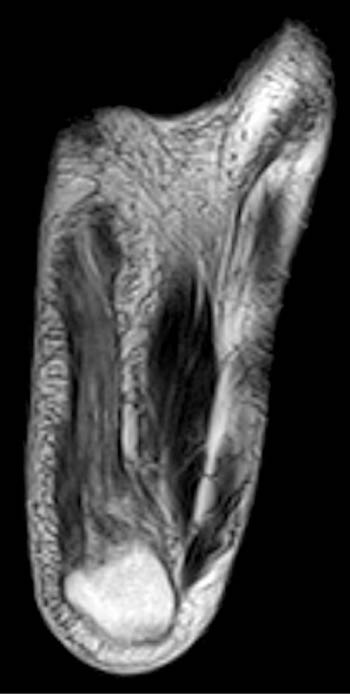
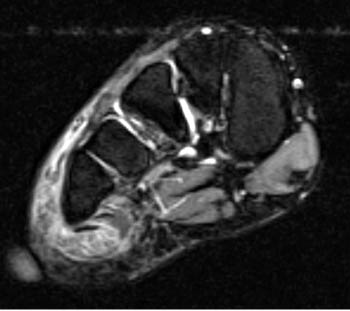
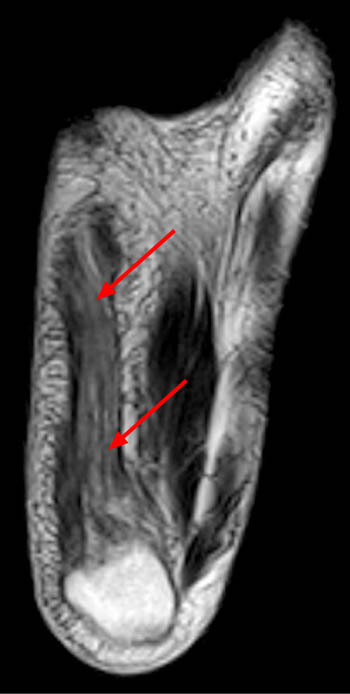
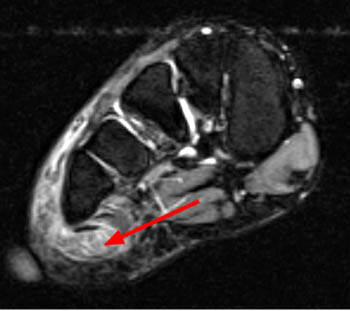
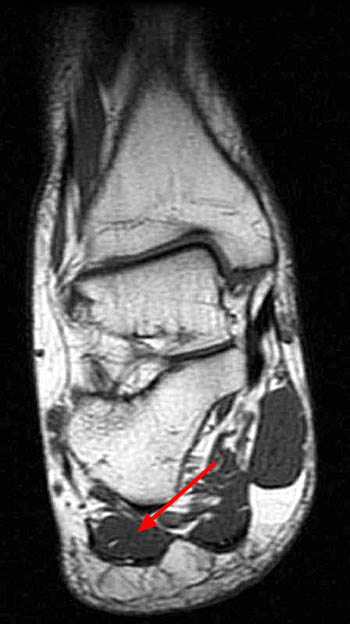
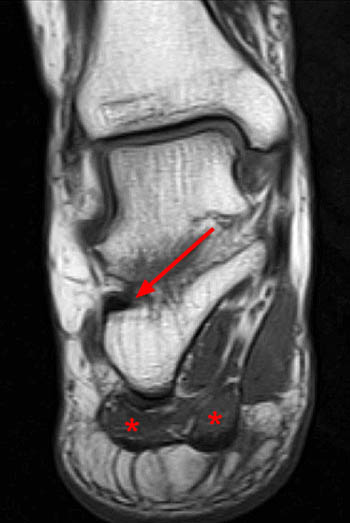
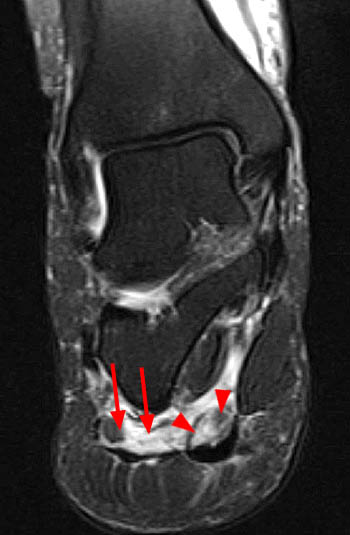
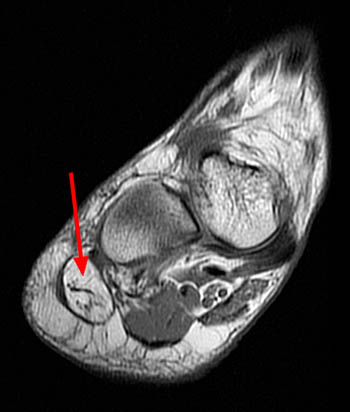
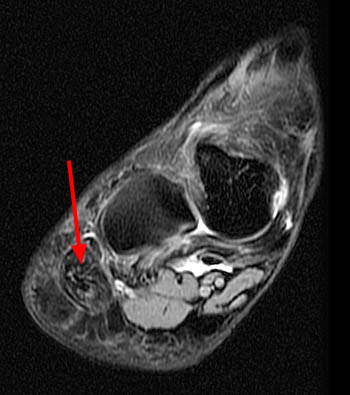
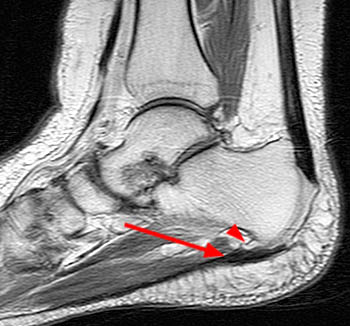
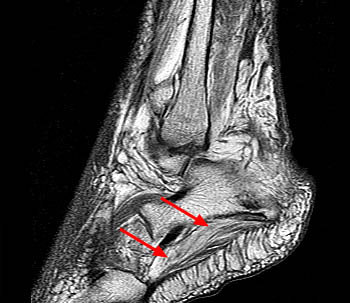
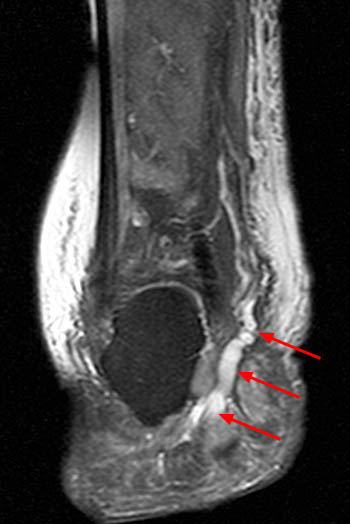
Clinical history: A 26 year-old female presents with lateral foot pain and no prior trauma. Axial T2-weighted (1a) and coronal STIR (1b) images are provided. What are the findings? What is your diagnosis?
Findings
Diagnosis
Baxter’s nerve (first branch of the lateral plantar nerve) impingement.
Introduction
Heel pain is a common presenting complaint to the foot and ankle specialist, with a wide differential diagnosis including plantar fasciitis, fat pad atrophy, calcaneal stress fracture or apophysitis, inflammatory arthropathy, neoplasia, and infection1. One of the more elusive diagnostic considerations in heel pain is entrapment of first branch of the lateral plantar nerve (Baxter’s nerve impingement)2,3. Baxter’s nerve is a mixed sensory and motor nerve, providing motor innervation to the abductor digiti minimi (ADM) muscle2,4,5. Baxter’s nerve impingement can produce symptoms indistinguishable from plantar fasciitis6,7,8,9. While this diagnosis has been said to account for up to 20% of heel pain, it is often overlooked relative to other causes of heel pain8,10,11. Weakness of the ADM may be present but is difficult to detect clinically9. Electrodiagnostic studies are invasive and the results in heel pain can be inconclusive9,13,14. MR can be used to detect denervation-related muscle changes in the ADM, confirming the diagnosis of Baxter’s nerve impingement3,6,8,9,12.
Anatomy
Within the ankle tarsal tunnel, the posterior tibial nerve (PTN) bifurcates into medial (MPN) and lateral (LPN) plantar nerves. These nerves exit the tarsal tunnel and continue along the plantar aspect of the foot.
The MPN travels anterior to the LPN, carrying sensory information from the medial two thirds of the plantar foot, and motor innervation to the flexor digitorum brevis, abductor hallucis, flexor hallucis brevis, and first lumbrical9.
The LPN carries sensory information from the lateral plantar aspect of the foot, 5th toe, and lateral half of the 4th toe. Motor innervation involves all the remaining foot muscles, not innervated by the MPN9.
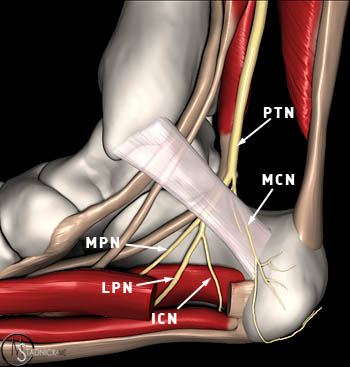
Figure 3:
Medial view of the ankle with the abductor hallucis partially removed depicting the posterior tibial nerve (PTN) branches. After giving off a small medial calcaneal nerve branch (MCN), the PTN bifurcates into the medial (MPN) and lateral (LPN) plantar nerves within the tarsal tunnel. The first branch of the LPN is Baxter's nerve also known as the inferior calcaneal nerve (ICN).
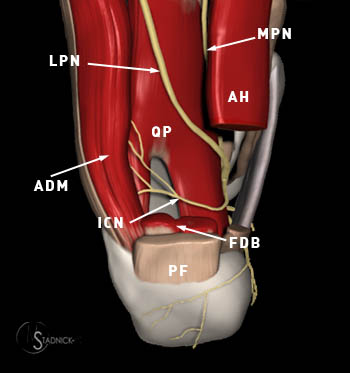
Figure 5:
Graphic representation of the plantar aspect of the hindfoot with the plantar fascia (PF), flexor digitorum brevis muscle (FDB), and abductor hallucis muscle (AH) partially resected reveals the plantar course of the medial plantar nerve (MPN) and lateral plantar nerve (LPN). The first branch of the LPN is Baxter's nerve (also known as the inferior calcaneal nerve) (ICN), provides motor innervation to the abductor digiti mini muscle (ADM). The quadratus plantae muscle (QP) is also indicated.
The first branch of the LPN, Baxter’s nerve (also known as the inferior calcaneal nerve), originates from the LPN at various levels beneath the deep fascia of the abductor hallucis muscle. The nerve courses vertically between the abductor hallucis and quadratus plantae muscles, then makes a sharp 90 degree horizontal turn, coursing laterally beneath the calcaneus to innervate the ADM muscle3,5,9,15. Motor innervation supplies the ADM, occasionally to the flexor digitorum brevis and lateral half of the quadratus plantae. Sensory information is carried from the calcaneal periosteum, long plantar ligament, and adjacent vessels3,4,6. While Baxter’s nerve is usually the first branch of the LPN, variation does exist and the nerve can originate directly from the PTN5,14,16.
Pathology
Two sites of entrapment have been described with Baxter’s nerve impingement. The first site is located as the nerve passes between the deep fascia of the abductor hallucis muscle and the medial plantar margin of the quadratus plantae muscle. The second site is more distally as the nerve passes along the anterior aspect of the medial calcaneal tuberosity2,3,14. A calcaneal plantar enthesophyte3,8 and/or soft tissue changes of plantar fasciitis9 may also contribute to entrapment at this second location.
Similar to entrapment neuropathies elsewhere, resultant effects from nerve compression depend on the severity and chronicity of entrapment. Early diagnosis of a nerve compression syndrome may result in reversible damage, whereas late diagnosis nerve compression damage is not typically reversible17. With motor nerve injuries, skeletal muscle will become edematous in the acute to subacute phases. Left untreated, denervated muscle will eventually undergo volumetric atrophy, ultimately with irreversible fatty infiltration. If dual or redundant innervation exists, these changes may not occur18,19.
Reported risk factors for Baxter’s nerve impingement include advancing age, the presence of a calcaneal spur, plantar fasciitis, underlying mass, vascular enlargement, muscular enlargement (such as in athletes), obesity, and foot hyperpronation3,8,9,20.
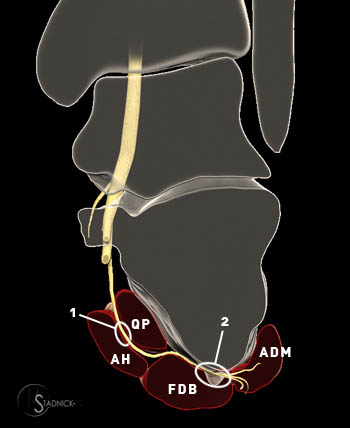
Figure 6:
Two potential sites of Baxter's nerve entrapment:
1. As the nerve passes between the deep fascia of the abductor hallucis muscle (AH)and the medial plantar margin of the quadratus plantae muscle (QP).
2. More distally as the nerve passes along the anterior aspect of the medial calcaneal tuberosity where plantar calcaneal enthesophytes and plantar fasciitis may contribute to entrapment.
Imaging
MRI has been shown to be extremely valuable in demonstrating muscular changes associated with denervation. MRI is more sensitive to tissue changes within muscle compared to ultrasound or computed tomography and has advantages compared to electrodiagnostic studies due to its non-invasive nature, superior anatomic detail, ability to demonstrate pathology in muscles with dual innervation18, and ability to exclude alternative diagnoses (fracture, neoplasia, fasciitis). Normal muscle demonstrates intermediate signal on T1 and fluid sensitive sequences.
Acute and subacutely muscle denervation is best evaluated with fluid sensitive sequences, such as T2-weighted imaging with fat suppression (T2FS) or short tau inversion recovery (STIR) images, exhibiting increased signal within the muscle belly compared to normal muscle, related to neurogenic muscular edema18,19. Gadolinium enhancement within muscle will also occur in the acute to subacute phases of denervation18. In the setting of Baxter’s nerve impingement, muscular edema will occur selectively within the ADM, and potentially within the flexor digitorum brevis and quadratus plantae, depending on the innervation anatomy of the patient.
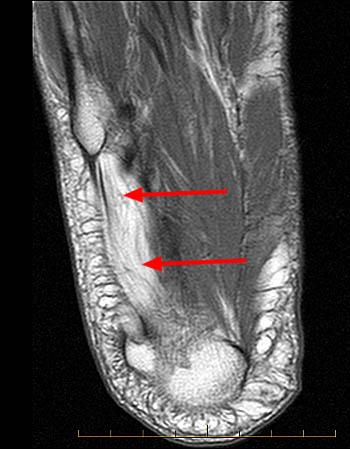
Figure 8:
Coronal T1 (8a) and Coronal T2 fat-suppressed (8b) images of the ankle. On the T2-weighted view, edema is noted within the ADM (arrows) and flexor digitorum brevis (arrowheads) muscle bellies compatible with subacute denervation injury. Muscle edema demonstrates bright T2 signal but is isointense to skeletal muscle on the T1 weighted image. No atrophy is present.
Chronically denervated muscle will eventually undergo volumetric atrophy, and subsequent irreversible fatty infiltration. These findings are best depicted on non-fat-suppressed T1-weighted images18,19. Typically, the atrophy and fatty infiltration occurs homogeneously within the muscle belly. If dual or redundant innervation exists, these changes may not occur or may occur heterogeneously18. In the case of Baxter’s nerve impingement, the ADM is typically involved homogeneously, unless dual innervation exists.
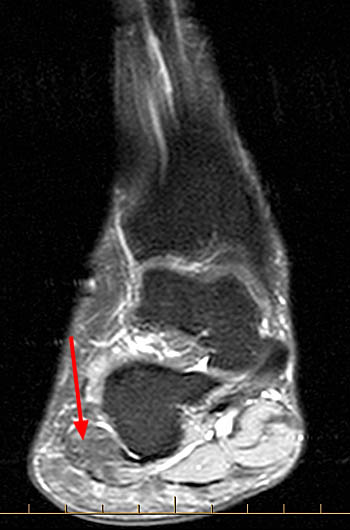
Figure 10:
Coronal T1 (10a) and coronal proton density-weighted (10b) images of the ankle in a patient with severe atrophy and fatty infiltration selectively involving the ADM due to chronic Baxter's nerve impingement. Note the signal intensity of the ADM (arrows) is similar to that of adjacent subcutaneous fat, with no significant edema.
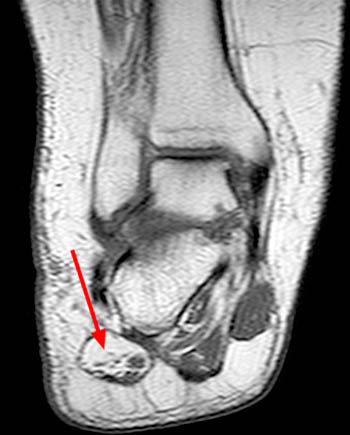
Figure 12:
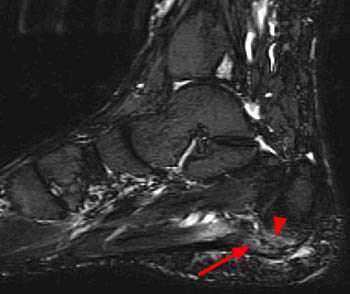
Coronal T1 (12a) and Sagittal T1 (12b) in a patient with chronic Baxter's nerve impingement. Figure 12a demonstrates moderate to severe atrophy and fatty infiltration of the ADM (arrow). Figure 12b demonstrates associated chronic plantar fasciitis (arrow) and a prominent plantar calcaneal enthesophytic spur (arrowhead).
Figure 13:
Sagittal T1-weighted (13a) and Coronal proton density-weighted fat-suppressed (13b) images. The patient had selective atrophy and severe fatty infiltration of the ADM (arrow, 13a). Prominently engorged veins were present in the tarsal tunnel (arrows, 13b), extending to the plantar medial aspect of the calcaneus, along the expected course of Baxter's nerve, presumably contributing to Baxter's nerve impingement.
Management
Initial treatment strategy of Baxter’s nerve entrapment is conservative, typically involving a combination of rest, non-steroidal anti-inflammatory medicines, corticosteroid injections, and orthotics1,21,22. If recalcitrant pain exists despite conservative treatment, operative intervention has proven successful1,21,23,24. Neurolysis of Baxter’s nerve is performed with deep fascia release of the abductor hallucis muscle. An impinging heel spur or tight plantar fascia is also partially removed or released, if it is associated with the entrapment2. Endoscopic approaches to the surgery11 and radiofrequency ablation techniques22 have also been described. The first patient above (Figures 1a,1b), underwent decompression of the tarsal tunnel in conjunction with Baxter’s nerve release, completely resolving her lateral foot pain.
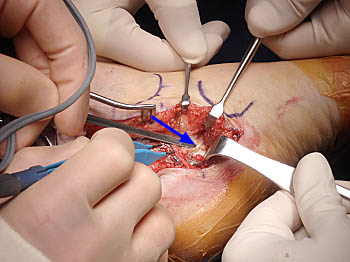
Figure 14:
Intraoperative photo demonstrating decompression of the tarsal tunnel in conjunction with Baxter's nerve release. The abductor hallucis muscle is pulled plantarly (with the large retractor) exposing the deep fascia of the muscle. The deep fascia of the abductor hallucis muscle (arrow) is in the process of being released in an act to decompress the lateral plantar nerve and branches. Photo courtesy of Shane York, DPM.
Conclusion
Baxter’s nerve impingement is a difficult clinical diagnosis and often overlooked in the presentation of heel pain. MRI can be used to evaluate for denervation effects of Baxter’s nerve impingement by identifying abnormalities of the ADM muscle belly. In addition, potential causes of impingement (e.g. calcaneal spur, soft tissue mass, enlarged vessels) and associated pathology (e.g. plantar fasciitis, tendon pathology) may be seen, and alternative differential diagnoses (e.g. stress fracture) can be excluded.
References
1 Thomas JL, Christensen JC, Kravitz SR, Mendicino RW, Schuberth JM, Vanore JV, Weil LS Sr, Zlotoff HJ, Bouche R, Baker J, American College of Foot and Ankle Surgeons heel pain committee. The diagnosis and treatment of heel pain: a clinical practice guideline-revision 2010. J Foot Ankle Surg 2010; 49(3 Suppl):S1-19.
2 Baxter DE, Thigpen CM. Heel pain: operative results. Foot Ankle 1989; 5:16-25.
3 Recht MP, Groof P, Ilaslan H, Recht HS, Sferra J, Donley BG. Selective Atrophy of the Abductor Digiti Quinti: An MRI Study. AJR 2007; 189:123-127.
4 Rondhuis JJ, Huson A. The first branch of the lateral plantar nerve and heel pain. Acta Morphol Neerl Scand 1986; 24:269-279.
5 Del Sol M, Olave E, Gsabrielli C, Mandiola E, Prates JC. Innervation of the abductor digiti minimi muscle of the human foot: anatomical basis of the entrapment of the abductor digiti minimi nerve. Surg Radiol Anat 2002; 24:18-22.
6 Delfaut EM, Demondion X, Bieganski A, Thiron MC, Mestdagh H, Cotten A. Imaging of foot and ankle nerve entrapment syndromes: from well-demonstrated to unfamiliar sites. Radiographics. 2003; 23:613-623.
7 Oztuna V, Ozge A, Eskandari MM, Colak M, Golpinar A, Kuyurtar F. Nerve entrapment in painful heel syndrome. Foot Ankle Int 2002; 23: 208-211.
8 Chundru U, Liebeskind A, Seidelmann F, Fogel J, Franklin P, Beltran J. Plantar fasciitis and calcaneal spur formation are associated with abductor digiti minimi atrophy on MRI of the foot. Skeletal Radiol. 2008; 37:505-10.
9 Donovan A, Rosenberg ZS, Cavalcanti CF. MR imaging of entrapment neuropathies of the lower extremity. Part 2. The knee, leg, ankle, and foot. Radiographics. 2010; 30:1001-1019.
10 Baxter DE. Release of the nerve to the abductor digiti minimi. In: Kitaoka HB, ed. Master techniques in orthopaedic surgery of the foot and ankle. Philadelphia, PA: Lippincott Williams and Wilkins; 2002: 359.
11 Lui, TH. Endoscopic decompression of the first branch of the lateral plantar nerve. Arch Orthop Trauma Surg 2007; 127:859-61.
12 Stanczak JD, McLean VA, Yao L. Atrophy of the abductor minimi muscle: marker of neuropathic heel pain syndrome. (abstr) Radiology 2001; 221(P): 522.
13 Schon LC, Glennon TC, Baxter DE. Heel pain syndrome: electrodiagnostic support for nerve entrapment. Foot Ankle 1993; 14:129-135.
14 Alshami AM, Souvlis T, Coppieters MW. A review of plantar heel pain of neural origin: differential diagnosis and management. Manual Therapy 2008; 13:103-111.
15 Louisia S, Masquelet AC. The medial and inferior calcaneal nerves: an anatomic study. Surg Radiol Anat 1999; 21:169-173.
16 Govsa F, Bilge O, Ozer A. Variations in the origin of the medial and inferior calcaneal nerves. Arch Orthop Trauma Surg 2006; 126:6-14.
17 Hochman MG, Zilberfarb JL. Nerves in a pinch: imaging of nerve compression syndromes. Radiol Clin North Am. 2004; 42:221-245.
18 Kim SJ, Hong SH, Jun WS, et al. MR imaging mapping of skeletal muscle denervation in entrapment and compressive neuropathies. Radiographics. 2011; 31:319-32.
19 Fleckenstein JL, Watumull D, Conner KE, et al. Denervated human skeletal muscle: MR imaging evaluation. Radiology. 1993; 187:213-8.
20 Henricson AS, Westlin NE. Chronic calcaneal pain in athletes: entrapment of the calcaneal nerve? Am J Sports Med 1984; 12:152-154.
21 Baxter DE, Pfeffer GB. Treatment of chronic heel pain by surgical release of the first branch of the lateral plantar nerve. Clin Orthop 1992; 279:229-236.
22 Cozzarelli J, Sollitto RJ, Thapar J, Caponigro J. A 12-Year Long-Term Retrospective Analysis of the Use of Radiofrequency Nerve Ablation for the Treatment of Neurogenic Heel Pain. Foot Ankle Spec; 2010 3:338-346.
23 Mesmar M, Amarin Z, Shatnawi N, Bashaireh K. Chronic heel pain due to the entrapment of the first branch of the lateral plantar nerve: analysis of surgical treatment. Eur J Orthop Surg Traumatol 2010; 20:563-567.
24 Goecker RM, Banks AS. Analysis of release of the first branch of the lateral plantar nerve J Am Podiatr Med Assoc 2000; 90:281-286.