Clinical History: A 31 year-old female presents with anterior pectoralis muscle hardening and swelling with extreme pain. She has a history of multiple episodes of MRSA infection over the previous 9 years. What are the findings? What is your diagnosis?
Findings
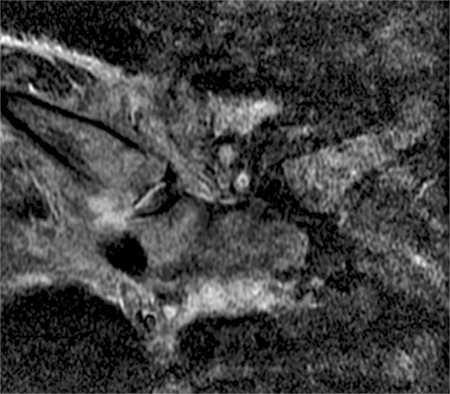
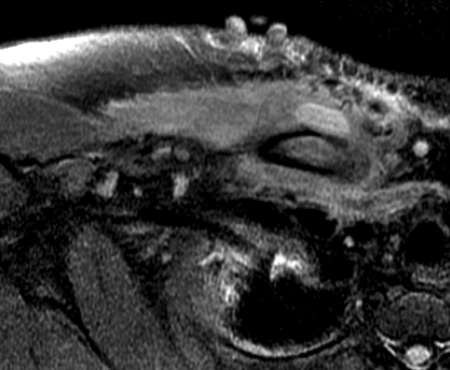
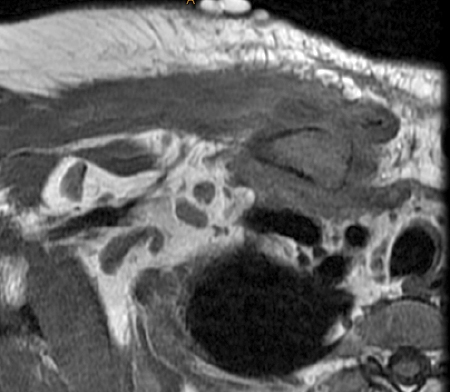
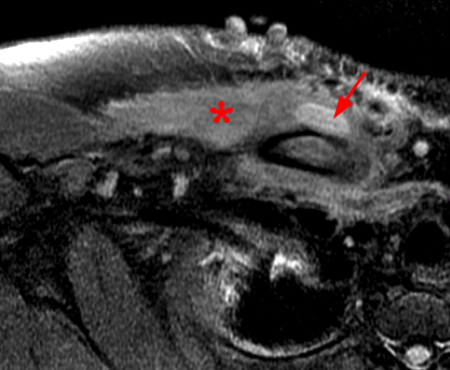
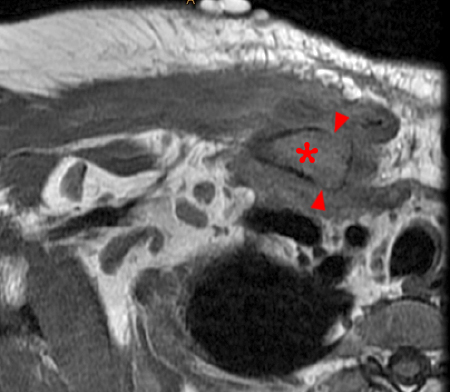
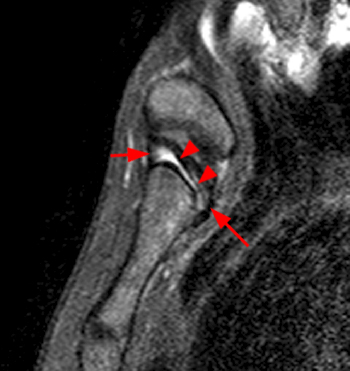
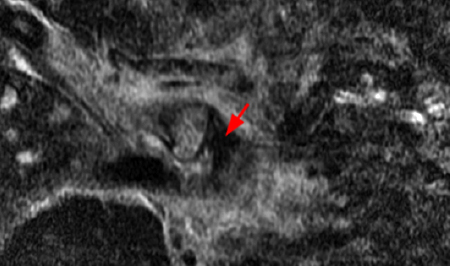
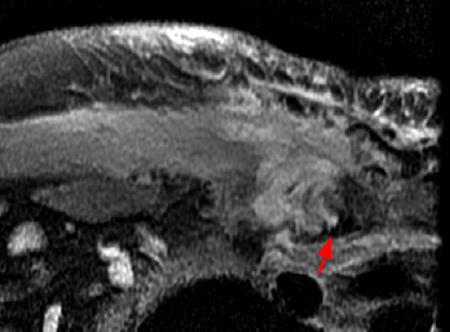
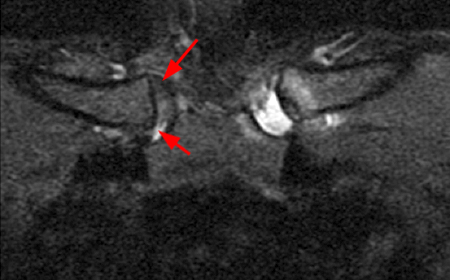
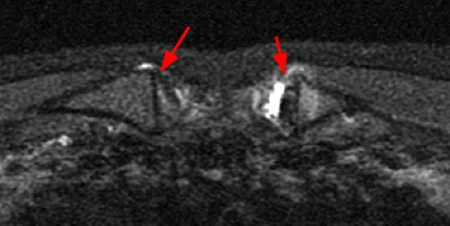
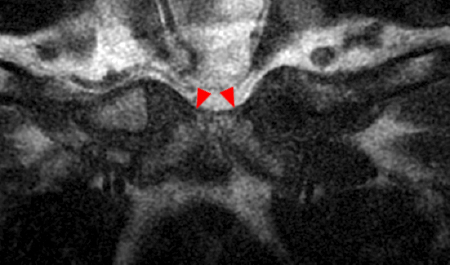
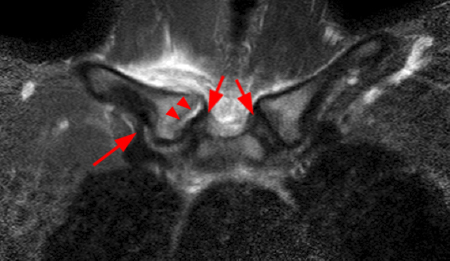
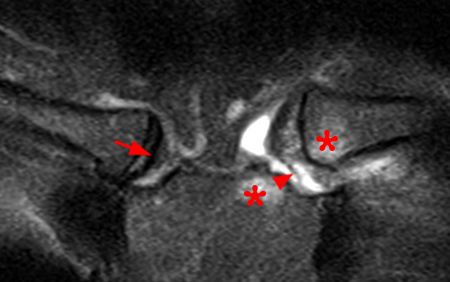
Figure 2:
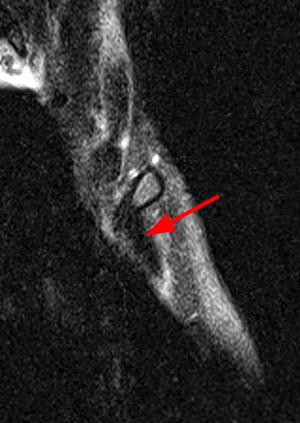
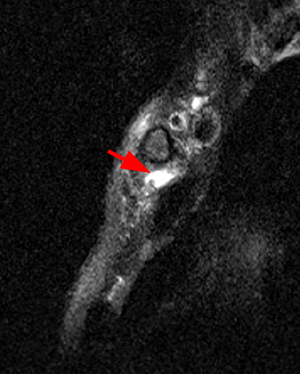
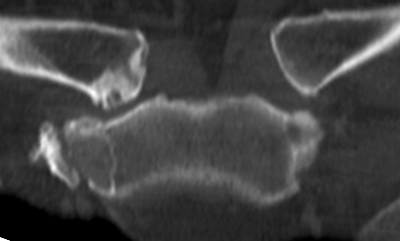
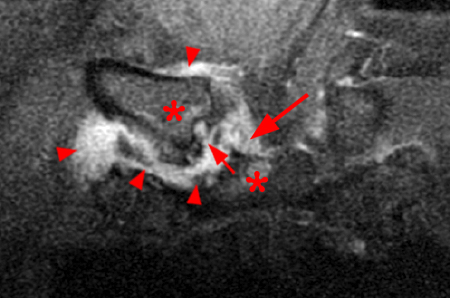
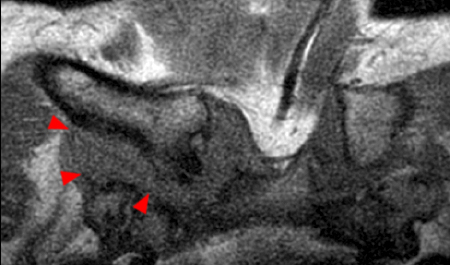
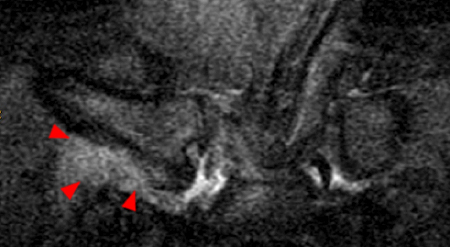
Coronal STIR (2a) and axial fat-suppressed proton density (2b) images demonstrate fluid within and extending caudal to the sternoclavicular joint (arrow), cortical loss of the caudal margin of the clavicular head (short arrow), mild clavicular and manubrial edema (asterisks), and surrounding soft tissue edema (arrowheads). The axial fat-suppressed proton density-weighted image demonstrates edema within the clavicular head of the pectoralis major muscle (asterisk) along with a small abscess (arrow). The axial T1-weighted image (2c) reveals intermediate signal in the medial aspect of the right clavicle (asterisk) reflective of edema as well as anterior and posterior cortical loss (arrowheads).
Diagnosis
Septic sternoclavicular joint with clavicular and manubrial osteomyelitis.
Introduction
The sternoclavicular joint is susceptible to pathology similar to other synovial joints, the most common being osteoarthritis, instability from injury, infection, and rheumatoid arthritis.1 The joint lies in a subcutaneous position and thus swelling of the joint or expansion of the medial clavicle is evident at an early stage of disease.1
The most common clinical presentation of pathology at the joint is pain and swelling in the area, with either an acute onset following injury or an insidious onset with no history of trauma. In both situations the pathology can usually be localized to the joint but the actual diagnosis frequently cannot be made without advanced imaging, particularly MRI.1
Normal Anatomy
The sternoclavicular joint is formed by the expanded medial end of the clavicle articulating in a saddle joint with the superolateral manubrium.1
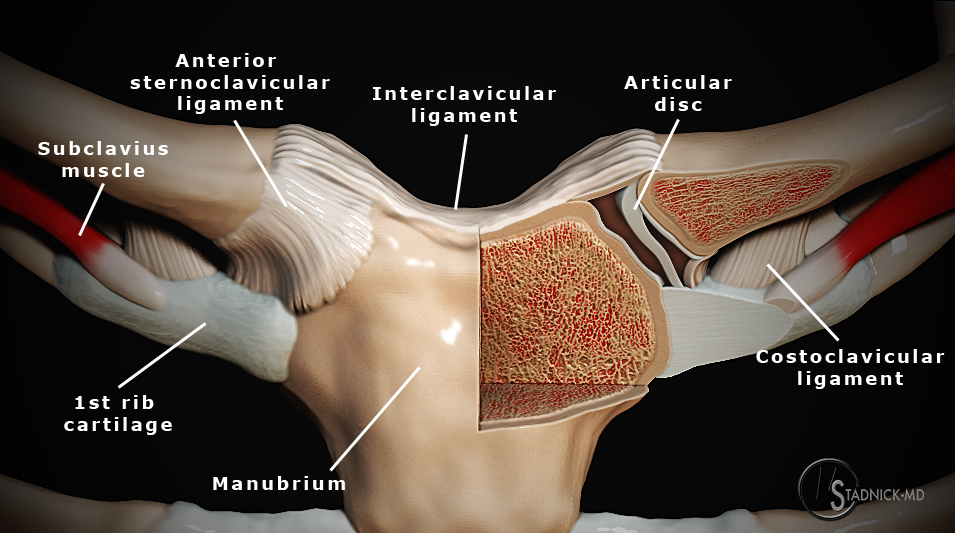
The joint contains two separate synovial cavities, divided by an articular disk (Figure 3) which is firmly attached at its caudal aspect to the cartilage of the 1st rib at its articulation with the sternum, and at its cephalad aspect to the clavicle.2
Figure 3:
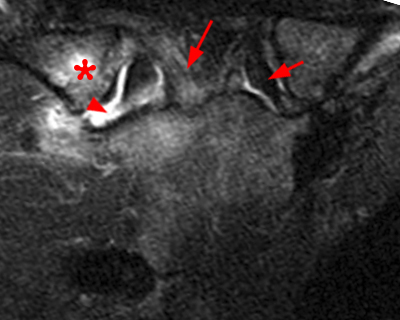
A sagittal fat-suppressed T2-weighted image of the left sternoclavicular joint in a patient with severe post-traumatic and degenerative changes of the right joint demonstrating a normal articular disc (arrowheads) and anterior (short arrow) and posterior (arrow) sternoclavicular ligaments.
The stability of this shallow joint is mainly dependent upon four distinct ligaments and the subclavius muscle.1 The fibrous capsule of the joint is strengthened by anterior and posterior sternoclavicular ligaments2 (Figures 4 and 5) which when disrupted can cause superior translation of the joint.3
Figure 5:
Coronal STIR (5a) and axial STIR (5b) images of a patient with a degenerative left sternoclavicular joint. The coronal STIR view (5a) demonstrates an intact right anterior sternoclavicular ligament (arrow). Note the small hole in the caudal aspect of the right sternoclavicular disc (short arrow). An axial STIR image (5b) demonstrates intact right (arrow) and disrupted left (short arrow) anterior sternoclavicular ligaments.
The sternoclavicular ligaments insert at the medial clavicular epiphysis, which usually doesn’t fuse until the age of 25 years.3 (Figure 8) As a result, many injuries to the sternoclavicular joint in teenagers and young adults may actually be physeal separations of the medial clavicle.1 (Figure 7)
The two clavicles are united across the upper sternum by the interclavicular ligament.2 (Figure 6)
The costoclavicular ligament (Figures 7 and 8), a major stabilizer of the joint, extends between the clavicle and the 1st rib, originating from the cartilage and the distal end of the bone of the 1st rib, passing upward, laterally, and backward to attach to the inferior surface of the clavicle.2
Figure 7:
Coronal STIR image of a 16 year-old who impacted his shoulder playing lacrosse resulting in a nondisplaced Salter-Harris 1 injury of the medial clavicle (arrowheads). Note the intact costoclavicular ligament (long arrow) as well as the intact bilateral anterior sternoclavicular ligaments (short arrows).
Sternoclavicular joint pathology
Septic joint
In cases of a septic sternoclavicular joint, MR images may depict bone marrow edema, bone destruction, joint effusion, and inflammatory changes in the surrounding soft tissues, with the earliest findings being effusion, widening of the joint space, or mild cortical irregularity. Osteomyelitis of the distal clavicle, the manubrium, or both may be present in up to 55% of cases.4
Septic arthritis of the sternoclavicular joint is uncommon in healthy adults, representing less than 0.5% of bone and joint infections.4 It may occur from hematogenous spread from a distant source or from contiguous spread from a nearby infection.5 It should be considered as part of the differential diagnosis of a unilateral, painful swelling of the joint or peri-articular region, particularly if the history is relatively acute and in the absence of trauma. In a previously fit individual, there may be a history of a recent systemic infection and associated systemic features of fever, chills and night sweats.1 Any patient complaining of unilateral SC joint pain in the absence of injury should be considered to have an infection until proven otherwise.5
Osteoarthritis
Osteoarthritis is the most frequent cause of pain and swelling of the sternoclavicular joint. Like other synovial joints, the characteristic signs are narrowing of the joint space, capsular hypertrophy, subchondral cysts and sclerosis, and the formation of osteophytes (Figure 10).
Figure 10:
Same patient as in Figure 3 with pain following a motor vehicle accident. The coronal fat-suppressed T2-weighted image (10a) demonstrates a tear of the caudal aspect of the articular disc (arrowhead), edema in the medial clavicle (asterisk), and thickening and edema of the rightward aspect of the interclavicular ligament (arrow). Notice the intact left articular disc (short arrow). A coronal CT reconstruction (10b) provides only limited findings of subarticular degenerative cysts, sclerosis, and joint space narrowing.
Rheumatoid arthritis
Up to one-third of patients with rheumatoid arthritis may have pannus formation, bony erosion, and degeneration of the articular disc of the sternoclavicular joints.6,7
Imaging characteristics are similar to rheumatoid arthritis at other synovial joints (Figure 11).
Figure 11:
A contrast-enhanced coronal fat-suppressed T1-weighted image (11a), coronal proton density-weighted (11b), and coronal STIR (11c) images from a 56 year-old with chronic pain and swelling demonstrate severely enhancing synovium (arrowheads), disruption of the articular disc (short arrow), irregular partial disruption of the interclavicular ligament (long arrow), and mild enhancement of the medial clavicle and manubrium (asterisks). The findings are typical for inflammatory arthritis, likely rheumatoid arthritis. The pannus (arrowheads) is prominently demonstrated even without gadolinium enhancement (11b, 11c).
Trauma
Dislocations of the sternoclavicular joint are less common than those of the glenohumeral and acromioclavicular articulations8 and comprise 1% of all joint dislocations, and 3% of those in the upper limb.3 Dislocation of the sternoclavicular joint is uncommon because the energy produced by blunt trauma usually causes injury of the more peripheral bones and joints of the shoulder girdle.1
Anterior dislocations are much more common than posterior dislocations,9 and if the ligamentous structures fail to heal after closed reduction of an acute traumatic dislocation, the patient may develop recurrent symptomatic instability of the joint.1 This most commonly affects adolescent females, who typically have evidence of generalized ligamentous laxity.10 Trauma to the joint usually results in a lesser degree of displacement than frank dislocation. Displacement is usually cephalad, and associated ligamentous injury as well as marrow and surrounding soft tissue may be identified (Figure 12).
Figure 12:
A coronal fat-suppressed T2-weighted image of a 52 year-old injured in an ATV accident 7 weeks prior demonstrating a tear of the left sternoclavicular articular disc (arrowhead), with an intact right articular disc (short arrow) as well as fluid in the injured left joint space, clavicular and manubrial edema (asterisks), and mild cephalad subluxation of the clavicle.
SAPHO syndrome
SAPHO is an acronym for synovitis, acne, palmoplantar pustulosis, hyperostosis, and osteitis. It is also called sternoclavicular hyperostosis. This spectrum of coexistent and chronic skin and osteoarticular conditions usually affecting middle aged females. The sternoclavicular joint is the joint most frequently affected and is involved in 65%–90% of cases11 with two thirds of patients having bilateral involvement.1 The skin lesions are typically pustular and include severe forms of acne (fulminans or conglobata), palmoplantar pustulosis and psoriasis.1
Condensing osteitis
Condensing osteitis occurs almost exclusively in women between the ages of 20 and 60 years,12 and is characterized by enlargement and osteosclerosis of the medial end of the clavicle and obliteration of its medullary cavity with little or no surrounding soft-tissue reaction.1 Trauma and chronic stress have been suggested as causes, and it has a resemblance to osteitis pubis and osteitis condensans ilii.12 The patient presents with pain and swelling at the sternoclavicular joint.
This condition can be distinguished from SAPHO by the location of abnormal findings isolated to the clavicle, with a normal appearance of the sternoclavicular joint, adjacent ribs and costal cartilages. However, distinction from a primary or metastatic bone tumor may be difficult without biopsy.1
Other conditions
The sternoclavicular joint is involved in 90% of patients with severe psoriatic arthropathy and is clinically significant in 50%,13 whereas involvement is present in only 4% of patients with ankylosing spondylitis.14 Rarely the sternoclavicular joint is affected by gout, appearing similar to other affected joints. The joint can also be disturbed by Reiter’s syndrome, pseudogout (calcium pyrophosphate dehydrate crystal deposition), Paget’s disease, chondrosarcoma, metastases, plasmacytoma, and multiple myeloma.
Treatment
Most disorders of the sternoclavicular joint are treated conservatively because of the poor results associated with surgical treatment and the potentially catastrophic surgical complications. However, injuries to the joint, as well as infective, inflammatory, and degenerative arthritides, are relatively common and may be the source of chronic disability if not adequately diagnosed and treated.1
Conclusion
The sternoclavicular joint may be affected by a wide range of pathologies. Although septic arthritis of the sternoclavicular joint is uncommon, with the joint much more frequently affected by osteoarthritis, infection should be considered in a patient with an acute onset of symptoms in the absence of trauma. In cases of sternoclavicular joint pain and/or swelling, MRI is frequently effective in making the correct diagnosis, allowing appropriate treatment to begin.
References
- Robinson CM, Jenkins PJ, Markham PE, Beggs I. Disorders of the sternoclavicular joint. J Bone Joint Surg (Br) 2008; 90-B:685-96 ↩
- Hollinshead WH, Rosse C. Textbook of anatomy, 4th Edition. Harper & Row. 1985 ↩
- Renfree KJ, Wright TW. Anatomy and biomechanics of the acromioclavicular and sternoclavicular joints. Clin Sports Med 2003; 22:219-37 ↩
- Ross JJ, Shamsuddin H. Sternoclavicular septic arthritis: review of 180 cases. Medicine 2004; 83:139 –48 ↩
- Womack J. Septic arthritis of the sternoclavicular joint. J Am Board Fam Med Nov-Dec 2012; 25(6):908-912 ↩
- Higginbotham TO, Kuhn JE. Atraumatic disorders of the sternoclavicular joint. J Am Acad Orthop Surg 2005; 13:138-45 ↩
- Restrepo CS, Martinez S, Lemos D, Washington L, McAdams HP, Vargas D, Lemos J, Carrillo J, Diethelm L. Imaging appearances of the sternum and sternoclavicular joints. Radiographics May-June 2009; 29(3):839-859. ↩
- Kocher MS, Dupré MM, Feagin JA Jr. Shoulder injuries from alpine skiing and snowboarding: aetiology, treatment and prevention. Sports Med 1998; 25:201-11 ↩
- Nettles JL, Linscheid RL. Sternoclavicular dislocations. J Trauma 1968; 8:158-64 ↩
- Rockwood CA Jr, Odor JM. Spontaneous atraumatic anterior subluxation of the sternoclavicular joint. J Bone Joint Surg (Am) 1989; 71-A:1280-8 ↩
- EarwakerJW, Cotten A. SAPHO: syndrome or concept?—imaging findings. Skeletal Radiol 2003; 32: 311–327 ↩
- Harden SP, Argent JD, Blaquiere RM. Painful sclerosis of the medial end of the clavicle. Clin Radiol 2004; 59:992-9 ↩
- Taccari E, Spadaro A, Riccieri V, et al. Sternoclavicular joint disease in psoriatic arthritis. Ann Rheum Dis 1992; 51:372-4 ↩
- Emery RJ, Ho EK, Leong JC. The shoulder girdle in ankylosing spondylitis. J Bone Joint Surg (Am) 1991; 73-A:1526-31 ↩