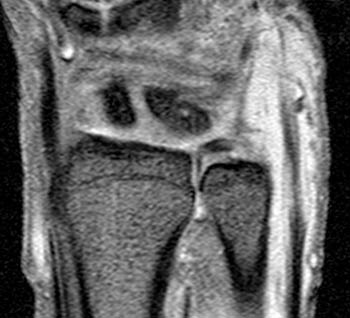
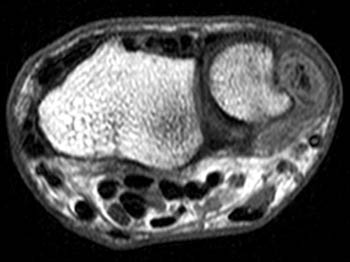
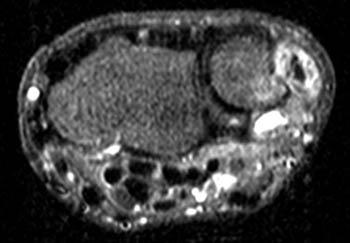
Clinical History: A 44 year old recreational tennis player complains of chronic, worsening ulnar sided wrist pain. (1a) Gradient echo coronal, (1b) T1-weighted axial, and (1c) STIR axial images of the wrist are provided. What are the findings? What is your diagnosis?
Findings
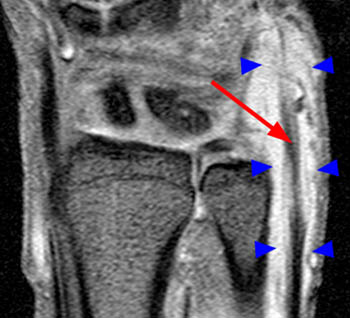
Figure 3:
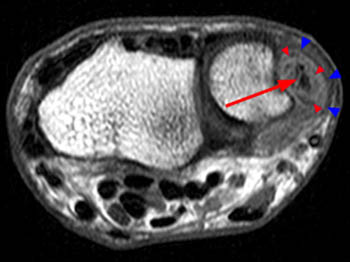
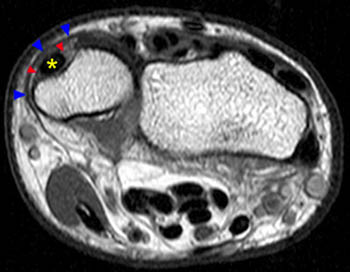
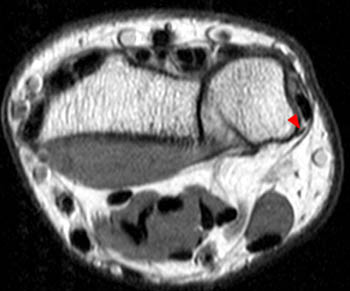
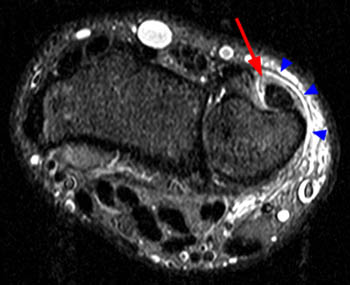
On the T1-weighted axial image at the level of the distal ulna, fluid is again noted to surround the ECU tendon (arrow), with irregular longitudinal splitting noted within the tendon. The tendon lies slightly more palmar than is typical. The ECU subsheath (red arrowheads) is diffusely fragmented. The overlying extensor retinaculum (blue arrowheads) is indicated.
Diagnosis
Severe extensor carpi ulnaris (ECU) tenosynovitis with partial tearing and mild palmar subluxation of the tendon. The ECU subsheath is diffusely torn and irregular.
Introduction
Ulnar sided wrist pain is a common clinical complaint and indication for MR imaging.” MR is able to detect and diagnose numerous ulnar sided abnormalities that may account for patient symptoms.” A not uncommon site of injury is the sixth extensor compartment, home of the extensor carpi ulnaris (ECU).
Relevant Anatomy
The ECU originates as two heads which attach to the lateral epicondyle and the middle third of the posterior ulna. It has a single distal insertion upon the posterior aspect of the base of the fifth metacarpal. The ECU functions to extend and adduct the hand, and is important in the ability to ulnar deviate the hand.
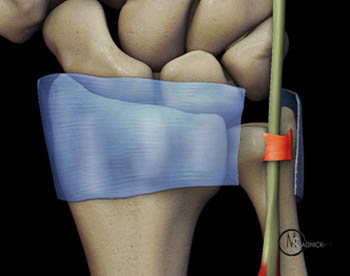
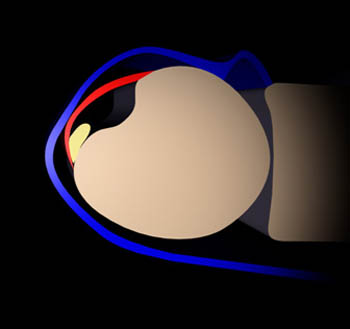
A unique anatomical characteristic of the ECU is the fibro-osseous tunnel which stabilizes the tendon at the level of the distal ulna.1 This fibro-osseous tunnel is formed by the distal ulna and a 1.5 to 2cm in length band of connective tissue referred to as the ECU subsheath (5a, 6a). The subsheath lies deep to the extensor retinaculum, which itself does not attach to or stabilize the ECU tendon. The ECU, its subsheath, and the extensor retinaculum are readily seen using MRI (7a).
ECU Tenosynovitis and Tendinosis
Tenosynovitis and tendinosis of the ECU are not uncommon, with these abnormalities being a frequent early finding in patients with rheumatoid arthritis.2 In athletes, the ECU is the second most common site of wrist tendinopathy,3 typically associated with rowing, racquet sports, and golf. In such patients, chronic stress upon the tendon results in inflammation of its synovial lining, causing tenosynovitis.4 Over time, stress may also lead to tendon degeneration and altered collagen content, resulting in tendinosis with or without partial tears (8a).
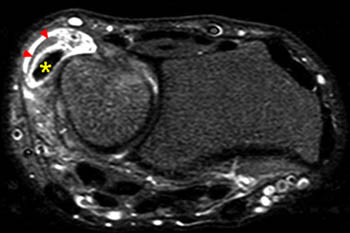
Figure 8:
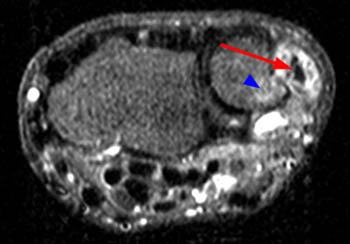
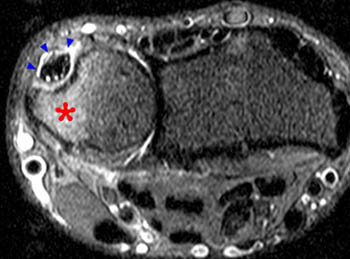
A STIR axial image reveals fluid (arrowheads) surrounding the ECU tendon at the distal ulna, compatible with tenosynovitis. The tendon is swollen and small interstitial splits are evident as bright foci within the tendon. These latter findings indicate tendinosis and interstitial tearing. Reactive marrow edema (asterisk) is seen within the adjacent ulna.
ECU Subluxation and Dislocation
Subluxation or dislocation of the ECU tendon requires an injury to the ECU subsheath. Although repetitive stress likely precedes injuries to the ECU subsheath, most patients who experience subluxation or dislocation of the ECU recall a traumatic event, typically occurring during supination, ulnar deviation, and wrist flexion. These positions increase the angulation of the ECU tendon relative to the ulna and result in maximal force upon the ECU subsheath.6 The most commonly reported sporting activities resulting in ECU subluxation or dislocation are tennis and golf.
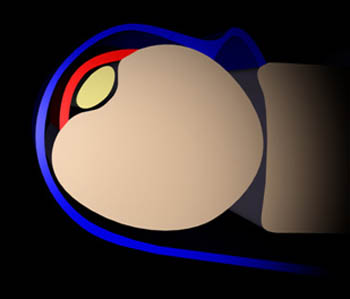
Three characteristic sites of injury have been reported in patients who experience ECU tendon dislocation and subsheath injuries.7 The subsheath may remain intact but be stripped at its palmar/ulnar attachment, forming a false pouch into which the ECU tendon can sublux or dislocate (10a,11a). Ulnar sided ruptures of the subsheath, likely the most common pattern of injury, usually result in dislocation followed by reduction in which the tendon returns to a location deep to the subsheath (12a, 13a,13b). With radial sided subsheath rupture (14a), the tendon is more likely to relocate in a manner that leaves it lying atop the ruptured subsheath (12a), preventing functional healing of the subsheath.
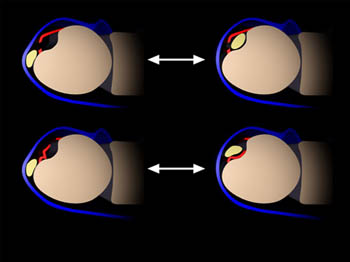
Figure 12:
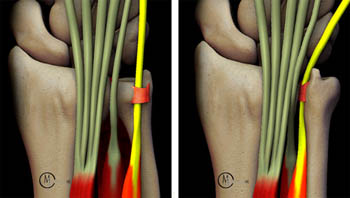
Patterns of ECU subsheath rupture. Ulnar sided tears (top row) typically result in transient dislocation of the tendon followed by relocation upon pronation, with the tendon returning to a position beneath the subsheath. With radial sided tears, the tendon is more likely to lie atop the torn subsheath following relocation.
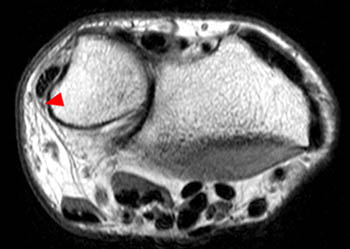
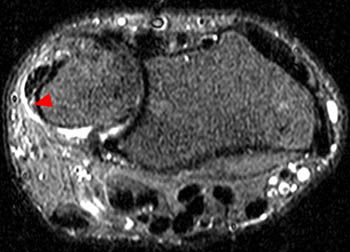
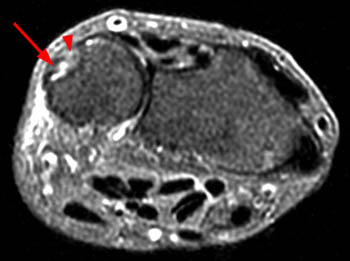
Figure 13:
(13a) T1-weighted and (13b) STIR axial images following an acute twisting injury with documented ECU tendon dislocation. The tendon has returned to its fibro-osseous tunnel, though it remains slightly subluxed and it contains small interstitial splits. The subsheath appears disorganized and its palmar attachment is lax and ill defined (arrowheads). Small amounts of adjacent edema and fluid are evident on the STIR image.
Patients who experience acute ECU subluxation or dislocation often describe a traumatic incident with immediate, searing pain. The sensation of tendon dislocation and an associated pop may accompany the injury. On clinical exam, findings include intense pain on passive supination, pain on palpation of the ECU tendon at the distal ulna, and localized swelling.5
If an acute ECU subluxation/dislocation is not appropriately treated, chronic ECU instability may result. In such cases, the ECU subsheath never heals, and the tendon may remain in an abnormally palmar location relative to its ulnar groove (P). Altered mechanics lead to chronic irritation, and thus many such patients experience persistent tenosynovitis. The chronically unstable tendon, if used repetitively, may even cause osseous erosion of the distal ulna.8
ECU Rupture
In rare cases, complete ECU tendon rupture may occur (16a,17a). In patients with tendon rupture, a characteristic cascade of events is often described.9,10 An initial acute luxation event is followed by lower grade but persistent pain, often with accompanying tenosynovitis. Local steroid injections may have provided temporary relief. Ultimately, increasing pain limits wrist activity, and subsequent imaging reveals the tendon rupture.
Figure 16:
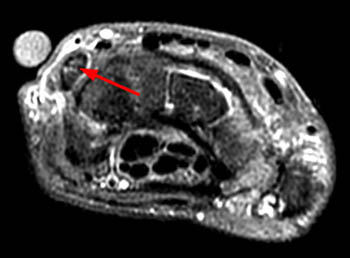
Fat-suppressed proton density weighted images from a patient with chronic ulnar sided wrist pain. At the level of the proximal carpal row, the ECU tendon (arrow) is severely thickened and demonstrates increased signal intensity throughout its substance, compatible with severe tendinosis.
Treatment
ECU tendinosis and tenosynovitis can often be managed conservatively. Splinting, rest, and non-steroidal anti-inflammatory medications are employed. Local steroid injection may also be of benefit, though it should be used with caution due to the increased risk of tendon degeneration and tearing. In patients who remain symptomatic despite conservative therapy, surgical release of the 6th extensor compartment yields excellent results.1 Release is accomplished via sectioning of the radial side of the ECU subsheath, followed by fixation of the extensor retinaculum over the region of release to prevent residual or recurrent ECU subluxation.
In patients with ECU subsheath tears and tendon instability, conservative therapy has also proven effective.5 The wrist is immobilized via casting in extension and radial deviation, which seats the tendon tightly within its ulnar groove. Activities that require movement of the elbow are limited. Depending on the severity of injury, immobilization is necessary for six weeks to three months.
Some authors, however, recommend surgical repair of ECU subsheath injuries, particularly when acute.6,11 Such an approach is particularly important in cases where the torn subsheath ends are widely separated, and is required if the tendon lies outside the torn subsheath. The most commonly utilized repair technique is a reconstruction of the subsheath using a strip of extensor retinaculum. The rare ECU ruptures are repaired via a graft from the palmaris longus.9,10 Associated injuries to the ECU subsheath are concurrently repaired. Following surgery, the wrist is casted in extension for a minimum of four weeks.
Conclusion
Ulnar sided wrist pain is both a frequent patient complaint and a common indication for MR imaging. Injuries to the extensor carpi ulnaris (ECU) are a well recognized but often poorly understood cause of such pain. Knowledge of the unique anatomy of the ECU and its subsheath must be gained in order to correctly diagnose patients with ECU tendon instability. The astute interpreter of MRI is able to accurately identify and characterize ECU tendon and subsheath abnormalities. Certain patterns of injury require operative repair, and thus MRI is a critical component of the treatment planning process.
A leading provider of teleradiology services in the United States, Radsource supplies experts in radiological image analysis and cutting-edge PACS systems. For more information, contact us today.
References
1 Maffuli N, Renstrom P, Leadbetter WB. Tendon injuries: basic science and clinical medicine. Ed. Springer, 2005:142-146.
2 Boutry N, Morel M, et al. Early rheumatoid arthritis: a review of MRI and sonographic findings. Am J Roentgen 2007; 189:1502-1507.
3 Rettib AC, Patel DV. Epidemiology of elbow, forearm, and wrist injuries in the athlete. Clin Sports Med 1995; 14(2):289-297.
4 Stoller DW. Magnetic resonance imaging in orthopaedics and sports medicine, 3rd edition, Lippincott Williams and Wilkins 2006:1828-1829.
5 Montalvan B, Parier J, et al. Extensor carpi ulnaris injuries in tennis players: a study of 28 cases. Br J Sports Med 2006; 40:424-429.
6 Inoue G, Tamura Y. Recurrent dislocation of the extensor carpi ulnaris tendon. Br J Sports Med 1998; 32:172-177.
7 Inoue G, Tamura Y. Surgical treatment for recurrent dislocation of the extensor carpi ulnaris tendon. J Hand Surg 2001; 26(6): 556-559.
8 Carneiro RS, Fontana R, Mazzer N. Ulnar wrist pain in athletes caused by erosion of the floor of the sixth dorsal compartment. Am J Sports Med 2205; 33:1910-1913.
9 Wang C, Gill TJ, et al. Extensor carpi ulnaris tendon rupture in an ice hockey player. Am J Sports Med 2003; 31:459-461.
10 Xarchas KC, Leviet D. Non rheumatoid closed rupture of extensor carpi ulnaris tendon. Report of case in a professional athlete. Acta Orthopaedica Belgica 2002; 68-4.
11 Rowland SA. Acute traumatic subluxation of the extensor carpi ulnaris tendon at the wrist. J Hand Surg 1986; 11A:809-811.