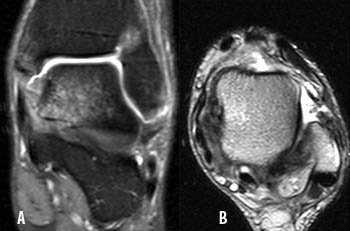
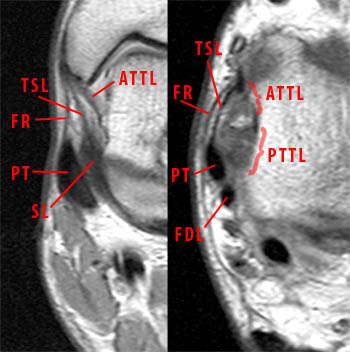
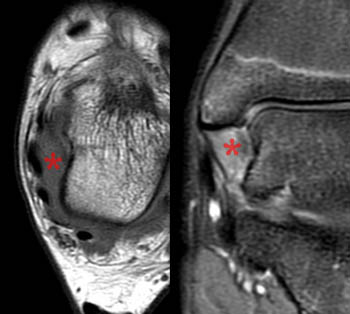
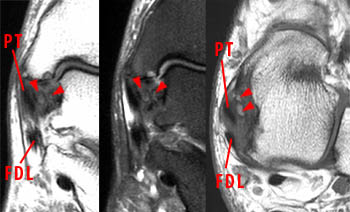
Clinical History: A 27 year-old male presents with severe ankle pain two weeks following an inversion injury of the ankle. Proton density-weighted fat-suppressed coronal (A) and T2-weighted FSE (B) axial images are provided. The syndesmotic ligaments between the tibia and fibula were found to be intact on the other views. Assess the extent of lateral and medial ligamentous injuries. What are the findings? What is your diagnosis?
Findings
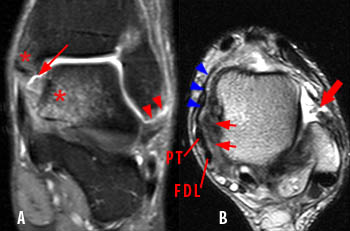
Figure 2:
The proton density-weighted fat-suppressed coronal image of the ankle (A) demonstrates partial avulsion of the anterior talofibular ligament at the distal fibula (arrowheads). The axial T2-weighted image (B) demonstrates a complete tear of the anterior talofibular ligament (thick arrow). Bone bruises are seen in the medial talus and medial malleolus (asterisks) resulting from impaction associated with a severe inversion injury. A proximal partial tear of the deep portion of the deltoid ligament complex is filled with fluid signal (arrow). Edema and loss of the normal architecture of the deep deltoid ligament fibers are demonstrated on the axial image (short arrows). The superficial components of the deltoid ligament complex (blue arrowheads) are intact. The posterior tibial (PT) and flexor digitorum longus (FDL) tendons are labeled.
Diagnosis
Complete (Grade III) tear of the anterior talofibular ligament with an accompanying proximal partial tear (Grade II) of the deep posterior tibiotalar component of the deltoid ligament complex.
Introduction
The deltoid ligament complex acts as the primary stabilizer of the axially loaded ankle. Recent evidence indicates that deltoid ligament injuries are associated with a wide variety of ankle injuries and are more common than earlier studies suggested. Failure to diagnose and appropriately treat deltoid ligament insufficiency may lead to debilitating medial ankle instability, osteoarthritis, and medial ankle impingement syndromes.
Anatomy and Function
The deltoid ligament complex arises from the medial malleolus and is commonly divided into a superficial and deep layer. Conceptually, the superficial layer provides stability to the naviculocalcaneal complex and resists external rotation of the talus relative to the tibia. The deep layer assists in stabilizing the talus and resists posterior translation of the talus, valgus angulation of the talus, and lateral displacement of the talus from the medial malleolus. The tibial attachments of the deep layer arise from the anterior and posterior colliculi of the inner surface of the medial malleolus as well as from the intervening sulcus known as the intercollicular groove. The superficial and deep components of the deltoid ligament complex are composed of multiple fused ligamentous fascicles that are difficult to distinguish on gross inspection. Anatomically, the division of the deltoid ligament complex into discrete components is somewhat artificial, and naming of the ligamentous fascicles is based on the origins and insertions of the ligamentous tissue.1
Not surprisingly, there is variation in the agreed upon components of the deltoid ligament complex. The most commonly recognized ligaments of the superficial layer are the tibionavicular ligament (TNL), the tibiospring ligament (TSL), and the tibiocalcaneal ligament (TCL). On anatomic dissection both the TNL and TSL are consistently found.2 The deep layer is comprised of the anterior tibiotalar ligament (ATTL) and the posterior tibiotalar ligament (PTTL) with the PTTL being a constant anatomic finding.2 Since the deep and superficial components of the deltoid ligament complex serve different stabilizing functions, recognizing which component is injured provides insight into the instability patterns that may be anticipated.
Deep Ligament Layer
The posterior tibiotalar ligament (PTTL) is the strongest component of the deltoid ligament complex. It is conical in shape and originates from the medial malleolus at the intercollicular groove, the entire anterior surface of the posterior colliculus and the upper segment of the posterior surface of the anterior colliculus. The ligament fibers are directed downward, posteriorly, and laterally, inserting on an oval elevation at the medial surface of the talus just plantar to the articular surface. The insertion reaches as far posteriorly as the posteromedial talar tubercle. The PTTL is an intra-articular but extrasynovial ligament. It is commonly fasciculated and may be divided into two distinct bands.1 This ligament prevents lateral shift of the talus and limits dorsiflexion of the ankle or anterior rotation of the leg when the foot is planted. In addition the PTTL resists internal rotation of the talus relative to the leg.3
The anterior tibiotalar ligament (ATTL) originates from the tip of the anterior colliculus and the anterior part of the intercollicular groove inserting on the medial surface of the talus distal to the margin of the anterior medial talar articular surface.1 The ATTL is commonly fasciculated and extremely variable in size. This ligament may be completely absent.2
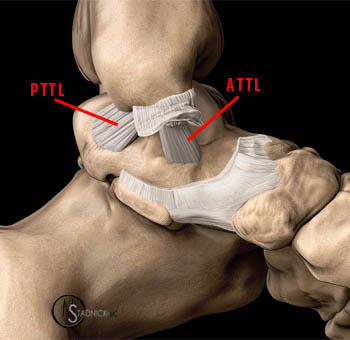
Figure 3:
With the superficial layers of the deltoid ligament complex removed, the components of the deep layer of the deltoid ligament complex are demonstrated. The deep layer of the deltoid ligament is formed by a small and variable anterior tibiotalar ligament (ATTL) and a very strong posterior tibiotalar ligament (PTTL).
Superficial Ligament Layer
The tibiocalcaneal ligament (TCL) is the strongest superficial component.1 The TCL arises at the medial aspect of the anterior colliculus and descends vertically to insert on the medial border of the sustentaculum tali. This ligament also shares interlacing fibers with the superomedial portion of the spring ligament and the tibiospring ligament (TSL). The TCL and TSL are typically continuous and inseparable by MRI and gross inspection.1 Occasionally, a layer of adipose separates the two fascicles.2 The TCL of the superficial deltoid limits eversion of the calcaneus at the subtalar joint and contributes to medial stability of the talus.3
The tibiospring ligament (TSL) is the only fascicle that inserts onto another ligament. The TSL originates at the anterior portion of the anterior colliculus of the medial malleolus and inserts on the superior border of the superomedial portion of the calcaneonavicular (spring) ligament. The TSL assists in the suspension of the calcaneonavicular ligament against gravity and inferomedially directed dynamic forces from the talar head.3 Because of the broad insertion of the TSL on the spring ligament complex, Hintermann postulates that the spring ligament complex reciprocally contributes to stabilization of the medial ankle joint.4,5
The tibionavicular ligament (TNL) is composed of fascicles that arise from the anterior border of the anterior colliculus of the medial malleolus. The TNL is contiguous with the more posterior TSL. The deeper fibers of the TNL, which are known as the anterior superficial tibiotalar fascicle, are variably present and insert on the dorsal aspect of the talar neck slightly posterior to the head of the talus. The more superficial fibers of the TNL insert more distally at the dorsomedial aspect of the navicular in a curvilinear fashion. The TNL limits external rotation of the talus in the ankle mortise and assists in transmitting the internal rotation forces of the tibia to the talus. The TNL also restricts plantar flexion of the foot and ankle, and combines with the tibiospring ligament (TSL) and calcaneonavicular (spring) ligament to support the talar head and stabilize the talocalcaneonavicular joint.1,4
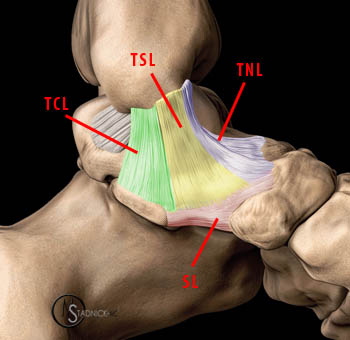
Figure 4:
The superficial layer is a broad and triangular structure composed of multiple fascicles. It is the weakest layer of the deltoid complex. The commonly recognized components of this layer are the tibionavicular ligament (TNL), the tibiospring ligament (TSL), and the tibiocalcaneal ligament (TCL). All three of these fascicles blend with the superomedial portion of the spring ligament complex (SL).
Normal MRI Anatomy
A study by Mengiardi et al. evaluating the MRI appearance of the medial collateral ligament complex in asymptomatic individuals found that only the TSL and PTTL were visible in all volunteers. The TCL was seen in 88%, and the TTL and TNL were seen in 55% of ankles.6 Similar findings have been found on gross anatomic dissection studies as well, with the exception that the TNL is consistently found on dissections.2,7 In their study, Mengiardi et al. felt that the relatively low percentage of TNL visibility by MRI was caused in part by the oblique course of the TNL relative to the axial and coronal planes employed.6
The PTTL is best seen in the coronal plane, but also routinely found on axial images. The normal PTTL of the deltoid ligament complex has a striated appearance on T1 and intermediate-weighted images due to fat interspersed between the ligament fibers (5a). This striated appearance is less apparent on T2-weighted fat-suppressed images. Mengiardi et al. found that the normal PTTL had a striated appearance in all patients younger than 45 years of age and in 75% of patients older than 45 years of age.6 The loss of striations in older individuals results from a reduced prominence of fat and is presumed to be caused by prior subclinical injuries.
The ATTL is variably present and is best seen on coronal images (6a). The ATTL is frequently striated in appearance with intermediate signal intensity on T1-weighted images and is most commonly low signal intensity on T2-weighted images. An inhomogeneous pattern of the ATTL on T1-weighted images was seen significantly more frequently in asymptomatic volunteers older than 45 years of age.6
Figure 6:
A coronal proton density-weighted image (left) through the anterior colliculus of the medial malleolus demonstrates the normal anatomic relationships of the anterior tibiotalar ligament (ATTL) which extends from the tip of the anterior colliculus to the medial talus just anterior and inferior to its articular surface. An axial T1-weighted image demonstrates both the anterior tibiotalar ligament (ATTL) and the more substantial posterior tibiotalar ligament (PTTL) at the level of their talar insertions. The superficial component of the deltoid complex is composed primarily of fibers forming the tibiospring ligament (TSL) at this level and can be seen on the coronal and axial images as a low signal curvilinear band superficial to the deep components. The flexor retinaculum (FR), posterior tibial tendon (PT), flexor digitorum longus tendon (FDL), and superomedial portion of the spring ligament complex (SL) are also indicated.
The TCL and TSL are best seen in the coronal plane. On T1-weighted images their signal intensity is typically intermediate and homogeneously low on T2-weighted images. Inhomogeneity is common in patients older than 45 years of age.6 On coronal and axial MRI, the TCL and TSL are most frequently seen as a continuous low signal sheet (7a,9a).
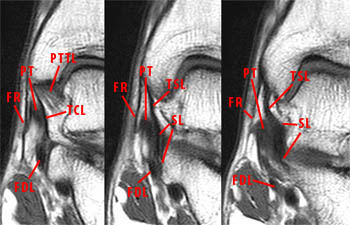
Figure 7:
This series of coronal T1-weighted images begin at the level of the intercollicular groove (far left) and moves anteriorly through the anterior colliculus (far right) and demonstrates the tibiocalcaneal ligament (TCL) bridging between the medial surface of the medial malleolus to the sustentaculum and overlying the anterior fibers of the posterior tibiotalar ligament (PTTL). The tibiocalcaneal ligament fibers are most commonly inseparable from the more anteriorly arising tibiospring ligament (TSL) which bridges from the medial malleolus to the superomedial portion of the spring ligament complex (SL). The flexor retinaculum (FR), posterior tibial tendon (PT), and flexor digitorum longus tendon (FDL) are labeled.
The TNL is best seen on coronal and axial images (8a,9a). On T1-weighted images, the signal intensity is overwhelmingly intermediate and inhomogeneous in signal. On T2-weighted images, the signal intensity and signal intensity pattern is more variable. The TNL commonly blends with fibers of the TSL and often has an indistinct border.6 The origin of the TNL from the anterior margin of the medial malleolus is best seen on the axial images as a smooth homogeneously low-signal curvilinear structure that blends with the periosteum of the tibia and the flexor retinaculum.8
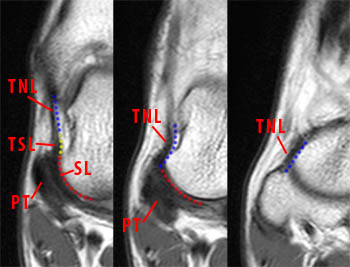
Figure 8:
A series of coronal T1-weighted images beginning at the anterior margin of the anterior colliculus and continuing to the level of the navicular demonstrate the normal continuity between the tibionavicular ligament (TNL) and the tibiospring ligament (TSL). The included portion of the superficial deltoid ligament is composed of fibers from the tibionavicular (blue) and the tibiospring ligament (yellow). Fibers from both commonly blend with the superomedial portion of the spring ligament complex (SL)(red). On the more anterior images, the tibionavicular ligament (TNL) can be followed to its insertion on the navicular.
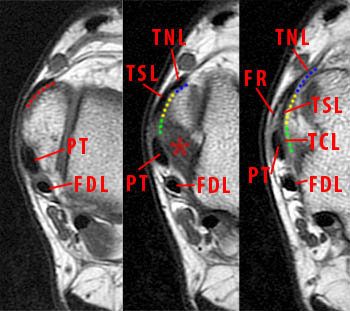
Figure 9:
Axial T1-weighted images at the level of the medial malleolus, just above the anterior colliculus (left), at the level of the anterior colliculus (middle) and plantar to the anterior colliculus (right) demonstrate the anterior superficial fibers that give rise to the tibiospring and tibionavicular ligaments as a smooth low signal condensation of fibers (red). At and plantar to the anterior colliculus, the fibers of the tibiocalcaneal (TCL) (green), tibiospring (TSL) (yellow), and tibionavicular (TNL) (blue) ligaments are inseparable. The deep posterior tibiotalar ligament (asterisk), posterior tibial tendon (PT) and flexor digitorum longus tendon (FDL) are indicated.
Mechanism of Injury and Physical Findings
Acute Deltoid Complex Injuries
Isolated deltoid ligament tears are very rare. Deltoid ligament injuries are most frequently seen in association with lateral ankle ligament and syndesmotic ligamentous injuries and with fibular and lateral malleolar fractures. Deltoid ligament disruptions are a well-known consequence of pronation-eversion and pronation-abduction injuries at the ankle (I). In both mechanisms the deltoid ligament or the medial malleolus is the initial structure that fails. However, recent evidence indicates that deltoid ligament injuries are more frequent, less predictable, and occur through a much wider variety of injury mechanisms. For instance, a significant percentage of patients with deltoid ligament complex injuries describe a supination injury as the primary injury or multiple ankle sprains without a clearly identified mechanism.9 In addition, deltoid complex injuries are more frequent in supination-external rotation (SER) injuries than predicted by the Lauge-Hansen classification of the progression of structural failure.10 Finally, a high incidence of deltoid ligament complex injuries is demonstrated in patients with inversion sprains of the ankle.
Acute deltoid ligament injuries may present with swelling or ecchymosis medially at the ankle and tenderness to palpation over the injured portion of the deltoid ligament complex. This finding is less reliable with certain injury mechanisms. For instance, a recent investigation provided no real correlation between medial gutter pain to palpation and the development of medial deltoid ligament instability in patients with supination-external rotation ankle injuries.11 With acute superficial deltoid injuries, the anterior portion of the medial malleolus is commonly painful to palpation.12
Chronic Deltoid Complex Injuries
Chronic deltoid ligament insufficiency may result if an acute deltoid ligament sprain is unrecognized or inadequately treated. A high incidence of deltoid ligament deficiency is seen in patients presenting with chronic lateral ankle instability.9 Deltoid ligament insufficiency may occur as a primary injury associated with ankle sprain and fracture mechanisms or as a secondary injury resulting from long-standing lateral instability. In these patients, surgical repair or reconstruction of the deficient lateral ligaments without addressing coexisting deltoid ligament insufficiency often results in a poor functional outcome, necessitating deltoid ligament repair.4 Other conditions that may lead to chronic deltoid ligament insufficiency include posterior tibial tendon dysfunction, triple arthrodesis, and ankle arthroplasty.13
Inadequately treated deltoid tears may result in medial ankle instability. In this condition, the patient describes a feeling of “giving way” at the ankle. These patients develop medial ankle pain and on weight bearing exhibit pronation of the foot and hindfoot valgus. Posterior tibial tendon dysfunction may present with a similar malalignment. To help differentiate deltoid ligament deficiency from posterior tibial dysfunction as the cause of malalignment, the patient is asked to toe-rise. With an intact functioning posterior tibial tendon, the hindfoot valgus corrects.4,9
Impingement Syndromes
Medial impingement syndromes have been recently described.14,15 Pain with accompanying mechanical limitation of ankle motion is most commonly the result of fibrosis, fibrocartilaginous metaplasia, synovial proliferation, and hypertrophic bony changes after inadequate healing of deep deltoid ligament injuries. Posteromedial impingement is a frequent complication of lateral ankle sprains. In this mechanism, the PTTL is crushed between the medial malleolus and a severely inverted talus.16 Posteromedial impingement leads to persistent posteromedial ankle pain, which worsens, with ankle inversion. Deep soft tissue induration may be found behind the medial malleolus.
Anteromedial impingement may occur from repetitive sports-related activities such as gymnastics, soccer, basketball, and football, but may also be seen in non-sports related trauma.17 Anteromedial impingement is felt to result from inversion injuries causing chronic injury of the anteromedial synovial tissues and the ATTL.14 A meniscoid lesion representing hypertrophied synovial tissue can be seen as an isolated lesion or associated with a partially torn ATTL.15 A thickened ATTL has also been identified as a cause of anteromedial impingement. Patients with anteromedial impingement experience pain anteromedially with eversion and dorsiflexion of the ankle.
Physical Testing
For both acute and chronic deltoid ligament complex injuries, physical examination attempts to demonstrate instabilities specific to the injured component of the deltoid ligament complex. On physical testing a torn superficial ligament allows enhanced external rotation of the tibia as anteriorly directed force increases anterior translation of the talus and foot relative to the mortise. In contrast, a normal ankle demonstrates internal rotation around an intact superficial deltoid ligament when undergoing the same maneuver. The integrity of the deep deltoid component is assessed by the extent of posterior translation of the talus relative to a stabilized tibia.12
Imaging Findings
Radiography findings
Radiographs are commonly used in evaluating ankle injuries. Malleolar fractures are demonstrated along with evidence for widening of the medial clear space (the distance between the articular surface of the medial malleolus and medial talus). Widening of the medial clear space on weight-bearing radiographs has long been utilized as a sign of deltoid insufficiency. However this measurement lacks sensitivity and has proven unreliable in assessing the presence of underlying deltoid ligament deficiency.18 Stress views even with the patient under general anesthesia are frequently unsuccessful in documenting an underlying deltoid ligament insufficiency.9 For these reasons, MRI is valuable in its ability to detect deltoid ligament injury and assist in treatment and surgical planning.
MRI Findings
Acute Deltoid Ligament Complex Injuries
Injuries of the deltoid ligament complex are categorized as superficial or deep. The level of disruption of the ligament is classified as proximal (type I), intermediate (type II), or distal (type III).9,19 Type I injuries are overwhelmingly the most common injury and type II injuries are the most rare. Ligament injuries are also categorized based on the severity of the sprain/tear; grade I sprain represents a stretching injury of the ligament with periligamentous edema, grade II represents a partial tear, and grade III represents complete disruption.
Grade I injuries of the deep deltoid ligament are evident on T1 and intermediate weighted images as loss of the striated appearance within the deep portion of the deltoid ligament. Fat-suppressed fluid sensitive sequences demonstrate increased signal within the ligament (10a). With type II and type III injuries there are partial or complete fluid-filled defects best seen on fluid sensitive sequences (1a). Lateral talar shift and widening of the medial clear space are ancillary findings that may be observed.
The superficial components of the deltoid ligament complex are less frequently injured and most commonly present as grade I injuries with thickening and loss of definition of the ligament fibers on T1-weighted images. Fat-suppressed fluid sensitive sequences demonstrate intrinsic increased signal with surrounding edema.13 Higher-grade tears of the superficial ligaments are most frequently proximal (type I) injuries. Type I tears of the TNL are seen on fluid sensitive series as focal edema and interruption of the normal low-signal condensation of fibers along the anteromedial surface of the anterior colliculus. With this injury, axial and sagittal images may be particularly useful in demonstrating the proximal avulsion of the TNL (11a).
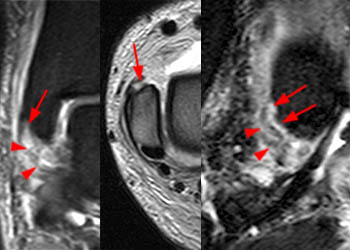
Figure 11:
46 year-old male who suffered a pronation external rotation mechanism of injury one week earlier. Coronal proton density fat-suppressed (left), axial T2-weighted FSE (middle), and sagittal T2-weighted fat-suppressed (right). In this pattern the anterior superficial ligaments fail initially. Proximal (type I) avulsion of the tibionavicular ligament is demonstrated at the anterior margin of the anterior colliculus (arrows) and ill-defined, lax and edematous distal ligament fibers (arrowheads) are apparent. The patient also had a tear of the anterior inferior tibiofibular ligament and a non-displaced spiral fracture of the distal fibular shaft.
Concurrent medial and lateral malleolar fractures, osteochondral injuries of the talus, lateral ligament, syndesmotic ligament, and spring ligament injuries, and tibialis posterior pathology are well depicted on a combination of sagittal, coronal, and axial images utilizing T1-, intermediate-, and T2-weighting.
Chronic Deltoid Ligament Complex Injuries
Chronically injured ligaments may appear thickened and distorted ligament. Signal intensity is typically reduced on fat-suppressed fluid-sensitive sequences reflecting the higher composition of fibrosis (12a,13a). Alternatively, the torn ligament may be discontinuous and/or severely attenuated (13a). In general, there is less associated edema in the periligamentous soft tissues compared to an acute ligament injury. Reactive bony changes including sclerosis, spurring, and marrow edema may be present due to the altered stresses that accompany chronic instability.
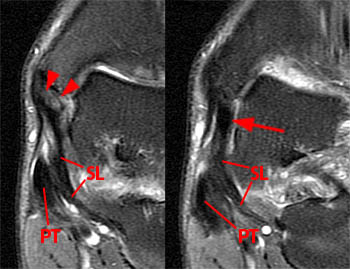
Figure 12:
48 year-old male with chronic medial pain and multiple ankle sprains. Coronal fat-suppressed images through the posterior (left) and anterior (right) portion of the anterior colliculus demonstrate a chronic partial avulsion of the tibiospring ligament (arrowheads). On the more anterior slice the tibionavicular ligament (arrow) is abnormally thickened and low in signal indicating fibrosis from remote trauma. The posterior tibial tendon (PT) and superomedial portion of the spring ligament complex (SL) are labeled.
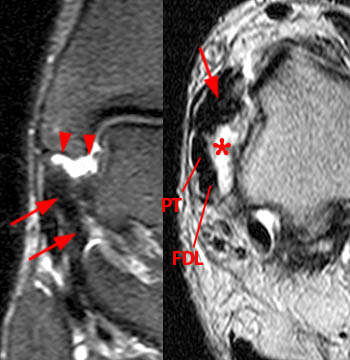
Figure 13:
44 year-old male with a history of remote eversion injury presents with chronic medial pain and instability. Coronal proton density fat-suppressed (left) and axial T2-weighted FSE (right) images demonstrate bare cortex at the intercollicular sulcus (arrowheads) with fluid signal filling the ligament defect (asterisk). In addition the superficial ligaments are scarred and appear abnormally thickened and irregular compatible with a chronic tear. The posterior tibial (PT) and flexor digitorum longus (FDL) tendons are indicated.
Impingement Syndromes
Impingement syndromes are named based on their location. On MRI a range of findings may be seen including loss of delineation of the ligament components replaced by amorphous or distorted architecture and signal related to scarring. Synvoitis may be evident and there may be capsular thickening, bony spurring, and small corticated ossicles embedded in the scarred ligament (14a,15a). Posteromedial impingement with prominent hypertrophic change may lead to medial displacement of the posterior tibial tendon.16 Osteochondral lesions of the talus are a frequent accompanying finding in posteromedial impingement.13
Figure 14:
50 year-old male with chronic anteromedial ankle pain on dorsiflexion. Fat-suppressed axial T2-weighted (left) and coronal proton density-weighted (right) images demonstrate amorphous soft tissue thickening (arrows) in the anteromedial capsular recess and adjacent osteophytes with marrow edema (arrowheads) consistent with anteromedial impingement.
Figure 15:
68 year-old male presents with 1 year history of posteromedial ankle pain and swelling. Coronal T1-weighted (left), coronal proton density-weighted fat-suppressed (middle), and axial T1-weighted images demonstrate distortion and thickening of the posterior tibiotalar ligament containing embedded ossicles (arrowheads) compatible with posteromedial impingement.
Treatment
Acute Deltoid Ligament Complex Injury
For acute injuries, conservative treatment is most commonly recommended consisting of rest, ice, compression, and elevation (RICE). In cases of lateral ankle ligament injury, the presence of a coexisting deltoid ligament injury may modify the physical therapy protocol to a less aggressive regimen.
Chronic Deltoid Ligament Complex Injury
In ankle instability associated with ankle fractures, if full mechanical stability is not achieved after internal fixation of an ankle fracture, reconstruction or repair of the deltoid ligament may be indicated. In some cases, interposition of the disrupted ligament between the medial malleolus and the talus may prevent appropriate healing and stability.
Surgical planning for deltoid ligament repair is dictated by the specific functional ligament deficiency. Two functional deltoid instability patterns are common. In the first the superficial ligament is insufficient with an intact deep ligament component. These patients present with increased rotational instability without tibiotalar joint instability with valgus stress or posterior translation. Proximal (Type I) injuries are frequent in this pattern and are often amenable to direct repair with reattachment of the avulsed TNL and TSL to the anterior medial malleolus.12
The second pattern is a more extensive injury that involves the superficial and deep components, resulting in increased rotational instability and coronal tibiotalar instability to valgus stress. Surgical reconstruction is commonly required and must fully address associated lateral ligamentous instability and/or posterior tibial tendon dysfunction, as well as abnormalities in limb alignment and mechanics. A variety of reconstruction techniques have been utilized to address deltoid ligament instability and associated posterior tibial tendon deficiencies. Surgical techniques include re-routing of the peroneus longus tendon through talar and medial malleolar bone tunnels, an autograft flexor hallucis longus tendon transfer, and tightening of the superficial deltoid ligament component by osteotomy of the ligament origin and proximal advancement of the ligament.12
In cases of progressive pronation and hindfoot valgus, calcaneus-lengthening osteotomy or tibiocalcaneal arthrodesis are additional options that may be considered.
Impingement
Both open and arthroscopic debridement procedures are successful in treating patients with anteromedial and posteromedial impingement syndrome.17,20
Conclusion
Deltoid ligament complex injuries are common. Both physical examination findings and radiographs are unreliable in detecting the presence of a deltoid ligament complex injury. MRI helps diagnose and assess the extent of acute deltoid ligament injuries and associated osseous and soft tissue injuries. MRI is also effective in evaluating the chronic complications of deltoid ligament injury, including medial ankle instability and medial impingement syndromes. The information MRI provides helps shape treatment strategies for patients with both acute and chronic deltoid ligament injuries.
References
1 Sarrafian SK: Anatomy of the Foot and Ankle: Descriptive, Topographical, Functional (ed 3). Philadelphia, PA, JB Lippincott Williams & Wilkins, 2011, pp 176-195.
2 Milner CE, Soames RW. The medial collateral ligaments of the human ankle joint: anatomical variations. Foot Ankle Int. 1998 May ;19 (5):289-92
3 Sarrafian SK: Anatomy of the Foot and Ankle: Descriptive, Topographical, Functional (ed 3). Philadelphia, PA, JB Lippincott Williams & Wilkins, 2011, pp 537-541.
4 Hintermann B. Biomechanics of the unstable ankle joint and clinical implications. Med Sci Sports Exerc 1999;31(Suppl 7):459-69.
5 Jahss MH, Gee RO, Kummer F. Deltoid insufficiency. Part II. Anatomy of the deltoid ligament. Presented at the AOFAS 9th Annual Summer Meeting, Vail, CO., July 21, 1993.
6 Mengiardi B, Pfirrmann CW, Vienne P, Hodler J, Zanetti M. Medial collateral ligament complex of the ankle: MR appearance in asymptomatic subjects. Radiology 2007;242(30):817-824.
7 Boss AP, Hintermann B. Anatomical study of the medial ankle ligament complex. Foot Ankle Int 2002;23:547-553.
8 Crim JR, Beals TC, Nickisch F, Schannen A, Saltzman CL. Deltoid Ligament Abnormalities in Chronic Lateral Ankle Instability. Foot Ankle Int 2011;32(9):873-878.
9 Hintermann B, Valderrabano V, Boss A, Trouillier HH, Dick W. Medial Ankle Instability An Exploratory, Prospective Study of Fifty-Two Cases. AJSM 2004;32(1):183-190.
10 Cheung Y, Perrich KD, Gui J, Koval KJ, Goodwin DW. MRI of Isolated Distal Fibular Fractures with Widened Medial Clear Space on Stressed Radiographs: Which Ligaments Are Interrupted. AJR 2009; 192:W7-W12.
11 DeAngelis NA, Eskander MS, French BG. Does medial tenderness predict deep deltoid ligament incompetence in supination-external rotation type ankle fractures? J Orthop Trauma 2007;21(4):244-247.
12 Beals TC, Crim J, Nickish F. Deltoid Ligament Injuries in Athletes: Techniques of Repair and Reconstruction. Oper Tech Sports Med 2010;18:11-17.
13 Chhabra A, Subhawong TK, Carrino JA. MR Imaging of Deltoid Ligament Pathologic Findings and Associated Impingement Syndromes. Radiographics 2010; 30:751-761.
14 Robinson P, White LM, Salonen D, Ogilvie-Harris D. Anteromedial impingement of the ankle: using MR arthrography to assess the anteromedial recess. AJR Am J Roentgenol 2002;178(3):601-604.
15 Egol KA, Parisien JS. Impingement syndrome of the ankle caused by a medial meniscoid lesion. Arthros-copy 1997;13(4):522-525.
16 Paterson RS, Brown JN, Roberts SNJ. The Posteromedial Impingement Lesion of the Ankle. AJSM 2001;29(5):550-557.
17 Manoli, Arthur. Medial Impingement of the Ankle in Athletes. Sports Health 2010;2(6):495-502.
18 Schuberth JM, Collman DR, Rush SM, Ford LA. Deltoid ligament integrity in lateral malleolar fractures: a comparative analysis of arthroscopic and radiographic assessments. J Foot Ankle Surg 2004;43:20-29.
19 Hintermann B, Knupp M, Pagenstert GI. Deltoid ligament injuries: diagnosis and management. Foot Ankle Clin 2006;11(3):625-637.
20 Robinson P. Impingement syndromes of the ankle. Eur Radiol 2007;17(12):3056-3065.