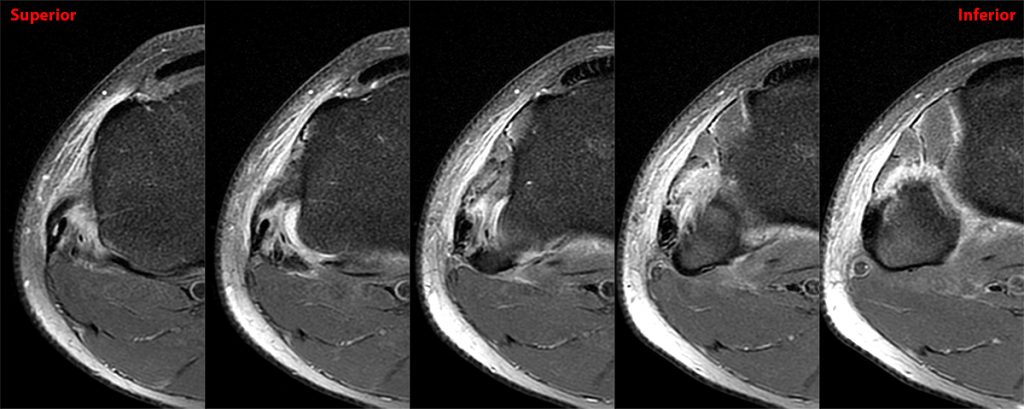
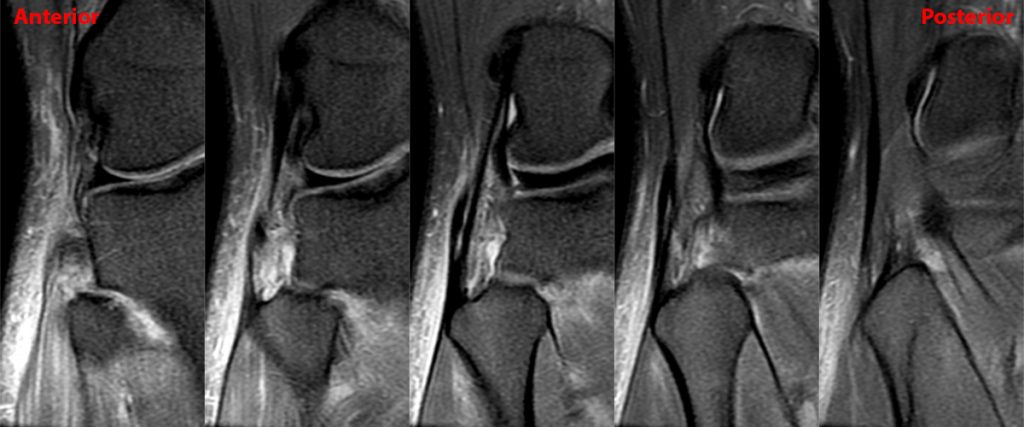
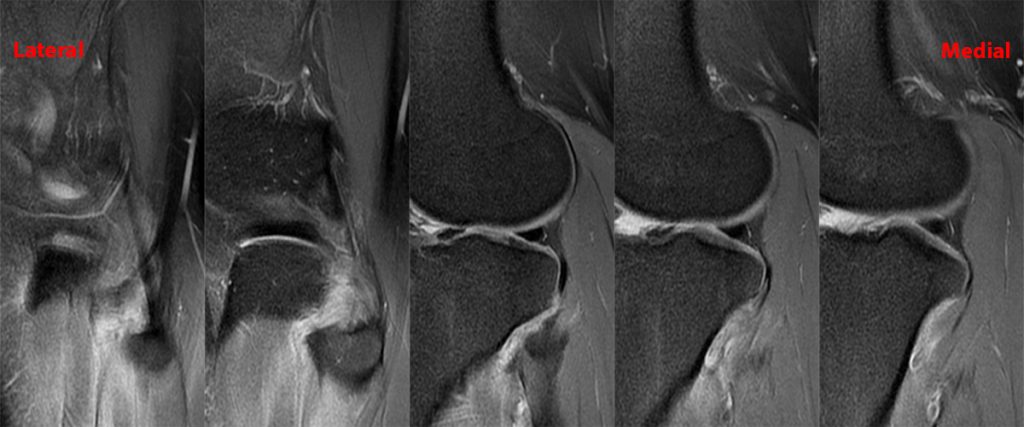
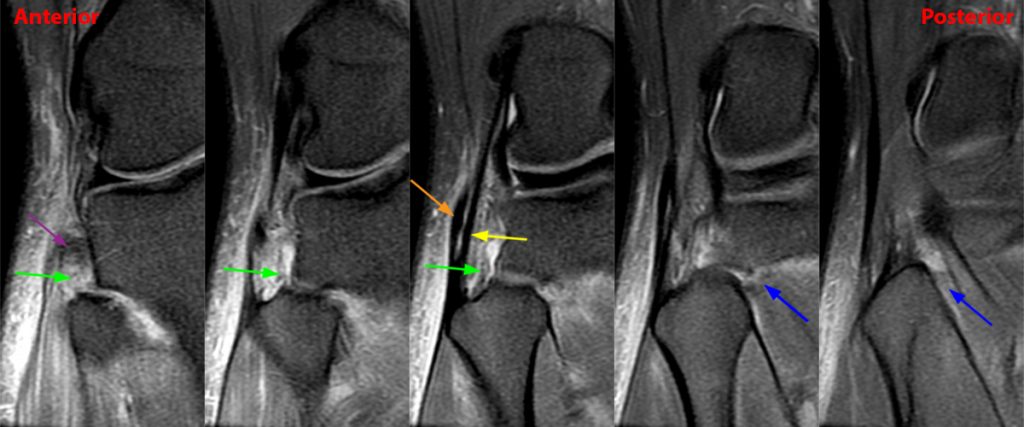
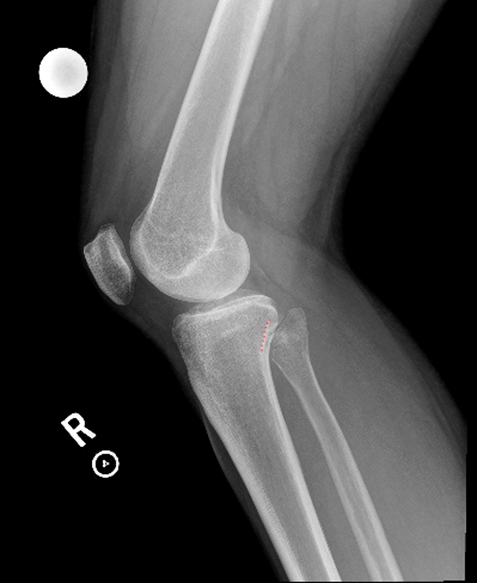
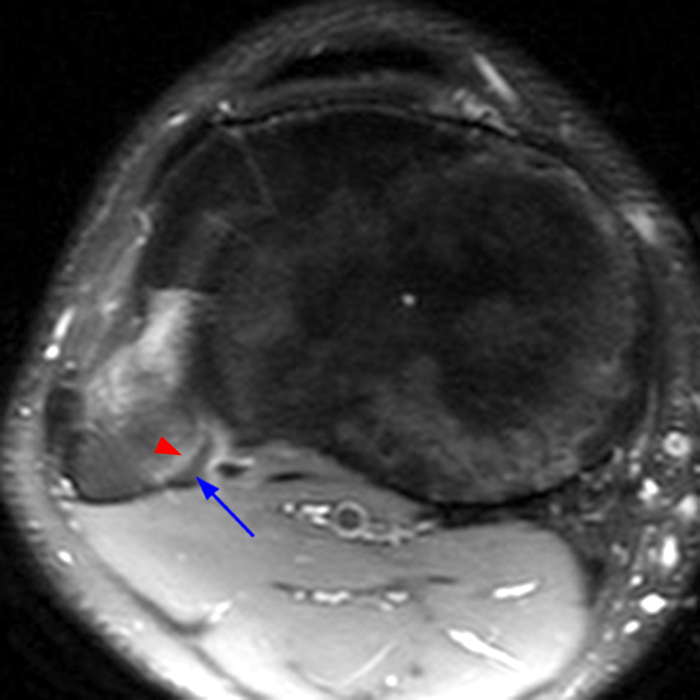
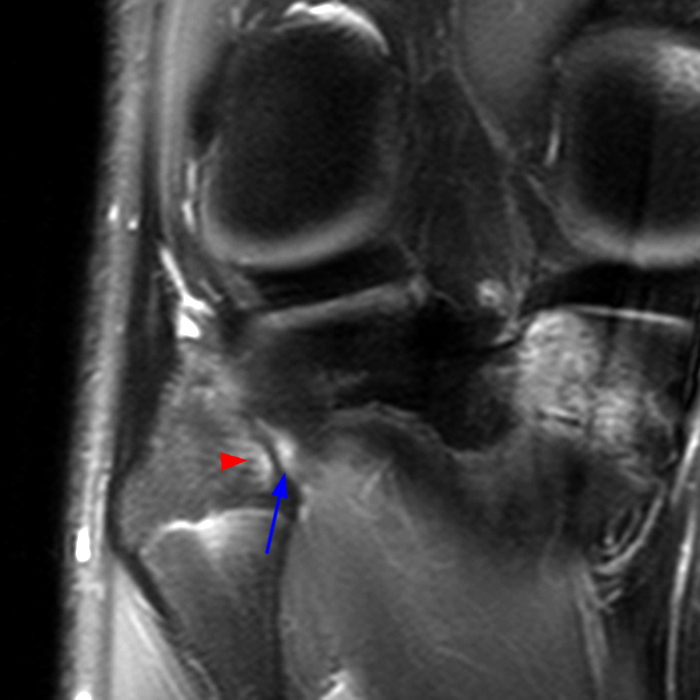
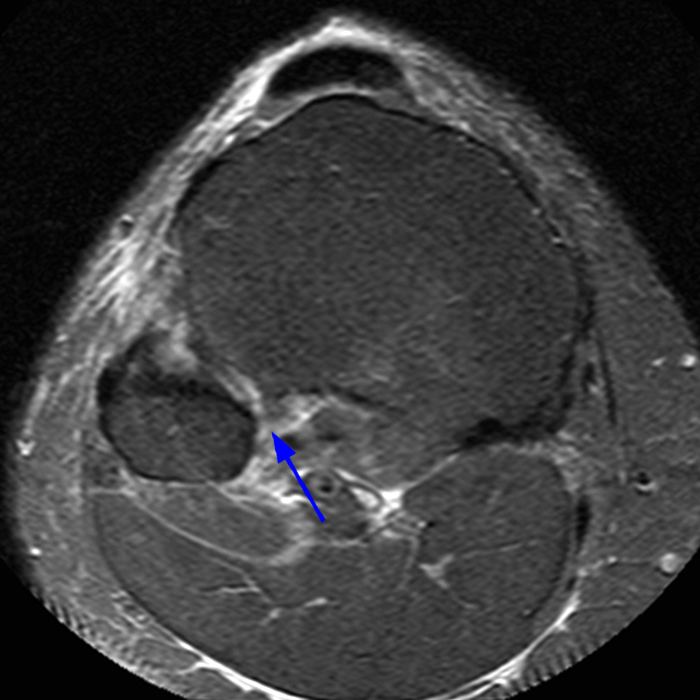
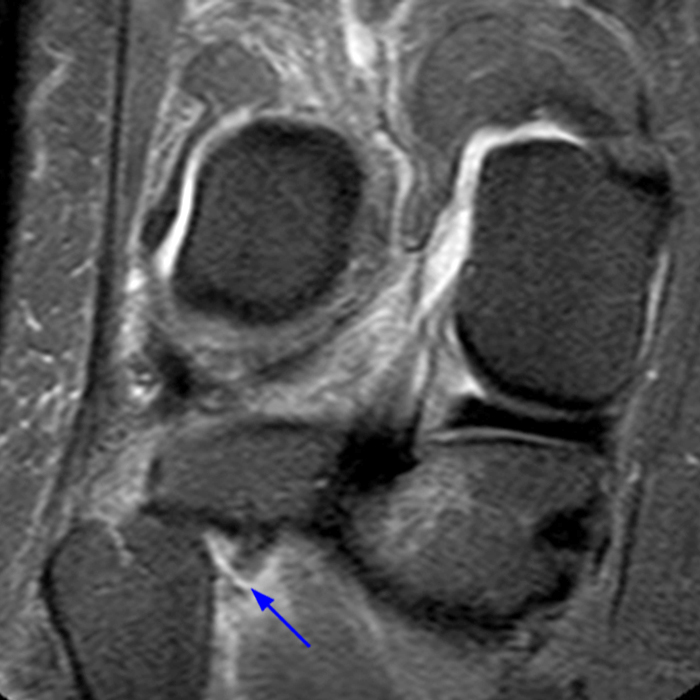
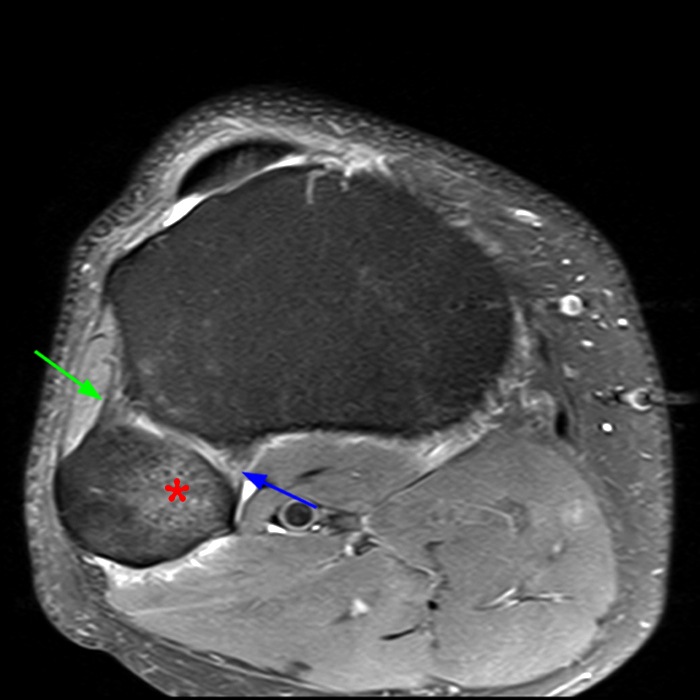
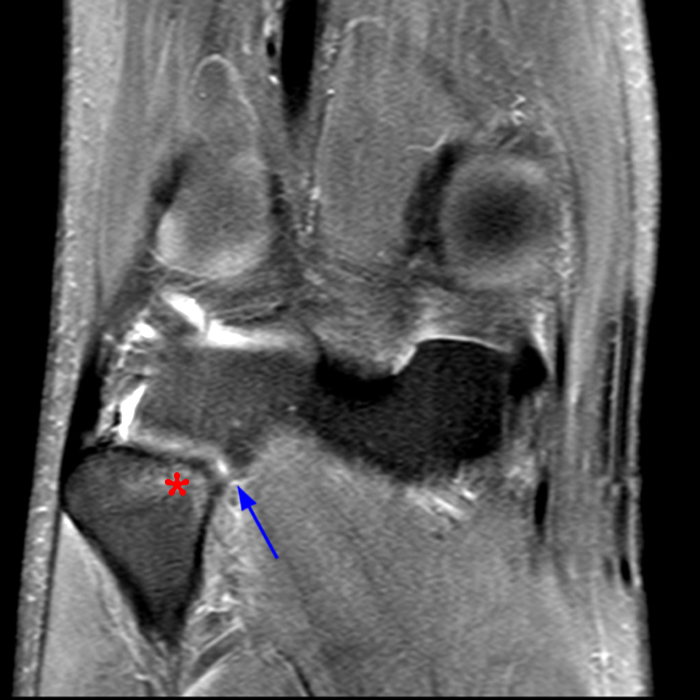
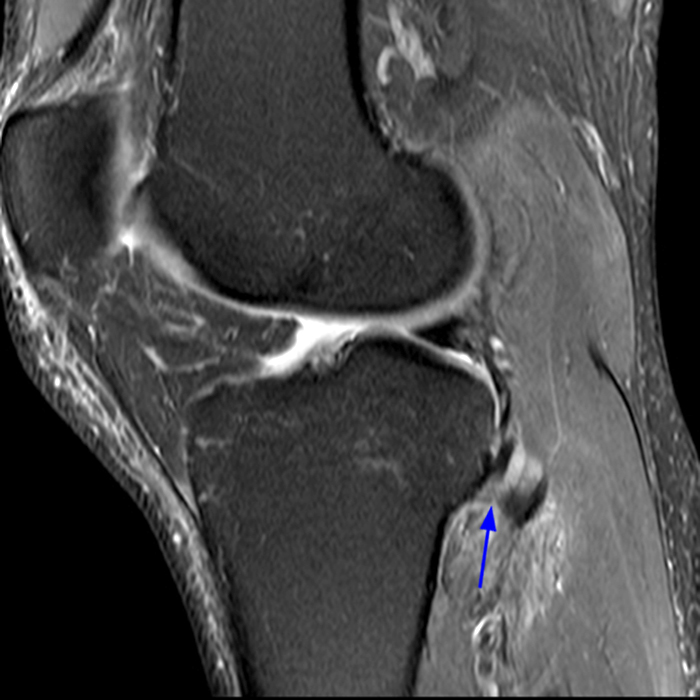
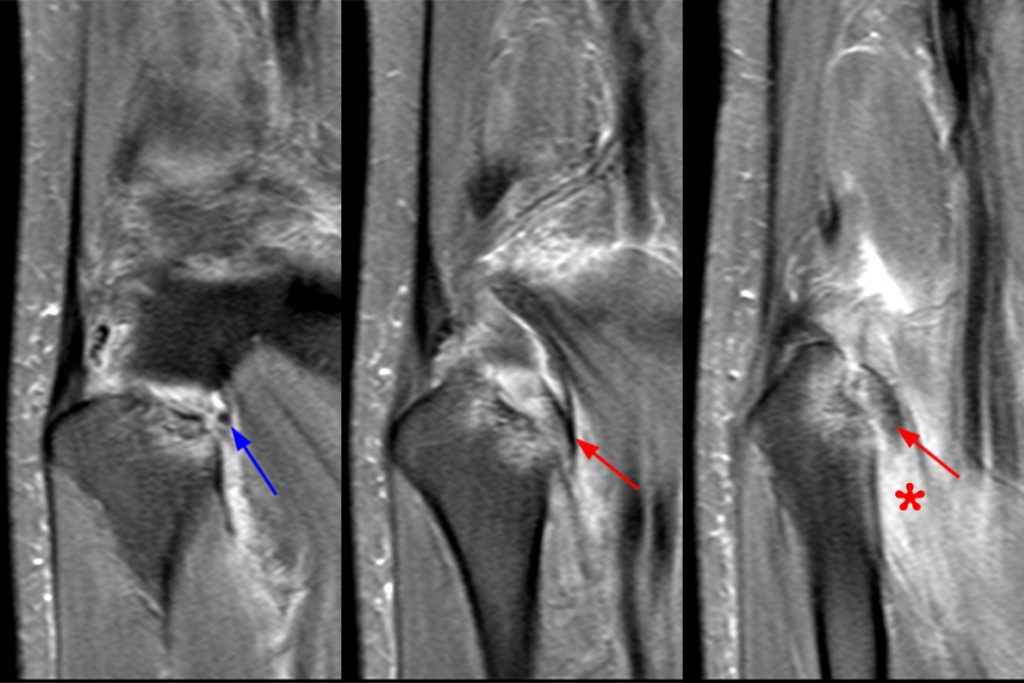
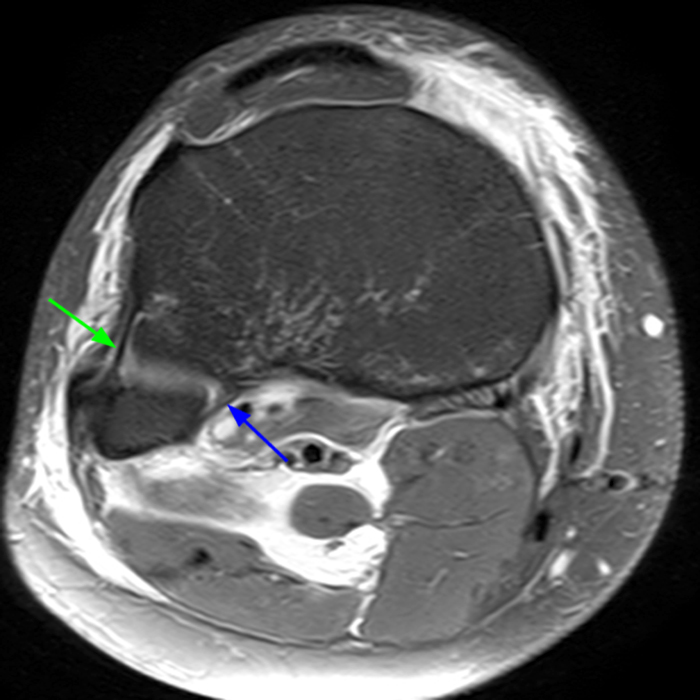
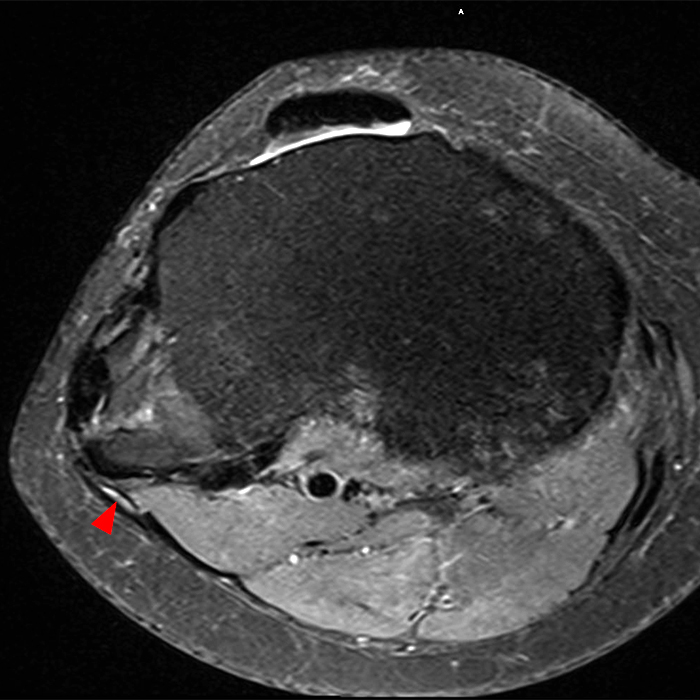
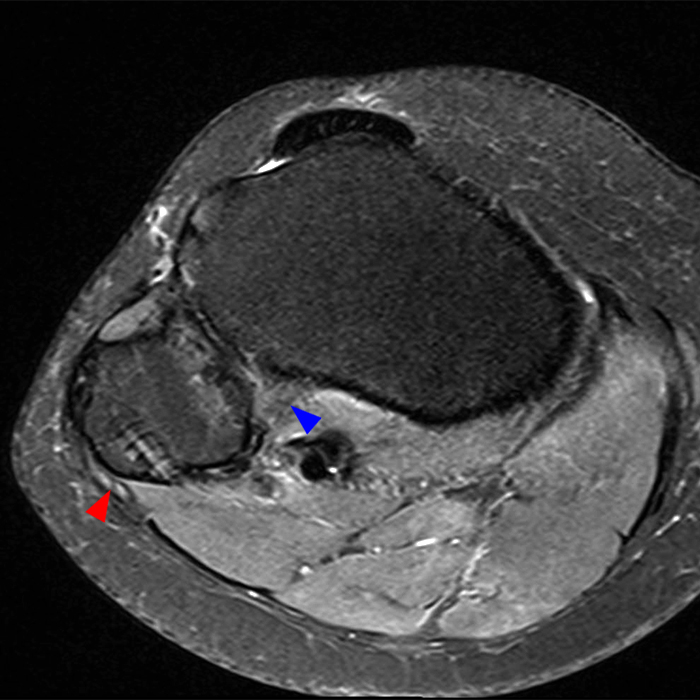
Clinical History: 21-year-old male with lateral knee pain radiating into the calf status-post soccer injury. Rule out lateral meniscus tear. Sequential axial (1A), coronal (1B), and sagittal (1C) fat-suppressed proton density-weighted images are provided through the proximal tibiofibular joint. What are the findings? What is your diagnosis?
Findings
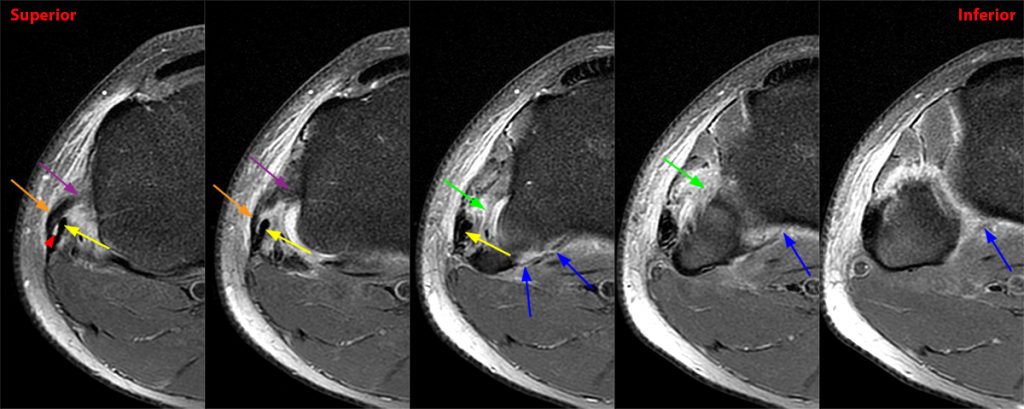
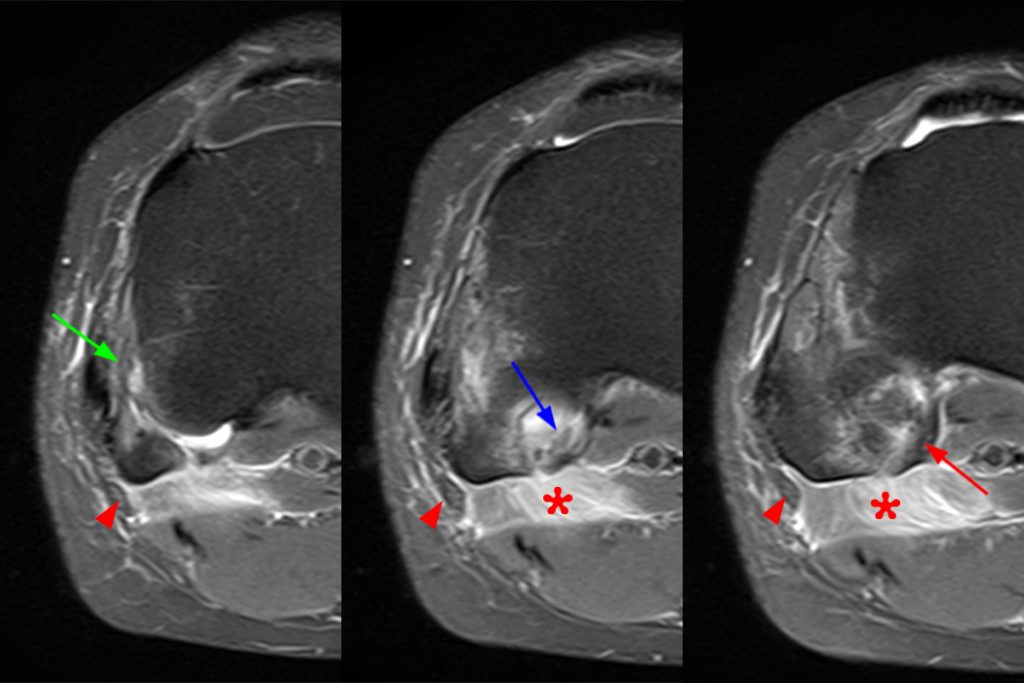
Figure 2:
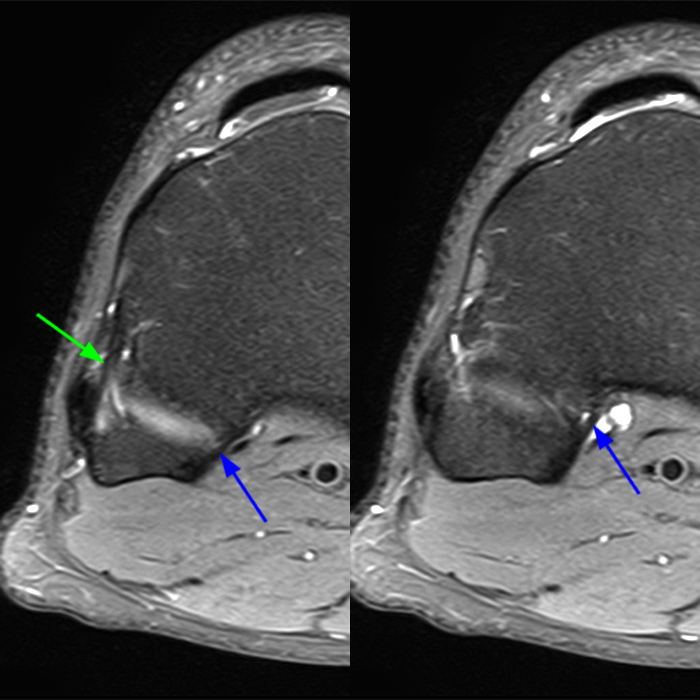
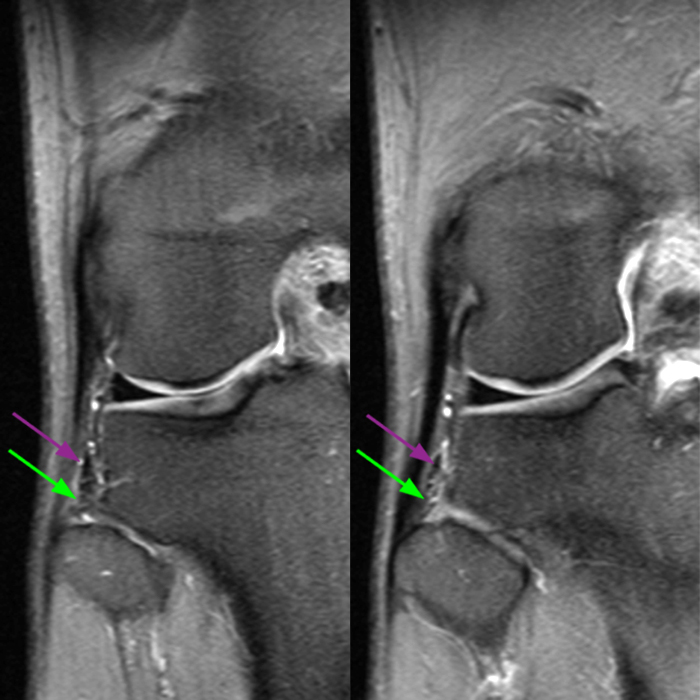
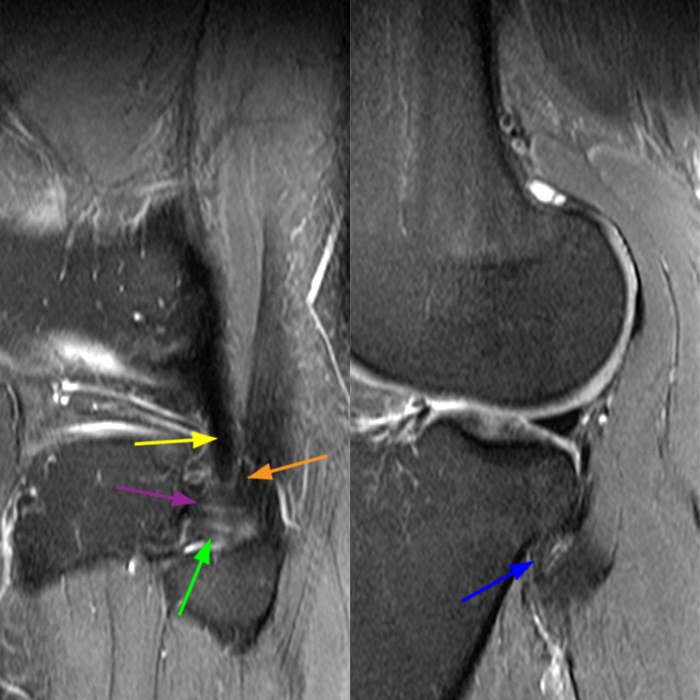
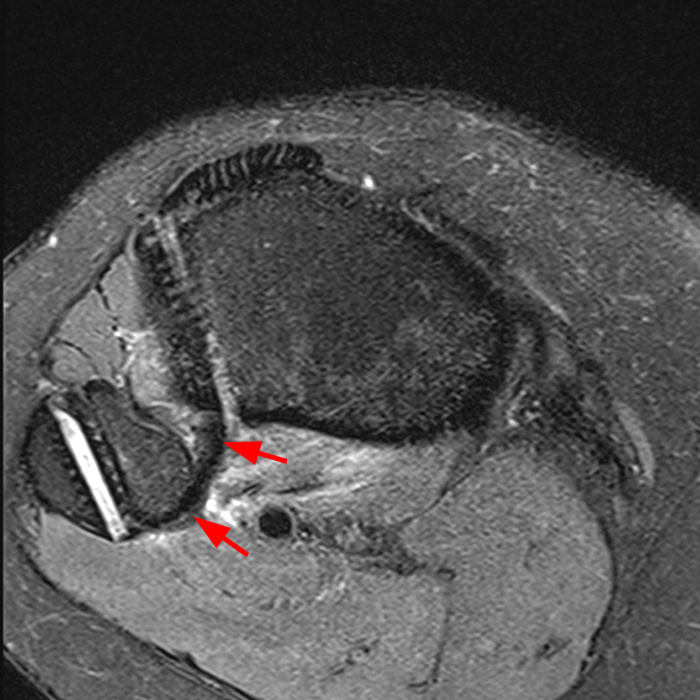
Axial images from superior to inferior demonstrate soft tissue edema surrounding the proximal tibiofibular joint. On the superior axial image, a small amount of fluid (arrowhead) in the fibular collateral ligament (FCL)-biceps femoris bursa delineates the relationship between the anterior arm of the long head of the biceps femoris tendon (orange arrows) and the FCL (yellow arrows). As the anterior arm of the long head of the biceps femoris tendon courses inferiorly, it contributes to the anterior aponeurosis and is intimately associated with the anterior tibiofibular ligament (green arrows). The anterior tibiofibular ligament lies just caudal to the anterior arm of the short head of the biceps femoris tendon (purple arrows) which courses anteromedial to the FCL to insert onto the tibia approximately 1 cm posterior to Gerdy’s tubercle. The anterior-most sagittal image demonstrates the relationship between the anterior arm of the short head of the biceps femoris tendon (purple arrow), the fibular insertion of the FCL (yellow arrow), and the anterior tibiofibular ligament (green arrow).
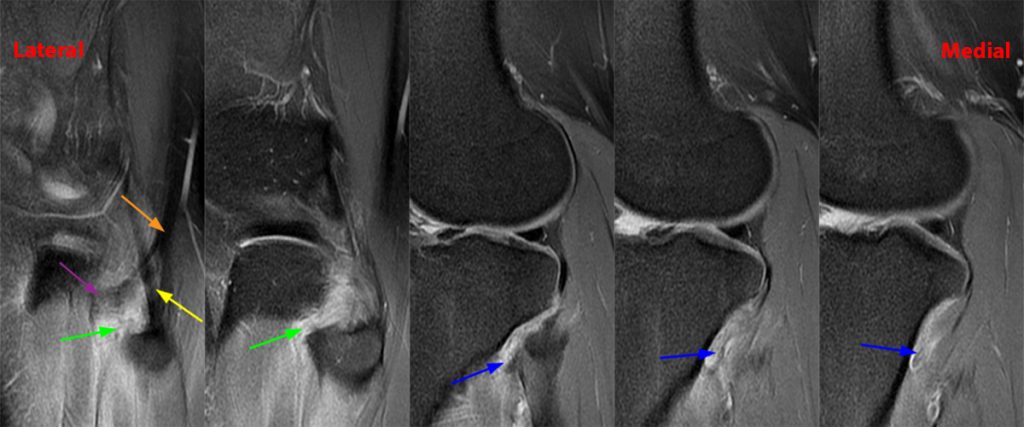
On the axial, sagittal, and coronal images, the anterior tibiofibular ligament (green arrows) is diffusely edematous and a portion of the ligament fibers are discontinuous. The posterior ligament (blue arrow) is edematous, the midportion of the ligament is abnormally thinned on the axial, coronal, and sagittal images, and the tibial insertion is torn on the posterior-most coronal image.
Diagnosis
Recent traumatic anterolateral proximal tibiofibular joint dislocation.
Introduction
Instability of the proximal tibiofibular joint (PTFJ) may be acute or chronic in etiology and four types of instability initially described by Ogden include anterolateral dislocation, posteromedial dislocation, superior dislocation, and atraumatic subluxation.1 Anterolateral dislocation is by far the most common form of instability and the focus of this discussion.
Anatomy
The proximal tibiofibular joint is a synovial sliding joint which dissipates torsional forces applied at the ankle and tensile forces generated during lateral tibial bending moments.2 The joint is stabilized by multiple ligaments including the anterior and posterior tibiofibular ligaments as well as the fibular collateral ligament (FCL).
The anterior ligament is composed of three to four bundles and is further reinforced by the anterior aponeurosis arising from the long head of the biceps femoris tendon (BFT).3,4 The posterior ligament is generally composed of three bundles and significantly weaker than the anterior ligament (Figure 3).5 The inherent joint stability is also directly related to the inclination of the articular-surface which is classically defined as horizontal or oblique. The horizontal variant has been associated with greater surface area and increased rotatory mobility, thus less prone to injury.
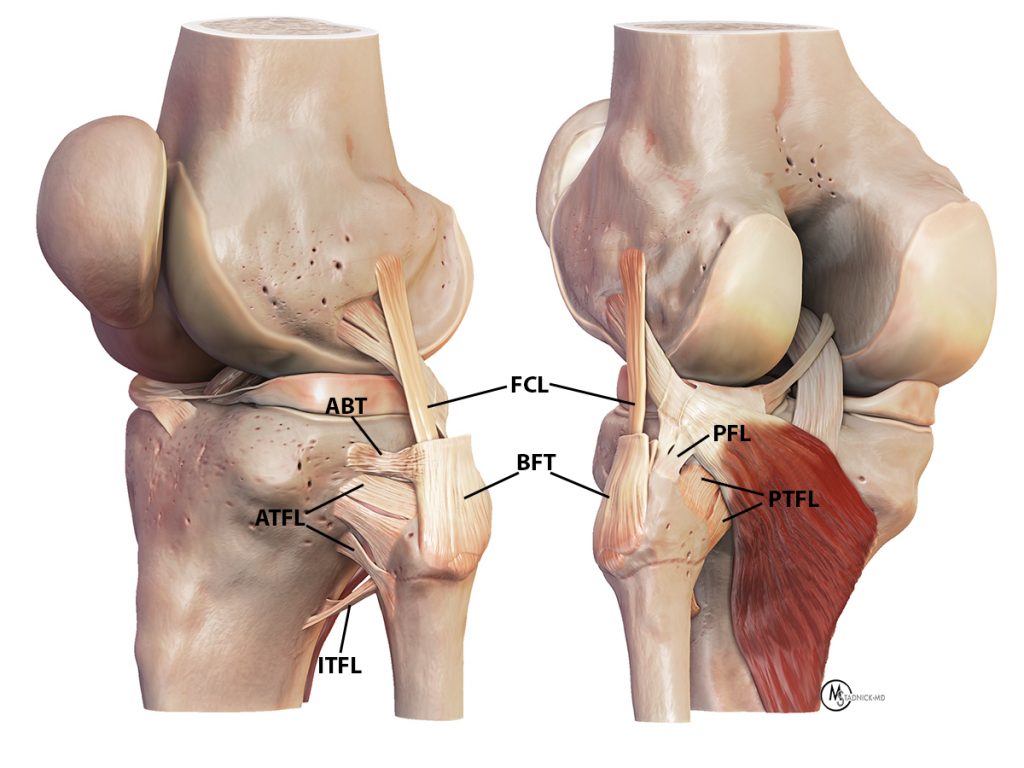
Figure 3:
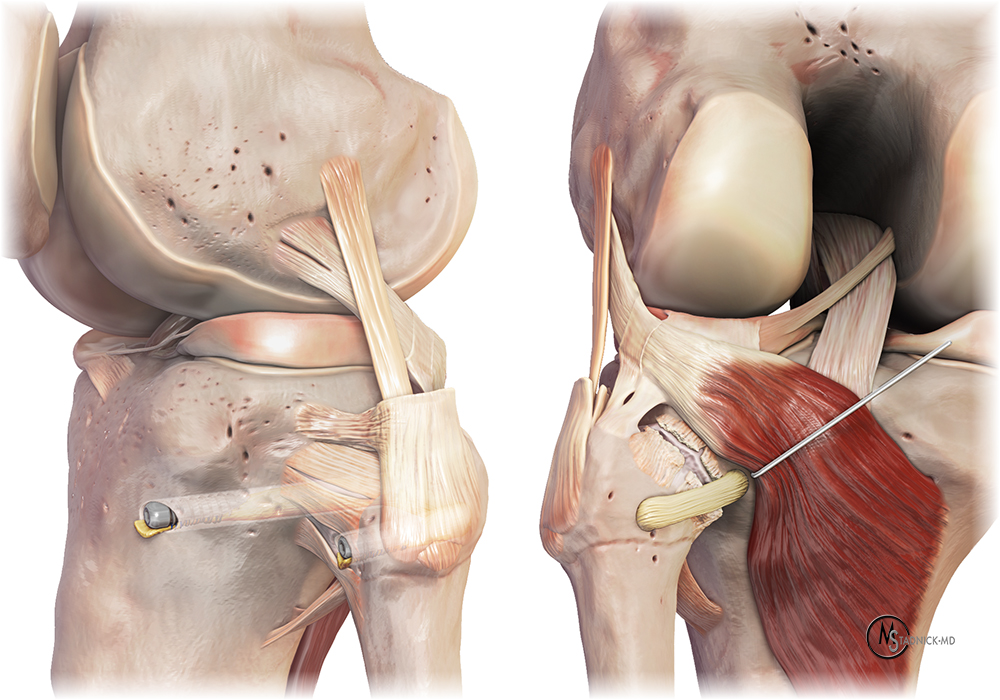
3D renders demonstrate the anterior proximal tibiofibular (ATFL) and posterior proximal tibiofibular (PTFL) ligaments and adjacent anatomy, including the fibular collateral ligament (FCL), biceps tendon (BFT), anterior arm of the biceps tendon (ABT), the popliteofibular ligament (PFL) and the inferior proximal tibiofibular ligament (ITFL).
Pathophysiology
While the role of the fibula and the posterolateral corner (PLC) in maintaining knee stability has received widespread attention, the contribution of the proximal tibiofibular joint to knee stability is often overlooked and injuries may easily go unnoticed.
At the time of clinical evaluation, patients report lateral knee pain or instability which invokes a broad differential diagnosis. A spectrum of sports-related injuries resulting in anterolateral dislocation occur due to a violent twisting of the flexed knee with an inverted foot. When the knee is flexed beyond 30 degrees, relaxation of the FCL and biceps femoris tendons allows the fibula to shift anteriorly which reduces joint stability and allows the fibular head to move approximately 7-10 mm in the anteroposterior plane.6,7 In the event of an added twisting element, external rotation of the tibia pulls the fibula laterally and tension in the anterolateral compartment musculature then further draws the fibula anteriorly.8
Imaging Evaluation
Optimal radiographic evaluation of the PTFJ is performed in 45-60 degrees internal rotation. More commonly, however, AP and lateral radiographs are performed (Figure 4). On the AP radiograph, the fibula should overlap the lateral margin of the lateral tibial condyle and lateral displacement will widen the interosseous space. Evaluation of the PTFJ on the lateral radiographs is less reliable due to variable degrees of knee rotation. However, on a true lateral radiograph, the fibular head should intersect a line created by the posteromedial portion of the lateral tibial condyle and anterior or posterior displacement of the fibular head will disrupt this relationship.9 In cases of transient traumatic dislocation, anatomic alignment may be within normal limits and therefore normal radiographic alignment does not exclude the possibility of recent dislocation or instability.
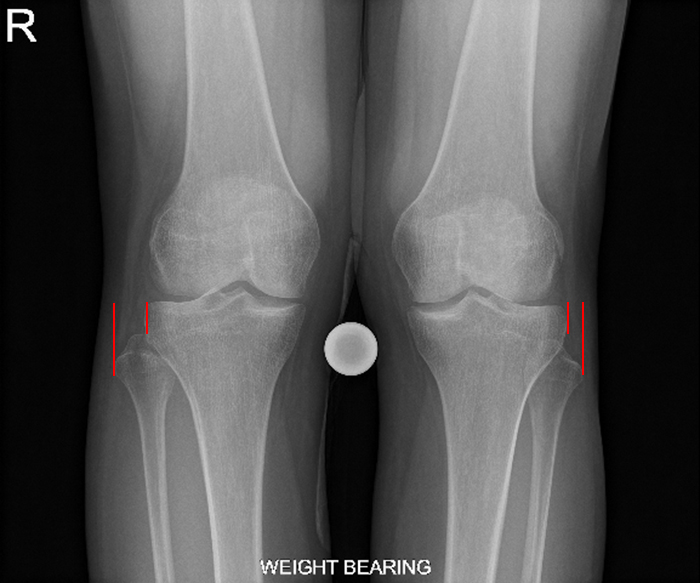
Figure 4:
AP weightbearing radiographs of both knees and lateral radiograph of the right knee in a 31-year-old female who fell while skiing. On the AP radiographs the right knee demonstrates decreased overlap between the fibular head and the lateral tibial condyle compared with the left indicating that the fibular head is displaced laterally. On the lateral radiograph the fibular head barely intersects the radio-dense line (dotted line) representing the posteromedial margin of the lateral tibial condyle. However, this is a fairly common finding due to variable degrees of knee rotation.
On MRI, the tibiofibular ligaments are obliquely oriented and extend cephalad from the fibula to the tibia and therefore multiplanar evaluation is essential.10 The anterior ligament is more readily identified given that it is thicker than the posterior ligament. It often appears striated due to the presence of multiple bundles, and it is located just caudal to the anterior arm of the short head of the biceps femoris tendon. The anterior ligament should be identified in all three planes. Because the posterior ligament is thinner it is often more difficult to identify and best evaluated on axial and sagittal images just anterior to the popliteus musculotendinous unit (Figure 5).
Figure 5:
Axial (5A), coronal (5B) and sagittal (5C) fat-suppressed proton density-weighted images demonstrate the anterior (green arrows) and posterior (blue arrows) PTFJ ligaments. The coronal images demonstrate the normal anterior ligament located just caudal to the anterior arm of the short head of the biceps femoris tendon (purple arrow). The anterior sagittal image demonstrates the normal anterior ligament (green arrow) and the relationship between the anterior ligament, the FCL (yellow arrow), the anterior arm of the short head of the BF tendon (purple arrow), and the anterior arm of the long head of the BF tendon (orange arrow). A sagittal image through the posterior aspect of the PTFJ demonstrates the normal posterior ligament.
MRI evaluation of recent injury will often reveal soft tissue edema both anterior and posterior to the joint, as well as within the ligaments. Both the anterior and posterior ligaments may be torn however the posterior ligament is weaker and more often torn (Figures 6-8).
Figure 6:
18 year-old male slipped on grass playing flag football with subsequent fibular dislocation. Axial and coronal fat-suppressed proton density-weighted images demonstrate soft tissue edema surrounding the PTFJ with subtle irregularity of the posterior ligament (blue arrow) near the fibular attachment and an underlying bone contusion (arrowhead). While it is often difficult to identify a complete tear, in the absence of a history of dislocation or instability, edema in the ligaments associated with a fibular bone bruise along the posterior ligament attachment should raise awareness of recent traumatic injury.
Figure 7:
55 year-old female status-post fibular head dislocation with stable reduction but lateral-sided laxity. Axial (7A) and coronal (7B) fat-suppressed proton density-weighted images demonstrate soft tissue edema at the PTFJ and a tear of the posterior ligament (blue arrows) near the fibular attachment.
Figure 8:
43 year-old male with lateral knee pain status-post snowboarding injury. Axial (8A), coronal (8B), and sagittal (8C) fat-suppressed proton density-weighted images. Soft tissue edema is present in the anterior (green arrow) and posterior (blue arrows) PTFJ ligaments. The posterior ligament is disrupted near the fibular attachment on the axial image with subtle irregularity on the sagittal image. A fibular bone bruise (asterisk) is present near the attachment of the posterior ligament.
Bone marrow contusions along both sides of the joint may or may not be present, and fractures are less common (Figures 9 and 10). When fractures are present, they are more often associated with the posterior ligament and it is important to distinguish these fractures from a posterolateral corner injury. The posterior ligament attaches to the fibula medial to the styloid and inferomedial to the insertion of the popliteofibular ligament.11 The integrity of the FCL and biceps femoris tendons should also be evaluated as posterolateral corner injuries will often demonstrate soft tissue edema surrounding the joint without disruption of the proximal tibiofibular ligaments. (For a review of the posterolateral corner, please refer to https://radsource.us/posterolateral-corner-injury)
Figure 9:
Same patient as radiographs in Figure 4. 31 year-old female status-post fall and twisting injury while skiing with lateral knee pain radiating down the calf. Sequential axial (9A) and coronal (9B) fat-suppressed proton density-weighted images demonstrate a 20 mm avulsion fracture of the fibular head (red arrows) medial to the styloid at the posterior tibiofibular ligament insertion (blue arrows). The fracture was extremely difficult to visualize on radiographs. The anterior tibiofibular ligament (green arrow) is edematous but in continuity. Focal edema is seen in the proximal soleus muscle (asterisks) adjacent to the fracture, and edema surrounds the common peroneal nerve (arrowhead).
MRI evaluation of chronic instability is more challenging given the lack of associated soft tissue edema (Figure 11). Patients often report a history of clicking, popping, and instability. Common considerations include lateral meniscus pathology, FCL injury/PLC instability, biceps tendonitis, and distal iliotibial band friction syndrome. In some cases, the posterior ligament will be notably absent, but given how small the ligaments are, chronic disruption and subsequent scarring may mask the underlying pathology and therefore isolated asymmetric osteoarthritis of the PTFJ may be the only clue.12
In both acute and chronic injuries, evaluation of the common peroneal nerve is also essential (Figure 11). Acute injury to the common peroneal nerve (CPN) may manifest as nerve thickening and increased T2 signal consistent with edema and swelling. A chronically injured CPN may appear atrophic with abnormally increased T2 signal as well as an abnormal contour due to surrounding scar tissue which often effaces the normal perineural fat.
Figure 11:
38 year-old with chronic posterolateral corner instability status-post failed FCL reconstruction with partially visualized fixation screw. The PTFJ is also unstable on physical examination. Axial fat-suppressed proton density-weighted images demonstrates a poorly defined chronically torn posterior PTFJ ligament (blue arrowhead). The CPN (red arrowhead) is abnormally flattened with increased T2 signal.
Surgical Treatment
In acute anterolateral PTFJ dislocation without spontaneous dislocation or fracture, closed reduction is performed. In cases of persistent instability, surgical treatment is indicated. In the past, chronic instability was treated with arthrodesis or fibular head resection; however, complications related to altered knee and ankle biomechanics rendered these options less desirable.13,14,15
As knee ligament reconstruction surgery has developed, various techniques to reconstruct the ligaments have been described. Reconstruction using the biceps femoris tendon16 and iliotibial band17 autograft have been detailed, and LaPrade has also described a technique to reconstruct solely the posterior ligaments (Figure 12).18,19 Reconstruction of the anterior and posterior ligaments utilizing hamstring grafts has been described by Kobbe et al.20 and Morrison et al.21 More recently, multiple technique papers have described PTFJ stabilization without reconstruction.22,23
Figure 12:
3D renders demonstrate posterior proximal tibiofibular reconstruction using LaPrade’s technique (12A). A fat-suppressed proton density-weighted axial image (12B) demonstrates post-surgical appearance after open PTFJ ligament reconstruction with hamstring autograft (arrows) in a 30 year-old competitive weightlifter with chronic PTFJ instability.
For the case discussed in Figure 9 above, stabilization with an adjustable loop cortical fixation device was selected for multiple reasons. In the setting of acute injury and subsequent stabilization, the posterior PTFJ ligaments have been shown to scar, thereby precluding the need for a full reconstruction.22 Moreover, the avulsion fracture portends bone-to-bone healing and any reconstruction technique requiring drilling through the posteromedial aspect of the fibular head risks comminuting and further displacing the fracture fragment.
A slightly curved lateral incision over the fibular head is made. Careful dissection to the posterior aspect of the joint is carried out after a peroneal nerve neurolysis is performed. The common peroneal nerve (CPN) is visualized and protected throughout the case. The posterior capsule is identified with the insertion of the biceps femoris tendon (BFT) and the FCL. Just below these structures, the posterior proximal tibiofibular ligament is inspected. Internal bracing is performed with a knotless suture button (TightRope syndesmosis implant; Arthrex). While protecting the CPN, sharp dissection to the fibular head is performed. The drill sleeve is applied to the lateral aspect of the fibular head, avoiding the insertions of the FCL and the BFT. The drill guide is directed in a posteroanterior direction toward the anteromedial aspect of the proximal tibia, making sure to avoid the MCL and pes anserinus. The drill is advanced through all 4 cortices. The TightRope needle is then passed through to the anteromedial aspect of the tibia until it exits the skin medially. The implant is pulled through, flipping the medial button on the outside of the anteromedial cortex. The implant is pulled back laterally to ensure that the medial button is engaged against the cortex. The TightRope is subsequently tightened by pulling and spreading the sutures until the lateral button reaches the fibular head. Tightening is gradually tested by manipulation of the proximal fibula, until appropriate stability is achieved. Comparison with the contralateral knee is useful to determine adequate tightness. The BFT, FCL, and nerve are inspected, and the wound is closed in layers.
Figure 13A:
Figure 13B:
Figure 13:
13C: Preoperative physical exam video demonstrating gross PTFJ instability (13A), intra-operative physical exam video demonstrating resolution of instability following PTFJ reconstruction utilizing suture button with TightRope fixation (13B), and an AP postoperative radiograph demonstrating restoration of anatomic alignment (compare with preoperative radiograph Figure 4). Surgical treatment discussion and videos courtesy of Jonathan A. Godin, MBA, MD, The Steadman Clinic and Steadman Philippon Research Institute.
Conclusion
Proximal tibiofibular joint dislocation and instability is an easily overlooked cause of lateral knee pain. Evaluation of the joint, the supporting ligaments, and the common peroneal nerve should be assessed alongside evaluation of the posterolateral corner. MRI’s ability to directly inspect the PTFJ supporting ligaments and relevant adjacent anatomy allows accurate characterization of the often unexpected injuries to the PTFJ.
References
- Ogden JA. Subluxation of the proximal tibiofibular joint. Clin Orthop Relat Res. 1974 Jun;(101):192-7. PMID: 4837931. ↩
- Ogden JA. The anatomy and function of the proximal tibiofibular joint. Clin Orthop Relat Res. 1974 Jun;(101):186-91. PMID: 4837930. ↩
- LaPrade RF, Hamilton CD. The fibular collateral ligament-biceps femoris bursa. An anatomic study. Am J Sports Med. 1997 Jul-Aug;25(4):439-43. doi: 10.1177/036354659702500404. PMID: 9240975. ↩
- LaPrade RF, Gilbert TJ, Bollom TS, Wentorf F, Chaljub G. The magnetic resonance imaging appearance of individual structures of the posterolateral knee. A prospective study of normal knees and knees with surgically verified grade III injuries. Am J Sports Med. 2000 Mar-Apr;28(2):191-9. doi: 10.1177/03635465000280020901. PMID: 10750995. ↩
- Marchetti DC, Moatshe G, Phelps BM, Dahl KD, Ferrari MB, Chahla J, Turnbull TL, LaPrade RF. The Proximal Tibiofibular Joint: A Biomechanical Analysis of the Anterior and Posterior Ligamentous Complexes. Am J Sports Med. 2017 Jul;45(8):1888-1892. doi: 10.1177/0363546517697288. Epub 2017 Mar 24. PMID: 28339288. ↩
- Espregueira-Mendes JD, da Silva MV. Anatomy of the proximal tibiofibular joint. Knee Surg Sports Traumatol Arthrosc. 2006 Mar;14(3):241-9. doi: 10.1007/s00167-005-0684-z. Epub 2005 Dec 22. PMID: 16374587. ↩
- Alves-da-Silva T, Guerra-Pinto F, Matias R, Pessoa P. Kinematics of the proximal tibiofibular joint is influenced by ligament integrity, knee and ankle mobility: an exploratory cadaver study. Knee Surg Sports Traumatol Arthrosc. 2019 Feb;27(2):405-411. doi: 10.1007/s00167-018-5070-8. Epub 2018 Jul 28. PMID: 30056605. ↩
- Klaunick G. Recurrent idiopathic anterolateral dislocation of the proximal tibiofibular joint: case report and literature review. J Pediatr Orthop B. 2010 Sep;19(5):409-14. doi: 10.1097/BPB.0b013e3283395f6f. PMID: 20440223. ↩
- Resnick D, Newell JD, Guerra J Jr, Danzig LA, Niwayama G, Goergen TG. Proximal tibiofibular joint: anatomic-pathologic-radiographic correlation. AJR Am J Roentgenol. 1978 Jul;131(1):133-8. doi: 10.2214/ajr.131.1.133. PMID: 97965. ↩
- Dirim B, Wangwinyuvirat M, Frank A, Cink V, Pretterklieber ML, Pastore D, Resnick D. Communication between the proximal tibiofibular joint and knee via the subpopliteal recess: MR arthrography with histologic correlation and stratigraphic dissection. AJR Am J Roentgenol. 2008 Aug;191(2):W44-51. doi: 10.2214/AJR.07.3406. PMID: 18647885. ↩
- Marchetti DC, Chahla J, Moatshe G, Slette EL, LaPrade RF. Quantitative radiographic assessment of the anatomic attachment sites of the anterior and posterior complexes of the proximal tibiofibular joint. Knee Surg Sports Traumatol Arthrosc. 2018 Apr;26(4):1104-1109. doi: 10.1007/s00167-017-4511-0. Epub 2017 Mar 21. PMID: 28326444. ↩
- Burke CJ, Grimm LJ, Boyle MJ, Moorman CT 3rd, Hash TW 2nd. Imaging of Proximal Tibiofibular Joint Instability: A 10 year retrospective case series. Clin Imaging. 2016 May-Jun;40(3):470-6. doi: 10.1016/j.clinimag.2015.12.011. Epub 2016 Jan 16. PMID: 27133689 ↩
- Anavian J, Marchetti DC, Moatshe G, Slette EL, Chahla J, Brady AW, Civitarese DM, LaPrade RF. The forgotten joint: quantifying the anatomy of the proximal tibiofibular joint. Knee Surg Sports Traumatol Arthrosc. 2018 Apr;26(4):1096-1103. doi: 10.1007/s00167-017-4508-8. Epub 2017 Mar 20. PMID: 28321475. ↩
- Dekker TJ, DePhillipo NN, Kennedy MI, Aman ZS, Schairer WW, LaPrade RF. Clinical Characteristics and Outcomes After Anatomic Reconstruction of the Proximal Tibiofibular Joint. Arthroscopy. 2020 Jun;36(6):1649-1654. doi: 10.1016/j.arthro.2020.01.056. Epub 2020 Feb 13. PMID: 32061975. ↩
- Halbrecht JL, Jackson DW. Recurrent dislocation of the proximal tibiofibular joint. Orthop Rev. 1991 Nov;20(11):957-60. PMID: 1749660. ↩
- Giachino A.A. Recurrent dislocations of the proximal tibiofibular joint. Report of two cases. J Bone Joint Surg Am. 1986;68:1104–1106. PMID: 3745254. ↩
- Shapiro G.S., Fanton G.S., Dillingham M.F. Reconstruction for recurrent dislocation of the proximal tibiofibular joint. A new technique. Orthop Rev. PMID: 8127606. ↩
- Horst PK, LaPrade RF. Anatomic reconstruction of chronic symptomatic anterolateral proximal tibiofibular joint instability. Knee Surg Sports Traumatol Arthrosc. 2010 Nov;18(11):1452-5. doi: 10.1007/s00167-010-1049-9. Epub 2010 Feb 3. PMID: 20127312. ↩
- Warner B.T., Moulton S.G., Cram T.R., LaPrade R.F. Anatomic reconstruction of the proximal tibiofibular joint. Arthrosc Tech. 2016;5:e207–e210. DOI: 1016/j.eats.2015.11.004. PMID: 27274455. ↩
- Kobbe P., Flohe S., Wellmann M., Russe K. Stabilization of chronic proximal tibiofibular joint instability with a semitendinosus graft. Acta Orthop Belg. 2010;76:830–833. PMID: 21302584. ↩
- Morrison T.D., Shaer J.A., Little J.E. Bilateral, atraumatic, proximal tibiofibular joint instability. orthopaedics. 2011;34:133. DOI: 10.3928/01477447-20101221-28. PMID: 21323280. ↩
- Oksum M, Randsborg PH. Treatment of Instability of the Proximal Tibiofibular Joint by Dynamic Internal Fixation With a Suture Button. Arthrosc Tech. 2018;7(10):e1057-e1061. Published 2018 Sep 24. doi:10.1016/j.eats.2018.08.004. PMID: 30377586. ↩
- McNamara WJ, Matson AP, Mickelson DT, Moorman CT 3rd. Surgical Management of Proximal Tibiofibular Joint Instability Using an Adjustable Loop, Cortical Fixation Device. Arthrosc Tech. 2018 Feb 26;7(3):e271-e277. doi: 10.1016/j.eats.2017.09.003. PMID: 29881700; PMCID: PMC5989917. ↩