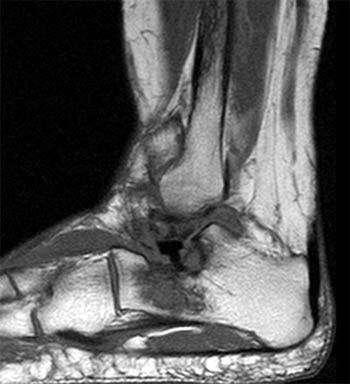
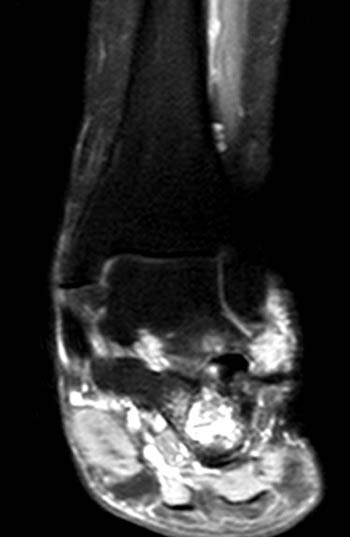
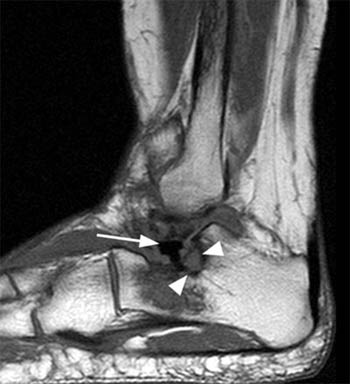
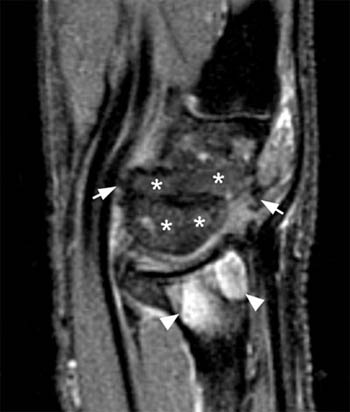
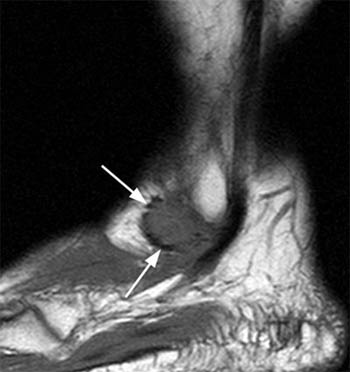
Clinical History: A 64 year-old female underwent a surgical procedure on her left ankle approximately 40 years ago. She now presents with pain and swelling. A sagittal T1-weighted image (1a) and a coronal proton-density, fat suppressed image (1b) are provided. What are the findings? What is your diagnosis?
Findings
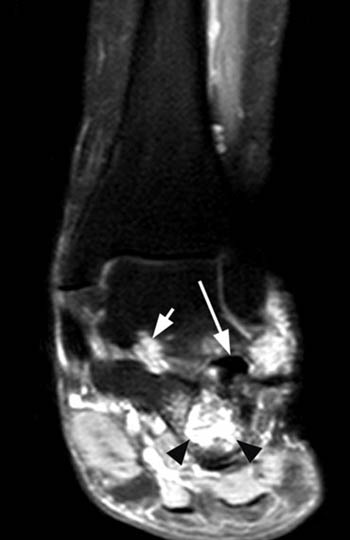
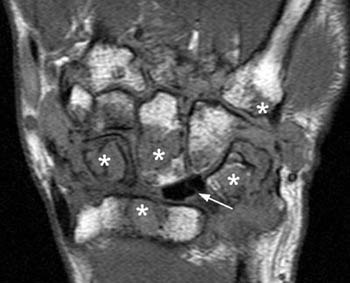
Figure 3:
(3a) The coronal proton-density fat suppressed image again shows the postoperative changes within the subtalar joint. The subtalar prosthesis (arrow) is somewhat irregular in appearance. The calcaneal erosions and subtalar synovitis are more conspicuous (arrowheads), and a small amount of synovitis is seen extending along the interosseous talocalcaneal ligament (short arrow) within the tarsal sinus.
Diagnosis
Postoperative changes in the hindfoot from arthroereisis utilizing a silastic spacer with subsequent development of silicone synovitis.
Introduction
Pes planus deformity, also known as flatfoot, refers to loss of the normal medial longitudinal arch of the foot. Pes planus in children and adults is usually flexible and on non-weight-bearing radiographs a normal arch is present. Flexible flatfoot is a common disorder, anatomically described as excessive pronation during weight bearing due to anterior and medial displacement of the talus. It may be developmental or may be acquired due to posterior tibial tendon dysfunction.
Non-operative treatments include orthotics or shoe modifications. Operative intervention, particularly for juvenile flexible flatfoot, is considered only after appropriate non-operative interventions have failed to relieve associated symptoms. Subtalar arthroereisis (also referred to as arthrorisis) has been utilized as a surgical treatment of pes planus. This procedure is most often performed on young children and is designed to correct excessive talar displacement and calcaneal eversion by placing an implant in the sinus tarsi. The subtalar implant acts as a spacer to block the anterior and inferior displacement of the talus, thus allowing normal subtalar joint motion but blocking excessive pronation and the resulting sequelae. In young children, insertion of the implant is frequently offered as a stand alone procedure, while older children and adults often require adjunctive surgical procedures on bone and soft tissue to correct additional deformities. Possible complications include peroneal spastic flatfoot, pain, locking or stiffness of the subtalar joint and foreign body reaction. Surgical alternatives to arthroereisis include tendon reconstruction or transfer, calcaneal osteotomy and arthrodesis, with the best results reported when a combination of these procedures is performed.1
History and Pathophysiology
The use of silicone elastomer implants was pioneered by Alfred B Swanson, MD in the 1960’s. Over the years, the techniques and implants have been refined and have improved the lives and restored function to countless patients. Indications for use include degenerative joint disease, rheumatoid arthritis, osteonecrosis of the scaphoid bone, and osteonecrosis of the lunate bone.2 Initially considered inert, long-term studies have demonstrated that the prostheses become encapsulated by a thin mesothelial lining.3
Most cases of silicone synovitis are related to carpal implants3 as opposed to implants at the interphalangeal or metacarpophalangeal joints. Small particulates of the silicone elastomer (10 – 100 microns), not the implant itself, are responsible for the synovial hypertrophy. In 1985, Swanson reported the occurrence of particulate synovitis and lytic bone changes around certain articulating silicone implants due to overloading, abrasion, and macrophage reactivity to wear debris.2 A research study to analyze particle-induced reactions from metals, plastics, and elastomers showed that wear debris and phagocytosis are the key events in the etiology of particulate synovitis. Scanning electron microscopy confirms that the surface of the prosthesis is coated with particulate matter thought to be the result of wear.4 Greater compression and shear forces, such as those sustained by carpal implants, is thought to increase the risk of this complication and its accompanying synovitis. The so-called “cement disease” associated with total knee and hip procedures has also been recognized as a particulate problem. It should be noted that the term “silicone synovitis”, while in common use, is a misnomer since the reactions are not generated by silicone, which is very well tolerated, but by silicone wear debris.
Clinical Presentation
The interval between surgical implantation and the complication of synovitis varies between 1 and 9 years with a mean of 5.5 years.4 Patients present with local pain and swelling. In one reported study, radiographic evidence of silicone synovitis was reported in 75% of scaphoid implants and 55% of lunate implants. The authors also reported the incidence of painful synovitis associated with scaphoid or lunate implants to be 30%.5 Physical examination reveals either loss of range of motion or, at the opposite end of the spectrum, subluxation of the prosthesis.
Radiographic changes are characteristic. They include nodular soft tissue swelling and well-defined subchondral “cysts” with the absence of articular cartilage loss. The cysts vary in size from 5 to 15mm and often have a thin sclerotic margin.4 It has been reported that these cysts increase in number and size over time. The prosthesis is often fractured, deformed, or obviously loosened with a wide lucent prosthesis-bone interface. The radiographic differential diagnosis includes other entities with rapidly expanding cysts and articular cartilage preservation such as amyloid arthropathy. The relatively normal articular cartilage helps differentiate silicone synovitis from infection.
Pathologic examination reveals intracellular and extracellular silicone particles. Silicone particles have been found in bone marrow sites remote from the implant. The particles can also be transported to regional lymph nodes and cause adenopathy.6
MR Appearance
Although routine radiographs generally are sufficient for correct diagnosis of silicone synovitis, MR imaging findings may be helpful in the diagnosis of silicone synovitis in selected patients. MR may be most useful in excluding other diagnoses or differentiating the lesions of silicone synovitis from degenerative cysts. In patients with suspected osteomyelitis, MR may help guide needle aspiration or biopsy for definitive diagnosis. MR is also of benefit in evaluating the articular cartilage in cases where proximal row carpectomy or limited arthrodesis is considered following implant removal.
As on radiographs, MR images will often demonstrate fracture, fragmentation, or subluxation of the prosthesis. The silicone elastomer used presents as a signal void on all pulse sequences (4a,5a).
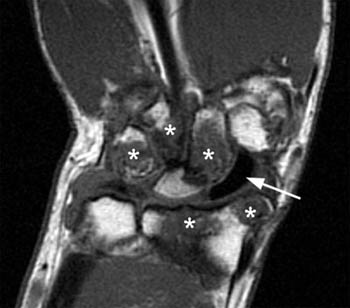
Figure 4:
(4a) Coronal T1-weighted image in a 58 year-old male 20 years following lunate arthroplasty. The lunate implant presents as a central signal void. A small fracture extends through the prosthesis (arrow) and the proximal margin of the prosthesis is somewhat irregular in appearance. Multiple intermediate signal cysts are seen throughout the carpus (asterisks).
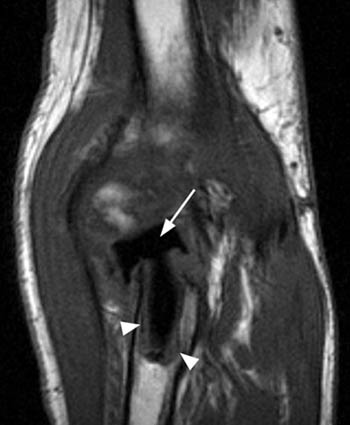
Figure 5:
(5a) A T1-weighted coronal image from a 71 year-old male elbow. A radial head prosthesis is seen as a signal void (arrow) within the proximal radius. The prosthesis is abnormally angulated without a definite fracture identified. The prosthesis-bone interface is enlarged (arrowheads), consistent with prosthesis loosening.
The cysts in patients with silicone synovitis are filled with hypertrophic synovium, not fluid like typical degenerative cysts. The signal intensity observed on MR images will reflect this pathology and the cysts will be of intermediate signal on T1 and T2-weighted images. In the first study to report MR imaging findings, the authors reported intermediate intensity to mild hyperintensity on proton-density and T2-weighted images in all patients.5 (Figures 6a,7a,8a) They also observed deformity or fracture of the prosthesis in all patients. In addition, all patients showed hypointense foci on all sequences felt to represent silicone fragments or fibrotic reaction. (Figures 8a and 9a)
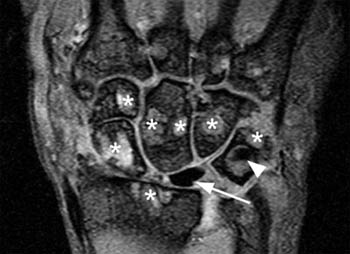
Figure 6:
(6a) A gradient-echo image in the same patient as (4a) at a slightly different location. The proximal margin of the prosthesis is irregular(arrow). A small linear signal void in the triquetral bone(arrowhead) represents the fractured fixation peg of the lunate prosthesis. Again, multiple carpal cysts are seen which are predominantly of intermediate signal intensity (asterisks).
Figure 8:
(8a) Same patient as Figure 7. Sagittal fat-suppressed proton-density weighted image. Extensive cyst formation in the capitate and lunate bones (asterisks) is of intermediate signal intensity. The subchondral cysts within the distal radius (arrowheads) are of high signal and may reflect degenerative cysts due to secondary osteoarthrosis. Small foci of low signal at the dorsal and volar aspects of the wrist (small arrows) may reflect debris or fragments from the prosthesis.
Figure 9:
(9a) A sagittal T1-weighted image from the same patient as images 1a and 1b, obtained at the lateral margin of the joint. The distal fibula and peroneal tendons are seen, as is the fifth metatarsal base. A region of synovitis anterior to the distal fibula has peripheral foci of low signal intensity (arrows) which may represent fragments of the subtalar prosthesis.
Treatment
It is generally believed that removal of the silastic implant will stop the progression of the disease. The synovitis is typically debrided with the larger cysts requiring bone grafting. However, removal of the implant and debridement of the cysts may not necessarily improve the patients” pain and limitation of motion. In a recent study comparing patients with silicone synovitis treated non-operatively with those treated operatively, the authors could not detect a significant difference between the two groups with respect to pain, limitation of motion, difficulty with activities of daily living, grip strength, or the total range of motion of the wrist. There was no significant difference between the two groups with regard to the age at the time of the initial procedure, the time to the diagnosis of the synovitis, and the duration of follow-up after treatment. There was no clear advantage to removal of the implant and d?bridement with or without arthrodesis of the wrist or other reconstructive procedures.7 Therefore, caution is recommended when selecting a surgical reconstruction procedure for the treatment of a patient with silicone synovitis.
Conclusion
Silicone synovitis is a form of particle disease related to wear particles or debris from silicone elastomer joint implants. The process is mediated by macrophages and results in a characteristic synovial hypertrophy with the formation of intraosseous cysts and the relative preservation of articular cartilage. In such cases, MR allows the correct diagnosis to be made, and the extent of joint involvement is readily assessed.
References
1 Morrison WB, Elias I, Zoga AC, Raikin, SM: Imaging Appearance of Arthroereisis in Severe Planovalgus Feet. Abstracts of the Society of Skeletal Radiology. Meeting held in Orlando Florida, 13-16 March 2005.
2 Swanson, AB, DeGroot Swanson G, Watermeier JJ: Arthroplasty of the thumb basal joints. Clin Orthop Rel Res 195:151, 1985.
3 Bogoch ER: Silicone Synovitis. J Rheumatol 14:1086, 9187.
4 Goldman AB, Bansal M. Amyloidosis and silicone synovitis. Radiol Clin North Am 1996; 34:375-394.
5 Chan M, Chowchuen P, Workman T, Eilenberg S, Schweitzer M, Resnick D. Silicone Synovitis: MR Imaging in five patients. Skeletal Radiol 1998 27:13-17.
6 Weissmn BN Imaging of Joint Replacement. In Diagnosis of Bone and Joint Dosorders Fourth Ed. Resnick D. W. B. Saunders 2002.
7 Murry PM, Wood MB. The results of treatment of synovitis of the wrist induced by particles of silicone debris. JBJS Am 1998 80:(3)397-406.