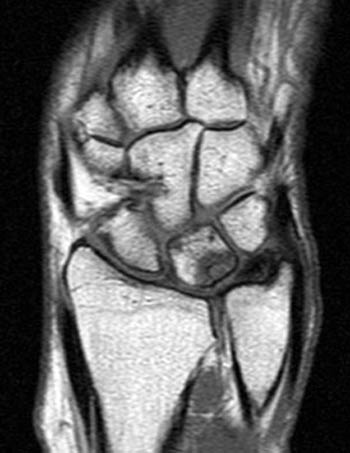
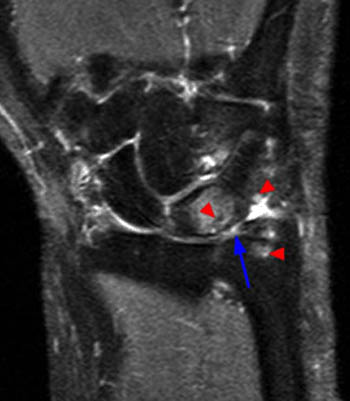
Clinical History: A 62 year old female presents with an 11 month history of ulnar sided wrist pain, swelling, and limited range of motion. (1a) Gradient echo and (1b) T1-weighted coronal images are provided. What are the findings” What is your diagnosis?
Findings
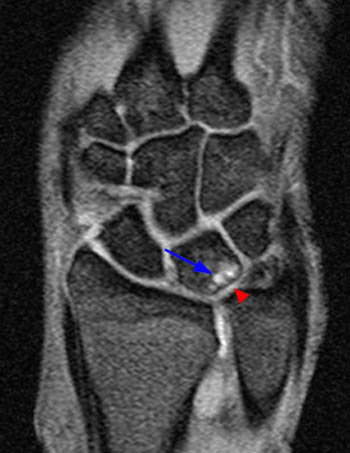
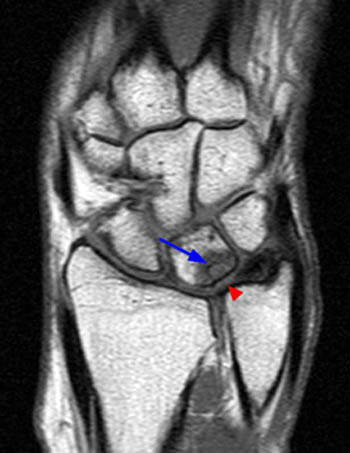
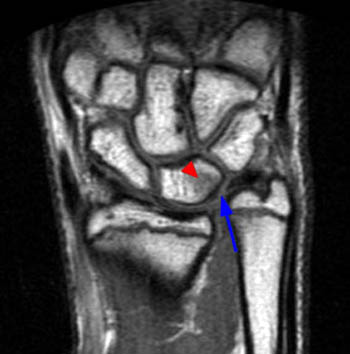
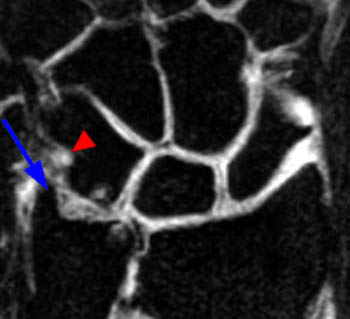
Figure 2:
(2a,2b) Both coronal images reveal chondral thinning at the ulnolunate articulation, subchondral cyst formation within the proximal aspect of the lunate (arrows), and severe attrition and degenerative perforation (arrowheads) of the membranous component of the triangular fibrocartilage.
Diagnosis
Ulnocarpal abutment
Discussion
Also known as ulnar impaction syndrome or ulnolunate abutment, ulnocarpal abutment (UCA) is a chronic degenerative condition related to repetitive loading from ulnar impaction. Affected structures include the membranous component of the triangular fibrocartilage (TFC), the ulnar head, the lunate, the triquetrum, and the lunotriquetral (LT) ligament. Predisposing factors include, but are not limited to, positive ulnar variance, malunion of the distal radius, premature closure of the distal radius, Essex-Lopresti fracture, and previous surgical resection of the radial head. Occasionally, UCA may occur in the absence of anatomic structural abnormalities, most commonly from daily activities that cause excessive ulnar carpal loading.
In patients with UCA, chronic and repetitive impaction between the ulnar head and ulnar carpus across the TFC complex produces a continuum of progressive deterioration, including central degenerative tearing of the TFC, chondromalacia of the proximal lunate, radial triquetrum, and distal ulnar head, and instability and/or ligamentous tearing at the LT articulation. Eventually, ulnocarpal osteoarthritis may also develop.
TFC lesions are classified by Palmer as I (traumatic) and type II (degenerative). The type II degenerative TFC lesions associated with UCA are subcategorized by Palmer into 5 types:
A – TFCC wear
B – TFCC wear + lunate, triquetrum osseous abnormalities, +/- ulnar chondromalacia
C – TFCC perforation + lunate, triquetrum, +/- ulnar chondromalacia
D ” TFCC perforation + lunate, triquetrum, +/- ulnar chondromalacia & LT ligament tear
E – TFCC perforation + lunate, triquetrum, +/- ulnar chondromalacia, LT perforation & ulnocarpal arthritis
This classification system is helpful not only to determine the mechanism of injury, but directing clinical management.
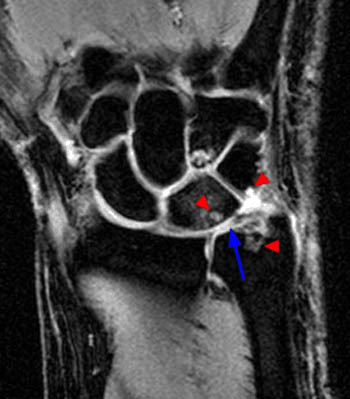
Figure 3:
(3a) Gradient echo and (3b) fat-suppressed proton density weighted coronal images of advanced UCA, demonstrating a severely degenerated TFC (arrows), subchondral edema and cyst formation involving ulnar head, lunate and triquetrum (arrowheads), severe ulnolunate chondromalacia, and disrupted LT ligament, consistent with Stage D UCA. Also note proximal hamate chondromalacia and subchondral cyst formation (short arrows), compatible with concurrent hamatolunate impingement.
Radiographic features in UCA include positive ulnar variance, lunate and +/- triquetral subchondral sclerosis, and subchondral cyst formation in the ulnar head, proximal ulnar lunate, and proximal radial triquetrum. In addition to the aforementioned radiographic findings, MRI can uncover much earlier manifestations of UCA, including subchondral edema, chondromalacia, subtle subchondral cyst formation, and LT ligament degeneration/tearing.
Figure 4:
(4a) T1-weighted and (4b) inversion recovery coronal images demonstrate positive ulnar variance, a severely thinned and perforated TFC (arrows), prominent lunate edema (arrowheads), and mild ulnolunate chondromalacia, consistent with Stage C UCA. Although a relatively advanced stage of disease, the majority of these findings would not be evident on plain radiographs.
MR arthrography may be useful in select cases of UCA to clarify the exact stage of ulnar impaction in pre-operative evaluation. Arthrography can assist in determining if full-thickness TFC perforation (Stage IIB vs. IIC) exists, and is useful to evaluate the integrity of the ulnocarpal and LT ligaments (Stage IIC vs. IID).
As a caveat, because asymptomatic TFC perforations are not uncommon, particularly in the elderly, careful correlation with clinical symptoms, which include ulnar sided wrist pain, swelling, and limited ROM, is necessary.
The differential diagnosis for UCA includes intraosseous ganglia, Kienbock disease, and ulnar styloid impaction. Kienbock disease lesions are typically more diffuse, affect the central or radial aspect of the lunate, and more often occur in isolation. Additionally, patients with Kienbock disease almost never demonstrate positive ulnar variance. Ganglion cysts typically have sharper margins, are randomly located, and are often asymptomatic. Ulnar styloid impaction is caused by an excessively long or traumatically altered ulnar styloid process repetitively impinging on the triquetrum, resulting in contusion, synovitis, chondromalacia, and subchondral cyst formation. Although a distinct entity, ulnar styloid impaction may occur in conjunction with ULA.
Figure 5:
(5a) Fat-suppressed proton density and (5b) gradient echo coronal images of a patient with ulnar styloid impaction syndrome. An elongated ulnar styloid (arrows), lunotriquetral and ulnar styloid chondromalacia, triquetral subchondral cyst formation (arrowheads), and reactive effusion/synovitis are present. Also note the macerated TFC, which is commonly associated with this entity.
Treatment of ULA is aimed at eliminating the mechanical impaction of the ulna with the TFC and ulnar carpal bones. The wafer procedure (performed both open and arthroscopically) and ulnar shortening are two methods performed to recede the ulnar head. The wafer procedure involves resection of the distal 2-3 mm of the ulnar head, while ulnar shortening is accomplished by performing an osteotomy in the distal ulnar shaft, followed by rigid fixation.
Conclusion
Ulnocarpal abutment (UCA) is a not uncommon cause of pain and limited motion at the ulnar side of the wrist. In patients with UCA, MRI provides accurate assessment of the stage of disease, and allows a specific diagnosis to be made in the majority of cases. The information provided by MRI is vital in determining the proper treatment approach in such patients.
References
1 Palmer AK, Werner FW. The triangular fibrocartilage complex of the wrist- function and anatomy. J Hand Surg 1981;6(2):153-62.
2 Palmer AK. Triangular fibrocartilage complex lesions: a classification. J Hand Surg 1989;14(4): 594-606
3 Cerezal L, del Pinal F, Faustino A. MR Imaging findings in ulnar-sided wrist impaction syndromes. Magn Reson Imaging Clin N Am 12 (2004) 281-299
4 Zlatkin MB, Rosner J. MR Imaging of Ligaments and TFCC of the Wrist. Magn Reson Imaging Clin N Am 2004; 12:301-331
5 Garcia-Elias M. Soft tissue anatomy and relationships about the distal ulna. Hand Clin 1998;14(2):165-76