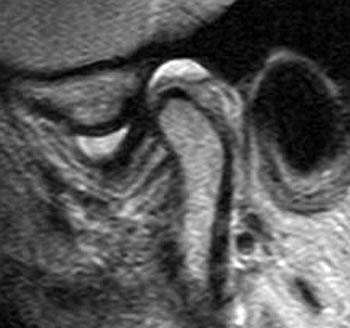
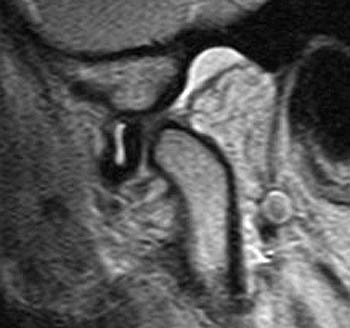
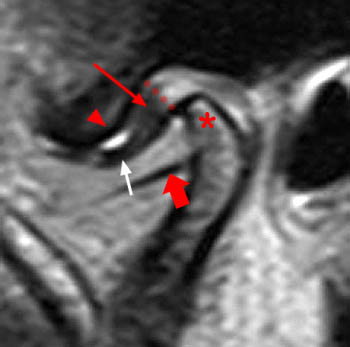
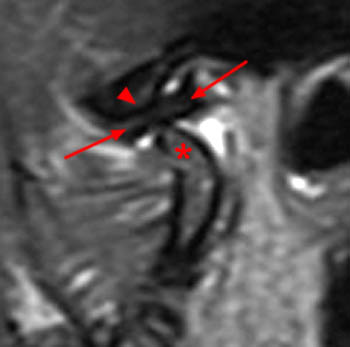
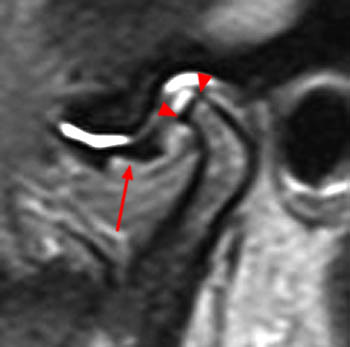
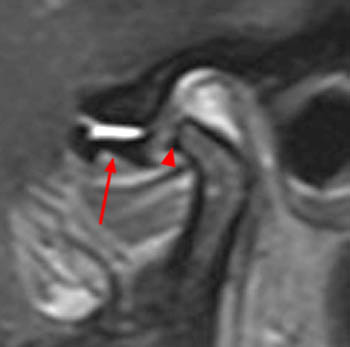
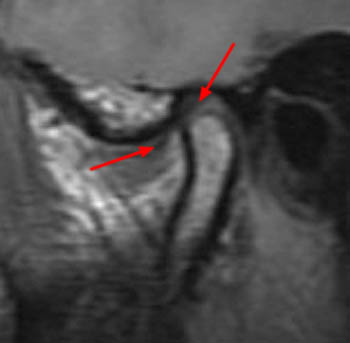
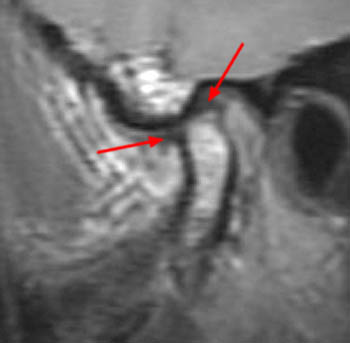
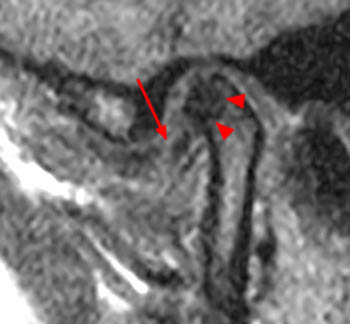
Clinical History: A 45 year-old female presents with a history of chronic ear pain and headaches. She recently experienced an episode of locking of her jaw. Oblique sagittal proton density-weighted images were obtained through the right temporomandibular joint in both the closed (1a) and open (1b) mouth positions. What are the findings? What is your diagnosis?
Findings
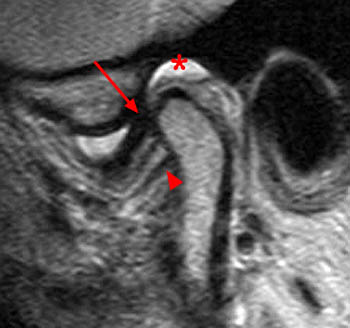
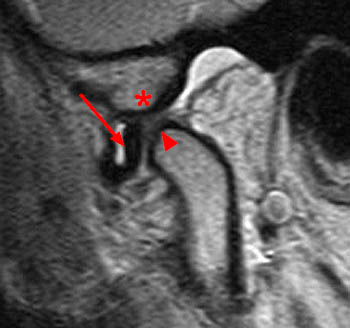
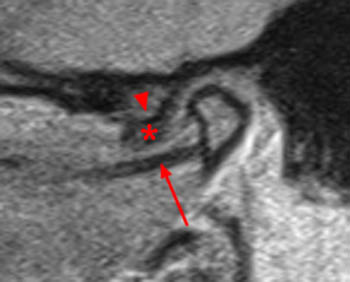
Figure 2:
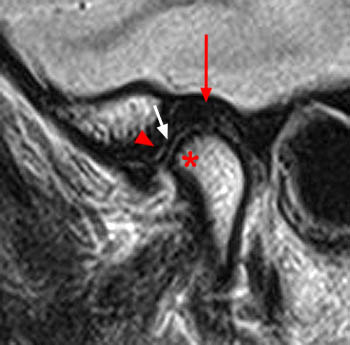
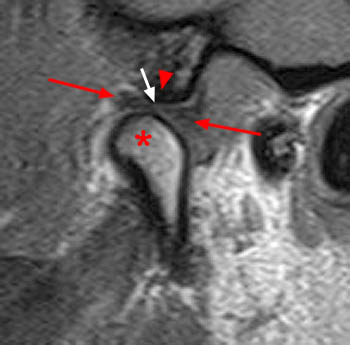
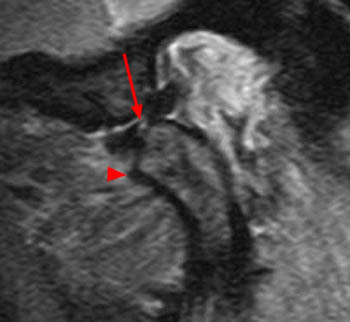
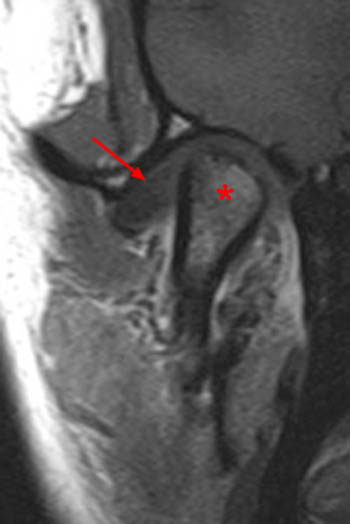
On the oblique sagittal image obtained with the mouth closed, the articular disc is displaced anteriorly (arrow). The articular disc has abnormal morphology with a thickened appearance of the central portion of the disc. In addition, the tendon of the inferior belly of the lateral pterygoid muscle is thickened (arrowhead). A moderate sized joint effusion is located in the superior joint compartment (asterisk). The mandibular condyle is normally located within the glenoid fossa of the temporal bone.
Diagnosis
Internal derangement of the right temporomandibular joint with anterior displacement of the articular disc without reduction.
Introduction/Background
The temporomandibular joint (TMJ) is undoubtedly one of the most actively used and least understood joints in the body. Up to 30% of the population experiences symptoms related to the TMJ and up to 7% seek treatment.1 The highest prevalence of temporomandibular disorders is in women aged 20 – 40 years, with women representing 80% of patients being treated for TMJ disorders.2 Common symptoms include joint pain and crepitus. Clinical diagnosis of TMJ disorders can be challenging, particularly considering the psychosocial factors that can be involved in pain disorders. Therefore, magnetic resonance imaging (MR) of the TMJ has gained an important role in the diagnosis of TMJ disorders. MRI can directly visualize the disc, accurately determine disc position and morphology, and evaluate condylar motion in a noninvasive manner.3
Anatomy and Biomechanics
An understanding of the normal anatomy and biomechanics of the TMJ is essential for the accurate interpretation of imaging studies. Much of the current understanding of the normal function of the TMJ has been gained through diagnostic imaging studies, including radiography, tomography, arthrography, and MR imaging.
The TMJ is divided into upper and lower compartments by a dense, fibrous disc or meniscus. (Figure 1) It is classified as a diarthrodial joint having two functional movements; a predominantly rotatory movement between the condylar head and disc in the lower compartment and a predominantly gliding motion in the upper compartment.
The TMJ has both osseous and soft tissue components. The osseous components are the condylar head of the mandible and the glenoid fossa and articular eminence of the temporal bone. The soft tissue components include the articular disc and the joint capsule. In contrast to other joints, which are lined with hyaline articular cartilage, the articular surfaces of the TMJ are lined by fibrous tissue. The normal condylar head has a more pronounced convexity from front to back and a more gradual convexity medial to lateral. As a result, the anteroposterior dimension of the normal condylar head is approximately one half of the medial-lateral dimension.4 In the closed-mouth position, the condylar head is normally directed toward the posterior aspect of the articular eminence and not the deepest portion of the glenoid fossa. (Figure 4a)
Figure 4:
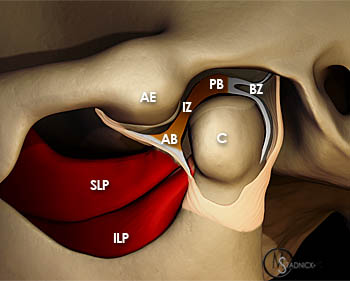
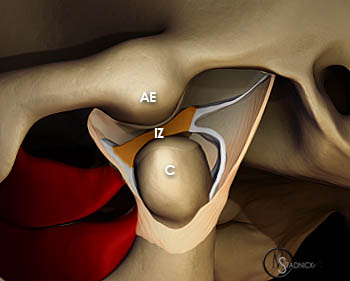
A 3D graphic lateral view of the temporomandibular joint with the capsule partially removed depicts the normal position of the articular disc between the articular eminence of the temporal bone (AE) and the mandibular condyle (C) with the mouth closed. The articular disc demonstrates a thicker anterior band (AB) and posterior band (PB) separated by a thinner intermediate zone (IZ). The bilaminar zone (BZ) and the superior (SLP) and inferior (ILP) bellies of the lateral pterygoid muscle are also indicated.
The intra-articular disc is a biconcave plate of dense fibrous tissue separating the condylar head from the glenoid fossa. This divides the joint into two synovial lined compartments. The outer margins of the disc are thickened. The thickened area anterior to the condylar head is termed the anterior band, while the thickened area located posterior to the condylar head is known as the posterior band. The central or intermediate zone is the thinnest segment of the disc located between the anterior and posterior bands. Anteriorly, the disc is attached to the joint capsule. In addition, tendinous fibers from the superior belly of the lateral pterygoid muscle insert on the anterior band. Fibers from the inferior belly of the lateral pterygoid muscle insert on the anterior aspect of the condylar head. The posterior band is continuous with the posterior attachment or bilaminar zone. The bilaminar zone is composed of fibroelastic tissue and collagen fibers and fills the posterior half of the glenoid fossa.
In the closed mouth position the junction of the posterior band and the bilaminar zone should lie immediately above the condylar head near the 12 o’clock position.(C) To be within the 95th percentile of normal, the junction of the posterior band and bilaminar zone should fall within 10 degrees of vertical.5 However, using this criterion will result in a diagnosis of anterior displacement in up to one third of asymptomatic volunteers. Other authors have suggested that a disc should be considered anteriorly displaced if it is located more than 30 degrees from the vertical.6 This controversy has led others to adopt the term partial anterior displacement when the disc is displaced more than 10 degrees from vertical but less than 30 degrees.7 Kaplan and Helms suggest that the position of the thin intermediate zone is more important. They state that the normal position of the articular disc, regardless of whether or not the mouth is open or closed, is with the thin intermediate zone interposed between the condyle and the temporal bone, wherever the two bones are most closely apposed.8
Figure 5:
Normal Closed Mouth. Oblique sagittal T2 weighted image of the left TMJ in a 22yo female. The mandibular condyle is normally located within the glenoid fossa. The articular disc has a normal biconcave appearance and is normally located. The junction of the posterior band and bilaminar zone lies at the superior or 12 o'clock position of the condyle (arrow). Also note the thin intermediate zone (white arrow) lies between the condyle (asterisk) and articular eminence (arrowhead) where the two bones are most closely apposed.
Two motions occur at the TMJ with mouth opening. (6a,7a) First, rotation occurs in the lower joint compartment with the condyle rotating on the disc in a hinge-like manner. Second, the condyle and disc translate anteriorly as a result of motion within the superior joint compartment. At the full open position, the condyle is positioned directly under or slightly anterior to the articular eminence.9 The elastic tissue of the bilaminar zone allows for the motion of the disc. In the open mouth position, the thin intermediate zone of the disc maintains its position between the articulating surface of the mandibular condyle and the articular eminence.
Figure 7:
Normal Open Mouth. Oblique sagittal T1-weighted image of the same patient in (5a), obtained with the mouth open. Normal anterior translation of the condyle results in the condyle (asterisk) articulating with the inferior aspect of the articular eminence (arrowhead). The articular disc maintains its normal biconcave appearance (arrows). The intermediate zone of the articular disc remains positioned between the surfaces of the condyle and the eminence that are most closely apposed (white arrow).
MR of Internal Derangement of the TMJ
The most common intra-articular abnormality of the TMJ is internal derangement, which has been defined as an abnormal position of the disc in relation to the mandibular condyle and temporal eminence. The etiology is uncertain, however, the condition is three to five times more common in females and symptoms typically become evident by the fourth decade.10
Internal derangement is a progressive process. Initially, anterior, medial, or lateral displacement of the disc may be evident in the closed mouth position that reduces with mouth opening. As the elastic fibers in the bilaminar zone become lax, the disc no longer reduces with mouth opening and anterior translation of the condyle may be limited. Over time, the disc becomes deformed, secondary osseous and articular degenerative changes occur, and perforations of the disc may develop.6,10
Wilkes described the clinical stages of internal derangement in 1989.11 {TABLE 1} During the early stage there is clicking with early mouth opening or later with the closing phase, with no pain or limited motion. Clicking is often the most common complaint, occurring in 53% of patients. This typically occurs when the anteriorly displaced disc reduces with mouth opening.12 Over time, there is a progressive increase in symptoms, with limited motion, pain, tenderness, and crepitus. Shellhas correlated the imaging and histologic features of internal derangement similar to the clinical and surgical correlation of Wilkes.10 {TABLE 2} MR findings must be correlated with clinical features, as up to 34% of patients may have some degree of disc displacement without symptoms.13
TABLE 1
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Stage | MR features |
| I | Anterior disc displacement, reduces with opening |
| II | Disc displacement and deformity, reduces with opening |
| +/- signal changes in disc, +/- joint effusion | |
| III | Disc displacement and deformity, no reduction with opening |
| +/- Joint effusion | |
| IV | Severe disc deformity and displacement, no reduction with opening |
| Joint effusion, Osseous changes | |
| V | Severe disc deformity, no reduction with opening |
| Disc perforation, progressive osseous deformity |
Although Wilkes and Shellhas described five stages of disc derangement, other authors simplify the categorization of internal derangement on imaging from least severe to most severe as follows8,14:
– Anterior disc displacement with reduction with mouth opening. (8a)(9a)
– Anterior disc displacement without reduction with mouth opening. (2a)(3a) and (10a)(11a)
– Chronic anterior disc displacement with disc perforation and features of degenerative joint disease. (12a)(13a)
Figure 8:
Anterior disc displacement with reduction. Oblique sagittal fat-suppressed proton density-weighted image of the closed right TMJ in a 64yo female with 8 weeks of jaw pain. The articular disc is anteriorly displaced. The junction of the posterior band and bilaminar zone (dotted line) lies at the anterior margin of the condyle (asterisk). Also note, the intermediate zone (white arrow) is not located between the articular surfaces of the condyle and eminence (arrowhead). The posterior band of the articular disc is slightly thickened (arrow). The tendon of the inferior belly of the lateral pterygoid muscle (broad arrow) is mildly thickened. A small effusion lies within the superior joint compartment.
Figure 9:
Anterior disc displacement with reduction. Same patient as (8a). Oblique sagittal fat-suppressed proton density-weighted image with the mouth open. The articular disc has reduced and is now normally located (arrows). Anterior translation of the condyle (asterisk) is slightly reduced as the condylar head still lies slightly posterior to the articular eminence (arrowhead). Small joint effusions are seen within both the superior and inferior joint compartments. Often, joint effusions are more easily seen on the open mouth images.
Figure 10:
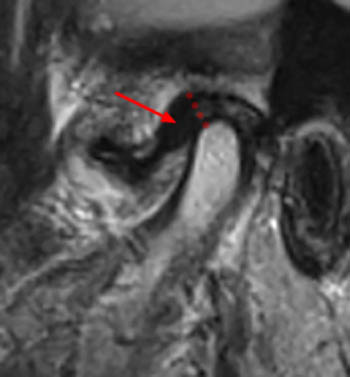
Anterior disc displacement without reduction. Same patient as (8a) and (9a). Oblique sagittal closed mouth image obtained through the left TMJ. The articular disc is displaced more anteriorly than seen on the right. and has a somewhat buckled appearance (arrow). The entire disc lies inferior to the articular eminence and is anterior to the condylar head. A moderate sized joint effusion lies within the superior joint compartment. The condylar head also demonstrates early osteophyte formation, with the margins of the condylar head appearing somewhat pointed (arrowheads).
Figure 11:
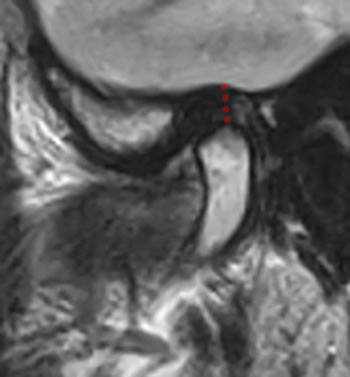
Anterior disc displacement without reduction. Same patient as (10a). Oblique sagittal image with the mouth open. The articular disc remains anteriorly displaced and is buckled centrally (arrow). The anterior translation is more limited than that seen on the right. Small condylar osteophytes (arrowhead) and a superior compartment joint effusion are again seen.
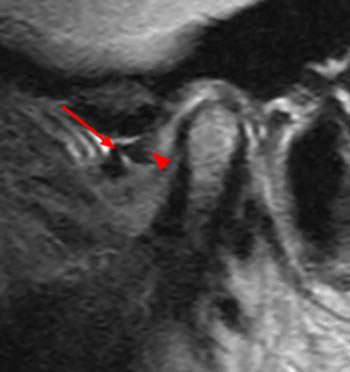
Figure 12:
Disc perforation and features of degenerative joint disease. Oblique sagittal fat suppressed proton density-weighted image in the open mouth position of the right TMJ in a 57 yo female with chronic jaw pain, popping, and clicking. The condylar head is slightly deformed with small anterior osteophytes (arrowhead). A small central perforation of the intermediate zone of the articular disc is seen (arrow).
With this understanding of the normal anatomy, biomechanics, and the features of internal derangement, the following features should be assessed on MR evaluation of the TMJ: the position and morphology of the articular disc, disc deformity or perforation, joint effusion and marrow edema, osteoarthrosis, the lateral pterygoid muscle, and the retrodiscal tissues.
Disc displacement – A key point in the evaluation of the TMJ is the position of the articular disc. Displacement of the disc is present in approximately 80% of symptomatic patients.15 It should be described as normally located, anteriorly displaced with reduction, or anteriorly displaced without reduction. This is best evaluated on sagittal images obtained through the joint. It is important to evaluate the articular disc along its entire width, from medial to lateral. In some patients with early stages of internal derangement, only the medial or lateral pole of the disc will be abnormal. (13a,14a)
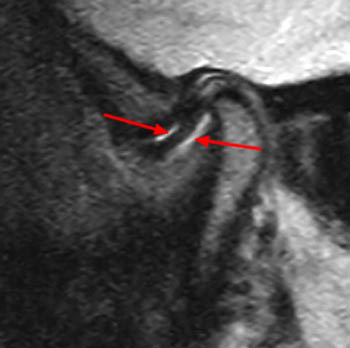
Figure 13:
Oblique sagittal T2 weighted image in the closed mouth position obtained through the lateral aspect of the right TMJ in a 55yo female with complaints of jaw pain and popping. The articular disc is slightly anteriorly displaced (dotted line) with slight thickening of the posterior band (arrow).
Mediolateral displacement of the disc is less common and is best identified on coronal oblique images. (15a)
In some cases, a “stuck disc” is identified, typically due to fibrous adhesions that prevent any disc motion. (16a,17a)
Figure 17:
Same patient as (16a). Oblique sagittal T1-weighted image with the mouth open. The degree of mouth opening and anterior translation was normal on the left side which was imaged at the same time. Only minimal anterior translation of the right condyle is seen. The articular disc is unchanged in position from the closed mouth images (arrows). This reflects a "stuck" disc and is likely related to fibrous adhesions within the joint.
Disc deformity and perforation – As degeneration of the joint becomes more advanced, the disc will appear deformed, losing its normal biconcave appearance. (18a) Disc morphology should be described as flattened, thickened, buckled, or folded. The abnormal disc contour can involve the entire disc or can be confined to one portion of the disc. Disc perforation can be difficult to recognize and is often found with changes of degenerative joint disease. (12a) Perforations are often easier to visualize in the open mouth position and in the presence of a joint effusion.
Joint effusion and marrow edema – These are best evaluated on T2-weighted or STIR images in the sagittal or oblique sagittal plane. A joint effusion may be confined to either the superior or inferior joint compartment, or may involve both. (19a) It has been postulated that marrow signal abnormalities may reflect marrow edema, osteonecrosis, or may be related to osteoarthrosis. Sano et al. reported that joints with bone marrow signal alterations were more painful than joints with normal marrow signal.16(20a)
Figure 19:
Oblique sagittal fat-suppressed proton density weighted-image through the closed left TMJ in a 23 yo female with jaw pain and popping. The articular disc is anteriorly displaced and is thickened centrally. Small joint effusions are seen within the superior and inferior joint compartments. (arrows)
Figure 20:
Oblique sagittal T1-weighted image of the closed left TMJ in a 30 yo female with jaw pain, clicking, and limited motion. The articular disc is anteriorly displaced and is thinned posteriorly (arrow). The joint is narrowed with early osteophytes at the condylar head. Marrow edema within the condylar head is reflected by decreased signal intensity of the marrow instead of the fatty marrow signal normally seen within the condyle (arrowheads). (Compare this appearance with the normal fatty marrow within the condyle seen on T1 images in figures 7a and 17a)
Osteoarthrosis – An erosion of the mandibular condyle may be the earliest osseous manifestation of degenerative change of the TMJ.8 More advanced changes include osteophyte formation, subchondral cyst formation, and low signal in the subchondral bone compatible with sclerosis.
Lateral pterygoid muscle abnormalities – Recent work has noted the importance of the lateral pterygoid muscle in internal derangement of the TMJ. 17,18 As described above, the lateral pterygoid muscle inserts on the articular disc and the mandibular condyle. Hypertrophy, atrophy, and fibrosis of the lateral pterygoid muscle have been described in patients with clinical symptoms of pain and limited motion. Thomas et al described a thickened appearance of the tendon insertions in symptomatic patients.18(21a)
Figure 21:
Oblique sagittal proton density weighted image through the closed left TMJ of a 30 y/o female with chronic jaw pain. The articular disc is anteriorly displaced and lies beneath the articular eminence (arrowhead). The disc is thickened and foreshortened (asterisk). Immediately below the displaced disc lies the markedly thickened tendon of the inferior belly of the lateral pterygoid muscle (arrow). This appearance has been described as a "double disc" sign.
Retrodiscal tissues – The retrodiscal tissues consist of the fibroelastic tissue and collagen fibers of the bilaminar zone as well as neurovascular elements that fill the posterior half of the glenoid fossa. Some authors feel that compression of the retrodiscal soft tissues is one of the factors in pain generation.11 Sano et al described increased retrodiscal soft tissue T2 signal in symptomatic joints, likely reflecting hyperemia and perivascular inflammation.16 More chronic pathology is likely reflected by fibrosis and decreased signal in the retrodiscal tissues.
As the decision to treat patients is made primarily on the basis of patient symptoms – most notably the range of motion and presence of pain19 – it may be prudent to focus on the imaging findings that are most associated with these symptoms. In a recent study by Emshoff et al.20, the MR findings most associated with TMJ pain were disc displacement without reduction and the presence of bone marrow edema.
Treatment/Clinical management
Nonoperative management of patients with TMJ disorders includes soft diet, heat, nonsteroidal anti-inflammatory drugs, muscle relaxants, occlusal splints, and physical therapy. Surgery is indicated when nonoperative management has failed to resolve disc displacement and significant symptoms persist. The surgical procedures that may be performed include disc plication, discectomy, and recontouring of the articular eminence. Following discectomy, either a synthetic or autogenous implant can be placed. The role of operative or nonoperative treatment is complicated by the fact that symptoms decrease with age and are often self-limiting.21
Conclusion
MRI examination of the TMJ is part of the current standard of care in the evaluation of patients with temporomandibular joint disorders. The anatomic information obtained can be combined with the clinical information to guide treatment decisions. An understanding of the normal anatomy and biomechanics of the joint will aid the radiologist in evaluating patients with internal derangement of the joint.
References
1 Solberg WK, Woo MW, Houston JB. Prevalence of mandibular dysfunction in young adults. J AM Dent Assoc 1979;98(1):25-34.
2 Kuttila M, Niemi PM, Kuttila S, et al. TME treatment need in relation to age, gender, stress, and diagnostic subgroup. J Orofac Pain. 1998;12(1):67-74.
3 Emhoffs R, Brandlmaier I, Bertram S, et al. Comparing methods for diagnosing temporomandibular joint disc displacement without reduction. J Am Dent Assoc 2002;133(4):442-451.
4 Goaz PW, White SC, Blasche DD: The temporomandibular joint. In Goaz PW, White SC 9eds): Oral Radiology: Principle and Interpretation, ed 2. St. Louis, CV Mosby, 1987, pp 654-682.
5 Drace JE, Enzmann DR. Defining the normal temporomandibular joint: closed-, partially open-, and open-mouth MR imaging of asymptomatic subjects. Radiology 1990;177(1):67-71.
6 Rammelsberg P, Pospiech PR, Jager L, et al. Variability of disc position in asymptomatic volunteers and patients with internal derangements of the TMJ. Oral Surg Oral Med Oral Path Oral Radiol Endod 1997;83(3):393-9.
7 Aiken A, Bouloux G, Hudgins P. MR Imaging of the Temporomandibular Joint. Magn Reson Imaging Clin N Am 2012;20:397-412.
8 Kaplan PA, Helms CA. Current status of temporomandibular joint imaging for diagnosis of internal derangements. Am J Roentgenol 1989;152:697-705.
9 Wang EY, Fleisher KA. MRI of temporomandibular joint disorders. Applied Radiol 2008;37(9):17-25.
10 Schellhas KP. Internal derangement of the temporomandibular joint; Radiologic staging with clinical, surgical, and pathological correlation. Magn Reson Imaging 1989;7:495-515.
11 Wilkes CH. Internal derangements of the temporomandibular joint. Pathologic variations. Arch Otolaryngol Head Neck Surg 1989;115:469-477
12 Cholitgul W, Nishiyama H, Sasai T, et al. Clinical and magnetic resonance imaging findings in temporomandibular joint disc displacement. DentoMaxilloFac Radiol 1997;26(3):183-188.
13 Katzberg RW, Westersson PL, Tallents RH, et al. Anatomic disorders of the temporomandibular joint disc in asymptomatic subjects. J Oral Maxillofac Surg 1996;54(2):147-53.
14 Rao VM, Bacelar MT. MR imaging of the temporomandibular joint. Neuroimaging Clin N Am 2004;14(4):761-75.
15 Tasaki MM, Westesson PL, Isberg AM, et al. Classification and prevalence of temporomandibular joint disc displacement in patients and symptom-free volunteers. Am J Orthod Dentofacial Orthop. 1996;109:249-262.
16 Sano T, Westesson PL, Larheim TA, Takagi R. The association of temporomandibular joint pain with abnormal bone marrow in the mandibular condyle. J Oral Maxillofac Surg. 2000;58:254-257.
17 Taskaya-Yilmaz N, Ceylan G, Incesu L, Muglali M. A possible etiology of the internal derangement of the temporomandibular joint based on the MRI observations of the lateral pterygoid muscle. Surg Radiol Anat. 2005;27(1):19-24.
18 Thomas X, Pomes J, Berenguer J, et al. MR imaging of temporomandibular joint dysfunction: A pictorial review. Radiographics 2006;26:765-781.
19 Widmark G. On surgical intervention in the temporomandibular joint. Swed Dent J Suppl. 1997;123:1-87.
20 Emshoff R, Brandlmaier I, Gerhard S, et al. Magnetic resonance imaging predictors of temporomandibular joint pain. J Am Dent Assos. 2003;134:705-714.
21 Rasmussen OC. Description of population and progress of symptoms in a longitudinal study of temporomandibular arthroplasty. Scand J Dent Res. 1981;889:196-302.