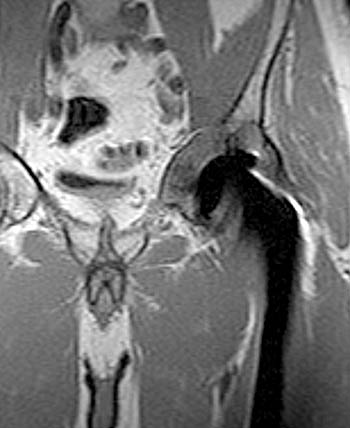
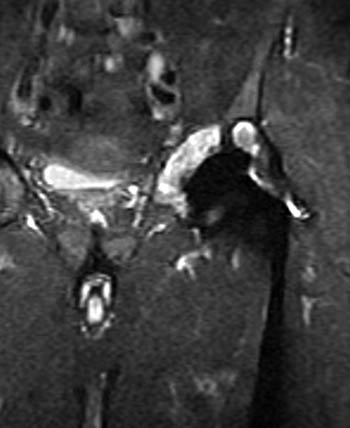
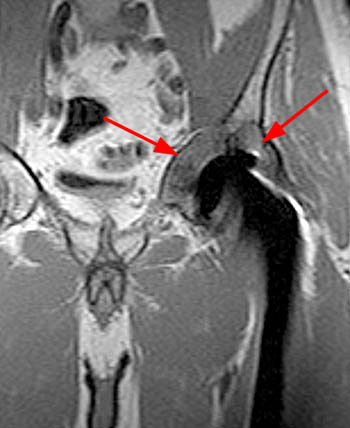
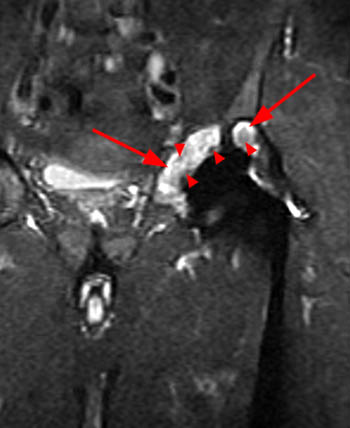
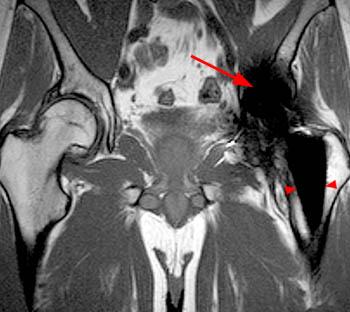
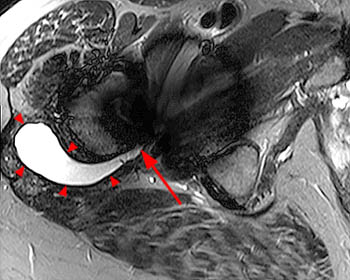
Clinical History: A 60 year-old male presents with recurrent left hip pain 13 years following total joint replacement of the left hip. (1a) Coronal T1-weighted and (1b) coronal STIR images of the hip are provided. What are the findings? What is your diagnosis?
Findings
Diagnosis
Left acetabular osteolysis following total hip arthroplasty.
Introduction
Traditionally, magnetic resonance imaging (MR) has been felt to have a limited role in the evaluation of the affected hip in patients who have undergone hip arthroplasty, as extensive magnetic susceptibility artifact related to the indwelling hardware resulted in images felt to be non-diagnostic. Additionally, some physicians and imaging sites may still question the safety of scanning patients with indwelling metal implants. Of course, most radiologists are now aware that there is no safety risk in performing MR in patients who have had a prior hip arthroplasty, and MR has been found to be an extremely effective tool for the evaluation and management of patients who present with pain following hip arthroplasty1.
The most frequent abnormality that affects the long term viability of a total hip arthroplasty is osteolysis2,3. Osteolyis is but one manifestation of particle disease, a complex response to the microdebris that is generated in arthroplasty patients. Plain radiographs have traditionally been the mainstay for the assessment of osteolysis, and remain the current clinical standard. Yet plain films are known to underestimate the existence and extent of osteolysis, and detection of osteolysis on plain films is influenced by lesion size and location4. Computed tomography (CT) with newer metal artifact reduction techniques can effectively detect osteolysis, but CT lacks the soft tissue contrast of MR, and serial CT evaluations have the potential of subjecting the patient to a hazardous amount of ionizing radiation. MR, with proper technique, has been found to be the most sensitive imaging test for the detection of osteolysis5. In addition, MR’s superior soft tissue contrast, multiplanar capability, and lack of ionizing radiation make it ideally suited for the evaluation of numerous other entities that may account for pain in a patient who has undergone hip arthroplasty.
MR Imaging Technique
Metal components of hip arthroplasties typically degrade image quality primarily because of magnetic susceptibility effects which distort the regional magnetic field, creating large areas of signal void with adjacent smaller areas of extremely high signal intensity. The degree of artifact is influenced by numerous factors, including the strength of the magnetic field, the shape of the implant, and the composition of the implant. Titanium is less ferromagnetic than cobalt-chrome and results in less artifact6(4a), as do newer materials such as ceramic surface oxidized zirconium7. Innovative pulse sequences have been devised for the reduction of MR metal artifact in arthroplasty patients, with examples being MARS (metal artifact reduction sequence)8, MAVRIC (multi-acquisition variable-resonance image contribution)9, and SEMAC (slice encoding for metal artifact correction)10. It is expected that such pulse sequences will become more routinely available on clinical scanners in the future. However, diagnostic images can be obtained today without the use of specialized pulse sequences, and simply require modifications to commercially available pulse sequences found on the vast majority of clinical scanners11.
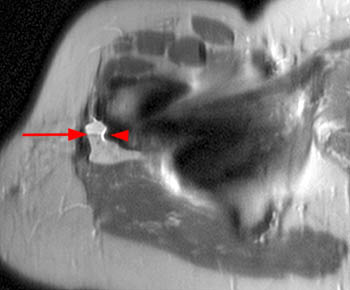
Figure 4:
Prominent susceptibility artifact is seen about the spherical cobalt-chrome femoral head component (arrow) of this left hip arthroplasty on a fast spin-echo T1-weighted coronal image utilizing artifact reducing techniques. The degree of "blooming" is significantly less surrounding the titanium femoral stem component (arrowheads).
The key modification to the technique is to use as wide a receiver bandwidth as possible. This significantly reduces the frequency shifts that distort MR images, though at the expense of a reduction in signal to noise. Fast spin-echo technique should be used whenever possible, even with T1-weighted images, as the refocusing pulses inherent to fast spin-echo serve to reduce metal artifact. Additional effective modifications included aligning the long axial of the metal components parallel to the axis of the frequency encoding gradient, the use of high resolution matrices in the frequency encoding direction, and the avoidance of spectral fat suppression or gradient echo techniques, both of which are known to be highly degraded in the presence of metal implants. Fast inversion recovery sequences are therefore the preferred method of fat-suppression and water sensitive imaging in patients with hip arthroplasty. Lastly, because magnetic susceptibility artifact is directly proportional to the strength of the magnetic field, imaging of hip arthroplasty is one of the relatively rare indications in which 3 Tesla magnets should be avoided, and in which the use of magnetic field strengths below 1.5 Tesla may even be preferable12.
MR of Particle Disease and Osteolysis
The majority of complications related to failure of total hip arthroplasties are thought to be related to particle disease. Particle disease refers to the reaction that occurs in response to small particles of debris that are released due to wear of arthroplasty components. In hip arthroplasty patients, this reaction can occur due to particles of metal, polyethylene, and/or cement. The presence of these microscopic particles within the joint leads to a cellular response primarily from macrophages. Inflammatory cells infiltrate the synovium, resulting in synovial hypertrophy and effusions13. The macrophages are unable to digest the particles, and as a result inflammatory cytokines and growth factors are released. A complex physiologic response ensues which may lead to bone resorption (osteolysis), primarily by osteoclasts14.
The earliest MR finding that results from particle disease is the presence of a joint effusion due to reactive synovitis (5a), and reactive synovitis in these patients may occur before symptoms arise15. MR images in affected patients may reveal capsular thickening and the presence of low signal intensity debris within the joint, though normal fluid signal intensity of the effusion may also be found. Unfortunately, visualization of the joint itself is perhaps the most challenging area for MR imaging following hip arthroplasty, as metal artifact tends to be greatest about the spherical femoral head component of the arthroplasty, and artifact in this region is even more pronounced with metal on metal cobalt-chrome prostheses. As a result, small effusions that do not distend the joint may be missed early in the course of particle disease.
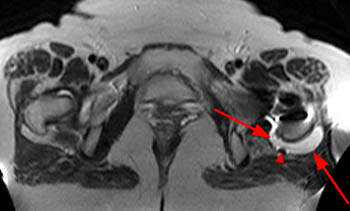
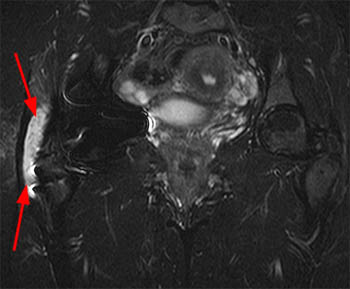
Figure 5:
An effusion distends the posteroinferior joint (arrows) in this 46 year-old female with recurrent pain one year following left hip arthroplasty. Note the small focus of susceptibility artifact (arrowhead) within the posterior aspect of the effusion, suggesting the presence of metal debris.
With particle disease progression, osteolysis ensues, and osteolysis is the most frequent serious complication in patients following hip arthroplasty. Bone resorption that occurs in osteolysis may be visible on plain films, though plain radiographs are less sensitive than MR and the sensitivity of plain radiographs is more dependent upon lesion location than is MR. Osteolysis may occur anywhere along the “effective joint space” of the hip, that is, the entire region surrounding the joint into which particles may migrate and contact bone16. As a result, osteolysis may be seen anywhere from the superior acetabulum to the distal tip of the prosthesis. On MR images, osteolysis has an intermediate signal intensity appearance, similar to or slightly brighter than skeletal muscle, on both T1- and T2-weighted images. A low signal intensity rim which outlines the lesion is typical (6a). Infection or malignancy, in distinction, is more hyperintense on T2-weighted images and a low signal intensity rim would not be expected. Osteolysis may also result in cortical expansion and disruption, and extraosseous deposits of similar signal intensity may be seen in such cases. Extraosseous components may result in symptoms due to compression of adjacent neural structures (7a,8a).
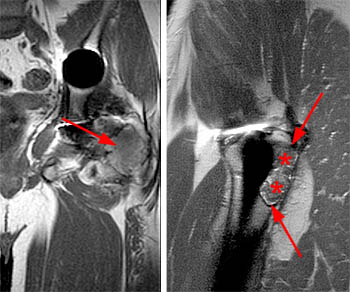
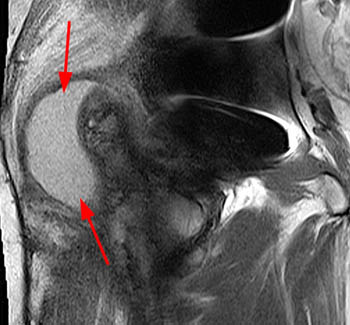
Figure 6:
(Left) T1-weighted coronal and (right) proton density-weighted sagittal images demonstrate intermediate signal intensity osteolysis (arrows) within the posterior greater trochanter in this patient 4 years s/p left hip arthroplasty. A low signal intensity rim is evident on both images, and areas of internal low signal intensity (asterisks) are more prominent on the proton density-weighted sagittal view.
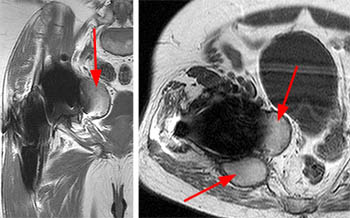
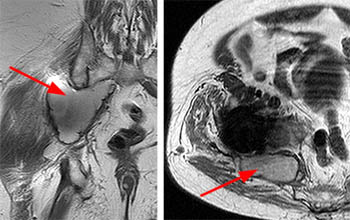
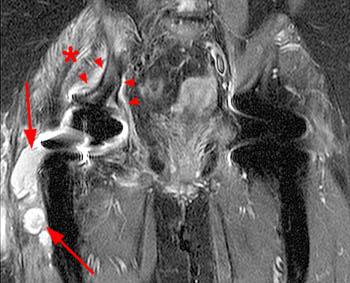
Figure 7:
A 67 year-old male with right foot drop and leg weakness years following placement of a right hip arthroplasty. Fast spin echo T1-weighted images demonstrate particle disease that markedly expands and destroys the medial acetabular wall (arrows) on (left) coronal and (right) axial views.
Pseudotumors and Metal-On-Metal Resurfacing Arthroplasty
Hip resurfacing arthroplasty has become increasingly utilized as an alternative to conventional arthroplasty, particularly in younger patients. Resurfacing arthroplasty is felt to have the advantages of longer viability, greater preservation of native bone, greater stability, improved range of motion, and optimization of stress loads upon the proximal femur17. These implants consist of metal-on-metal articulations, unlike the metal on polyethylene articulations of most conventional hip arthroplasties. The metal-on-metal implants are typically made of cobalt-chrome. Wear particles from these implants are known to be smaller than those from conventional implants, but appear to be at least ten times more numerous18. Metal ions are released both within the joint and systemically.
In 2005, Willert et al. described pronounced perivascular lymphocyte and plasma cell infiltrates around metal on metal articulations, presumably as a reaction to metal ions19. These were termed aseptic lymphocytic vasculitis-associated lesions, or ALVALs. More recently periarticular fluid collections or masses have been reported in numerous patients who had undergone metal-on-metal hip resurfacing20, and have been termed “pseudotumors”. These lesions have similar inflammatory changes to those described in ALVAL lesions, but have greater lymphocytic infiltrates and tissue necrosis. The mechanism of formation of these masses/fluid collections may be multifactorial, as elements of delayed hypersensitivity reactions as well as direct toxic effects of metal ions have been found histologically in these patients. Of interest is the high preponderance of female patients who develop pseudotumors following metal-on-metal resurfacing. Although mechanical factors and variances in implant size may in part account for the gender discrepancy, many authors suggest that prior sensitization to metal from ear piercing may increase the frequency of hypersensitivity reactions to metal implants in female patients.
On MR images, pseudotumors are most commonly located at the posterolateral aspect of the joint, often in continuity with the greater trochanter (9a,10a). Such posterior lesions are typically cystic in nature, though layering of contents, a low signal intensity wall, and foci of susceptibility artifact due to metal content result in an appearance unlike that of pure fluid. Anterior lesions may also be seen, generally involving the region of the iliopsoas bursa, and these anterior lesions are more likely to have solid components. Pseudotumors are characteristically contiguous with the joint capsule, and it is likely that these lesions represent a response to joint inflammation and distension in these patients, with anterior lesions representing distension of the iliopsoas bursa, and posterior lesions representing extension through posterior capsular defects caused by the typical surgical approach for placement of hip arthroplasties. At surgery, pseudotumors may have a grossly dark appearance due to the high metal content within the fluid of these lesions (11a).
Figure 11:
An intraoperative photo from a patient undergoing revision of a metal-on-metal hip arthroplasty. The image is taken from behind with the patient prone. The greater trochanter (GT) is indicated. Arrows point to a small mass along the lateral aspect of the greater trochanter. Upon resection, the lesion was filled with black fluid, presumably secondary to high metal content.
Although pseudotumors have been reported most frequently in association with metal-on-metal hip implants, it should be noted that pseudotumors are simply an additional manifestation of particle disease, and therefore they may be seen in hip arthroplasties of any type, including metal-on-polyethylene implants. However, an implant of particular note is the Depuy (Johnson and Johnson) ASR Hip Resurfacing System. This particular implant appears prone to complications of particle disease, including pseudotumor (12a,13a), with revision rates in patients receiving these implants being greater than 5%21. In light of the high rate of device failure, on August 24, 2010, Depuy/Johnson and Johnson announced a voluntary recall of all ASR products. The manufacturer’s recommendations for the management of patients with ASR implants includes the use of MR for surveillance of symptomatic patients or certain asymptomatic patients with significantly elevated metal ion levels on blood tests. In part because of the attention and increased utilization of MR from this recall, the need for MR of hip arthroplasties is likely to significantly increase in the future.
Figure 12:
Despite extensive metal artifact in this patient 1.5 years following placement of a Depuy ASR metal-on-metal hip resurfacing implant, a pseudotumor at the posterolateral aspect of the greater trochanter (arrow) is readily apparent on the fast spin-echo proton density-weighted coronal view.
Differential Diagnosis
Osteolysis in patients following hip arthroplasty may be confused with malignancy, but recognition of the distribution and typical lower signal intensity appearance of osteolysis allows the differentiation to be easily made in most cases. Low signal intensity internal components on T2-weighted images and in particular a low signal intensity rim are unlikely to be found in patients with osseous malignancy.
With regard to pseudotumors, which often have a predominantly fluid-signal appearance, there are two important alternative diagnostic alternatives that should be considered. Infection is a known complication in patients following hip arthroplasty, and infection can of course cause large fluid collections/abscesses to form in the region of the prosthesis. On MR images, infected fluid collections tend to be less well defined than pseudotumors, and they lack a low signal intensity rim (14a). Soft-tissue edema may be seen with either infection or pseudotumor, but extensive, ill-defined perifascial fluid is more suggestive of infection.
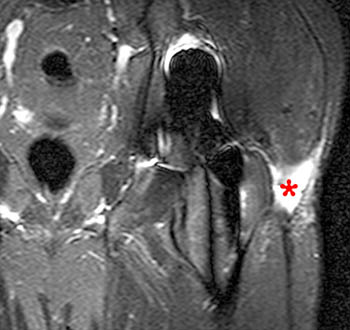
Figure 14:
A 56 year-old female presented with clinical signs of infection 5 years s/p bilateral total hip arthroplasties. A STIR coronal image is provided. Lobulated fluid (arrows) is seen lateral to the proximal femur, with surrounding edema and fluid extending into subcutaneous fat. Soft-tissue edema is present within the adjacent gluteal muscles (asterisk), and ill-defined fluid extends about the acetabular and iliac regions (arrowheads). Note the lack of a low signal intensity rim surrounding the largest fluid collection. Infected fluid was confirmed at the time of revision surgery.
Abductor tendon avulsion is a known cause of recurrent pain and/or dysfunction in patients following hip arthroplasty, particularly when an anterolateral approach is utilized22. Fluid collections are often present in association with these abductor avulsions (15a). These collections tend to be of pure fluid signal and lack a low signal intensity rim. Their typical location at the site of abductor avulsion provides another clue to the etiology. It should be noted, however, that particle disease including pseudotumors may coexist with abductor tendon avulsions following hip arthroplasty.
Treatment implications
In patients with recurrent pain or dysfunction following hip arthroplasty, MR provides a sensitive and comprehensive means with which to evaluate for the presence of complications. The spectrum of particle disease has characteristic features which in most cases will allow differentiation from entities such as infection or neoplasm. When MR findings of a peri-hip fluid collection are not distinctive, accurate localization of fluid at least allows guidance for needle aspiration. In cases of osteolysis, MR allows the most accurate characterization of the extent of bone loss, an important consideration in determining whether bone graft or other adjunctive measures will be necessary at the time of hip revision. Better quantification of osteolysis burden may also be of benefit in conservative therapies, such as the use of oral bisphosphonates (currently being evaluated), allowing serial evaluations of progress in such patients. Lastly, in the high risk patient, such as one who has elevated serum metal levels and an indwelling high risk implant, MR allows non-invasive evaluation for complications of particle disease, even before symptoms arise.
Conclusion
With proper adjustments to imaging technique, conventional MR scanners are able to provide highly diagnostic images of patients who have had prior hip arthroplasty. The study of particle disease (including synovitis, osteolysis, and pseudotumor formation) is an evolving field but one that will likely only increase in importance as our understanding of the imaging appearance, clinical effects, and treatment options are further elucidated. MR is able to distinguish particle disease from other entities which may cause pain following arthroplasty, and MR’s ability to accurately detect and quantify the extent of particle disease is important in guiding treatment decisions.
References
1 Potter HG, Foo LF, Nestor BJ. What is the role of magnetic resonance imaging in the evaluation of total hip arthroplasty? HSSJ 2005, 1:89-93.
2 Harris WH. Wear and periprosthetic osteolysis: The problem. Clin Orthop 2001, 393:66-70.
3 Zicat B, Engh CA, Gokcen E. Patterns of osteolysis around total hip components inserted with and without cement. J Bone Joint Surg 1995, 77A:432-439.
4 Claus AM, Engh Jr CA, Sychterz CJ, et al. Radiographic definition of pelvic osteolysis following total hip arthroplasty. J Bine Joint Surg 2003, 85A:1519-1526.
5 Walde TA, Weiland DE, Leung SB, et al. Comparison of CT, MRI, and radiographs in assessing pelvic osteolysis. Clin Orthop and Related Research 2005, 437:138-144.
6 Ebrahelm NA, Savolaine ER, Zeiss J, Jackson WT. Titanium hip implants for improved magnetic resonance and computed tomography examinations. Clin Orthop 1992, 275:194-198.
7 Raphael B, Haims AH, Wu JS, et al. MRI comparison of periprosthetic structures around zirconium knee prostheses and cobalt chrome prostheses. AJR 2006, 186:1771-1777.
8 Olsen RV, Munk PL, Lee MJ, et al. Metal artifact reduction sequence: early clinical applications. Radiographics 2000, 20:699-712.
9 Koch KM, Brau AC, Chen W, et al. Imaging near metal with a MAVRIC-SEMAC hybrid. Magn Reson Med 2010, 65:71-82.
10 Lu W, Pauly KB, Gold GE, et al. SEMAC: slice encoding for metal artifact correction in MRI. Magn Reson Med 2009, 62(1):66-76.
11 Potter HG, Nestor BJ, Sofka CM. Magnetic resonance imaging after total hip arthroplasty: evaluation of periprosthetic soft tissue. J Bone Joint Surg Am 2004, 86:1947-1954.
12 Sugimoto H, Hirose I, Miyaoka E. Low field strength MR imaging of failed hip arthroplasty: association of femoral periprosthetic signal intensity with radiographic, surgical, and pathologic findings. Radiology 2003, 229:718-723.
13 Weissman BN, Scott RD, Brick GW, Corson JM. Radiographic detection of metal induced synovitis as a complication of arthroplasty of the knee. J Bone Joint Surg Am 1991, 73A:1002-1007.
14 Athanasou NA, Quinn J, bulstrode CJK. Resorption of bone by inflammaroty cells derived from the join capsule of hip arthroplasties. J Bone Joint Surg Br 1992, 74:57-62.
15 Cooper HJ, Ranawat AS, Potter HG, et al. Early reactive synovitis and osteolysis after total hip arthroplasty. Clin Orthop Rel Res 2010, 468(12):3278-3285.
16 Harris WH. Osteolysis and particle disease in hip replacement: a review. Acta Orthop Scand 1994, 65(1):113-123.
17 Fang CSJ, Harvie P, Gibbons CLMH et al. The imaging spectrum of peri-articular inflammatory masses following metal-on-metal hip resurfacing. Skel Rad 2008, 37:715-722.
18 Firkins PJ, Tipper H, Saadatzadeh MR, et al. Quantitative analysis of wear and wear debris from metal-on-metal hip prostheses tested in a physiological hip joint simulator. Biom mater Eng 2001, 11:143-157.
19 Willert HG, Buchhorn GH, Fayyazi A, et al. Metal-on-metal bearings and hypersensitivity in patients with artificial hip joints, a clinical and histomorphological study. J Bone Joint Surg Am 2005, 87:18-27.
20 Pandit H, Glyn-Jones S, McLarky-Smith P, et al. Pseudotumors associated with metal-on-metal hip resurfacings. J Bone Joint Surg Br 2008, 90-B:847-851.
21 Jameson SS, Langton DJ, Nargo AVF. Articular surface replacement of the hip: a prospective single surgeon series. J Bone Joint Surg Br 2010, 92-B:28-37.
22 Twair A, Ryan M, O’Connell M, et al. MRI of failed total hip replacement caused by abductor muscle avulsion. AJR 2003, 181:1547-1550.