Case 1
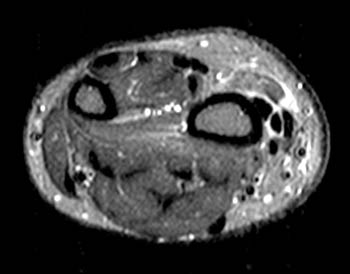
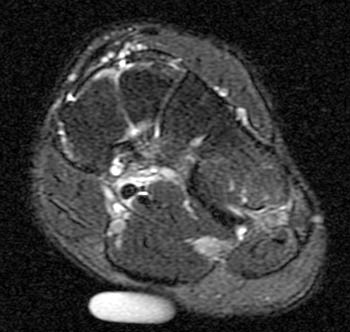
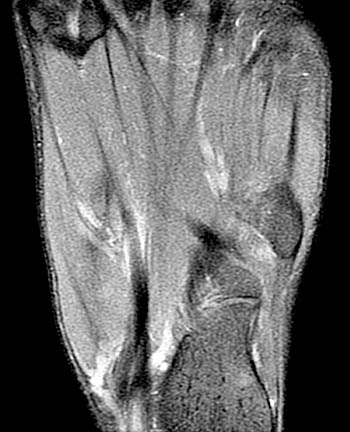
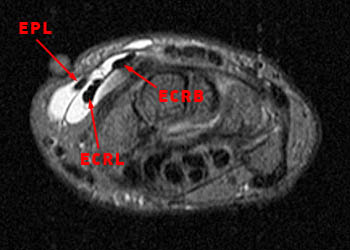
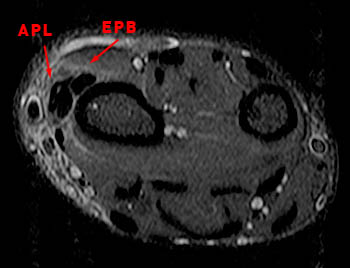
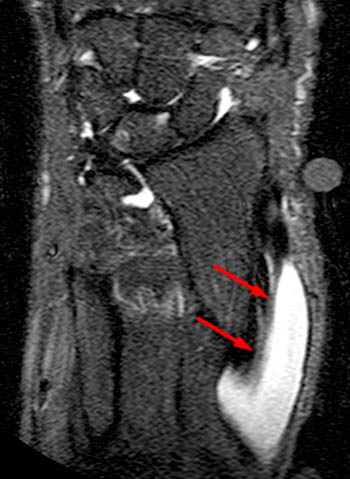
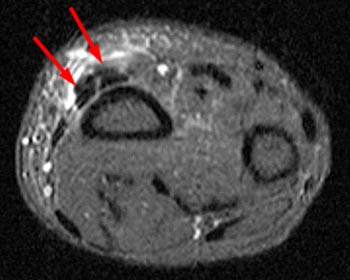
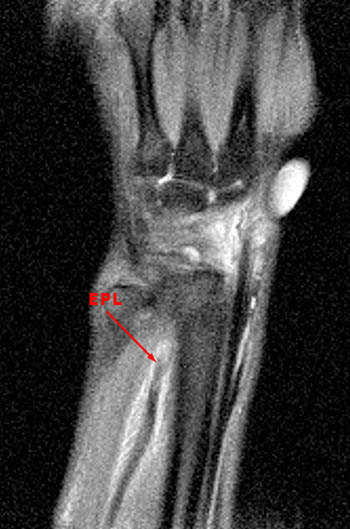
A 43 year old female presents with radial side forearm pain after working in her garden for several days. MRI was obtained with axial fat-suppressed fast spin-echo T2-weighted (1a) and coronal inversion recovery-weighted (1b) images.
Case 2
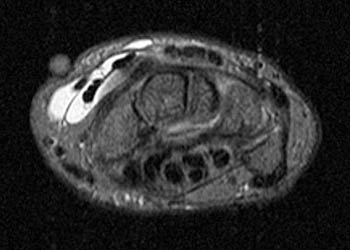
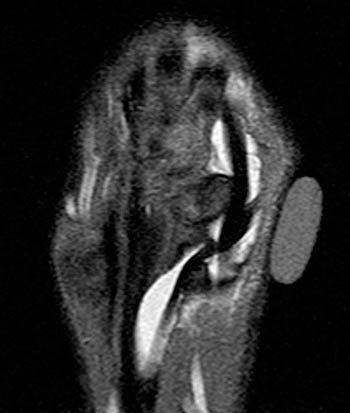
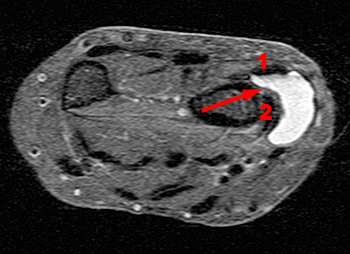
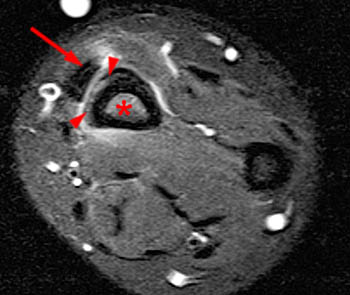
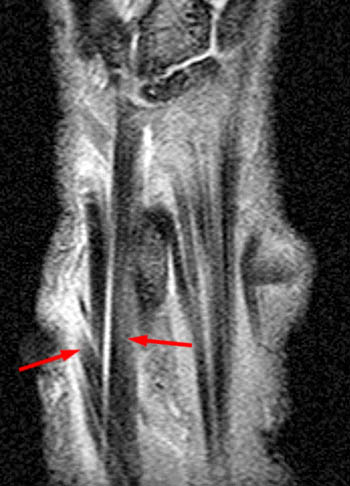
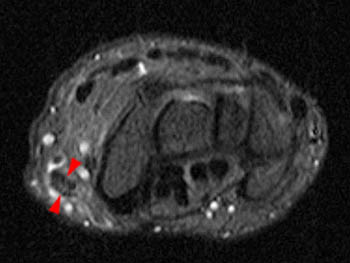
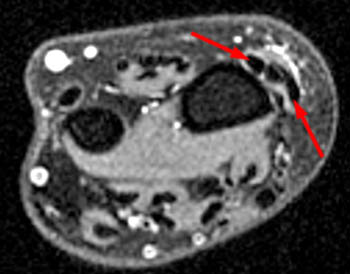
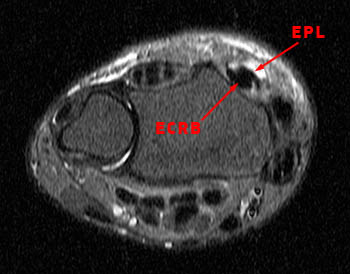
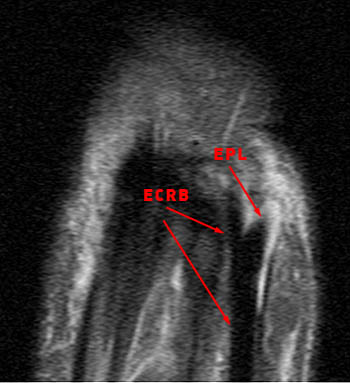
A 60 year old female returned from a week long ski vacation with a tender palpable mass over the dorsal wrist. She does not recall any specific wrist injury during the trip. MRI was obtained with axial (2a) and coronal (2b) inversion recovery-weighted images.
Case 3
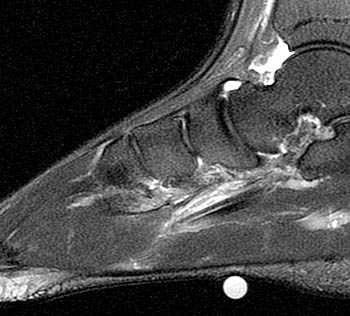
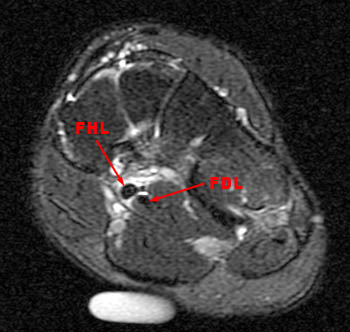
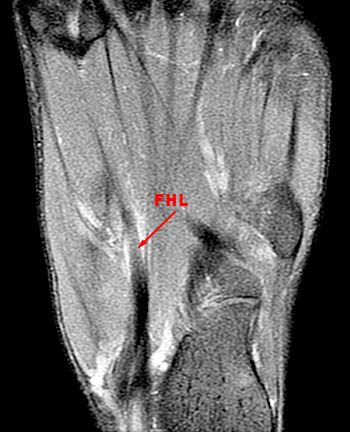
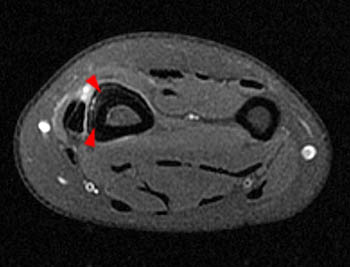
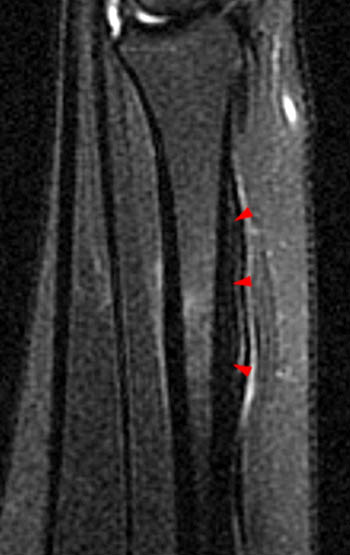
A 20 year old male runner developed plantar midfoot pain while training for a marathon. MRI was obtained with sagittal fat-suppressed fast spin-echo T2-weighted (3a), coronal inversion recovery-weighted (3b), and axial fat-suppressed fast spin-echo proton density-weighted (3c) images.
What are the findings? What is your diagnosis? What do all three cases have in common?
Findings
Case 1:
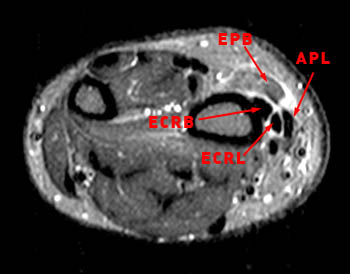
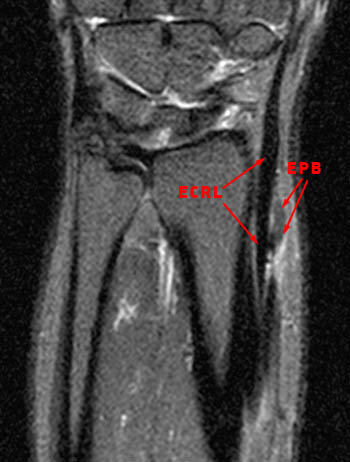
Figure 4:
The axial fat suppressed fast spin-echo T2-weighted image demonstrates peritendinous edema (arrow) around the abductor pollicis longus tendon (APL) and the myotendinous junction of the extensor pollicis brevis (EPB) of the first dorsal extensor compartment and around the extensor carpi radialis longus (ECRL) and extensor carpi radialis brevis (ECRB) tendons of the second dorsal extensor compartment at their point of intersection over the lateral radius.
Diagnosis
Intersection syndrome of the forearm.
Case 2:
Figure 6:
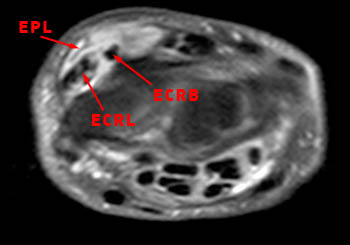
The axial inversion recovery-weighted image obtained at the level of the pisotriquetral joint shows fluid intensity signal distending the tendon sheaths of the extensor pollicis longus (EPL), extensor carpi radialis longus (ECRL) and extensor carpi radialis brevis (ECRB). Stranded hypointense material in the paratenon is consistent with synovial hypertrophy due to tenosynovitis. A skin marker has been placed by the technologist to indicate the location of the patient's palpable abnormality.
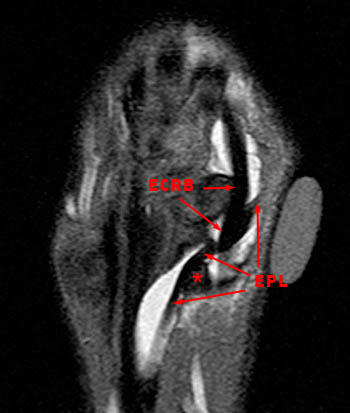
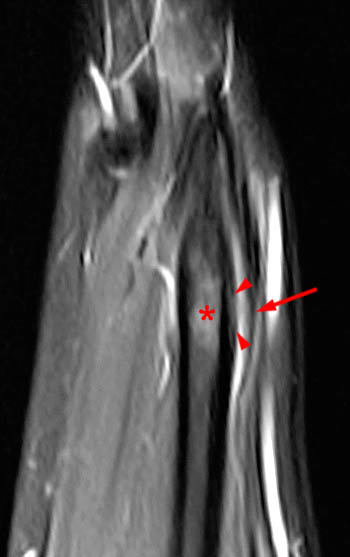
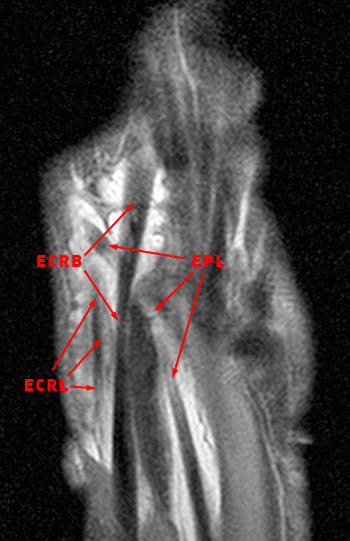
Figure 7: The coronal inversion recovery-weighted image visualizes the skin marker directly over the intersection of the extensor pollicis longus (EPL) and extensor carpi radialis brevis (ECRB). Tenosynovitis is again seen, with fluid intensity signal distending the paratenons and internal synovial hypertrophy. Note the angulation of the extensor pollicis longus tendon as it crosses Lister's tubercle (asterisk), which acts as a mechanical pulley for the tendon.
Diagnosis
Distal intersection tenosynovitis of the wrist.
Case 3:
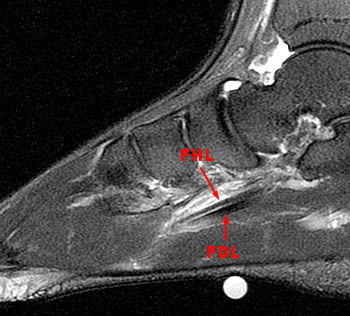
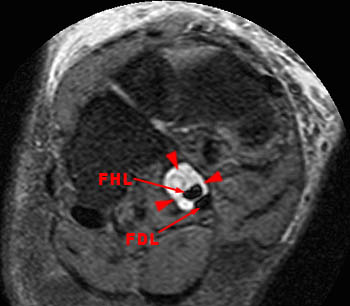
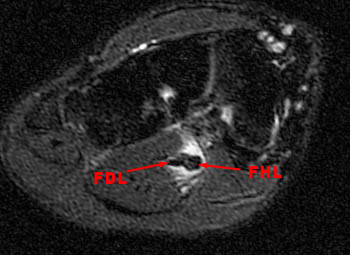
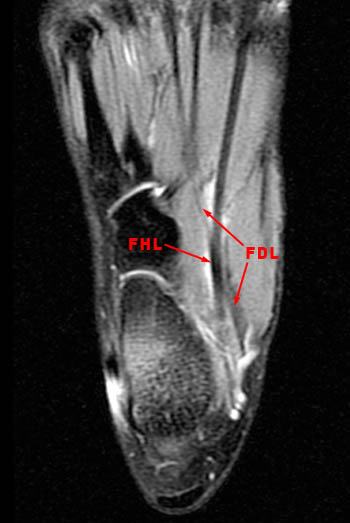
Figure 8:
A sagittal fat suppressed fast spin-echo T2-weighted image through the midfoot reveals peritendinous edema and fluid around the flexor hallucis longus at the level of the navicular and medial cuneiform. In this region, the flexor hallucis longus tendon (FHL) crosses deep to the adjacent flexor digitorum longus tendon (FDL). This intersection point is called the master knot of Henry.
Diagnosis
Flexor hallucis longus tenosynovitis at the knot of Henry.
All three cases can be categorized as tendon intersection syndromes.
INTERSECTION SYNDROME OF THE FOREARM
Forearm pain and swelling at the junction of the first and second dorsal extensor tendon compartments due to overuse was first described by Velpeau in 1841, and subsequently termed “intersection syndrome” by Dobyns et al. in 1978.1 This entity has been known by numerous other names, including “crossover syndrome” or “APL syndrome” for its anatomic location, “peritendinitis crepitans” or “squeaker’s wrist” due to audible crepitus in some patients, “oarsmen’s wrist” or “Bugaboo forearm” from associated activities, and “subcutaneous perimyositis” as a description of the pathology.2,3,4
The main abnormality is noninfectious peritendinous inflammation in the first and second dorsal extensor tendon compartments around their site of intersection, located 4 to 8 cm proximal to Lister’s tubercle. The etiology was originally thought to be due to mechanical friction between the two tendon compartments.5 In 1985, Grundberg et al. proposed stenosis of the second extensor compartment as the underlying primary abnormality, with secondary inflammation and involvement of the adjacent first compartment tendons. Surgical release of only the second extensor compartment resulted in relief of symptoms in their series.6 Subsequent research by Idler et al. suggested that the extensor fascia of the forearm may also contribute to stenosis of the tendon compartments in this region.7 The exact etiology is still unclear, and may be multifactorial.8
Most patients report activities involving repetitive flexion and extension of the wrist. Athletes performing rowing, weightlifting, skiing and racquet sports are frequently seen.9,10,11 Patients working with agricultural or digging tools have been specifically reported in the literature, along with carpenters, secretaries, and supermarket checkout clerks.12,13 Onset and tempo of the disorder is highly variable, with some patients presenting after a single ski run or a brief episode of activity.2,10 Other patients have harvested rice with hand tools for weeks before reporting symptoms.13 Severity is also variable, with most cases being mild and responsive to conservative treatment. Severe cases can lead to complications such as tendon rupture or stenosing tenosynovitis, which may require surgical intervention.13,14,15
Anatomy
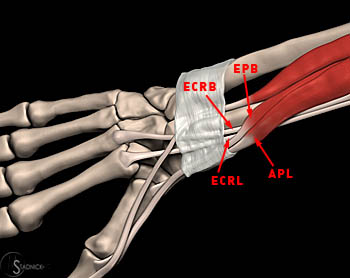
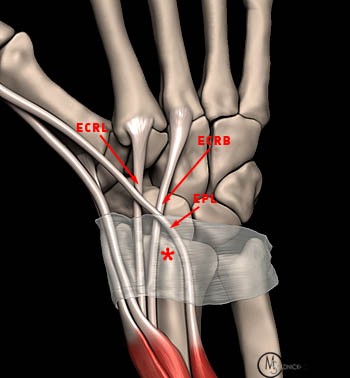
The abductor pollicis longus and extensor pollicis brevis muscles originate from the posterior radius and interosseous membrane. The tendons course in the first dorsal extensor tendon compartment toward their insertions on the thumb. The extensor carpi radialis brevis and longus originate at the lateral humeral epicondyle, and course in the second dorsal extensor tendon compartment toward their metacarpal insertions. The first compartment tendons cross over the second compartment tendons in the radial dorsal forearm, approximately 4 cm proximal to Lister’s tubercle.4,5,16 This intersection creates a mechanically disadvantageous arrangement where thumb and wrist motion results in friction between the crossing tendons.17,18
Because the crossover is located on average 4 cm proximal to the radiocarpal joint, most standard wrist MRI protocols will not include the intersection. Additional images of the forearm may be needed to evaluate this region if the clinician orders a wrist examination. Marking the area of symptoms can be useful to ensure imaging of the correct anatomic region.4,5
MR Findings
The most commonly reported MR finding in intersection syndrome is peritendinous edema and fluid around the abductor pollicis longus (APL), extensor pollicis brevis (EPB), extensor carpi radialis brevis (ECRB) and extensor carpi radialis longus (ECRL) tendons at the point of intersection. Adjacent subcutaneous edema, proximal and distal extension of peritendinous edema and fluid from the intersection are also common findings.4,5,17,18,19 (Case 12) Tendinosis, muscular edema, adjacent adventitial bursitis, ganglion cyst and periosteal edema are less commonly seen.18 (Cases 13 and 14) After intravenous contrast, enhancement is usually present in the areas of peritendinous edema, but is not particularly helpful in the diagnosis.5
12. Intersection syndrome with associated muscular edema and subcutaneous edema.
13. Ganglion cyst associated with intersection syndrome.
14. Periosteal reaction and marrow edema associated with intersection syndrome
Figure 14:
A 19 year-old female rower developed forearm pain after competition. MRI was obtained at the time of initial presentation. Axial (14a) and coronal (14b) fat-suppressed proton density-weighted images reveal peritendinous edema at the first and second compartment intersection (arrow), with adjacent periosteal reaction (arrowheads) and marrow edema (asterisk). A follow-up MRI obtained 6 months later after conservative treatment with axial (14c) and sagittal (14d) fat-suppressed proton density-weighted images shows significant decrease in peritendinous and periosteal edema, with cortical thickening due to periosteal bone formation (arrowheads).
Intersection syndrome needs to be differentiated from de Quervain’s tenosynovitis, as treatment of de Quervain’s tends to be more aggressive with earlier utilization of injections and surgery.3 Usually, the distal location of symptoms in de Quervain’s tenosynovitis is sufficient to make the correct diagnosis, but occasionally the symptoms may overlap, or both entities may be present. (Case 15) In these cases, MRI can be very helpful for accurate diagnosis. Other causes of forearm pain such as Wartenberg’s syndrome, muscle strain, or ganglion cyst can also be differentiated from intersection syndrome by MRI.5,16
15. Coexistence of intersection syndrome and de Quervain’s tenosynovitis.
Figure 15:
A 58 year old female patient reported forearm and wrist pain. MRI of the forearm with inversion recovery axial (15a) and coronal 2D GRE images (15b) demonstrate tendinosis and peritendinous edema (arrows) around the APL, EPB, ECRL and ECRB consistent with intersection syndrome. Adjacent subcutaneous edema is also present. MRI of the wrist was also obtained with axial (15c) and coronal (15d) inversion recovery-weighted images, revealing tendinosis and peritendinous edema involving the APL and EPB(arrowheads) distal to the radial styloid over the triscaphe joint, consistent with de Quervain's tenosynovitis.
Clinical Management
Initial treatment is similar to most overuse syndromes with rest and modification of activity, oral NSAIDs, ice, and splinting with the wrist in mild extension.3,14 Taping the forearm has also been reported to reduce symptoms.20
A course of oral corticosteroids and injection of a local anesthetic and corticosteroid mixture adjacent to the site of swelling may be performed in patients who do not respond to conservative treatment.3,4,14 Most patients will respond to nonoperative treatment, but some may require surgical synovectomy and decompression.15
DISTAL INTERSECTION TENOSYNOVITIS OF THE WRIST
Noninfectious tenosynovitis involving the extensor pollicis longus (EPL), extensor carpi radialis brevis (ECRB) and longus (ECRL) tendons over the wrist is less commonly reported in the literature than the classic forearm intersection syndrome. Patients present with dorsal wrist pain and swelling, sometimes after a traumatic event. Anecdotal occupational or recreational overuse in skiers and kickboxers has been reported. Symptoms may mimic those of osteoarthritis or a ganglion cyst.21,22,23 Autoimmune diseases such as rheumatoid arthritis or lupus may predispose to tendinopathy in this region, particularly involving the EPL.21,24
Severity is variable; most cases are mild and respond to conservative treatment, but some patients are much more symptomatic and may progress to a complete tear of the extensor pollicis longus. Synovectomy and tendon repair may be necessary in these cases.22
Anatomy
The EPL, ECRB and ECRL tendons intersect distal to the radiocarpal joint and Lister’s tubercle. The tubercle acts as a pulley, altering the angle of the EPL tendon so that it crosses superficially over the ECRB and ECRL. This creates a mechanically disadvantageous arrangement, where motion of the thumb and hand may cause friction between the tendons.21,22,24
Several other anatomic factors may contribute to pathology in this location. Lister’s tubercle can irritate the EPL due to mechanical friction, particularly if there has been previous fracture or deformity of the tubercle.24 The second and third extensor compartments communicate with each other in this area, allowing inflammation in one compartment to spread to the adjacent compartment. The extensor retinaculum may limit the space available around the tendons in this region, constricting the compartments and resulting in increased pressure on the tendons. Finally, the EPL tendon has a watershed vascular supply in this region, making it vulnerable to ischemia.21,22,24
MRI Findings
The main finding is peritendinous edema, fluid and distention of the tendon compartments of the EPL, ECRB and ECRL at their point of intersection. Associated findings include tendinosis with thickening and/or increased signal in the involved tendons, partial tendon tears, and reactive marrow edema in adjacent osseous structures such as Lister’s tubercle.21,22 (Cases 17 and 18) Complete tear with discontinuity of the EPL and retraction of the proximal fragment may be seen in severe cases. (Case 19) Distal intersection tenosynovitis can coexist with the more proximal forearm intersection syndrome. (Case 20) Anomalous position of the EPL lateral to Lister’s tubercle is rare, but predisposes patients to tenosynovitis.25 (Case 21)
17. Distal intersection tenosynovitis with tendinosis of the EPL and ECRB.
Figure 17:
An axial fat-suppressed proton density-weighted image at the distal intersection in a 58 year old female patient with dorsal wrist pain demonstrates thickening of the ECRB with increased intrasubstance signal in the EPL and ECRB, consistent with tendinosis. Peritendinous fluid and edema around the EPL, ECRB and ECRL indicate tenosynovitis (arrowheads).
18. Severe distal intersection tenosynovitis with partial tears of the EPL, ECRB and ECRL.
Figure 18:
Axial (18a) and coronal (18b) fat-suppressed proton density-weighted images in a 60 year old female with a palpable mass and pain over the dorsal wrist. The EPL and ECRB are attenuated, and the ECRL is thickened with internal splitting of the tendon at the intersection site. Prominent fluid signal and synovial hypertrophy are present in the tendon compartments.
19. Severe distal intersection tenosynovitis with complete tears of the EPL and ECRB.
Figure 19:
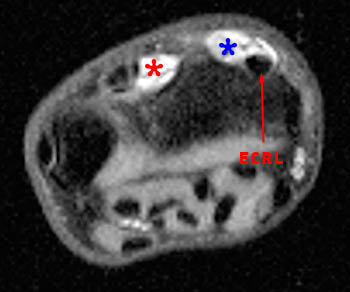
A 43 year old female presented with dorsal wrist pain and loss of thumb extension. Axial (N19a) fat-suppressed proton density-weighted image at the level of Lister's tubercle reveals absence of the EPL(red asterisk) and ECRB(blue asterisk), with fluid and synovial hypertrophy distending the compartments. A coronal (19b) fat-suppressed proton density-weighted image visualizes the retracted proximal fragment of the torn EPL tendon in the distal forearm.
20. Coexistence of forearm intersection syndrome and distal intersection tenosynovitis.
Figure 20:
A 45 year old female tennis player presented with forearm and wrist pain. Axial fat-suppressed proton density-weighted image of the forearm (20a) reveals mild peritendinous edema and subcutaneous edema (arrows) at the crossover of the first and second dorsal extensor compartments, consistent with mild intersection syndrome of the forearm. Axial fat-suppressed proton density-weighted image of the wrist (20b) obtained on the same day reveals mild fluid and edema around the EPL, ECRB and ECRL (arrows), consistent with mild distal intersection tenosynovitis.
21. Anomalous lateral position of the EPL with tenosynovitis of the EPL and ECRB.
Figure 21:
A 47 year old female patient presented with dorsal radial pain in the distal forearm and wrist. Axial and coronal fat-suppressed T2-weighted images through Lister's tubercle reveal an abnormal lateral position of the EPL tendon. At this level, the EPL should be medial to the tubercle. In this patient, the EPL tendon is located adjacent to the ECRB, with fluid and edema around the EPL and ECRB.
Clinical Management
Most cases of distal intersection tenosynovitis not related to autoimmune disease or radial fracture tend to be mild, and respond well to conservative treatment. Severe cases may progress to EPL tendon rupture and require surgical treatment.21,22,23,24 Direct EPL tendon repair is often difficult due to tendon retraction and poor quality of remaining tendon tissue. Tendon transfer or graft may be necessary in such cases.24
FLEXOR HALLUCIS LONGUS TENOSYNOVITIS AT THE KNOT OF HENRY
The flexor hallucis longus tendon has a long course from its muscular origin to the distal insertion in the great toe, with several points of anatomic vulnerability to wear and friction. Tendinopathy is most commonly seen at the tibiotalar joint as the tendon curves over the posterior talus. Distal disease at the hallux sesamoids is next most frequent, followed by the intersection of the flexor hallucis longus with the flexor digitorum longus. This intersection is known variously as the “knot of Henry”, “Henry’s knot”, or the “master knot of Henry”.26
Anatomy
The flexor hallucis longus (FHL) muscle originates from the lower fibula and interosseous membrane, lateral to the flexor digitorum longus (FDL) muscle which originates from the inferior tibia. The FDL tendon crosses superficially over the FHL in the plantar midfoot at the knot of Henry, which is usually located over the navicular and medial cuneiform in most patients. This anatomic relationship creates a mechanically disadvantageous site similar to the intersection syndromes of the upper extremity.26,27,28 A fibrous slip connects the FHL and FDL at the knot of Henry, which tends to maintain their anatomic relationship at this location.29 The tendon sheaths of the FHL and FDL usually communicate, which allows inflammation of one structure to spread to the adjacent tendon.27
Another tendon intersection site has been identified in the lower leg as the FDL crosses superficially over the posterior tibial tendon, called the chiasma crurale. However, there is no reported clinical impingement syndrome at this site, and histologic examination of cadaveric tendons at this location did not reveal significant tendon degeneration.30
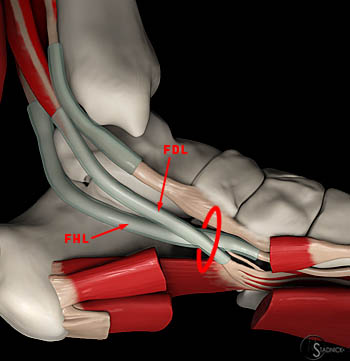
Figure 22:
Anatomic diagram showing the relationship of the FHL with adjacent structures. At the ankle, the FHL is located posterior and lateral to the FDL, between the posterior talar tuberosities. As the tendons curve under the medial malleolus and talus, they begin to converge and eventually cross at the knot of Henry (oval).
MRI Findings
MRI findings in mild cases are typical of tenosynovitis, including peritendinous fluid and edema around the FHL and FDL at the knot of Henry.26,27 (Cases 23 and 24) More severe cases may demonstrate synovial hypertrophy in the tendon sheath, outpouching of the tendon sheath, tendinosis, partial or complete tendon tears. Stenosing tenosynovitis with thickening and fibrosis of the tendon sheath can be difficult to diagnose on MRI due to relatively scant peritendinous fluid signal; tenography may be useful for diagnosis and treatment in these patients.27,28,31
23. Flexor hallucis longus tenosynovitis.
Figure 23:
A coronal fat-suppressed proton density-weighted image in a 32 year-old male patient with plantar pain. Note prominent distention of the tendon sheath with internal debris (arrowheads) at the knot of Henry at the intersection of the flexor hallucis longus (FHL) and the flexor digitorum longus (FDL) tendons.
24. Flexor hallucis longus and flexor digitorum longus tenosynovitis centered at the knot of Henry.
Figure 24:
Coronal (24a) and sagittal (24b) fat-suppressed T2-weighted images and an axial (24c) fat-suppressed proton density-weighted image in a 19 year old female track athlete with plantar foot pain reveal fluid and peritendinous edema around the FHL and FDL at the knot of Henry. Mild increased intrasubstance signal in the FHL is consistent with tendinosis.
Clinical Management
As with other overuse syndromes, mild FHL or FDL tenosynovitis is initially treated conservatively with rest and oral anti-inflammatory agents. Tenography can be diagnostic and therapeutic in persistently symptomatic patients. Injection of contrast material distends the tendon sheath and can visualize stenosis, synovial hypertrophy and outpouching. Injection of steroid and local anesthetic into the tendon sheath produces symptomatic improvement in most patients.27,28
Some cases, especially those with FHL tears and severe symptoms may require surgery. In these patients, surgical release of the knot of Henry with debridement of fibrotic tissue and tendon repair has been reported to produce symptomatic relief and functional improvement.28,32
Conclusion
Tendon intersection syndromes occur at several specific locations in the upper and lower extremities. Incidence is difficult to determine, since many cases are self-limited and may not come to clinical attention. Many patients are diagnosed based on clinical findings and treated conservatively, not requiring advanced imaging. Published reports in the radiology literature are sparse. Review of the Radsource experience over the past 8 years by keyword search revealed 38 cases of forearm intersection syndrome, 29 cases of distal intersection tenosynovitis, and 4 cases of flexor hallucis longus tenosynovitis at the knot of Henry.
MR imaging can be helpful in tendon intersection syndromes when history and physical examination are atypical or inconclusive. In some cases, intersection syndromes may coexist with other pathology which can also be diagnosed by MR. Early accurate diagnosis is important for appropriate treatment and optimal patient outcome.
References
1 Dobyns JH, Sim FH, Linscheid RL. Sports stress syndromes of the hand and wrist. Am J Sports Med. 1978 Sep-Oct;6(5):236-54.
2 Palmer DH, Lane-Larsen CL. Helicopter skiing wrist injuries. A case report of “bugaboo forearm”. Am J Sports Med. 1994 Jan-Feb;22(1):148-9.
3 Hanlon DP, Luellen JR. Intersection syndrome: a case report and review of the literature. J Emerg Med. 1999 Nov-Dec;17(6):969-71.
4 Costa CR, Morrison WB, Carrino JA. MRI features of intersection syndrome of the forearm. AJR Am J Roentgenol. 2003 Nov;181(5):1245-9.
5 de Lima JE, Kim HJ, Albertotti F, Resnick D. Intersection syndrome: MR imaging with anatomic comparison of the distal forearm. Skeletal Radiol. 2004 Nov;33(11):627-31. Epub 2004 Sep 10.
6 Grundberg AB, Reagan DS. Pathologic anatomy of the forearm: intersection syndrome. J Hand Surg Am. 1985 Mar;10(2):299-302.
7 Idler RS, Strickland JW, Creighton JJ Jr. Intersection syndrome. Indiana Med. 1990 Sep;83(9):658-9.
8 Allison DM. Pathologic anatomy of the forearm: intersection syndrome. J Hand Surg Am. 1986 Nov;11(6):913-4.
9 Tagliafico AS, Ameri P, Michaud J, Derchi LE, Sormani MP, Martinoli C. Wrist injuries in nonprofessional tennis players: relationships with different grips. Am J Sports Med. 2009 Apr;37(4):760-7. Epub 2009 Mar 6.
10 McNally E, Wilson D, Seiler S. Rowing injuries. Semin Musculoskelet Radiol. 2005 Dec;9(4):379-96.
11 Rumball JS, Lebrun CM, Di Ciacca SR, Orlando K. Rowing injuries. Sports Med. 2005;35(6):537-55.
12 Descatha A, Leproust H, Roure P, Ronan C, Roquelaure Y. Is the intersection syndrome is an occupational disease? Joint Bone Spine. 2008 May;75(3):329-31. Epub 2007 Aug 31.
13 Pantukosit S, Petchkrua W, Stiens SA. Intersection syndrome in Buriram Hospital: a 4-yr prospective study. Am J Phys Med Rehabil. 2001 Sep;80(9):656-61.
14 Servi JT. Wrist pain from overuse: detecting and relieving intersection syndrome. Phys Sportsmed. 1997 Dec;25(12):41-4.
15 Williams JG. Surgical management of traumatic non-infective tenosynovitis of the wrist extensors. J Bone Joint Surg Br. 1977 Nov;59-B(4):408-10.
16 Clavero JA, Golanó P, Fariñas O, Alomar X, Monill JM, Esplugas M. Extensor mechanism of the fingers: MR imaging-anatomic correlation. Radiographics. 2003 May-Jun;23(3):593-611.
17 Browne J, Helms CA. Intersection syndrome of the forearm. Arthritis Rheum. 2006 Jun;54(6):2038.
18 Lee RP, Hatem SF, Recht MP. Extended MRI findings of intersection syndrome. Skeletal Radiol. 2009 Feb;38(2):157-63. Epub 2008 Sep 23.
19 De Maeseneer M, Marcelis S, Jager T, Girard C, Gest T, Jamadar D. Spectrum of normal and pathologic findings in the region of the first extensor compartment of the wrist: sonographic findings and correlations with dissections. J Ultrasound Med. 2009 Jun;28(6):779-86.
20 Kaneko S, Takasaki H. Forearm pain, diagnosed as intersection syndrome, managed by taping: a case series. J Orthop Sports Phys Ther. 2011 Jul;41(7):514-9. Epub 2011 Apr 6.
21 Parellada AJ, Gopez AG, Morrison WB, Sweet S, Leinberry CF, Reiter SB, Kohn M. Distal intersection tenosynovitis of the wrist: a lesser-known extensor tendinopathy with characteristic MR imaging features. Skeletal Radiol. 2007 Mar;36(3):203-8. Epub 2006 Dec 20.
22 Cvitanic OA, Henzie GM, Adham M. Communicating foramen between the tendon sheaths of the extensor carpi radialis brevis and extensor pollicis longus muscles: imaging of cadavers and patients. AJR Am J Roentgenol. 2007 Nov;189(5):1190-7.
23 Kardashian G, Vara AD, Miller SJ, Miki RA, Jose J. Stenosing synovitis of the extensor pollicis longus tendon. J Hand Surg Am. 2011 Jun;36(6):1035-8.
24 Wheeless III CR, “Extensor Pollicis Longus Rupture”, in Wheeless’ Textbook of Orthopaedics Online, http://www.wheelessonline.com/ortho/extensor_pollicis_longus_rupture, retrieved 11 August 2012.
25 Rubin G, Wolovelsky A, Rinott M, Rozen N. Anomalous course of the extensor pollicis longus: clinical relevance. Ann Plast Surg. 2011 Nov;67(5):489-92.
26 Bencardino J, Rosenberg Z, “Radiologic Perspective: Magnetic Resonance Imaging of the Ankle”, in Pedowitz R, Chung C, Resnick D, eds., Magnetic Resonance Imaging in orthopaedic Sports Medicine, Springer, Chapter 11A, 2008.
27 Na JB, Bergman AG, Oloff LM, Beaulieu CF. The flexor hallucis longus: tenographic technique and correlation of imaging findings with surgery in 39 ankles. Radiology. 2005 Sep;236(3):974-82.
28 Lui TH, Chow FY. “Intersection syndrome” of the foot: treated by endoscopic release of master knot of Henry. Knee Surg Sports Traumatol Arthrosc. 2011 May;19(5):850-2. Epub 2011 Feb 3.
29 Coghlan BA, Clarke NM. Traumatic rupture of the flexor hallucis longus tendon in a marathon runner. Am J Sports Med. 1993 Jul-Aug;21(4):617-8.
30 Buck FM, Gheno R, Nico MA, Haghighi P, Trudell DJ, Resnick D. Chiasma crurale: intersection of the tibialis posterior and flexor digitorum longus tendons above the ankle. Magnetic resonance imaging-anatomic correlation in cadavers. Skeletal Radiol. 2010 Jun;39(6):565-73. Epub 2009 Oct 30.
31 Gelbart MS, Parikh A, Chong W, Gilula LA. A novel approach to flexor hallucis longus tenography. AJR Am J Roentgenol. 2006 Dec;187(6):1432-5.
32 Boruta PM, Beauperthuy GD. Partial tear of the flexor hallucis longus at theknot of Henry: presentation of three cases. Foot Ankle Int. 1997 Apr;18(4):243-6.