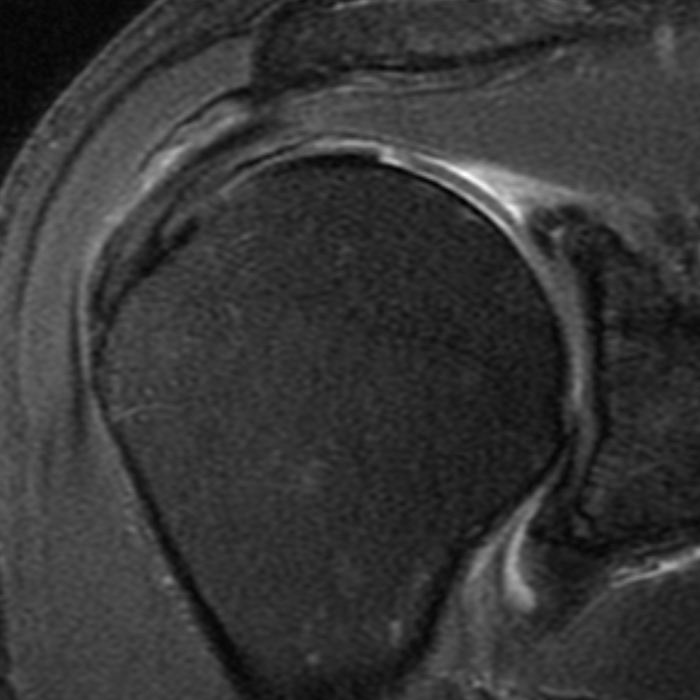
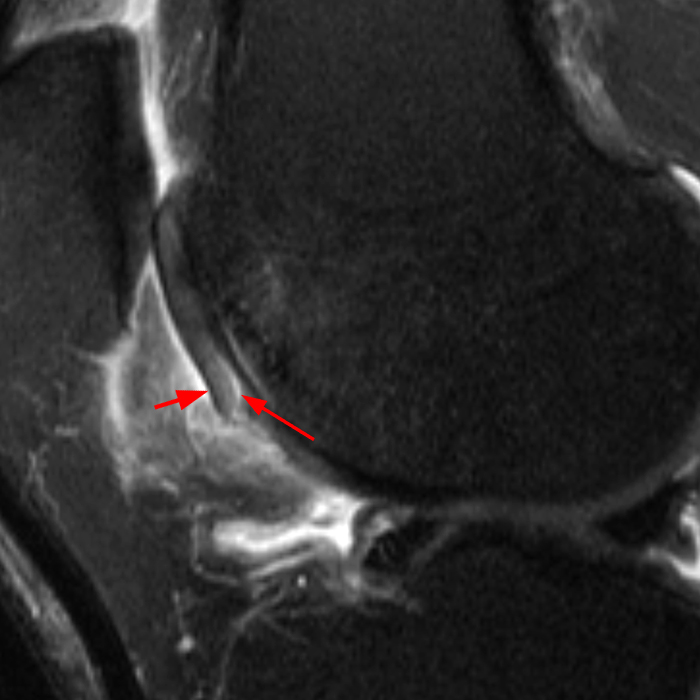
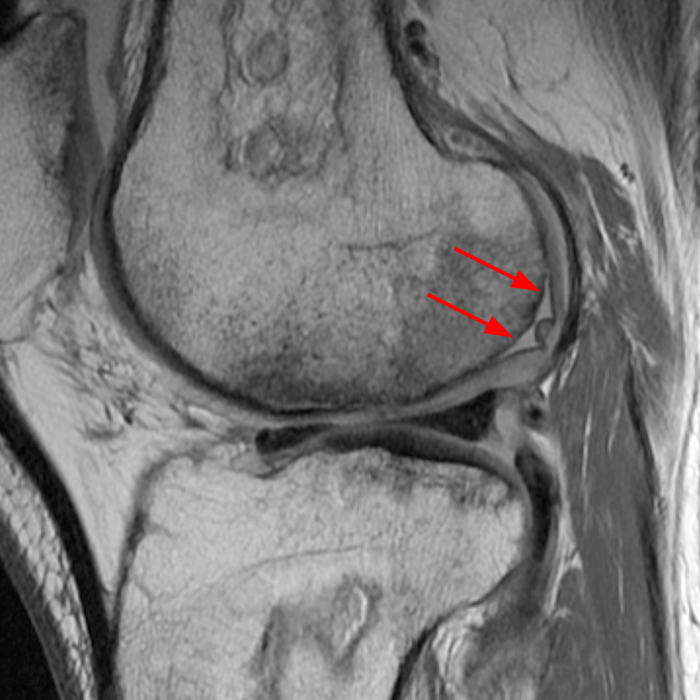
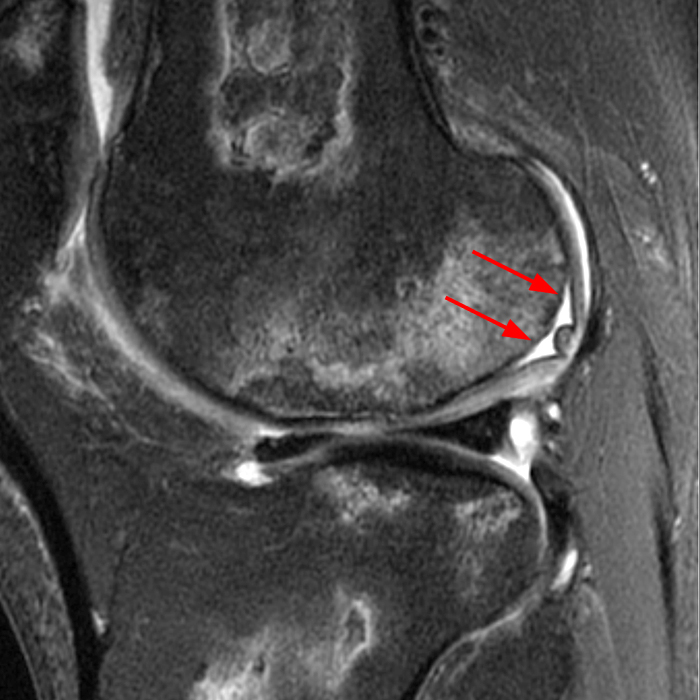
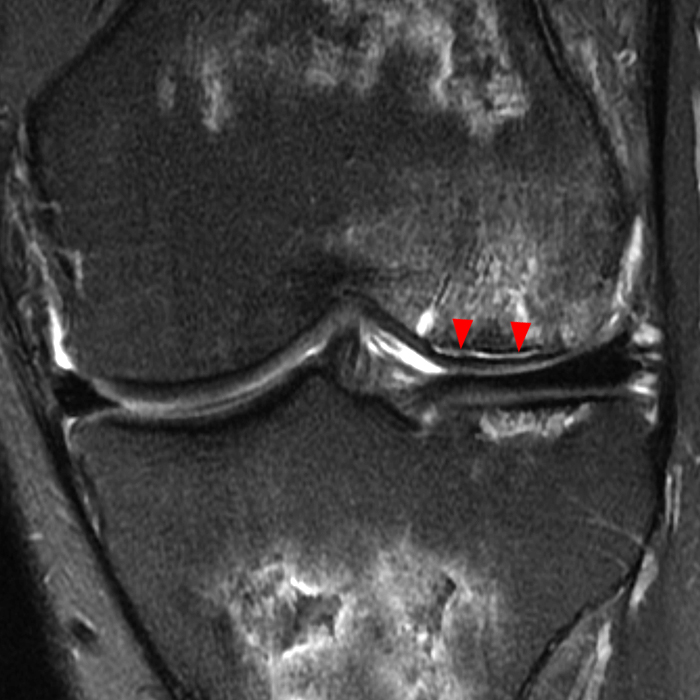
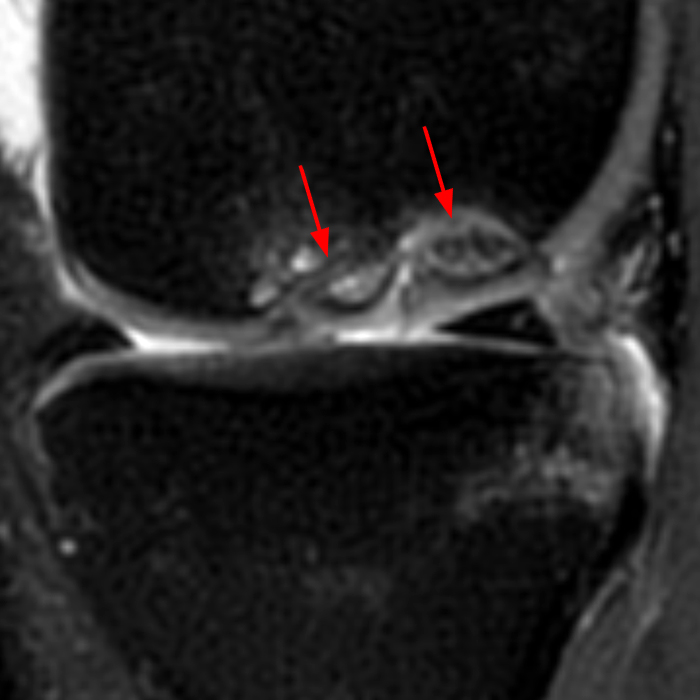
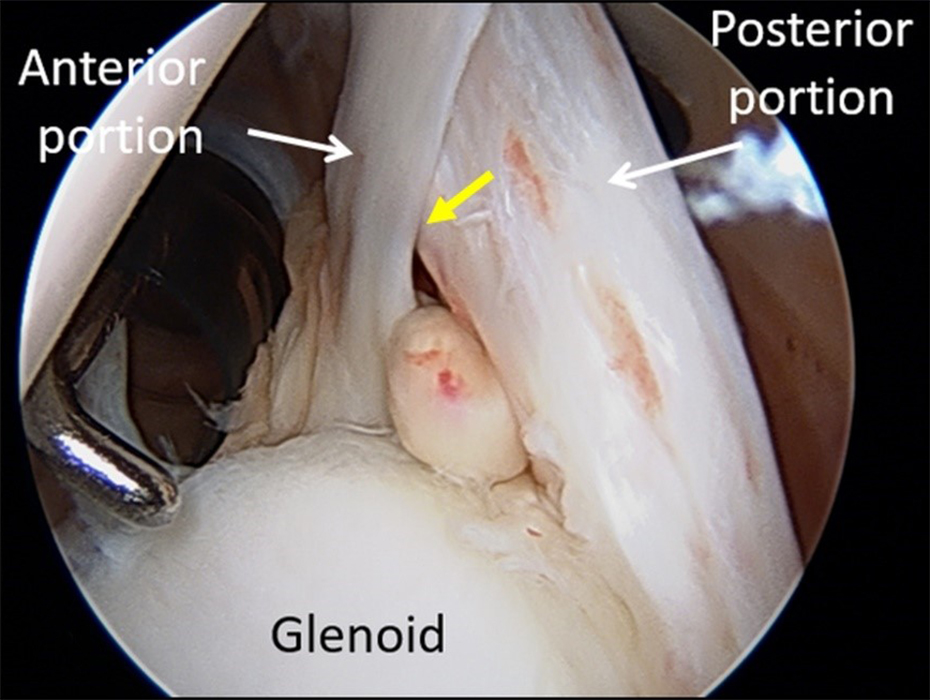
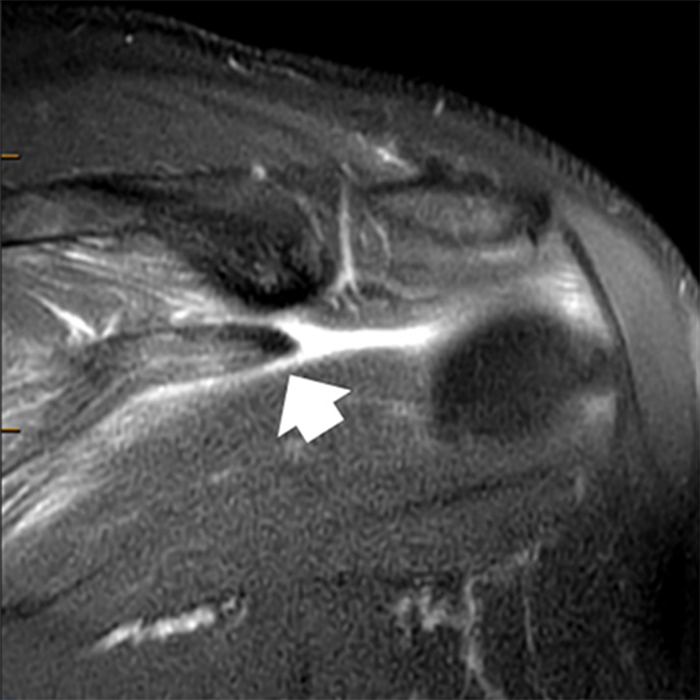
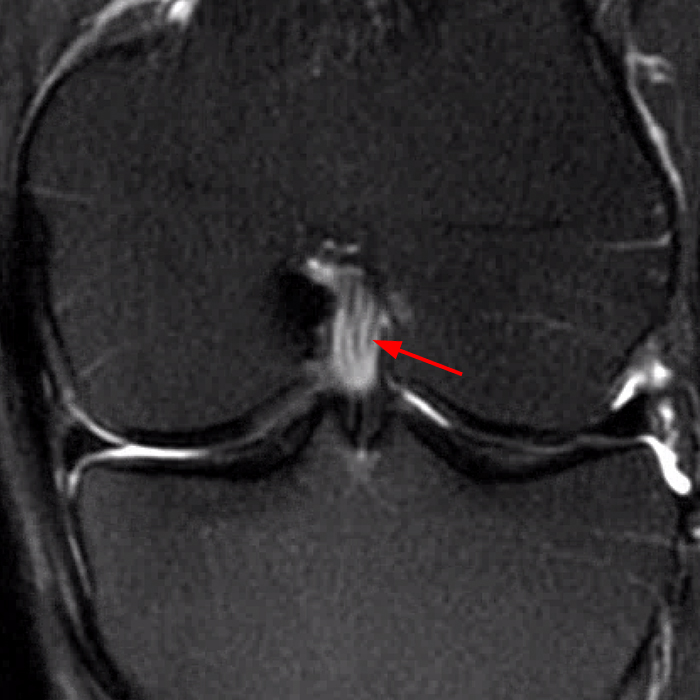
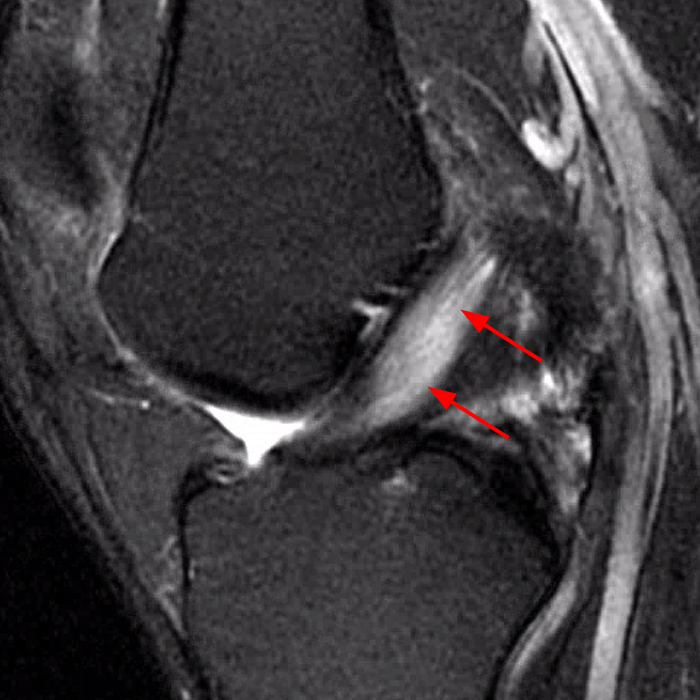
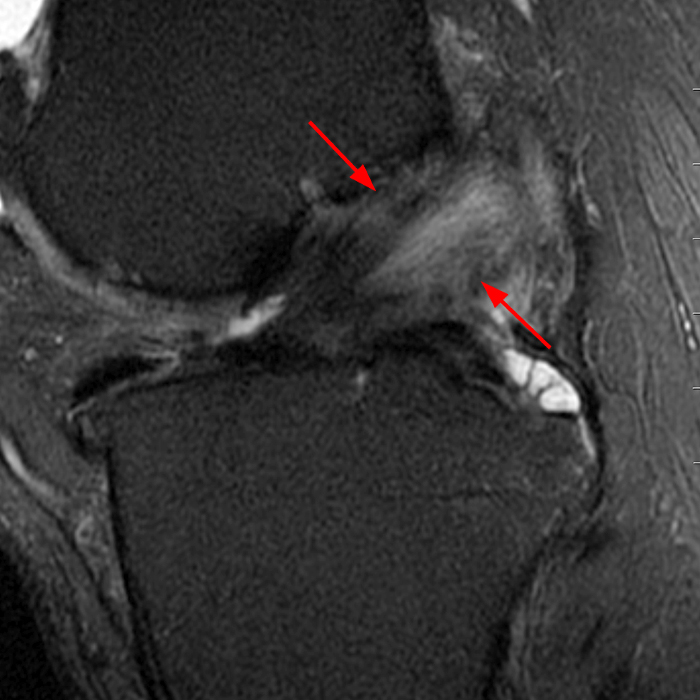
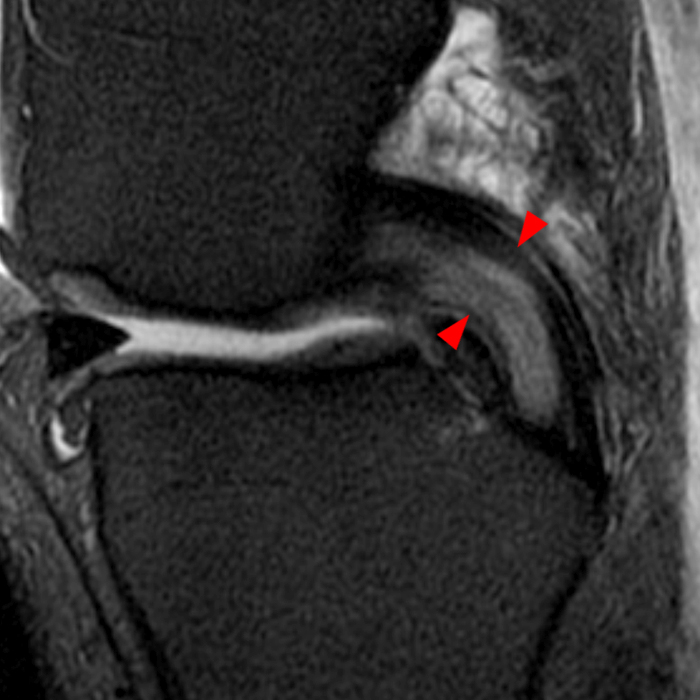
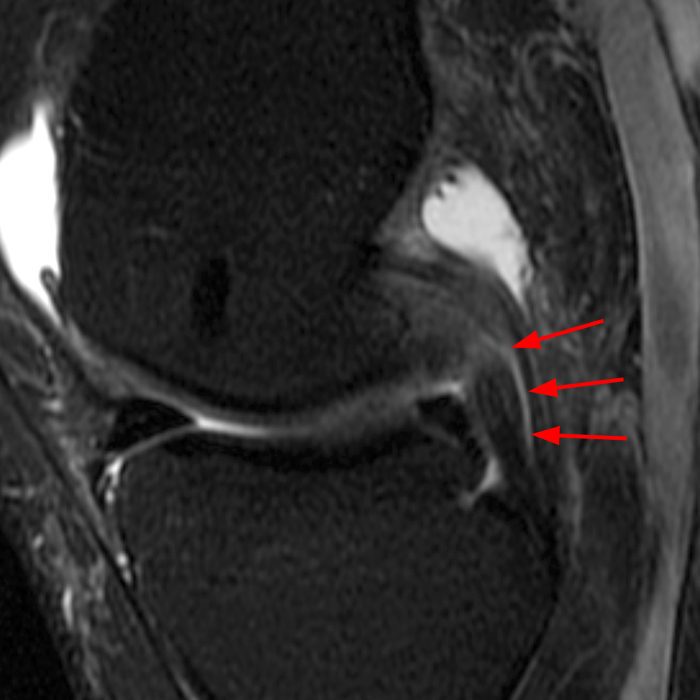
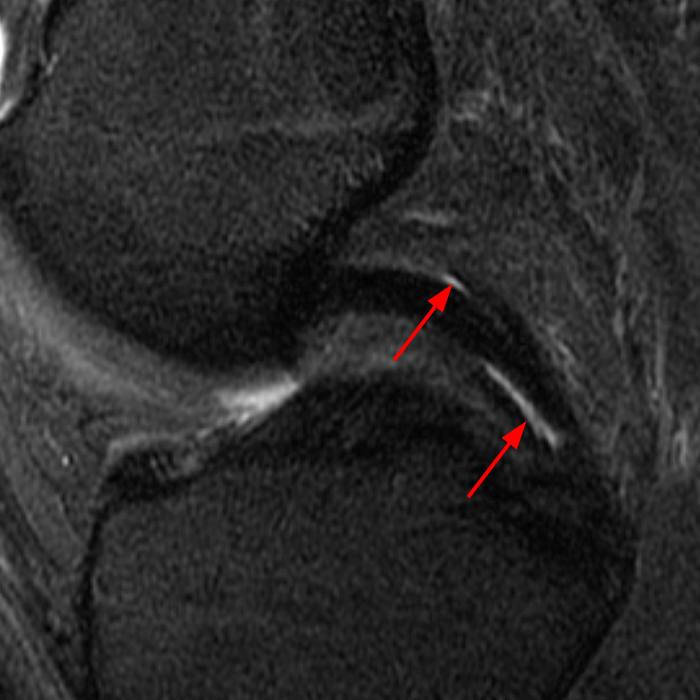
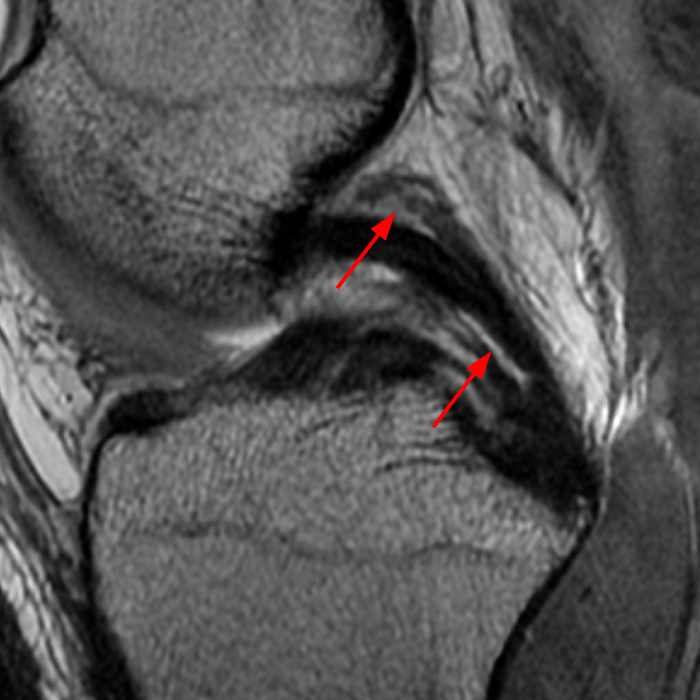
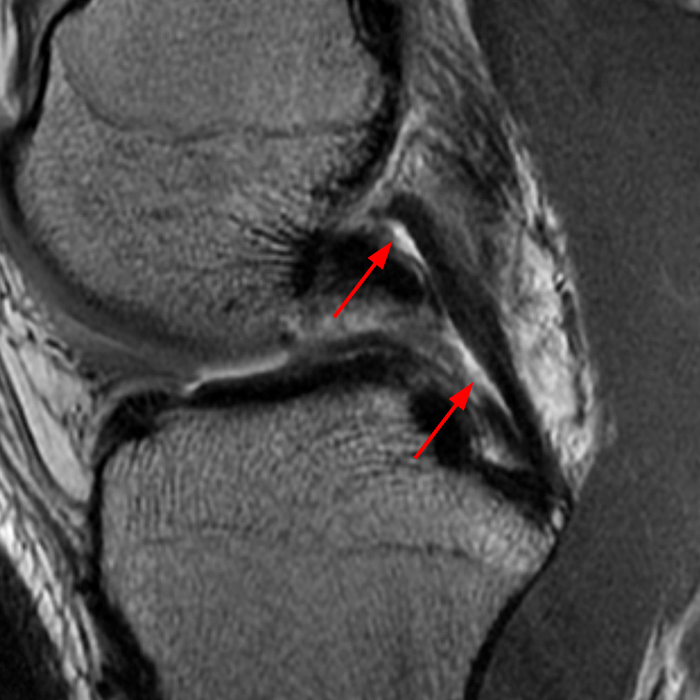
Clinical History: A 66 year-old man presents with persistent right shoulder pain, accompanied by painful clicking. (1A,B) T2-weighted fat-suppressed coronal MR images of the right shoulder are provided. What are the findings? What is your diagnosis?
Findings
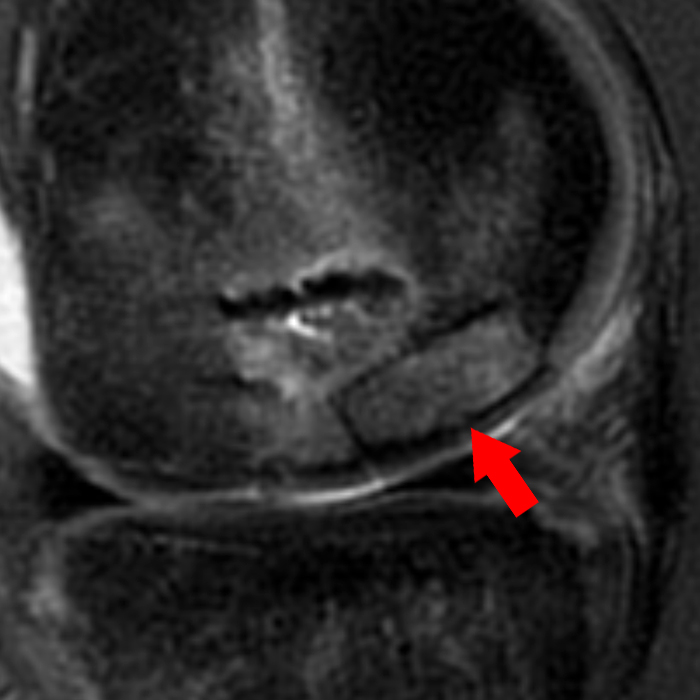
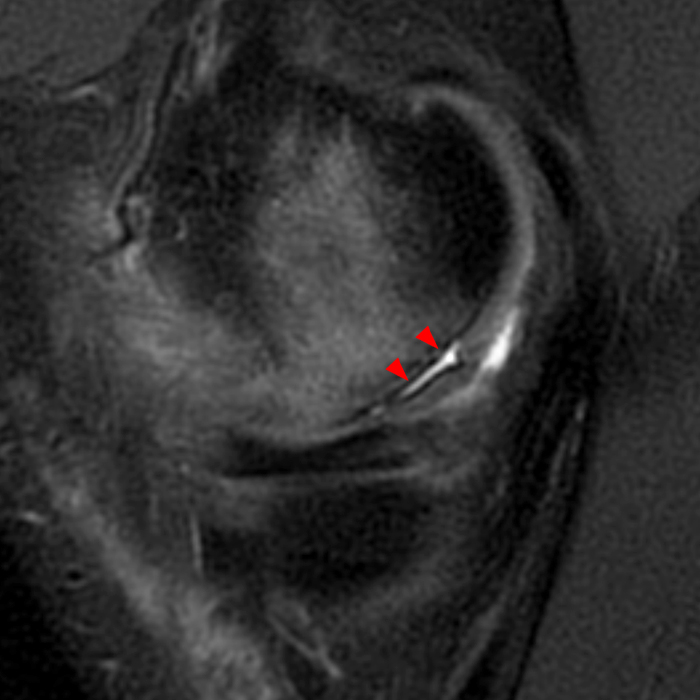
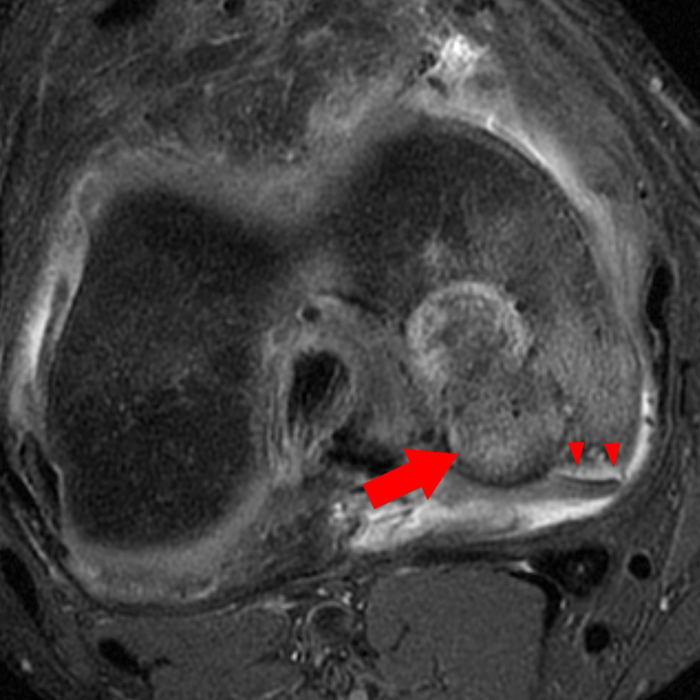
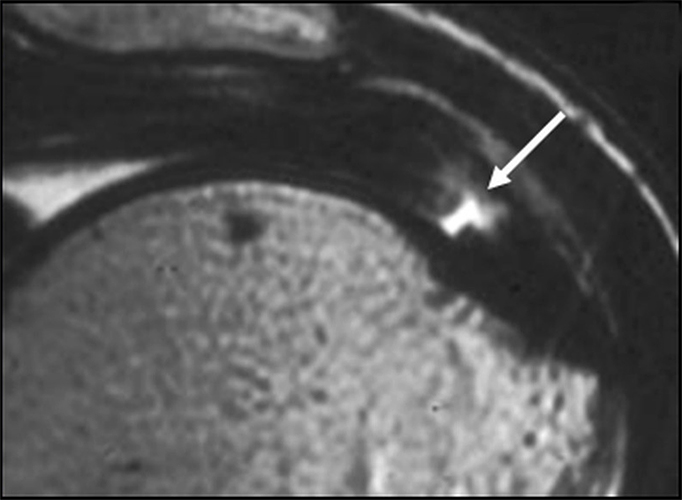
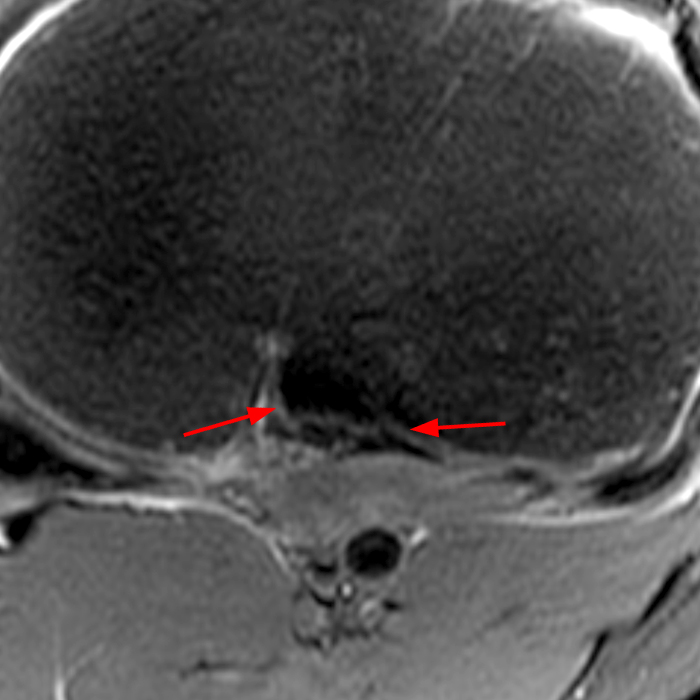
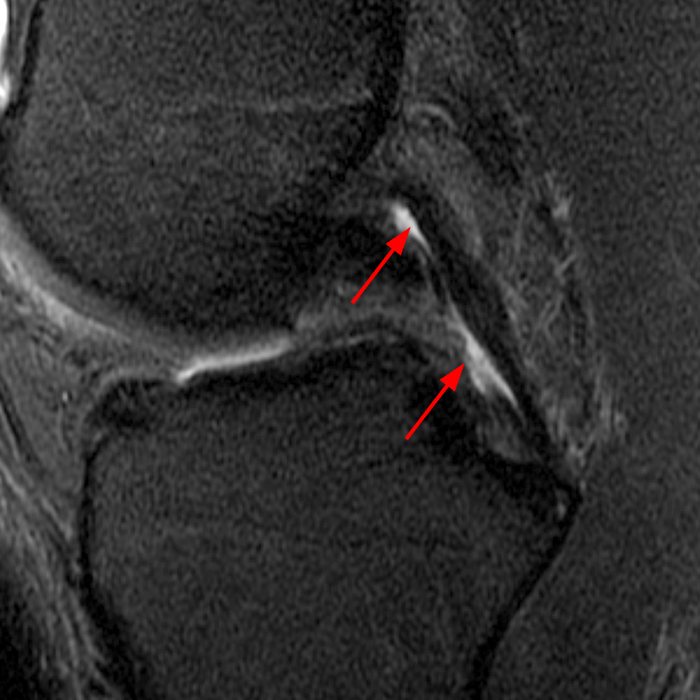
Figure 2:
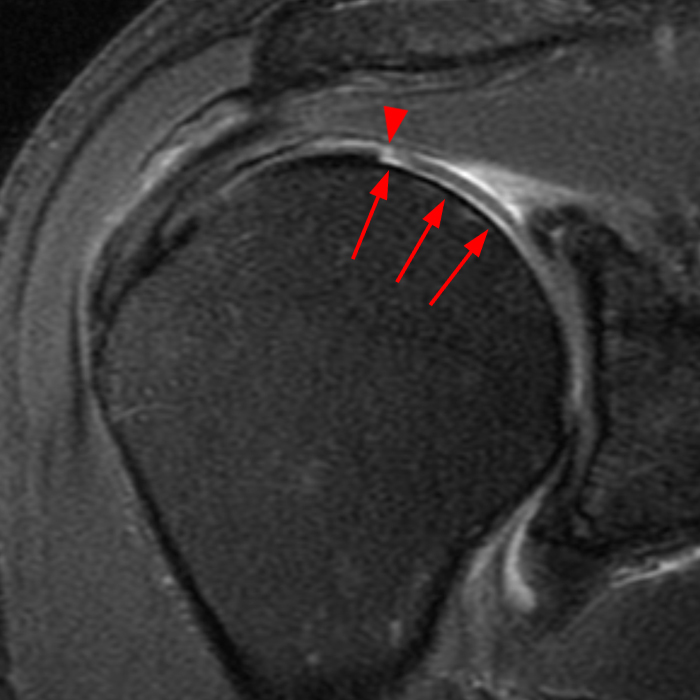
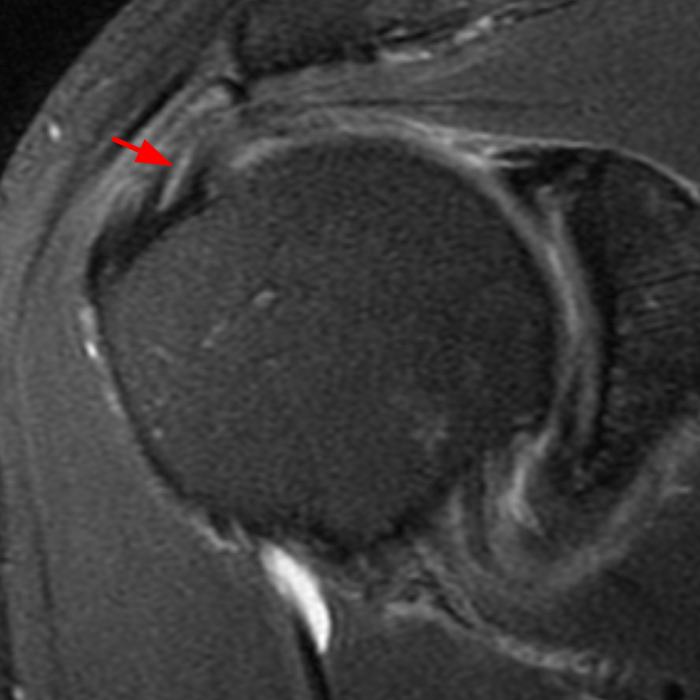
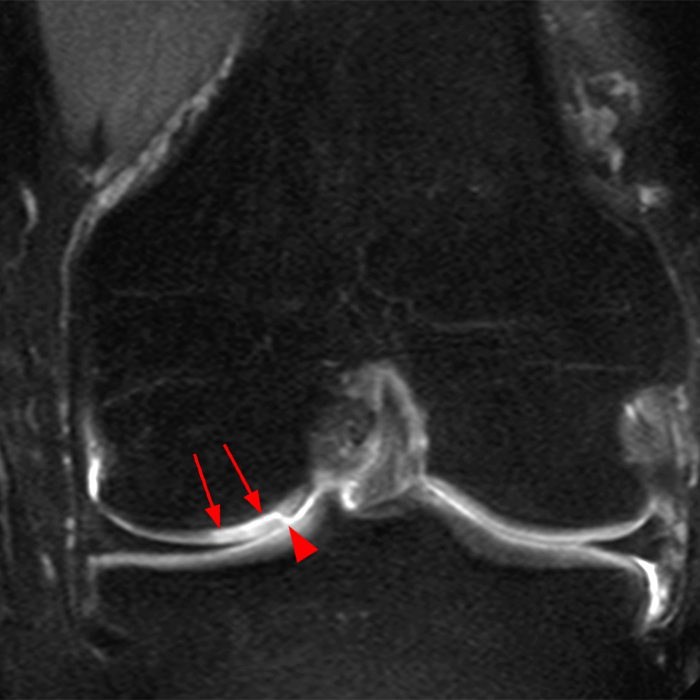
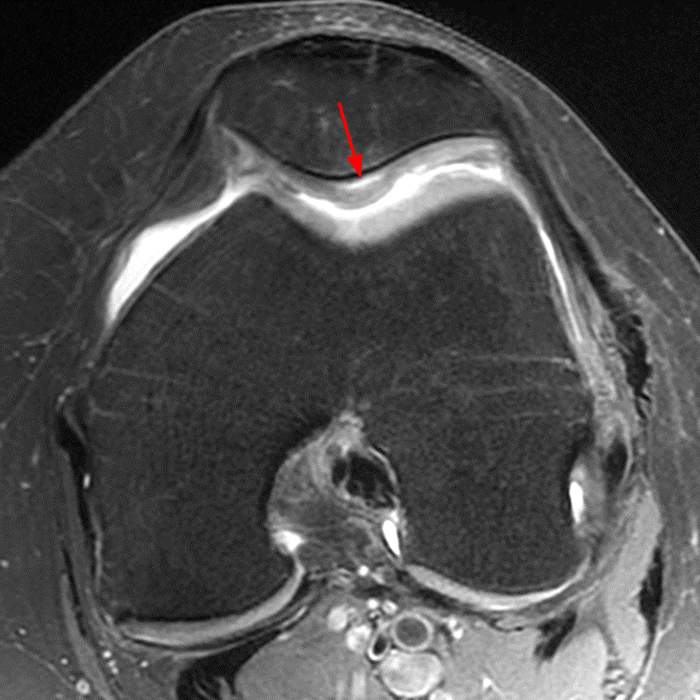
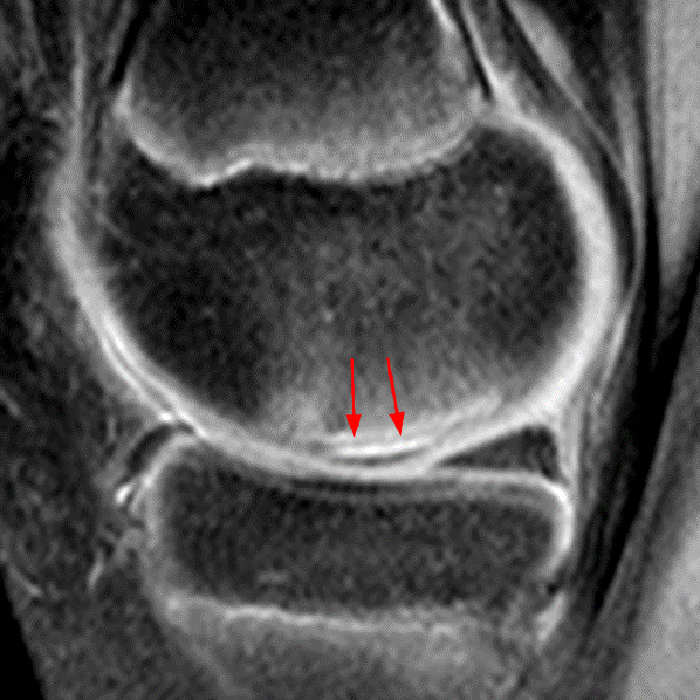
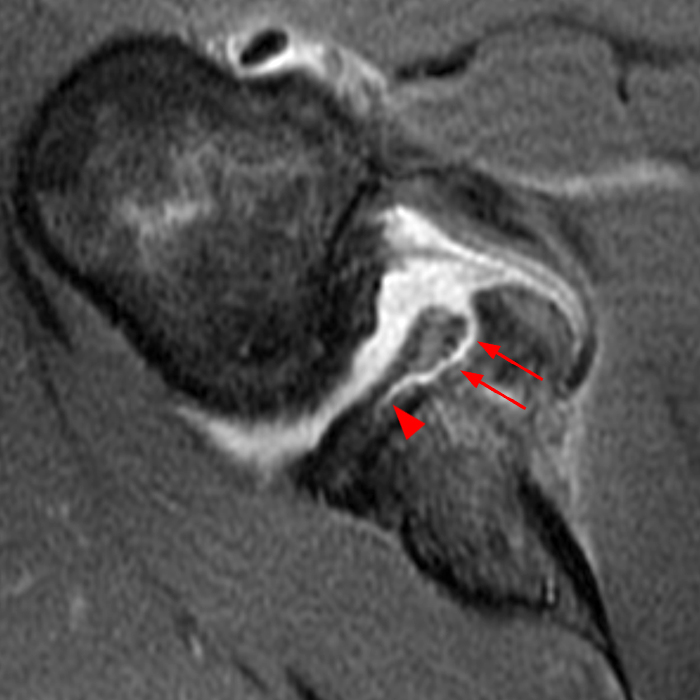
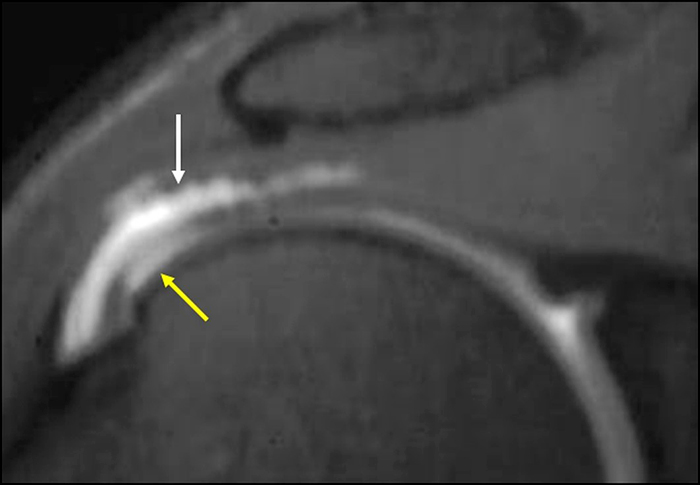
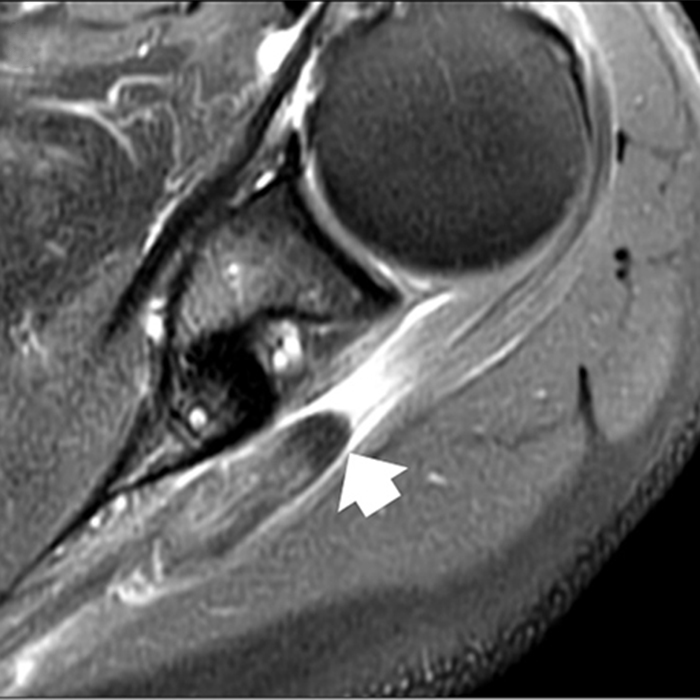
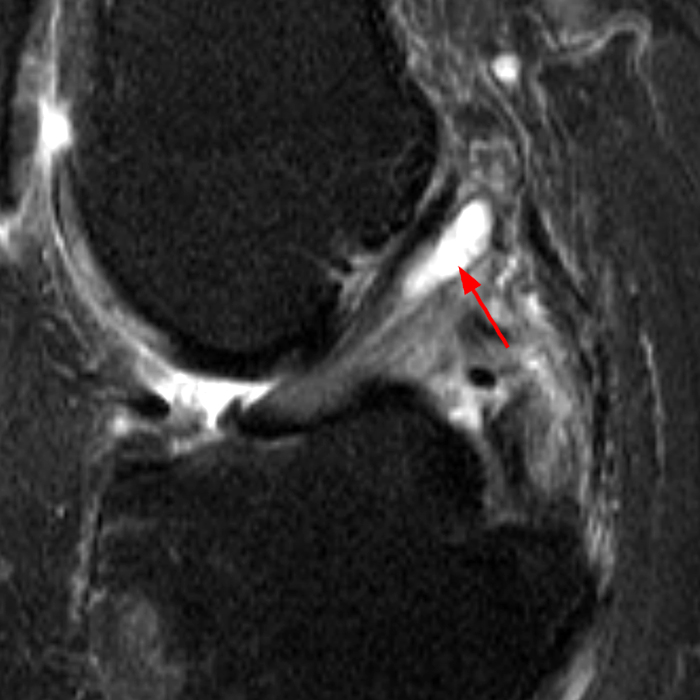
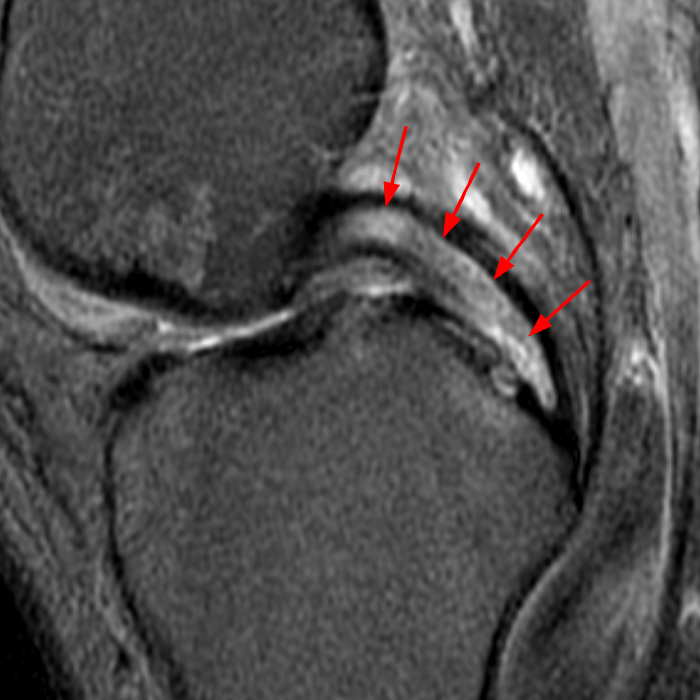
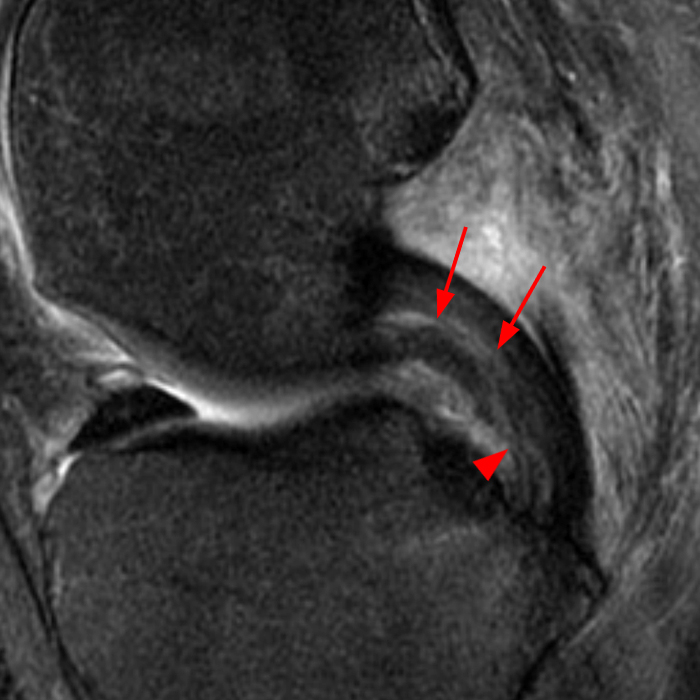
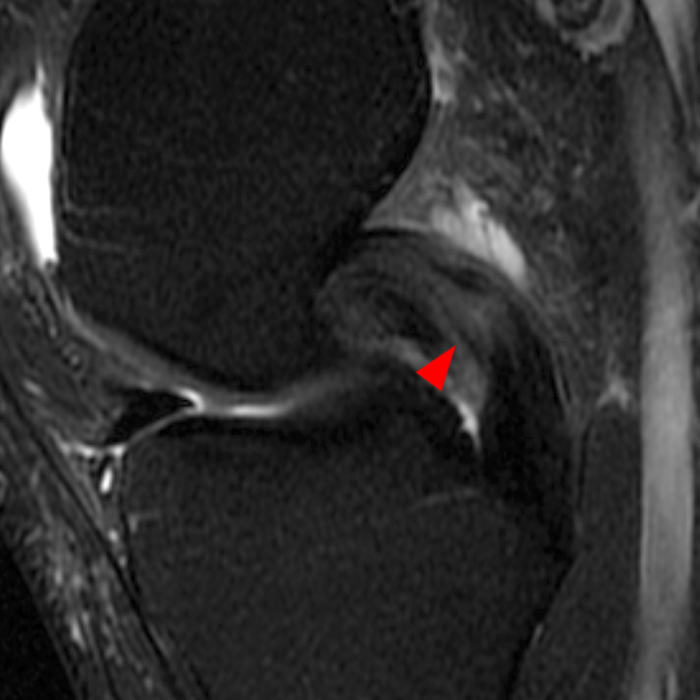
(2A) Coronal T2-weighted fat-suppressed image of the shoulder demonstrates chondral delamination (arrows) involving a large region of the articular cartilage of the humeral head, appearing as a curvilinear region of high signal at the tidemark, separating the noncalcified cartilage from the underlying subchondral bone and calcified cartilage. There is associated disruption of the surface of the articular cartilage (arrowhead). Note that the delamination extends far beyond the margin of the superficial chondral defect. (2B) Additional coronal T2-weighted fat-suppressed image of the shoulder shows a low-grade intrasubstance delaminated tear (arrow) of the distal fibers of the supraspinatus tendon, which would likely escape detection at the time of arthroscopy and bursoscopy. In addition, there is tendinosis and articular-sided and bursal-sided fraying of this tendon.
Diagnosis
Extensive chondral delamination involving the humeral head.
Low-grade intrasubstance delaminated tear of the supraspinatus tendon.
Introduction
In the English language, a lamina is a thin layer or plate. A similar term, lamella, is defined as a thin plate-like layer or structure. Lamination is a process of manufacturing a material into multiple layers, and lamellation is an arrangement or structure in which there are thin layers or plates. Delamination, the subject of this web clinic, is defined as a mode of failure in which a material fractures or separates into layers. Of note, the word “delamellation” is not found in most English dictionaries.
Delamination is a well-known pattern of failure in composite material, related typically to the presence of weak adhesions between layers within that material, such as the failure of weak fiber polymers that are located between sheets of plastic. Delamination is recognized in cement, ceramics, and even in wood logs in which it is designated “shake”, representing failure of timber related to delamination along growth rings. The occurrence of delamination in many of these materials has been attributed to compression, shear, or tensile force, alone or in combination.
Delamination of human tissue is also well known. With regard to the musculoskeletal system, even a quick review of the recent scientific literature will confirm a large number of publications describing in detail delamination of cartilage and tendons. Although a similar process occurring in ligaments, menisci, and labra has received little or no attention, the term delamination can be used to describe certain patterns of failure in these tissues as well. An understanding of delamination in cartilage, tendons, ligaments, and menisci requires knowledge of the anatomic arrangement of the collagen framework in these tissues. Specifically, with regard to failure of human tendons, the plane of separation, or delamination, is along the longitudinal axis of the major collagen fibers, not through them, a situation that also occurs in ligaments. The collagen arrangement in articular cartilage and menisci, however, is more complex, creating confusion as to what represents true delamination in those tissues.
Cartilage
In most regions of the human body, articular cartilage is hyaline in type. Cartilage has low cellular content, with the chondrocytes constituting only about 2% of its total volume.1 The arrangement of the chondrocytes varies with depth. Near the articular surface, the chondrocytes are disc-shaped and oriented horizontally, while in the deeper portions of the cartilage, the chondrocytes are rounded in shape and arranged into columns.2,3 In the deep zone of cartilage, the highly ordered perpendicularly-oriented collagen fibers propagate around these columns of chondrocytes.3
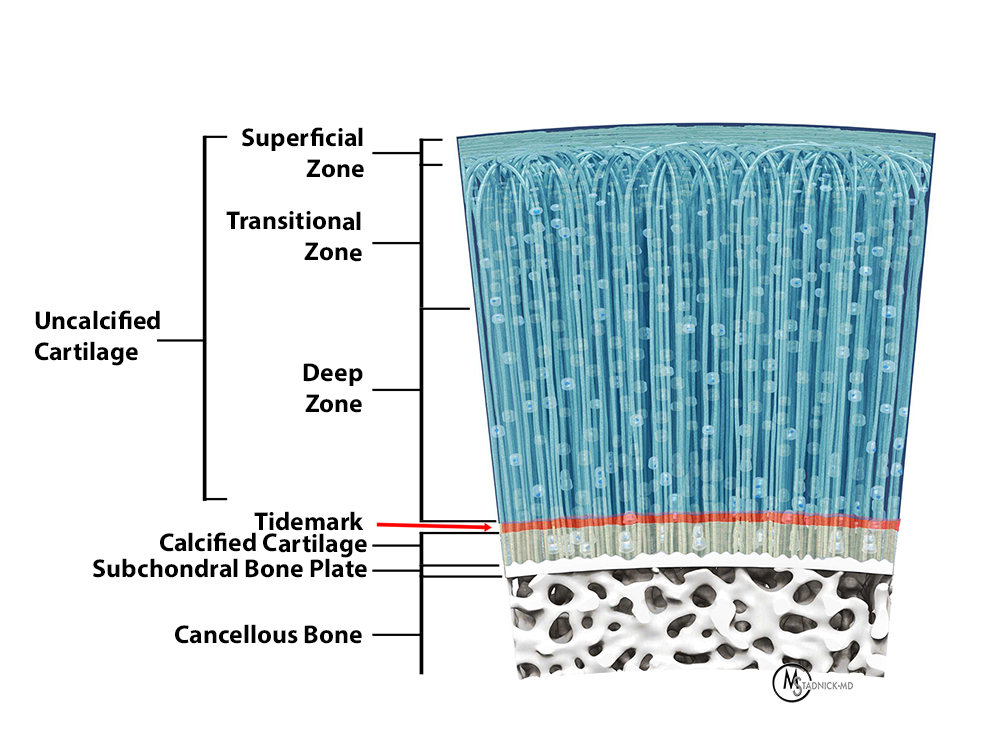
The collagen framework of articular cartilage that, along with the proteoglycans, fulfills the mechanical role of the tissue, is painted on this cellular background. The lamina splendens is the most superficial layer of articular cartilage, being characterized by a high density of collagen fibers oriented parallel to the articular surface, loosely anchored to the underlying superficial zone.4 The collagen fibers in articular cartilage are arranged parallel to the surface in the superficial zone, arching through the transitional zone, and are oriented perpendicular to the surface in the deep zone (Figures 3 and 4).5,6 These arc-like columns of collagen are known as the arcades of Benninghoff. They extend through the entire thickness of the uncalcified cartilage to the tidemark and below, anchoring the cartilage to the subchondral bone plate.6,7 The tidemark represents the line between the uncalcified cartilage in the deep zone and the subjacent calcified cartilage.7 In the calcified zone, the collagen fibers maintain a perpendicular orientation, with deposits of calcification along their length.2
Figure 3:
Illustration of articular cartilage showing the collagen fibers oriented parallel to the surface in the superficial zone, curved in the transitional zone, and perpendicular to the surface in the deep zone. The tidemark represents the interface between the uncalcified cartilage and the calcified cartilage. Note the arrangement of the chondrocytes, which are flat and disc-shaped near the articular surface, and round in shape in the deeper portions.
Figure 4:
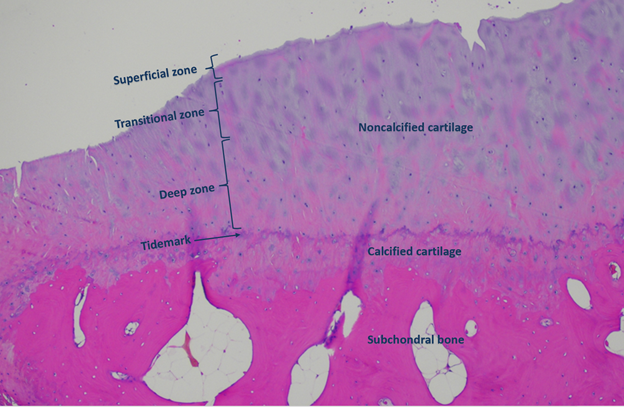
Histologic image of articular cartilage, with the superficial, transitional, and deep zones labeled. The tidemark (arrow) separates the noncalcified cartilage from the calcified cartilage. Note superficial areas of chondral fissuring (arrowheads). Image courtesy of Dr. P. Haghighi, San Diego, California.
A review of the available literature indicates that cartilage delamination is generally described as occurring at the tidemark (Figure 5), where shear forces cause separation of the uncalcified articular cartilage superficial to the tidemark from the calcified cartilage and bone deep to the tidemark.8 The calcified cartilage, therefore, remains attached to the subchondral bone plate.
Figure 5:
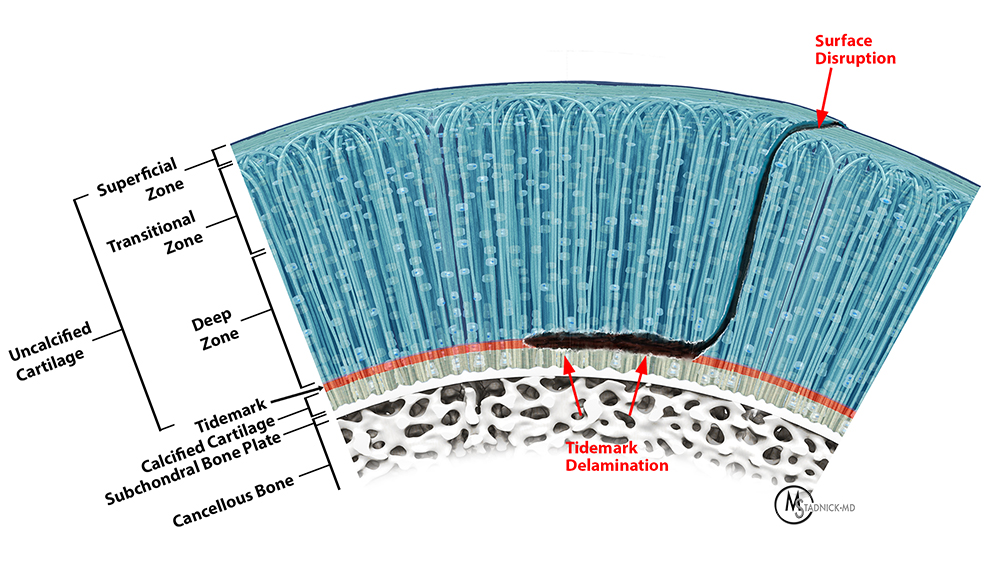
Illustration of chondral delamination occurring at the tidemark, separating the uncalcified cartilage above from the calcified cartilage and bone below. When delamination occurs at the tidemark, the overlying articular surface may be disrupted, as shown in this diagram, or may remain intact.
In order to understand the shear forces that act at the tidemark, we must first discuss compressive forces and introduce the concept of “buckling”. Buckling is a mode of failure that occurs in slender structural columns, such as collagen fibrils, in which compressive forces lead to lateral deflection, or bending, of the column.9 Buckling of collagen fibers occurs mostly in the transitional zone, with the collagen fibers in the deep zone demonstrating a greater stiffness.10 When the cartilage is compressed, it deforms, leading to bulk outflow of water through the extracellular matrix. As a result of the discrepancy in compressive stiffness between the noncalcified cartilage and the much stiffer underlying calcified cartilage and bone, the lateral deformation of the articular cartilage is constrained by the calcified cartilage bed, and resultant shear forces develop at the tidemark, causing delamination.11 Therefore, the tidemark delaminates much more easily than the deeper junctional region between cartilage and subchondral bone.12
With MRI, chondral delamination usually appears as a thin line of near-fluid signal intensity beneath the deep zone of articular cartilage, at the tidemark, separating the noncalcified cartilage from the underlying bone and calcified cartilage (Figures 6-9). In some cases, however, the zone of separation is thicker and even irregular in appearance, and marrow edema-like signal may be present in the subchondral bone.13 Whether the zone of separation is thin and regular or thick and irregular, it is critical to realize that the overlying cartilage surface may or may not be violated. Therefore, even with extensive delamination in the deeper region of the chondral coat, at the time of arthroscopy the surface of the articular cartilage may appear entirely normal, or there may only be a subtle bulge of the cartilage surface.14 Furthermore, when violation of the chondral surface does occur, the extent of delamination often extends beyond the margin of the superficial chondral defect.8
Figure 6:
Delamination of the articular cartilage of the medial femoral condyle (arrows) as displayed in a coronal fat-suppressed T2-weighted MR image. Note that there is disruption of the surface of the articular cartilage (arrowhead) and that the delamination extends well beyond the location of this chondral defect.
Figure 7:
Delamination of the patellar cartilage in a 40 year-old female runner with anterior knee pain. An axial proton density-weighted fat-suppressed image demonstrates chondral delamination involving the patellar median ridge (arrow). Note that there is no disruption of the cartilage surface in this case.
There are additional chondral abnormalities in both the medial and lateral facets of the patella and central region of the trochlea.
Figure 8:
14 year-old basketball player with concealed delamination involving the articular cartilage of the medial femoral condyle as displayed in sagittal and coronal fat-suppressed fluid-sensitive MR images (arrows). The surface of the articular cartilage is normal, which may preclude arthroscopic identification of the significant area of delamination that lies below. A helpful clue in this case is the presence of subjacent marrow abnormalities.
Figure 9:
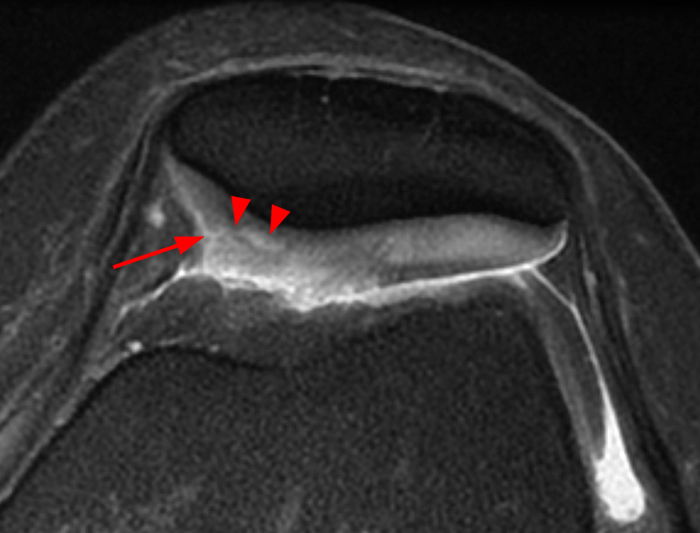
In a 40 year-old man with a prior anterior dislocation of the glenohumeral joint, this axial T2-weighted fat-suppressed MR image shows delamination of the anterior glenoid cartilage at the tidemark (arrows), with propagation of a transversely-oriented tear extending into the midzone of the cartilage (arrowhead), which does not yet reach the articular surface, resulting in a chondral flap. Also note the deformity of the adjacent anteroinferior surface of the glenoid and labrum, indicative of a chronic bony Bankart lesion.
When one cartilage surface translates over another, shear stress develops at the articular surface. The normal articular cartilage surface has a coefficient of friction that is much lower than that of man-made materials, due to the smooth surface of the lamina splendens and the presence of specialized molecules in the surface layer that provide lubrication, such as lubricin.11 When excessive shear forces develop near the surface, surface-layer damage of the articular cartilage can occur, including fibrillation or fissuring (Figures 10 and 11). Fibrillation is defined as a process of forming fine fibers or fibrils. In articular cartilage, fibrillation results in surface irregularity of the cartilage, related to disorganization of the horizontally-oriented collagen bundles in the superficial cartilage layers.15 As the superficial collagen fibers have been described as layered or leaf-like in distribution, fibrillation can be considered a process of delamination, separating one surface layer of collagen from another. Fissuring is defined as a split or crack that is long and narrow. Chondral fissuring occurs primarily as a result of delamination between the obliquely and vertically oriented collagen fibrils, rather than by breakage of collagen fibrils.15 Specifically, a chondral fissure propagates by breaking bonds between the collagen fibrils.15,16
Figure 10:
Fissuring involving the patellar cartilage (arrow) as shown in this axial fluid-sensitive fat-suppressed MR image. Note that in this case, the fissure extends from the chondral surface through most of the entire thickness of the cartilage. Of interest, the medial surface of the patella is flat and vertically oriented, representing the so-called Jagerhut-patella.
Figure 11:
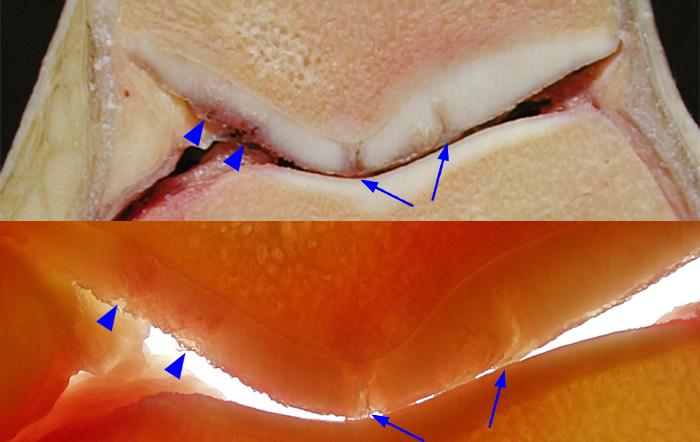
Fissuring involving the patellar cartilage as displayed in two transverse sections of the patella and adjacent trochlea in a cadaver. Note that the fissures (arrows) are vertically oriented and of various length involving mainly the median ridge and lateral facet of the patella. There is also both fissuring and fibrillation of the articular cartilage in the medial patellar facet (arrowheads). In comparison, note the normal smooth surface of the trochlear cartilage.
A transversely oriented region of failure in the midzone of articular cartilage is sometimes seen in association with chondral fissures on MRI (Figures 12 and 13). The interpretation of this finding and even its pathogenesis are not clear. One explanation might relate to the transverse nature of some of the cellular components of articular cartilage, appearing in rows. Thus, the process might be designated cartilage delamination of cellular rows, rather than collagen fibers, with the cellular architecture being used as the point of reference. Such a process, however, would intersect the classically described vertical arcades of collagen, unless these arcades have been modified as a response to a preexisting disorder. Specifically, in osteoarthrosis, extensive changes in the normal collagen organization have been reported, with the orientation of the collagen fibers demonstrating a wide range of angles, as well as regions with parallel collagen fibrils. There is also loosening of the collagen matrix, chondral fibrillation, and replacement of type II collagen with type I collagen in osteoarthritis.17 Therefore, it is possible that the transversely-oriented region of failure that is sometimes seen in the midzone of articular cartilage may represent delamination between pathologically disorganized collagen fibers. Until this process is better understood, however, there will be inconsistencies in the manner in which it is described and lack of agreement whether midzonal chondral failure should be designated as delamination.
Figure 13:
Sagittal T2-weighted fat-suppressed MR image demonstrating fissuring of the trochlear cartilage with the component of failure in the mid/deep zone of the cartilage (long arrow) occurring parallel to the chondral surface, but superficial to the tidemark. An associated chondral flap is noted (short arrow).
Failure of the subchondral bone plate undermines the integrity of the overlying articular cartilage.11 As one final extension of the term delamination, in the presence of a process that weakens the subchondral bone plate or adjacent subchondral bone, shear forces could lead to delamination of the entire chondral layer and even portions of the subchondral bone plate (Figure 14). Some processes that might cause this include primary or secondary hyperparathyroidism with skeletal involvement and osteonecrosis. With hyperparathyroidism, subchondral resorption of bone is the culprit. In osteonecrosis, the situation is complicated as fractures, which manifest as the crescent sign, develop in regions of necrotic bone and may be located in the subchondral bone or in the subchondral bone plate itself, from where they may extend as a cleavage plane into the adjacent articular cartilage, even disrupting the chondral surface.
Figure 14:
A 42 year-old man with a history of plasmacytoma of the left humerus and polyneuropathy, treated with long-term chemotherapy and corticosteroid medication, the latter resulting in multiple foci of osteonecrosis and bone infarcts about both knees. He presented with posterolateral left knee pain, stiffness, swelling, and weakness. (A) Proton density-weighted sagittal, (B,C) fat-suppressed T2-weighted sagittal, (D) coronal and (E) axial fat-suppressed T2-weighted images demonstrate separation of the entire chondral coat from the subchondral bone (arrows) over a large area of the lateral femoral condyle, as well as a smaller area of separation seen more anteriorly (arrowheads in C and D), which may be contiguous with the larger area. There is irregularity of the underlying subchondral bone plate in these regions. In this case, due to the presence of multiple regions of bone necrosis that undermine the integrity of the bone-cartilage interface, the delamination occurs not at the tidemark, but deep to it, and portions of the subchondral bone plate may have separated along with the cartilage. This type of phenomenon has been described in cases of osteonecrosis, as the fractures that develop in the necrotic bone, leading to the well-known crescent sign, may be located in the subchondral bone or subchondral bone plate itself and then extend into the adjacent articular cartilage, producing an appearance similar to that of classic chondral delamination.
As classically described, cartilage delamination is considered a surgical lesion. If it is not appropriately recognized and treated, such delamination can result in significant morbidity. The process occurs most commonly in the young adult population and, without proper treatment, can lead to early-onset degenerative changes.13 Surgical options for treatment of chondral delamination include microfracture or bone marrow stimulation, osteochondral autograft or allograft transplantation, autologous chondrocyte implantation, particulated juvenile cartilage allograft transplantation, and cell-based and scaffold treatments.18,19 When the articular surface is intact, chondral delamination is effectively managed with bioabsorbable pin fixation to avoid propagation to a full-thickness chondral lesion.20
Delamination is a frequent complication after surgical repair of cartilage (Figure 15), and it occurs more commonly with autologous chondrocyte implantation.21 In delamination of surgically repaired cartilage, there is failure of the repair tissue to integrate with the subchondral bone, resulting in separation of the repaired cartilage from the underlying subchondral bone. The delaminated repair tissue may remain in situ or be displaced into the joint space. Delamination of the repaired cartilage often requires surgical revision.14
Figure 15:
(A) Osteochondritis dissecans of the medial femoral condyle with two unstable osteochondral fragments (thin arrows) in a 25 year-old man, as shown in a sagittal fluid-sensitive fat-suppressed MR image. The patient subsequently underwent OATS procedure with allograft. On postoperative imaging obtained 3 months after surgery, (B,C) fluid-sensitive fat-suppressed sagittal and (D) axial MR images demonstrate an area of chondral delamination (arrowheads) occurring immediately adjacent to the osteochondral allograft (block arrows). (E) On follow-up MRI obtained 8 months later, a displaced chondral body arising from the site of prior delamination is seen within a large joint effusion (short arrow), displayed in an axial fat-suppressed image.
Tendons
Structurally, tendons are composed of distinct fascicular subunits that contain bundles of collagen fibrils and constituent cells, the collagen bundles generally oriented along the long axis of the tendon (Figure 16).22 The cellular connective tissue lies between and separates adjacent collagen bundles. When tensile force is applied along the longitudinal axis of the tendon, the individual fascicles elongate to different degrees, leading to interfascicular movement (Figure 16). Histologic analysis has suggested that the lubricant protein lubricin facilitates such interfascicular sliding motion during loading. A deficit of this protein may contribute to tendon wear.23 One common pattern of tendon wear is designated a delaminating tear, which is defined as a separation oriented along the long axis of the tendon and located predominantly between and not through the collagen fibers. Thus, a purely delaminated tear is a collagen sparing tear of the tendon. The direction of delamination may be vertical, horizontal, or oblique, and the tear may be full-thickness or partial-thickness. Therefore, a delaminated tendon tear may violate one or more surfaces of the tendon or lie completely within its substance. Full-thickness delaminating tears are designated split tears (Figure 17), and these are most commonly encountered in the peroneus brevis tendon at the level of the ankle (Figure 18) and the biceps tendon at the level of the glenohumeral joint (Figure 19). A review of the available literature confirms that delaminated tendon tears have been studied predominantly with regard to the rotator cuff. Immunohistologic analysis of delaminated rotator cuff tendons has shown that delamination predominantly occurs between layers of the tendon with differing collagen fiber orientation, although delamination may also occur between collagen fibers of parallel orientation within the same layer of a tendon.24
Figure 16:
Graphical depiction of the structural morphology of tendons. On the left, the collagen fibers are shown in dark blue-green, the collagen bundles in light blue, and the tendon itself in red. Note that the collagen bundles are oriented along the longitudinal axis of the tendon. On the right, the double-headed arrows indicate that tensile forces result in differing degrees of collagen elongation, leading to interfascicular movement, which without lubricin would lead to failure in the connective tissue (pink layer) between the collagen bundles, resulting in tendon delamination.
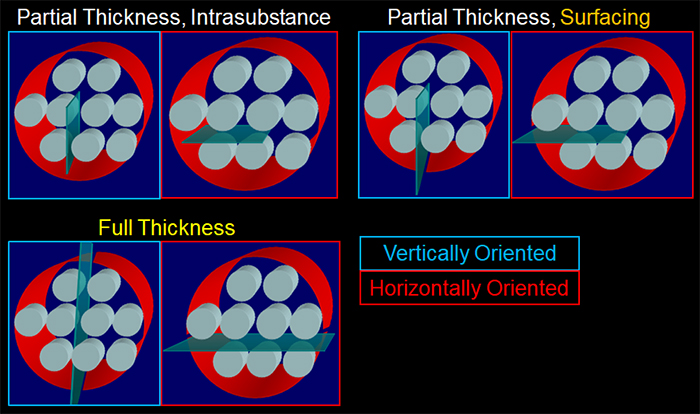
Figure 17:
Graphical depiction of potential types of delaminating tears. Note that although these tears extend between and not through collagen bundles, they may be oriented in any direction (i.e., horizontal, vertical, oblique) and they may violate one or both surfaces of the tendon or lie entirely within the tendon substance. In these drawings, the collagen bundles are displayed in light blue, the tendon in red, and the delaminated tear in dark blue-green.
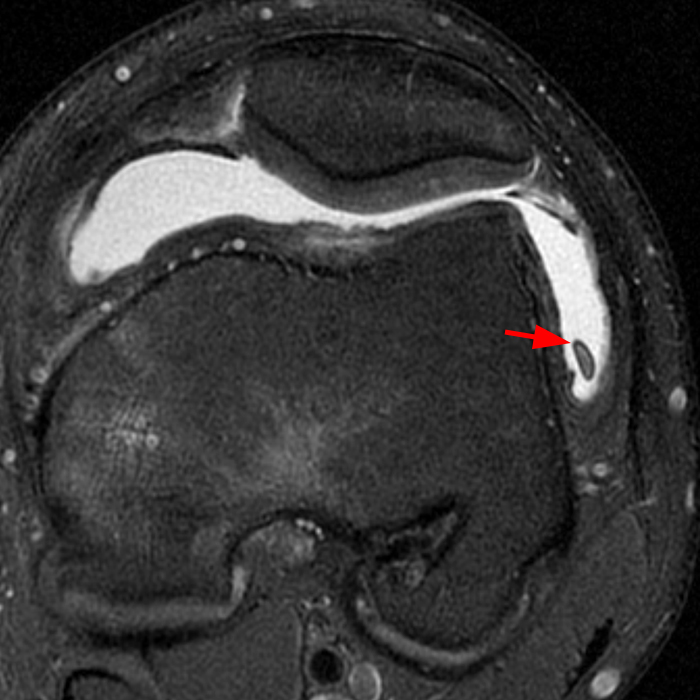
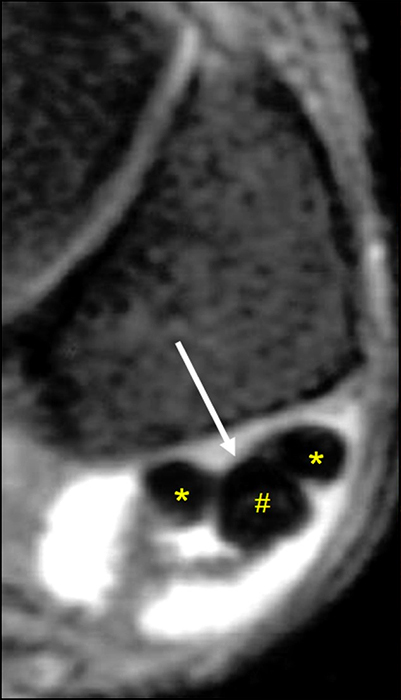
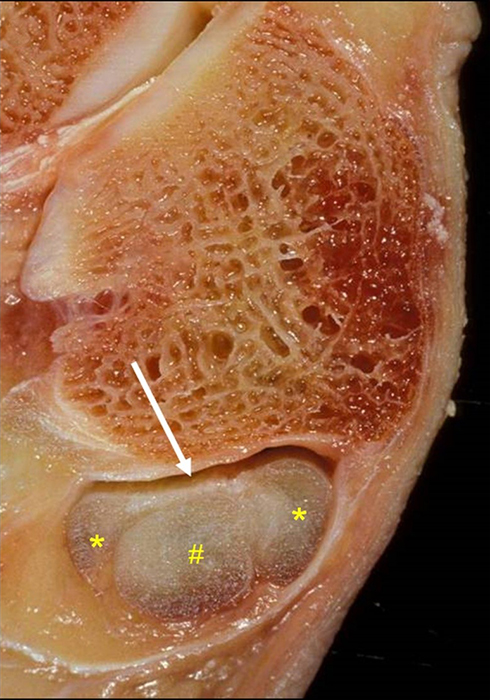
Figure 18:
Longitudinal split tear (arrow) of the peroneus brevis tendon (*) at the level of the distal fibula as displayed on (A) an axial T2-weighted fat-suppressed MR image and (B) corresponding transverse section of a cadaveric specimen, producing a C-shaped appearance of the peroneus brevis tendon draping around the peroneus longus tendon (#).
On MRI, the appearance of tendon delamination is varied and related in part to whether the tear is full-thickness or partial-thickness. With regard to the rotator cuff, tendon delamination is suggested by the presence of an intrasubstance longitudinal fluid cleft separating articular and bursal fibers. In the presence of a full-thickness tear, delamination is also confirmed by differential retraction of the torn tendon fibers (Figure 20). With a partial-thickness intrasubstance delaminated tear, the plane of cleavage may be concealed at the time of arthroscopy (Figure 21). Alternatively, if the partial-thickness delaminated tear extends to the articular surface (Figure 22) or bursal surface, it can be detected by arthroscopy or bursoscopy, respectively. Delamination may also result in cysts at or adjacent to the myotendinous junction or within the muscle belly itself (Figure 23), the cysts being referred to as “sentinel cysts”.25 Sentinel cysts may occur with either full-thickness or partial-thickness delaminated tears, in relatively equal proportions.26
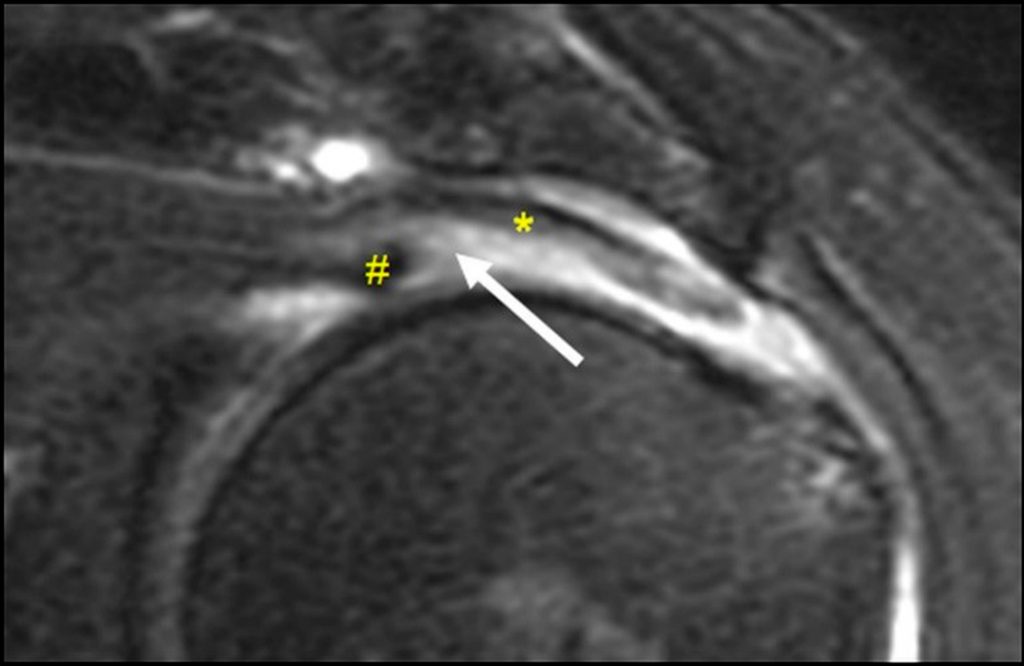
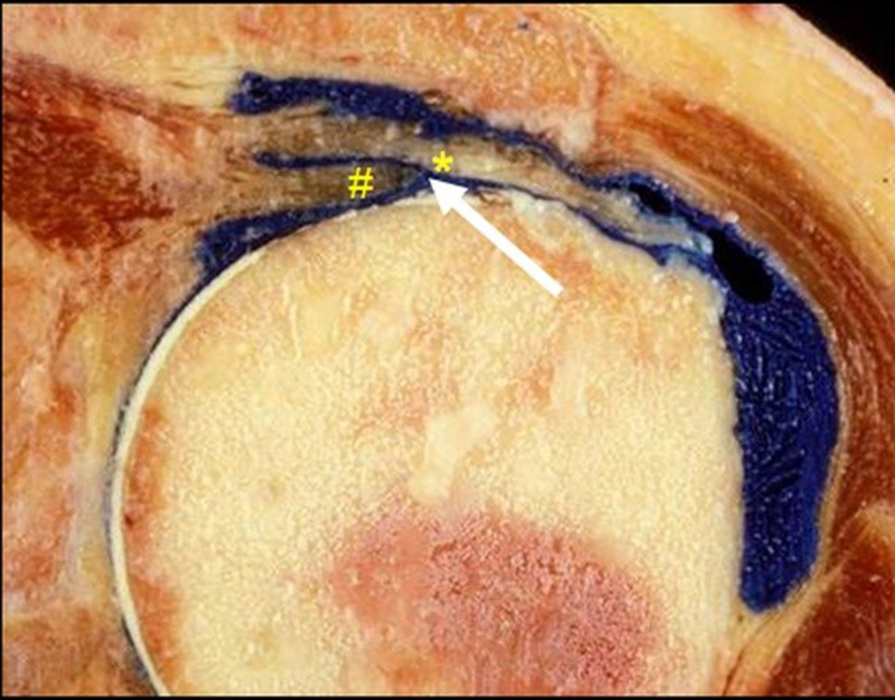
Figure 20:
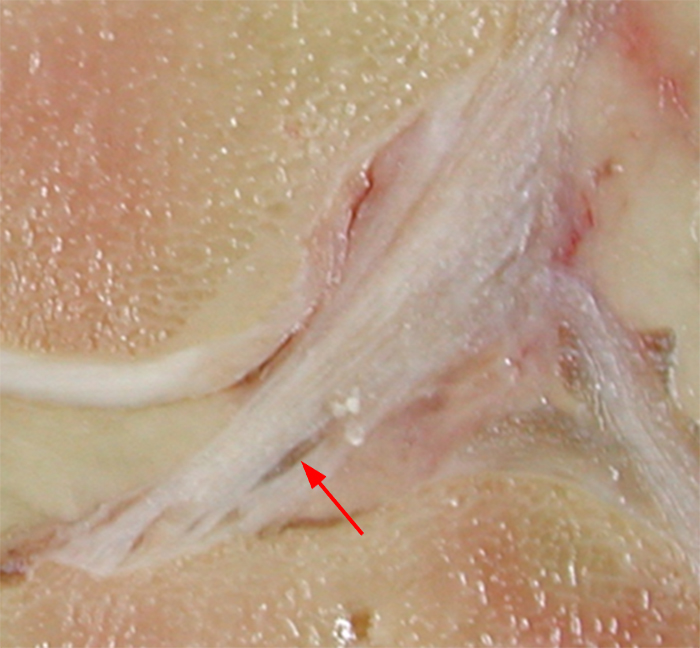
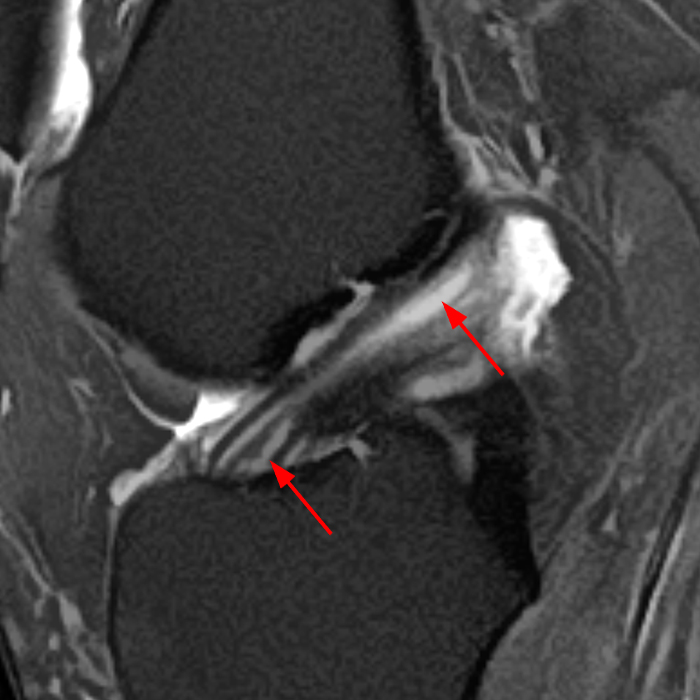
Full-thickness delaminating supraspinatus tendon tear, as evidenced by a longitudinal fluid cleft (arrows) separating articular (#) and bursal (*) sided tendon fibers, as displayed in (A) a coronal T2-weighted fat-suppressed MR image and in (B) a coronal section of a cadaveric shoulder following the injection of blue latex into the glenohumeral joint. As is usually the case, note that the articular-sided, or deep, layer of the torn tendon is retracted more medially than the bursal-sided, or superficial, layer.
Figure 21:
Diagram and (B) coronal T2-weighted MR image demonstrating a partial thickness intrasubstance tear (arrows) at the footprint of the supraspinatus tendon that does not extend to the articular or bursal tendon surface, likely to be concealed at the time of arthroscopy and bursoscopy. This appearance has been designated concealed interstitial delamination, or CID.
Figure 23:
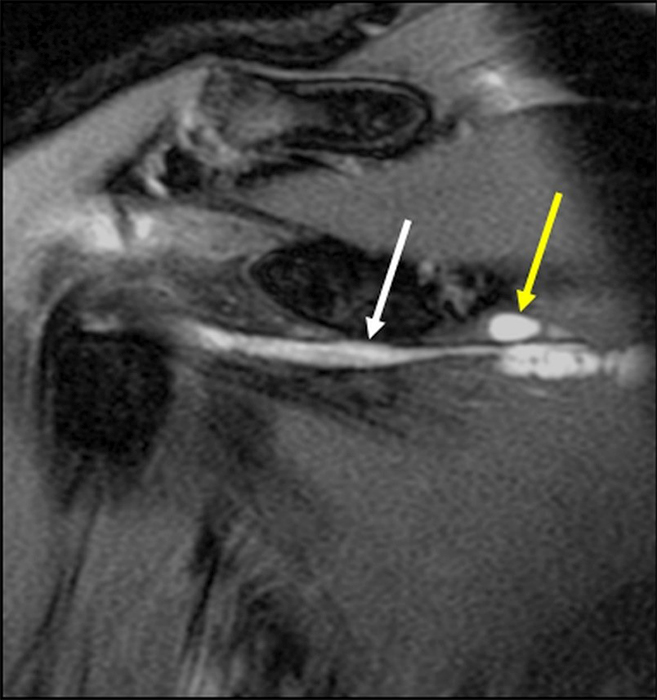
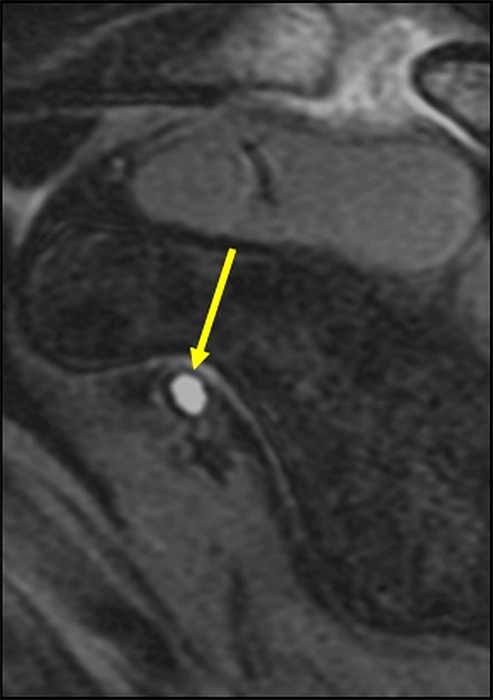
(A) Coronal T2-weighted fat-suppressed MR image and (B) sagittal T2-weighted fat-suppressed MR image demonstrating an intrasubstance delaminating tear of the subscapularis tendon (white arrow) extending medially in a linear fashion, terminating as “sentinel” cysts at the myotendinous junction (yellow arrows).
With full-thickness tears, delamination results in separation of the tendon into superficial and deep layers. The characteristic pattern of delaminated rotator cuff tendons is that the articular-sided (deep) layer is retracted more than the bursal-sided (superficial) layer (see Figure 20).27 Arthroscopic studies have demonstrated that the predominant direction of retraction of delaminated tears that involve both the supraspinatus and infraspinatus tendons is posteromedial if the superficial layer of tearing contains a larger amount of infraspinatus tendon than supraspinatus tendon, and is anteromedially directed if the superficial layer of tearing contains a larger amount of the supraspinatus tendon.28 Furthermore, the articular-sided (deep) layer of the delaminated tendon is more frequently thicker than the bursal-sided (superficial) layer, owing to muscle atrophy that is more often associated with the superficial layer.29
The concept of delamination is also relevant in the discussion of so-called novel lesions of the infraspinatus tendon, which in general are regarded as a characteristic pattern of edema within the infraspinatus tendon anywhere from the distal tendon to the myotendinous junction.30 These lesions are associated with persistent tendon abnormalities on follow-up imaging, with or without muscle atrophy. Cadaveric studies of the infraspinatus muscle architecture have delineated two muscle bellies, a transverse portion and an oblique portion.31 The oblique portion contains a long and thick tendon that attaches to the greater tuberosity, and the transverse portion contains a thin and short tendon that attaches to the tendon of the oblique head (Figure 24).
Figure 24:
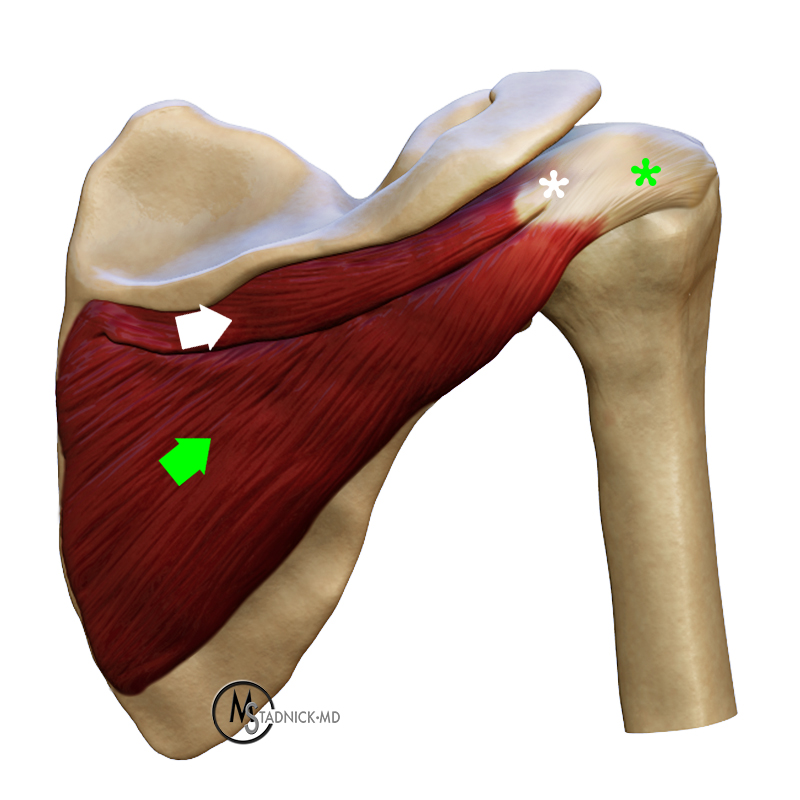
Diagram demonstrating the two muscle bellies of the infraspinatus, a deeper oblique portion (green arrow) that contains a long and thick tendon that attaches to the greater tuberosity (green asterisk), and a superficial transverse portion (white arrow) that contains a thin and short tendon that attaches to the oblique head tendon (white asterisk).
Retrospective analysis of MRI studies demonstrating novel lesions has postulated that these novel lesions reflect a delaminating infraspinatus tendon injury with differential retraction of the transverse and oblique components (Figure 25).32 However, a review of the current literature demonstrates a lack of consensus on the precise location of this injury with regard to whether failure occurs at the myotendinous junction or distal tendon with tendon delamination. These lesions may be occult on arthroscopy when the deep oblique tendon fibers are intact, as well as on bursoscopy when the superficial transverse tendon fibers are intact.
Figure 25:
(A) Coronal and (B) axial T2-weighted fat-suppressed MR images demonstrate a novel lesion of the infraspinatus tendon (white arrows), characterized by edema along the myotendinous junction as well as a partial thickness tear of the infraspinatus tendon with retraction of the involved upper transverse tendon fibers, reflecting tendon delamination.
Delaminated rotator cuff tears have been associated with impaired tendon healing following repair as compared to non-delaminated tears.33,34,35 However, the presence of delamination may be a confounding rather than an independent risk factor for the failure of cuff healing36 as some studies have shown similar clinical outcomes between repairs of delaminated and non-delaminated tears.35-36 Regardless, the identification of tendon delamination remains important whether it is accomplished by a radiologist at the time of interpretation of the MRI study or by an orthopaedic surgeon during arthroscopy as its presence may influence the surgical technique. Some delaminating tears have demonstrated a synovial lining, suggesting that curetting should be performed prior to suture repair to facilitate healing.24 Additionally, in the setting of delamination, some surgeons preferentially utilize mini-open rather than fully arthroscopic techniques37 or would perform a double layered repair of the superficial and deep tendon layers rather than a single row repair.28-29
Ligaments
Ligaments connect bone to bone, demonstrating a collagen architecture that is similar to that of tendons, with most of the collagen bundles oriented along the long axis of the ligament, in the general direction of the tensile forces applied to the ligament. The main differences in composition are a higher proteoglycan and water content and lower collagen content in ligaments relative to tendons. Additionally, the collagen structure in ligaments tends to be slightly less uniform, with more of a weaving pattern of the collagen bundles.38
At rest, ligaments demonstrate crimp, or slight laxity. Failure of ligaments can occur as complete tears or partial tears. These tears may be non-delaminated or delaminated, the latter leading to separation of adjacent collagen bundles. As one example, delamination of collagen fibers in ligaments forms the basis for what has been designated mucinous (cystic) degeneration (Figure 26). Although this process has been emphasized in the anterior cruciate ligament, occurring with increased frequency with advancing age, mucinous degeneration occurs in other ligaments as well, including the posterior cruciate ligament. Mucoid degeneration of the posterior cruciate ligament commonly coexists with mucoid degeneration of the anterior cruciate ligament.39 Histologically, mucoid degeneration reflects degradation of collagen and deposition of glycosaminoglycans between the collagen bundles, thereby reflecting a form of delamination between the collagen bundles, followed by progressive loss of collagen fiber structure and bundle integrity.40,41 While distorted, these collagen fibers remain uninterrupted and, therefore, mucoid degeneration does not truly represent a tear, although it may be misinterpreted as such when viewed with MRI.42
Typically, with MRI, mucinous degeneration of the anterior cruciate ligament (Figures 27-31) is characterized by thickening and increased intraligamentous signal, with intact fibers, often demonstrating a “celery stalk” appearance. Mucinous degeneration of the posterior cruciate ligament may manifest as the so-called “tram-track” appearance, with diffuse thickening and longitudinally increased signal intensity in the ligament and a peripheral rim of hypointense intact fibers (Figures 30 and 32).39 Paracruciate or intraosseous ganglion cysts, or both, are associated with mucinous degeneration of either cruciate ligament.42
Although mucinous degeneration is often regarded as a phenomenon of middle-aged and elderly persons, the MRI appearance of linear regions of altered signal and even enlargement of a ligament, especially in the anterior cruciate ligament, can be seen in children and young adults. Anecdotally, we have noticed this phenomenon in young athletes (Figure 29), especially soccer players, runners, and American football players, related to repetitive stress owing to vigorous activity rather than a single episode of trauma.
Figure 29:
28 year-old professional rugby player with mucoid delamination (arrow) of the anterior cruciate ligament, demonstrated on this sagittal T2-weighted fat-suppressed MR image. In this young athletic person, the process of delamination is more likely related to stress-induced alterations between the collagen fibers within the ligament, rather than ligament degeneration as is typically described in older persons.
Indeed, there are several theories regarding the pathogenesis of mucoid degeneration, including: (a) a theory of tissue degeneration that proposes an important causative role of aging; (b) a theory emphasizing injury, which highlights the fact that fibroblasts in the anterior cruciate ligament secrete glycosaminoglycans in the setting of trauma and, in response to joint and tissue motion, the deposited mucin substance dissects between the ligament fibers and causes fusiform dilatation of the ligament; and (c) a theory of “multiple microtrauma”, which states that multiple insignificant injuries result in formation of microcysts that merge into larger mucoid formations, probably as a result of injury to the protective synovium overlying the anterior cruciate ligament. The anatomy of the intercondylar notch may be a contributing factor, as a smaller and more vertically-oriented notch may predispose to ligamentous impingement and resultant microtrauma.43
Whether related to degeneration or repetitive stress, mucoid degeneration is associated with a stable ligament on physical examination. Mucoid degeneration has a predilection for the posterolateral bundle of the anterior cruciate ligament, and it may cause pain on terminal extension related to mechanical impingement of the hypertrophied ligament on the roof and lateral wall of the intercondylar notch.44 Mucoid degeneration of the anterior cruciate ligament is also associated with posterior knee pain and limited flexion. Some of the affected patients may be treated by partial or complete arthroscopic resection of the abnormal ligament, with resultant resolution of symptoms.45 At arthroscopy, there is a hypertrophic ligament with yellowish mucoid material along the length of its fibers; however, mucoid degeneration of the anterior cruciate ligament is frequently undetectable at arthroscopy using the standard anterior portal approach.42
Figure 31:
Sagittal T2-weighted fat-suppressed MR image showing thickening and increased signal of the anterior cruciate ligament compatible with mucoid degeneration, with an associated intraligamentous cyst (arrow). This was misinterpreted as a high-grade partial tear of the anterior cruciate ligament at the time of imaging, although there had not been a recent injury and the ligament was stable on physical examination.
Figure 32:
52 year-old man with severe knee pain demonstrating increased intrasubstance signal in the posterior cruciate ligament with a “tram-track” appearance (arrows) suggestive of mucoid degeneration, as shown in a T2-weighted sagittal MR image. The patient did not have instability of the ligament on physical examination.
Similar to tendons, partial tears of ligaments can occur, and sometimes such tears demonstrate delaminating components on MRI, with the delaminating component propagating parallel to the direction of the collagen fibers. Delaminating tears, or split tears, of the posterior cruciate ligament (Figures 33-35) have been documented in the literature, manifesting as increased linear signal intensity within the ligament. Although intrasubstance delamination of the posterior cruciate ligament has been associated with functional impairment or insufficiency in the majority of cases in one report, the true significance of this finding awaits further clarification through additional investigations.46
Figure 33:
40 year-old man with a delaminated partial tear (arrows) of the posterior cruciate ligament and surrounding soft tissue edema, as shown on this sagittal T2-weighted fat- suppressed MR image. Discontinuity of some of the ligament fibers is noted (arrowhead). The patient had laxity on a posterior drawer test.
Figure 34:
33 year-old man status post fall, with (A,B) sagittal and (C) axial T2-weighted fat- suppressed MR images demonstrating a partial tear of the posterior cruciate ligament (arrowhead) with a delaminating component (arrows). There is diffuse thickening of the ligament. The patient had instability on a posterior drawer test.
Figure 35:
24 year-old professional rugby player with an acute partial tear of the posterior cruciate ligament with interstitial delamination (arrows), as shown in (A,B) sagittal T2-weighted fat-suppressed images and (C,D) proton density-weighted images. The patient had grade 2 instability on posterior drawer testing.
Menisci
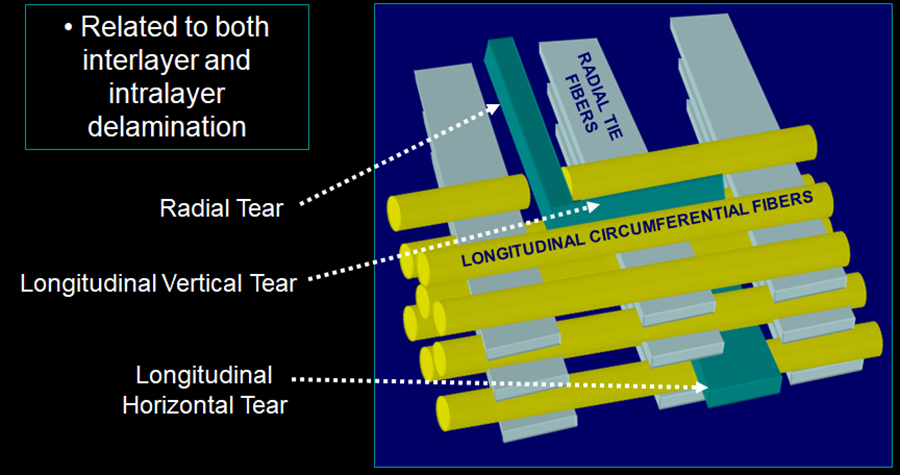
The menisci of the knee are crescent-shaped fibrocartilaginous structures, composed of approximately 70% water and 20% collagen interposed with fibrochondrocyte cells.47 The remaining dry weight is composed of proteoglycans, non-collagenous proteins, and glycoproteins. The interaction of water with the matrix framework influences the viscoelastic properties of the meniscus, and the collagens account for the meniscal tensile strength. Electron microscopic analysis of the collagen framework has revealed three layers (Figure 36).48 The superficial layer (1, Figure 36) is composed of a meshwork of thin fibrils without preferred orientation. The lamellar layer (2, Figure 36) is deep to the superficial layer and demonstrates radially oriented fibers peripherally and variably oriented fibers more internally. In simple terms, the collagen fibers, or bundles, in the central layer of the meniscus (3, Figure 36) are divided into two types based on their predominant orientation. The first of these are often designated longitudinal, or circumferential, collagen bundles. These bundles are found mainly in the outer two-thirds of the meniscus and extend in a circumferential pattern, connecting the anterior horn, midportion, and posterior horn of the meniscus. The second type are designated the radial tie fibers (blue, Figure 36), extending in from the periphery toward the apex of the meniscus, connecting the peripheral and central portions of the meniscus to provide structural integrity. The menisci serve important roles in load transmission, shock absorption, and stability.47 The longitudinal fibers of the central layer translate compressive loads into circumferential hoop stresses, and the anterior and posterior insertional, or root, ligaments of the menisci prevent peripheral meniscal extrusion during loading.
Figure 36:
Graphic representation of the collagen framework of the meniscus, composed of superficial (1), lamellar (2), and deep (3) layers. The deep layer contains longitudinally oriented collagen bundles (yellow) along the circumferential axis of the meniscus, as well as radial tie fibers (blue) extending from the periphery towards the inner apex.
There is no uniformly accepted classification system for meniscal tears. One system, introduced by the International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine (ISAKOS), classifies meniscal tears based on seven factors: tear depth; rim width; radial location; central to the popliteal hiatus; tear pattern; quality of tissue; and length of tear.49 With regard to tear pattern, longitudinal, horizontal, radial, and flap tears are the categories that are used. For our discussion of meniscal delamination, it is useful to look at three of these tear patterns: longitudinal tears, horizontal tears; and radial tears. Identification of these tear patterns aids in management as longitudinal vertical tears are more likely to heal when compared to longitudinal horizontal or radial tears.50
Longitudinal (circumferential) vertical tears, frequently simply referred to as longitudinal or vertical tears, (Figure 37) are generally related to axial loading and are found in the outer half or two-thirds of the meniscus. They extend for a variable distance from a more anterior position to a more posterior position, and they often do so along the path of least resistance, parallel to the long axis of the longitudinal collagen bundles. Such extension represents one pattern of meniscal delamination. If these tears deviate from this path, becoming oblique in direction, violation of some of these collagen fibers is required, the tear pattern being designated longitudinal (circumferential) vertical oblique in direction. Furthermore, longitudinal vertical tears that extend for a considerable distance in an anteroposterior direction will violate radial tie fibers along their course. Longitudinal (circumferential) horizontal tears (Figure 38), often simply described as horizontal tears or cleavage tears, are generally related to shear forces. These tears generally begin at or near the inner apex of the meniscus and propagate in a peripheral direction, sometimes violating the outer surface of the meniscus and accompanied by parameniscal cysts. These tears often extend along the path of least resistance, between and not through the longitudinal (circumferential) collagen fibers, representing a second pattern of meniscal delamination. If these tears have a large anteroposterior component, they too will violate the radial tie fibers. Radial meniscal tears (Figure 39) also begin in the inner margin of the meniscus. Their path of least resistance is parallel to and not through the radial tie fibers, as they extend to the periphery of the meniscus, a pathway that represents a third pattern of delamination. Radial tears that extend into the outer half of the meniscus will violate some of the longitudinal (circumferential) collagen fibers. Further, those radial tears that are obliquely oriented, so-called parrot beak tears, will violate some of the radial tie fibers. Of note, one can use this same rationale to illustrate that some multidirectional meniscal tears are associated with interlayer and intralayer delamination (Figure 40).
Figure 37:
Diagrams and sagittal T2-weighted MR image demonstrate a longitudinal vertical tear (arrows) involving the outer third of the posterior horn of the medial meniscus, extending parallel to the long axis of the longitudinal collagen bundles. The radial tie collagen fibers are shown in blue, and the longitudinal collagen bundles are shown in yellow.
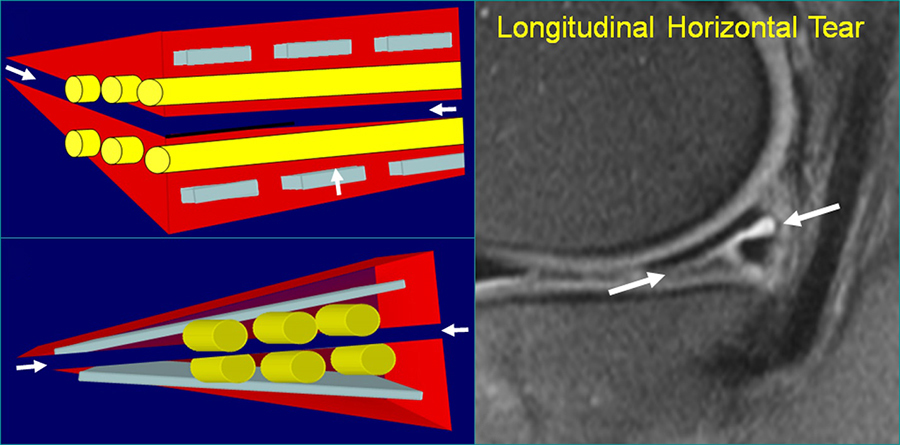
Figure 38:
Diagrams and sagittal T2-weighted fat-suppressed MR image demonstrate a longitudinal horizontal tear (arrows) involving the posterior horn of the medial meniscus, extending from the inner apex to the periphery between the longitudinal collagen bundles (shown in yellow). Note that such horizontal tears may branch peripherally to extend about the many longitudinal collagen bundles.
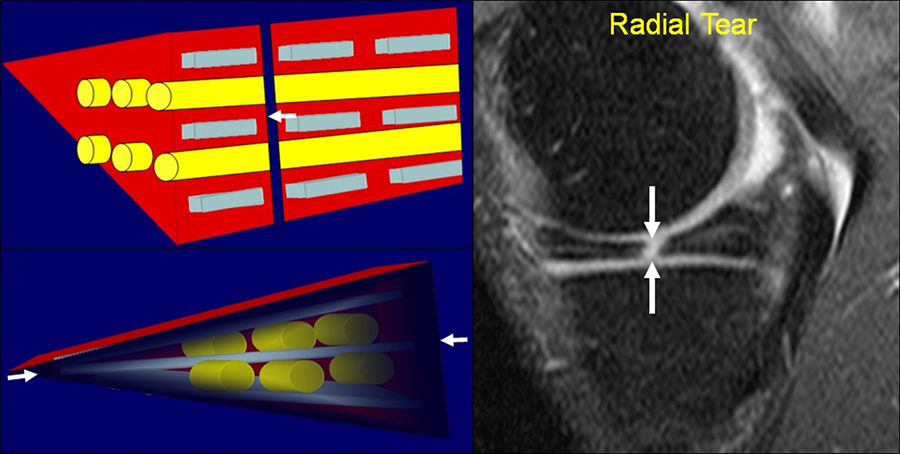
Figure 39:
Diagrams and sagittal T2-weighted fat-suppressed MR image demonstrate a radial tear (arrows) involving the body of the medial meniscus, extending from the inner apex towards the periphery and parallel to the radial tie fibers. At the periphery, the meniscal tear disrupts the normal “bow tie” appearance of the meniscus.
Figure 40:
Multidirectional meniscal tears. The delaminated portions of radial tears, longitudinal vertical tears, and longitudinal horizontal tears are shown. The radial tie collagen fibers are shown in blue, and the longitudinal collagen bundles are shown in yellow. A multidirectional meniscal tear is shown in green. Note that a multidirectional tear may reveal segments of interlayer and intralayer delamination.
Conclusion
Delamination is a mode of failure in which a material separates into layers, and it is a process that is commonly seen in human tissues including articular cartilage, tendons, ligaments, and menisci. Knowledge of the collagen architecture of these tissues is important for understanding how delamination occurs. Delamination of cartilage and tendons is well-described in the literature, and both are of significance to the orthopaedic surgeon. In particular, chondral delamination occurring at the tidemark is a surgical lesion. As delamination of the deeper zone of articular cartilage may be concealed at the time of arthroscopy, recognition of this pattern of failure becomes an important diagnostic exercise for the radiologist. Tendon delamination alters surgical management, particularly when it occurs in the rotator cuff tendons. A similar process of tissue delamination may occur in ligaments and menisci, a process that has received little or no attention in the literature.
References
- Alford JW, Cole BJ. Cartilage restoration, part 1: basic science, historical perspective, patient evaluation, and treatment options. The American journal of sports medicine. 2005;Feb;33(2):295-306. ↩
- Hughes LC, Archer CW, Ap Gwynn I. The ultrastructure of mouse articular cartilage: collagen orientation and implications for tissue functionality. A polarised light and scanning electron microscope study and review. Eur Cell Mater. 2005 Jan;9(68):e84. ↩
- Eyre D. Articular cartilage and changes in arthritis: collagen of articular cartilage. Arthritis Research & Therapy. 2001;Oct;4(1):1-6. ↩
- Teshima R, Otsuka T, Takasu N, Yamagata N, Yamamoto K. Structure of the most superficial layer of articular cartilage. The Journal of bone and joint surgery British. 1995 May;77(3):460-4. ↩
- Yao X, Wang Y, Ravanfar M, Pfeiffer FM, Duan D, Yao G. Nondestructive imaging of fiber structure in articular cartilage using optical polarization tractography. Journal of biomedical optics. 2016;(v;21(11):116004). ↩
- Bloebaum RD, Wilson AS, Martin WN. A Review of the Collagen Orientation in the Articular Cartilage. Cartilage. Published online 2021. ↩
- Fawns HT, Landells JW. Histochemical studies of rheumatic conditions. I. Observations on the fine structures of the matrix of normal bone and cartilage. Ann Rheum Dis. 1953;12:105–113. ↩
- Kendell SD, Helms CA, Rampton JW, Garrett WE, Higgins LD. MRI appearance of chondral delamination injuries of the knee. American Journal of Roentgenology. 2005;May;184(5):1486-9. ↩
- Pathria MN, Chung CB, Resnick DL. Acute and stress-related injuries of bone and cartilage: pertinent anatomy, basic biomechanics, and imaging perspective. Radiology. 2016 Jul;280(1):21-38. ↩
- Buckley MR, Gleghorn JP, Bonassar LJ, Cohen I. Mapping the depth dependence of shear properties in articular cartilage. Journal of biomechanics. 2008;7;41(11):2430-7. ↩
- Mosher TJ. Chapter 2: Functional anatomy and structure of the “osteochondral unit”. Arthritis in color: advanced imaging of arthritis. Philadelphia: Elsevier Saunders. 2009:23-32. ↩
- Levy AS, Lohnes J, Sculley S, LeCroy M, Garrett W. Chondral delamination of the knee in soccer players. Am J Sports Med. 1996;24:634–639. ↩
- White CL, Chauvin NA, Waryasz GR, March BT, Francavilla ML. MRI of native knee cartilage delamination injuries. American Journal of Roentgenology. 2017;(v;209(5):W317-21). ↩
- Brittberg M, Winalski CS. Evaluation of cartilage injuries and repair. J Bone Joint Surg Am. 2003:58–69. ↩
- Lewis JL, Johnson SL. Collagen architecture and failure processes in bovine patellar cartilage. Journal of anatomy. 2001;Oct;199(4):483-92. ↩
- Broom ND, Ngo T, Tham E. Traversing the intact/fibrillated joint surface: a biomechanical interpretation. Journal of anatomy. 2005;Jan;206(1):55-67. ↩
- Mansfield JC, Mandalia V, Toms A, Winlove CP, Brasselet S. Collagen reorganization in cartilage under strain probed by polarization sensitive second harmonic generation microscopy. Journal of the Royal Society Interface. 2019;31;16(150):20180611. ↩
- Bedi A, Feeley BT, Williams RJ. Management of articular cartilage defects of the knee. J Bone Joint Surg Am. 2010;92:994–1009. ↩
- Yanke AB, Tilton AK, Wetters NG, Merkow DB, Cole BJ. DeNovo NT particulated juvenile cartilage implant. Sports Med Arthrosc. 2015;23:125–129. ↩
- Theodorides AA, Williams A, Guthrie H, Church S. Diagnosis and management of chondral delamination injuries of the knee. The Knee. 2019;1;26(3):647-52. ↩
- Chalmers PN, Vigneswaran H, Harris JD, Cole BJ. Activity-related outcomes of articular cartilage surgery: a systematic review. Cartilage. 2013 Jul;4(3):193-203. ↩
- Clark JOHN, Sidles JOHNA, Matsen FA. The relationship of the glenohumeral joint capsule to the rotator cuff. Clinical orthopaedics and related research. 1990;254:29–34. ↩
- Funakoshi T, Schmid T, Hsu HP, Spector M. Lubricin distribution in the goat infraspinatus tendon: a basis for interfascicular lubrication. JBJS. 2008;1;90(4):803-14. ↩
- Sonnabend DH. Laminated tears of the human rotator cuff: a histologic and immunochemical study. ” Journal of shoulder and elbow surgery. 2001;10.2:109–115. ↩
- Opsha O, Malik A, Baltazar R, et al. MRI of the rotator cuff and internal derangement. European journal of radiology. 2008;1;68(1):36-56. ↩
- Manvar AM, Kamireddi A, Bhalani SM, Major NM. Clinical significance of intramuscular cysts in the rotator cuff and their relationship to full-and partial-thickness rotator cuff tears. American Journal of Roentgenology. 2009;192(3):719-724. ↩
- Bierry G, Palmer WE. Patterns of tendon retraction in full-thickness rotator cuff tear: comparison of delaminated and nondelaminated tendons. ” Skeletal radiology. 2019;48. 1:109–117. ↩
- Cha SW, Lee CK, Sugaya H, Kim T, Lee SC. Retraction pattern of delaminated rotator cuff tears: dual-layer rotator cuff repair. Journal of orthopaedic surgery and research. 2016;Dec;11(1):1-10. ↩
- Tanaka M, Nimura A, Takahashi N, et al. Location and thickness of delaminated rotator cuff tears: cross-sectional analysis with surgery record review. JSES Open Access. 2018;1;2(1):84-90. ↩
- Lunn JV, Castellanos-Rosas J, Tavernier T, Barthélémy R, Walch G. A novel lesion of the infraspinatus characterized by musculotendinous disruption, edema, and late fatty infiltration. Journal of shoulder and elbow surgery. 2008;1;17(4):546-53. ↩
- Kato A, Nimura A, Yamaguchi K, Mochizuki T, Sugaya H, Akita K. An anatomical study of the transverse part of the infraspinatus muscle that is closely related with the supraspinatus muscle. Surgical and radiologic anatomy. 2012;Apr;34(3):257-65. ↩
- Huang BK, Chang EY. Delaminating infraspinatus tendon tears with differential retraction: imaging features and surgical relevance. ” Skeletal radiology. 2017;46. 1:41–50. ↩
- Boileau P, Andreani O, Schramm M, Baba M, Barret H, Chelli M. The effect of tendon delamination on rotator cuff healing. The American journal of sports medicine. 2019;Apr;47(5):1074-81. ↩
- Flurin PH, Landreau P, Gregory T, et al. Cuff integrity after arthroscopic rotator cuff repair: correlation with clinical results in 576 cases. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2007;1;23(4):340-6. ↩
- Kim CW, Kim JH, Gwak HC, Park JH. The comparison of outcomes between delaminated and nondelaminated rotator cuff tear repair: is delamination a negative prognostic factor? Journal of Shoulder and Elbow Surgery. 2017;1;26(2):216-24. ↩
- Kwon J, Lee YH, Kim SH, Ko JH, Park BK, Oh JH. Delamination does not affect outcomes after arthroscopic rotator cuff repair as compared with nondelaminated rotator cuff tears: a study of 1043 consecutive cases. The American journal of sports medicine. 2019;Mar;47(3):674-81. ↩
- MacDougal GA, Todhunter CR. Delamination tearing of the rotator cuff: prospective analysis of the influence of delamination tearing on the outcome of arthroscopically assisted mini open rotator cuff repair. ” Journal of shoulder and elbow surgery. 2010;19. 7:1063–1069. ↩
- Nordin M, Frankel VH, eds. Basic Biomechanics of the Musculoskeletal System. Lippincott Williams & Wilkins; 2001: 102-125. ↩
- McMonagle JS, Helms CA, Garrett Jr WE, Vinson EN. Tram-track appearance of the posterior cruciate ligament (PCL): correlations with mucoid degeneration, ligamentous stability, and differentiation from PCL tears. American Journal of Roentgenology. 2013 Aug;201(2):394-9. ↩
- Nelissen RG, Hogendoorn PC. Retain or sacrifice the posterior cruciate ligament in total knee arthroplasty? A histopathological study of the cruciate ligament in osteoarthritic and rheumatoid disease. Journal of clinical pathology. 2001;1;54(5):381-4. ↩
- Hasegawa A, Otsuki S, Pauli C, et al. Anterior cruciate ligament changes in the human knee joint in aging and osteoarthritis. Arthritis & Rheumatism. 2012 Mar;64(3):696-704. ↩
- Bergin D, Morrison WB, Carrino JA, Nallamshetty SN, Bartolozzi AR. Anterior cruciate ligament ganglia and mucoid degeneration: coexistence and clinical correlation. American Journal of Roentgenology. 2004;May;182(5):1283-7. ↩
- Pandey V, Suman CP, Sharma S, Rao SP, Acharya KK, Sambaji C. Mucoid degeneration of the anterior cruciate ligament: Management and outcome. Indian journal of orthopaedics. 2014 Apr;48:197-202. ↩
- Kim TH, Lee DH, Lee SH, Kim JM, Kim CW, Bin SI. Arthroscopic treatment of mucoid hypertrophy of the anterior cruciate ligament. Arthroscopy: The Journal of Arthroscopic & Related Surgery. 2008;1;24(6):642-9. ↩
- Lintz F, Pujol N, Dejour D, Boisrenoult P, Beaufils P. Anterior cruciate ligament mucoid degeneration: selecting the best treatment option. Orthopaedics & Traumatology: Surgery & Research. 2010;1;96(4):400-6. ↩
- Cha JH, Chung HW, Kwon JW, Choi BK, Lee SH, Shin MJ. Longitudinal split of the posterior cruciate ligament: description of a new MR finding and evaluation of its potential clinical significance. Clinical radiology. 2011;1;66(3):269-74. ↩
- Fox AJS, Bedi A, Rodeo SA. The basic science of human knee menisci: structure, composition, and function. ” Sports health. 2012;4. 4:340–351. ↩
- Petersen W, Tillmann B. Collagenous fibril texture of the human knee joint menisci. Anatomy and embryology. 1998;197(4):317–324. ↩
- Anderson AF, Irrgang JJ, Dunn W, Beaufils P, Cohen M, Cole BJ, Coolican M, Ferretti M, Glenn Jr RE, Johnson R, Neyret P. Interobserver reliability of the International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine (ISAKOS) classification of meniscal tears. The American journal of sports medicine. 2011;May;39(5):926-32. ↩
- Woodmass JM, LaPrade RF, Sgaglione NA, Nakamura N, Krych AJ. Meniscal repair: reconsidering indications, techniques, and biologic augmentation. JBJS. 2017;99(14): 1222-1231. ↩