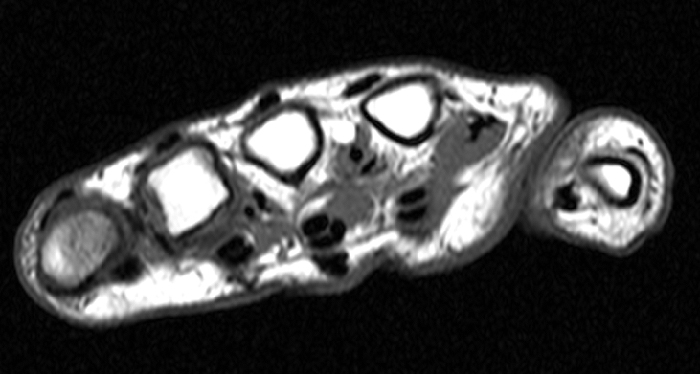
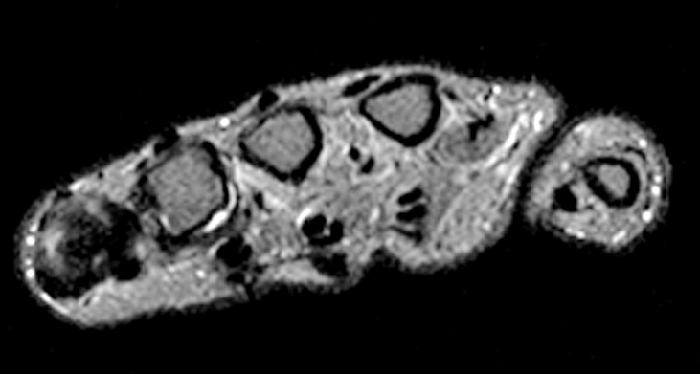
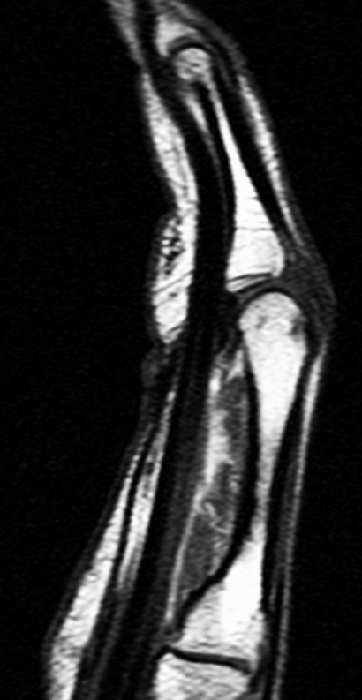
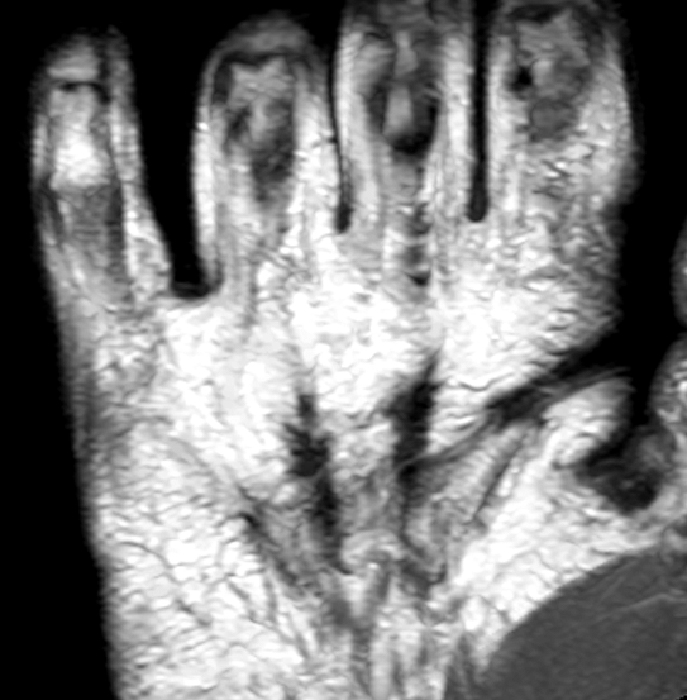
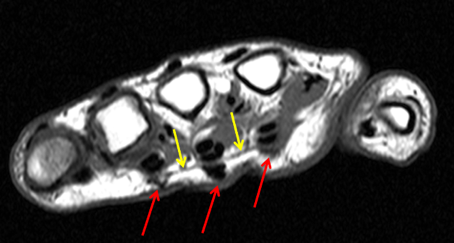
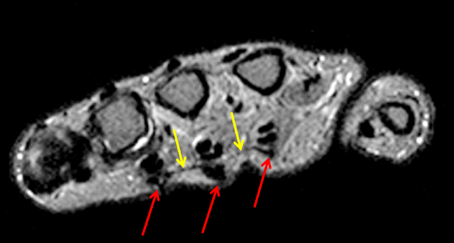
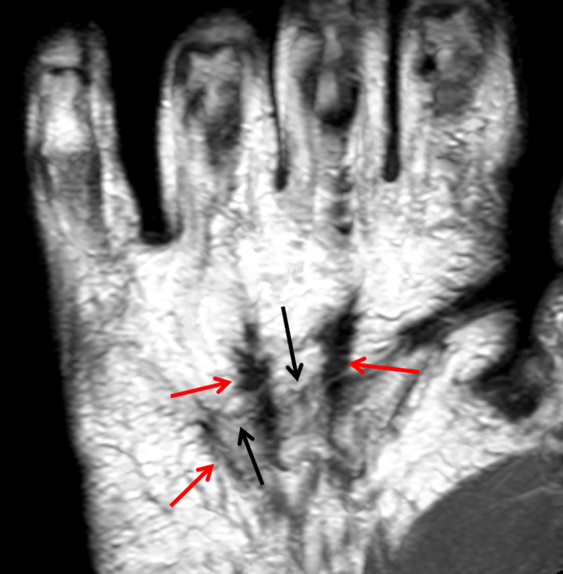
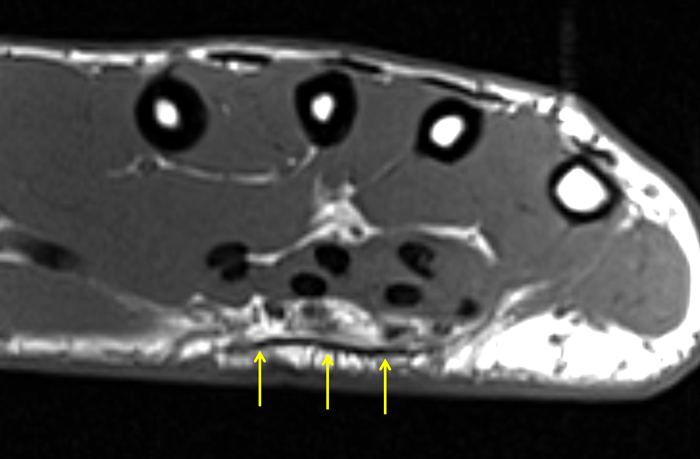
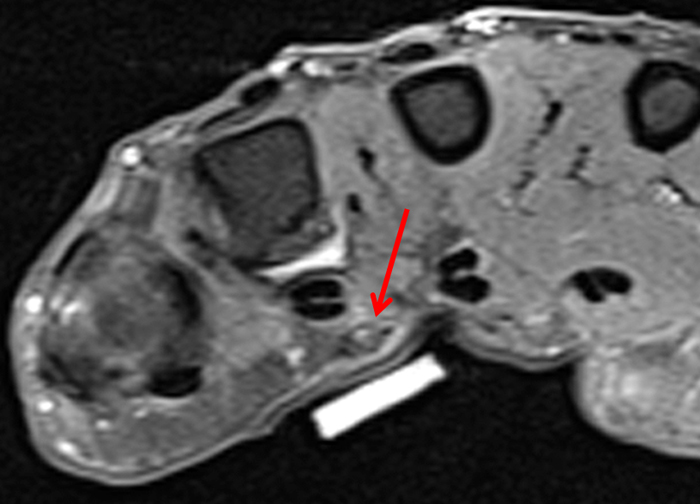
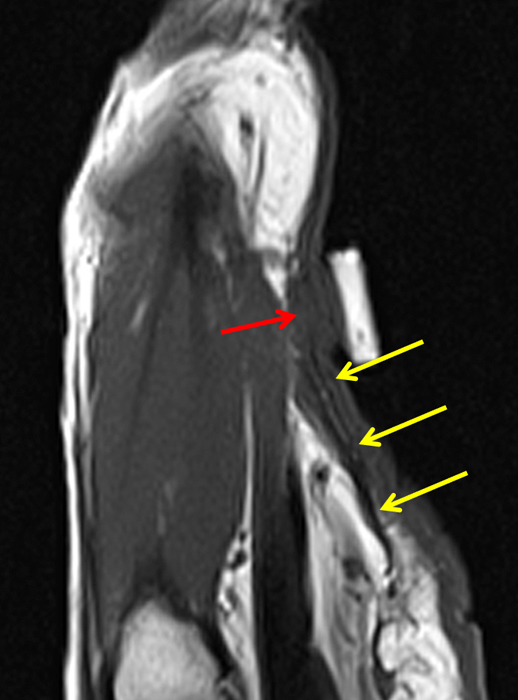
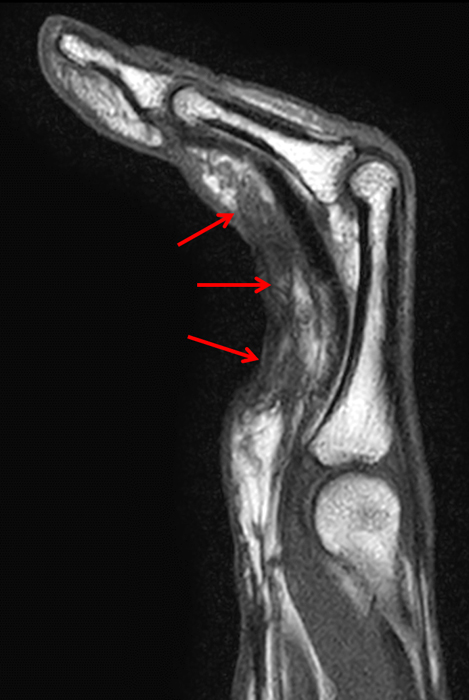
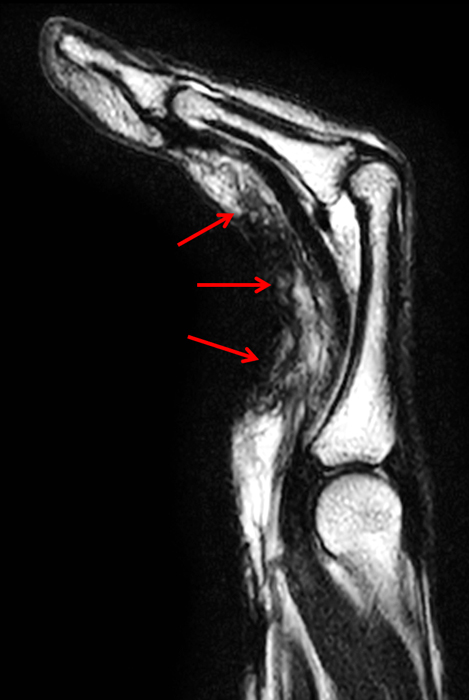
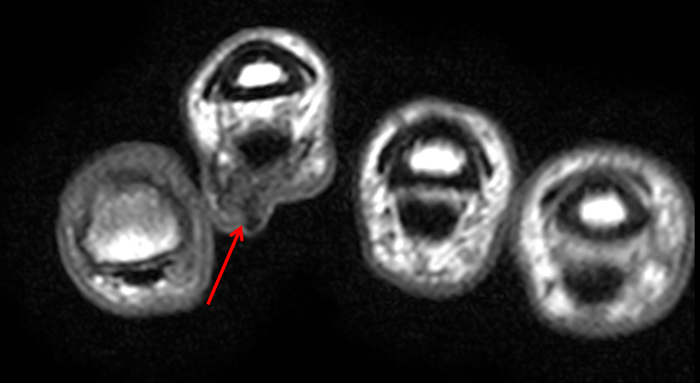
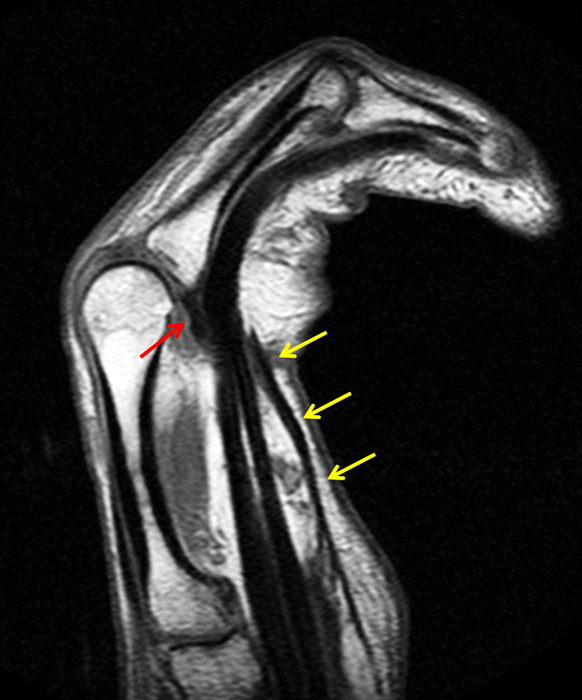
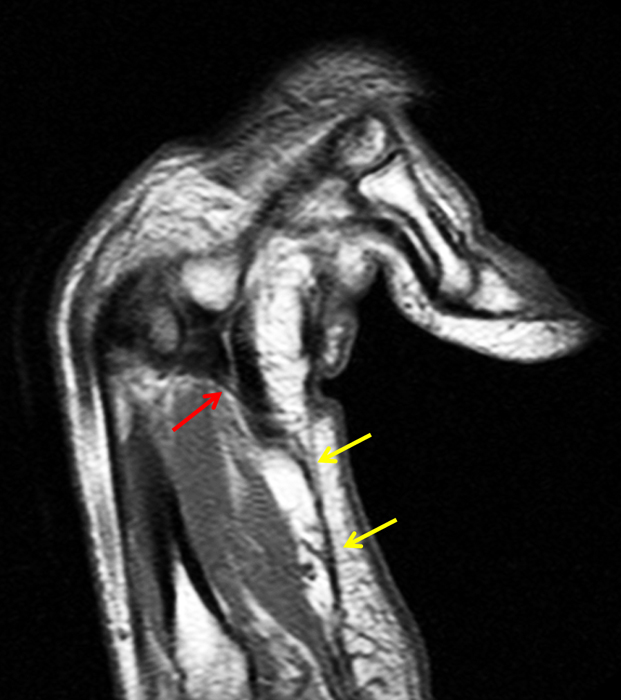
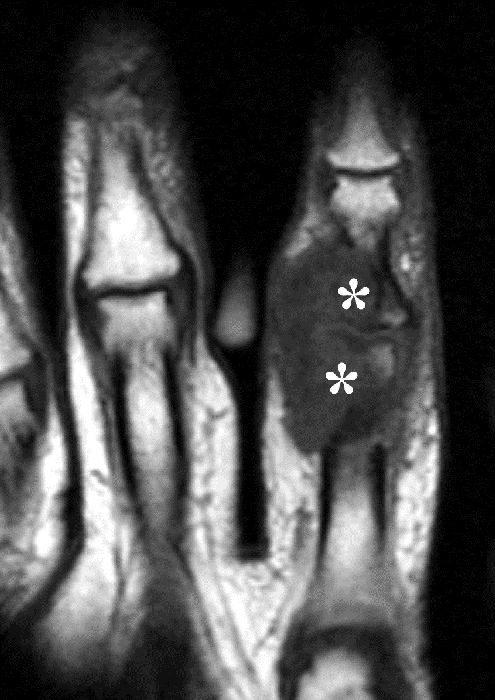
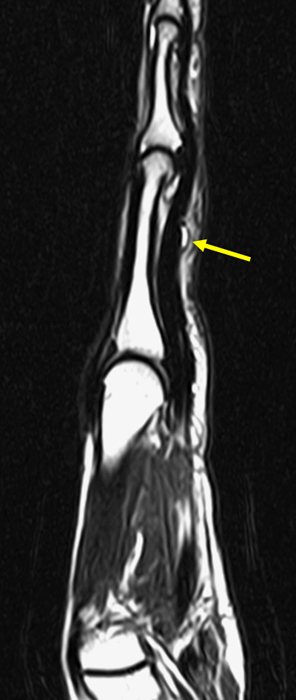
Clinical History: A 53 year-old woman with no prior medical history noted small masses in her palm a few months ago and since has developed the inability to fully straighten her long finger. Axial T1-weighted (1a) and fat-suppressed T2-weighted (1b) images through the distal palm and a sagittal T1-weighted image of the long finger (1c) are shown. A relatively thick, maximum intensity projection (MIP) image was also created in the coronal plane (1d). What are the pertinent imaging findings and diagnosis?
Findings
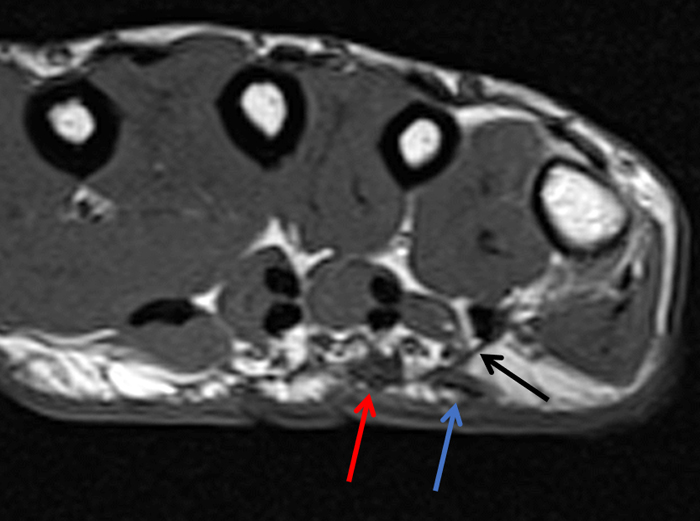
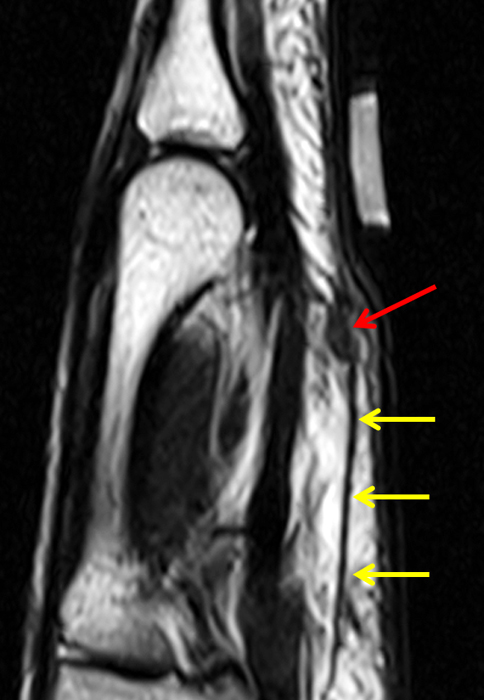
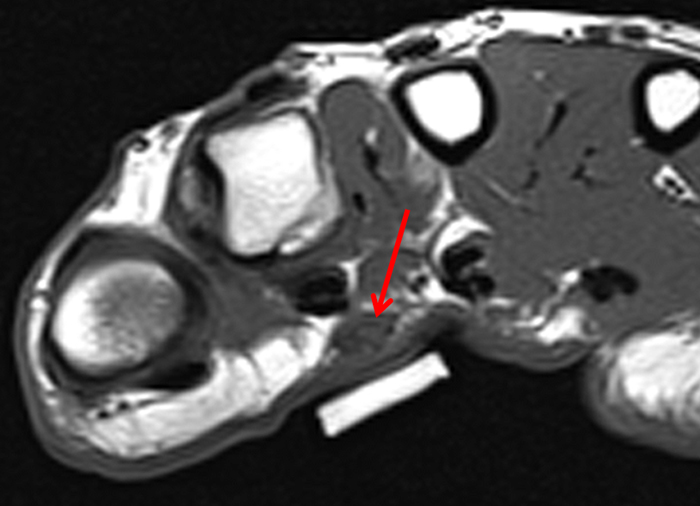
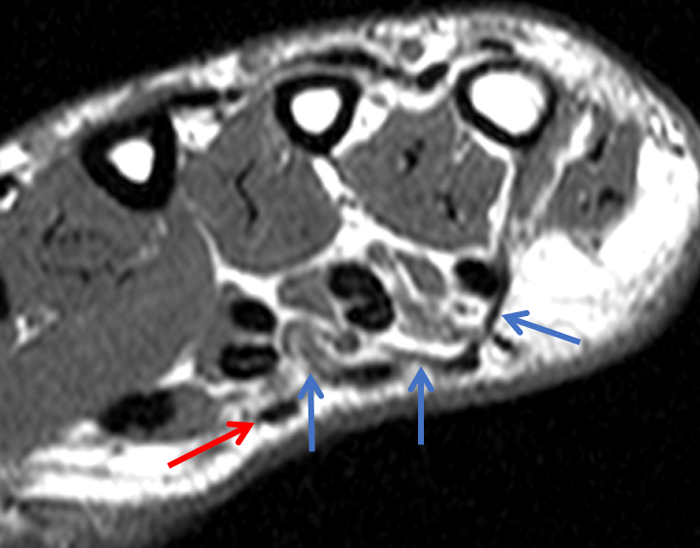
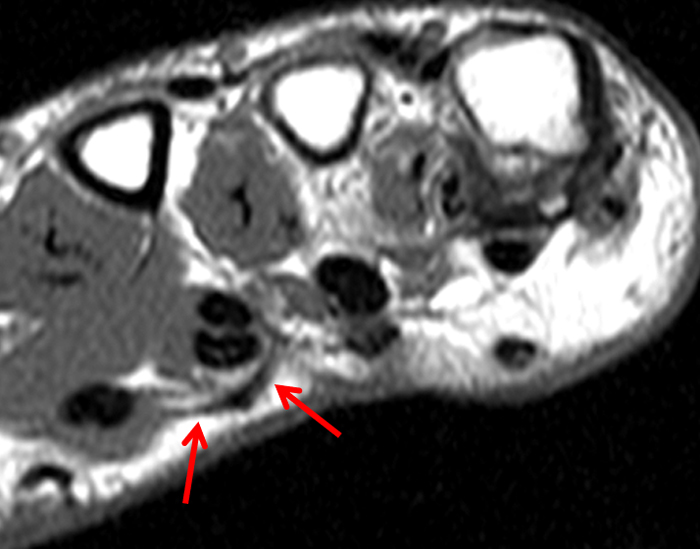
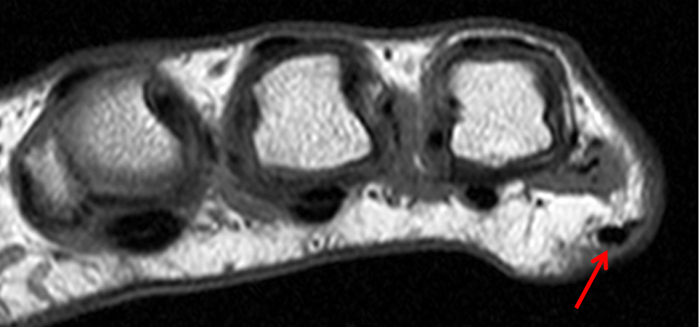
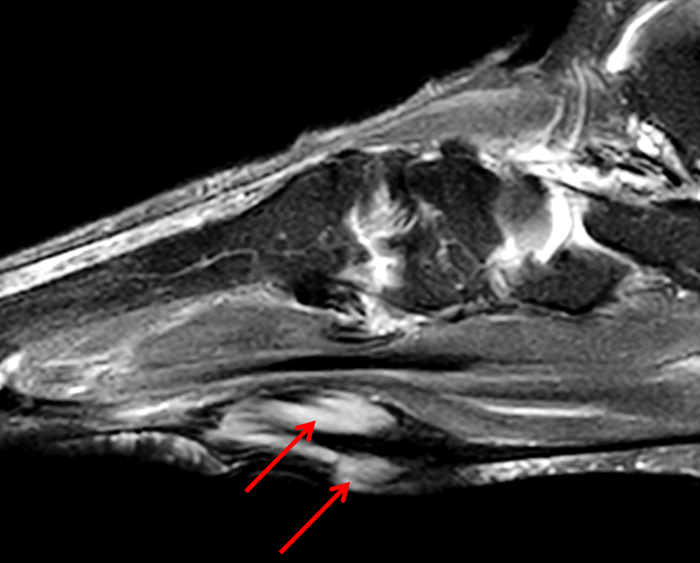
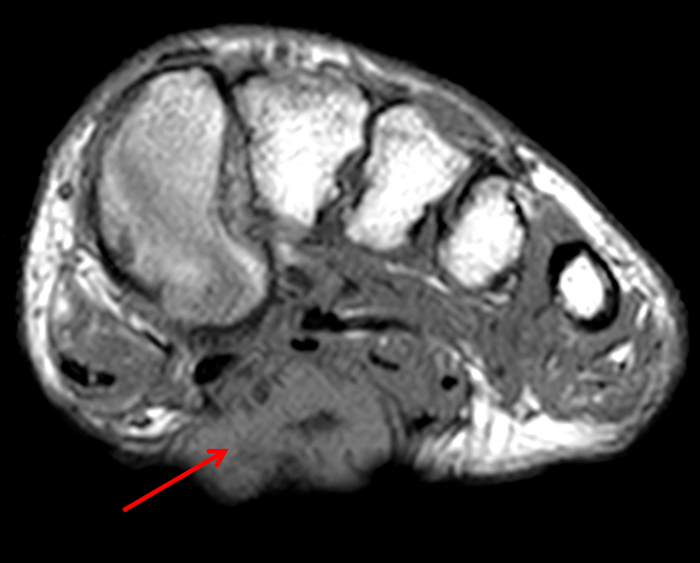
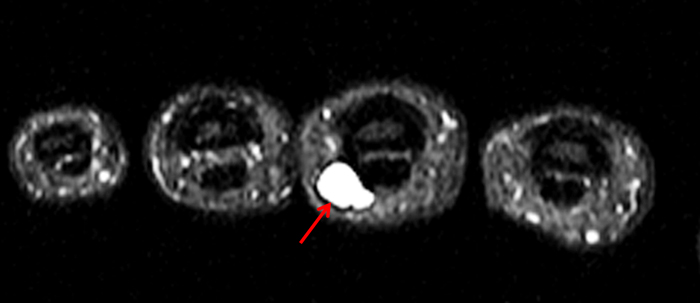
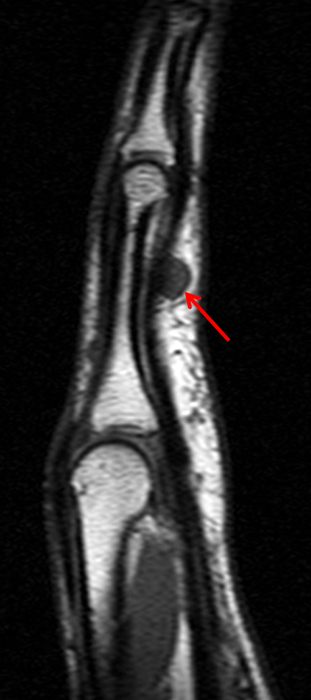
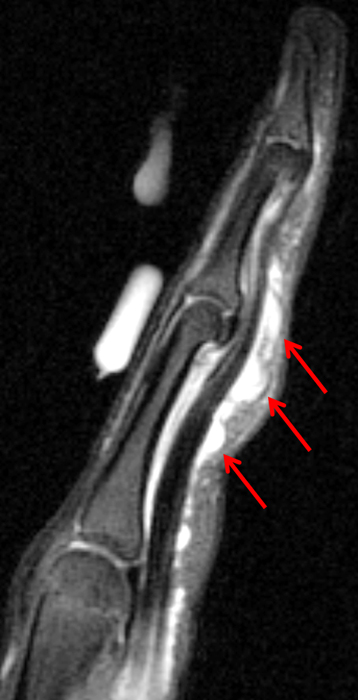
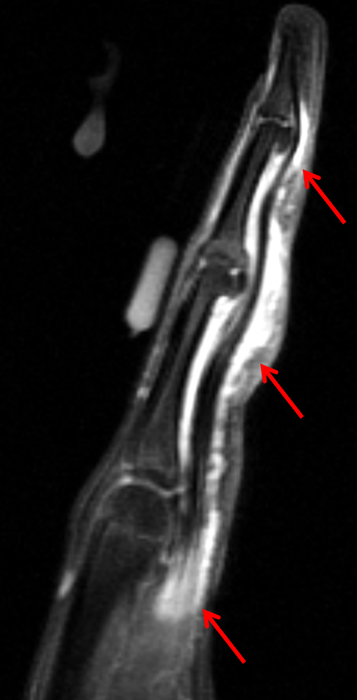
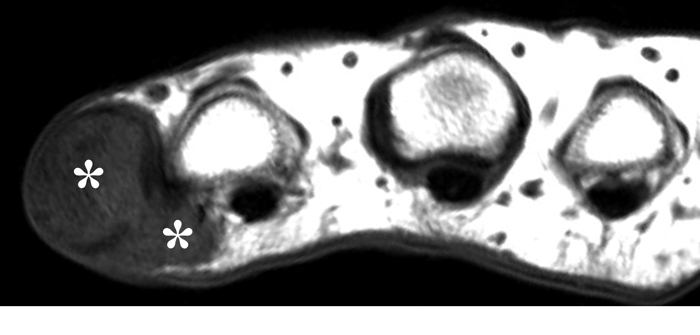
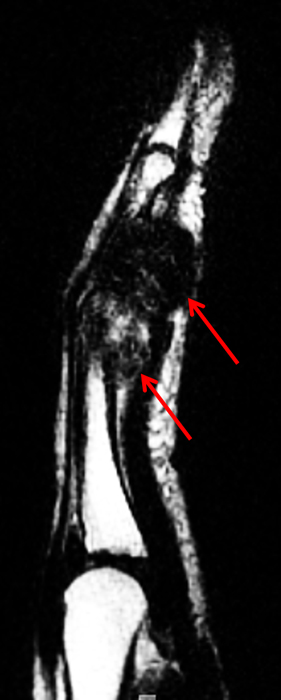
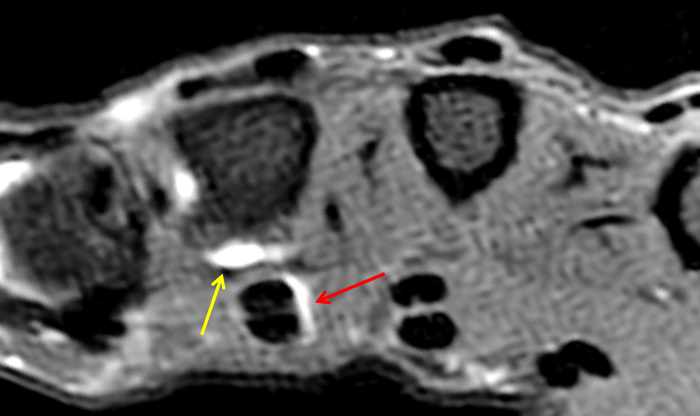
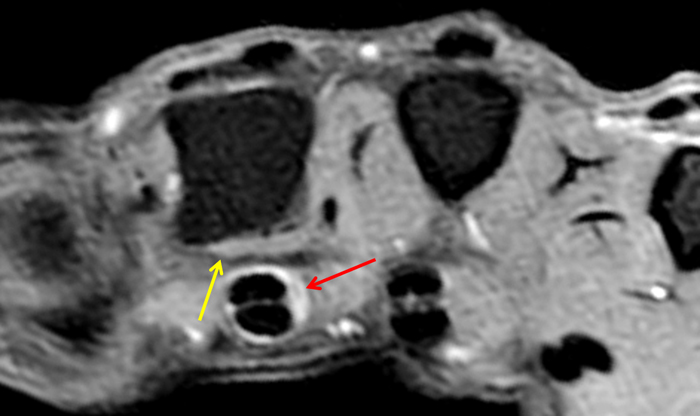
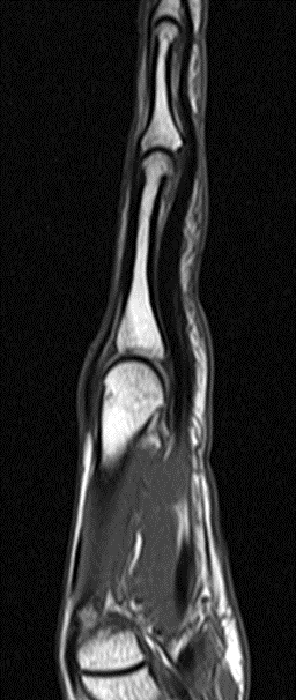
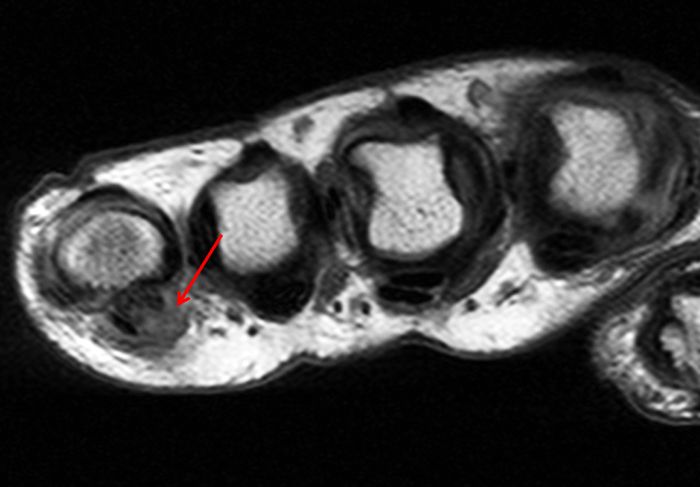
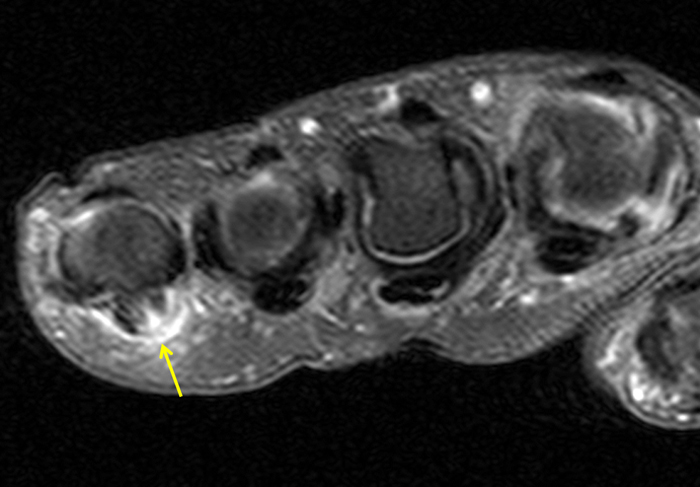
Figure 2:
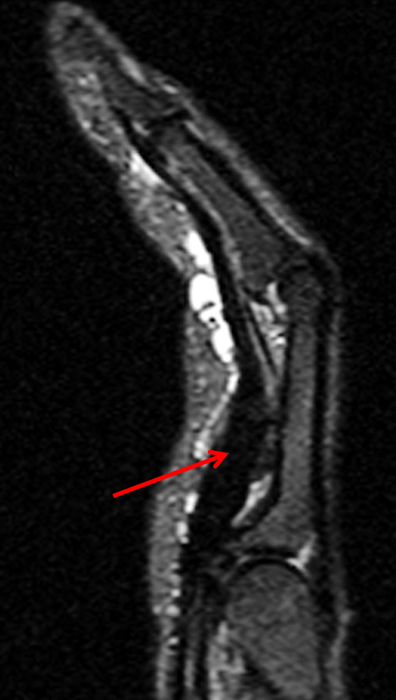
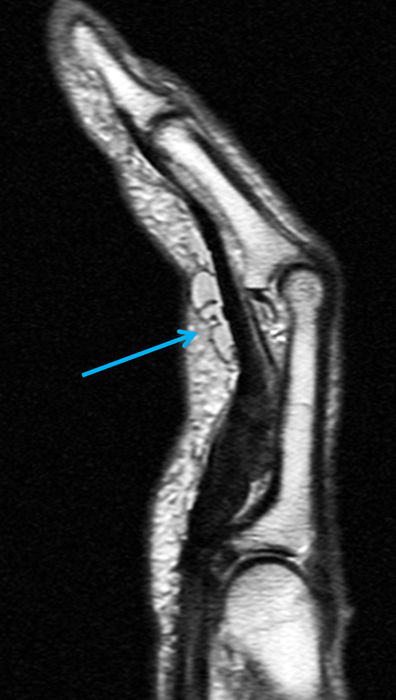
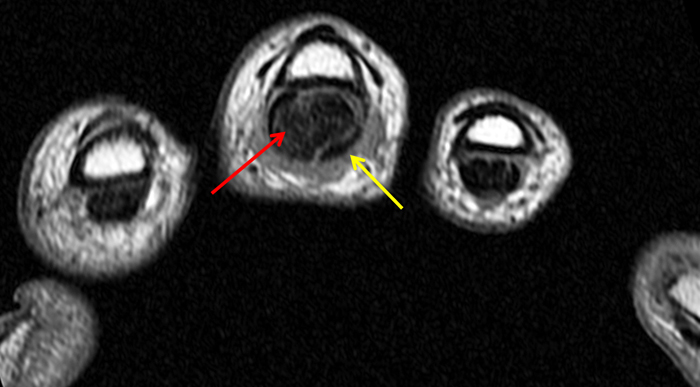
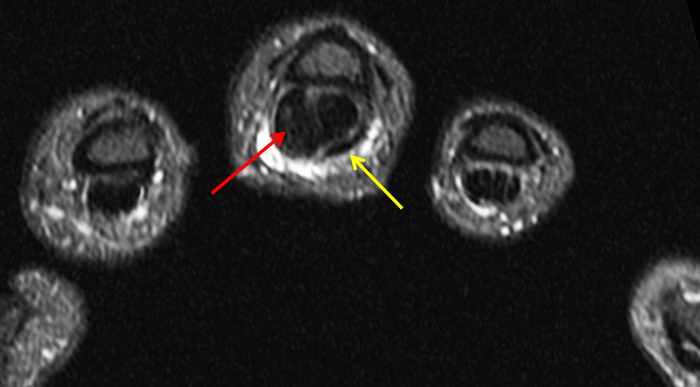
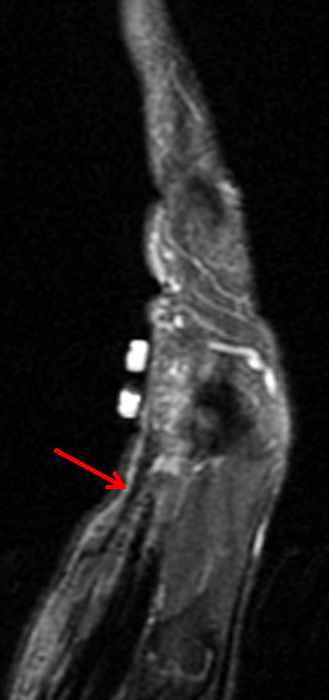
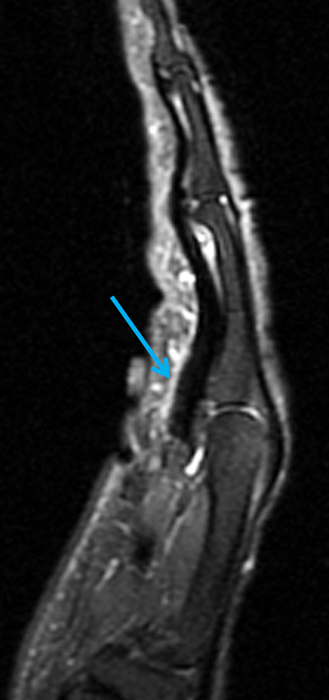
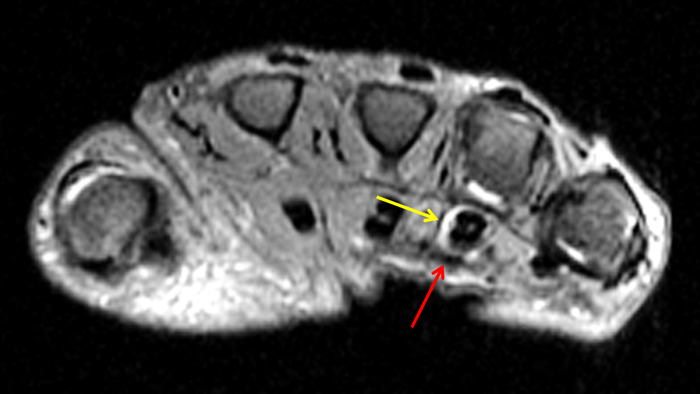
On both the T1-weighted and T2-weighted axial images (2a and 2b), very low-signal structures (red arrows) are present in the midline, palmar subcutaneous fat of the long finger and to a lesser extent the ring and index fingers, between the flexor tendons and skin, superficial to the natatory ligaments (yellow arrows). The sagittal image through the long finger (2c) shows a corresponding longitudinally-oriented fibrous cord (red arrows) extending distally from the palm and ending just proximal to the metacarpophalangeal joint. The cord is inseparable from a small nodular lesion (blue arrow) that slightly puckers the overlying skin. Mild flexion is present at the metacarpophalangeal joint, while the proximal interphalangeal joint is fully extended. On both the axial and sagittal images, the flexor tendons and sheaths appear normal. The coronal MIP projection (2d) demonstrates portions of the subcutaneous cords (red arrows) paralleling the expected course of the underlying metacarpals. Strand-like linear fibers (black arrows) in the palm perpendicular to the cords likely represent portions of the normal proximal transverse palmar ligaments.
Diagnosis
Dupuytren’s disease with pre-tendinous cords involving the long finger, and to a lesser extent the index and ring fingers, with a mild flexion contracture of the long finger metacarpophalangeal (MCP) joint.
Clinical Overview
Dupuytren’s disease (also called Dupuytren’s contracture) is an idiopathic fibroproliferative condition that affects the superficial palmar tissues of the hands and fingers. While the disorder is benign, associated morbidity is high due to limitations in daily activity.1 Progressive fibrosis develops in the subcutaneous fat, first forming nodules that contract the tissues, and later elongated cords that may lead to flexion contractures of the finger MCP and proximal interphalangeal (PIP) joints. Cords can develop as thickenings along the normal fascial structures or separate from them.2,3 While Dupuytren’s can involve any digit, the small finger is most common.4 Insidious onset with either painless nodules/thickening in the palm or limited finger extension typically occurs between ages 40 and 60, with men affected much more frequently than women.2 The incidence is higher in patients who are smokers, alcoholics, manual laborers, and those with diabetes or infected with human immunodeficiency virus.1,5 A genetic component has also been identified.5,6 Abnormal, overactive myofibroblasts are the cells responsible for the condition. Three stages are recognized histologically: an initial proliferative stage characterized by high cellularity, increased vascularity, and large myofibroblasts with increased mitoses; a second involutional (fibrocellular) stage, which is still highly cellular (without mitoses), but where a dense myofibroblast network produces excess type 3 collagen; and a late residual (fibrotic) stage with decreased number of myofibroblasts, increased fibrocytes, and dense collagen bundles.7,8
Normal Fascial Anatomy
The normal palmar and digital fascia consists of a series of volar subcutaneous bands whose main function is to stabilize the skin during grasping. The palmar aponeurosis (Figure 3) begins at the distal edge of the carpal tunnel, taking origin from the transverse carpal ligament and distal aponeurosis of the palmaris longus. In the hand it spreads out in a flattened triangular shape, and then splits into four pretendinous bands that parallel the finger metacarpals, located volar to the flexor tendons and sheaths.5 In the proximal palm the normal fascia appears on axial MR images as a thin, low-signal-intensity structure in the adipose tissue superficial to the branches of the median and ulnar nerves (Figure 3c). Occasionally the more distal normal pretendinous bands may be identified on sagittal images, although if one is easily identified it may be an indication of early pathologic thickening (Figure 4). Proximal transverse palmar ligaments run between the pretendinous bands in the mid palm – rarely a MIP image may show these (Figure 2d). The pretendinous bands terminate at approximately the MCP joints. Located at the distal ends of the pretendinous bands, the natatory ligaments are the main transverse component of the palmar fascia, oriented perpendicular to the flexor apparatus and coursing between adjacent digits; these ligaments are palpable as taut tracts in the base of each web space between the spread fingers.5 Normal natatory ligaments are sometimes visible on axial MR images at the level of the metacarpal heads (Figure 2a).
In the fingers, the digital fascia is comprised of multiple interconnected structures (Figure 3), none of which are routinely visible on standard MR images unless they are pathologically thickened into cords. Lateral digital sheets extend along the radial and ulnar surfaces of each finger from the natatory ligaments to the level of the distal interphalangeal joint. Paired, oblique spiral bands begin at the distal ends of the superficial pretendinous bands, then extend distally travelling deep to the natatory ligaments, dorsal to the neurovascular bundles. The spiral bands terminate on the proximal aspects of the lateral sheets. Striated fibers (Grayson’s ligaments palmarly and Cleland’s ligaments dorsally) bridge between the lateral digital sheets and the centrally-located phalanges and flexor tendon sheaths/pulleys along both sides of each finger, situated volar and dorsal, respectively, to the digital neurovascular bundles. Additional specialized fascial bands invest the thumb, as well as the thenar and hypothenar eminences.5
Figure 3:
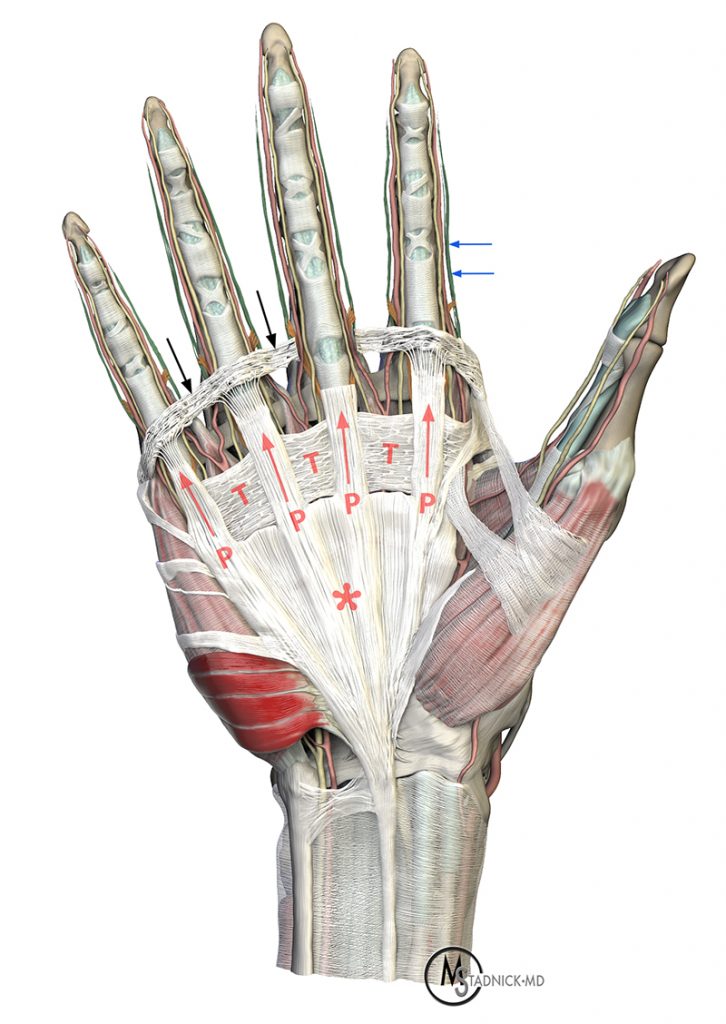
Normal palmar and digital fascia. (3a) 3D render of the volar hand and fingers with the skin removed. The palmar aponeurosis (asterisk) forms a broad fascial sheet, dividing into four pretendinous bands (P), with connecting transverse palmar ligaments (T) in the distal palm. Natatory ligaments (black arrows) join the pretendinous bands in the web spaces between the fingers. Lateral digital sheets (blue arrows) extend from the deep surfaces of the natatory ligaments along the radial and ulnar border of each finger, connected to the phalanges and flexor sheath by thin Grayson’s and Cleland’s ligaments (not included). Additional normal bands are present in the thenar and hypothenar eminences. (3b) An enlargement showing detail at the long finger MCP joint, where the natatory ligament and distal pretendinous band have been removed for demonstration purposes. Note the spiral band (orange arrows) running from the deep aspect of the pretendinous band to the lateral digital sheet (blue arrows), passing dorsal (deep) to the neurovascular bundle. (3c) AxialT1-weighted image through the proximal palm shows the normal palmar aponeurosis (arrows). The normal fascial structures in the fingers are too thin to be routinely visible on MR images.
Pathoanatomy and MR appearance
The nodules of Dupuytren’s disease are most common around the distal palmar crease. On MR images these nodules appear as subcutaneous masses with ill-defined margins. Nodules that are cellular histologically are approximately isointense compared to muscle on T1- and T2-weighted images; hypocellular nodules tend to be darker on all pulse sequences (Figures 4 and 5).9 Intravenous contrast administration is unnecessary for evaluation but nodules in the proliferative phase can show mild enhancement.
Figure 4:
Dupuytren’s nodules in a 50 year-old man. (4a) Axial T1-weighted and (4b) sagittal T2-weighted images demonstrate subcutaneous nodules superficial to the flexor sheaths and deep to the skin, volar to the fourth (red arrow) and fifth (blue arrow) metacarpal necks. The nodule associated with the ring finger is inseparable from the pretendinous band (yellow arrows), which may be mildly thickened. The low-signal-intensity structure (black arrow) extending deep from the small finger nodule may be a thickened spiral band, representing the beginning of a spiral cord.
Figure 5:
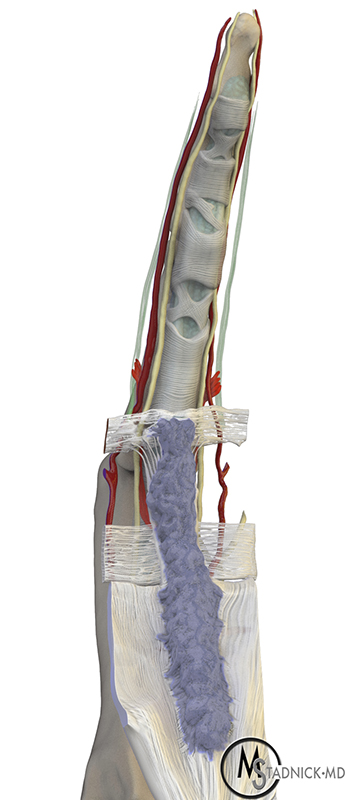
Dupuytren’s nodule and pretendinous cord in a 56 year-old man presenting with a palpable mass. Axial (5a) T1-weighted and (5b) fat-suppressed T2-weighted images and (5c) sagittal T1-weighted image of the ring finger show a palmar, subcutaneous soft tissue nodule (red arrows) deep to the marker placed on the palpable abnormality. The nodule is isointense compare to skeletal muscle on the T1-weighted images and isointense to mildly hyperintense on the T2-weighted image, suggesting that it is relatively cellular. A thickened pretendinous cord (yellow arrows) is forming in association with the nodule. (5d) Drawing of a pretendinous cord consisting of a thickened, nodular pretendinous band extending to the natatory ligament. Note flexion contracture at the MCP joint.
The fibrous, cable-like structures of Dupuytren’s disease occur in several recognized patterns. orthopaedic and hand surgeons recognize at least 7 distinct patterns of pathologic cords, and some of these are recognizable on MR images. The clinical importance of identifying the cord type relates to the different relative risks of flexion contractures and neurovascular bundle involvement, which in turn affects prognosis and surgical approach. Unfortunately, the terminology can be somewhat confusing. One rule to remember is that normal structures are named bands, ligaments, or sheets, while the term “cord” denotes an abnormal structure. Second, some cords carry the same name as the normal structure from which they derive (e.g., pretendinous cords arise from pretendinous bands), while other cords involve additional normal fascial elements (spiral cords, for example, involve several structures in addition to the normal spiral bands), and still other cords arise de novo (central cords form where there is no corresponding normal fascial structure). In any given patient, a single cord may be present, multiple fingers may be affected by the same cord type, or multiple different cord types can occur in the same or different fingers.
The most common cords are pretendinous, representing fibrous thickenings of the normal pretendinous bands (Figure 5).5 These cords are located superficial to and separate from the flexor tendon sheaths, volar to the affected metacarpal. A pretendinous cord ends at approximately the natatory ligament and can cause a flexion contracture at the MCP joint but should not affect the PIP joint (Figure 2). These cords do not course near the neurovascular bundles.4
Central cords occur in the fingers, volar to the proximal phalanges and PIP joints (Figure 6). They develop in the subcutaneous adipose tissue palmar to the flexor tendon sheaths, distal to the termination of the normal pretendinous bands.1,4 A central cord can lead to a PIP joint contracture but typically will not affect the neurovascular bundle, lying completely superficial to the nerves and vessels.10 In some cases a pretendinous cord will be contiguous with a central one, resulting in fixed flexion at both the MCP and PIP joints.
Figure 6:
Dupuytren’s disease in a 65 year-old woman with a central cord. Sagittal (6a) T1-weighted and (6b) T2-weighted, and (6c) axial T1-weighted images reveal a central cord (arrows) in the subcutaneous fat volar to the ring finger flexor tendons, located palmar to the proximal phalanx and PIP joint. Note the flexion contracture at the PIP joint. (6d) 3D rendering showing a central cord superficial to the flexor tendon sheath, extending from the natatory ligament to the contracted PIP joint.
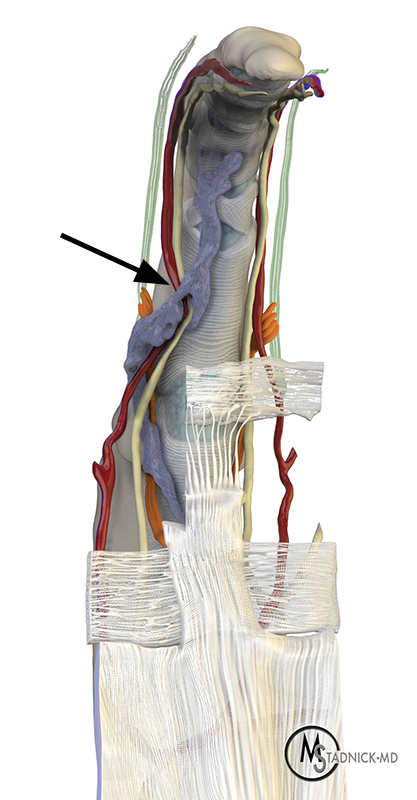
Spiral cords begin along the dorsal surfaces of the pretendinous bands near the MCP joints. Distally they extend deeper into the soft tissues (Figure 7), thickening the normal spiral bands and lateral digital sheets. However, more distally spiral cords extend back towards the midline of the digit superficial to the middle phalanx base, usually along the course of Grayson’s ligaments.5 In doing so the cord will often encircle the neurovascular bundle and displace it centrally and volarly.11 Unlike pretendinous cords, spiral cords often produce flexion contractures at the both the MCP and PIP joints of the affected fingers.4
Figure 7:
Dupuytren’s disease in a 47 year-old man with multiple cords and flexion contractures. Sagittal T1-weighted images through the (7a) ring and (7b) small fingers show spiral cords (red arrows) extending deep to the flexor tendons in addition to pretendinous cords (yellow arrows). The PIP flexion contractures would not be expected if only pretendinous cords were present. (7c) An axial T1-weighted image demonstrates the proximal aspect of the spiral cords (blue arrows) travelling deep from the pretendinous cords, adjacent to the digital nerves. A pretendinous cord has also formed volar to the long finger (red arrow). (7d) An axial T1-weighted image slightly more distally shows additional natatory cords (red arrows) oriented perpendicular to the long finger pretendinous cord. (7e) 3D rendering with partial removal of the distal pretendious band and natatory ligament demonstrates a spiral cord with associated flexion of the MCP and PIP joints, displacing the neurovascular bundle towards the midline of the finger and volarly (arrow).
Less frequently, thickening of other normal fascial bands in the fingers will form additional cord types.4,10 Natatory cords represent fibrosis of the normal natatory ligaments that run between the fingers. By themselves natatory cords do not cause flexion deformities or affect the neurovascular bundles, but they can occur in combination with other cords (Figure 7). Lateral cords that form along the normal lateral digital sheets and retrovascular cords that involve the fat alongside the proximal and middle phalanges dorsal to the neurovascular bundles both can produce PIP flexion contractures. Both types of cord also lie close to the digital nerves but only retrovascular cords tend to displace the vessels and nerves. The best clue for the surgeon that a cord potentially places the digital neurovascular bundle at risk is the presence of a PIP flexion contracture.11 Any imaging studies should specifically note whether a flexion deformity is present at the MCP joint, PIP joint, or both for any affected fingers. Lastly, additional unique cords have been described for the border digits within the thenar and hypothenar spaces, and within the proximal and distal first web spaces (Figure 8).2
Figure 8:
Dupuytren’s disease in a 61 year-old man with a hypothenar cord, presenting with a mild small finger MCP joint contracture. Axial T1-weighted images through the proximal (8a) and distal (8b) palm demonstrate a thick, subcutaneous cord (arrows) in the ulnar hand superficial to the hypothenar muscles.
Associated conditions
Patients with Dupuytren’s may also have fibromatoses elsewhere in the body. These other disorders include knuckle pads on the dorsum of the fingers, Peyronie’s disease affecting the penis, and plantar fibromatosis in the foot (Figure 9).4 Coexistence of one of these related conditions seems to be more common in patients who have “Dupuytren’s diathesis”, a disease variant characterized by earlier onset and a more aggressive disease course.10
Value of Imaging in Dupuytren’s Disease
Most cases of Dupuytren’s present with characteristic clinical findings and require no imaging to confirm the diagnosis. While it is optimistic to posit that MR imaging would contribute to the diagnosis when clinical findings are uncertain, disappointingly there is little in the literature to support that idea. Five case reports describe patients with atypical clinical presentations for whom MR was performed (ultrasound was also done in three cases) and in all 5, preoperative imaging either suggested no specific diagnosis or an incorrect one, compared to the final diagnosis of Dupuytren’s revealed at surgery.12 A prospective series of 10 patients (11 hands) did show that in patients with a known clinical diagnosis of Dupuytren’s, MR imaging was able to accurately depict the anatomic extent of disease (number, size, and depth of nodules and cords).9 However, currently surgical decision making is based on patient symptoms and contracture severity, not on the extent of disease, so using MR to map out disease extent is unlikely to be cost-effective in most cases.12 At least theoretically, identifying cords in close proximity to the neurovascular bundles would alert the surgeon about increased risk to those structures during dissection.
Yacoe et al.9 showed that the signal intensity of nodules correlated with their cellularity histologically, with nodules that were isointense compared to muscle (on both T1- and T2-weighted images) being relatively cellular (the patients in this study were likely in the second, involutional stage of disease) and those with low signal intensity being hypocellular (residual stage). This observation has potential relevance for management: The post-operative recurrence rate for nodules that are cellular (in the proliferative or involutional stages) is much higher compared to those resected in the late stage, so surgeons try to avoid operating in early stage disease.13,14 However, no imaging studies have specifically evaluated patients in the earliest proliferative stage where mitotic activity is high and the post-operative recurrence rate is highest. The signal intensity of cords does not seem to correlate with histologic findings, with most cords being hypocellular and collagenous pathologically regardless of their MR signal intensities.9 One study that correlated the ultrasound echogenicity of cords with their recurrence risk following treatment, suggested that cords with a nodular sonographic appearance were at greater risk compared with ones that appeared fibrillar, although the inter-observer agreement for these categories was low.15
Differential Diagnosis
The clinical differential diagnosis in Dupuytren’s disease depends on the initial presenting symptoms. In patients with palpable nodules or masses other potential etiologies include ganglion cysts, epidermoid inclusion cysts, rheumatoid nodules, distended tendon sheaths, tenosynovial giant cell tumor (previously called giant cell tumor of tendon sheath), and tumors. The great majority of these are readily distinguished based on clinical and imaging findings.
In the hand and fingers, ganglion cysts can form in association with the flexor tendon sheaths.16 They appear as fluid-filled unilocular or multilocular structures on MR or ultrasound examinations (Figure 10). Epidermoids develop in superficial locations following penetrating injuries that introduce skin elements into the deeper tissues;17 in the fingers they may progress to invade the underlying bone and present as a lytic lesion.18 On MR images, subcutaneous epidermoids are sharply-marginated cystic lesions, with contents that are isointense to fluid on T2-weighted images, but with variable amounts of low signal intensity debris.19 The cystic appearance of both ganglion cysts and epidermoids distinguishes them from Dupuytren’s nodules. Rheumatoid nodules have a propensity for the extensor surfaces of the hands and fingers, are variable in size and MR signal characteristics,20,21 but typically occur in patients with evidence of long-standing rheumatoid arthritis.
Figure 10:
46 year-old man with flexor tendon sheath ganglion cyst. Axial (10a) T1-weighted and (10b) fat-suppressed T2-weighted images, and (10c) sagittal T1-weighted image through the long finger show an encapsulated, fluid-filled cyst (arrows) arising from the flexor tendon sheath at the level of the A2 pulley.
Patients with hypertrophic flexor tenosynovitis – whether due to trauma/overuse, infection, inflammatory arthritis, or collagen vascular disease – may perceive a distended tendon sheath as a mass (Figure 11).16,22 While synovial-based proliferative conditions like tenosynovial giant cell tumor can extend into the subcutaneous fat of the fingers (Figure 12), relatively deep extension in continuity with a joint or the tendon sheath23 helps distinguishes these conditions from Dupuytren’s nodules. Lastly, both benign and malignant tumors within the hand can present as palpable masses.24 Those arising from bone like osteochondromas and Nora’s lesion will be identifiable on radiographs. Some primary soft tissue tumors such as encapsulated lipomas, low-flow vascular malformations (venous malformations), and benign nerve sheath tumors have characteristic signal intensities on MR images.25 Other soft tissue tumors demonstrate nonspecific signal characteristics, but any mass effect or invasion of adjacent structures would indicate a tumor rather than Dupuytren’s disease (Figure 13).
Figure 11:
28 year-old woman with chronic flexor tenosynovitis. (11a) A sagittal fat-suppressed T2-weighted image shows high signal-intensity material expanding the long finger flexor tendon sheath. The patient perceived the volar sacculations (arrows) as masses. (11b) A sagittal, IV-contrast-enhanced, fat-suppressed T1-weighted image demonstrates that the tissue represents enhancing synovitis, not fluid, extending throughout the entire length of the flexor sheath (arrows). (11c) On an axial post-contrast, fat-suppressed T1-weighted image, the abnormality surrounds the flexor tendons (arrows), and is confined to the tendon sheath, in contradistinction to Dupuytren’s disease, which occurs outside of the tendon sheath. All cultures were negative and the tenosynovitis resolved spontaneously.
Figure 12:
35 year-old man with tenosynovial giant cell tumor. Axial (12a) T1-weighted and (12b) fat-suppressed T2-weighted images demonstrate a lobulated, dumbbell-shaped mass (asterisks) in the ulnar and volar subcutaneous fat of the small finger. While the mass does extend into the fat just deep to the skin, it also involves the deeper tissues near the proximal phalanx base and tendons, which would be unusual for a Dupuytren’s nodule. At surgery, a bridge of tissue (arrow) connected the lesion to the flexor tendon sheath from which it arose.
Figure 13:
61-year-old man with an unclassified soft tissue sarcoma. (13a) A sagittal T2-weighted image shows a relatively low-signal intensity, bilobed soft tissue mass (arrows) volar to the index finger PIP joint. While these signal characteristics could be seen in Dupuytren’s nodules, the location deep to the flexor tendons and adjacent to the bone, like in Figure 12, should suggest an alternate diagnosis. (13b) Frank bone invasion (asterisks) shown on a coronal T1-weighted image excludes Dupuytren’s disease and indicates a neoplasm.
For patients presenting with flexion contractures, structural causes like prior fracture malunions will be evident on radiographs while clinical history, laboratory studies, and radiographs usually suffice to identify inflammatory arthritis (typically rheumatoid or a seronegative arthritis), and collagen-vascular diseases (e.g., scleroderma) that cause finger deformities.
Diabetic cheiroarthropathy causes painless flexion contractures. This condition occurs in approximately 16-28% of patients with long-standing type 1 or 2 diabetes mellitus.26,27 Patients present with waxy, thickening of the skin on the dorsum of the hand and joint stiffness, followed by inability to fully extend the fingers. The etiology is thought to be abnormal cross-linking of collagen related to poor glycemic control.28 Diagnosis is typically made clinically; little literature exists describing the imaging findings of cheiroarthropathy. Thickening and enhancement of the flexor tendon sheaths are the cited abnormalities.29,30
The other main differential diagnoses for flexion deformities are disorders of the flexor tendons and sheaths. Stenosing flexor tenosynovitis (known clinically as “trigger finger”) results from chronic irritation that thickens the A1 pulley of the MCP joint, most commonly involving the thumb or ring finger.31 Hypertrophic tendinosis and nodularity of the associated flexor tendon can impede normal tendon gliding under the affected pulley, causing intermittent clicking or painful snapping of the digit.32 Similar to Dupuytren’s and cheiroarthropathy, stenosing tenosynovitis is more prevalent in diabetic patients, especially those with elevated hemoglobin A1c levels.33 MR images demonstrate a spectrum of findings in patients with stenosing tenosynovitis. Unlike cases with inflammatory or proliferative synovitis (See Figure 11), hands with stenosing tenosynovitis tend to have minimal or mild distension of the tendon sheaths and intravenous contrast administration may be necessary to distinguish a small amount of fluid from tenosynovitis (Figure 14). Thickening of the A1 pulley (usually > 1 mm, with the normal pulley measuring approximately 0.5 mm in thickness) at the level of the MCP is characteristic (Figure 15).34 The thickened pulley will appear edematous, and will enhance if intravenous contrast is administered; additionally a focal intratendinous nodule may be present in the affected tendon.35 In more severe cases further hypertrophy and scarring of the underlying tendons will cause the finger to become locked in a flexed position (Figure 16), which can mimic a Dupuytren’s contracture clinically. Stenosing tenosynovitis can coexist with Dupuytren’s disease in the same or different fingers (Figure 17).36 Management is with nonsteroidal anti-inflammatory drugs, orthotics, and corticosteroid injections. Refractory cases require percutaneous or open A1 pulley release.37,38
Figure 14:
72 year-old woman with early stenosing tenosynovitis. Axial, fat-suppressed T2-weighted (14a) and intravenous contrast-enhanced T1-weighted (14b) images show a minimal volume of enhancing synovitis in the ring finger flexor tendon sheath (red arrows). Note that the small amount of high-signal-intensity material in the fourth MCP joint on the T2-weighted images does not enhance (yellow arrows) and represents simple joint fluid, not synovitis.
Figure 15:
51 year-old woman with triggering of the index and long fingers. Axial (15a) T1-weighted and (15b) fat-suppressed T2-weighted images reveal thickening and edema of the A1 pulleys (red arrows), which are usually barely perceptible. The sagittal (15c) T1-weighted and (15d) T2-weighted images show no enlargement of the underlying tendons or joint contractures in this relatively mild example. Note tiny amount of fluid or synovitis in the more distal flexor tendon sheath (yellow arrow).
Figure 16:
72 year-old woman with severe stenosing tenosynovitis and flexion contracture. Sagittal (16a) STIR and (16b) T2-weighted images show a PIP flexion contracture and severe enlargement and indistinctness of the long finger flexor tendons at the level of the proximal phalanx (red arrow). Observe that tenosynovial fluid/synovitis tends to collect in regions where the tendons are not thickened (blue arrow). Axial (16c) T1-weighted and (16d) fat-suppressed T2-weighted images demonstrate that the findings are limited to the flexor apparatus, distinguishing this condition from Dupuytren’s disease. The long finger flexor tendons are severely enlarged (red arrows) and the A2 pulley is thickened and edematous (yellow arrows).
Figure 17:
74 year-old woman with combined stenosing tenosynovitis and Dupuytren’s disease. (17a and 17b) Sagittal STIR images through the ring finger demonstrate a pretendinous cord (red arrow) as well as an edematous A1 pulley (blue arrow). Note the developing mild MCP flexion contracture. (17c) On the axial, fat-suppressed T2-weighted image abnormalities are present both superficial to the tendon sheath (pretendinous cord, red arrow) and within the sheath (small amount of fluid or tenosynovitis, yellow arrow).
Complete ruptures of the flexor tendons or pulleys result in limitations of finger flexion, but usually do not cause triggering or contractures. However, in some cases of partial tendon tear, a loose piece of the torn tendon or hypertrophic granulation tissue will create a focal mass within the tendon sheath, with or without irritation of the adjacent pulley, and produce clinical findings analogous to those of stenosing tenosynovitis (Figure 18).39 Again, recognizing that the MR imaging findings are associated with the tendons and sheaths helps distinguish this condition from Dupuytren’s disease, where all the abnormalities should be outside of the flexor sheath.
Figure 18:
60-year-old woman with intermittent small finger triggering that developed after a partial flexor tendon tear. Axial (18a) T1-weighted and (18b) fat-suppressed T2-weighted images show hypertrophied granulation tissue (red arrow) associated with a healing partial-thickness tear of the flexor digitorum profundus tendon, as well as a thickened, edematous A1 pulley (yellow arrow).
Management
In general, conservative measures like physical therapy and splinting do not slow the progression or reverse the symptoms of Dupuytren’s disease. While disease progression is common, the natural history is variable and some patients will never develop contractures.10,40 Thus, mild cases are simply observed. When symptoms interfere with hand function, several treatment options are available. Percutaneous needle aponeurotomy and collagenase injection (“enzymatic fasciotomy”) can be used to rupture cords and decrease symptoms.41,42,43 Radiotherapy has also been tried with one study suggesting that lesions with higher signal intensity on pre-treatment T2-weighted images may respond better to electron beam radiation.8 As contractures and functional limitation progress (30° flexion contracture at the MCP joint and 15° at the PIP joint are typical cut-offs), surgery is the next step – most commonly a partial or subtotal fasciotomy with the aim of removing diseased fascia.1,6 Recurrent and progressive disease is common following any treatment, but even in such cases, there is usually a gain in finger extension despite the return or new development of cords.44 Surgical resection carries a higher recurrence risk when performed during the proliferative phase of the disease.7 The main risk of surgery is iatrogenic injury to the digital nerves,44,45 which is highest in patients with spiral bands.
Conclusion
Dupuytren’s disease is an idiopathic fibrosing condition affecting the hands and fingers of middle age and older individuals. The pathologic findings consist of painless, volar subcutaneous contracting nodules and thickened fibrotic cords, which form along normal palmar and digital fascial elements or de novo. The cords tend to occur in predictable patterns, pretendinous being the most common and spiral being the one with the most severe clinically implications. The cord location and type determines whether flexion contractures will develop at the MCP and/or PIP joints and whether the neurovascular bundles will be involved or at risk of iatrogenic injury if surgery is needed. On MR images, the radiologist should try to identify the location of any cords and note their relationship to the digital nerves and the presence of joint contractures, as these findings influence surgical management. Imaging (with MR, supplemented by radiographs or ultrasound in selected cases) is also useful in cases where the cause of a nodule or flexion abnormality is uncertain. In the latter case, the main differential diagnoses are conditions involving the flexor tendons, sheaths, and pulleys.
References
- Grazina R, Teixeira S, Ramos R, Sousa H, Ferreira A, Lemos R. Dupuytren’s disease: where do we stand? EFORT Open Rev. 2019;4(2):63-69. doi:10.1302/2058-5241.4.180021 ↩
- Rayan GM. Clinical presentation and types of Dupuytren’s disease. Hand Clin. 1999;15(1):87-96, vii. ↩
- Strickland JW, Leibovic SJ. Anatomy and pathogenesis of the digital cords and nodules. Hand Clin. 1991;7(4):645-657; discussion 659-660. ↩
- Shaw RB, Jr., Chong AK, Zhang A, Hentz VR, Chang J. Dupuytren’s disease: history, diagnosis, and treatment. Plast Reconstr Surg. 2007;120(3):44e-54e. doi:10.1097/01.prs.0000278455.63546.03 ↩
- Rayan GM. Dupuytren disease: Anatomy, pathology, presentation, and treatment. J Bone Joint Surg Am. 2007;89(1):189-198. doi:10.2106/00004623-200701000-00026 ↩
- Mella JR, Guo L, Hung V. Dupuytren’s Contracture: An Evidence Based Review. Ann Plast Surg. 2018;81(6S Suppl 1):S97-S101. doi:10.1097/SAP.0000000000001607 ↩
- Balaguer T, David S, Ihrai T, Cardot N, Daideri G, Lebreton E. Histological staging and Dupuytren’s disease recurrence or extension after surgical treatment: a retrospective study of 124 patients. J Hand Surg Eur Vol. 2009;34(4):493-496. doi:10.1177/1753193408103729 ↩
- Banks JS, Wolfson AH, Subhawong TK. T2 signal intensity as an imaging biomarker for patients with superficial Fibromatoses of the hands (Dupuytren’s disease) and feet (Ledderhose disease) undergoing definitive electron beam irradiation. Skeletal Radiol. 2018;47(2):243-251. doi:10.1007/s00256-017-2792-5 ↩
- Yacoe ME, Bergman AG, Ladd AL, Hellman BH. Dupuytren’s contracture: MR imaging findings and correlation between MR signal intensity and cellularity of lesions. AJR Am J Roentgenol. 1993;160(4):813-817. doi:10.2214/ajr.160.4.8456670 ↩
- Townley WA, Baker R, Sheppard N, Grobbelaar AO. Dupuytren’s contracture unfolded. BMJ. 2006;332(7538):397-400. doi:10.1136/bmj.332.7538.397 ↩
- Umlas ME, Bischoff RJ, Gelberman RH. Predictors of neurovascular displacement in hands with Dupuytren’s contracture. J Hand Surg Br. 1994;19(5):664-666. doi:10.1016/0266-7681(94)90140-6 ↩
- Molenkamp S, van Straalen RJM, Werker PMN, Broekstra DC. Imaging for Dupuytren disease: a systematic review of the literature. BMC Musculoskelet Disord. 2019;20(1):224. doi:10.1186/s12891-019-2606-0 ↩
- Rombouts JJ, Noel H, Legrain Y, Munting E. Prediction of recurrence in the treatment of Dupuytren’s disease: evaluation of a histologic classification. J Hand Surg Am. 1989;14(4):644-652. doi:10.1016/0363-5023(89)90183-4 ↩
- Adam RF, Loynes RD. Prognosis in Dupuytren’s disease. J Hand Surg Am. 1992;17(2):312-317. doi:10.1016/0363-5023(92)90413-j ↩
- Vanek P, Stromberg J, Friden J, Aurell Y. Morphological patterns of the pretendinous cord in Dupuytren’s disease: a predictor of clinical outcome? J Plast Surg Hand Surg. 2018;52(4):240-244. doi:10.1080/2000656X.2018.1470521 ↩
- Kato H, Minami A, Hirachi K, Kasashima T. Treatment of flexor tendon sheath ganglions using ultrasound imaging. J Hand Surg Am. 1997;22(6):1027-1033. doi:10.1016/S0363-5023(97)80043-3 ↩
- Nahra ME, Bucchieri JS. Ganglion cysts and other tumor related conditions of the hand and wrist. Hand Clin. 2004;20(3):249-260, v. doi:10.1016/j.hcl.2004.03.015 ↩
- Simon K, Leithner A, Bodo K, Windhager R. Intraosseous epidermoid cysts of the hand skeleton: a series of eight patients. J Hand Surg Eur Vol. 2011;36(5):376-378. doi:10.1177/1753193411401987 ↩
- Shibata T, Hatori M, Satoh T, Ehara S, Kokubun S. Magnetic resonance imaging features of epidermoid cyst in the extremities. Arch Orthop Trauma Surg. 2003;123(5):239-241. doi:10.1007/s00402-003-0509-9 ↩
- el-Noueam KI, Giuliano V, Schweitzer ME, O’Hara BJ. Rheumatoid nodules: MR/pathological correlation. J Comput Assist Tomogr. 1997;21(5):796-799. doi:10.1097/00004728-199709000-00027 ↩
- Starok M, Eilenberg SS, Resnick D. Rheumatoid nodules: MRI characteristics. Clin Imaging. 1998;22(3):216-219. doi:10.1016/s0899-7071(97)00116-2 ↩
- Tehranzadeh J, Ashikyan O, Anavim A, Tramma S. Enhanced MR imaging of tenosynovitis of hand and wrist in inflammatory arthritis. Skeletal Radiol. 2006;35(11):814-822. doi:10.1007/s00256-006-0129-x ↩
- Kitagawa Y, Ito H, Amano Y, Sawaizumi T, Takeuchi T. MR imaging for preoperative diagnosis and assessment of local tumor extent on localized giant cell tumor of tendon sheath. Skeletal Radiol. 2003;32(11):633-638. doi:10.1007/s00256-003-0689-y ↩
- Kransdorf MJ, Murphey MD. MR imaging of musculoskeletal tumors of the hand and wrist. Magn Reson Imaging Clin N Am. 1995;3(2):327-344. ↩
- Kransdorf MJ. Benign soft-tissue tumors in a large referral population: distribution of specific diagnoses by age, sex, and location. AJR Am J Roentgenol. 1995;164(2):395-402. doi:10.2214/ajr.164.2.7839977 ↩
- Abourazzak FE, Akasbi N, Houssaini GS, Bazouti S, Bensbaa S, Hachimi H, et al. Articular and abarticular manifestations in type 2 diabetes mellitus. Eur J Rheumatol. 2014;1(4):132-134. doi:10.5152/eurjrheumatol.2014.140050 ↩
- Larkin ME, Barnie A, Braffett BH, Cleary PA, Diminick L, Harth J, et al. Musculoskeletal complications in type 1 diabetes. Diabetes Care. 2014;37(7):1863-1869. doi:10.2337/dc13-2361 ↩
- Hill NE, Roscoe D, Stacey MJ, Chew S. Cheiroarthropathy and tendinopathy in diabetes. Diabet Med. 2019;36(8):939-947. doi:10.1111/dme.13955 ↩
- Ismail AA, Dasgupta B, Tanqueray AB, Hamblin JJ. Ultrasonographic features of diabetic cheiroarthropathy. Br J Rheumatol. 1996;35(7):676-679. doi:10.1093/rheumatology/35.7.676 ↩
- Khanna G, Ferguson P. MRI of diabetic cheiroarthropathy. AJR Am J Roentgenol. 2007;188(1):W94-95. doi:10.2214/AJR.06.0672 ↩
- Ryzewicz M, Wolf JM. Trigger digits: principles, management, and complications. J Hand Surg Am. 2006;31(1):135-146. doi:10.1016/j.jhsa.2005.10.013 ↩
- Chuang XL, Ooi CC, Chin ST, Png MA, Wong SK, Tay SC, et al. What triggers in trigger finger? The flexor tendons at the flexor digitorum superficialis bifurcation. J Plast Reconstr Aesthet Surg. 2017;70(10):1411-1419. doi:10.1016/j.bjps.2017.05.037 ↩
- Vance MC, Tucker JJ, Harness NG. The association of hemoglobin A1c with the prevalence of stenosing flexor tenosynovitis. J Hand Surg Am. 2012;37(9):1765-1769. doi:10.1016/j.jhsa.2012.06.007 ↩
- Guerini H, Pessis E, Theumann N, Le Quintrec JS, Campagna R, Chevrot A, et al. Sonographic appearance of trigger fingers. J Ultrasound Med. 2008;27(10):1407-1413. doi:10.7863/jum.2008.27.10.1407 ↩
- Chang EY, Chen KC, Chung CB. MR imaging findings of trigger thumb. Skeletal Radiol. 2015;44(8):1201-1207. doi:10.1007/s00256-015-2172-y ↩
- Yang K, Gehring M, Bou Zein Eddine S, Hettinger P. Association between Stenosing Tenosynovitis and Dupuytren’s Contracture in the Hand. Plast Reconstr Surg Glob Open. 2019;7(1):e2088. doi:10.1097/GOX.0000000000002088 ↩
- Giugale JM, Fowler JR. Trigger Finger: Adult and Pediatric Treatment Strategies. Orthop Clin North Am. 2015;46(4):561-569. doi:10.1016/j.ocl.2015.06.014 ↩
- Lunsford D, Valdes K, Hengy S. Conservative management of trigger finger: A systematic review. J Hand Ther. 2019;32(2):212-221. doi:10.1016/j.jht.2017.10.016 ↩
- Couceiro J, Fraga J, Sanmartin M. Trigger finger following partial flexor tendon laceration: Magnetic resonance imaging-assisted diagnosis. Int J Surg Case Rep. 2015;9112-114. doi:10.1016/j.ijscr.2015.03.001 ↩
- Gudmundsson KG, Arngrimsson R, Jonsson T. Eighteen years follow-up study of the clinical manifestations and progression of Dupuytren’s disease. Scand J Rheumatol. 2001;30(1):31-34. doi:10.1080/030097401750065292 ↩
- Dritsaki M, Rivero-Arias O, Gray A, Ball C, Nanchahal J. What do we know about managing Dupuytren’s disease cost-effectively? BMC Musculoskelet Disord. 2018;19(1):34. doi:10.1186/s12891-018-1949-2 ↩
- Hurst LC, Badalamente MA, Hentz VR, Hotchkiss RN, Kaplan FT, Meals RA, et al. Injectable collagenase clostridium histolyticum for Dupuytren’s contracture. N Engl J Med. 2009;361(10):968-979. doi:10.1056/NEJMoa0810866 ↩
- Karkampouna S, Kreulen M, Obdeijn MC, Kloen P, Dorjee AL, Rivellese F, et al. Connective Tissue Degeneration: Mechanisms of Palmar Fascia Degeneration (Dupuytren’s Disease). Curr Mol Biol Rep. 2016;2(3):133-140. doi:10.1007/s40610-016-0045-3 ↩
- Henry M. Dupuytren’s disease: current state of the art. Hand (N Y). 2014;9(1):1-8. doi:10.1007/s11552-013-9563-0 ↩
- Chen NC, Srinivasan RC, Shauver MJ, Chung KC. A systematic review of outcomes of fasciotomy, aponeurotomy, and collagenase treatments for Dupuytren’s contracture. Hand (N Y). 2011;6(3):250-255. doi:10.1007/s11552-011-9326-8 ↩