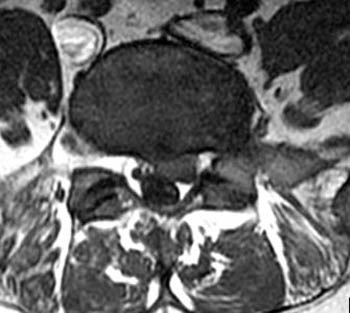
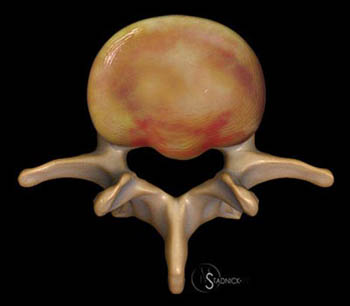
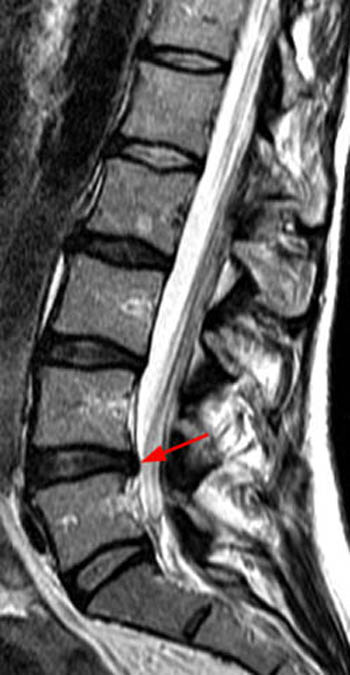
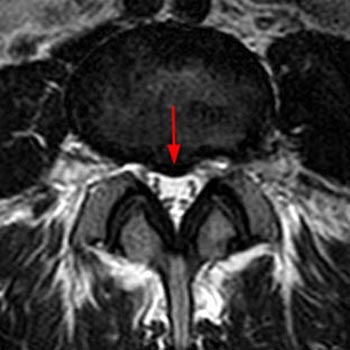
Clinical History: A 32-year old female presents with back and left leg pain. (1a) T2-weighted sagittal and (2a) T1-weighted axial images are provided.
The best diagnosis in this case is:
- Herniated nucleus pulposus
- Disc protrusion
- Disc extrusion
- Disc sequestration
Findings
Answer
This is indeed a disc herniation (preferred term to herniated nucleus pulposus), but the best answer is 3, a disc extrusion. Utilizing the recommendations of the combined task force of the North American Spine Society, the American Society of Spine Radiology, and the American Society of Neuroradiology, a disc extrusion refers to a herniated disc that has an apex that is larger than its base in any plane.
Introduction
Significant historical variations in terminology are found in the reporting of intervertebral disc abnormalities. Juan Taveras, M.D, one of the founding members of the American Society of Neuroradiology, preferred to call a herniated disc just that, a herniated disc.1 Though this may seem like a simplification of a complex process, there is merit in this approach.
The basis of variations in spine terminology is in part secondary to the varying perspectives of physicians who manage patients with disc herniations. Surgeons, radiologists and pain management specialists may look at the same patient differently. The seeds of the present situation were sewn in the days of cross sectional imaging, using computed axial tomography, or CT.2 The situation intensified in the late 1980s with magnetic resonance imaging (MRI), when visualization of the soft tissue differences of the nucleus pulposus, anulus fibrosus and surrounding structures became achievable. The ability to directly visualize disc material extending through tears in the anulus fibrosus was an exciting improvement over being merely able to see an impression on the spinal canal with myelography or CT myelography. With MRI, we are now able to describe a disc herniation in such detail that merely saying a disc is herniated or not is no longer sufficient.
History of Spine Lexicon
MRI’s ability to directly visualize a wide variety of pathologic states of the intervertebral disc led to a veritable Tower of Babel phenomenon in terms of disc nomenclature. Haughton3, Modic, Ross4 and countless others authored excellent papers and textbooks on the radiologic and pathologic description of disc herniations. The North American Spine Society (NASS) is a multidisciplinary task force that formulated terminology recommendations regarding disc herniations in 1995. The recommendations were published in 1997 by the NASS and the American Academy of orthopaedic Surgeons.5 Their approach, however, was not universally accepted or recognized, and thus in 2001 a Joint Task Force of the NASS, the American Society of Neuroradiology (ASNR) and the American Society of Spine Radiology (ASSR) convened and developed a spine lexicon.6 This was strengthened in 2003 with an update including endorsing societies from virtually every professional organization with an interest in managing patients with disc herniations.7 The current article is in large part derived from the guidelines of this joint task force.
Definitions
Normal: Residents in radiology are taught what normal looks like since one must be able to know what normal is to appreciate that which is not. A normal disc (4a,4b) is “fully and normally developed, free of disease, trauma or aging”. This part of the definition does not take into account that clinically normal people may have abnormal discs and that aging is a normal process.
Figure 4:
The normal intervertebral disc has maintained height and demonstrates diffuse hyperintensity of the disc space on T2-weighted (4a) sagittal and (4b) axial images. A central horizontal band of lower signal (arrows) due to fibrous tissue is a sign of normal maturation. On the axial view, the normal disc has a mildly concave posterior margin (arrowheads).
Degeneration: This broad term includes a multitude of abnormalities including desiccation, annular tears, bulges, mucinous degeneration, endplate defects or sclerosis, and osteophytes. These changes can be further subdivided into spondylosis deformans, possibly a consequence of normal aging, and intervertebral osteochondrosis, presumably due to a more pathologic state.7 The latter is typically characterized by disc space narrowing, vacuum discs, and endplate reactive changes.8 From a practical standpoint, disc degeneration is often used descriptively in MR interpretation to refer to loss of the usual T2-hyperintensity within the discs, and this appearance may be a normal consequence of aging (5a).
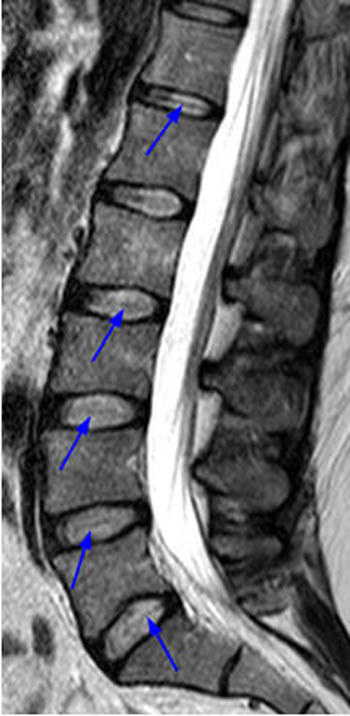
Figure 5:
(5a)A T2-weighted sagittal image reveals diffuse disc degeneration, characterized by low signal intensity on T2-weighted images throughout the discs. This terminology is preferred to "disc desiccation", as studies have shown that the change in T2 signal characteristics involve more than just differences in water content. At L4-5, additional features of intervertebral osteochondrosis are present, with disc space narrowing and reactive endplate signal changes (arrows) being apparent.
Disc Bulge: A disc is bulging if it extends in a circumferential fashion beyond the edges of the vertebral apophyses (6a). Though bulges may have a rightward, leftward, or lateral predominance, they must involve greater than 50% of the circumference of the disc. The mildest disc bulges simply result in the loss of the slightly concave appearance to the posterior disc margin on axial images, and this appearance may be considered a normal variant at L5-S1. Although bulges are most commonly a result of disc degeneration, they may also occur as a response to vertebral remodeling due to factors such as osteoporosis or trauma.
Anular Tears/Fissures: An anular tear involves loss of integrity of the anulus with a radial, transverse, or concentric pattern. Some prefer the term anular fissure since tear may imply trauma. Common practice by literature review shows preference for tear and as a result this is the accepted terminology. Anular tears appear as a hyperintense zone on T2-weighted imaging (7a,7b). Though debatable, some tears are felt to have clinical importance, especially if they involve the outer third of the anulus fibrosus.
Disc Herniation: A herniated disc is defined as “Localized displacement of nucleus, cartilage, fragmented apophyseal bone or fragmented annular tissue beyond the intervertebral disc space.”7 This definition explains why the older term of “herniated nucleus pulposus” is not preferred, as herniations may involve more than simply the nucleus pulposus. The boundaries of the disc are defined by the vertebral endplates superiorly and inferiorly and peripherally by the apophyses, not including any osteophytes that may be present. Localized is defined by 50% or less of the circumference of the disc being involved. Disc herniations may be termed “broad-based” if 25-50% of the circumference of the disc is involved. If greater than 50% of the disc circumference is involved, a bulge rather than a herniation is present.
Subclassification of Disc Herniations
Protrusion: A disc protrusion (I,J,K) is defined as “A herniated disc in which the greatest distance, in any plane, between the edges of the disc material beyond the disc space is less than the distance between the edges of the base in the same plane.”7 Protrusions are the most common form of herniation, and morphologically are the most “mild” appearing. A test for a disc protrusion is that if you measure the herniated disc from edge to edge in any plane, that measurement cannot be larger than the measurement of the base of the lesion in that same plane. Because the height of the base of a herniation in the sagittal plane is at most the height of the disc itself, any herniation that extends above or below the level of the disc will measure larger than its base in cephalocaudal dimension, and thus cannot be a protrusion.
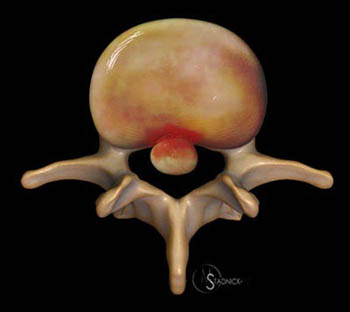
Extrusion: “A herniated disc in which, in at least one plane, any one distance between the edges of the disc material beyond the disc space is greater than the distance between the edges of the base in the same plane, or when no continuity exists between the disc material beyond the disc space and that within the disc space.”7 Extrusions (10a) can be thought of as akin to the appearance of toothpaste squeezed from the tube. Though not a requirement for extrusion, any herniation that extends above or below the level of the disc is an extrusion (11a,12a). At times, a disc herniation may have features of protrusion in one imaging plane and extrusion in another. In such cases, the herniation is an extrusion. Disc extrusions that have become displaced from the site of origin can be described as migrated, and if all continuity to the site of origin has been lost, the abnormality can be further characterized as a sequestration, or free fragment. It should be noted that such free fragments are frequently hyperintense on T2-weighted images, becoming relatively isointense to epidural fat on T2-weighted views, and therefore can be missed if care is not taken to correlate with T1-weighted images.
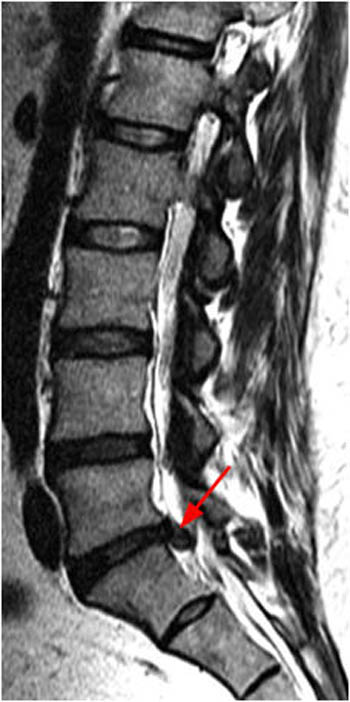
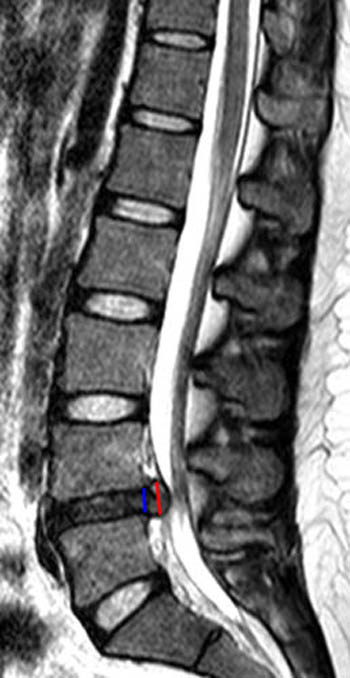
Figure 12:
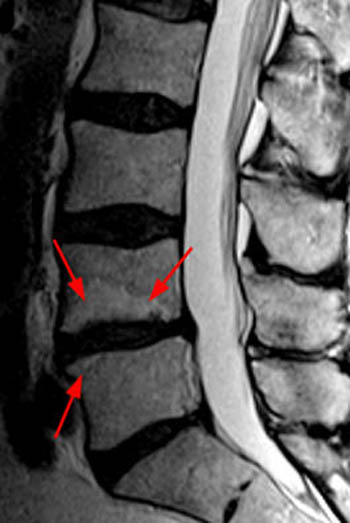
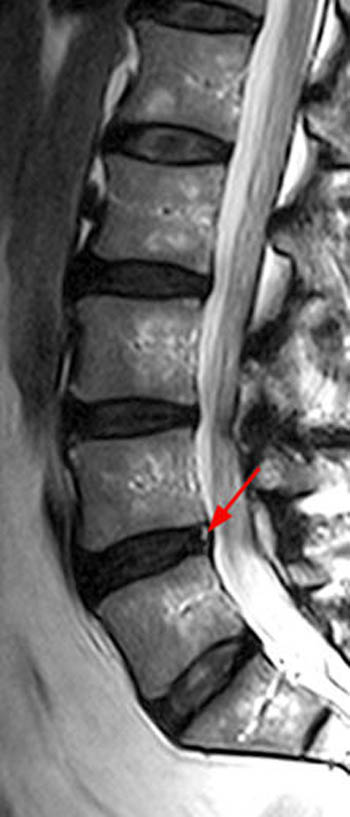
The (12a) T2-weighted sagittal image, however, reveals extension of disc material above and slightly below the level of the disc. Any such superior or inferior migration results in a herniation (red line) larger than its base (blue line) in the sagittal plane, and thus by definition, this abnormality is a disc extrusion.
Further Characterization of Disc Pathology
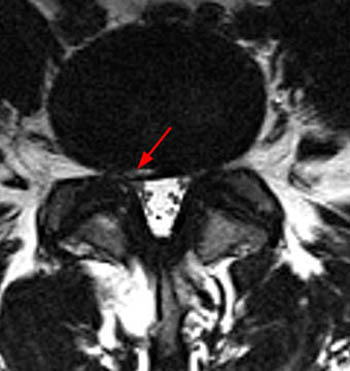
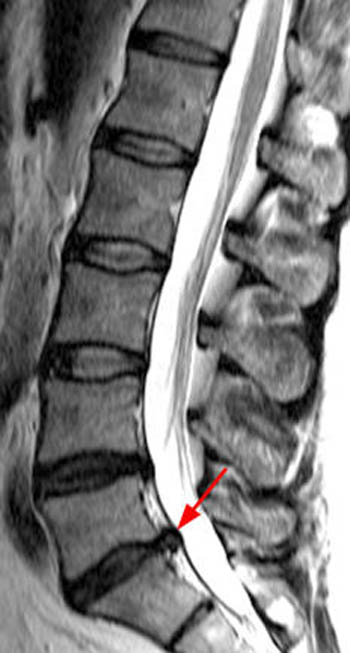
When describing any disc herniation, the experienced interpreter of MR should reflexively characterize the abnormality with regard to its effect upon adjacent exiting or traversing nerve roots (13a,14a). If the nerve root is contacted or displaced, that should be reported, allowing the clinician to correlate for radicular signs. Such correlation is critical when one considers the fact that many herniations seen on MRI have been found to be asymptomatic.
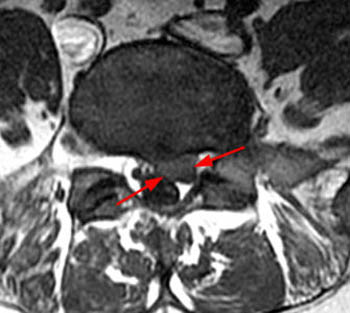
Figure 14:
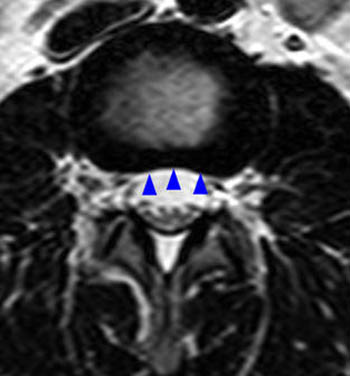
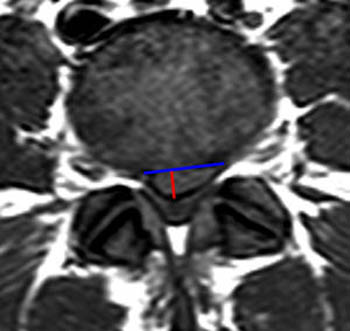
The corresponding (14a) T1-weighted axial image demonstrates protrusion morphology that can also be described as broad-based, as the protrusion (dotted red) involves between 25-50% of the circumference of the disc. The traversing right S1 nerve root (red arrowhead) is posteriorly displaced, and there is contact of the left S1 nerve root (blue arrowhead).
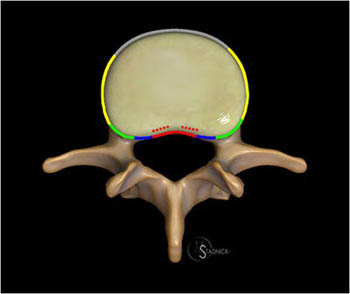
The Wiltse zones for localization of disc herniations are depicted (15a): central (red), subarticular (blue), foraminal (green), extraforaminal (yellow), and anterior (grey). The central zone is large and a common site of herniations, and thus some prefer to describe those herniations off midline within the zone as either paracentral or right/left central (dotted red). Posterolateral and far lateral are generally accepted alternatives for subarticular and extraforaminal, respectively.
Central stenosis may result from a disc herniation, though it is of course more commonly seen secondary to diffuse disc bulges and concomitant facet/ligamentous hypertrophy. When describing central stenosis, a simple, reliable approach to estimating the severity of stenosis leads to greater consistency and usefulness of MR reports. AP dimensions do not adequately account for the overall effects of stenosis factors, and cross sectional area measurements are poorly reproducible and effected by imaging technique. We favor a visual estimation of the degree of canal compromise relative to a normal level. Central stenosis is described as mild if significant volume loss has occurred but less than 1/3 of the volume of the canal is lost. Stenosis is moderate if between 1/3-2/3 of the original volume has been lost and severe if over 2/3 of original volume is occupied.
Conclusion
Although keen observational skills are critical for accurate spinal MRI interpretation, that ability is dramatically offset if observations are not accurately described and characterized. In part because of its long history as one of the original applications for MRI, spine imaging is an area particularly prone to variations in terminology and approach. A reliable and consistent approach to MR evaluation allows the effective communication of findings, leading to more effective outcomes in the treatment of the numerous pathologies that affect the spine.
References
1 Taveras JM. Herniated intervertebral disk: a plea for a more uniform terminology. AJNR Am J Neuroradiol 1989; 10:1283-1284.
2 Newton TH, Potts DG. Computed tomography of the spine and spinal cord. San Anselmo CA: Clavadel Press, 1983.
3 Haughton BM, Williams AL. Computed Tomography of the Spine. St. Louis: CV Mosby, 1982.
4 Modic M, Masaryk T, Ross J,. Magnetic resonance imaging of the spine. Chicago: Year Book Medical Publishers, 1989.
5 Fardon DF, Herzog RJ, Mink JF et al. Nomenclature of Lumbar disc Disorders, In: Garfin SR, Vaccaro AR, eds. Orthopaedic Knowledge Update-Spine, Rosemont IL: American Academy of Orthopaedic Surgeons, 1997, A3-A14.
6 Fardon DF, Milette PC. Nomenclature and classification of lumbar disc pathology: recommendations of the combined task forces of the North American Spine Society, American Society of Spine Radiology and American Society of Neuroradiology. Spine 2001; 26:E93-113.
7 Fardon DF, Milette PC. Nomenclature and Classification of Lumbar Disc Pathology. 2003 Update. Website, American Journal of Neuroradiology.
8 Resnick D, Niwayama G. Degenerative diseases of the spine. In: Resnick D, ed. Bone and Joint Imaging. Philadelphia: W.B Saunders, 1989; 413-439.