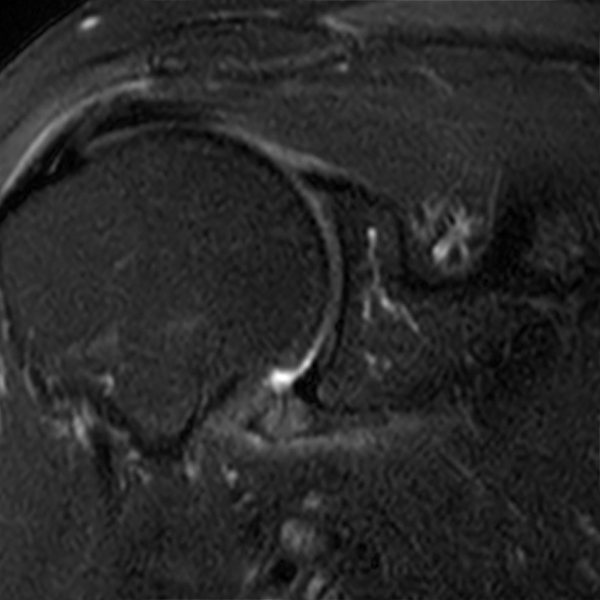
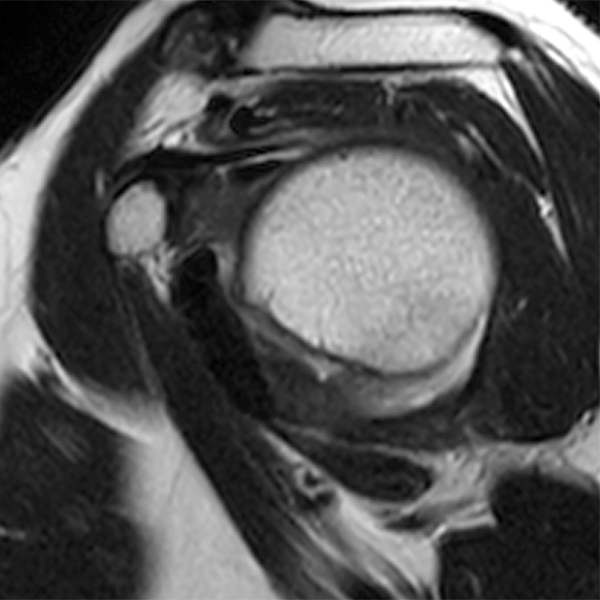
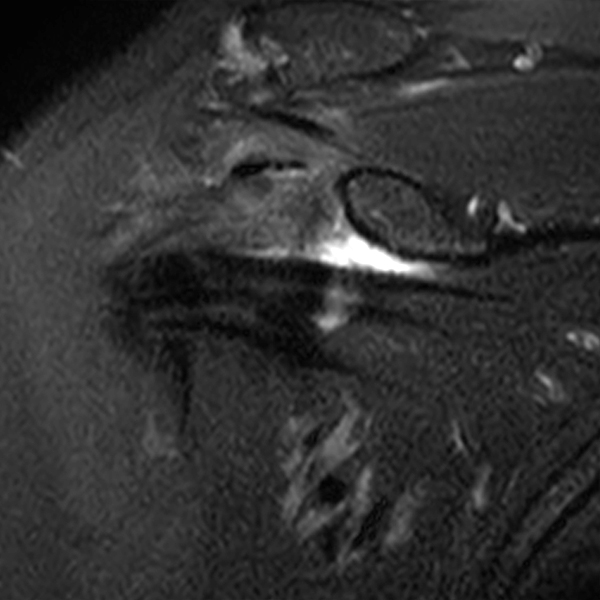
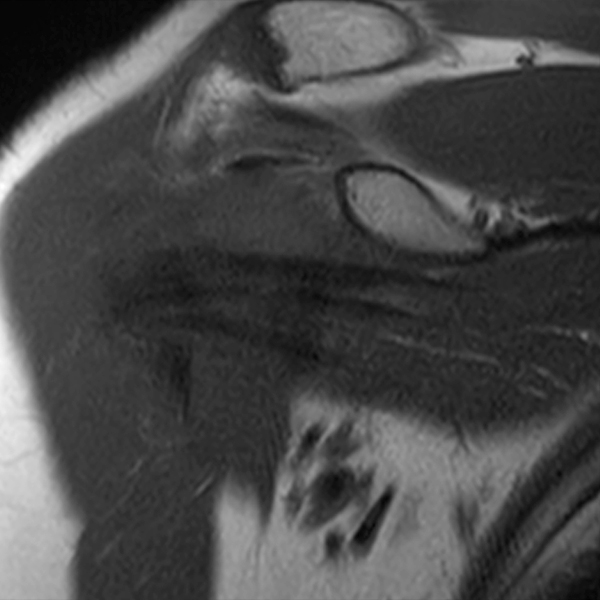
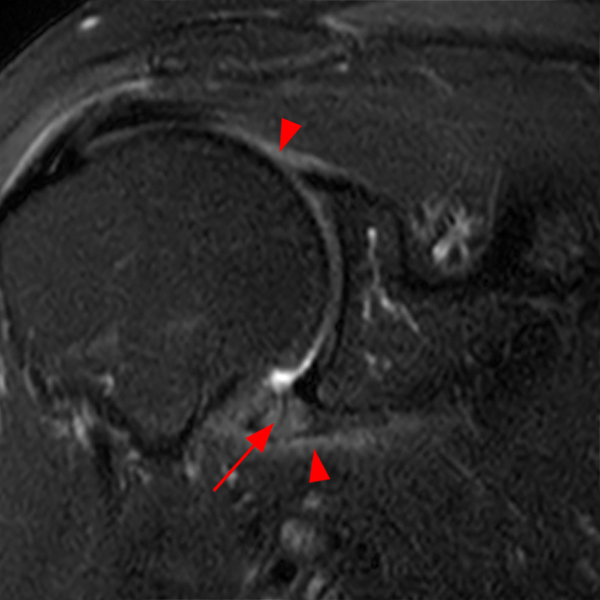
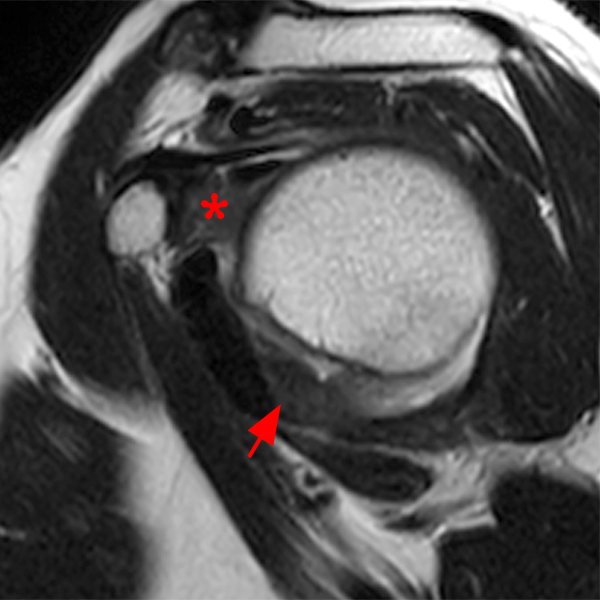
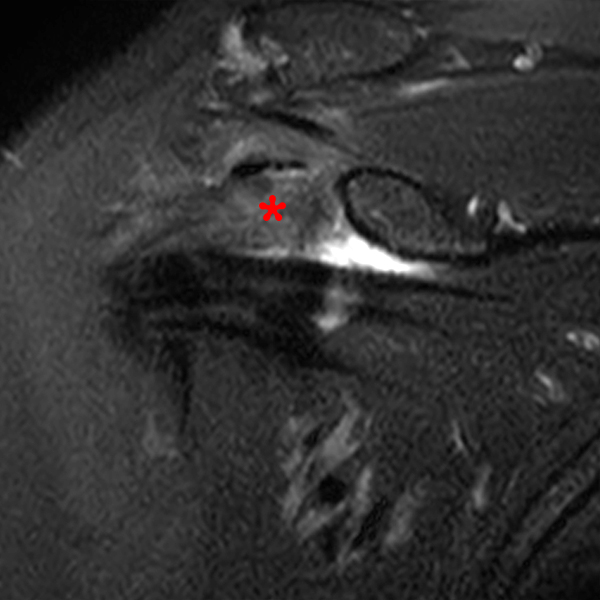
Clinical History: A 48 year-old female presents with right shoulder stiffness and pain for 3 months with no known injury and no relief with ice, rest, and NSAIDs. Coronal fat-suppressed T2-weighted (1A and 1C), sagittal T2-weighted (1B), and coronal T1-weighted (1D) images are provided. What are the findings? What is the diagnosis?
Findings
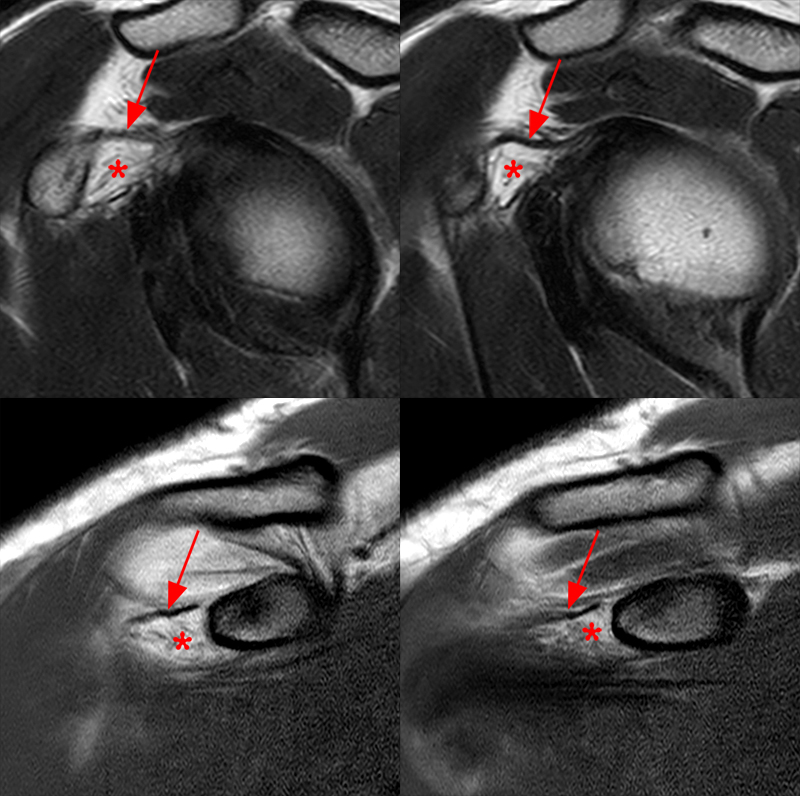
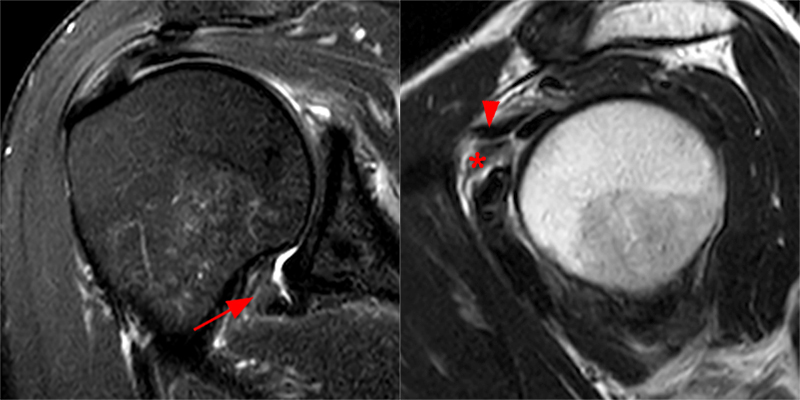
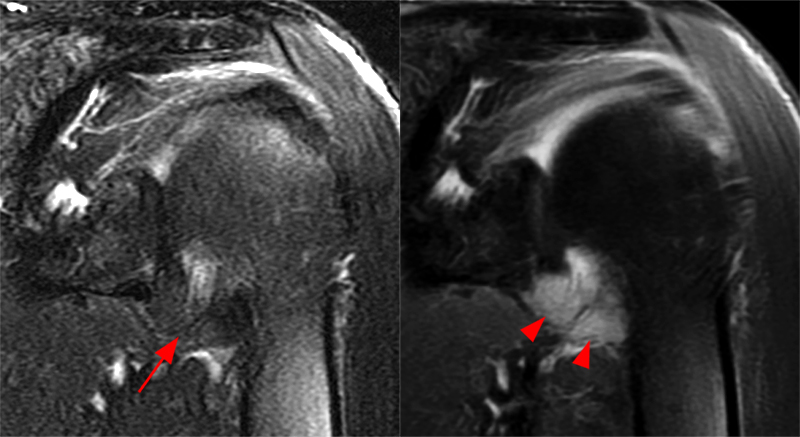
Figure 2:
The coronal fat-suppressed T2-weighted image through the mid-glenoid (2A) demonstrates a thickened and edematous inferior glenohumeral ligament at the axillary pouch (arrow). Pericapsular edema is demonstrated inferior to the axillary pouch and at the superior aspect of the glenohumeral joint (arrowheads). The sagittal T2-weighted image (2B) shows replacement of the subcoracoid fat by intermediate signal soft tissue thickening (asterisk), with synovial and capsular thickening at the anterior inferior aspect of the glenohumeral joint (short arrow). The coronal fat-suppressed T2-weighted (2C) and T1-weighted (2D) images through the rotator interval region demonstrate replacement of the subcoracoid fat (asterisk)(2C) with superimposed edema (asterisk)(2D).
Diagnosis
Primary adhesive capsulitis of the shoulder.
Introduction
Adhesive capsulitis of the shoulder (frozen shoulder) is a common cause of pain and limitation of motion with an incompletely understood and complex pathogenesis. The diagnosis is commonly made through a combination of clinical history and physical examination findings, but early signs of adhesive capsulitis can be nonspecific and overlap with other causes of shoulder stiffness.1,2 Recognizing the characteristic MRI findings of adhesive capsulitis enables the radiologist to make an earlier diagnosis of adhesive capsulitis in clinically confusing cases.
Epidemiology
Adhesive capsulitis occurs in 2-5% of the general population and most commonly affects patients in the 5th to 7th decade, with an estimated 70% of cases occurring in women.3,4 The non-dominant shoulder is affected in approximately 70% of cases and 20-30% will also develop adhesive capsulitis in the opposite shoulder.3,5 There is a strong association between adhesive capsulitis and diabetes mellitus. The incidence of adhesive capsulitis in diabetics is five times that of the general population, and 30% of patients with adhesive capsulitis have diabetes.6 Additional associated risk factors include thyroid disease, rheumatological diseases, hypoadrenalism, dyslipidemia, hypercholesterolemia, Parkinson’s disease, cardiopulmonary disease, and cerebrovascular disease.7,8,9,10,11,4,12 Dupuytren contracture is also associated with adhesive capsulitis and appears to share a similar underlying pathophysiology.13,4
Clinical Presentation
Several classification schemes for adhesive capsulitis are utilized.14,15,5 Adhesive capsulitis is most often categorized as primary or secondary.16,17 Primary adhesive capsulitis occurs without any specific trauma and in the absence of other shoulder lesions.14,2 Some authors include adhesive capsulitis in association with diabetes mellitus and other comorbidities within this category.5,16,17 Secondary adhesive capsulitis is related to articular or periarticular trauma, surgery, rotator cuff tear, or underlying arthritis.14,5,17
The typical presentation of primary adhesive capsulitis is slowly progressing shoulder pain followed by limitations in active and passive range of motion with normal radiographs of the shoulder, except for osteopenia. Restricted external rotation is the most common limitation in range of motion, and limited forward flexion is also commonly seen. Eventually, a global reduction in the range of motion can develop. Four clinical stages of adhesive capsulitis have been described, reflecting a continuum of the clinical and arthroscopic findings18
Stage 1 (Pre-freezing): The patient typically presents with symptoms for less than 3 months. Gradual onset of pain is typically referred to the deltoid insertion. Achy pain at rest becomes more intense and sharper with active and passive motion. Motion can be normal or nearly normal and is restored by intra-articular anesthetic. Arthroscopic and histologic examination reveals a hypertrophic fibrinous and hypervascular synovitis with a normal underlying capsule.2
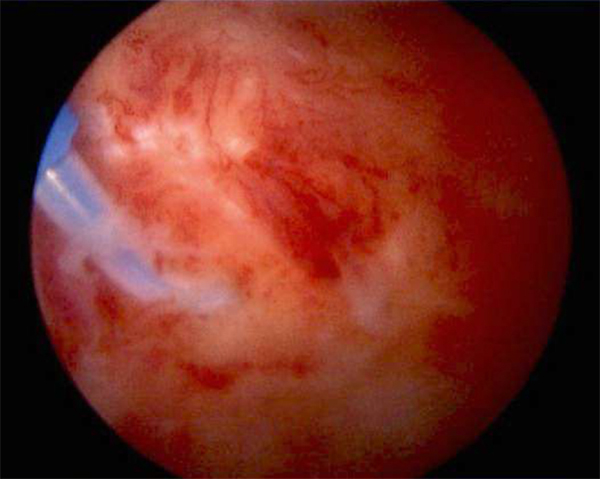
Stage 2 (Freezing): Patients report symptoms lasting approximately 3 to 9 months. Clinically, there is chronic pain with active and passive motion and significant limitations in forward flexion, abduction, internal rotation, and external rotation. Pain often becomes more severe at night. Arthroscopic inspection and pathologic examination demonstrate both a considerable inflammatory component and fibrosis with hypertrophic, hypervascular glenohumeral synovitis, perivascular scar, and significant capsular thickening with early loss of the axillary pouch (Figure 3).2 Range of motion is improved but not completely normal following intra-articular anesthetic.
Stage 3 (Frozen): Patients usually present after symptoms lasting 9 to 15 months. Minimal pain is typical except at the end ranges of motion. There is significant loss of motion with a solid endpoint or block at the end of motion. No improvement in motion is seen with intra-articular anesthetic. Arthroscopic and histologic evaluations demonstrate atrophic synovitis and dense capsular scar with loss of the axillary recess.
Stage 4 (Thawing): The patient experiences minimal pain and gradual improvement in motion may ensue.2,19 Arthroscopically, mature scar is present and can distort and obscure intra-articular structures.18
Pathophysiology
Multiple pathways appear to be causative in adhesive capsulitis.20 However, the exact mechanism is unknown with both inflammatory and fibroproliferative mediators appearing to play a role.21 Histologically, synovial cells and fibroblasts are the dominant cell populations, and there is new collagen deposition.22 Initially, a diffuse inflammatory response is triggered within the synovium with inflammatory cell infiltration, leading to synovial proliferation. This is followed by an increase in fibroblasts and dense collagenous tissue deposition within the capsule. Edema and thickening of the capsule and synovium results in contraction of the joint space.
Anatomy
The pathologic changes of adhesive capsulitis can affect the capsule diffusely, but the rotator interval, coracohumeral ligament, axillary joint capsule, and the inferior glenohumeral ligament have been most closely investigated because involvement in these locations is believed to be most closely associated with the early clinical findings of pain and limitation in motion.23,24,23,25,19,26
The changes that occur in the rotator interval capsule and coracohumeral ligament (CHL) are best visualized on sagittal T1-weighted or T2-weighted fast spin-echo (FSE) images. The coronal and axial views can also be helpful. The coracohumeral ligament is identified as a curvilinear low-signal structure that extends laterally from the coracoid process and is surrounded by fat in the rotator interval. The subcoracoid fat triangle is a normal region of fat bounded by the coracoid process, joint capsule and the coracohumeral ligament (Figure 4).
The axillary capsule is formed by the inferior glenohumeral ligament and is best visualized on coronal images at the mid-glenoid level. T2-weighted images provide the best depiction of thickness as T1-weighted images tend to overestimate capsular thickness (Figure 5). Cross-referencing coronal views with sagittal views through the axillary recess is recommended to confirm true capsular thickening. An artifactually thickened appearance can occur through volume averaging, which results when the coronal slices extend obliquely through a normal collapsed axillary capsule.
MRI Findings
Adhesive capsulitis is a clinical diagnosis, but the physical exam findings can be confusing, especially in the early stages or with concomitant shoulder pathologies such as rotator cuff impingement, bursitis, and labral pathology which may present with overlapping clinical features.23,5,26 With its widespread availability, multiplanar capability, anatomic detail, and soft tissue differentiation, MRI is the favored imaging modality for the evaluation of shoulder pathology. The findings associated with adhesive capsulitis are depicted by routine MRI, MRI with intravenous contrast, and MR arthrography. In our practice, identification and evaluation of adhesive capsulitis is most often by routine MRI, followed by intravenous contrast-enhanced MRI. MR arthrography appears to improve diagnostic accuracy but it is unlikely to be necessary to confirm the diagnosis when clinical history and less invasive imaging procedures are considered.20
Multiple MRI findings are associated with the clinical features of adhesive capsulitis. These changes often affect the joint diffusely, but they are most widely identified as coracohumeral ligament thickening, obliteration of fat in the rotator interval, enhancement of the rotator interval, inferior glenohumeral ligament thickening, inferior glenohumeral ligament edema, and axillary joint capsule enhancement.24,27,23,25 For most patients the MRI findings of adhesive capsulitis present as a constellation of multiple findings.
Coracohumeral ligament thickening demonstrates the highest specificity for adhesive capsulitis, but was found to be lowest in sensitivity in a meta-analysis study by Suh.25 Proposed cutoff values for abnormal thickening of the CHL range from 2-4 mm with a value of > 4 mm used most commonly.25,24,28,1 The CHL is best visualized on sagittal oblique studies utilizing T1- or T2-weighted images without fat suppression (Figure 6).
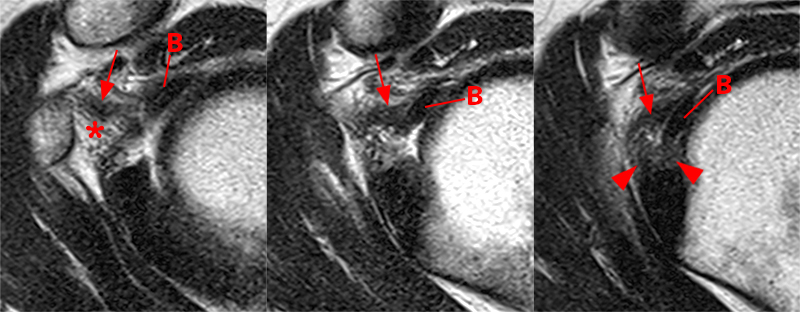
Figure 6:
54 year-old female with 5 months of shoulder pain and no known injury. Medial to lateral (left to right) sequential T2-weighted images demonstrate thickening of the coracohumeral ligament (arrows), which measures up to 5 mm in thickness, mild subjacent infiltration of the subcoracoid fat (asterisk), and soft tissue thickening and synovitis (arrowheads) adjacent to the long head of the biceps tendon (B).
Synovitis and fibrosis replacing fat in the rotator interval commonly accompanies CHL thickening. Replacement of fat in the subcoracoid fat triangle has been dubbed the subcoracoid triangle sign and is best seen on sagittal T2-weighted FSE images (Figure 7).24 This finding is more commonly seen in patients with early stage adhesive capsulitis (stage 1 or 2).25,29,19 Several authors have reported that fatty infiltration of the rotator interval has no association with clinical impairment.26,28
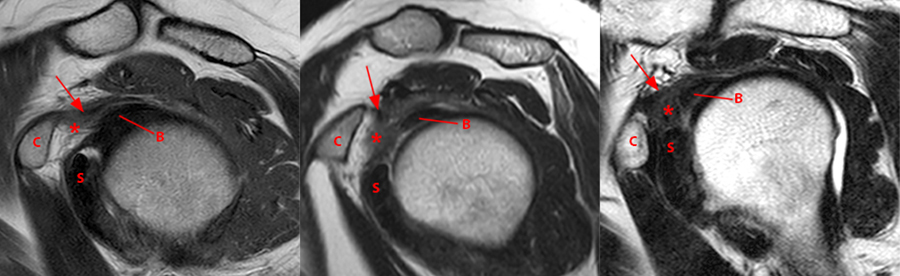
Figure 7:
Sagittal T2-weighted images in 3 patients demonstrate mild(left), moderate (middle), and severe (right) infiltration and replacement of fat in the subcoracoid fat triangle(asterisks). The coracohumeral ligament (arrows) borders the subcoracoid fat triangle superiorly and often appears to blend with the fat pad changes. The coracoid process (C), subscapularis muscle (S), and the long head of the biceps tendon (B) are also indicated.
A wide range of values have been used to determine abnormal thickening of the synovium and inferior glenohumeral ligament at the axillary capsule. For routine MRI without joint distension a value of > 4mm is most commonly used.28,30,31 With MR arthrography an axillary pouch thickness of >3 mm has been shown to result in improved accuracy.32 Coronal T2-weighted images provide the most accurate measure of capsule thickness.
Axillary capsular thickening most often occurs in conjunction with T2 hyperintensity of the capsule, which represents underlying hyperemia and edema. T2 hyperintensity of the axillary capsule carries a sensitivity of 88% and specificity of 81% for adhesive capsulitis.25 This finding is most often observed in the early stages of adhesive capsulitis (stage 1 or 2) and is felt to reflect the early synovial inflammatory process that precedes reactive capsular fibrosis.29,19,33 Capsular edema can range from focal to diffuse, and involvement near the humeral insertion appears to be most closely correlated with limitations in the range of motion(Figure 8).29 Often, a more diffuse pattern of synovial and capsular involvement can be observed, as well as periarticular edema external to the capsule (Figure 9).
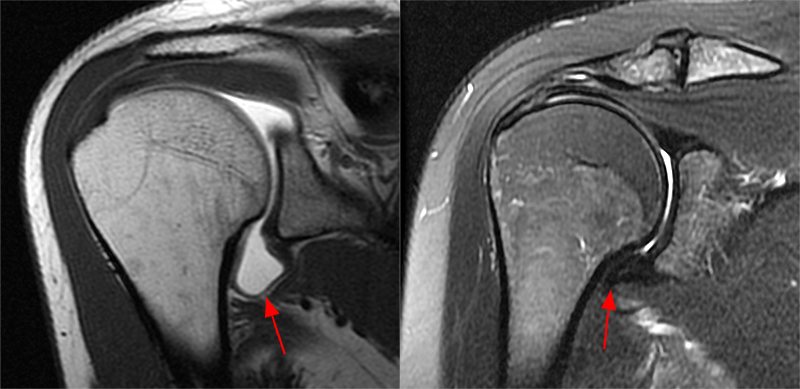
Figure 8:
A coronal fat-suppressed T2-weighted image (left) of the right shoulder in a 47 year-old female complaining of worsening shoulder pain at night for approximately 3 months demonstrates mild focal edema and thickening of the axillary capsule (arrow). Additional MR features of adhesive capsulitis were identified including a thickened coracohumeral ligament (arrowhead) and infiltration of the subcoracoid fat (asterisk), seen on the sagittal T2-weighted image (right).
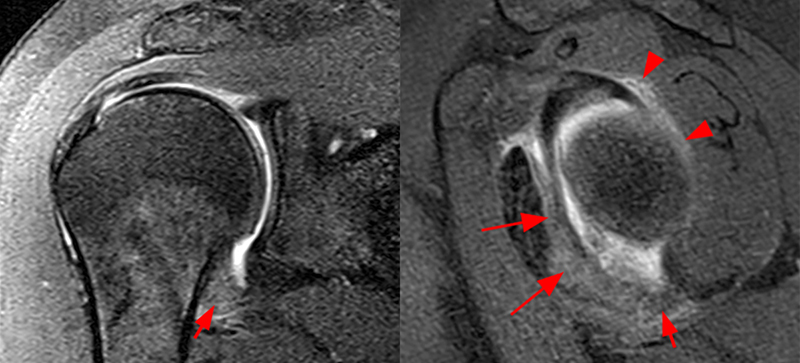
Figure 9:
Coronal (left) and sagittal (right) fat-suppressed proton density-weighted images of a 54 year-old female with pain and limited motion for 6 months demonstrates diffuse thickening and edema of the inferior glenohumeral ligament in the axillary pouch (short arrows) blending with similar changes involving the anterior inferior capsule and inferior glenohumeral ligament (arrows). Posterior pericapsular edema is also seen (arrowheads).
Axillary capsular T2 hyperintensity is less often an imaging feature in the later stages of adhesive capsulitis (stage 3 and 4) (Figure 10).29
Figure 10:
A coronal fat-suppressed T2-weighted image from an MR arthrogram performed on a 40 year-old female with chronic shoulder pain and decreased range of motion demonstrates low signal thickening of the axillary capsule (arrow) suggestive of later stage adhesive capsulitis. Also note extension of fluid along the tendon sheath of the long head of the biceps (arrowhead) resulting from overdistension of the contracted glenohumeral joint.
Enhancement of the rotator interval and of the axillary joint capsule following intravenous gadolinium contrast administration shows the highest sensitivity (90%) for adhesive capsulitis with a specificity of >80%.25 Enhancement is often associated with increased T2 hyperintensity and thickening of these structures (Figure 11).
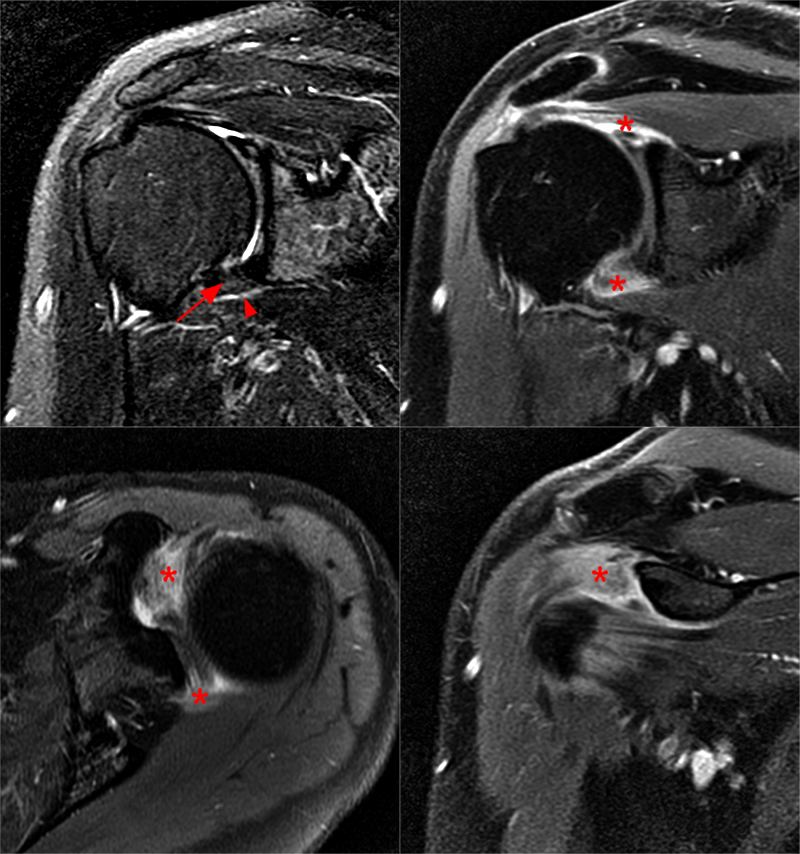
Figure 11:
43 year-old female with shoulder pain for 3 months and no known injury demonstrates a thickened axillary capsule with mildly increased signal (arrow) and mild pericapsular edema (arrowhead) on the coronal fat-suppressed T2-weighted image (top left). Following contrast administration, diffuse synovial, capsular, and pericapsular enhancement (asterisks) demonstrates the extent of inflammatory changes in this patient with idiopathic adhesive capsulitis.
Adhesive capsulitis often coexists with other glenohumeral joint pathology. Rotator cuff tears are frequently complicated by secondary adhesive capsulitis, which can affect the rehabilitation and surgical management (Figure 12).34
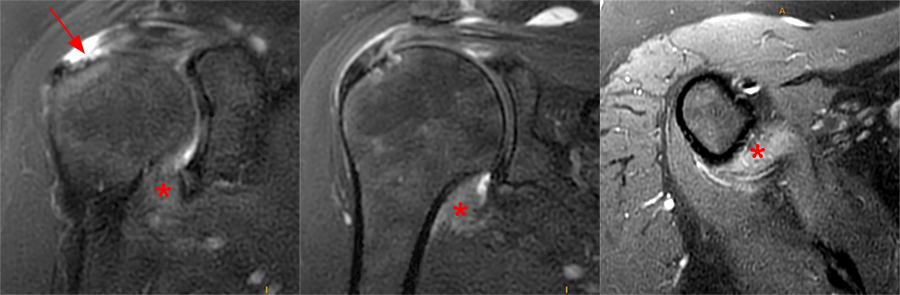
Figure 12:
69 year-old female who bumped into a cabinet 4 months prior with shoulder pain and limited range of motion. Coronal fat-suppressed T2-weighted images at the anterior (left) and mid (middle) glenoid and an axial fat-suppressed proton-density weight image at the inferior glenohumeral joint (right) demonstrate a full-thickness tear of the supraspinatus tendon (arrow) with a thickened and edematous axillary capsule (asterisks) compatible with secondary adhesive capsulitis.
Secondary adhesive capsulitis following shoulder surgery occurs with a prevalence of 5-11%.35 Rehabilitation regimen requiring a limited range of motion can make post-operative management of adhesive capsulitis difficult. The MRI findings are similar to primary adhesive capsulitis (Figure 13).
Figure 13:
A 65 year-old male 5 months after rotator cuff repair with slow recovery of range of motion. A coronal fat-suppressed T2-weighted image (left) through the posterior aspect of the axillary recess demonstrates a prominently thickened and mildly edematous axillary capsule (arrow). Following contrast administration there is prominent diffuse enhancement (arrowheads) consistent with secondary adhesive capsulitis.
Differential Diagnosis
Calcific tendinitis, rotator cuff injury, biceps tendon pathology, and glenohumeral and acromioclavicular arthritis can all present with similar clinical findings of shoulder stiffness and pain. The MRI features of synovial and capsular thickening can be observed following severe shoulder trauma, such as with a shoulder dislocation. A careful clinical history in conjunction with familiarity with the MRI findings help to effectively identify and differentiate adhesive capsulitis from these other conditions.
Treatment
While idiopathic adhesive capsulitis is generally considered a self-limited disease, resolving between 1 and 3 years, several studies have shown that a significant percentage of patients can have persistent symptoms with a more protracted and disabling course.36,5,16,37,38,20
Conservative management is preferred in primary adhesive capsulitis. Nonsteroidal anti-inflammatory medication is helpful with pain relief in the early stages but has not been shown to shorten the course of adhesive capsulitis. Physical therapy is considered of limited value beyond the early stages. Contrasted with physiotherapy alone, intra-articular corticosteroid injections during stage 1 and 2 appear to provide a more rapid improvement in pain and range of motion.16,39,40 Early intervention when pain is the dominant feature has been effective with a combination of physiotherapy, NSAIDs, and intra-articular corticosteroids.16,41 Intra-articular hyaluronate injections have been used with similar clinical outcomes to intra-articular corticosteroids.42,43
Intra-articular hydraulic distension (brisement procedure) is effective in improving pain and function, with the benefit typically limited to 3 months. Diabetics have a poorer response to capsular distension than non-diabetics.44 Dilatation to capsular rupture is no longer the favored approach. Capsular preservation appears to improve short-term outcomes.45
More invasive management includes manipulation under anesthesia (MUA) and arthroscopic release. These procedures are typically reserved for recalcitrant cases that have failed conservative therapy. MUA is well tolerated with improved range of motion within days.46,47 MUA carries the risk of iatrogenic injuries including humeral fracture. Some authors advocate utilizing arthroscopic release in conjunction with manipulation, which results in a greater improvement in pain and range of motion compared with MUA alone.40,48,49,50
Open capsulotomy is effective but rarely performed, typically being reserved for patients that fail arthroscopic release or repeat manipulation under anesthesia.16,40
Pre-existing adhesive capsulitis is commonly encountered in patients requiring rotator cuff repair.51 Past approaches to managing these patients favored preoperative physical therapy to improve range of motion prior to rotator cuff repair. However, the effectiveness of this approach may be compromised by poor patient compliance, progression of the rotator cuff tear resulting from the physical therapy, and potential interval fatty infiltration of the muscle. Current trends call for capsular release and/or manipulation under anesthesia to be performed concurrently with the rotator cuff repair. Presumably because of the hyperemia and inflammation accompanying adhesive capsulitis, tendon repairs appear to heal more quickly, which allows acceleration of mobility in the rehabilitation protocol.52,51
Conclusion
Adhesive capsulitis of the shoulder is a common cause of pain and limitation of motion with an incompletely understood etiology. The diagnosis is commonly made through the combination of clinical history and physical examination findings, but early in the disease process the physical exam findings can be confusing. Shoulder pathologies such as rotator cuff tear, bursitis, and labral pathology may present with similar clinical features and often coexist with adhesive capsulitis. In the early stages of disease, MRI is often able to identify and differentiate adhesive capsulitis from other shoulder pathologies, affording an earlier diagnosis and a more clinically effective treatment plan.
References
- Chi AS, Kim J, Long SS, Morrison WB, Zoga AC. Non-contrast MRI diagnosis of adhesive capsulitis of the shoulder. Clin Imaging. 2017;44(2):46-50. doi:10.1016/j.clinimag.2017.04.002 ↩
- Neviaser AS, Hannafin JA. Adhesive capsulitis: A review of current treatment. Am J Sports Med. 2010;38(11):2346-2356. doi:10.1177/0363546509348048 ↩
- Sheridan MA, Hannafin JA. Upper Extremity: Emphasis on Frozen Shoulder. Orthop Clin North Am. 2006. doi:10.1016/j.ocl.2006.09.009 ↩
- Bunker TD. Frozen shoulder: Unravelling the enigma. Ann R Coll Surg Engl. 1997;79(3):210-213. ↩
- Fields BKK, Skalski MR, Patel DB, et al. Adhesive capsulitis: review of imaging findings, pathophysiology, clinical presentation, and treatment options. Skeletal Radiol. 2019;48(8):1171-1184. doi:10.1007/s00256-018-3139-6 ↩
- Zreik NH, Malik RA, Charalambous CP. Adhesive capsulitis of the shoulder and diabetes: A meta-analysis of prevalence. Muscles Ligaments Tendons J. 2016;6(1):26-34. doi:10.11138/mltj/2016.6.1.026 ↩
- Wohlgethan JR. Frozen shoulder in hyperthyroidism. Arthritis Rheum. 1987;30(8):936-939. doi:10.1002/art.1780300815 ↩
- Bowman CA, Jeffcoate WJ, Patrick M, Doherty M. Case Report: Bilateral Adhesive Capsulitis, Oligoarthritis and Proximal Myopathy as Presentation of Hypothyroidism. Rheumatology. 1988;27(1):62-64. doi:10.1093/rheumatology/27.1.62 ↩
- Choy EHS, Corkill MM, Gibson T, Hicks BH. Isolated acth deficiency presenting with bilateral frozen shoulder. Rheumatology. 1991;30(3):226-227. doi:10.1093/rheumatology/30.3.226 ↩
- Cleeves L, Findley L. Frozen shoulder and other shoulder disturbancies in Parkinson’s disease. J Neurol Neurosurg Psychiatry. 1989;52(6):813-814. doi:10.1136/jnnp.52.6.813-b ↩
- Tuten HR, Young DC, Douoguih WA, Lenhardt KM, Wilkerson JP, Adelaar RS. Adhesive capsulities of the shoulder in male cardiac surgery patients. orthopaedics. 2000;23(7):693-696. doi:10.3928/0147-7447-20000701-16 ↩
- Sung CM, Jung TS, Park H Bin. Are serum lipids involved in primary frozen shoulder? A case-control study. J Bone Jt Surg – Am Vol. 2014;96(21):1828-1833. doi:10.2106/JBJS.M.00936 ↩
- Smith SP, Devaraj VS, Bunker TD. The association between frozen shoulder and Dupuytren’s disease. J Shoulder Elb Surg. 2001;10(2):149-151. doi:10.1067/mse.2001.112883 ↩
- Lundberg BJ. The frozen shoulder. Clinical and radiographical observations. The effect of manipulation under general anesthesia. Structure and glycosaminoglycan content of the joint capsule. Local bone metabolism. Acta Orthop Scand Suppl. 1969;119:1-59. doi:10.3109/ort.1969.40.suppl-119.01 ↩
- Zuckerman JD, Rokito A. Frozen shoulder: A consensus definition. J Shoulder Elb Surg. 2011;20(2):322-325. doi:10.1016/j.jse.2010.07.008 ↩
- Le H V., Lee SJ, Nazarian A, Rodriguez EK. Adhesive capsulitis of the shoulder: review of pathophysiology and current clinical treatments. Shoulder Elb. 2017;9(2):75-84. doi:10.1177/1758573216676786 ↩
- Wang K, Ho V, Hunter-Smith DJ, Beh PS, Smith KM, Weber AB. Risk factors in idiopathic adhesive capsulitis: A case control study. J Shoulder Elb Surg. 2013. doi:10.1016/j.jse.2012.10.049 ↩
- Neviaser RJ, Neviaser TJ. The Frozen Shoulder Diagnosis and Management. Clin Orthop Relat Res. 1987;(223):59-64. doi:10.1097/00003086-198710000-00008 ↩
- Sofka CM, Ciavarra GA, Hannafin JA, Cordasco FA, Potter HG. Magnetic resonance imaging of adhesive capsulitis: Correlation with clinical staging. HSS J. 2008. doi:10.1007/s11420-008-9088-1 ↩
- Gordon JA, Breitbart E, Austin DC, et al. Adhesive Capsulitis: Diagnosis, Etiology, and Treatment Strategies. (Kelly JD, ed.). Springer International Publishing; 2016:149-168. doi:10.1007/978-3-319-25103-5_14 ↩
- Kim Y-S, Kim J-M, Lee Y-G, Hong O-K, Kwon H-S, Ji J-H. Intercellular Adhesion Molecule-1 (ICAM-1, CD54) Is Increased in Adhesive Capsulitis. J Bone Jt Surgery-American Vol. 2013;95(4):e18-1-8. doi:10.2106/JBJS.K.00525 ↩
- Rodeo SA, Hannafin JA, Tom J, Warren RF, Wickiewicz TL. Immunolocalization of cytokines and their receptors in adhesive capsulitis of the shoulder. J Orthop Res. 1997. ↩
- Gondim Teixeira PA, Balaj C, Chanson A, Lecocq S, Louis M, Blum A. Adhesive capsulitis of the shoulder: Value of inferior glenohumeral ligament signal changes on T2-weighted fat-saturated images. Am J Roentgenol. 2012;198(6):589-596. doi:10.2214/AJR.11.7453 ↩
- Mengiardi B, Pfirrmann CWA, Gerber C, Hodler J, Zanetti M. Frozen Shoulder: MR Arthrographic Findings. Radiology. 2004;233(2):486-492. doi:10.1148/radiol.2332031219 ↩
- Suh CH, Yun SJ, Jin W, et al. Systematic review and meta-analysis of magnetic resonance imaging features for diagnosis of adhesive capsulitis of the shoulder. European Radiology. 2018. ↩
- Ahn K-S, Kang CH, Oh Y-W, Jeong W-K. Correlation between magnetic resonance imaging and clinical impairment in patients with adhesive capsulitis. Skeletal Radiol. 2012;41(10):1301-1308. doi:10.1007/s00256-012-1391-8 ↩
- Ahn KS, Kang CH, Kim Y, Jeong WK. Diagnosis of adhesive capsulitis: Comparison of contrast-enhanced MRI with noncontrast-enhanced MRI. Clin Imaging. 2015;39(6):1061-1067. doi:10.1016/j.clinimag.2015.08.006 ↩
- Lee S-Y, Park J, Song S-W. Correlation of MR Arthrographic Findings and Range of Shoulder Motions in Patients With Frozen Shoulder. Am J Roentgenol. 2012;198(1):173-179. doi:10.2214/AJR.10.6173 ↩
- Park S, Lee DH, Yoon SH, Lee HY, Kwack KS. Evaluation of adhesive capsulitis of the shoulder with fat-suppressed T2-weighted MRI: Association between clinical features and MRI findings. Am J Roentgenol. 2016;207(1):135-141. doi:10.2214/AJR.15.15200 ↩
- Sasanuma H, Sugimoto H, Fujita A, et al. Characteristics of dynamic magnetic resonance imaging of idiopathic severe frozen shoulder. J Shoulder Elb Surg. 2017;26(2):e52-e57. doi:10.1016/j.jse.2016.06.003 ↩
- Yoon JP, Chung SW, Lee BJ, et al. Correlations of magnetic resonance imaging findings with clinical symptom severity and prognosis of frozen shoulder. Knee Surgery, Sport Traumatol Arthrosc. 2017;25(10):3242-3250. doi:10.1007/s00167-015-3887-y ↩
- Jung JY, Jee WH, Chun HJ, Kim YS, Chung YG, Kim JM. Adhesive capsulitis of the shoulder: Evaluation with MR arthrography. Eur Radiol. 2006;16(4):791-796. doi:10.1007/s00330-005-0020-5 ↩
- Bunker TD, Reilly J, Baird KS, Hamblen DL. Expression of growth factors, cytokines and matrix metalloproteinases in frozen shoulder. J Bone Jt Surg. 2000;82(5):768-773. doi:10.1302/0301-620X.82B5.9888 ↩
- Yoo JC, Ahn JH, Lee YS, Koh KH. Magnetic Resonance Arthrographic Findings of Presumed Stage-2 Adhesive Capsulitis: Focus on Combined Rotator Cuff Pathology. orthopaedics. 2009;32(1):22-26. doi:10.3928/01477447-20090101-29 ↩
- Redler LH, Dennis ER. Treatment of Adhesive Capsulitis of the Shoulder. J Am Acad Orthop Surg. 2019;27(12):E544-E554. doi:10.5435/JAAOS-D-17-00606 ↩
- Binder AI, Bulgen DY, Hazleman BL, Roberts S. Frozen shoulder: A long-term prospective study. Ann Rheum Dis. 1984;43(3):361-364. doi:10.1136/ard.43.3.361 ↩
- Hand C, Clipsham K, Rees JL, Carr AJ. Long-term outcome of frozen shoulder. J Shoulder Elb Surg. 2008;17(2):231-236. doi:10.1016/j.jse.2007.05.009 ↩
- GRIGGS SM, Ahn A, GREEN A. Idiopathic Adhesive Capsulitis. J Bone Jt Surgery-American Vol. 2000;82(10):1398-1407. doi:10.2106/00004623-200010000-00005 ↩
- Marx RG, Malizia RW, Kenter K, Wickiewicz TL, Hannafin JA. Intra-articular corticosteroid injection for the treatment of idiopathic adhesive capsulitis of the shoulder. HSS J. 2007;3(2):202-207. doi:10.1007/s11420-007-9044-5 ↩
- Maria D’Orsi G, Giai Via A, Frizziero A, Oliva F. Treatment of Adhesive Capsulitis: A Review. Vol 2.; 2012. ↩
- Levine WN, Kashyap CP, Bak SF, Ahmad CS, Blaine TA, Bigliani LU. Nonoperative management of idiopathic adhesive capsulitis. J Shoulder Elb Surg. 2007. doi:10.1016/j.jse.2006.12.007 ↩
- Calis M, Demir H, Ulker S, Kirnap M, Duygulu F, Calis HT. Is intraarticular sodium hyaluronate injection an alternative treatment in patients with adhesive capsulitis? Rheumatol Int. 2006;26(6):536-540. doi:10.1007/s00296-005-0022-2 ↩
- Tamai K, Mashitori H, Ohno W, Hamada J, Sakai H, Saotome K. Synovial response to intraarticular injections of hyaluronate in frozen shoulder: A quantitative assessment with dynamic magnetic resonance imaging. J Orthop Sci. 2004;9(3):230-234. doi:10.1007/s00776-004-0766-7 ↩
- Rymaruk S, Peach C. Indications for hydrodilatation for frozen shoulder. EFORT Open Rev. 2017;2(11):462-468. doi:10.1302/2058-5241.2.160061 ↩
- Kim K, Lee KJ, Kim HC, Lee KJ, Kim DK, Chung SG. Capsule preservation improves short-term outcome of hydraulic distension in painful stiff shoulder. J Orthop Res. 2011;29(11):1688-1694. doi:10.1002/jor.21446 ↩
- Dodenhoff RM, Levy O, Wilson A, Copeland SA. Manipulation under anesthesia for primary frozen shoulder: Effect on early recovery and return to activity. J Shoulder Elb Surg. 2000;9(1):23-26. doi:10.1016/S1058-2746(00)90005-3 ↩
- Kivimäki J, Pohjolainen T, Malmivaara A, et al. Manipulation under anesthesia with home exercises versus home exercises alone in the treatment of frozen shoulder: A randomized, controlled trial with 125 patients. J Shoulder Elb Surg. 2007;16(6):722-726. doi:10.1016/j.jse.2007.02.125 ↩
- Manske RC, Prohaska D. Diagnosis and management of adhesive capsulitis. Curr Rev Musculoskelet Med. 2008;1(3-4):180-189. doi:10.1007/s12178-008-9031-6 ↩
- Baums MH, Spahn G, Nozaki M, Steckel H, Schultz W, Klinger HM. Functional outcome and general health status in patients after arthroscopic release in adhesive capsulitis. Knee Surgery, Sport Traumatol Arthrosc. 2007;15(5):638-644. doi:10.1007/s00167-006-0203-x ↩
- Ogilvie-Harris DJ, Biggs DJ, Fitsialos DP, MacKay M. The Resistant Frozen Shoulder. Clin Orthop Relat Res. 1995;(319):238-248. doi:10.1097/00003086-199510000-00026 ↩
- Zhang K, de SA D, Kanakamedala A, Sheean AJ, Vyas D. Management of Concomitant Preoperative Rotator Cuff Pathology and Adhesive Capsulitis: A Systematic Review of Indications, Treatment Approaches, and Outcomes. Arthrosc – J Arthrosc Relat Surg. 2019;35(3):979-993. ↩
- McNamara WJ, Lam PH, Murrell GAC. The relationship between shoulder stiffness and rotator cuff healing a study of 1,533 consecutive arthroscopic rotator cuff repairs. J Bone Jt Surg – Am Vol. 2016;98(22):1879-1889. doi:10.2106/JBJS.15.00923 ↩