Clinical History: A 50 year-old female presents with pain along the ulnar side of her distal long finger. (1a) Proton-density weighted coronal, (1b) STIR coronal and (1c) contrast-enhanced fat-suppressed T1-weighted axial images are provided. What are the findings? What is your diagnosis?
Findings
Figure 2:
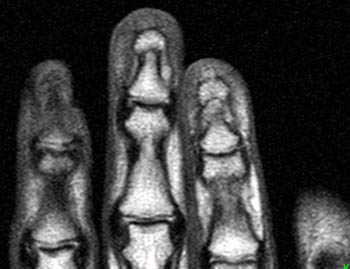
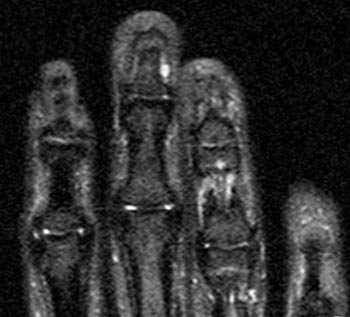
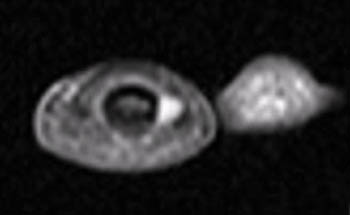
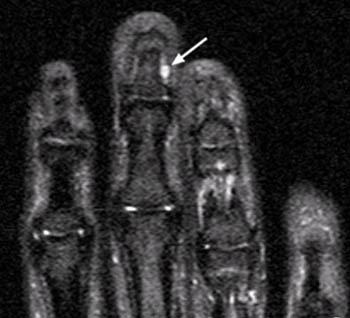
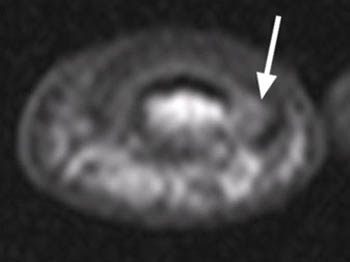
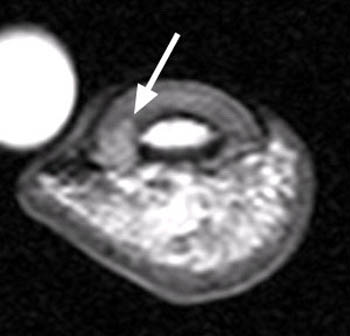
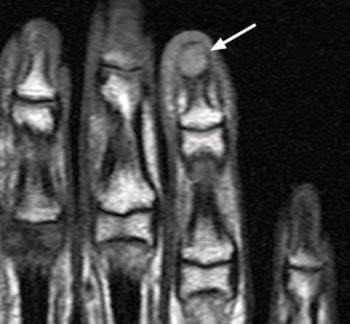
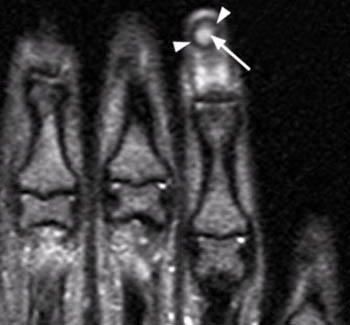
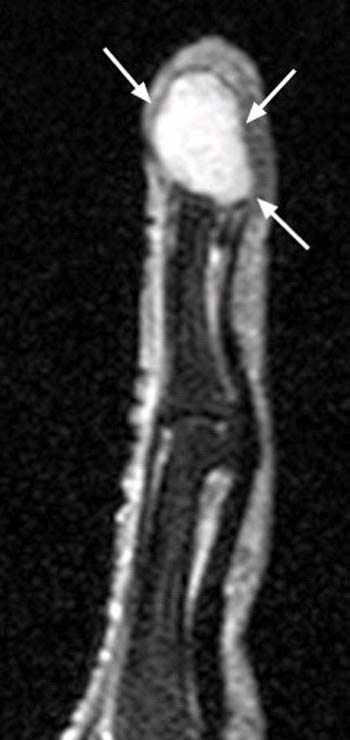
A well-defined nodular lesion (arrows) is evident on the (2a) proton density-weighted and (2b) STIR coronal images of the distal long finger. The abnormality is mildly hyperintense on proton density-weighted images and becomes markedly hyperintense on T2-weighted scans. On T1-weighted images (not shown), the lesion was of diffusely low signal intensity. (2c) Following contrast administration, the abnormality (arrow) demonstrates intense, homogeneous enhancement. The subungual location of the lesion is well-demonstrated on the axial view.
Diagnosis
Glomus tumor.
Introduction
The glomus tumor is one of several characteristic fingertip masses that may be diagnosed with MR imaging. The glomus tumor is actually a hamartoma that arises from the glomus body, an arteriovenous shunt within the dermis that contributes to temperature regulation of the fingers.1 Glomus tumors comprise up to 5% of soft-tissue tumors in the hand,2 and are one of the more common masses to present at the fingertip. These lesions are most common in females in the third and fourth decades.
Clinical Presentation
The classic clinical presentation of a glomus tumor is a triad of fingertip pain, tenderness, and sensitivity to cold. Ridging of the nail bed may be found, and pain may be reproduced by immersing the affected digit in cold water. Another clinical test involves the use of a tourniquet, in which the disappearance of pain after application is virtually diagnostic of a glomus tumor (Hildreth sign).3 Despite these characteristics, delays in diagnosis are not uncommon, with symptoms often being present for several years before an actual diagnosis is made.4 Once the diagnosis is suspected, the tumor may be localized by eliciting pain via the use of focal pressure to areas of suspicion, using a small object such as a straightened paper clip. This maneuver, however, has variable success, and thus in suspected cases MR is invaluable to confirm the presence of a mass and to provide exact localization of the lesion, the latter being necessary to avoid nail dystrophy after surgery.
MR Appearance
On MR imaging, a subungual position is the most common site for a glomus tumor.5 With proper MR technique, tumors less than 2mm in size can be detected and localized. On T1-weighted images, glomus tumors have variable signal characteristics, ranging from low in signal intensity to moderately hyperintense (3a,4a). Hyperintensity within some glomus tumors on T1-weighted images is felt to be due to the presence of hemorrhage or due to the large vascular channels within the mass itself. The high vascularity of glomus tumors also accounts for the typical uniform hyperintensity of these lesions on T2-weighted images, and for the intense enhancement found within these tumors following contrast administration. Indeed, contrast-enhanced MR angiography may be used in these patients to demonstrate the characteristic vascular nidus found within these lesions.6
In our experience, bone erosion or destruction in glomus tumors is less common than pure soft tissue involvement. The literature varies, with the prevalence of bone erosion estimated at 15-65%.7 On MR images, osseous involvement in glomus tumors results in smooth bony expansion (5a,5b), with plain films revealing a sclerotic rim typical for a slow growing process.
Differential Diagnosis
A number of characteristic fingertip lesions may appear similar to a glomus tumor on MR images, including mucous cysts, giant cell tumors of the tendon sheath, and epidermoid inclusion cysts. Mucous cysts are simply a ganglion that arises most commonly at the dorsal aspect of the DIP joint. These lesions should be isointense to fluid on all pulse sequences, and they do not enhance following contrast administration, making the MR exclusion of this diagnosis fairly simple in patients with glomus tumors.
Epidermoid inclusion cysts can appear quite similar to glomus tumors in signal characteristics, being well defined and of homogeneous T2-hyperintensity (6a,6b). Bone expansion is also not uncommon in patients with an epidermoid inclusion cyst (7a,7b). The key to the diagnosis in the patients without osseous involvement is the location of the lesion, as the nail bed is unlikely to be the center of involvement in these patients. Even more important is the clinical history and presentation. Epidermoid inclusion cysts result from prior penetrating trauma, with subsequent proliferation of the implanted dermal elements causing the cyst. In addition, epidermoid inclusion cysts are usually painless, and present due to expansion of the affected digit.
Figure 6:
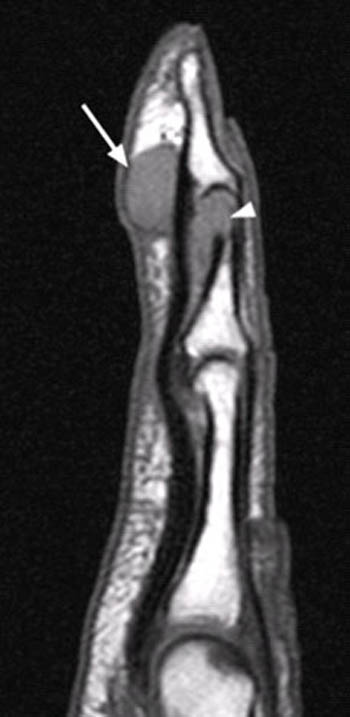
(6a) T1-weighted sagittal and (6b) fat-suppressed proton density-weighted oblique coronal images in a patient with a history of slamming his thumb in a car door reveal a well-circumscribed lesion (arrows) within the subcutaneous fat at the palmar aspect of the thumb tip. This abnormality was found at surgery to represent an epidermoid inclusion cyst.
Figure 7:
(7a) T1-weighted coronal and (7b) fat-suppressed T2-weighted sagittal images in a patient with a history of dog bite to the fingertip reveal an expansile mass causing marked bony expansion (arrows) at the distal phalanx of the finger. Despite this appearance, the abnormality was relatively painless and the patient sought treatment for cosmetic reasons.
Another fingertip lesion that may be confused for a glomus tumor on MR images is the giant cell tumor of the tendon sheath. This is a very common finger lesion, in fact being the most common finger mass other than a ganglion cyst. These lesions are closely related histologically to pigmented villonodular synovitis, and typically present with painless swelling. On MR images (8a,9a), proximity to a tendon sheath is invariably present. The lesions are usually isolated to the soft tissues, but osseous involvement is not uncommon, and if contrast is given, enhancement is typically relatively intense and uniform. These lesions are usually not as hyperintense on T2-weighted images as a glomus tumor. In addition, the presence of hemosiderin is frequently seen, manifested as foci of low signal intensity within the lesion, most pronounced on gradient echo pulse sequences. Recognition of hemosiderin and the characteristic proximity to tendon allows one to make a confident diagnosis of a giant cell tumor in the majority of these patients.
Figure 8:
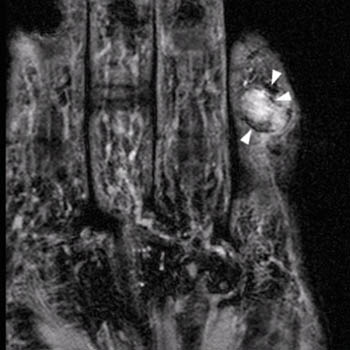
(8a) A T1-weighted sagittal image in a 36 year old patient who presented with painless swelling of the index finger is provided. A palmar soft tissue mass (arrow) adjacent to the flexor tendon demonstrates diffusely intermediate signal intensity. Extension of the process into the distal aspect of the middle phalanx (arrowhead) is also apparent.
Treatment
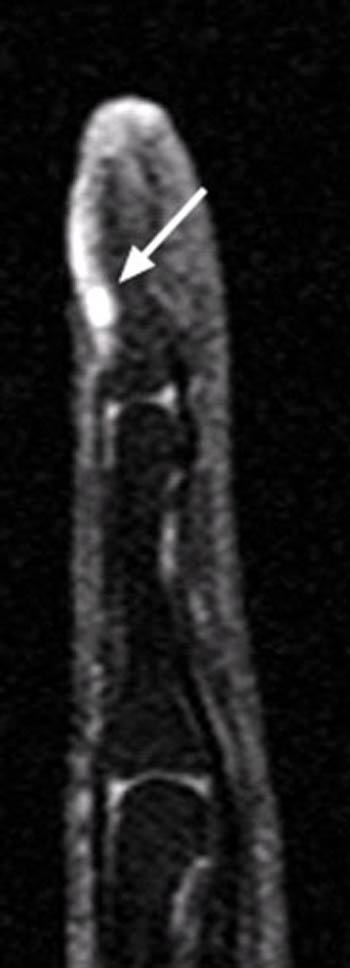
The preferred treatment for a symptomatic glomus tumor is surgical resection, and MR is quite helpful prior to resection in order to localize the lesion and plan the operative approach. The prognosis following resection is excellent, with immediate resolution of pain and a low likelihood of recurrence seen in most patients. If the capsule of a glomus tumor, however, is incompletely resected, recurrence may happen, and in such cases, MR is again useful to localize the recurrent lesions, which are often quite small (10a,11a).
Conclusion
The glomus tumor is a relatively rare yet characteristic abnormality that may present as a fingertip mass. Other fingertip lesions such as mucous cysts, epidermoid inclusion cysts, and giant cell tumors of the tendon sheath may appear similar, but the clinical presentation and specific MR imaging characteristics of the entities usually allow a definitive diagnosis to be made. In patients with glomus tumors, MR provides valuable confirmation and localization of the lesion prior to resection, and is able to visualize the rare recurrence in affected individuals.
References
1 Baran R, Dawber RPR, Tosti A, Haneke E, Bristow I. A text atlas of nail disorders: techniques in investigation and diagnosis, 2nd ed. London, England: Martin Dunitz,1996 : 107-108
2 Drape JL, Idy-Peretti I, Goettmann S, et al. Subungual glomus tumors: evaluation with MR imaging. Radiology1995; 195:507 “51
3 Hildreth DH. The ischemia for glomus tumours: a new diagnostic test. Rev Surg 1970; 27:147-148.
4 Carroll RE, Berman AT. Glomus tumors of the hand: review of the literature and report on 28 cases. J Bone Joint Surg 1972; 54:691-703.
5 Drape JL, Idy-Peretti I, Goettmann S, et al. Subungual glomus tumors: evaluation with MR imaging. Radiology 1995; 195:507-515.
6 Van Ruyssevelt CE, Vranckx P. Subungual glomus tumor: emphasis on MR angiography. AJR 2004; 182:263-264.
7 Resnick D, Kyriakos M, Greenway GD. Tumors and tumor-like lesions of bone: imaging and pathology of specific lesions. In: Resnick D, ed. Diagnosis of bone and joint disorders. 3rd ed. Philadelphia, Pa: Saunders, 1995; 3821-3840.