Clinical History:
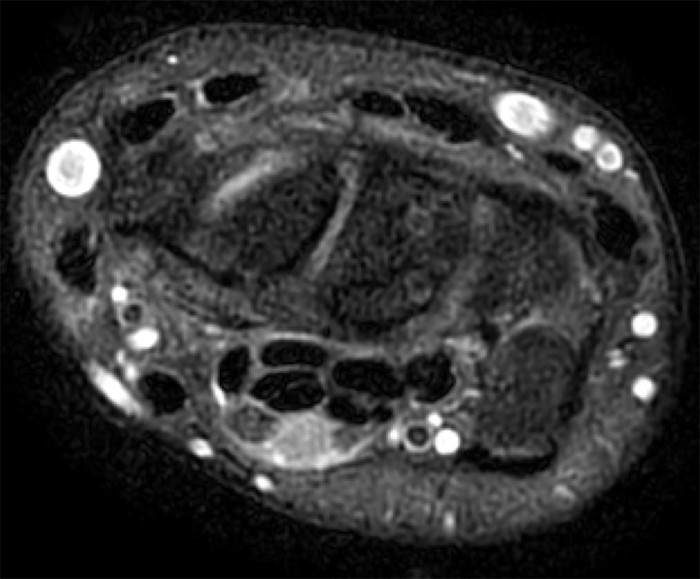
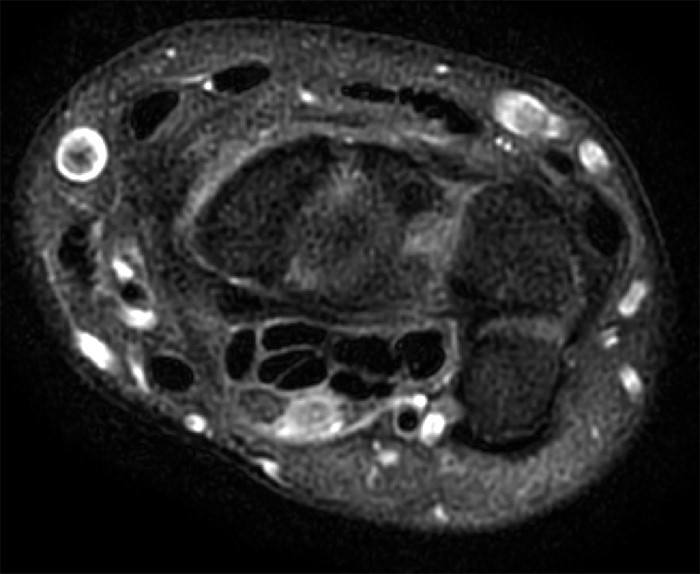
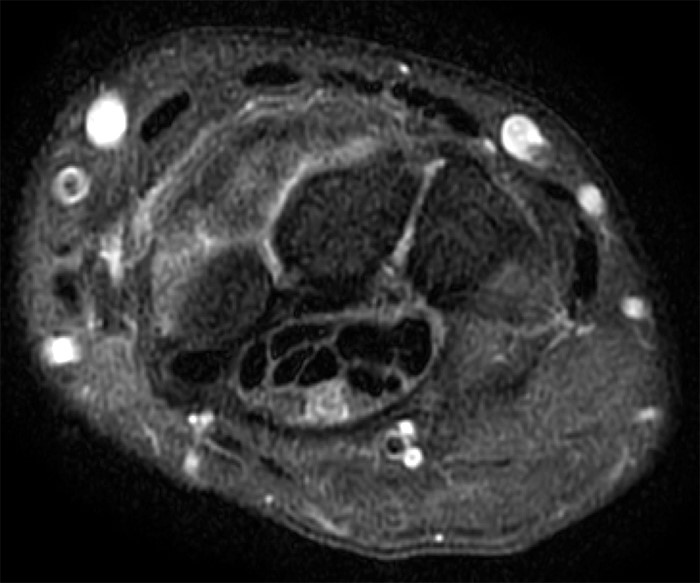
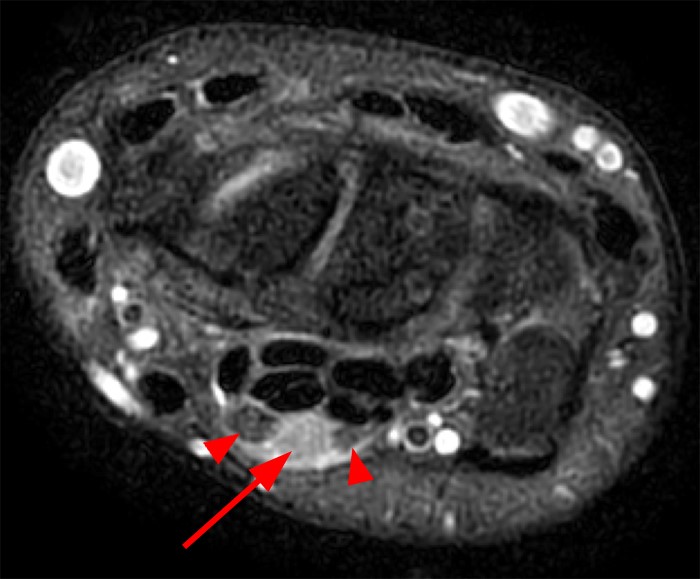
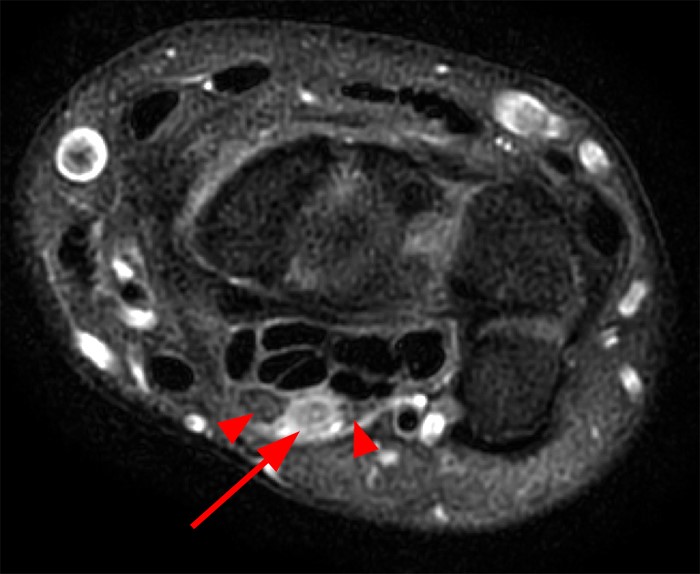
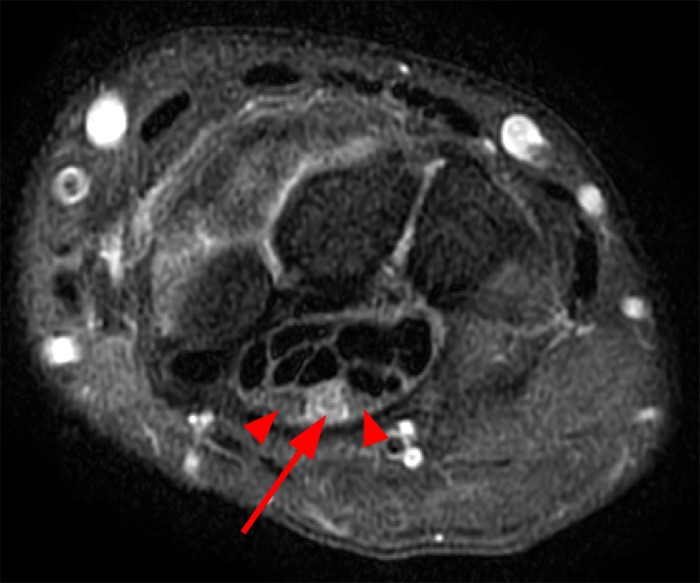
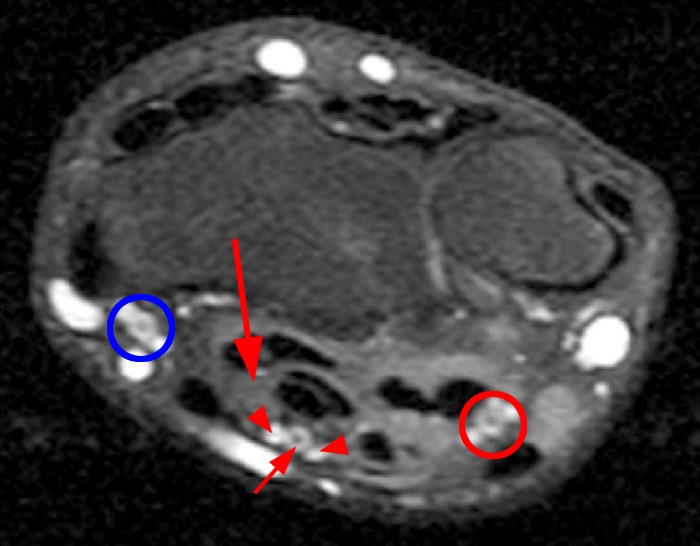
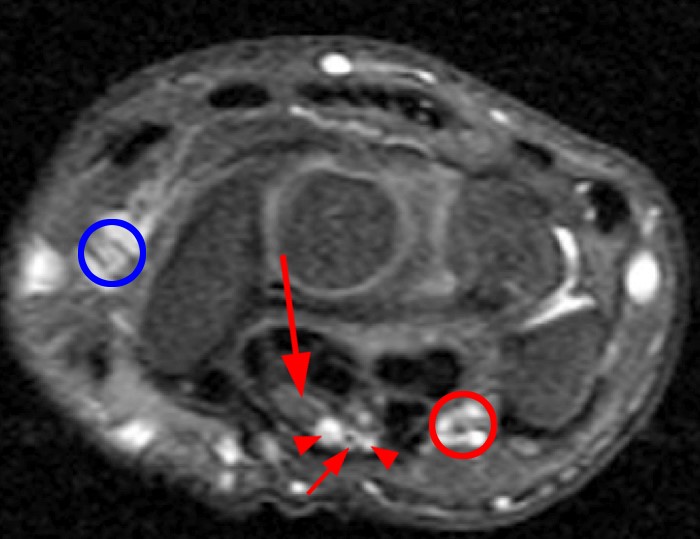
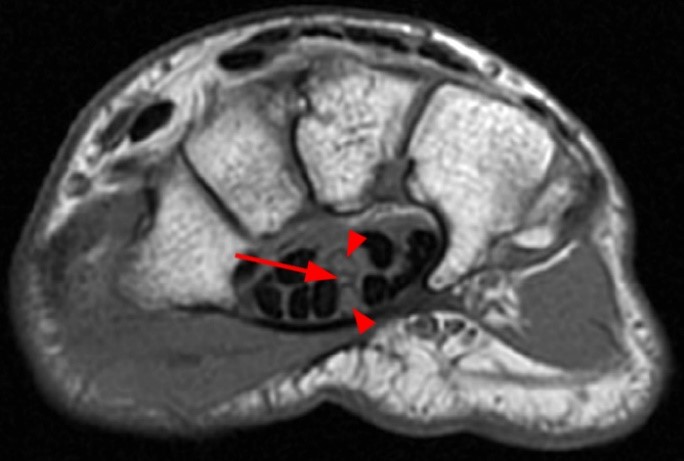
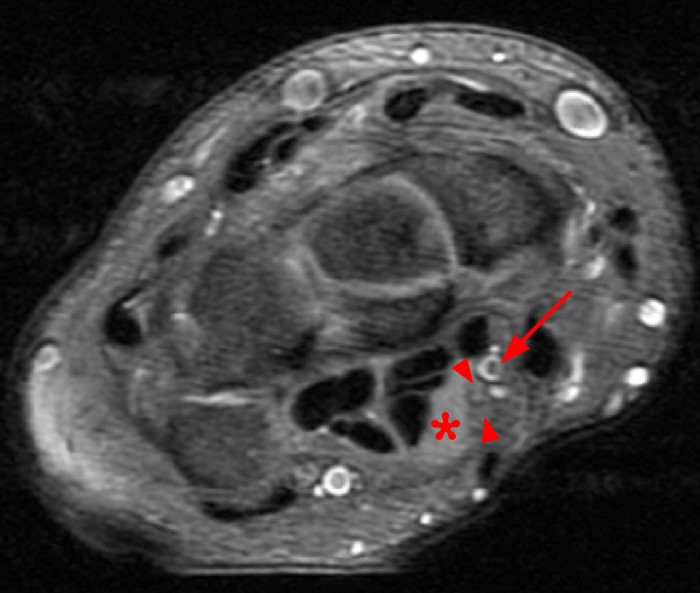
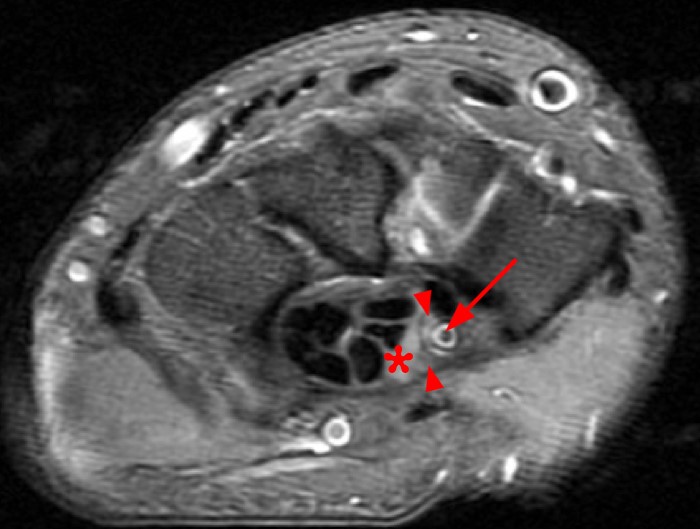
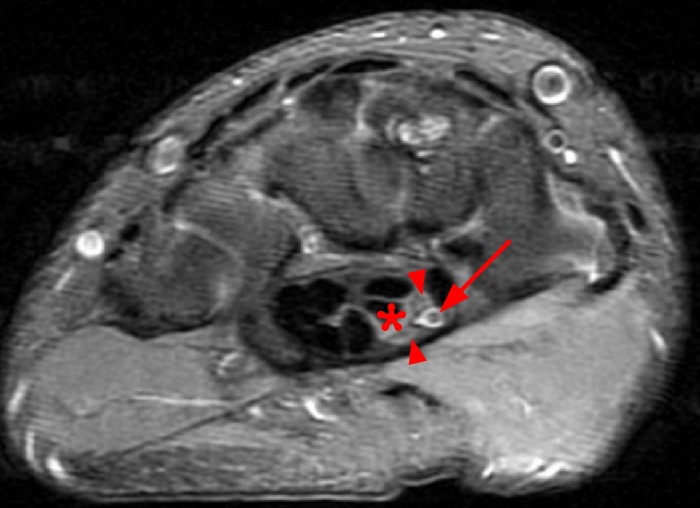
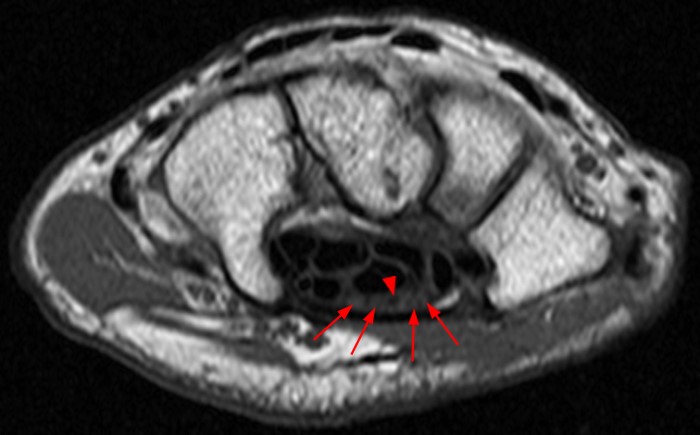
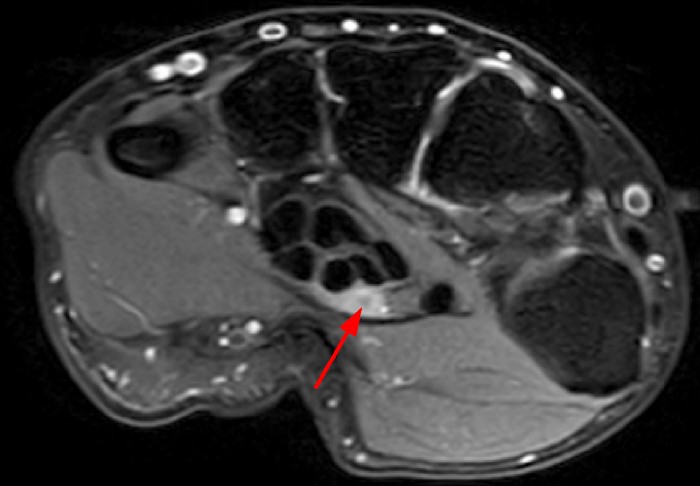
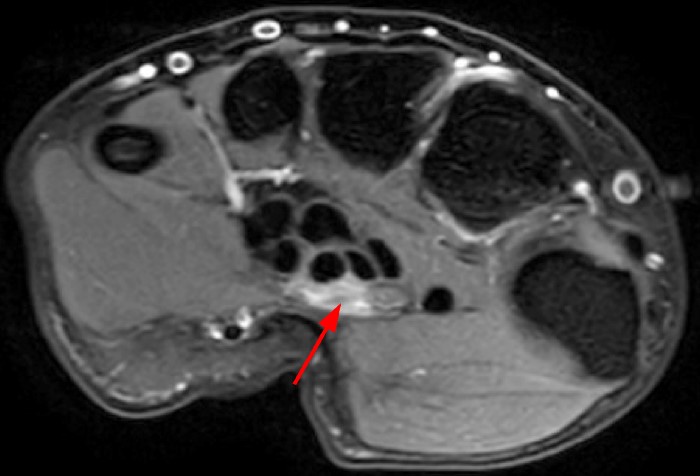
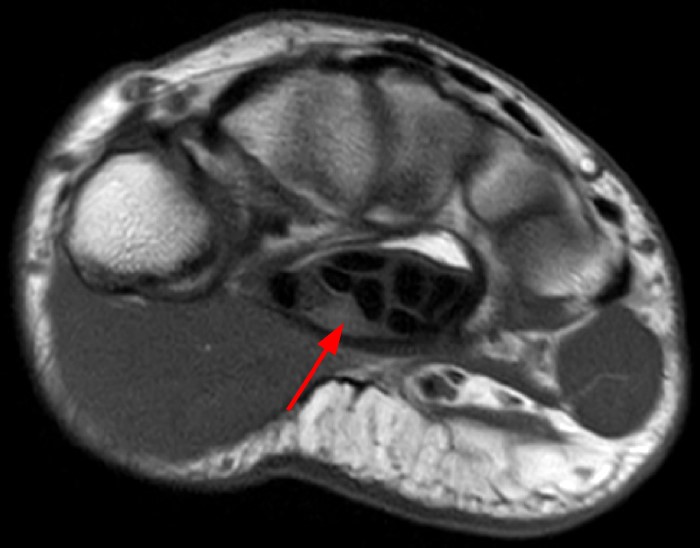
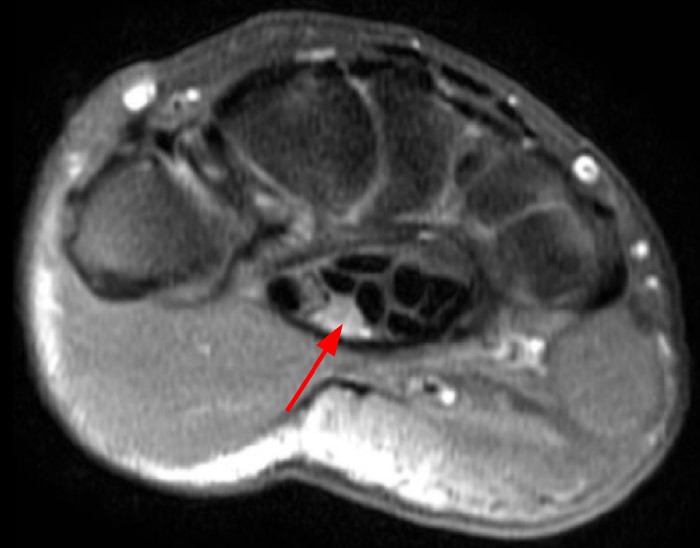
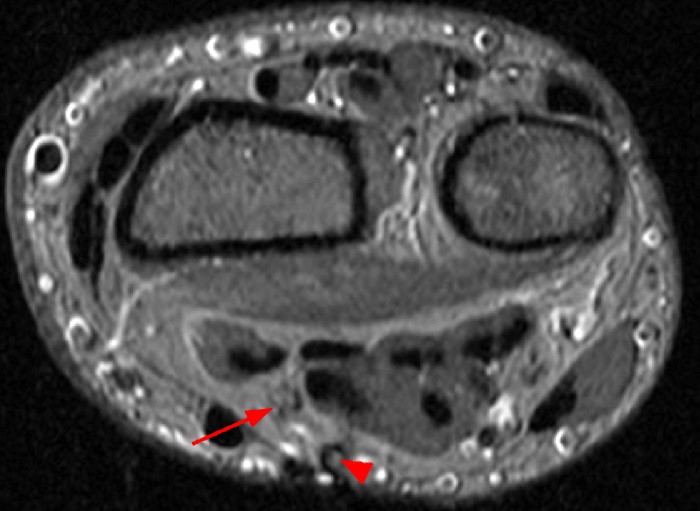
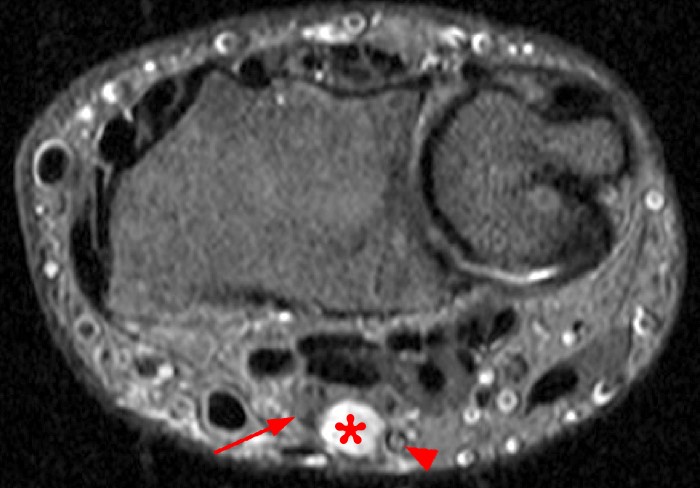
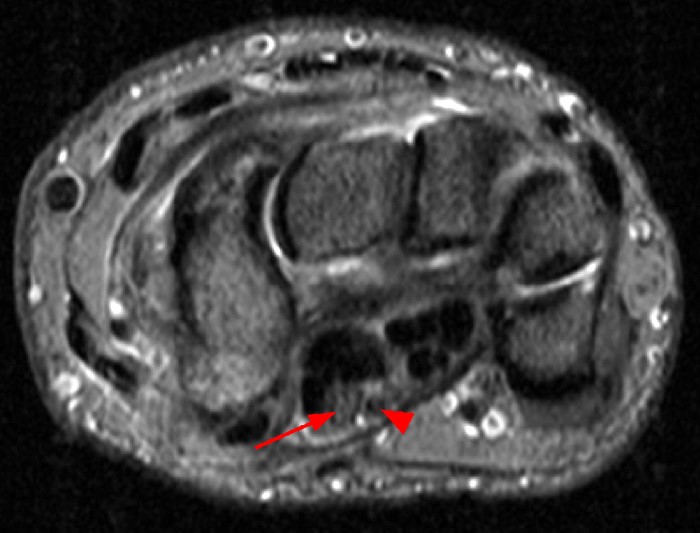
A 35 year-old male patient presents with index finger ischemia and volar wrist pain. Fat-suppressed proton density-weighted axial (1a-c) and sagittal T2-weighted (1d) images through the wrist near the level of the carpal tunnel are provided. What are your findings? What is your diagnosis?
Findings
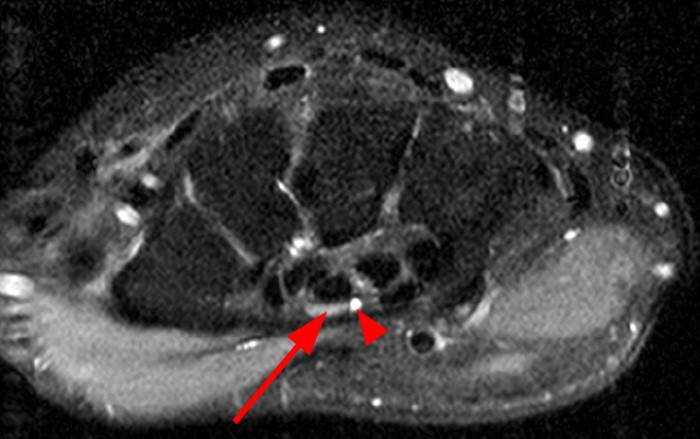
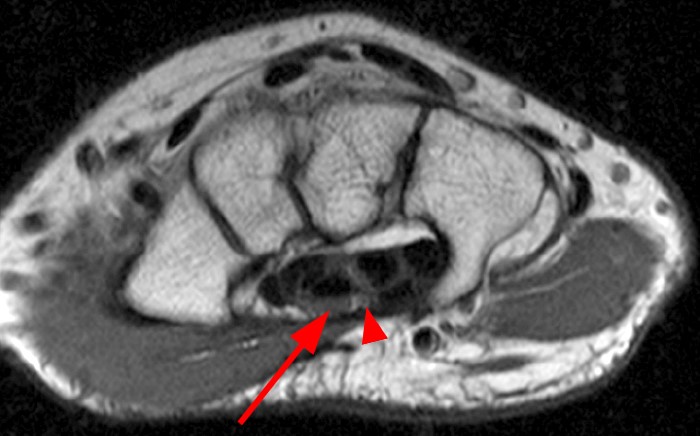
Figure 2:
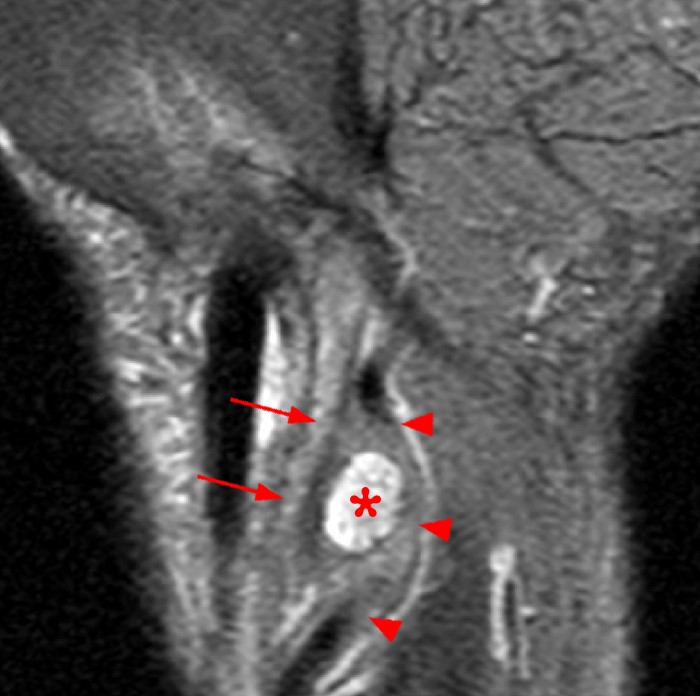
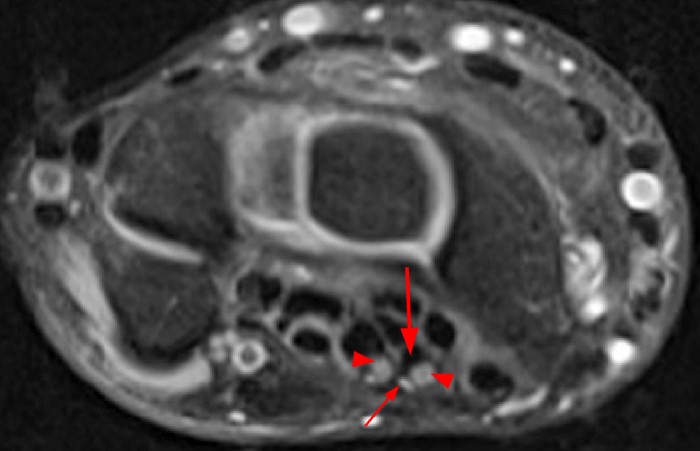
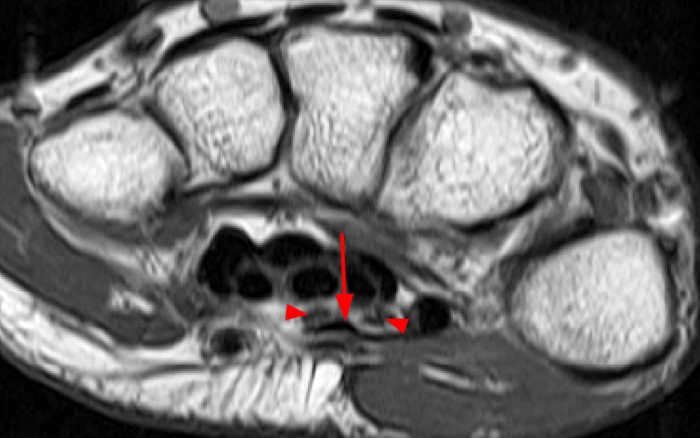
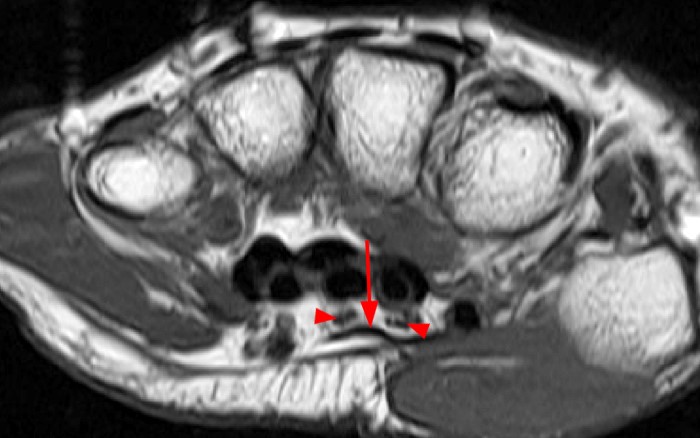
Axial fat-suppressed proton density-weighted (2a-c) and sagittal T2-weighted images (2d) demonstrate a sizeable vessel along the course of the median nerve, which is increased in caliber near the carpal tunnel with loss of the normal flow void (arrow), compatible with a thrombosed persistent median artery. There is a split appearance to the median nerve (arrowheads) consisted with a bifid median nerve, with the persistent median artery located between the two trunks of the nerve.
Diagnosis
Thrombosis of a persistent median artery, and bifid median nerve.
Introduction
The ulnar and radial arteries are the major arteries at the level of the wrist and are well visualized on MRI. Not infrequently, a persistent median artery (PMA) is also present within the wrist at the level of the carpal tunnel, although has received relatively little attention in the radiology literature. While typically asymptomatic, radiologists should be aware of the potential presence and associated pathophysiology of the PMA, particularly in patients with symptoms of carpal tunnel syndrome.
Anatomy
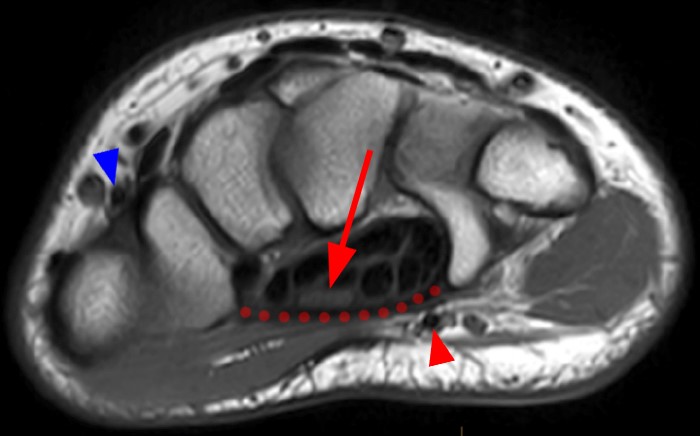
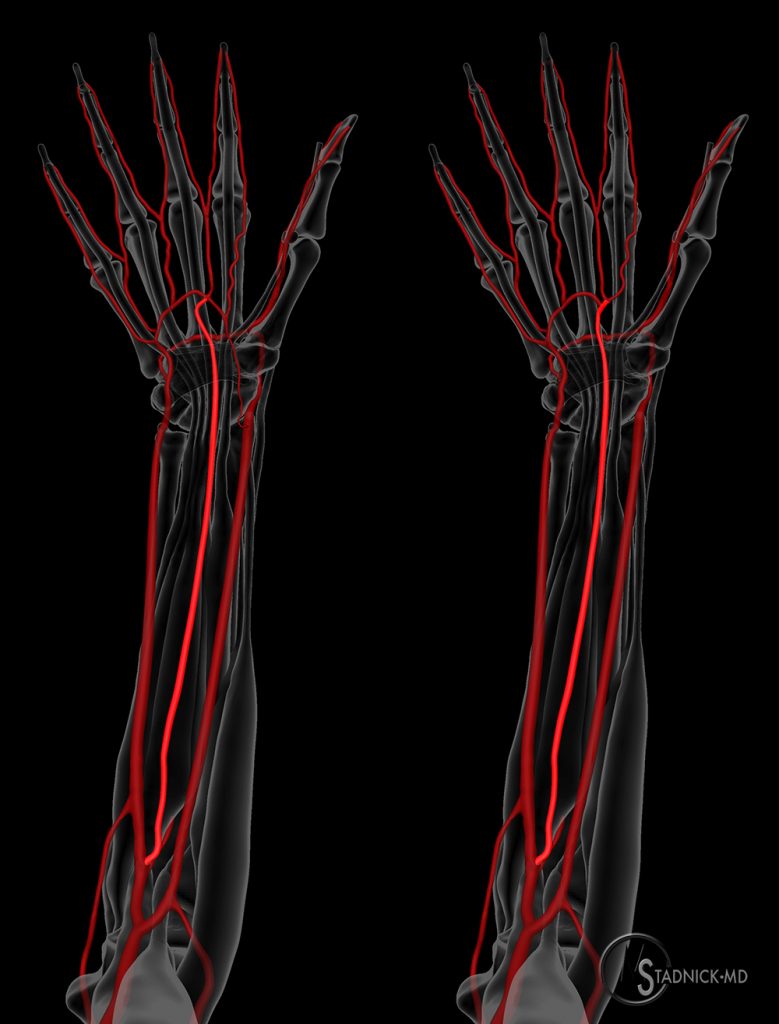
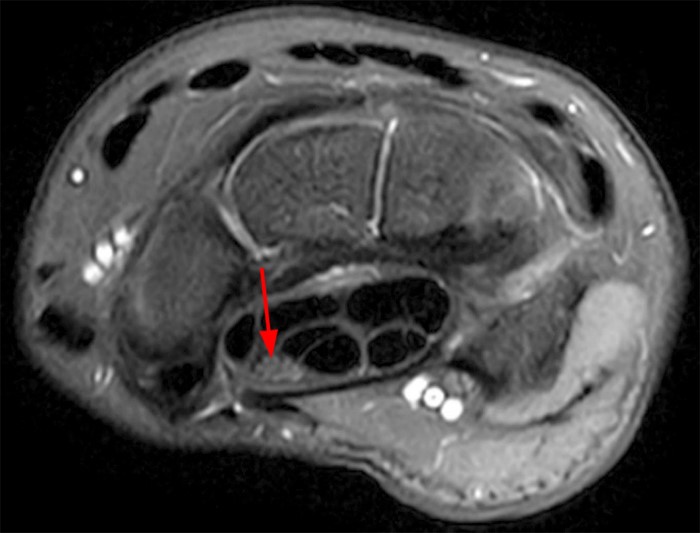
The brachial artery is a continuation of the axillary artery, dividing into the radial and ulnar arteries at the cubital fossa near the level of the radial neck. The radial artery courses laterally to the distal forearm/wrist and terminates in the deep palmar arch of the hand. The ulnar artery gives off the common interosseous artery near the distal aspect of the cubital fossa, then travels to the medial aspect of the forearm/wrist. At the wrist, typically no artery is visible on MRI adjacent to the median nerve (Figure 3).
During early embryonic development, the median artery is a major route of blood supply to the forearm and hand. Following development of the ulnar and radial arteries, the median artery typically regresses during intrauterine life, with its vestige being a small vessel accompanying the median nerve within the carpal tunnel 1; occasionally, the median artery can remain patent as a sizeable vessel into adulthood. In adults, two arterial patterns of the median artery have been described2: 1) an antebrachial type, which is a small and short vessel that terminates in the forearm before reaching the wrist; 2) the palmar type, which is a large, long vessel that accompanies the median nerve in the carpal tunnel and reaches the hand as the persistence of the embryonic form, commonly referred to as the persistent median artery (PMA) (Figure 4). The PMA has an incidence of ~11-15%.2,3,4,5
The PMA most frequently originates near the distal aspect of the cubital fossa from either the ulnar artery, common interosseous artery or the anterior interosseous artery.2,5 The PMA is intimately associated with the median nerve, and when present, is the main blood supply for the median nerve. In the upper third of the forearm, the median artery passes near the anterior interosseous nerve (which arises from the median nerve), and can occasionally pierce the median nerve from posterior to anterior.2
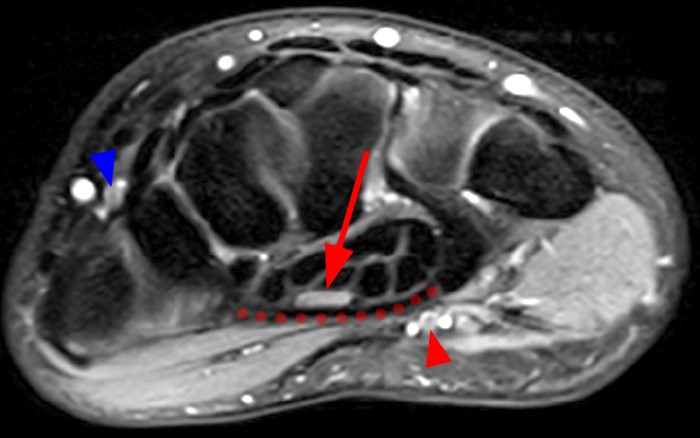
The PMA accompanies the median nerve within the carpal tunnel deep to the flexor retinaculum, passing through the carpal tunnel and entering the palm, terminating as either a contributor to a superficial arch or as a primary blood supply to the index and long fingers.2 Within the carpal tunnel, the PMA is most commonly palmar or medial to the median nerve.5 On MRI, the PMA can be recognized by its well-defined circular shape, its location close to the median nerve, its higher signal intensity compared to the nerve (Figure 5), and occasionally by the presence of linear flow artifact within the artery (Figure 6). Accompanying veins may also be present (Figure 6). The PMA may occur unilaterally (Figure 7) or bilaterally, without a marked tendency for either.6
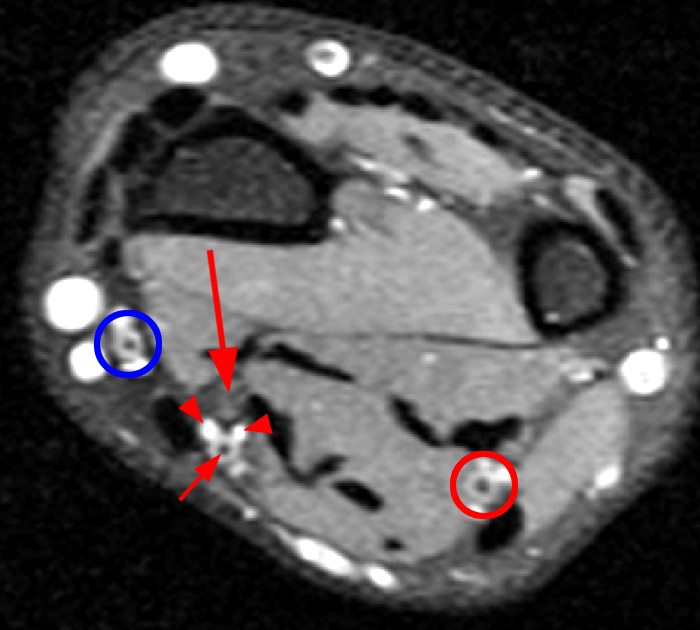
Figure 6:
Axial fat-suppressed proton density-weighted images proximal to (6a,b) and at the carpal tunnel (6c). 18-year-old with history of carpal tunnel surgery 5 years ago. PMA with normal median nerve with single branch (large arrow), a PMA with flow void (small arrow) and adjacent veins (arrowheads). Flow within the radial (blue circle) and ulnar (red circle) arteries is also visible.
Figure 7:
Axial fat-suppressed proton density-weighted images in a 22 year-old female with bilateral wrist pain. Within the left wrist (7a), small vessels (arrowhead) adjacent to the median nerve (arrow) within the carpal tunnel are consistent with a small persistent median artery and veins. On the right (7b), a normal median nerve (arrow) without a PMA is present.
Associated Median Nerve Variations
The median nerve normally branches just distal to the carpal tunnel, with any branching proximal to or within the tunnel considered an anatomical variant.3 The reported prevalence of a bifid median nerve has been widely variable, which likely reflects inconsistency in the methods of the various studies, including imaging versus cadaver studies, and the location of nerve branching evaluated (proximal or within the carpal tunnel). Studies have shown the presence of nerve branches proximal to the tunnel in 1 – 6%7,3, with a higher prevalence of bifid nerve within the tunnel. A bifid median nerve has been demonstrated at the level of the carpal tunnel in 9 – 19%.8,3 The bifid nerve can be divided by a large fibrous tissue barrier or small septum.9
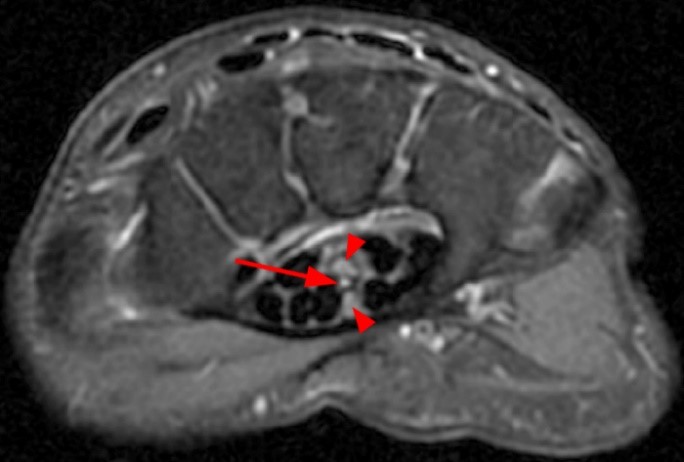
In nearly half of patients with a bifid median nerve, a concomitant persistent median artery can be found.8 Similarly, of patients with PMA, there are frequently anatomic variations of the median nerve, such as a bifid nerve. In a study by Gasner4, 63% of the PMAs in the study were associated with either a bifid nerve / high division of the nerve, and in most cases, the PMA was situated between the two trunks of the nerve (Figure 8), although it can be located along the periphery of the nerve (Figure 9). Rarely, more than two branches of the nerve can be seen within the carpal tunnel (Figure 10).
Figure 9:
Sequential axial fat-suppressed proton density-weighted images (9a-d) beginning just proximal to the carpal tunnel in a 24-year-old with wrist pain. There are two branches of the median nerve (arrowheads) and a persistent median artery (arrow). An anomalous muscle belly of the flexor digitorum superficialis (asterisk) extends into the proximal carpal tunnel.
Increased risk of carpal tunnel syndrome
Carpal tunnel syndrome (CTS) is the most common entrapment neuropathy of the upper extremity. Typically, the contents of the carpal tunnel include the median nerve, the flexor digitorum profundus and flexor digitorum superficialis tendons, and the flexor pollicis longus tendon. The median nerve lies superficial to the flexor tendons and beneath the flexor retinaculum, also known as the transverse carpal ligament, which is the palmar boundary of the carpal tunnel. Any conditions that crowd the structures within the carpal tunnel may lead to compression of the median nerve affecting its conductivity, causing pain, paresthesia or sensory loss in the median nerve distribution and progressive atrophy of the thenar musculature.
Given its close relationship with the median nerve, the PMA can contribute to carpal tunnel syndrome, particularly if large or if thrombosed.10 The presence of a patent PMA of similar size to the radial or ulnar artery can potentially cause compressive symptoms on the median nerve.4 In this scenario, symptoms predominate during work, presumably associated with mass effect that may become more pronounced with vasodilatation during activity.11 The PMA can also increase in caliber due to aneurysm12, AVM13, or calcification14, which can lead to CTS.
If thrombosed (Figures 1, 11, 12), the PMA can cause pressure on the nerve, particularly when they share a common sheath. Thrombosis of the PMA can cause sudden onset of pain and paresthesia, or can be chronic. Repeated stretch and vibration has been described as potential causes for thrombosis.15 Digital ischemia secondary to thrombosis of a persistent median artery has been described.16 Adjacent veins can also become thrombosed (Figure 13).
Figure 13:
Axial fat-suppressed proton density-weighted (13a-c, proximal to distal) and coronal STIR (13d,e) images demonstrate a 8 x 7 x 5mm ovoid hyperintense structure (asterisk) between the PMA (arrowheads) and the median nerve (arrows); pathology results described organized thrombus within a varix.
The association of PMA with a bifid median nerve can also increase the likelihood of CTS. A bifid median nerve occurs relatively frequently in patients with CTS, as it may facilitate compression of the median nerve in the carpal tunnel because of its relatively higher cross-sectional area compared with a non-bifid median nerve8, occupying more room in the carpal tunnel. These anatomic variations have been frequently discussed in the literature in association with CTS, as well as with complications during surgical treatment of CTS because of the presence of several branches of the median nerve within the tunnel.17
Additionally, aberrant muscles associated with a bifid median nerve have been reported to cause carpal tunnel syndrome18, including an accessory first lumbrical, an accessory palmaris longus, a prolonged flexor superficialis muscle belly, or a palmaris profundus (Figures 9, 14).
Figure 14:
Axial fat-suppressed proton density-weighted (14a,b) and T1-weighted (14c,d) images reveal a bifid median nerve (arrowheads), with the medial and lateral bundles of the median nerve separated by an anomalous palmaris profundus (long arrow) which extends through the carpal tunnel, and a small PMA (small arrow).
Pronator syndrome
As discussed in the previous web clinic on Median Nerve Entrapment, entrapment of the median nerve within the proximal forearm can cause a pain syndrome known as the pronator syndrome, which is most commonly caused by compression of the median nerve between the two heads of the pronator teres muscle. The PMA has been described as a rare potential cause of pronator syndrome19,20, related to the PMA piercing the median nerve in the upper forearm in up to 41% of the cases studied.2
Patients with pronator syndrome typically present with chronic volar pain and numbness in the median nerve distribution. MRI findings of pronator syndrome include denervation changes within the pronator teres muscle and/or other muscles innervated by the median nerve, including the flexor carpi radialis, palmaris longus, flexor digitorum superficialis, flexor pollicis longus, and the radial portion of the flexor digitorum profundus. Intramuscular edema is present in the acute to subacute setting, with muscle atrophy developing in cases of chronic denervation.
Anterior interosseous nerve syndrome
The PMA has been implicated as a potential cause of the anterior interosseous nerve (AIN) syndrome21, which is caused by compression or injury of the AIN. The AIN is a motor branch of the median nerve arising at the distal margin of the pronator teres muscle. The PMA is closely related to the AIN soon after its origin, crossing in front of the nerve, behind it, or rarely piercing it.2 Patients with AIN syndrome may present with dull pain of the volar forearm, and muscle weakness affecting the thumb and index finger, with a characteristic impairment of the pincer movement of the thumb and index finger. The flexor pollicis longus, radial half of the flexor digitorum profundus, and variably the pronator quadratus are affected, and MRI may demonstrate muscle edema or atrophy related to denervation changes.
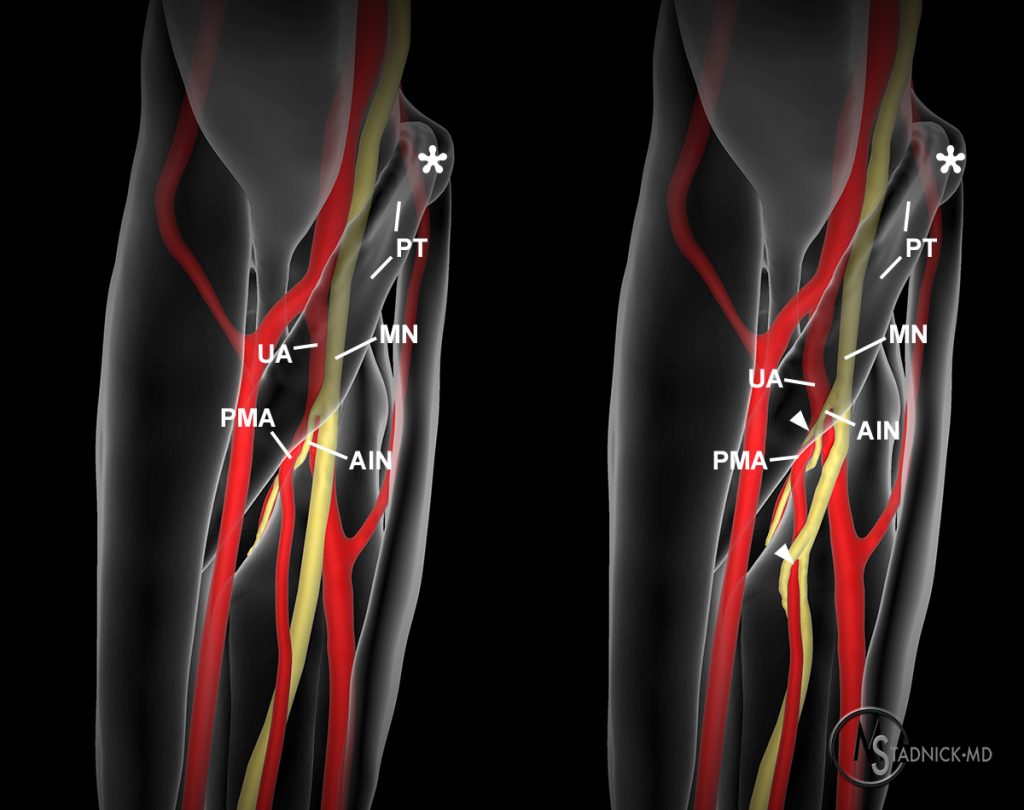
Figure 15:
Anterior views of the proximal forearm demonstrate two examples of the close proximity of the median nerve (MN) and anterior interosseous nerve (AIN) with the persistent median artery (PMA). The image on the right demonstrates the persistent median artery piercing the anterior interosseous nerve and median nerve (arrowheads). The pronator teres (PT) and medial epicondyle (asterisk) are also indicated.
Treatment
The PMA is usually an incidental, asymptomatic finding. In patients with carpal tunnel syndrome, surgical treatment of carpal tunnel syndrome involves release of the flexor retinaculum for decompression. In patients with a thrombosed PMA, the symptoms can improve upon treatment with anticoagulants, with recanalization of the thrombosed artery.10,22 Excision of the artery is typically avoided because of risk of vascular compromise to the digits.
In patients with pronator syndrome or anterior interosseous syndrome, initial conservative treatment includes physical therapy, activity modification, and anti-inflammatory medications, with surgery reserved for patients failing conservative measures.
Conclusion
The PMA is a relatively common anatomic variant. While usually asymptomatic, it can contribute to carpal tunnel syndrome, whether by acute thrombosis, dilatation, and/or by its association with a bifid median nerve. The PMA can also contribute to pronator syndrome or AIN syndrome by compressing or piercing the median nerve or AIN, respectively, within the proximal forearm. Knowledge about the origin, course and relations of the PMA to the median nerve and AIN will aid the radiologist and the surgeon.
References
- Singer E (1933) Embryological pattern persisting in the arteries of the arm. Anat Rec, 55: 403–409. ↩
- Rodríguez-Niedenfuhr M, Sanudo JR, Vãzquez T, Nearn L, Logan B, Parkin I. Median artery revisited. J Anat. 1999; 195:57–63. ↩
- Pierre-Jerome C, Smitson RD, Jr, Shah RK, Moncayo V, Abdelnoor M, Terk MR. MRI of the median nerve and median artery in the carpal tunnel: prevalence of their anatomical variations and clinical significance. Surg Radiol Anat. 2010; 32:315–322. ↩
- Gassner EM, Schocke M, Peer S, Schwabegger A, Jaschke W, Bodner G. Peristent median artery in the carpal tunnel: color Doppler ultrasonographic findings. J Ultrasound Med. 2002; 21:455–461. ↩
- Nayak SR, Krishnamurthy A, Kumar SM, Prabhu LV, Potu BK, D’Costa S, et al. Palmar type of median artery as a source of superficial palmar arch: A cadaveric study with its clinical significance. Hand (N Y) 2010; 5:31–6. ↩
- Henneberg M, George BJ. High incidence of the median artery of the forearm in a sample of recent southern African cadavers. J Anat. 1992; 180:185–8. ↩
- Lindley SG, Kleinert JM (2003) Prevalence of anatomic variations encountered in elective carpal tunnel release. J Hand Surg Am 28(5):849–855. ↩
- Bayrak IK, Bayrak AO, Kale M, Turker H, Diren B (2008) Bifid median nerve in patients with carpal tunnel syndrome. J Ultrasound Med 27(8):1129–1136. ↩
- Walker FO, Cartwright MS, Blocker JN, Arcury TA, Suk JI, Chen H, et al. Prevalence of bifid median nerves and persistent median arteries and their association with carpal tunnel syndrome in a sample of Latino poultry processors and other manual workers. Muscle Nerve. 2013;48((4)):539–44. ↩
- Salter M, Sinha NR, Szmigielski W. Thrombosed persistent median artery causing carpal tunnel syndrome associated with bifurcated median nerve: A case report. Pol J Radiol. 2011; 76(2):46–8. ↩
- Fumière E, Dugardeyn C, Roquet ME, Delcour C. US Demonstration of a Thrombosed Persistant Median Artery in Carpal Tunnel Syndrome. JBR-BTR 2002; 85: 1–3. ↩
- Toranto IR. Aneurysm of the median artery causing recurrent carpal tunnel syndrome and anatomic review. Plast Reconstr Surg 1989; 84:510–512. ↩
- Gutowski KA, Olivier WA, Mehrara BJ. Arteriovenous malformation of a persistent median artery with a bifurcated nerve. Plast Reconstr Surg. 2000; 106:1336–1339. ↩
- Dickinson JC, Kleinert JM (1991) Acute carpal-tunnel syndrome caused by a calcified median artery. J Bone Joint Surg, 73A: 610–611. ↩
- Nather A., Chacha P.B., Lim P.: Acute carpal tunnel syndrome secondary to thrombosis of a persistent median artery (with high division of the median nerve). A case report. Ann Acad Med Singapore, 1980, 9: 118-121. ↩
- Aulicino P.L., Klavans S.M., Dupuy T.E.: Digital ischemia secondary to thrombosis of a persistent median artery. J Hand Surg, 1984, 9: 820-823. ↩
- Bozentka DJ, Osterman AL (1995) Complications of endoscopic carpal tunnel release. Hand Clin 11:91–95. ↩
- Park JJ, Choi JG, Son BC.Carpal Tunnel Syndrome Caused by Bifid Median Nerve in Association with Anomalous Course of the Flexor Digitorum Superficialis Muscle at the Wrist. 2017;3 (1): 21-23. ↩
- Gainor BJ, Jeffries JT. Pronator syndrome associated with a persistent median artery. A case report. J Bone Joint Surg Am. 1987; 69:303–4. ↩
- Jones NF, Ming NL. Persistent median artery as a cause of pronator syndrome. J Hand Surg Am. 1988; 13:728–732. ↩
- Proudman TW, Menz PW. An anomaly of the median artery associated with the anterior interosseous nerve syndrome. J Hand Surg Br. 1992; 17:507–9. doi:10.1016/S0266-7681(05)80231-1.) ↩
- Srivastava A, Sharma P, Pillay s. Persistent median artery thrombosis: a rare cause of carpal tunnel syndrome. Australas J Ultrasound Med, 18 (2015), pp.82-85. ↩