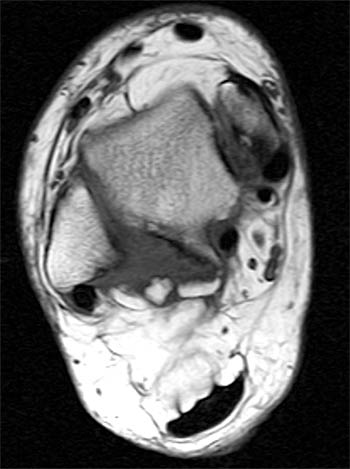
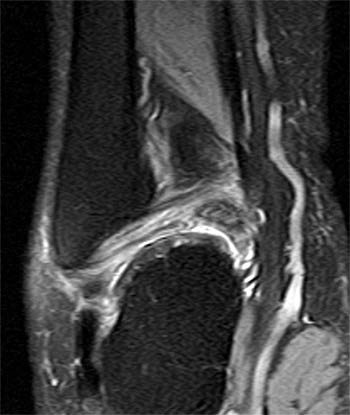
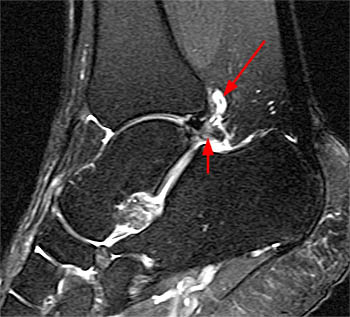
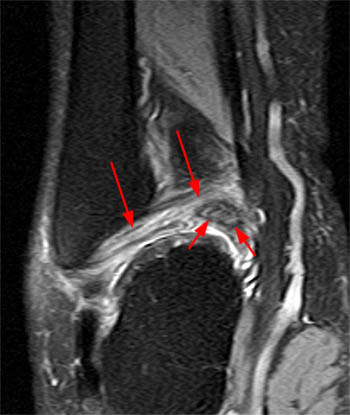
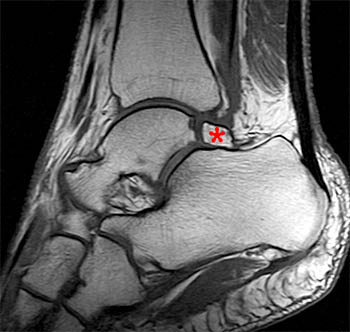
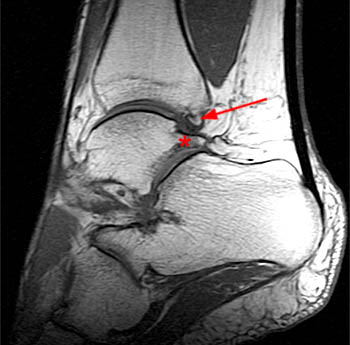
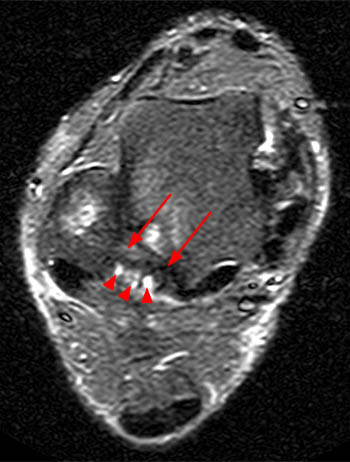
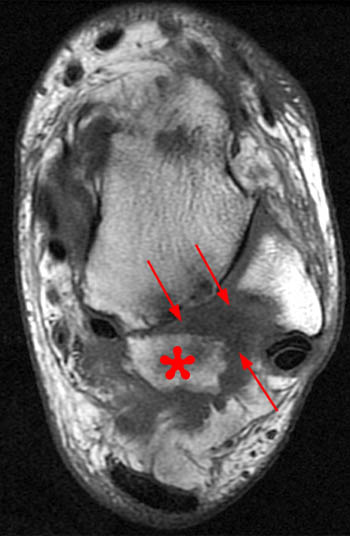
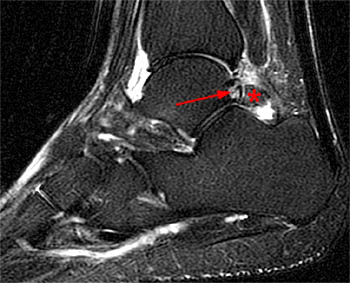
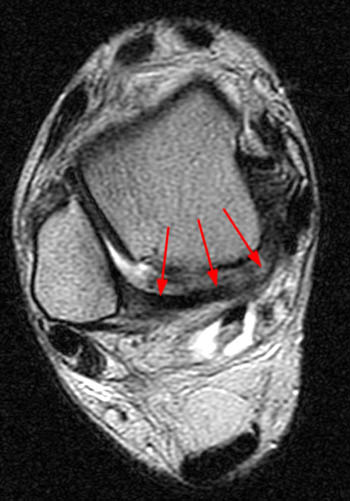
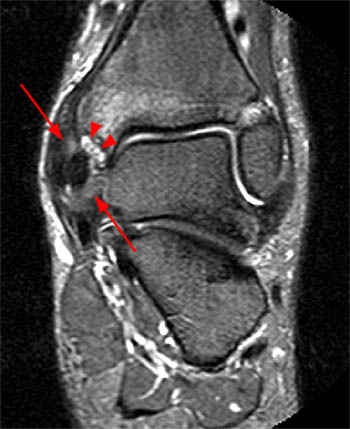
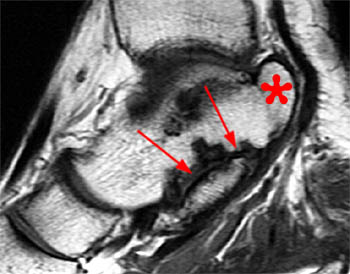
Clinical History: A 48 year-old female presents with persistent lateral ankle pain and edema 5 months following trauma. (1a) Sagittal T2-weighted with fat-saturation, (1b) axial T1-weighted, and (1c) coronal intermediate-weighted with fat-saturation images of the right ankle are provided. What are the findings? What is your diagnosis?
Findings
Diagnosis
Posterior Ankle Impingement (Os Trigonum Syndrome)
Introduction
Ankle impingement is defined as entrapment of an anatomic structure that leads to pain and decreased range of motion of the ankle, and can be classified as either soft tissue or osseous.1 Posterior ankle impingement syndrome refers to a group of abnormal entities that result from repetitive or acute forced plantar flexion of the foot.2 Posterior ankle impingement is more common in ballet dancers and soccer players though it can be seen in any patient active in sports.
Clinical Presentation
Patients who have posterior impingement complain of chronic deep posterior ankle pain worsened by forced plantar flexion or push-off forces as occur during activities such as ballet dancing, jumping, or running downhill. In such positions, compression of soft tissue or bony structures between the posterior aspect of the distal tibia and calcaneus or between the posterior tibia and the posterolateral process of the talus can occur. In some patients, forced dorsiflexion is also painful. In this dorsiflexed position, traction is applied to the posterior joint capsule and posterior talofibular ligament, which both attach to the posterolateral talar process.3
Physical examination reveals pain on palpation over the posterolateral talar process, which is located along the posterolateral aspect of the ankle between the Achilles and peroneal tendons. Passive forced plantar flexion results in pain and often a grinding sensation as the posterolateral talar process is entrapped between the posterior tibia and calcaneus. The diagnosis can be confirmed if pain abates following injection of an anesthetic into the posterolateral capsule of the tibiotalar joint.3,4
Normal Anatomy
Normal and variant anatomy at the posterior aspect of the ankle are important in the development of posterior ankle impingement (5a). A groove containing the flexor hallucis longus tendon along the posterior talus separates the medial and lateral tubercles of the posterior talus. The medial talocalcaneal and posterior tibiotalar ligaments insert upon the medial tubercle, whereas the lateral tubercle contains the attachment site of the posterior talofibular ligament. An intermalleolar ligament is present in most individuals, most commonly coursing from the medial malleolus to the lateral malleolus near the fibular attachment of the posterior talofibular ligament.
The lateral tubercle of the talus, when elongated, is referred to as Stieda’s process (7a,8a). In addition, the lateral tubercle may articulate with a separate ossification center known as the os trigonum (6a). The os trigonum is corticated and articulates with the lateral tubercle via a synchondrosis. The posterior surface of the os trigonum is non-articular but serves as a point of attachment for capsuloligamentous structures, in particular the posterior talofibular and posterior talocalcaneal ligaments.6
Figure 5:
This 3-D graphic representation of the posterior ankle depicts normal anatomy: os trigonum (OT), flexor hallucis longus (FHL), flexor digitorum longus (FDL), tibialis posterior (TP), posterior inferior tibiofibular ligament (PITFL), inferior transverse ligament (ITL), intermalleolar ligament (IML), posterior talofibular ligament (PTF), calcaneofibular ligament (CCF), posterior tibiotalar ligament (PTTL), peroneus longus (PL), and peroneus brevis (PB).
Mechanism of Injury
Posterior ankle impingement may complicate an acute traumatic plantar hyperflexion event, such as an ankle sprain, or may be related to repetitive low-grade trauma associated with plantar hyperflexion, especially as can be seen in the female ballet dancer. It is important to differentiate between these two, because posterior impingement from overuse has a better prognosis,7 in part because of other injuries that may be sustained after an acute traumatic event.3
The anatomy of the posterior aspect of the ankle is a key factor in the occurrence of posterior impingement syndrome. The more common causes are osseous in nature, such as the os trigonum, an elongated posterolateral tubercle of the talus (Stieda’s process), a downward sloping posterior lip of the tibia, an osteophyte from the posterior distal tibia (9a), or a prominent posterior process of the calcaneus.2,8 However, posterior impingement can also be soft tissue related, as with a thickened posterior joint capsule (10a), posttraumatic scar tissue, posttraumatic calcifications of the posterior joint capsule, or loose bodies in the posterior part of the ankle joint. Any of these structures may become compressed during plantar hyperflexion.3
Pain may result from osseous structures of the posterior ankle impacting on one another (posterolateral talar process against the posterior tibial plafond or against the posterior calcaneal process) (11a) or from the compression of soft tissues between the two opposing osseous structures.9 Symptoms for all of these conditions relate to physical impingement of osseous or soft tissue structures, resulting in painful limitation of the full range of ankle movement.
The most common cause of posterior impingement is the presence of an os trigonum. The mineralized os trigonum appears between the ages of 7 and 13 years and usually fuses with the talus within 1 year, forming the trigonal (Stieda) process. It may remain as a separate ossicle in 7-14% of patients, and is often bilateral.10 An os trigonum can be a focus of osseous abutment against other structures. Pain can also be caused by disruption of the cartilaginous synchondrosis between the os trigonum and the lateral talar tubercle as a result of repetitive microtrauma and chronic inflammation.11
Soft tissue impingement usually results from scarring and fibrosis associated with synovial, capsular, or ligamentous injury.9 The capsular soft tissues involved in the setting of posterior ankle impingement include the posterior capsule and the posterior talofibular, intermalleolar, and tibiofibular ligaments. It is thought that the syndrome usually manifests clinically when a significant soft-tissue component forms.12 The soft-tissue component can consist of synovial thickening throughout the posterior capsule or be more focal, involving the posterior intermalleolar or talofibular ligament.13,14 The flexor hallucis longus tendon runs in the groove between the lateral and medial processes of the talus and can also be injured in posterior impingement, resulting in stenosing tenosynovitis.11,12
MRI Findings
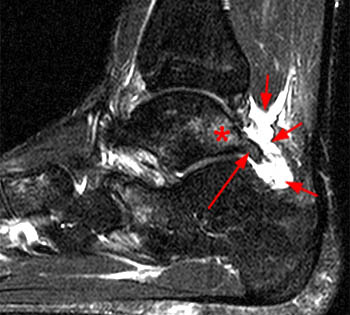
MR imaging is useful in establishing the diagnosis of posterior ankle impingement syndrome. Numerous MR findings have been described in association with posterior ankle impingement or os trigonum syndrome. (12a,13a) These findings include bone marrow edema located with the posterior talus, the posterolateral talar process, and/or in an os trigonum, fluid surrounding an os trigonum, fluid in the os synchondrosis, downward sloping and marrow edema of the posterior tibia, and a prominent posterior calcaneal process with marrow edema.2,11,15,16 The marrow edema in posterior impingement is believed to be the result of bone impaction and thus represents bone contusions or occult fractures.2,8
MR imaging also depicts inflammatory changes in the soft tissues of the posterior ankle-namely, the posterior synovial recess of the subtalar and tibiotalar joints2,8 with posterior capsular thickening, a fluid-distended posterior joint space, and increased T2-weighted signal along the posterior margin of the ankle indicative of synovitis.2,11,15,16 Synovitis is often centered on the posterior talofibular ligament and may extend to involve the posterior recess of the ankle or the subtalar joint and the flexor hallucis longus tendon sheath. Occasionally, a localized proliferative synovitis in the posterior recess of the ankle or subtalar joint may cause posterior impingement symptoms.5 The combined presence of bone marrow edema and posterior ankle synovitis suggests the diagnosis of posterior ankle impingement.2,8
Detection of an abnormal posterior intermalleolar ligament on MR imaging requires visualization of a thickened posterior intermalleolar ligament that can readily be separated from the surrounding posterior talofibular ligament and the transverse inferior tibiofibular ligament.13 (14a) Concurrent injury to the flexor retinaculum may result in partial scar encasement of the posterior tibial tendon between the retinaculum and the scarred posterior talotibial ligament.17,18
An os trigonum is usually easily identified on MR imaging. The synchondrosis may vary in orientation from coronal to oblique sagittal, the latter often not evident on sagittal images and only appreciable on straight axial images. When present, the synchondrosis should be evaluated for fluid signal intensity, indicating destabilization. Assessment should also be made for the presence of bone marrow edema at the synchondrosis margins and adjacent synovitis in the posterior recesses of the ankle and posterior subtalar joint. When present, these findings are suggestive of active posterior impingement, without being totally specific. Cystic change at the synchondrosis margins indicates a degree of chronic stress across the synchondrosis.5
Differential Diagnosis
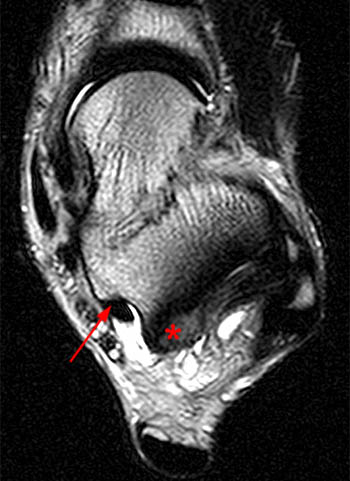
Posterior ankle impingement can be confused with the similar clinical entity of posteromedial ankle impingement syndrome. In this condition a patient experiences chronic posteromedial ankle pain following a severe ankle inversion injury resulting in a crushing injury of the deep posterior fibers of the deltoid ligament complex between the medial talus and the medial malleolus.9 Initially there is edema with subsequent immature scarring of the posterior talotibial ligament, with some protrusion into the posteromedial gutter, and an overlying posttraumatic synovitis with thickening of and displacement of the posteromedial ankle capsule.19 This leads to the formation of scar tissue and fibrosis located along the posteromedial joint line that becomes entrapped between the posterior talus and medial malleolus. (15a,16a) Posteromedial ankle impingement may exist as an isolated injury but most often coexists with symptoms of anterolateral ankle pain and instability. If the lesion remains unrecognized and untreated, posteromedial ankle impingement may result in persistent pain following lateral ankle reconstruction.19,20 On axial MR imaging, there is usually loss of the normal striated appearance of the posterior talotibial ligament and protrusion of scar response and synovitis into the medial gutter posteriorly, with loss of the normal clear space in the posteromedial gutter between the levels of the flexor digitorum longus and flexor hallucis longus tendons and thickening of the posteromedial ankle capsule.5
Numerous other clinical entities can mimic posterior impingement, including talar and calcaneal fractures (17a,18a), Achilles tendinopathy, isolated flexor hallucis longus tendinopathy, retrocalcaneal bursitis, Haglund’s deformity, posterior tibial osteochondral injuries, tarsal coalition, and tarsal tunnel syndrome.4
Treatment
Initial treatment of posterior impingement consists of rest, ice, and non-steroidal anti-inflammatory medications. Injection of steroids, perhaps under ultrasound guidance, is also effective for symptom relief and for reduction of swelling. If conservative measures fail, operative treatment may be recommended. Areas of soft-tissue impingement are debrided. Bone spurs or an os trigonum are resected, typically in an open procedure in light of the proximity of the sural nerve, tibial nerve, and flexor hallucis longus tendon. In general, operative results are excellent, as the offending structures that caused the mechanical impingement have been removed. Many athletes are able to resume running four to six weeks after surgery.
Conclusion
Posterior ankle impingement should always be included in the differential diagnosis when evaluating a patient with chronic, deep posterior ankle pain, particularly in the very active patient or in a patient with a previous ankle injury. The pathology associated with it as well as potential other pathology is well demonstrated with MRI. Identification of the offending structures via MRI provides a valuable roadmap in cases where operative intervention becomes necessary.
References
1 Van Den Bekerom MPJ, Raven EEJ. The distal fascicle of the anterior inferior tibiofibular ligament as a cause of tibiofibular impingement syndrome: a current concepts review. Knee Surg Sports Traumatol Arthrosc 2007;15:465-71
2 Bureau NJ, Cardinal E, Hobden R, Aubin B. Posterior ankle impingement syndrome: MR imaging findings in seven patients. Radiology 2000;215: 497-503
3 Van Dijk NC. Anterior and Posterior Ankle Impingement. Foot Ankle Clin N Am 2006;11:663-683
4 Maquirriain J. Posterior ankle impingement. J Am Acad Orthop Surg 2005;13:365-71
5 Linklater J. MR Imaging of Ankle Impingement Lesions. Magn Reson Imaging Clin N Am 2009;17:775-800
6 Marotta JJ, Micheli LJ. Os trigonum impingement in dancers. Am J Sports Med 1992;20:533-536
7 Stibbe AB, Van Dijk CN, Marti RK. The os trigonum syndrome. Acta Orthop Scand 1994;(Suppl 262):59-60
8 Robinson P, White LM. Soft-tissue and osseous impingement syndromes of the ankle: role of imaging in diagnosis and management. RadioGraphics 2002;22:1457-1469
9 Sanders TG, Rathur SK. Impingement Syndromes of the Ankle. Magn Reson Imaging Clin N Am 2008;16:29-38
10 Lawson JR Clinically significant radiologic anatomic variants of the skeleton. AJR i994;1 63:249-255
11 Karasick D, Schweitzer ME. The Os Trigonum Syndrome: Imaging Features. AJR 1996;166:125-129
12 Hamilton WG, Geppert MJ, Thompson FM. Pain in the posterior aspect of the ankle in dancers: differential diagnosis and operative treatment. J Bone Joint Surg Am 1996; 78:1491-1500
13 Fiorella D, Helms CA, Nunley JA II. The MR imaging features of the posterior intermalleolar ligament in patients with posterior impingement syndrome of the ankle. Skeletal Radiol 1999; 28:573-576
14 Rosenberg ZS, Cheung YY, Beltran J, Sheskier S, Leong M, Jahss M. Posterior intermalleolar ligament of the ankle: normal anatomy and MR imaging features. AJR Am J Roentgenol 1995; 165: 387-390
15 Peace KAL, Hillier JC, Hulme A, et al. MRI features of posterior ankle impingement syndrome in ballet cancers: a review of 25 cases. Clin Radiol 2004; 59:1025-33
16 Wakeley CJ, Johnson DP, Watt I. The value of MR imaging in the diagnosis of the os trigonum syndrome. Skeletal Radiol 1996;25:133-136
17 Koulouris G, Connell D, Schneider T, et al. Posterior tibiotalar ligament injury resulting in the posteromedial impingement. Foot Ankle Int 2003;24:575-83
18 Messiou C, Robinson P, O’Connor PJ, et al. Subacute posteromedial impingement of the ankle in athletes: MR imaging evaluation and ultrasound guided therapy Skeletal Radiol 2006;35:88-94
19 Paterson RS, Brown JN. The posteromedial impingement lesion of the ankle. A series of six cases. Am J Sports Med 2001;29(5):550-7
20 Liu SH, Mirzayan R. Posteromedial ankle impingement. Arthroscopy 1993;9:709-11