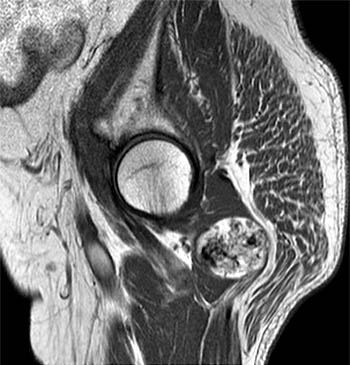
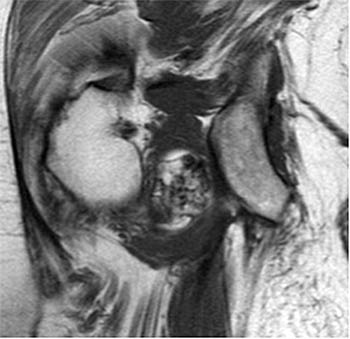
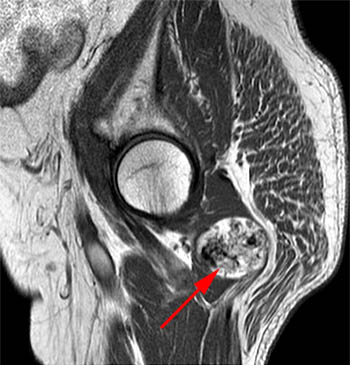
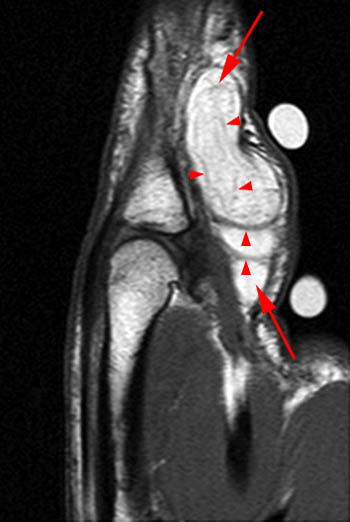
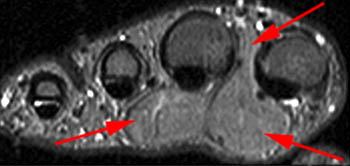
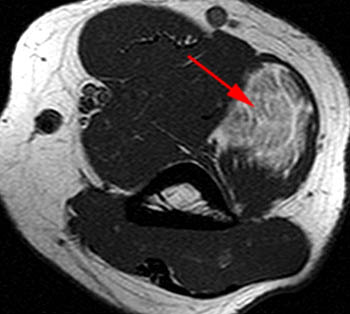
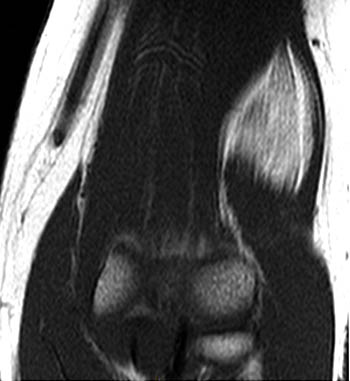
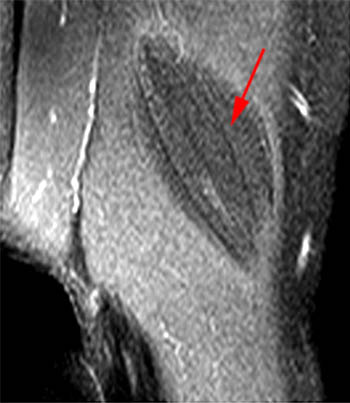
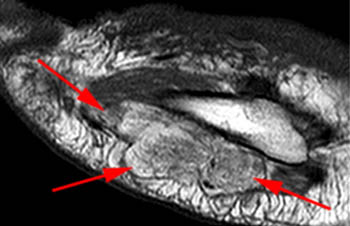
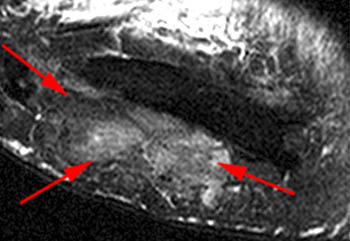
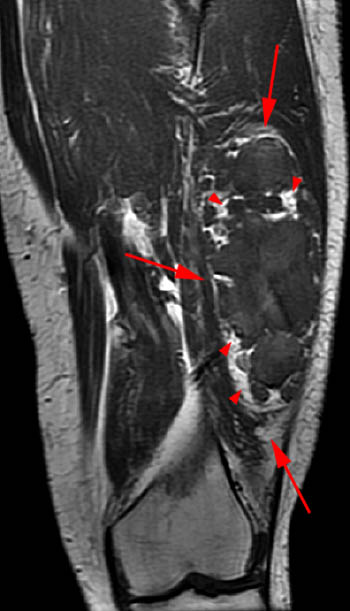
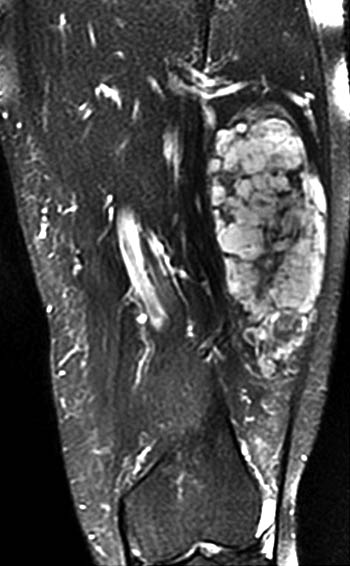
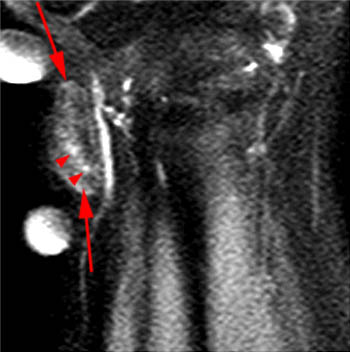
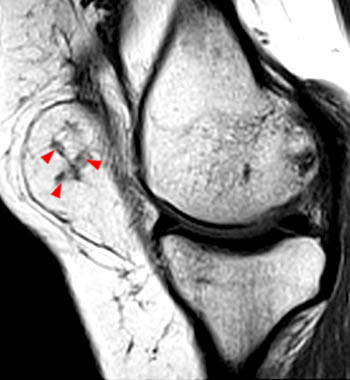
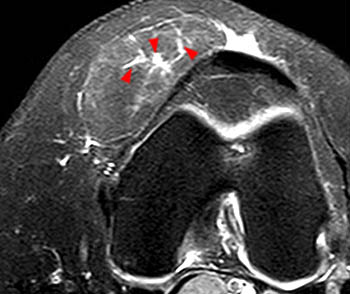
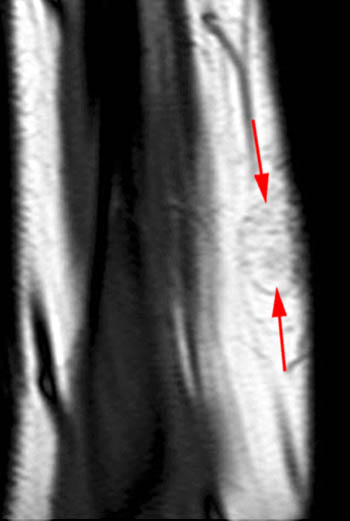
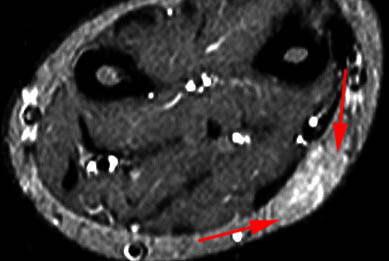
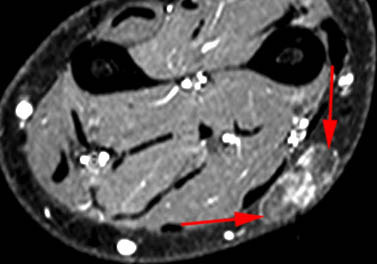
Clinical History: A 65 year-old male presents with right flank pain and sensation of a mass. (1a,1b) T1-weighted sagittal and coronal images and a (1c) STIR coronal image are provided. What are the findings? What is your diagnosis?
Findings
Diagnosis
Intramuscular lipoma with fat necrosis.
Introduction
Lipomas are the most common soft-tissue mass encountered, accounting for 50% of soft-tissue masses1 and found in 2% of the population. Simple lipomas have a highly characteristic appearance on MR images and when typical can be diagnosed with 100% accuracy. However, significant variations in the appearance of lipomas exist, and a number of other fat containing lesions may be found on MR examinations, some of which offer a much more worrisome prognosis.
Lipoma
Simple lipomas are circumscribed masses composed of mature adipocytes that demonstrate no cellular atypia2. Though lipomas cannot be differentiated from normal fat histologically, biochemical and ultrastructural differences have been found3. The majority of simple lipomas are superficial lesions, and these varieties are extremely common (4a, 4b, 5). They are frequently found in the upper back, neck, and shoulder, and typically occur in the 5th to 7th decades of life4. Most superficial lipomas are small and they are only very rarely greater than 10cm in size.
Deep lipomas are less common, are often larger, and are found in a relatively younger patient population. They are most often found within the large muscle groups of the lower extremity, but are also found in the thorax, shoulder, and upper extremities5. Deep lipomas in the retroperitoneum are exceedingly rare, so much so that some authors suggest that any lipomatous tumor in the retroperitoneum should be considered a well-differentiated liposarcoma6.
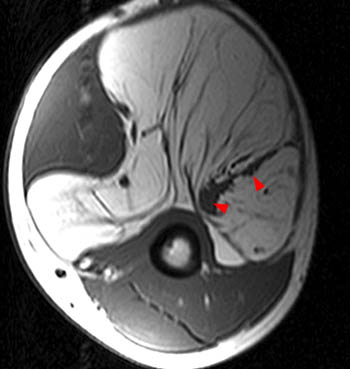
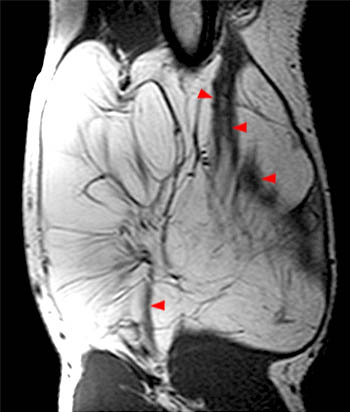
The majority of simple lipomas are of homogeneous fat signal intensity on all MR pulse sequences, have few and thin fibrous septa, are well-circumscribed, and suppress homogeneously on fat-suppressed techniques. When this appearance is found, a benign lipoma can be diagnosed with high reliability7. When intramuscular, muscle fibers coursing through the lesion may mimic thickened septa, though the typical striated appearance and the isointensity to normal muscle on all pulse sequences should prevent this appearance from causing diagnostic confusion (6,7,8).
Atypical lipoma and liposarcoma
Many MR interpreters do not realize that atypical lipomas and well-differentiated liposarcomas are histologically identical lesions. The term atypical lipoma was coined by Evans et al.8 in 1979 as a designation for well-differentiated liposarcomas that occur in a subcutaneous or intramuscular location. Since then, the World Health Organization has further refined the terminology and suggests that the term atypical lipoma should be applied only to subcutaneous extremity lesions, and that all other such masses should be designated well-differentiated liposarcomas.
The reason for the distinction is to recognize the differences in behavior of superficial extremity liposarcomas as opposed to deeper lesions, the latter being much more likely to recur after resection and more likely to develop into higher grade sarcomas. Various surgical correlation studies have pegged the rate of local recurrence for superficial extremity lesions at 0 to 50%9,10,11. Rates for local recurrence of deep extremity lesions have been more consistent, estimated at 43 to 69%12. Retroperitoneal lesions fare even worse, with rates of local recurrence for these lesions estimated as high as 91%. When recurrence does happen, a similar pattern of worsening behavior is seen with regard to dedifferentiation into higher grade malignancies. Whereas there has been only one report of a superficial extremity lesion recurring as a higher grade malignancy13, deep lesions recur with dedifferentiation in the range of 6-13%, and retroperitoneal lesions exhibit this behavior in the range of 17-30%. Both deep extremity and retroperitoneal lesions have been reported to metastasize14, and local extension of disease in retroperitoneal tumors results in death in as many as 38% of patients.
Simple lipomas may be locally or marginally resected when symptomatic or causing cosmetic deformities. Well-differentiated liposarcomas are typically resected with wide margins in light of their propensity to locally recur. In addition, well-differentiated liposarcomas, because they may dedifferentiate, require long term follow-up. These differences explain why it is important for the interpreter of MRI to capably report when a well-differentiated liposarcoma should be considered.
A number of investigators have studied the MR appearance of lipomas versus well-differentiated liposarcomas. As discussed above, when a lesion is of pure fat signal intensity and fibrous septa, if present, are few and thin, the diagnosis of simple lipoma can be made with certainty. Kransdorf found that features that suggest malignancy in a fatty tumor included an older patient age, the presence of thick septa (generally greater than 2mm), larger size (>10cm), decreased fat composition, and nodular/globular areas of non-fat within the lesion15. Incomplete fat-suppression, particularly when nodular or septated, also favors the diagnosis of well-differentiated liposarcoma16. In cases where contrast is administered, well differentiated liposarcomas have been found to exhibit more dramatic enhancement of septae than simple lipomas17. (9-12)
Liposarcomas are among the most common soft tissue malignancy in adults. 4 categories have been recognized: well-differentiated, myxoid (including round cell), pleomorphic, and dedifferentiated. Though well-differentiated liposarcomas often carry a generally benign prognosis, all the other subtypes are higher grade lesions with a more worrisome prognosis, with the overall 5-year survival rate of patients with deep high grade liposarcomas being less than 50%. Metastases are not uncommon in poorly differentiated liposarcomas.
In general, liposarcomas demonstrate increasing heterogeneity and contrast enhancement with increasing grades18. In general, myxoid liposarcomas are mildly heterogeneous on MR images, and pleomorphic liposarcomas are markedly heterogeneous, often with areas of necrosis. Although any liposarcoma subtype may contain fatty elements, higher grade tumors such as pleomorphic liposarcomas may contain no visible fat and be indistinguishable from other soft-tissue sarcomas. Dedifferentiated liposarcomas by definition are biphasic, containing components of well-differentiated sarcomas and components of non-adipose sarcomas19. As a result, fat will be seen within the lesion on MR imaging (13, 14). In cases of suspicious lesions with high fat content, biopsies should be directed to the regions of non-fat signal intensity as these are the sites where dedifferentiated cells will be found.
“Complicated” lipomas and lipoma variants
Although in many cases the diagnosis of simple lipoma or liposarcoma appears obvious, there are many instances where considerable overlap in the imaging features is present. Indeed, a recent study estimated that experienced observers using MRI have a 69% chance of rendering the correct diagnosis when attempting to distinguish between lipoma and a well differentiated liposarcoma20. The reason for this relative lack of specificity is that many lipomas demonstrate areas that do not behave as pure fat on MR imaging. Secondary changes such as fat necrosis (1,2), traumatized fat (15,16), calcification, fibrosis, and myxoid change (17,18) may result in complex imaging features. Importantly, numerous lipoma variants exist, and typically demonstrate complex imaging characteristics that may mimic liposarcoma. Examples of these variants include chondrolipoma, osteolipoma, hibernoma, and angiolipoma (19,20,21).
Conclusion
Lipomas are the most common soft tissue mass encountered, and liposarcomas are among the most common soft tissue malignancies. Liposarcoma terminology has been inconsistently applied in musculoskeletal imaging, and it is important to understand that the term “atypical lipoma” is analogous to a well-differentiated liposarcoma, and is intended to distinguish the less aggressive behavior of liposarcomas when found in the superficial extremity regions. When a discrete wholly fat-signal intensity lesion with homogeneous fat-suppression is encountered, the diagnosis of simple lipoma can be made with high reliability. Similarly, large fat containing lesions with thick septae and areas of non-fat signal nodularity in an older patient usually represent well-differentiated liposarcomas. Although MRI is highly sensitive for the diagnosis of well-differentiated liposarcoma, it is relatively non-specific, as “complicated lipomas” and lipoma variants demonstrate considerable imaging overlap with well-differentiated liposarcomas. Although many lesions found on MRI to be suspicious for well-differentiated liposarcoma ultimately are found to be benign, the risk posed by liposarcoma mandates that masses with complex imaging features be biopsied or treated with wide local excision.
References
1 Murphey MD, Carroll JF, Flemming DJ, Pope TL, Gannon FH, Kransdorf MJ. From the archives of the AFIP: benign musculoskeletal lipomatous lesions. Radiographics. 2004 Sep-Oct;24(5):1433-66.
2 Kumar V, Abbas AK, Fausto N et-al. Robbins and Cotran pathologic basis of disease. W B Saunders Co. (2005) ISBN:0721601871.
3 Weiss SW. Lipomatous tumors. In: Weiss SW, Brooks JSJ, eds. Soft tissue tumors. Baltimore, Md: Williams & Wilkins, 1996; 207-251.
4 Myhre-Jensen O. A consecutive 7-year series of 1331 benign soft tissue tumors. Clinicopathologic data. Comparison with sarcomas. Acta Orthop Scand 1981; 52:287-293.
5 Rydholm A, Berg N. Size, site and clinical incidence of lipoma: factors in the differential diagnosis of lipoma and sarcoma. Acta Orthop Scand 1983; 54:929-934.
6 Kransdorf MJ. Malignant soft-tissue tumors in a large referral population: distribution of diagnoses by age, sex, and location. AJR Am J Roentgenol 1995; 164:129-134.
7 Gaskin CM, Helms CA. Lipomas, lipoma variants, and well-differentiated liposarcomas (atypical lipomas): results of MRI evaluations of 126 consecutive fatty masses. AJU 2004, 182: 733-739.
8 Evans HL, Soule EH, Winkelmann RK. Atypical lipoma, atypical intramuscular lipoma, and well-differentiated liposarcoma: a reappraisal of 30 cases formerly classified as well-differentiated liposarcoma. Cancer 1979; 43:574-584.
9 Rozental TD, Khoury LD, Donthineni-Rao R, Lackman RD. Atypical lipomatous masses of the extremities: outcome of surgical treatment. Clin Orthop 2002; 398:203 -211.
10 Allen PW, Strungs I, MacCormac LB. Atypical subcutaneous fatty tumors: a review of 37 referred cases. Pathology 1998; 30:123 -135.
11 Kindblom LG, Angervall L, Fassina AS. Atypical lipoma. Acta Pathol Microbiol Immunol Scand [A] 1982; 90:27 -36
12 Weiss SW, Rao VK. Well-differentiated liposarcoma (atypical lipoma) of deep soft tissue of the extremities, retroperitoneum, and miscellaneous sites: a follow-up study of 92 cases with analysis of the incidence of “dedifferentiation.” Am J Surg Pathol 1992; 16:1051 -1058.
13 Lucas DR, Nascimento AG, Sanjay BK, Rock MG. Well-differentiated liposarcoma: the Mayo Clinic experience with 58 cases. Am J Clin Pathol 1994; 102:677 -683.
14 Forus A, Larramendy ML, Meza-Zepeda LA, et al. Dedifferentiation of a well-differentiated liposarcoma to a highly malignant metastatic osteosarcoma: amplification of 12q14 at all stages and gain of 1q22-q24 associated with metastases. Cancer Genet Cytogenet 2001; 125:100 -111
15 Kransdorf MJ, Bancroft LW, Peterson JJ, et al. Imaging of fatty tumors: distinction of lipoma and well-differentiated liposarcoma. Radiology 2002; 224:99-104.
16 Galant J, Marti-Bonmati L, Saez F et al. The value of fat-suppressed T2 or STIR sequences in distinguishing lipoma from well-differentiated liposarcoma. Eur Radiol 2003; 13(2):337-43.
17 Hosono M, Kobayashi H, Fujimoto R, et al. Septum-like structures in lipoma and liposarcoma: MR imaging and pathologic correlation. Skeletal Radiol 1997; 26:150 -154.
18 Arkun R, Memis A, Akalin T, Ustun EE, Sabah D, Kandiloglu G. Liposarcoma of soft tissue: MRI findings with pathologic correlation. Skeletal Radiol. 1997 Mar;26(3):167-72.
19 Murphey MD, Arcara LK, Fanburg-Smith J. Imaging of musculoskeletal liposarcoma with radiologic-pathologic correlation. Radiographics 2005, 25:1371-1395.
20 O’Donnell PW, Griffin AM, Eward WC, et al. Can experienced observers differentiate between lipoma and well-differentiated liposarcoma using only MRI? Sarcoma 2013 , Article ID 982784, 6 pages.