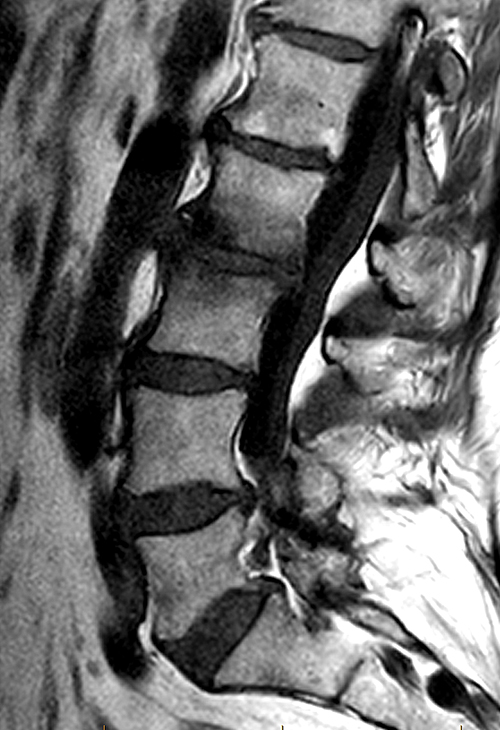
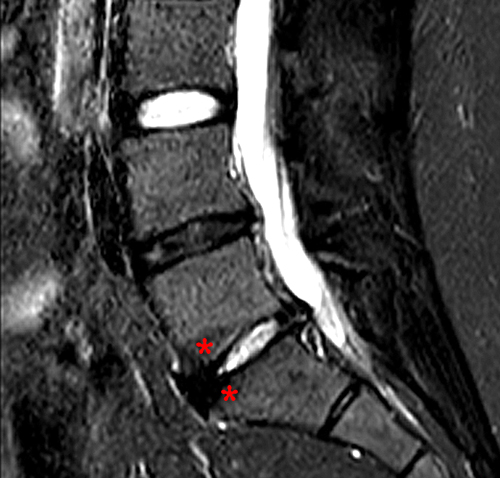
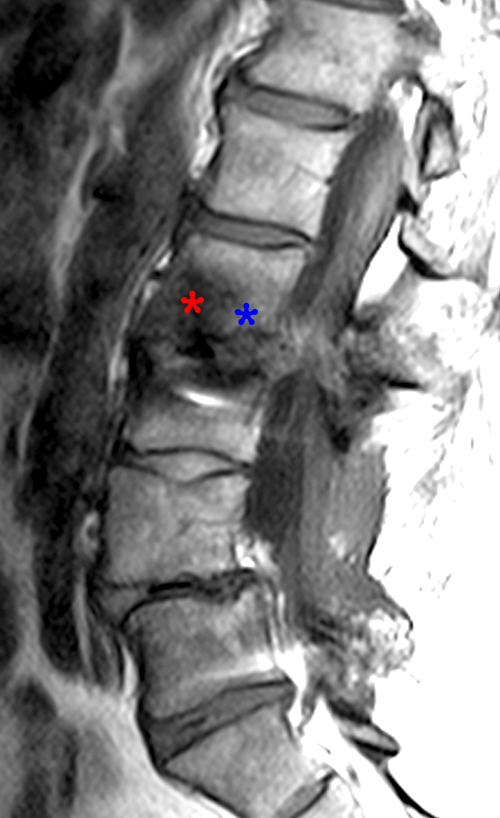
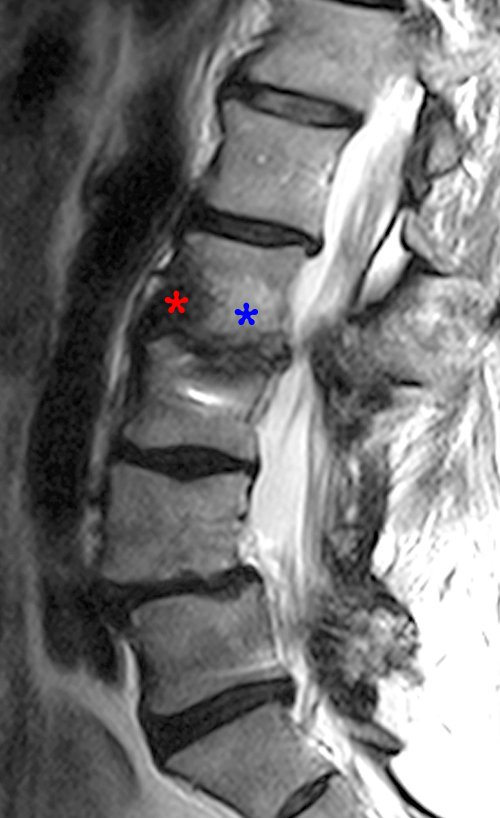
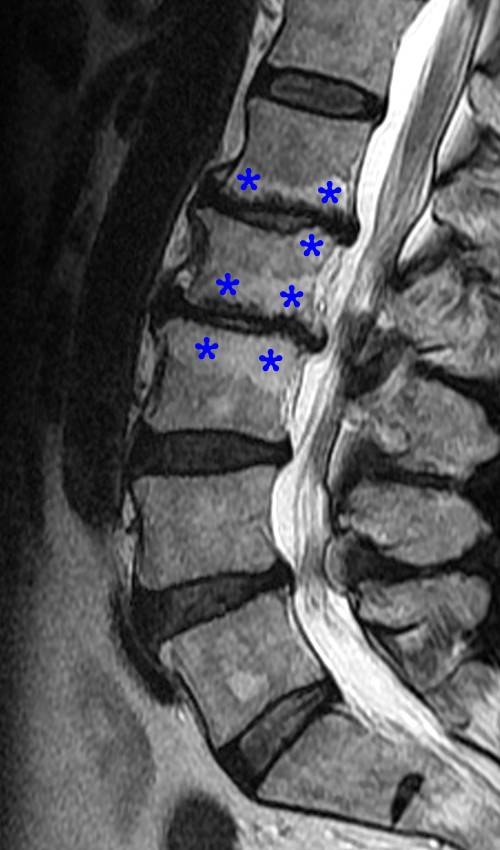
Clinical history: A 70 year-old female presents with persistent low back pain. MRI of the lumbar spine was performed. Sagittal T1-weighted (1a) and T2-weighted (1b) images of the lumbar spine are provided. What are the findings? What is the most likely diagnosis?
Findings
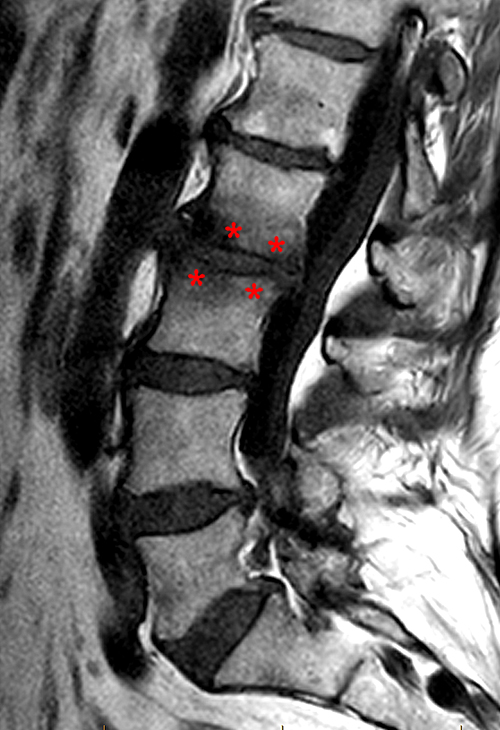
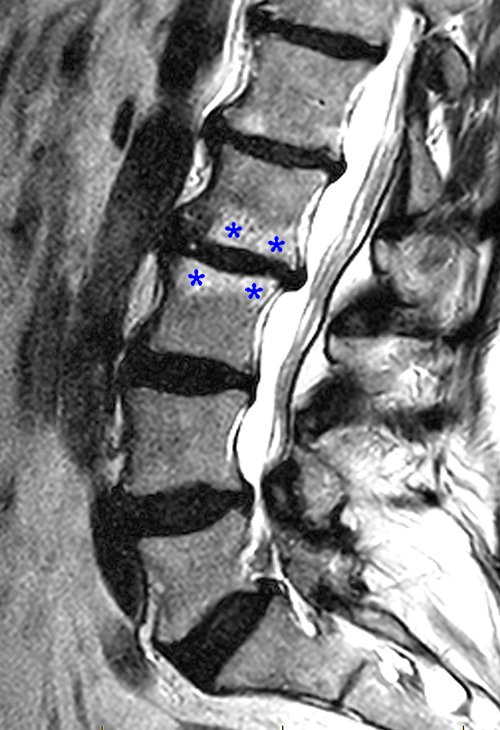
Figure 2:
The sagittal MR series reveal hypointensity (red asterisks) on T1- weighted image (2a) and hyperintensity (blue asterisks) on T2-weighted images (2b) in the endplates adjacent to the L2-3 disc, consistent with Modic type 1 changes. All lumbar discs demonstrate loss of signal on T2 weighted images, consistent with degeneration.)
Diagnosis
Modic type 1 vertebral endplate changes.
Introduction
Vertebral endplate changes were redefined with the advent of MRI, which enabled visualization of previously unrecognized alterations in marrow signal. Modic et al. proposed a formal classification of these changes in 1988.1 Two types of endplate changes were originally described, with a third type subsequently added in a later publication: 2,3
Type 1: Decreased signal intensity on T1-weighted images and increased signal intensity on T2-weighted images.
Type 2: Increased signal intensity on T1-weighted images and isointense to marrow or mildly increased signal intensity on T2-weighted images.
Type 3: Decreased signal intensity on both T1- and T2-weighted images.
On histopathologic section, type 1 changes are associated with fissuring of the endplates and infiltration of vascularized fibrous tissue. Increased osteoclasts, osteoblasts, and reactive woven bone are also found, indicating that type 1 changes are due to an inflammatory-type response. Type 2 changes occur due to conversion of red marrow to fatty marrow, and type 3 changes represent subchondral sclerosis.
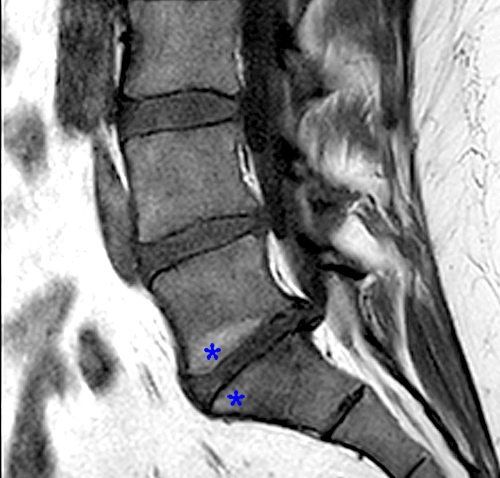
Figure 3:
29 year-old female with leg pain. Sagittal T1-(3a) and T2-(3b) weighted images of the lumbar spine demonstrate hyperintensity in the endplates (blue asterisks) adjacent to the L5-S1 level on both sequences, consistent with Modic type 2 changes. The endplate signal changes suppress (red asterisks) on the STIR sequence (3c), consistent with fatty marrow. Degenerative disc disease is noted at L5-S1, with loss of disc space height and a disc protrusion.
Type 2 endplate changes are the most commonly seen, followed by type 1. Type 3 changes are the least commonly identified. The L4-5 and L5-S1 levels are most commonly affected.
Vertebral endplate degenerative changes are significantly associated with back pain, with type 1 changes showing the strongest association.4,5 Most patients with Modic changes also have concurrent evidence of disc degeneration.6 Modic changes are rare in asymptomatic patients.7
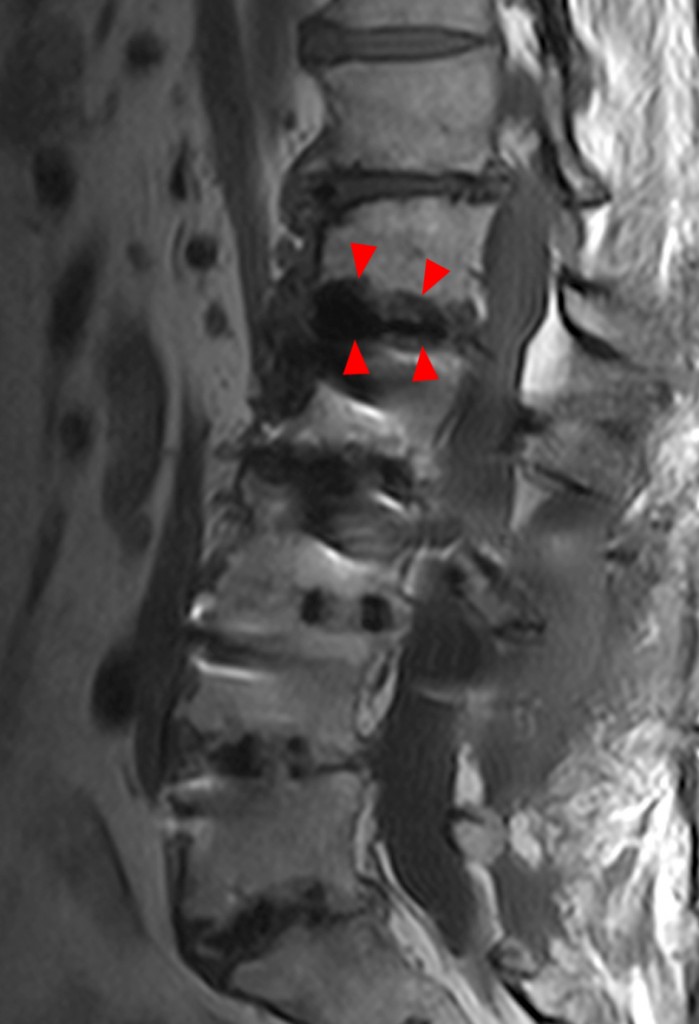
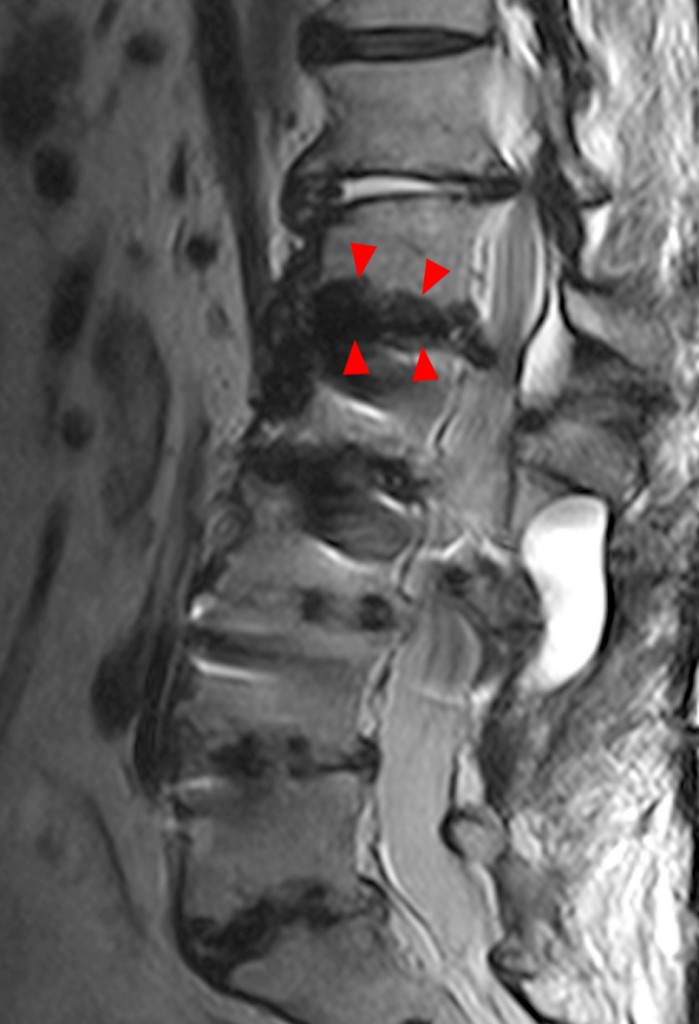
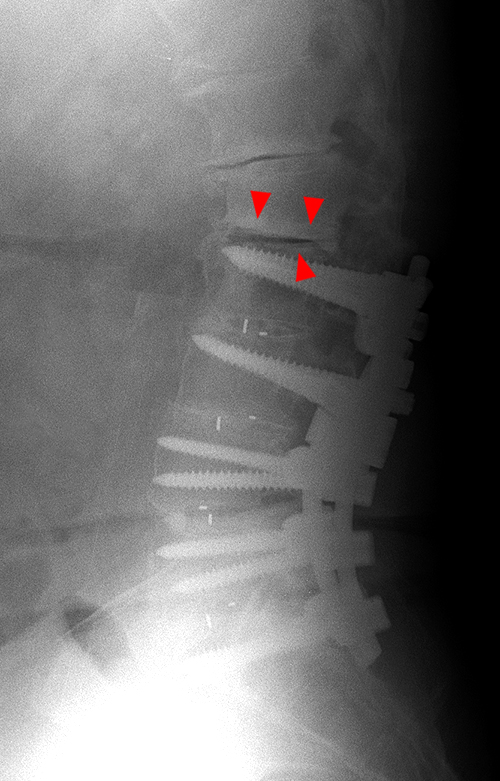
Figure 4:
62 year-old female with back pain and history of spinal fusion. Sagittal T1-(4a) and T2- (4b) weighted images of the lumbar spine demonstrate hypointensity (arrowheads) in the endplates adjacent to the L2-3 level, above the level of the fusion, consistent with Modic type 3 changes. A lateral radiograph (4c) confirms endplate sclerosis (arrowheads) at this level.
Etiology
There are several current theories about the etiology of vertebral endplate changes. In their initial paper, Modic et al. postulated that the changes were a result of primary mechanical stress on the endplates. Subsequent studies identified lumbar instability as a mechanical factor associated with type 1 changes.8 Other authors have suggested that repeated trauma to the disc causes the release of inflammatory mediators that diffuse into the endplates and cause marrow alterations; this theory is supported by Burke et al.’s finding that patients with Modic type 1 changes who underwent fusion had an increased number of proinflammatory mediators in the removed disc material.9 Others have also found increased levels of tumor necrosis factor and immunoreactive nerve fibers in the endplates.10
An interesting and more recent theory proposes indolent infection as an etiology for Modic type 1 endplate changes. Stirling et al. conducted a series of studies in which disc material removed from patients undergoing surgery for lumbar disc disease was shown to be infected with low virulence organisms. No infection was identified in disc material removed for other indications.11 Other investigators have replicated these findings, raising the question of whether the endplate changes seen on MRI are a localized inflammatory response to chronic, low grade infection. Some authors speculate that common mouth and skin organisms may gain access to the endplates during transient bacteremias via neovascularization associated with degenerative disc disease.
In further support of the theory of an infectious etiology, Ohtori et al. followed 71 patients with Modic type 1 changes for a period of 2 years and found that 4.2% developed biopsy-proven pyogenic discitis during that time frame. It is important to note that none of these patients had initial laboratory or clinical findings to indicate infection.12
Differential Diagnosis
The primary differential consideration for Modic type 1 changes is discitis, which can cause marrow edema in the endplates. Although multiple additional findings are usually associated with pyogenic discitis, severe type 1 changes can be difficult to distinguish from discitis.13 Patel et al. have proposed the use of diffusion imaging as a tool to aid in differentiation. The authors describe well-demarcated, linear restricted diffusion at the border between endplate changes and normal marrow in patients with type 1 changes. This so-called “claw sign” is highly suggestive of a degenerative etiology.14
Treatment and Progression
Conventional treatment for patients with back pain and associated type 1 degenerative endplate changes has traditionally been conservative, including anti-inflammatory medication, steroid injections, and physical therapy. However, in a 2012 study, Albert et al. reported clinical improvement in patients with back pain and Modic type 1 endplate changes who were treated with antibiotics15 Modic Antibiotic Spinal Therapy, or MAST, is now advocated by several clinics based on Albert’s findings.16 However, these findings are considered controversial by some, and additional clinical trials are ongoing.17
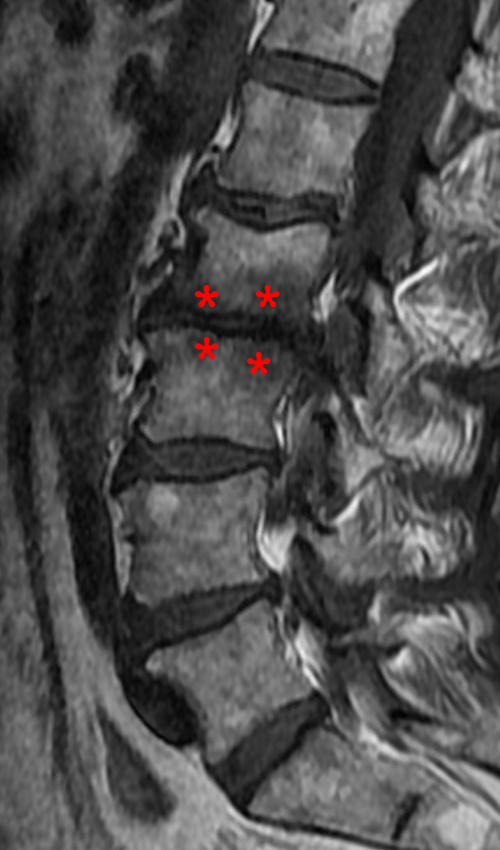
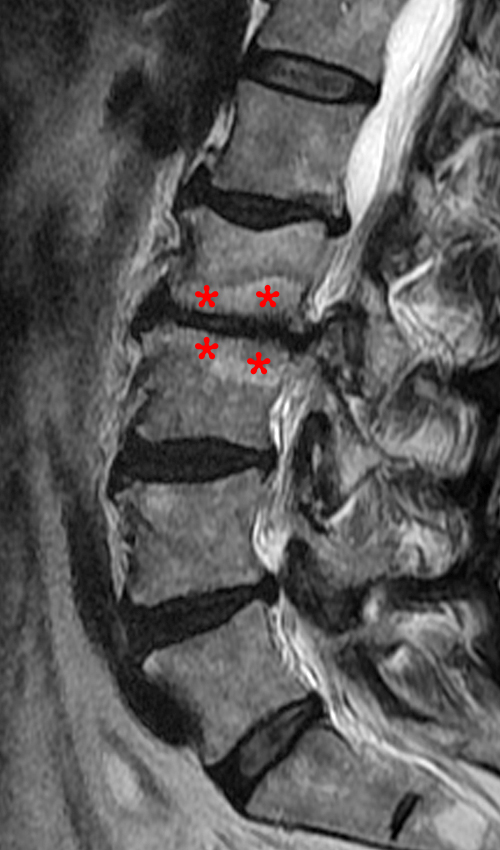
Figure 5:
Mixed Modic type changes are seen at the L2-3 level in this patient. Sagittal T1-weighted (5a) and T2-weighted (5b) images demonstrate T1 and T2 hypointensity (red asterisks) at the anterior margins of the endplates consistent with type 3 changes, and T1 hypointensity/T2 hyperintensity (blue asterisks) at the mid to posterior margins of the endplates consistent with type 1 changes. The coexistence of different types of Modic changes suggests stages of the same process.
In early studies, Modic changes were thought to progress along a spectrum from normal endplates to type 3, with type 1 being acute change and types 2 and 3 considered more chronic. However, later studies have shown that endplate changes can fluctuate between types, and some changes can regress completely. Mixed Modic endplate changes are commonly seen, and support the contention that all of the changes are manifestations of the same process at different stages. Modic changes can also regress following lumbar fusion.
Conclusion
The ability of MRI to assess marrow signal alterations has enabled more detailed evaluation of vertebral endplate changes, which can be independently associated with back pain. Although mechanical and/or inflammatory etiologies have been traditionally proposed, recent studies raise the question of an indolent infectious etiology, making accurate assessment of vertebral endplate changes by the radiologist increasingly important in determining appropriate treatment options.
Radsource is the United States’ trusted Teleradiology services provider. We would love the opportunity to show you our sub-specialized abilities for your healthcare network. Contact us today!
References
- Modic MT, Steinberg PM, Ross JS, Masaryk TJ, Carter JR. “Degenerative Disk Disease: Assessment of Changes in Vertebral Body Marrow with MR Imaging.” Radiology (1988) 166:193-99. ↩
- Rahme R, Moussa R. “The Modic Vertebral Endplate and Marrow Changes: Pathologic Significance and Relation to Low Back Pain and Segmental Instability of the Lumbar Spine.” American Journal of Neuroradiology (2008) 29: 838-42. ↩
- Modic MT, Masaryk TJ, Ross JS, and Carter JR. “Imaging of Degenerative Disk Disease.” Radiology (1988) 168: 177-86. ↩
- Brinjikji W, Diehn FE, Jarvik JG, Carr CM, Kallmes DF, Murad MH, Luetmer PH. “MRI Findings of Disc Degeneration Are More Prevalent in Adults with Low Back Pain than in Asymptomatic Controls: A Systematic Review and Meta-Analysis.” American Journal of Neuroradiology (2015) 36: 2394-399. ↩
- Jensen TS, Karppinen J, Sorensen JS, Niinimaki J, Lebouef-Yde C. “Vertebral endplate signal changes (Modic change): a systematic literature review of prevalence and association with non-specific low back pain.” European Spine Journal (2008) 17: 1407-1422. ↩
- Kuisma M, Karppinen J, Niinimäki J, Kurunlahti M, Haapea M, Vanharanta H, Tervonen O. “A Three-Year Follow-up of Lumbar Spine Endplate (Modic) Changes.” Spine 2006) 31: 1714-718. ↩
- Toyone T, Takahashi K, Kitahara H, Yamagata M, Murakami M, and Moray H. “Vertebral Bone-marrow Changes in Degenerative Lumbar Disc Disease. An MRI Study of 74 Patients with Low Back Pain.” Journal of Bone and Joint Surgery Br (1994): 757-64. ↩
- Crock, HV. “Internal Disc Disruption: A Challenge to Disc Prolapse Fifty Years on.” Spine (1986): 650-53. ↩
- Burke JG, Watson RWG, McCormack D, Dowling FE, Walsh MG, Fitzpatrick JM. “Intervertebral Discs Which Cause Low Back Pain Secrete High Levels of Proinflammatory Mediators.” The Journal of Bone and Joint Surgery (2002) 84: 196-201. ↩
- Ohtori S, Inoue G, Ito T, Koshi T, Ozawa T, Doya H, Saito T, Moriya H, Takahashi K. “Tumor Necrosis Factor-Immunoreactive Cells and PGP 9.5-Immunoreactive Nerve Fibers in Vertebral Endplates of Patients With Discogenic Low Back Pain and Modic Type 1 or Type 2 Changes on MRI.” Spine 31.9 (2006): 1026-031. ↩
- Stirling, Alistair, Tony Worthington, Mohammed Rafiq, Peter A. Lambert, and Tom Sj Elliott. “Association between Sciatica and Propionibacterium Acnes.” The Lancet 357.9273 (2001): 2024-025. ↩
- Ohtori S, Koshi T, Yamashita M, Yamauchi K, Inoue G, Munetaka Suzuki M, Takaso M, Orita S, Eguchi Y, Nobuyasu Ochiai N, Shunji Kishida S, Kazuki Kuniyoshi K, Junichi Nakamura J, Aoki Y, Ishikawa T, Arai G, Miyagi M, Kamoda H, Takahashi K. “Existence of Pyogenic Spondylitis in Modic Type 1 Change without Other Signs of Infection: 2-year Follow-up.” European Spine Journal (2010) 7: 1200-205. ↩
- Viroslav AB. “Discitis.” Radsource. N.p., 1 July 2012. Web. 17 Apr. 2016. www.radsource.us/discitis. ↩
- Patel KB, Poplawski MM, Pawha PS, Naidich TP, Tanenbaum LN. “Diffusion-Weighted MRI “Claw Sign” Improves Differentiation of Infectious from Degenerative Modic Type 1 Signal Changes of the Spine.” American Journal of Neuroradiology (2014) 35: 1647-652. ↩
- Albert HB, Sorensen J. “Antibiotic Treatment in Patients with Chronic Low Back Pain and Vertebral Bone Edema, a Double-Blind RCT of Efficacy.” European Spine Journal (2013) 22:697-707. ↩
- McCartney M. “Antibiotics for Back Pain: Hope or Hype?” BMJ (2013) 346: f3122. ↩
- Storheim K. “Antibiotics In Modic Changes (AIM).” ClinicalTrials.gov. U.S. National Institutes of Health, 18 Jan. 2016. Web. 17 Apr. 2016. ↩