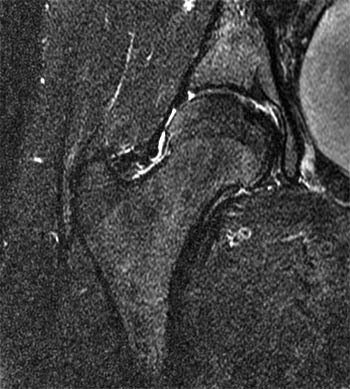
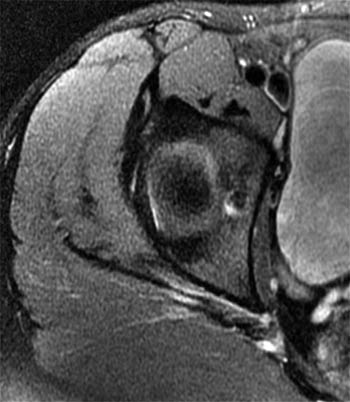
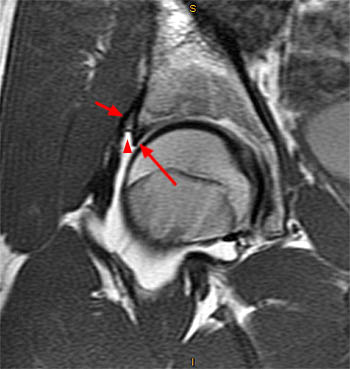
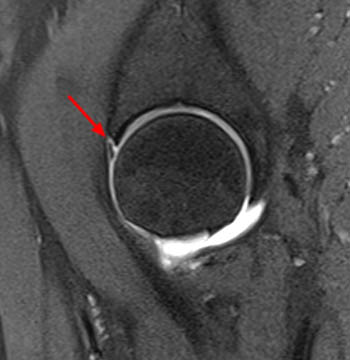
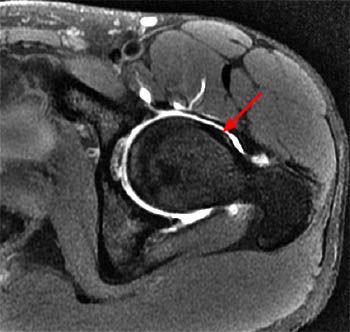
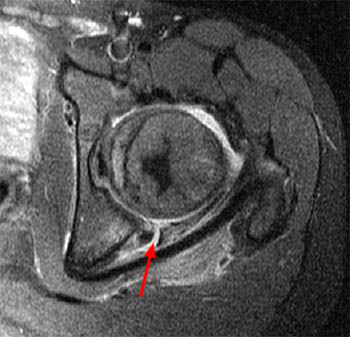
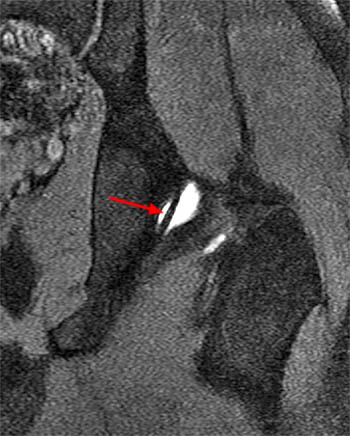
Clinical History: A 15 year-old female runner with a history of pain and possible stress fracture. (1a) Coronal T2-weighted with fat saturation and (1b) Axial proton density-weighted with fat saturation images of the right hip are provided. What are the findings? What is your diagnosis?
Findings
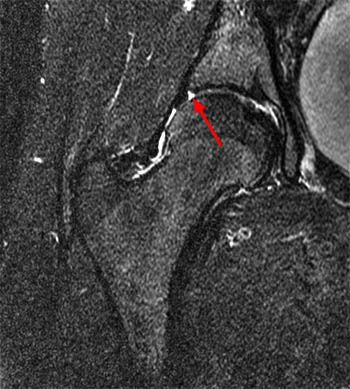
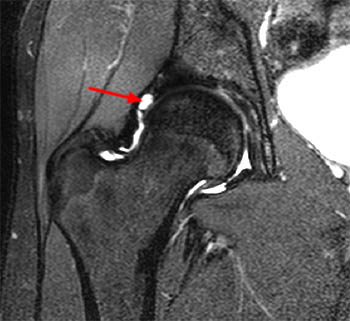
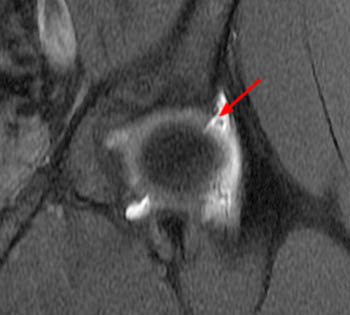
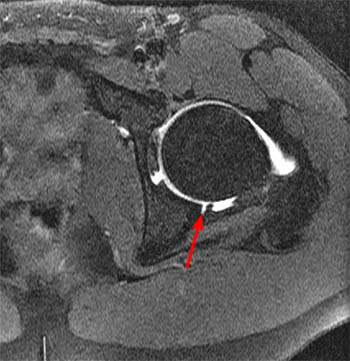
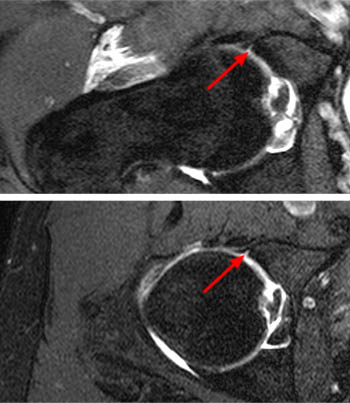
Figure 2:
The coronal T2-weighted image with fat saturation (2a) demonstrates a small undersurface tear of the posterior superior acetabular labrum at the labrocartilaginous junction (arrow). The corresponding axial proton density-weighted image with fat saturation (2b) reveals a thin band of increased signal, corresponding to the fluid-filled cleft (arrows).
Diagnosis
Undersurface detachment of the posterior superior right acetabular labrum.
Introduction
Although previously thought to be a relatively uncommon injury, acetabular labral tears are becoming diagnosed with increasing frequency because of improvements in MRI and arthroscopic techniques.1 The prevalence of labral tears in patients with hip or groin pain has been reported to be 22–55%.5-9 Labral tears of the hip are often subtle and difficult to diagnose, particularly in light of the normal variants that exist. Though tears can often be identified on routine, high-field MR imaging, many consider MR arthrography the gold standard for imaging.
Normal Anatomy
The normal acetabular labrum is a triangular-shaped, fibrocartilaginous structure that attaches to the rim of the acetabulum at the perimeter of hyaline cartilage.6-7 (3a) It is incomplete at its inferior aspect, attaching to the transverse acetabular ligament. It functions to deepen the acetabular fossa and increase the articular surface by 22%.8 It functions to seal the joint fluid in the fossa, resulting in a more even distribution of compressive forces applied to articular cartilage.9 The posterior labrum is slightly larger than the anterior labrum, possibly accounting for the increased incidence of anterior tears.
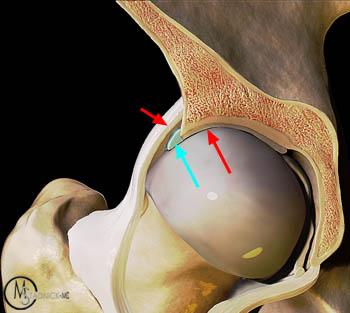
Figure 3:
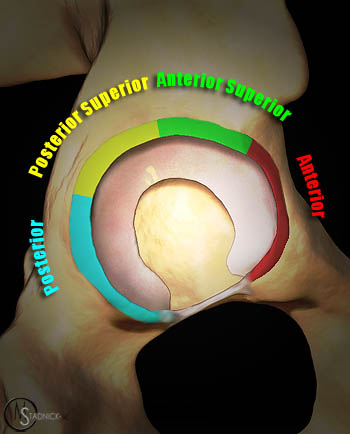
3D representation of the hip joint with the anterior acetabulum removed demonstrates the acetabular labrum (blue arrow) attaching to the acetabular rim and to the lateral margin of the articular cartilage (red arrow). The lateral recess is bounded by the capsule (short red arrow) and the acetabular labrum.
The hip capsule also attaches along the osseous rim of the acetabulum near the base of the labrum, creating the perilabral rececess.6,10 Thus, normal sulci exist may be confused with tears. Such sulci have generated a great deal of controversy in the literature.
Figure 4:
Coronal T-weighted MR arthrographic image of a 14 year-old female demonstrating a normal triangular-shaped labrum (long arrow), capsular attachment (short arrow), and normal contrast-filled lateral recess (arrowhead). Notice the normal transition between the labral tissue and articular cartilage.
Clinical presentation
Clinical findings of acetabular labral tears are highly variable and usually include groin pain. Aside from acute traumatic events, the symptom presentation is subtle, characterized by dull activity-induced or positional pain that fails to improve over time.11 Patients may describe a deep discomfort within the anterior groin or lateral hip pain proximal to the greater trochanter or posteriorly.12,13,14 A clicking mechanical symptom may suggest an acetabular labral tear although other entities, such as snapping iliopsoas tendon, may have a similar presentation.
Labral tears may also be present in association with femoroacetabular impingement25, osteoarthritis, hip dysplasia, slipped capital femoral epiphysis, and Legg-Calve-Perthes disease.11 Athletic activities that involve repetitive pivoting movements or repetitive hip flexion are recognized as additional causes of acetabular labral injury, and tears of the acetabular labrum have become an increasingly recognized disorder in young adult and middle-aged patients.4,11,12,15,16,17
MRI Findings
MR imaging of the hip is best if performed on 1.5-T or 3T magnets using small fields-of-view and high-resolution imaging. Ziegert and colleagues18 found the axial oblique plane to have the highest detection rate of arthroscopically proven acetabular labral tears and more than 95% of tears were identified with the use of 3 imaging planes.
MR arthrography is preferred by many as the imaging technique of choice in the evaluation of the acetabular labrum. The normal appearance of the labrum and its attachment must be well understood in order to properly diagnose pathology. The labrum is generally triangular in cross-section6,19 because it arises from the rim of the acetabulum, although it can have a variable shape at MR imaging.20 These labral shapes include triangular (most common), round, flat, or absent.20 A previous study by Abe and colleagues21 showed a triangular labral shape in 96% of patients who are 10 to 19 years old but in only 62% of patients older than 50 years of age, possibly due to normal aging degeneration.
The labrum is thinner anteriorly and thicker posteriorly,6,19 thus the greater incidence of anterior tears. The labrum is diffusely low signal intensity on all pulse sequences due to its fibrocartilage composition. Intermediate or high signal intensity can be present within the acetabular labrum as seen in asymptomatic individuals.22 This intermediate to high signal intensity may be due to mucoid degeneration, the presence of intralabral fibrovascular bundles, or due to magic angle artifact.11 Such labral signal may mimic a tear on conventional MR imaging.
In the assessment of the acetabular labrum for tears, the morphology of the labrum should be evaluated in all imaging planes. Is the labrum triangular in shape, rounded, thickened, distorted, or irregular? If the labrum is distorted and irregular, this is considered a labral tear.11 (5) The second assessment is to determine if contrast extends into the labrum, indicating a tear, or if contrast extends between the labrum and acetabulum, indicating labral detachment. Finally, if the signal intensity within the labrum is increased, this may represent mucoid degeneration rather than a tear.
Labral abnormalities include partial tears of the labrum or labral detachments at the labral-chondral junction(5), with detachments more common than tears, with up to 90% of cases representing labral detachments.10,16,19 The most common location for labral tears is anterosuperiorly.2,16,23 This is the location commonly affected by femoroacetabular impingement (FAI).24 (6)
Figure 5:
57 y/o female with right groin pain for 2 months and no relief with intraarticular steroid injection. A sagittal T1-weighted fat-suppressed MR arthrogram image demonstrates contrast fully extending across the base of the labrum at the labral-cartilaginous juncture (arrow) representing a tear. Note the irregular shape of the torn labrum, with loss of the normal triangular morphology.
Posterior labral tears have been described in younger athletic patients and have been associated with discrete episodes of hip trauma, typically involving impact loading of the extremity, causing the femoral head to be driven posteriorly within the acetabulum.2,11,26 (7)
The location of tears can be divided into quadrants-anterior, anterior superior, posterior superior, and posterior-or can be described by the extent of the tear using a clock face.27 However, the author and colleagues have found that using a clock face description, whether for the hip or shoulder, can be confusing between the right and left articulations and whether or not the numbering should be reversed or a fixed number always anterior.
Recognizing a paralabral cyst is helpful in the MR evaluation of the hip and may help confirm the diagnosis of a nondisplaced labral tear. Paralabral cysts are typically low to intermediate signal intensity on T1-weighted images and high signal intensity on T2-weighted images. (9) A recent study by Magerkurth and colleagues28 found paralabral cysts are most commonly anterosuperior in location, multilocular, and often extend superiorly. Paralabral cysts were highly associated with full-thickness labral tears, seen in almost all patients (94%) in their study of 18 patients.28
Tears of the acetabular labrum are identified on MR arthrography by the presence of labral distortion, high signal intensity on T2-weighted imaging, or gadolinium contrast material extending into the labral substance (10 and 11) or into the acetabular labral junction.11 The signal intensity within a labral tear does not have to be equal to gadolinium or fluid to represent a tear.18 Fraying of the free edge of the labrum is commonly encountered in the middle-aged and elderly patients and occurs at all regions of the hip and often coexists with labral tearing.11
Radsource Teleradiology Partnerships for MRI Interpretation
Boost your diagnostic confidence with RadSource’s Teleradiology services & partnership. Reliable MRI interpretation is just a click away.
Pitfalls and Normal Variants
When evaluating labral tears, normal variants must be considered. The most important and often controversial problem is the presence of normal sulci. There is controversy about the existence of the anterior superior sublabral sulcus. Some studies have found no evidence of labral sulci, whereas others speculate about, suggest, or support its existence.6,7,10,11,19,20,22,29,30,31 Some authors even believe that a sulcus may actually be a healing labral tear.16
A normal posteroinferior acetabular sublabral sulcus (12 and 13) or groove (also called a posterior labrocartilaginous cleft) is present in up to 23% of hips.32
The frequency of these reported sulci can be helpful in the determination of whether a finding is a tear or sulcus. In one study, of those with a single sulcus (25 patients), 11 (44%) were located anterosuperiorly, 12 (48%) posteroinferiorly, 1 (4%) anteroinferiorly, and 1 (4%) posterosuperiorly.11
In a study by Studler and colleagues,31 of 57 patients evaluated surgically or arthroscopically, a sublabral recess was found in 18% at the anterior aspect of the joint (typically the 8 o’clock position), and was almost invariably linear in shape on MR imaging (14). A finding at the 9-10 o’clock position could be either a recess or tear, and a recess at the anterior superior quadrant (10-12 o’clock) position was only found in 2% of the patients with this location being more typical for a labral tear.
When contrast material on MR arthrography extends into the labral substance, this is indicative of a labral tear. Additionally, if there is adjacent cartilage or osseous abnormalities or a paralabral cyst, a labral tear should be suspected.31 Additionally, if a patient gets pain relief after intra-articular anesthetic injection and there are MR imaging findings of subtle changes within the anterosuperior acetabular labrum, this likely is a labral tear.
MR imaging features of labral recesses include:31,33
- a shallow depth (less than one-half labral thickness)
- linear shape
- smooth borders
- location at the labral-chondral junction
- not accompanied by perilabral acetabular abnormalities
- only partial separation of the labrum from its acetabular attachment
However, these features can be variable and there is often overlap in the appearance of tears versus recesses. Also of note is that the anterior labrum is absent in 10-14% of the population.34,35
Figure 14:
43 y/o male with chronic hip pain. Axial oblique fat-suppressed proton density-weighted images (above) and an axial T-weighted image with fat suppression (below) demonstrate a normal anterior sublabral recess at the 9 o'clock position (arrows). Note the normal triangular shaped labral tissue lateral to the recess.
Treatment
Nonsurgical, conservative treatment of labral tears is preferred, including NSAIDs, corticosteroid injections, and physical therapy. If conservative measures fails or there are significant mechanical symptoms, arthroscopic reattachment and/or debridement may be performed.
Summary
The cause of labral tears can be degenerative, dysplastic, traumatic, idiopathic, or impingement.11 Degenerative tears may be related to old trauma, osteoarthritis, or inflammatory arthropathies. Traumatic labral tears are typically isolated to one particular location dependent upon the force vector of the traumatic event. These tears occur in the same region as those seen in athletes, femoroacetabular impingement, or in mild hip dysplasia.15,36 In addition to the obvious visualization of the tear, the study should be evaluated for secondary signs of tear such as paralabral cysts and chondral lesions.
References
1 Robertson WJ, Kadrmas WR, Kelly BT. Arthroscopic Management of Labral Tears in the Hip: A Systematic Review. Clin Orthop Relat Res. 2007; 455:88-92.
2 McCarthy JC, Noble PC, Schuck MR, et al. The Otto E Aufranc Award the role of labral lesions to development of early degenerative hip disease. Clin Orthop. 2001; 393:25-37.
3 Lewis CL, Sahrmann SA. Acetabular labral tears. Phys Ther. 2006; 86:110-121.
4 McCarthy JC, Busconi B. The role of hip arthroscopy in the diagnosis and treatment of hip disease. orthopaedics. 1995; 18(8):753-756
5 Narvani AA, Tsiridis E, Kendall S, Chaudhuri R, Thomas P. A preliminary report on prevalence of acetabular labrum tears in sports patients with groin pain. Knee Surg Sports Traumatol Arthrosc. 2003; 11:403-408.
6 Keene GS, Villar RN. Arthroscopic anatomy of the hip: an in vivo study. Arthroscopy. 1994; 10(4):392-399
7 Hodler J, Yu JS, Goodwin D, et al. MR arthrography of the hip: improved imaging of the acetabular labrum with histologic correlation in cadavers. AJR Am J Roentgenol. 1995; 165(4):887-891
8 Seldes RM, Tan V, Hunt J, Katz M, Winiarsky R, Fitzgerald RH Jr. Anatomy, histologic features, and vascularity of the adult acetabular labrum. Clin Orthop Relat Res 2001; (382):232-240.
9 Ferguson SJ, Bryant JT, Ganz R, Ito K. An in vitro investigation of the acetabular labral seal in hip joint mechanics. J Biomech 2003; 36(2):171-178.
10 Petersilge CA. MR arthrography for evaluation of the acetabular labrum. Skeletal Radiol. 2001; 30(8):423-430
11 Blankenbaker DG, Tuite MJ. Acetabular Labrum. MRI Clin of North America. 2013; 21(1):21-33.
12 Mason JB. Acetabular labral tears in the athlete. Clin Sports Med. 2001; 20(4):779-790
13 Burnett RS, Della Rocca GJ, Prather H, et al. Clinical presentation of patients with tears of the acetabular labrum. J Bone Joint Surg Am. 2006; 88(7):1448-1457
14 Arnold DR, Keene JS, Blankenbaker DG, et al. Hip pain referral patterns in patients with labral tears: analysis based on intra-articular anesthetic injections, hip arthroscopy, and a new pain “circle” diagram. Phys Sportsmed. 2011; 39(1):29-35
15 McCarthy J, Noble P, Aluisio FV, et al. Anatomy, pathologic features, and treatment of acetabular labral tears. Clin Orthop Relat Res. 2003; (406):38-47
16 Fitzgerald RH. Acetabular labrum tears. Diagnosis and treatment. Clin Orthop Relat Res. 1995; (311):60-68
17 Farjo LA, Glick JM, Sampson TG. Hip arthroscopy for acetabular labral tears. Arthroscopy. 1999; 15(2):132-137
18 Ziegert AJ, Blankenbaker DG, De Smet AA, et al. Comparison of standard hip MR arthrographic imaging planes and sequences for detection of arthroscopically proven labral tear. AJR Am J Roentgenol. 2009; 192(5):1397-1400
19 Czerny C, Hofmann S, Neuhold A, et al. Lesions of the acetabular labrum: accuracy of MR imaging and MR arthrography in detection and staging. Radiology. 1996;200(1):225-230
20 Lecouvet FE, Vande Berg BC, Malghem J, et al. MR imaging of the acetabular labrum: variations in 200 asymptomatic hips. AJR Am J Roentgenol. 1996; 167(4):1025-1028
21 Abe I, Harada Y, Oinuma K, et al. Acetabular labrum: abnormal findings at MR imaging in asymptomatic hips. Radiology. 2000; 216(2):576-581
22 Cotten A, Boutry N, Demondion X, et al. Acetabular labrum: MRI in asymptomatic volunteers. J Comput Assist Tomogr. 1998; 22(1):1-7
23 Lage LA, Patel JV, Villar RN. The acetabular labral tear: an arthroscopic classification. Arthroscopy. 1996; 12(3):269-272
24 Pfirrmann CW, Mengiardi B, Dora C, et al. Cam and pincer femoroacetabular impingement: characteristic MR arthrographic findings in 50 patients. Radiology. 2006; 240(3):778-785
25 Bodor DB. MRI Web Clinic, Femoroacetabular Impingement. 2011. https://radsource.us/femoroacetabular-impingement/
26 Ikeda T, Awaya G, Suzuki S, et al. Torn acetabular labrum in young patients. Arthroscopic diagnosis and management. J Bone Joint Surg Br. 1988; 70(1):13-16
27 Blankenbaker DG, De Smet AA, Keene JS, et al. Classification and localization of acetabular labral tears. Skeletal Radiol. 2007; 36(5):391-397
28 Magerkurth O, Jacobson JA, Girish G, et al. Paralabral cysts in the hip joint: findings at MR arthrography. Skeletal Radiol. 2012; 41(10):1279-1285
29 Byrd JW. Labral lesions: an elusive source of hip pain case reports and literature review. Arthroscopy. 1996; 12(5):603-612
30 Saddik D, Troupis J, Tirman P, et al. Prevalence and location of acetabular sublabral sulci at hip arthroscopy with retrospective MRI review. AJR Am J Roentgenol. 2006; 187(5):W507-W511
31 Studler U, Kalberer F, Leunig M, et al. MR Arthrography of the Hip: Differentiation between an Anterior Sublabral Recess as a Normal Variant and a Labral Tear. Radiology 2008; 249(3):947-954
32 Dinauer PA, Murphy KP, Carroll JF. Sublabral sulcus at the posteroinferior acetabulum: a potential pitfall in MR arthrography diagnosis of acetabular labral tears. AJR Am J Roentgenol 2004; 183(6):1745-1753.
33 Blankenbaker DG, Tuite MJ. The painful hip: new concepts. Skeletal Radiol. 2006; 35(6):352-370
34 Cotten A, Boutry N, Demondion X, et al. Acetabular labrum: MRI in asymptomatic volunteers. J Comput Assist Tomogr 1998;22(1):1-7.
35 Lecouvet FE, Vande Berg BC, Malghem J, et al. MR imaging of the acetabular labrum: variations in 200 asymptomatic hips. AJR Am J Roentgenol 1996; 167(4):1025-1028.
36 Kassarjian A, Yoon LS, Belzile E, et al. Triad of MR arthrographic findings in patients with cam-type femoroacetabular impingement. Radiology. 2005; 236(2):588-592