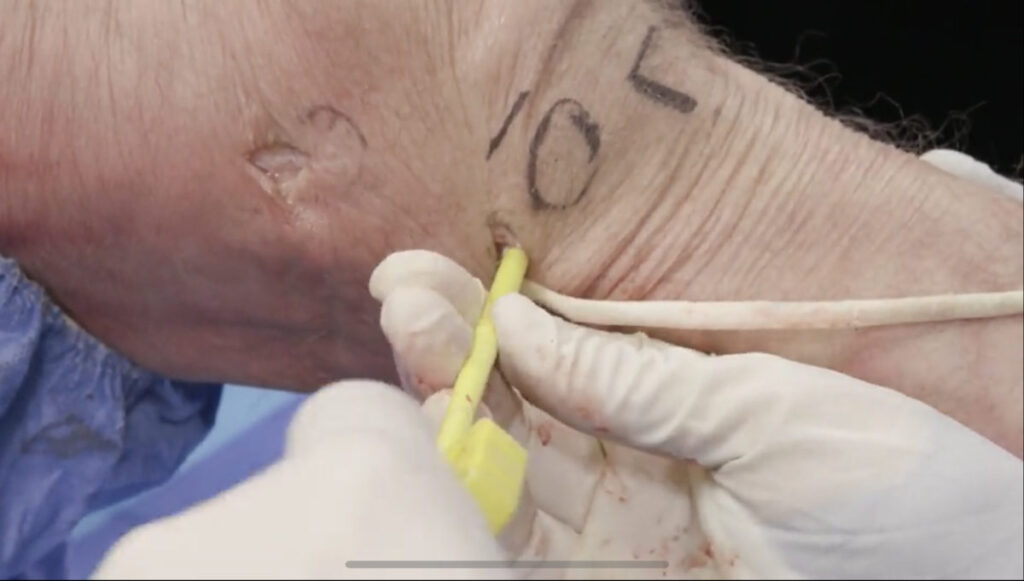
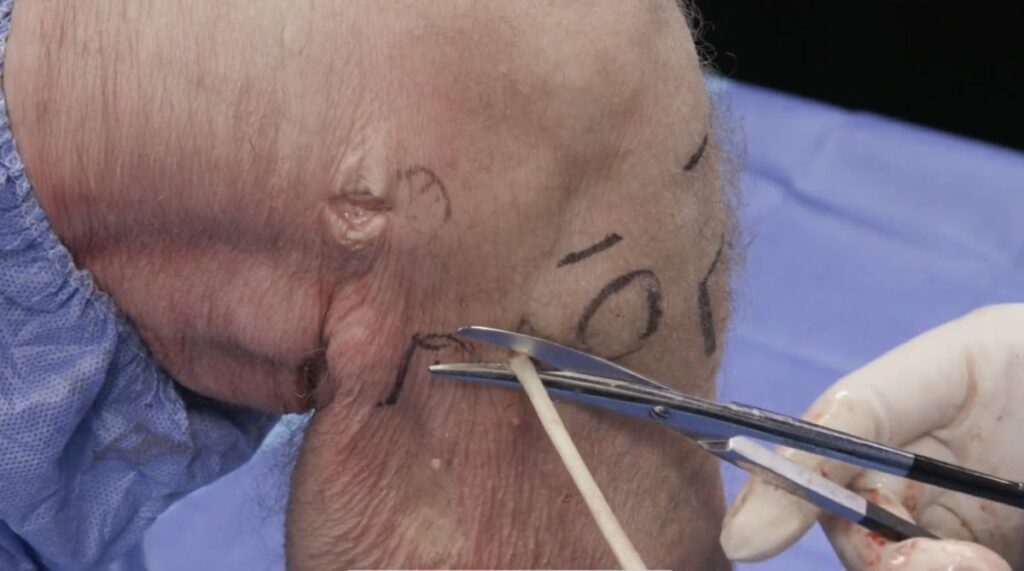
Surgical reconstruction of the ALL
The surface anatomy is first identified and labeled, including Gerdy’s tubercle (GT), the fibular head (F), and lateral femoral condyle (LFC). The tibial attachment site of the ALL lies approximately halfway between the fibular head and Gerdy’s tubercle. A gracilis tendon graft is then extra-articularly anchored to the LFC (figures 12a, b). A tunnel is created between the LFC and ALL attachment (figure 12c). The graft is then pulled through the tunnel (figures 12d-f). Next, the ALL graft is anchored to the tibial attachment site (figure 12g) and the remaining graft tissue is excised (figure 12h). Images used with copyright permission, courtesy of Arthrex, Inc.
Figure 13:
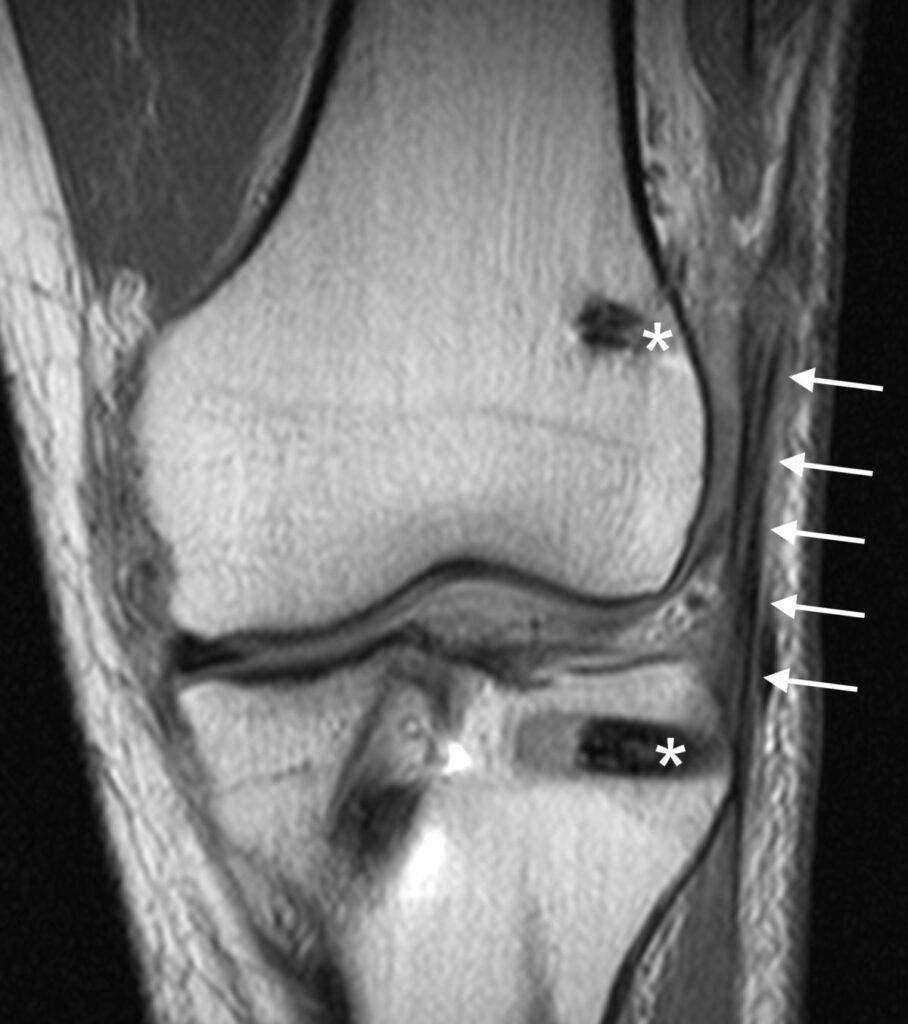
MR appearance of ALL reconstruction
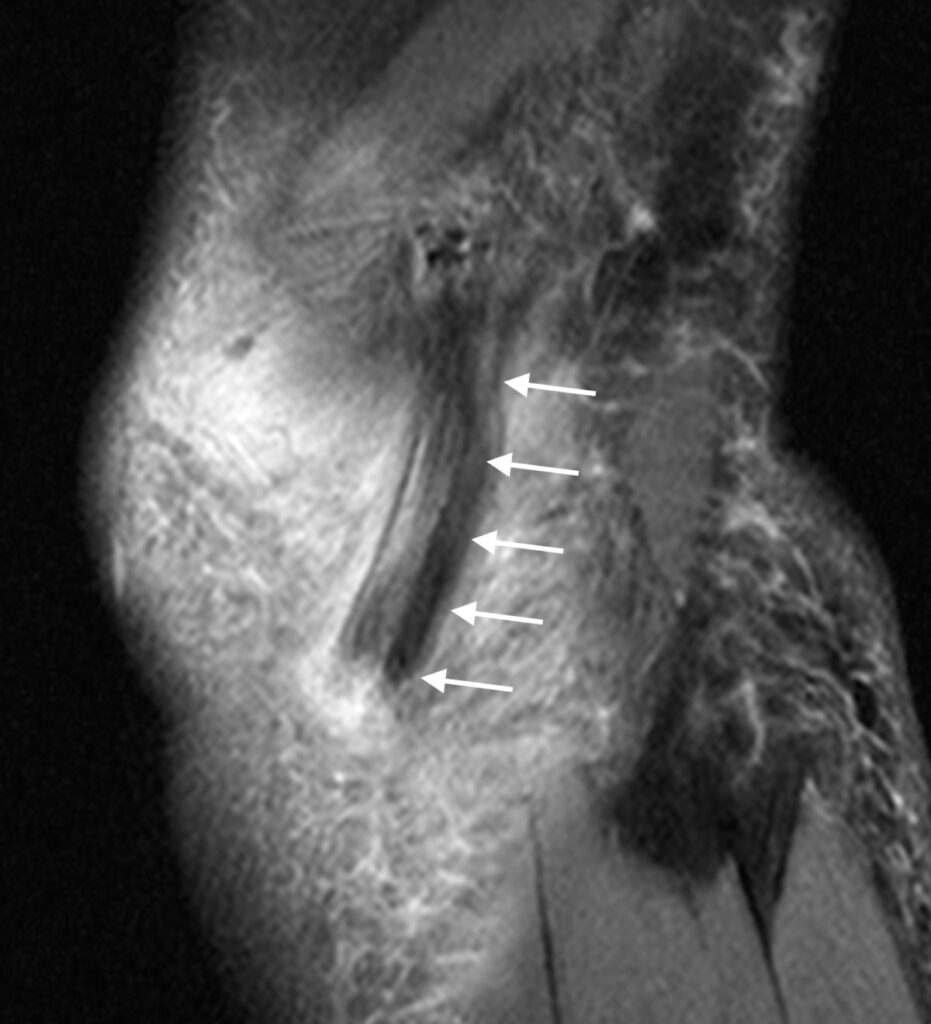
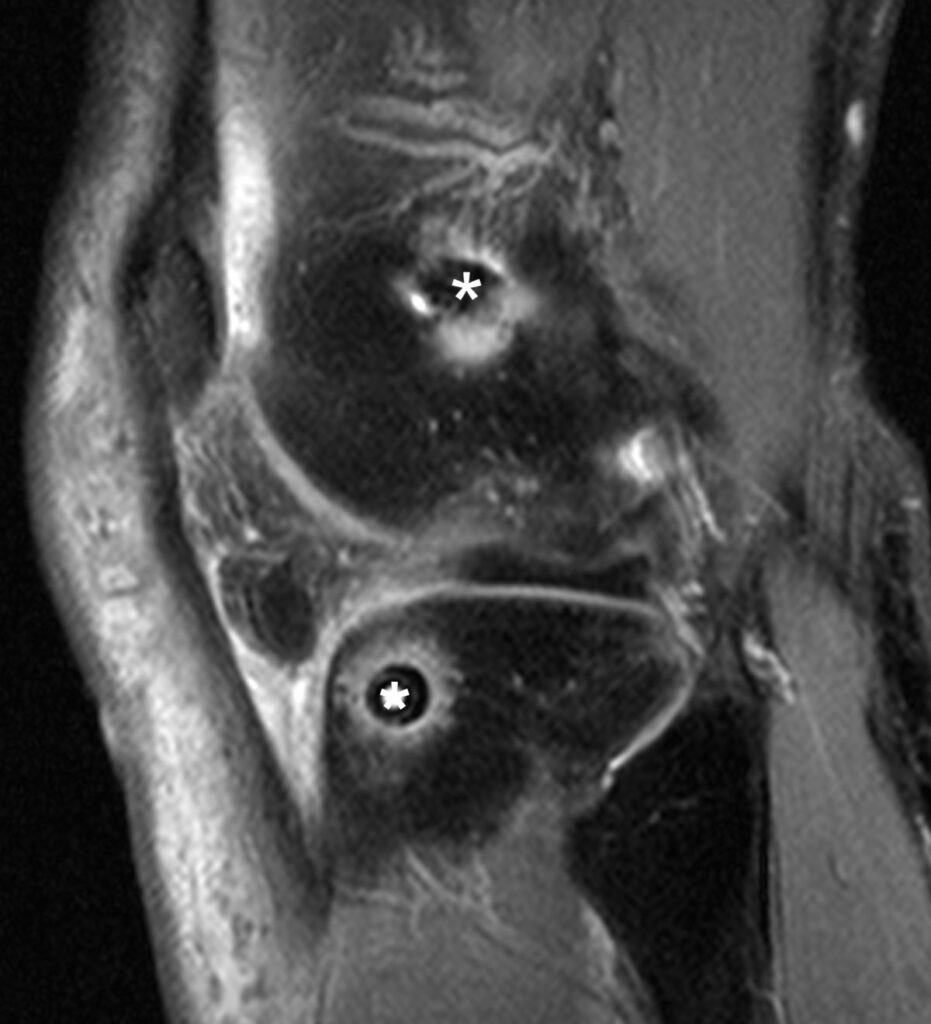
13a: Coronal proton density-weighted image demonstrates an ALL graft (arrows) with the femoral and tibial anchor sites (*).
13b: Sagittal fat-suppressed proton density-weighted image shows the extra-articularly located ALL graft (arrows).
13c: A more medially located sagittal image shows the femoral and tibial anchors (*) of the graft.
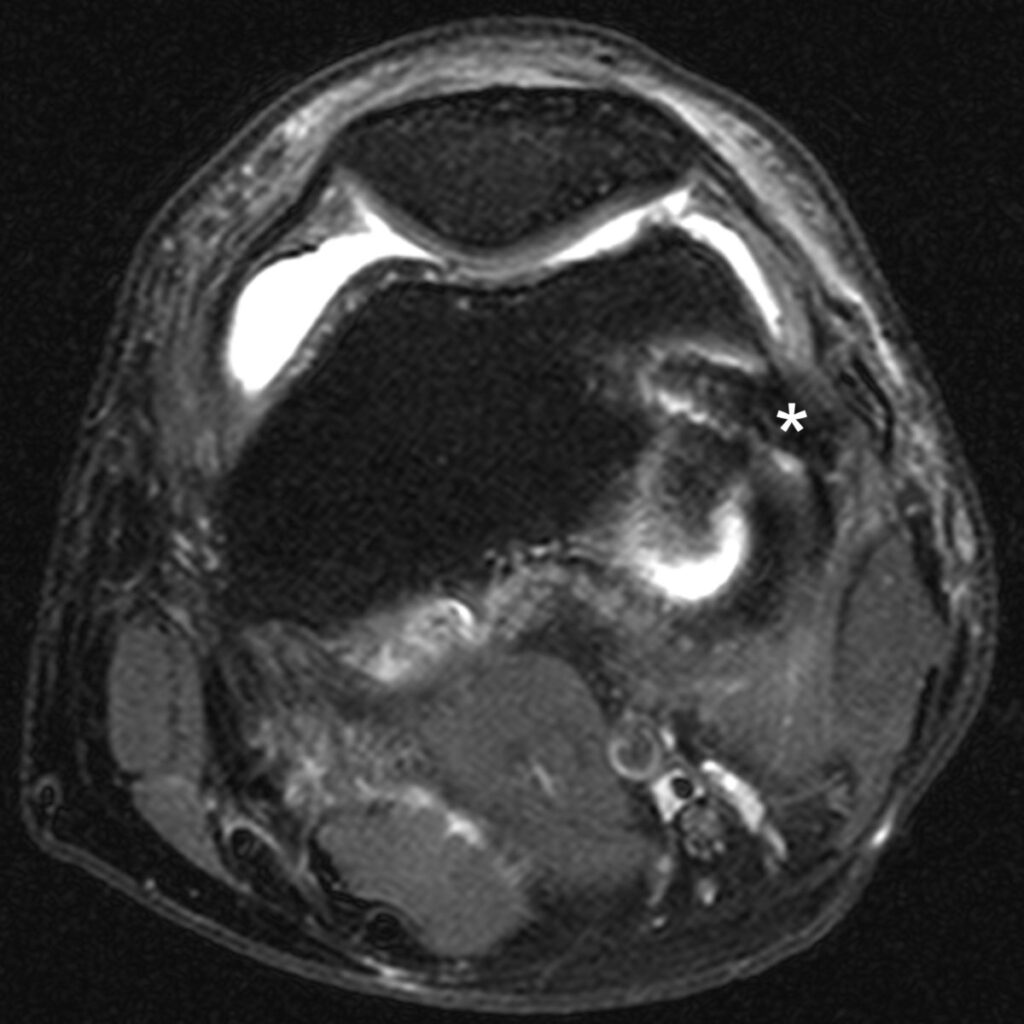
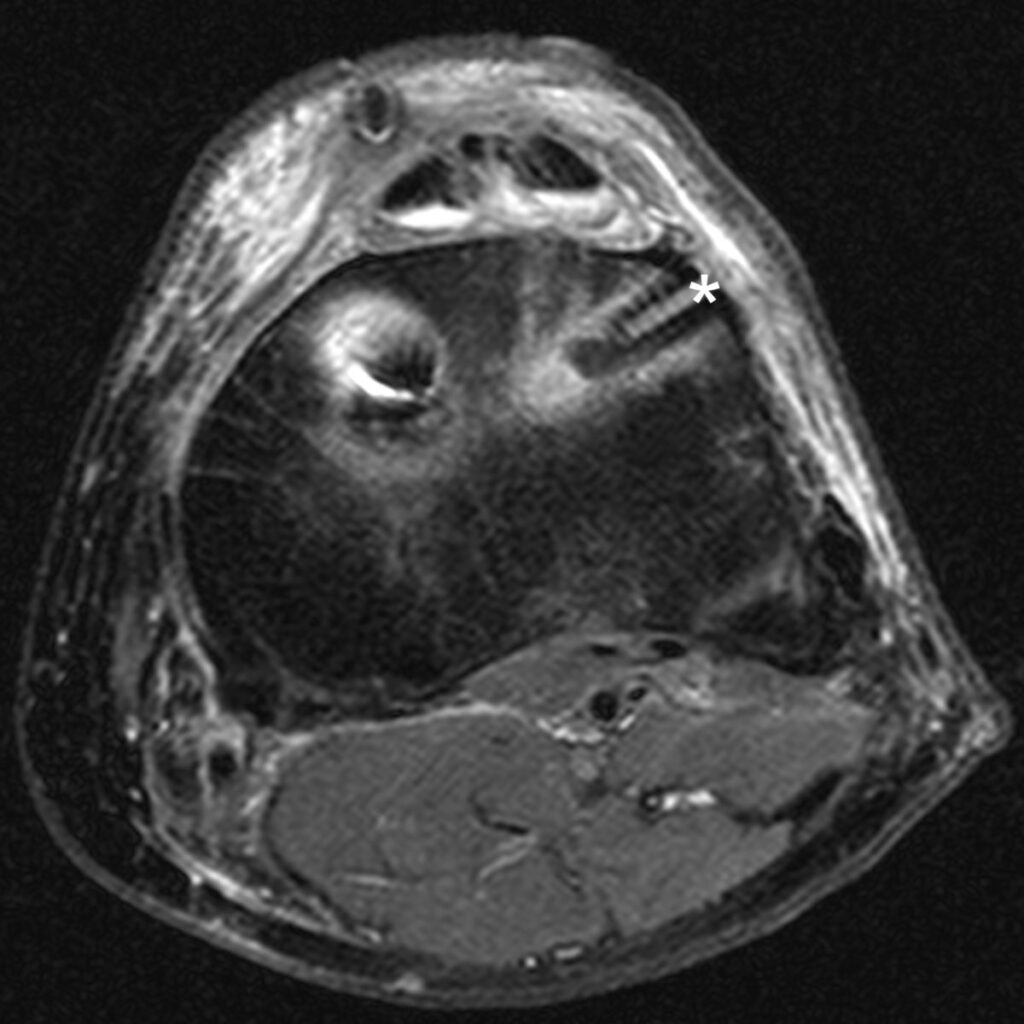
13d, e: Axial fat-suppressed proton density-weighted images showing the femoral and tibial anchors sites. In this case, the tibial anchor was placed anterior to the native anatomic attachment, closer to Gerdy’s tubercle.
Summary
The ALL is a distinct ligamentous structure of the knee, connecting the lateral femur with the lateral tibia. Tears of the ALL can be diagnosed with MRI and are best appreciated on fat-suppressed proton density-weighted axial and coronal images. ALL tears typically occur in conjunction with tears of the ACL. Once an ACL tear is diagnosed (particularly with a Segond fracture) it is helpful to maintain a high index of suspicion for a concomitant ALL tear, scrutinizing the anterolateral anatomy. In select situations, some surgeons may opt to extra-articularly repair the ALL during an ACL reconstruction.
References
- Segond P. Recherches Cliniques et Expérimentales Sur Les Épanchements Sanguins Du Genou Par Entorse. Aux Bureaux Du Progrès Médical. Paris; 1879. ↩
- Claes S, Vereecke E, Maes M, Victor J, Verdonk P, Bellemans J. Anatomy of the anterolateral ligament of the knee. 2013:321-328. doi:10.1111/joa.12087 ↩
- Karan A. Patel, M.D., Anikar Chhabra, M.D., Jill A. Goodwin, M.D. and D. Identification of the Anterolateral Ligament on Magnetic Resonance Imaging. Arthrosc Tech. 2017;6(1):e137-e141. doi:10.1016/j.eats.2016.09.015 ↩
- Appearance KMRI, Porrino J, Chew FS. The Anterolateral Ligament of the Knee: MRI Appearance, Association With the Segond Fracture, and Historical Perspective. 2015;(February):367-373. doi:10.2214/AJR.14.12693 ↩
- Anatomic A, Analysis B, Kennedy MI, et al. The Anterolateral Ligament. 2015:1606-1615. doi:10.1177/0363546515578253 ↩
- Lima LL De, Silva DDC, Luzete M, et al. Anatomy of the Anterolateral Ligament of the Knee : A Systematic Review. Arthrosc J Arthrosc Relat Surg. 2018:1-12. doi:10.1016/j.arthro.2018.09.006 ↩
- Anderson AF, Irrgang JJ, Dunn W, et al. Interobserver reliability of the International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine (ISAKOS) classification of meniscal tears. Am J Sports Med. 2011;39(5):926-932. doi:10.1177/0363546511400533 ↩
- Sonnery-Cottet B, Vieira TD, Ouanezar H. Anterolateral Ligament of the Knee: Diagnosis, Indications, Technique, Outcomes. Arthrosc J Arthrosc Relat Surg. 2019;35(2):302-303. doi:10.1016/j.arthro.2018.08.019 ↩
- Musahl V, Getgood A, Neyret P, et al. Contributions of the anterolateral complex and the anterolateral ligament to rotatory knee stability in the setting of ACL Injury: a roundtable discussion. Knee Surgery, Sport Traumatol Arthrosc. 2017;25(4):997-1008. doi:10.1007/s00167-017-4436-7 ↩
- Kawanishi Y, Kobayashi M, Yasuma S, Fukushima H, Kato J, Murase A. Anterolateral ligament reconstruction in addition to primary double ‑ bundle anterior cruciate ligament reconstruction for grade 3 pivot shift improves residual knee instability during surgery. 2021. doi:10.1186/s40634-021-00369-4 ↩
- Arthrex Anterolateral Ligament Reconstruction Surgical Technique. https://cdn.arthrex.io/image/upload/23f5b11c-9b0c-4eb7-97b1-cfa2fdbd536e.pdf. ↩