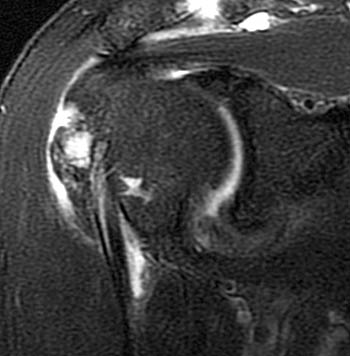
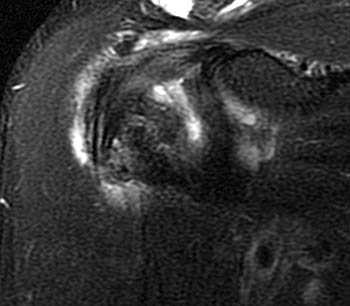
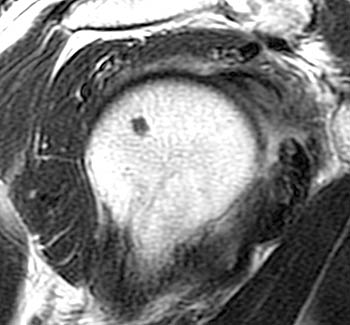
Clinical History: A 68 year-old male presents with a 2 month history of pain and limited range of motion. Coronal oblique T2-weighted fat-suppressed (1a,1b), axial proton density-weighted fat-suppressed (1c), and sagittal oblique T2-weighted FSE (1d) images are provided. What are the findings? What is your diagnosis?
Findings
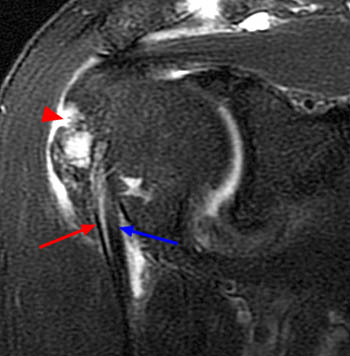
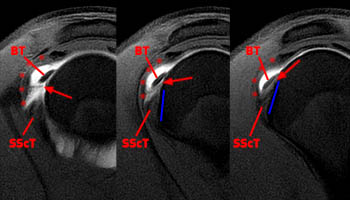
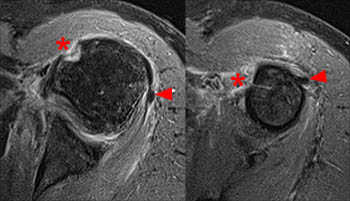
Figure 2:
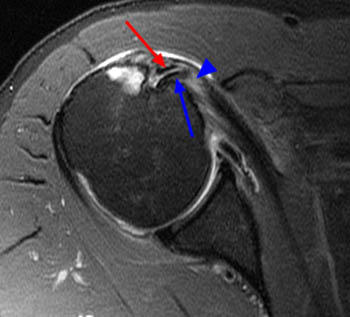
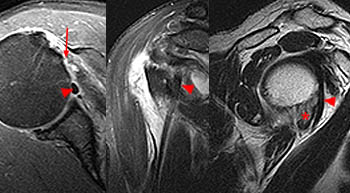
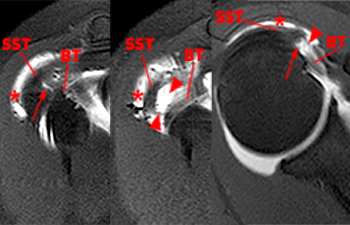
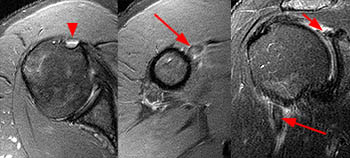
The coronal oblique T2-weighted fat-suppressed image through the anterior humerus demonstrates a bursal sided fluid-signal discontinuity of the anterior supraspinatus tendon (arrowhead). Two low-signal vertically oriented structures are identified along the normal course of the long head of the biceps tendon within the distal bicipital groove (blue arrow and red arrow).
Figure 3:
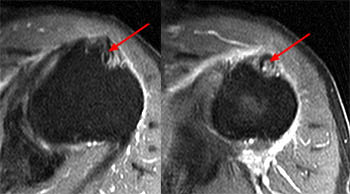
A coronal oblique T2-weighted fat-suppressed image slightly more anterior to image A demonstrates divergence of the 2 vertically oriented structures. The thinner lateral structure maintains a more vertical orientation (red arrows). The medial structure (blue arrows) follows a more typical course for the long head of the biceps tendon toward the superior glenoid and appears thickened and increased in signal at the anterior superior aspect of the glenohumeral joint (upper blue arrow).
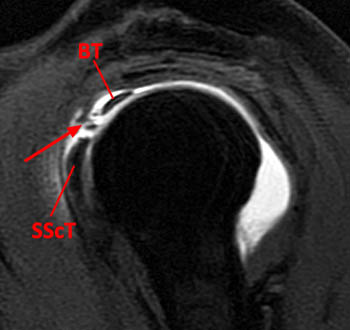
Figure 4:
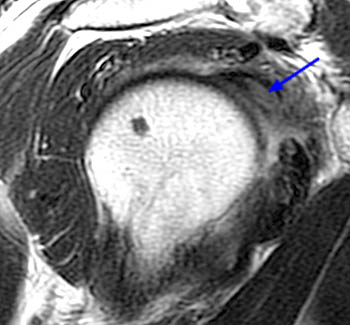
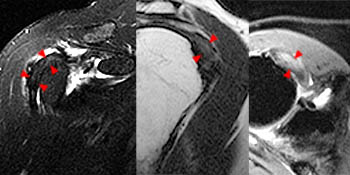
This axial fat-suppressed proton density-weighted image through the bicipital groove demonstrates focally increased signal involving the superiorly-most inserting subscapularis tendon (arrowhead) with a flattened and medially subluxed long head of the biceps tendon (blue arrow). The linear structure within the anterior aspect of the bicipital groove corresponds to the lateral tendinous structure seen in images 2a and 3a.
Diagnosis
Bursal sided insertional partial tear of the anterior supraspinatus tendon, insertional partial tear of the superior-most subscapularis tendon, medial subluxation of the long head of the biceps tendon with moderately severe intra-articular tendinosis. Accessory head of the long biceps tendon arising from the anterior capsule.
Introduction
The long head of the biceps tendon (LHBT) is widely recognized as an important pain generator. As in the test case, LHBT injuries are rarely an isolated injury and are frequently accompanied by significant shoulder pathology. Consequently, a diagnosis of LHBT injury by physical examination is frequently inconclusive or masked by accompanying shoulder injuries. In addition, the detection of LHBT pathology in certain locations may be difficult at shoulder arthroscopy. Failure to adequately address LHBT injuries or instability often results in suboptimal outcomes to conservative therapy or surgery. MRI plays an important role in evaluating the LHBT and in identifying significant LHBT pathology.
Anatomy and Function
The long biceps tendon arises from the supraglenoid tubercle and partly from the superior glenoid labrum (7a). The tendon is intra-articular but extrasynovial, with a surrounding synovial-lined sheath that communicates with the glenohumeral joint and extends into the bicipital groove. As it passes anteriorly and laterally to the bicipital groove, the intra-articular portion of the LHBT is cradled and stabilized by the superior glenohumeral ligament (SGHL) and coracohumeral ligament (CHL), which fuse along the lateral half of the rotator interval with fibers from the subscapularis and supraspinatus to form the biceps pulley (8a). The LHBT undergoes a rather abrupt angulation of 30 to 40 degrees as it passes through the pulley and into the bicipital groove1. The intra-articular portion of the long biceps tendon has a flattened and slightly larger cross-sectional contour and transitions to a more rounded and smaller cross-section as it passes into the bicipital groove (9a)2. The tendon is smallest in caliber as it exits the bicipital groove3. Within the bicipital groove the deeper, sliding surface of the tendon is avascular and composed of fibrocartilage2. The LHBT is 5-6 mm in diameter and approximately 10 cm in length with the musculotendinous junction found deep to the pectoralis major tendon4. Further distally the long head of the biceps muscle joins with the short head of the biceps muscle to form the biceps muscle belly. Cheng described the arterial supply to LHB tendon as arising from 3 potential sources consisting of branches of the brachial artery entering the tendon at the musculotendinous junction, thoracoacromial artery branches that cross the tendon-bone interface at the glenoid, and a more variable supply via branches of the anterior circumflex humeral artery that travel in a mesotenon to supply the mid-portion of the LHBT5. A relatively consistent zone of hypovascularity is seen 1.2 – 3 cm from the tendon origin5. The tendon of the long head of the biceps is innervated by a network of sensory and sympathetic fibers that are asymmetrically distributed with a higher concentration of innervating fibers at the tendon origin. This distribution is felt to play a role in the pathogenesis of shoulder pain arising from biceps tendon injury6.
Figure 6:
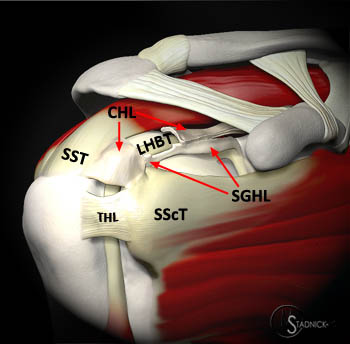
A 3D graphic view of the anterior shoulder with the coracohumeral ligament (CHL) largely resected to demonstrate the close proximity of the CHL and superior glenohumeral ligament (SGHL) to the long head of the biceps tendon (LHBT) as it traverses the rotator interval. The CHL and SGHL join with fibers from the subscapularis tendon (SScT) and supraspinatus tendon (SST) to form the biceps pulley, stabilizing the LHBT as it enters the bicipital groove where it continues deep to the transverse humeral ligament (THL).
MR Imaging
MRI with or without intra-articular contrast is the preferred imaging modality for evaluating the intra-articular and extra-articular LHBT and the adjacent structures of the shoulder7. Evaluation of the LHBT by MRI relies on a variety of sequences performed in the axial, coronal oblique, and sagittal oblique planes with emphasis on certain angles depending on the portion of the tendon being assessed. Imaging of the biceps anchor relies primarily on coronal oblique images. The rotator interval structures including the biceps pulley and traversing long head of the biceps tendon are best evaluated with sagittal oblique images (8a). Axial images are best for evaluating the LHBT at the level of the bicipital groove (9a). In all instances, correlation with orthogonal views provides important confirmatory and complementary information. By distending the rotator interval, MR arthrography allows more detailed evaluation of the biceps pulley and rotator interval structures which are best seen in the sagittal oblique plane (8a). MR arthrography typically depicts a well-defined proximal superior glenohumeral ligament and a distal superior glenohumeral fold that helps to form the biceps pulley (7a,8a). The intervening rotator interval ligamentous structures are less well delineated7.
Figure 7:
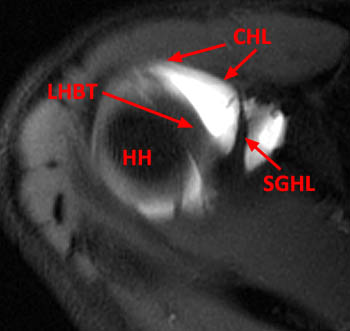
MR arthrogram axial fat-suppressed T1-weighted image through the superior glenohumeral joint demonstrates the superior glenohumeral ligament (SGHL) arising from the supraglenoid and anterior labrum and its course anteriorly to fuse with the coracohumeral ligament (CHL). The Long head of the biceps tendon (LHBT) arising near the SGHL at the supraglenoid tubercle and superior labrum and curves anterolaterally over the humeral head (HH) to the bicipital groove.
Figure 8:
Sequential sagittal oblique T1-weighted fat-suppressed images from an MR arthrogram study moving from medial (left) to lateral (right) demonstrate the typical landmarks associated with the medial portion of the biceps pulley in the lateral aspect of the rotator interval medial to the bicipital groove. The SGHL forms a fold of tissue (arrow) from the anterior fused SGHL and CHL (dotted line) and wraps inferior to the LHBT (BT). Laterally this fold of the SGHL attaches along with the superior subscapularis tendon under the LHBT at the upper margin of the lesser tuberosity (blue line) forming a layer between the LHBT (BT) and subscapularis (SScT). The intra-articular portion has a slightly flattened contour.
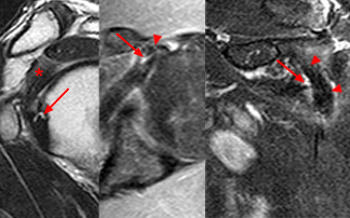
Figure 9:
Sequential axial T1-weighted fat-suppressed MR arthrogram images progressing from inferior to superior demonstrate the superior subscapularis insertion at the level of the lesser tuberosity (red arrowheads) and the superior-most subscapularis tendon insertion (red arrow) over the upper margin of the lesser tuberosity. The lateral limb of the coracohumeral ligament (blue arrow) is identified covering the LHBT. Subscapularis tendon fibers continue laterally to the greater tuberosity (blue arrowheads). Within the bicipital groove the LHBT typically has a more rounded cross-sectional contour.
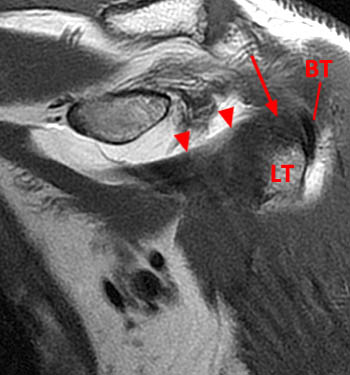
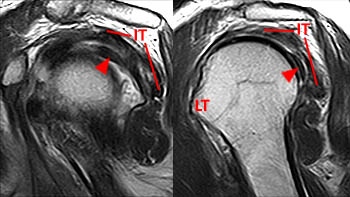
Figure 10:
A coronal oblique T1-weighted image from a MR arthrogram of the shoulder, demonstrates the superior margin of the subscapularis, which can be followed medially to its insertion at the upper margin (arrow) of the lesser tuberosity (LT). The biceps tendon (BT) lies in close proximity to this portion of the subscapularis tendon insertion.
Variants of LHBT
A wide range of anatomic variations have been reported for the LHBT and proximal biceps. Aberrant intra-articular and extra-articular origins of the LHBT have been described as well as congenital absence. The LHBT has been reported to arise from the rotator cuff and glenohumeral capsule (11a). Bifurcated origins have been described including tendon origins from the supraglenoid tubercle and posterior superior labrum, a bifid tendon originating from the supraglenoid tubercle, and tendon origins from the rotator cable and the scapula without an origin from the superior labrum or glenoid8. While variants of biceps origin are common and typically benign, congenital absence of the long head of the biceps has a higher reported association with other congenital abnormalities and shoulder instability. The association with other congenital anomalies is felt to arise because of a fetal insult at around 7 weeks of gestation during biceps differentiation9. Congenital absence of the LHBT has been reported in one patient with spina bifida, congenital inguinal hernia, and undescended testicle10. Other reported abnormalities in patients with congenital absence of the LHBT include VATER syndrome11, congenital limb abnormalities, multidirectional instability, and glenoid dysplasia with posterior instability. Less commonly congenital absence of the LHBT may occur without associated congenital anomalies or shoulder instability12.
Figure 11:
Incidental and asymptomatic anomalous origin of the LHBT in a 19 year-old female who was injured while lifting weights. Axial proton density-weighted fat-suppressed images at the inferior bicipital groove (far left)and superior to the bicipital groove (middle left) demonstrate the LHBT within the bicipital groove (arrow) which can be followed superiorly to the anterior supraspinatus and capsular region. The anomalous course is confirmed on the sagittal T2-weighted (middle left) and coronal T1-weighted images (far left). No LHBT was identified in the typical biceps anchor location at the superior glenoid.
Accessory heads of the biceps brachii are common, ranging from 9.1-22.9% depending on the ethnic group, being most common in the Asian population. Supernumerary bicipital heads include additional origins from the articular capsule of the glenohumeral joint (12a), from the tuberosities of the humerus, and from the coracoid process13,14,15. By MRI an accessory tendon is seen as an additional hypointense structure within the biceps groove that is often flattened and can be misinterpreted as a longitudinal tear of the LHBT without carefully tracing the accessory tendon to its origin (12a)15.
Figure 12:
Accessory head of the biceps brachii in a 25 year-old female with work-related shoulder injury. Axial T1-weighted fat-suppressed (left), coronal oblique T1-weighted (middle), and sagittal oblique T1-weighted fat-suppressed MR arthrographic images demonstrate a second tendinous structure(arrowhead) located anterior to the LHBT(arrow) within the bicipital groove. The accessory tendon can be followed superiorly along a different course than the LHBT into the region of the anterior supraspinatus.
Function
The biceps functions primarily as a flexor and supinator at the elbow. The function of the LHB tendon at the shoulder remains controversial and unclear. Because the biceps muscle spans two joints, the functional contributions of the LHBT at the shoulder are difficult to isolate. Both cadaveric and electromyographic studies suggest a range of functions served by the LHBT. Mainly through cadaveric studies the LHBT has been variably characterized as a depressor of the humeral head, an anterior stabilizer, a posterior stabilizer, a limiter of external rotation, a lifter of the glenoid labrum, and a head compressor of the shoulder. Earlier electromyographic studies have attributed a relatively weak abduction force to the LHB at the shoulder16, while more recent studies have shown that when elbow and forearm motion are eliminated, there is virtually no activity in the long head of the biceps tendon with motion at the shoulder17,18. These latter findings suggest a passive role of the LHBT with motion at the shoulder in the absence of loading from forearm or elbow activity17. A subsequent study by Youm, et al. supports the role of activity at the elbow in loading the LHBT and confirmed earlier cadaveric studies by demonstrating that progressively loading the long head of the biceps tendon centers the humeral head on the glenoid surface and decreases anterior-posterior and superior-inferior translation, while limiting internal and external rotation19. Additional studies demonstrate an increased role for the LHBT as a glenohumeral joint stabilizer in the presence of rotator cuff tears and in the presence of glenohumeral instability20,21.
Clinical Findings
Symptoms
Symptoms of LHBT pathology are variable. The usual presentation is pain over the anterior shoulder and the bicipital groove. Often the pain is poorly localized or vague, and the clinical presentation is commonly complicated by other shoulder pathology including rotator cuff injury, impingement, and shoulder instability. Pain may occur at rest or be worse at night, and may radiate into the biceps muscle and distally into the radial aspect of the hand. Overhead activities may exacerbate symptoms. Rarely, the patient may experience a “clunk” with shoulder abduction and rotation with an unstable LHBT2. Rupture of the LHBT is usually noticed as an audible pop, often with immediate resolution of previous anterior shoulder pain22.
Physical Exam
Physical examination is unreliable in the diagnosis of LHBT pathology. With dislocations, pain and tenderness are more medial over the lesser tuberosity. The dislocated tendon may also be palpable. With tendon rupture, distal retraction of the long head of the biceps muscle and tendon result in the characteristic “Popeye” deformity with accompanying ecchymosis, if acute. Provocative tests for LHBT pathology include Yergason’s, Speed’s, uppercut, bear hug, belly press, O’Brien’s, anterior slide, and dynamic labral shear tests. Kibler et al. demonstrated through regression analysis that the combination of Speed’s test and the uppercut test were best at clinically detecting biceps pathology23. Speed’s test is positive when bicipital groove pain is reproduced with resisted forward flexion of the shoulder with the elbow fully extended, and the forearm fully supinated. A positive upper cut test occurs when the patient experiences pain or a painful pop over the anterior shoulder while trying to perform a boxing uppercut punch against resistance with the elbow flexed to 90 degrees, the forearm supinated, and the patient making a fist23.
Pathogenesis
Various schemes have been proposed to classify LHBT injuries with no clearly unified classification system. The difficulties in categorizing LHBT injuries arise because more than one type of tendon lesion may be present at the same time and in more than one tendon location, and additional shoulder pathology is common. Furthermore, coexisting shoulder pathology may be related to LHBT pathology or may be incidental24. LHBT injury has been broadly classified into intrinsic tendon degeneration, mechanical causes including instability, and traumatic causes2. Other authors have classified biceps lesions based on the underlying pathologic process and the status of the biceps tendon. Despite these different classification schemes, injury of the LHBT is commonly multifactorial22, and a practical approach is to classify LHBT pathology based on location.
Intra-articular LHBT injuries include injuries at the origin of the LHBT or within the rotator interval. SLAP tears can undermine the biceps tendon or extend into the biceps tendon. Injuries of the LHBT at the rotator interval may result from the repetitive mechanical stresses of internal and external impingement. Subluxation and dislocation of the LHBT occur with damage to the biceps pulley, and are most commonly associated with tears of the subscapularis and supraspinatus tendons. All of these factors contribute to tendinosis and tears of the LHBT.
Extra-articular LHBT pathology occurs in the bicipital groove from mechanical insults to the LHBT associated with subluxation, dislocation, and constriction of the bicipital groove and results in tenosynovitis, tendinosis, and LHBT tears.
SLAP tears
SLAP tears have been more fully discussed in a previous Web Clinic. Certain SLAP tears may undermine or extend into the LHBT. Type II lesions consist of superior labral fraying with stripping of the labrum undermining the attached biceps tendon. Type IV SLAP tears consist of a bucket handle tear of the superior labrum with tear extension into the biceps tendon. The more recently described Type X lesion consists of a superior labral tear extending into the SGHL. In addition SLAP tears are also associated with rotator interval lesions and medial biceps pulley lesions25,26.
Subluxation and Dislocation of the Long Head of the Biceps Tendon
The structures that contribute to intra-articular stability of the long biceps tendon include the glenoid labrum and capsuloligamentous structures of the glenohumeral joint, the structures of the rotator interval including the coracohumeral and superior glenohumeral ligaments, and the supraspinatus and subscapularis tendons. Extra-articular structures that contribute to LHBT stability include the transverse humeral ligament, the pectoralis major muscle and tendon, and the bicipital groove. The role of the transverse humeral ligament, once thought to be a major contributor to stability of the LHBT, has been deemphasized. Instead, increasing focus has been placed on the role of the biceps pulley mechanism in maintaining LHBT stability.
Conceptually, the biceps pulley mechanism is composed of fibers from the superior glenohumeral and coracohumeral ligaments with contributions from the subscapularis and supraspinatus tendons. This complex attaches at the lesser and greater tuberosities forming a sling around the LHBT as it enters the bicipital groove and acting as a pulley to buttress the LHBT medially as it undergoes a bend to enter the bicipital groove. The primary medial stabilizers are the medial limbs of the superior glenohumeral and coracohumeral ligaments and the subscapularis tendon. Recent anatomic and histologic studies emphasize the importance of the superior insertion of the subscapularis tendon in preventing medial LHBT instability27,28. Arai et al demonstrated a tendinous slip that extends superiorly from the insertion of the superior-most intramuscular tendon of the subscapularis which extends deep to the LHBT and inserts into the fovea capitis of the humerus, represented by a somewhat flattened region superior to the lesser tuberosity and deep to the path of the LHBT. This anatomic configuration serves to lengthen the channel of the LHBT superiorly from the intertubercular groove. The SGHL attaches to this tendinous slip and is interposed between the LHBT and the subscapularis tendon and helps to prevent anteromedial displacement of the LHBT27. Because of the close proximity and interdigitation of the structures that contribute to the biceps pulley, stability is affected by nearby tears of the bordering subscapularis and supraspinatus tendons that extend to involve structures of the biceps pulley29,30.
Not surprisingly, subscapularis tears are most commonly associated with LHBT instability. Direct injuries of the rotator interval and biceps pulley may also be caused by acute trauma, repetitive microtrauma, and degenerative change2. Traumatic injury of the rotator interval and biceps pulley mechanism may result from a fall on an outstretched arm in combination with full external or internal rotation, a fall backward on the hand or elbow, or direct anterior impact31. Anterosuperior impingement has also been proposed as a mechanism of superior subscapularis and pulley mechanism injury32.
The initial findings of biceps instability are subtle, depicted by only minor displacement or shift of the LHBT within the bicipital groove and may be difficult to demonstrate by imaging or arthroscopy. Subluxation results from more severe displacement of the biceps tendon but with continued contact with the bicipital groove. With dislocation, the long biceps tendon loses all contact with the bicipital groove. Several classifications have been proposed for patterns of biceps instability. Walch described 4 types of biceps dislocations29. Bennett proposed 5 patterns of biceps instability33, and Habermeyer1 described 4 types of biceps pulley lesions leading to subluxation and dislocation of the LHBT.
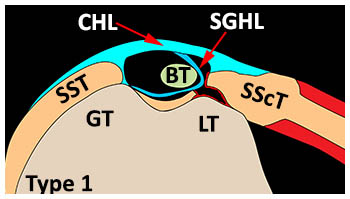
A more recent modification of the Habermeyer system incorporates 6 patterns of tendon instability which can be grouped into the categories of tendon displacement or subluxation, extra-articular dislocation, and intra-articular dislocation24:
Figure 13:
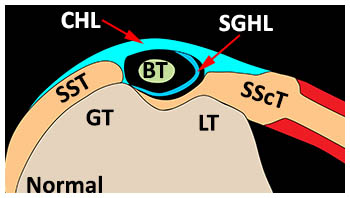
(Adapted from Resnick24) Normal: Graphic depicting the biceps pulley region from an oblique axial perspective, perpendicular to the course of the LHBT just superior and medial to the bicipital groove. The coracohumeral ligament (CHL) is the most superficial layer of the biceps pulley mechanism and extends over the subscapularis (SScT) and supraspinatus (SST) tendons. The superior glenohumeral ligament fuses with the CHL laterally and forms a ligament layer between the biceps tendon (BT) and the superior-most inserting subscapularis tendon (SScT) at the lesser tuberosity (LT).
Figure 16:
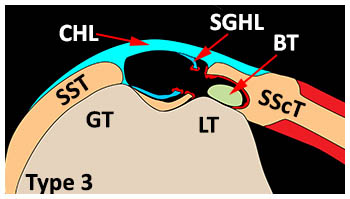
Type III: Extra-articular tendon dislocation-tears of the medial ligaments and subscapularis tendon. A partial intrasubstance tear of the subscapularis tendon allows the biceps tendon to dislocate medially without entering the joint because of intact deep fibers of the subscapularis tendon.
Figure 17:
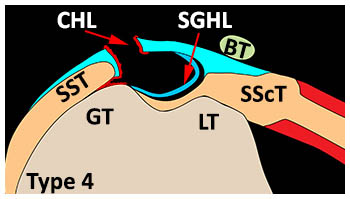
Type IV: Extra-articular tendon dislocation-tears of the lateral limbs of the ligaments with an intact subscapularis tendon. The biceps tendon dislocates anteriorly becoming located anterior to the intact subscapularis tendon. This pattern has a high association with partial or full-thickness tears of the supraspinatus tendon. Although a full-thickness tear of the subscapularis is not required for this pattern, partial articular-sided, bursal-sided, and interstitial tears may be seen.
Figure 18:
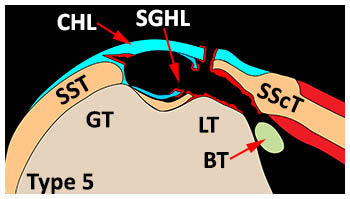
Type V: Intra-articular tendon dislocation-Tears of the medial and lateral limbs of the coracohumeral and superior glenohumeral ligaments with a full-thickness tear of the subscapularis allows medial dislocation of the LHBT into the joint. Most commonly the superior subscapularis tendon demonstrates a full-thickness tear while the lower portion of the tendon remains attached along the inferior portion of the lesser tuberosity and surgical neck. The course of the LHBT moves from a dislocated intra-articular position superiorly to an extra-articular location anterior to the intact subscapularis fibers inferiorly.
Figure 19:
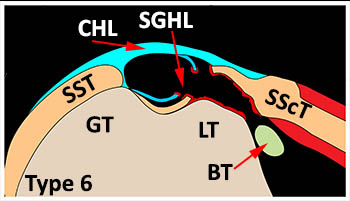
Type VI: Intra-articular tendon dislocation-tear of the medial limbs of the ligaments and detachment of the subscapularis from the lesser tuberosity. Bridging fibers from the subscapularis to the greater tuberosity remain intact. Medial dislocation of the biceps tendon remains deep to the subscapularis and enters the glenohumeral joint.
Although the classification of biceps instability provides valuable information regarding pathogenesis, at present this information results in little modification of the clinical decision-making and surgical approach to treating the unstable LHBT. Attempts at repair of the biceps pulley injury have met with limited success, and since there are few surgical options, most of these patients undergo tenodesis or tenotomy of the LHBT and repair of the associated rotator cuff tendon pathology.
MRI findings
Dislocation
The MRI diagnosis of a dislocated long biceps tendon is typically straightforward. Axial MR images demonstrate an empty bicipital groove. The dislocated tendon may be seen anterior to the subscapularis tendon (20a), within an intratendinous tear of the subscapularis tendon (21a), or deep to the subscapularis tendon in an intra-articular location (22a). Sequential axial images help confirm the structure as the LHBT, and utilizing the orthogonal sagittal oblique or coronal oblique views, the descending portion of the displaced LHBT can frequently be identified. A rare presentation of posterior dislocation of the LHBT (23a,24a) may be seen associated with anterior glenohumeral dislocations and with fractures of the greater tuberosity.
Figure 20:
44 year-old male with chronic shoulder pain. Axial proton density-weighted fat-suppressed images at the upper (left) and mid (right) bicipital groove demonstrate extra-articular dislocation of the LHBT(arrow) anterior to the subscapularis(SScT) which remains attached at the lesser tuberosity associated with tear of the supraspinatus extending into the coracohumeral ligament at the lateral aspect of the biceps pulley(arrowheads).
Figure 21:
55 year-old female with chronic shoulder pain. Axial proton density-weighted fat-suppressed image at the upper margin of the lesser tuberosity (left) and sagittal oblique T2-weighted FSE medial to the bicipital groove at the level of the lesser tuberosity (right) images demonstrate intratendinous dislocation of the LHBT. The LHBT (arrowhead) is medially dislocated into an intrasubstance tear of the superiorly inserting subscapularis tendon (arrow). On the sagittal oblique view, the subscapularis tendon tear is seen as a lack of tendon inserting at the upper margin of the lesser tuberosity(blue line). The remaining intact fibers of the subscapularis tendon (asterisk) prevent intra-articular dislocation of the LHBT.
Figure 22:
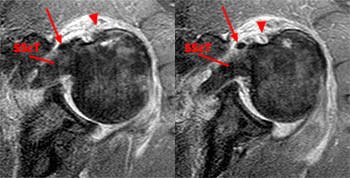
68 year-old male with recent fall. Axial proton density-weighted fat-suppressed image (left) at the upper margin of the bicipital groove demonstrates a full-thickness tear of the superior subscapularis tendon (arrow) that allows intra-articular dislocation of the LHBT (arrowhead). The coronal T2-weighted fat-suppressed image through the anterior humeral head (middle image) demonstrates medial displacement of the LHBT (arrowhead). A sagittal T2-weighted FSE image (left), the LHBT (arrowhead)can be seen extending anteriorly and distally passing anterior to the remaining intact more inferiorly inserting subscapularis (asterisk) to resume a more normal course.
Figure 23:
45 year-old man with recent fall and shoulder dislocation. Axial proton density-weighted fat-suppressed images at the level of the bicipital groove(left) and at the proximal humeral shaft (right) demonstrate absence of the LHBT anteriorly along it normal course(asterisks). The LHBT is identified at the posterior aspect of the humeral head and at the posterior lateral aspect of the proximal humeral shaft (arrowheads).
Subluxation
Subluxation is much more subtle and difficult to demonstrate, not only with MRI and MRI arthrography, but also at arthroscopy. Axial images at the level of the superior bicipital groove are useful in detecting subluxation by demonstrating medial displacement of the LHBT over the lesser tuberosity. Care must be taken to ensure that the MR image being evaluated is the superior-most cut through the lesser tuberosity demonstrating a convex contour. Immediately above the lesser tuberosity the humeral contour becomes more flattened and at this level the normal medial course of the LHBT should not be confused with subluxation. It is in this region however, that very small tears of the superior-most subscapularis tendon insertion may be seen. Small tears of the superior subscapularis may be identified on T2-weighted images as small fluid-containing tendon defects at the medial margin of the biceps pulley offering a clue to potential biceps pulley injury and LHBT instability (25a). Anterior and inferior displacement of the LHBT on sagittal oblique MR arthrogram images (displacement sign) has been proposed to identify early evidence for LHBT instability and tear of the biceps pulley34.
MRI arthrography is better suited for directly visualizing the biceps pulley anatomy and structures of the rotator interval because of the ability to distend and displace the rotator interval structures away from the glenohumeral joint. Interruption and irregularity of the superior glenohumeral ligament, coracohumeral ligament and subtle alterations in the position of the LHBT on sagittal images are helpful in identifying subtle biceps pulley tears (26a). Commonly associated abnormalities include tears of the superior subscapularis tendon which extend to involve the medial limb of the biceps pulley and tears of the anterior supraspinatus which may extend into the lateral aspect of the biceps pulley(27a)33. MR arthrography may depict contrast extending beyond the confines of the anterior joint capsule or along the footprint of the subscapularis over the lesser tuberosity35.
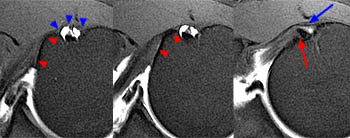
Figure 25:
Sagittal oblique T2-weighted FSE image medial to the bicipital groove at the lesser tuberosity (left), Axial proton density-weighted fat-suppressed image at the superior aspect of the bicipital groove (middle), coronal oblique T2-weighted fat-suppressed image just anterior to the humeral head. A small tear of the superior most inserting subscapularis tendon (arrows) allows mild intratendinous subluxation of the LHBT (arrowheads). Thickening and edema of the coracohumeral ligament (asterisk) are suspicious for coexistent adhesive capsulitis.
Figure 27:
T1-weighted fat-suppressed MR arthrographic images in the coronal oblique (left and middle) and axial (right) imaging planes in a 46 year-old female with chronic shoulder pain. Contrast extends into the subdeltoid bursa (asterisk) indicating communication across a rotator cuff or rotator interval defect. A linear focus containing contrast (arrow) is demonstrated at the anterior aspect of the supraspinatus tendon (SST) insertion near its junction with the biceps pulley. The axial image confirms a small articular-sided partial thickness tear of the supraspinatus at the far anterior insertion (arrow) with an adjacent tear of the lateral limb of the coracohumeral ligament (arrowheads) allowing contrast extension into the subdeltoid bursa. The LHBT (BT) is normally positioned.
Tendon Degeneration
Tendon degeneration or tendinosis encompasses a range of histopathologic changes within the tendon that can occur at any level. The LHBT is subjected to traction, pressure, friction, and shearing forces along its intra- and extra-articular course36, and the effects are hastened in the setting of overuse and instability. In addition, tendon quality may be affected by systemic diseases and aging37. Repetitive mechanical stresses associated with anatomic narrowing may be seen distally within the bicipital groove. Impingement beneath the acromion and the coracoacromial arch may occur with flexion, and this process may be accelerated with thinning or absence of the intervening rotator cuff3. Repetitive traction as is seen in overhead sports may account for the proximal tendon degenerative changes seen at the biceps anchor and may represent precursors to SLAP lesions3. Although degenerative changes within the LHBT are most commonly mechanical in origin, a consistently hypovascular zone of the LHB tendon is found 1.2-3 cm from the tendon origin at the margin of 2 vascular territories5, which may also contribute to tendon degeneration.
Initially, microscopic tears of the tendon occur, and the healing response results in disorganization of collagen fibers and an increase in ground substance. Eventually, macroscopic changes in the tendon occur with loss of the normal glistening surface. If unchecked, repetitive stresses progress to tendon fibrillation, tendon hypertrophy or attenuation, macroscopic partial tears, and eventual complete rupture (28a). An accompanying tenosynovitis representing peritendinous inflammation may be seen. This is frequently brought about by lesions within the bicipital groove, such as a narrowed bicipital groove or may be seen with younger individuals associated with overuse. Because the LHBT sheath communicates with the glenohumeral joint, fluid surrounding the LHBT in the bicipital groove may reflect tenosynovitis or fluid extension from a glenohumeral joint effusion.
On MR, tendon degeneration or tendinosis is diagnosed on the basis of changes in diameter and signal alteration. These signal changes are often subtle and may be mimicked by partial volume averaging and magic-angle artifacts. Tendon thickening, flattening, and a reduced caliber are all reliably associated with tendon degeneration. However, a lack of diameter change does not exclude the presence of tendon degeneration. Tendinosis may result in increased T1, T2, and proton-density weighted signal changes, or the tendon may demonstrate normal signal (29a). Tendon signal alteration is less consistently related to degeneration, likely in part due to magic angle phenomenon and partial volume artifact related to the curved and oblique course of the tendon over the humeral head and into the intertubercular sulcus. Magic angle artifact is most common just before the entrance of the tendon into the intertubercular groove where the tendon and collagen fibers are closest to the magic angle of 55 degrees relative to the main magnetic field. Magic angle artifact typically involves a short segment of the LHBT with well-defined increased signal on short TE images. In contrast,T2-weighted images demonstrate normal signal at the corresponding locations of the tendon38.
Severe hypertrophy of the intra-articular portion of the LHBT, most often accompanying a rotator cuff tear, may result in entrapment of the tendon within the joint because the tendon diameter is too large to slide freely through the intertubercular sulcus leading to a loss of passive elevation of the humerus and bicipital groove tenderness. This condition has been coined the hourglass biceps (30a). At arthroscopy, the hypertrophied tendon can be seen to buckle in the joint with forward elevation of the arm with the elbow extended39.
Figure 30:
This 74 year-old male presented with a massive rotator cuff of the supraspinatus and infraspinatus tendons. Coronal oblique T2-weighted fat-suppressed (left), sagittal oblique T2-weighted FSE (middle), and axial proton density-weighted fat-suppressed (right) images depict a severely thickened intra-articular LHBT with heterogeneous increased signal typical for an "hour-glass biceps".
Tenosynovitis typically demonstrates a fluid distended tendon sheath that is out of proportion to the amount of fluid in the glenohumeral joint and is best depicted on axial proton density or T2-weighted sequences.
Tendon Tears
The normal LHBT can withstand a high tensile force of 667 to 890 newtons40,41. Consequently, rupture of a healthy biceps tendon is extremely rare. Instead, partial and complete tears of the LHBT are usually associated with underlying tendon pathology such as tendon degeneration. Additional shoulder pathologies that contribute to weakening of the tendon include external and internal impingement syndromes, rotator cuff tears, SLAP tears, and tendon instability.
Partial and complete tears of the LHBT typically occur along a hypovascular segment of the LHBT found 1.2-3 cm from the tendon origin extending from the intra-articular portion of the tendon at the mid humeral head level into the superior portion of the intertubercular sulcus5. A subset of patients has been identified that present with shoulder pain and an often isolated subtle partial tear of the LHBT just proximal to the bicipital groove. This particular LHBT injury has been named the “groove entry lesion”42. Because of magic angle artifact prevalent at this portion of the LHBT, these injuries are most reliably depicted on T2-weighted, long TE sequences. Complete rupture of the LHBT is most common in males aged 50 and older43 and most commonly occurs in the bicipital groove or just proximal to the goove24. LHBT injuries account for 96% of all biceps brachii injuries including the distal tendon at the elbow and the short head43. A complete rupture of the LHBT is commonly accompanied by a “Popeye” deformity, a characteristic bulge over the anterior lateral aspect of the proximal arm that results from distal retraction of the LHB tendon and muscle. Frequently complete rupture may relieve pain associated with pre-existing tendinosis or a partial LHBT tear. Because of frequent pre-existing LHBT pathology, complete rupture may occur from relatively minor trauma.
Failure of the biceps tendon in young patients is rare. Complete failure of the biceps at the biceps anchor has been reported in weightlifters44. Rupture at the LHBT musculotendinous junction has also been seen in weightlifters and correlated with anabolic steroid use24. Transection of the long and short head muscle bellies has been reported in military parachutists resulting from forced abduction of the arm against a static line45. A dramatic presentation of displacement of the proximal biceps muscle has been reported in wakeboarders when a slackened towrope suddenly becomes taut while being gripped with flexed elbows. The sudden force ruptures the proximal heads of the biceps muscle and the extreme recoil displaces the proximally torn muscle distally into the volar subcutaneous soft tissues of the forearm beyond the attached distal biceps tendon41,46. This phenomenon was described as “slingshot displacement of the biceps brachii muscle”. Biceps muscle resection may be necessary in these injuries because of delayed presentation and associated devascularization and denervation of the displaced muscle41,46.
Partial tendon tears are depicted by an abrupt, often severe reduction in tendon caliber and irregularity of the tendon contour. Intratendinous increased T2 signal may be seen within partial tears (31a). Intrasubstance delamination tears appear as longitudinally oriented intratendinous increased signal on fluid-sensitive sequences. Complete tears of the biceps are indicated by absence of tendon within the bicipital groove (32a). Careful inspection of the images confirms that the tendon is not dislocated. With acute ruptures edema tracks distally ventral to the proximal humerus. The retracted irregular long biceps tendon is frequently identified in this region outlined by T2 hyperintense signal
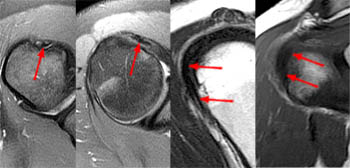
Figure 31:
Axial proton density-weighted fat-suppressed images through the bicipital groove (left) and just inferior to the bicipital groove (right) demonstrate partial tears of the LHBT. The LHBT is medially subluxed with a thinned and flattened contour and subtle intrinsic linear signal consistent with a partial tear. The alteration of the tendon signal is more apparent in the image on the right, however this partial tear likely lies beyond the region of tendon that can be evaluated at arthroscopy.
Figure 32:
Fat-suppressed axial proton density-weight images at the level of the bicipital groove (left) and distal to the bicipital groove (middle) and fat-suppressed T2-weighted coronal oblique view (right) in a 51 year-old male complaining of swelling and bruising in the upper arm after feeling a pop with heavy lifting 2 weeks prior. The bicipital groove is empty with no biceps tendon (arrowhead). A thickened and edematous LBT (arrows) is identified anterior to the humerus at a level distal to the bicipital groove outlined by surrounding mild edema. An irregular tear of the superior glenoid labrum is also demonstrated (short arrow).
Arthroscopy
Visualization of the subscapularis tendon and its footprint on the lesser tuberosity is best performed through a posterior viewing portal. Abduction and internal rotation of the arm allows visualization of the subscapularis insertion and footprint47. The 70 degree arthroscope allows improved visualization of the bicipital groove and subscapularis insertion. Nevertheless, a persistent blind spot for the arthroscopist is the LHBT within the bicipital groove. 3-5 cm of the LHBT can be pulled into the joint and inspected during arthroscopy, allowing only partial visualization of the tendon in the groove48. Lesions within the distal bicipital groove and beyond will not be seen. MRI allows preoperative assessment of the LHBT within and distal to the bicipital groove.
Treatment
Initial management of patients with symptoms attributed to the LHBT begin with nonoperative therapies including modification of activity, nonsteroidal anti-inflammatory medication, and physical therapy focused on any coexisting underlying shoulder pathology. Steroid injections into the glenohumeral joint or directly into the bicipital tendon sheath at the bicipital groove may be utilized.
For patients presenting with a cosmetic deformity from LHBT rupture, biceps muscle spasm is common initially with resolution of pain and spasm after 6-8 weeks, with little residual dysfunction of the LHBT49,50. However more recent studies suggest that the nonoperative treatment of LHBT rupture may not be completely benign, especially in younger patients. Long term follow-up in these patients revealed decreased elbow flexion strength of 8-29% and a decrease in forearm supination strength of 21-23% with continued complaints of pain or disability51,52.
Surgical treatment is necessary for patients with LHBT pathology that remain symptomatic after nonoperative therapeutic measures. Repair of concomitant impingement, rotator cuff tears, and labral pathology is performed in conjunction with a tenodesis or tenotomy of the LHBT. The indications for tenodesis or tenotomy for biceps tendon injuries include partial tears of the long head of the biceps tendon affecting greater than 25-50% of the tendon diameter, longitudinal tears affecting tendon gliding in the bicipital groove, medial subluxation of the tendon, disruption of the biceps sling, and pain associated with subscapularis tears, massive rotator cuff tears, shoulder arthroplasty, and some SLAP tears49.
Evidenced-based studies are limited in the current literature in regards to the efficacy of tenotomy versus tenodesis of the LHBT. In general, tenotomy is recommended for older patients who are more sedentary, patients with obese arms, or patients unconcerned with cosmesis. Tenodesis is recommended for young (<40 year-old) physically active patients with thin arms or for those with concern for cosmesis. Tenotomy can be performed arthroscopically by transecting the LHBT at the superior labrum or supraglenoid tubercle, allowing the tendon to retract distally and out of the glenohumeral joint and into the bicipital groove. In the setting of an hourglass tendon, the intra-articular portion of the tendon is resected to allow distal retraction.
Further debate has centered on the proper location and method of performing a tenodesis. Tenodesis may be performed arthroscopically or as an open procedure depending on the site of fixation. Reattachment sites include fixation to the lesser tuberosity, coracoid, and bicipital groove, transverse humeral ligament, short head of the biceps, and pectoralis major tendon. Fixation may be provided by interference screws, suture anchors, or soft tissue suture fixation.
Conclusion
Pathology of the long head of the biceps (LHB) tendon is a frequent cause of pain. While injuries of the long biceps tendon can be the result of a single traumatic event, they most often occur due to repetitive microtrauma and degeneration. Damage of the supporting biceps pulley mechanism leads to LHBT instability and is most closely associated with subscapularis tendon tears. Because the detection of LHBT pathology is frequently nonspecific by physical examination and may be difficult to identify with shoulder arthroscopy, LHBT injuries may be overlooked during arthroscopic repairs of rotator cuff and labral tears, leading to poor outcomes and necessitating additional surgery. MRI offers the best imaging option for detecting the varied manifestations of biceps tendon pathology and helps to evaluate the adjacent frequently injured shoulder structures.
References
1 Habermeyer P, Magosch P, Pritsch M, Scheibel MT, Lichtenberg S. Anterosuperior impingement of the shoulder as a result of pulley lesions: a prospective arthroscopic study. J. Shoulder Elb. Surg. 2004;13(1):5-12. Available at: http://linkinghub.elsevier.com/retrieve/pii/S1058274603002568.
2 Ahrens PM, Boileau P. The long head of biceps and associated tendinopathy. J. Bone Joint Surg. Br. 2007;89:1001-1009.
3 Refior H, Sowa D. Long tendon of the biceps brachii: sites of predilection for degenerative lesions. J. Shoulder Elb. Surg. 1995;4(6):436-440. Available at: http://www.sciencedirect.com/science/article/pii/S1058274605800357.
4 Denard PJ, Dai X, Hanypsiak BT, Burkhart SS. Anatomy of the biceps tendon: implications for restoring physiological length-tension relation during biceps tenodesis with interference screw fixation. Arthroscopy. 2012;28(10):1352-8. Available at: http://www.ncbi.nlm.nih.gov/pubmed/22925883.
5 Cheng NM, Pan W-R, Vally F, Le Roux CM, Richardson MD. The arterial supply of the long head of biceps tendon: Anatomical study with implications for tendon rupture. Clin. Anat. 2010;23(6):683-692.
6 Alpantaki K, McLaughlin D, Karagogeos D, Hadjipavlou A, Kontakis G. Sympathetic and sensory neural elements in the tendon of the long head of the biceps. J. Bone Joint Surg. Am. 2005;87:1580-1583.
7 Morag Y, Bedi A, Jamadar D a. The rotator interval and long head biceps tendon: anatomy, function, pathology, and magnetic resonance imaging. Magn. Reson. Imaging Clin. N. Am. 2012;20(2):229-59, x. Available at: http://www.ncbi.nlm.nih.gov/pubmed/22469402.
8 Wittstein J, Lassiter Jr. T, Taylor D. Aberrant origin of the long head of the biceps: a case series. J Shoulder Elb. Surg. 2012;21(3):356-360. Available at: http://www.ncbi.nlm.nih.gov/pubmed/21835645.
9 Gardner E, Gray D. Prenatal development of the human shoulder and acromioclavicular joints. Am. J. Anat. 1953;92:219-76. Available at: http://onlinelibrary.wiley.com/doi/10.1002/aja.1000920203/abstract.
10 Franco JC, Knapp TP, Mandelbaum BR. Congenital absence of the long head of the biceps tendon. A case report. J. Bone Joint Surg. Am. 2005;87(7):1584-6. Available at: http://www.ncbi.nlm.nih.gov/pubmed/15995127.
11 SMITH E, MATZKIN E. Congenital absence of the long head of the biceps brachii tendon as a VATER association. Am. J. …. 2002;31(8):452-454. Available at: http://cat.inist.fr/?aModele=afficheN&cpsidt=13907526.
12 Mariani P, Bellelli A, Botticella C. Arthroscopic absence of the long head of the biceps tendon. Arthrosc. J. Arthrosc. Relat. Surgery… J. Arthrosc. Relat. …. 1997;13(4):499-501. Available at: http://www.sciencedirect.com/science/article/pii/S0749806397901304.
13 Warner J, Paletta G, Warren R. Accessory head of the biceps brachii: case report showing clinical relevance. Clin Orthop Relat Res. 1992;(280):179-181.
14 Nakatani T, Tanaka S, Mizukami S. Bilateral four-headed biceps brachii muscles: The median nerve and brachial artery passing through a tunnel formed by a muscle slip from the accessory head. Clin. Anat. 1998;11:209-212. Available at: http://onlinelibrary.wiley.com/doi/10.1002/(SICI)1098-2353(1998)11:3<209::AID-CA10>3.0.CO;2-N/abstract.
15 Gheno R, Zoner CS, Buck FM, et al. Accessory head of biceps brachii muscle: anatomy, histology, and MRI in cadavers. AJR. Am. J. Roentgenol. 2010;194(1):W80-3. Available at: http://www.ncbi.nlm.nih.gov/pubmed/20028895.
16 Furlani J. Electromyographic study of the m. biceps brachii in movements at the glenohumeral joint. Acta Anat. (Basel). 1976;96:270-284.
17 Levy AS, Kelly BT, Lintner S a, Osbahr DC, Speer KP. Function of the long head of the biceps at the shoulder: electromyographic analysis. J. Shoulder Elbow Surg. 2001;10(3):250-5. Available at: http://www.ncbi.nlm.nih.gov/pubmed/11408907.
18 Yamaguchi K, Riew KD, Galatz LM, Syme JA, Neviaser RJ. Biceps activity during shoulder motion: an electromyographic analysis. Clin. Orthop. Relat. Res. 1997;(336):122-9. Available at: http://www.ncbi.nlm.nih.gov/pubmed/9060495.
19 Youm T, ElAttrache N, Tibone J. The effect of the long head of the biceps on glenohumeral kinematics. J. Shoulder …. 2009;18(1):122-9. Available at: http://www.ncbi.nlm.nih.gov/pubmed/18799325.
20 Su W-R, Budoff JE, Luo Z-P. The effect of posterosuperior rotator cuff tears and biceps loading on glenohumeral translation. Arthroscopy. 2010;26(5):578-86. Available at: http://www.ncbi.nlm.nih.gov/pubmed/20434653.
21 Kim S-H, Ha K, Kim H-S, Kim S. Electromyographic activity of the biceps brachii muscle in shoulders with anterior instability. Arthrosc. J. Arthrosc. Relat. Surg. 2001;17(8):864-868. Available at: http://www.arthroscopyjournal.org/scripts/om.dll/serve?action=searchDB&searchDBfor=art&artType=abs&id=a0170864.
22 Snyder GM, Mair SD, Lattermann C. Tendinopathy of the long head of the biceps. Med. Sport Sci. 2012;57:76-89. Available at: http://www.ncbi.nlm.nih.gov/pubmed/21986047.
23 Ben Kibler W, Sciascia AD, Hester P, Dome D, Jacobs C. Clinical utility of traditional and new tests in the diagnosis of biceps tendon injuries and superior labrum anterior and posterior lesions in the shoulder. Am. J. Sports Med. 2009;37(9):1840-7. Available at: http://www.ncbi.nlm.nih.gov/pubmed/19509414.
24 Resnick D, Kang HS, Pretterklieber M. Shoulder. In: Internal Derangement of Joints. 2nd ed. Philadelphia: Saunders Elsevier; 2007:713-1122.
25 Walch G, Nove-Josserand L, Levigne C, Renaud E. Tears of the supraspinatus tendon associated with “hidden” lesions of the rotator interval. J. Shoulder Elbow Surg. 1994;3(6):353-60. Available at: http://www.ncbi.nlm.nih.gov/pubmed/22958839.
26 Bennett WF. Correlation of the SLAP lesion with lesions of the medial sheath of the biceps tendon and intra-articular subscapularis tendon. Indian J. Orthop. 2009;43(4):342-346.
27 Arai R, Mochizuki T, Yamaguchi K, et al. Functional anatomy of the superior glenohumeral and coracohumeral ligaments and the subscapularis tendon in view of stabilization of the long head of the biceps tendon. J. Shoulder Elbow Surg. 2010;19(1):58-64. Available at: http://www.ncbi.nlm.nih.gov/pubmed/19535271.
28 Arai R, Sugaya H, Mochizuki T, Nimura A, Moriishi J, Akita K. Subscapularis tendon tear: an anatomic and clinical investigation. Arthroscopy. 2008;24(9):997-1004. Available at: http://www.ncbi.nlm.nih.gov/pubmed/18760206.
29 Walch G, Nové-Josserand L, Boileau P, Levigne C. Subluxations and dislocations of the tendon of the long head of the biceps. J. Shoulder Elb. Surg. 1998;7(2):A1. Available at: http://www.jshoulderelbow.org/article/S1058-2746(98)70004-7/abstract.
30 Nho SJ, Strauss EJ, Lenart BA, et al. Long head of the biceps tendinopathy: diagnosis and management. J. Am. Acad. Orthop. Surg. 2010;18:645–656.
31 Baumann B, Genning K, Böhm D. Arthroscopic prevalence of pulley lesions in 1007 consecutive patients. J. Shoulder …. 2008;17(1):14-20. Available at: http://www.ncbi.nlm.nih.gov/pubmed/17931909.
32 Gerber C, Sebesta a. Impingement of the deep surface of the subscapularis tendon and the reflection pulley on the anterosuperior glenoid rim: a preliminary report. J. Shoulder Elbow Surg. 2000;9(6):483-90. Available at: http://www.ncbi.nlm.nih.gov/pubmed/11155300.
33 Bennett WF. Subscapularis, medial, and lateral head coracohumeral ligament insertion anatomy. Arthrosc. J. Arthrosc. Relat. Surg. 2001;17(2):173-180. Available at: http://linkinghub.elsevier.com/retrieve/pii/S0749806301670750.
34 Schaeffeler C, Waldt S, Holzapfel K, et al. Lesions of the biceps pulley: diagnostic accuracy of MR arthrography of the shoulder and evaluation of previously described and new diagnostic signs. Radiology. 2012;264(2):504-513. Available at: http://www.ncbi.nlm.nih.gov/pubmed/22692037.
35 Morag Y, Jacobson JA, Shields G, et al. MR arthrography of rotator interval, long head of the biceps brachii, and biceps pulley of the shoulder. Radiology. 2005;235(1):21-30. Available at: http://radiology.rsna.org/content/235/1/21.short.
36 Joseph M, Maresh CM, McCarthy MB, et al. Histological and molecular analysis of the biceps tendon long head post-tenotomy. J. Orthop. Res. 2009;27(10):1379-1385.
37 Abate M, Silbernagel KG, Siljeholm C, et al. Pathogenesis of tendinopathies: inflammation or degeneration? Arthritis Res. Ther. 2009;11(3):235. Available at: http://www.biomedcentral.com/content/pdf/ar2723.pdf.
38 Buck F, Grehn H. Degeneration of the long biceps tendon: comparison of MRI with gross anatomy and histology. Am. J. …. 2009;193(5):1367-1375. Available at: http://www.ncbi.nlm.nih.gov/pubmed/19843755.
39 Boileau P, Ahrens PM, Hatzidakis AM. Entrapment of the long head of the biceps tendon: the hourglass biceps-a cause of pain and locking of the shoulder. J. Shoulder Elb. Surg. 2004;13(3):249-257. Available at: http://linkinghub.elsevier.com/retrieve/pii/S1058274604000187.
40 Curtis A, Snyder S. Evaluation and treatment of biceps tendon pathology. Orthop. Clin. North Am. 1993;24:33-43. Available at: http://www.ncbi.nlm.nih.gov/pubmed/8421614.
41 Moorman III C, Silver S, Potter H, Warren R. Proximal Rupture of the Biceps Brachii with Slingshot Displacement into the Forearm. A Case Report*. J. Bone Jt. Surg. Case Connect. 1996;78(11):1749-52. Available at: http://caseconnector.jbjs.org/article.aspx?articleID=33392.
42 Gaskin CM, Anderson MW, Choudhri A, Diduch DR. Focal partial tears of the long head of the biceps brachii tendon at the entrance to the bicipital groove: MR imaging findings, surgical correlation, and clinical significance. Skeletal Radiol. 2009;38(10):959-65. Available at: http://www.ncbi.nlm.nih.gov/pubmed/19533121.
43 Carter AN, Erickson SM. Proximal biceps tendon rupture: primarily an injury of middle age. Phys. Sportsmed. 1999;27(6):95-101.
44 Cope M, Ali A, Bayliss N. Biceps rupture in bodybuilders: Three case reports of rupture of the long head of the biceps at the tendon-labrum junction. J. shoulder Elb. Surg. 2004;13(5):580-582. Available at: http://linkinghub.elsevier.com/retrieve/pii/S1058274604000898.
45 Heckman JD, Levine MI. Traumatic closed transection of the biceps brachii in the military parachutist. J. Bone Joint Surg. Am. 1978;60(3):369-72. Available at: http://www.ncbi.nlm.nih.gov/pubmed/649641.
46 Pascual-Garrido C, Swanson BL, Bannar SM. Closed proximal muscle rupture of the biceps brachii in wakeboarders. Knee Surgery, Sport. Traumatol. Arthrosc. 2012;20(6):1019-1021.
47 Lo IKY, Burkhart SS. The comma sign: An arthroscopic guide to the torn subscapularis tendon. Arthroscopy. 2003;19(3):334-7. Available at: http://www.ncbi.nlm.nih.gov/pubmed/12627163.
48 Favorito PJ, Harding WG, Heidt RS. Complete arthroscopic examination of the long head of the biceps tendon. Arthrosc. J. Arthrosc. Relat. Surg. 2001;17(4):430-432. Available at: http://linkinghub.elsevier.com/retrieve/pii/S0749806301163620.
49 Khazzam M, George MS, Churchill RS, Kuhn JE. Disorders of the long head of biceps tendon. J Shoulder Elb. Surg. 2012;21(1):136-145. Available at: http://www.ncbi.nlm.nih.gov/pubmed/22005126.
50 Carroll R, Hamilton L. Rupture of biceps brachii—a conservative method of treatment. J Bone Jt. Surg Am. 1967;49:1016. Available at: http://scholar.google.com/scholar?hl=en&btnG=Search&q=intitle:Rupture+of+biceps+brachii.+a+conservative+method+of+treatment.#0.
51 Mariani E, Cofield R, Askew L. Rupture of the tendon of the long head of the biceps brachii surgical versus nonsurgical treatment. Clin. Orthop. Relat. Res. 1988;228:233-9. Available at: http://journals.lww.com/corr/Abstract/1988/03000/Rupture_of_the_Tendon_of_the_Long_Head_of_the.36.aspx.
52 Deutch SR, Gelineck J, Johannsen HV, Sneppen O. Permanent disabilities in the displaced muscle from rupture of the long head tendon of the biceps. Scand. J. Med. Sci. Sports. 2005;15(3):159-62. Available at: http://onlinelibrary.wiley.com/doi/10.1111/j.1600-0838.2004.00421.x/full.