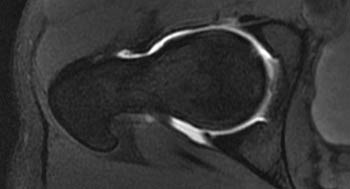
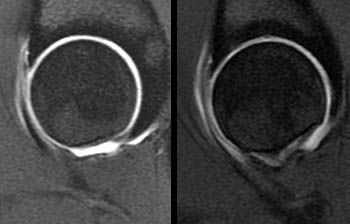
Clinical History: A 22 year old collegiate soccer player presents with bilateral groin pain. MR arthrography was performed bilaterally. What are the findings? What is your diagnosis?
Findings
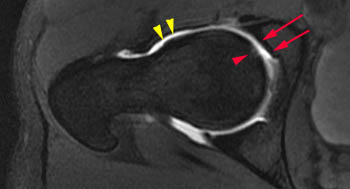
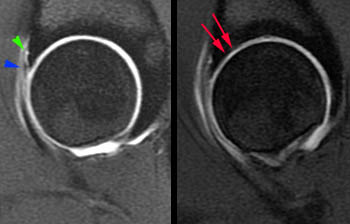
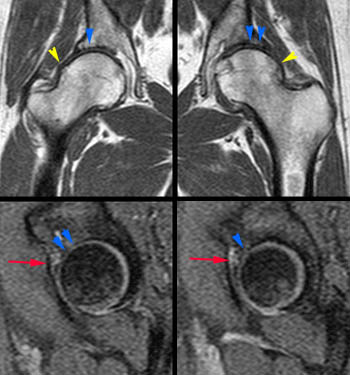
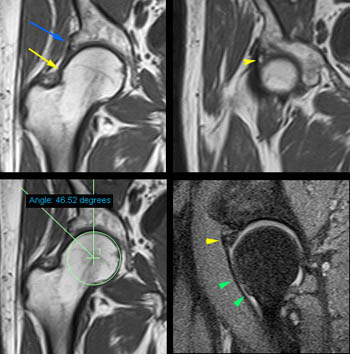
Figure 3:
A convex bump (yellow arrowheads) is present at the anterior femoral head-neck junction. An area of chondral loss (red arrows) is present on the acetabular side of the joint. Subtle subchondral degenerative changes (red arrowhead) are located on the corresponding femoral side of the joint.
Diagnosis
Cam-type femoroacetabular impingement with bilateral acetabular labral tears and chondral loss.
Discussion
Femoroacetabular impingement (FAI) is not a disease, but a common pathomechanical process which occurs when the proximal femur comes into contact with the acetabular rim. This can occur in normal hips in extreme flexion and internal rotation or may be from morphologic changes that cause premature contact between the structures. Chronic microtrauma from recurrent impingement can lead to acetabular labral tears and breakdown of the articular cartilage, subsequently resulting in osteoarthritis. FAI from radiographically subtle morphologic abnormalities has been suggested to be the underlying cause of most cases of idiopathic or primary osteoarthritis9. Timely diagnosis is therefore important. Surgical intervention can give immediate pain relief and, if it is performed before cartilage breakdown has begun, it may prevent later cartilage loss and development of osteoarthritis. FAI can occur from abnormal morphology on either the femoral or acetabular side of the joint.
Cam-type FAI
In order for the hip to flex normally without impingement, the femoral head needs to be round and there must be a suitable space at the femoral head-neck junction (aka the femoral waist). If instead the femoral head is aspherical or there is not a suitable femoral head-neck offset, then this area of the proximal femur will abnormally pressurize the cartilage at the acetabular rim during hip flexion, causing chondral and subsequent labral damage. A mechanical cam, such as part of a combustion engine camshaft, is an aspherical structure that rotates and thereby lifts an adjacent structure, hence the term “cam-type FAI.”
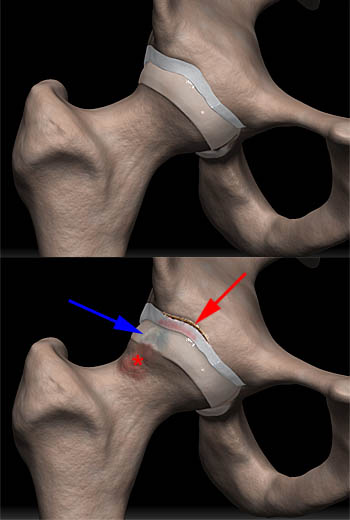
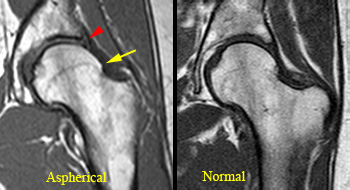
Figure 5:
Cam-type FAI. The normal hip above has enough space at the femoral waist to accommodate the acetabular rim throughout the normal range of motion. The hip below has localized osseous protuberance (asterisk) and an aspherical humeral head (blue arrow) that impinge on the superolateral portion of the acetabulum during flexion and internal rotation, injuring the hyaline cartilage and adjacent labrum, resulting in labral detachment (red arrow).
In a hip with a cam lesion, rotation of the femoral head brings a broader radius into the acetabular margin, typically anterosuperiorly, compressing the hyaline cartilage at this site and pushing it medially. This initially forms a wavy appearance to the cartilage with separation from the underlying bone, followed by a chondral flap tear, similar to that of a carpet that has been pushed from the side, a “carpet lesion.” Subsequent to chondral injury, pressure at this site also causes the labrum to tear or detach from the hyaline cartilage margin. With labral injury and further progression of chondral damage, the hip may then later develop instability and femoral head cartilage damage.
We have long known that patients with a history of slipped capital femoral epiphysis or Perthes disease that have developed a pistol grip deformity are prone to developing secondary osteoarthritis, but it was not until more recently that FAI has been recognized as the underlying mechanism. Most commonly, an aspherical femoral head or a bump at the femoral head-neck junction creates cam-type FAI. There are several underlying possible causes (Table 1).
Table 1. Causes of Cam Lesions1
- Idiopathic
- Developmental
- Nonspherical femoral head
- Coxa vara
- Traumatic
- Malunited femoral neck fracture
- Post-traumatic retroversion of the femoral head
- Childhood orthopaedic condition
- Perthes disease
- Slipped capital femoral epiphysis (SCFE)
- Iatrogenic
- Femoral osteotomy
Pincer-type FAI
Since a prominent acetabular rim pressing down on the proximal femur resembles the action of a pincer, this has been termed “pincer-type” impingement. An overly prominent acetabular rim is reflected by the presence of acetabular overcoverage of the femoral head.
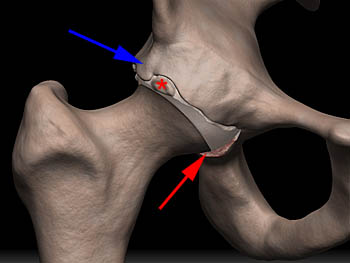
Figure 6:
Pincer-type impingement. With a pincer lesion, the acetabular rim is prominent (blue arrow) often with os acetabuli (asterisk) and focally impacts the femur during flexion and internal rotation, resulting in labral degeneration and tearing. Cartilage damage occurs after the labral injury, initially limited to a thin strip anterosuperiorly, later involving larger areas posteroinferiorly (red arrow) as a "contrecoup lesion."
There are several possible underlying causes of pincer lesions, developmental and acquired, and the abnormality may be local (e.g. acetabular retroversion) or global (e.g. coxa profunda) (Table 2). Labral ossification and osseous proliferation are most frequently seen, which are likely chronic changes secondary to prior labral injury.
Table 2. Causes of Pincer Lesions1
- Idiopathic
- Developmental
- Retroverted acetabulum
- Coxa profunda
- Os acetabuli
- Protrusio acetabuli
- Chronic residual dysplasia of the acetabulum
- Traumatic
- Post-traumatic deformity of the acetabulum
- Iatrogenic
- Overcorrection of retroversion in dysplastic hips
As with cam-type FAI, the initial injury site is typically anterosuperior in position from hip flexion and internal rotation. However, with pincer-type impingement, the initial injury is to the labrum, which develops myxoid degeneration and tearing. To a lesser degree there may be damage to a thin adjacent strip of acetabular cartilage. Later in this process, when dystrophic ossification has developed in the injured labrum, the prominent acetabular rim acts as fulcrum, leveraging the femoral head posteroinferiorly and causing more significant chondral injury at that site.
Mixed-type FAI
Most cases of FAI are a combination of both cam and pincer-type mechanisms, with cam-type usually predominating. It is possible that the femoral head-neck junction bump found in cam-type impingement may be initiated by microtrauma from pincer-type impingement at this site. Once formed, both mechanisms may have a role in bump enlargement, as well as development of cystic changes at this site. Additionally, if more advanced osteoarthritis develops, marginal osteophytes at the acetabular rim or ossification of the damaged labrum become pincer lesions and remodeling at the femoral head-neck junction creates an aspherical femoral head that acts as a cam lesion. However, once there is advanced osteoarthritis, noting the underlying FAI biomechanics is probably a moot point, since correcting them has not been shown to reverse or slow disease progression.
Clinical Findings
Patients with FAI typically present with deep intermittent groin discomfort during or after activities involving repetitive or persistent hip flexion. Groin pain in an athlete is a nonspecific complaint with a large differential diagnosis, including adductor strain, iliopsoas tendinitis, and stress fracture. With FAI, limitation of the range of motion develops long before the onset of pain but may go unnoticed. Additionally mechanical symptoms may be present if there is an associated labral tear. FAI is frequently bilateral but asynchronous, such that presenting symptoms are often unilateral.
The typical patient with cam-type impingement is a young active male in his 20s or 30s. Pincer-type impingement typically presents a decade later in women engaged in activities such as yoga or aerobics. Nevertheless, FAI can be found in other age groups and one recent study found pincer lesions to be very common among both sexes12.
Clinical examination can reveal an “anterior impingement sign,” which is present when pain is elicited with forced internal rotation while the hip is in 90 degree flexion. In more extreme cases, the bone morphology forces the hip to externally rotate during hip flexion, a positive “Drehmann’s sign.” A “posterior impingement sign” (associated with uncommon posterior pincer lesions) is positive when the hip is placed in hyperextension and forced external rotation elicits pain.
Imaging Assessment
If clinical features are suggestive of FAI, radiographs may reveal the underlying femoral and/or acetabular structural abnormality. The AP view may show a typical “pistol grip” deformity (lack of a normal concavity to the femoral waist), coxa vara, an aspherical femoral head, or a femoral head-neck junction cyst. An additional helpful finding that reflects an aspherical femoral head is a “horizontal growth plate sign” (growth plate extending lateral to a best-fit circle of the femoral head)22. A characteristic femoral head-neck junction bump or aspherical femoral head may be visible on the lateral view and alpha angle and head-neck offset ratio can be measured. However, since these structural abnormalities primarily occur superolaterally, standard AP and lateral views may miss them. Some advocate a specially obliqued view (modified Dunn view) for greater sensitivity15.
Acetabular prominence with femoral overcoverage may also be apparent, confirmed on AP radiographs by parameters such as lateral center edge angle >39° (increased femoral head coverage), acetabular index of elevation =0 (aka Tönnis angle; diminished slope of acetabular roof or “sourcil”), or femoral head extrusion index ~0 (diminished amount of femoral head extruding beyond the acetabular margin)22. Acetabular retroversion can be detected with the “cross-over sign” and posterior wall deficiency with the “posterior wall sign.” These assessments are subject to pelvic tilt/positioning, though compensating measurements and calculations can be made. Occasionally, a damaged acetabular labrum may develop ossification. If this becomes large enough it may act as a pincer lesion. If detached, it may be seen as an os acetabuli. Potential pincer lesion mimics include DISH and ankylosing spondylitis, which do not produce impingement. Detailed reviews of the radiographic assessments have been published in the orthopaedic4 and radiology22 literature. However, some of the same authors later determined that in practical use, the reliability of these radiographic measurements is limited5.
MRI Evaluation
In addition to demonstrating the osseous structural abnormalities visible on radiographs as above described, including cam-type deformities, acetabular overcoverage, or acetabular retroversion, MRI (or MR arthrography) allows better visualization of anterosuperior lesions and provides an important assessment for labral tears and hyaline cartilage loss.
MRI evaluation is directed to both femoral and acetabular causes of impingement. The proximal femur must be scrutinized in multiple imaging planes with special attention to the anterior and anterosuperior aspects of the femoral head-neck junction.
One or more features (which frequently coexist) are sought for identifying a cam-type deformity:
- focal bony protuberance or bump at the anterior or anterosuperior aspect of the femoral head-neck junction
- aspherical femoral head at the femoral head-neck junction (such as a flattened lateral femoral head margin)
- diminished femoral head-neck offset (aka “femoral waist deficiency,” or “pistol grip deformity” if seen on coronal images)
Additionally, small cysts at the femoral head-neck junction are a useful indicator of FAI. They have been found in 33% of patients with FAI13 and there is a high likelihood of a causal relationship. Since these may contain fibrous or gelatinous material, some refer to them as fibrocysts. A study suggesting that the cysts may not be related to FAI11 was limited in that the only criterion for cam-type FAI was a pistol grip deformity on an AP view. The study thereby had a low sensitivity for an anterior or anterosuperior asphericity or a femoral head-neck bump, the structural abnormality that is most often associated with the cysts. Another study confirmed that radiographs are not adequately sensitive for asphericity of the femoral head7.
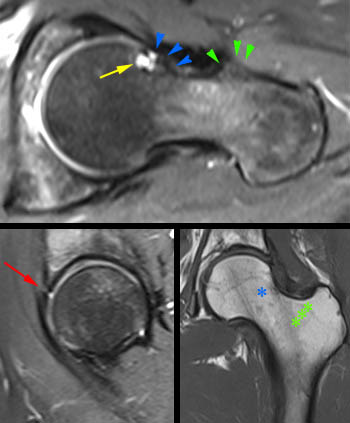
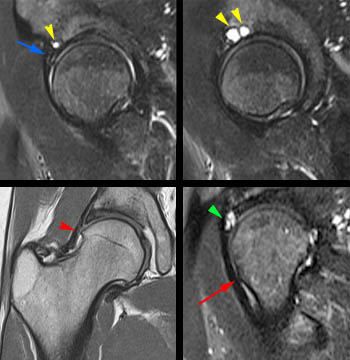
Figure 7:
Femoral head-neck junction bump (cam-type FAI) in a 31yo female runner with left groin pain, popping, and catching. The oblique axial PD FS (fat-suppressed proton density) image demonstrates a bump (blue arrowheads) at the anterior aspect of the femoral head-neck junction that is characteristic of cam-type FAI. Bumps are occasionally accompanied by cystic changes (yellow arrow) that are often easier to spot than the bump itself. Since the abnormalities are anterosuperior in position, the coronal images may be deceivingly normal in appearance, such as in this case. A small anterosuperior labral tear was also present (red arrow), best seen on the sagittal PD FS sequence. Note that the protuberance located more laterally (green arrowheads) is a normal anatomic structure, the femoral tubercle, of variable size, which may be mistaken for a cam lesion. Corresponding positions of the femoral head-neck bump and cysts (blue asterisk) and the femoral tubercle (green asterisks) are marked on the coronal image.
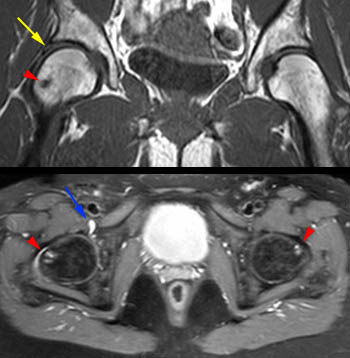
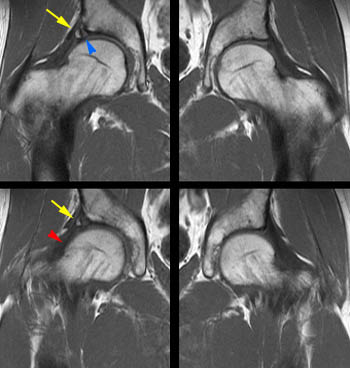
Figure 8:
Cam-type FAI in a 43 yo female with right hip pain for 3 months. Bilateral pistol grip deformities and an anterosuperior right acetabular labral tear (yellow arrow) were well seen on coronal images. Femoral head-neck junction bumps and cysts (arrowheads) were better seen on the axial images, particularly while scrolling through the images as a stack, due to their anterosuperior positions. A small right hip effusion was present with mild distention of the iliopsoas bursa (blue arrow).
Figure 9:
Cam-type FAI and labral tear in a 40yo male with left hip pain of 3 days duration. Subtle asphericity of the femoral head (arrow). The physis extends beyond the circular area of the femoral head, helping to confirm the abnormal shape. Normal hip from a different patient for comparison. A labral tear is also present (red arrowhead). Both femoral heads were aspherical and bilateral labral tears were also present, larger and more prominent on the left.
Figure 10:
Cam-type FAI and premature osteoarthritis in a 44yo male with worsening left hip pain for 1 year. The femoral heads are aspherical bilaterally with flattening and enlargement at the lateral femoral head margins (yellow arrowheads). Note that the physes extend beyond circular portions of femoral heads. Premature osteoarthritis has developed with advanced chondral loss bilaterally, left worse than right (blue arrowheads). Bilateral anterosuperior acetabular labral tears were best seen on the sagittal PD FS views (red arrows).
Figure 11:
Irregular labral tear, large paralabral cyst and cam-type FAI in a 67yo male with right hip, leg, and buttock pain and difficulty walking. A large paralabral cyst (blue arrowheads) stands out on coronal T1 (upper left), axial PD FS (upper and lower right), and sagittal PD FS (lower left) images, projecting superiorly adjacent to the iliac wing. Increased T1 signal in the cyst fluid indicates proteinaceous or hemorrhagic content. The underlying irregular tear (red arrows) involves anterosuperior, superior, and posterosuperior portions of the labrum. Paralabral cysts are reportedly not common in patients with cam-type FAI. This patient however had a pistol grip (cam-type) deformity. Pistol grip deformity and a labral tear were also present at the left hip (not shown).
With cam-type impingement, the femoral neck has a below normal offset from the femoral head and demonstrates a diminished or lost transition (“femoral waist deficiency”). Several types of MRI measurements have been developed to confirm and quantify these findings. The alpha angle is the most widely used (abnormal > 55 degrees), indicating the angle at which the femoral head departs from its normal spherical outline. Femoral head-neck offset distance (abnormal < 8 mm) and associated ratios can also be used to demonstrate a cam-type structural abnormality.
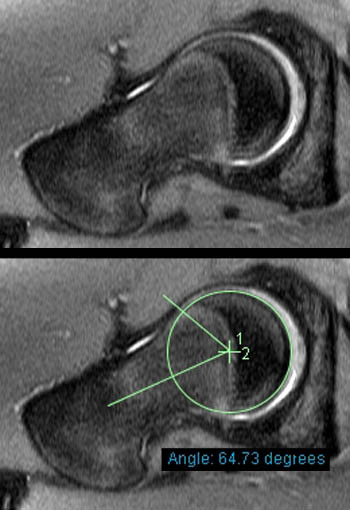
Figure 12:
14 year old male with cam-type morphology. The patient's presenting symptoms were from an avulsion injury to the anterior superior iliac spine (not shown). Abnormal alpha angle measurement of 65 degrees (normal < 55 degrees) on an oblique axial PD FS image. Note that the proper positioning of the circle does not include the overlying hyaline cartilage16.
Measurement of an abnormal alpha angle from an oblique axial image along the femoral neck16 has generally been the standard for confirmation of cam-type lesions. However, a more recent study comparing radial slices to standard oblique axial images showed a significant discrepancy in 54% of subjects, where the alpha angle was normal (less than 55°) on the conventional oblique axial plane images but positive for cam-lesion (55° or greater) on the radial plane images19. This is understandable since an anterosuperiorly positioned femoral head-neck junction bump will often be just above the image plane typically utilized for alpha angle calculation. It may in part explain why a study comparing subjective assessments of alpha angles did not correlate well with measured alpha angles except in cases where an obvious bone deformity was present17. An additional source of measurement error is the placement of the circle, which should be along the subchondral bone cortex, excluding the femoral head cartilage. Slight variations of circle radius or placement can cause significant differences in measured alpha angles. A less frequent problem with the alpha angle measurement can be the definition of the femoral neck axis. Nötzli defined it as a line between the center of the femoral head and the middle of the narrowest portion of the femoral neck. However, in cases of femoral head retroversion such as from SCFE, this method will yield an incorrect femoral neck axis and an erroneously undervalued alpha angle. In cases where the femoral head and neck are not aligned, a better approach appears to be to draw this line parallel to the visible neck axis. See diagrams at http://www.boneandjoint.org.uk/content/focus/overview-femoroacetabular-impingement8.
While radial imaging planes reconstructed from a high resolution 3D gradient echo sequence would be the most ideal for visualizing and measuring predominantly anterosuperior abnormalities, this method may not be available on many MRI units due to technical limitations.
The acetabulum is assessed for pincer-type lesions related to abnormal acetabular depth or version as well as the presence of labral ossification or bony overgrowth at the acetabular rim. Femoral head overcoverage may be localized from retroversion, localized hypertrophy, osteophytes, or an ossified labrum, or it may be global from coxa profunda or protrusio acetabuli. The lateral center edge angle (LCE) appears to be a better measure of overcoverage than the extrusion index, since LCE will not be affected by enlargement of the lateral portion of the femoral head when there is a concomitant cam lesion.
Figure 14:
Os acetabuli and mixed-type FAI. This 79yo male with a history of right hip pain for 1 month has features of both pincer and cam-type FAI. Femoral head asphericity (yellow arrow), irregular anterosuperior bump (green arrowheads), os acetabuli (yellow arrowhead) and hypertrophic acetabular rim (blue arrow). The os acetabuli in this case is likely from detachment of an area of heterotopic ossification along the anterosuperior acetabular rim, possibly from the repeated microtrauma of impingement. The acetabular hyaline cartilage is markedly thinned beneath the os acetabuli. All of the findings were present bilaterally, though slightly worse on the right. Note that there is acetabular overcoverage (increased LCE angle >39 degrees) despite the aspherical portion of the femoral head remaining uncovered.
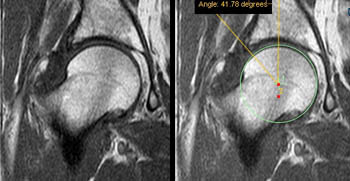
Figure 15:
Unilateral os acetabuli and aspherical femoral head, suggestive of mixed type FAI, in a 42 yo male karate enthusiast. The os acetabuli (arrows) is located along the anterior half of the lateral acetabular margin. Localized chondral loss (blue arrowhead) is seen adjacent to the os acetabuli. The right femoral head asphericity (red arrowhead) was located anterosuperiorly, most notable on the more anterior image, where a "horizontal growth plate sign" is also apparent.
Acetabular depth can be measured between the center of the femoral head and a line connecting the anterior and posterior acetabular rims. One study showed an average depth of 5mm with pincer-type FAI and 1mm with cam-type18. Deficient acetabular coverage (lateral center edge angle < 25 degrees) limited to the anterosuperior portion may instead indicate the presence of developmental dysplasia of the hip (DDH). Differentiating these conditions is important and other features may also be helpful in this regard. Paralabral cysts and labral enlargement from myxoid degeneration are reportedly more common in DDH than with FAI14. Anterosuperior femoral neck cysts are not present in DDH13. Hypertrophy of the pulvinar and of the ligamentum teres are also features of DDH. In both conditions, labral tears are primarily anterosuperior in position.
Labral tears are important abnormalities that can lead to hip instability and faster hyaline cartilage breakdown. They are increased in patients with FAI, particularly anterosuperiorly, with both cam and pincer types of FAI, and are usually best seen on sagittal or oblique sagittal imaging sequences, followed by coronal images. A useful indicator for a labral tear is that of a paralabral cyst. This is frequently more conspicuous than the tear itself and may be very large, very small, or nonexistent. They are usually in the soft tissues adjacent to the labrum, frequently projecting superiorly. They also frequently have an intraosseous component, which may be difficult to distinguish from subchondral cystic changes associated with hyaline cartilage damage. A potential false positive for labral tears is a sublabral sulcus or recess, but these occur posteroinferiorly6 and anteroinferiorly21, away from the usual anterosuperior labral pathology.
Figure 16:
39 year old female with bilateral primarily cam-type FAI and labral tears. Sagittal fat-suppressed T2-weighted images and a coronal proton density-weighted image demonstrate a cleavage type anterosuperior labral tear (blue arrow), an associated paralabral cyst anteriorly (green arrowhead), and anterosuperior acetabular subchondral cysts (yellow arrowheads). The subchondral cysts may be from overlying chondral fissures that are not directly visualized or may represent intraosseous extension of the paralabral cysts. Flattening/asphericity at the femoral head periphery (red arrowhead) visible on coronal images and a small anterosuperior bump (red arrow) that was best seen on the sagittal sequence, are compatible with cam-type deformities. All of the findings were present bilaterally.
Chondral damage occurs first on the acetabular side of the joint with FAI, only involving the femoral head late in the process. It is located anterosuperiorly with cam-type FAI, due to local compression by the cam, beginning with focal delamination (visible arthroscopically as a “wave sign“) and progressing to a chondral flap tear (“carpet lesion“). With pincer-type FAI, chondral injury is more common posteroinferiorly18 or diffusely3. MR arthrography can allow better delineation of open chondral defects than standard MRI, though intraarticular contrast will not outline early delamination lesions. These must be assessed on T2 weighted images, but remain very difficult to identify. A potential false positive pitfall for an acetabular chondral defect is a supra-acetabular fossa, which can be striking, but has a characteristic location, no associated marrow edema, and is often bilateral.
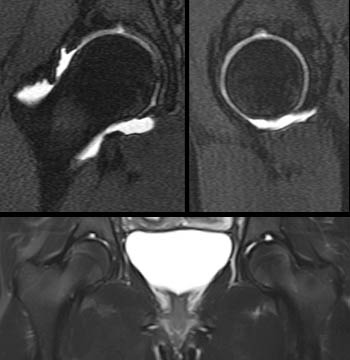
Figure 17:
Supra-acetabular fossa, an incidental finding that mimics chondral injury. These have a characteristic 12 o'clock position and are often bilateral with some asymmetry. Upper row coronal and sagittal MR arthrogram images show an incidental small unilateral supra-acetabular fossa in a patient with a cam deformity. A coronal fat-suppressed proton density-weighted image of a different patient shows bilateral prominent supra-acetabular fossae.
Treatment
Since FAI occurs at extremes of the range of motion, behavior modification may be enough to avoid pain and subsequent joint injury. For those whose activities require repeated extreme hip flexion, such as serious athletes or carpet layers, surgery is an option. Surgical treatment has shown good results in midterm follow-up for patients that do not have significant chondral loss prior to surgery2. Open and arthroscopic techniques have been utilized and shown to be equally effective1.
For cam lesions, osteoplasty/cheilectomy is performed to remove excess bone and restore the femoral head-neck offset23. For pincer lesions, overcoverage can be reduced focally by bone removal or if acetabular retroversion is present a periacetabular osteotomy can be performed to reorient the entire acetabulum. Chondral lesions are debrided and labral tears repaired.
In most cases, both cam and pincer type lesions are present and require treatment. However, caution must be exercised to not overcorrect a pincer lesion and create instability from a surgically induced acetabular dysplasia.
Additional Words of Caution
Since many of the morphologic findings of FAI can be found in asymptomatic individuals, it is possible that some of the abnormalities reflect anatomic variations that may predispose them to FAI but do not indicate its presence. For example, cam-type deformities have been found in as many as one in four asymptomatic young men and in half of men with decreased internal rotation20. Pistol grip deformities have been found in one in five males and the crossover sign in half of men and women12. Additionally, there are differences in opinion about the significance of an ossicle adjacent to the acetabular rim, some considering it evidence of a pincer lesion and others an incidental normal developmental variant. A diagnosis of FAI should not be based on imaging findings alone. Correlation must be made with the clinical findings.
Additionally, the natural course of osteoarthritis is not entirely clear. While it is likely that early intervention prevents or delays development of osteoarthritis in the long term, a conclusive study is difficult to conduct due to the need for sham surgery controls. A recent retrospective study showed that 82% of patients with FAI that were asymptomatic at the time of diagnosis remained free of osteoarthritis for a mean of 18.5 years follow-up without surgery10. Only the presence of idiopathic osteoarthritis in the contralateral hip was predictive of the development of osteoarthritis on the asymptomatic side. This also reemphasizes that prophylactic surgery should not be undertaken in the absence of symptoms.
Conclusions
- FAI is an important diagnosis to make and is currently underdiagnosed
- diagnosis can lead to appropriate behavior modification or intervention and pain relief
- early intervention may prevent later development of osteoarthritis
- FAI can be diagnosed by characteristic imaging findings in the appropriate clinical setting
- cam-type FAI is characterized by an aspherical femoral head or diminished femoral head-neck offset
- pincer-type FAI is characterized by a prominent acetabular rim
- most cases have components of both, though cam-type typically predominates
- both types of FAI are associated with anterosuperior labral tears
- both types of FAI are associated with chondral damage, typically anterosuperior in cam-type FAI and posteroinferior or diffuse in pincer-type FAI
- alpha angle measurements on oblique axial MRI images and assessments on radiographs have limited sensitivity, since FAI structural abnormalities are primarily anterosuperior in position
- since there is a high prevalence of FAI-type morphologies in asymptomatic individuals, the diagnosis of FAI should not be made in the absence of clinical symptoms
References
1 Banerjee P and Mclean CR. Femoroacetabular impingement: a review of diagnosis and management. Curr Rev Musculoskelet Med. 2011 March; 4(1): 23-32.
2 Beck M, Leunig M, Parvizi J, Boutier V, Wyss D, Ganz R. Anterior femoroacetabular impingement. Part II. Midterm results of surgical treatment. Clin Orthop, 2004; 418(67-73).
3 Bittersohl B, Steppacher S, Haamberg T, Kim YJ, Werlen S, Beck M, Siebenrock KA, Mamisch TC. Cartilage damage in femoroacetabular impingement (FAI): preliminary results on comparison of standard diagnostic vs delayed gadolinium-enhanced magnetic resonance imaging of cartilage (dGEMRIC). Osteoarthritis Cartilage. 2009 Oct;17(10):1297-306. Epub 2009 May 3.
4 Clohisy JC, Carlisle JC, Beaulé PE, Kim YJ, Trousdale RT, Sierra RJ, Leunig M, Schoenecker PL, Millis MB. A systematic approach to the plain radiographic evaluation of the young adult hip. J Bone Joint Surg Am. 2008 Nov;90 Suppl 4:47-66.
5 Clohisy JC, Carlisle JC, Trousdale R, Kim YJ, Beaulé PE, Morgan P, Steger-May K, Schoenecker PL, Millis M. Radiographic evaluation of the hip has limited reliability. Clin Orthop Relat Res. 2009 Mar;467(3):666-75. Epub 2008 Dec 2.
6 Dinauer PA, Murphy KP, Carroll JF. Sublabral sulcus at the posteroinferior acetabulum: a potential pitfall in MR arthrography diagnosis of acetabular labral tears. AJR Am J Roentgenol 2004; 183: 1745-1753.
7 Dudda M, Albers C, Mamisch TC, Werlen S, Beck M. Do normal radiographs exclude asphericity of the femoral head-neck junction? Clin Orthop Relat Res. 2009 Mar;467(3):651-9. Epub 2008 Nov 20.
8 Fern ED, Norton MR. Focus On Femoroacetabular Impingement. The Journal of Bone and Joint Surgery. Epub 2010.
9 Ganz R, Leunig M, Leunig-Ganz K, Harris WH. The Etiology of Osteoarthritis of the Hip, An Integrated Mechanical Concept. Clin Orthop Relat Res. 2008 February; 466(2): 264-272.
10 Hartofilakidis G., Bardakos N. V., Babis G. C., and. Georgiades G. An examination of the association between different morphotypes of femoroacetabular impingement in asymptomatic subjects and the development of osteoarthritis of the hip. J Bone Joint Surg Br, May 1, 2011; 93-B(5): 580 – 586.
11 Kim JA, Park JS, Jin W, Ryu K. Herniation pits in the femoral neck: a radiographic indicator of femoroacetabular impingement? Skeletal Radiol. 2011 Feb;40(2):167-72. Epub 2010 May 22.
12 Laborie LB, Lehmann TG, Engesæter IØ, Eastwood DM, Engesæter LB, Rosendahl K. Prevalence of Radiographic Findings Thought to Be Associated with Femoroacetabular Impingement in a Population-based Cohort of 2081 Healthy Young Adults. Radiology. August 1, 2011 260:494-502
13 Leunig M, Beck M, Kalhor M, Kim YJ, Werlen S, Ganz R. Fibrocystic changes at anterosuperior femoral neck: prevalence in hips with femoroacetabular impingement. Radiology. 2005 Jul;236(1):237-46.
14 Leunig M, Podeszwa D, Beck M, Werlen S, Ganz R. Magnetic resonance arthrography of labral disorders in hips with dysplasia and impingement. Clin Orthop. 2004; 418:74-80.
15 Meyer DC, Beck M, Ellis T, Ganz R, Leunig M. Comparison of six radiographic projections to assess femoral head/neck asphericity. Clin Orthop Relat Res. 2006 Apr;445:181-5.
16 Nötzli HP, Wyss TF, Stoecklin CH, Schmid MR, Treiber K, Hodler J. The contour of the femoral head-neck junction as a predictor for the risk of anterior impingement. J Bone Joint Surg Br. 2002 May;84(4):556-60.
17 Nouh MR, Schweitzer ME, Rybak L, Cohen J. Femoroacetabular impingement: can the alpha angle be estimated? Am J Roentgenol. 2008;190:1260-2.
18 Pfirrmann CW, Mengiardi B, Dora C, Kalberer F, Zanetti M, Hodler J. Cam and Pincer Femoroacetabular Impingement: Characteristic MR Arthrographic Findings in 50 Patients Radiology. September 2006, 240, 778-785.
19 Rakhra KS, Sheikh AM, Allen D, Beaulé P. Comparison of MRI alpha angle measurement planes in femoroacetabular impingement. Clin Orthop 2009;467:660-5
20 Reichenbach S, Jüni P, Werlen S, Nüesch E, Pfirrmann CW, Trelle S, Odermatt A, Hofstetter W, Ganz R, Leunig M. Prevalence of cam-type deformity on hip magnetic resonance imaging in young males: a cross-sectional study. Arthritis Care Res (Hoboken). 2010 Sep;62(9):1319-27.
21 Studler U, Kalberer F, Leunig M, Zanetti M, Hodler J, Dora C, Pfirrmann CW. MR arthrography of the hip: differentiation between an anterior sublabral recess as a normal variant and a labral tear. Radiology 2008;249 : 947-954
22 Tannast M, Siebenrock KA, Anderson SE. Femoroacetabular impingement: radiographic diagnosis-what the radiologist should know. AJR Am J Roentgenol 2007;188(6):1540-1552.
23 Vaughn ZD, Safran MR. Arthroscopic femoral osteoplasty/cheilectomy for cam-type femoroacetabular impingement in the athlete. Sports Med Arthrosc. 2010 Jun;18(2):90-9.