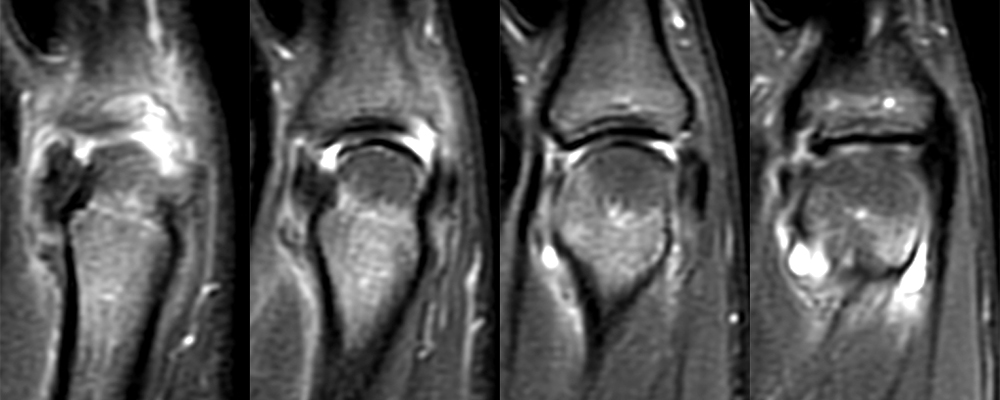
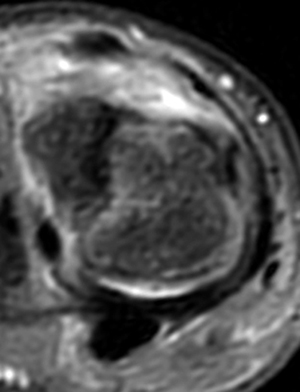
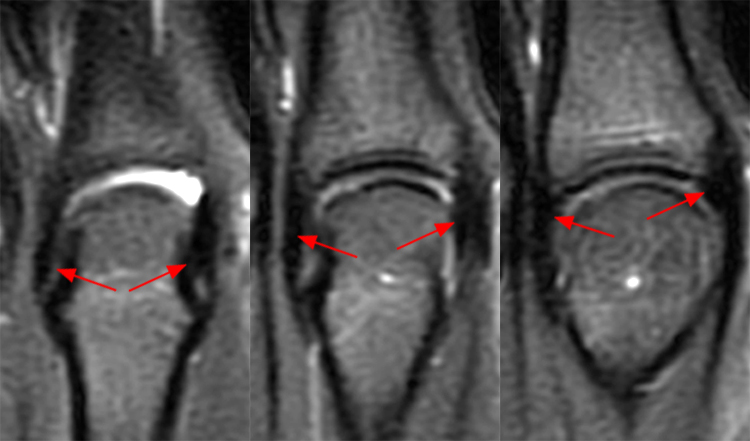
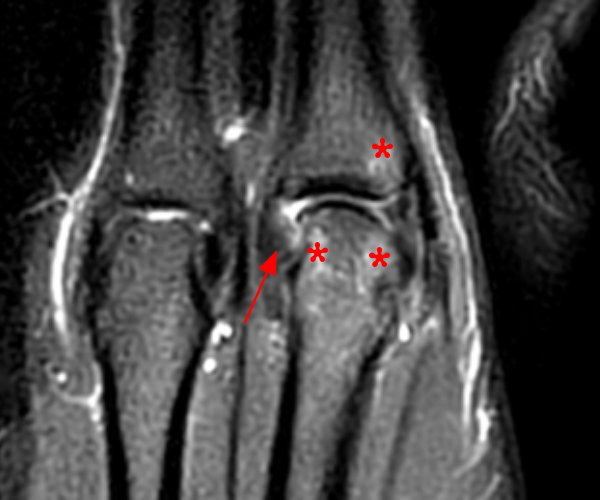
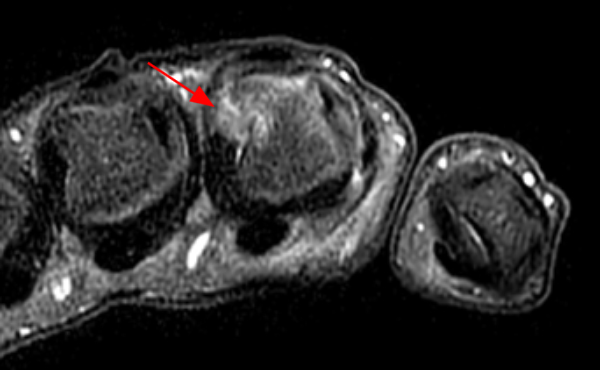
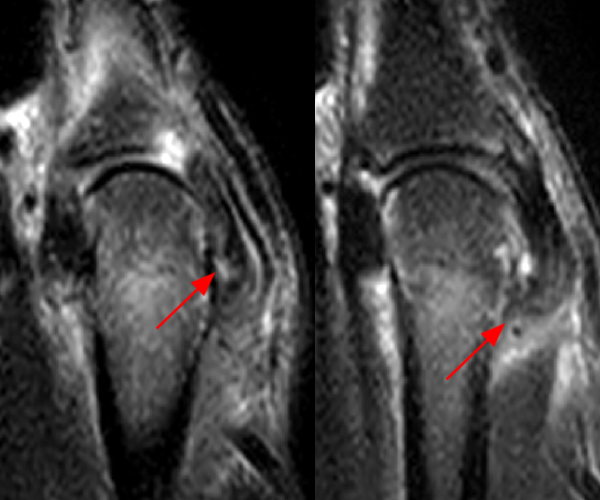
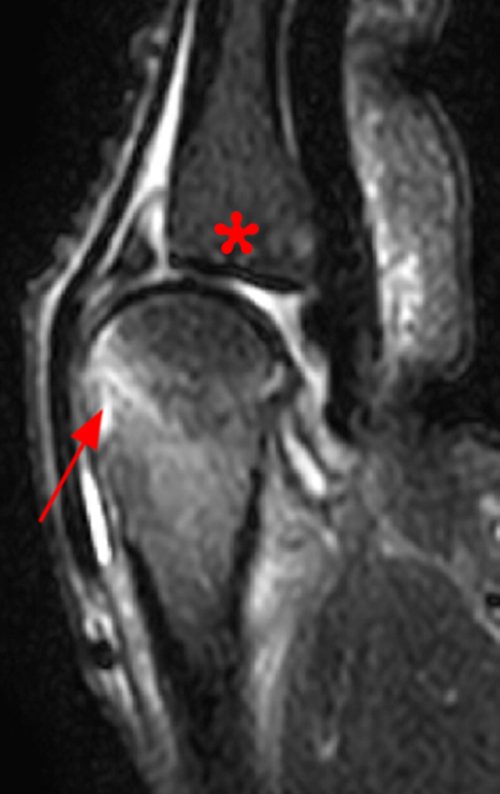
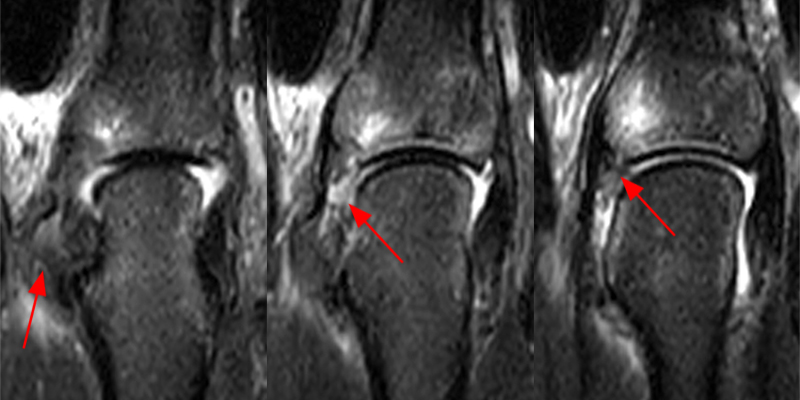
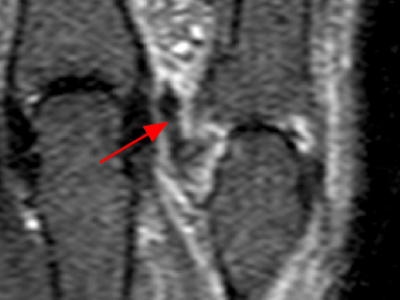
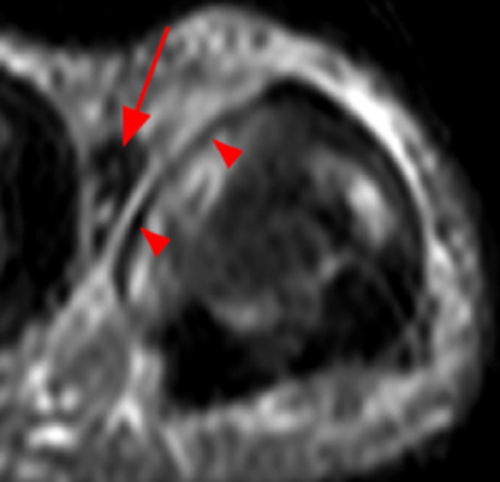
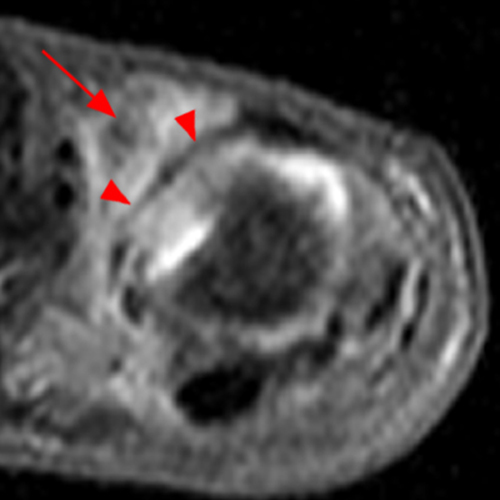
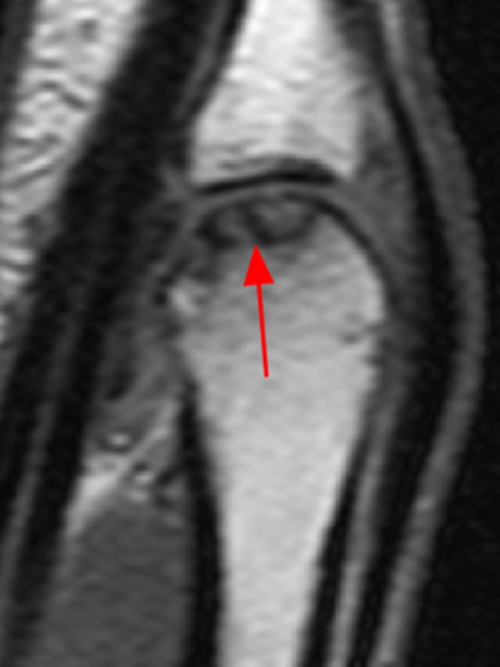
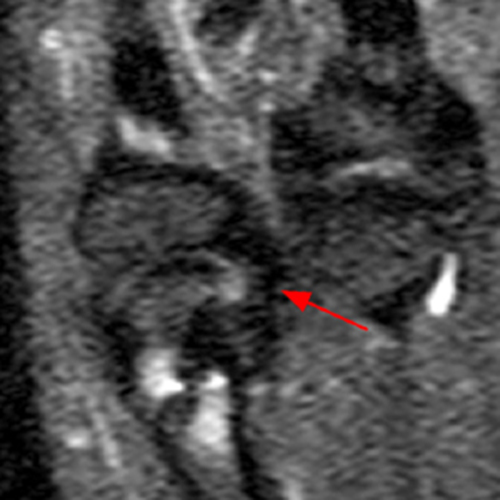
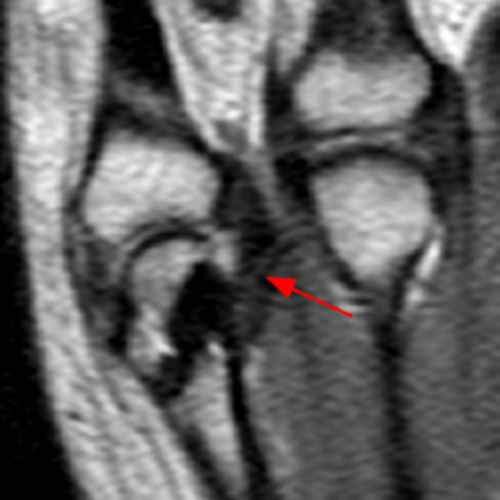
Clinical History: A 16 year-old male presents for MRI of the hand following a wrestling injury. The patient complains of pain at the metacarpal-phalangeal joint (MPJ) of the small finger. Consecutive (1A) fat-suppressed T2-weighted images of the small finger MPJ from dorsal to palmar and a (1B) single fat-suppressed proton density-weighted axial image are provided. What are the findings? What is the diagnosis?
Findings
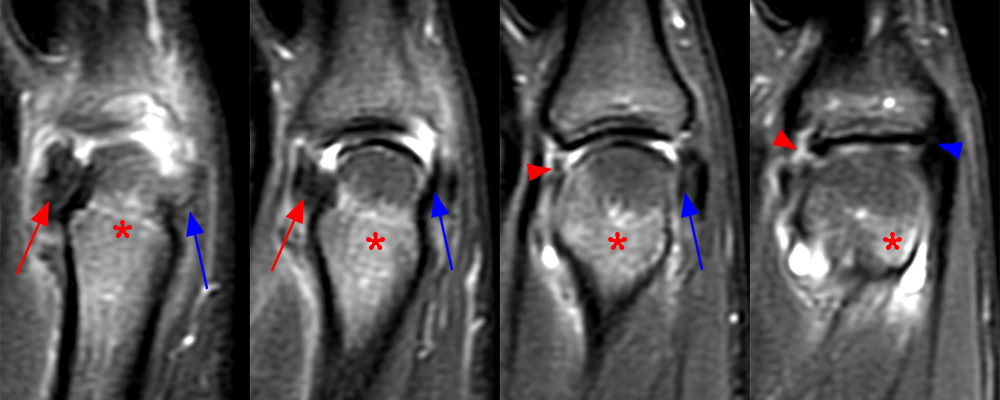
Figure 2:
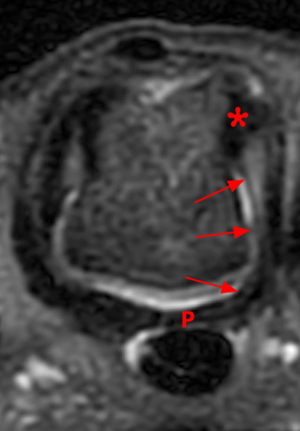
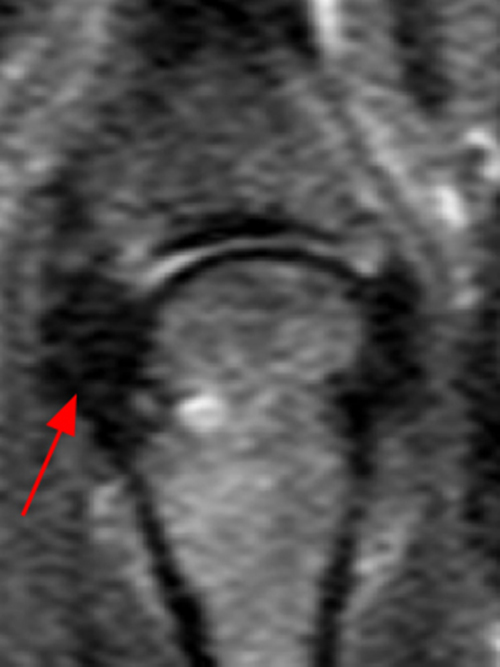
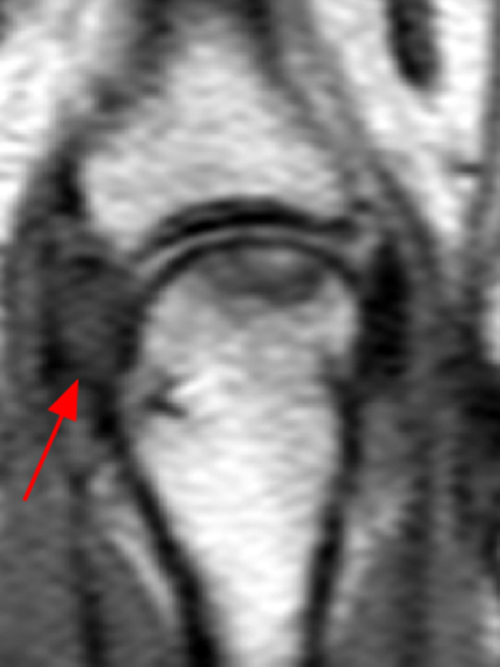
The (1A) consecutive coronal images demonstrate a bulky retracted radial collateral ligament (arrows) on the first two, most dorsal slices. The ulnar collateral ligament (blue arrows) demonstrates proximal edema but is intact. On the 3rd image, attenuated midsubstance radial collateral ligament (RCL) fibers are present (red arrowhead). A fluid filled gap is present at the normal distal insertion site of the RCL on the final provided slice (red arrowhead). The normal distal ulnar collateral ligament (UCL) (blue arrowhead) is well seen on the final slice. Marrow edema within the distal metacarpal (asterisks) is compatible with a bone bruise. The (2B) proton density-weighted axial image at the level of the metacarpal head confirms the bulky retracted fibers (arrow) of the RCL.
Diagnosis
Complete retracted distal tear of the radial collateral ligament at the small finger metacarpal-phalangeal joint.
Introduction
Injuries to the fingers are quite common, as it has been estimated that 20% of emergency department visits are due to traumatic finger injuries.1 Many such injuries involve the collateral ligaments, the best known of these being the ulnar collateral ligament tear of the thumb. Collateral ligament injuries in the fingers are thought to be less common and are relatively less reported in the literature. But clinical experience indicates that these injuries are much more frequent than once believed.2 Although the majority of reported cases involve the RCL of the index finger3, collateral ligament tears have been described in all digits.4,5 Though some reports describe relatively low accuracy and sensitivity for MRI in the evaluation of digital collateral ligament injuries6, advances in technique and a proper understanding of collateral ligament anatomy allow these injuries to be routinely diagnosed with MRI.
Anatomy and Physiology
Finger collateral ligaments range in width from 4-8 mm and measure 12-14 mm in length.7 Proper and accessory collateral ligaments are present. The proper collateral ligaments originate from small depressions along either side of the metacarpal head and their origins lie approximately one-third of the way down from the dorsal surface of the metacarpal head. The ligaments course obliquely to insert at the palmar aspect of the proximal phalanx. Throughout this web clinic, the proper collateral ligaments will be referred to for simplicity as collateral ligaments. The accessory collateral ligaments arise at the same depression as the proper collateral ligaments but in a more palmar location. These structures extend in a palmar direction to attach firmly to the volar plate.8
The collateral ligaments passively restrain the joint by preventing excess motion, but also are innervated in such a way that their nerves send signals to adjacent muscles that influence active protection of the joint in the event of stress.9 The collateral ligaments are taut in flexion and relaxed in extension whereas the accessory collateral ligaments are taut in extension and more relaxed in flexion. The collagen fibers of the ligaments are able to elongate under stress to reach maximum stiffness. Excessive stress overcomes this viscoelastic elongation resulting in ligamentous disruption.
Normal MRI Appearance:
The key anatomical point when evaluating the collateral ligaments on MRI is recognition of the oblique course of the ligament when the fingers are in their usual extended position for MRI scanning. Theumann et al. described a novel MR approach in which scans are obtained in flexion of the MCP, in which case the collateral ligaments can be visualized on a single orthogonal axial slice (Figure 4). Though an elegant technique, this approach is not practical for routine imaging as other anatomical structures become more difficult to evaluate. Therefore, in routine clinical practice, images are obtained with the fingers in extension, and the interpreter of MRI must recognize that the ligament should be followed from proximal to distal as one moves from dorsal to palmar in the coronal plane (Figure 5).
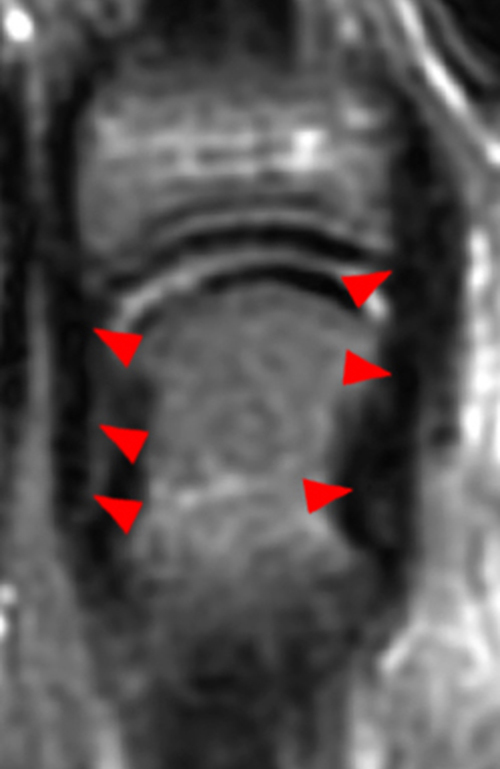
Figure 5:
Consecutive 3mm thick fat-suppressed T2-weighted coronal images (5A) from dorsal to palmar at the ring finger MCP joint demonstrate the normal appearance of the proximal, mid, and distal components of the collateral ligaments (arrows). The accessory collateral ligaments are best seen on axial images at the level of the metacarpal head. On (5B) a fat-suppressed proton density-weighted axial image, the accessory collateral ligament (arrows) is best seen on the ulnar side, coursing from its origin just palmar to the proximal ulnar collateral ligament (asterisk) to its attachment to the volar plate (P).
Although not routinely necessary, knowledge of the oblique course of the collateral ligaments allows depiction of the ligaments in their entirety through the use of oblique image reconstructions, a feature that is readily available on a number of modern PACS solutions. By creating an angled coronal slice along the typical course of the ligaments, revealing images can be obtained even when utilizing conventional 2D datasets (Figure 6).
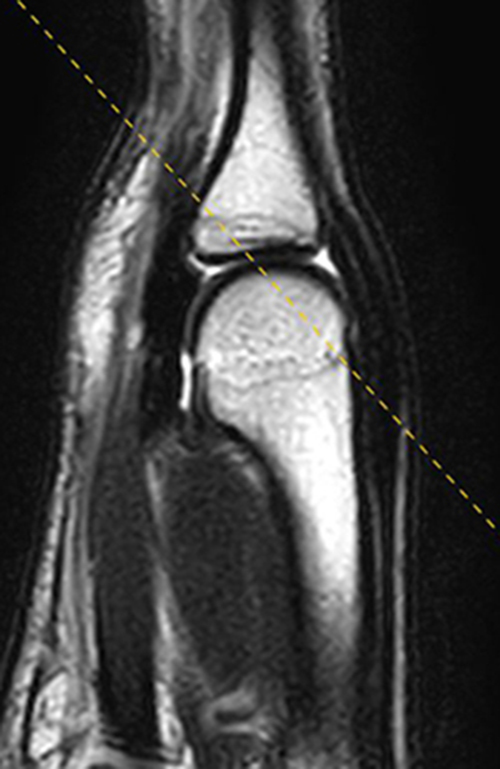
Figure 6:
A fat-suppressed T2-weighted coronal oblique reformatted image (6A) of the ring finger MCP joint (same patient as in 5) demonstrates the normal radial and ulnar collateral ligaments from proximal to distal (arrowheads). The T2-weighted sagittal reference image (6B) indicates the imaging plane utilized.
MRI of Collateral Ligament Tears of the Fingers
The literature is relatively inconsistent in its descriptions of incidence and locations of collateral ligament tears of the fingers.10,11 In our experience at Radsource, radial collateral ligament tears are more common than those on the ulnar side. The index (Figure 7) and small fingers (Figure 2) are most commonly affected, presumably because they are not buttressed on both sides by adjacent fingers. Ulnar collateral ligament tears are most common at the index finger as it is susceptible to unsupported radial deviation, but high grade radial collateral ligament tears of the index finger (Figure 8) are imporant to recognize as if not properly treated such tears are more likely to result in significant functional impairment with loss of pinch and grasp strength.12
Figure 7:
A fat-suppressed T2-weighted coronal image from a 26 year-old male who suffered a twisting injury to the index finger reveals a thickened and edematous proximal UCL (arrow) compatible with a relatively mild partial tear. No ligamentous gap is seen. Avulsive marrow edema is present deep to the ligament origin and bone bruising is evident along the radial aspect of the joint (asterisks), the latter presumably due to valgus force. The thickened and edematous proximal UCL (arrow) is confirmed in its typical dorsal location on a fat-suppressed proton density-weighted axial image at the level of the metacarpal head.
Figure 8:
A 58 year-old female presents two weeks after injury to the index MCP joint from a fall when playing tennis. 2 consecutive fat-suppressed T2-weighted coronal images (8A) from dorsal to palmar are provided. On the first image, an undersurface partial tear (arrow) is seen at the proximal attachment of the RCL. On the next more palmar slice, stripped ligamentous tissue (arrow) is noted to extend more proximally than is typical. Joint instability is apparent on a corresponding fat-suppressed T2-weighted sagittal image (8B), with clear palmar subluxation of the proximal phalanx (asterisk). A bone bruise (arrow) is apparent within the dorsal aspect of the metacarpal head.
Collateral ligament tears at the MCP joints can be proximal, distal, or least commonly midsubstance (Figure 9). One particular pattern of injury is quite important to recognize. In some cases of collateral ligament tears of the MCP joint, ligamentous tissue can become interposed between its attachment site and the sagittal band or extensor hood, resulting in a “Stener-like lesion”.13 We have seen this appearance at multiple digits, but most commonly the tear involves the RCL of the small finger. Such cases (Figures 10-13) result in a ligament tear that can never reattach with conservative treatment, and as with similar lesions at the MCP joint of the thumb, are an absolute indication for surgical repair.
Figure 9:
MRI of the long finger MCP joint in a 43 year-old male 5 weeks after injury with persistent pain and instability despite conservative therapy. Consecutive fat-suppressed T2-weighted coronal images from dorsal to palmar (9A) demonstrate a thickened edematous proximal RCL likely due to retracted ligamentous fibers (arrow) on the most dorsal image. The middle image reveals a near-complete midsubstance ligamentous gap (arrow). The 3rd, most palmar view demonstrates residual intact ligamentous fibers at the distal insertion (arrow). A coronal oblique reconstruction (9B) demonstrates the entirety of the ligament with its midsubstance defect (arrow). The normal UCL (asterisk) is well seen on this oblique view.
Figure 10:
STIR coronal (10A) andn axial (10B) images from a 75 year-old male injured in a fall demonstrate a complete distal tear of the small finger MCP joint RCL with displaced ligamentous tissue (arrows). The displaced ligament clearly lies peripheral to the radial sagittal band (arrowheads) on the axial view.
Figure 11:
A 47 year-old male plumber presented 4 weeks after striking the dorsum of his hand after falling from a ladder. He complained of a tender mass between the ring and small metacarpal heads. A STIR coronal image (11A) reveals a retracted distal tear of the RCL at the small finger MCP joint. As a mass was suspected, the study included post-contrast images. A post-coontrast fat-suppressed T1-weighted axial view demonstrates enhancement which nicely delineates the torn retracted RCL (arrow 11B). The RCL clearly lies superficial to the radial sagittal band (arrowheads).
Figure 12:
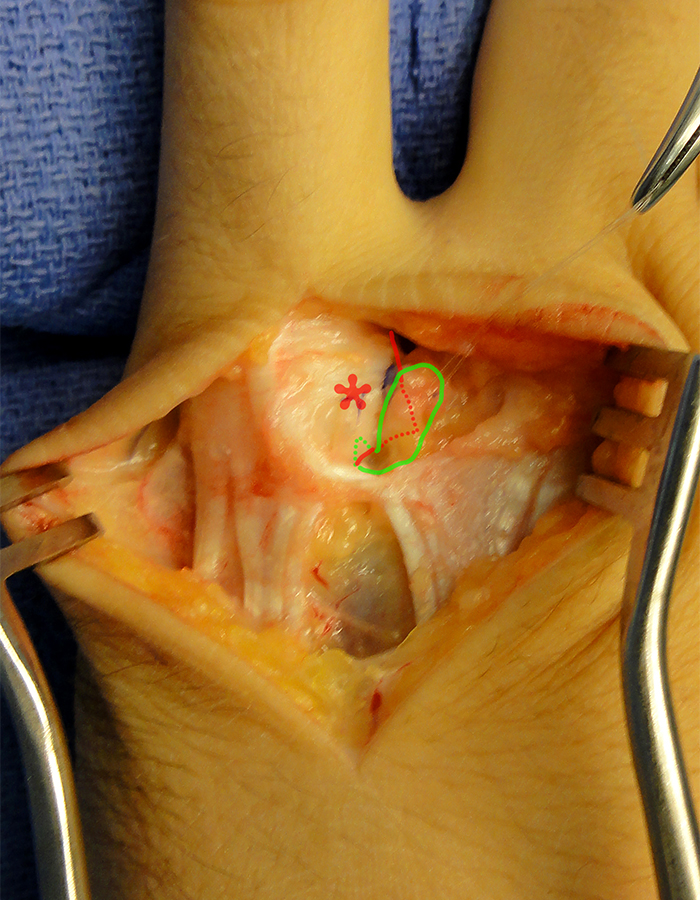
Operative photos from another patient with a “Stener-like” lesion of the small finger MCP joint RCL. The RCL (arrow) was distally torn and retracted to lie peripheral to the radial sagittal band (asterisk). The involved structures are outlined in 12B (red-sagittal band, green-RCL). Photos courtesy of Sunil Thirkannad, MD, Kleinert Kutz Hand Center, Louisville, KY.
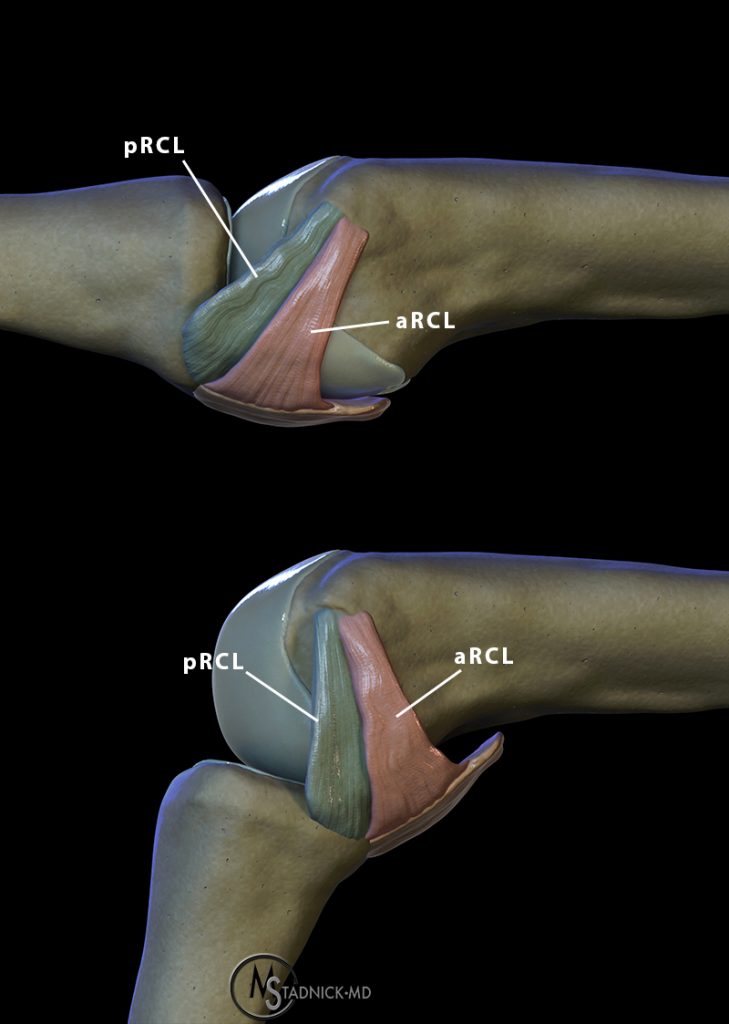
Figure 13:
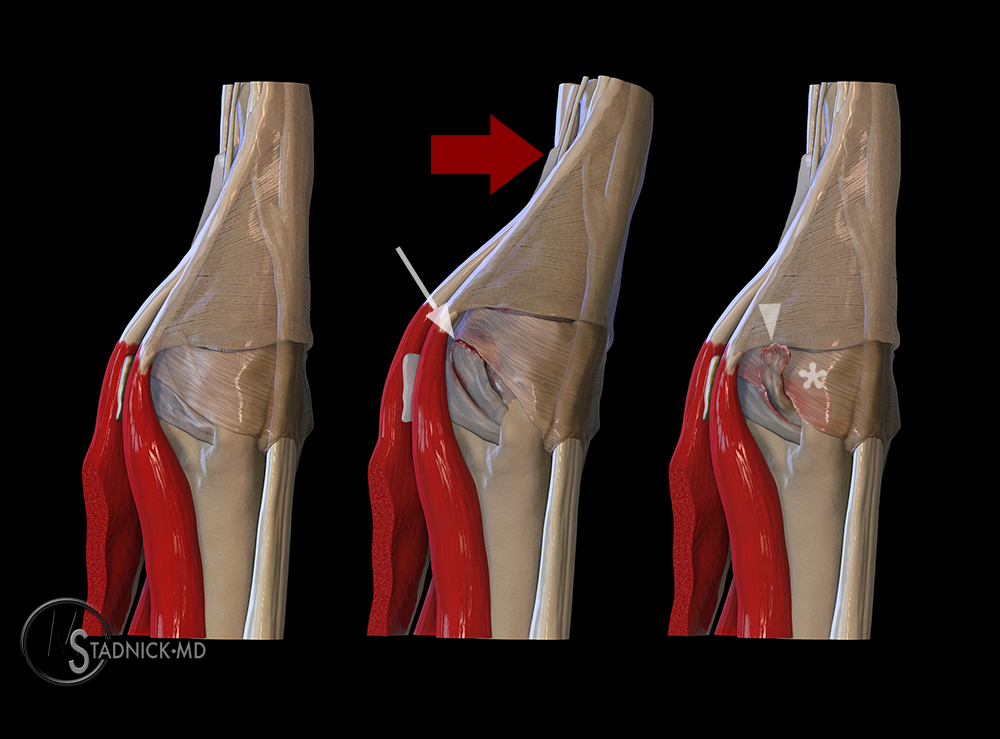
3D dorsal radial views of the 5th metacarpophalangeal joint demonstrate the mechanism of the Stener-like lesion. The normal position of the radial collateral ligament is depicted deep to the radial sagittal band (left image). With a sufficient abduction stress the radial collateral ligament tears white arrow (middle image), and with progressive ulnar deviation the radial collateral ligament (arrowhead) can displace superficial to the radial sagittal band (asterisk), which prevents apposition of the torn ligament and spontaneous healing.
Treatment
Conservative treatment such as splinting and buddy taping is recommended by most surgeons for stable partial collateral ligament tears and for tears with non-displaced or minimally displaced avulsion fractures. In such cases splinting is typically required for 3-6 weeks. Typical indications for operative intervention include the presence of intra-articular fractures, large avulsion fragments, and Stener-like lesions. However, any high grade collateral ligament tear with joint instability should be considered for surgical repair, as there is a well known risk of chronic instability and secondary osteoarthritis in patients with such tears that are treated conservatively (Figure 14). Ligaments left to heal conservatively often appear thicker due to scarring and disorganized collagen, but these thicker structures lack the strength of a normal collateral ligament. Highly active individuals such as athletes or people whose work demands active gripping are candidates for operative intervention, as are patients with chronic tears who have failed conservative therapy.
Figure 14:
A 65 year-old female with a history of long finger MCP joint RCL tear treated conservatively presents with pain and swelling at the joint. STIR (14A) and proton density-weighted coronal (14B) images reveal thickening of the proximal RCL (arrows) at the long finger MCP joint with metacarpal marrow edema on the STIR image and increased signal within the ligament on the proton density-weighted view. Loss of joint space is apparent. The T1-weighted sagittal image (14C) demonstrates prominent subchondral degenerative changes at the metacarpal head (arrow).
Although arthroscopic repair of MCP collateral ligaments has been described14, the vast majority of surgeries for MCP collateral ligament injuries are performed as open procedures, typically utilizing interference screws or anchors. The joint is approached dorsolaterally, incising the extensor apparatus at the junction of the extensor tendon and the sagittal band. The ligament should be reattached in 45 degrees of flexion in order to achieve correct tensioning, and post-operatively the patient is typically splinted in 30-45 degrees of flexion.15 Surgical results are generally excellent with patients often achieving full recovery in 10-11 weeks without residual laxity. As with most other body parts in the musculoskeletal system, MRI can be of benefit in the evaluation of post-operative patients who have persistent symptoms (Figure 15).
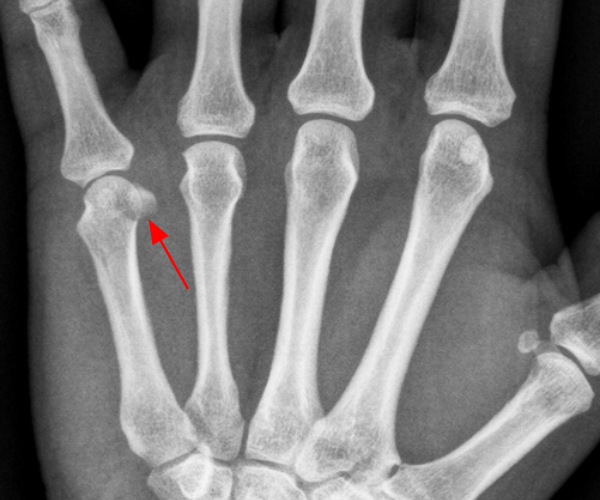
Figure 15:
A radiograph at the time of initial injury in a 46 year-old female who suffered a RCL proximal avulsion fracture (arrow) at the small finger MCP joint. The patient returned for MR imaging 2 years after surgery with complaints of recurrent instability. STIR (15B) and proton density-weighted (15C) coronal images demonstrate an intact ligamentous repair (arrows) with proximal artifact from a metallic anchor. Though the ligament is intact it appears longer and more lax than a typical collateral ligament, perhaps accounting for instability in this patient.
Conclusion
Collateral ligament injuries at the MCP joints of the fingers are under-unreported in the literature, but are routinely encountered in a busy musculoskeletal radiology practice. The key to accurate diagnosis is the understanding of the anatomy and the oblique course of the collateral ligaments with the fingers in extension. Knowledge of this anatomy allows the astute interpreter of MRI to diagnose the injury and gauge the degree of severity, including ligamentous retraction or gaps. In rare cases, a “Stener-like” lesion may be found, and in this situation surgery is required to achieve an acceptable clinical result.
References
- Clark DP, Scott RN, Anderson IW. Hand problems in an accident and emergency department. J Hand Surg (Br) 1985;10(3):297–299. ↩
- Delaere OP, Suttor PM, Degolla R, et al. Early surgical treatment for collateral ligament rupture of the metacarpophalangeal joints of the fingers. J Hand Surg (Am) 2003; 28A:309–315. ↩
- Gaston RG, Lourie GM. Radial collateral ligament injury of the index metacarpophalangeal joint: an underreported but important injury. J Hand Surg (Am). 2006;31(8):1355–61. ↩
- Dray G, Millender LH, Nalebuff EA. Rupture of the radial collateral ligament of a metacarpophalangeal joint to one of the ulnar three fingers. J Hand Surg Am 1979;4:346-350. ↩
- Ishizuki M. Injury to collateral ligament of the metacarpophalangeal joint of a finger. J Hand Surg Am 1988;13:444-448. ↩
- Lutsky K, Levi D, Beredjiklian P. Utility of MRI for diagnosing complete tears of the collateral ligaments of the metacarpophalangeal joints of the lesser digits. HAND (2014) 9:112–116. ↩
- Dy CJ, Tucker SM, Kok PPL, Hearns KA, Carlson MG. Anatomy of the radial collateral ligament of the index metacarpophalangeal joint. J Hand Surg Am. 2013;38(1):124e128. ↩
- Theumann NH, Pfirrmann CW, Drape JL, et al. MR Imaging of the Metacarpophalangeal Joints of the Fingers. Part I. Conventional MR Imaging and MR Arthrographic Findings in Cadavers. Radiology 2002; 222:437–445. ↩
- Rozmaryn LM. The Collateral Ligament of the Digits of the Hand: Anatomy, Physiology, Biomechanics, Injury, and Treatment. J Hand Surg Am. 2017;42(11):904e915. ↩
- Lourie GM, Baston RG, Freeland AE. Collateral Ligament Injuries of the Metacarpophalangeal Joints of the Fingers. Hand Clin 22 (2006) 357–364. ↩
- Theumann NH, Pessis E, Lecompte M. MR imaging of the metacarpophalangeal joints of the fingers: evaluation of 38 patients with chronic joint disability. Skeletal Radiol (2005) 34:210–216. ↩
- Doyle JR, Atkinson RE. Rupture of the radial collateral ligament of the metacarpophalangeal joint of the index finger: a report of three cases. J Hand Surg (Br) 1989;14(2):248–50. ↩
- Coffey MJ, Stadnick ME, Thirkannad SM. Stener-like lesion in the little finger (letter). The Journal of Hand Surgery Vol. 34E No. 2 April 2009 ↩
- Abernathie BL, Lovy AJ, Koehler SM, Hausman MR. Arthroscopic Repair of Collateral Ligaments in Metacarpophalangeal Joints. Arthrosc Tech. 2015 Apr; 4(2): e97–e100. ↩
- Kang L, Rosen A, Potter HG, Weiland AJ. Rupture of the Radial Collateral Ligament of the Index Metacarpophalangeal Joint: Diagnosis and Surgical Treatment. The Journal of Hand Surgery / Vol. 32A No. 6 July–August 2007. ↩