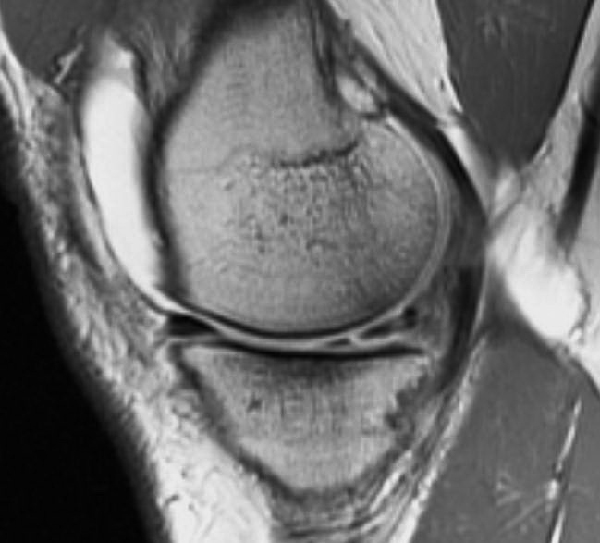
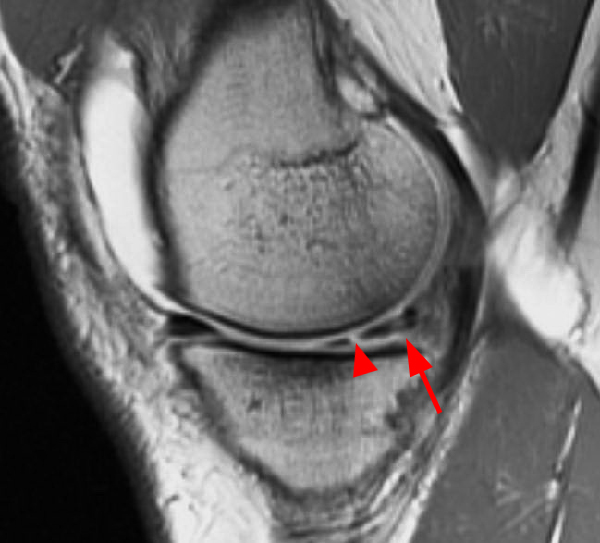
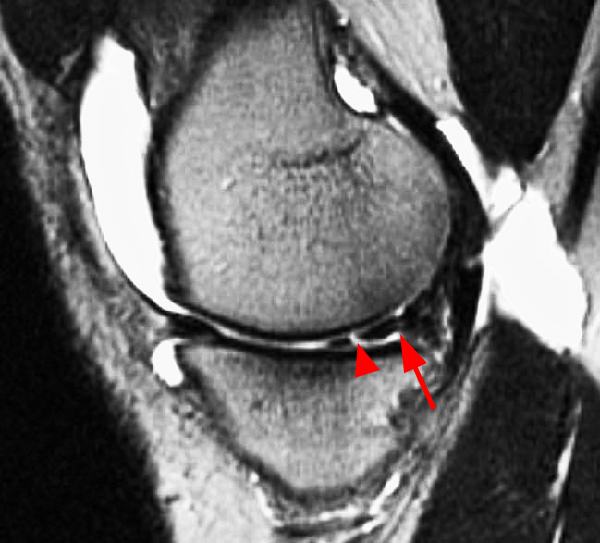
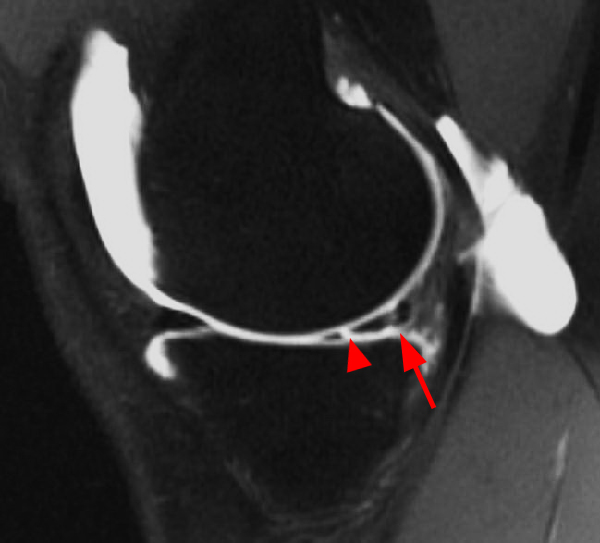
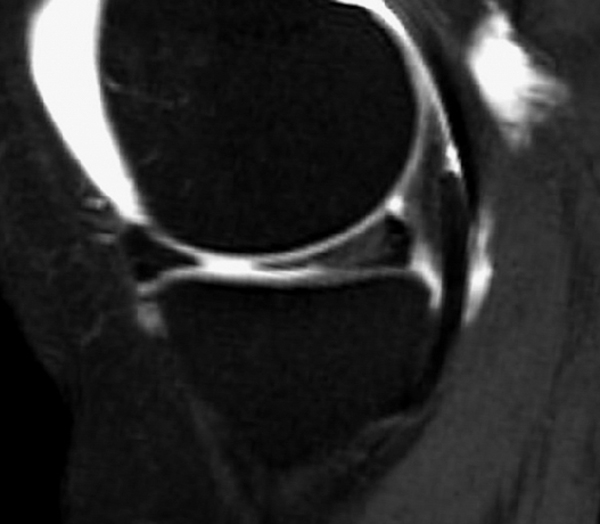
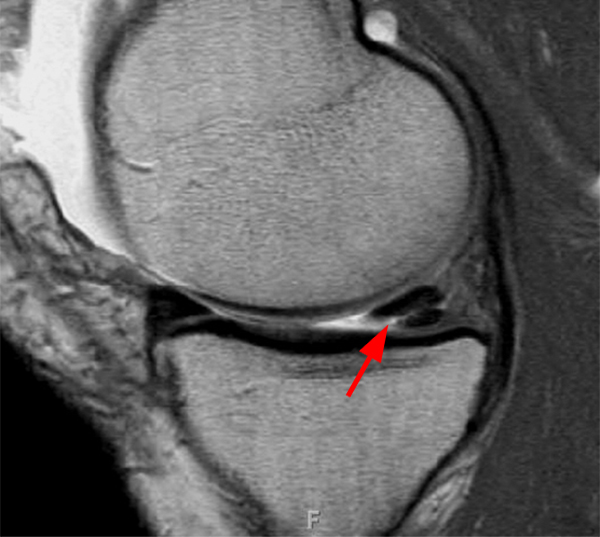
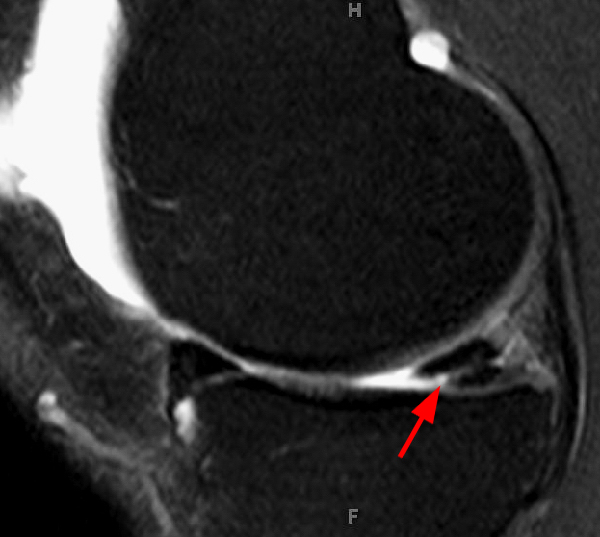
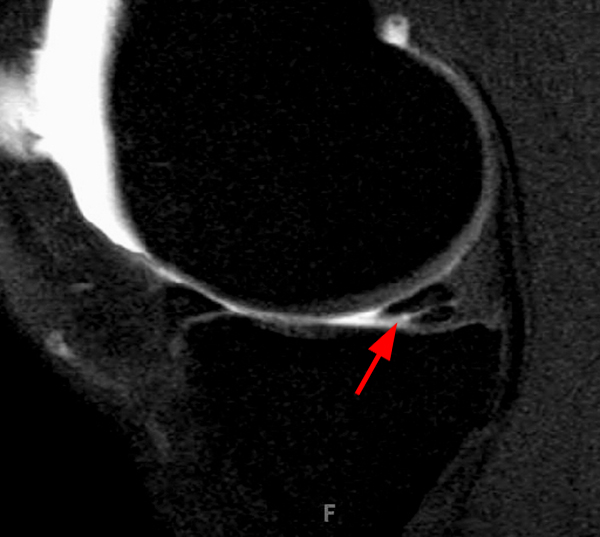
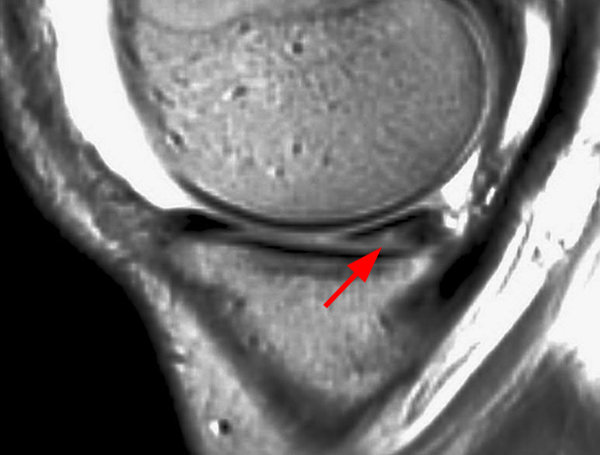
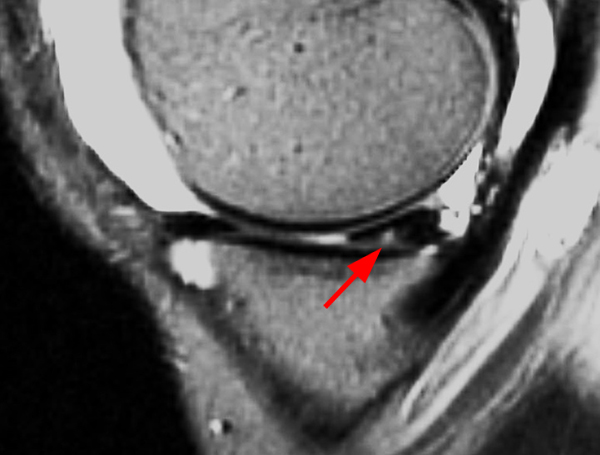
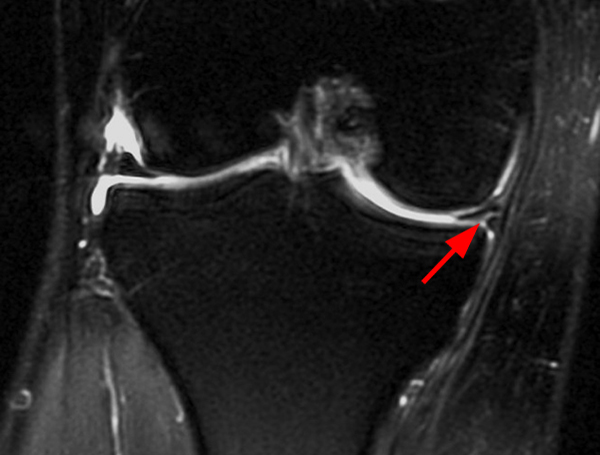
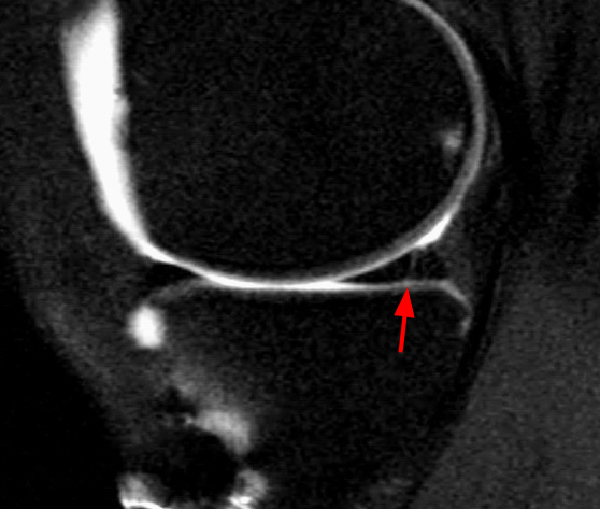
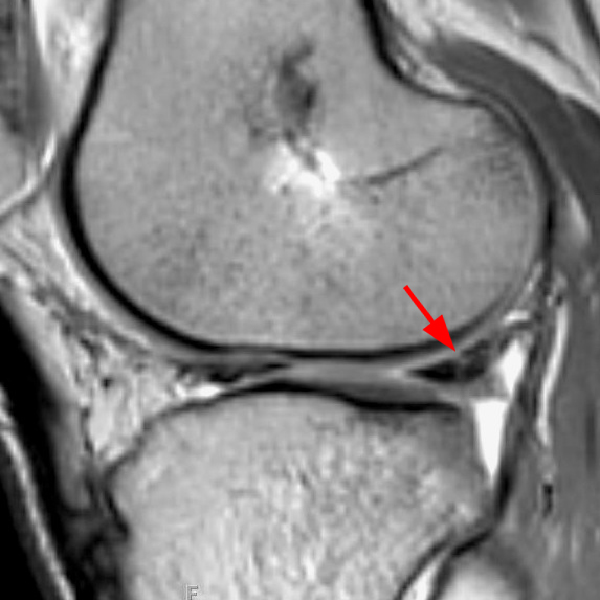
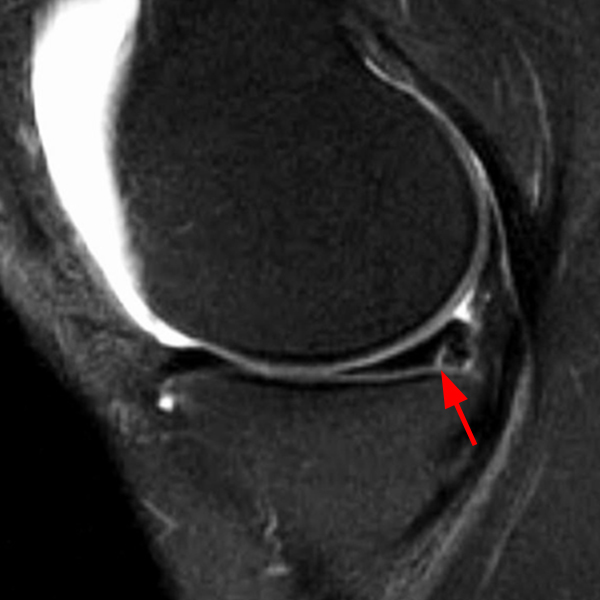
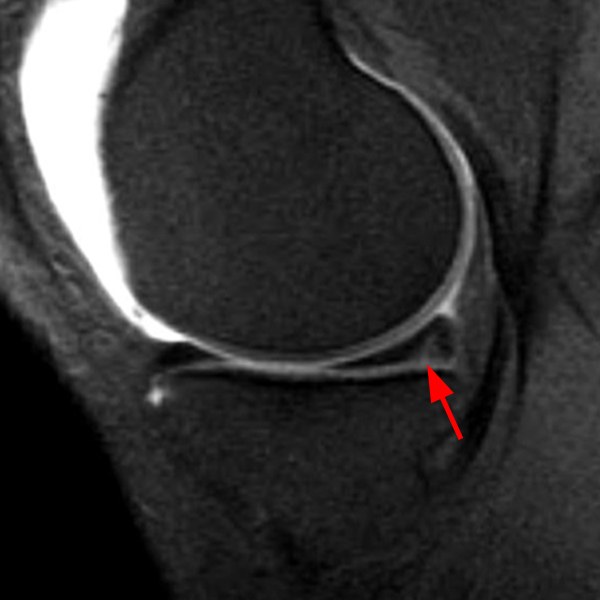
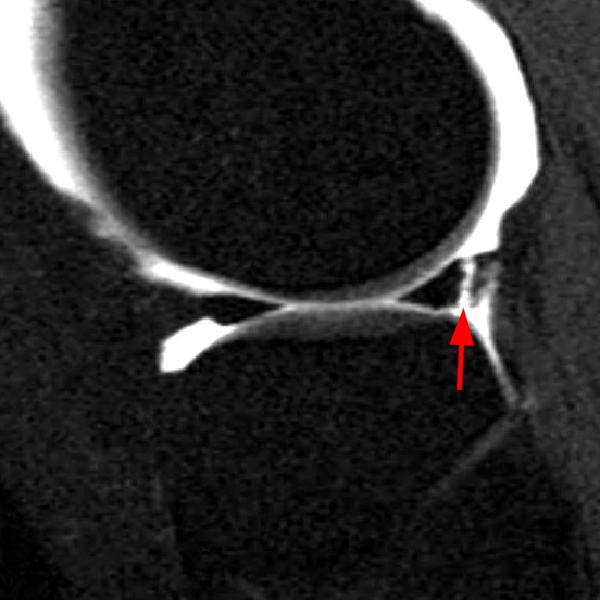
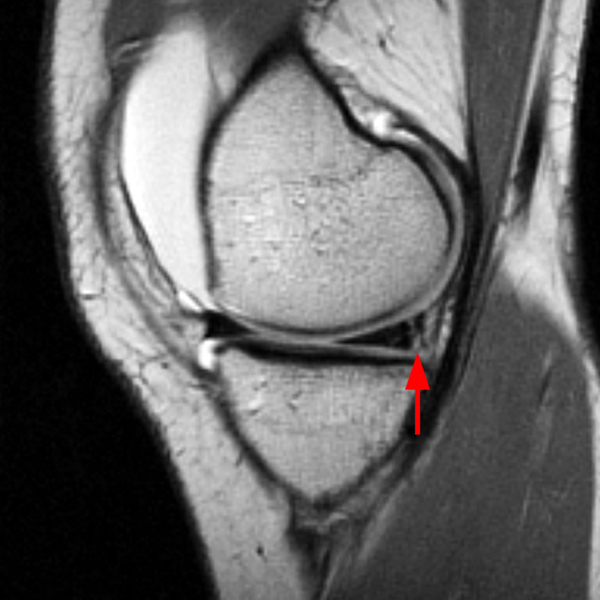
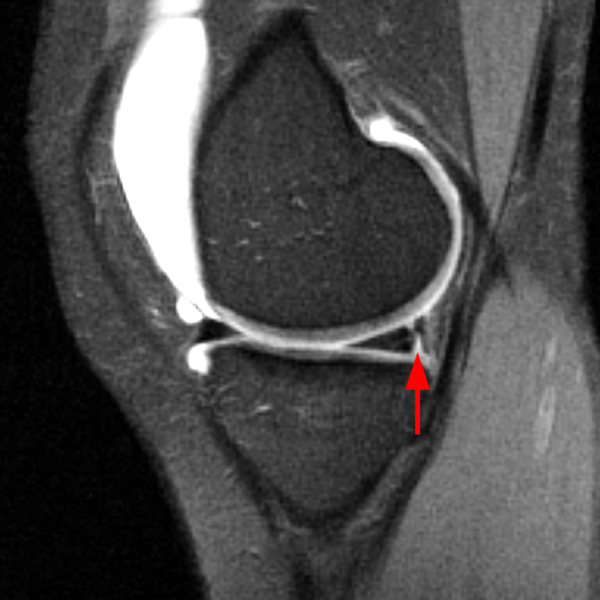
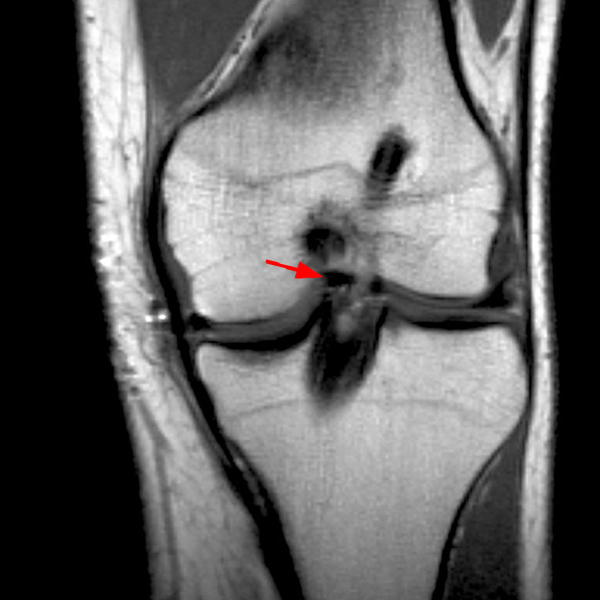
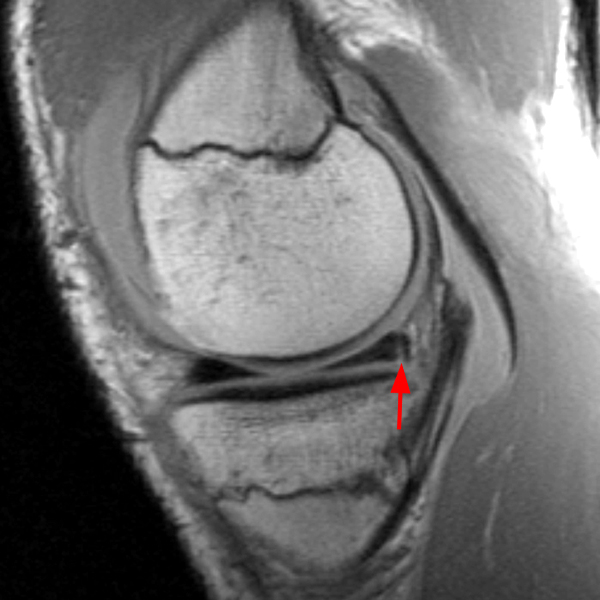
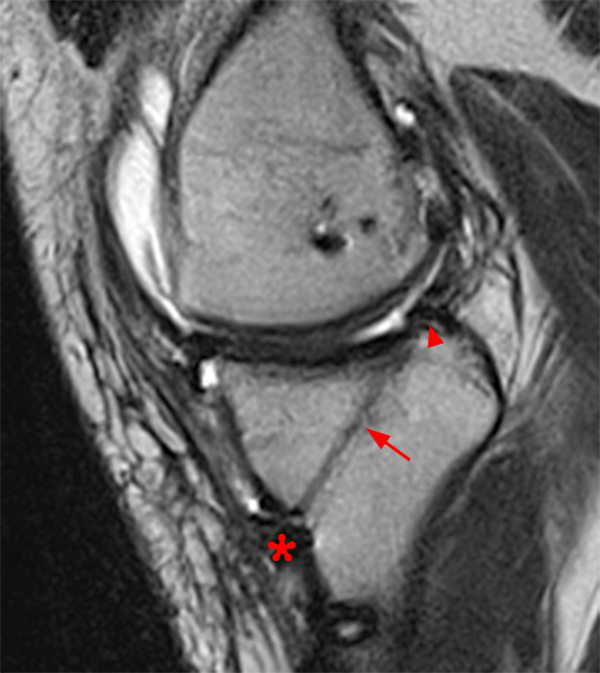
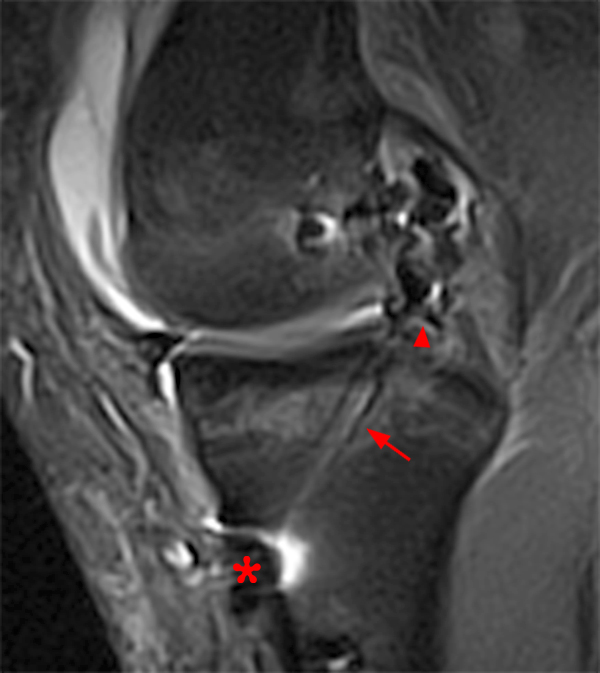
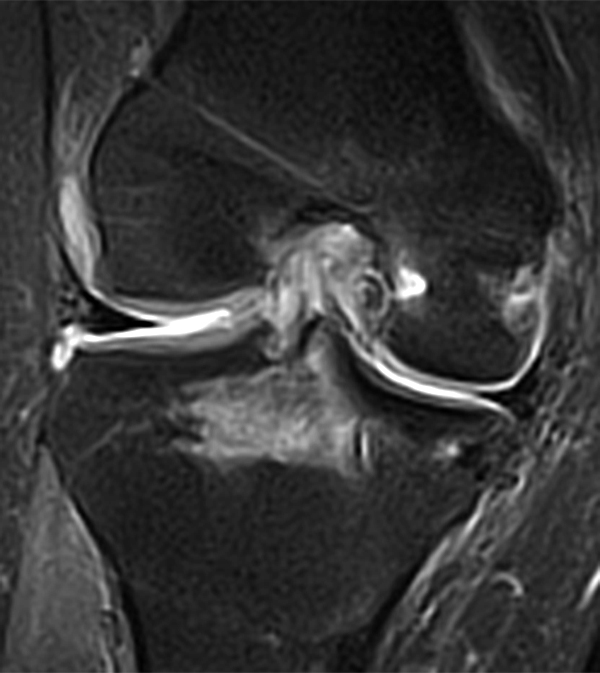
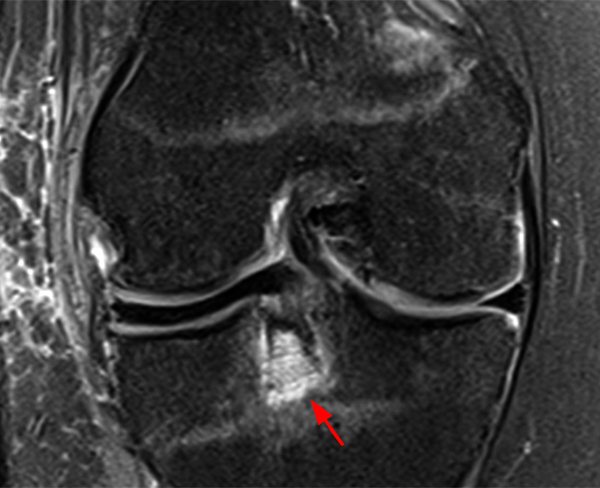
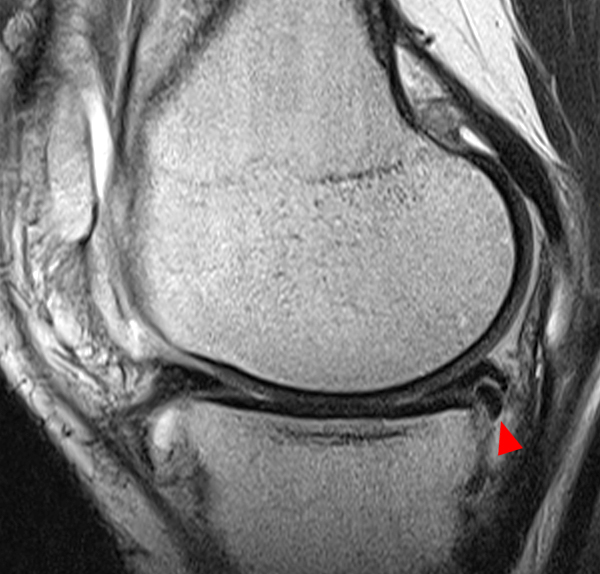
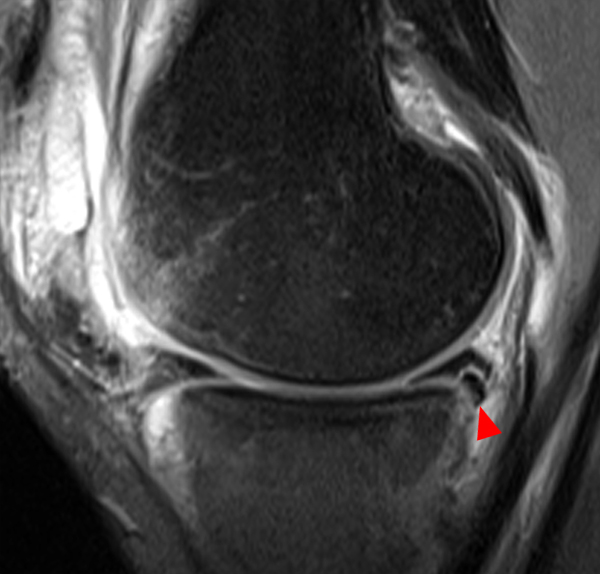
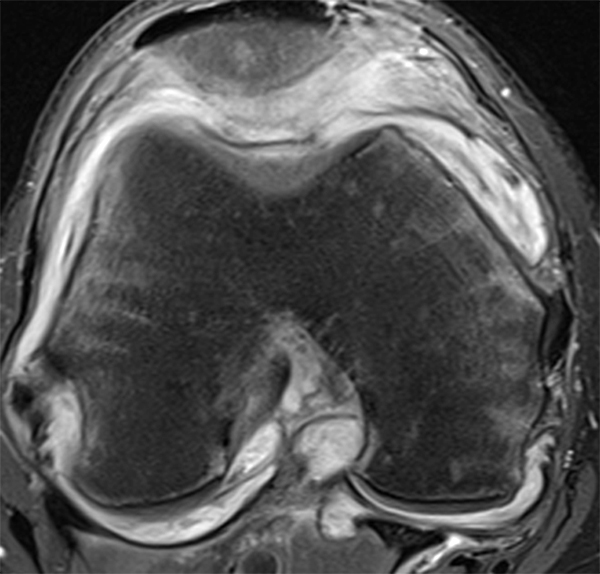
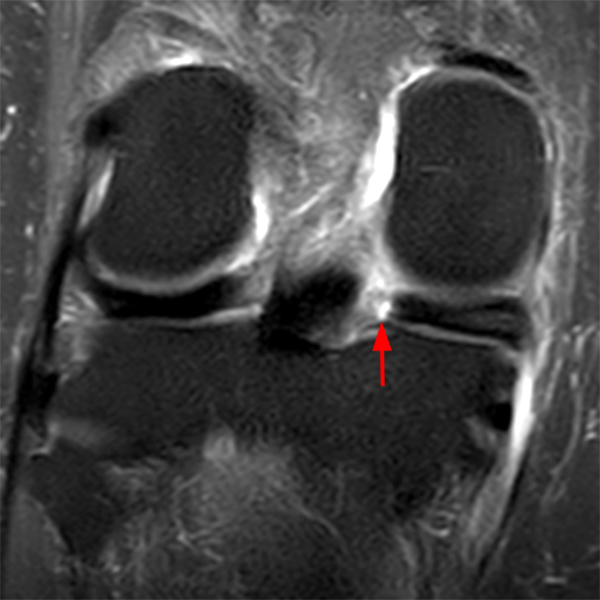
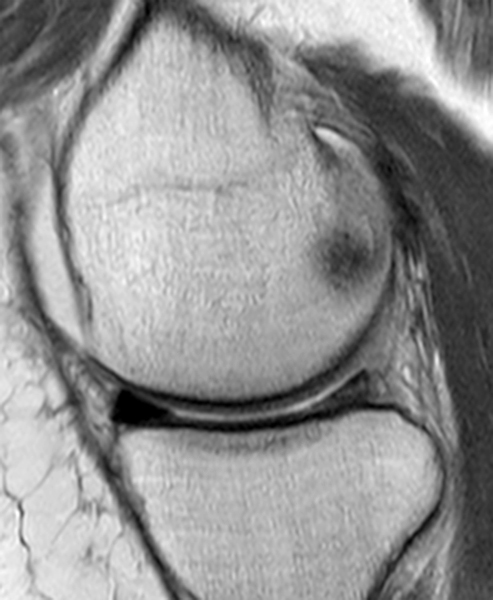
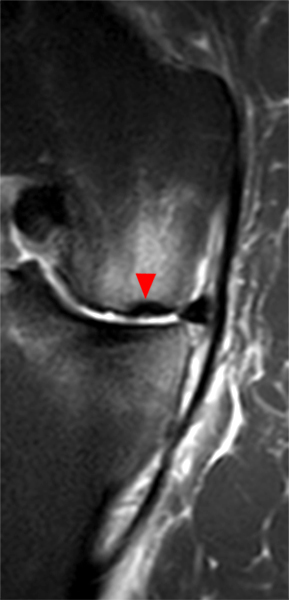
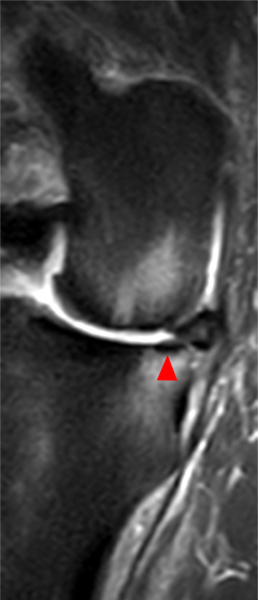
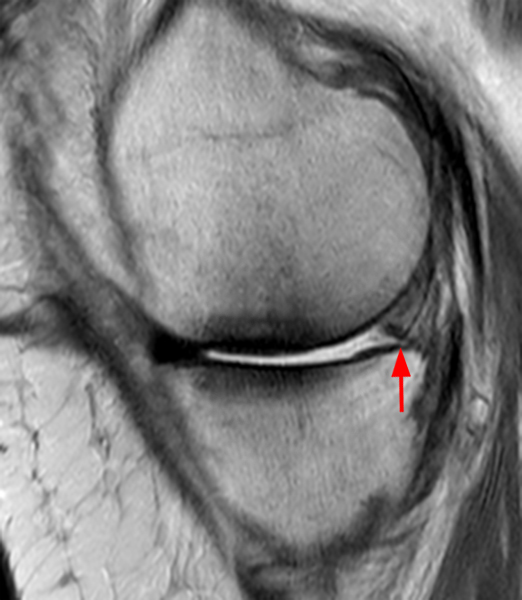
Clinical History: An 18 year-old male with a history of a posterior horn medial meniscus peripheral longitudinal tear treated with meniscal repair at age 16 presents for MR imaging. The patient had a recent new injury with increased pain. (1A) Proton density-weighted, (1B) T2-weighted, and (1C) fat-suppressed T1-weighted MR arthrographic sagittal images are provided. What are the findings? What is your diagnosis?
Findings
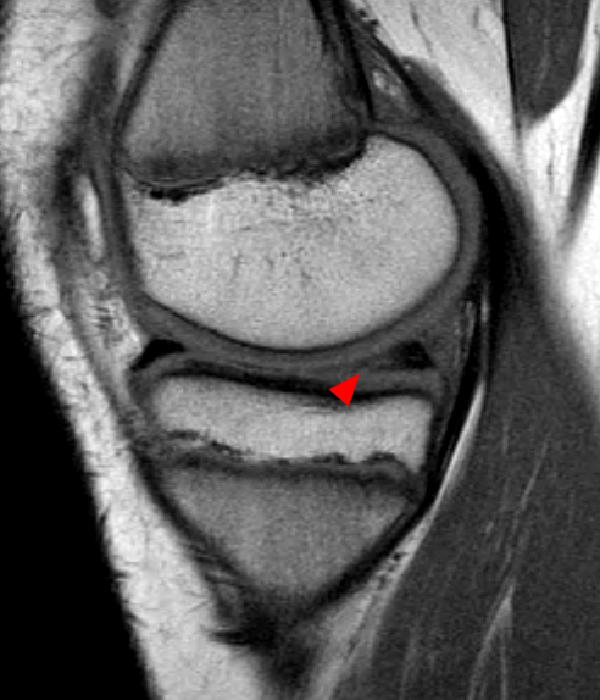
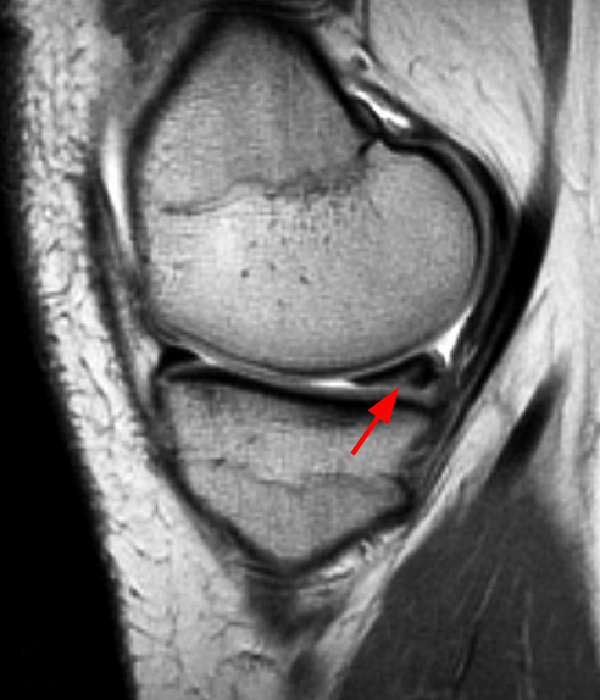
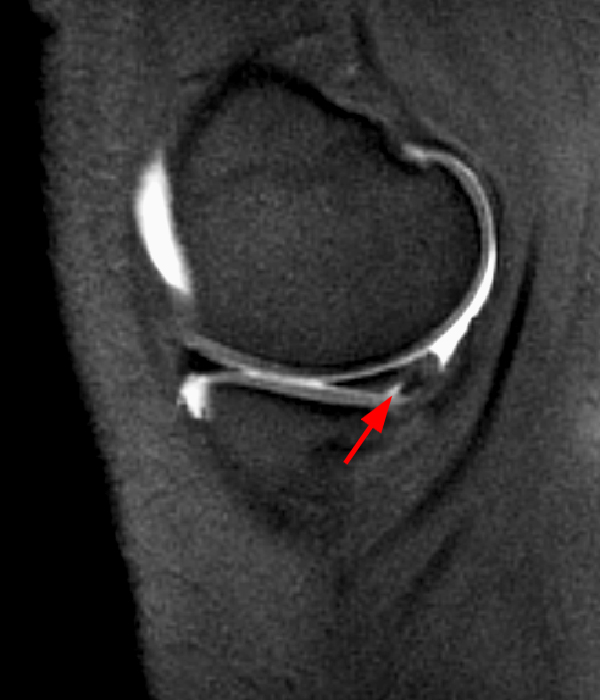
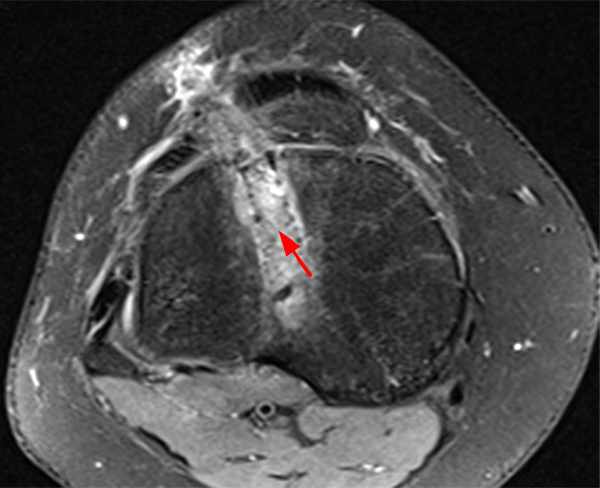
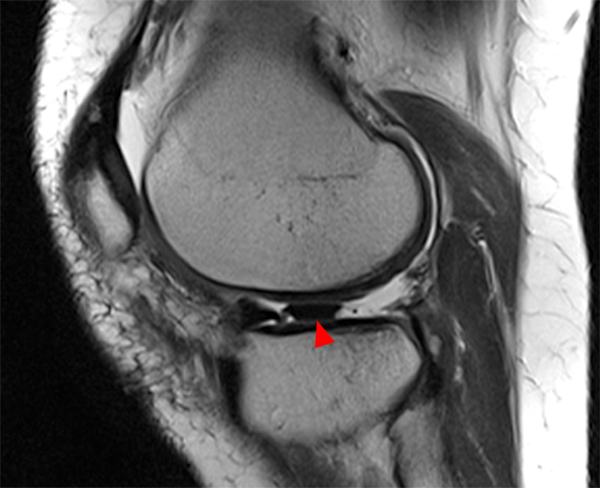
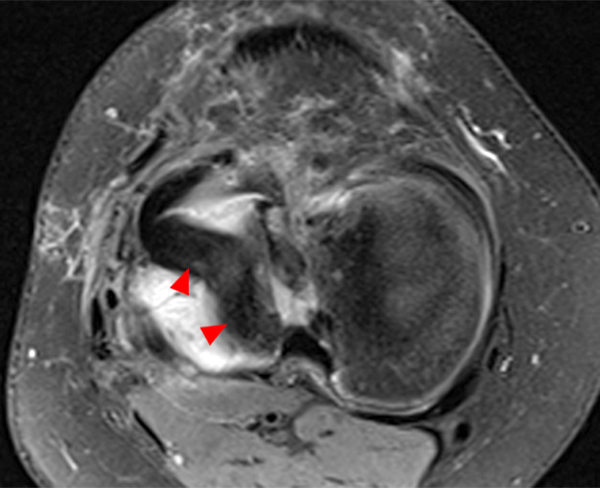
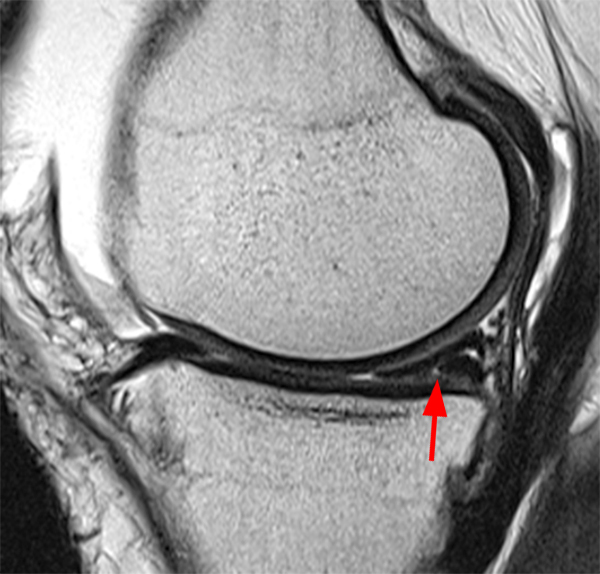
Figure 2:
The sagittal proton density-weighted image (2A) demonstrates increased signal intensity at the periphery of the medial meniscus posterior horn (arrow) but no fluid signal on the sagittal T2-weighted image (2B) and no gadolinium extension into this area on the MR arthrogram sagittal fat-suppressed T1-weighted arthrographic image (2C) consistent with a healed repair. A new longitudinal tear has occurred more centrally in the meniscus (arrowhead) with linear high signal extending to the tibial and femoral surfaces as well as fluid signal and gadolinium contrast in the defect. Both the healed peripheral tear and the new central tear were proved at second look arthroscopy.
Diagnosis
Healed peripheral medial meniscus posterior horn repair and new longitudinal tear in a different location.
Introduction
Meniscal tears are common and often associated with knee pain. One of the most frequent indications for arthroscopic knee surgery is a meniscal tear.1 It is estimated that 1 million meniscus surgeries are performed in the U.S. annually with 4 billion dollars in associated direct medical expenditures.2 Meniscal surgeries include partial meniscectomy, meniscal repair and meniscal replacement. Partial meniscectomy is by far the most common procedure. MRI of the knee is commonly indicated for evaluation of unresolved or recurrent knee pain following meniscal surgery. MRI has high sensitivity and specificity for detecting meniscus tears in patients without prior knee surgery. Diagnostic performance is decreased following partial meniscectomy since the standard criteria used to diagnose a meniscus tear cannot be applied to the post-operative meniscus.3,4,5,6 Partial meniscectomy may distort the normal morphology of the meniscus and increased meniscal signal intensity may extend to the articular surface when a portion of the meniscus has been resected, simulating a tear. 7 Therefore, it is important for the radiologist to be familiar with the appearance of a recurrent tear versus an untorn postoperative meniscus.
Anatomy
The menisci are C-shaped fibrocartilaginous structures composed of radial and circumferential collagen fibers that have several roles, including joint stabilization, load distribution, articular cartilage protection and joint lubrication. Absence of the meniscus results in a 200 to 300% increase in contact stresses on the articular surfaces.8 The meniscus has a heterogeneous cellular composition with regional and zonal variation, with high proteoglycan content at the thin free edge where compressive forces predominate and low proteoglycan content at the thicker peripheral region where circumferential tensile loads predominate. Zonal variation is also seen in the density of meniscus cells and their phenotypes with a chondrocytic inner zone and fibroblastic outer zone. Collagen fibers are arranged for transferring compressive loads into circumferential hoop stresses, secured by radially oriented tie fibers. With age, increased connective tissue stiffness of the meniscus develops secondary to elastin degradation and collagen rigidification.2
The medial meniscus covers 60% of the medial compartment. Both horns of the medial meniscus are triangular with sharp points. The posterior horn is always larger than the anterior horn. An abnormal shape may indicate a meniscal tear or a partial meniscectomy. The posterior root lies anterior to the posterior cruciate ligament. If missing on MR images, a posterior root tear is present. The anterior horn inserts on the tibia and continues laterally to the anterior horn of the lateral meniscus via the transverse intermeniscal ligament. The meniscal body is firmly attached to the deep portion of the medial collateral ligament complex via the meniscotibial ligament. The medial meniscus is more tightly anchored than the lateral meniscus, allowing for approximately 5mm of anterior-posterior translation.
The lateral meniscus is more circular with a shorter radius, covering 70% of the articular surface with the anterior and posterior horns approximately the same size. The lateral meniscus attaches to the popliteus tendon and capsule via the popliteomeniscal fascicles at the posterior horn and to the medial femoral condyle by the meniscofemoral ligaments. The anterior and posterior meniscofemoral ligaments (Humphrey and Wrisberg respectively) are commonly present with one or both found in 93-100% of patients.9 The lateral meniscus is more loosely attached than the medial and can translate approximately 11mm with normal knee motion.10
The superior, middle and inferior geniculate arteries are the main vascular supply to the menisci. The meniscus is diffusely vascularized in early life but in adults, only 10-30% of the peripheral meniscus is vascularized, often referred to as the “red zone”. Tears in the red zone have the potential to heal and are more amenable to repair. Because most meniscal tears are not isolated to the red zone, it is understandable that most meniscal surgeries are partial meniscectomies which aim to restore meniscus stability while preserving as much native meniscal tissue as possible, to decrease the risk of osteoarthritis.
Partial meniscectomy
Indications for a partial meniscectomy include meniscal tears not amenable to repair which includes non-peripheral tears with a horizontal, oblique or complex tear pattern and nontraumatic tears in older patients. Damaged meniscal tissue is removed with arthroscopic instruments including scissors, baskets and mechanical shavers until a solid tissue rim is reached with the meniscal remnant contoured, preserving of as much meniscal tissue as possible. Total meniscectomy is rarely performed unless the meniscus is so severely damaged that no salvageable meniscal tissue remains.
Meniscal repair
Meniscus repair is superior to partial meniscectomy in preventing osteoarthritis and facilitating return to athletic activity.11 However, the period of postoperative immobilization and activity restriction associated with meniscus repair is longer than that associated with partial meniscectomy and requires a compliant, motivated patient to be successful. Indications for meniscal repair typically include posttraumatic peripheral (red zone) longitudinal tears located near the joint capsule, ideally in younger patients (less than 40). Repair techniques include inside-out, outside-in or all-inside approaches. Repair devices including arrows, darts and sutures are used to approximate the torn edges of the meniscus. Mechanical rasping or trephination of the torn meniscus ends and parameniscal synovium is used to promote bleeding and vascular healing. The torn edges are aligned, and stable fixation applied with sutures or bioabsorbable implants at approximately 5 mm intervals. Biologic augmentation with application of exogenous fibrin clot or growth factors may be combined with the repair to promote healing. Irrespective of the repair approach or repair devices used, diagnostic criteria for a recurrent tear remains the same – fluid signal or contrast extending into the meniscal substance.
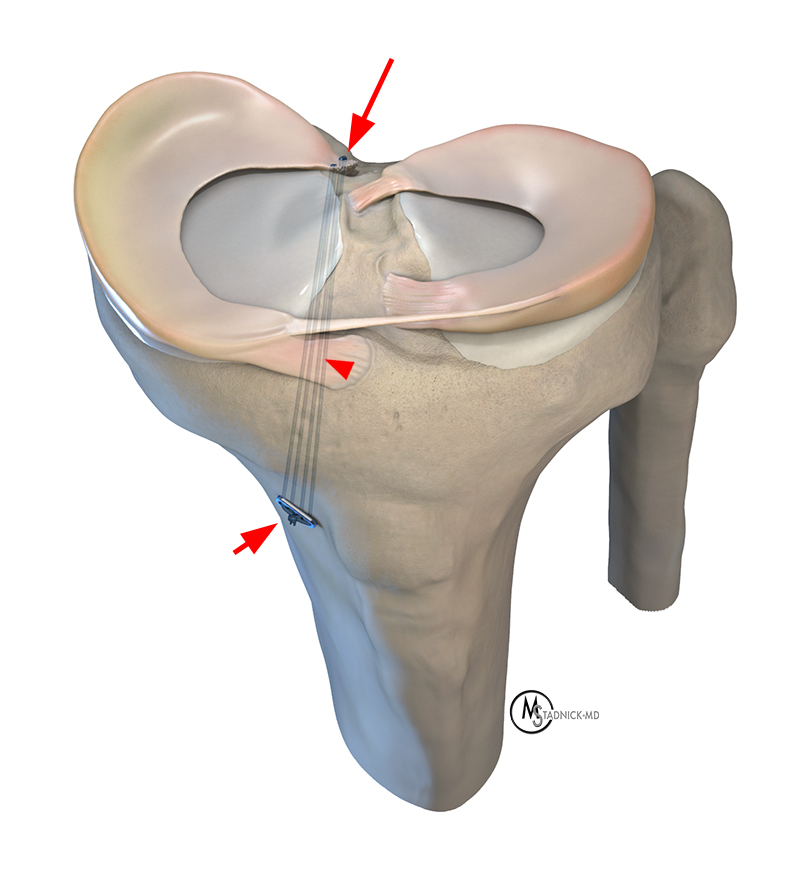
Repair of posterior root tears are being performed with increased frequency over the past several years. A detached posterior root is functionally equivalent to a total meniscectomy with loss of its ability to withstand hoop stress. Root tears are associated with a high risk for osteoarthritis. Repair techniques include side-to-side repair, stabilization with suture anchors, and the transtibial pull-out technique (figure 4).12
Figure 4:
Illustration of the transtibial pullout repair for a tear of the posterior horn medial meniscal root (arrow). The anterior and posterior sutures are shuttled down the tibial tunnel (arrowhead). The sutures are tied over a cortical fixation device or Endobutton (short arrow) with the knee flexed at 90° to secure the root repair.
Meniscal transplant
Meniscal transplant is usually reserved for patients younger than 50 years who have normal axial alignment. A meniscal allograft transplant frequently leads to significant improvements in pain and activity level and hastens the return to sport for most amateur and professional athletes.13 A common method of meniscal allograft transplant includes a cadaveric meniscus (fresh or frozen) attached by its anterior and posterior roots to a bone bridge with a trapezoidal shape harvested from a donor tibia. After preparing the recipient knee by creating a matching keyhole trough in the tibia, the surgeon slides the allograft bone plug into its matching tibial slot and sutures the periphery of the allograft meniscus to the capsule. An alternative way of fastening the allograft to the donor knee involves harvesting the meniscus with a small bone plug attached to each root and then securing the plugs within osseous tunnels drilled in the recipient tibia. Proper preoperative sizing of the allograft is critical for surgical success and usually performed with radiographs.
Postoperative imaging
The ideal technique for imaging the postoperative meniscus is a matter of active controversy and depends on the operation performed, surgeon preference and clinical question (concern for recurrent meniscal tear versus articular cartilage). Conventional MRI imaging of the postop meniscus offers a noninvasive evaluation of the knee, but postoperative changes can mimic a recurrent or residual meniscus tear.
Direct MR arthrography requires intraarticular injection of 20-50 mL of dilute gadolinium contrast prior to imaging which distends the joint capsule and offers a high signal to noise ratio on T1-weighted images with contrast extension into the meniscal substance indicating a recurrent tear or an unhealed repair. Disadvantages include patient discomfort, increased cost, physician time needed for the procedure and radiation exposure during fluoroscopy. In the U.S., intraarticular injection of gadolinium-based contrast is off label. And, some tears do not fill with contrast during arthrography. A previous study by De Smet et al. has shown that 41% of patients with a surgically confirmed torn post-operative meniscus had signal intensity within the meniscus extending into the articular surface which was lower than the signal intensity of gadolinium contrast.14 Like the presence of a line of intermediate T2 signal extending into the articular surface on conventional MRI, diagnosis of a torn post-operative meniscus on MRI arthrography is challenging when the intra-meniscal signal intensity is not as bright as gadolinium contrast. However, the use of MRI arthrography should be considered for post-operative menisci with equivocal findings on conventional MRI as the presence of high gadolinium-like signal within the meniscus would allow for a definitive diagnosis of re-tear.
Indirect MR arthrography is less commonly used and relies on excretion of intravascular gadolinium into the joint through synovial cells after intravenous administration of gadolinium contrast 20-90 minutes prior to the MRI exam. Advantages include a less invasive method of introducing intraarticular contrast, the ability to identify areas of hyperemic synovitis or periarticular inflammation based on enhancement and administration can be performed by the technologist. Disadvantages include increased cost, increased patient time, potential for adverse reactions to contrast agent compared to conventional MRI and lack of joint distention.
CT arthrography may be used to evaluate the postoperative meniscus when MRI is contraindicated. Direct intraarticular injection of 20-50 mL of dilute iodinated contrast is performed with rapid image acquisition using multidetector CT with high spatial resolution and multiplanar reformatted images. Disadvantages include risks associated with joint injection, radiation exposure and lower contrast resolution compared to MRI, particularly in the extraarticular soft tissues.
Regardless of the imaging protocol chosen for evaluation of the postoperative meniscus, optimal imaging interpretation includes:
- Accurate patient history including site and duration of symptoms
- Prior MRI studies for comparison
- Operative report
MRI Imaging Findings
The normal MRI appearance after partial meniscectomy is volume loss and morphologic change, commonly truncation or blunting of the meniscal free edge. Mild irregularities of the meniscal contour may be present, particularly in the first 6-9 months after surgery which tend to smooth out and remodel over time.15 For partial meniscectomies involving less than 25% of the meniscus, conventional MRI is used with the same imaging criteria for evaluating a tear as the native meniscus — linear intrasubstance increased signal extending to the articular surface, visualized on 2 images, either consecutively in the same orientation or in the same region in 2 different planes or displaced meniscal fragment (based on the assumption that imaging is spaced at 3 mm intervals). Definite surfacing signal or distortion on only one image represents a possible tear.
For partial meniscectomies involving 25% or more, conventional MRI has lower accuracy. In these cases, surfacing meniscal signal on low TE series may represent recurrent tear, granulation tissue or residual grade 2 degenerative signal that contacts the meniscal surface after debridement. Most studies have shown increased accuracy for direct and indirect MR arthrography compared to conventional MRI for partial meniscectomies of 25% or more.16
However, many clinicians opt to use conventional MRI as the initial postoperative imaging study and reserve MR arthrography for equivocal cases. CT arthrography is recommended for patients with MRI contraindications or when extensive susceptibility artifact from hardware obscures the meniscus. Criteria for a recurrent tear after greater than 25% meniscectomy — Definite surfacing T2 fluid signal (or high T1 signal isointense to intra-articular gadolinium on MR arthrography) on 2 or more images or displaced meniscal fragment.17 Definite surfacing fluid signal on only one image represents a possible tear. Kijowski et al. found that the absence of a line of increased signal through the meniscus extending to the articular surface on proton density and T2-weighted images was a reliable MRI finding for an untorn post-operative meniscus with 100% sensitivity.
Kijowski et al. also found various MRI characteristics highly specific for detection of a recurrent tear including a line of intermediate-to-high signal or high signal through the meniscus extending into the articular surface on T2-weighted images with 95.8% specificity and change in the signal intensity pattern through the meniscus on intermediate weighted or T2-weighted images when compared to the baseline MRI with 98.2% specificity. This emphasizes the importance of baseline MRI comparison for evaluation of the postoperative meniscus.3
Figure 5:
Sagittal proton density-weighted image (5A) through the medial meniscus at age 12 shows the initial horizontal tear in the posterior horn (arrow) subsequently treated with partial meniscectomy. Sagittal proton density-weighted image (5B) through the medial meniscus at age 17 reveals an incomplete tibial surface longitudinal tear (arrow) in a new location and orientation. Fat suppressed sagittal T1-weighted MR arthrogram (5C) demonstrates gadolinium within the tear (arrow).
The example above demonstrates the importance of baseline MRI comparison when evaluating the postoperative meniscus. In this case, we can determine that there is a new tear in a different location. Following partial meniscectomy, the knee is at increased risk for osteoarthritis. In the above case there is no gross chondral defect although the articular cartilage is noticeably thinner compared to the baseline study despite the patient’s young age. Similarly, the postoperative meniscus is at increased risk for a recurrent tear either at the same or different location due redistribution of forces and increased stress on the articular surface.
Figure 6:
Sagittal proton density-weighted image (6A) through the medial meniscus following partial meniscectomy and debridement of the inferior articular surface shows increased PD signal contacting the inferior articular surface (arrow) but no T2 fluid signal at the surgical site (6B) and no gadolinium signal in the meniscus (6C). Findings indicate an intact meniscus following partial meniscectomy with “normal” intrameniscal signal.
Figure 7:
History of medial meniscus posterior horn partial meniscectomy. Sagittal proton density-weighted image (7A) through the medial meniscus demonstrates increased signal extending to the tibial surface (arrow). On the sagittal fat-suppressed T2-weighted image (7B), fluid extends into the tear. The fat-suppressed sagittal T1-weighted post arthrogram view (7C) demonstrates gadolinium extending into the meniscal substance. A recurrent tear was proved at second look arthroscopy.
Figure 8:
History of medial meniscus posterior horn and body partial meniscectomy. Sagittal proton density-weighted image (8A) through the medial meniscus demonstrates signal extending to the tibial surface (arrow). Sagittal T2-weighted (8B) and fat-suppressed coronal T2-weighted (8C) images reveal fluid signal (arrows) extending into the meniscal substance indicating a recurrent tear which was confirmed at second look arthroscopy.
Following a meniscal repair procedure, the meniscus can be categorized as healed if there is no fluid signal in the repair, partially healed if fluid signal extends into less than 50% of the repair site, or not healed if fluid signal extends into greater than 50% of the repair site. Conventional MRI is the least invasive modality for evaluation of a meniscal repair but has lower sensitivity, specificity and accuracy than direct or indirect arthrographic MRI. Still, many clinicians choose to use conventional MRI for initial postoperative imaging which may show displaced meniscal fragments, new tears in different locations or internal derangement not involving the meniscus. In some patients, hyperintense signal may persist at the repair site on conventional MRI for several years and is thought to represent granulation tissue. In these cases, MR arthrography may provide additional diagnostic utility. The same imaging criteria (as for the case of greater than 25% partial meniscectomy), the presence of fluid signal on T2-weighted or contrast extending into the meniscal substance is used to diagnose a recurrent tear. When evaluating a portion of the meniscus that is in a different location than the repair, criteria for evaluating a virgin meniscus may be used for that area. Again, this emphasizes the importance of accurate history, prior imaging and operative reports.
Figure 9:
History of longitudinal medial meniscus tear managed by meniscal repair (arrows). Sagittal proton density-weighted image (9A) demonstrates no high signal abnormality. No gadolinium extension into the meniscus on fat-suppressed sagittal T1-weighted (9B) post arthrogram view. The meniscal repair is intact.
Figure 10:
Longitudinal lateral meniscus tear status post repair (arrow). Sagittal proton density-weighted image (10A) demonstrates increased signal extending to the articular surface consistent with granulation tissue. Sagittal T2-weighted image (10B) reveals no fluid at the repair site. An intact meniscal repair was confirmed at second look arthroscopy.
Figure 11:
Longitudinal medial meniscus tear managed by repair (arrow). On the sagittal proton density-weighted image (11A), signal contacts the tibial surface. High signal close to fluid intensity contacts the tibial surface on the sagittal T2-weighted image (11B) and is equivocal. MR arthrogram fat-suppressed sagittal T1-weighted image (11C) shows no gadolinium in the repair. An intact meniscal repair was confirmed at second look arthroscopy. Sometimes T2 signal in a healed tear may look similar to fluid. In cases like this, MR arthrography is quite helpful.
Figure 12:
Lateral meniscus posterior horn peripheral longitudinal tear managed by repair. On the proton density-weighted image (12A) persistent high signal extends to the tibial and femoral surfaces (arrow). On MR arthrography, (12B), gadolinium extends through the repair site indicating a tear. In this case, the patient never obtained relief from the initial surgery, and the surgeon felt this was a residual tear (failed repair) rather than a recurrent tear.
Figure 13:
Medial meniscus posterior horn peripheral longitudinal tear treated with repair. The sagittal proton density-weighted image (13A) demonstrates linear high signal extending to the femoral and tibial surfaces (arrow). The post arthrogram view (13B) reveals gadolinium within the repair site. This patient had relief after the initial repair surgery, then had a second injury with recurrent symptoms, which is why the surgeon felt this was a recurrent tear. A tear was found and the repair was revised at second look arthroscopy. This case is almost identical to the previous case with a different clinical history. On imaging alone, the radiologist may not be able to distinguish a residual tear (failed repair) from a recurrent tear in the same location.
Figure 14:
History of a longitudinal medial meniscus tear managed by repair and concurrent ACL reconstruction. Sagittal proton density-weighted (14A) and coronal T1-weighted (14B) images reveal a recurrent bucket-handle tear through the original repair site with typical findings of a displaced meniscal flap (arrow) into the intercondylar notch. The tear was treated by partial meniscectomy at second surgery.
Figure 15:
Medial meniscus posterior horn peripheral longitudinal tear (arrow) seen on the sagittal proton density-weighted image (15A) and managed by repair. 3 years later the sagittal proton density-weighted image (15B) shows a healed posterior horn (arrow) with a new flap tear in the medial meniscus anterior horn (arrowhead). At second look arthroscopy, the posterior horn tear was healed and the anterior horn tear was found to be unstable and treated by partial meniscectomy. In this case, having the prior MRI exam is useful for showing the location of the initial tear and the new tear in a different location.
Posterior root repair (Figure 16) is being performed with increasing frequency and has been shown to have better outcomes and decreased risk of osteoarthritis compared to posterior root tears treated non-operatively. Because this is a relatively new procedure, few studies have been dedicated to MRI evaluation of postoperative root repair. Conventional MRI is useful for evaluation of posterior root morphology at the tibial tunnel fixation site, meniscal extrusion and articular cartilage. Extrusion is commonly seen following root repair. Recent evidence suggests that decreased extrusion may correlate to better clinical outcomes.18
Figure 16:
22 year-old male with a history of ACL and MCL reconstruction and medial meniscus posterior root repair. Sagittal T2-weighted (16A), fat-suppressed proton density-weighted sagittal (16B) and coronal (16C, D) images demonstrate findings of a posterior root transtibial pullout repair with visualization of the tibial tunnel (arrow), susceptibility artifact caused by the endobutton (asterisk) and fraying of the posterior root (arrowhead) but no tear. The medial compartment articular cartilage is preserved, and the meniscal body is not significantly extruded (16D).
Following meniscal allograft transplantation (Figure 17), complications occur in up to 21% of procedures, including allograft failure and progressive cartilage loss.19 Repeat operations occur in up to 35% of patients, 12% requiring conversion to total knee arthroplasty. Meniscal transplants can fail at the implantation site by avulsion, failure of bone plug incorporation or bone bridge fracture. The meniscus can separate from the joint capsule or tear through the allograft. Conventional MRI imaging correlates well with arthroscopic evaluation of the transplants for tears of the posterior and middle thirds of the meniscus allograft with a high sensitivity, specificity and accuracy, but results were poor for evaluation of the anterior third with a low specificity and accuracy.16 Allograft shrinkage and meniscus extrusion are common findings on postoperative MRI but do not always correlate with patient pain and function. Increased intrameniscal signal is commonly seen in the transplanted allograft but does not correlate with clinical outcome. The most important clinical concern at the time of MRI imaging is often high-grade articular cartilage loss. Arthrofibrosis and synovitis are also relatively common.
Figure 17:
15 year old patient with prior extensive lateral partial meniscectomy was treated with lateral chondroplasty and lateral meniscal allograft transplant with continued pain and clicking 6 weeks post-operative. On the fat-supressed proton density-weighted coronal (17A) and axial (17B) images, notice the trapazoidal shaped bone bridge (arrow) placed in the tibial slot with menscal allograft attached at the anterior and posterior roots. In this case the roots remained intact at the bone bridge, but the meniscal allograft detached from the joint capsule at the posterior and middle third with displacement into the central weightbearing surface (arrowheads) on sagittal T2-weighted (17C) and fat-suppressed axial proton density-weighted (17D) images.
Complications following meniscus surgery
MR imaging is useful for evaluation of many possible complications following meniscal surgery. The self-reported complication rate for partial meniscectomy is 2.8% and meniscus repair is 7.6%. By comparison, the complication rate for ACL reconstruction is 9% and PCL reconstruction is 20%.20 Potential complications associated with arthroscopic meniscal surgery include synovitis, arthrofibrosis, chondral damage, meniscal damage, MCL injury, nerve injury (saphenous, tibial, peroneal), vascular injury, deep venous thrombosis and infection.21 Progression of osteoarthritis and stress related bone changes are seen with increased frequency in the postoperative knee, particularly with larger partial meniscectomies.
Figure 18:
36 year old male with history of meniscus surgery 7 years ago. Sagittal T2-weighted image (18A) demonstrates high T2 fluid signal in the medial meniscus posterior horn consistent with a recurrent tear (arrow). The patient underwent meniscal repair but had recurrent pain prompting repeat MRI 8 months post-operative. Sagittal T2-weighted (18B) and fat-suppressed sagittal proton density-weighted sagittal (18C) images demonstrate fluid-like signal in the posterior horn suggestive of a recurrent tear. Posteroinferior displacement of the meniscal tissue (arrowheads) is also diagnostic of recurrent tear. Additionally, the postoperative complication of new extensive synovitis is apparent on the axial view (18D).
Figure 19:
70 year-old female with history of medial meniscus posterior horn radial tear. Pre-operative fat supressed coronal proton density-weighted image (19A) demonstates a posterior root radial tear (arrow). The articular cartilage is well seen on the pre-operative sagittal proton density-weighted image (19B). 6 months post-operative she had increased pain prompting follow-up MRI. Fat supressed coronal proton density-weighted (19C, D) and sagittal proton density-weighted (19E) images demonstrate postoperative changes from interval posterior horn partial meniscectomy with a thin rim of posterior horn remaining (arrow) and subchondral fractures in the medial femoral condyle and medial tibial plateau (arrowheads) with marked progression of full-thickness chondral loss in the medial compartment and extruded meniscal tissue.
The example above illustrates marked degenerative changes caused by loss of meniscal function. Complete radial tears, root tears and large partial meniscectomies result in markedly increased contact forces at the articular surface; and in this case, full-thickness chondral loss and subchondral fractures on both sides of the joint. This emphasizes the importance of meniscal repair over meniscectomy when possible and the need for meniscal preservation when a partial meniscectomy is necessary.
Conclusion
Meniscal surgery is common and requires accurate post-operative imaging interpretation to guide the treatment approach. Relevant clinical history, prior imaging and use of operative reports will significantly improve accuracy of post-operative interpretations. Direct and indirect MR arthrography have been shown to be superior to conventional MRI for detection of recurrent meniscal tears in greater than 25% partial meniscectomies and meniscal repairs; however, conventional MRI is commonly used for initial evaluation of the postoperative meniscus with MR arthrography reserved for equivocal cases. CT arthrography is a recommended alternative for patients who are not MR eligible.
Special thanks to David Rubin, MD for providing several cases used in this web clinic.
References
- Garrett WE Jr, Swiontkowski MF, Weinstein JN, et al. American Board of Orthopaedic Surgery Practice of the Orthopaedic Surgeon: Part-II, certification examination case mix. The Journal of bone and joint surgery American volume. 2006; 88:660–667 ↩
- Boutin RD, Fritz RC, Marder RA. Magnetic resonance imaging of the postoperative meniscus: resection, repair, and replacement. Magn Reson Imaging Clin N Am 2014;22(4): 517–555 ↩
- Kijowski, R., Rosas, H., Williams, A. et al.MRI characteristics of torn and untorn post-operative menisci. Skeletal Radiol 46, 1353–1360 (2017). ↩
- White LM, Schweitzer ME, Weishaupt D, Kramer J, Davis A, Marks PH. Diagnosis of recurrent meniscal tears: prospective evaluation of conventional MR imaging, indirect MR arthrography, and direct MR arthrography. Radiology. 2002; 222:421–429 ↩
- Ciliz D, Ciliz A, Elverici E, Sakman B, Yuksel E, Akbulut O. Evaluation of postoperative menisci with MR arthrography and routine conventional MRI. Clinical imaging. 2008; 32:212–219 ↩
- Magee T. Accuracy of 3-Tesla MR and MR arthrography in diagnosis of meniscal retear in the post-operative knee. Skeletal radiology. 2014; 43:1057–1064 ↩
- McCauley TR. MR imaging evaluation of the postoperative knee. Radiology. 2005; 234:53–61 ↩
- Baratz ME, Fu FH, Mengato R. Meniscal tears: the effect of meniscectomy and of repair on intraarticular contact areas and stress in the human knee. A preliminary report. Am J Sports Med 1986; 14 (04) 270-275 ↩
- Cho JM, Suh JS, Na JB, et al. Variations in meniscofemoral ligaments at anatomical study and MR imaging. Skeletal Radiol. 1999;28(4):189-195 ↩
- Thompson WO, Thaete FL, Fu FH, Dye SF. Tibial meniscal dynamics using three-dimensional reconstruction of magnetic resonance images. Am J Sports Med. 1991;19(3):210-216 ↩
- Stein T, Mehling AP, Welsch F, von EisenhartRothe R, Jäger A. Long-term outcome after arthroscopic meniscal repair versus arthroscopic partial meniscectomy for traumatic meniscal tears. Am J Sports Med 2010; 38:1542–1548 ↩
- LaPrade RF, Matheny LM, Moulton SG, James EW, Dean CS. Posterior meniscal root repairs: outcomes of an anatomic transtibial pull-out technique. Am J Sports Med 2017; 45:884–891 ↩
- Zaffagnini S, Grassi A, Marcheggiani Muccioli GM, et al. Is sport activity possible after arthroscopic meniscal allograft transplantation? Midterm results in active patients. Am J Sports Med 2016; 44:625–632 ↩
- De Smet AA, Horak DM, Davis KW, Choi JJ. Intensity of signal contacting meniscal surface in recurrent tears on MR arthrography compared with that of contrast material. AJR American journal of roentgenology. 2006; 187:W565–568. (PubMed: 17114506) ↩
- Newman AP, Daniels AU, Burks RT. Principles and decision making in meniscal surgery. Arthroscopy 1993; 9 (01) 33-51 ↩
- Baker JC, Friedman MV, Rubin DA (2018) Imaging the postoperative knee meniscus: an evidence-based review. AJR Am J Roentgenol 211(3):519–527 ↩
- De Smet AA. MR imaging and MR arthrography for diagnosis of recurrent tears in the postoperative meniscus. Semin Musculoskelet Radiol 2005;9(2):116–24 ↩
- Chung KS, Ha JK, Ra HJ, Nam GW, Kim JG. Pullout fixation of posterior medial meniscus root tears: correlation between meniscus extrusion and midterm clinical results. Am J Sports Med 2017; 45:42–49 ↩
- ElAttar M, Dhollander A, Verdonk R, Almqvist KF, Verdonk P. Twenty six years of meniscal allograft transplantation: is it still experimental? A meta-analysis of 44 trials. Knee Surg Sports Traumatol Arthrosc 2011; 19:147–157 ↩
- Gwathmey F.W., Golish S.R., Diduch D.R., et al: Complications in brief: meniscus repair. Clin Orthop Relat Res 2012; 470: pp. 2059-2066 ↩
- Kinsella S.D., and Carey J.L.: Complications in brief: arthroscopic partial meniscectomy. Clin Orthop Relat Res 2013; 471: pp. 1427-143 ↩