Clinical History:
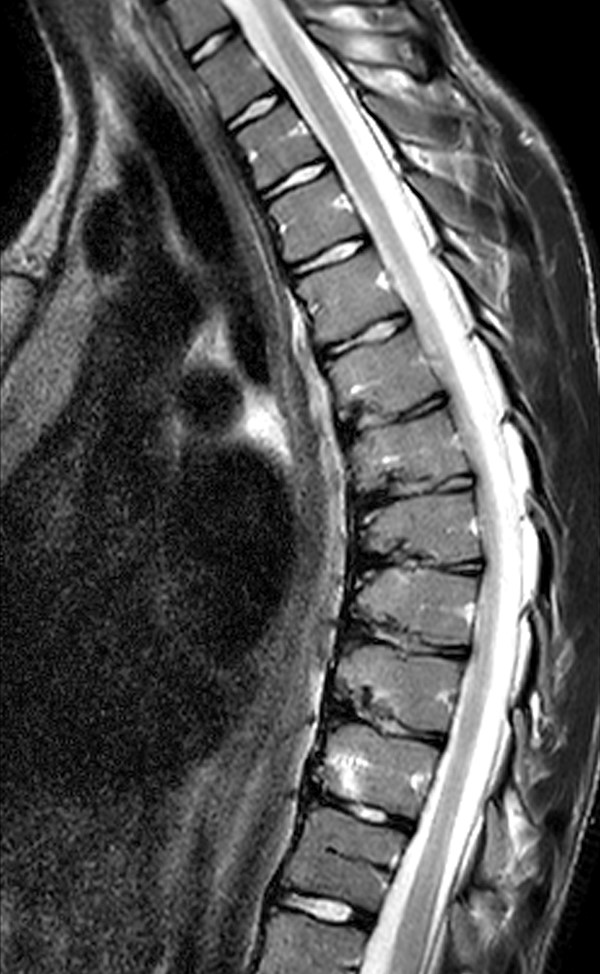
A 14 year-old male complains of back pain during exercise. A sagittal T2-weighted view of the thoracic spine is provided. What are the findings? What is the diagnosis?
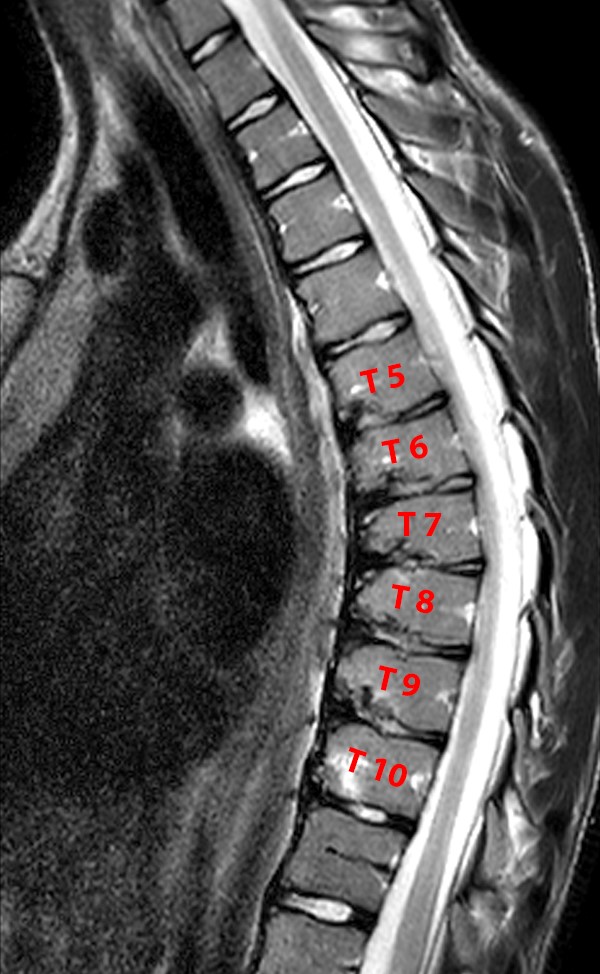
Findings
Diagnosis
Scheuermann’s disease
Introduction
Scheuermann’s disease (SD), also known as Scheuermann’s juvenile kyphosis or juvenile osteochondrosis of the spine, was first described by Holger Scheuermann in 1920. SD develops prior to the onset of puberty, typically presenting during the adolescent growth spurt as a rigid, sometimes painful thoracic kyphosis.1
Prevalence and etiology:
The prevalence of SD is reported to be between 1% and 8% with a self-reported incidence of about 3%. Although some studies report a male predominance, the literature is variable on this point.2
Several theories exist regarding the etiology of SD. Defective formation of the endplate related to abnormal collagen formation has been proposed, and there is a reported increased incidence of concurrent juvenile osteoporosis. Twin studies by Damborg et al. have demonstrated a significant genetic component, with suspected autosomal dominant transmission.3,4 Mechanical stress is generally accepted as a contributing factor, with increased incidence seen in athletes who participate in sports requiring significant flexion/extension, and in young manual laborers. Increased release of growth hormone may also be a factor; patients with SD are typically taller and heavier than their peers.
Imaging:
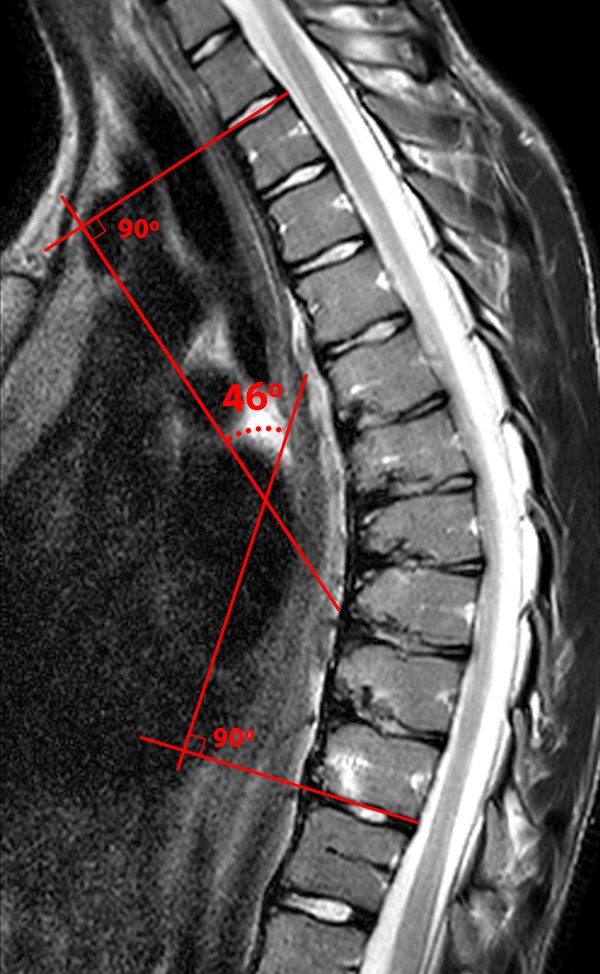
In 1964, Sorensen introduced the classic diagnostic criteria for SD of three consecutive vertebral bodies with anterior wedging of at least 5 degrees.5 Additional imaging findings include endplate irregularities, commonly manifested as Schmorl’s nodes, lengthening of the vertebral bodies, and thoracic kyphosis with a Cobb angle of at least 40-45 degrees (measured by drawing intersecting vectors parallel to the superior endplate of the vertebral body at the top of the kyphotic curve and the inferior end plate of the vertebral body at the bottom of the curve) (Figure 3).6 Of note, the Cobb angle is more accurate when measured with computer assistance. When the criteria of vertebral wedging, endplate irregularity, and kyphosis are used, there is good intraobserver agreement on the diagnosis of SD.7
“Atypical SD” has been used to describe patients who do not meet the classic criteria of three consecutive wedged vertebral bodies and kyphosis but have other features of SD (Figure 4); some advocate a definitive diagnosis of SD if endplate irregularities and at least one wedged vertebral body are present.8,9
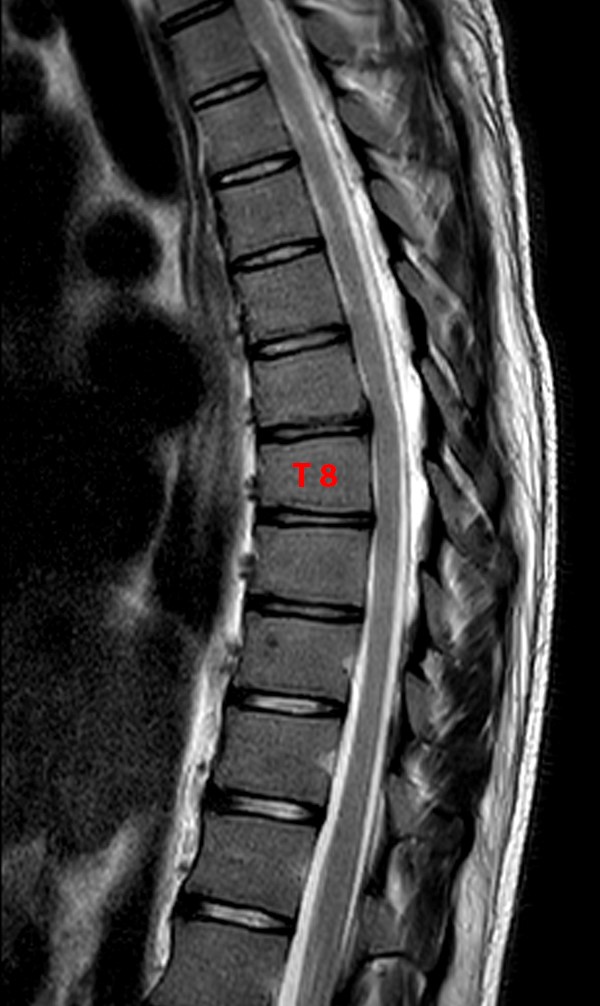
Figure 4:
A Sagittal T2-weighted image of the thoracic spine in this 21 year-old male reveals mild anterior wedging of the T8 vertebral body without significant associated kyphosis. Mild endplate irregularity is present in the mid thoracic spine. These findings do not meet the classic diagnostic criteria for Scheuermann’s disease, but could be described as “atypical Scheuermann’s disease.”
A second type of SD has been described, affecting the thoracolumbar junction or the lumbar spine, referred to as “lumbar Scheuermann’s”, “Type 2 Scheuermann’s”, or “Scheuermann-like disease”;10 although anterior wedging of vertebral bodies and endplate irregularities are seen, thoracic kyphosis may not be a prominent feature (Figure 5).11
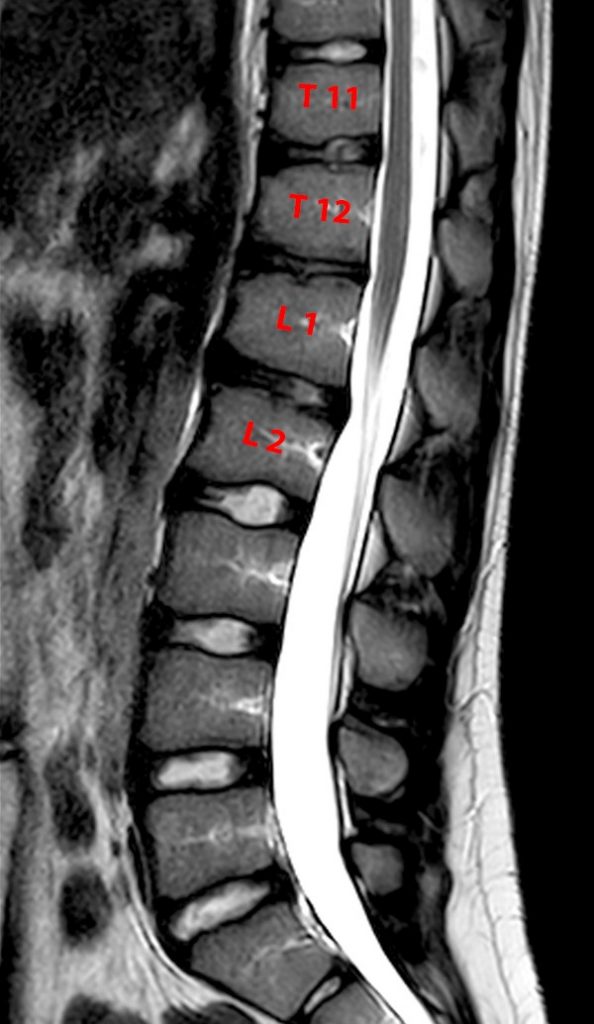
Figure 5:
A Sagittal T2-weighted image of the lower thoracic and lumbar spine in this 15 year-old female shows anterior wedging of the T11, T12, and L1 vertebral bodies, with associated endplate irregularity from T11 to L2. Mild posterior wedging of the L2 vertebral body is also noted. The findings are consistent with “Scheuermann-like disease” involving the thoracolumbar junction. Note that kyphosis is not a prominent feature.
Treatment and prognosis:
For patients with a kyphosis of less than 80%, treatment is generally conservative, utilizing physical therapy and bracing, with a high rate of success. Surgery is usually reserved for patients with a kyphosis of greater than 80%, or in cases of refractory pain or neurological symptoms. Untreated SD has a higher risk of back pain that limits daily activities, independent of the degree of kyphosis.12
There is a higher long-term incidence of back pain and disc disease in patients with “Scheuermann-like disease” affecting the thoracolumbar or lumbar spine than in patients with classic thoracic SD.
Conclusion:
Scheuermann’s disease is a notable cause of back pain and kyphosis in adolescents. Identification of features of SD and determination of the degree of kyphosis is helpful in determining operative vs. non-operative management. “Scheuermann-like disease” at the thoracolumbar junction or in the lumbar spine is an important prognostic indicator of back pain in later life.
References
- Bezalel T, Carmeli E, Been E, and Kalichman L. Scheuermann’s disease: Current diagnosis and treatment approach. J Back Musculoskel Rehabil (2014) 27:383-390. ↩
- Palazzo C, Sailhan F, Revel M. Scheuermann’s disease: an update. Joint Bone Spine (2014) 81:209-214. ↩
- Damborg F, Engell V, Andersen M, Kyvik KO, Thomsen K. Prevalence, concordance, and heritability of Scheuermann kyphosis based on a study of twins. J Bone Joint Surg Am (2006) 88(10): 2133-2136. ↩
- Damborg F, Engell V, Nielsen J, Kyvik KO, Andersen M, Thomsen K. Genetic epidemiology of Scheuermann’s disease: Heritability and prevalence over a 50-year period. Acta Orthopaedica (2011) 82(5): 602-605. ↩
- Sorensen K. Scheuermann’s juvenile kyphosis. Copenhague: Munskgaard: 1964. ↩
- Goh S, Price RI, Leedman PJ, Singer KP. A comparison of three methods for measuring thoracic kyphosis: implications for clinical studies. Rheumatology (2000) 39(3): 310-315. ↩
- Ater A et al. Scheuermann Disease: Evaluation of Radiological Criteria and Population Prevalence. Spine (2013) 38 (19) 1690-1694. ↩
- Bradford DS. Vertebral osteochondrosis (Scheuermann’s kyphosis). Curr Opin Pediatr (1999) 11:70-75. ↩
- Liu N et al. Radiological signs of Scheuermann Disease and Low Back Pain: Retrospective Categorization of 188 Hospital Staff Members With 6-Year Follow-up. Spine (2014) 39(20): 1666-1675. ↩
- Guo X, Chen Z, Liu N, Guo Z, Qi Q, Li W, Zeng Y, Sun C. Comparison between two types of “Scheuermann-disease like people”: thoracolumbar disc herniation patients and healthy volunteers with radiological signs of Scheuermann’s disease. Chin Med J (Engl) (2014) 172(22): 3862-3866. ↩
- Gocke E, Beyhan M. Radiological imaging findings of Scheuermann disease. World J Radiol (2016) 8(11): 895-901. ↩
- Ristolainen L, Kettunen JA, Heliovaara M, Kujala UM, Heinonen A, Schlenzka D. Untreated Scheuermann’s disease: a 37-year follow up study. Eur Spine J (2012) 21:819-824. ↩