Clinical History:
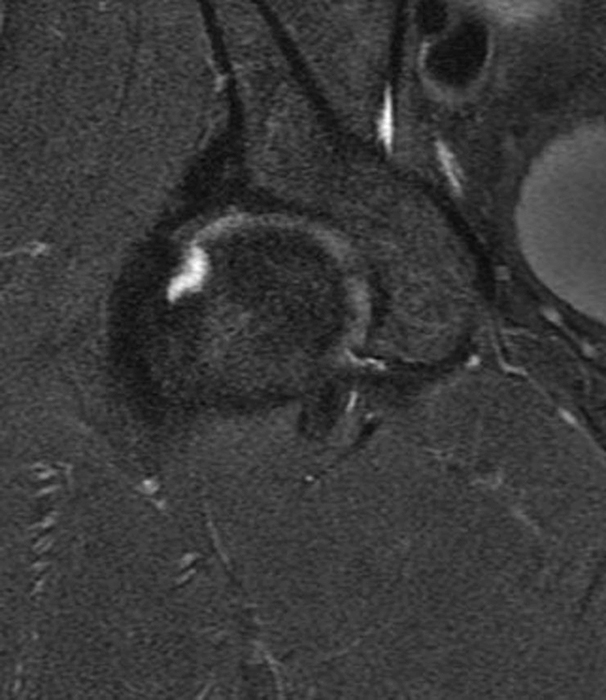
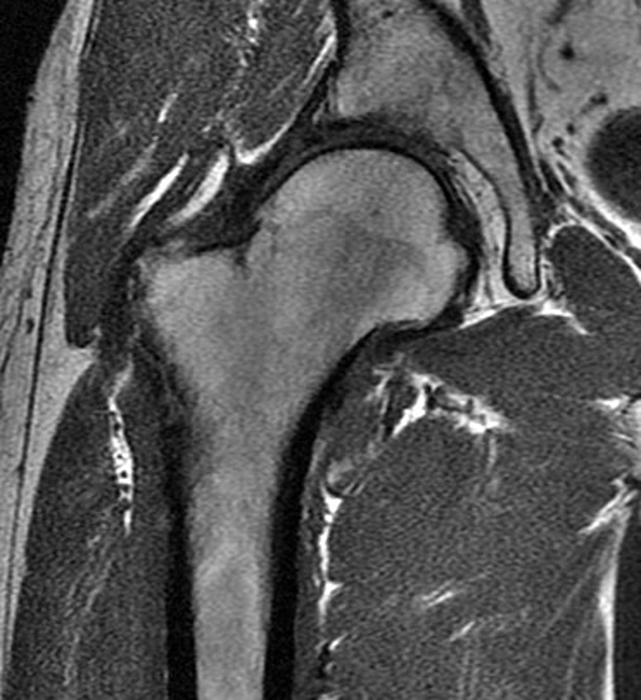
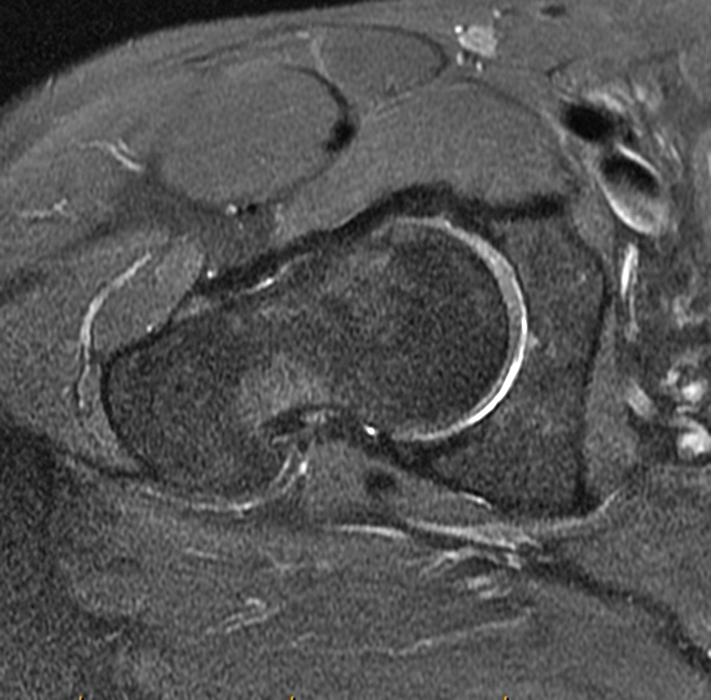
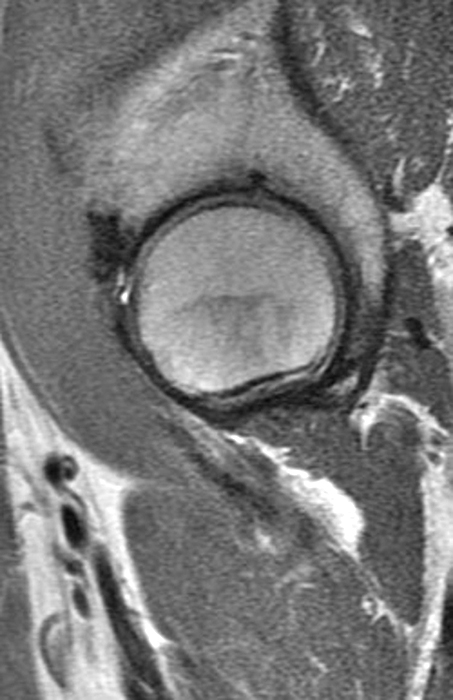
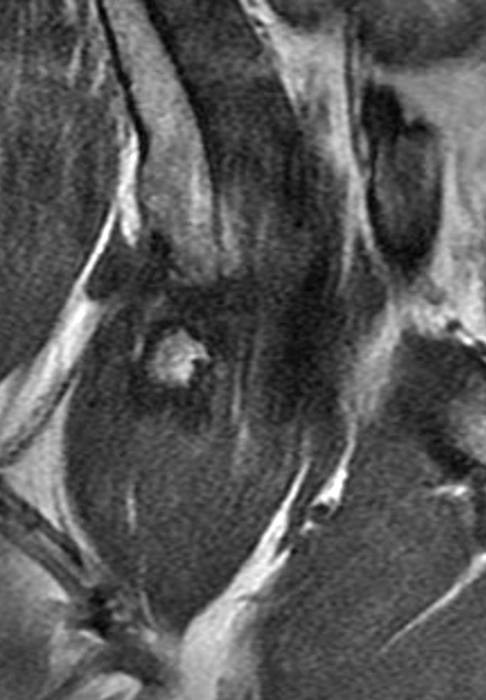
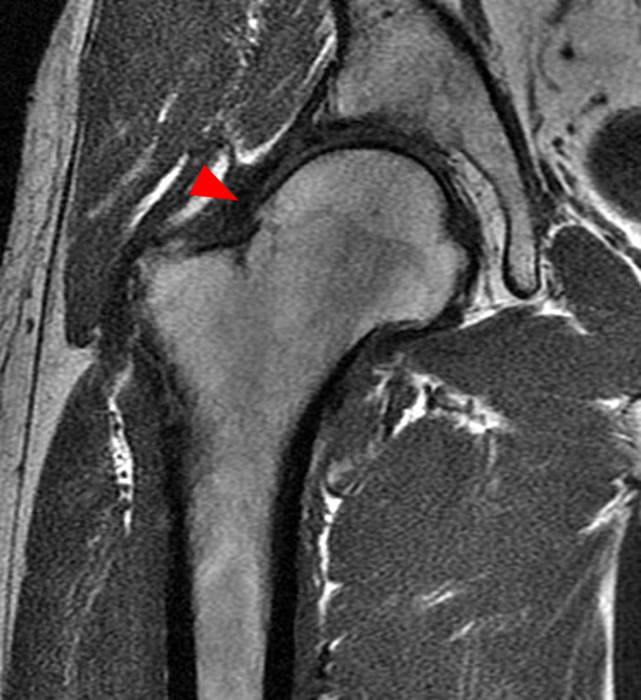
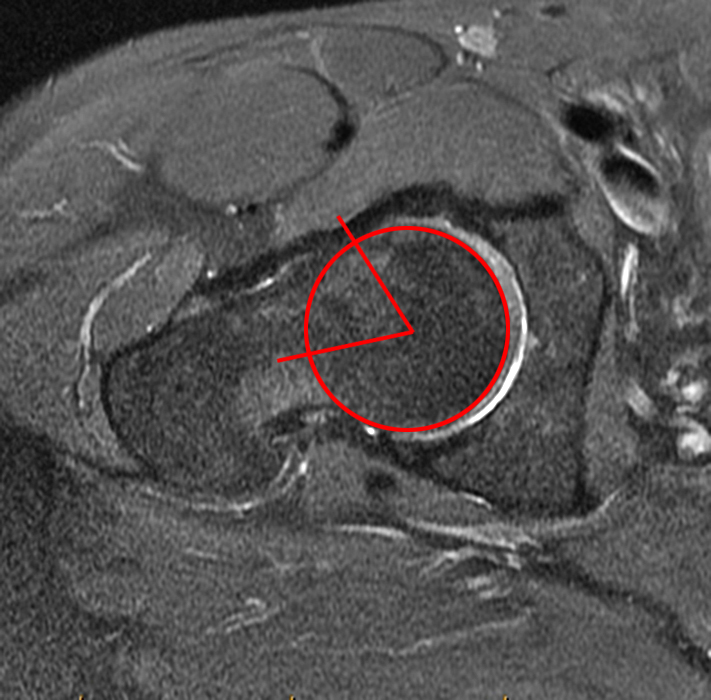
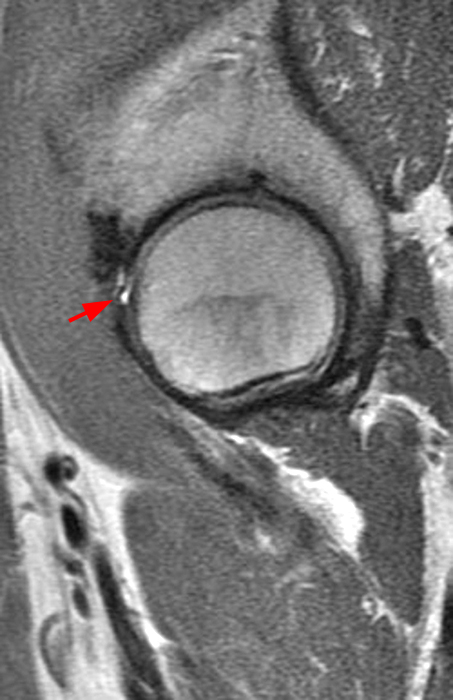
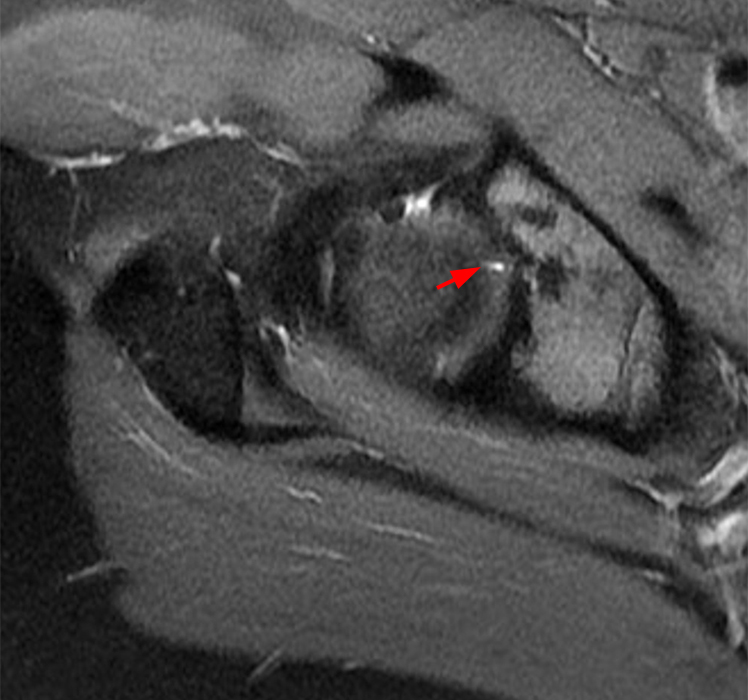
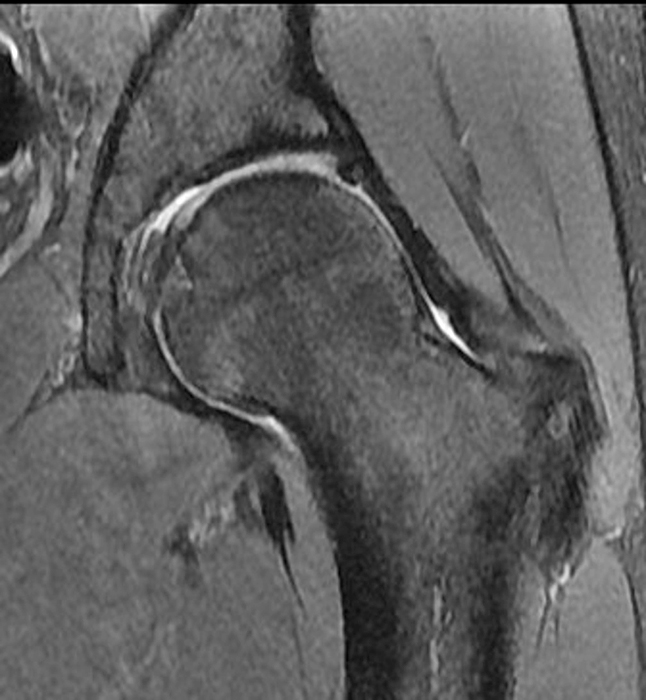
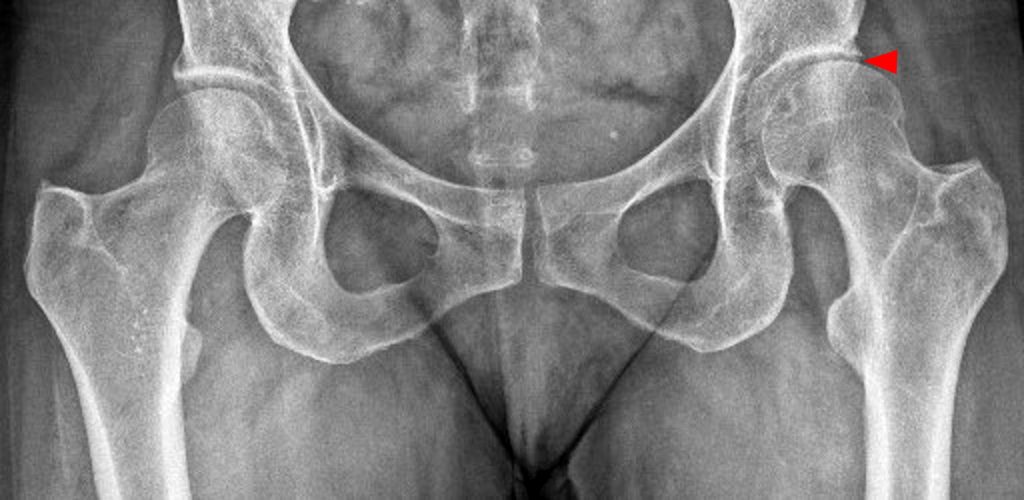
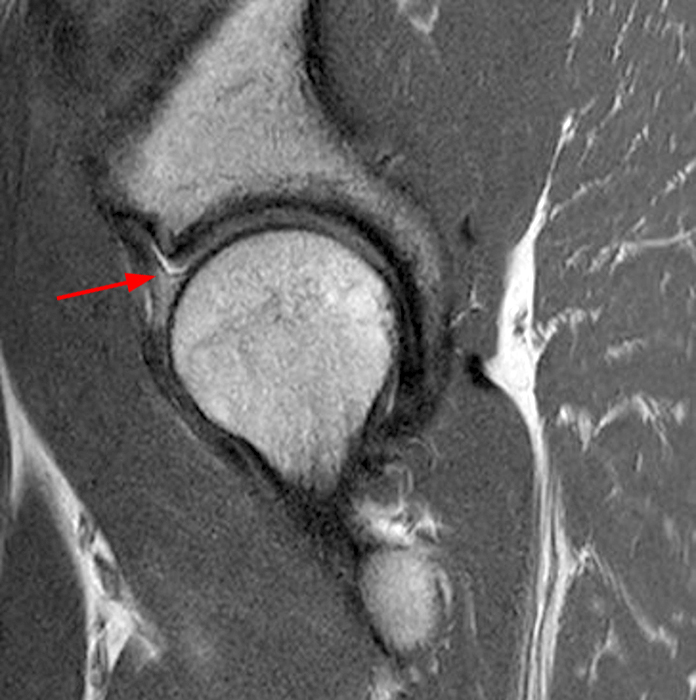
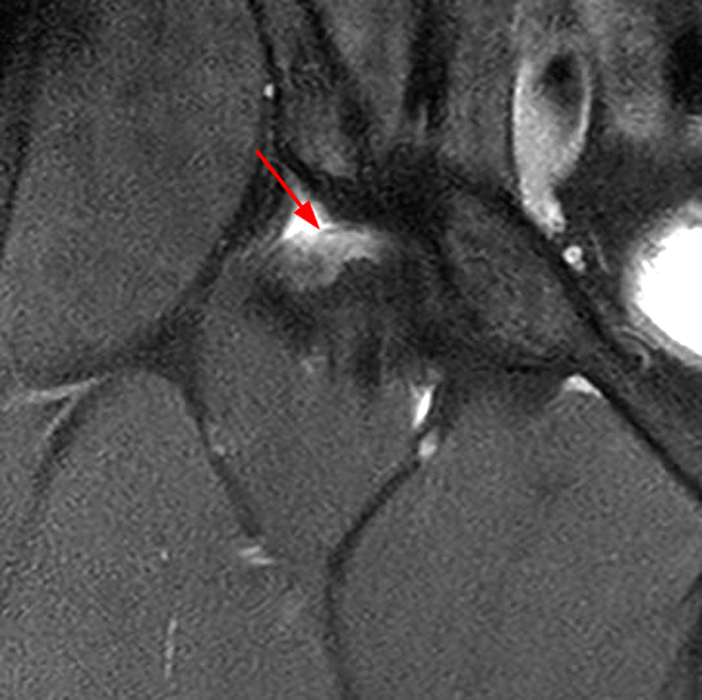
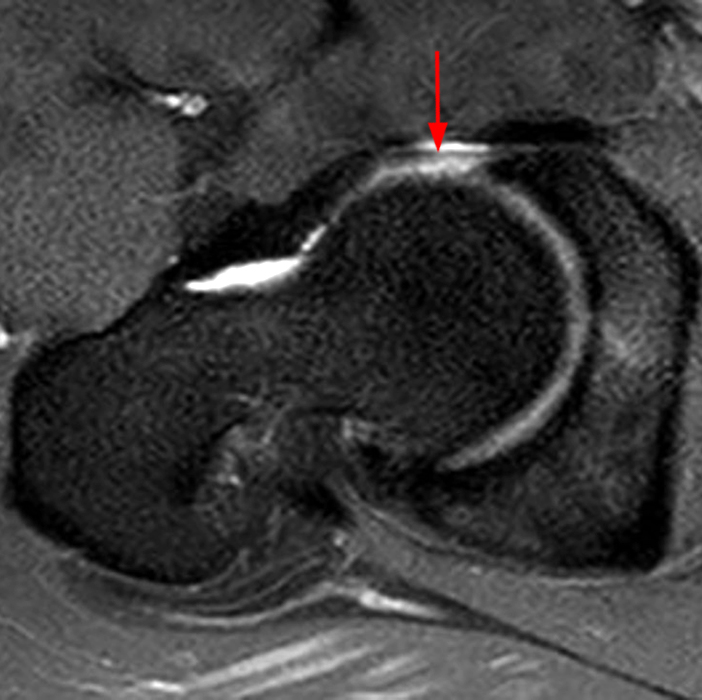
A 40-year-old male presents with progressive right hip pain status-post labral repair and femoroplasty 18 months prior. Pre-operative images are not available for review. Coronal fat-suppressed T2-weighted (1A), coronal T1-weighted (1B), axial oblique fat-suppressed proton density-weighted (1C), sagittal proton density-weighted (1D), coronal fat-suppressed proton density-weighted (1E), and a coronal T1-weighted image anterior to the joint (1F) are provided. What are the findings? What is your diagnosis?
Findings
Figure 2:
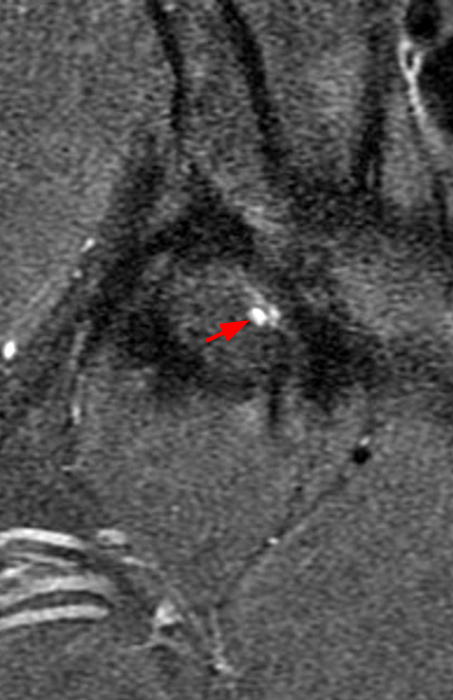
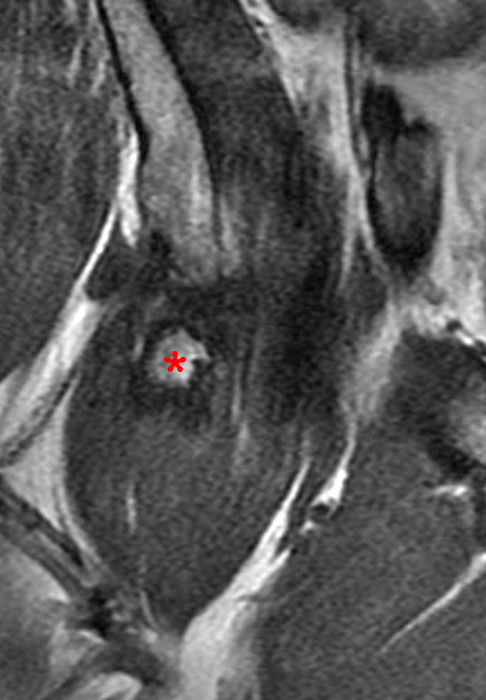
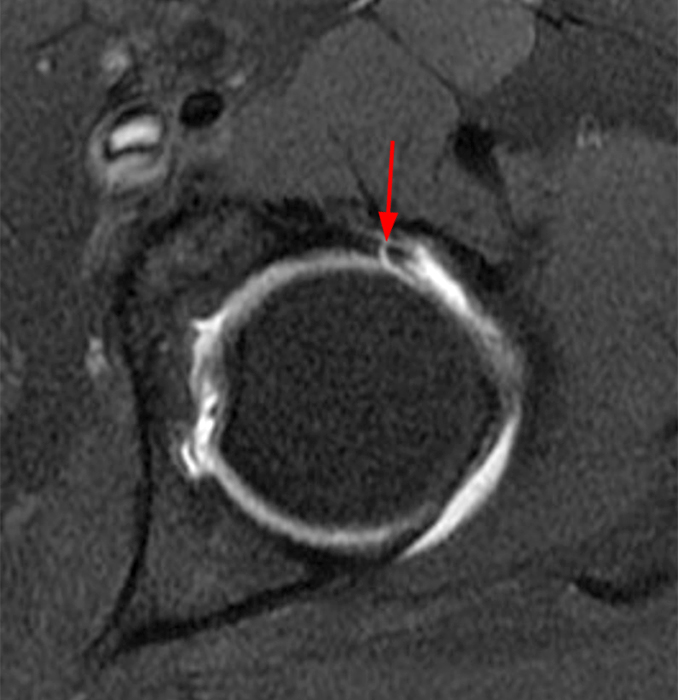
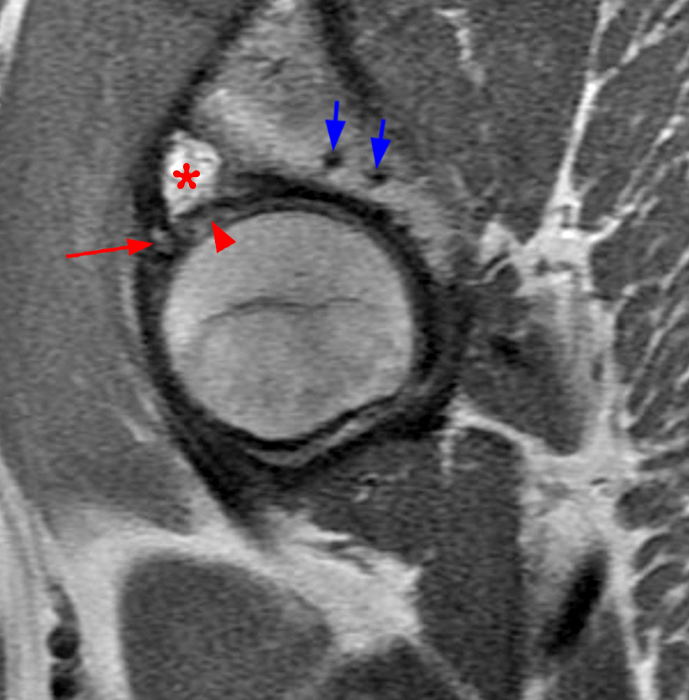
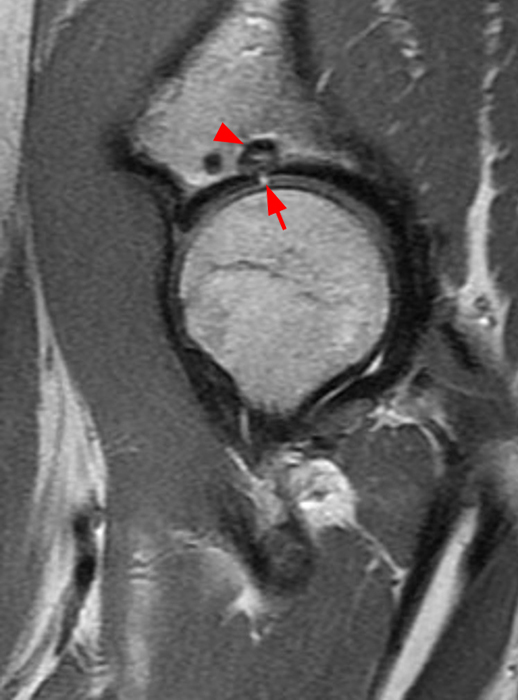
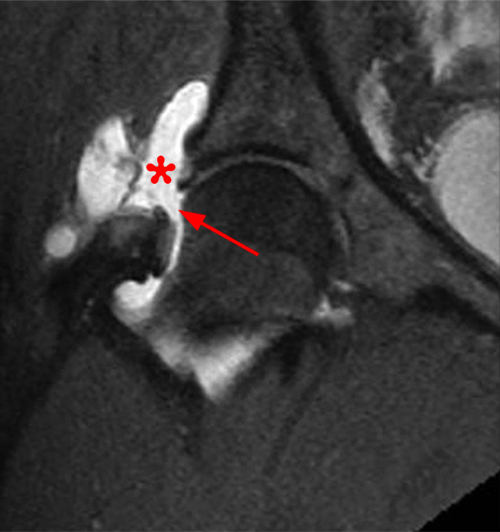
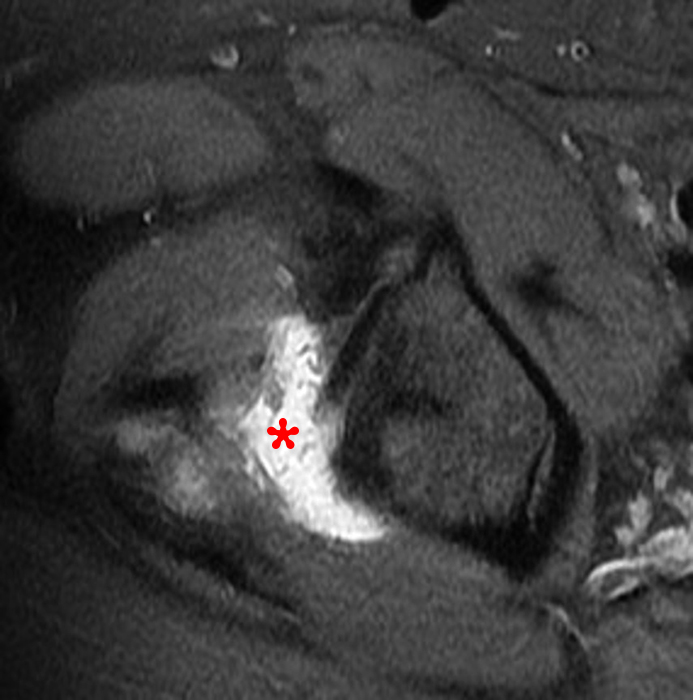
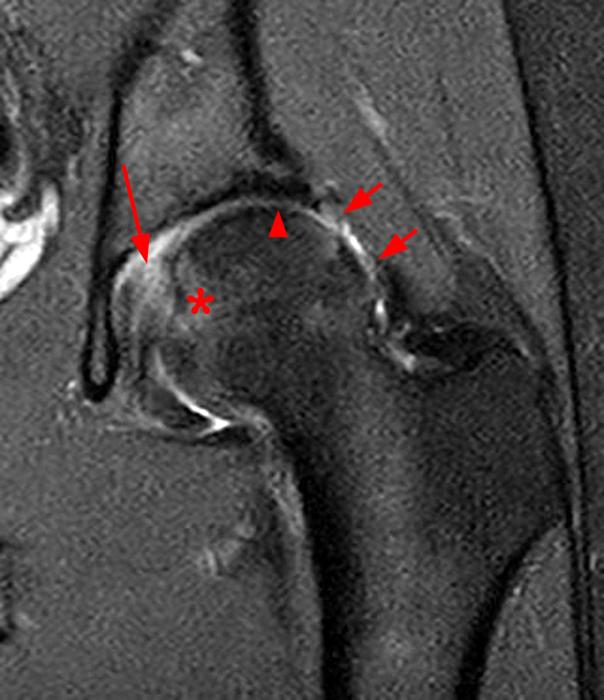
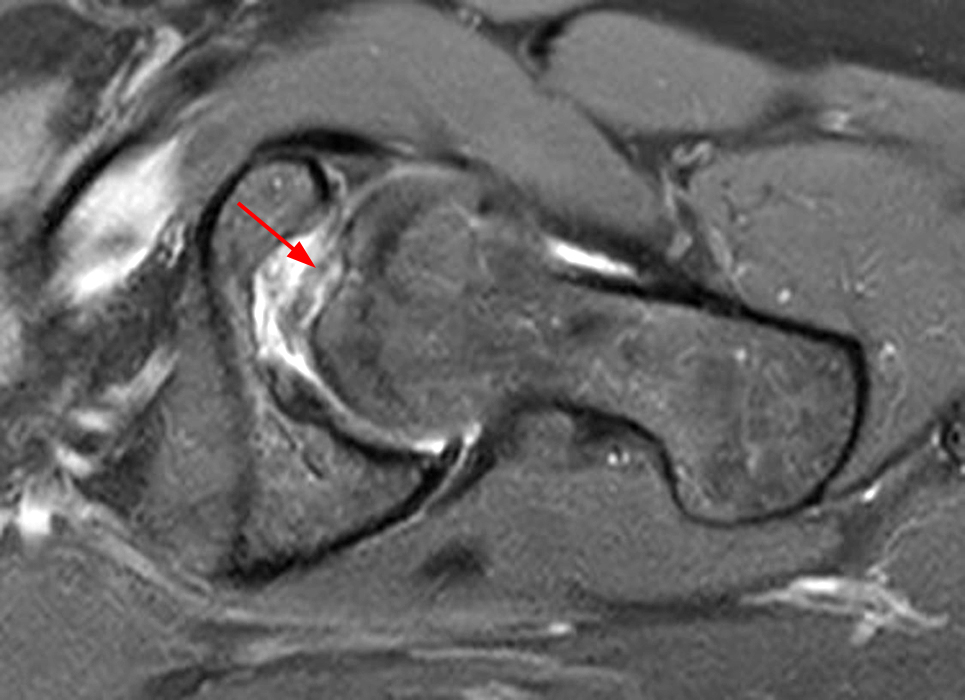
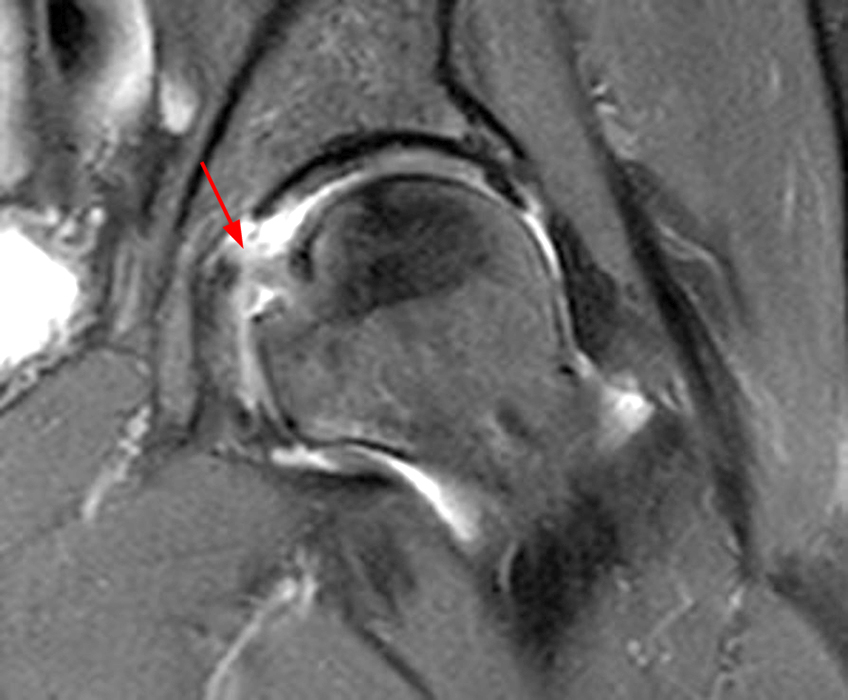
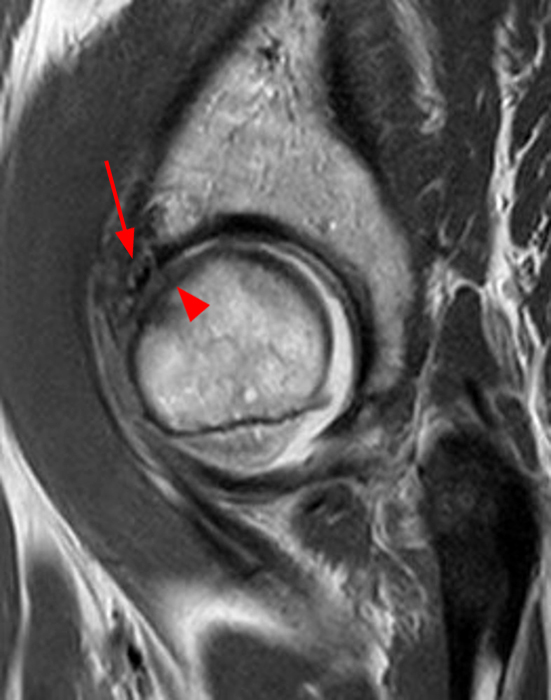
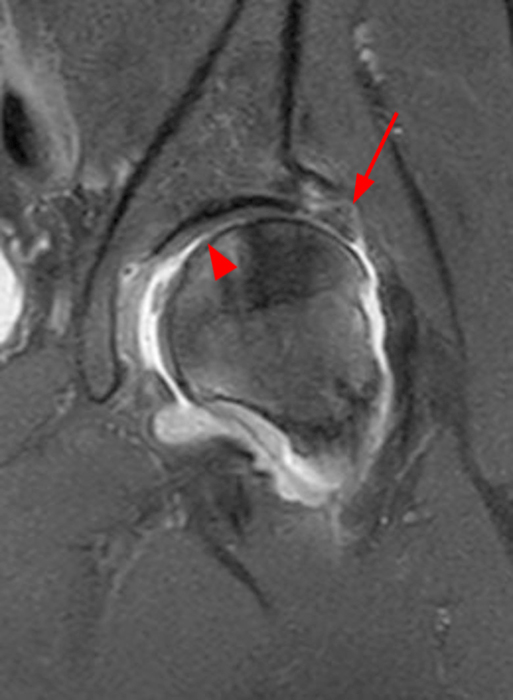
The coronal T2-weighted fat-suppressed image (2a) demonstrates a femoroplasty defect (arrow) along the anterior aspect of the femoral head/neck junction. Incomplete resolution of a cam deformity (arrowhead) is seen on the coronal T1-weighted image (2b). The alpha angle measures 68 degrees on the axial oblique fat-suppressed proton density-weighted image (2c). The sagittal proton density-weighted (2d) and coronal fat-suppressed proton density-weighted (2e) images demonstrate irregular attenuation and increased signal along the anterior labrum with a small paralabral cyst (short arrows). These findings are compatible with a recurrent tear. Anterior to the joint on the coronal T1-weighted image (2f), a large focus of heterotopic ossification (asterisk) is embedded within the iliofemoral ligament.
Diagnosis
Prior femoroplasty with incomplete resolution of a cam deformity, new anterior labral tear, and heterotopic ossification within the iliofemoral ligament.
Discussion
Evolution in the treatment of femoroacetabular impingement (FAI) through hip preservation surgery to delay the advancement of osteoarthritis has led to an increase in primary and revision hip arthroscopy. The goal of hip preservation surgery is to restore the anatomy and function of the labrum to maintain joint stability and intra-articular pressure.1,2 For this reason, primary labral repair is preferred to labral excision or debridement, and patients who undergo primary labral repair report better outcomes.3,4
While many patients experience symptom resolution or improvement following hip preservation surgery, a subset of patients do report persistent or recurrent pain. In patients with postoperative pain, a recent national consensus-based guideline recommends MRI as part of the initial work-up.5 The purpose of this Web Clinic is to highlight several important postoperative findings which may contribute to recalcitrant pain.
Recurrent femoroacetabular impingement
While FAI is most accurately assessed through dynamic maneuvers on physical examination, one way in which radiologists can communicate risk factors for recurrent intra-articular impingement is evaluation of femoral and acetabular morphology. This is especially important given that one of the leading indications for revision hip arthroscopy is recurrent impingement.
In general, the hip arthroscopist determines the depth of femoral and acetabular resection utilizing preoperative radiographs, intraoperative dynamic examination, and fluoroscopy. The femoroplasty should restore the femoral head-neck offset, appear as a smooth concavity on postoperative imaging, and bone marrow edema should resolve three months after surgery.6 When there is decreased femoral head/neck offset on postoperative imaging (Figures 2b and 2c, Figure 3a), it is helpful to describe the location of the deformity, especially in reference to the femoroplasty.
The acetabulum should be evaluated for persistent over-coverage of the femoral head, evidence of dysplasia (congenital or iatrogenic), or ossification along the acetabular rim and within the base of the labrum (Figure 3b). Postsurgical change related to acetabuloplasty is subtler but can be identified as truncation of the acetabular rim.
Although there is no threshold value which can differentiate between symptomatic and asymptomatic patients, measurement of the alpha angle and the lateral center edge angle may aid in the identification of recurrent impingement. A review of MRI measurements in the evaluation of FAI can be found here: https://radsource.us/femoroacetabular-impingement/
Figure 3:
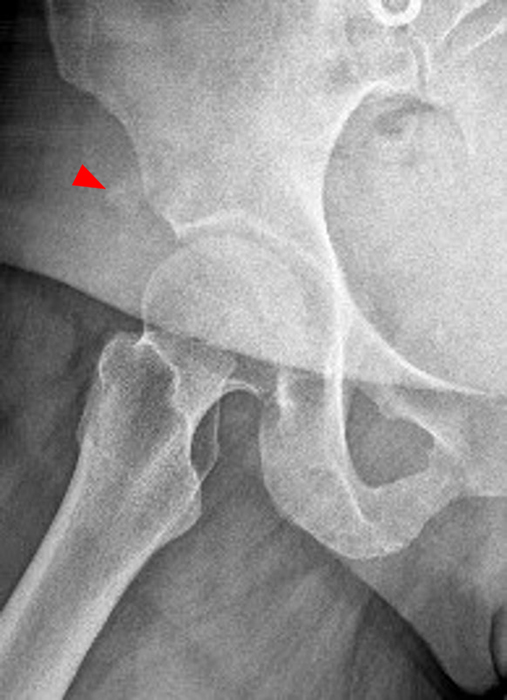
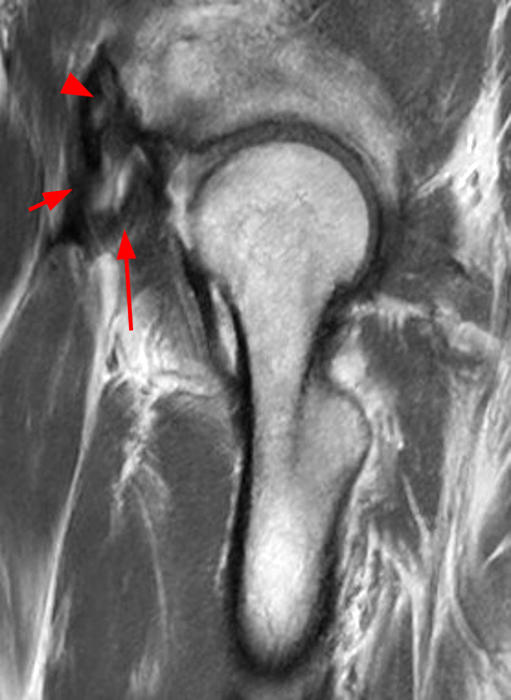
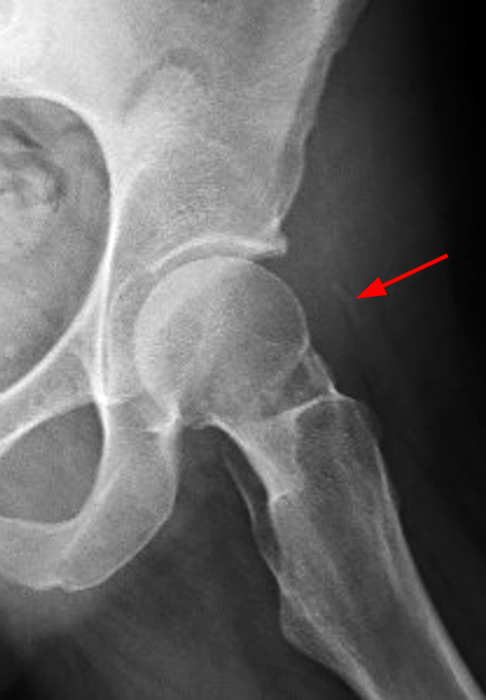
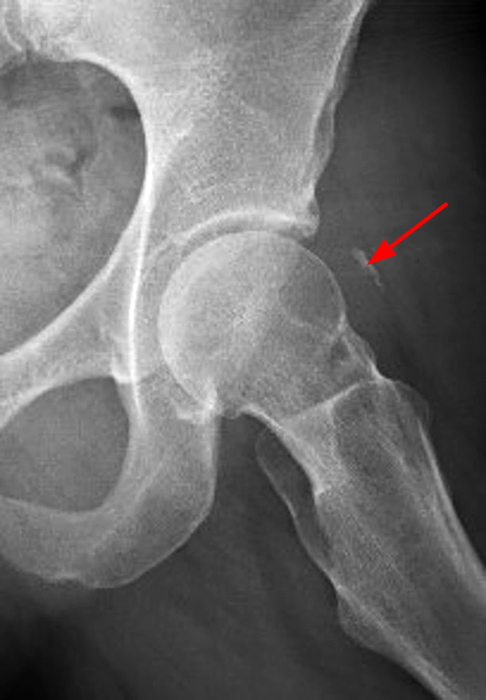
A 32 year-old female with a history of labral repair two years prior presents with left hip pain.
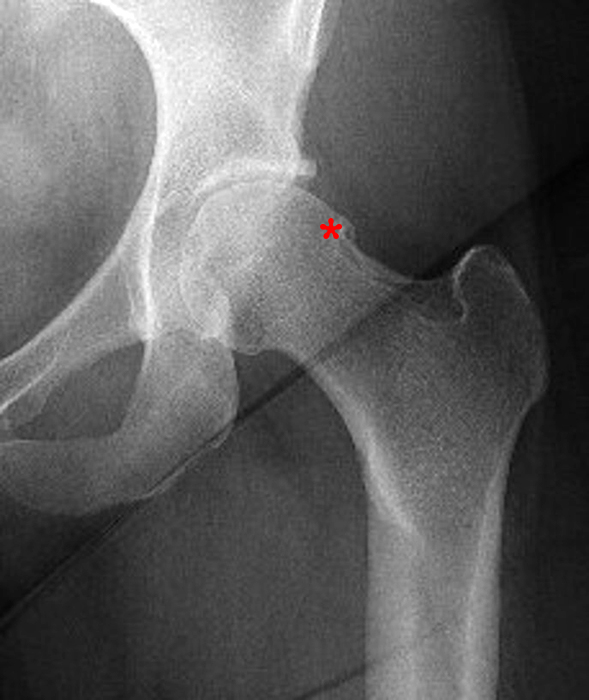
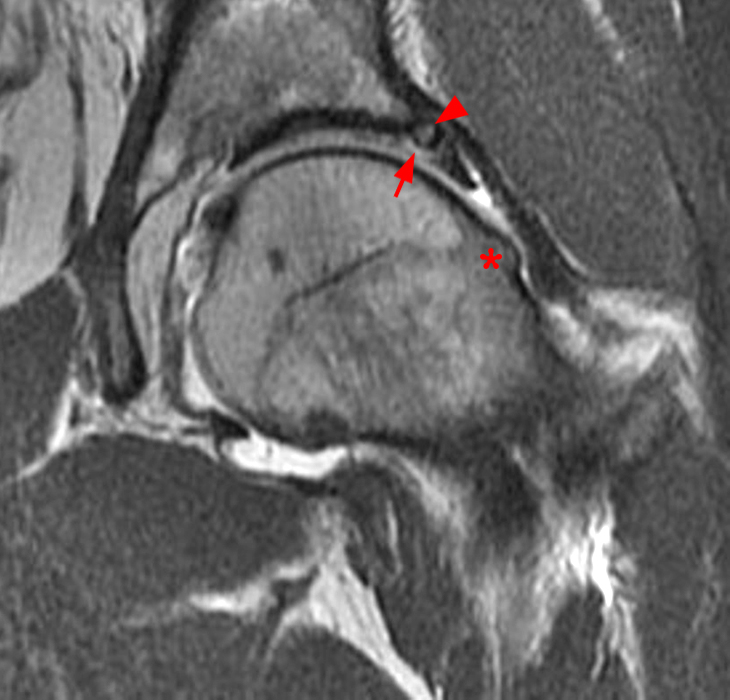
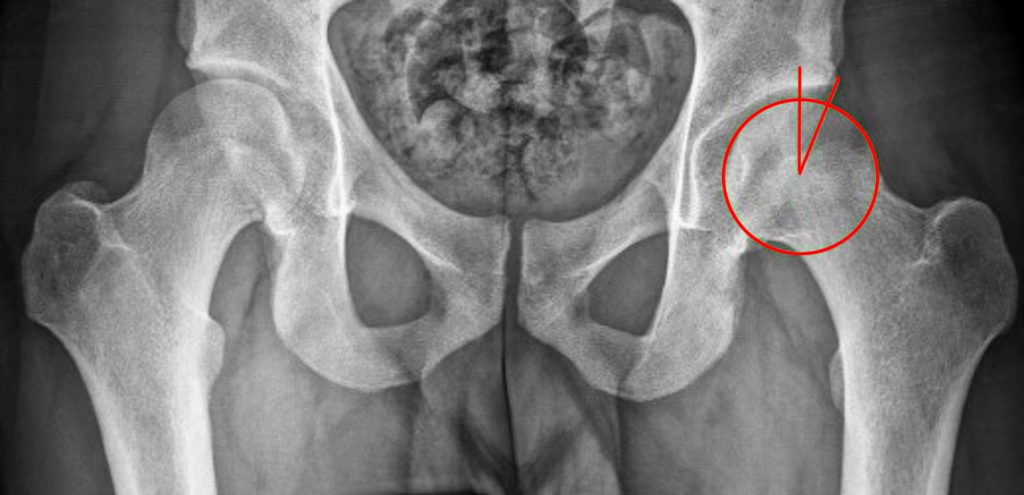
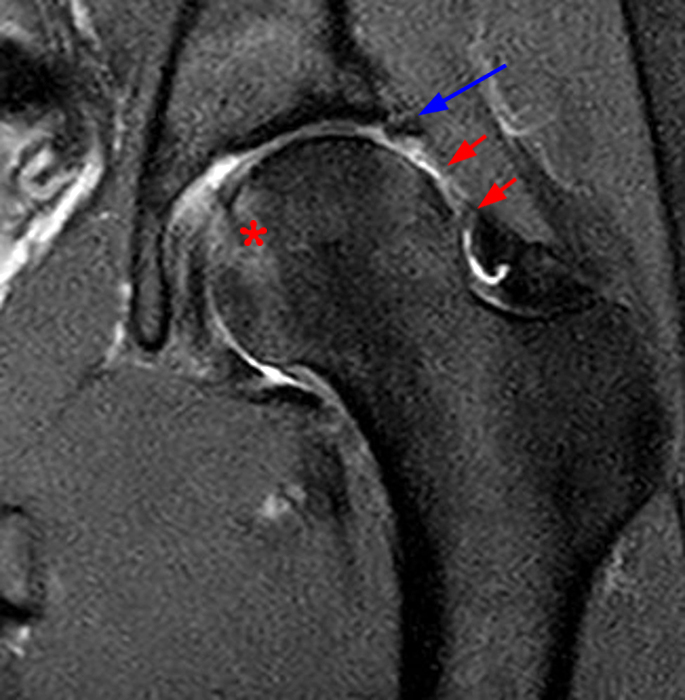
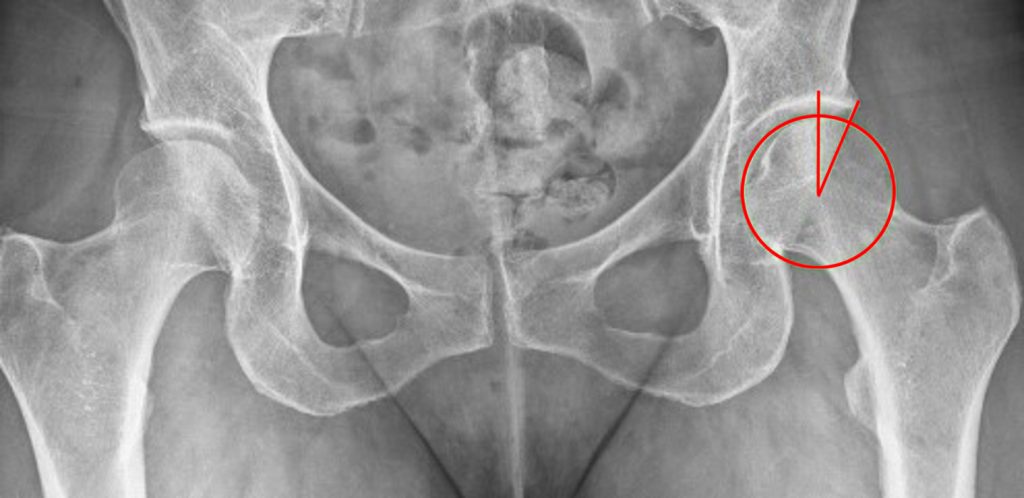
The AP radiograph of the left hip (3A) demonstrates an aspherical femoral head with a small osseous protuberance (asterisk) consistent with a cam deformity. Coronal T1-weighted (3B) and fat-suppressed T1-weighted MR arthrogram (3C) images demonstrate a cam deformity (asterisk) with a small ossicle (arrowhead) along the lateral acetabular rim, which may contribute to pincer impingement. Acetabular chondral thinning, fissuring, and delamination is present along the chondrolabral junction (short arrows). Abnormal morphology of the anterosuperior labrum on the fat-suppressed T1-weighted sagittal image (3D) (red arrow) and cross referencing with the coronal fat-suppressed T1-weighted Image (3E) demonstrates the presence of a suture (blue arrow). An adjacent labral defect is present on the axial fat-suppressed T1-weighted image (3F), and these findings suggest that the suture may be cutting through the labral tissue.
Labral healing and Recurrent Labral Tear
In general, labral tears are classified as a detachment of the labrum along the chondrolabral transition zone (type 1), or as a cleavage plane of variable depth extending through the substance of the labrum (type 2).7 While type 1 tears are thought to be repairable due to the presence of a blood supply along the capsule, type 2 tears are thought to be less amenable to healing but may be debrided to a stable outer rim and reattached to the acetabulum.8,9 The depth of the tear and the overall quality of the labral tissue is also important and should be described in the MRI report.
During arthroscopy, if enough healthy labral tissue is present to perform a repair, the most widely used technique consists of debriding the unstable tissue, detaching the labrum from the acetabulum, suturing the labral tear, and then re-implanting the labrum onto the acetabulum using suture anchors. When suturing the labral tear, the surgeon may either pass the sutures through the substance of the labrum or loop the sutures around the labrum.10
In the native hip and the post-arthroscopic hip, labral tears often do not demonstrate signal intensity equivalent to fluid or gadolinium.11 Therefore, it is important to compare the morphology of the labrum on postoperative imaging with preoperative imaging (when available). Similarly, the location, signal intensity, and thickness of the labral tear, the presence of a new tear in a different location, and the resolution or development of paralabral cysts are additional findings which are important to describe in the MRI report.12,13
On post-operative MRI, the suture anchors should span the entire length of the tear. They should be positioned close to the acetabular rim and angled away from the joint surface, but they should not penetrate the subchondral bone or the articular cartilage (Figure 4).14 In cases where the suture anchor appears to extend through the subchondral bone, the overlying cartilage should be scrutinized for a focal defect, adjoining delamination, or signal alteration without a discernible defect (Figures 5 and 6).
Although the sutures themselves are often beyond the resolution of MRI, interval development of a segmental labral defect may represent a suture cutting through the substance of the labrum (Figure 3).15
Figure 4:
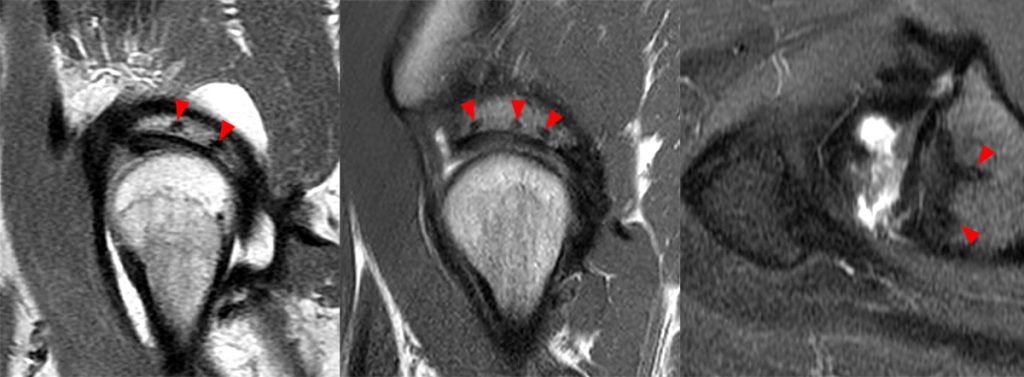
Sagittal proton density-weighted (left and middle) and axial fat-suppressed proton density-weighted (right) images in three different patients who underwent labral repair with acetabular suture anchors. The suture anchors (arrowheads) are most conspicuous on sagittal images. The anchors are positioned close to the acetabular rim, angled away from the joint surface, do not penetrate the subchondral bone plate, and no overlying chondral abnormality is identified. On axial imaging, the suture anchors are generally less conspicuous.
Figure 5:
29 year-old male with recurrent right hip pain status-post labral repair three months ago. Pre-operative imaging is not available. Sagittal proton density-weighted (5A,C) and axial fat-suppressed proton density-weighted (5B) images demonstrate full-thickness chondral delamination along the anterosuperior acetabulum (arrowhead) with prominent subchondral cystic change and marrow edema (asterisks). Linear increased signal extending through the anterosuperior labrum is associated with a small paralabral cyst (arrows), and these findings are indicative of a tear. Given the severity of these findings in a patient who underwent surgery only three months prior, comparison with pre-operative imaging or the operative report would be helpful, but when these are unavailable, it is important to objectively describe the findings and note that the suture anchors do not span the entire length of the tear. Normally positioned suture anchors (blue short arrows) are demonstrated. The posterior-most acetabular suture anchor extends through the subchondral bone and protrudes into the articular cartilage (short red arrows).
Figure 6:
18 year-old female with worsening right hip pain and a history of labral repair two years prior. Sagittal proton density-weighted (6A), coronal fat-suppressed T2-weighted (6B), and contiguous axial fat-suppressed proton density-weighted (6C,D) images demonstrate intra-articular extension of two acetabular suture anchors (short arrows). One of the suture anchor tracts also appears abnormally wide (arrowheads).
Capsular Healing and Post-arthroscopic Instability
In addition to the labrum, the capsule confers stability to the hip joint, and is composed of three main ligaments: the iliofemoral ligament (also known as the Y ligament or the ligament of Bigelow), the ischiofemoral ligament, and the pubofemoral ligament. The iliofemoral ligament is the strongest ligament in the human body, it is the largest of the capsular ligaments, and it reinforces the anterior aspect of the capsule.16 The ischiofemoral ligament reinforces the posterior aspect of the capsule.
While there are several capsular approaches the hip arthroscopist may choose, the standard anterior and anterolateral portals broach the medial and lateral borders of the iliofemoral ligament. The anterolateral portal is established first and is located approximately 2 cm anterior and 2 cm superior to the anterosuperior border of the greater trochanter. The anterior portal is then created utilizing arthroscopic visualization.
Iatrogenic instability is increasingly recognized as a potential complication of hip arthroscopy, and clinical symptoms are usually non-specific.17 Macroinstability includes a subluxation or dislocation event which may occur in the setting of minor trauma, especially with external rotation, extension, and abduction. Microinstability is a relatively recent concept which applies to patients with borderline acetabular dysplasia or ligamentous laxity prior to the index surgery.
In contradistinction to hip dislocations in the setting of a sports-related injury or a motor vehicle accident, post-arthroscopic dislocations are most often anterior, and iatrogenic risk factors include excessive cam osteoplasty or acetabular rim resection, labral debridement, iliopsoas tenotomy, unrepaired capsulotomy, and ligamentum teres debridement.18,19 As a result, many hip arthroscopists routinely close the capsule, and capsular plication is recommended in patients with borderline acetabular dysplasia or ligamentous laxity. On MRI, the plicated capsule is usually significantly thicker than the contralateral hip. In cases where the capsulotomy is not repaired, the defect has been found to “heal” on MRI six months postoperatively, however Figure 7 demonstrates that we should always evaluate the integrity of the capsule.20,21
While the role of the ligamentum teres in hip pain and stability is still being elucidated, it is believed to be an important secondary stabilizer of the hip joint, and partial or complete tears have been documented with varying degrees of trauma.22,23 Pre-operative and post-operative imaging should be evaluated for ligamentum teres pathology, and partial or complete tears may be identified through focal fiber discontinuity, abnormal attenuation with a distorted contour, and abnormal ligamentous edema (Figures 8 and 9).
Figure 7:
Fat-suppressed coronal T2-weighted (7A) and axial proton density-weighted (7B) images from a 24 year-old female with recurrent right hip pain six months status-post arthroscopic labral repair and femoroplasty. A large capsular defect (arrow) is associated with joint fluid decompressing into the soft tissues (asterisks) along the abductor tendons.
Figure 8:
24 year-old male with left anterior hip pain for 10 days. History of labral repair and subspine decompression 8 months prior. Preoperative AP radiograph of the pelvis (8A) and coronal proton density-weighted fat-suppressed imaging of the left hip (8B) demonstrate borderline acetabular dysplasia. The lateral center edge angle measures 22 degrees. Postoperative coronal proton density-weighted fat-suppressed imaging (8C,D) demonstrates interval narrowing of the superolateral joint and progressive high-grade chondral loss along the superolateral aspect of the femoral head (arrowhead) with mild subchondral marrow edema. The ligamentum teres is thickened, edematous, a portion of the fibers appear torn (arrow), and marrow edema is present within the fovea capitis (asterisk). The iliofemoral ligament is diffusely thinned (short arrows) but no fluid-filled defect is present. These findings are suspicious for instability in a patient with borderline acetabular dysplasia prior to surgery. Capsular plication is now recommended in patients with borderline acetabular dysplasia or ligamentous laxity. The labrum appears everted (blue arrow), possibly due to an adhesion between the labrum and the capsule.
Figure 9:
45 year-old male with worsening left hip pain six months status-post labral repair and femoroplasty. Preoperative AP radiograph of the pelvis (9A) and proton density-weighted fat suppressed axial oblique (9B) and coronal (9C) imaging of the left hip demonstrates borderline acetabular dysplasia. The left lateral center edge angle measures 23 degrees. The ligamentum teres is irregularly attenuated and frayed but intact fibers are present. Postoperative axial oblique proton density-weighted fat suppressed (9D), sagittal proton density-weighted (9E), coronal proton density-weighted fat suppressed (9F), and AP pelvis radiograph (9G) imaging demonstrates superolateral migration of the femoral head with anterior subluxation. Mild subchondral flattening and marrow edema is present along the anterior femoral head/neck junction (short arrow), anterior to the femoroplasty. Progressive chondral loss along the anterosuperior and superomedial aspects of the femoral head (arrowheads) is associated with subchondral marrow edema and mild subchondral flattening. The labrum appears re-torn and is everted (arrows). No intact ligamentum teres fibers are present, and it is unclear whether this is related to surgical debridement or traumatic rupture. This constellation of findings is suggestive of anterior instability.
Post-arthroscopic Adhesions
Post-arthroscopic adhesions may be intra-articular or extra-articular, and a recent study indicated that capsular adhesions were present in 35% of both asymptomatic and symptomatic patients.24 Intra-articular adhesions generally appear on MRI as linear intermediate to hypointense bands of soft tissue arising between the capsule and labrum along the site of the labral repair, or between the capsule and femur along the femoral osteoplasty (Figure 10).
Adhesions between the capsule and the labrum may result in tethering of the labral fibers, eversion of the labrum, and a recurrent tear.25 Extra-articular adhesions are also possible, especially in patients who have undergone iliopsoas tenotomy or subspine decompression (Figure 11).
Figure 10:
38 year-old with recurrent right hip pain eight months status-post arthroscopic labral debridement, acetabuloplasty, and femoroplasty. Postoperative sagittal proton density-weighted (10A), coronal (10B) and axial oblique (10C) fat-suppressed proton density-weighted imaging demonstrates a thick band of scar tissue extending from the anterior acetabular rim and along the anterior capsule to the femoral head, which is consistent with an adhesion (arrows). Post-arthroscopic adhesions are common and may be asymptomatic, therefore, a description of the findings without assessing causality is important. Initial management is usually conservative.
Figure 11:
45 year-old female with recurrent right hip pain twenty months status-post arthroscopic labral debridement and acetabuloplasty, complicated by rectus femoris avulsion one month post-operatively. Postoperative Dunn radiograph (11A) and sagittal proton density-weighted (11B) imaging demonstrate heterotopic ossification along the AIIS (arrowhead) with a thickened band of scar tissue (arrow) tethering the rectus femoris tendon (short arrow) to the anterior capsule.
Heterotopic Ossification
Heterotopic ossification is a known complication of hip arthroscopy and prophylactic NSAID therapy has been shown to decrease the prevalence from 46% to 4%.26 While the majority of HO is thought to be asymptomatic and not requiring intervention, it is important to comment on the presence of HO as it may be a source of pain or decreased range of motion.27
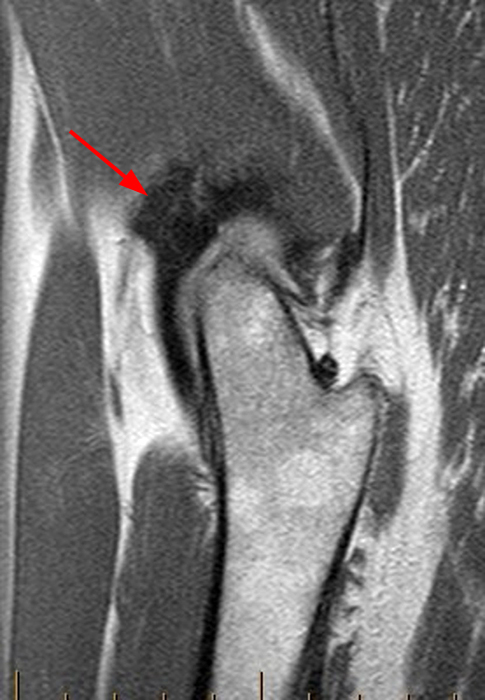
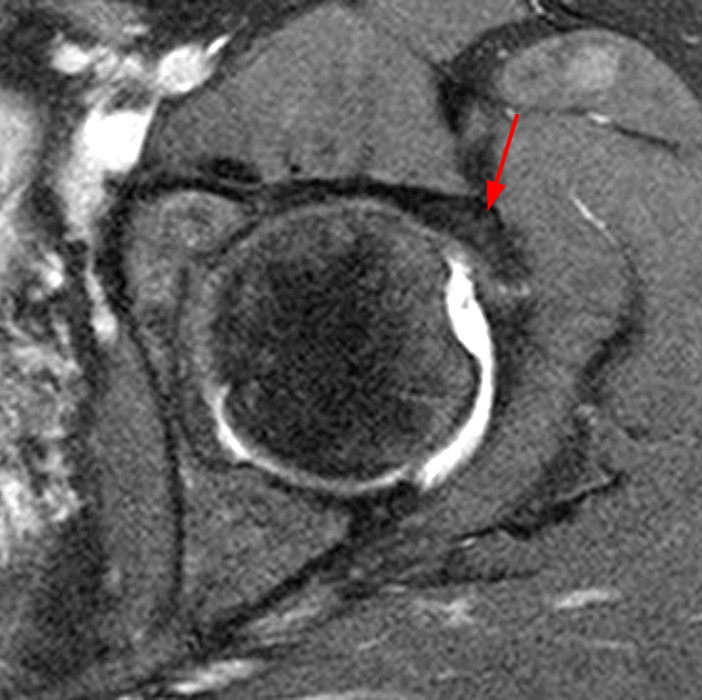
Heterotopic ossification most often occurs along the anterior aspect of the hip, and concomitant radiographic evaluation is helpful as the MRI findings may be subtle (Figure 12). In cases where heterotopic ossification is present, it is helpful to be aware of the Brooker classification (Figure 13).
Figure 12:
41 year-old female with recurrent left hip pain two years status-post arthroscopic labral repair, acetabuloplasty, and femoroplasty. Postoperative Dunn radiograph at 5 months (12A) and 2 years (12B) after surgery demonstrate increased conspicuity of heterotopic ossification along the anterolateral aspect of the joint in the location of the iliofemoral ligament. Postoperative sagittal proton density-weighted (12C), coronal (12D) and axial (12E) fat-suppressed proton density-weighted imaging denotes heterotopic ossification embedded (arrows) within the iliofemoral ligament.
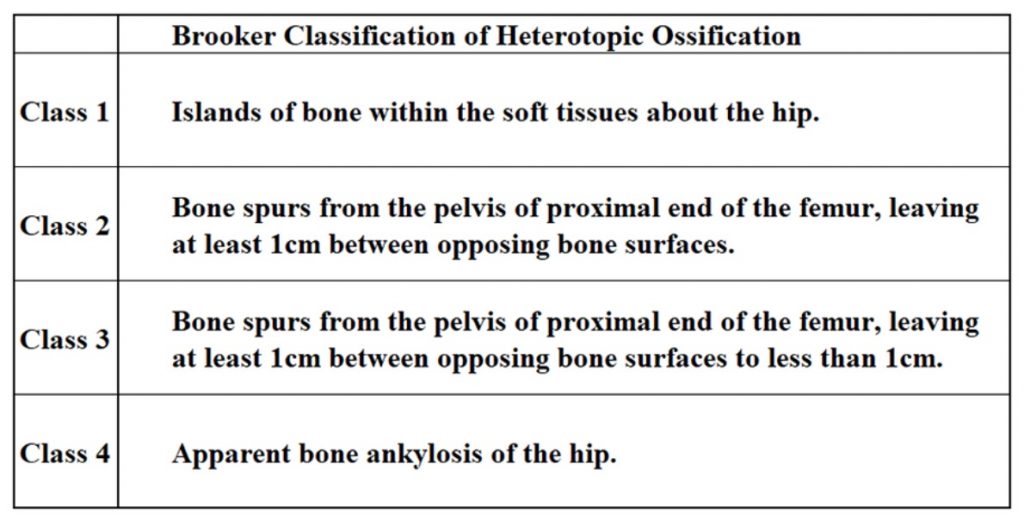
Brooker classification of heterotopic ossification.28
Conclusion
The etiology of persistent or recurrent pain following hip preservation surgery is multifactorial, and MRI is the imaging modality of choice in evaluating the patient with postoperative pain. Knowledge of how hip preservation surgery is performed, the complications that may arise, and how to objectively describe the imaging findings should improve our ability to evaluate preoperative risk factors and identify clinically relevant postoperative complications.
References
- Philippon, M. J., Nepple, J. J., Campbell, K. J., Dornan, G. J., Jansson, K. S., LaPrade, R. F., & Wijdicks, C. A. (2014). The hip fluid seal—Part I: the effect of an acetabular labral tear, repair, resection, and reconstruction on hip fluid pressurization. Knee Surgery, Sports Traumatology, Arthroscopy, 22(4), 722–729. doi:10.1007/s00167-014-2874-z ↩
- Riff, A. J., Kunze, K. N., Movassaghi, K., Hijji, F., Beck, E. C., Harris, J. D., & Nho, S. J. (2019). Systematic Review of Hip Arthroscopy for Femoroacetabular Impingement: The Importance of Labral Repair and Capsular Closure. Arthroscopy: The Journal of Arthroscopic & Related Surgery, 35(2), 646–656.e3.doi:10.1016/j.arthro.2018.09.005 ↩
- Domb, B. G., Hartigan, D. E., & Perets, I. (2017). Decision Making for Labral Treatment in the Hip. Journal of the American Academy of Orthopaedic Surgeons, 25(3), e53–e62.doi:10.5435/jaaos-d-16-00144 ↩
- Larson, C. M., Giveans, M. R., & Stone, R. M. (2012). Arthroscopic Debridement Versus Refixation of the Acetabular Labrum Associated With Femoroacetabular Impingement. The American Journal of Sports Medicine, 40(5), 1015–1021.doi:10.1177/0363546511434578 ↩
- Lynch, T.S., Minkara, A., Aoki, S., Bedi, A., Bharam, S., Clohisy, J., Harris, J., Larson, C., Nepple, J., Nho, S., Philippon, M., Rosneck, J., Safran, M., Stubbs, A.J., Westermann, R., Byrd, J.W.T. (2019). Best Practice Guidelines for Hip Arthroscopy in Femoroacetabular Impingement: Results of a Delphi Process. Journal of the American Academy of Orthopaedic Surgeons. doi: 10.5435/JAAOS-D-18-00041 ↩
- Li, A. E., Jawetz, S. T., Greditzer, H. G., Burge, A. J., Nawabi, D. H., & Potter, H. G. (2016). MRI Evaluation of Femoroacetabular Impingement After Hip Preservation Surgery. American Journal of Roentgenology, 207(2), 392–400. doi:10.2214/ajr.15.15427 ↩
- Seldes, R. M., Tan, V., Hunt, J., Katz, M., Winiarsky, R., & Fitzgerald, R. H. (2001). Anatomy, Histologic Features, and Vascularity of the Adult Acetabular Labrum. Clinical Orthopaedics and Related Research, 382, 232–240.doi:10.1097/00003086-200101000-00031 ↩
- Botser, I., & Safran, M. R. (2013). MR Imaging of the Hip. Magnetic Resonance Imaging Clinics of North America, 21(1), 169–182.doi:10.1016/j.mric.2012.08.008 ↩
- Kelly, B. T., Weiland, D. E., Schenker, M. L., & Philippon, M. J. (2005). Arthroscopic Labral Repair in the Hip: Surgical Technique and Review of the Literature. Arthroscopy: The Journal of Arthroscopic & Related Surgery, 21(12), 1496–1504.doi:10.1016/j.arthro.2005.08.013 ↩
- Gédouin, J.-E. (2012). Arthroscopic treatment of femoroacetabular impingement: Technical review. Orthopaedics & Traumatology: Surgery & Research, 98(5), 583–596.doi:10.1016/j.otsr.2012.06.001 ↩
- Ziegert, A. J., Blankenbaker, D. G., De Smet, A. A., Keene, J. S., Shinki, K., & Fine, J. P. (2009). Comparison of Standard Hip MR Arthrographic Imaging Planes and Sequences for Detection of Arthroscopically Proven Labral Tear. American Journal of Roentgenology, 192(5), 1397–1400.doi:10.2214/ajr.08.1609 ↩
- Blankenbaker, D. G., De Smet, A. A., & Keene, J. S. (2011). MR Arthrographic Appearance of the Postoperative Acetabular Labrum in Patients With Suspected Recurrent Labral Tears. American Journal of Roentgenology, 197(6), W1118–W1122. doi:10.2214/ajr.11.6671 ↩
- Crim, J. (2017). Imaging evaluation of the hip after arthroscopic surgery for femoroacetabular impingement. Skeletal Radiology, 46(10), 1315–1326. doi:10.1007/s00256-017-2665-y ↩
- Matsuda, D. K., Bharam, S., White, B. J., Matsuda, N. A., & Safran, M. (2015). Anchor-induced chondral damage in the hip. Journal of Hip Preservation Surgery, 2(1), 56–64.doi:10.1093/jhps/hnv001 ↩
- Woodward, R. M., & Philippon, M. J. (2018). Persistent or recurrent symptoms after arthroscopic surgery for femoroacetabular impingement: A review of imaging findings. Journal of Medical Imaging and Radiation Oncology. doi:10.1111/1754-9485.12822 ↩
- Telleria, J. J. M., Lindsey, D. P., Giori, N. J., & Safran, M. R. (2013). A quantitative assessment of the insertional footprints of the hip joint capsular ligaments and their spanning fibers for reconstruction. Clinical Anatomy, 27(3), 489–497.doi:10.1002/ca.22272 ↩
- Ortiz-Declet, V., Mu, B., Chen, A. W., Litrenta, J., Perets, I., Yuen, L. C., & Domb, B. G. (2018). Should the Capsule Be Repaired or Plicated After Hip Arthroscopy for Labral Tears Associated With Femoroacetabular Impingement or Instability? A Systematic Review. Arthroscopy: The Journal of Arthroscopic & Related Surgery, 34(1), 303–318. doi:10.1016/j.arthro.2017.06.030 ↩
- Aoki, S. K. (2019). Editorial Commentary: Hip Arthroscopy Capsular Approaches: Periportal, Puncture, Interportal, T-Cut…Does It Really Matter? Arthroscopy: The Journal of Arthroscopic & Related Surgery, 35(4), 1128–1129. doi:10.1016/j.arthro.2019.01.021 ↩
- Duplantier, N. L., McCulloch, P. C., Nho, S. J., Mather, R. C., Lewis, B. D., & Harris, J. D. (2016). Hip Dislocation or Subluxation After Hip Arthroscopy: A Systematic Review. Arthroscopy: The Journal of Arthroscopic & Related Surgery, 32(7), 1428–1434. doi:10.1016/j.arthro.2016.01.056 ↩
- Weber, A. E., Kuhns, B. D., Cvetanovich, G. L., Lewis, P. B., Mather, R. C., Salata, M. J., & Nho, S. J. (2017). Does the Hip Capsule Remain Closed After Hip Arthroscopy With Routine Capsular Closure for Femoroacetabular Impingement? A Magnetic Resonance Imaging Analysis in Symptomatic Postoperative Patients. Arthroscopy: The Journal of Arthroscopic & Related Surgery, 33(1), 108–115. doi:10.1016/j.arthro.2016.07.022 ↩
- Kraeutler, M. J., Strickland, C. D., Brick, M. J., Garabekyan, T., Woon, J. T. K., Chadayammuri, V., & Mei-Dan, O. (2018). A multicenter, double-blind, randomized controlled trial comparing magnetic resonance imaging evaluation of repaired versus unrepaired interportal capsulotomy in patients undergoing hip arthroscopy for femoroacetabular impingement. Journal of Hip Preservation Surgery, 5(4), 349–356.doi:10.1093/jhps/hny045 ↩
- Brady, A. W., Chahla, J., Locks, R., Mikula, J. D., Slette, E. L., LaPrade, R. F., & Philippon, M. J. (2018). Arthroscopic Reconstruction of the Ligamentum Teres: A Guide to Safe Tunnel Placement. Arthroscopy: The Journal of Arthroscopic & Related Surgery, 34(1), 144–151.doi:10.1016/j.arthro.2017.08.308 ↩
- Byrd, J. W. T., & Jones, K. S. (2004). Traumatic rupture of the ligamentum teres as a source of hip pain. Arthroscopy: The Journal of Arthroscopic & Related Surgery, 20(4), 385–391.doi:10.1016/j.arthro.2004.01.025 ↩
- Kim, C.-H. O., Dietrich, T. J., Zingg, P. O., Dora, C., Pfirrmann, C. W. A., & Sutter, R. (2017). Arthroscopic Hip Surgery: Frequency of Postoperative MR Arthrographic Findings in Asymptomatic and Symptomatic Patients. Radiology, 283(3), 779–788. doi:10.1148/radiol.2016161078 ↩
- Locks, R., Bolia, I., Utsunomiya, H., Briggs, K., & Philippon, M. J. (2018). Current concepts in revision hip arthroscopy. HIP International, 112070001877192.doi:10.1177/1120700018771927 ↩
- Beckmann, J. T., Wylie, J. D., Potter, M. Q., Maak, T. G., Greene, T. H., & Aoki, S. K. (2015). Effect of Naproxen Prophylaxis on Heterotopic Ossification Following Hip Arthroscopy. The Journal of Bone and Joint Surgery-American Volume, 97(24), 2032–2037.doi:10.2106/jbjs.n.01156 ↩
- Kurz, A. Z., LeRoux, E., Riediger, M., Coughlin, R., Simunovic, N., Duong, A., … Ayeni, O. R. (2019). Heterotopic Ossification in Hip Arthroscopy: an Updated Review. Current Reviews in Musculoskeletal Medicine.doi:10.1007/s12178-019-09543-9 ↩
- Banaszkiewicz, P. A. (2013). Ectopic Ossification Following Total Hip Replacement: Incidence and a Method of Classification. Classic Papers in Orthopaedics, 105–107.doi:10.1007/978-1-4471-5451-8_25 ↩