Clinical History:
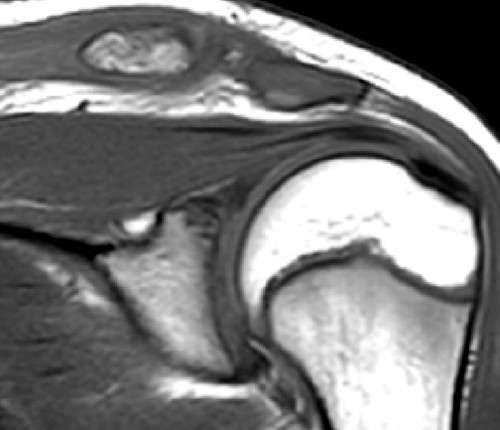
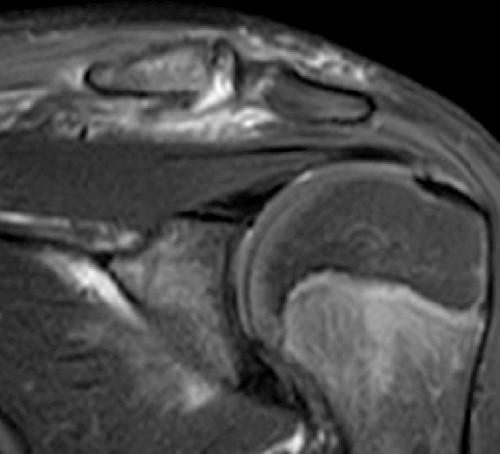
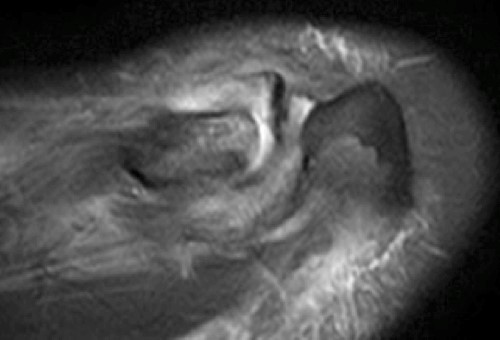
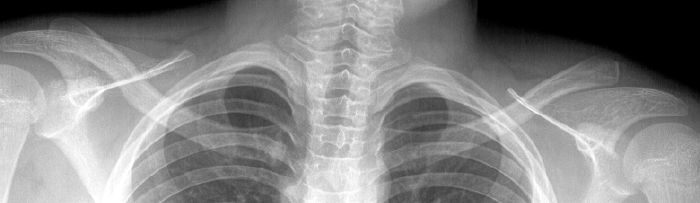
An 11 year-old boy presents with shoulder pain after a fall from a tree 4 days previously. T1-weighted (1a) and T2-weighted (1b) coronal oblique fat-suppressed images, and a fat-suppressed T2-weighted (1c) axial image through the left shoulder are provided. In addition, a frontal radiograph (1d) of both shoulder regions is included. What are the findings? What is your diagnosis?
Findings:
Figure 2:
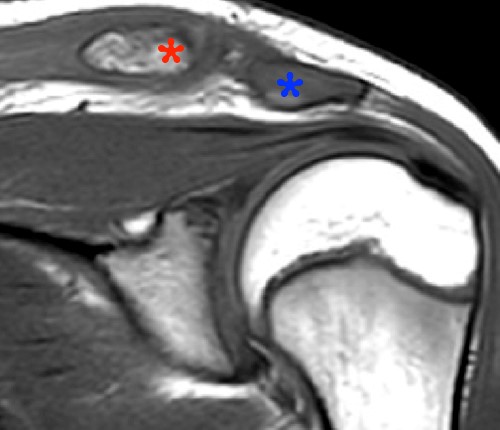
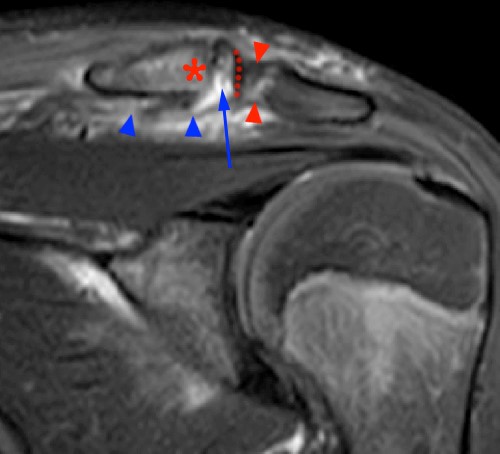
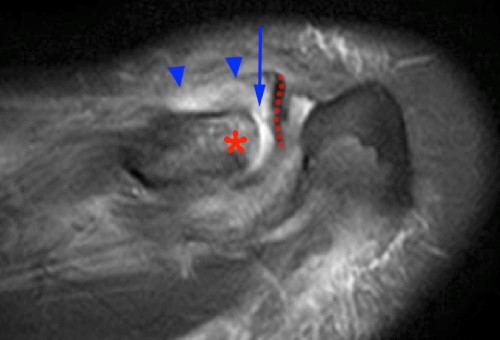
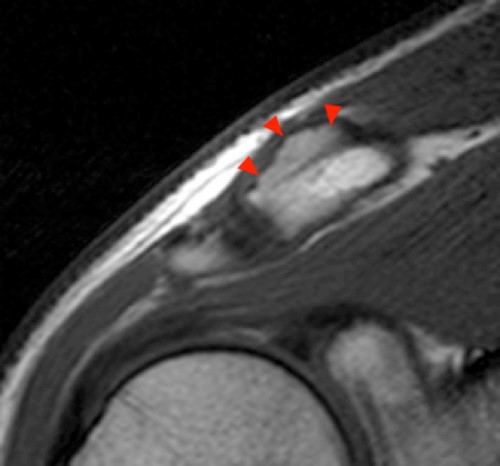
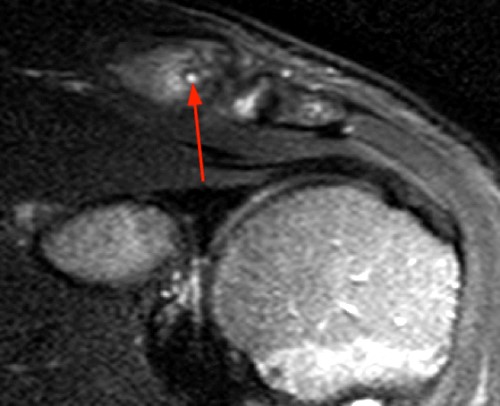
The (2a) T1-weighted coronal image reveals mild superior subluxation of the clavicle (red asterisk) with respect to the acromion (blue asterisk). The acromioclavicular ligaments are well demonstrated on the (2b) T2-weighted coronal oblique fat-suppressed image and are intact (red arrowheads). The zones of hyperintense and hypointense signal at the distal end of the clavicle on the (2b) T2-weighted coronal oblique and (2c) axial images (blue arrows) represent the site of metaphyseal-epiphyseal separation. The distal clavicular metaphysis (red asterisk) is superiorly (2b) and posteriorly (2c) displaced with respect to the epiphysis (dotted lines), which remains normally aligned with the acromion. The periosteal sleeve of the distal clavicle is thickened and has indistinct margins inferiorly (2b) and anteriorly (2c) (blue arrowheads). On the frontal radiograph there is a significant increase of the coracoclavicular distance (double arrow) on the left as compared to the uninvolved right side, indicating high grade injury of the coracoclavicular ligaments, which are not included on the MR images that are provided.
Diagnosis
Distal clavicular epiphyseal avulsion with periosteal sleeve injury.
Introduction
Injury to the acromioclavicular region in a child is much more likely to result in a fracture of the growth plate of the distal clavicle than a true acromioclavicular joint separation, because of anatomical factors that are unique to children.1,2
The false appearance of a joint dislocation on radiographs is related to the small and unossified epiphysis of the distal clavicle, which maintains its normal relationship to the acromioclavicular joint, while the distal metaphysis is superiorly displaced through a tear of the surrounding periosteal sleeve.3,4
The developmental anatomy and different patterns of injury will be discussed with emphasis on MR imaging.
Epidemiology and clinical presentation
The mechanism of acromioclavicular (AC) injury is a fall onto the shoulder or a direct blow, and has been described in detail, along with the Rockwood classification system, in the Radsource Web Clinic April 2010. Sports activities that are commonly associated with injuries to the AC region in children and teenagers include football, ice hockey, snowboarding, biking and wrestling. The patient typically presents with pain and tenderness over the superior aspect of the shoulder. A focal deformity and tenting of the skin may be present in a displaced injury. Only about 10 % of clavicular fractures involve the lateral aspect, and have been classified by Dameron and Rockwood, with type I being a nondisplaced extraarticular fracture, type II, a displaced extraarticular fracture, and type III, a fracture extending into the acromioclavicular joint.1
Developmental anatomy of the distal clavicle and its implications in traumatic injury
The development of the distal clavicle has been thoroughly studied with MRI, which allows visualization of non-ossified cartilage and secondary ossification centers.5
In young children (<5 years), the cartilaginous clavicle is relatively large and the primary ossification center of the clavicle has a smooth margin at the chondro-osseous junction. With increasing age (10-14-years), the cartilaginous lateral portion of the clavicle becomes smaller, and in older teenagers, the zone of non-mineralization of the clavicle is very thin and blends in with articular cartilage on MR imaging (Figure 3). Complete lateral advancement of the chondro-osseous junction occurs at the age of about 18 years.
Secondary ossification centers of the distal clavicle are uncommon (<10%), but can appear as early as 11 years. When these centers are present they typically appear at the age of 19-20 years and fuse with the diaphyseal portion within a few months.
The periosteal layer in skeletally immature individuals is quite thick, surrounds the clavicle in a sleeve-like fashion, and is firmly adherent, along with the AC ligaments, to the perichondrium at the epiphysis. Distal clavicular fractures, typically at the physeal-metaphyseal junction in children and teenagers, are frequently associated with a longitudinal tear in the periosteum, through which an ossified distal clavicular metaphysis can herniate (Figure 4). The epiphysis of the distal clavicle remains aligned with the AC joint, but is radiolucent, which gives the radiographic appearance of AC separation; hence, the terms “pseudodislocation” and “childhood and adolescent analogue of AC separation”, have been coined.6
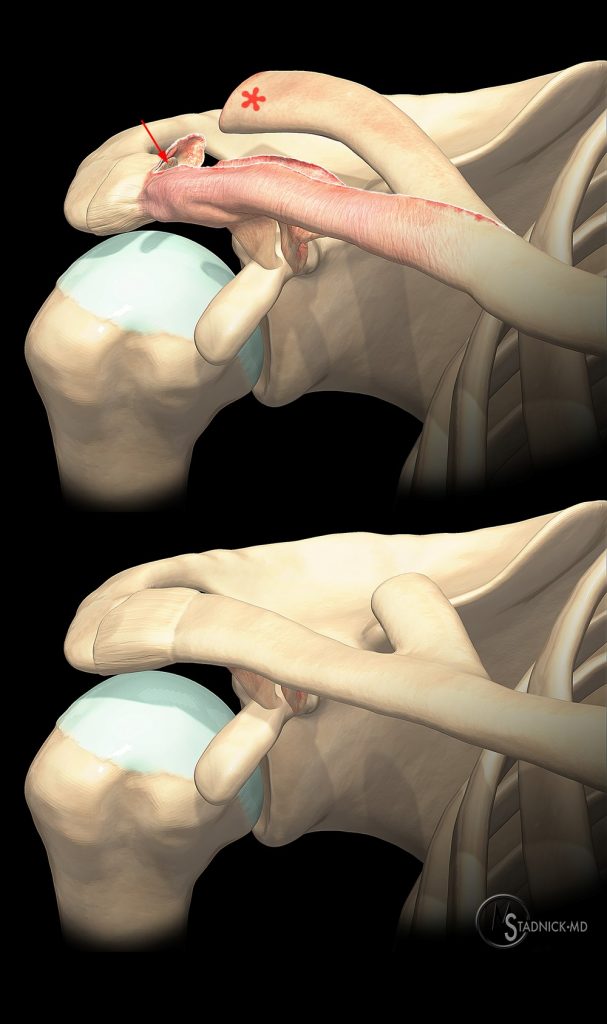
Figure 4:
This 3D representation of a “pseudodislocation” demonstrates separation of the metaphysis (asterisk) and epiphysis (arrow) of the distal clavicle with posterior displacement of the metaphysis through the torn periosteum (above). If not reduced, ossification of the periosteum and remodeling of the displaced metaphysis results in chronic clavicular deformity (below).
The injured periosteal sleeve has strong osteogenic properties, which will result in bone formation and, occasionally, in significant chronic deformity between the periosteum and the clavicular metaphysis.
MRI findings of the analogue of AC joint injury in skeletally immature patients
The role of MR imaging in the evaluation of pediatric AC joint injuries has not been delineated, but because of its superior ability to visualize non-mineralized cartilage, ossification centers, and ligamentous structures it can add important information in selected cases to guide therapy. Despite the distal clavicular physis being very small, metaphyseal-epiphyseal separation type injuries are well demonstrated on MRI (Figure 5). In displaced epiphyseal avulsion injuries, the relationship of the clavicle to the periosteal sleeve and trapezius muscle can be depicted with MRI (Figure 6a), which may be helpful prior to closed or open reduction. In addition, MRI may be more useful than radiographs in the evaluation of acromioclavicular (AC) and coracoclavicular (CC) ligaments (Figure 6b), because the radiographic assessment is performed with weights fastened to the patient’s wrist, which may not be well tolerated in the pediatric patient population. Before the advent of MRI it was thought that the CC ligaments would remain intact even in the more severe cases, however these ligaments are sometimes avulsed along with the periosteal sleeve. MR imaging also offers the advantage of evaluating adjacent structures, such as the glenoid labrum and rotator cuff.
Imaging findings in chronic injury to the AC region in skeletally immature patients include enlargement or a duplicated appearance of the distal clavicle (Figure 7), which is a result of the marked osteogenic capability of the periosteal sleeve.6 Chronic AC joint injury can also manifest itself as small T2 hyperintense foci in the distal clavicle (Figure 8), most likely representing displacement of physeal cartilage into the metaphysis, which should not be misdiagnosed as subchondral cyst formation and chronic arthritis.
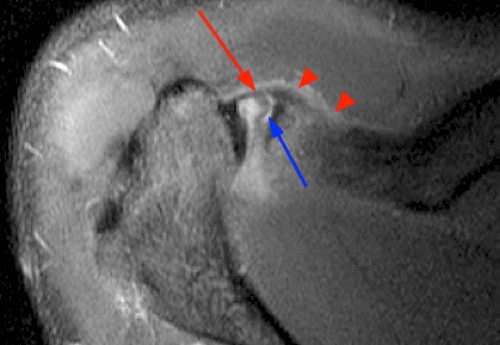
Figure 5:
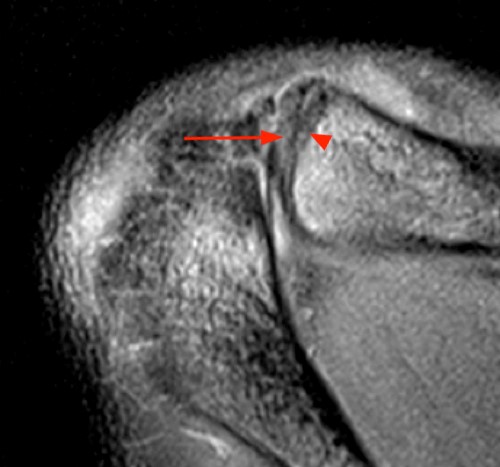
A T2-weighted axial image of the acromioclavicular joint in a 19 year-old male with recent snowboarding injury shows a nondisplaced epiphyseal avulsion (blue arrow) of the distal clavicle with mild diffuse periosteal edema (arrowheads). The portion of the AC ligaments that is included is intact and is attached to the perichondrium at the epiphysis (red arrow).
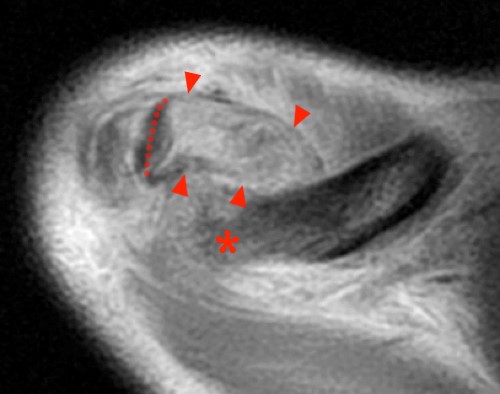
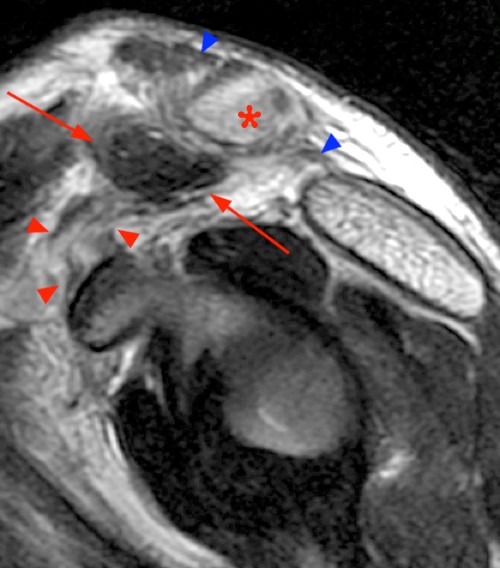
Figure 6:
6a: A T2-weighted axial image of the acromioclavicular joint in a 14 year-old male with recent snowboarding injury demonstrates extensive periosteal sleeve disruption (arrow heads) and posterior displacement of the distal clavicle (asterisk) through the periosteum. The distal clavicle epiphysis (dotted lines) is not displaced from the AC joint.
6b: A corresponding T2-weighted sagittal image of the shoulder reveals complete avulsion of the CC ligaments (red arrowheads) along with the periosteal sleeve (arrows) of the distal clavicle. The coracoclavicular distance is increased and the distal clavicle (asterisk) is elevated with respect to the acromion, and buttonholed through the fibers of the trapezius muscle (blue arrowheads).
Figure 8:
Coronal T2-weighted image of the shoulder in an 18 year-old male with football related injury 4 months previously. Mild diffuse edema and a small focus of hyperintense signal (arrow) in the distal clavicle consistent with old epiphyseal avulsion injury and displacement of growth cartilage into the metaphysis.
Treatment
Considering the impressive osseous remodeling capability of the distal clavicle in skeletally immature patients, most of these injuries should be treated non-surgically, with simple immobilization.7
A report describes successful closed reduction of a superiorly displaced, buttonholed clavicle in a 13 year-old patient.8
Significantly displaced fractures may however require open reduction and internal fixation, and have been reported with good or excellent results,9 which is not surprising in the presence of the osteogenic periosteal sleeve and the intact AC joint in these injuries.
Conclusion
A distal clavicular epiphyseal injury can result in a false appearance of a dislocation at the AC joint on radiographs, based on the non-ossified distal epiphysis and a periosteal sleeve tear, which allows the distal clavicular metaphysis to be displaced upward. MRI allows understanding of the pattern of injuries in the AC region in the skeletally immature patients and is useful in diagnosing additional abnormalities, such as tears of the CC ligaments and the trapezius muscle. The majority of patients with distal clavicular epiphyseal injury can be treated non-operatively with good results. In selected cases, MRI may be helpful for preoperative guidance.
References
- Dameron TB, Jr, Rockwood CA. Fractures and dislocations of the shoulder. In: Rockwood CA, Wilkins KE, King RE, eds. Fractures in Children. Philadelphia: Lippincott, 1984: 577-682. ↩
- Black GB, McPherson JA, Reed MH. Traumatic pseudodislocation of the acromioclavicular joint in children: a fifteen year review. The American Journal of sports medicine 1991 Dec; 19(6):644-6. ↩
- Todd TW, D’Errico J. The clavicular epiphyses. Developmental Dynamics, 1928 Mar 1;41(1):25-50. ↩
- Rockwood CA. Fracture of the outer clavicle in children and adults. Abstract. J Bone Joint Surg 1982, 64B:642. ↩
- Kothary P, Rosenberg ZS. Skeletal developmental patterns in the acromial process and distal clavicle as observed by MRI. Skeletal radiology 2015 Feb 1; 44(2): 207-15. ↩
- Ogden JA. Distal clavicular physeal injury. Clinical orthopaedics and related research. 1984 Sep 1; 188:68-73. ↩
- Sanders JO, Rockwood CA, Curtis RJ. Fractures and dislocations of the humeral head and shoulder. In: Rockwood CA, Wilkins KE, Beaty JH, eds. Fractures in Children. Philadelphia: Lippincott, 1991; 970-977. ↩
- Richards, DP, Howard A. Distal clavicle fracture mimicking type IV acromioclavicular joint injury in the skeletally immature athlete. Clinical Journal of Sports Medicine 2001 Jan 1;11(1):57-9. ↩
- Eidman DK, Siff SJ, Tullos HS. Acromioclavicular lesions in children. The American journal of sports medicine. 1981 Jun 1; 9(3):150-4. ↩