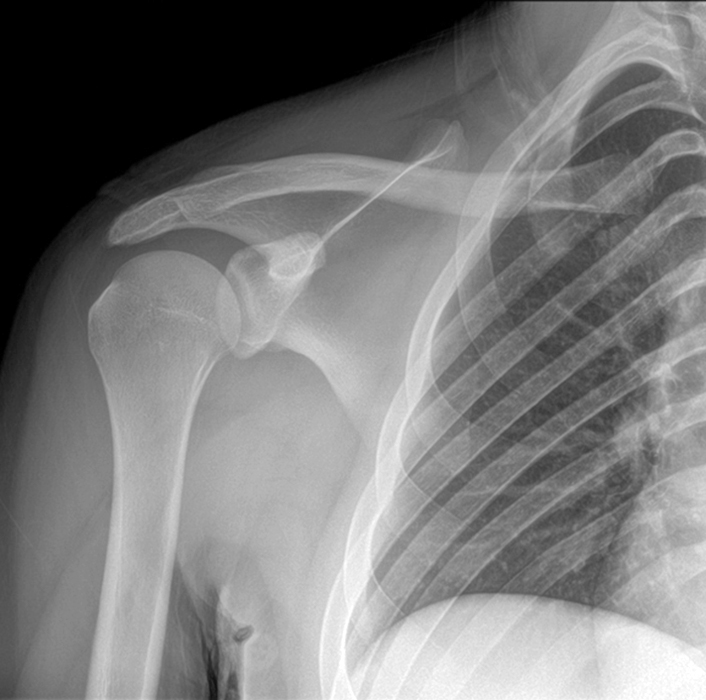
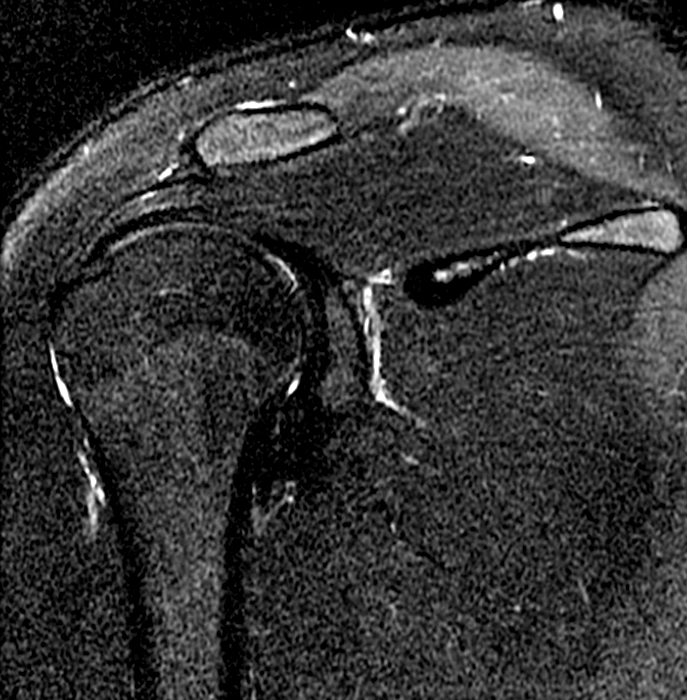
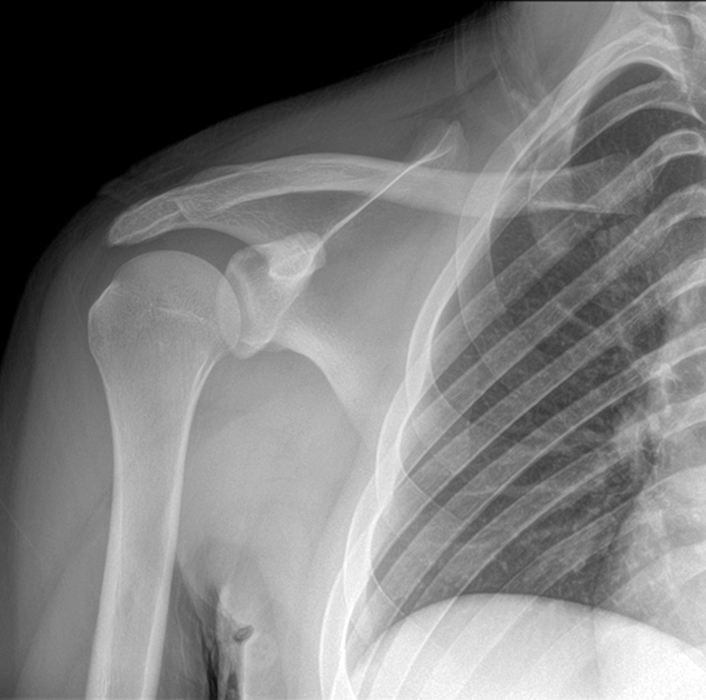
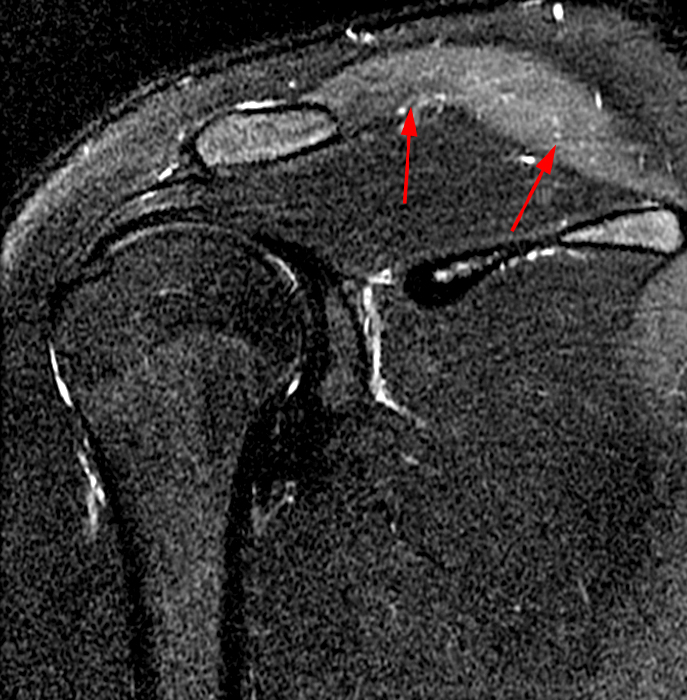
Clinical History: An 18-year-old was involved in a motor vehicle accident 8 weeks prior. He reports pain and weakness with deformity of the scapula. MRI was performed to assess for muscle tear or other injury. Initial radiograph frontal radiograph (1a) performed 4 weeks prior to the MRI. Coronal T2 fat-suppressed image provided (1b). What clinically is the patient presenting with? What is your diagnosis?
Findings
Diagnosis
Isolated trapezius muscular denervation from injury to the spinal accessory nerve (cranial nerve XI), clinically presenting with scapular winging.
Introduction
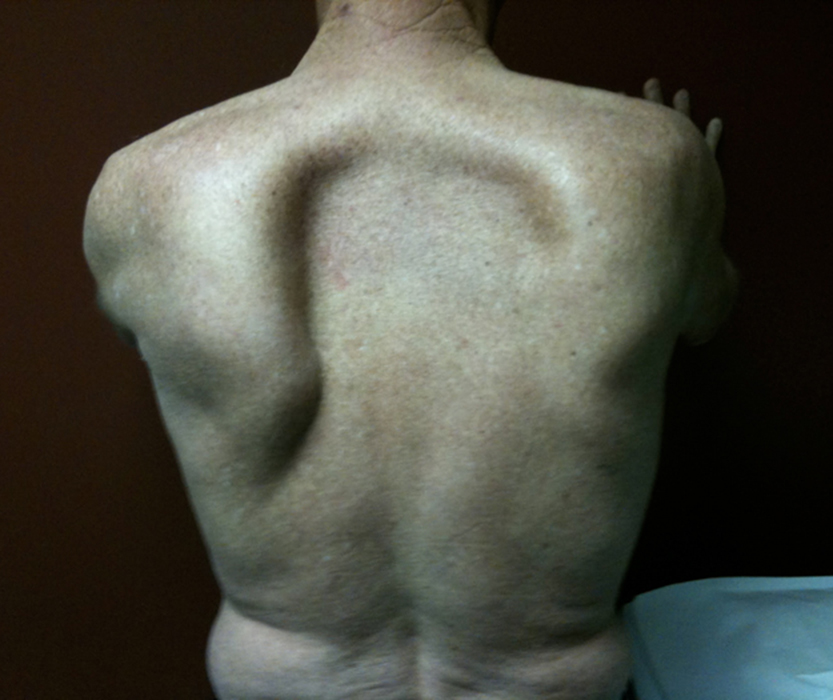
Scapular winging is a finding seen with clinical examination of the shoulder. The shoulder blade effectively “sticks out”, rather than lying flat along the back. This outward and upward motion (Figure 3) causes the scapula to resemble a bird’s wing. Trauma is usually the inciting cause although a variety of etiologies can cause injury to the associated nerves, including viral illness, allergic reactions, toxin exposure, surgical complications, medications, and pre-existing or developmental medical conditions. The nerve injury results in subsequent weakness and paralysis.
Anatomy and Function
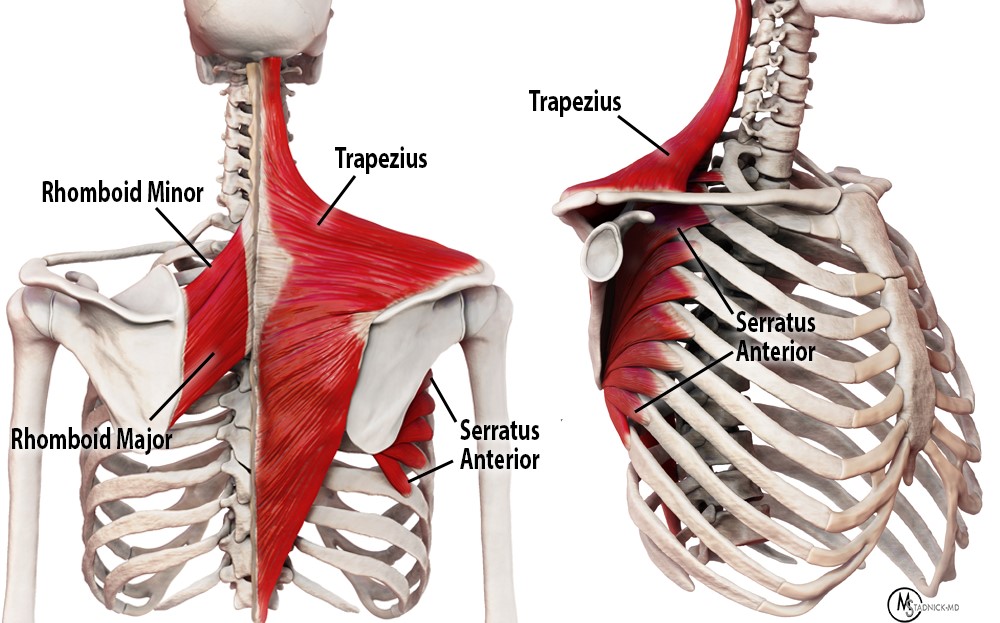
The scapula is the largest bone in the shoulder region and contains 17 muscular attachments. It is triangular shaped and is responsible for 6 movements including shoulder elevation, depression, upward rotation, downward rotation, retraction/adduction, and protraction/abduction.1 The condition of scapular winging, or scapular protraction, occurs because of injury to one of the three medial stabilizing muscles that include the serratus anterior, trapezius and rhomboids. The function of these three muscles is to keep the scapula stabilized medially against the posterior chest wall, with injury to these muscles causing the scapula to lift from the chest wall. Based upon which muscle is involved, the scapula can then deviate either medially or laterally due to the unopposed contraction of the remaining functioning other muscles. Medial winging occurs from injury to the serratus anterior and lateral occurs from trapezius or rhomboid paralysis.2
Serratus Anterior
The muscle originates from the first nine ribs and swings across the back to insert at varying levels from superior to inferior along the scapular margin. The muscle is solely innervated by the long thoracic nerve which originates from the anterior rami of the C5-C7 nerves. This nerve passes posterior to the brachial plexus, over the first rib and descends inferiorly into the muscle fibers. An intact long thoracic nerve allows proper function of this muscle to protract and rotate the scapula, helping to maintain alignment of the glenoid and stabilize when the arm is lifted overhead.
Trapezius
This muscle originates partially from the skull with the remainder from the nuchal ligament and the spinous processes of the T1-T12 vertebra. The muscle fibers extend laterally to mostly insert on the scapular spine. A component also inserts onto the lateral third of the clavicle and onto the acromion. This muscle is solely innervated by cranial nerve XI, the spinal accessory nerve. The nucleus of the nerve is long, and the “accessory” component arises in the cervical cord from the C1-C5 levels. After exiting the cord, the nerve roots ascend into the cranial vault through the foramen magnum, exit the jugular foramen, and descend along the jugular vein near cranial nerve X (vagus nerve). It descends to supply both the sternocleidomastoid and the trapezius. The main function of the trapezius is also to elevate, retract and rotate the scapula.3
Rhomboids
This muscle group consists of the rhomboid minor and rhomboid major. The smaller minor muscle arises from the C7 and T1 spinous processes and descends inferiorly and laterally to the scapular spine while the larger more inferior muscle arises from the T2-T5 spinous processes and descends similarly, inserting on the medial scapular spine. These muscles are innervated by the dorsal scapular nerve. This nerve arises from mostly the C5 nerve root, extends through the strap muscles, courses within or around the levator scapulae while supplying that muscle, and then extends inferior to the brachial plexus innervating the anterior surface of the muscle bellies. This muscle, like the trapezius, also mainly functions to retract and rotate the scapula.
Clinical Presentation and Symptoms
Scapular winging is usually a painful and incapacitating condition.4 The loss of scapular apposition against the posterior chest wall can produce varying levels of pain and tenderness. A key to the diagnosis is often a history of acute neurogenic pain in the shoulder or arm lasting for days to weeks. The actual scapular winging is usually gradual occurring over 10 days to 2 weeks after the onset of the initial injury. This pain is commonly aggravated by movements of the shoulder but not typically by movement in the neck or Valsalva maneuvers.5 The weakness that ensues can make activities of daily living difficult such as carrying heavy objects, sitting on a chair, lifting the arm overhead, and brushing teeth. Psychologically the deformity can be cosmetically displeasing. A thorough clinical history should be taken to avoid other potential causes for simulation of a scapular winging problem. The clinician should determine handedness, as the more dominant side can produce a lower scapular position on visualization than the non-dominant side. Other medical conditions can visually mimic the wing, including atrophy of rotator cuff musculature although this is usually without the pain involved in a true winging. Other areas, such as the cervical spine can produce a “pseudowinging” from positional issues thereby masking the pain.6 To exclude such a process a Spurling Test is performed, which is highly specific for cervical radiculopathy, by bending the neck sideways while rotating to the affected side eliciting radiating pain. A push wall test is also performed by placing the patient in full forward flexion position, with the wing noticeably present when viewing from posteriorly or from the side. A movement of the affected inferior scapula medially, called medial scapular winging, is a result of serratus anterior pathology (Fig 4). Often the inciting injury occurs at the preganglionic nerves and the preclavicular brachial plexus should be assessed. Several case reports of serratus anterior aplasia7 have also been ascribed to medial scapular winging. Lateral scapular winging is typically a result of trapezius muscle weakness. Commonly, lateral scapular winging results from surgery in the neck, most notably in the region of the posterior cervical triangle.
Another test, called the “scapular compression test”, occurs with the physician actively applying anterior-posterior force on the posterior scapula with one hand while stabilizing the anterior chest wall with the other hand and having the patient perform forward flexion. This allows greater motion of the affected side during flexion. A clinical condition, called Snapping Scapula syndrome, occurs when a loud pop or crack, known as crepitus, is heard with movement of the arm raised overhead. This sound is elicited by movement of the scapula over the chest wall. This may occur in conditions such as our case above with accessory nerve denervation, but other conditions are more common. Osseous considerations such as a morphologically abnormal superomedial scapular angle, atypical hooked bony protuberance from the upper medial scapular border (Luschka tubercle), and ununited clavicular fractures are more common. Scapulothoracic bursitis often, resulting from rib fractures, can produce this phenomenon, as can neoplastic etiologies such as osteochondromas and elastofibromas. EMG is the only definitive test for determining paralysis of the affected muscles and helps to determine the degree of denervation. Radiologic imaging is usually not needed but can help in cases of equivocal EMG results or to elucidate potential other causes for the symptomatology, such as an impinging disc on a nerve root or soft tissue masses.Diagnostic Imaging Patterns
Plain films play a limited role in diagnosis of scapular winging. These exams, as shown in the case example, are usually normal. Rarely there can be visualization of skeletal deformities such as osteochondromas or rib abnormalities. Occasionally a secondary condition can be seen at the edge of the field of view, such as calcific tendinitis. MRI is the imaging modality of choice. The high resolution for soft tissues often allows great visualization of the posterior musculature, particularly when the clinical diagnosis is equivocal. MRI allows the aging and severity of the peripheral neuropathy, as characteristic patterns of signal changes can be correlated to the clinical findings. It also allows visualization of other conditions that could mimic a peripheral nerve injury. MRI patterns of injury are shown below.
Serratus Anterior
The serratus anterior is critical for allowing the shoulder to tilt and move forward, increasing upward reach. This movement is exaggerated with activities such as punching a bag or swimming crawl and butterfly strokes. Conditions affecting the nerve and producing winging include blunt trauma caused by pressure from crutches, sharp trauma from causes such as shoulder surgery, and most commonly repetitive action trauma from sports activities. Other non-traumatic causes include infection such as influenza, tumor, toxin, autoimmune and inflammatory condition of nerves such as Parsonage-Turner syndrome. A long thoracic nerve injury elicits changes in the muscle and this nerve is particularly susceptible given its superficial course along the side of the chest wall. Typical compression sites on the nerve include at the level of the scalenus muscle and more distally at the level of the second rib. Injury to the serratus is typically caused by an entrapment syndrome, whereby the long thoracic nerve is stretched in an incompressible space.8 Early findings show muscle edema best appreciated on T2 fat-suppression or STIR (Fig 5). Enhancement may also be seen in the muscle on post-contrast imaging (Fig 6). Longer duration of compression can eventually produce muscle atrophy (Fig 7).
Trapezius
The trapezius, with the largest area origin of any muscle in the human body9, begins from the medial third of the superior nuchal line, the nuchal ligament, the spinous processes of C7-12 vertebrae including the adjacent supraspinous ligaments, and the external occipital protuberance. The muscle sits superficial to multiple muscles including the splenius, levator scapulae, rhomboids, and the latissimus dorsi, and extends from the cervical to the thoracic region, inserting onto the lateral third of the clavicle, acromion, and spine of the scapula. Damage to the spinal accessory nerve usually occurs because of surgery and this is most common in lymph node biopsies in the neck. The resulting weakened muscle causes limitations in overhead activities. Symptoms of pain, weakness and stiffness are common. Aside from the lateral scapular winging, these patients have shoulder drooping. The patient has difficulty abducting the arm. Injury to the accessory nerve can be difficult to discern from other conditions including paralysis of the serratus anterior and rhomboids, disc herniations, scoliosis, progressive neuromuscular disease, scapular osteochodroma, fracture malunion, stroke, herpes zoster infection, and glenohumeral instability.10 On MRI, trapezius T2 hyperintensity can clue into this diagnosis (fig. 8, 8A).
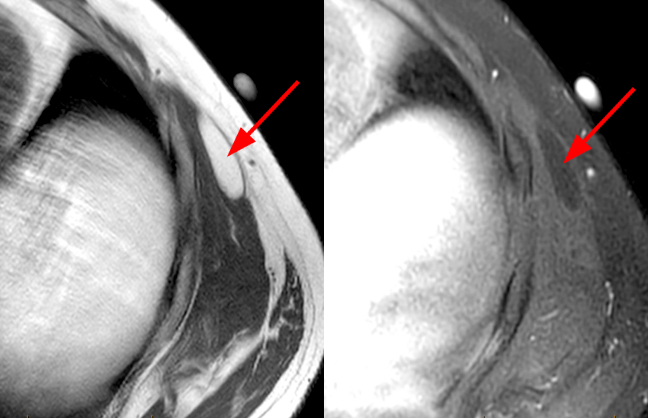
Figure 8:
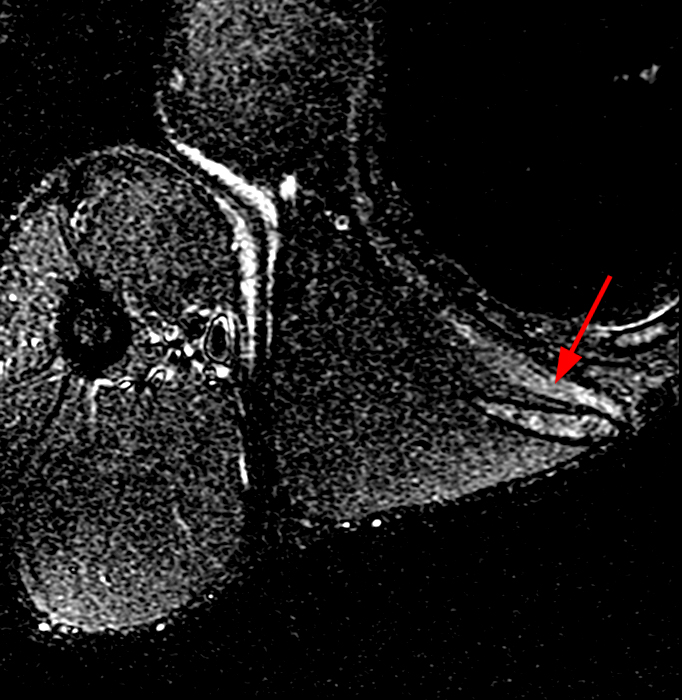
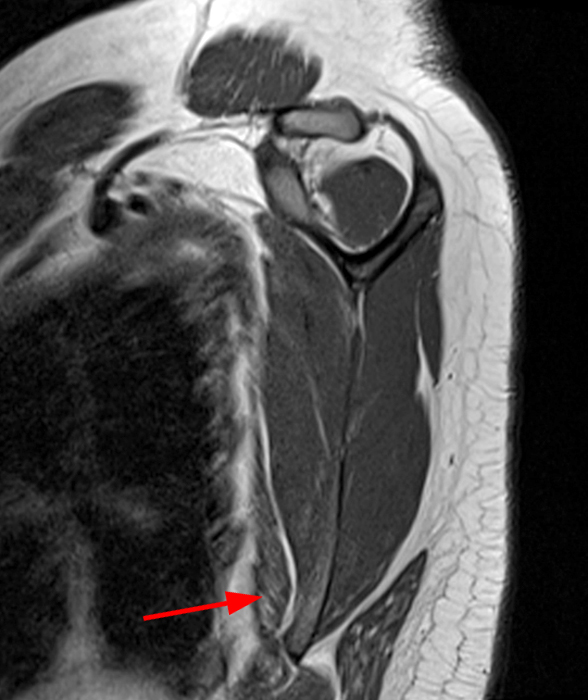
8a: Sagittal oblique STIR image parallel to the scapular axis and medial to the scapula shows hyperintensity throughout the trapezius muscle (arrows) with maintained muscle bulk suggesting acute denervation. The muscle lies immediately superficial to the rhomboid muscle.
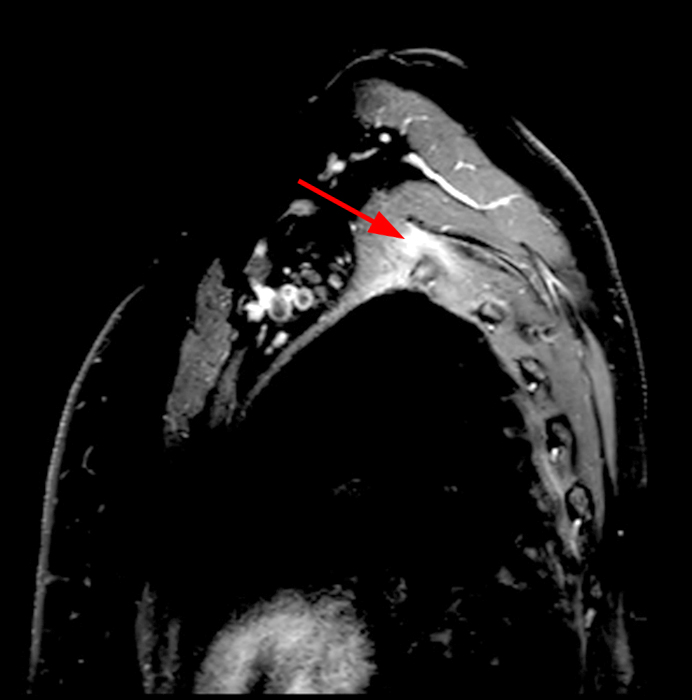
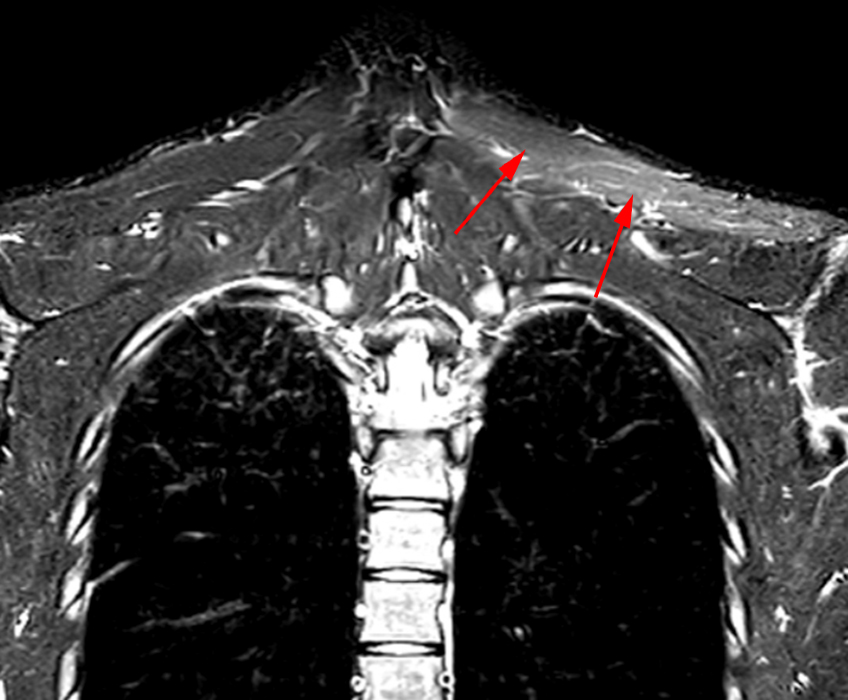
8b: In a different patient than 8a, a 15-year-old male presents with trapezius pain with C3-4 denervation on EMG. Coronal STIR image showing asymmetric diffuse left trapezius muscle edema (arrows) corresponding to denervation injury of the spinal accessory nerve.
Rhomboids
The rhomboid muscles lie deep to the trapezius, and both the major and minor components pass inferolateral from the vertebrae to the medial scapular margin. Denervation to this muscle is caused by injury to the dorsal scapular nerve, which is often thought to occur as the nerve passes through the scalenus muscle. This is a rare injury with the inciting cause usually sports activities. Damage causes winging of the scapula, and results in difficulty with throwing and overhead movement. MRI can show denervation changes both acute and chronic (fig 9).
Differential Diagnoses
Elastofibroma can simulate scapular winging. If large enough, these tumors can produce mass effect and uplifting of the scapula. These tumors are slow growing with benign characteristics and thought to possibly occur from repetitive friction between the scapula and thoracic wall, often producing clinical snapping scapula syndrome (fig 10). This entity is covered in detail in a prior Web Clinic.
Figure 10:
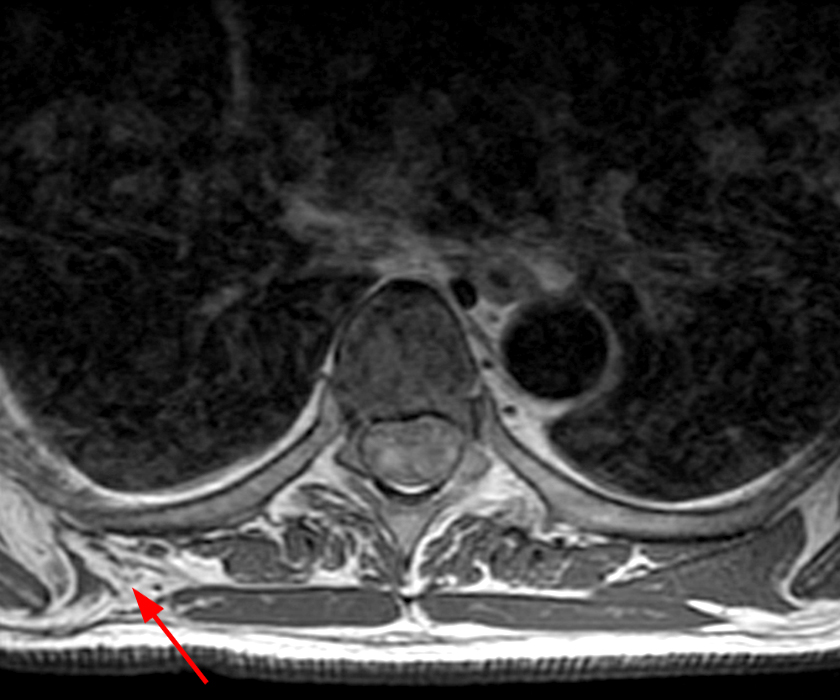
Axial T1-weighted image demonstrates a mass lesion between the chest wall and more superficial serratus anterior at the level of the inferior angle of the scapula containing internal elements of low signal and increased signal (arrows) corresponding to fibrous and fatty elements of an elastofibroma.
Figure 11:
Sagittal T2-weighted image in a 16-year-old female demonstrates a large bony excrescence contiguous with the inferior ventral scapula cortex (arrows) projecting anteriorly to abut the chest wall. Notice the distended scapulothoracic bursa (asterisk) with a thick walled pseudocapsule consistent with bursitis.
Other lesions
Space-occupying regions can be seen in the region of interest and discovered incidentally. Venous malformations (fig 12), ganglion cysts (fig 13) lipomas (fig 14), tumors (figs 15,16) and other rare conditions (fig 16) are sometimes visualized in or around the muscles in question. Muscular strains can also produce abnormal signal in the muscle in question (fig 17).
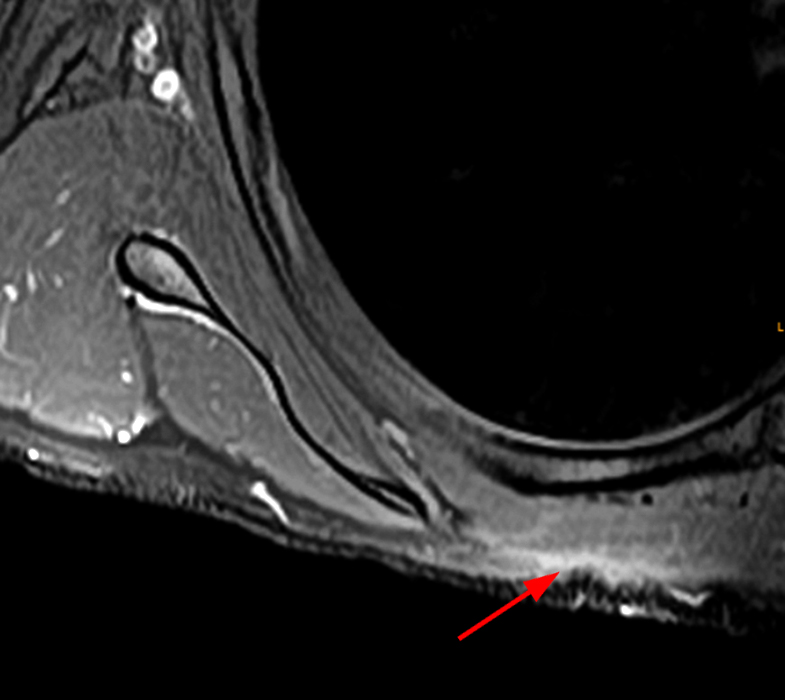
Figure 13:
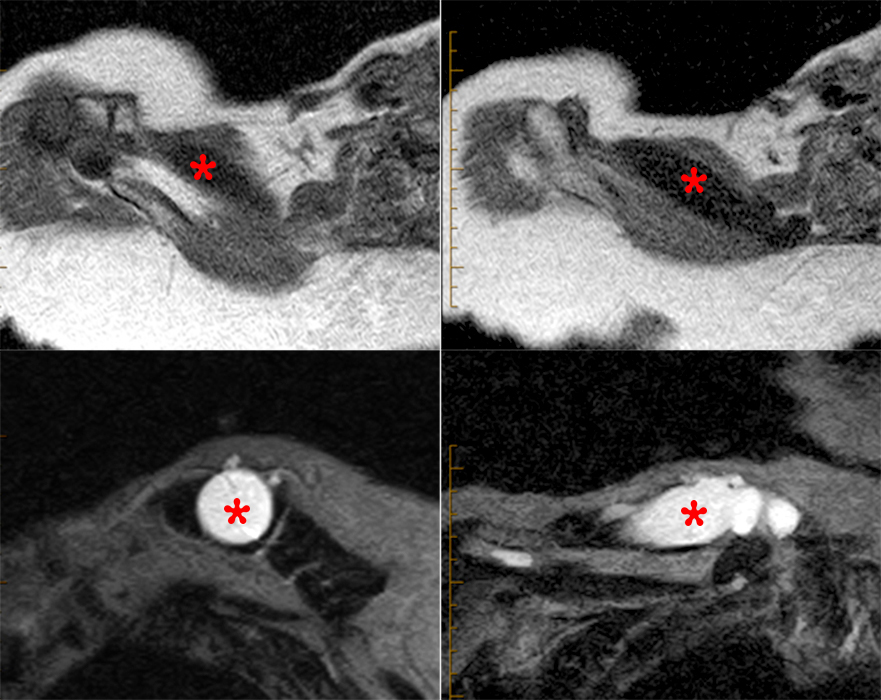
Axial T1-weighted sequential images (top) demonstrate a dissecting intramuscular ganglion cyst (asterisk) within the trapezius emanating from the AC joint and coursing medially. Sagittal (bottom left) and coronal (bottom right) fat-suppressed T2-weighted images reveal the intramuscular position and cystic characteristics of the lesion (asterisks).
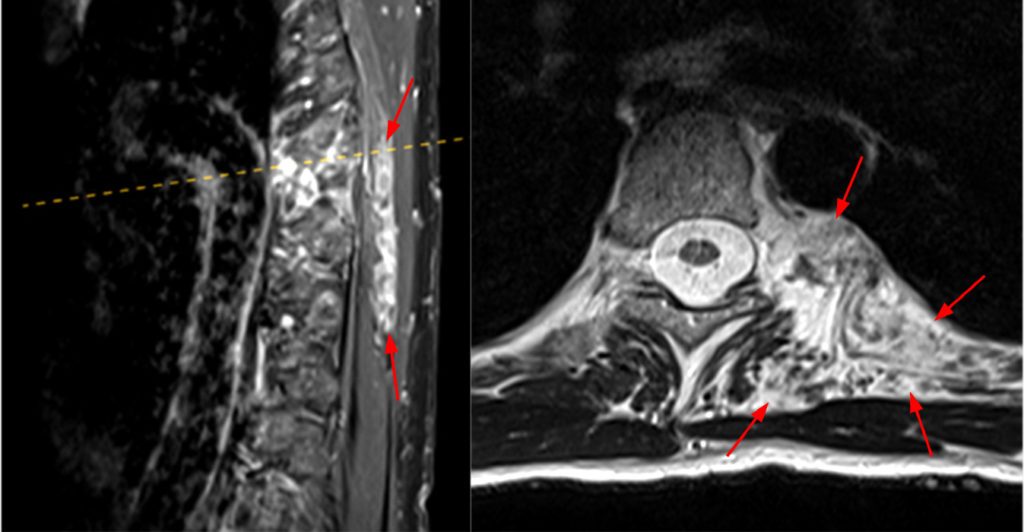
Figure 15:
Fat-suppressed sagittal post-contrast T1-weighted (left) and axial T2-weighted (right) images reveal a large infiltrating enhancing mass (arrows) deep to the left trapezius muscle remodeling the left T6 rib and extending from the left neural foramen, consistent with a plexiform neurofibroma.
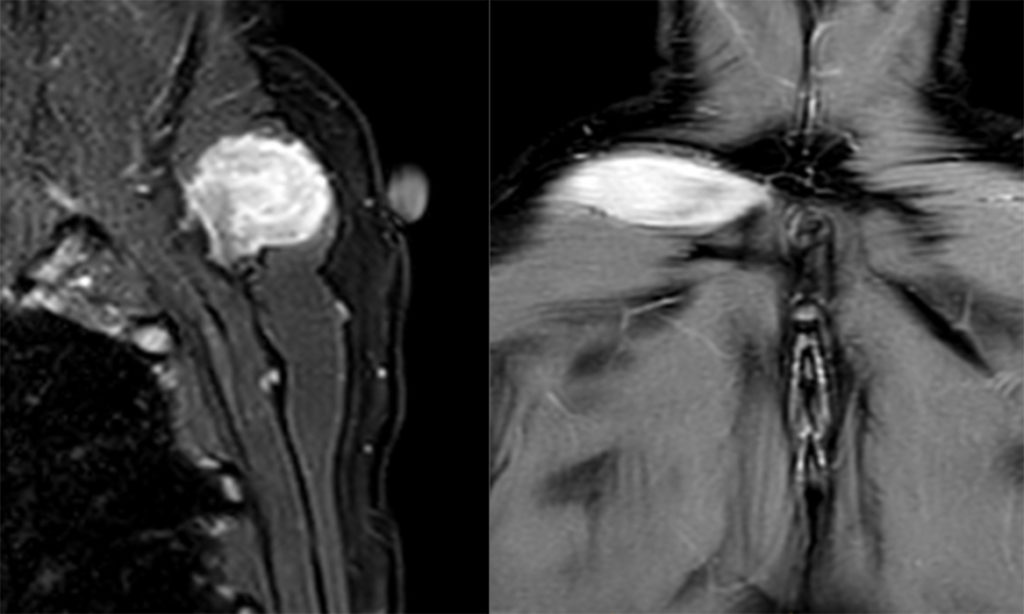
Figure 16:
Sagittal fat-suppressed T2-weighted (left) and coronal fat-suppressed proton density weighted (right) images in 23-year-old female with an enlarging mass over 3 months reveals an intramuscular mass within the right trapezius. The differential included nerve sheath tumor and sarcoma with a pathological diagnosis of proliferative myositis (notice the preserved low signal hypointense striations).
Treatment
Medial scapular winging is usually treated conservatively, with observation for at least 6 months to allow for nerve healing. During this time physical therapy for muscle strengthening and taping/bracing is performed. This is a long process and recovery can usually take up to a year or longer for resolution, but is successful in the great majority of patients. Surgical options for failure of conservative treatment include a split pectoralis major transfer whereby the sternal head of the pectoralis major is transferred to the inferior border of the scapula. Lateral scapular winging from injury to the accessory nerve often does not respond to conservative treatment. Surgical considerations for failed conservative treatment include exploration of the injury site with neurolysis obtaining more favorable results compared to end-end suturing and nerve repair. Most patients post recovery from surgery continue to have a winged deformity. If the injury is isolated to the trapezius muscle, a special procedure called the Eden-Lange muscle transfer can be performed whereby portions of the levator scapulae, rhomboid major, and rhomboid minor are diverted to the sites of trapezius attachment. Lateral scapular winging from injury to the rhomboid dorsal scapular nerve is usually treated conservatively by cervical spine stabilization and physical therapy. Steroid injections and massaging have been noted to occasionally help. Surgery in this condition involves two fascia lata slings, the first connecting the lower medial border of the scapula to the spinal muscles and the second spanning from the inferior angle of the scapula to the latissimus dorsi.
Conclusion
Scapular winging is a dysmorphic abnormality usually caused by injury to one of the innervating nerves of the posteromedial muscle stabilizers of the scapula. This condition causes pain and produces significant limitations of movement thereby making activities of daily living difficult. Weakness is a commonality amongst all patients with scapular winging. The diagnosis of a scapular wing is usually made clinically but the inciting cause is often not obvious. Electromyographic studies can help localize the muscle involvement producing the scapular winging. Diagnostic imaging is not always necessary but high-resolution imaging such as MRI can assist in identifying muscle involvement and allow localization of the affected area where nerve impingement or damage occurs. Treatment is usually conservative and focuses on strengthening the surrounding non-affected muscles while providing pain relief. Sometimes surgery is performed for refractory cases that do not respond to less invasive treatments.
References
- Miniato MA, Mudreac A, Borger J. Anatomy, Thorax, Scapula. (Updated 2021 Jul 26). In: StatPearls (Internet). Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538319/ ↩
- Martin RM, Fish DE. Scapular winging: anatomical review, diagnosis, and treatments. Curr Rev Musculoskelet Med. 2008 Mar;1(1):1-11. ↩
- Wiater JM, Bigliani LU. Spinal accessory nerve injury. Clin Orthop Relat Res 1999;368:5–16. ↩
- Benjamin W. T. Gooding, John M. Geoghegan, W. Angus Wallace, Paul A. Manning. Scapular Winging. Shoulder Elbow. 2014 Jan; 6(1): 4–11. Published online 2013 Jul 15. doi: 10.1111/sae.12033 ↩
- Smith CC, Bevelaqua AC. Challenging pain syndromes: Parsonage-Turner syndrome. Phys Med Rehabil Clin N Am 2014; 25(2): 265-277. ↩
- Robert Manske, Todd Ellenbecker. Current Concepts in Shoulder Examination of the Overhead Int J Sports Phys Ther. 2013 Oct; 8(5): 554–578 ↩
- Chernev I, Pessina MA. Unilateral complete congenital serratus anterior muscle aplasia: a case report. PM R 2009;1:587–589 ↩
- Blum, A, Lecocq, S, Louis, M, Wassel, J, Moisei, A and Teixeira, P. The nerves around the shoulder. Eur J Radiol. 2013; 82: 2–16. DOI: https://doi.org/10.1016/j.ejrad.2011.04.033 ↩
- Lindman R, Eriksson A, Thornell LE. Fiber type composition of the human male trapezius muscle: Enzyme‐histochemical characteristics. American Journal of anatomy. 1990 Nov;189(3):236-44. ↩
- Wiater JM, Bigliani LU. Spinal accessory nerve injury. Clin Orthop Relat Res 1999;368:5–16. ↩