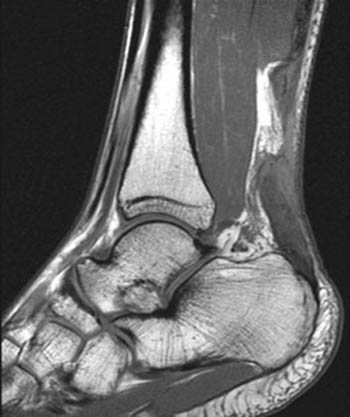
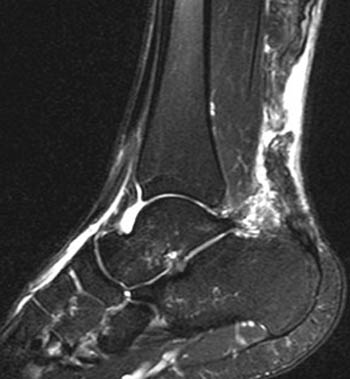
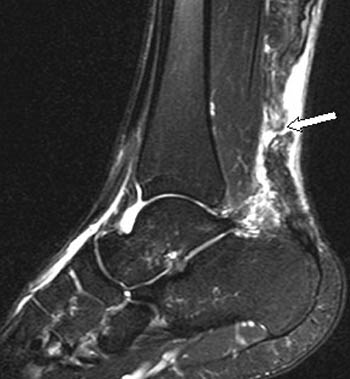
Clinical History: A jolly, white-haired gentlemen presented on December 23rd with sudden onset of pain at the back of the heel after pushing a sled (1a). (1b) T1-weighted and (1c) fat-suppressed T2-weighted sagittal images of the ankle are provided. What are the findings? What is your diagnosis?
Findings
Diagnosis
Chronic Achilles tendinosis and Achilles tendon rupture.
Discussion
The Achilles tendon, formed by the confluence of the gastrocnemius and soleus tendons, is the largest and strongest tendon in the body, and is a frequent source of pain at the ankle. Acute rupture of a normal tendon may occur with forced dorsiflexion, or may occur following relatively minor trauma in patients in whom the tendon is already weakened secondary to chronic inflammation or connective tissue disorders. The Achilles tendon does not possess a true tendon sheath, and thus inflammatory disorders are classified as tendinitis, paratendinitis, and peritendinitis. Tendinitis generally manifests on MR as regions of increased signal intensity and/or tendon enlargement on T1 and T2-weighted images (4a, 4b). Histologically, Achilles tendinitis is actually more of a degenerative phenomenon, with few inflammatory cells being present.1 Similar to the rotator cuff, the more correct term for this condition is thus Achilles tendinosis.
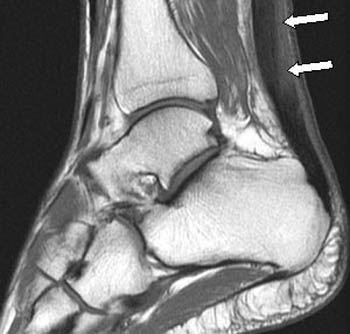
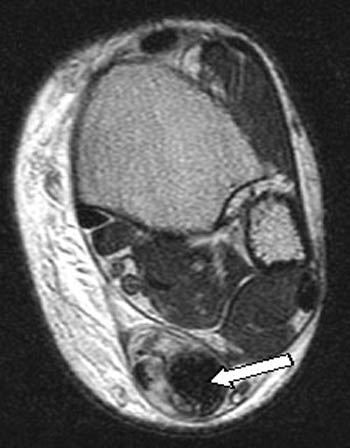
Figure 4:
(4a) The Achilles tendon is severely thickened and demonstrates diffusely increased signal intensity throughout its substance (arrows) on the T1-weighted sagittal view. (4b) The markedly thickened tendon (arrow) is confirmed on a T2-weighted axial image from a patient with severe, chronic Achilles tendinosis.
Tears of the Achilles tendon are revealed by the presence of fluid signal intensity within the tendon. Partial tears and longitudinal splits (5a) are well seen with MR. Complete Achilles ruptures usually occur approximately 4-5 cm from the calcaneal attachment,2 that region thought to be a relative watershed zone in the Achilles blood supply. However, trauma to the contracted Achilles musculotendinous unit may result in a distal rupture at the calcaneal attachment.
Rupture of the Achilles tendon may be a dramatic event, particularly when acute and complete. Typical patients are middle-aged men participating in activities requiring forceful push-off maneuvers. Severe pain with localized hemorrhage is often present, and the Thompson test is positive, such that the patient is unable to stand tiptoe on the injured leg and a diminished plantar flexion response to calf squeezing is present.3
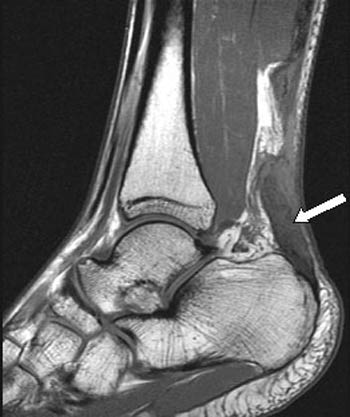
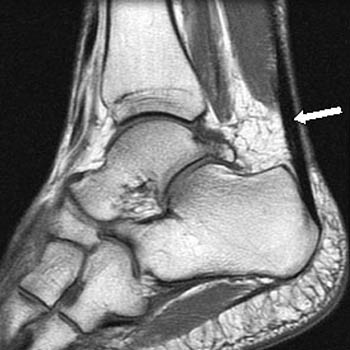
The patient in the current case was scheduled for surgery on December 24th, but refused treatment, stating that he was “far too busy during the holidays”. However, a follow-up MRI was obtained on the 24th, with a (6a) T1-weighted sagittal image provided below:
In this particular case, the patient, Mr. K. Kringle, demonstrated a miraculous response to one day of conservative therapy. Our first inclination was to write up the findings as a case report, but the patient was lost to follow-up, simply stating that he had to return to his home “up North”. Unfortunately, most patients do not possess a similar capacity to heal. Indeed, the majority of orthopaedists now feel that complete Achilles ruptures should be treated surgically, as tendon function is superior and the recurrence rate for re-tearing is lower in patients who undergo operative treatment.4 It is thus reasonable to obtain a pre-operative MR in most patients in order to assess the status of the residual tendon and evaluate the size of the tendon gap that is often present.
Conclusion
This case demonstrates the importance of MRI in the evaluation and management of Achilles tendon injuries. In the interest of disclosure, we admit that certain components of this Web Clinic have not been fully documented. Happy Holidays from your friends at Radsource!
References
1 Mink JH: Tendons. In AL Deutsch, JH Mink, R Kerr (Eds): MRI of the Foot and Ankle. New York, Raven Press, 1992, p.135.
2 Kelikian H, Kelikian AS. Disorders of the Ankle. Philadelphia, WB Saunders Co, 1985.
3 Jahss MH: Tendon disorders of the foot and ankle. In MH Jahss (Ed): Disorders of the Foot and Ankle. 2nd Ed. Philadelphia, WB Saunders Co, 1991, p.1461.
4 Soma CA, Mandelbaum BR: Repair of acute Achilles tendon ruptures. Orthop Clin North Am 1995; 26:239.