Clinical History: A 53 year old female presents with back and left leg pain. A T1-weighted sagittal image (1a) and a fast spin-echo T2 weighted axial (1b) image are provided. What are the findings” What is your diagnosis?
Findings
Figure 2:
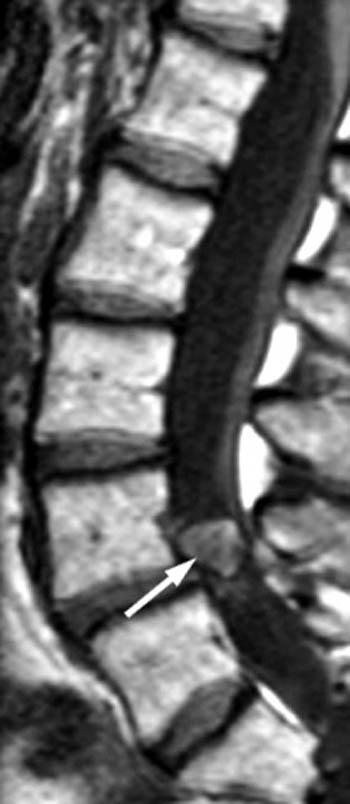
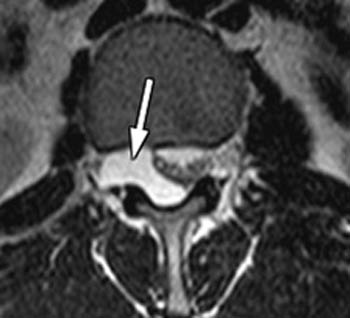
On the T1-weighted sagittal image (2a), an intraspinal lesion (arrow) is identified just above the level of the L4-5 disc. Grade I spondylolisthesis is apparent at L4-5.
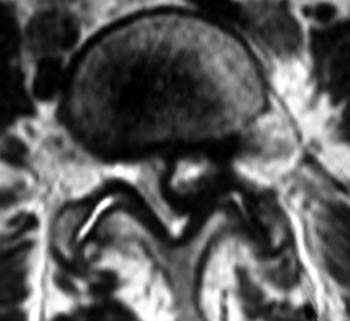
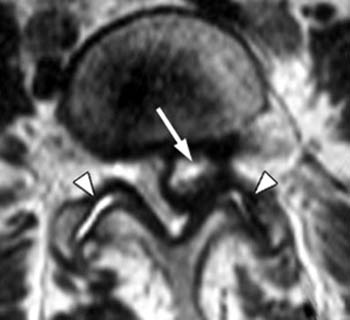
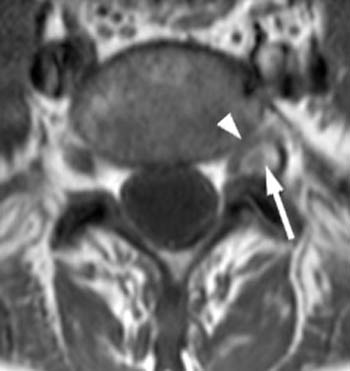
The lesion is hyperintense, with a low signal-intensity rim (arrow), on (2b) the T2-weighted axial view. The thecal sac is displaced towards the right and effacement of the left L5 nerve root is present. Prominent bilateral facet hypertrophic changes are also evident (arrowheads).
Diagnosis
Lumbar synovial cyst, arising from the left L4-5 facet.
Discussion
Facet joint synovial cysts are a well known cause of back pain and radiculopathy.1 Although originally felt to be uncommon, the advent of cross sectional imaging techniques such as CT and MR have led to a large increase in the recognition of these lesions. Synovial cysts typically arise in association with osteoarthritis of the facet joints. They are most often found in patients over 50 and are more common in females. Degenerative spondylolisthesis is frequently present in these patients, and L4-5 is the most common level of abnormality. Such associations are useful in differentiating synovial cysts from other cystic structures within the spinal canal, such as arachnoid cysts or perineural cysts. Synovial cysts can also be differentiated from other cysts histologically, as they are lined by synovial cells.
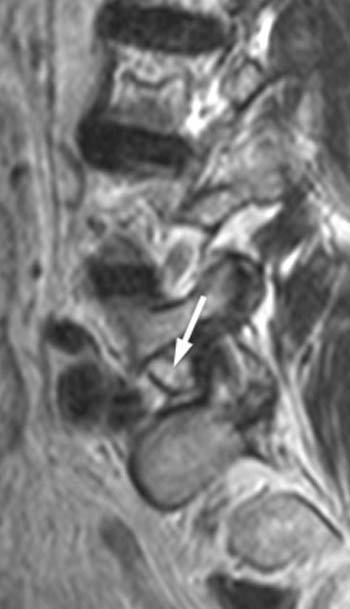
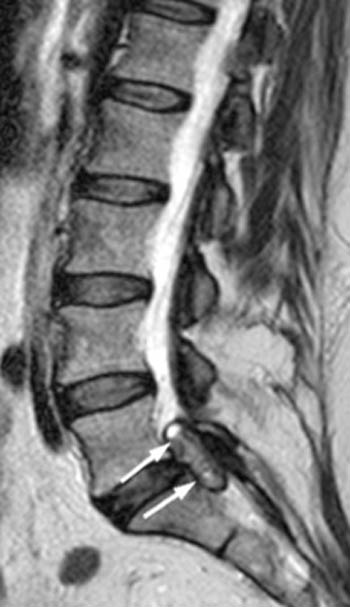
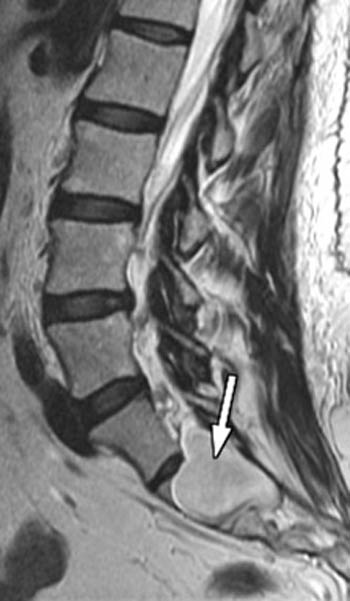
Patients with clinically significant synovial cysts usually present with lumbar radiculopathy, often preceded by generalized back pain, the latter perhaps being related to facet disease. Because the cysts characteristically project anteromedially from the facet joint, the radiculopathy in such cases involves the traversing nerve root. Rarely, the cyst can extend anterolaterally relative to the facet, and in such cases compression of the exiting nerve root may be seen within the neural foramen (3a, 4a).
In cases of very large cysts, patients may present with neurogenic claudication due to central stenosis (5a,5b). Acute hemorrhage within a cyst may also result in a rapid exacerbation of symptoms, with severe cases resulting in cauda equina syndrome.2,3
Figure 5:
Fast spin-echo T2-weighted sagittal (5a) and post-contrast T1-weighted axial (5b) images reveal a very large synovial cyst (arrows) at L5-S1 in this patient who presented with both radiculopathy and neurogenic claudication. The thecal sac (arrowheads) is narrowed and displaced towards the right. As is typical, the cyst enhances peripherally (asterisks) but not centrally following contrast administration.
MR’s superior soft tissue contrast and resolution allow accurate and confident diagnosis of synovial cysts. Though some cysts may simply be of fluid signal intensity, more commonly, as demonstrated in the cases above, the signal characteristics of the cysts are complex. On T1-weighted images, hyperintensity may be present within the cyst due to the presence of hemorrhage (2a, 4a). On T2-weighted images, areas of fluid signal intensity are usually present, but hemorrhage, calcification, or vacuum phenomena often lead to a heterogeneous appearance.4 If gadolinium is given, peripheral enhancement of the cysts is seen (5b). The keys to the diagnosis of synovial cysts, however, are to recognize the association of the lesion with the facet joint, and to visualize the highly characteristic peripheral low signal intensity rim on T2-weighted images (2b,3a,5a). This rim is caused by the synovial lining, and is not an imaging feature of other intraspinal cysts such as arachnoid cysts, ganglia, or perineural cysts (6a,6b).
Figure 6:
A T2-weighted axial image (6a) of an intradural arachnoid cyst (arrow) and a (6b) T2-weighted sagittal image of a large sacral perineural cyst (arrow) are provided. These intraspinal cysts are typically of relatively homogeneous fluid signal intensity, and lack the characteristic hypointense peripheral rim that is found on T2-weighted images of synovial cysts.
In patients with symptomatic synovial cysts, surgical decompression may be indicated to relieve the mass effect upon nerve roots and/or the thecal sac. MR provides a valuable preoperative roadmap in such cases. Instability or spondylolisthesis at the level of the synovial cyst may also be addressed through operative fixation. An alternative approach in select patients is the use of percutaneous steroid and local anesthetic injections into the cysts, performed under CT or fluoroscopic guidance. This approach has been shown to be an effective alternative to surgery, providing both immediate and long term relief of symptoms in many patients.5
Summary
Synovial cysts arising from lumbar facet joints are a not uncommon cause of radiculopathy and spinal stenosis in older patients. Symptoms from these cysts are often indistinguishable from those caused by other space occupying lesions in the lumbar spine, such as disc herniations, and indeed may arise acutely in association with cyst hemorrhage. MR allows accurate diagnosis in such patients, as the appearance of synovial cysts on MR is characteristic. In patients requiring intervention, MR provides a valuable roadmap of the level, location, and size of the lesion, all factors which may influence the operative or percutaneous approach to treatment.
References
1 Kao C, Uihlein A, Bickel W, Soule E. Lumbar intraspinal extradural ganglion cyst. J Neurosurg 1968; 29:168-172.
2 Howling SJ, Kessel D. Case report: acute radiculopathy due to a haemorrhagic lumbar synovial cyst. Clin Radiol 1997; 52:73-74.
3 Tatter S, Cosgrove GR. Haemorrhage into a lumbar synovial cyst causing acute cauda equina Syndrome: Case report. J Neurosurgery 1994; 81: 449-452.
4 Liu SS, Williams KD, Drayer BP, Spetzler RF, Sonntag VK. Synovial cysts of the lumbosacral spine: diagnosis by MR imaging. AJR 1990; 154:163-166.
5 Bureau NJ, Kaplan PA, Dussault RG. Lumbar Facet Joint Synovial Cyst: Percutaneous Treatment with Steroid Injections and Distention-Clinical and Imaging Follow-up in 12 Patients. Radiology 2001;221:179-185.