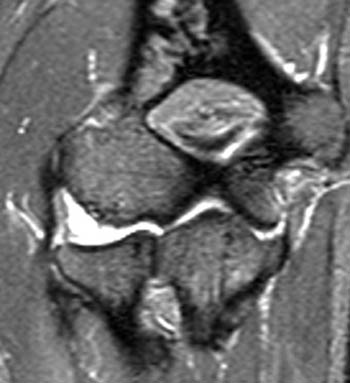
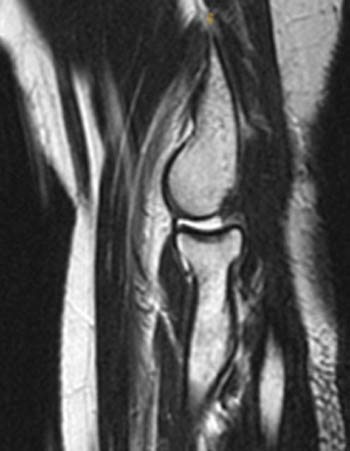
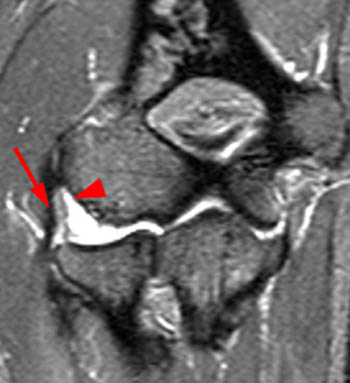
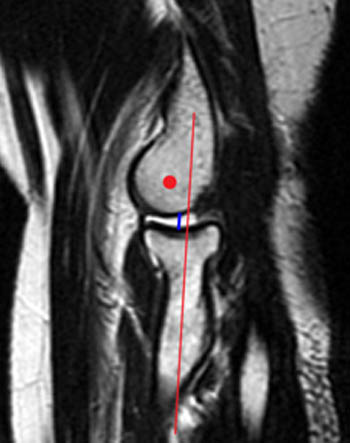
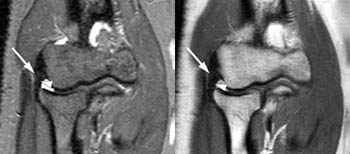
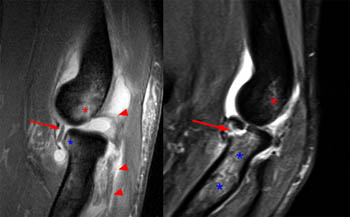
Clinical History: A 51 year old female with a history of lateral release for treatment of lateral epicondylitis presents with posterolateral pain and difficulty achieving full elbow extension. The patient was reported as being very anxious when extending the elbow during positioning for the MRI examination. Fat-suppressed T2-weighted coronal (1a) and T2-weighted sagittal (1b) images are made available for review. What are the findings? What is your diagnosis?
Findings
Diagnosis
Lateral ulnar collateral ligament tear with posterolateral rotatory instability of the elbow.
Introduction
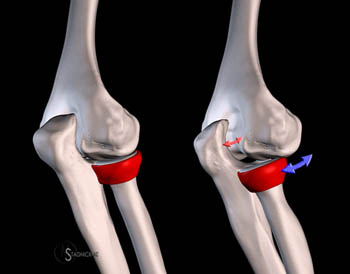
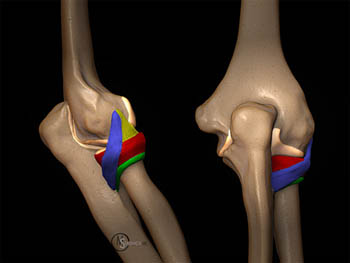
Posterolateral rotatory instability of the elbow is the most common chronic elbow instability. O’Driscoll originally described the concept of posterolateral rotatory instability (PLRI), a specific instability pattern which results when the ulna rotates on its long axis, distracting the radial aspect of the ulnotrochlear joint.1 Because the proximal radioulnar joint is stabilized by an intact annular ligament, the radius remains tightly coupled to the ulna. Thus the rotation of the ulna is transmitted to the radius resulting in posterior displacement of the radius relative to the capitellum (4a). This pattern of instability typically follows a history of significant elbow trauma, but may also be seen in other clinical settings. Subtle PLRI may cause functional impairment but may be difficult to diagnose.
Figure 4:
3D renderings of the posterolateral elbow demonstrate the concept of posterolateral rotatory instability. On the left the normal alignment of the ulnohumeral and radiocapitellar joints is demonstrated. On the right posterolateral rotatory instability occurs when loss of functional stability allows the ulnohumeral joint to rotate open laterally (red arrow). With an intact annular ligament indicated in red, the radius moves in conjunction with the ulna and is displaced posterior to the capitellum (blue arrow).
Anatomy and Function
Posterolateral stability of the elbow is maintained by the static and dynamic interaction of the articular contours and the supporting ligamentous and soft tissues at the elbow. The primary constraint to PLRI is the lateral collateral ligament complex (LCL), which is made up of the radial collateral ligament (RCL), lateral ulnar collateral ligament (LUCL), annular ligament, and accessory lateral collateral ligament.2 O’Driscoll determined that the key anatomic structure preventing this pattern of instability is the lateral ulnar collateral ligament, which extends from the lateral epicondyle to the supinator crest of the ulna, traversing the posterolateral aspect of the radial head.1,3 Subsequent anatomic studies have questioned the role of the LUCL as the primary stabilizer against PRLI, instead emphasizing the importance of the entire lateral collateral ligament complex4,5,6 the overlying extensor musculotendinous structures,7 and the osseous anatomy at the elbow. Nevertheless, the primary focus of correcting PRLI is the reconstruction or augmentation of that portion of the lateral collateral ligament complex which extends from the lateral epicondyle to the ulna, the course of the lateral ulnar collateral ligament.
The anatomy of the lateral collateral ligament complex varies significantly among individuals. The RCL and LUCL represent capsular thickenings that originate from a common origin, measuring approximately 5 mm at the distal portion of the lateral epicondyle.5 At their origin, the LUCL and RCL are deep to and slightly distal to the common extensor tendon origin. The LUCL and RCL blend with the overlying extensor tendons and intermuscular fascia.8 The RCL and LUCL are inseparable proximal to the annular ligament. The anterior fibers are typically thinner and comprise the RCL, fanning out distally to insert on the annular ligament and blend with the origin of the supinator muscle. The more posteriorly arising fibers originate at the center of the elbow’s axis of rotation1,2,9,10 and pass posterolateral to the head of the radius, continuing medially and distally to insert on the proximal ulna at the supinator crest. This bundle of capsuloligamentous tissue comprises the LUCL (D).2 At its mid-portion, the LUCL fibers lie deep to the intermuscular fascia between the supinator and extensor carpi ulnaris muscles and blends with the fibers of the annular ligament. Macroscopically, the LUCL is most distinct at its insertion with a frequently well-defined, strong anterior band inserting at the tubercle of the supinator crest. A thinner fan-like insertion extends proximally along the supinator crest, adjacent to the base of the annular ligament.2 At the tubercle insertion, the LUCL is deep and adherent to the fascia of the anconeus, supinator, and extensor carpi ulnaris muscles.14
The annular ligament encircles the radial head and tapers distally as it extends over the proximal portion of the radial neck. The annular ligament originates from the anterior and posterior margins of the lesser sigmoid notch of the ulna and acts to stabilize the radial head to the ulna throughout the range of pronation and supination of the forearm.10 The annular ligament has been shown to be important in maintaining stability at the elbow (D). Several studies have shown instability patterns similar to PRLI resulting from defects of the annular ligament, alone or in combination with defects of the LUCL and RCL.4,5 The accessory lateral collateral ligament arises from the distal annular ligament anteriorly and attaches distally at the tubercle of the supinator crest. The accessory lateral collateral ligament stabilizes the annular ligament, particularly during varus stress (5a).5,11
The key osseous anatomy and articular contours contributing to stability at the elbow are the coronoid process of the ulna and the radiocapitellar joint. The coronoid process is becoming increasingly recognized as an important structure in maintaining elbow stability, serving as a constraint to posterior ulnohumeral displacement.12 Fractures of the coronoid process are most commonly the result of elbow dislocation. Indeed, visualization of a coronoid process fracture can be regarded as evidence of a previous subluxation or dislocation.13 In one cadaver study, fractures involving 50% or greater of the coronoid height resulted in a 28% increase in external rotation of the forearm relative to the humerus.14 Clinical results demonstrate that bone grafting and reconstruction of the coronoid have successfully restored stability in those patients with PRLI following an ununited coronoid fracture.15 The radiocapitellar joint assists in providing stability by the congruency of the radial head with the capitellum. In addition, a normal length of the proximal radius is important for maintaining normal tension of the lateral ligament complex. Resection of the radial head can result in laxity of the lateral ligament complex and instability.16
Clinical History and Presentation
Patients with PRLI may present with a wide variety of complaints, ranging from vague symptoms to frank posterolateral dislocation. Mechanical symptoms are common, including painful clicking, locking or snapping, or a sense of giving way when the elbow is placed in an unstable position resulting from external rotation of the forearm with valgus and axial loading, which typically occurs when pushing up from a chair. Factors that may contribute to PRLI include a history of previous trauma, chronic resistant lateral epicondylitis, prior lateral elbow surgery, serial steroid injections, and chronic malalignment at the elbow.
PRLI most commonly results from elbow trauma resulting in posterolateral dislocation or subluxation of the elbow. Disruption of the supporting structures occurs in a circular fashion from lateral to medial. In stage I, the lateral ligament complex is disrupted. Stage II injuries result from progression of the tear to involve the anterior and posterior capsule, evidenced by a perched incomplete elbow dislocation.17 In stage III, the medial collateral ligament complex ruptures and there is complete elbow dislocation. Associated fractures of the coronoid process or radial head or avulsion fractures at the origin of the collateral ligaments may complicate the ligamentous injury.18 In a small subset of patients, adequate healing of the lateral supporting structures does not occur and posterolateral rotatory instability may ensue.
Lateral epicondylitis resistant to conservative measures is frequently the result of coexisting LUCL injury. LUCL abnormalities are seen in up to 63% of patients with lateral epicondylitis by MRI.19 The repetitive varus stresses and degenerative changes that lead to the common extensor tendon tears are felt to involve the subjacent LUCL, resulting in ligamentous weakening and potential rupture. When such changes of the LUCL and instability are not recognized preoperatively, surgical release of the extensor tendon may then further destabilize the elbow. Treatment of lateral epicondylitis with serial steroid injections may also compromise the integrity of the LUCL.20
Arthrotomy of the elbow may result in PRLI, because surgical approaches to the lateral elbow may damage the LUCL. To minimize this risk, arthrotomy anterior to the LUCL is favored to preserve ulnohumeral stability. When greater exposure is required, a posterior capsular flap release from the humerus may be performed, followed by a transosseous ligament repair.21 Recently developed surgical approaches to the radiocapitellar joint focus on preserving the lateral collateral ligament complex proximally by gaining exposure through an osteotomy at the ulnar attachment of the ligament complex, which is subsequently reattached.22
Physical Examination
The diagnosis of PLRI is a clinical one based on history and physical exam. Several clinical tests for diagnosing PLRI have been described, including the lateral pivot-shift test and the posterolateral rotatory drawer test. These provocative maneuvers place the elbow in a position of maximal instability, with a combination of external rotation of the forearm, valgus, and axial loading, which try to reproduce the symptoms or radial head subluxation.1 In the awake patient, these maneuvers generally cannot be tolerated to a point of subluxation or dislocation of the radial head because of patient discomfort.23 General anesthesia is typically required in order to demonstrate subluxation or dislocation of the radius utilizing these maneuvers.
Plain Film Findings
Plain radiography may show an avulsion fracture at the origin or insertion of the lateral collateral ligament complex, and can demonstrate the integrity of the radial head, capitellum, and coronoid process. Fractures of the radial head and of the capitellum may be seen on plain films secondary to posterior dislocation of the radial head impacting the capitellum. The drop sign has also been described, which is seen with an ulnohumeral distance of greater than 4mm on the plain lateral film of the unstressed elbow.24
MRI Findings
In the acute or chronic setting, MRI can directly demonstrate tears of the lateral collateral ligament complex and injuries of the adjacent soft tissue and osseous structures.
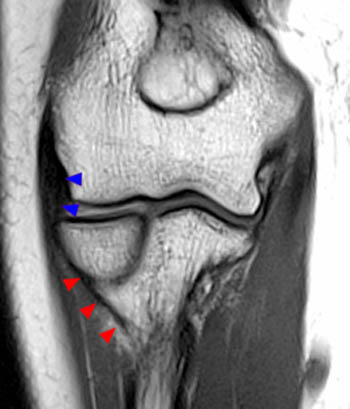
Because injuries of the LUCL most commonly occur as avulsions from the distal humerus,25 an understanding of the anatomy and normal MRI appearance, focusing on the ligament origin enables a more precise assessment of underlying lesions of the lateral collateral ligament complex and the overlying tendinous structures. The normal lateral ulnar collateral and radial collateral ligaments are low in signal on all sequences. A bilaminar appearance may be demonstrated over the proximal ligament (6a), which presumably delineates the ligamentous from the overlying tendinous structures, but the LUCL, RCL, and the common extensor tendon and fascial structures are frequently inseparable as discrete structures on MR images at the level of the epicondyle (7a). Coronal or coronal oblique imaging planes are best for evaluating the integrity of the lateral ulnar collateral ligament and radial collateral ligament. On coronal images, the LUCL does not occupy a single plane, and sequential images are necessary for complete visualization. Coronal oblique images are posteriorly angled approximately 20 degrees in relation to the humeral shaft with elbow extended (8a).26
Careful correlation and cross-reference with the sagittal and especially the axial images ensures the coronal slice being viewed actually includes the LUCL origin (9a,17a). For instance, if the coronal slice is slightly posterior, volume averaging from posterior capsule and the anconeus muscle may be mistaken for pathology of the LUCL origin (10a). GRE images achieve high resolution of the ligaments and tendons, but frequently introduce inherent signal that may be confused with subtle ligament abnormality. In these instances, comparison with T2 weighted sequences proves useful in confirming or disproving the ligament abnormality.
Figure 9:
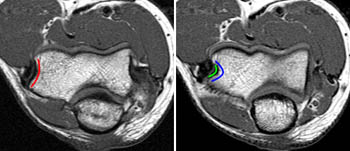
Axial T1 weighted images through the distal humerus demonstrate typical bony contours that assist in identifying the origin of the RCL, LUCL. The image on the left demonstrates a smooth convexity subjacent to the origin of the extensor tendons (red). The right image, obtained one slice more distally demonstrates a more acute angle (blue) formed between the anterior capitellum and the anteroinferior convexity of the lateral epicondyle. The RCL and LUCL arise from an approximately 5 mm origin (green) at the center of axis of the radiocapitellar joint, with the LUCL fibers arising from the posterior portion.
Figure 10:
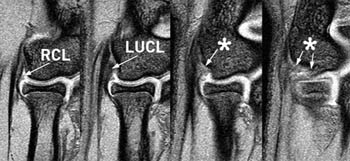
Sequential gradient echo coronal images from anterior (left) to posterior (right) through the lateral epicondyle demonstrates a bilaminar appearance of the common extensor tendon and subjacent RCL and LUCL. When visible, the RCL is typically a thinner structure than the LUCL. Images posterior to the origins of the LUCL typically demonstrate increased signal (asterisks) resulting from volume averaging of the posterior capsule and the anconeus muscle and tendon and should not be confused with a proximal LUCL tear.
As the LUCL passes posterolateral to the radial head, it overlies and partially blends with the subjacent annular ligament and is typically indistinguishable (11a). The insertion of the LUCL along the supinator crest can be demonstrated on coronal, coronal oblique (8a) and axial images (11a). The LUCL fibers insert distally on the supinator crest posterior to and commonly indistinguishable from the annular ligament fibers. A distal, more distinct band is frequently seen inserting at the tubercle of the supinator crest (12a).
Figure 11:
Axial T1-weighted image at the level of the radial demonstrates typical anatomic features of the posterolateral elbow. The annular ligament encircles the radial head inserting at the anterior and posterior margins of the lesser sigmoid notch (arrowheads). At this level the LUCL ligament is closely apposed to the annular ligament at the posterolateral aspect of the radial head (green) and lies deep to the extensor digitorum longus and extensor carpi ulnaris tendons (asterisk). The LUCL is indistinguishable as a separate structure at this level. The tendon of the extensor carpi radialis brevis is demonstrated anteriorly (arrow) and the anconeus muscle and tendon are identified posteriorly (short arrow).
The most common injury leading to PLRI is elbow dislocation. In the acute injury setting, T2 weighted images with or without fat-suppressed or STIR images best depict the extent of involvement of the lateral and medial collateral ligaments and the overlying musculotendinous structures, demonstrating fluid-filled tendon or ligament defects and intrinsic signal abnormalities (13a) compatible with sprain or partial tears. Associated fractures of the coronoid process are readily demonstrated (14a). Fractures or bone bruises of the radial head and posterior capitellum may be seen, which are analogous to Hill-Sachs deformity of the humeral head and Bankart injury of the radial head (15a).27 Rarely, injuries of the distal LUCL or annular ligament may be demonstrated (16a).
Figure 13:
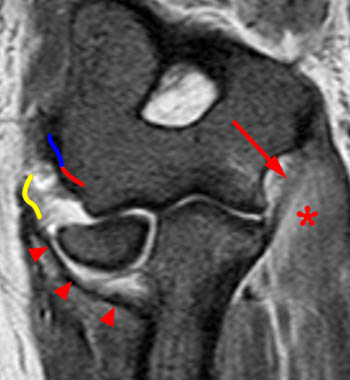
A fat-suppressed T2-weighted coronal image of a patient with evidence of recent elbow dislocation. The injury pattern begins with avulsion of the common extensor tendon and LUCL (yellow line). The LUCL (arrowheads) demonstrates laxity to the site of attachment at the tubercle of the supinator crest of the ulna. Sprain of the anterior band of the ulnar collateral ligament is demonstrated by intrinsic increased signal and loss of definition (arrow). Edema reflecting contusion of the overlying flexor digitorum muscle is seen as mildly increased T2 signal (asterisk).
Figure 15:
Fat-suppressed T2-weighted sagittal images in 2 patients demonstrate the "Hill-Sachs" injury pattern of the elbow indicative of recent elbow dislocation. On the left, bone bruises are present in the anterior portion of the radial head (blue asterisk) and posterior capitellum (red asterisk) resulting from impaction of the posteriorly displaced radial head with the posterior capitellum during posterior dislocation. Associated posterior muscular and soft tissue injuries result in periarticular edema (arrowheads). A sheared articular cartilage fragment is present in the anterior aspect of the joint (arrow) outlined by joint effusion. The image on the right demonstrates a similar bone bruise pattern with more extensive marrow edema in the radius accompanying a radial head fracture.
Figure 16:
Sequential axial STIR images in a patient following an elbow dislocation demonstrate an avulsion fracture of the ulna at the posterior insertion of the annular ligament (arrow) with subjacent marrow edema of the ulna (red asterisk) and bone bruise of the radial head (blue asterisk) in the left image. An associated tear of the distal LUCL is demonstrated at the ulnar insertion in the right image (arrowhead).
For chronic post-traumatic injuries, T1-weighted images and GRE images may be useful in establishing the amount of ligament and overlying tendon loss. T2-weighted images depict fluid containing ligament and tendon defects which are common in chronic tears. Ligament partial tears may appear as thickened ligament with intrinsic signal abnormality. In addition, MRI can identify ligament laxity and other signs of remote elbow trauma such as post-traumatic bony deformity of the radial head or coronoid process. Chronic avulsion fractures of the posterolateral aspect of the distal humerus and lateral epicondyle indicate remote posterolateral capsuloligamentous injury and instability. Posterior subluxation of the radius relative to the capitellum may be demonstrated on sagittal views and supports a diagnosis of LUCL ligament laxity.
Lateral epicondylitis is a common degenerative injury of the common extensor tendon. Many of these patients exhibit associated LUCL tears or degenerative changes. MRI evaluation prior to surgical release demonstrates any co-existent RCL, LUCL, or annular ligament injuries, which might affect the extent and approach of the extensor release (17a). In addition, MRI evaluation is helpful in those patients which are refractory to conservative measures, often demonstrating an underlying RCL or LUCL tear (18a,19a).
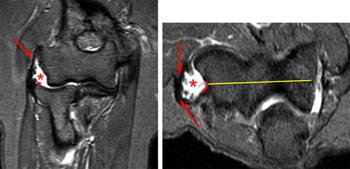
Figure 17:
71 year old female with persistent lateral epicondylitis, evaluated prior to extensor tendon release . STIR coronal and axial images demonstrate complete tear of the RCL and LUCL from its origin (red line). Fluid fills the defect (asterisk) created by torn and retracted RCL and LUCL (arrowhead) and partial tear of the overlying extensor tendon (arrow). The yellow line indicates the location of the coronal image.
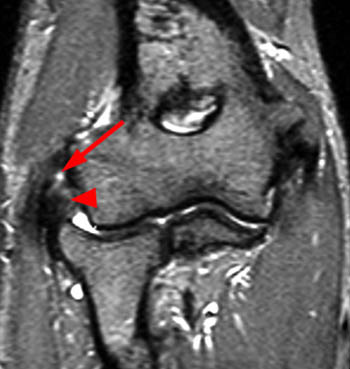
Figure 18:
50 year old man with chronic elbow pain and no history of trauma. A coronal STIR image demonstrates a complete tear of the common extensor tendon and subjacent LUCL(arrow) from the lateral epicondyle. The origin of the extensor tendon (red asterisk) is more proximal on the lateral epicondyle compared to the origin of the LUCL (blue asterisk). The annular ligament (arrowheads) is lax and slightly distally retracted due to loss of stabilization by the RCL.
Figure 19:
STIR coronal image demonstrates a thickened LUCL with intrinsic increased signal (arrowhead) of the proximal LUCL compatible with partial tear and severe degeneration. A small focus of increased signal indicates a small intrinsic partial tear of the overlying common extensor tendon (arrow).
Management
Management of chronic PRLI depends on the severity of the patient’s symptoms. Bracing and avoiding provocative maneuvers may provide satisfactory outcome for some. In significantly affected individuals, surgery is recommended. Various surgeries are focused on reconstructing the LUCL, addressing any bone deficiency of the radiocapitellar or ulnohumeral joint by replacing the radial head or coronoid reconstruction, and correcting any varus deformity of the humerus by osteotomy.
Ligament reconstruction methods include reattachment of the lateral ligament complex with imbrication and advancement and reconstruction utilizing graft, which appears to provide a more stable construct and better long-term results. Current techniques focus on repair of the LUCL. Palmaris tendon autograft is most commonly employed, but other graft materials include triceps fascia, semitendinosus, gracilis, plantaris, and Achilles tendons, as well as synthetic materials.28 Both arthroscopically assisted repair of the avulsed ligament and arthroscopic electrothermal shrinkage of the lateral ligament complex have been reported in treating patients with PLRI.
Conclusion
The LUCL is injured in patients suffering elbow dislocation and is commonly injured in patients with lateral epicondylitis. In a small subset of patients suffering elbow dislocation, PRLI may develop. Among patients with lateral epicondylitis, PRLI instability may develop in conjunction with the underlying degenerative process or iatrogenically from an overly aggressive extensor tendon release or from serial steroid injections. Once regarded as the key anatomic structure, there is now debate regarding the essential nature of the LUCL in providing stability. Recent investigations suggest that the LUCL is only one part of a complex interaction of ligaments, musculotendinous and osseous structures that maintain stability, yet surgical treatment of PLRI focuses primarily on reconstructing the function of the LUCL. MRI provides a noninvasive means of evaluating the anatomy involved in maintaining stability at the elbow and can identify lesions that contribute to PRLI, providing invaluable information for the management of affected patients.
References
1 O’Driscoll SW, Bell DF, Morrey BF. Posterolateral rotatory instability of the elbow. J Bone Joint Surg (Am) 73:440-446, 1991.
2 Morrey BF, An KN. Articular and ligamentous contributions to the stability of the elbow joint. Am J Sports Med 1983;11:315-9.
3 O’Driscoll SW, Horii E, Morrey BF, Carmichael SW: Anatomy of the Ulnar Part of the Lateral Collateral Ligament of the Elbow. Clin Anatomy 5:296-303, 1992.
4 McAdams TR, Masters GW, Srivastava S. The effect of arthroscopic sectioning of the lateral ligament complex of the elbow on posterolateral rotator instability. J Shoulder Elbow Surg 14:3 298-301.
5 Hannouche D, Begue T. Functional anatomy of the lateral collateral ligament complex of the elbow. Surgical and Radiologic Anatomy 21:3 187-191, 1999.
6 Dunning CE, Zarzour ZD, Patterson SD, Johnson JA, King GJ: Ligamentous stabilizers against posterolateral rotator instability of the elbow. J Bone Joint Surg (Am) 2001;83:1823-1828.
7 Cohen, MS, Hastings H2nd. Rotatory instability of the elbow. The anatomy and role of lateral stabilizers. J Bone Joint Surg (Am) 79:225-33, 1997.
8 Imatani J, Ogura T, Morito Y, Hashizume H, Inoue H: Anatomic and histoplogic studies of lateral collateral ligament complex of the elbow joint. J Shoulder Surg 8:6 625-27,1999.
9 Nestor BJ, O’Driscoll SW, Morrey BF. Ligamentous reconstruction for posterolateral rotatory instability of the elbow. J Bone Joint Surg (Am) 1992;74:1235-1241.
10 Berg EE, DeHoll D: The Lateral Elbow Ligaments: A Correlative Radiographic Study. Am J Sports Med 27: 796-800, 1999.
11 Bozkurt M et al. The Annular Ligament: An Anatomical Study. Am J Sports Med 33:114-118, 2005.
12 Schneeberger AG, Sadowski MM, Jacob HAC. Coronoid process and Radial Head as Posterolateral Rotatory Stabilizers of the Elbow. J Bone Joint Surg (Am) 86(5):975-982, 2004.
13 Mehta JA, Bain GI. Posterolateral Rotatory Instability of the Elbow. J Am Acad Orthop Surg 12:405-414, 2004.
14 Regan W, Morrey BF. Fractures of the coronoid process of the ulna. J Bone Joint Surg (Am) 1989;71-A:1348-54.
15 Okazaki M, Takayama S, Seki A, Ikgami H, Nakamura T. Posterolateral rotatory instability of the elbow with insufficient coronoid process of the ulna: a report of 3 patients. J Hand Surg (Am)2007;32:236-9.
16 Hall JA, McKee MD. Posterolateral rotator instability of the elbow following radial head resection. J Bone Joint Surg (Am) 2005;87-A:1571-9.
17 O’Driscoll SW, Jupiter JB, King GJW, Hotchkiss RN, Morrey BF. The unstable elbow. J Bone Joint Surg (Am) 2000;82-A:724-737.
18 Jeon I, Micic ID, Yamamoto N, Morrey BF. Osborne-Cotterill Lesion: An Osseous Defect of the Capitellum Associated with Instability of the Elbow. AJR 191:727-729, 2008.
19 Bredella MA, Tirman PFJ, Fritz R, Feller JF, Wischer TK, Genant HK. MR Imaging Findings of Lateral Ulnar Collateral Ligament Abnormalities in Patients with Lateral Epicondylitis. AJR 173:1379-1382, 1999.
20 Kalainov DM, Cohen MS. Posterolateral Rotatory Instability of the Elbow in Association with lateral epicondylitis. A Report of Three Cases. J Bone Joint Surg (Am) 87:1120-1125, 2005.
21 Osborne G, Cotterill P: Recurrent dislocation of the elbow. J Bone Joint Surg (Br)1966;48:340-346.
22 Stanley JK, Penn DS, Wasseem M. Exposure of the head of the radius using the Wrightington approach. J Bone Joint Surg (Br) 2006;88-B:1178-82.
23 Nestor BJ, O’Driscoll SW, Morrey BF. Ligamentous reconstruction for posterolateral rotatory instability of the elbow. J Bone Joint Surg (Am) 1992;74:1235-1241.
24 Coonrad RW, Roush TF, Major NM, Basamania CJ. The drop sign, a radiographic warning sign of elbow instability. J Shoulder Elbow Surg 2005; 14:312-17.
25 McKee MD, Schemitsch EH, Sala MJ, O’Driscoll SW. The pathoanatomy of lateral ligamentous disruption in complex elbow instability. J Shoulder Elbow Surg 2003;12:391-6.
26 Cotten A, Jacobson J, Brossmann Joachim, Pedowitz R, Haghighi P, Trudell D, Resnick D. Collateral Ligaments of the Elbow: Conventional MR Imaging and MR Arthrography with Coronal Oblique Plane and Elbow Flexion. Radiology 204:806-812, 1997.
27 Rosenberg ZS, Blutreich SI, Schwitzer ME, Zember JS, Fillmore K. MRI Features of Posterior Capitellar Impaction Injuries. AJR 190: 435-441, 2008.
28 Sanchez-Sotelo J, Morrey BF, O’Driscoll SW. Ligamentous repair and reconstruction for posterolateral rotator instability of the elbow. J Bone Joint Surg (Br) 87-B:54-61, 2005.