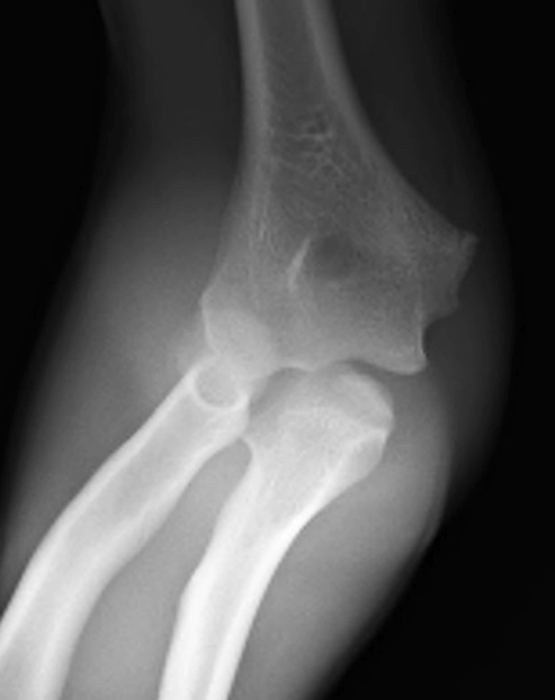
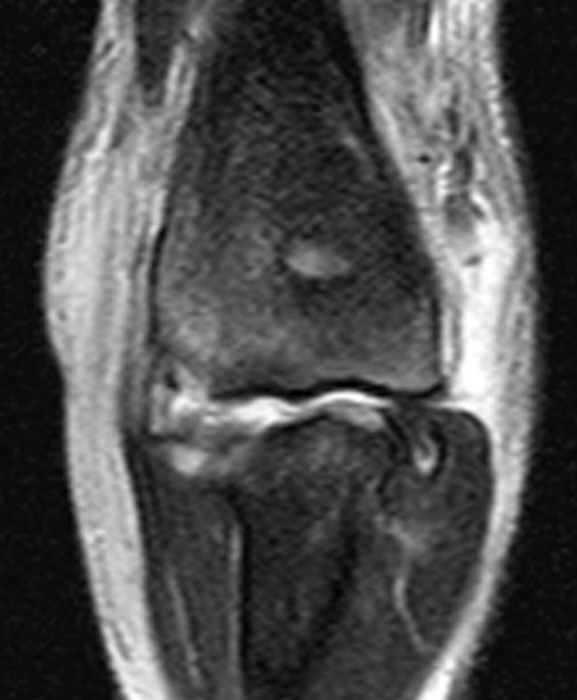
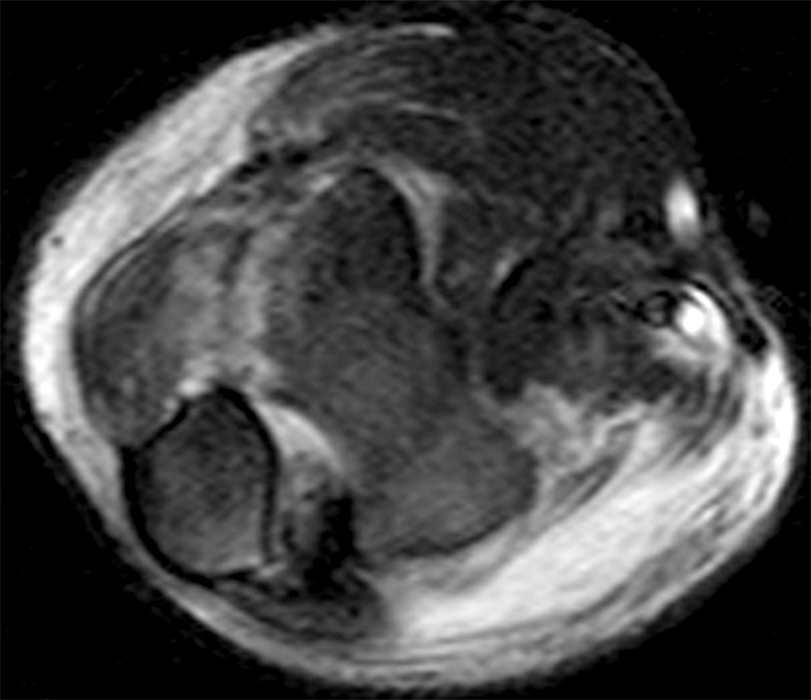
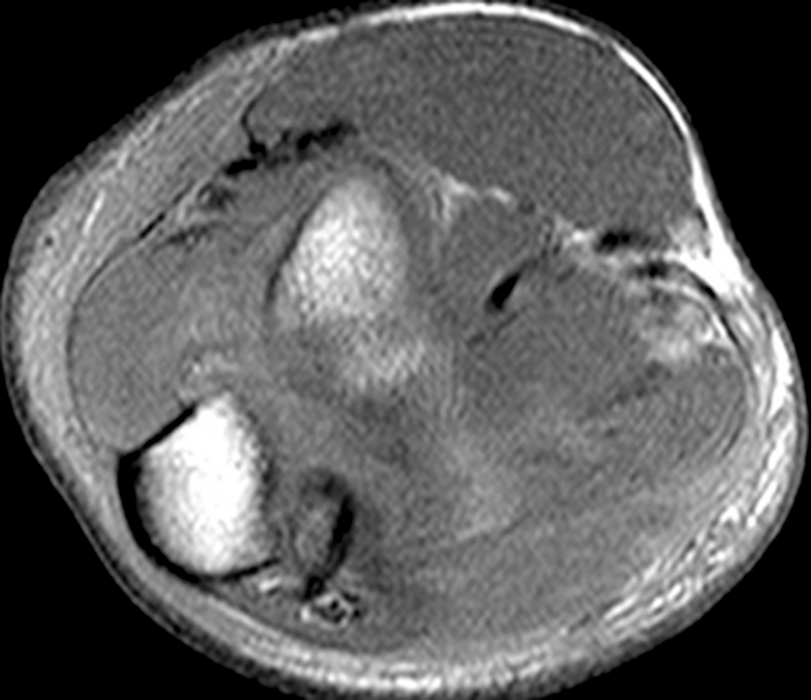
Clinical History: A 15-year-old boy presents with elbow pain, limited range of motion and ulnar neuropraxia after a recent wrestling injury. An AP radiograph (1a), coronal STIR (1b) and (1c) fat-suppressed T2-and (1d) T1-weighted axial images are provided. What are the findings? What is your diagnosis?
Findings
Figure 2:
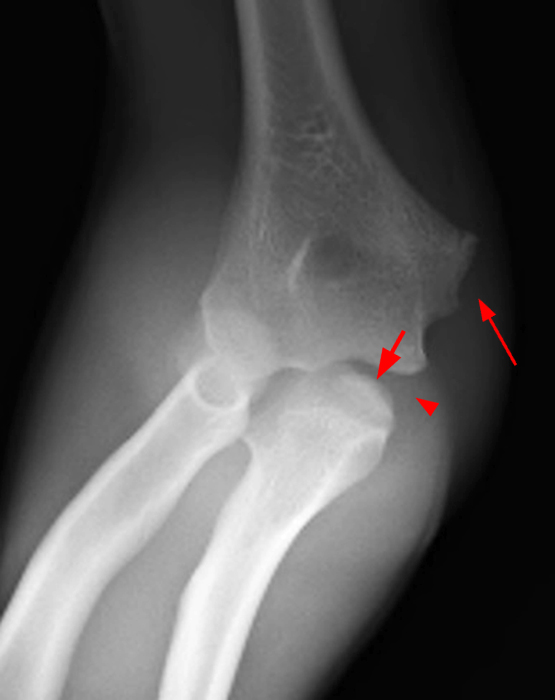
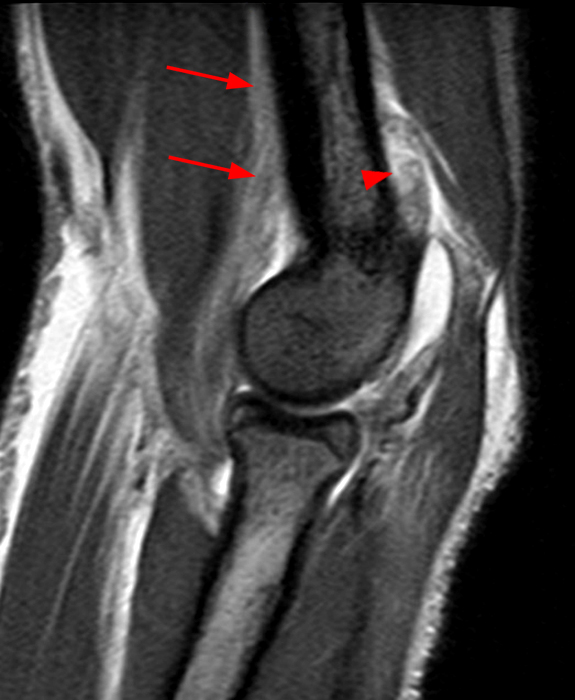
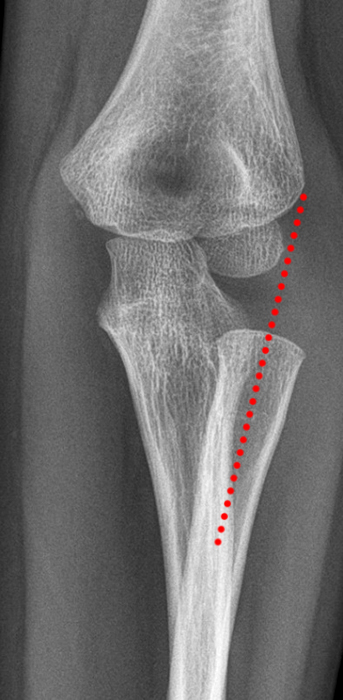
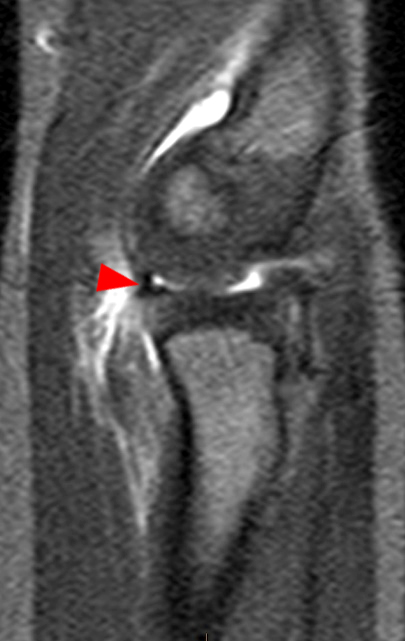
(2A) A frontal radiograph taken with the elbow in flexion, because of the inability to fully extend it, shows widening of the humeroulnar joint space (arrowhead) and truncation of the medial humeral epicondyle (arrow). A bone fragment projects over the proximal ulna (short arrow).
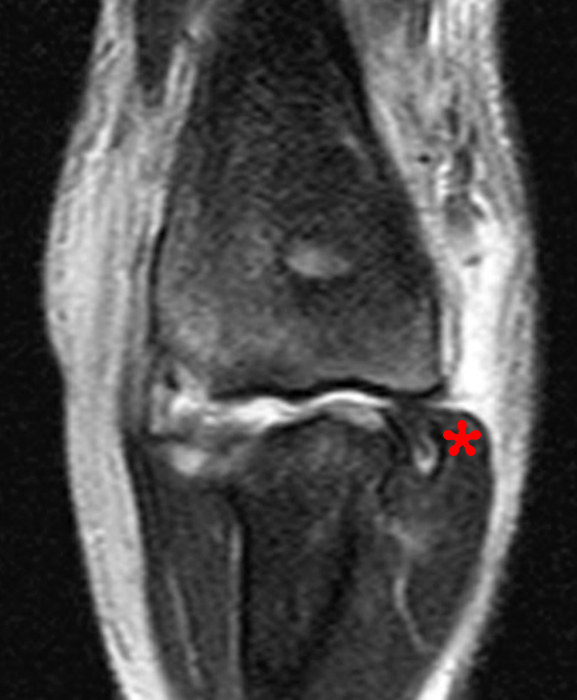
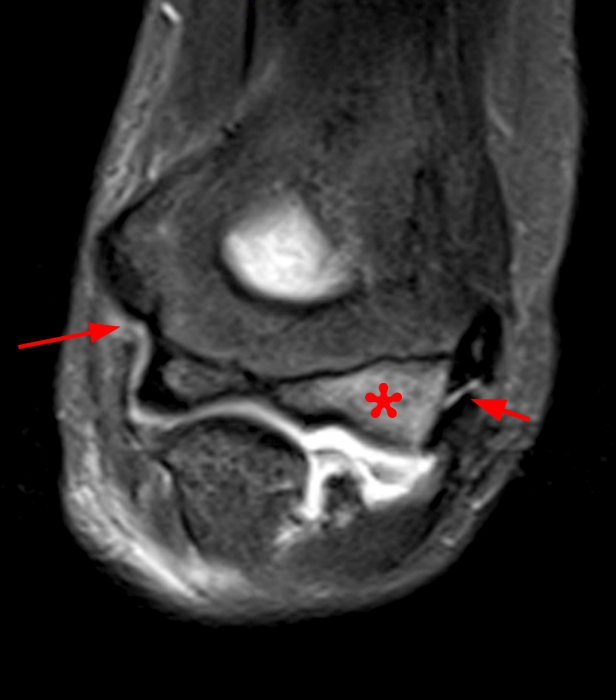
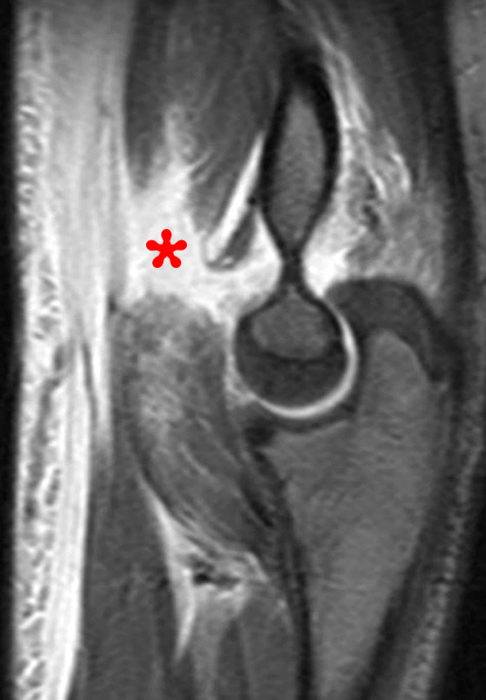
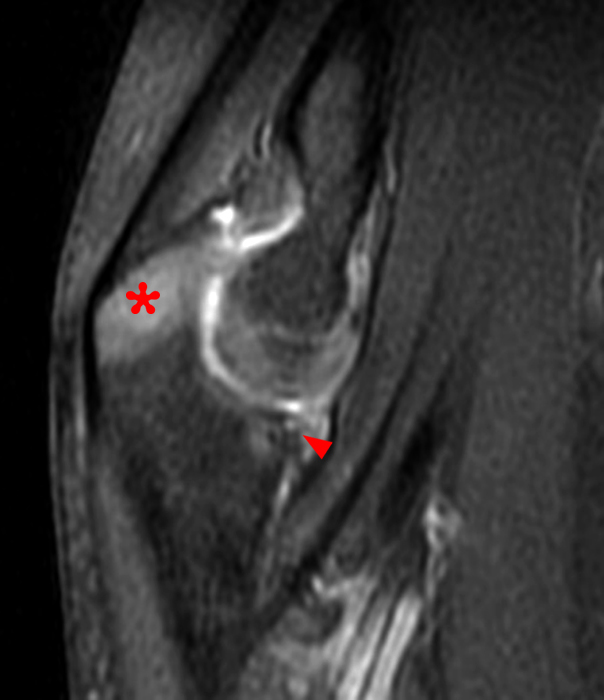
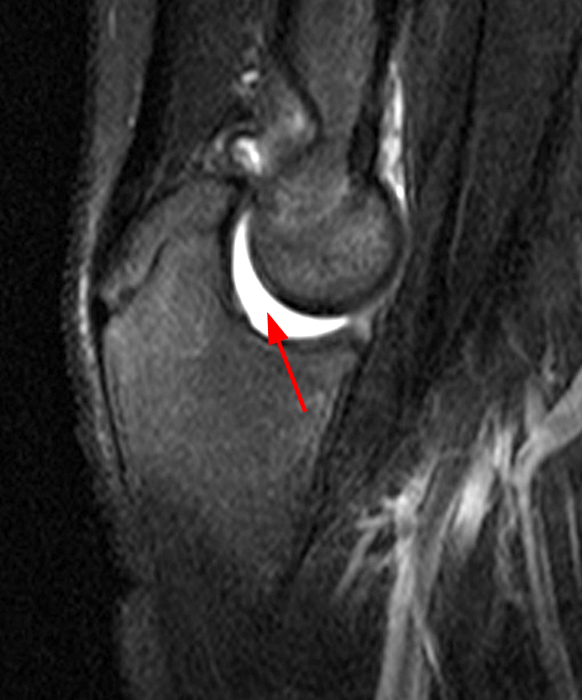
(2B) A coronal STIR image demonstrates complete disruption of the medial capsular structures and a small pericapsular hematoma. The common flexor tendon is retracted to the medial joint line (asterisk).
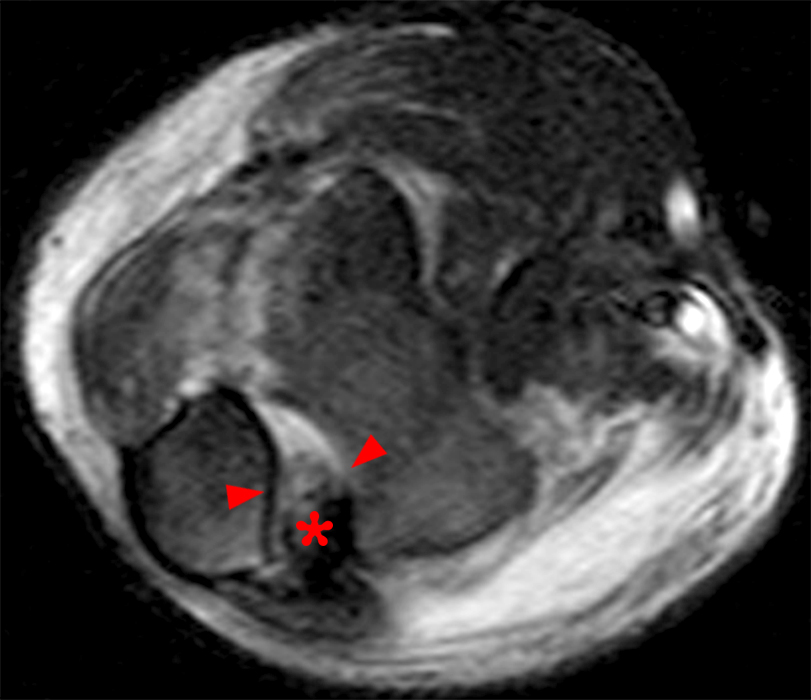
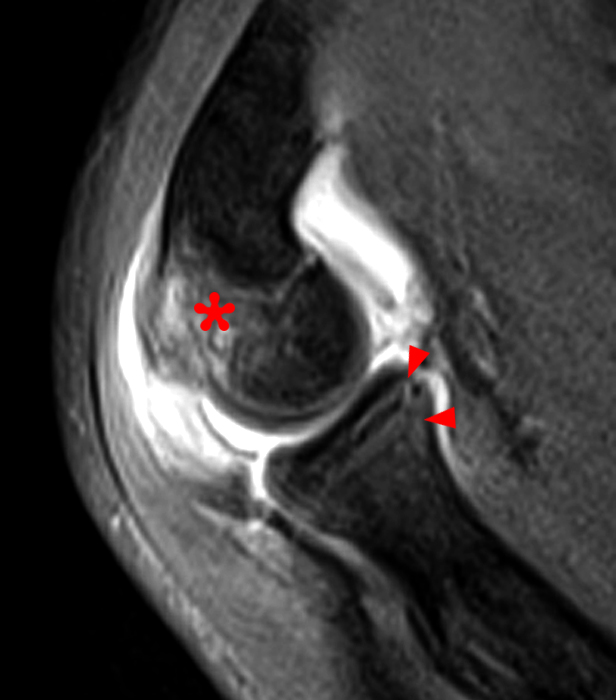
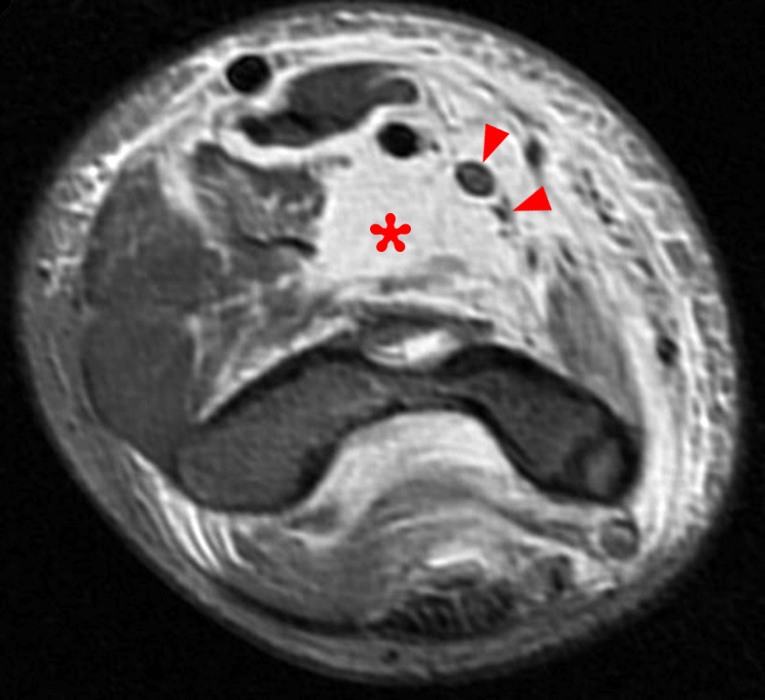
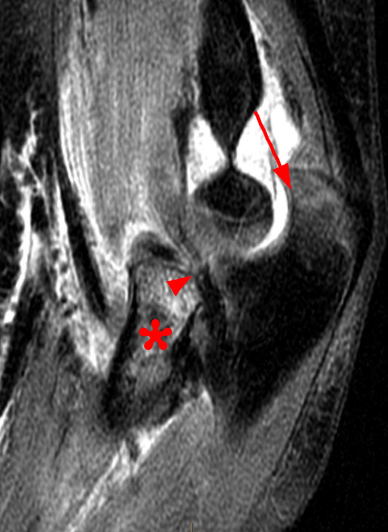
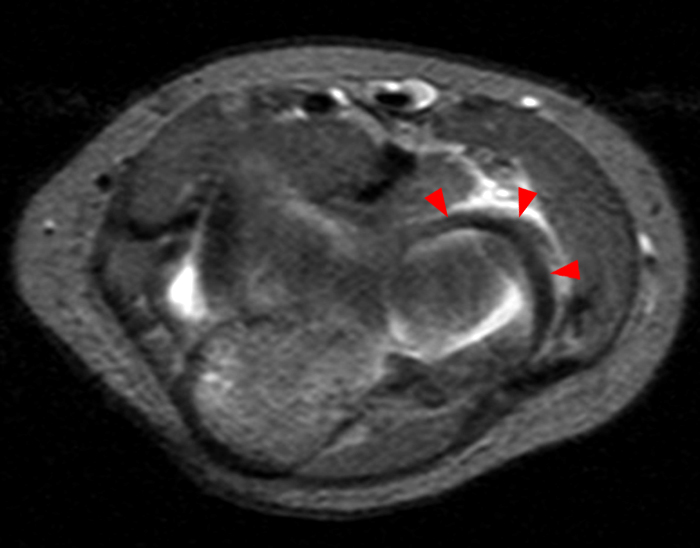
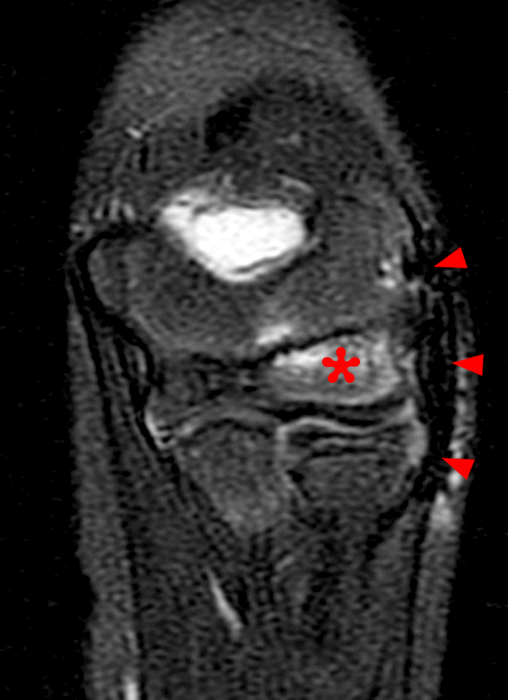
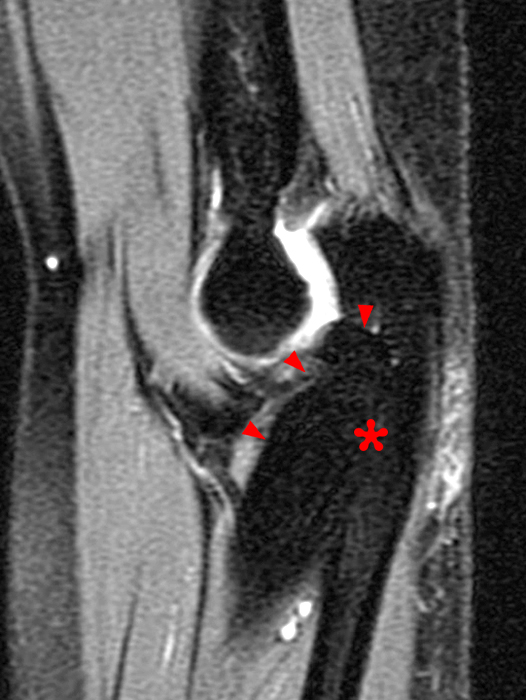
(2C) An axial fat-suppressed T2-weighted image at the level of the humeroulnar joint. Diffuse medial pericapsular fluid and edema are present. The joint is widened (arrowheads) with interposition of soft tissue (asterisk) between the articular surfaces.
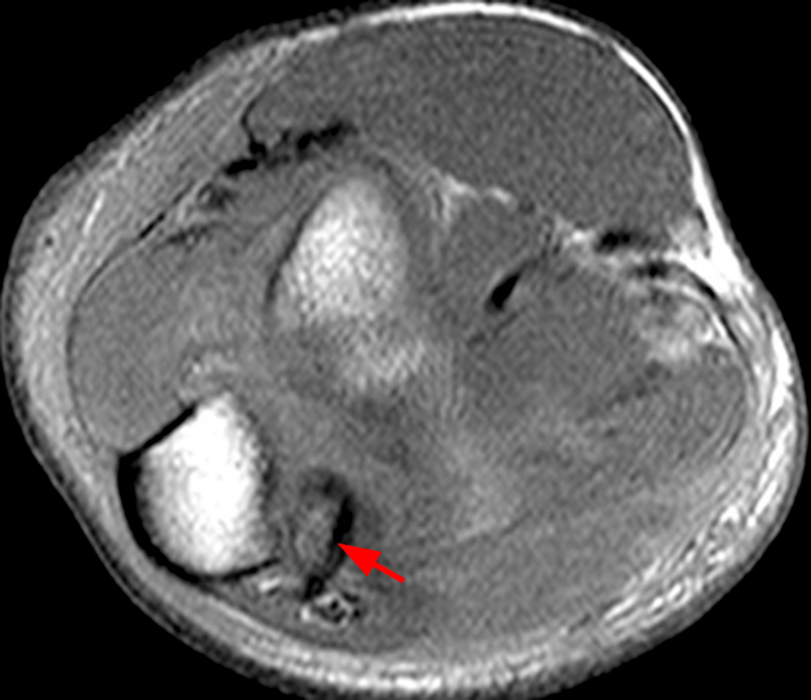
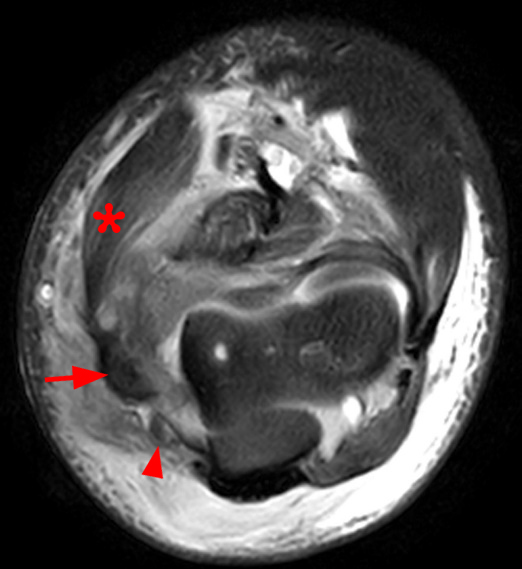
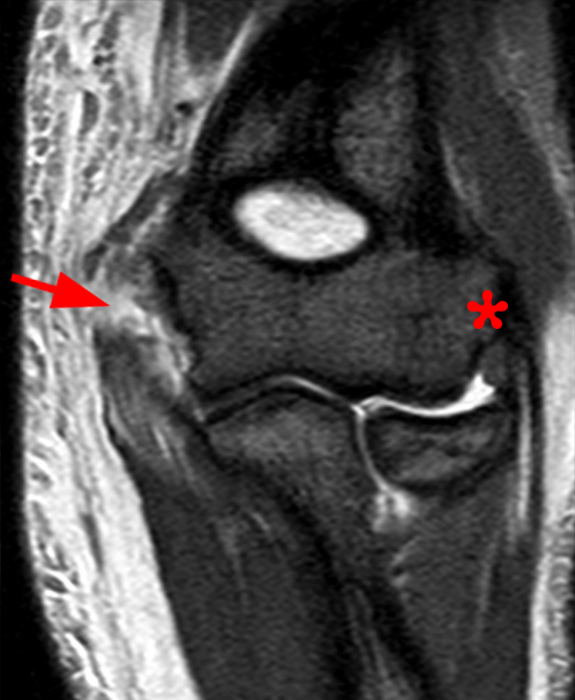
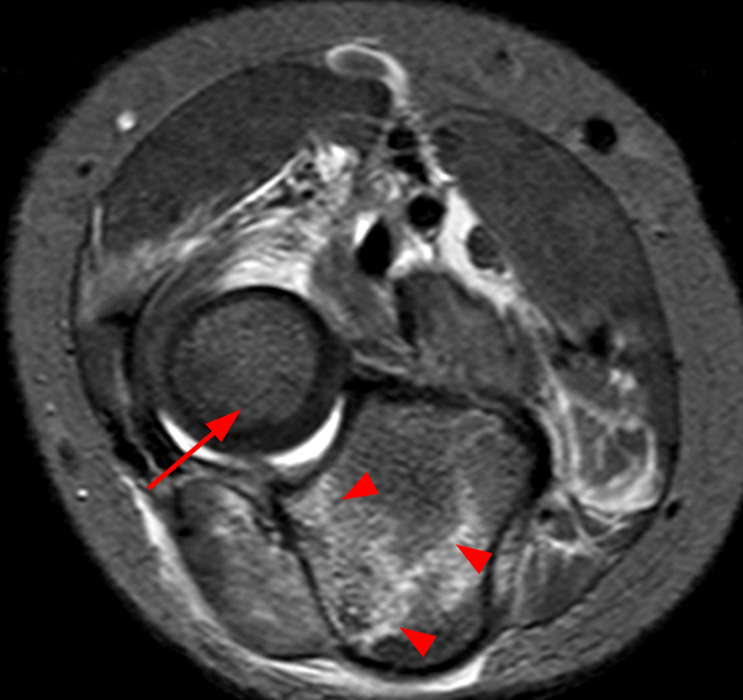
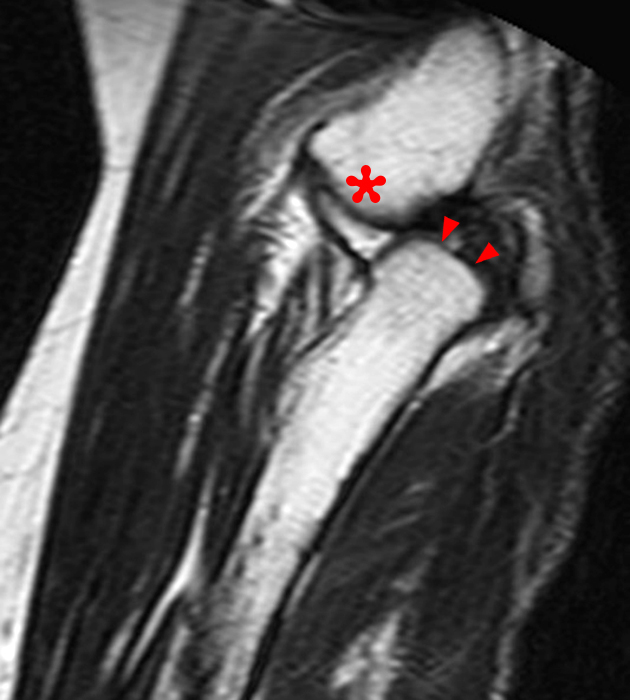
(2D) An axial T1-weighted image at the level of the humeroulnar joint just distal to the level on image 2C. An osseous fragment representing the avulsed medial humeral epicondyle (short arrow) is entrapped in the joint.
Diagnosis
Elbow dislocation with intraarticular entrapment of a medial humeral epicondyle fracture fragment.
Introduction
Elbow dislocation has an incidence of 5.21 per 100,000 persons per year in the U.S population and is more common in males and in younger individuals. The highest incidence is found in the 10 to 19-year age group (6.9 per 100 000 person per year) and are often related to sports, such as football, rollerblading, skateboarding, gymnastics, and wrestling.1 It is the most common large joint dislocation in children but constitutes only 3-5 % of all pediatric elbow injuries.2
Understanding of the mechanism and patterns of injury is important for accurate diagnosis and optimal treatment. The most common mechanism for elbow dislocation is falling on an outstretched, hyperextended upper extremity with axial compression, valgus stress and supination forces.3
The usual order of disruption of the supporting structures has previously been thought to extend circumferentially starting in the lateral aspect and ending in the medial aspect, however, MR imaging in patients with acute elbow dislocation has shown that a medial injury pattern is more common than lateral injuries, which suggests an initial strong valgus load and subsequent forces extending laterally.4
A less common mechanism is a direct impact on the posterior aspect of the ulna during elbow flexion with an anteriorly directed force, which could result in a radial head dislocation and proximal ulnar fracture, also known as the Monteggia injury. Four different types and additional mechanisms for this injury have been proposed.5
Sudden pulling on an upper extremity in a young child, typically age 1-4, can result in nursemaid’s elbow, or “pulled elbow”, which is due to a displacement of the annular ligament resulting in subluxation of the radius at the radiocapitellar joint.6 This is a common injury that is often recurrent and is frequently diagnosed based on history and clinical data.
Anatomically, elbow dislocations are classified based on the position of the proximal radioulnar joint with respect to the distal humerus and include posterolateral, posteromedial, anterior, and divergent types. The most common type is posterolateral dislocation.2
The classification should also address if it is a simple or complex dislocation. In a simple dislocation the injury is limited to the capsular and/or ligamentous structures, while in a complex dislocation, the surrounding osseous structures are also involved, such as the medial humeral epicondyle, radial head, coronoid process, and olecranon.7
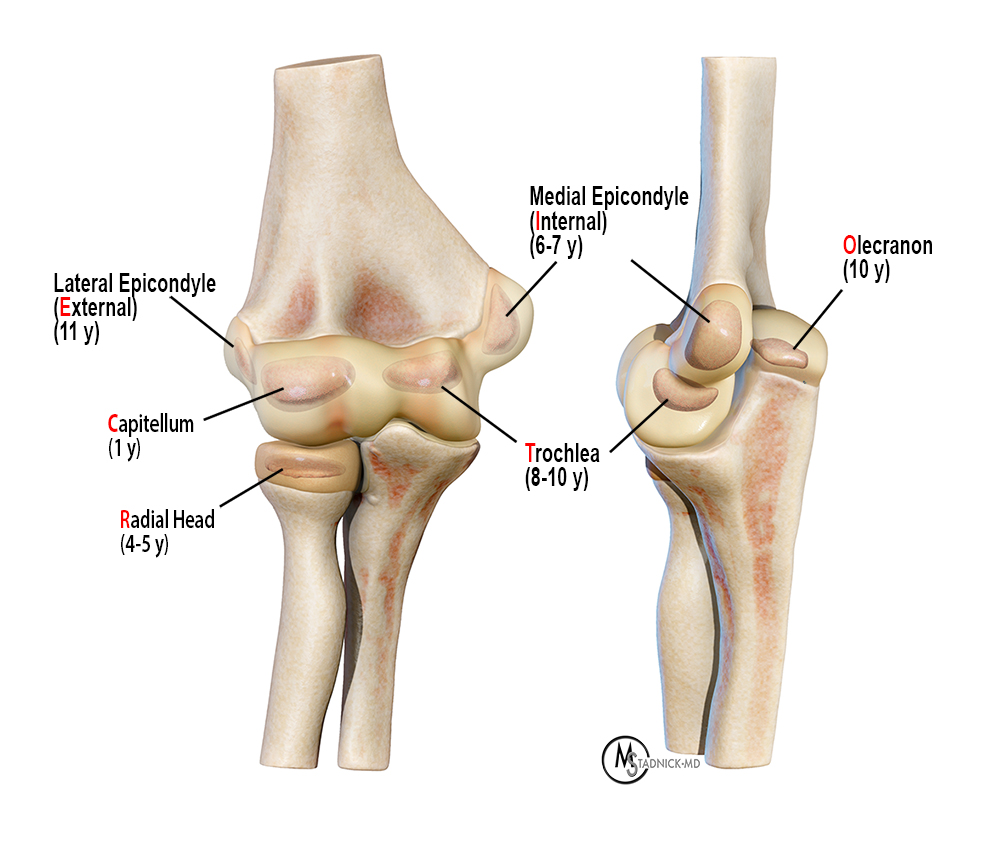
In children it is often difficult to obtain an accurate history and a good physical examination of the injured elbow, but a thorough search for neurovascular injury, specifically brachial artery and median and ulnar nerve injury must be part of the examination. The minimum standard radiographic evaluation includes a frontal view of the straight elbow and a lateral view of the flexed elbow. Oblique views and comparison with the contralateral elbow may be helpful.8 Accurate diagnosis may still be a challenge due to the multiple ossification centers which remain mostly cartilaginous until the age of 11-12 years. It is beyond the scope of this article to describe the radiographic evaluation of the elbow and the spectrum of elbow injuries.
MRI offers a way to evaluate elbow injuries more clearly because of its ability to depict unossified cartilage and the surrounding ligaments, muscles, and tendons. Patterns of injury on MRI can shed light on mechanics. The focus of this Web Clinic is on the spectrum of MR imaging findings in pediatric elbow dislocation. The Radsource June 2019 Web Clinic has an excellent overview of normal elbow anatomy and function.
Imaging Findings
Dislocation and medial humeral epicondylar fracture
The most common fractures in elbow dislocation in children involve the medial epicondyle, followed by the coronoid process and the radial neck. Of all pediatric elbow fractures the medial epicondyle is the third most common location (12%) after supracondylar and lateral condylar fractures and occur in the 8 to 15-year age group.9 Of all medial epicondylar fractures, an associated acute elbow dislocation is found in 30 to 55% of cases.10 The typical mechanism is hyperextension and valgus stress with traction forces on the medial epicondyle, which typically fails at the physis, the weakest link in the immature skeleton. Contraction of forearm muscles can result in displacement of the avulsed fragment and ulnar nerve injury at the adjacent cubital tunnel. In 5-18% of cases, the epicondyle may become entrapped within the ulnohumeral joint, which results in reduced joint mobility.11 Knowledge of the normal sequence of ossification of the distal humerus is important to avoid diagnostic errors on radiographs, because the displaced epicondylar fragment may be confused with the normal trochlear ossification center.12 Ossification of the trochlea before the medial epicondyle can occur but is extremely rare. Radiographs of the contralateral elbow may increase the accuracy in diagnosis.
Figure 4:
A 7-year-old who injured the elbow recently in a fall. An axial T2-weighted image at the level of the humeral condyles shows an avulsion of the medial epicondyle (short arrow). Contraction of the pronator teres muscle (asterisk) at the time of injury typically pulls the avulsed fragment proximally and medially. The ulnar nerve (arrowhead) is mildly enlarged and increased in signal consistent with contusion.
Simple dislocation
In simple elbow dislocations there are no fractures except for small periarticular avulsions measuring 1-2 mm at the most. Identification of soft tissue injury involving the lateral ulnar collateral and ulnar collateral ligaments, the anterior capsule, the origins of the common extensor and flexor tendons and the muscles that cross the elbow joint along with the pattern of bone marrow edema on MRI can give insights into the initial direction of elbow dislocation and can be helpful in the management and treatment.13 Joint incongruity on MRI related to tendon avulsions of the elbow have been found to be associated with chronic instability.13,14
Figure 5:
A 12-year-old boy who was involved in an altercation a week ago. The only finding on radiographs was a joint effusion. A coronal T2-weighted image demonstrates disruption of the anterior band of the ulnar collateral ligament (arrow). Avulsion of the lateral ulnar collateral ligament at the lateral humeral epicondyle (short arrow) and contusion of the capitellum (asterisk) are also present. The findings are consistent with a simple dislocation.
Figure 6:
(6A) A 9- year-old who fell recently. Radiographs showed a joint effusion, a tiny avulsed fragment at the distal margin of the medial epicondyle and diffuse soft tissue swelling and edema in the medial aspect. A T2-weighted sagittal image shows a large tear of the brachialis muscle with a wide gap (asterisk). The findings are consistent with a simple dislocation.
(6B) A T2-weighted axial image at the level of the distal humerus demonstrates the brachialis muscle defect with a hematoma (asterisk). The brachial artery and median nerve (arrow heads) are surrounded by fluid.
Figure 7:
(7A) 12-year-old girl with recent cheerleading injury. A coronal STIR image shows complete avulsion of the common flexor tendon (short arrow). There was also a large tear of the proximal pronator teres muscle (not shown). The lateral ulnar collateral ligament and the common extensor tendon are intact at the lateral epicondyle (asterisk).
(7B) A sagittal T2-weighted image demonstrates extensive capsular stripping at the distal humeral shaft (arrowhead) and a brachialis muscle strain at the humeral origin (arrows). The findings are consistent with a simple dislocation.
Figure 8:
A 10-year-old boy with history of two episodes of elbow dislocation. Radiographs were negative. A small focus of marrow edema and subtle deformity of the coronoid process (arrowhead), consistent with a subacute fracture, is demonstrated on a fat-suppressed proton-density-weighted sagittal image. The coronoid process in children is relatively small and does not have the same ability as in adults to resist posterior displacement of ulna. Note the unossified olecranon process (asterisk), not to be confused with a marrow abnormality or osseous injury.
Figure 9:
Divergent elbow dislocation in a 10- year-old boy who fell. A sagittal fat-suppressed T2-weighted image reveals anterior dislocation of the radial head (asterisk) and posterior subluxation of the ulna (arrow). There was an acute osteochondral fracture of the radial head (partially shown, arrowhead). This is an uncommon injury and occurs when the distal humerus is forced between the proximal radius and ulna.
Figure 11:
(11A) Frontal radiograph of the elbow in a 5-year-old child who refused to move the arm. The line bisecting the radial diaphysis does not align with the capitellum.
(11B) A fat-suppressed T2-weighted sagittal image shows proximal displacement of the annular ligament (arrowhead) with diffuse soft tissue edema, consistent with nursemaid elbow.
(11C) An axial T2-weighted image at the level of the radiocapitellar joint demonstrates diffuse thickening of the annular ligament (arrowheads) and pericapsular edema.
Treatment
The treatment of medial epicondylar fractures is controversial, but the outcome is generally good regardless of what type of treatment. Nondisplaced or minimally displaced fractures can be treated nonoperatively. If displacement is more than 15 mm, operative fixation utilizing K-wires is the treatment of choice, but the accuracy of measurements based on radiographs has been questioned.15 Surgery is also required for open dislocation and significant joint instability.
In most cases of simple elbow dislocation, satisfactory results are achieved by closed reduction. Standard treatment then includes immobilization for 1-2 weeks in a long arm splint with the elbow in 90 degrees of flexion followed by early mobilization including early active range of motion. After two weeks the splint can be removed and physical therapy can start if the elbow is stable. Prolonged immobilization should be avoided.16
Complications of pediatric elbow dislocations
Loss of elbow extension is the most common complication following elbow dislocation and related to prolonged immobilization, but children generally do better than adults and have a greater chance of regaining normal range of motion.17
Transient ulnar neuropathy is present in 10%. Median nerve entrapment, brachial artery injury and compartment syndrome are rare complications.2,18
Heterotopic periarticular ossification/myositis ossificans is common but rarely limits range of motion. In cases of restricted motion surgical excision may be necessary, but it is recommended to wait until the ossification has matured.16
Chronic instability after elbow dislocation can manifest itself as valgus instability or recurrent dislocation. Valgus instability is a result of nonunion or malunion of a medial epicondylar fracture and ulnar collateral ligament insufficiency and recurrent episodes of dislocation are related to lateral ulnar collateral ligament failure. Both entities often require ligament reconstruction.19
Figure 14:
11-year-old boy with a history of two episodes of elbow dislocation and coronoid process fracture. Lateral ulnar collateral ligament repair had been performed (arrowheads), but the patient presented with a new injury after minor trauma. A coronal T2-weighted image shows diffuse contusive changes of the capitellum (asterisk) consistent with recurrent dislocation. The reconstructed ligament remains intact (arrowheads).
Figure 15:
13-year-old boy with persistent elbow popping and pain during pitching and wrestling after elbow dislocation 3 years prior. He had been treated with closed reduction. The T2-weighted sagittal image shows mild widening and incongruity of the ulnohumeral spaces (arrow) consistent with chronic instability.
Differential diagnosis
Congenital dislocation of the radial head may be an isolated anomaly or occur with other conditions, such as scoliosis, anomalies of the lower extremities and mental retardation. Hereditary cases are typically autosomal dominant. The dislocation is posterior in 65%, anterior in 18% and lateral in 17%. Bilateral congenital dislocations can occur. The capitellum is hypoplastic, the radial head is flat or dome-shaped and the proximal radius has a tapered configuration. Radioulnar synostosis can coexist with congenital dislocation of the radial head. Chronic radial head dislocation in a Monteggia injury could result in osseous remodeling, which could cause diagnostic difficulties, but usually the deformity in traumatic dislocation is not as severe as in the congenital type.20
Figure 16:
(16A) A T2-weighted sagittal image shows congenital posterior dislocation of the radial head in an older adult. The radial head is convex (arrowhead) and the capitellum is relatively small (asterisk).
(16B) Radial synostosis shown in a young adult on a T2-weighted sagittal image. The proximal radius is fused with the ulna (asterisk) and is posteriorly dislocated (arrowheads) with respect to the capitellum.
Conclusion
Pediatric elbow dislocations are in many aspects similar to adult elbow dislocations and include simple and complex types. A common associated injury in children is avulsion fracture of the medial epicondyle, which is the last ossification center in the distal humerus to fuse. Diagnostic difficulties can arise when the avulsed fragment is incarcerated in the joint and knowledge of the normal order of appearance of ossification centers on radiographs is essential to avoid mistakes. MRI may aid in the diagnosis and can identify associated injuries, such as ulnar nerve contusion. MRI also provides a means of gaining information regarding the integrity of ligaments, tendons, joint capsule, muscles, and cartilage in elbow dislocation. The patterns of injury may enhance the understanding of the mechanics which in turn can lead to improvements in patient management and outcome.
References
- Stoneback, Jason W. MD1; Owens, Brett D. MD2; Sykes, Joshua MD1; Athwal, George S. MD, FRCSC3; Pointer, Lauren MS4; Wolf, Jennifer Moriatis MD5 Incidence of Elbow Dislocations in the United States Population, The Journal of Bone & Joint Surgery: February 1, 2012 – Volume 94 – Issue 3 – p 240-245 doi: 10.2106/JBJS.J.01663 ↩
- Lins RE, Simovitch RW, Waters PM. Pediatric elbow trauma. Orthop Clin North Am. 1999 Jan;30(1):119-32. doi: 10.1016/s0030-5898(05)70066-3. PMID: 9882730. ↩
- Wyrick, John D. MD; Dailey, Steven K. MD; Gunzenhaeuser, Jacob M. MD; Casstevens, E. Christopher MD Management of Complex Elbow Dislocations, Journal of the American Academy of Orthopaedic Surgeons: May 2015 – Volume 23 – Issue 5 – p 297-306 ↩
- Schreiber JJ, Potter HG, Warren RF, Hotchkiss RN, Daluiski A. Magnetic resonance imaging findings in acute elbow dislocation: insight into mechanism. The Journal of hand surgery. 2014 Feb 1;39(2):199-205. ↩
- Wiley JJ, Galey JP. Monteggia injuries in children. The Journal of bone and joint surgery. British volume. 1985 Nov;67(5):728-31. ↩
- Petrushin AL, Bragina SV, Berezin PA. Current views on radial head subluxation. Pediatric Traumatology, Orthopaedics and Reconstructive Surgery. 2019;7(4):113-24. ↩
- Hildebrand KA, Patterson SD, King GJ. Acute elbow dislocations: simple and complex. Orthop Clin North Am. 1999 Jan;30(1):63-79. doi: 10.1016/s0030-5898(05)70061-4. PMID: 9882725. ↩
- John SD, Wherry K, Swischuk LE, Phillips WA. Improving detection of pediatric elbow fractures by understanding their mechanics. Radiographics. 1996 Nov;16(6):1443-60. ↩
- Pathy, Rubini; Dodwell, Emily R. Medial epicondyle fractures in children, Current Opinion in Pediatrics: February 2015 – Volume 27 – Issue 1 – p 58-66 ↩
- Louahem DM, Bourelle S, Buscayret F, Mazeau P, Kelly P, Dimeglio A, Cottalorda J. Displaced medial epicondyle fractures of the humerus: surgical treatment and results. A report of 139 cases. Archives of orthopaedic and trauma surgery. 2010 May 1;130(5):649-55. ↩
- Tarallo L, Mugnai R, Fiacchi F, Adani R, Zambianchi F, Catani F. Pediatric medial epicondyle fractures with intra-articular elbow incarceration. Journal of Orthopaedics and Traumatology. 2015 Jun;16(2):117-23. ↩
- Shrader MW. Pediatric supracondylar fractures and pediatric physeal elbow fractures. Orthop Clin North Am. 2008 Apr;39(2):163-71, v. doi: 10.1016/j.ocl.2007.12.005. PMID: 18374807. ↩
- Schnetzke M, Ellwein A, Maier D, Wagner FC, Grützner PA, Guehring T. Injury patterns following simple elbow dislocation: radiological analysis implies existence of a pure valgus dislocation mechanism. Archives of orthopaedic and trauma surgery. 2021 Oct;141(10):1649-57. ↩
- Hackl M, Wegmann K, Ries C, Leschinger T, Burkhart KJ, Müller LP. Reliability of Magnetic Resonance Imaging Signs of Posterolateral Rotatory Instability of the Elbow. J Hand Surg Am. 2015 Jul;40(7):1428-33. doi: 10.1016/j.jhsa.2015.04.029. PMID: 26095056. ↩
- Pezzutti, Dante BS*; Lin, James S. MD*; Singh, Satbir BS*; Rowan, Mallory BS*; Balch Samora, Julie MD, PhD*,† Pediatric Medial Epicondyle Fracture Management: A Systematic Review, Journal of Pediatric Orthopaedics: September 2020 – Volume 40 – Issue 8 – p e697-e702 doi: 10.1097/BPO.0000000000001532 ↩
- Layson J, Best BJ. Elbow Dislocation. In: StatPearls. StatPearls Publishing, Treasure Island (FL); 2020. PMID: 31747224. ↩
- Cohen MS, Hill Hastings II. Acute elbow dislocation: evaluation and management. JAAOS-Journal of the American Academy of Orthopaedic Surgeons. 1998 Jan 1;6(1):15-23. ↩
- Carlioz H, Abols Y. Posterior dislocation of the elbow in children. J Pediatr Orthop. 1984 Jan;4(1):8-12. doi: 10.1097/01241398-198401000-00002. PMID: 6693573. ↩
- Kozin SH, Abzug JM, Safier S, Herman MJ. Complications of pediatric elbow dislocations and Monteggia fracture-dislocations. Instr Course Lect. 2015 Jan 1;64(6):493-8. ↩
- Stein-Wexler R, Wootton-Gorges SL, Ozonoff MB, editors. Pediatric orthopaedic imaging. Springer; 2014 Dec 8.p 174-8 ↩