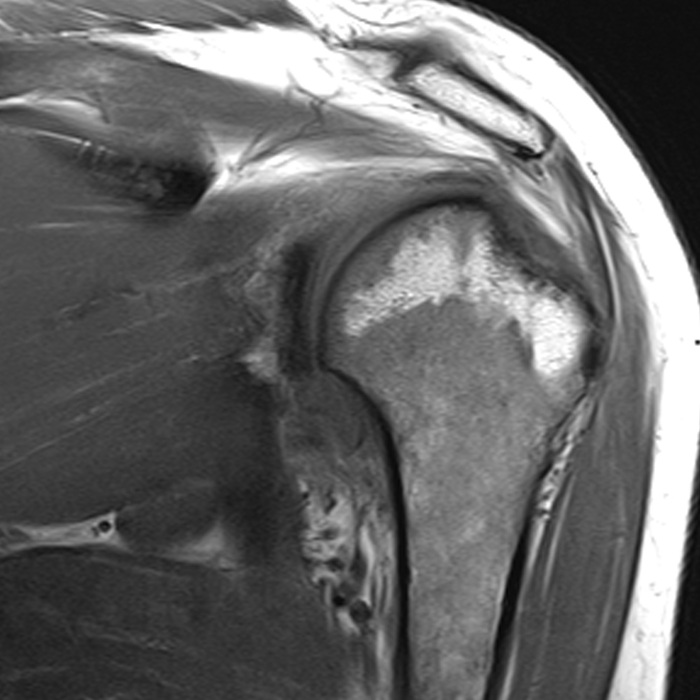
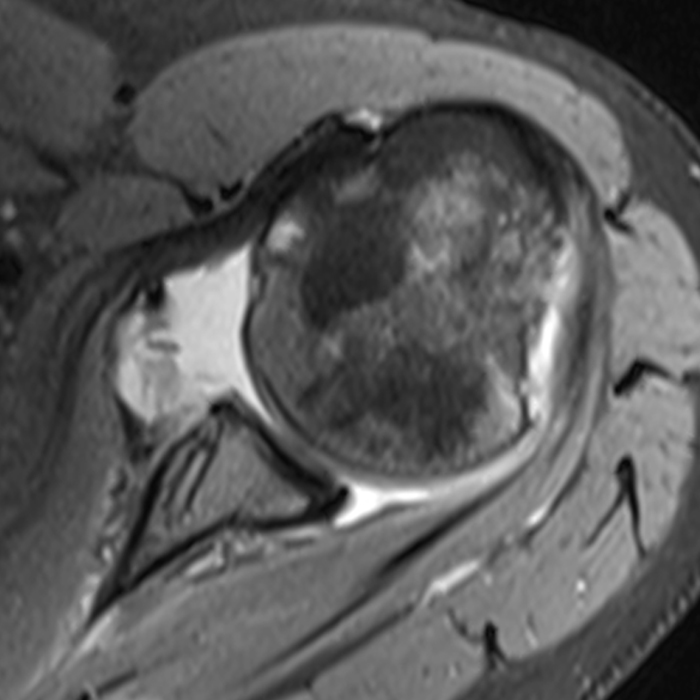
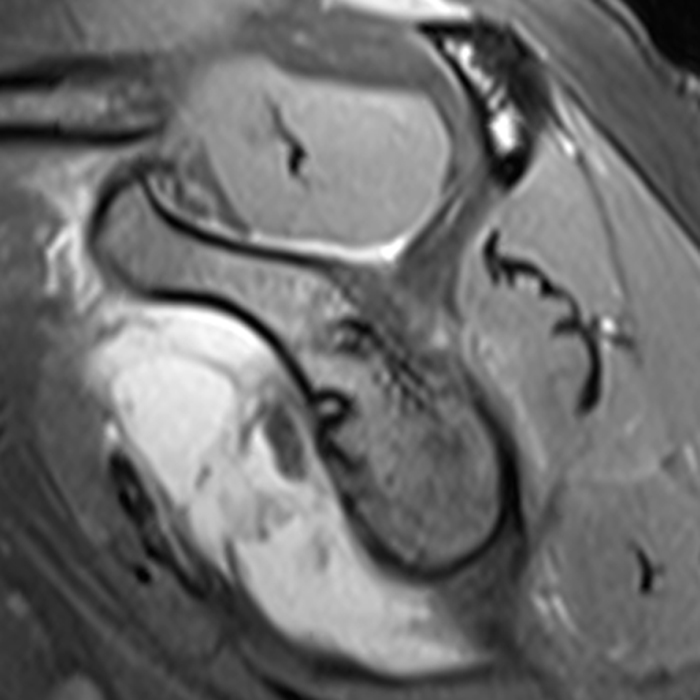
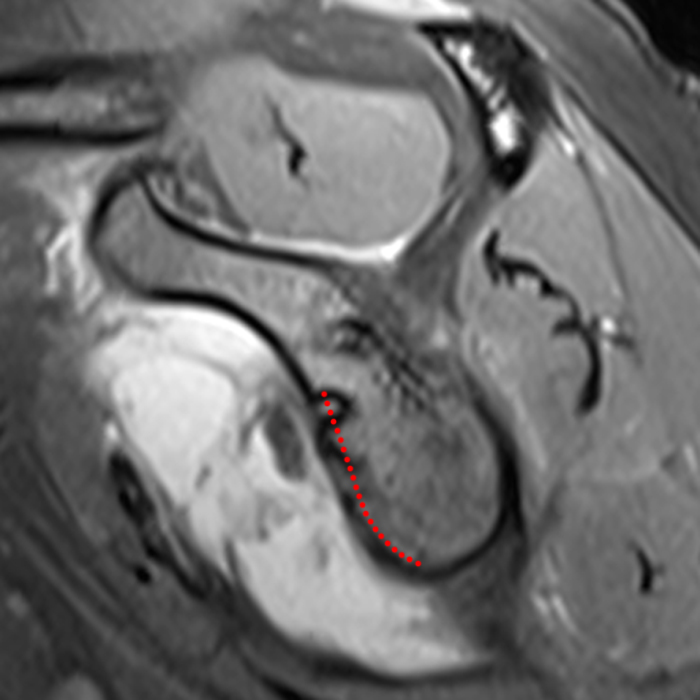
Clinical History: A 36 year-old female with a history of shoulder instability and prior surgery presents after suffering a recurrent dislocation. (1A) T1-weighted coronal, and (1B,C) fat-suppressed proton density-weighted axial and sagittal images are provided. What are the findings? What is your diagnosis?
Findings
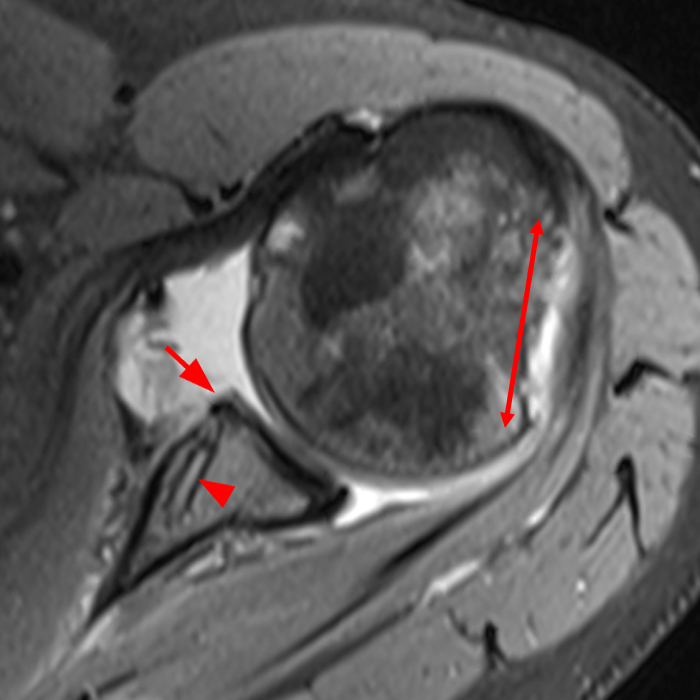
Figure 2:
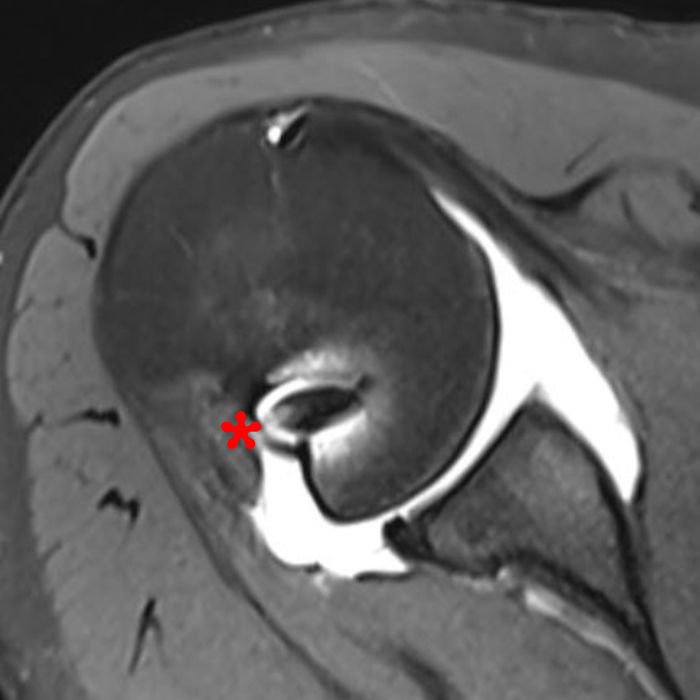
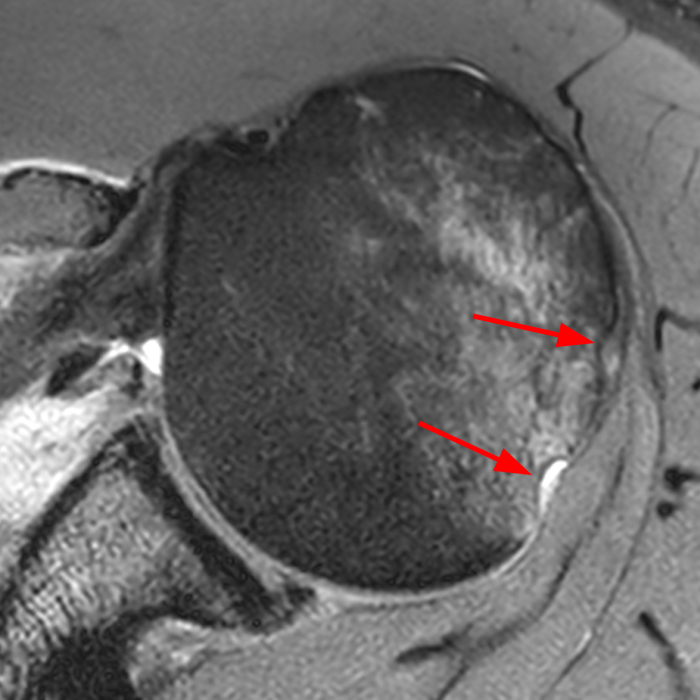
The (2A) T1-weighted coronal image through the posterior shoulder demonstrates an impaction deformity (arrow) at the posterolateral humeral head compatible with a Hill-Sachs lesion. The (2B) axial fat-suppressed proton density weighted image reveals an anchor tract compatible with prior labral repair (arrowhead) with virtually no normal residual labral tissue at the anterior glenoid (short arrow). The large size of the Hill-Sachs lesion (red line) is readily apparent. On the corresponding (2C) fat-suppressed proton density-weighted sagittal image, the glenoid is noted to be abnormally small with loss of bone stock along the anterior-inferior glenoid (dotted line).
Diagnosis
Status post recurrent anterior dislocation with an engaging, off-track Hill-Sachs lesion.
Introduction
The shoulder has the greatest range of motion of any human joint, and this requires a degree of natural instability. As a result, the shoulder is the most commonly dislocated joint in adults. Recurrent dislocations of the shoulder are not uncommon, and surgeons have long recognized that anteroinferior glenoid bone loss is associated with recurrent dislocations.1 It has been stated that a bony defect of one-third to one-fourth of the glenoid width requires repair to address the defect, as simply performing a soft tissue repair in such patients results in an unacceptable rate of recurrent dislocations.2,3
The other osseous abnormality commonly found following shoulder dislocation is the Hill-Sachs lesion, found in greater than two thirds of initial dislocations and approaching 100% in patients with recurrent dislocation.4,5 This lesion forms following anterior shoulder dislocation as the anterior glenoid causes a compression fracture at the posterolateral humeral head.6 It has been recognized that large or medially placed Hill-Sachs lesions are associated with recurrent anterior instability.7,8
Our understanding of the impact of osseous deformities following shoulder dislocation has evolved. In 2000, Burkhart and De Beer discussed the need to assess the relationship between glenoid bone loss and Hill-Sachs lesions, and how potential engagement of the abnormalities impact the surgical approach.9 In 2007, Yamamoto et al. refined our understanding of this relationship with the introduction of the concept of the glenoid track, and described how measurement of glenoid bone loss and its relationship to the size of a Hill-Sachs lesion can be used to predict the risk of recurrent dislocation.10
The Glenoid Track
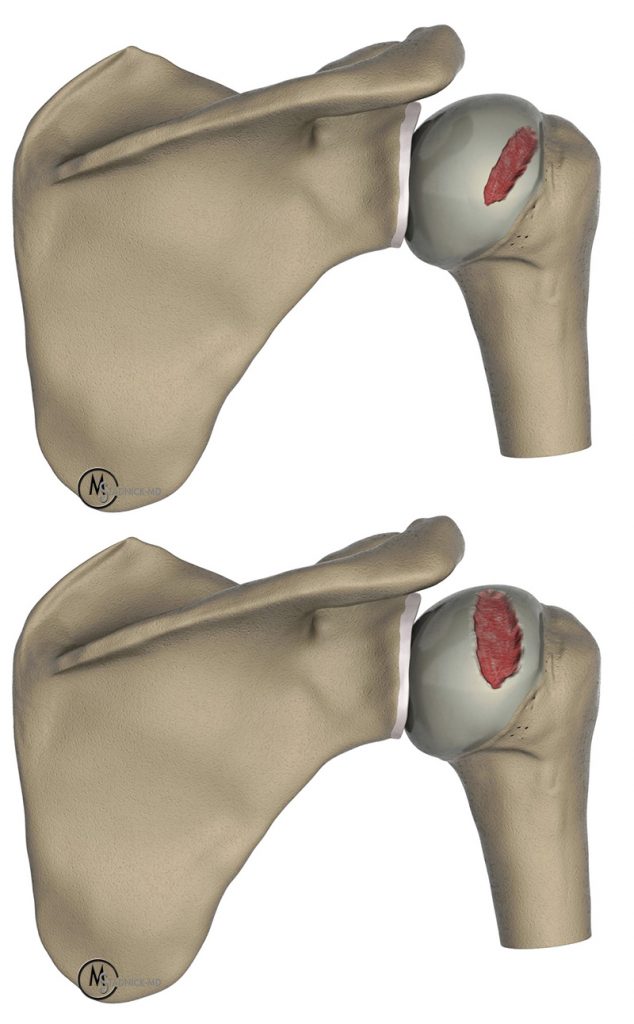
Yamamoto et al. described the glenoid track as the zone of contact between the glenoid and humeral head that occurs as the arm is elevated, moving from neutral position to full abduction, extension, and external rotation (Figure 3). As the shoulder transitions through this motion, the contact of the glenoid shifts from the inferomedial articular surface of the humeral head to the superolateral articular surface. In normal shoulders without bone loss, the intact track results in a stable shoulder. Using cadaveric shoulders, they determined that the glenoid track could be calculated as 84% of AP glenoid width, subsequently modified to 83% in a study of live shoulders.11
The concept of the glenoid track allowed Yamamoto et al to assess the risk of a Hill-Sachs lesion overriding the anterior glenoid rim in abduction, resulting in engagement (Figure 4). In patients with anterior glenoid bone loss after dislocation, the amount of bone loss must be subtracted from 83% of the glenoid width. This measurement is then compared to the Hill-Sachs interval, calculated by determining the width of the Hill-Sachs lesion from its medial aspect to the rotator cuff insertion, typically including an intact bone bridge between the cuff insertion and the lateral margin of the Hill-Sachs lesion. If the Hill-Sachs interval is larger than the glenoid track, the lesion is off-track and likely to engage, whereas if the interval is smaller than the glenoid track, it is on-track and unlikely to engage. Off-track lesions have a much higher incidence of recurrent instability and require a different surgical approach than on-track lesions. Most importantly, this concept recognizes that bone loss following shoulder dislocation is a bipolar process, and though glenoid bone loss and Hill-Sachs lesions may independently predict recurrent instability, it is the relationship between the two that is most important in determining the risk of engagement and subsequent recurrent dislocation.
Figure 4 Animation: For an interactive animation of the dislocation mechanism, click on the image, then hold-left click and drag to the right. The animation demonstrates the motion of the shoulder as it goes into abduction, extension, and external rotation. At the endpoint of this motion, the Hill-Sachs lesion is seen to engage with the anterior glenoid rim.
On and off-track imaging
Although initial descriptions of the technique for determining on-track versus off-track lesions depended upon CT, it has subsequently been shown that MRI can be used to accurately assess bipolar bone loss and to predict whether an engaging lesion is present.12 Compared to CT, MRI has the advantages of a lack of ionizing radiation, the ability to concomitantly evaluate soft tissue injuries, and the potential to more accurately measure the Hill-Sachs interval due to the ability to directly visualize the rotator cuff insertion. Further, it has been determined that the measurement of the glenoid track and the Hill-Sachs interval via MRI to determine the risk of engagement is more accurate than dynamic intraoperative assessment, particularly when the dynamic assessment is performed prior to repair, when laxity has not yet been addressed.13 Intraoperative assessment of engagement following surgical stabilization rather than before is likely more accurate, but this approach risks failure of the surgical repair due to the early application of abnormal stress.14
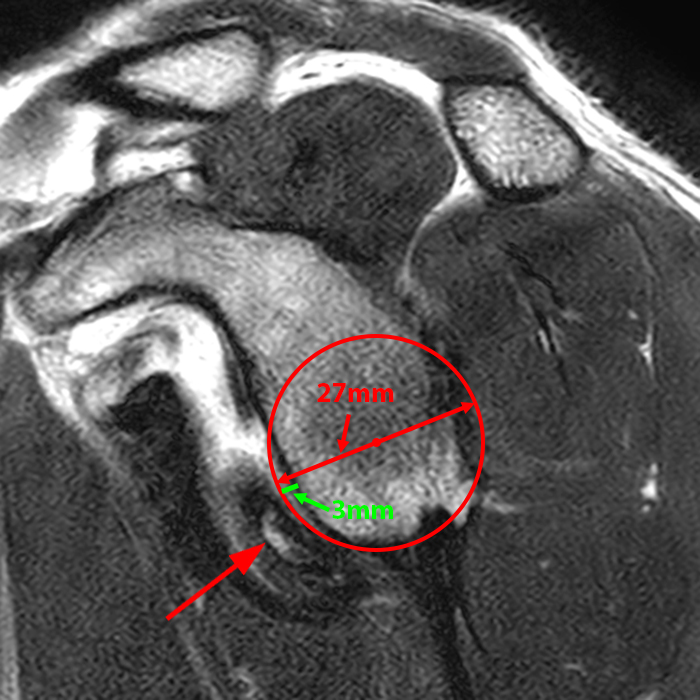
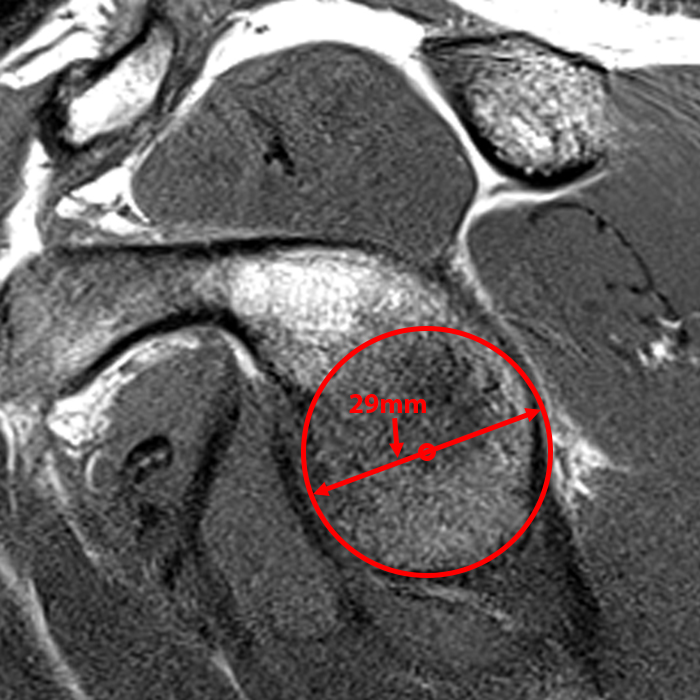
The two key measurements necessary to determine whether a shoulder is likely to engage are the width of the glenoid track and the Hill-Sachs interval. Both are relatively easy to determine with modern PACS systems. Glenoid bone loss is determined using the best fit circle technique (Figure 5).15 A best fit circle is drawn along the posterior and caudal margins of the glenoid. Next, a horizontal line is drawn through the center of the circle, perpendicular to the long axis of the glenoid, estimating the width of the intact glenoid. A second horizontal line at the same level is then measured from the anterior border of the glenoid to the anterior aspect of the circle, indicating the amount of glenoid bone loss. The glenoid track is then calculated as 0.83 x (the width of the intact glenoid) – (the width of glenoid bone loss).
After calculating the glenoid track, the Hill-Sachs interval must then be determined. The Hill-Sachs interval is measured as the width of the Hill-Sachs lesion plus the width of any intact bone bridge between the lateral margin of the lesion and the rotator cuff insertion. From a practical standpoint, this means that one measures from the medial border of the Hill-Sachs lesion to the cuff insertion. The measurement is performed on the axial image demonstrating the greatest medial extent of the Hill-Sachs lesion (Figure 6).
If the Hill-Sachs interval is greater than the glenoid track, the Hill-Sachs lesion is considered off-track, and therefore likely to engage since the lesion will not be entirely covered by the glenoid at the end range of motion. If the lesion measures less than the glenoid track, it should remain covered by the glenoid at end range motion and thus the anterior rim of the glenoid will not engage with the lesion (Figure 7).
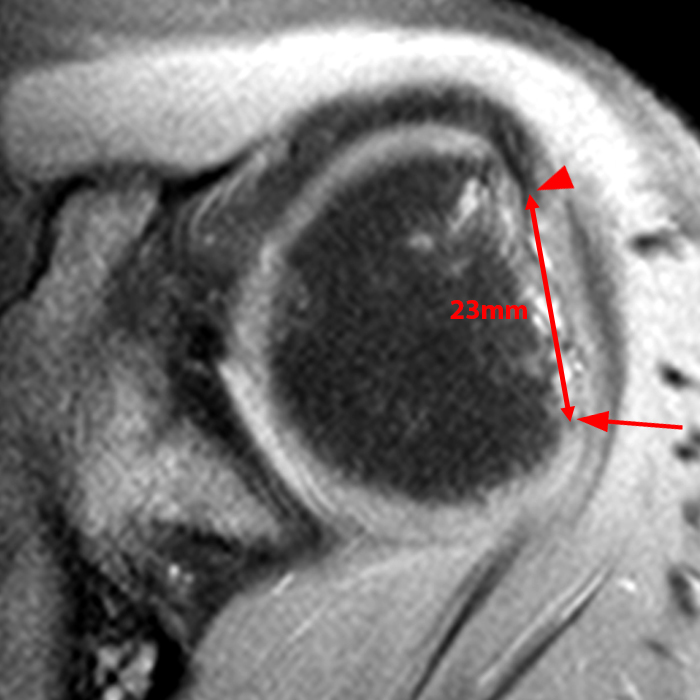
Figure 7:
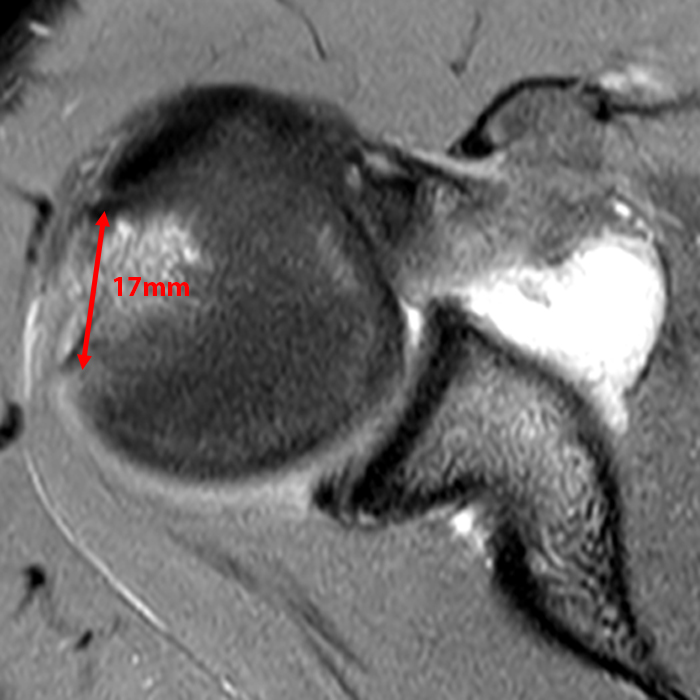
(7A) A T2-weighted sagittal image from a 22 year-old male who dislocated his shoulder playing football is provided. A displaced bony Bankart is present (arrow). The intact glenoid width measures 27mm and the amount of bone loss measures 3mm, which is equivalent to the width of the bony Bankart fragment. The glenoid track thus measures 0.83 x 27 – 3 = 19.4mm. (7B) on the fat-suppressed proton density-weighted axial image demonstrating the most medial extent of the Hill-Sachs lesion, the Hill-Sachs interval measures 17mm, less than the glenoid track, and thus compatible with an on-track, non-engaging lesion. This case demonstrates that even with significant bone loss, a relatively small Hill-Sachs lesion my remain on-track.
There are a variety of morphologies that result in off-track Hill-Sachs lesions. As in the introductory case, when there is significant anterior glenoid bone loss and a large Hill-Sachs lesion, the lesion is almost certain to be off-track. In the absence of significant glenoid bone loss, a large Hill-Sachs lesion may still be off-track, and similarly, a small Hill-Sachs lesion may be off-track if there is substantial glenoid bone loss. Finally, even small Hill-Sachs lesions may be off-track if they are more medially positioned, as more medial lesions result in a larger Hill-Sachs interval (Figure 8).
Figure 8:
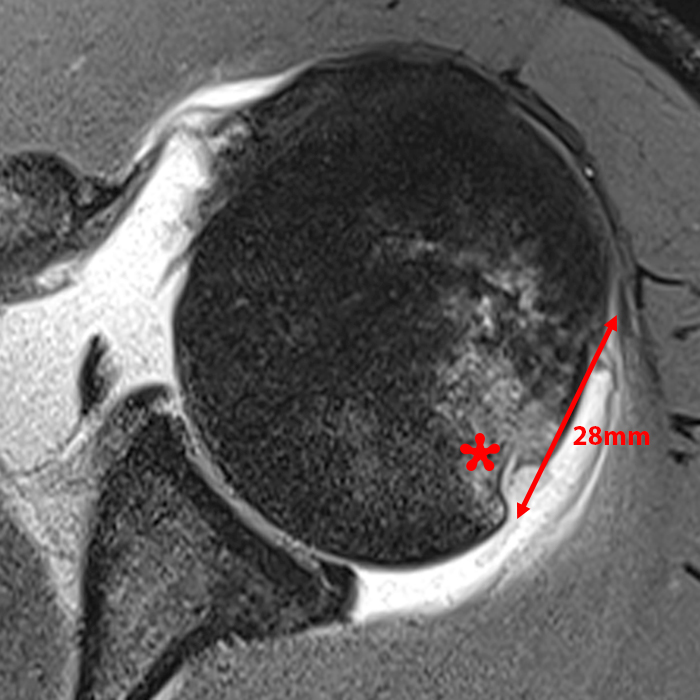
A 24 year-old professional football player dislocated his shoulder in a game. (8A) The T1-weighted sagittal image demonstrates normal glenoid morphology without significant bone loss. The glenoid track is calculated as 24mm. On (8B) the axial proton density-weighted view, a small Hill-Sachs lesion is apparent (asterisk). Though small, the lesion is medially positioned, resulting in a Hill-Sachs interval measurement of 28mm, compatible with an off-track lesion.
Clinical Implications and Treatment of On and Off-Track Lesions
It is now well recognized that bipolar bone loss has an additive and negative effect upon glenohumeral instability.16 Further, off-track lesions have been found to be an important risk factor for recurrent instability and the need for revision surgery after arthroscopic Bankart repair.17 There is increasing recognition that evaluation of the glenoid track status should be a routine component of the diagnostic work-up of anterior instability, and that isolated arthroscopic Bankart repair should not be performed in patients with an unstable, off-track shoulder.18
The two most commonly employed surgical adjuncts to arthroscopic Bankart repair in patients with off-track lesions are arthroscopic remplissage and the Laterjet procedure. Remplissage is the French term for “to fill in”, and was first described by Wolf et al. as an arthroscopic solution for an engaging Hill-Sachs lesion.19 The procedure involves tenodesis of the infraspinatus tendon and posterior capsule to fill the Hill-Sachs lesion (Figure 9). This technique prevents engagement by essentially converting the Hill-Sachs lesion into an extra-articular lesion. The procedure tends to limit external rotation and anterior translation of the humeral head, also lowering the risk of engagement. Remplissage has been found to significantly reduce the incidence of recurrent instability following arthroscopic Bankart repair.20 Because of the limitation of external rotation, it is avoided in patients such as overhead athletes who require full range of motion.
Figure 9:
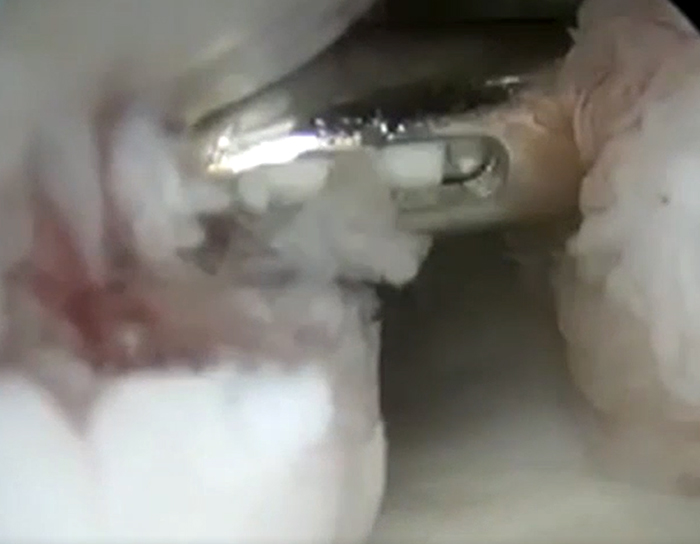
Arthroscopic images demonstrate (9A) anchor placement and (9B) passing of sutures in preparation for remplissage of a large Hill-Sachs lesion. (9C) A postoperative MR arthrographic axial image following remplissage demonstrates filling of the lateral aspect of the Hill-Sachs lesion by the medialized infraspinatus tendon (asterisk), significantly reducing the Hill-Sachs interval. Images courtesy of Matthew Provencher, MD, The Steadman Clinic.
In 1954 Laterjet first described the technique of coracoid process transfer to the anteroinferior glenoid as a treatment for anterior glenohumeral instability21(Figure 10). A portion of the coracoid process and the attached conjoined tendons of the coracobrachialis and short head of the biceps are passed through the subscapularis tendon prior to being secured to the glenoid. The resultant sling formed by the conjoined tendon limits anterior humeral translation during abduction and external rotation, and the coracoid graft acts as a bone block and restores anterior glenoid bone loss.22 The Laterjet procedure is a complex operation that has a higher complication rate than remplissage, but it appears to be the better choice in patients with high collision risk such as contact athletes and in patients with greater glenoid bone loss.23 Patients who undergo the Laterjet procedure typically have excellent long term outcomes with regard to glenohumeral instability. The most common long term complication of the procedure is postoperative arthritis.24
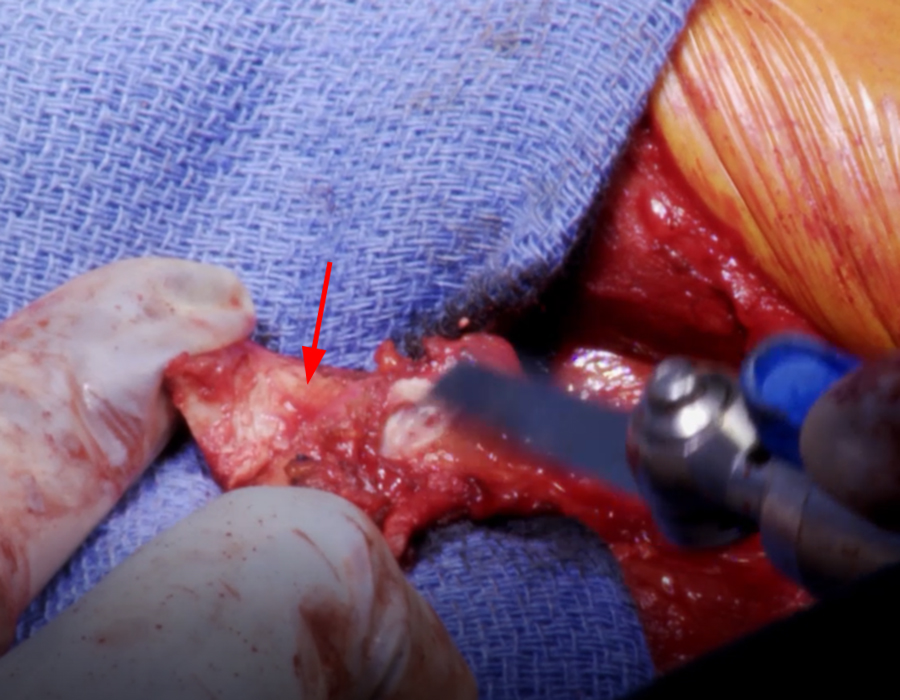
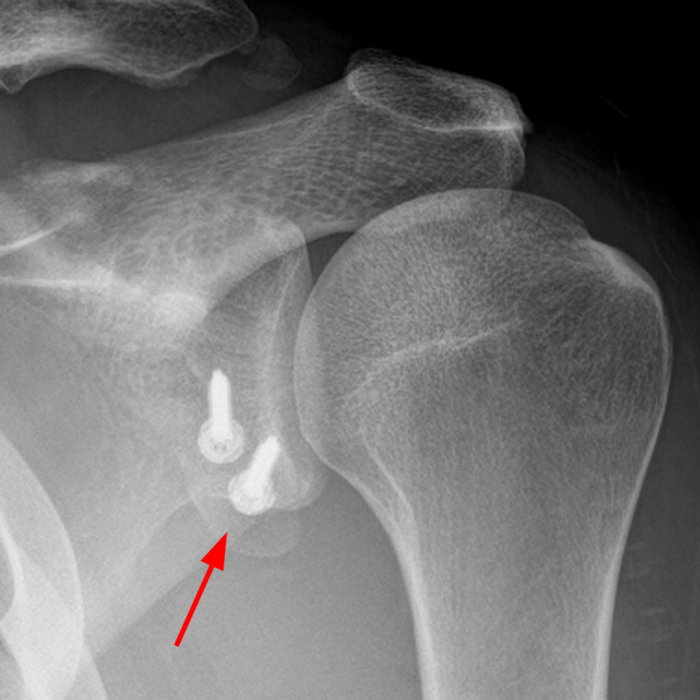
Figure 10:
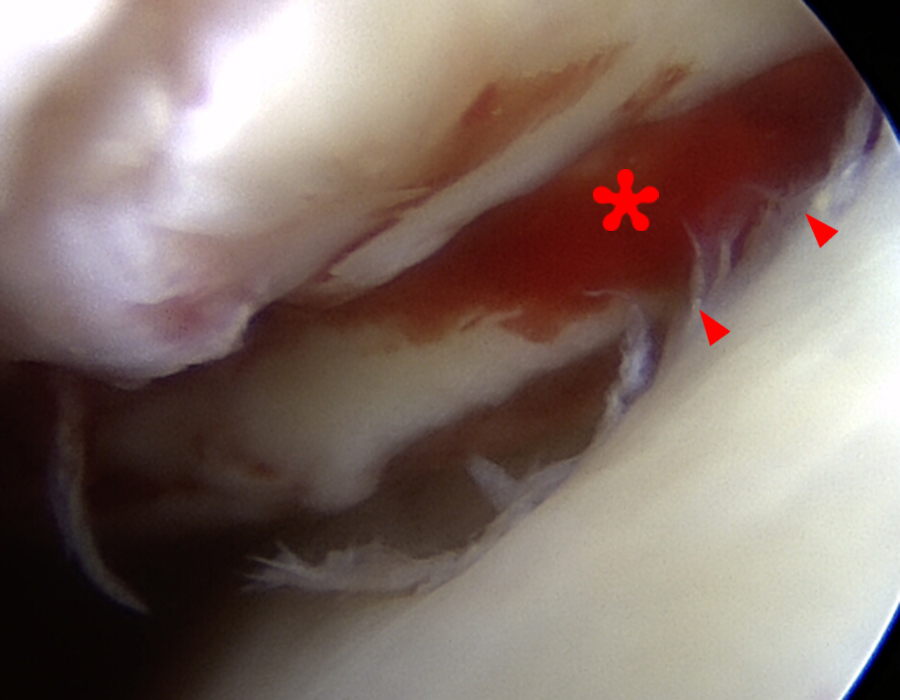
The same professional football player from Figure 8 suffered a recurrent dislocation. (10A) A fat-suppressed proton density-weighted axial image demonstrates enlargement of the Hill-Sachs lesion, which now has a bilobed appearance (arrows). The lesion was off-track. An (10B) arthroscopic view from the posterior portal demonstrates the Hill-Sachs lesion (asterisk) engaging with the anterior glenoid rim (arrows) in abduction and external rotation. (10C) An intraoperative photo demonstrates preparation of the coracoid graft (arrow) prior to its fixation upon the glenoid. (10D) The postoperative radiograph depicts the bone graft (arrow) affixed to the anterior-inferior glenoid. Operative photographs courtesy of Matthew Provencher, MD, The Steadman Clinic.
Itoi describes guidelines to their surgical approach that rely upon evaluation of bone loss and the on-track/off-track status.25 For shoulders that are on-track and with less than 25% glenoid bone loss, he recommends only soft-tissue repair. Remplissage is a reasonable approach for off-track lesions with glenoid bone loss of less than 25%, unless the patient requires full range of motion such as a throwing athlete. With an off-track lesion and greater than 25% bone loss, Laterjet is recommended.
Conclusion
Anterior shoulder instability is a commonly encountered clinical entity, and MRI has long proven valuable in its evaluation. Glenoid bone loss and large Hill-Sachs lesions are known to be associated with a greater risk of recurrent dislocation, but we now recognize that it is the relationship between these bipolar sites of bone loss that is critical in estimating the risk. By determining whether a Hill-Sachs lesion is on-track or off-track, one can predict the likelihood that the lesion will engage in abduction, a status known to be highly correlated to recurrent instability. The astute interpreter of MRI should determine whether a Hill-Sachs lesion is on- or off-track in all cases of anterior shoulder instability. Careful evaluation of this status as well as the extent of glenoid bone loss provides valuable guidance towards the operative approach.
References
- Gerber C, Nyffeler RW. Classification of glenohumeral joint instability. Clin Orthop Relat Res 2002;(400):65-76. ↩
- Matsen FA III, Thomas SC, Rockwood CA Jr, Wirth MA. Glenohumeral instability. In: The Shoulder. Rockwood CA Jr, Matsen FA III, eds. Philadelphia: W. B. Saunders, 1998:611-754. ↩
- Yamamoto N, Muraki T, Sperling JW, et al. Stabilizing mechanism in bone grafting of a large glenoid defect. J Bone Joint Surg (Am) 2010;92-A:2059-2066. ↩
- Yiannakopoulos CK, Mataragas E, Antonogiannakis E. A comparison of the spectrum of intra-articular lesions in acute and chronic anterior shoulder instability. Arthroscopy. 2007;23(9):985–990. ↩
- Welsh MF, Willing RT, Giles JW, Athwal GS, Johnson JA. A rigid body model for the assessment of glenohumeral joint mechanics: influence of osseous defects on range of motion and dislocation. J Biomech. 2016;49(4):514–519. ↩
- Provencher MT, Frank RM, Leclere LE, et al. The Hill-Sachs lesion: diagnosis, classification, and management. J Am Acad Orthop Surg. 2012;20(4):242–252. ↩
- Kurokawa D, Yamamoto N, Nagamoto H, et al. The prevalence of a large Hill-Sachs lesion that needs to be treated. J Shoulder Elbow Surg 2013;22:1285-1289. ↩
- Rowe CR, Zarins B, Ciullo JV. Recurrent anterior dislocation of the shoulder after surgical repair. Apparent causes of failure and treatment. J Bone Joint Surg Am 1984;66:159-68 ↩
- Burkhart SS, Debeer JF. Traumatic glenohumeral bone defects and their relationship to failure of arthroscopic Bankart repairs: significance of the inverted-pear glenoid and the humeral engaging Hill-Sachs lesion. Arthroscopy 2000;16:677-94. ↩
- Yamamoto N, Itoi E, Abe H, et al. Contact between the glenoid and the humeral head in abduction, external rotation, and horizontal extension: A new concept of glenoid track. J Shoulder Elbow Surg 2007;16:649-656. ↩
- Di Giacomo G, Itoi E, Burkhart SS. Evolving concept of bipolar bone loss and the Hill-Sachs lesion: From “engaging/non-engaging” lesion to “on-track/off-track” lesion. Arthroscopy 2014;30:90-98. ↩
- Gyftopoulos S, Beltran LS, Bookman J, Rokito A. MRI evaluation of bipolar bone loss using the on track off-track method: a feasibility study. AJR 2015; 205:848–852. ↩
- Kelkar R, Wang VM, Flatow EL, et al. Glenohumeral mechanics: a study of articular geometry, contact, and kinematics. ↩
- Trivedi S, Pomerantz ML, Gross D, Golijanan P, Provencher MT. Shoulder Instability in the setting of bipolar (glenoid and humeral head) bone loss: the glenoid track concept. ↩
- Sugaya H, Moriishi J, Dohi M, Kon Y, Tsuchiya A. Glenoid rim morphology in recurrent anterior glenohumeral instability. J Bone Joint Surg Am 2003; 85:878–884 ↩
- Arciero RA, Parrino A, Bernhardson AS et al. The effect of a combined glenoid and Hill-Sachs defect on glenohumeral stability: a biomechanical cadaveric study using 3-dimensional modeling of 142 patients. Am J Sports Med. 2015 Jun;43(6):1422-9 ↩
- Locher J, Wilken F, Beitzel K et al. Hill-Sachs Off-track Lesions as Risk Factor for Recurrence of Instability After Arthroscopic Bankart Repair. Arthroscopy. 2016 Oct;32(10):1993-1999 ↩
- Shaha JS, Cook JB, Rowles DJ et al. Clinical Validation of the Glenoid Track Concept in Anterior Glenohumeral Instability. J Bone Joint Surg Am. 2016;98:1918-23 ↩
- Wolf EM, Pollack M, Smalley C. Hill-Sachs “Remplissage:” An arthroscopic solution for the engaging Hill-Sachs lesion. Arthroscopy. 2007; 23(6)e1-e2 ↩
- Purchase RJ, Wolf EM, Hobgood ER, Pollock ME, Smalley CC. Hill-sachs “remplissage”: an arthroscopic solution for the engaging hill-sachs lesion. Arthroscopy 2008 Jun ;24(6):723-6 ↩
- Latarjet M. Treatment of recurrent dislocation of the shoulder. Lyon Chir 1954;49:994-7. ↩
- Yamamoto N, Muraki T, An KN, Sperling JW, Cofield RH, Itoi E, et al. The stabilizing mechanism of the Latarjet procedure: a cadaveric study. J Bone Joint Surg Am 2013;95:1390-7. ↩
- Yang JS, Mehran N, Mazzocca AD et al. Remplissage Versus Modified Latarjet for Off-Track Hill-Sachs Lesions With Subcritical Glenoid Bone Loss. Am J Sports Med. 2018 Jul;46(8):1885-1891. ↩
- Hurley ET, Jamal MS, Ali ZS et al. Long-term outcomes of the Latarjet procedure for anterior shoulder instability: a systematic review of studies at 10-year follow-up. J Shoulder Elbow Surg. 2019 Feb;28(2):e33-e39. ↩
- Itoi E. ‘On-track’ and ‘off-track’ shoulder lesions. EFORT Open Rev. 2017 Aug; 2(8): 343–351. ↩