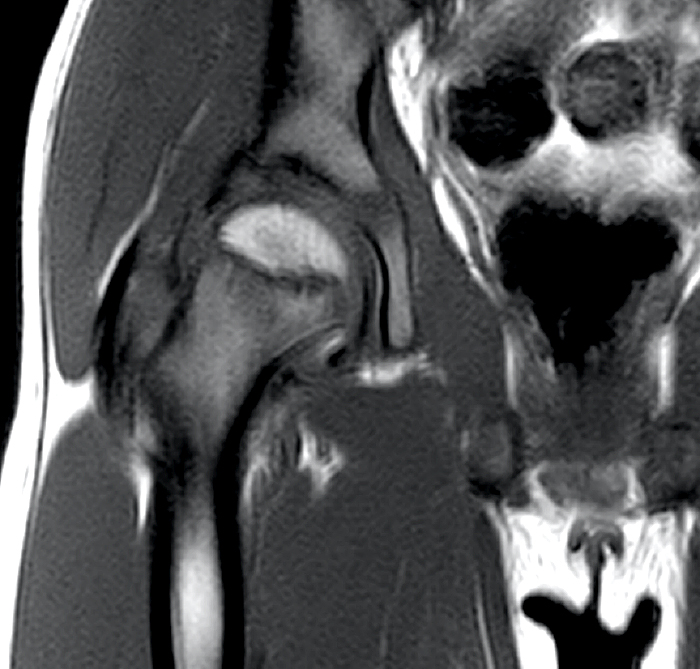
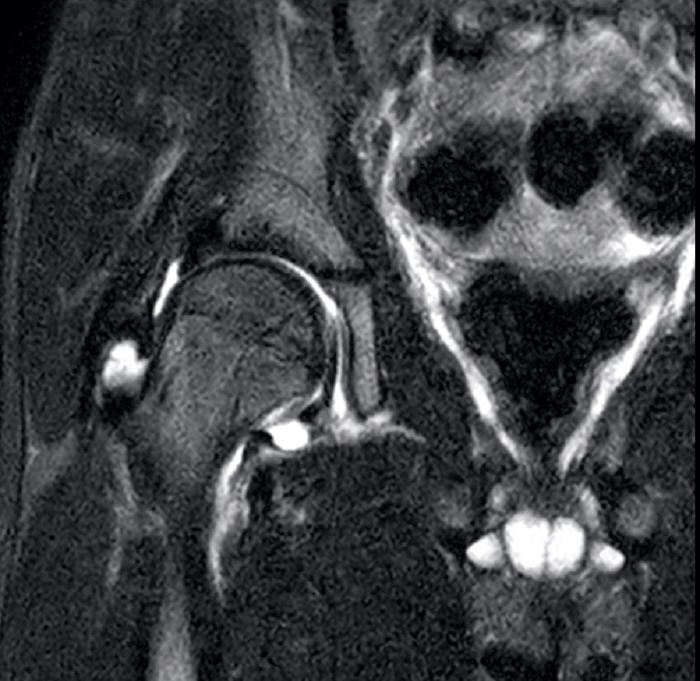
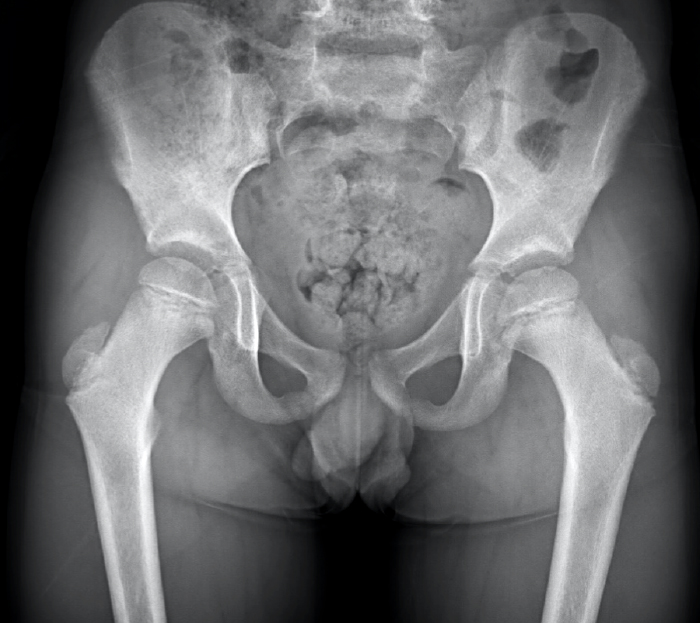
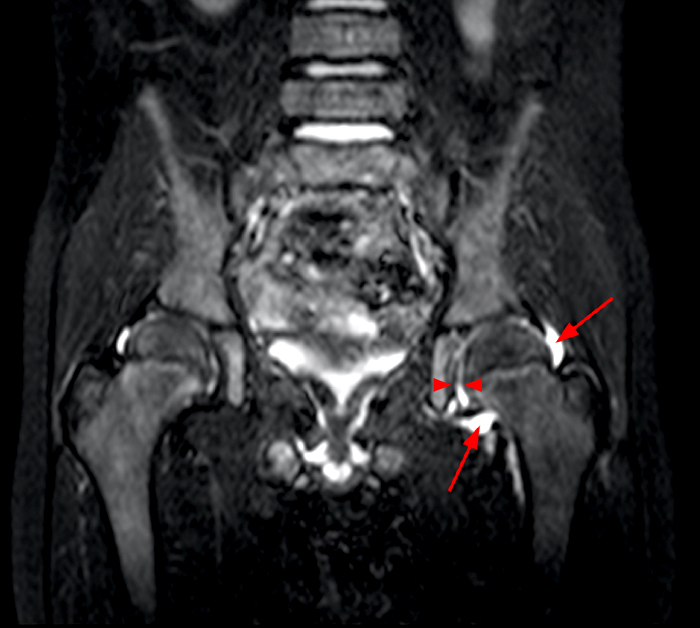
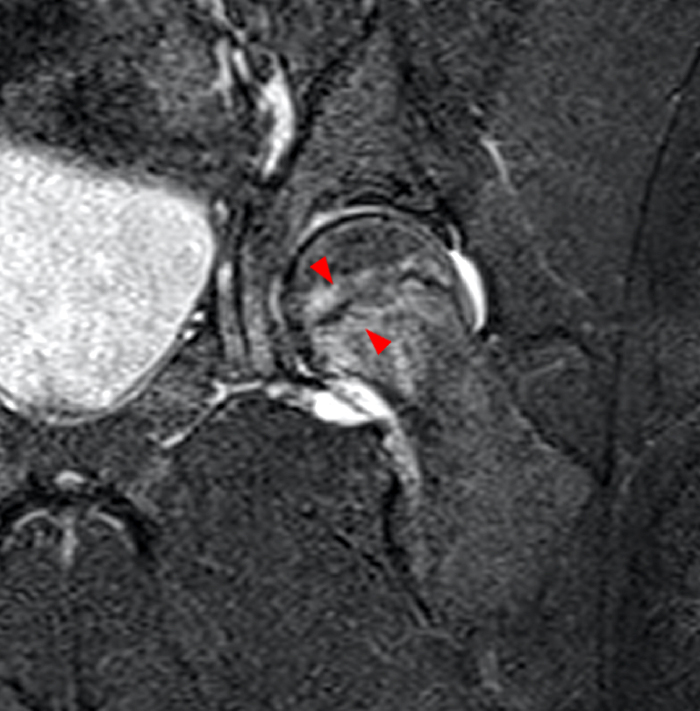
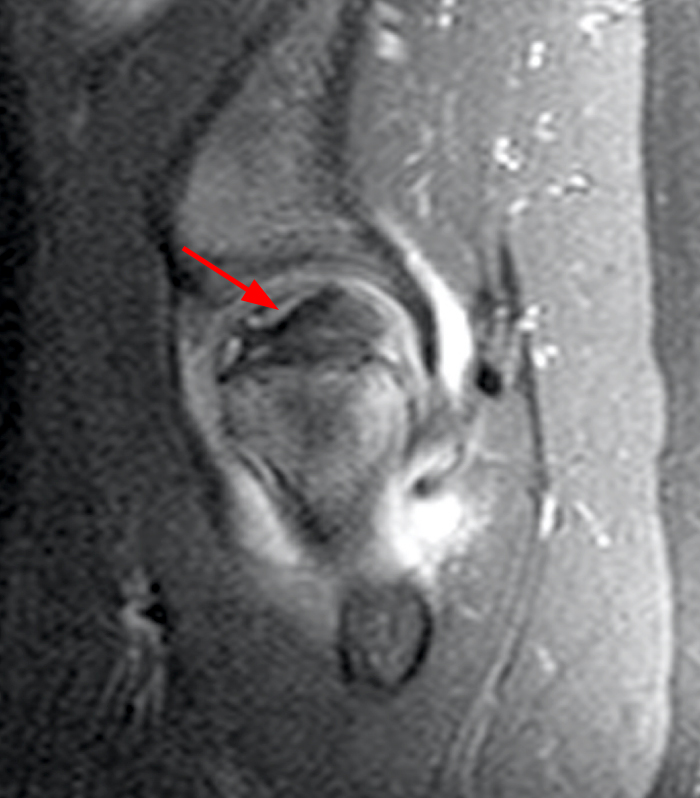
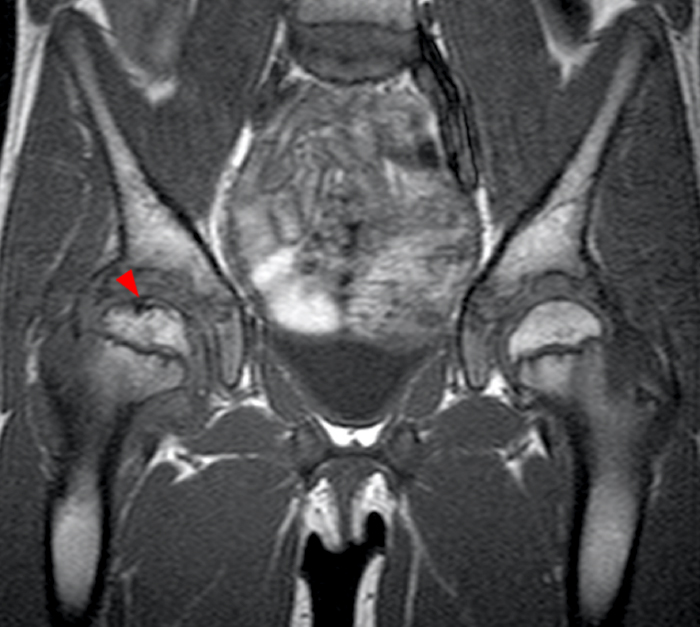
Clinical History: A 6-year-old boy presents to the orthopaedic surgeon with a one-week history of right groin pain with no known trauma or injury. Coronal T1 and fat-suppressed T2-weighted MR images (1A, 1B) through the right hip were performed, with x-ray correlate also provided (1C). What is the major finding and what is the likely diagnosis?
Diagnosis
Transient Synovitis of the Hip.
Introduction
Transient synovitis of the hip is a self-limiting disorder of unknown etiology in which the patient presents with acute hip pain, limp and possibly an inability to walk. The condition, first reported in 1892 by Lovett1, described a “transient or ephemeral form of hip disease that disappears in a few months instead of years.” Many labels for the condition have been coined since then including “simple transient coxitis,”2 termed to differentiate this condition from tuberculous infection of the hip, “transitory arthritis of the hip-joint,”3 “transitory synovitis of the hip-joint”4, “irritable hips,”5 “observation hip”6 and “toxic synovitis” to name a few. The thought of this condition being associated with upper respiratory infection was refuted in 1963 by Valderrama7 but many opposing studies have both supported and contradicted the theory that there is a link between this condition and antecedent viral infection. The importance in recognizing this condition is to differentiate this from the more serious septic arthritis.
Pathogenesis
The cause of transient synovitis remains unknown despite being one of the most common pediatric musculoskeletal disorders. The aspirate of fluid from affected joints has been shown to contain elevated levels of proteoglycan fragments as byproducts of breakdown of the underlying articular cartilage.8 There is a subsequent transient inflammatory reaction that ensues. The sampling of this fluid can help differentiate between Perthes disease and hip dislocations but does not allow differentiation from septic arthritis. Postulated associations include upper respiratory illness, gastrointestinal etiologies such as an antecedent bout of diarrhea, urinary tract infections, and trauma but none have been shown definitively to be the cause.
Epidemiology
Transient synovitis remains poorly understood and most often occurs in children. The typical age range of this disease occurs from 3 to 10 years old with a mean presentation at 4.7 years old.9 There have been case reports as young as 6 months old, but this is exceedingly rare and consideration for other etiologies should be considered in younger age brackets. Similarly, there have been reports of this condition in adults, but this is also rare. The condition overwhelmingly occurs in one joint with reports of contralateral asymptomatic effusions also possible.10 The condition is also more than twice as common in the male versus female population. There is a possibility of a relapse after the initial incident and the condition can occur bilaterally but is rare, occurring bilaterally 1-4% of the time.11
Clinical Presentation and Course
The patient can present with varying degrees of hip disability, ranging from no limp with nonspecific pain to mild limping to severe limping and inability to bear weight. Symptoms usually are confined to a single hip joint with examination revealing motion restriction, particularly during abduction and internal rotation; however, almost a third of patients have normal range of motion. Clinical examination performing the FABER (flexion, abduction, external rotation) maneuver often elicits the pain response on the affected side. Transient synovitis can occur in both febrile and afebrile patients. Laboratory evaluation demonstrating normal white blood cell count (WBC), sedimentation rate (ESR) and C-reactive protein with the presence of an effusion suggests transient synovitis for which short term clinical follow-up should be performed. However, febrile patients with effusion and elevated WBC, ESR, and CRP could represent either transient synovitis or septic arthritis and therefore hip aspiration is warranted.
Imaging
Radiograph evaluation of patients with transient synovitis are usually normal, but there can be occasional medial joint space widening. (Figure 3, 4) Ultrasound is a reliable mechanism of evaluating for joint effusion, but its utility is limited given its lack of bone assessment and false-negative results12 which can delay treatment. The best examination is MRI, which can aid in revealing additional abnormalities, thereby removing transient synovitis as a cause.
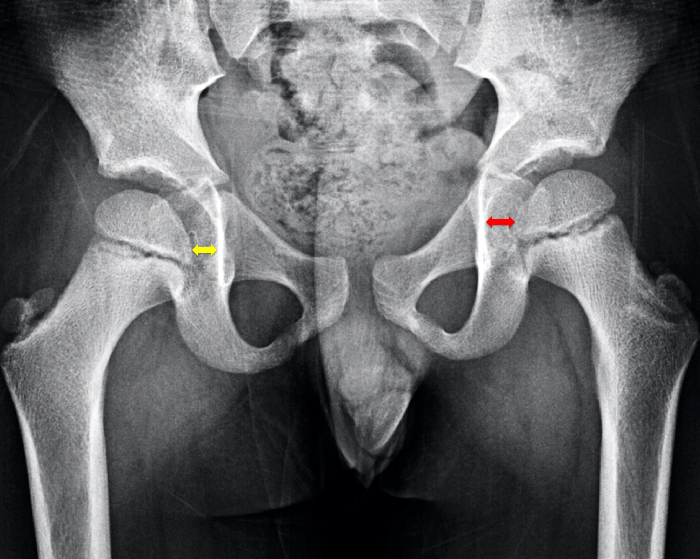
Figure 3:
6 year-old male presenting with intermittent left hip pain for a month. The AP pelvic radiograph demostrates medial hip compartment widening on the left (red arrow) compared to the contralateral right medial hip joint interval (yellow arrow). This patient was subsequently diagnosed with transient synovitis.
Figure 4:
5-year-old girl with 2-week history of limping and suspicion for osteomyelitis. A coronal fat suppressed T2-weighted image demonstrates a large left hip joint effusion (arrows) with medial joint space widening (arrowheads). There are no other findings, and this ultimately resolved on its own.
Additional MRI findings that can help point to other diagnoses include the presence of bone marrow edema, fracture, infiltrative osseous lesion, and medial slippage of the femoral head.
Differential Diagnoses
There are multiple other conditions in the pediatric hip that can present with hip joint effusions. The most important exclusion is that of infection. Septic arthritis is uncommon but can present with effusion and often imaging can help differentiate between the conditions. Findings can include periarticular bone marrow edema, bone marrow replacement on T1-weighted images, and surrounding areas of nonspecific soft tissue signal hyperintensity (Figure 5). In addition, decreased perfusion at the femoral epiphysis on fat-suppressed contrast enhanced T1 weighted images has been described.13 Later stage findings could also include erosive bony changes and fragmentation.
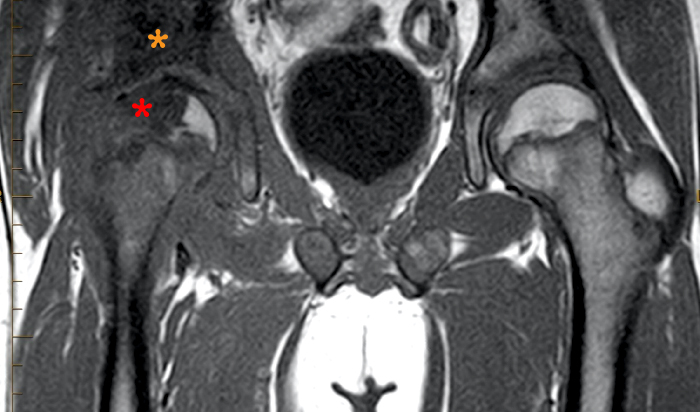
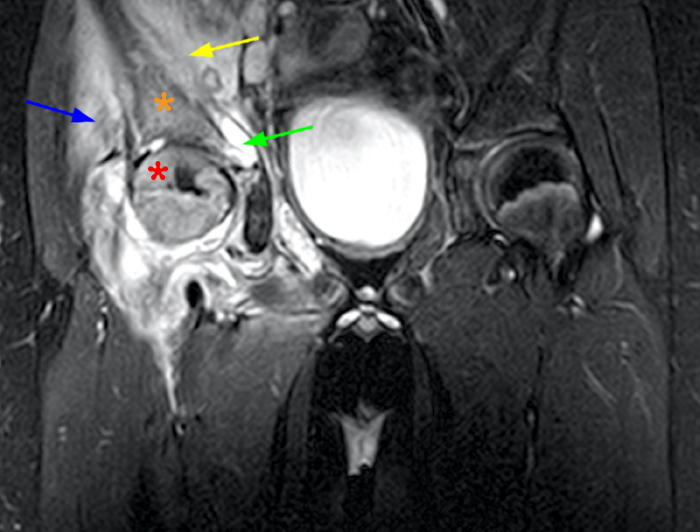
Figure 5:
Coronal T1 (5a) and fat suppressed T2-weighted images in a 9 year old male with confirmed septic arthritis and a large effusion. There is significant marrow signal abnormality with low signal replacement on T1 weighting corresponding to marrow edema on T2 weighting involving the right femoral epiphysis (red asterisk) and acetabulum (orange asterisk). There is abnormal edematous signal along the right gluteal musculature (blue arrow) and right iliacus muscle (yellow arrow) denoting myositis. Infectious iliopsoas bursitis creeping into the pelvis is also seen (green arrow).
The presence of a unilateral hip joint effusion can also be present with a slipped capital femoral epiphysis. This injury is described in detail in a prior Radsource Web Clinic and is most common in African-American and Hispanic children, particularly those with obesity. Typical age range for boys is from 10-17 years old and girls from 8-15 years old. Differentiating MRI signs include marrow edema, irregularity of the physis with widening (Figure 6) and medial slipping of the femoral head.
Figure 6:
12-year-old female with left hip pain and tightness after running injury with coronal T1-weighted (6a) and STIR (6b) images revealing joint effusion and characteristic irregular widening along the physis (red arrow) and paralleling marrow edema along both sides of the physeal plate (arrowheads).
Younger patients presenting with joint effusion also may have Legg-Calve-Perthes Disease, a painful osteochondrosis occurring in the hip, typically in males and Caucasians. This is described in more detail in a previous Web Clinic. X-rays can be normal or abnormal and MRI is more sensitive in the discovery of early disease. Observation of subchondral fracture, marrow edema, and necrosis of the femoral head can all point to this diagnosis and late stage findings including a small femoral ossification center, can also be seen (Figure 7).
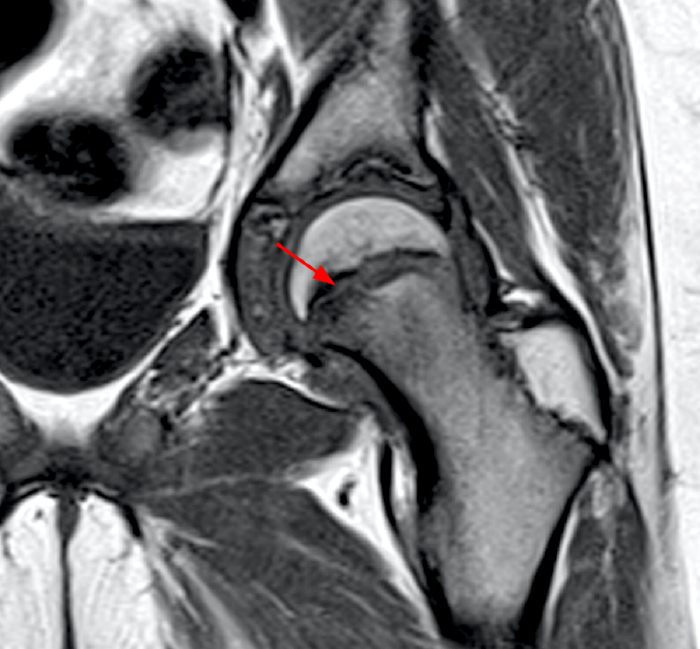
Figure 7:
8 year-old female with right hip pain presenting with joint effusion. A sagittal fat-suppressed proton density-weighted (7a) image of the right hip reveals a subchondral fracture (red arrow) along the anterosuperior weight bearing femoral head. The coronal T1 sequence (7b) reveals a smaller right femoral epiphysis and associated cortical flattening (arrowhead).
Treatment and Long Term Outcome
Patients with transient synovitis of the hip are usually instructed to stay home from school, refrain from athletic participation, and to rest. The physician will usually prescribe rest in a comfortable position, usually with the knee bent and externally rotated. Often anti-inflammatory medication such as NSAIDS or acetaminophen will be prescribed for pain relief. Hip aspiration in the setting of transient synovitis may have an immediate palliative effect14; however, it is of limited value as effusions are shown to recur after drainage. The self-limited course allows for resumption of normal activities usually within a week or two, and typically not longer than a month beyond the onset of symptoms. Transient synovitis tends to recur in approximately 20-25 percent of patients. There has been a higher reported frequency of associated coxa magna (asymptomatic overgrowth of the femoral head by 2mm or more) after a follow-up of one year in these patients15, which is thought to possibly play a part in development of hip osteoarthritis later in life.
Conclusion
Transient synovitis is an important diagnosis to consider in young children presenting with hip pain and effusion. This condition is self-limited and managed with conservative treatment. MR imaging is useful to help exclude other etiologies of pediatric hip pain.
References
- Lovett, R. a. (1892). A Transient or Ephemeral Form of Hip-Disease, with a Report of Cases. Boston Med Surg J, 127:161-163. ↩
- Todd, A. (1925). Discussion on the differential diagnosis of non-tuberculous coxitis in children and adolescents. Proc Roy Soc Med, 18: 31-6. ↩
- Butler, R. (1933). Transitory arthritis of the hip joint-in childhood: an investigation of the arthritis of the hip in ninety-seven children. BMJ, 1(3778): 951-4. ↩
- JG, F. (1936). Transitory synovitis of the hip joint in childhood,. JAMA, 107: 3-5. ↩
- Caravias, D. (1956). The signficance of the so-called “irritable hips” in children. . Arch Dis Child, 31: 415-8. ↩
- Monty, C. (1962). Prognosis of ‘observation hip’ in children. Arch Dis Child, 37: 539-42. ↩
- Valderrama, J. D. (1963). The “observation hip” syndrome and its late sequelae. J Bone Joint Surg Br, 45: 462-70. ↩
- Lohmander, L., Wingstrand , H., & Heinegard, D. (1988). Transient synovitis of the hip in the child: increased levels of proteoglycan fragments in joint fluid. J Orthop Res, 6(3): 420-4. ↩
- Caird MS, F. J. (2006). Factors distinguishing septic arthritis from transient synovitis in the hip in children. A prospective study. J Bone Joint Surg Am, 88(6):1251-7. ↩
- Ehrendorfer S, LeQuesne G, Penta M, Smith P, Cundy P. Bilateral synovitis in symptomatic unilateral transient synovitis of the hip: an ultrasonographic study in 56 children. Acta Orthop Scand. 1996 Apr;67(2):149-52. ↩
- Ehrendorfer S, LeQuesne G, Penta M, Smith P, Cundy P. Bilateral synovitis in symptomatic unilateral transient synovitis of the hip: an ultrasonographic study in 56 children. Acta Orthop Scand. 1996 Apr;67(2):149-52. ↩
- Zamzam MM. The role of ultrasound in differentiating septic arthritis from transient synovitis of the hip in children. J Pediatr Orthop B 2006; 15: 418–422. ↩
- Kwack K.-S., Cho, J. H., Lee, J. H., Cho, J. H., Oh, K. K., & Kim, S. Y. (2007) Septic Arthritis Versus Transient Synovitis of the Hip: Gadolinium-Enhanced MRI Finding of Decreased Perfusion at the Femoral Epiphysis. AJR, 189(2), 437-45. ↩
- Nouri A, Walmsley D, Pruszczynski B, Synder M. (2014) Transient Synovitis of the hip: a comprehensive review. Journal of Pediatric Orthopaedics B, (23), 32-36. ↩
- Kallio PE. (1988). Coxa magna following transient synovitis of the hip. Clin Orthop Relat Res. (228):49-56. ↩