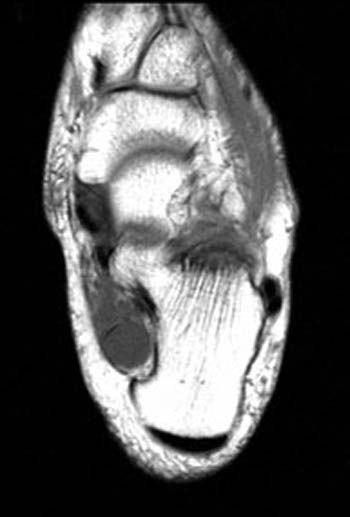
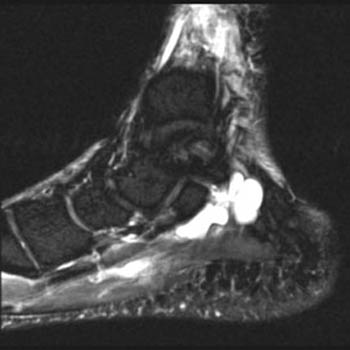
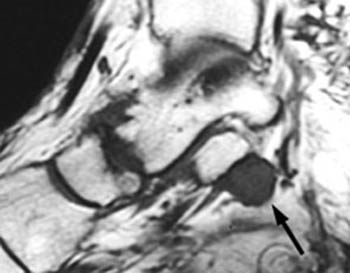
Clinical History: 34 year old female complains of medial foot pain and numbness. (1a) A T1 weighted axial image and (1b) fat-suppressed T2 weighted sagittal image are provided. What are the findings? What is your diagnosis?
Findings
Diagnosis
Ganglion cyst resulting in tarsal tunnel syndrome.
Discussion
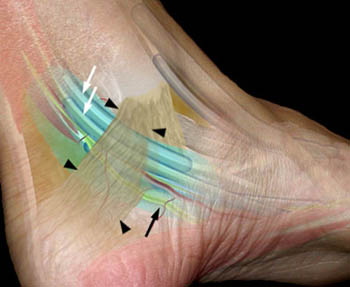
Numerous entrapment neuropathies have been described in the musculoskeletal system. At the foot and ankle, tarsal tunnel syndrome refers to a particular entrapment neuropathy that is caused by compression of the posterior tibial nerve along the medial aspect of the hindfoot. In this region, the posterior tibial nerve passes through a confined space, the tarsal tunnel or tarsal canal (Figure C). The tarsal tunnel is bound by the bones of the foot laterally and by the flexor retinaculum medially.1 This fibro-osseous tunnel contains the posterior tibial tendon, flexor digitorum longus tendon, flexor hallucis longus tendon, the posterior tibial artery, and the posterior tibial nerve. Any process that occupies space or causes inflammation in this region may result in the symptoms of tarsal tunnel syndrome.
Figure 3:
(3a) The posterior tibial nerve (arrow) is seen coursing beneath the flexor retinaculum (arrowheads) in this illustration of the tarsal tunnel, viewed from the medial side. The posteromedial ankle tendons(white arrows) lie along the anterior aspect of the posterior tibial neurovascular bundle.
Patients with tarsal tunnel syndrome often complain of burning, unremitting pain and/or parasthesias.2 The pain often radiates into the toes. Numbness may occur at the medial foot, and in severe cases, atrophy of intrinsic foot musculature with alterations in gait may ensue. Eversion and dorsiflexion may exacerbate symptoms, whereas rest, massage and elevation may result in symptom relief.
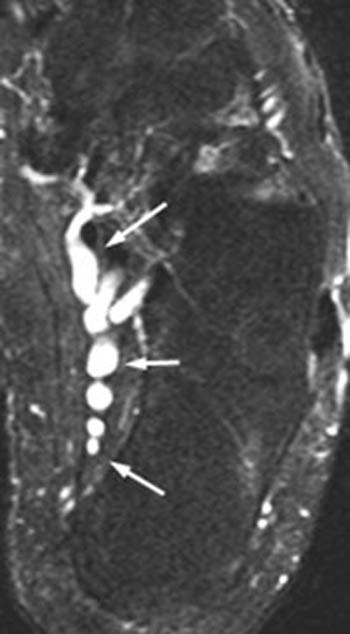
About half of cases of tarsal tunnel syndrome are idiopathic. Certain anatomic variations such as pes planus and hindfoot valgus deformity increase the risk of the syndrome, as these configurations increase the tensile load upon the posterior tibial nerve. Trauma with subsequent scarring and fibrosis within the tarsal canal has been implicated, and the syndrome is found with greater frequency in patients with rheumatoid arthritis and diabetes. MRI is particularly helpful in detecting masses that may cause tarsal tunnel syndrome. Mass-like etiologies include ganglion cysts, neurogenic tumors (Fig 4), varicosities (Fig 5), lipomas, severe tenosynovitis, and accessory muscles.
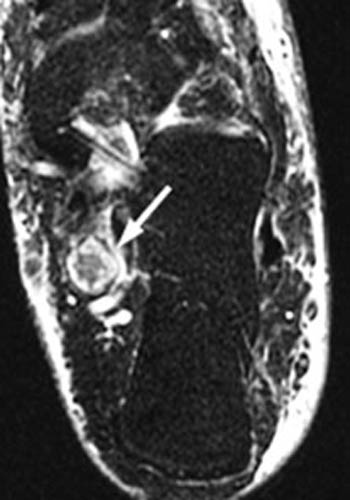
Figure 4:
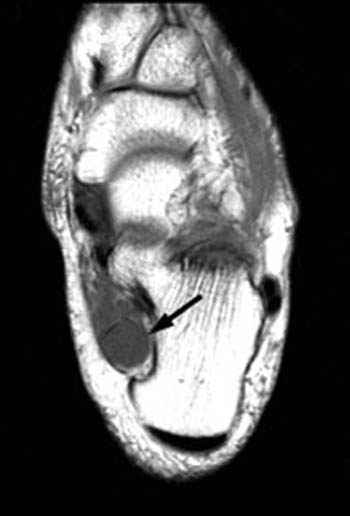
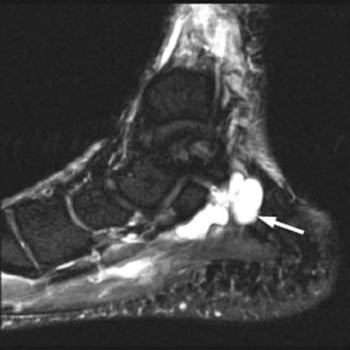
A schwannoma (arrows) is identified within the tarsal tunnel on (4a) T1 weighted sagittal and (4b) fat-suppressed T2 weighted axial images. Note that unlike the fluid-signal intensity ganglion seen in (2a,2b), this abnormality demonstrates soft-tissue signal intensity on both T1- and T2-weighted images.
Treatment of tarsal tunnel syndrome includes injection of local anesthetics and steroids into the tarsal canal, which also serves as a useful diagnostic aid. Physical therapy including stretching exercises may be of benefit. When conservative therapy fails, or when space-occupying lesions are present, surgery to release the flexor retinaculum and entrapped posterior tibial nerve is indicated.3
Conclusion
The tarsal tunnel syndrome is a less well-known compressive neuropathy that results from compression of the posterior tibial nerve at the medial foot. Pain, sensory deficits, and muscle weakness may occur in these patients. MR is useful for identifying space occupying lesions or inflammatory changes that may result in tarsal tunnel syndrome.
References
1 Sarrafian SK. Cross sectional and topographic anatomy. Sarrafian SK. Anatomy of the foot and ankle. 2nd ed. Philadelphia, Pa: Lippincott, 1993; 433-437.
2 Erickson, SJ, Quinn, SF, Kneeland JB, et al. MR imaging of the tarsal tunnel and related spaces: normal and abnormal findings with anatomic correlation. Am J Roentgenol 1990; 155: 323-328.
3 Bailie DS, Kelikian AS: Tarsal tunnel syndrome: diagnosis, surgical technique, and functional outcome. Foot Ankle Int 1998 Feb; 19(2): 65-72.