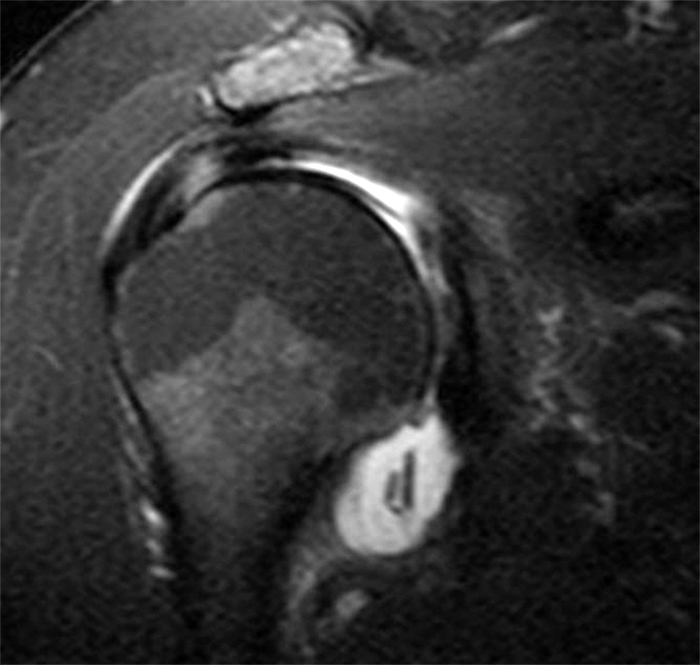
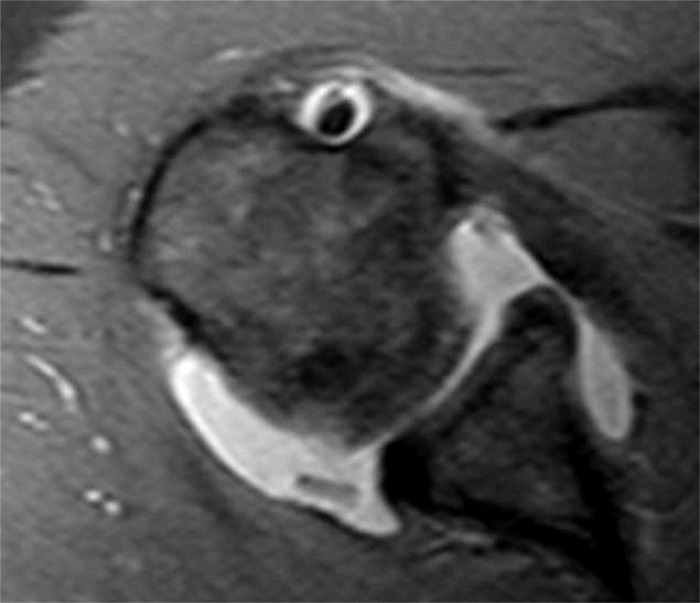
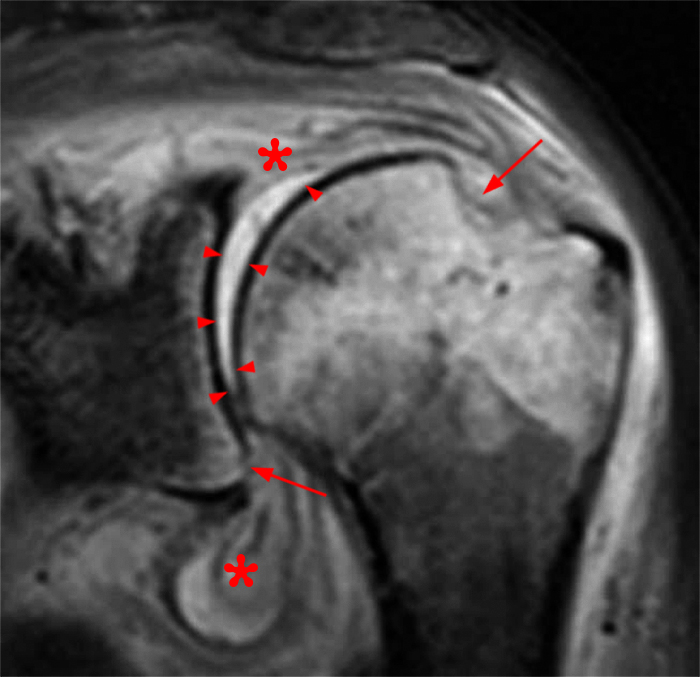
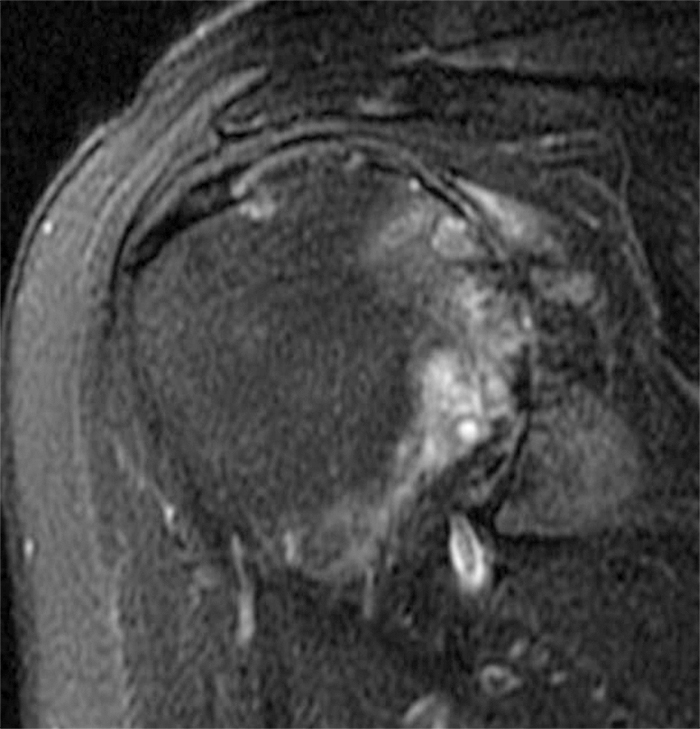
Clinical History: A 48 year-old female presents with right shoulder pain and limited range of motion for 5 months and no known injury. (1A) Fat-suppressed T2-weighted coronal and (1B) fat-suppressed proton density-weighted axial images are provided. What are the findings? What is your diagnosis?
Findings
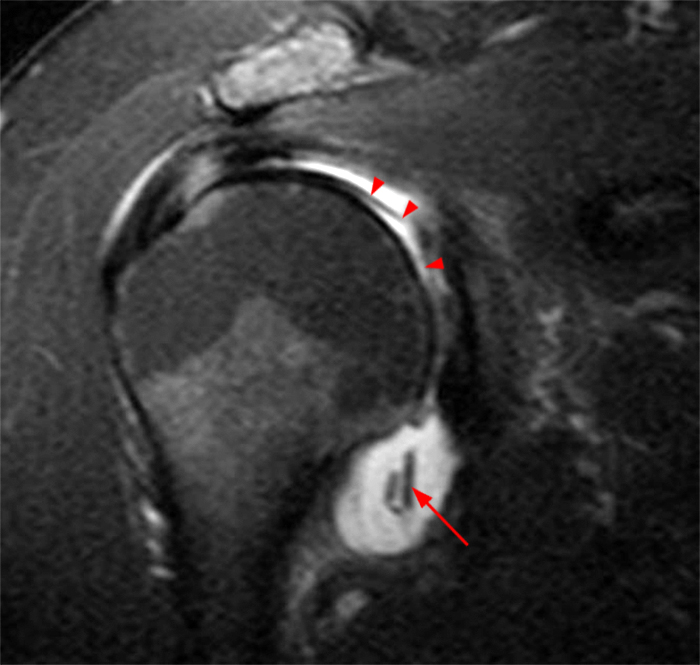
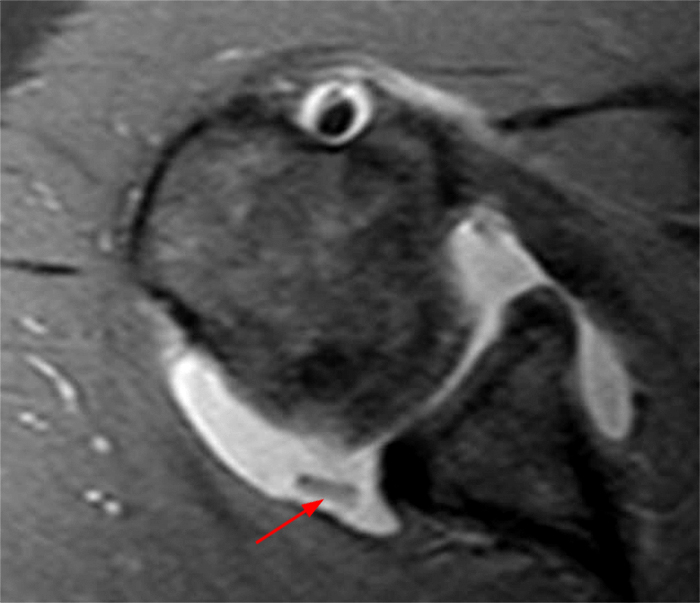
Figure 2:
(2A) A coronal T2-weighted image of the shoulder with fat suppression reveals diffuse delamination of the articular cartilage of the humeral head (arrowheads), a large joint effusion and loose intraarticular chondral fragments in the axillary recess (arrow). (2B) The axial fat-suppressed proton density-weighted image demonstrates a large joint effusion and a loose intraarticular chondral fragment in the posterior joint recess (arrow). Glenoid articular cartilage remains intact.
Diagnosis
Idiopathic glenohumeral chondrolysis with a joint effusion and loose intraarticular chondral fragments.
Introduction
Glenohumeral chondrolysis, progressive articular cartilage loss occurring over a relatively short period of time, is an uncommon diagnosis, but has been reported multiple times over the last 10 years as a devastating postoperative complication. In the absence of previous surgery, causes include infection and trauma, but frequently the entity is idiopathic. Chondrolysis usually leads to chronic pain, stiffness and loss of range of motion. MRI plays an important role in documenting the extent of cartilage loss and to exclude other entities that can present in a similar way.
Etiology and clinical presentation
Patients with glenohumeral chondrolysis encompass a wide age range and typically present within 12 months after a surgical intervention or other insult. They are often young and have fairly rapid progression of pain with limited range of motion, crepitus and mechanical catching.1 The pain may be out of proportion to the clinical findings, which could lead to an incorrect diagnosis of complex regional pain syndrome. The most common cause is surgery in which there has been violation of the articular cartilage, including placement of pins, screws, suture anchors and knots, usage of electrocautery, radiofrequency probes and YAG laser, and intraarticular administration of local anesthetics with pain pump, chlorhexidine, and gentian violet.2 In a retrospective cohort study of 375 patients that underwent shoulder arthroscopy 13% developed glenohumeral chondrolysis, and each one of those patients had received an intra-articular postoperative infusion of an anesthetic.3 The risk of glenohumeral chondrolysis was greater for those with one or more suture anchors in the glenoid, and for younger patients. Preexisting glenohumeral chondromalacia and joint instability may predispose to chondrolysis, but there is no way to definitively predict who is at risk for chondrolysis . The exact pathogenesis and biomechanical pathways of cartilage destruction remain unclear, and theories include inflammatory cellular responses and early disruption of cartilage extracellular organization.4,5
MRI Diagnosis
Diffuse cartilage loss with progressive narrowing of the joint space may be evident on radiographs, but sensitivity is limited.6 MRI is routinely used for assessment of the degree and extent of articular cartilage abnormalities and surpasses other imaging modalities in this regard. Early MRI findings in glenohumeral chondrolysis have previously not been published, but the subacute or chronic imaging appearance on low-field MRI was recorded in a study of four patients who developed chondrolysis after shoulder arthroscopy. Features include extensive, uniform, diffuse loss of articular cartilage of the glenoid and humeral head, focal areas of subchondral cortical irregularity as well as focal subchondral marrow edema and sclerosis on the glenoid and medial aspect of the humeral head.7 No synovitis, intraarticular body or marginal osteophyte formation was detected.
MRI has been used for the diagnosis of chondrolysis in other joints, including the hip. Early MRI findings in idiopathic chondrolysis of the hip in children include a geometric or polygonal focal marrow edema pattern centered in the middle one third of the proximal femoral epiphysis, adjacent acetabular bone marrow edema, mild synovial hypertrophy, and little or no joint fluid.8
Figure 3:
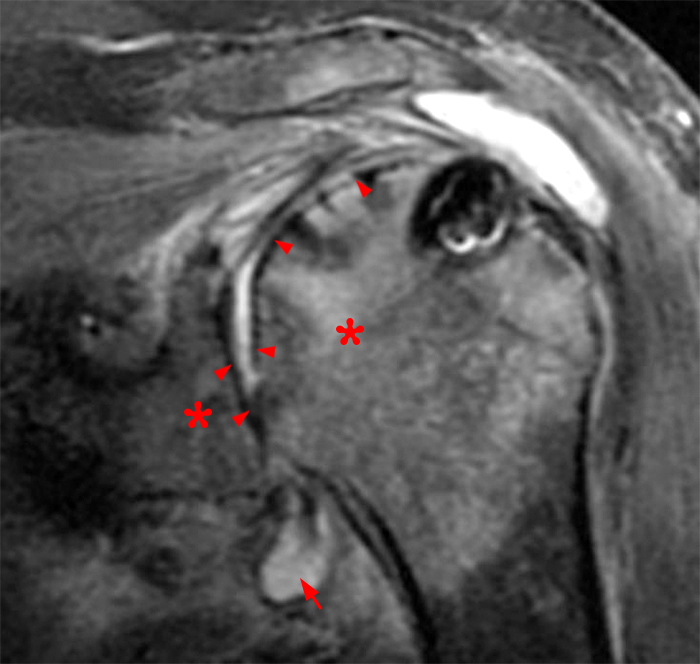
(3A) A 35 year-old male with chondrolysis 10 days after rotator cuff repair. The glenohumeral articular cartilage was normal on the preoperative MRI (not included). A coronal T2-weighted image of the shoulder with fat suppression shows extensive severe diffuse cartilage loss with bone-on-bone appearance (arrowheads) and diffuse marrow edema along both sides of the joint (asterisks). Synovitis is present in the axillary recess (short arrow). A subacromial-subdeltoid bursal fluid collection is also present. The joint was aspirated and septic arthritis was excluded.
Figure 4:
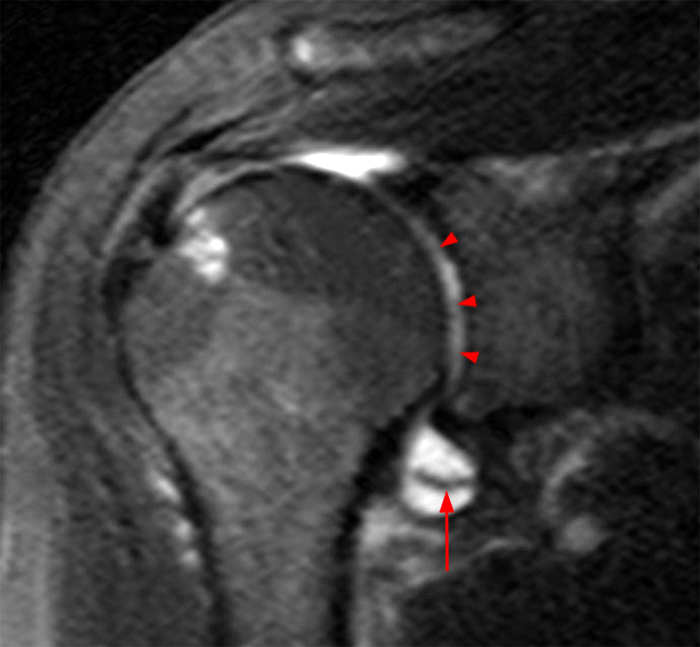
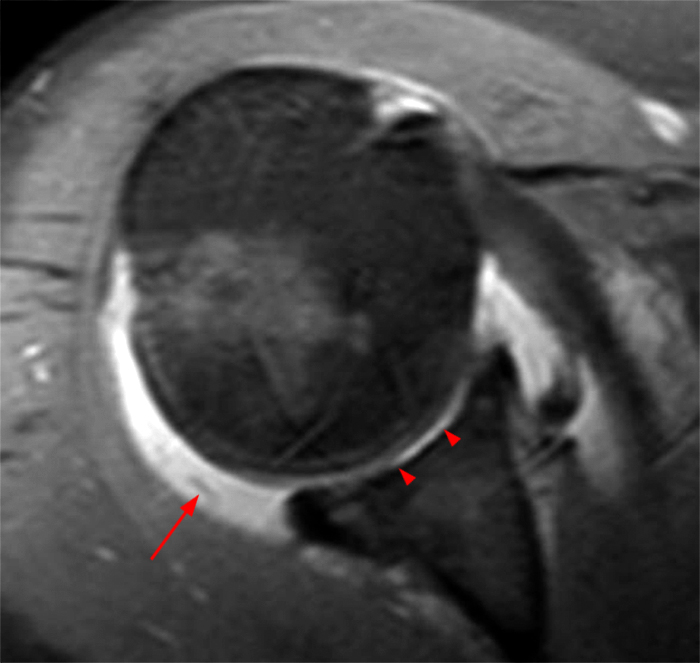
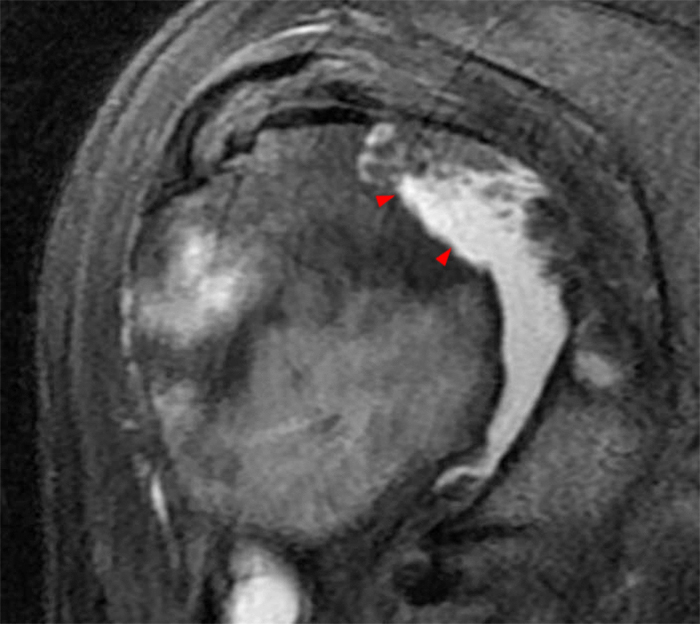
(4A) 55 year-old female with sharp right shoulder pain and decreased range of motion for 10 days. No known injury. (4A) A coronal T2-weighted image of the shoulder with fat suppression demonstrates diffuse cartilage loss of the glenoid (arrowheads) and a moderate sized joint effusion. A corresponding loose intraarticular chondral fragment is located in the axillary recess (arrow). There is no significant articular cartilage abnormality of the humeral head. (4B) An axial proton density-weighted image of the shoulder with fat suppression demonstrates the area of chondrolysis in the central glenoid (arrowheads), a joint effusion and a loose intraarticular body posterior to the humeral head (arrow).
Figure 5:
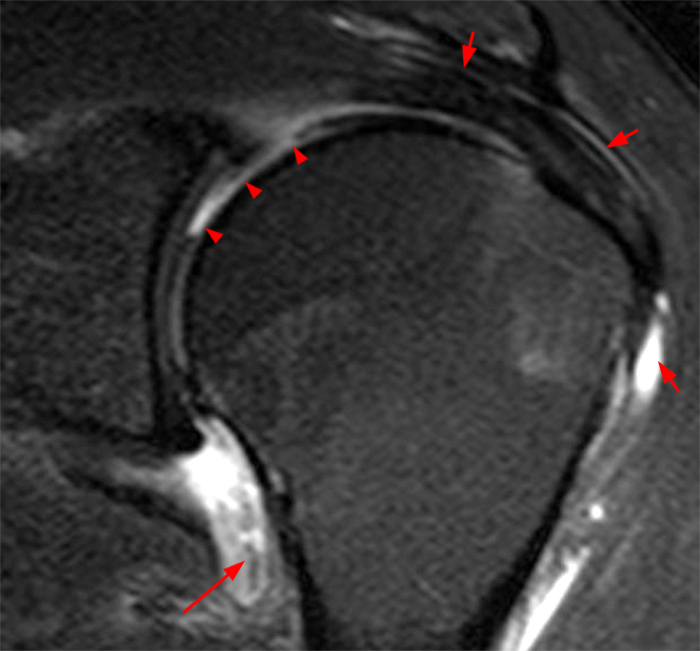
(5A) 50 year-old female who was injured 3 weeks prior to the MR study while working out. A coronal T2-weighted image of the shoulder with fat suppression reveals diffuse cartilage loss of the superomedial aspect of the humeral head (arrowheads). Several chondral fragments are located in the axillary recess (arrow). There is no articular cartilage abnormality identified at the glenoid. A subacromial subdeltoid bursal fluid collection and bursal thickening are also present (short arrows).
Differential Diagnosis on MRI
Septic arthritis after arthroscopy develops in less than 1 % of cases,9 but the findings on MRI may be identical to those in acute or subacute chondrolysis, with complete loss of articular cartilage and synovitis.10 When septic arthritis is suspected clinically, a diagnostic joint aspiration should be performed.
Extensive articular cartilage loss is a feature of untreated rheumatoid arthritis, and is often accompanied by subchondral cysts and erosions, and variable degrees of synovitis (MRI Web Clinic June 2016). Patients with rheumatoid arthritis are susceptible to septic arthritis, especially those that receive immunosuppressant therapy.11
Neuropathic arthropathy of the shoulder, a rare condition, with syringomyelia being the most common cause, has hypertrophic and atrophic forms.12 Imaging features include osteocartilaginous resorption, joint disorganization, large joint effusions, synovitis and intraarticular debris and loose bodies
Acute posttraumatic chondral delamination injury is a result from shearing stress to cartilage and leads to separation of the articular cartilage from the underlying subchondral bone.13 The cartilage defects are typically localized and not always associated with signal abnormalities of adjacent subchondral bone on MRI.
Figure 6:
(6A) A 26 year-old male with left shoulder pain for two weeks and septic arthritis. The joint was aspirated and cultures grew Fusibacterium nucleatum. A coronal T2-weighted image of the shoulder with fat suppression demonstrates diffuse glenohumeral cartilage loss with a bone-on- bone appearance (arrowheads), diffuse marrow edema, marginal erosions on the glenoid and humeral head (arrows), and extensive synovitis (asterisks).
Figure 7:
(7A) A 69 year-old male with a long history of rheumatoid arthritis. A coronal T2-weighted image of the shoulder with fat suppression demonstrates high grade loss of the articular cartilage of the glenohumeral joint with subchondral cyst formation and edema. Long standing inflammation has resulted in remodeling and loss of the subchondral bone which is more prominent in the glenoid. The osteophyte formation is mild and is out of proportion to the degree of chondromalacia, which is typical for synovial inflammatory disease.
Figure 8:
(8A) A 76 year-old female with severe degenerative changes of the cervical spine (not included) and long segment central canal stenosis which has resulted in neuropathic arthropathy. A fat-suppressed T2-weighted coronal image demonstrates severe diffuse glenohumeral chondromalacia with extensive subchondral bone resorption (arrowheads). A joint effusion, synovial thickening and intraarticular debris are also present.
Treatment
Non-operative measures, such as intra-articular steroids and hyaluronic acid, have had limited success in restoring function and decreasing pain in glenohumeral chondrolysis. Arthroscopic intervention such as debridement, chondroplasty and capsular release may result in improvement. Within a few years of the onset of symptoms, shoulder arthroplasty is often required.14,15 MRI may be useful for preoperative planning and decision-making in terms of what type of arthroplasty is needed (resurfacing arthroplasty, hemiarthroplasty, or total arthroplasty).
Conclusion
Glenohumeral chondrolysis is an uncommon entity with multifactorial etiologies, and may be seen after shoulder arthroscopy, intraarticular infusion of local anesthetics, use of radiofrequency devices, and placement of suture anchors and knots. The patients, who are often young, present with progressive pain, stiffness and limited function that develop over a period of months. The process should be differentiated from osteoarthritis, which typically requires years to develop. MRI is an effective tool to evaluate the extent of articular cartilage injury in cases of suspected chondrolysis.
References
- Bailie DS, Ellenbecker TS. Severe chondrolysis after shoulder arthroscopy: a case series. J Shoulder Elbow Surg. 2009 Sep-Oct;18(5). ↩
- Provencher MT, Navaie M, Solomon DJ, Smith JC, Romeo AA, Cole, BJ. Joint Chondrolysis. J Bone Joint Surg Am. 2011 Nov 2;93(21):2033-44. ↩
- Wiater BP, Neradilek MB, Polissar NL, Matsen FA 3rd. Risk factors for chondrolysis of the glenohumeral joint: a study of three hundred and seventy-five shoulder arthroscopic procedures in the practice of an individual community surgeon. J Bone Joint Surg Am. 2011 Apr 6;93(7):615-25. ↩
- Knudson W, Casey B, Kuettner K, et al. Hyaluronan oligosaccharides perturb cartilage matrix homeostasis and induce chondrocyte chondrolysis, Arthritis Rheum. 2000; 43:1165-1774. ↩
- Homandberg GA, Meyers R, Xie Fibronectin fragments cause chondrolysis of bovine articular cartilage slices in culture. J Biol Chem. 1992 Feb 25;267(6):3597-604. ↩
- Peterfy C, Kothari M. Imaging osteoarthritis: magnetic resonance imaging versus x-ray. Curr Rheumatol Rep. 2006 Feb;8(1):16-21. ↩
- Sanders TG, Zlatkin MB, Paruchuri NB, Higgins RW. Chondrolysis of the glenohumeral joint after arthroscopy: findings on radiography and low-field-strength MRI. Am J Roentgenol 2007 Apr;188(4):1094-8. ↩
- Laor, T, Crawford AH. Idiopathic chondrolysis of the hip in children: early MRI findings. Am J Roentgenolog.2009 Feb;192(2):526-31. ↩
- Kirchoff, C, Braunstein V, Paul J, Imhoff AB, Hinterwimmer S. Septic arthritis as a severe complication of elective arthroscopy: clinical management strategies. Patient Saf Surg. 2009; 3:6 ↩
- Karchevsky M, Schweitzer ME, Morrison WB, Parellada JA. MRI findings of septic arthritis and associated osteomyelitis in adults. Am J Roentgenol. 2004 Jan;182(1):119- 22. ↩
- Abdulaziz Al-Ahaideb. Septic arthritis in patients with rheumatoid arthritis. J Orthop Surg. 2008; 3:33. ↩
- Jones EA, Manaster BJ, May DA, Disler DG. Neuropathic osteoarthropathy: diagnostic dilemmas and differential diagnosis. Radiographics. 2000 Oct;20 Spec No: S279-93. ↩
- White CL, Chauvin NA, Waryasz GR, March BT, Francavilla ML. MRI of native knee cartilage delamination injuries. Am J Roentgenol 2017 Nov;209(5): W317-W321. ↩
- Levy JC, Virani NA, Frankle MA, Cuff D, Pupello DR, Hamelin JA. Young patients with shoulder chondrolysis following arthroscopic shoulder surgery treated with total shoulder arthroplasty. J Shoulder Elbow Surg. 2008 May-Jun;17(3):380-9. ↩
- Hasan SS, Fleckenstein CM. Glenohumeral chondrolysis: part II-result of treatment. Arthroscopy 2013 Jul;29(7):1142-8. ↩