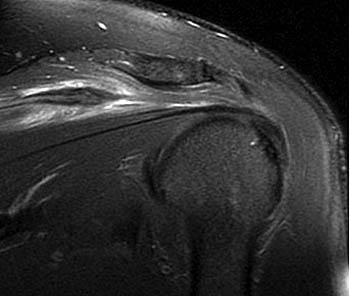
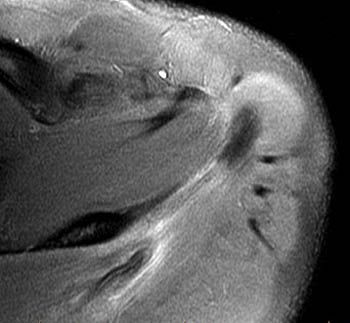
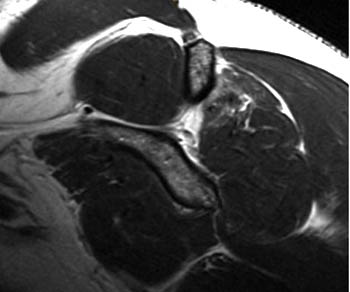
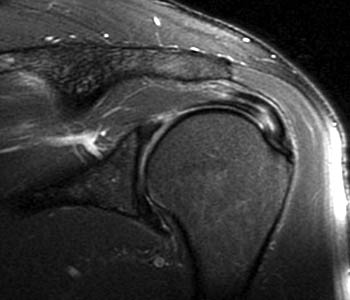
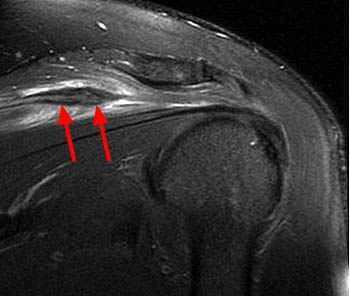
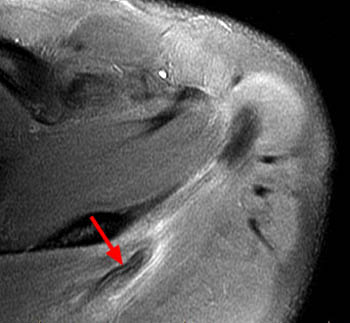
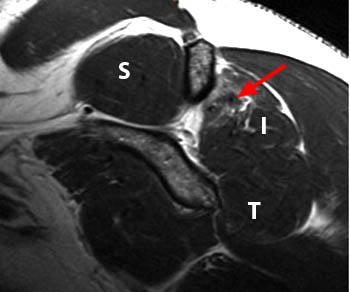
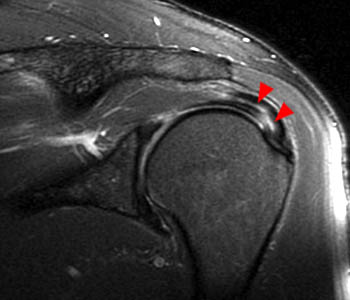
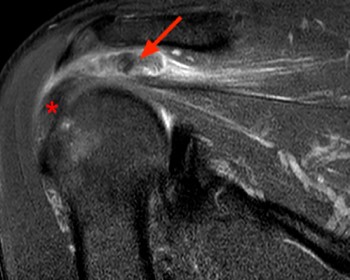
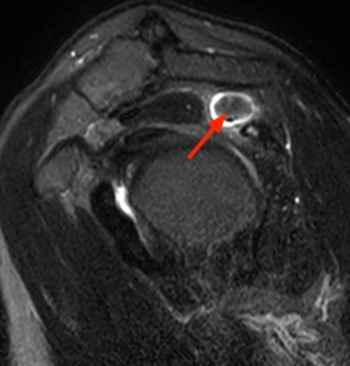
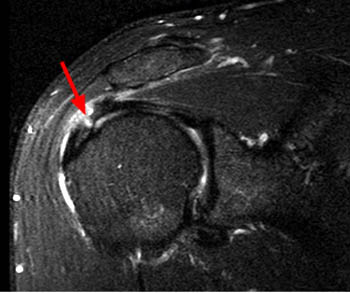
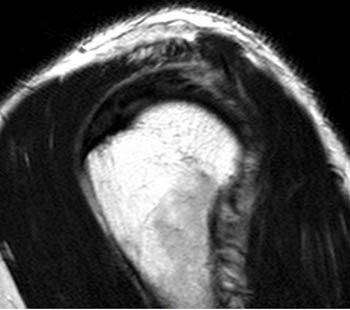
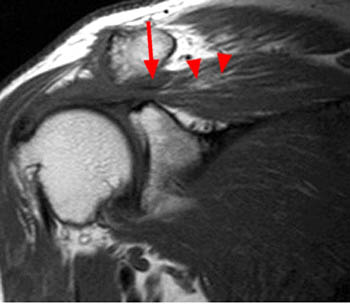
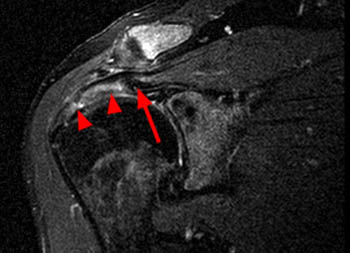
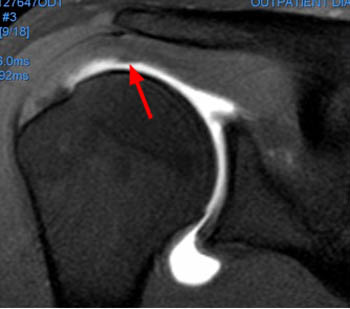
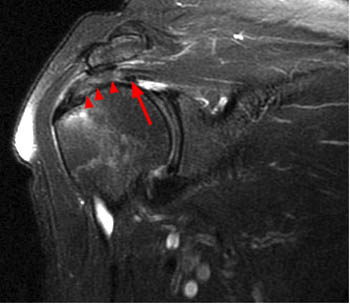
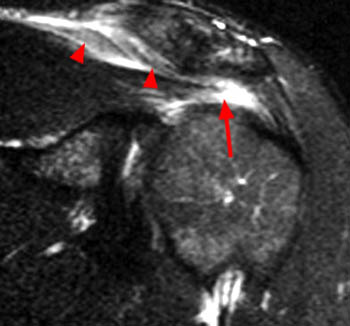
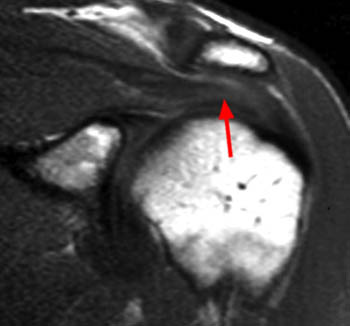
Clinical History: An orthopaedic surgeon requests an over-read of a pre-operative MRI that was presumed to be false positive, as no rotator cuff tear was found at surgery. The patient is a 54 year-old male who experienced shoulder pain following a pulling injury. (1a,1d) Fat-suppressed T2 weighted coronal obliques, (1b) fat-suppressed proton density axial, and (1c) T2-weighted sagittal images are provided. What are the findings? What is your diagnosis?
Findings
Diagnosis
Retracted, delaminating interstitial tear of the infraspinatus.
Introduction
Evaluation of the rotator cuff is the most common indication for shoulder MR. Pitfalls in the correct interpretation of shoulder MR may arise either from suboptimal descriptions of pathology or from atypical appearances of the normal or abnormal rotator cuff.
Interstitial Tears of the Infraspinatus
Partial tears of the rotator cuff are known to be more difficult to reliably detect on MR than full thickness tears1,2, and of these tears, delaminating tears with horizontal components are felt to be particularly challenging3,4. The infraspinatus tendon is more prone to delaminating tears than the supraspinatus, likely due to its bipennate anatomy5. The infraspinatus is composed of oblique and transverse components, with the oblique part comprising the main tendinous component and the weaker, more cephalad transverse part inserting upon the oblique component tendon as a thin tendinous membrane.
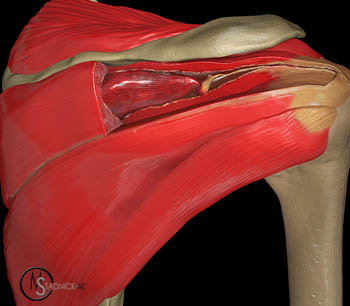
Figure 6:
A 3D graphic of the posterior shoulder with the posterior portion of the superior infraspinatus muscle removed depicts a retracted, delaminating interstitial tear of the infraspinatus. Such tears typically involve the anterosuperior infraspinatus and may be completely contained within the substance of the infraspinatus.
The above case demonstrates a situation where a combination of an unusual tear pattern and a suboptimal tear description resulted in what was felt to be a false positive MR report, but in reality the case is of a false negative shoulder arthroscopy. The MR clearly demonstrates a rotator cuff tear, as retracted tendon fibers are undoubtedly present. However, to the surgeon, the cuff appeared intact both from the articular side and the bursal surface, as the tear is completely contained within the substance of the infraspinatus muscle and tendon. The key in such cases is to carefully describe the delaminating, interstitial nature of the tear, so that in cases where surgery is deemed necessary, the surgeon knows that exploration of the musculotendinous unit will be necessary in order to identify the region of tearing.
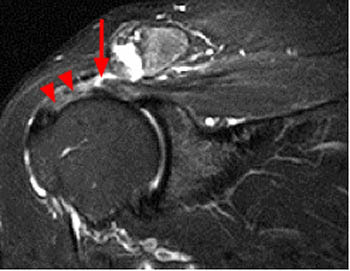
Another characteristic infraspinatus interstitial tear pattern involves those that primarily occur at the musculotendinous junction. These tears can involve large portions of the infraspinatus but despite a dramatic appearance on MRI can appear normal to the surgeon at arthroscopy. The following case is one in which the radiologist incorrectly described an infraspinatus tear as full thickness, when in reality thin intact components of the infraspinatus tendon are present at both the articular and bursal sides, effectively hiding the tear from the surgeon at arthroscopy. This case is of a 62 year-old male who experienced pain beginning 4 weeks earlier due to a pulling injury (7a-9a).
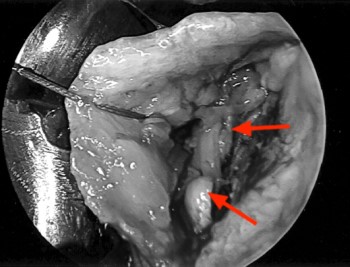
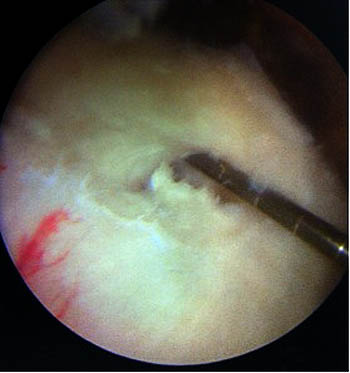
Figure 9:
At arthroscopy, no tear was visible from the articular or bursal sides of the cuff. The infraspinatus tendon was then opened from the bursal side and the retracted stump (arrows) was readily identified and subsequently repaired. Operative photo courtesy of Allen F. Anderson, MD, Tennessee Orthopaedic Alliance, Nashville, TN.
Such musculotendinous junction tears of the infraspinatus have been described in the surgical literature as the “novel lesion of the infraspinatus”.6 Patients tend to average 50 years of age and intense intramuscular edema is common at MR imaging. The lesions are important to correctly characterize and describe, as the majority of these patients will develop severe fatty atrophy of the infraspinatus over time. Although surgical results in such cases have not been encouraging, it is possible that early diagnosis and tendon repair may restore muscle tension and prevent complete functional muscle loss7.
Low signal intensity rotator cuff tears
The diagnosis of a rotator cuff tear is typically made by the identification of a fluid signal intensity gap within the cuff, appearing markedly hyperintense on T2-weighted images, particularly when fat suppression is applied. However, not all rotator cuff tears demonstrate this classic appearance, and indeed some tears are of relatively low signal intensity on T2-weighted images due to the development of scar and/or granulation tissue that fills the defect (10a-17a). In such cases, accurate interpretation of the MR is more challenging, and detection of findings such as an abrupt change in tendon signal or contour, retraction of tendon fibers, retraction of the musculotendinous junction, or identification of fatty atrophy are useful for making the diagnosis.
Figure 12:
The patient was treated conservatively but returned for repeat imaging after 3 months of failed conservative therapy. The fat-suppressed T2-weighted coronal image now reveals ill-defined increased signal intensity (arrow) in the region of the previously seen tear, appearing considerably less hyperintense than on the prior exam.
Figure 14:
At surgery, despite the low signal intensity in the region of abnormality, debridement from the bursal surface leads to identification of a high grade bursal surface tear. The arthroscopic probe lies within the defect. Photo courtesy of Thomas Dovan, MD. Elite Orthopaedics and Sports Medicine, Nashville, TN.
Figure 15:
A fat-suppressed T2-weighted oblique coronal image in a patient with shoulder pain reveals moderately increased signal intensity throughout much of the supraspinatus tendon (arrowheads), with focal bursal sided irregularity (arrow) just lateral to the musculotendinous junction. A discrete fluid-filled gap is not apparent.
Figure 16:
The corresponding T1-weighted image reveals that the musculotendinous junction (arrow) of the supraspinatus lies at or just medial to the glenohumeral joint. Mild fatty atrophy of the supraspinatus (arrowheads) is also apparent. As the musculotendinous junction of the supraspinatus typically lies at a level of the mid humeral head, this degree of retraction allows one to more confidently suggest that a significant tear of the rotator cuff is present.
Figure 17:
A T2-weighted fat-suppressed oblique coronal image from another patient with chronic shoulder pain. A rotator cuff tear is evident along the articular side of the supraspinatus (arrowheads), where abnormal, though relatively low signal intensity is apparent. Lax, redundant articular sided fibers (arrow) are seen medial to the region of tearing.
It should be noted that low signal intensity tears may not leak at arthrography as the scar/granulation tissue can maintain a water-tight seal. Similarly, these tears may not be initially apparent at surgery. However, if correctly identified and described on MR, the surgeon can probe and/or debride the area of interest, identifying the friable tissue that represents the rotator cuff tear.
The Rotator Cable
The rotator cable was named by Burkhart and colleagues9, who characterized and described the biomechanical role of this fibrous band that courses along the undersurface of the supraspinatus and infraspinatus tendons. The rotator cable lies perpendicular to the cuff tendon fibers, and blends with the coracohumeral ligament and transverse ligament of the bicipital groove anteriorly. Those fibers of the rotator cuff that lie lateral to the cable are referred to as the crescent. Burkhart feels that in younger patients, the crescent plays the primary biomechanical role in rotator cuff function, but with age, as the crescent weakens, the cable undergoes hypertrophy and assumes an important role in shielding the crescent from stress10. Burkhart described that the rotator cable functions as a “suspension bridge”, and as long as its anterior and posterior attachments remain intact, the cable is able to absorb load upon the cuff even in the presence of tears of the crescent.
The rotator cable is visible on MR images as a low signal intensity band along the undersurface of the supraspinatus and infraspinatus tendons11(19,20). Although some authors suggest that the cable can be seen in all imaging planes in all patients, in our experience the cable is inconsistently visible, and tends to be less well seen in younger patients and those with intact rotator cuffs.
With regard to MR interpretation, the rotator cable can serve as both a minor pitfall and an aide to diagnosis in the evaluation of the rotator cuff. If one is unaware of this structure, it may be confused for retracted undersurface fibers in the context of a rotator cuff tear. However, such a mistake may actually lead to the correct overall diagnosis, as Sheah found that when the cable is readily visible on routine MR images, that a partial articular surface tear of the rotator cuff is more likely to be present12(21,22). The more prominent cable is likely due to a combination of cable hypertrophy and cable redundancy in response to laxity of the undersurface of the cuff when an articular sided tear is present. Thus if one is uncertain whether a tear is truly present, visualization of the cable serves as an ancillary finding that supports the existence of a rotator cuff tear (23).
Figure 23:
A fat suppressed T2-weighted oblique coronal image demonstrates prominent visualization of the rotator cable (arrow) in a patient with an arthroscopically proven low signal intensity partial tear of the rotator cuff. A classic fluid signal intensity rotator cuff tear is not apparent, but a low signal intensity articular sided tear is strongly suggested due to the abrupt change in morphology of the articular surface (arrowheads) lateral to the cable.
Rotator cuff contusion
Rotator cuff contusions are another example where an atypical cuff appearance may result in a diagnostic challenge. Rotator cuff contusions occur in the setting of direct or indirect trauma, and are a not uncommon injury in athletes who participate in contact sports. On MR images of rotator cuff contusion, tendon edema can be striking and result in hyperintensity on T2-weighted images that approaches the brightness of fluid (24), particularly when fat suppression is applied. However, unlike rotator cuff tears, tendon fiber continuity is preserved and the musculotendinous junction should remain taught and normally positioned (25). Ancillary findings such as peri-tendon edema and bone bruises are frequently present13.
Figure 24:
A fat-suppressed T2-weighed oblique coronal image from a 28 year-old professional football player who suffered a direct painful blow to the shoulder when making a tackle. An area of marked T2 hyperintensity (arrow) is evident at and adjacent to the musculotendinous junction of the supraspinatus. Edema and hemorrhage are also apparent within the subacromial bursa and along the cephalad margin of the supraspinatus muscle belly (arrowheads).
Figure 25:
On the corresponding T1-weighted image, normal linear appearing tendon fibers are visible in the region of previous T2 hyperintensity (arrow). The musculotendinous junction remains taught and normally positioned. At surgery, the rotator cuff was edematous but intact, with surrounding soft-tissue edema and hemorrhage. The patient returned to play in several weeks without sequelae.
Conclusion
When interpreting MR of the rotator cuff, it is important to recognize atypical cuff findings and thus avoid pitfalls that may lead to suboptimal results. Certain tear patterns must be accurately described in order for the orthopaedic surgeon to identify the abnormality at surgery and provide appropriate care. Additional understanding that signal intensity patterns of the torn and untorn rotator cuff are not always classic allows the astute interpreter of shoulder MR to more likely make a correct diagnosis.
References
1 de Jesus JO, Parker L, Frangos AJ, Nazarian LN. Accuracy of MRI, MR arthrography, and ultrasound in the diagnosis of rotator cuff tears: A meta-analysis. AJR Am J Roentgenol. 2009;192:1701
2Balich SM, Sheley RC, Brown TR, Sauser DD, Quinn SF. MR imaging of the rotator cuff tendon:Interobserver agreement and analysis of interpretive errors. Radiology. 1997;204:191-194.
3Polster JF, Schickendantz MS. Shoulder MRI: What do we miss? AJR 2010; 195(3):577-584.
4Lee SY, Lee JK. Horizontal component of partial thickness tears of rotator cuff: imaging characteristics and comparison of ABER view with oblique coronal view at MR arthrography-initial results. Radiology 2002; 224:470-476.
5Kato A, Nimura A, Yamaguchi K, et al. An anatomical study of the transvers part of the infraspinatus muscle that is closely related with the supraspinatus muscle. Surg Radiol Anat 2012; 34(3):257-65.
6Lunn JV, Castellanos-Rosas J, Tavernier T, et al. A novel lesion of the infraspinatus characterized by musculotendinous disruption, edema, and late fatty infiltration. J Shoulder Elbow Surg 2008; 17(4):546-53.
7Walch G, Nove-Josserand L, Liotard JP, Noel E. Musculotendinous infraspinatus ruptures: an overview. Orthopaedics and Traumatology: Surgery and Research. 2009; 95(7):463-470.
8Rafii M, Firooznia H, Sherman O, et al. Rotator cuff lesions: signal patterns at MR imaging. Radiology 1990; 177:817-23.
9Burkhart SS, Esch JC, Jolson RS. The rotator crescent and rotator cable: an anatomic description of the shoulder’s “suspension bridge”. Arthroscopy. 1993;9:611-616
10Burkhart SS. Fluoroscopic comparison of kinematic patterns in massive rotator cuff tears: a suspension bridge model. Clin Orthop. 1992;284:144-152
11Kask K, Kolts I, Lubienski A, et al. Magnetic resonance imaging and correlative gross anatomy of the ligamentum semicirculare humeri (rotator cable). Clin Anat. 2008;21:420-426
12Sheah K, Bredella MA, Warner JJ, et al. Transverse thickening along the articular surface of the rotator cuff consistent with the rotator cable: identification with MR arthrography and relevance in rotator cuff evaluation. Am J Roentgenol. 2009;193:679-686
13Cohen SB, Towers JD, Bradley JP. Rotator cuff contusion of the shoulder in professional football players. Epidemiology and magnetic resonance imaging findings. Am J Sports Med 2007; 35:442-47