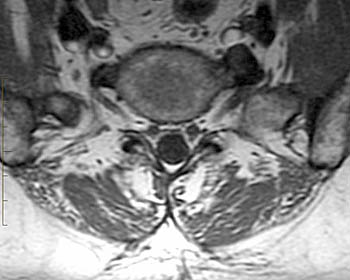
Clinical History: A 66 year-old male presents to his doctor’s office with a longstanding history of low back and leg pain. On physical exam he demonstrates a left L5 radiculopathy. The patient is referred for an MRI of the lumbar spine. (1a,b) T2-weighted coronal and T1-weighted axial images are provided. What are the findings? What is your diagnosis?
Findings
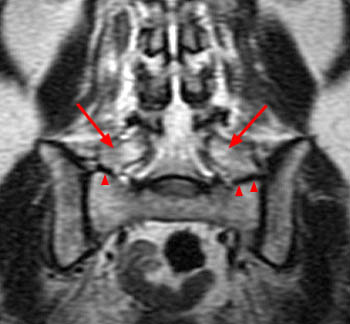
Figure 2:
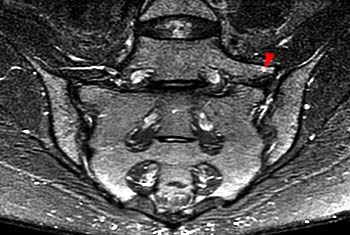
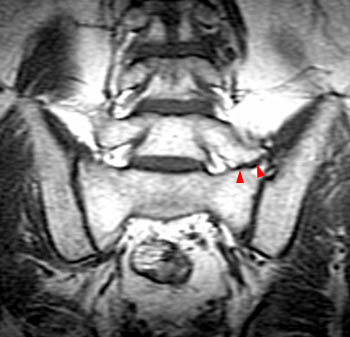
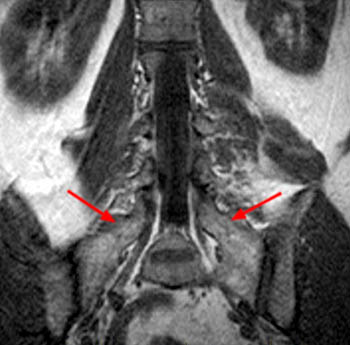
The T2-weighted coronal image demonstrates a developmental transitional lumbosacral junction with enlargement of the "L5" transverse processes (arrows) which articulate with the sacral alae (arrowheads), a configuration referred to as a pseudarthrosis, pseudoarticulation or alternatively a mega-apophysis.
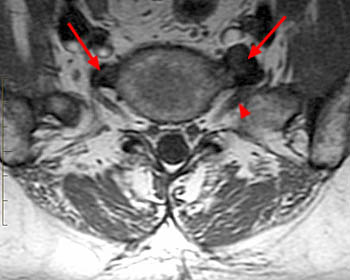
Figure 3:
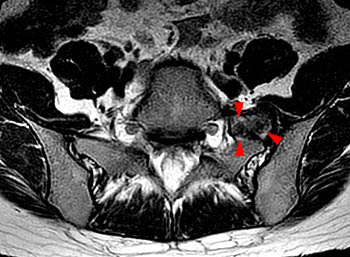
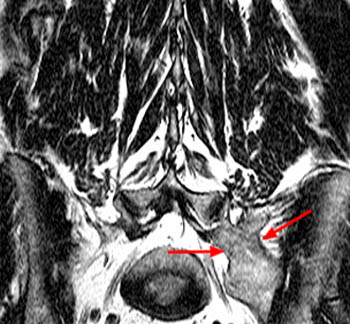
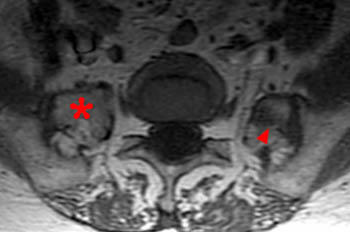
A T1-weighted axial image demonstrates bilateral osteophytes at the transitional level (arrows). The spurs are larger on the left, deforming the L5 ventral spinal root in the paravertebral gutter. The root is enlarged and "swollen." (arrowhead) The findings are responsible for the L5 radicular symptoms.
Diagnosis
Bertolotti’s Syndrome related to a transitional lumbosacral junction. The findings are present bilaterally consistent with a Type IIb transition according to the Castellvi classification.
Introduction
The relationship between low back pain and lumbosacral transitional vertebra (LSTV) has been debated since Bertolotti, an Italian surgeon first described it in 19171. His initial description postulated low back pain caused by arthritic changes occurring at the site where an enlarged transverse process articulated with the sacrum, termed a pseudarthrosis. Over time the syndrome however has been enveloped in controversy and has come to represent a variety of pain syndromes related to adjacent pathologies associated with developmental variations in segmentation referred to as transitional lumbosacral junctions.
In 1984 Castellvi reported an imaging classification system for LSTV. His system is summarized in Figure 4. Type I is simply an enlarged L5 transverse process which is not felt to be clinically significant. Type II includes formation of either a unilateral or bilateral diarthroidal joint between the enlarged transverse process and the sacrum. Type III is a solid fusion either unilaterally or bilaterally and type IV is mixed with a pseudarthrosis on one side2.
Clinical Significance and Pathology
Although the prevalence of transitional segments varies in reports between 4% and over 35%, Bron et al. in 2007 found an average incidence of 12.3% in their review of the literature3. LSTV is a common finding at imaging but may be overlooked. Most patients with this find are asymptomatic. Part of the importance of its observation is to improve communication about vertebral body numbering to help prevent wrong level surgery. It is interesting to note that McCulloch and Waddell demonstrated that the functional L5 nerve root originates at the most caudal “mobile” segment4. This work was confirmed by Chang and Nakagawa5. This observation would suggest that LSVT which are of Type I or II should be labeled L5-S1 and LSTV which are Type III or IV should be labeled S1-2 on MR imaging. However there is no consensus on this matter.
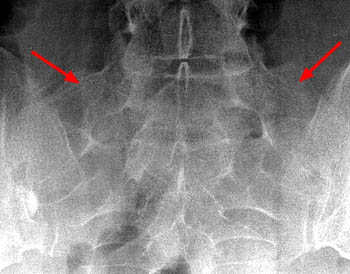
Clinical and imaging studies conflict as to the importance of the presence of a LSTV as it relates to symptoms and imaging findings. There are many case reports and reviews which include a variable number of patients which advocate the existence of Bertolotti’s Syndrome6-19. However many studies and commentaries do not. Brohn reported that about half of observational studies found a positive correlation between a LSTV and low back pain3. In looking at diverse studies over a long period of time, it is important to consider how a LSTV was established in the patient population as some types of imaging are more sensitive to transitional segments than others. Certainly, MRI with coronal series, a CT scan with coronal reconstructions, and a Ferguson radiographic view of the lumbar spine are more sensitive than a standard AP radiograph of the spine.
The original description of Bertolotti’s syndrome referenced arthritis of the “transverse-sacral pseudarthrosis” as a source of back pain. This arthritis or “stress reaction” may be observed as edema within this structure on MRI, isotope avidity on bone scan particularly on SPECT, or as marginal spurring, hypertrophy and sclerosis on MR, CT or radiographs (Figure 5). Pain related to this “stress reaction” may respond with relief of symptoms following fluoroscopic or CT guided injection of anesthetics6,7,9,12,14,15,17,19.
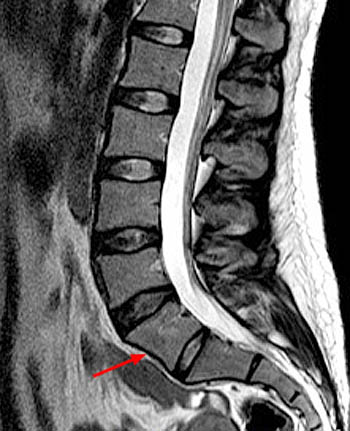
Figure 5:
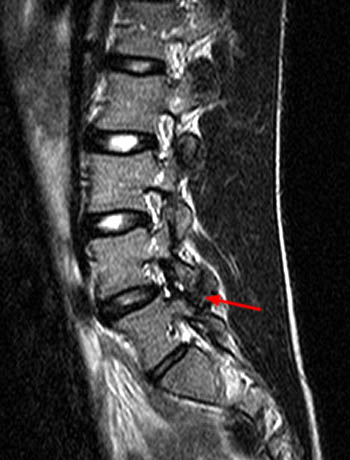
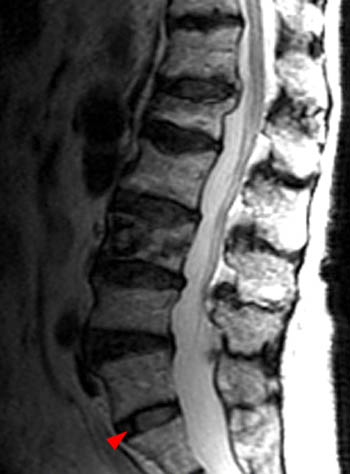
A T2-weighted sagittal image of the lumbar spine in a 32 year-old woman who presented with left SI joint region pain. A transitional lumbosacral junction is suggested on this image by a slightly inferiorly wedged segment mimicking the S1 vertebral body (arrow) in this plane despite a relatively large subjacent intervertebral disc. A LSTV can only be confirmed by referencing other planes.
Figure 6:
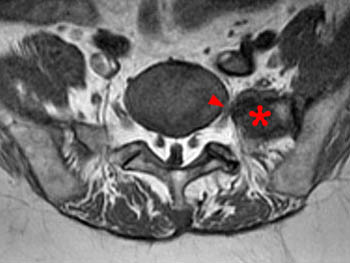
In the same patient as in 5, T2-weighted axial (6a) and T2-weighted fat-suppressed coronal (6b) images at the lumbosacral junction confirm a left Castellvi IIa transition. Additionally the signal within the components making up the 'pseudoarticulation' is heterogeneous suggesting premature degeneration of this diarthrodial joint and reactive edema (arrowheads).
Hypertrophic changes can also compress or displace the ventral spinal root in the paravertebral gutter, so called extraforaminal stenosis (Figure 7). This may be obvious on ‘routine’ MR or CT depending on slice selection and angulation but may require specific coronal sequences or reconstructions to highlight the finding10.
There is an increased incidence of disc degeneration, disc herniation and facet degeneration at vertebral levels just cephalad to the transitional vertebral body. Aihara et al. reported in cadavers that the iliolumbar ligaments were thinner and weaker at the level above the LSTV20. In some circumstances the transitional segment is postulated to act as a “blocked” or fused segment leading to hypermobility at the segment above. Therefore discogenic or facetogenic pain can arise indirectly from a subjacent LSTV. Disc herniation is much more likely at the level immediately above the transitional disc as well21 (Figure 8). Relative stability or lack of mobility of the transitional segment is felt to be responsible for the observation of reduced degeneration of discs subjacent to a transitional vertebral body.
Figure 8:
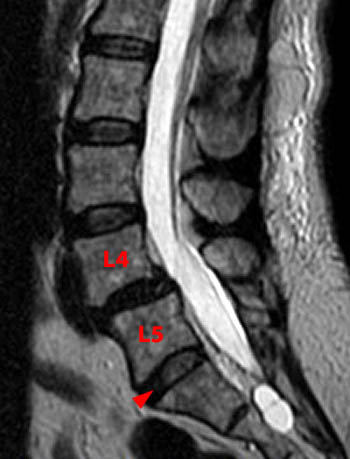
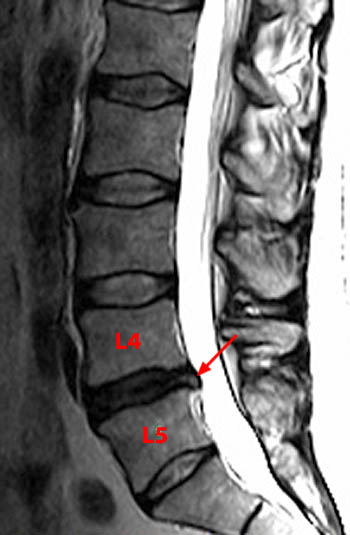
A T2-weighted sagittal image in a patient with a Castellvi IIb transition (not shown) demonstrates selective disc and facet degeneration and subsequent spondylolisthesis at the segment (L4) cephalad to the transitional segment (L5). Note the relatively normal appearance of the disc just caudal to the transitional vertebral body (arrowhead).
Contralateral facet arthrosis and hypertrophy are also commonly found in relation to LSVT, and could theoretically create facetogenic pain. (Figure 10)
Although the literature lacks a consensus on the causal relationship between low back pain and LSTV, there is evidence that biomechanical function and load bearing are altered. This potentially impacts those involved in athletics or physical labor more than those with sedentary lifestyles. Connolly found abnormal isotope uptake at LSTV in some young athletes with low back pain11. Back et al. described two avid golfers felt to have Bertolotti’s Syndrome who had negative responses to medial branch RF denervation and discography but responded to diagnostic anesthetic injections into what they referred to as the “sacrotransverse pseudoarticulation” and subsequently responded to radiofrequency ablation of that joint7 (Figure 13). Dougherty also reported results of a small number of patients who failed to respond to CT-guided SI joint injection and epidural steroid injection but did respond to CT guided injection of the pseudarthrosis12.
In a review of 769 consecutive patients with low back pain and an MRI, Quinlan found 35 or 4.6% with Bertolotti’s Syndrome, More than half of their patients with this syndrome were under 30 years old and 11.4% of their patients less than 30 years old had Bertolotti’s Syndrome. The authors felt that Bertolotti’s Syndrome must be considered in younger patients with back pain16.
Additional Examples
Treatment
Since there is controversy about the existence of Bertolotti’s Syndrome and the significance of LSTV, one would expect a lack of consensus as to the best way to treat these patients. Various approaches include: percutaneous injection of anesthetic and steroids, radiofrequency ablation of the anomalous diarthroidal joint, posterior surgical fusion of the pseudarthrosis, and resection of the enlarged transverse process3,6,7,8,9,13,14,15,17. Cox in his classic textbook on chiropractic care stated that low back pain associated with a transitional segment requires the greatest number of therapeutic sessions to obtain maximal results22.
Conclusion
Lumbosacral transitional vertebral bodies are a commonly encountered abnormality on MR Imaging. Recognition and description of these anomalies are important as the transitional segments and their related pathologies may account for the patient’s pain. In addition, proper communication of vertebral body numbering in cases of transitional segments is necessary to reduce the risk of intervention at an incorrect lumbosacral level.
References
1 Bertolotti M: Contributo alla conoscenza dei vizi differenza-zione regionale del rachide con speciale riguardo all assimilazione sacrale della V. lombare. Radiol Med 1917, 4:113-144.
2 Castellvi AE, Goldstein LA, Chan DPK: Lumbosacral transitional vertebra and their relationship with lumbar extradural defects. Spine 1984, 9:493-495.
3 Brohn JL, van Royen BJ, Wuisman P. The Clinical Significance of Lumbosacral Transitional Anomalies. Acta Orthop Belg, 2007,73: 687-695.
4 McCulloch JA, Waddell G. Variation of the lumbosacral myotomes with bony segmental anomalies. J Bone Joint Surg 1980 ; 62-B : 475-480.
5 Chang HS, Nakagawa H. Altered function of lumbar nerve roots in patients with transitional lumbosacral vertebrae. Spine 2004 ; 29 : 1632-1635.
6 Avimadj M, et al. Can an Anomalous Lumbosacral or Lumboiliac Articulation cause Low Back pain? A Retrospective Study of 12 Cases. Rev Rhum Engl Ed 1999; 66:35-39.
7 Back JD, Wyss JF, Lutz GE. Bertolotti Syndrome as a Potential cause of Low Back pain in Golfers. PM&R 2011; 3:771-775
8 Benzecry de Almeida D, et al. Transitional Lumbosacral Vertebrae and Back Pain: Diagnostic Pitfalls and Management of Bertolotti’s Syndrome. Arq Neuropsiqiatr 2009; 67: 268-272
9 Burnham R. Radiofrequency Sensory Ablation as a treatment for Symptomatic Unilateral Lumbosacral Junction Pseudarticulation. Pain Med. 2010: 11:853-855.
10 Byun WM, Kim JW, Lee JK. Differentiation Between Symptomatic and Asymptomatic Extraforaminal Stenosis in Lumbosacral Transitional Vertebra: Role of Three-Dimensional Magnetic Resonance Lumbosacral Radiculography. Korean J Radiol. 2012; 13: 403-411.
11 Connolly LP, Drubach LA, Connolly SA, Treves ST. Young athletes with low back pain : skeletal scintigraphy of conditions other than pars interarticularis stress. Clin Nucl Med 2004 ; 29 : 689-693.
12 Dougherty PE. Pain Generators Associated with Type IIA Lumbosacral Transition Segments. Presented at Symposium conducted at the meeting of the International Conference for Spinal Manipulation, Toronto Canada. October 2002.
13 Konin GP, Walz DM. Lumbosacral Transitional Vertebrae: Classification, Imaging Findings, and Clinical Relevance. Am J Neuroradiol 2010; 31: 1778-1786.
14 Mitra R, Carlisle M. Bertolotti’s Syndrome: a case report. Pain Pract. 2009; 9:152-154.
15 Paraskevas G, et al. Lumbosacral Transitional Vertebra Causing Bertolotti’s Syndrome: A Case Report and Review of the Literature. Cases Journal 2009; 2:8320.pp1-3.
16 Quinlan JF, Duke D, Eustace S: Bertolotti’s syndrome. A cause of back pain in young people. J Bone Joint Surg (Br) 2006; 88:1183-1186.
17 Santavirta S, et al. Surgical Treatment of Bertolotti’s syndrome. Follow up of 16 patients. Arch OrthopTrauma Surg 1993, 112:82-87.
18 Shimbayama M, et al. Unsuspected Reason for Sciatica in Bertolotti’s Syndrome. J Bone Joint Surg (Br) 2011; 93:705-707.
19 Ugokwe KT, et al. Minimally Invasive Surgical Treatment of Bertolotti’s Syndrome: Case Report. Neurosurg 2008;62(Suppl 2):ONSE454-5;discussion ONSE456.
20 Aihara T, Takahashi K, Ogasawara A, Itadera E, Ono Y, Moriya H:Intervertebral disc degeneration associated with lumbosacral transitional vertebrae: a clinical and anatomical study. J Bone Joint Surg Br 2005, 87:687-691.
21 Elster AD: Bertolotti’s syndrome revisited. Transitional vertebrae of the lumbar spine. Spine 1989, 14:1373-1377.
22 Cox, James M. Low Back Pain: Mechanism, Diagnosis and Treatment 7th ed. Lippincott Williams & Wilkins, 2011, Chapter 12: Transitional Segment.